Professional Documents
Culture Documents
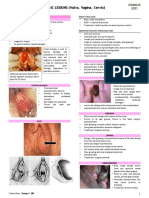
A 35-Year-Old Carpenter With Peripheral Neuropathy and Skin Lesions
Uploaded by
nabila auliaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
A 35-Year-Old Carpenter With Peripheral Neuropathy and Skin Lesions
Uploaded by
nabila auliaCopyright:
Available Formats
1.
Case Study 1
A 35-year-old carpenter with peripheral neuropathy and skin lesions
A 35-year-old, fair-skinned male is referred to your clinic for evaluation. His symptoms began
approximately 3 months ago, with the insidious onset of numbness and tingling in his toes and
fingertips, progressing slowly in the ensuing weeks to involve the feet and hands in a symmetric
“stocking-glove” fashion. In the past 2 to 3 weeks, the tingling has taken on a progressively
painful, burning quality and he has noted weakness in gripping tools. No ataxia, dysphagia,
visual symptoms, or bowel or bladder incontinence have been noted, and he has not complained
of headaches, back or neck pain, or confusion. Except as noted, the review of systems is
otherwise negative.
The patient’s medical history is remarkable for a flu-like illness approximately 4 months ago
characterized by 3 to 4 days of fever, cough, diarrhea, and myalgias, which resolved
spontaneously. Further questioning reveals the patient has been a carpenter since completing
high school 17 years ago. For the last 10 years, he has lived in a rural, wooded area in a home he
built. Approximately 10 months ago he was married and moved with his wife, an elementary
school teacher, into a newly built home on an adjacent parcel of land. The patient consumes one
to two alcoholic drinks a week, and quit smoking 2 years ago after a 15-pack-year history. He
takes one multivitamin a day but no prescription medications. Family history is unremarkable;
his wife, parents, and two younger brothers are in good health.
Neurologic examination reveals diminished proprioception in the hands and feet, with a
hyperesthetic response to pinprick sensation on the soles. Motor bulk and tone are normal, but
there is slight bilateral muscular weakness in dorsiflexors of the toes and ankles, wrist extensors,
and hand intrinsics. Reflexes are absent at the ankles and 1+ at the biceps and knees.
Coordination and cranial nerve function are within normal limits. Dermatologic examination
reveals brown patches of hyperpigmentation, with scattered overlying pale spots in and around
the axillae, groin, nipples, and neck. The palms and soles show multiple hyperkeratotic corn-like
elevations 4 to 10 mm in diameter. Three irregularly shaped, sharply demarcated, erythematous,
scaly plaques, measuring 2 to 3 cm, are noted on the patient’s torso. The remainder of the
physical examination is normal.
On initial laboratory evaluation, the CBC shows slight macrocytic anemia with hematocrit 35%
(normal range 40% to 52%), and MCV 111 fL (normal range 80 to 100 fL). White blood cell
count is 4.3×103/mm3 (normal range 3.9 to 11.7×103/mm3); the differential reveals moderate
elevation of eosinophils at 9% (normal range 0% to 4%). Occasional basophilic stippling is noted
on the peripheral smear. Liver transaminases are slightly elevated. BUN, creatinine, and
urinalysis are normal.
(a) What problem list is suggested for this patient?
_________________________________________________________________
(b) What further investigations would you undertake at this time?
_________________________________________________________________
(c) What treatment options would you consider?
_________________________________________________
2. Case Study 2
Low back pain and waddling gait in a 60-year-old woman
A 60-year-old woman comes to your office with complaints of low back pain, which is causing
progressive difficulty in walking. The pain has gradually increased since the onset of menopause
5 years ago. This discomfort is especially noticeable after prolonged sitting.
Social history reveals that the patient has been a housewife since her marriage 38 years ago. Her
husband, who is in good health, owns and operates a small retail shop in their home. The patient
has been making jewelry for sale in her husband’s shop and as a hobby for about 35 years. They
have two adult sons who are in good health.
The patient denies a personal or family history of kidney disease, hypertension, diabetes mellitus,
or cardiovascular disease; she also denies history of back trauma or weight loss. She has smoked
one to two packs of cigarettes a day for the past 40 years. She does not take estrogens, calcium
supplements, vitamins, or other medications.
On examination you find a thin female with a slightly stooped posture and a waddling gait.
Blood pressure is 120/70. Her teeth have a yellow discoloration above the crown, and her
fingernails are stained with nicotine. She is anosmic on cranial nerve examination. Results of
cardiovascular and abdominal examination are normal. The lower lumbar spine is tender to
percussion, but the patient does not complain of pain on straight leg raising. Her deep tendon
reflexes are intact, and the remainder of the physical examination, including neurologic testing,
is normal. Sensation and strength are normal in legs and feet. Range of motion is normal in hips
and knees.
Initial laboratory data include a urinalysis showing 3+ proteinuria and glycosuria. BUN,
creatinine, and albumin levels are normal. Roentgenograms of the pelvis and lumbosacral spine
reveal pseudofractures and other evidence of severe osteomalacia and mild osteoporosis. There
are no osteolytic or osteoblastic lesions.
(a) What should be included on the patient’s problem list?
_________________________________________________________________
(b) What additional information would be helpful in diagnosing this woman’s condition?
_________________________________________________________________
(c) What further tests, if any, would you recommend?
_________________________________________________________________
(d) What treatment would be appropriate for this patient?
__________________________________________________
3. Case Study 3
A hyperactive 5-year-old with disturbed hearing and hypochromic anemia
A 5-year-old boy is brought to your office by his mother, who is concerned that her child is
hyperactive. At a parent-teacher conference last week, the kindergarten teacher said that the boy
seems impulsive and has trouble concentrating, and recommended evaluation by a physician as
well as by the school psychologist. The mother states that he has always seemed restless and
easily distracted, but that these first 6 months in kindergarten have been especially trying.
Family history reveals that the boy lives with his sister, mother, and maternal grandparents in an
older suburb of your community. The child’s monthly weekend visits to his father’s house are
working out fine. However, he seems to be fighting more with his sister, who has an attention-
deficit disorder and is repeating first grade. Since the mother moved in with her parents after her
divorce 4 years ago, she has worked with the grandfather in an automobile radiator repair shop,
where her children often come to play after school. She was just laid off, however, and expressed
worry about increasing financial dependence on her parents. She also worries that the
grandfather, who has gout and complains increasingly of abdominal pain, may become even
more irritable when he learns that she is pregnant. Her third child is due in 4 months.
On chart review, you see that the boy was last seen in your clinic for his preschool physical 1
year ago, results of which were normal. A note describes a very active 4-year-old who could
dress himself without help but could not correctly name the primary colors. His vision was
normal, but hearing acuity was below normal, and speech and language were slightly delayed.
Immunizations are up to date.
Further history on that visit indicated adequate diet, with no previous pica. Spun hematocrit was
diminished at 30%. Peripheral blood smear showed hypochromia and microcytosis. There was
no evidence of blood loss, and stool examination was negative for occult blood. The diagnosis
was “mild iron deficiency anemia,” and iron therapy was prescribed. The family failed to keep
several follow-up appointments, but the child did apparently complete the prescribed 3-month
course of iron supplements. He receives no medications at this time and has no known allergies.
On physical examination today, you note that the boy is in the tenth percentile for height and
weight. His attention span is very short, making him appear restless, and he has difficulty
following simple instructions. Except for language and social skills, he has reached most
important developmental milestones.
(a) What should be included in this boy’s problem list?
_________________________________________________________________
(b) List several possible causes for the anemia.
_________________________________________________________________
(c) What tests would you order to confirm or rule out your diagnosis?
_____________________________________________________
4. Case Study 4
A 3-year-old boy with irritability, digital erythema, and leg pain
A 3-year-old boy is brought to your office by his parents, who state that the child refuses to play
and prefers to lie on his bed. His parents note that about a month ago, he seemed to withdraw and
become cranky. Recently, he has experienced night sweats. On those nights the child has felt
warm, but his parents did not take his temperature. The child has had no other symptoms, such as
a runny nose or cough, and has not lost weight.
History reveals that the patient had recurring ear infections this past winter, which were treated
with oral antibiotics. His growth and development have been normal; he is in the 90th percentile
for weight and height. The child’s immunizations are up to date, and he is on no medications.
During physical examination, the boy is uncooperative and crying. He refuses to walk or stand
and says that his legs “hurt.” He is afebrile, has a heart rate of 130 per minute and respirations of
16 per minute. He is sweating, and his nose, fingers, and toes are erythematous; the skin on his
fingers and toes is peeling. The oral pharynx and abdomen appear normal upon examination; his
lungs are clear. He does not have point tenderness in his legs, and he has full range of motion in
knees and hips. His ankles are not edematous. Results of the neurologic examination are normal;
there is no muscular atrophy. Other findings are unremarkable.
Three months ago, the child, his parents, and his 6-year-old sister moved into a freshly painted
house. The parents report that their daughter appears healthy and is doing well in first grade.
Both parents are school teachers in good health. The family has no pets and has not traveled
within the past year. Until recently, the boy has enjoyed most social activities with his family.
(a) What should be included on the patient’s problem list?
_________________________________________________________________
(b) What is the differential diagnosis for this patient?
_________________________________________________________________
(c) What tests would you recommend to confirm or rule out a diagnosis?
_________________________________________________________________
(d) What treatment and follow-up would you recommend?
__________________________________________________
You might also like
- American Board of Family MedicineDocument66 pagesAmerican Board of Family MedicineEhab Elkady100% (3)
- Case Study AnemiaaaaDocument40 pagesCase Study Anemiaaaageniziz rafaelNo ratings yet
- Case For Small Group Discussion For StudentsDocument4 pagesCase For Small Group Discussion For StudentsMuhmd shiyas.HNo ratings yet
- Trabalho de Inglês - Caso ClínicoDocument3 pagesTrabalho de Inglês - Caso ClínicoFabriti SokolowskiNo ratings yet
- USMLE Step 1: Integrated Vignettes: Must-know, high-yield reviewFrom EverandUSMLE Step 1: Integrated Vignettes: Must-know, high-yield reviewRating: 4.5 out of 5 stars4.5/5 (7)
- College of Health Sciences: INTRUCTIONS: Use The Information Checklist Below To Collect Subjective and Objective DataDocument4 pagesCollege of Health Sciences: INTRUCTIONS: Use The Information Checklist Below To Collect Subjective and Objective DataNICOLE ANNE PENTECOSTESNo ratings yet
- Acalculous Cholecystitis CaseDocument35 pagesAcalculous Cholecystitis CaseSaada Enok MedtamakNo ratings yet
- Case 1Document3 pagesCase 1איתי עוזרNo ratings yet
- NBME Syllabus For All Exams W QuestionsDocument143 pagesNBME Syllabus For All Exams W QuestionsНваневу СильванусNo ratings yet
- Subject Examinations: Content Outlines and Sample ItemsDocument147 pagesSubject Examinations: Content Outlines and Sample ItemscpopperpenguinNo ratings yet
- All CasesDocument32 pagesAll CasesMona NasrNo ratings yet
- NBME Shelf Samples Step 2Document144 pagesNBME Shelf Samples Step 2William Blair100% (5)
- Sample Questions For Emstrex 2012Document6 pagesSample Questions For Emstrex 2012Dr.2020100% (1)
- Model Paper 4Document22 pagesModel Paper 4Mobin Ur Rehman KhanNo ratings yet
- Mccee Sae 5Document45 pagesMccee Sae 5Karthikeyan GanapathyNo ratings yet
- A Case Study On Obstructive JaundiceDocument84 pagesA Case Study On Obstructive JaundiceMonna Llee Monte DimarananNo ratings yet
- Pediatric Care PlanDocument13 pagesPediatric Care PlanAlyssa Van VarkNo ratings yet
- MBChB Year 4 & 5 Past Papers + AnswersDocument170 pagesMBChB Year 4 & 5 Past Papers + AnswersHariharan NarendranNo ratings yet
- Full download Test Bank For Bates Guide To Physical Examination And History Taking 11Th Edition Bickley pdfDocument40 pagesFull download Test Bank For Bates Guide To Physical Examination And History Taking 11Th Edition Bickley pdfryan.owens420100% (13)
- NBME 10 Unsolved QuestionsDocument88 pagesNBME 10 Unsolved QuestionsMisbah Kaleem100% (3)
- MCQ2 QuestionDocument100 pagesMCQ2 Question9hjk6wpxyfNo ratings yet
- Pedia With LeukemiaDocument14 pagesPedia With LeukemiaAlynna ValbuenaNo ratings yet
- Elderly Man With Alzheimer's Presented To ER With Fever, Respiratory DistressDocument7 pagesElderly Man With Alzheimer's Presented To ER With Fever, Respiratory DistressDr Sumant SharmaNo ratings yet
- Essential Medical Disorders of the Stomach and Small Intestine: A Clinical CasebookFrom EverandEssential Medical Disorders of the Stomach and Small Intestine: A Clinical CasebookNo ratings yet
- Posting ElectiveDocument7 pagesPosting ElectiveThulasi tootsieNo ratings yet
- 3rd Year Precept Pedia Case 4 HydroceleDocument4 pages3rd Year Precept Pedia Case 4 Hydrocelekristel_nicole18yaho100% (1)
- NBME Sample QuestionsDocument144 pagesNBME Sample QuestionsYear Tentacle100% (3)
- Ppe (2016-2017) #31Document23 pagesPpe (2016-2017) #31باقر كاظم عبد الشريفNo ratings yet
- Groups ABCD - Family Medicine End Block QuestionsDocument10 pagesGroups ABCD - Family Medicine End Block QuestionsHisham ChomanyNo ratings yet
- Surg Week 4Document75 pagesSurg Week 4Casey YanoNo ratings yet
- Step 3 Form 3 CorrectedDocument41 pagesStep 3 Form 3 CorrectedSBG BPT100% (2)
- Cases Scenario (Question)Document13 pagesCases Scenario (Question)elavarkuzhali2019No ratings yet
- Infectious Disases Paper Case For StudentsDocument2 pagesInfectious Disases Paper Case For StudentsLINDSLEY GONo ratings yet
- Chronic Diseases - Lymes, Hpv, Hsv Mis-Diagnosis and Mistreatment: A New Approach to the EpidemicFrom EverandChronic Diseases - Lymes, Hpv, Hsv Mis-Diagnosis and Mistreatment: A New Approach to the EpidemicRating: 5 out of 5 stars5/5 (1)
- CaseDocument4 pagesCaseCamille Ann Robante CastilloNo ratings yet
- GI Case Studies-StudentDocument7 pagesGI Case Studies-StudentRhina FutrellNo ratings yet
- Medicine OSCEDocument21 pagesMedicine OSCEAakash KsNo ratings yet
- Case Study - OTITIS MEDIADocument9 pagesCase Study - OTITIS MEDIAHasing Amado100% (1)
- PEDIA Case 4.1. Dengue FeverDocument10 pagesPEDIA Case 4.1. Dengue Feverotartil_nimanNo ratings yet
- Integration of Osteopathic Findings into Item WritingDocument9 pagesIntegration of Osteopathic Findings into Item WritingBethNo ratings yet
- Group C Clinical Case Study Diabetic Foot InfectionDocument4 pagesGroup C Clinical Case Study Diabetic Foot InfectionHari EshwaranNo ratings yet
- FNP 3 - JiaDocument16 pagesFNP 3 - Jiaapi-551073862100% (1)
- Case Scenario 1 For StudentsDocument9 pagesCase Scenario 1 For StudentsPrince DetallaNo ratings yet
- CARDIOVASCULAR QUIZDocument2 pagesCARDIOVASCULAR QUIZmichelleNo ratings yet
- Cardiac Care PlanDocument6 pagesCardiac Care PlanMelanie DuttonNo ratings yet
- Aplastic AnemiaDocument26 pagesAplastic AnemiaMark Anthony S. Castillo100% (1)
- MED4000Document28 pagesMED4000eunice_lee_48No ratings yet
- PCOS Patient with FatigueDocument9 pagesPCOS Patient with FatiguelorrainebarandonNo ratings yet
- LIVER CIRRHOSIS CASE STUDYDocument18 pagesLIVER CIRRHOSIS CASE STUDYJerome GonezNo ratings yet
- Paediatric Gastroenteritis Case StudiesDocument3 pagesPaediatric Gastroenteritis Case StudiesJohnrey DadorNo ratings yet
- High Yield ReviewDocument8 pagesHigh Yield ReviewfrabziNo ratings yet
- Cirrhosis Case For PrintingDocument12 pagesCirrhosis Case For PrintingSean Mercado100% (1)
- Acute Cholecystitis CaseDocument16 pagesAcute Cholecystitis CaseZharif Fikri100% (3)
- The Primary Patient Assessment Form Date Patient Nationality Chief Complaint HPIDocument6 pagesThe Primary Patient Assessment Form Date Patient Nationality Chief Complaint HPIViviaNo ratings yet
- Mentalt Health 6-116Document16 pagesMentalt Health 6-116Osama NasrNo ratings yet
- Hazing Aging: How Capillary Endothelia Control Inflammation and AgingFrom EverandHazing Aging: How Capillary Endothelia Control Inflammation and AgingNo ratings yet
- At the Precipice: My Three-Year Journey from Stroke to Good Health with Type 2 DiabetesFrom EverandAt the Precipice: My Three-Year Journey from Stroke to Good Health with Type 2 DiabetesNo ratings yet
- Kelompok 1 - TacrolimusDocument13 pagesKelompok 1 - Tacrolimusnabila auliaNo ratings yet
- Kelompok 1Document8 pagesKelompok 1nabila auliaNo ratings yet
- Doxfxka VD (Ka K) : 0 - Ke - Tmaks - Ka - Tmaks ODocument2 pagesDoxfxka VD (Ka K) : 0 - Ke - Tmaks - Ka - Tmaks Onabila auliaNo ratings yet
- Nabila Aulia - Tugas KwuDocument1 pageNabila Aulia - Tugas Kwunabila auliaNo ratings yet
- TDM UtsDocument285 pagesTDM Utsnabila auliaNo ratings yet
- Alcoholic Liver Disease, Case StudyDocument2 pagesAlcoholic Liver Disease, Case Studynabila auliaNo ratings yet
- Citation-339216541 RisDocument1 pageCitation-339216541 Risnabila auliaNo ratings yet
- Perhitungan Keracunan PestisidaDocument1 pagePerhitungan Keracunan Pestisidanabila auliaNo ratings yet
- Output Kasus I (Ral) : Tests of NormalityDocument4 pagesOutput Kasus I (Ral) : Tests of Normalitynabila auliaNo ratings yet
- List Bahan Eksipien CrosslinkerDocument1 pageList Bahan Eksipien Crosslinkernabila auliaNo ratings yet
- Output Kasus I (Ral) : Tests of NormalityDocument4 pagesOutput Kasus I (Ral) : Tests of Normalitynabila auliaNo ratings yet
- List Bahan Eksipien CrosslinkerDocument1 pageList Bahan Eksipien Crosslinkernabila auliaNo ratings yet
- Diagnosis, Treatment, and Prevention of Adenovirus Infection - UpToDateDocument28 pagesDiagnosis, Treatment, and Prevention of Adenovirus Infection - UpToDateMisael TaverasNo ratings yet
- Liquid Oxygen MSdsDocument8 pagesLiquid Oxygen MSdssalcabesNo ratings yet
- Aortic StenosisDocument3 pagesAortic StenosisZweNo ratings yet
- Handbook of Burns 2012Document485 pagesHandbook of Burns 2012angella elfNo ratings yet
- Problem Sheet Agr244 - Muhammad Alif Bin Azizan - 2021469618Document3 pagesProblem Sheet Agr244 - Muhammad Alif Bin Azizan - 2021469618szkipper 03100% (1)
- Indispensable Companion To Dr. Pagano's: Praise For Dr. John's Healing Psoriasis Cookbook "This Valuable Cookbook Is TheDocument12 pagesIndispensable Companion To Dr. Pagano's: Praise For Dr. John's Healing Psoriasis Cookbook "This Valuable Cookbook Is TheСергей ОлейникNo ratings yet
- Effects of EstrogenDocument10 pagesEffects of Estrogenapi-547359341No ratings yet
- Mathematical Models in Epidemiology: by Peeyush ChandraDocument50 pagesMathematical Models in Epidemiology: by Peeyush ChandraSachin R10C08No ratings yet
- 100 MCQs Public Health Entrance ExamDocument33 pages100 MCQs Public Health Entrance ExamBijay kumar kushwaha50% (8)
- Gyne - Benign LesionsDocument4 pagesGyne - Benign LesionsIsabel CastilloNo ratings yet
- Selena Gomez - A Description of The CharacterDocument9 pagesSelena Gomez - A Description of The CharacterMarjanaNo ratings yet
- Glaucoma Management and Target IOPDocument24 pagesGlaucoma Management and Target IOPElfi RisalmaNo ratings yet
- Localización en Neurología ClínicaDocument1 pageLocalización en Neurología ClínicaDanielGiraldoNo ratings yet
- Analysis of Turmeric (Curcuma Longa) Tea As A Weight Loss AgentDocument35 pagesAnalysis of Turmeric (Curcuma Longa) Tea As A Weight Loss Agentairrahn25No ratings yet
- B.8 Situation - Care of Client With Problems in OxygenationDocument11 pagesB.8 Situation - Care of Client With Problems in OxygenationSOLEIL LOUISE LACSON MARBASNo ratings yet
- How To Give An Astrological Health ReadingDocument196 pagesHow To Give An Astrological Health Readingalex100% (9)
- v4 A7 Tudor-Costinel Serban IchtyosisDocument3 pagesv4 A7 Tudor-Costinel Serban IchtyosisMinnossNo ratings yet
- UI-RADS (Uterus Imaging Reporting and Data System) : April 2019Document3 pagesUI-RADS (Uterus Imaging Reporting and Data System) : April 2019Jenniffer FlorenciaNo ratings yet
- Reflective Essay For CSDocument2 pagesReflective Essay For CScammel ramos100% (1)
- WatermelonDocument27 pagesWatermelonSunny Mae T PuigNo ratings yet
- Reiki For Depression and Anxiety (Review) : Joyce J, Herbison GPDocument36 pagesReiki For Depression and Anxiety (Review) : Joyce J, Herbison GPHenry CogoNo ratings yet
- Petitioner vs. vs. Respondent: Second DivisionDocument8 pagesPetitioner vs. vs. Respondent: Second DivisionCassie GacottNo ratings yet
- Prof DR Akram ICUDocument233 pagesProf DR Akram ICUramzi MohamedNo ratings yet
- Recent Progress in Gene Therapy For HemophiliaDocument10 pagesRecent Progress in Gene Therapy For HemophiliaSo BaNo ratings yet
- Cracking The MRCS Viva A Revision GuideDocument554 pagesCracking The MRCS Viva A Revision GuideAnonymous ZUW1pT100% (1)
- 03-01 Slides Innate Immune System IntroDocument5 pages03-01 Slides Innate Immune System Introlow ah keongNo ratings yet
- OsteoarthritisDocument4 pagesOsteoarthritisDharti PatelNo ratings yet
- DapusDocument3 pagesDapussutisnoNo ratings yet
- Aplastic Anemia: Definition, Diagnosis, Treatment and Response CriteriaDocument24 pagesAplastic Anemia: Definition, Diagnosis, Treatment and Response CriteriaAnna Puteri GozaliNo ratings yet
- Greenmedinfo Intentional Movement The Path To Restoring Your Vital SelfDocument21 pagesGreenmedinfo Intentional Movement The Path To Restoring Your Vital SelfsiesmannNo ratings yet