Professional Documents
Culture Documents
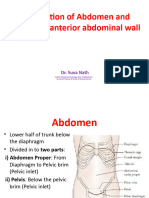
239 Transversus Abdominus Plane Block
Uploaded by
Ramesh lal ShahCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
239 Transversus Abdominus Plane Block
Uploaded by
Ramesh lal ShahCopyright:
Available Formats
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.
com
TRANSVERSUS ABDOMINIS PLANE BLOCK
ANAESTHESIA TUTORIAL OF THE WEEK 239
5TH SEPTEMEBER 2011
Dr Paul Townsley, Fellow in Regional Anaesthesia
Dr James French, Consultant Anaesthetist
Nottingham University Hospitals NHS Trust.
QUESTIONS
1. Regarding the anterior abdominal wall:
a. This is supplied by the posterior primary rami of intercostal nerves T7-T12.
b. The muscles of the lateral abdominal wall are the external, internal and innermost
oblique muscles.
c. The Ilioinguinal and Iliohypogastric nerve are branches of T12 and L1.
d. The transversus abdominis plane is between the deep fascia of internal oblique and
the superficial fascia of transversus abdominis muscles.
e. The Lumbar Triangle of Petit lies between the anterior and mid-axillary lines.
2. The TAP block:
a. Reliably provides anaesthesia to the entire abdominal wall.
b. Is best performed using a high-concentration, low-volume technique.
c. Short-bevelled needles provide the best feedback during passage through fascial
layers.
d. Can be used reliably as the sole mode of analgesia.
e. Must always be performed bilaterally.
3. With regards to the Ultrasound-Guided TAP block:
a. The transversus abdominis plane is best visualised in the midline of the abdomen.
b. When advancing the needle during TAP blocks, the needle tip is best seen with an in-
plane needle view.
c. There is no need to visualise the spread of local anaesthetic with this technique.
d. Saline can be used as the initial injectate to open the fascial plane.
e. A “posterior” TAP block will spread to cover T7-T9 dermatomes only
INTRODUCTION
The Transversus Abdominis Plane (TAP) Block is a local anaesthetic block used to provide analgesia
to the anterior and lateral abdominal wall. Rafi et al (2001)[1] and McDonnell et al (2004)[2] were the
first to describe this novel abdominal field block. They described an anatomical landmark technique
and provided evidence of blockade to the mid/lower thoracic and upper lumbar spinal nerves as they
travelled in the fascial plane between the transversus abdominis and internal oblique muscles. Hebbard
et al (2007)[3] have subsequently described an ultrasound-guided approach to the TAP block.
This tutorial will outline the relevant anatomy, the landmark and ultrasound techniques described for
TAP Blocks, and some of the evidence for the use of these blocks.
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 1 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
ANATOMY
Muscles of the Abdominal Wall relative to the TAP Block
As we will discuss later, the TAP Block is performed in the lateral part of the anterior abdominal wall.
In this region of the abdominal wall there are 3 muscle layers (Fig 1).
The External Oblique Muscle
The external oblique muscle is the largest and most superficial of the 3 muscles. It runs inferiorly from
the external, inferior surfaces of the lower 8 ribs. The fibres originating from the lower ribs run
inferiorly and insert into the iliac crest. The fibres originating from the middle and uppermost ribs run
infero-anteriorly and end in a thick aponeurosis. Anteriorly, the aponeurosis joins the aponeurosis from
the transversus abdominis and internal oblique muscles forming the linea alba. Inferiorly the
aponeurosis forms the inguinal ligament.
The Internal Oblique Muscle
The internal oblique muscle is a smaller thinner muscle than the external oblique. It originates from the
inguinal ligament and the iliac crest. Its’ fibres cover the anterolateral part of the abdomen inserting
anteriorly into the linea alba, above the transversus abdominis muscle, and superiorly into the cartilages
of the lower 6 ribs.
The Transversus Abdominis Muscle
The transversus abdominis muscle is the most internal of the 3 muscle layers, lying directly beneath the
internal oblique muscle. Its’ fibres arise from the inguinal ligament, the iliac crest, the lumbodorsal
fascia and the inner surfaces of the cartilages from the lower 6 ribs. Its’ fibres run transversely across
the abdomen ending in a broad aponeurosis. This aponeurosis is formed more laterally than the
aponeuroses of the external and internal oblique muscles. It continues medially and inserts into the
linea alba.
External oblique muscle
Internal oblique muscle
Transversus abdominis
Quadratus lumborum
Figure 1: Cross section though the abdomen. The 3 muscle layers of the lateral / anterior
abdominal wall can be seen.
Sensory Supply of the Abdominal Wall
The lower 6 thoracic nerves and the first lumbar nerve supply sensation to the abdominal wall (Fig 2).
Thoracic Nerves T6 – T11
The anterior divisions of nerves from T6 – T11 travel along their relevant intercostal space, before
passing under the costal cartilages where they enter into the fascial plane between transversus
abdominis muscle and internal oblique muscle. The nerves continue on to pierce the rectus abdominis
muscle terminating as the anterior cutaneous branches supplying sensation to the skin of the anterior
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 2 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
abdomen. About half way along their course the thoracic nerves give off lateral cutaneous branches,
which travel posteriorly, piercing the external oblique muscle to supply sensation to the skin of the
lateral abdomen and back.
Thoracic Nerve 12
The anterior division of the nerve from T12 is a large nerve. It runs anteriorly along the inferior border
of the 12th nerve and then passes under the lumbocostal arch to run along with the other lower
intercostal nerves between the transversus abdominis muscle and the external oblique muscle. The T12
nerve gives a communicating branch to the L1 nerve as part of the upper part of the lumbar plexus. The
lateral cutaneous branch of T12 supplies the skin over the upper gluteal region.
The Ilioinguinal and Iliohypogastric Nerves (T12 / L1)
The Iliohypogastric and Ilioinguinal nerves of the lumbar plexus both enter the transverse abdominis
plane near to the iliac crest. The Iliohypogastric nerve divides into an anterior cutaneous branch,
supplying the skin over the hypogastrium, and a lateral cutaneous branch supplying skin over the
gluteal region. The Ilioinguinal nerve travels within the inguinal canal and supplies sensation to the
skin of the upper thigh, base of penis and scrotum.
Lateral
cutaneous
nerves
of
T6-‐T11
Lateral
cutaneous
nerves
of
T12
Iliohypogastric n.
Figure 2: Nerve supply to the anterior abdominal wall. Each Roman numeral indicates the
thoracic nerve seen below it.
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 3 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
INDICATIONS FOR TAP BLOCK
The TAP block can be used as part of an analgesic regimen for abdominal surgery. Initial studies were
able to demonstrate blocks extending from T7-L1 using bilateral injections[4]. Subsequent studies have
been unable to reproduce these findings with most studies achieving uppermost sensory levels around
T9/10. This lower block is supported by findings in a cadaveric study, looking at spread of local
anaesthetic after a single posterior TAP injection[5]. It therefore sensible to recommend that the TAP
block can only reliably be used for analgesia in surgery on the lower abdomen, for example:
• Hernia repair
• Open appendicectomy
• Caesarian section
• Total abdominal hysterectomy
• Radical prostatectomy
A subcostal TAP block has been described in addition to the posterior TAP injection. This can be
performed to provide analgesia for abdominal surgery extending above the umbilicus[6].
For a comprehensive review of the evidence for the use of the TAP block please refer to an article
published in ‘Update in Anaesthesia’. The article gives an in-depth description of the results of recent
studies[7].
CONTRAINDICATIONS TO TAP BLOCK
Absolute
• Patient refusal
• Allergy to local anaesthetic
• Localised infection over injection point
Relative
• Coagulopathy
• Surgery at injection site
COMPLICATIONS
The TAP block is a relatively safe technique with only a few case reports of significant complications.
Complications reported include:
• Failure
• Local anaesthetic toxicity
• Intraperitoneal injection
• Bowel injury
• Hepatic injury
TECHNIQUES
The aim of the TAP block is to deposit a large volume of local anaesthetic into the transversus
abdominis plane with at least 20 ml of solution being for used each side. The concentration of solution
used will depend on the calculated maximum dose of local anaesthetic allowed. There are both
landmark and ultrasound guided techniques to the TAP block and we will describe each below.
General Preparation
You will need:
• Full resuscitation equipment
• Patient monitoring (ECG, pulse oximeter, BP)
• Antiseptic skin preparation and sterile gloves
• Short bevel (30o) block needle (50 – 100 mm), or 16-G Tuohy needle, with an extension set
• 20 ml syringes
• Local anaesthetic – a long acting local anaesthetic (Levobupivacaine, Ropivacaine) should be
used in the majority of cases. 0.3-0.6 ml/kg per side can be used as to a guide for volume
calculation.
The blocks can be performed awake but are most commonly performed with the patient under general
anaesthetic.
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 4 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
Landmark Technique
The landmark technique, described by McDonnell et al, accesses the transversus abdominis plane via
the lumbar triangle of petit. This is a surface landmark bound by the external oblique muscle anteriorly,
the latissimus dorsi muscle posteriorly and the iliac crest inferiorly (Fig 3).
Costal
Margin
EO
Iliac
Crest
TOP
LD
Figure 3: Landmarks outlining the Triangle of Petit (EO, external oblique muscle; TOP,
triangle of petit; LD, latissimus dorsi muscle).
The Block
• Identify the triangle of petit using the anatomical landmarks described above. A depression can
sometimes be palpated between the posterior border of the external oblique muscle and the
anterior border of the latissimus dorsi muscle. As a guide this normally found in the region of the
posterior axillary line, directly above the iliac crest.
• Insert the short bevel regional block needle perpendicular to the skin. A Tuohy needle can also be
used.
• After piercing the skin, the needle is advanced until a ‘pop’ is felt - this is the needle piercing the
fascial extension of the external oblique muscle. The needle should be advanced until a second
’pop’ is felt, as the needle passes through the fascial extension of the internal oblique muscle. A
loss of resistance technique can also be combined with this ‘fascial click’ technique to satisfy the
operator that the fascia has been breached. The needle should now lie superficial to the transversus
abdominis muscle, in the transversus abdominis plane (Fig 4).
• After aspiration, to exclude malposition of the needle tip, the local anaesthetic is injected. A
minimum of 20 ml of local anaesthetic per side should be used.
• Be careful not to exceed the maximum safe dose of local anaesthetic
Figure 4: Diagram of transverse section of abdominal wall during landmark TAP block
performance (N, needle; ST, subcutaneous tissue; EO, external oblique muscle; IO, internal
oblique; TA, transversus abdominis; LD latissumis dorsi; QL, quadratus lumborum)
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 5 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
Ultrasound Guided Technique
We will discuss first the technique for the ultrasound guided posterior TAP block, which can be
reliably used for lower abdominal incisions. We will then describe the subcostal modification to
achieve analgesia for the upper abdomen.
This technique is more time-consuming than the landmark approach, due to preparation of ultrasound
equipment. However it can be recommended due to the benefit of viewing the needle during insertion,
therefore ensuring that the needle is placed correctly and that no other structures are injured. It must be
emphasised that the needle should be continuously seen during insertion.
Preparation
• As for the landmark technique
• Ultrasound machine
• High frequency (6-13MHz) linear array probe with probe cover and sterile gel.
• The use of vascular access probes (e.g. Sonosite iLook) for this block cannot be recommended
unless already proficient in ultrasound-guided regional anaesthesia. Intra-abdominal injury has
resulted from inadequate needle visualisation with this equipment.
• An assistant to perform injection of the local anaesthetic (optional)
The Block (Posterior Injection)
• The ultrasound transducer is positioned horizontally across the abdomen
• The muscle layers in the antero-lateral part of the abdomen can be traced by scanning from the
midline towards the area between the iliac crest and the costal margin, in the mid-axillary line.
• The rectus abdominis muscle is identified, just off the midline, as an oval / elliptical structure.
• As you scan laterally the rectus abdominis abuts a fascial plane (linea semilunaris). This
fascial plane then gives rise to 3 muscle layers: external oblique, internal oblique and
transversus abdominis (Fig 5)
Lateral Medial
External
oblique
Internal
oblique
Rectus
abdominis
Transversus
abdominis
Figure 5: Ultrasound image of the view if probe is place adjacent to the midline to visualise
the rectus abdominis muscle medially and the origins of the external oblique, internal oblique
and transversus abdominis muscles laterally.
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 6 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
• The ultrasound transducer is moved to scan laterally where the 3 muscle layers can be seen
running parallel to one another (Fig 6)
Lateral Medial External
oblique
Internal
oblique
Transversus
abdominis
plane
Transversus
abdominis
Figure 6: Ultrasound image obtained as the probe is moved laterally away from the midline
• The ultrasound transducer is moved more posteriorly, aiming to view the point where the
transversus abdominis muscle begins to tail off. With an adequate ultrasound image, the
regional block needle is inserted anterior to the transducer. This allows an in plane view of the
needle as you pierce the transversus abdominis plane (Fig 7 & 8)
Figure 7: Picture showing the ultrasound transducer position and in-plane needle
technique for the posterior TAP block on the right side of the patient.
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 7 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
External
needle
oblique
Internal
oblique
Transversus
abdominis
plane
Transversus
Posterior Anterior abdominis
Figure 8: Ultrasound image during posterior TAP Block. The transversus abdominis muscle
can be seen to taper into a fascial line. The approximate needle insertion angle is indicated.
• The local anaesthetic is then slowly injected. If the needle is correctly positioned, the fascial
plane is seen to separate and form a well-defined, hypoechoic, elliptical shape between the
internal oblique and transversus abdominis muscles.
• It is essential to watch for the spread of local anaesthetic. If a patchy opacity appears within
the muscle either superficial or deep to the transversus abdominis plane, then the needle
should be repositioned until local is seen to spread within the plane, separating the fascia
between the muscles. Obviously if no local is seen to appear – stop; the needle tip may not be
where you think it is, or the local is being injected into a vessel or the peritoneal cavity (Fig
9).
Too superficial Too deep TAPtastic
Figure 9: Figure highlighting the optimal needle position during ultrasound-guided TAP block.
The Block (Subcostal Injection)
• This should be performed if analgesia of the abdominal wall above the umbilicus is required.
It will provide analgesia for areas of the upper abdomen that are not usually adequately
covered by the landmark or posterior TAP approaches.
• The ultrasound transducer should be placed under the costal margin, close to the midline, and
the upper portion of the rectus muscle identified. In the midline of the subcostal region the
transversus abdominis muscle can be seen deep to the rectus abdominis muscle, unlike near
the umbilicus where it is seen only lateral to the rectus muscle. (Fig 10 & 11).
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 8 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
Figure 10: Picture showing the ultrasound transducer position and in-plane needle technique
for the oblique subcostal TAP block on the left side of the patient.
Medial
Lateral
Rectus
abdominis
Transversus
abdominis
plane
Transversus
abdominis
Peritoneal
cavity
Figure 11: Ultrasound image of rectus abdominis and transversus abdominis muscles
immediately adjacent to the midline. Dotted white line indicates the desired needle position.
• Insert the needle at the medial end of the transducer to obtain an in-plane view. Use a long
regional block needle for a single-shot technique or a Tuohy needle if a catheter is to be
placed as for a continuous technique.
• Once the tip of the needle is placed between the posterior rectus sheath and superficial border
of transversus abdominis, inject a small amount of local anaesthetic (after aspiration). The
needle should then be cautiously advanced into the space created by the local anaesthetic.
• Further injection and needle advancement should continue following along an oblique line
from the xiphoid process towards the anterior part of the iliac crest. As you scan along this
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 9 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
line you reach the lateral border of rectus abdomins. Here you find the origin of the internal
and external oblique muscles. The transversus abdominis muscle continues to run deep to the
IO muscle. (Fig 12 and Fig 13)
Medial Lateral
Rectus
abdominis
External
oblique
Transversus
LS
abdominis
plane
Transversus
abdominis
Peritoneal
cavity
Figure 12: Ultrasound image of the subcostal transversus abdominis plane as you scan
laterally from the midline along an oblique line form the xiphoid process towards the anterior
superior iliac spine. Note the lateral border of rectus abdominis and the origin of external
oblique muscle. LS=linea semilunaris.
Medial Lateral
External
Transversus
oblique
abdominis
plane
Internal
oblique
Transversus
abdominis
Peritoneal
cavity
Figure 13: Ultrasound image of the lateral subcostal transversus abdominis abdominis plane
as the ultrasound probe continues further toward the ASIS. Note the continuation of
transversus abdominis muscle and the origins of external and internal oblique muscles.
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 10 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
• Up to 20mls of local anaesthetic may be needed to fill the TA plane along this oblique
subcostal line. Some recommend using higher volumes of more dilute local anaesthetic.
• It should be said that this is an advanced level block, as significant needle-guidance skills are
required to safely perform this block.
IMPORTANT POINTS
• TAP blocks are adjunctive techniques for analgesia. They
do not adequately provide anaesthesia for surgery as it
provides no visceral anaesthesia or analgesia.
• Landmark and Posterior USG TAP blocks, if performed
correctly, will reliably provide analgesia for operations at or
below the umbilicus.
• Oblique Subcostal TAP blocks can be considered for areas
above the umbilicus.
• These are fascial plane techniques, and rely on the
deposition of large volumes of local anaesthetic to
anaesthetise multiple small abdominal wall nerves.
Maximum local anaesthetic doses must be calculated to
avoid the effects of systemic toxicity.
ANSWERS TO QUESTIONS
1 a) F The nerve supply originates from the anterior primary rami of T7-T12
b) F The muscles of the lateral abdominal wall are: external oblique, internal oblique and
transversus abdominis
c) T
d) T
e) F The lumbar triangle of petit lies posterior to the mid axillary line
2 a) F TAP block reliably provides analgesia for operations at or below the umbilicus (T10 – L1)
b) F TAP block is best performed using a high volume technique. The concentration should be
guided by the maximum calculated dose for the patients weight
c) T
d) F The TAP block provides analgesia to the abdominal wall but provides no visceral analgesia. It
should be used in combination with an oral or intravenous analgesia
e) F The TAP block can be used for unilateral procedures e.g. appendicectomy / inguinal hernia
repair
3 a) F The rectus abdominis muscle is best viewed close to the midline of the abdomen. The
transversus abdominis plane can be traced from its’ insertion to the linea alba (lateral to rectus
abdominis) and is best viewed in the lateral part of the abdomen.
b) T
c) F Observing the spread of local anaesthetic is key to ensuring you are in the transversus
abdominis plane. It is important to identify if your needle is intramuscular and reposition your
needle as necessary
d) T
e) F A posterior TAP block will reliably provide analgesia to dermatomes T9/10 – L1. Some
studies have reported higher blocks, upto T7[4], from a single posterior injection. However,
consideration should be given to a second injection using the oblique subcostal technique if
analgesia is required for the upper abdomen.
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 11 of 12
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
REFERENCES and FURTHER READING
1. AN Rafi, Abdominal Field Block: a New Approach Via The Lumbar Triangle; Anaesthesia; 2001;
56:1024-6
2. JG McDonnell, BD O’Donnell, D Tuite, T Farrell, C Power, The Regional Abdominal Field
Infiltration Technique Computerised Tomographic and Anatomical Identification of a Novel Approach
to the Transversus Abdominis Neuro-Vascular Fascial Plane; Anaesthesiology; 2004; 101: A899
3. P Hebbard, Y Fujiwara, Y Shibata, C Royse. Ultrasound Guided Transversus Abdominis Plane
Block. Anaesthesia & Intensive Care; 2007; 35(4): 616-7
4. JG McDonnell, B O’Donnell, G Curley, A Heffernan, C Power, JG Laffey. The analgesic Effect of
Transversus Abdominis Plane Block After Abdominal Surgery. Anaesthetsia & Analgesia; 2007;
104(1): 193-7
5. TMN Tran, JJ Ivanusic, P Hebbard, MJ Barrington. Determination of Spread of Injectate After
Ultrasound Guided Transversus Abdominis Plane Block: A Cadaveric Study. British Journal of
Anaesthesia; 2009; 102(1): 123-7.
6. P Hebbard, M Barrington, C Vasey. Ultrasound-Guided Continuous Oblique Subcostal Transversus
Abdominis Plane Block. Regional Anesthesia & Pain Medicine; 2010; 35(5): 436-41
7. K Webster. The Transervsus Abdominis Plane (TAP) block: Abdominal plane regional anaesthesia.
Update in Anaesthesia; 2008; 24(1): 25-30. http://update.anaesthesiologists.org/wp-
content/uploads/2009/10/Transversus-Abdominis-Plane-TAP-Block.pdf
The anatomy section was written with help from Gray's Anatomy: The Anatomical Basis of Clinical
Practice, 40th edition (2008), 1576 pages, Churchill-Livingstone, Elsevier. ISBN 978-0-443-06684-9
SOURCES of IMAGES
Figure 1 – Regional Anatomy Atlas Viewer. Robert Livingston. March 2010 (RAA Viewer is
a free resource and may be freely distributed for non-commercial use)
Other images provided by Authors
ATOTW 239 Transversus Abdominus Plane Block 05/09/2011 Page 12 of 12
You might also like
- Nerve Blocks of The Anterior AbdominalDocument5 pagesNerve Blocks of The Anterior AbdominalBinas GirmaNo ratings yet
- Transversus Abdominis Plane (Tap) BlockDocument6 pagesTransversus Abdominis Plane (Tap) BlockSuresh KumarNo ratings yet
- Anterolateral Abdominal WallDocument22 pagesAnterolateral Abdominal Wallvalerie obehiNo ratings yet
- Abdomen and ThoraxDocument7 pagesAbdomen and ThoraxchadNo ratings yet
- Transversus Abdominis Plane (Tap)Document5 pagesTransversus Abdominis Plane (Tap)Edwin mudumiNo ratings yet
- 2 B Anterior Abdominal Wall and StomachDocument29 pages2 B Anterior Abdominal Wall and StomachArif NabeelNo ratings yet
- Abdomen 2023Document131 pagesAbdomen 2023Fenot YBNo ratings yet
- Anterior Abdominal Wall SonaliiiDocument36 pagesAnterior Abdominal Wall Sonaliiisonali swainNo ratings yet
- Trans Versus Abdominis Plane BlockDocument7 pagesTrans Versus Abdominis Plane BlockIvette M. Carroll D.No ratings yet
- Anterior Abdominal WallDocument108 pagesAnterior Abdominal WallMunikrishna Salavakam100% (1)
- TAP Block 2Document5 pagesTAP Block 2Parvathy R NairNo ratings yet
- Anterior Abdominal WallDocument39 pagesAnterior Abdominal WallZllison Mae Teodoro MangabatNo ratings yet
- Miller2018 PDFDocument15 pagesMiller2018 PDFAnis BergerNo ratings yet
- Dinding Abdomen PSIKDocument79 pagesDinding Abdomen PSIKSondang DamanikNo ratings yet
- Musculature and Fascia: Station 1: The Anterior Abdominal WallDocument10 pagesMusculature and Fascia: Station 1: The Anterior Abdominal WallAlia SahniNo ratings yet
- Spinal Anesthesia - Technique - UpToDateDocument37 pagesSpinal Anesthesia - Technique - UpToDateSamir Perez CasadiegoNo ratings yet
- Lecture - One: Anatomy of The Anterior Abdominal WallDocument25 pagesLecture - One: Anatomy of The Anterior Abdominal WallAhmed OudahNo ratings yet
- Anatomy Materials AbdomenDocument21 pagesAnatomy Materials AbdomenEmilee TuNo ratings yet
- Anatomy of The Abdomen and PelvisDocument20 pagesAnatomy of The Abdomen and PelvishanifsharNo ratings yet
- 263 Lumbar Plexus Block - Psoas Compartment BlockDocument9 pages263 Lumbar Plexus Block - Psoas Compartment Blockarif AjiNo ratings yet
- Analgesia For Iliac Crest Bone GraftDocument9 pagesAnalgesia For Iliac Crest Bone GraftDominik Chirito PastorNo ratings yet
- Anterior Abdominal Wall and Inguinal CanalDocument35 pagesAnterior Abdominal Wall and Inguinal Canalapi-3698357100% (3)
- Snell AbdomenDocument43 pagesSnell AbdomenBenNo ratings yet
- Abdomen: By: DR Tegene Gizaw (MD)Document202 pagesAbdomen: By: DR Tegene Gizaw (MD)abdishakurNo ratings yet
- L1 Anatomy of The Lungs, Pleural Cavities and Respiratory Muscles - L4 - Anatomy of The Chest Wall and DiaphragmDocument8 pagesL1 Anatomy of The Lungs, Pleural Cavities and Respiratory Muscles - L4 - Anatomy of The Chest Wall and DiaphragmAurora TamNo ratings yet
- Peretul AbdominalDocument9 pagesPeretul AbdominalBotond LukacsNo ratings yet
- Anterior Abdominal WallDocument22 pagesAnterior Abdominal WallBhavana VallakattiNo ratings yet
- Muscles of Anterior Abdominal WallDocument30 pagesMuscles of Anterior Abdominal WallShimmering MoonNo ratings yet
- Overview of AbdomenDocument27 pagesOverview of AbdomenEmmanuel NarayanNo ratings yet
- 10,11,12muscles, Function, and Nerve Supply Slides.Document50 pages10,11,12muscles, Function, and Nerve Supply Slides.hawazinNo ratings yet
- Peripheral Nerve BlocksDocument21 pagesPeripheral Nerve Blocksmarianela1988No ratings yet
- LG 3 (Abdominal Wall Muscles and Inguinal Canal)Document33 pagesLG 3 (Abdominal Wall Muscles and Inguinal Canal)allanNo ratings yet
- Ischiococcygeus MuscleDocument4 pagesIschiococcygeus MusclemcwnotesNo ratings yet
- Chapter 2 Maternal AnatomyDocument9 pagesChapter 2 Maternal AnatomyRem Alfelor100% (2)
- Abdomen and Abdominal WallDocument40 pagesAbdomen and Abdominal WallAlex ChagalaNo ratings yet
- Dr. Reynaldo V. Lopez Senior Lecturer Department of AnatomyDocument55 pagesDr. Reynaldo V. Lopez Senior Lecturer Department of AnatomyMohammad AliNo ratings yet
- AnatomyAbdomenandPelvisPosteriorAbdominalWallNerves StatPearls NCBIBookshelfDocument11 pagesAnatomyAbdomenandPelvisPosteriorAbdominalWallNerves StatPearls NCBIBookshelfKavya KavyasujathaNo ratings yet
- 3-Muscles Involved in Respiration-1Document24 pages3-Muscles Involved in Respiration-1MuskanNo ratings yet
- Muscles of The Thoracic Wall, Pectoral Region - 2023 - 1Document28 pagesMuscles of The Thoracic Wall, Pectoral Region - 2023 - 1202112360No ratings yet
- 10.1007@s40140 019 00333 0Document10 pages10.1007@s40140 019 00333 0TM AnNo ratings yet
- ,11,12 Muscles, Function, and Nerve Supply Slides.Document30 pages,11,12 Muscles, Function, and Nerve Supply Slides.hawazinNo ratings yet
- Repaso 1 Anatomy Andominal Wall 0 CavityDocument7 pagesRepaso 1 Anatomy Andominal Wall 0 CavityAngelitza AlmodóvarNo ratings yet
- Maternal AnatomyDocument14 pagesMaternal AnatomyRachel Lalaine Marie SialanaNo ratings yet
- Abdominal Muscles - AnatomyDocument35 pagesAbdominal Muscles - AnatomyDr. SUVA NATHNo ratings yet
- Diaphragm: Mr. Abdur Rehman BS-cardiology Kmu-IpmsDocument19 pagesDiaphragm: Mr. Abdur Rehman BS-cardiology Kmu-IpmsAbdurrehman SafiNo ratings yet
- Anatomy and Physiology of EpiduraDocument50 pagesAnatomy and Physiology of EpiduraParvathy R NairNo ratings yet
- Abdomin: Dr. Qandeel Hamidullah KhanDocument24 pagesAbdomin: Dr. Qandeel Hamidullah Khanقندیل محسودNo ratings yet
- Anatomy of The AbdomenDocument107 pagesAnatomy of The AbdomenmichaelhossianNo ratings yet
- General Zoology Muscular System of The Frog - NotesDocument15 pagesGeneral Zoology Muscular System of The Frog - NotesMarian CordanoNo ratings yet
- Abdominal Stab Wound Case StudyDocument36 pagesAbdominal Stab Wound Case StudyMean Elepaño80% (5)
- Abdominal WallDocument17 pagesAbdominal WallSema KurdNo ratings yet
- 6.3 Peritoneum Abdominal Viscera f2f s1b2Document18 pages6.3 Peritoneum Abdominal Viscera f2f s1b2shlokNo ratings yet
- Musl of CHESTDocument4 pagesMusl of CHESTVrushab ManojNo ratings yet
- Abdominal Wall - HoDocument71 pagesAbdominal Wall - HoMekuriya BeregaNo ratings yet
- Anatomy, Lecture 4, Thoracic Wall (2) (Slides)Document23 pagesAnatomy, Lecture 4, Thoracic Wall (2) (Slides)Ali Al-QudsiNo ratings yet
- Chapter 2 Maternal AnatomyDocument9 pagesChapter 2 Maternal AnatomyRem AlfelorNo ratings yet
- Lecture 1 Abdominal Walls MainDocument52 pagesLecture 1 Abdominal Walls MainBarkinismNo ratings yet
- AnatomyDocument14 pagesAnatomyMaliha SiddiquiNo ratings yet
- IntJHealthAlliedSci24225-5153688 141856Document5 pagesIntJHealthAlliedSci24225-5153688 141856Ramesh lal ShahNo ratings yet
- Hyponatraemia: Dr. Peter Allan Dr. Saibal GangulyDocument8 pagesHyponatraemia: Dr. Peter Allan Dr. Saibal Gangulynur khadijahNo ratings yet
- 275 Wrist Block - Landmark TechniqueDocument10 pages275 Wrist Block - Landmark TechniqueEllappa GhanthanNo ratings yet
- Hemchandra Bhatt - 210209 - 095108Document1 pageHemchandra Bhatt - 210209 - 095108Ramesh lal ShahNo ratings yet
- 70 Neonatal Anaesthesia 2 Anaesthesia For Neonates With Abdominal Wall DefectsDocument10 pages70 Neonatal Anaesthesia 2 Anaesthesia For Neonates With Abdominal Wall DefectsParvathy R NairNo ratings yet
- Practical Guide For The Intensive Care Management of COVID ATOTWDocument15 pagesPractical Guide For The Intensive Care Management of COVID ATOTWRamesh lal ShahNo ratings yet
- Aditya Kumar Chauhan, Hem Chandra Bhatt, Shailesh Kumar LohaniDocument6 pagesAditya Kumar Chauhan, Hem Chandra Bhatt, Shailesh Kumar LohaniRamesh lal ShahNo ratings yet
- Upload 8Document2 pagesUpload 8cingyaNo ratings yet
- Form1a Medical FitnessDocument2 pagesForm1a Medical FitnessAnkur RastogiNo ratings yet
- The Vedas and Upanishads For Children, Roopa Pai 2019 PDFDocument367 pagesThe Vedas and Upanishads For Children, Roopa Pai 2019 PDFSachin Kangralkar100% (3)
- 399 ImagesDocument11 pages399 ImageskhalidNo ratings yet
- HTET of Sanskrit by Shivkumar ShastriDocument20 pagesHTET of Sanskrit by Shivkumar ShastriMuditNo ratings yet
- Perioperative Management of Suspected/ Confirmed Cases of COVID-19Document13 pagesPerioperative Management of Suspected/ Confirmed Cases of COVID-19Dimensi FKUNHASNo ratings yet
- Cocaine Toxicity in The Intensive Care UnitDocument6 pagesCocaine Toxicity in The Intensive Care UnitRamesh lal ShahNo ratings yet
- Perioperative Management of Infants and Children With DiabetesDocument10 pagesPerioperative Management of Infants and Children With DiabetesRamesh lal ShahNo ratings yet
- AStudyofProlongedFasting 10266160Document427 pagesAStudyofProlongedFasting 10266160Ramesh lal ShahNo ratings yet
- Diabetes Reversal by Plant Based Diet Dr. BiswaroopDocument7 pagesDiabetes Reversal by Plant Based Diet Dr. Biswaroopsatya_vanapalli3422100% (1)
- Toxic Threats in Our Food That Trigger Autoimmune Disease How To Reverse The EffectsDocument41 pagesToxic Threats in Our Food That Trigger Autoimmune Disease How To Reverse The Effectssiesmann100% (1)
- COVID1981 Ebook PDFDocument105 pagesCOVID1981 Ebook PDFMexico English100% (2)
- Your Medicine Your-DiabetesDocument3 pagesYour Medicine Your-Diabetespawan bindNo ratings yet
- The Insider's Ultimate Guide To: Banishing Back Pain For GoodDocument11 pagesThe Insider's Ultimate Guide To: Banishing Back Pain For GoodRamesh lal ShahNo ratings yet
- Severe Vitamin B12 Deficiency in An Exclusively Breastfed 5-Month-Old Italian Infant Born To A Mother Receiving Multivitamin Supplementation During PregnancyDocument5 pagesSevere Vitamin B12 Deficiency in An Exclusively Breastfed 5-Month-Old Italian Infant Born To A Mother Receiving Multivitamin Supplementation During PregnancyRamesh lal ShahNo ratings yet
- Clinical Pain Management Cancer PainDocument464 pagesClinical Pain Management Cancer PainSantiago Herrera100% (1)
- COVID-19 Vaccine Efficacy and Effectiveness-The Elephant Not in The RoomDocument2 pagesCOVID-19 Vaccine Efficacy and Effectiveness-The Elephant Not in The RoomMarcusNo ratings yet
- A& P NotesDocument178 pagesA& P NotesJSeashark100% (3)
- Tanarajan Orthopaedic McqsDocument245 pagesTanarajan Orthopaedic McqsIgin GintingNo ratings yet
- Pulse Points Nursing Assessment PDFDocument8 pagesPulse Points Nursing Assessment PDFERANo ratings yet
- 03.05 Module Three Wellness PlanDocument8 pages03.05 Module Three Wellness Plandavisao68100% (1)
- Fetal Skull and Maternal PelvisDocument28 pagesFetal Skull and Maternal PelvisAshwanee Jharia0% (1)
- Subclavian ArteryDocument8 pagesSubclavian ArteryPatalie HettihewaNo ratings yet
- Os Coxae: Pelvic Limb A. Os Coxae B. Femur C. D. Tarsals E. FDocument4 pagesOs Coxae: Pelvic Limb A. Os Coxae B. Femur C. D. Tarsals E. FFor AstroNo ratings yet
- Bone AnatomyDocument11 pagesBone AnatomyLiam Jacque LapuzNo ratings yet
- Orthopedic Study Guide 2018Document9 pagesOrthopedic Study Guide 2018Alif AllahNo ratings yet
- Lumbar Disc HerniationDocument4 pagesLumbar Disc HerniationChester NicoleNo ratings yet
- F Muscular System MDocument32 pagesF Muscular System MFitzgerald PachecoNo ratings yet
- Clinical Orthopaedic RehabilitationDocument3 pagesClinical Orthopaedic RehabilitationJeevan VelanNo ratings yet
- Computer Assisted Orthopaedic Surgery For Hip and Knee 2018 Sugano PDFDocument202 pagesComputer Assisted Orthopaedic Surgery For Hip and Knee 2018 Sugano PDFValdete FigueiredoNo ratings yet
- One System - A Wealth of Options: Instrument System For Arthroscopic Cruciate Ligament SurgeryDocument16 pagesOne System - A Wealth of Options: Instrument System For Arthroscopic Cruciate Ligament Surgeryعايد التعزيNo ratings yet
- Lumbal Spine 9 OPA Export PDFDocument10 pagesLumbal Spine 9 OPA Export PDFHijrana PutriNo ratings yet
- FIFA Soccer 11 Plus ManualDocument76 pagesFIFA Soccer 11 Plus ManualtheroguetrainerNo ratings yet
- Acl InjuriesDocument2 pagesAcl InjuriesFrnz RiveraNo ratings yet
- Fracture ManagementDocument21 pagesFracture ManagementPatrickk WandererNo ratings yet
- Infraspinatus Muscle AtrophyDocument4 pagesInfraspinatus Muscle AtrophysudersonNo ratings yet
- Developmental MilestonesDocument13 pagesDevelopmental Milestonesaalocha_25100% (1)
- Radiological Assessment of Lower Limb Alignment: Instructional Lecture: KneeDocument8 pagesRadiological Assessment of Lower Limb Alignment: Instructional Lecture: KneeChristopher Freddy Bermeo RiveraNo ratings yet
- Nerve Damage Part 1bDocument19 pagesNerve Damage Part 1bAntonio CandelarioNo ratings yet
- Pelvic Floor Muscle & The Perineal BobyDocument28 pagesPelvic Floor Muscle & The Perineal BobysanthiyasandyNo ratings yet
- A Paediatric Musculoskeletal Competence FrameworkDocument18 pagesA Paediatric Musculoskeletal Competence FrameworkPT Depart AMCHNo ratings yet
- Shoulder JointDocument37 pagesShoulder JointsandeepNo ratings yet
- New Roods ApprochDocument50 pagesNew Roods ApprochMonicca GV100% (1)
- Football Injury: Literature: A ReviewDocument11 pagesFootball Injury: Literature: A Reviewaldo123456789No ratings yet
- Muscle Specialization Guide PDFDocument104 pagesMuscle Specialization Guide PDFKanwal Preet Singh100% (2)
- Fundamentals of Nursing PracticeDocument6 pagesFundamentals of Nursing PracticeHanna BuadaNo ratings yet
- Tennis Elbow (Lateral Epicondylitis) - OrthoInfo - AAOSDocument8 pagesTennis Elbow (Lateral Epicondylitis) - OrthoInfo - AAOSnoony 98No ratings yet