Professional Documents
Culture Documents
Endogenous Endophthalmitis Successfully Treated With Intravitreal Povidone-Iodine Injection: A Case Report
Uploaded by
kasandraharahapOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Endogenous Endophthalmitis Successfully Treated With Intravitreal Povidone-Iodine Injection: A Case Report
Uploaded by
kasandraharahapCopyright:
Available Formats
Tanaka et al.
BMC Ophthalmology (2020) 20:217
https://doi.org/10.1186/s12886-020-01487-w
CASE REPORT Open Access
Endogenous Endophthalmitis successfully
treated with Intravitreal Povidone-iodine
injection: a case report
Hiroki Tanaka1,2, Hiroyuki Nakashizuka2,3* , Yoshinobu Mizuno2,4 and Takayuki Hattori2,3
Abstract
Background: The usefulness of povidone-iodine as an alternative to antimicrobial agents, for endophthalmitis, has
recently been documented. We report a case of endogenous endophthalmitis successfully treated with intravitreal
injection of povidone-iodine.
Case presentation: An 88-year-old woman underwent small bowel bypass surgery for postoperative ileus
following rectal cancer resection. She developed a fever during total parenteral nutrition and was diagnosed with
gram-positive cocci bacteremia of central venous catheter origin. The patient was referred to our department with
chief complaints of ocular pain, hyperemia and decreased vision in the right eye, which had manifested during the
febrile period. The initial examination revealed the visual acuity in her right eye to be finger counting and that in
her left eye 0.2. The right eye showed a severe inflammatory reaction in the anterior chamber, fibrin deposition,
and hypopyon. The fundus was difficult to visualize. Endogenous endophthalmitis due to bacteria was diagnosed.
Surgical treatment was judged to be difficult based on the patient’s poor general condition and mental status, and
intravitreal injection of 0.1 ml of 1.25% povidone-iodine was performed on the same day. The inflammation rapidly
diminished, and the hypopyon had disappeared 4 days after treatment. The fundus became visible 7 days after
treatment and there was no recurrence of endophthalmitis findings. The visual acuity in her right eye recovered to
that in the left eye (0.2).
Conclusion: Intravitreal injection of povidone-iodine is potentially useful and effective as an alternative treatment
of antibiotics for endogenous endophthalmitis patients, especially in whom surgical therapy is difficult.
Keywords: Endogenous endophthalmitis, Intravitreal injection, Povidone iodine
Background However, vitrectomy is not applicable to all patients, be-
Endogenous endophthalmitis is a severe eye infection cause some are in poor systemic condition. Therefore,
that can rapidly lead to irreversible blindness. In cases intravitreal antimicrobial therapy has greater clinical sig-
with severe and sight-threatening endogenous endoph- nificance for endogenous endophthalmitis than for post-
thalmitis, vitrecomy is the preferred treatment strategy. operative endophthalmitis. Furthermore, there is a broad
range of causative organisms including both bacterial
and fungal species. Recently, multidrug-resistant bacteria
and vancomycin resistant bacteria have also been re-
* Correspondence: nkshizuk@gmail.com ported in endogenous endophthalmitis [1, 2]. In
2
Edogawa Hospital, Tokyo, Japan addition, vancomycin-associated hemorrhagic occulusive
3
Division of Ophthalmology, Department of Visual Sciences, Nihon University
Hospital, Nihon University School of Medicine, Tokyo, Japan
retinal vasculitis was reported following prophylactic use
Full list of author information is available at the end of the article of an intracameral injection for cataract surgery [3].
© The Author(s). 2020 Open Access This article is licensed under a Creative Commons Attribution 4.0 International License,
which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give
appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if
changes were made. The images or other third party material in this article are included in the article's Creative Commons
licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons
licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain
permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the
data made available in this article, unless otherwise stated in a credit line to the data.
Tanaka et al. BMC Ophthalmology (2020) 20:217 Page 2 of 4
Therefore, we need to develop antimicrobial agents that to poor visibility caused by vitreous opacity. As gram
have broad-spectrum anti-bactericidal and anti-fungal positive cocci were detected by blood culture, the en-
actions even against multidrug-resistant bacteria. dogenous endophthalmitis was attributed to these bac-
The usefulness of povidone-iodine (PI) as an alterna- teria. However, not only surgical treatment but also
tive to antibiotics for the treatment of endophthalmitis repeated intravitreal injections and even a vitreous tap
has been experimentally investigated, and the intravitreal were judged to be difficult based on her poor general
concentrations of PI, safe for ocular tissues and effective condition and mental status, including dementia. Fur-
for treating endophthalmitis, have been calculated to thermore, the details of the gram-positive cocci detected
range from 0.013 to 0.027% [4, 5]. Furthermore, the use- from blood culture and the antibiotic sensitivities were
fulness of vitrectomy for endophthalmitis employing still being examined at the time. Thus, after written in-
0.025% PI irrigation [6] and that of 1.25% PI/0.1 ml in- formed consent had been obtained from her daughter,
travitreal injection (IVI) as the initial treatment for en- we selected IVI of 1.25% / 0.1 ml PI, which has broad-
dophthalmitis have also been reported [7]. spectrum efficacy including against antibiotic-resistant
We herein present a case of endogenous endophthal- bacteria, instead of IVI of antibiotics. This treatment was
mitis successfully treated with IVI of PI. performed by one of the authors (H.N.). Adjustment of
1.25% / 0.1 ml for IVI of PI was conducted as follows;
Case presentation 0.1 ml of 10% PI, which is an undiluted solution, and 0.7
An 88-year-old female underwent small bowel bypass ml of saline solution are mixed and diluted, and 0.1 ml is
surgery for postoperative ileus following rectal cancer re- then injected into the vitreous (Fig. 2). This treatment
section and was receiving care in the surgical depart- was approved by the Ethics Committee of Nihon Univer-
ment of Edogawa Hospital. Postoperatively, the patient sity Hospital. Levofloxacin 6 times daily, tropicamide 3
developed a fever of unknown origin and was diagnosed times daily and atropine 1 time daily were also instilled,
with bacteremia associated with a central venous cath- and the antibacterial venous infusion was changed to ce-
eter. After catheter removal, cefmetazole sodium 1 g/day fepime hydrochloride 1 g daily after the gram-positive
was started. cocci were revealed to be Staphylococcus aureus and the
She had conjunctival hyperemia and decreased visual antibiotic sensitivities were determined.
acuity in the right eye during the febrile period, and she Two days after the IVI, the hypopyon was diminished
was thus referred to the ophthalmology department on and her ocular pain resolved. Then, 4 days after the IVI,
August 10th, 2017. The initial examination showed vis- the inflammation in the anterior chamber showed rapid
ual acuity in the right eye to be finger counting, that in resolution and the hypopyon had disappeared com-
the left eye 0.2. Slit-lamp examination revealed conjunc- pletely. The fundus was visible 7 days after the IVI
tival hyperemia in the right eye, as well as a marked in- (Fig. 3). The patient showed gradual recovery of her gen-
flammatory reaction in the anterior chamber with eral condition, and there was no recurrence of endoph-
hypopyon (Fig. 1). Moderate cataract was also noted, but thalmitis findings, such that she was discharged from
the ocular fundus could not be visualized in detail due our hospital 11 days after the IVI.
One month after the IVI, the inflammatory findings
had completely disappeared, and the visual acuity of the
right eye (0.2) was the same as that of the left eye (Fig. 4).
This condition was maintained for 4 months after treat-
ment. She discontinued visiting our hospital thereafter
due to deterioration of her systemic condition.
Discussion and conclusions
The effects of IVI of PI on experimental endophthalmitis
were reported by Kim et al. [8]. Four groups of rabbits
treated with 0.1% / 0.1 ml and 0.3% / 0.1 ml PI once or
three times every second day were compared for en-
dophthalmitis caused by Staphylococcus epidermidis.
Fourteen days later, 40% of the single dose group receiv-
ing 0.1% showed positive cultures and 30% of the single
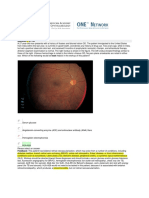
Fig. 1 Anterior segment photograph obtained at the first visit. dose group receiving 0.3% showed positive cultures, in
Conjunctival hyperemia and marked inflammation and hypopyon in other words 60 and 70% of cases treated with IVI of 0.1
the anterior chamber (arrow) were noted on the first examination.
and 0.3% PI, respectively, were culture negative even
This patient also has arcus senilis on the peripheral cornea
with injection of a single dose, whereas all cases treated
Tanaka et al. BMC Ophthalmology (2020) 20:217 Page 3 of 4
Fig. 2 Adjustment of 1.25%/0.1 ml for IVI of PI. A. 0.1 ml of 10% PI (arrowhead), an undiluted solution, and 0.7 ml of saline solution (arrow) are
prepared. B. These are mixed and diluted to achieve a concentration of 1.25%. C. 1.25% / 0.1 ml of PI is then injected into the vitreous
three times every second day showed culture negativity our study was higher, and it is likely that high efficacy
in both the 0.1% and the 0.3% group. Assuming the vit- was thus obtained by a single administration. If endoph-
reous volume of the rabbit eye to be 1.5 ml, the intravit- thalmitis is unresponsive to the initial treatment, re-
real PI concentrations were estimated to be 0.0067 and peated administrations of 1.25% / 0.1 ml PI, possibly as
0.02% at 0.1% / 0.1 ml and 0.3% / 0.1 ml, respectively. many as three times every second day, might achieve
The PI half-life was 3.3–3.6 h, and no retinal damage efficacy.
was detected by electroretinograms (ERGs) in any of the Adjusting 1.25%/0.1 ml for IVI of PI is simple and ra-
groups indicating PI three times every second day to be ther easily achieved as compared with IVI of an anti-
effective and safe for treating endophthalmitis. microbial agent. Furthermore, PI use has advantages
In our present patient, a single IVI at a dose of 1.25%/ including cost-effectiveness, that it can easily be ob-
0.1 ml PI was curative. Assuming the vitreous volume to tained almost anywhere, and has broad-spectrum effi-
be 5 ml, the intravitreal concentration of PI would be cacy against resistant bacteria. Furthermore, it is said
0.025%, and this concentration has been confirmed to be that vancomycin exerts a bacteriostatic effect after injec-
safe for ocular tissues in previous experimental studies, tion, though 8 h are needed for the bactericidal action to
with no abnormalities having been observed on ERGs or fully manifest [9], while PI requires only 15 s at low con-
by histopathological examination [5]. Compared to the centrations to kill infection-causing bacteria [10].
vitreous PI concentrations of 0.0067 and 0.02% reported
by Kim et al. [8], the concentration of 0.025% used in
Fig. 4 Anterior segment photograph obtained 1 month after IVI. The
Fig. 3 Anterior segment photograph obtained 7 days after IVI. The inflammation in the anterior chamber has completely disappeared
inflammation in the anterior chamber rapidly diminished, resulting and the right eye visual acuity has improved to 0.2, the same as that
in improved transparency of the ocular fundus of the left eye.
Tanaka et al. BMC Ophthalmology (2020) 20:217 Page 4 of 4
In our previous clinical study, 1.25% / 0.1 ml for IVI of Ethics approval and consent to participate
PI was used as the primary treatment for endophthalmi- This study complied with the tenets of the Declaration of Helsinki. The
procedure and possible risks associated with the treatment administered to
tis and was followed by vitrectomy using 0.025% PI Bal- this patient were explained and written informed consent for participation
anced Salt Solution Plus. No adverse events were was obtained according to the policy of the Ethics Review Board of Nihon
detected on ERGs, by Goldmann perimetry, or on exam- University hospital.
ination of corneal endothelial cells [7]. Consent for publication
There are endogenous endophthalmitis cases not eli- We obtained written consent from the patient’s daughter to publish this
gible for operative medical treatment due to poor gen- report. A copy of the written consent is available for review by the journal
Editor.
eral condition. In these cases, IVI of antibiotics should
be selected as the main treatment as well as systemic Competing interests
antibiotic therapy. However, sampling the vitreous might The authors have no competing interests to declare.
be difficult and, even if a sample could be obtained, sev- Author details
eral days would be needed to obtain the details of the 1
Nishikasai Inouye Eye Hospital, Tokyo, Japan. 2Edogawa Hospital, Tokyo,
bacteria detected and to confirm antibiotic sensitivities. Japan. 3Division of Ophthalmology, Department of Visual Sciences, Nihon
University Hospital, Nihon University School of Medicine, Tokyo, Japan.
Furthermore, endogenous endophthalmitis caused by 4
Department of Ophthalmology, Teikyo University School of Medicine, Tokyo,
vancomycin resistant bacteria has also been reported Japan.
[1, 2]. Thus, we consider IVI of 1.25% / 0.1 ml PI to be a
Received: 31 March 2020 Accepted: 27 May 2020
potential treatment option, to be administered in se-
lected cases, instead of IVI of antibiotics.
Our present patient’s general condition was quite References
1. Das T, Deshmukh HS, Mathai A, Reddy AK. Stenotrophomonas maltophilia
poor, such that we could not perform detailed examina- endogenous endophthalmitis: clinical presentation, sensitivity spectrum and
tions. Thus, only visual acuity, slit-lamp microscopy and management. J Med Microbiol. 2009;58(Pt 6):837–8. https://doi.org/10.1099/
fundus examination were performed. Another shortcom- jmm.0.009431-0.
2. Relhan N, Albini T, Pathengay A, Flynn HW. Bilateral endogenous
ing of this case report is that the quality of the anterior endophthalmitis caused by vancomycin-resistant Staphylococcus
segment photographs is poor due to the patient’s facial epidermidis in a neonate. J Ophthalmic Inflamm Infect. 2015;5:11. https://
instability. Based on the aforementioned experimental doi.org/10.1186/s12348-015-0039-y.
3. Witkin AJ, Shah AR, Engstrom RE, Kron-Gray MM, Baumal CR, Johnson MW,
reports and our previous clinical study results [7], the Witkin DI, Leung J, Albini TA, Moshfeghi AA, Batlle IR, Sobrin L, Eliott D.
vitreous concentration of PI used in this case appears to Postoperative hemorrhagic occlusive retinal Vasculitis: expanding the clinical
be safe for ocular tissues including the retina. However, Spectrum and possible association with Vancomycin. Ophthalmology. 2015;
122(7):1438–51. https://doi.org/10.1016/j.ophtha.2015.03.016.
the possibility of endophthalmitis causing corneal and 4. Brozou CG, Karabatakis V, Giannousis M, Mandraveli K, Karkavelas G, Alexiou-
retinal weakening and unexpected complications cannot Daniel S. The efficacy of Intravitreal Povidone iodine application in
be ignored. Meticulous follow-up is thus essential. Be- experimental Staphylococcus epidermidis Endophthalmitis. Ophthalmic Res.
2009;41(4):181–5. https://doi.org/10.1159/000217721.
fore recommending this treatment strategy for endoph- 5. Trost LW, Kivilcim M, Peyman GA, Aydin E, Kazi AA. The effect of
thalmitis patients in general, we need to accumulate intravitreally injected povidone-iodine on Staphylococcus epidermidis in
more cases, with detailed examination findings such as rabbit eyes. J Ocul Pharmacol Ther. 2007;23(1):70–7. https://doi.org/10.1089/
jop.2006.0076.
those of corneal endothelial cells, ERG and perimetry. 6. Nakashizuka H, Shimada H, Hattori T, Noguchi T, Kokubo N, Yuzawa M.
This is the first report, to our knowledge, describing Vitrectomy using 0.025% povidone-iodine in balanced salt solution plus for
IVI of PI, administered without other treatments, as the treatment of postoperative endophthalmitis. Retina. 2015;35(6):1087–94.
https://doi.org/10.1097/IAE.0000000000000634.
achieving full resolution of endophthalmitis. 7. Nakashizuka H, Shimada H, Hattori T, Tanaka K, Kitagawa Y, Shinoda K.
Intravitreal Injection of 1.25% Povidone Iodine Followed by Vitrectomy
Abbreviations Using 0.025% Povidone Iodine Irrigation for Treating Endophthalmitis. Transl
PI: povidone-iodine; IVI: intravitreal injection; ERG: electroretinogram Vis Sci Technol. 2019;8(1):21. https://doi.org/10.1167/tvst.8.1.21.
8. Kim KH, Cao J, Yoo J-W, Yoon I-S, Jung JW, Lee JE, Byon IS. Intraocular
Acknowledgements pharmacokinetics of Povidone-iodine and its effects on experimental
Not applicable. Staphylococcus epidermidis Endophthalmitis. Invest Ophthalmol Vis Sci.
2015;56(11):6694–700. https://doi.org/10.1167/iovs.15-17739.
Authors’ contributions 9. Libre PE, Della-Latta P, Chin NX. Intracameral antibiotic agents for
HT first wrote the manuscript in Japanese and HN performed the literature endophthalmitis prophylaxis: a pharmacokinetic model. J Cataract Refract
review and was the major contributor to drafting and revising the Surg. 2003;29(9):1791–4.
manuscript in English. YM and TH helped to draft and revise the manuscript. 10. Berkelman RL, Holland BW, Anderson RL. Increased bactericidal activity of
The manuscript was professionally edited by a native speaker of English. All dilute preparations of povidone-iodine solutions. J Clin Microbiol. 1982;15(4):
authors have read and approved the final manuscript. 635–9.
Funding
No funding or grant support was used for the writing of this case report. Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in
Availability of data and materials published maps and institutional affiliations.
The datasets used and/or analyzed during the current study are available
from the corresponding author upon reasonable request.
You might also like
- 2020 Article 1487Document7 pages2020 Article 1487kasandraharahapNo ratings yet
- 1945892419851312Document10 pages1945892419851312kasandraharahapNo ratings yet
- Acta Anaesthesiologica Taiwanica: Obstructive Jaundice and Perioperative ManagementDocument8 pagesActa Anaesthesiologica Taiwanica: Obstructive Jaundice and Perioperative ManagementkasandraharahapNo ratings yet
- SinglaDocument25 pagesSinglakasandraharahapNo ratings yet
- Dewi MegawatiDocument15 pagesDewi MegawatikasandraharahapNo ratings yet
- Perspective: New England Journal MedicineDocument3 pagesPerspective: New England Journal MedicinekasandraharahapNo ratings yet
- Topical Propranolol Improves Epistaxis in PatientsDocument4 pagesTopical Propranolol Improves Epistaxis in PatientskasandraharahapNo ratings yet
- J Ijporl 2018 01 022Document5 pagesJ Ijporl 2018 01 022kasandraharahapNo ratings yet
- DeteksionDocument9 pagesDeteksionkasandraharahapNo ratings yet
- BN2016 4938154Document6 pagesBN2016 4938154kasandraharahapNo ratings yet
- The Chemical Constituents and Pharmacological Effects of Bryophyllum Calycinum. A ReviewDocument6 pagesThe Chemical Constituents and Pharmacological Effects of Bryophyllum Calycinum. A ReviewkasandraharahapNo ratings yet
- NIH Public Access: Propionibacterium AcnesDocument15 pagesNIH Public Access: Propionibacterium AcneskasandraharahapNo ratings yet
- HHS Public Access: Association of Antipsychotic Use With Mortality Risk in Patients With Parkinson DiseaseDocument17 pagesHHS Public Access: Association of Antipsychotic Use With Mortality Risk in Patients With Parkinson DiseasekasandraharahapNo ratings yet
- HHS Public Access: Prevalence of and Indications For Antipsychotic Use in Parkinson DiseaseDocument8 pagesHHS Public Access: Prevalence of and Indications For Antipsychotic Use in Parkinson DiseasekasandraharahapNo ratings yet
- JurnalDocument8 pagesJurnalkasandraharahapNo ratings yet
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Jorge G Arroyo, MD, MPH Jonathan Trobe, MD Howard Libman, MD Contributor Disclosures Peer Review ProcessDocument13 pagesJorge G Arroyo, MD, MPH Jonathan Trobe, MD Howard Libman, MD Contributor Disclosures Peer Review ProcessLis Borda MuñozNo ratings yet
- BRVO PPT by Dr. Chinmay KharadeDocument31 pagesBRVO PPT by Dr. Chinmay KharadeChinmay KharadeNo ratings yet
- Service Manual - 12 - 2016 - Rev F Bousch LombDocument521 pagesService Manual - 12 - 2016 - Rev F Bousch LombcadburyberyNo ratings yet
- Agujero MacularDocument39 pagesAgujero MacularKate CastañoNo ratings yet
- NCM 0114 Module 3 - Nursing Care Management of The Older Person With Chronic IllnessDocument84 pagesNCM 0114 Module 3 - Nursing Care Management of The Older Person With Chronic IllnessKristine Kim100% (1)
- Retinal DetachmentDocument32 pagesRetinal Detachmentc/risaaq yuusuf ColoowNo ratings yet
- Vitrectomy Surgery For Primary Retinal DetachmentDocument8 pagesVitrectomy Surgery For Primary Retinal DetachmentAvluz AdiansuhNo ratings yet
- Case RRDDocument56 pagesCase RRDRana AhmedNo ratings yet
- MasonDocument208 pagesMasongdvfwqeguewguqfgNo ratings yet
- Endophthalmitis Harry Flynn MD OEDocument31 pagesEndophthalmitis Harry Flynn MD OEMsai AhyarNo ratings yet
- AAO Network UveitisDocument72 pagesAAO Network UveitisSafa Abdualrahaman Ali HamadNo ratings yet
- Bausch & Lomb PDFDocument4 pagesBausch & Lomb PDFAnonymous D8ay3BMJ5No ratings yet
- Disturbances in Visual PerceptionDocument25 pagesDisturbances in Visual PerceptionShamsa AfdalNo ratings yet
- Retinal Detachment SlideDocument54 pagesRetinal Detachment SlideHerin NataliaNo ratings yet
- Terson Syndrome: Don't Let It Go Unrecognized: Ophthalmic PearlsDocument2 pagesTerson Syndrome: Don't Let It Go Unrecognized: Ophthalmic PearlsSherley CruzNo ratings yet
- KMC Alos Rev23 Aug 2022Document2 pagesKMC Alos Rev23 Aug 2022dhimanbasu1975No ratings yet
- What Is An Epiretinal Membrane?Document6 pagesWhat Is An Epiretinal Membrane?Chip MorrisNo ratings yet
- OPTHA 2.1 RETINAL DISORDERS, CHOROID AND VITREOUS - Dr. MarinDocument9 pagesOPTHA 2.1 RETINAL DISORDERS, CHOROID AND VITREOUS - Dr. MarinPatricia ManaliliNo ratings yet
- Management of Retinal Detachment: A Guide For Non-OphthalmologistsDocument6 pagesManagement of Retinal Detachment: A Guide For Non-OphthalmologistsadriantiariNo ratings yet
- Retinal Detachment: Case Report Operating RoomDocument30 pagesRetinal Detachment: Case Report Operating RoomCarlo Joseph Intal LlacerNo ratings yet
- Retina: Product CatalogDocument60 pagesRetina: Product CatalogMohamed GamalNo ratings yet
- IMJ 10 133 enDocument4 pagesIMJ 10 133 encilmeli.irem.55No ratings yet
- DT - Normal Eyes With Sudden Painless Loss of VisionDocument34 pagesDT - Normal Eyes With Sudden Painless Loss of VisionIzzatul Yazidah100% (1)
- Advances in Vitreoretinal SurgeryDocument63 pagesAdvances in Vitreoretinal Surgerybharti100% (6)
- Referat Cystoid Macular Edema Periode 17 Juni - 20 Juli 2019Document25 pagesReferat Cystoid Macular Edema Periode 17 Juni - 20 Juli 2019CharlotteGraceNusiferaNo ratings yet
- ETDRSDocument60 pagesETDRSRohit Sanatkumar KundapNo ratings yet
- Asrs Common Retina CPT CodesDocument3 pagesAsrs Common Retina CPT Codesapi-405859281No ratings yet
- Ryan's Retina 6th EdDocument2,754 pagesRyan's Retina 6th EdGarsa Garnol100% (2)
- CH42 Management of Complicated Retinal DetachmentDocument36 pagesCH42 Management of Complicated Retinal DetachmentriveliNo ratings yet
- Management of Giant Retinal TearsDocument6 pagesManagement of Giant Retinal TearsAlejandro LondoñoNo ratings yet