Professional Documents
Culture Documents
Astigmatic Change in Manual Small Incision Cataract Surgery (MSICS) With Chevron Type of Incision
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Astigmatic Change in Manual Small Incision Cataract Surgery (MSICS) With Chevron Type of Incision
Copyright:
Available Formats
Volume 7, Issue 4, April – 2022 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
Astigmatic Change in Manual Small Incision Cataract
Surgery (MSICS) with Chevron Type of Incision
Dr.Sujit Kumar Biswas, Dr. Quamrul Islam, Dr. Rajib Husain, Dr. Suborna Sultana, Dr. Nahid Anjum.
Dr. Sujit Kumar Biswas
MBBS, DCO, FCPS, FICO, MRCS (Glasgow), MRCS (Edinburgh).
Consultant
Chittagong Eye Infirmary and Training Complex,
Zakir Hossain Road, Chittagong, Bangladesh
Abstract:- induced astigmatism was significant, outcome of chevron
Aim: To evaluate the astigmatic change after Manual incision in term of final postoperative vision is excellent.
Small Incision Cataract Surgery with chevron type of Tunnel construction was somewhat difficult. We have to
incision. compare with other type of incision to assess the efficacy
of Chevron incision.
Design: A prospective interventional study.
Keywords:- Chevron incision, manual small incision
Materials & Methods: A total 100 cases were selected cataract surgery (MSICS), with the rule astigmatism (WTR),
who underwent manual small incision cataract surgery against the rue astigmatism (ATR).
with chevron incision for that one year period
irrespective of gender. This study was done in cataract I. INTRODUCTION
clinic at Chittagong Eye Infirmary and Training
Complex. Related all pre- and postoperative data were Modern cataract surgery aims to achieve a better
recorded according to the protocol of the hospital. All unaided visual acuity with rapid post surgical recovery,
surgeries were done under peribulbar anesthesia. A “V” minimal surgery related complications and less surgically
shaped chevron partial thickness sclera incision was induced astigmatism. Postoperative astigmatism plays an
done on the superior quadrant of every patient by a important role in the evaluation of final outcome of
keratome. Pocket tunnel is dissected with a crescent surgery.1 The basis of manual small incision cataract surgery
knife. All other steps of were done like standard small are the tunnel construction, the location of the wound on the
incision cataract surgery. All intraocular lenses (IOLs) sclera with respect to the limbus and the shape of the
were implanted in capsular bag. Post operatively wound.2,3,4 Geometric shape of the external incision affects
patients were treated with topical corticosteroid six times surgically induced astigmatism significantly.5 There are
daily approximately four weeks then tapered, topical different types of incision for tunnel construction such as
antibiotic four times daily for one week and topical smile, straight, frown, Blumenthal side cuts and chevron
cycloplegic once daily for two weeks. All patients were incision3. Chevron incision involves giving a “inverted V”
followed up on 1st postoperative day, 7th postoperative shaped incision with an angle of approximately 120 degree
day and after one month. (100-120 degree) between the two arms and the apex about
1.5 mm from the limbus 2-5 [Fig1-7]. In literature review, 5 it
Results: Mean ages of these patients were 59.66 ± 10.81 has been found that a chevron incision is best amongst all
years (ranged 30-70 years). Here we found that Chevron the incisions for Manual Small Incision Cataract Surgery
Incision is relatively more stable in ATR astigmatism (MICS). The main advantage of chevron incision is that it is
group than WTR astigmatism (63.04% and 72.71% very stable and gives excellent reduction in surgically
respectively). But in NO astigmatism group it gives induced astigmatism over other incision even in hard brown
opposite results, that that was changed to WTR cataract.5 In the present study, we were trying to find out the
astigmatism more than ATR astigmatism (60% and 40% astigmatic change, outcome and complication of Manual
respectively). A significant change occurred between Small Incision Cataract Surgery (MSICS) with Chevron
pre- and post-operative astigmatism in different groups type of incision.
(p-0.001). Sixty nine percent (69%) gain Complete
success i.e, incision induced astigmatism was up to 0.50 II. MATERIAL AND METHODS
D, 27% were in Qualified success and only 4% were
failed. Post operative final visual outcome of this study This prospective study was done at Chittagong Eye
Infirmary and Training Complex (CEITC), from 01.11.2013
group is excellent, 98% achieved BCVS equal or better
to 31.10.2014 (1 year). A total 100 cases were selected for
than 6/18. No patient showed significant post operative
complication. Tunnel construction was the most difficult surgery. All surgeries were done by the one qualified
step in this type of incision through the sclera. ophthalmologists of the cataract clinic of CEITC. Inclusion
criteria were senile age related cataract with ‘with the rule
Conclusion: This prospective study showed chevron astigmatism’, ‘against the rule astigmatism’, and ‘no
incision causes a significant change in astigmatism astigmatism’. Complicated cataract, traumatic cataract,
postoperatively. Although magnitude of surgically secondary cataract, hypermature cataract with phacodonesis,
IJISRT22APR961 www.ijisrt.com 794
Volume 7, Issue 4, April – 2022 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
subluxated lens, cataract with corneal opacities, cataract
with abnormal pupil, posterior segment disease like vitreous
opacity, macular diseases, optic nerve diseases, glaucoma or
any other retinopathy causing functional impairment of
vision were excluded from this study. Related all pre- and
postoperative data were recorded according to the protocol
of the hospital.
Every patient surgery was done under peribulbar
anesthesia. An inverted “V” shaped Chevron partial Fig. 2: Straight incision3
thickness sclera incision was done on the superior quadrant
of every patient by a keratome, the apex which lies one
millimeter from the limbus. . The pocket tunnel was
dissected with a metal crescent disposable knife. All other
steps of were done like standard small incision cataract
surgery. All intraocular lens (IOL) were implanted in
capsular bag. Post operatively patients were treated with
topical corticosteroid six times daily approximately four
weeks then tapered, topical antibiotic four times daily for
one week and topical cycloplegic once daily for two weeks.
Doses and duration of topical corticosteroid was increased Fig. 3: Frown incision3
according to postoperative inflammation. All patients were
followed up on 1st postoperative day, 7th postoperative day
and after one month.
Visual acuity was assessed using Snellen’s charts in
each follow up and the need for further surgical procedures
assessed. Refraction and keratometry was done at final
follow-up to detect post operative astigmatism. Any
complication or any intervention during operation was also
Fig. 4: Blumenthal side cuts3
noted.
Post-operative astigmatism was expressed as the power
of the cylinder lens needed for best correction. All
cylindrical lens power pre-and postoperatively was
converted into minus and categorized as "acceptable
astigmatism” (0 to ≤ 0.50 DCyl), "moderate astigmatism" (>
0.50 to ≤ 1.50 DCyl) and "large astigmatism" (>1.50 DCyl).
Although there are no clear definitions for acceptable,
moderate and large astigmatism in the literature, but in this
Fig. 5: Chevron ‘V’ incision3
study, acceptable astigmatism will be defined as 0 to 0.50
DCyl, assuming that this range would not hamper the
patient's vision.5
Internationally accepted post-operative corneal
astigmatism is 0.50D 5,11. So, complete success was defined
as post operatively astigmatic change 0 diopter to - 0.50
diopters cylinder; qualified success as an astigmatic
changes - 0.50 to - 1.50 diopters cylinder and failure as an
astigmatic changes more than - 1.50 diopters cylinder
Fig. 6: Postoperative view of operated eye before
Statistical analysis relevant data were done by using conjunctival apposition with Chevron incision.
SPSS16 software. A statistically significant difference was
being assumed for ‘p’- values lower than 0.05.
Fig. 7: Postoperative view of operated eye after conjunctival
apposition with Chevron incision.
Fig. 1: Smile incision3
IJISRT22APR961 www.ijisrt.com 795
Volume 7, Issue 4, April – 2022 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
III. RESULTS hypertension and rest 42% (n-42) patients have hypertension
associated with other systemic diseases.
Mean ages of these patients were 59.66 ± 10.81 years
(ranged 30-70 years). The most of the patients belonged to In the study group preoperative WTR astigmatism was
older age groups, particularly in 50-59 and 60-69 years. 46% (n-46), ATR was 44% (n-44) and NO was 10% (n-10),
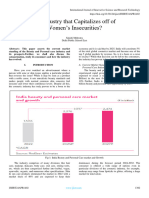
where as postoperative WTR astigmatism was 46% (n-46),
Fifty percent (n-50) patients were presented with ATR became 52% (n-52) that was increased and NO
different systemic diseases. Hypertension was the most reduced to 2% (n-2) [Fig 08].
common, found in 26% (n-26) of patients as only
Fig. 8: Comparison between pre- and postoperative astigmatism
Preoperative Post-operative Astigmatism
Astigmatism WTR ATR NO Total
n (%) n (%) n (%) n (%)
WTR 29.0 (63.04%) 16.0 (34.28%) 1.00 (2.17%) 46
ATR 11.0 (25.0%) 32.0 (72.71%) 1.00 (2.27%) 44
NO 6.0 (60.0%) 4.0 (40.0%) 0.00 (0.0%) 10
Total 46.0 (%) 52.0 (%) 2.0 (%) 100
(x2=14.31; Cramers’s V= 0.267; df= 4; sig; p=0.006 (p< 0.05)
Table 01 Distribution of Pre- and Post Operative Rule Astigmatism
Note: WTR- With the rule astigmatism, ATR- Against the rule astigmatism, NO- No astigmatism.
The differences among the pre- and post-operative that in each group postoperatively astigmatic change
astigmatic changes are statistically significant at < 0.05 level occurred significantly (p=0.006).
(x2=14.31; Cramers’s V= 0.267; df= 4; sig; p=0.006 (p<
0.05). Among the WTR astigmatism, 63% (n=29) of this The post-operative changes of astigmatism shows
group remains at the same group and about 34% (n=16) turn difference about the distribution of the pre-operative cases.
to ATR astigmatism and only 2% (n= 1) had diminished Among the 100 cases, 61 cases had acceptable astigmatism
astigmatism after surgery. About 44 cases of pre-operative (0 to ≤ 0.50 D), and postoperatively 42 cases (69%)
ATR astigmatism, post-operatively more than 72% (n=32) remained at same categorized group whereas 18 cases (29%)
was remain at the same group while only 25% (n=11) turned moved to the group of moderate (>0.50 to ≤1.50 D)
over to the group of WTR astigmatism and only 2% (n=1) astigmatism group and only 01 case (2%) moved to the
move in the group of no astigmatism. About 10% cases was group of large (>1.50D) astigmatism group. About 35 cases
present preoperatively at the group of “no astigmatism” and were in the group of moderate (>0.50 to ≤1.50 D)
dramatically all of them distributed between WTR astigmatism and in the post operative cases 60% (n=21)
astigmatism (60%, n=6) and ATR astigmatism (40%, n=4) remained at the same group while the other 29% (n=10) of
group in post-operative cases. [Table 01]. In this study it is cases jumped over to the group of acceptable (0 to ≤ 0.50 D)
observed that Chevron Incision is relatively more stable in astigmatism group and 11% (n=11) of cases moved to the
ATR astigmatism group than WTR astigmatism (72.71% vs group of large (>1.50 D) astigmatism. Moreover only 4 pre-
63.04%), that means Chevron incision causes flattening of operative cases of large (>1.50D) astigmatism, 25% (n=1)
vertical meridian more in ATR astigmatism group. remained at the same group whereas 50% (n=2) moved to
Conversely No astigmatism group changed into WTR the group of moderate (>0.50 to ≤1.50 D) astigmatism and
astigmatism relatively more than ATR astigmatism (60% vs 25% (n=1) moved to the group of acceptable (0 to ≤ 0.50 D)
40%), that means this incision causes steepening of vertical astigmatism [Table 02]. In this study, majority of the
meridian more in NO astigmatism group. So it is concluded patients of acceptable and moderate astigmatism group
IJISRT22APR961 www.ijisrt.com 796
Volume 7, Issue 4, April – 2022 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
remained in the same group post-operatively (68% and 60% moderate astigmatism group and remaining 25% into
respectively), whereas in large astigmatism group it was acceptable group.
25%. 50% of large astigmatism group changed into
Pre-operative Post-operative Astigmatism
Astigmatism (0- ≤ 0.50) D (>0.50 - ≤1.50)D >1.50 D Total
n (%) n (%) n (%) n
(0 to ≤ 0.50) D 42 (68.82%) 18 (29.50%) 01 (1.64%) 61
Acceptable astigmatism
(>0.50 to ≤1.50)D 10 (28.57%) 21 (60.0%) 04 (11.43%) 35
Moderate astigmatism
>1.50D 01 (25.0%) 02 (50.0%) 01 (25.0%) 04
Large astigmatism
TOTAL 53 (%) 41 (%) 6 (%) 100 (%)
Table 02 Distribution of Pre and Post Operative magnitude of Astigmatism.
In comparison between the acceptable, moderate and decreased and became 53%. Moreover, at the group of
large groups of astigmatism there are statistically significant “Moderate” group, the number increased from 35% to 41%
change observed between the pre-operative and post- and the increasing tendency was same for the “Large” where
operative status of the cases (p= 0.001). In the group of post-operative cases were increased from 4% to 6%. [Table
“Acceptable” astigmatism the pre-operative cases were 61% 03]. In this study it is clear that Chevron incision induce a
where as in the post-operative cases percentage was significance change in post-operative astigmatism.
Astigmatism Preoperative Postoperative
Diopter N % N % ‘p’- value
0 to ≤ 0.50 61 61% 53 53%
Acceptable astigmatism
0.001
> 0.50 to ≤ 1.50 35 35% 41 41% (<0.05)
Moderate astigmatism
> 150 4 4% 6 6%
Large astigmatism
TOTAL 100 100% 100 100%
Table 03 Comparison of pre- and post-operative astigmatic change
Pre-operative mean astigmatism was 0.478 ± 0.4647 Astigmatism Mean ± SD ‘p’ - value
and post-operative astigmatism was 0.587 ± 0.4788. After Pre-operative 0.478 ± 0.4647
statistical analysis of 2-tailed t- test, the change of Post-operative 0.587 ± 0.4788 0.028
astigmatism was significantly different between pre- and Table 4: Pre- and postoperative mean astigmatism
post-operative astigmatism. The change of astigmatism was
also significantly correlated (p= 0.000, Pearson correlation- In this study, majority of the patients (69%) gain
0.466) between the pre and post operative astigmatism of Complete success i,e. incision induced astigmatism was up
the patients. [Table 04] to 0.50 D, 27% were in Qualified success and only 4% were
failed. (Table 05)
Operational definition Induced Astigmatism Frequency Percentage
Complete success 0 to ≤ 0.50 D 69 69%
Qualified success > 0.50 to ≤ 1.50 D 27 27%
Failed > 150 D 04 04%
TOTAL 100 100%
Table 5: Incision induced post-operative astigmatism.
Final post operative visual outcome of this study group month post-operatively) 98% patients achieved BCVS equal
was excellent. Dramatic improvement of BCVS of Good or better than 6/18, 1% (n=1) achieved borderline BCVS
category and rapid reduction of Borderline category were due to post operative large astigmatism (-2.00 Dcyl ATR)
observed from first post –operative day to one month and another 1% (n=1) felt in poor outcome due to macular
follow-up (67% to 98% and 32% to 1% respectively) where scar. [Table 06].
as Poor category was same. At final follow up (after 1
IJISRT22APR961 www.ijisrt.com 797
Volume 7, Issue 4, April – 2022 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
VA (BCVS) 1st POD 7th POD 1month POD WHO standard
6/6 to 6/18 (Good) 67% 73% 98% >80%
6/24 to 6/60 (Borderline) 32% 26% 1% <15%
< 6/60 (Poor) 1% 1% 1% <5%
TOTAL 100% 100% 100% 100%
Table 6: Post operative visual acuity
Note: VA- Visual acuity, BCVS-Best corrected visual acuity.
No patient showed significant post operative making and maneuverability are difficult. The ideal distance
complication. Intra operatively premature entry occurred in is around 1–2 mm.3 Kimura et al. have shown that
3 patients and intra operatively suturing was done with 10-0 surgically induced astigmatism is less with an oblique
nylon suture and among them one patient developed incision (Frown and Chevron) than with a straight incision.8
hyphema and evacuation of blood clot done on the first
POD. These 3 patients were achieved good visual outcome The aim of the study was to assess the surgery induced
(6/9) finally. One patient had posterior capsular rent and post-operative astigmatism in patients undergoing MSICS
fortunately there was no vitreous loss and finally achieved with Chevron incision with rigid IOL implantation. Our
good visual outcome (6/9). Ninety six percent (96%) study included 100 patients adhering to the inclusion and
showed uneventful surgery. exclusion criteria who underwent MSICS with Chevron
incision with rigid IOL implantation by a same surgeon over
IV. DISCUSSION a span of one year. Study patients were divided into 3
groups WTR astigmatism, ATR astigmatism and NO
Cataract surgery has changed tremendously in recent astigmatism.
years mainly to fulfill the expectation of the patients that is
early visual rehabilitation and minimal induced astigmatism. The most of the patients belonged to older age groups,
Small incision manual cataract surgery is an effective particularly in 50-69 years age groups (68%). Mean age of
alternative to phacoemulsification in countries where very these patients were 59.66 ± 10.81 years. There is no
high volume surgery with inexpensive instrumentation is correlation between the pre-operative age or sex of cases in
required. Wound construction plays a major role in MSICS. study groups which will influence the final outcome of the
Reduction in the amount of surgery induced astigmatism are surgery with the type of incision used.
now obtainable with newer techniques in the wound
construction. In our study we try to find out the relationship between
the preoperative astigmatism and postoperative astigmatism
Different types of incision for tunnel construction in with Chevron type of incision and we also tried to analyze
Manual Small Incision Cataract Surgery (MSICS) are Smile, magnitude of induced astigmatism with this type of incision.
Straight, Frown, Blumenthal side cuts and Chevron
incision.6 Smile incision is easy to make, but results in In this study we found that in WTR and ATR
increased astigmatism Smile incision is a curvilinear astigmatism groups, a significant percentage of patients
incision which runs parallel to the limbus. With this (63.04% and 72.71% respectively) remain in the same group
incision, there is an increased chance of corneal flattening where as a least percentage (2.17% and 2.27% respectively)
after surgery in the vertical meridian with increased induced fall in the NO astigmatism group postoperatively. In this
astigmatism [Fig.01]. Straight incision as the name suggests, study it is observed that Chevron Incision is relatively more
is a straight line incision about 2 mm away from the limbus. stable in ATR astigmatism group than WTR astigmatism
This incision induces moderate flattening and consequently (72.71% vs 63.04%), that means Chevron incision in
moderate astigmatism after surgery [Fig.02]. Frown incision patients with ATR astigmatism causes flattening of vertical
is difficult to make for a beginner. The base of the curve is meridian in majority of cases (72.71%) and patients with
about 2 mm from the limbus. This induces minimal WTR astigmatism causes steepening of vertical meridian in
astigmatism [Fig.03]. Blumenthal side cuts involve straight majority of cases (63.04%). In NO astigmatism group 60%
incision with oblique cuts placed at its either ends. This patients convert to WTR astigmatism group and remaining
increases the space in the tunnel for an easy delivery of the 40% patients convert to ATR astigmatism group. This
nucleus [Fig.04]. Chevron ‘V’ incision involves giving an means Chevron incision causes steepening of vertical
“inverted V” shaped incision with an angle of approximately meridian more than horizontal meridian of NO astigmatism
120 degree between the two arms and the apex about 1.5 group. This gives a mixed result in different groups [Table
mm from the limbus. [Fig. 05] This incision is quite 01].
difficult to make. The tunnel size in this incision is relatively
smaller. This incision has least/nil induced astigmatism. 6 When we were comparing pre-and post-operative
astigmatism in “Acceptable”, “Moderate” and “Large” for
All these incisions induce less astigmatism if placed how much change occurred we got a p-value of 0.001 which
more posteriorly on the sclera.3 Burgansky et al. have is statistically significant [Table 03]. This means there is
shown an increase in astigmatism with an increase in the significant changes occurred between pre- and post-
incision size.7 More the distance from the limbus (on operative astigmatism in different groups. After statistical
sclera), less is the induced astigmatism although tunnel analysis (2-tailed t-test) between pre- and post-operative
IJISRT22APR961 www.ijisrt.com 798
Volume 7, Issue 4, April – 2022 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
mean astigmatism we got a p-value of 0.028 that is also REFERENCES
statistically significant. We have to compare with other type
of incision to assess the efficacy of Chevron incision. In one [1.] Raj swasthya. Small incision cataract surgery. Chapter:
comparative study between straight, frown and chevron 6 http://www.rajswasthya.nic.in cataract surgery with
incision among 100 patient by Nidhi et al showed mean IOL. Indian Journal of Ophthalmology. 2009 Jan-Feb;
surgery induced astigmatism (SIA) was minimum (- 57(1): 9–13.
0.88±0.61Dx900) with chevron incision.9 Another study by [2.] Pallin SL. Chevron incision for cataract surgery. J
Dhiraj et al on 100 patients in a comparison study between Cataract Refract Surg. 1990;16: 779–81.
chevron incision and frown incision of same size showed [3.] Haldipurkar SS, Gokhale VN. Astigmatic
chevron incision had more stable configuration in term of Considerations in SICS. J International Soc Manual
surgery induced astigmatism (SIA).10 Small Incision Cataract Surgeons. 2005 Nov 01; 46–8.
[4.] Ashok Garg. Jorge L. Alio. Surgical technique
Post operative visual outcome of this study group is ophthalmology- cataract surgery. Jaypee- highlight,
excellent. Dramatic improvement of best corrected visual Medical Publishers, Inc.2010; 38; 205-6.
acuity (BCVA) of Good category and rapid reduction of [5.] American Academy of Ophthalmology Basic and
Borderline category were observed from first post – Clinical Science Course. Section 3: Clinical Optics,
operative day to one month follow-up (67% to 98% and 2007-2008. San Francisco, CA. American Academy of
32% to 1% respectively) where as Poor category was same. Ophthalmology; 2007:117-118.
At final follow up (after 1 month post-operatively) 98% [6.] Basti S, Vasavada AR, Thomas R, Padhmanabhan P.
patients achieved BCVS equal or better than 6/18, 1% (n=1) Extra capsular cataract extraction: Surgical techniques.
achieved borderline BCVS due to post operative large Indian J Ophthalmology. 1993;41:195–210
astigmatism (-2.00 Dcyl ATR) and another 1% (n=1) fell in [7.] Burgansky Z, Isakov I, Avizemer H, Bartov E.
poor outcome due to macular scar (Table 3.11). Nidhi et al Minimal astigmatism after sutureless planned
also showed in her comparison study 95.70% patients of extracapsular cataract extraction. J Cataract Refract
chevron incision group achieved post operative best Surg. 2002;28: 499–503.
corrected visual acuity (BCVA) 6/18 or better.9 [8.] Kimura H, Kuroda S, Mizoguchi N, Terauchi H,
Matsumura M, Nagata M. Extracapsular cataract
No patient showed significant post operative extraction with a suture less incision for dense
complication. Tunnel construction was the most difficult cataracts. J Cataract Refract Surg. 1999; 25:1275–9.
step in this type of incision through the sclera. Three [9.] Nidhi Jauhari, Deepak Chopra, Rajan Kumar
premature entries occurred in 100 patients even by an Chaurasia, and Ashutosh Agarwal. Comparison of
experienced surgeon. It is quite difficult in beginner surgically induced astigmatism in various incisions in
surgeon. manual small incision cataract surgery. Int J
Ophthalmol. 2014; 7(6): 1001–1004.
V. CONCLUSION [10.] B.Dhiraj, Y. Sidhdharth. a randomized study to
evaluate SIA in patient of SICS operated by chevron
This comprehensive prospective study on the and frown incision. Journal of Forensic Medicine,
astigmatic changes in 100 cataract patients who underwent Science and Law - A Journal of Medicolegal
MSICS with Chevron incision with rigid PMMA IOL Association of Maharashtra. 2013; 22 (1).
implantation has helped us to arrive certain conclusions. [11.] Dieudonne Kaimbo, Wa Kaimbo. Astigmatism –
This prospective study showed Chevron incision causes Definition, Etiology, Classification, Diagnosis and
significant change in astigmatism postoperatively. Non-Surgical Treatment. Department of
Magnitude of surgically induced astigmatism (SIA) also Ophthalmology, University of Kinshasa, DR Congo.
significant. Outcome of Chevron incision in term of final
postoperative vision is excellent in this study. Although
tunnel construction is somewhat difficult, no devastating
complications have occurred in this study. We have to
compare with other type of incision to assess the efficacy of
Chevron incision.
Conflict of interest: None.
Financial support: None
Acknowledgement: Ms. Rahnoma Tarannom for
statistical analysis.
IJISRT22APR961 www.ijisrt.com 799
You might also like
- Practical Handbook for Small-Gauge Vitrectomy: A Step-By-Step Introduction to Surgical TechniquesFrom EverandPractical Handbook for Small-Gauge Vitrectomy: A Step-By-Step Introduction to Surgical TechniquesNo ratings yet
- Comparision of Surgical Induced Astigmatism BetweeDocument5 pagesComparision of Surgical Induced Astigmatism BetweeHoly DishNo ratings yet
- 1 - Siva CharanDocument5 pages1 - Siva CharanJugalKishor DhirNo ratings yet
- 297 1289 1 SMDocument7 pages297 1289 1 SMRaissaNo ratings yet
- Phacoemulsification Versus Manual Small Incision Cataract Surgery in Hard NuclearDocument6 pagesPhacoemulsification Versus Manual Small Incision Cataract Surgery in Hard NuclearRagni MishraNo ratings yet
- Bhargavaetal 17Document7 pagesBhargavaetal 17Flor ArenasNo ratings yet
- Telaah Jurnal Rhizky Shasqia Putri NurDocument23 pagesTelaah Jurnal Rhizky Shasqia Putri NurrhizkyNo ratings yet
- Femto Vs Phaco 2Document6 pagesFemto Vs Phaco 2Bonita AsyigahNo ratings yet
- Phacoemulsification Versus Small Incision Cataract Surgery in Patients With UveitisDocument6 pagesPhacoemulsification Versus Small Incision Cataract Surgery in Patients With UveitisYahya Iryianto ButarbutarNo ratings yet
- Jurnal New1Document5 pagesJurnal New1Nurul Qomariah TNo ratings yet
- 06 Small Incision Cataract SurgeryDocument21 pages06 Small Incision Cataract SurgeryApriliani SanitiNo ratings yet
- Rotational Stability of Toric Intraocular - 2022 - Medical Journal Armed ForcesDocument6 pagesRotational Stability of Toric Intraocular - 2022 - Medical Journal Armed ForcesAnisha RanaNo ratings yet
- Out 3Document7 pagesOut 3Oldi Nelson PatadunganNo ratings yet
- Mertens - The Staar Toric ICLDocument4 pagesMertens - The Staar Toric ICLAndreea L. MihalceaNo ratings yet
- Therapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismDocument7 pagesTherapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismStephanie PfengNo ratings yet
- Oftalmologi 2Document3 pagesOftalmologi 2Jericho JeruzalemNo ratings yet
- Ascrs 2Document7 pagesAscrs 2leokapilNo ratings yet
- Penetrating Keratoplasty vs. Epikeratoplasty For The Surgical Treatment of KeratoconusDocument9 pagesPenetrating Keratoplasty vs. Epikeratoplasty For The Surgical Treatment of KeratoconusAbhilash AntonyNo ratings yet
- Referat SMILEDocument10 pagesReferat SMILEarumNo ratings yet
- Advanced Ophthalmic Diagnostic Procedures and InbstrumentationDocument5 pagesAdvanced Ophthalmic Diagnostic Procedures and InbstrumentationSayoki GhoshNo ratings yet
- 69 EdDocument10 pages69 EdAnna ListianaNo ratings yet
- Ebn RugayDocument6 pagesEbn RugayJeffrey Barcelon TanglaoNo ratings yet
- Ijsrmjournal, Journal Manager, 17 IjsrmDocument9 pagesIjsrmjournal, Journal Manager, 17 IjsrmashishNo ratings yet
- Comparison of Surgically Induced Astigmatism in Manual Small Incision Cataract Surgery & Phacoemulsification SurgeryDocument6 pagesComparison of Surgically Induced Astigmatism in Manual Small Incision Cataract Surgery & Phacoemulsification SurgerycriticseyeNo ratings yet
- Coscarelli, 2012Document8 pagesCoscarelli, 2012vitor auzierNo ratings yet
- Predisposing Factors and Surgical Outcomes of Intraocular Lens Dislocation After PhacoemulsificationDocument7 pagesPredisposing Factors and Surgical Outcomes of Intraocular Lens Dislocation After PhacoemulsificationUmmul AzizahNo ratings yet
- Complications and Outcomes of Phacoemulsification Cataract Surgery Complicated by Anterior Capsule TearDocument7 pagesComplications and Outcomes of Phacoemulsification Cataract Surgery Complicated by Anterior Capsule Teareder510No ratings yet
- 3 Piece IOL SCL FixDocument6 pages3 Piece IOL SCL FixTvrtka BenašićNo ratings yet
- Clinical Study: Aspheric Intraocular Lenses Implantation For Cataract Patients With Extreme MyopiaDocument6 pagesClinical Study: Aspheric Intraocular Lenses Implantation For Cataract Patients With Extreme MyopiaKevin ArdiansyahNo ratings yet
- Surgical Procedure SmileDocument8 pagesSurgical Procedure SmilearumNo ratings yet
- Shankar Ganvit END PDFDocument4 pagesShankar Ganvit END PDFgyogi1989No ratings yet
- 1 s2.0 S1319453417301418 MainDocument4 pages1 s2.0 S1319453417301418 MainEzra MargarethNo ratings yet
- Jurnal PterigiumDocument6 pagesJurnal PterigiumMonica Lauretta Sembiring IINo ratings yet
- BSN Reading (Scleral Buckling) RosalesDocument8 pagesBSN Reading (Scleral Buckling) RosalesYvonnie RosalesNo ratings yet
- Evisceration With Autogenous Scleral Graft and Bioceramic Implantation Within The Modified Scleral Shell 133 Cases Over 17 YearsDocument6 pagesEvisceration With Autogenous Scleral Graft and Bioceramic Implantation Within The Modified Scleral Shell 133 Cases Over 17 YearsSaraelsy MonterrosoNo ratings yet
- Pars Plana VitrekDocument8 pagesPars Plana VitrekAnggisari Danastri DharmaNo ratings yet
- Postoperative Astigmatic Considerations in Manual Small-Incision CataractDocument6 pagesPostoperative Astigmatic Considerations in Manual Small-Incision Cataractsanchanaa anbalaganNo ratings yet
- Astigma Pterigium 11Document5 pagesAstigma Pterigium 11amro7190No ratings yet
- Toric ICLDocument8 pagesToric ICLjbahalkehNo ratings yet
- Delta Wiring Technique To Treat Bony Mallet Fracture Technique Description and Case SeriesDocument4 pagesDelta Wiring Technique To Treat Bony Mallet Fracture Technique Description and Case SeriesInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Comparison of A New, Minimally Invasive Strabismus Surgery Technique With The Usual Limbal Approach For Rectus Muscle Recession and PlicationDocument7 pagesComparison of A New, Minimally Invasive Strabismus Surgery Technique With The Usual Limbal Approach For Rectus Muscle Recession and PlicationvikrizkaNo ratings yet
- 100159-Article Text-824-1-10-20210225Document6 pages100159-Article Text-824-1-10-20210225Silvia OktavianiNo ratings yet
- Jurnal 1Document6 pagesJurnal 1r_ayuNo ratings yet
- A Clinical Study On Visual Outcome and Complications of Penetrating KeratoplastyDocument12 pagesA Clinical Study On Visual Outcome and Complications of Penetrating KeratoplastyIOSRjournalNo ratings yet
- Pterygium Excision With Free Conjunctival Limbal AutograftDocument7 pagesPterygium Excision With Free Conjunctival Limbal AutograftIOSRjournalNo ratings yet
- Corneal Endothelial Morphologic Assessment in Pediatric Cataract Surgery With Intraocular Lens Implantation - A Comparison of Preoperative and Early Postoperative Specular MicrosDocument8 pagesCorneal Endothelial Morphologic Assessment in Pediatric Cataract Surgery With Intraocular Lens Implantation - A Comparison of Preoperative and Early Postoperative Specular MicrosRael Rodrigues Dos SantosNo ratings yet
- Single-Step Transepithelial PHDocument9 pagesSingle-Step Transepithelial PHlenniNo ratings yet
- Persistent Corneal Edema After Collagen Cross-Linking For KeratoconusDocument6 pagesPersistent Corneal Edema After Collagen Cross-Linking For KeratoconusRestu MegantaraNo ratings yet
- Cataract PPT JournalDocument18 pagesCataract PPT JournalKulesh WaranNo ratings yet
- Original Article Astigmatic Changes Following Pterygium Removal: Comparison of 5 Different MethodsDocument0 pagesOriginal Article Astigmatic Changes Following Pterygium Removal: Comparison of 5 Different MethodsDinka RoselyNo ratings yet
- 2016 Article 229Document7 pages2016 Article 229nisa_kartikaNo ratings yet
- Jurnal Mata 5Document6 pagesJurnal Mata 5Dahru KinanggaNo ratings yet
- Evaluation of SuturlessDocument7 pagesEvaluation of SuturlesskenapayaNo ratings yet
- Advances in Vitreoretinal SurgeryDocument63 pagesAdvances in Vitreoretinal Surgerybharti100% (6)
- The Effect of Trabeculectomy On Astigmatism .99150Document5 pagesThe Effect of Trabeculectomy On Astigmatism .99150Yulias YoweiNo ratings yet
- Visual Acuity Outcome After Cataract SurgeryDocument10 pagesVisual Acuity Outcome After Cataract SurgeryAi AisyahNo ratings yet
- Postkeratoplasty Astigmatism: Anita Raghavan, Soly NaveenDocument7 pagesPostkeratoplasty Astigmatism: Anita Raghavan, Soly NaveenPraveen MNo ratings yet
- Complication Rates of Phacoemulsification and Manual Small-Incision Cataract Surgery at Aravind Eye HospitalDocument10 pagesComplication Rates of Phacoemulsification and Manual Small-Incision Cataract Surgery at Aravind Eye HospitalErwin XuNo ratings yet
- Complication Rates of Phacoemulsification and Manual Small-Incision Cataract Surgery at Aravind Eye HospitalDocument10 pagesComplication Rates of Phacoemulsification and Manual Small-Incision Cataract Surgery at Aravind Eye Hospitaltimoti100% (1)
- Detection of Phishing WebsitesDocument6 pagesDetection of Phishing WebsitesInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Vertical Farming System Based on IoTDocument6 pagesVertical Farming System Based on IoTInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Detection and Counting of Fake Currency & Genuine Currency Using Image ProcessingDocument6 pagesDetection and Counting of Fake Currency & Genuine Currency Using Image ProcessingInternational Journal of Innovative Science and Research Technology100% (9)
- Osho Dynamic Meditation; Improved Stress Reduction in Farmer Determine by using Serum Cortisol and EEG (A Qualitative Study Review)Document8 pagesOsho Dynamic Meditation; Improved Stress Reduction in Farmer Determine by using Serum Cortisol and EEG (A Qualitative Study Review)International Journal of Innovative Science and Research TechnologyNo ratings yet
- Influence of Principals’ Promotion of Professional Development of Teachers on Learners’ Academic Performance in Kenya Certificate of Secondary Education in Kisii County, KenyaDocument13 pagesInfluence of Principals’ Promotion of Professional Development of Teachers on Learners’ Academic Performance in Kenya Certificate of Secondary Education in Kisii County, KenyaInternational Journal of Innovative Science and Research Technology100% (1)
- The Impact of Music on Orchid plants Growth in Polyhouse EnvironmentsDocument5 pagesThe Impact of Music on Orchid plants Growth in Polyhouse EnvironmentsInternational Journal of Innovative Science and Research Technology100% (1)
- Consistent Robust Analytical Approach for Outlier Detection in Multivariate Data using Isolation Forest and Local Outlier FactorDocument5 pagesConsistent Robust Analytical Approach for Outlier Detection in Multivariate Data using Isolation Forest and Local Outlier FactorInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Realigning Curriculum to Simplify the Challenges of Multi-Graded Teaching in Government Schools of KarnatakaDocument5 pagesRealigning Curriculum to Simplify the Challenges of Multi-Graded Teaching in Government Schools of KarnatakaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Sustainable Energy Consumption Analysis through Data Driven InsightsDocument16 pagesSustainable Energy Consumption Analysis through Data Driven InsightsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Entrepreneurial Creative Thinking and Venture Performance: Reviewing the Influence of Psychomotor Education on the Profitability of Small and Medium Scale Firms in Port Harcourt MetropolisDocument10 pagesEntrepreneurial Creative Thinking and Venture Performance: Reviewing the Influence of Psychomotor Education on the Profitability of Small and Medium Scale Firms in Port Harcourt MetropolisInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- An Overview of Lung CancerDocument6 pagesAn Overview of Lung CancerInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Digital Finance-Fintech and it’s Impact on Financial Inclusion in IndiaDocument10 pagesDigital Finance-Fintech and it’s Impact on Financial Inclusion in IndiaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Impact of Stress and Emotional Reactions due to the Covid-19 Pandemic in IndiaDocument6 pagesImpact of Stress and Emotional Reactions due to the Covid-19 Pandemic in IndiaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Utilization of Waste Heat Emitted by the KilnDocument2 pagesUtilization of Waste Heat Emitted by the KilnInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- An Efficient Cloud-Powered Bidding MarketplaceDocument5 pagesAn Efficient Cloud-Powered Bidding MarketplaceInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Designing Cost-Effective SMS based Irrigation System using GSM ModuleDocument8 pagesDesigning Cost-Effective SMS based Irrigation System using GSM ModuleInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Effect of Solid Waste Management on Socio-Economic Development of Urban Area: A Case of Kicukiro DistrictDocument13 pagesEffect of Solid Waste Management on Socio-Economic Development of Urban Area: A Case of Kicukiro DistrictInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Predictive Analytics for Motorcycle Theft Detection and RecoveryDocument5 pagesPredictive Analytics for Motorcycle Theft Detection and RecoveryInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Auto Tix: Automated Bus Ticket SolutionDocument5 pagesAuto Tix: Automated Bus Ticket SolutionInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Examining the Benefits and Drawbacks of the Sand Dam Construction in Cadadley RiverbedDocument8 pagesExamining the Benefits and Drawbacks of the Sand Dam Construction in Cadadley RiverbedInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Ambulance Booking SystemDocument7 pagesAmbulance Booking SystemInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Comparative Evaluation of Action of RISA and Sodium Hypochlorite on the Surface Roughness of Heat Treated Single Files, Hyflex EDM and One Curve- An Atomic Force Microscopic StudyDocument5 pagesComparative Evaluation of Action of RISA and Sodium Hypochlorite on the Surface Roughness of Heat Treated Single Files, Hyflex EDM and One Curve- An Atomic Force Microscopic StudyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Study Assessing Viability of Installing 20kw Solar Power For The Electrical & Electronic Engineering Department Rufus Giwa Polytechnic OwoDocument6 pagesStudy Assessing Viability of Installing 20kw Solar Power For The Electrical & Electronic Engineering Department Rufus Giwa Polytechnic OwoInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Computer Vision Gestures Recognition System Using Centralized Cloud ServerDocument9 pagesComputer Vision Gestures Recognition System Using Centralized Cloud ServerInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Cyber Security Awareness and Educational Outcomes of Grade 4 LearnersDocument33 pagesCyber Security Awareness and Educational Outcomes of Grade 4 LearnersInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Forensic Advantages and Disadvantages of Raman Spectroscopy Methods in Various Banknotes Analysis and The Observed Discordant ResultsDocument12 pagesForensic Advantages and Disadvantages of Raman Spectroscopy Methods in Various Banknotes Analysis and The Observed Discordant ResultsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Blockchain Based Decentralized ApplicationDocument7 pagesBlockchain Based Decentralized ApplicationInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- An Industry That Capitalizes Off of Women's Insecurities?Document8 pagesAn Industry That Capitalizes Off of Women's Insecurities?International Journal of Innovative Science and Research TechnologyNo ratings yet
- Factors Influencing The Use of Improved Maize Seed and Participation in The Seed Demonstration Program by Smallholder Farmers in Kwali Area Council Abuja, NigeriaDocument6 pagesFactors Influencing The Use of Improved Maize Seed and Participation in The Seed Demonstration Program by Smallholder Farmers in Kwali Area Council Abuja, NigeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Unmasking Phishing Threats Through Cutting-Edge Machine LearningDocument8 pagesUnmasking Phishing Threats Through Cutting-Edge Machine LearningInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 3599 6786 2 PBDocument36 pages3599 6786 2 PBratihNo ratings yet
- Eye Care Through Eye Exercise A Critical ReviewDocument3 pagesEye Care Through Eye Exercise A Critical ReviewEditor IJTSRDNo ratings yet
- Dysfunction of Magnocellular/dorsal Processing Stream in SchizophreniaDocument11 pagesDysfunction of Magnocellular/dorsal Processing Stream in SchizophreniatratrNo ratings yet
- Certificate For Visual Standards For Driving (See Instructions Overleaf Before Filling Up The Certificate)Document2 pagesCertificate For Visual Standards For Driving (See Instructions Overleaf Before Filling Up The Certificate)AVIN JOSEPHNo ratings yet
- Eye Path12Document45 pagesEye Path12JillKellyNo ratings yet
- Vision Therapy PDFDocument72 pagesVision Therapy PDF4nsan4o4luNo ratings yet
- GlucomaDocument14 pagesGlucomametalheavy9993No ratings yet
- Ophthalmology (4.0)Document241 pagesOphthalmology (4.0)Ashima GautamNo ratings yet
- Disorders of Perception: Primary Section Objective: Know The DefinitionsDocument32 pagesDisorders of Perception: Primary Section Objective: Know The DefinitionsMukesh VagadreNo ratings yet
- ProP - Differentiating Nuclear Sclerosis From CataractsDocument6 pagesProP - Differentiating Nuclear Sclerosis From CataractsDita TaepangNo ratings yet
- Compile Soal Mata PreklinikDocument77 pagesCompile Soal Mata PreklinikFika RahmawatiNo ratings yet
- CATALOGO RUSTY SS23 - Act 26-07Document68 pagesCATALOGO RUSTY SS23 - Act 26-07Theo MalloNo ratings yet
- Presentation - Colors Combinations and HarmonyDocument97 pagesPresentation - Colors Combinations and HarmonySunil TalekarNo ratings yet
- Class 8 - Chapter 16 - LightDocument30 pagesClass 8 - Chapter 16 - LightsanaNo ratings yet
- Case Presentation: DR - Prathibha.M.ChachadiDocument28 pagesCase Presentation: DR - Prathibha.M.ChachadiPrathibha M ChachadiNo ratings yet
- Branch Retinal Vein OcclusionDocument8 pagesBranch Retinal Vein OcclusionTasya BhatoNo ratings yet
- Binocular Balancing: Presented By: Hina Hafeez TOD (1 Semester)Document14 pagesBinocular Balancing: Presented By: Hina Hafeez TOD (1 Semester)Xid KhanNo ratings yet
- Special Senses) 3. Photoreceptors - Rods and Cones - KeyDocument1 pageSpecial Senses) 3. Photoreceptors - Rods and Cones - Keyranag59100No ratings yet
- Basic Ocular Surgeries: Fatima Medical Center Dr. Vicente O. Santos JR., MDDocument53 pagesBasic Ocular Surgeries: Fatima Medical Center Dr. Vicente O. Santos JR., MDMiguel C. DolotNo ratings yet
- Colour VisionDocument34 pagesColour VisionIshmeet SinghNo ratings yet
- Presenter Notes: Slide 1: Hello My Name Is Taylor Brown I Am A Teacher For TheDocument9 pagesPresenter Notes: Slide 1: Hello My Name Is Taylor Brown I Am A Teacher For TheTaylor BrownNo ratings yet
- Eye ExaminationDocument6 pagesEye ExaminationChellamani UmakanthanNo ratings yet
- The Eye HistologyDocument16 pagesThe Eye HistologyFarah AkhwanisNo ratings yet
- Viusal Pathway: DR Raghuveer Choudhary Dept. of Physiology DR S.N.Medical College JodhpurDocument35 pagesViusal Pathway: DR Raghuveer Choudhary Dept. of Physiology DR S.N.Medical College JodhpurPhysiology by Dr RaghuveerNo ratings yet
- Role of Ophthalmic Nurses With Visually Impaired PatientsDocument6 pagesRole of Ophthalmic Nurses With Visually Impaired PatientsIsaac Aleman0% (1)
- Anterior Chamber Depth and Chamber Angle and Their Associations With Ocular and General Parameters: The Beijing Eye StudyDocument9 pagesAnterior Chamber Depth and Chamber Angle and Their Associations With Ocular and General Parameters: The Beijing Eye StudyDesyifa Annisa MursalinNo ratings yet
- Ipd B: Finals - Heent: Techniques of Examination For Head (From Bates')Document13 pagesIpd B: Finals - Heent: Techniques of Examination For Head (From Bates')Janica Marie Ragsac100% (1)
- Ophthalmology High YieldDocument91 pagesOphthalmology High YieldAnish ShresthaNo ratings yet
- Notification Admit Card Results Exam AnalysisDocument10 pagesNotification Admit Card Results Exam AnalysisChellamani UmakanthanNo ratings yet
- MEDSURG II (2nd Sem - ENDTERM NOTES)Document39 pagesMEDSURG II (2nd Sem - ENDTERM NOTES)Meryville JacildoNo ratings yet
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (5)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (39)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 4 out of 5 stars4/5 (5)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 4.5 out of 5 stars4.5/5 (84)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Rating: 3 out of 5 stars3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- The Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeFrom EverandThe Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeRating: 4.5 out of 5 stars4.5/5 (3)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (44)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (267)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- I Shouldn't Feel This Way: Name What’s Hard, Tame Your Guilt, and Transform Self-Sabotage into Brave ActionFrom EverandI Shouldn't Feel This Way: Name What’s Hard, Tame Your Guilt, and Transform Self-Sabotage into Brave ActionNo ratings yet
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (46)
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsFrom EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsRating: 4.5 out of 5 stars4.5/5 (39)
- The Fun Habit: How the Pursuit of Joy and Wonder Can Change Your LifeFrom EverandThe Fun Habit: How the Pursuit of Joy and Wonder Can Change Your LifeRating: 4.5 out of 5 stars4.5/5 (19)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesFrom EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesRating: 4.5 out of 5 stars4.5/5 (1412)
- Summary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedRating: 4 out of 5 stars4/5 (11)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingFrom EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingRating: 4 out of 5 stars4/5 (1138)
- The Story of Philosophy: The Lives and Opinions of the Greater PhilosophersFrom EverandThe Story of Philosophy: The Lives and Opinions of the Greater PhilosophersNo ratings yet