Professional Documents
Culture Documents
Apophysitis of The Tibial Tuberosity (Osgood-Schlatter Disease) : A Review
Apophysitis of The Tibial Tuberosity (Osgood-Schlatter Disease) : A Review
Uploaded by
BreechesCopyright:
Available Formats
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5819)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Anterior Knee Pain - Sorting Out The CausesDocument30 pagesAnterior Knee Pain - Sorting Out The CausesHula XdNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Osgood-Schlatter DiseaseDocument6 pagesOsgood-Schlatter DiseaseDonny KurniawanNo ratings yet
- Kss Taos Good PrintDocument10 pagesKss Taos Good PrintAfifah Nur FauzaniNo ratings yet
- 10.1016@j.csm.2009.09.004 2Document26 pages10.1016@j.csm.2009.09.004 29661jackNo ratings yet
- Leadership: Activity Modification: Because Osgood-SchlatterDocument4 pagesLeadership: Activity Modification: Because Osgood-Schlatterberndjulie726No ratings yet
- Aaos Pediatric 2020Document57 pagesAaos Pediatric 2020ABUBAKER ZANBOUZINo ratings yet
- 668-Osgood-Schlatter Powerpoint Spring 2015Document38 pages668-Osgood-Schlatter Powerpoint Spring 2015api-280210660No ratings yet
- Injuri & Trauma Saat Olahraga & Penatalaksanaannya (DR - Arief Faisal, SP - OT)Document53 pagesInjuri & Trauma Saat Olahraga & Penatalaksanaannya (DR - Arief Faisal, SP - OT)Wulan Nindira WarasudiNo ratings yet
- Osgood Schlatter DiseaseDocument6 pagesOsgood Schlatter DiseaseJoni MokodoNo ratings yet
- Activity Modification and Knee Strengthening For Osgood-Schlatter DiseaseDocument9 pagesActivity Modification and Knee Strengthening For Osgood-Schlatter DiseaseSebastian FandiñoNo ratings yet
- Youth Fitness Course 2013 PDFDocument334 pagesYouth Fitness Course 2013 PDFCarlos AguilarNo ratings yet
- Clinical Review: Osgood-Schlatter SyndromeDocument11 pagesClinical Review: Osgood-Schlatter SyndromeAlejandra RomeroNo ratings yet
- PatellofemoralPainSyndrome AAFP2019Document7 pagesPatellofemoralPainSyndrome AAFP2019Stephanie SennaNo ratings yet
- Lesi MeniskusDocument115 pagesLesi MeniskusHanif AhmadNo ratings yet
- Osgood-Schlatter Disease For HealthDocument10 pagesOsgood-Schlatter Disease For Healthapi-346839713No ratings yet
- Osteochondroses: Franklin Danger, MD Christopher Wasyliw, MD Laura Varich, MDDocument7 pagesOsteochondroses: Franklin Danger, MD Christopher Wasyliw, MD Laura Varich, MDadrianNo ratings yet
- Best Homeopathic Remedies For Knee PainDocument29 pagesBest Homeopathic Remedies For Knee PainKrish MotupalliNo ratings yet
- Osgood-Schlatter DiseaseDocument10 pagesOsgood-Schlatter DiseaseAli AmearNo ratings yet
- Disorders of Epiphyses and Epiphyseal Growth - IGNDocument11 pagesDisorders of Epiphyses and Epiphyseal Growth - IGNWigunaNo ratings yet
- The Epiphyseal Plate: Physiology, Anatomy, and TraumaDocument12 pagesThe Epiphyseal Plate: Physiology, Anatomy, and TraumaLaura Mérida CáceresNo ratings yet
- Osgood-Schlatter Disease: Journal ReadingDocument4 pagesOsgood-Schlatter Disease: Journal ReadingfitriarsNo ratings yet
- Janu Basti Treatment in AyurvedaDocument17 pagesJanu Basti Treatment in AyurvedaAP AyurvedaNo ratings yet
- Affections of The KneeDocument92 pagesAffections of The KneeJudy Ann Bahom SantiagoNo ratings yet
- Prentice9e Im Chap25Document6 pagesPrentice9e Im Chap25api-281340024No ratings yet
- Ortho - OSCE 1 1Document120 pagesOrtho - OSCE 1 1Santosh DahitNo ratings yet
- Frequently Missed Fractures in Pediatric TraumaDocument13 pagesFrequently Missed Fractures in Pediatric Traumaalejasuarez248No ratings yet
- BursitisDocument21 pagesBursitisJigisha ChavdaNo ratings yet
- OsgoodDocument8 pagesOsgooddiretoriacmbaNo ratings yet
- Orthopedic Surgery - Specific Considerations - Schwartz's Principles of Surgery ABSITE and Board Review, 9th EdDocument16 pagesOrthopedic Surgery - Specific Considerations - Schwartz's Principles of Surgery ABSITE and Board Review, 9th Edvnnv101.raceacNo ratings yet
- Osgood Schlatter Disease With Exercises ChocDocument4 pagesOsgood Schlatter Disease With Exercises ChocJoni MokodoNo ratings yet
Apophysitis of The Tibial Tuberosity (Osgood-Schlatter Disease) : A Review
Apophysitis of The Tibial Tuberosity (Osgood-Schlatter Disease) : A Review
Uploaded by
BreechesOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Apophysitis of The Tibial Tuberosity (Osgood-Schlatter Disease) : A Review
Apophysitis of The Tibial Tuberosity (Osgood-Schlatter Disease) : A Review
Uploaded by
BreechesCopyright:
Available Formats
Open Access Review
Article DOI: 10.7759/cureus.780
Apophysitis of the Tibial Tuberosity
(Osgood-Schlatter Disease): A Review
Raju Vaishya 1 , Ahmad Tariq Azizi 2 , Amit Kumar Agarwal 1 , Vipul Vijay 1
1. Orthopaedics, Indraprastha Apollo Hospitals 2. Orthoapedics, Herat Regional Hospital, Herat,
Afghanistan
Corresponding author: Amit Kumar Agarwal, amitorthopgi@yahoo.co.in
Disclosures can be found in Additional Information at the end of the article
Abstract
Osgood-Schlatter disease (OSD) is a condition in which the patellar tendon insertion on the
tibial tuberosity becomes inflamed. It is a well-known condition in late childhood characterized
by pain and a bony prominence over the tibial tuberosity. The pain is usually exacerbated by
physical activities like running, jumping, and climbing stairs. In the acute stage, the margins of
the patellar tendon become blurred in radiographs due to the soft tissue swelling. After three to
four months, bone fragmentation at the tibial tuberosity is viewed. In the sub-acute stage, soft
tissue swelling resolves, but the bony ossicle remains. In the chronic stage, the bone fragment
may fuse with the tibial tuberosity which can appear normal.
The primary goal in the treatment of OSD is the reduction of pain and swelling over the tibial
tuberosity. The patient should limit physical activities until the symptoms are resolved. In some
cases, the patient should restrict physical activities for several months. The presence of pain
with kneeling because of an ossicle that does not respond to conservative measures is the
indication for surgery. In these cases, the removal of the ossicle, surrounding bursa, and the
bony prominence is the treatment of choice.
Categories: Orthopedics
Keywords: tibial tuberosity, osgood-schlatter disease, apophysitis
Introduction And Background
Osgood-Schlatter disease (OSD, also called Lannelongue’s disease) is a condition in which the
patellar tendon insertion on the tibial tuberosity becomes inflamed [1-2]. It is a well-known
condition in late childhood characterized by pain over the tibial tuberosity along with a bony
prominence. Usually, it resolves at the end stages of skeletal growth. Boys are affected more
often than girls, and the age of affection is typically in the second decade of life (10 to 15 years
Received 08/01/2016
Review began 08/25/2016 in boys and eight to twelve years in girls) [3]. Usually, less than 25% of patients complain of
Review ended 09/02/2016 pain over the tibial tuberosity. In the early stages of OSD, the patients have pain on the tibial
Published 09/13/2016 tuberosity after physical activities, but over time, the pain becomes permanent and steady
© Copyright 2016 regardless of activity. In x-rays, a regular ossification (ossicle) is demonstrated over the tibial
Vaishya et al. This is an open access tuberosity. Treatment includes conservative and surgical options. Conservative treatment
article distributed under the terms of includes modifying physical activities, using ice packs, nonsteroidal anti-inflammatory drugs
the Creative Commons Attribution
(NSAIDs), braces, and pads. Symptoms usually resolve after the closure of the physis without
License CC-BY 3.0., which permits
unrestricted use, distribution, and
any treatment, but symptoms may remain in some cases. In almost ten percent of patients, the
reproduction in any medium, bone fragments do not fuse, and these patients complain of pain in front of the knee, even after
provided the original author and slight physical activity but especially after kneeling [4-6]. This pain typically relates to the
source are credited. mobile and unfused bone fragments, which may require surgical excision.
How to cite this article
Vaishya R, Azizi A, Agarwal A, et al. (September 13, 2016) Apophysitis of the Tibial Tuberosity (Osgood-
Schlatter Disease): A Review. Cureus 8(9): e780. DOI 10.7759/cureus.780
Review
Clinical Presentation
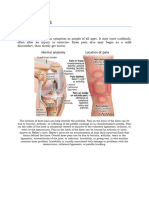
Pain and swelling are the primary symptoms felt in the lower aspect of the knee, around the
patellar attachment to the tibial tuberosity (Figure 1) [7-8].
FIGURE 1: Bony prominence over the tibial tuberosity in OSD
The pain is usually exacerbated by physical activities like running, jumping, and climbing stairs.
Knee extension against resistant and other sports-related activities may worsen the symptoms.
In 20% to 30% of cases, both knees are affected, but symptom intensity can vary in each knee.
Investigations
In the acute stage, the margins of the patellar tendon become blurred in radiographs due to the
soft tissue swelling. After three to four months, bone fragmentation at the tibial tuberosity is
viewed. In the sub-acute stage, soft tissue swelling resolves, but the bone ossicle remains. In
the chronic stage, the bone fragment may fuse with the tibial tuberosity which can appear
normal. However, sometimes the bone fragment is displaced (Figure 2).
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 2 of 9
FIGURE 2: Separated ossicle and bony prominence seen in
lateral radiography of knee in OSD.
Ultrasound may be useful as it determines any swelling in the soft tissue, cartilage, bursa, and
tendon [9-10]. It also detects any new bone formation if present in the area. Magnetic resonance
imaging is more sensitive than ultrasound and determines soft tissue swelling in front of the
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 3 of 9
tibial tuberosity, edema of the patellar tendon, infrapatellar bursitis (a deep infrapatellar
bursitis is a frequent finding) [11], and bone marrow edema.
Differential diagnosis
There are some other diseases that should be considered in the differential diagnosis of OSD,
such as Sinding-Larsen-Johansson syndrome, Hoffa’s syndrome, soft tissue or bone tumors,
patellar tendon avulsion or rupture, chondromalacia patella, patellar tendinitis, infectious
apophysitis, accessory ossification centers, osteomyelitis of the proximal tibia, and tibial
tubercle fracture (Table 1, Figure 3) [12].
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 4 of 9
Condition Signs/symptoms Investigations
A history of trauma is present, the onset of symptoms is An irregular line is present on x-ray
Fracture of tibial
sudden, and the patient is not able to extend the knee or without fragmentation of tibial
tuberosity
bear weight on the knee. tuberosity.
Hoffa’s disease (Fat pad Tenderness in the anterior joint line lateral to the patellar
X-ray is normal in Hoffa’s disease.
hypertrophy/impingement) tendon.
Sinding-Larsen and On x-ray, the tibial tuberosity is
Johansson syndrome Maximal tenderness is at the inferior pole of the patella, normal, and an ossicle or
(Inferior patellar pole not at the tibial tubercle. osteophyte in the lower pole of the
traction apophysitis) patella is present.
X-ray is normal or may show a soft
It is difficult to differentiate infrapatellar bursitis from OSD
tissue swelling. In MRI, tibial
clinically; the location of pain is at or near the attachment
Infrapatellar bursitis tuberosity is normal, but it shows
of the patellar tendon to the tibial tuberosity, but there
the fluid collection in the
may be no tenderness when palpating the tibial tuberosity.
infrapatellar region.
In blood exam, there are increased
levels of ESR, CRP, and WBC.
Pain may be present with activity or rest, and systemic
Osteomyelitis Blood culture is positive, and soft
symptoms and signs of infection are present.
tissue swelling periosteal reaction
are seen in x-ray.
The lesion is apparent via x-ray in
Pain is located in the anterior or anteromedial aspect of
Osteochondritis the lateral aspect of the medial
the knee. Tenderness is localized to the joint line (usually
dissecans of the knee femoral condyle. Otherwise, an MRI
medial), with no tenderness on tibial tuberosity.
is needed for diagnosis.
Radiographic studies are normal or
may show a soft tissue swelling.
It is difficult to differentiate from OSD, and may occur as a
Patellar tendonitis Tibial tuberosity appears normal in
complication of OSD.
MRI or may show increased signal
in the patellar tendon.
Pain is present in the knee region (patellofemoral pain). On
In the radiographic study, there may
examination, pain becomes apparent with pressure on
Chondromalacia patella be bone damage, or signs of
patella or manipulating patella above femoral condyle [14].
(runner’s knee) arthritis seen. MRI will reveal
A grinding or cracking feel is present during extension and
any cartilage damage.
flexion of the knee joint.
TABLE 1: Table showing the differential diagnosis of OSD
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 5 of 9
FIGURE 3: Other conditions that should be considered in
differential diagnosis of OSD have been marked over the bone
model
Management
The primary goal in the treatment of OSD is the reduction of pain and swelling over the tibial
tuberosity. For this reason, the patient should limit physical activities until the symptoms are
resolved, which can sometimes take several months. Other conservative treatments include the
use of ice packs, NSAIDs like ibuprofen and naproxen (to reduce pain and swelling), protective
padding, and physiotherapy.
Physiotherapy
Exercises for the improvement of the quadriceps, hamstrings, and gastrocnemius muscles are
recommended. Immobilizing the knee (using a cast or brace) can reduce strain on the tibial
tuberosity [13,14].
Surgery
Surgery is indicated when ossicle pain on kneeling persists despite conservative treatment
measures. In these cases, removal of the ossicle, surrounding bursa, and the bony prominence
is the treatment of choice [15]. For a growing child, surgery does not seem to offer any benefit.
A five-year follow-up trial reviewed two groups of patients with these symptoms. One group
was treated surgically by tibial sequestrectomy, and the other group was treated conservatively.
No benefit was found in the first method versus the second [16]. Binazzi, et al. found that the
excision of the ossicle is the standard surgical method and removal of the prominent tibial
tuberosity is optional [17].
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 6 of 9
Pihlajamäki, et al. studied the outcomes of the patients who did not respond to conservative
measures and were surgically treated [18]. In a ten-year study period, they found that 93
patients (87%) participated in daily activities normally, 80 (75%) patients reached their pre-
surgery level of sports activity. Forty-one patients (38%) could kneel without restriction or
pain. Mild postsurgical complications were seen in six patients.
The detailed algorithm for treatment of OSD is presented in Figure 4.
FIGURE 4: The algorithm for treatment of OSD
Rehabilitation
In this period, the focus is on muscle strengthening, gait training, and pain control to restore a
functional knee.
Discussion
OSD is usually a self-limiting disease, and symptoms may resolve without any particular
treatment or with simple conservative treatment, like activity restriction or immobilization in a
cast for three to six weeks. Surgery is rarely indicated for OSD. Krause, et al. studied the natural
history of untreated OSD. In 69 affected knees in 50 patients, they found that 76% of patients
had no activity restriction, but only 60% of patients [PME1] could kneel without pain [19]. They
suggested that persistent symptoms of OSD for more than two years warranted exploration.
Krause, et al. noted that symptoms of OSD are resolvable in most of the cases, and, in those
cases that persist, x-rays may show a fragmentation of the tibial tuberosity. Lynch and Walsh
described that among the patients they followed, just two patients had premature fusion of the
tibial apophysis with conservative treatment [6].
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 7 of 9
If the symptoms persist, surgery may be indicated. One trial noted, however, that after tibial
sequestrectomy (removal of the fragments), clinical results were no better than those seen with
conservative treatments [20]. Bosworth recommended inserting bone pegs into the tibial
tubercle; this is a simple procedure and usually, resolves the symptoms [20]. Thomson and
Ferciot, et al. pointed out, however, that an indecent prominence remains after this surgery
[21-22]. They recommended a longitudinal incision in the patellar tendon for the excision of the
bony prominence. Longitudinal growth of the tibia was not disturbed in a series of 41
operations by Thomson, et al., 11 in the Ferciot series, and 42 in the Flowers and Bhadreshwar
series [21-22,5]. The reported complications of OSD in the patients treated conservatively or
surgically, include patellar subluxation, patella alta, non-fusing fragments or a premature
fusion that could result in genu recurvatum. Høgh and Lund recommended delaying surgery
until the apophysis has fused [23].
Conclusions
Osgood-Schlatter disease (OSD) is usually a self-limiting disease mainly seen in late childhood.
The symptoms usually resolve without any specific treatment or with simple conservative
treatment such as the restriction of activity or immobilization in a cast for three to six weeks.
Surgery is rarely indicated for OSD. If the symptoms persist and become disabling to the
patient, surgery may be indicated especially after the fusion of the apophysis. The excision of
the ossicle is the common surgical method, and removal of any prominences on the tibial
tuberosity is optional.
Additional Information
Disclosures
Conflicts of interest: The authors have declared that no conflicts of interest exist.
References
1. Grimm NL, Weiss JM, Kessler JI, et al.: Osteochondritis dissecans of the knee: pathoanatomy,
epidemiology, and diagnosis. Clin Sports Med. 2014, 33(2):181-8. 10.1016/j.csm.2013.11.006
2. Nowinski RJ, Mehlman CT: Hyphenated history: Osgood-Schlatter disease . Am J Orthop (Belle
Mead NJ). 1998, 27(8):584-5.
3. Gholve PA, Scher DM, Khakharia S, et al.: Osgood Schlatter syndrome. Curr Opin Pediatr.
2007, 19(1):44–50.
4. Mital MA, Matza RA, Cohen J: The so-called unresolved Osgood-Schlatter lesion: a concept
based on fifteen surgically treated lesions. J Bone Joint Surg Am. 1980, 62(5):732–9.
5. Flowers MJ, Bhadreshwar DR: Tibial tuberosity excision for symptomatic Osgood-Schlatter
disease. J Pediatr Orthop. 1995, 15(3):292–7.
6. Lynch MC, Walsh HP: Tibia recurvatum as a complication of Osgood-Schlatter’s disease: a
report of two cases. J Pediatr Orthop. 1991, 11:543–544.
7. Atanda A, Shah SA, O’Brien K: Osteochondrosis: common causes of pain in growing bones .
American family physician. 2011, 83(3):285–91.
8. Cakmak, S, Tekin, L, &Akarsu, S: Long-term outcome of Osgood-Schlatter disease: not always
favorable. Rheumatol int. 2014, 34(1):135-6. 10.1007/s00296-012-2592-0
9. Nakase J, Aiba T, Goshima K, et al.: Relationship between the skeletal maturation of the distal
attachment of the patellar tendon and physical features in preadolescent male football
players. Knee Surg Sports Traumatol Arthrosc. 2014, 22(1):195-9. 10.1007/s00167-012-2353-3
10. Carr JC, Hanly S, Griffin J, et al.: Sonography of the patellar tendon and adjacent structures in
pediatric and adult patients. Am J Roentgenol. 2001, 176:1535-9. 10.2214/ajr.176.6.1761535
11. Rosenberg ZS, Kawelblum M, Cheung YY, et al.: Osgood-Schlatter lesion: fracture or
tendinitis? Scintigraphic, CT, and MR imaging features. Radiology. 1992, 185(3):853-8.
10.1148/radiology.185.3.1438775
12. Duri ZA, Aichroth PM, Wilkins R, et al.: Patellar tendonitis and anterior knee pain . Am J Knee
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 8 of 9
Surg. 1999, 12(2):99-108.
13. Frank JB, Jarit GT, Bravman JT, et al.: Lower extremity injuries in the skeletally immature
athlete. J Am Acad Orthop Surg. 2007, 15(6):356–366.
14. Kujala UM, Kvist M, Heinonen O: Osgood-Schlater’s disease in adolescent athletes.
Retrospective study of incidence and duration. Am J Sports Med. 1985, 13:236–241.
15. Orava S, Malinen L, Karpakka J, et al.: Results of surgical treatment of unresolved Osgood-
Schlatter lesion. Ann Chir Gynaecol. 2000, 89(4):298–302.
16. Trail IA: Tibial sequestrectomy in the management of Osgood-Schlatter disease . J Pediatr
Orthop. 1988, 8(5):554-7.
17. Binazzi R, Felli L, Vaccari V, et al.: Surgical treatment of unresolved Osgood-Schlatter lesion .
Clin Orthop Relat Res. 1993, 289:202–4.
18. Pihlajamäki HK, Mattila VM, Parviainen M, et al.: Long-term outcome after surgical treatment
of unresolved Osgood-Schlatter disease in young men. J Bone Joint Surg Am. 2009,
91(10):2350-58.
19. Krause BL, Williams JPR, Catterall A: Natural history of Osgood-Schlatter disease . J Pediatr
Orthop. 1990, 10:65-68.
20. Bosworth DM: Autogenous bone pegging for epiphysitis of the tibial tubercle . J Bone Joint
Surg. 1934, 16:829.
21. Thomson JEM: Operative treatment of osteochondritis of the tibial tubercle . J Bone Joint Surg.
1956, 38:142-148.
22. Ferciot C: Surgical management of anterior tibial epiphysis . Clin Orthop Relat Res. 1955,
5:204-6.
23. Høgh J, Lund B: The sequelae of Osgood-Schlatter's disease in adults . Int Orthop. 1988,
12(3):213-5.
2016 Vaishya et al. Cureus 8(9): e780. DOI 10.7759/cureus.780 9 of 9
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5819)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Anterior Knee Pain - Sorting Out The CausesDocument30 pagesAnterior Knee Pain - Sorting Out The CausesHula XdNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Osgood-Schlatter DiseaseDocument6 pagesOsgood-Schlatter DiseaseDonny KurniawanNo ratings yet
- Kss Taos Good PrintDocument10 pagesKss Taos Good PrintAfifah Nur FauzaniNo ratings yet
- 10.1016@j.csm.2009.09.004 2Document26 pages10.1016@j.csm.2009.09.004 29661jackNo ratings yet
- Leadership: Activity Modification: Because Osgood-SchlatterDocument4 pagesLeadership: Activity Modification: Because Osgood-Schlatterberndjulie726No ratings yet
- Aaos Pediatric 2020Document57 pagesAaos Pediatric 2020ABUBAKER ZANBOUZINo ratings yet
- 668-Osgood-Schlatter Powerpoint Spring 2015Document38 pages668-Osgood-Schlatter Powerpoint Spring 2015api-280210660No ratings yet
- Injuri & Trauma Saat Olahraga & Penatalaksanaannya (DR - Arief Faisal, SP - OT)Document53 pagesInjuri & Trauma Saat Olahraga & Penatalaksanaannya (DR - Arief Faisal, SP - OT)Wulan Nindira WarasudiNo ratings yet
- Osgood Schlatter DiseaseDocument6 pagesOsgood Schlatter DiseaseJoni MokodoNo ratings yet
- Activity Modification and Knee Strengthening For Osgood-Schlatter DiseaseDocument9 pagesActivity Modification and Knee Strengthening For Osgood-Schlatter DiseaseSebastian FandiñoNo ratings yet
- Youth Fitness Course 2013 PDFDocument334 pagesYouth Fitness Course 2013 PDFCarlos AguilarNo ratings yet
- Clinical Review: Osgood-Schlatter SyndromeDocument11 pagesClinical Review: Osgood-Schlatter SyndromeAlejandra RomeroNo ratings yet
- PatellofemoralPainSyndrome AAFP2019Document7 pagesPatellofemoralPainSyndrome AAFP2019Stephanie SennaNo ratings yet
- Lesi MeniskusDocument115 pagesLesi MeniskusHanif AhmadNo ratings yet
- Osgood-Schlatter Disease For HealthDocument10 pagesOsgood-Schlatter Disease For Healthapi-346839713No ratings yet
- Osteochondroses: Franklin Danger, MD Christopher Wasyliw, MD Laura Varich, MDDocument7 pagesOsteochondroses: Franklin Danger, MD Christopher Wasyliw, MD Laura Varich, MDadrianNo ratings yet
- Best Homeopathic Remedies For Knee PainDocument29 pagesBest Homeopathic Remedies For Knee PainKrish MotupalliNo ratings yet
- Osgood-Schlatter DiseaseDocument10 pagesOsgood-Schlatter DiseaseAli AmearNo ratings yet
- Disorders of Epiphyses and Epiphyseal Growth - IGNDocument11 pagesDisorders of Epiphyses and Epiphyseal Growth - IGNWigunaNo ratings yet
- The Epiphyseal Plate: Physiology, Anatomy, and TraumaDocument12 pagesThe Epiphyseal Plate: Physiology, Anatomy, and TraumaLaura Mérida CáceresNo ratings yet
- Osgood-Schlatter Disease: Journal ReadingDocument4 pagesOsgood-Schlatter Disease: Journal ReadingfitriarsNo ratings yet
- Janu Basti Treatment in AyurvedaDocument17 pagesJanu Basti Treatment in AyurvedaAP AyurvedaNo ratings yet
- Affections of The KneeDocument92 pagesAffections of The KneeJudy Ann Bahom SantiagoNo ratings yet
- Prentice9e Im Chap25Document6 pagesPrentice9e Im Chap25api-281340024No ratings yet
- Ortho - OSCE 1 1Document120 pagesOrtho - OSCE 1 1Santosh DahitNo ratings yet
- Frequently Missed Fractures in Pediatric TraumaDocument13 pagesFrequently Missed Fractures in Pediatric Traumaalejasuarez248No ratings yet
- BursitisDocument21 pagesBursitisJigisha ChavdaNo ratings yet
- OsgoodDocument8 pagesOsgooddiretoriacmbaNo ratings yet
- Orthopedic Surgery - Specific Considerations - Schwartz's Principles of Surgery ABSITE and Board Review, 9th EdDocument16 pagesOrthopedic Surgery - Specific Considerations - Schwartz's Principles of Surgery ABSITE and Board Review, 9th Edvnnv101.raceacNo ratings yet
- Osgood Schlatter Disease With Exercises ChocDocument4 pagesOsgood Schlatter Disease With Exercises ChocJoni MokodoNo ratings yet