Professional Documents
Culture Documents
Ob Postpartum-Gyne
Uploaded by
Zhantelle A. SantosOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ob Postpartum-Gyne
Uploaded by
Zhantelle A. SantosCopyright:
Available Formats
ANNE MARIS L.
RELLAMA, RN, MAN POSTPARTUM CONDITIONS
ANOMALIES OF THE PLACENTA AND THE CORD Placenta Circumvallata
● “Whatever is wrong with the placenta and the cord will surely ● The fetal side of the placenta is covered to
affect the mother and the baby” some extent with chorion wherein it formed
a certain ridge but still covering the
Cord Insertions and Placental Variations placenta
● Involves abnormalities in the size of the placenta, how it looks ● There is a lowered portion or an indentation
like, or the blood vessels connected to it cannot actually be ● The membrane covering is altered
pinpointed ● The placenta has a central depression on its
● Placenta fetal surface to the margins of which the
○ Weight: 460 or 500gms fetal membranes are attached
○ Diameter: 15 to 20cm ● Termed as “Circumvallate Placenta”
○ Thickness: 1.5 to 3.0cm
● Cause: unknown
CONTRIBUTORY FACTORS
Helps us understand the development of different variations
1. Women with DM may have an unusually large placenta
● Woman with DM may have a very large baby
Placenta Marginata
(macrosomia), thereby to compensate for the needs
● The fold of the chorion reaches just to the edge of the placenta
of the big baby, the placenta may also be larger than
normal in size
2. Diseases as syphilis or erythroblastosis fetalis, placenta may be Velamentous Insertion of the Cord / Placenta Velamentosa
● The cord separates into small vessels that reach the placenta by
so large weighing half as much as the fetus
spreading across a fold of amnion
3. Placenta wider in diameter may occur if the uterus has scars from
● It would appear in a funnel-like shape
previous surgeries or a septum (opening), due to it being forced
● The umbilical cord is attached to the membranes some distance
to spread out to find an implantation space
● The placenta looks for a wider space for it to implant from the margin of the placenta and the umbilical vessels pass
itself so that it would spread out along the membrane to reach the margin
● Very rare but is still possible to occur
Types of Placental Variants
Battledore Placenta
● Alteration in the way the cord is attached, it is inserted
marginally rather than centrally
● Alteration on how the placenta looks like
Vasa Previa
● The umbilical cord insertion crosses the cervical OS, with the
cord being delivered before the fetus
● Pathological specimen of a velamentous cord insertion showing
Placenta Succenturiata the umbilical cord insertion into the placental membranes and
● One or more accessory lobes are connected to the main the unprotected fetal vessels
placenta (the mother) by blood vessels ● There is distance between the cord
● Sometimes in a hospital setting, there was already a placenta ● Blood vessels grow out of the cord and along the membranes
delivered and yet there is one more placenta attached ● Presents with painless vaginal bleeding at the time of
● Sometimes it is not just one but two or more attached accessory spontaneous or artificial rupture of the membranes
lobes ● Could be a complication of placenta previa
● A cause of antepartum hemorrhage ○ Placenta Previa - the implantation of the placenta is
● Attached to a mother placenta is a baby placenta not in the anterior surface but on the side covering the
cervix or the internal OS and in the margin
○ Left: Fetal side
○ Right: Maternal side
1 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
Placenta Accreta ○ Avoid using medical jargons or terms usually used in
● The chorionic villi are deeply attached onto or into the the labor and delivery room so that the patient
myometrium or deeper into the uterine wall and uterine muscle understands us better
resulting to the placenta not being able to loosen and be ● Monitor the patient closely in the immediate postpartum
delivered normally as it should during placental separation period
● There is no placental separation because it is inserted deeply ○ In a case of atomy, assess the patient and hearing and
● Normally, it could separate in 15 to 20 mins and from that you acting on particular complaints of the patient would
could already track and deliver the placenta prevent complications from happening or further
● There is resistance when you do traction of the cord → do not danger for the life of both the mother and the fetus
pull and pull and pull → the uterus might be inverted inside out ○ Ang isang nurse ay kailangang mabilis mag-isip and
when you pull on the cord with all you might kumilos because the life of the mother and the fetus is
● Placenta Increta in our hands
○ Occurs when the placenta attaches even deeper into
the uterine wall and uterine muscle TREATMENT
○ Nakaibabaw siya uterine wall and sa uterine muscles ● Complete inspection of placenta is necessary after birth
○ It does not invade the wall of the uterus ○ Verify the number of cotyledons
● Placenta Percreta ○ Check placenta for completeness (chorion and
○ The placenta extends through the entire wall of the amnion)
uterus ■ Presence of tear would indicate that there are
○ Di lang siya nakaibabaw, actually invading the entire still remains inside the uterus → doctor has to
wall of the uterus perform a manual evacuation otherwise the
○ The placenta pushes through the uterine wall and uterus will relax and the mother will bleed
invades into other organs like the bladder ● For Succenturiata
○ Can be detected through ultrasound → allows the ○ Should have manual removal of the placenta
doctor to consider doing a surgical procedure as to ○ Do it slowly as it may cause pain to the mother
remove the deeply attached placenta (Vaginal ● For Vasa Previa
Hysterectomy) ○ CS to prevent blood loss from tearing
○ Mother should be prepared for a possibility of a CS
● For Placenta Accreta
○ Methotrexate to destroy remaining attached tissue
○ Hysterectomy may be necessary if adhering
persistently
Other Placental Anomalies
Placenta Bipartita or Tripartita
● The placenta has two or three incomplete lobes and the
NURSING INTERVENTIONS
umbilical vessels pass off one lobe to the other before joining
● Make sure the placenta is inspected after delivery
the umbilical cord
○ Observe for the number of cotyledons present
● There is separation of the placenta
(normal: 20-25)
○ Make sure the membranes are complete and intact
(amnion and chorion)
○ The cord should have 2 arteries and 1 vein (AVA)
● Assist with manual removal of the placenta in succenturiata
○ Huwag mauuna sa doctor mag-examine ng patient or
dumukot ng accessory placenta
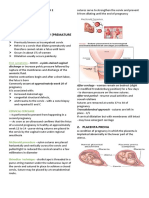
Placental Infarction
○ Sometimes the doctor allows the nurse to feel the
● In most cases, the cause is
accessory lobe
unknown but in some it may be
● Prepare patient for possibility of CS
caused by trauma or blow applied
○ Prepare the patient for the occurrence any
to the mother's abdomen during
eventualities
pregnancy
○ Ask for the patient to sign a consent form for possible
● Producing shearing forces on the
CS delivery
placental uterine junction which
○ Reassure and update the patient of the plan of action
locally interferes with the maternal
● Emotional support and explain all treatment and
circulation
procedures
○ Circulation is cut off because it was separated
○ Nurses should go down to the level of their patient →
prematurely
explain in layman's term
2 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
● There is premature detachment of a part of the placenta →
causes atrophy → lead to scarring (while the rest of the part of
the placenta is still attached)
POSTPARTUM HEMORRHAGE
● Normal amount of blood loss after delivery
○ NSD: 350-500 mL
○ CS: 1000mL
● Any blood loss beyond these values, we consider the woman
suffering from postpartum hemorrhage
CAUSES (4T’s)
2 MAJOR TYPES ● Tone: uterine atony
● Early or primary postpartum hemorrhage - w/n 24 hours after ● Tissue: retained placenta
delivery ● Trauma: lacerations (perineal, vaginal, or cervical), uterine
● Late or secondary postpartum hemorrhage - beyond 24 hours rupture, and even uterine inversion
to 6 weeks postpartum ● cloTTing/Thrombin: coagulopathy
SIGNS AND SYMPTOMS OF AN IMPENDING HYPOVOLEMIC SHOCK TONE: Uterine Atony
NOTE: When your body experiences extensive blood loss, your body tries ● Intrapartally, during labor & delivery, the uterus contracts → pain
to compensate ○ Pain may not just be because of the compression of
● Changes in vital signs the surrounding structures
○ Earliest change: tachycardia / increase in pulse rate ○ It is also because there is no blood flow going into the
■ When blood volume is diminished, the heart uterus
tries to pump harder so that somehow there ○ The blood volume of the mother during contraction is
will be an increase in the cardiac output that actually confined in the periphery
will supply the vital organs of the body and they ○ When you have to monitor the BP of the woman, it
will not lead to damage should not be during the contraction
■ PR will become thready → nonpalpable → dies ○ During the contraction - increased BP
from shock ○ Painful because the area is ischemic (has
○ Increase and decrease in blood pressure vasoconstriction)
■ Will increase then later on → hypotension → no ● Uterus should be well contracted after the delivery to prevent the
BP woman from bleeding
○ Increased RR ● If the uterus is not well contracted, blood flow continues
■ Oxygenation is also affected
■ Dyspnea because of the lack of O2
■ Breathes fast to expand the lungs, to
compensate, to breathe more O2
○ Decreased and increased temperature
■ Dehydration may cause an increase in
temperature
■ If no interventions are done, since the
circulation going inside the body is affected, ● NOT WELL CONTRACTED: There are endometrial arteries
the patient will have cool, clammy skin later on connecting the endometrium to the placenta → once the
● Decreased urine output placenta is delivered, there will be tearing of endometrial
○ Since the circulation to the vital organs is affected, arteries → the arteries are opened → if not contracted, blood
one of these are the kidneys continuously flows from the open vessels to the uterus →
○ As a nurse, you should monitor the kidney function excreted via the vagina → extensive bleeding
○ Kidneys are not functioning well → decreased output ● WELL CONTRACTED: If the uterus is well contracted, there is
● Cerebral hypoxia vasoconstriction → promotes closure and drying for the open
○ Lack of oxygen in the brain endometrial arteries → bleeding will stop
○ Restlessness, dizziness, change in the level of
consciousness CAUSES
○ Glasgow Coma Scale (GCS)- best way to check the
● Overdistention
level of consciousness
○ Uterus is like a rubber band; if you stretch it to the maximum
capacity, it will not return to its original position and will not
be that elastic
3 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
■ If the uterus keeps on being distended, myometrial THERAPEUTIC MANAGEMENT
muscles will have a poorer tone which prevents it from ● Bimanual uterine massage
contracting ○ One hand just above the s.pubis and
○ Possible causes of overdistention of uterus: multiparity, the dominant hand on the fundus
polyhydramnios, macrosomia, advance in age, dystocia ■ Nondominant hand over the
■ Polyhydramnios - more amniotic → bigger uterus s.pubis will prevent possible
● Multiparity uterine inversion when you’re
○ more pregnancies, poorer muscle tone doing the massage
● Advanced age ■ Massage the fundus with a little
○ Old age - everything sags; including the muscles of the pressure
uterus especially because estrogen (w/c keeps the muscle ■ Do not tickle
tone good) is decreased ● Vital signs
● Prolonged/Precipitate delivery ○ Tachycardia is usually the first sign of excessive bleeding
○ Dystocia/prolonged difficult labor - oxytocin is ○ BP, RR, temperature may also be affected
administered → there’s hypertonicity and ● Voiding
hyperstimulation → muscles overwork → will soon not ○ There are times when the uterus does not contract
contract effectively → uterine atony effectively because the bladder is full
■ Proper regulation of oxytocin drip, syntocinon, ○ If the bladder is full in front, it occupies the space of the
pitocin, and other possible uterotonic uterus. The uterus runs out of space to contract effectively
■ Uterus should be well-monitored so that there is no → possible hemorrhage
hyperstimulation that may lead to postpartum atony ○ Sometimes a uterus is well contracted but the fundus is
● Chorioamnionitis - will not promote effective uterine contraction displaced to the side or above the expected location
● Anesthesia ○ If you palpate the fundus is well contracted but is on the
○ Anesthesia → decreases tone → relaxes muscles (esp if side, you should not automatically suspect that there is
general anesthesia; will include the uterus) atony. The first thing that you have to assess is the bladder
○ When the bladder is full, it pushes the uterus up. Even if it
MANIFESTATIONS is contracted, it somehow prevents the uterine involution
NOTE: The most common cause of postpartum hemorrhage is uterine or the descent of the uterus
atony. If the woman is bleeding profusely, the first thing that a nurse should ○ Promote voiding; around 4-6 hours the patient should have
check is the uterus. It should be well contracted and firm upon palpation; voided already
fundus located in the midline and a little above the umbilicus immediately ● Positioning and activity restrictions
after the delivery. ○ If the patient is already and she doesn't have any cardiac
● Soft, boggy fundus problem, the best position is to raise the legs
○ 1st thing to do: uterine massage (Trendelenburg)
● Fundal location ■ When you raise the
○ Location of the fundus depends on the time after delivery legs, by gravity it
■ Right after: fundus above the umbilicus concentrates the
■ Few hours after: on the umbilical level blood flow on the
■ 1 day postpartum: 1 fingerbreadth below the upper parts of the
umbilicus body of the patient
■ 10th day: non-palpable where the vital
● Excessive lochia (bright red) organs are located
○ NOTE: the napkin is replaced every 15 minutes and is fully ■ More activity = higher oxygen demand
soaked ● Oxygen is compromised and blood volume
○ Take note of the bleeding deficit is present already
○ Weigh the pad to have an ● Oxygen
estimate of the blood loss ○ Once O2 sats are decreasing
(approx. 1g = 1cc) ○ Via nasal cannula or face mask depending on the order
● Excessive clots ● Blood replacement (plasma extenders)
○ Large clots ○ Packed RBC if HgB is really low
○ For the first 2 days, it could be ○ Cold blood if all components are decreased
moderate ○ Plasma extenders for diminished plasma
○ Should gradually decrease (rubra ○ Platelet concentrate transfusion for decreased platelet
→ serosa → alba) ● Iron supplement
○ To help in erythropoiesis postpartum and to help the
patient recover
4 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
● Infection ○ If the patient is NPO, per IM.
○ Antibiotics may be prescribed ● Prostaglandin analogs (OGF) - IM or intramyometrial
● Bimanual compression → Carboprost tromethamine (Hemabate, Prostin)
○ If bimanual massage is not ○ Together with methergine, they may cause persistent
effective uterine contraction and hyperstimulation
○ Principle: just like when you have ○ Less prefered but can be chosen if oxytocin is not
a wound and you bleed, you effective
apply pressure ○ Side effects: nausea, diarrhea, tachycardia (but the
○ It stops the flow most common is hypertension)
○ Pressure → formation of plug → prevent bleeding
○ One hand inserted vaginally to the uterus, other one on the TRAUMA: Lacerations
fundus → applying pressure on the open
Types of Lacerations
vessels
● Vaginal packing Cervical Perineal
○ Also serves as compression/pressure
● Uterine balloon tamponade (balloon catheter with
sterile water)
○ Applies pressure on the open vessels
Vaginal
CAUSES
● Dystocia or precipitate births
○ Dystocia bc if the baby is big, it can lacerations
● Primigravida
○ Secondary power of labor may not be effective because the
● Suturing mother does not how to push effectively
○ Embolization of pelvic and uterine vessels (angiographic ○ Difficulty to descend may cause laceration
technique) ● Large infant
■ Computer/ultrasound/monitor guided ● Lithotomy position and instrumental delivery
■ The doctor will inject an agent that wills top the ○ This is why we promote upright positioning nowadays
bleeding to the arteries because by gravity it promotes more fetal descent
■ They will insert a catheter and will inject this ○ Instrumental delivery - metals may be traumatic on the
thrombotic agent that will tissues
promote clot formation and
bleeding will stop PERINEAL LACERATIONS
○ Ligation ● First degree - involves the skin
■ They will suture the open ● Second degree - perineal
vessels to stop bleeding muscles
● Hysterectomy ● Third degree - partial anal
○ Last resort sphincter involvement
○ Removal of the uterus ● Fourth degree - involves the
○ To prevent hypovolemic shock that can lead to possible rectal and bowel lining
death ● The higher the degree, the
deeper the laceration, the
MEDICATIONS more painful, and more
When uterine massage does not work, uterotonics may be prescribed possibility for infection
● Oxytocin (Pitocin Drip)
○ Most common and most preferred MANAGEMENT
○ In terms of side effects of increasing the BP, it has a lesser ● Suturing (with anesthesia)
vasoconstrictor effect ○ Whatever the type of laceration, whether in the cervix or
○ Usually per drip or incorporated per IV vaginal, the doctor will usually do ligation/suturing
○ To promote uterine contraction ○ Usually with absorbable suture such as chromic suture
● Methylergonovine (Methergine) ○ Lidocaine may be used as the anesthetic
○ If oxytocin is not effective ● Avoid constipation
○ However, very potent ○ If the patient wants to defecate and has this laceration, she
○ Always monitor the BP will try to do the valsalva maneuver which could strain the
○ Usually per IM or this may be taken PO incision site
5 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
○ Can cause dehiscence (matatanggal yung tahi) ○ The placenta may have been delivered but some
○ There is pressure on the suture/incision site which can be fragments may be left which will cause the bleeding
painful
○ Doctors may prescribe laxatives such as castor oil in order
for the patient to defecate without any difficulty
● No rectal temperature and suppositories
○ If perineal path
○ Can cause on pressure and pain to the incision site
● Indwelling catheter (vaginal)
○ Where the patient will void
○ The vagina and the urinary meatus are close
MANAGEMENT
○ If urine falls on the incision site, it will be very painful
● Dilatation and curettage
because it is acidic
○ If early, manual removal of the retained fragments may be
○ Ensure adequate emptying of the bladder
done
○ If not effective, D&C may be done
○ Curette - spoon-like instrument that will clean the uterus
and remove the fragment
● Methotrexate - destroy the retained fragments
● Lochial discharge
○ Rubra, serosa, alba
○ Should not be interchanged
○ The number of pads and how heavy
When will I consider lacerations? ○ If soaked every 15 mins, suspect persistence of bleeding
● The first thing to consider is uterine atony ● Balloon occlusion or embolization
○ First possible cause of early postpartum hemorrhage ○ If manual removal is not effective
○ Assess if firm and well-contracted ○ Ultrasound-guided to instill the thrombic agent
● If ruled out, atony, the presence of laceration is suspected ● Hysterectomy
○ If well-contracted but the woman is still bleeding
profusely especially if it is bright red, consider
lacerations
● Third is retained placental fragments
TISSUE: Retained Placental Fragments
● Deep placental implantation
○ Placenta may have been implanted deeper on the
myometrium (normally, it should be implanted on the
endometrium only) Uterine Inversion
○ Increta - 70% is implanted on the myometrium CAUSES
○ Acreta - 75-78%
● Fundal push
○ Percreta - implanted on the perimetrium
○ Not recommended in EINC anymore
○ The deeper the implantation, the harder to remove
○ Applying pressure to the fundus during delivery
● Ultrasound and (high) presence of HCG
○ When you push the fundus too vigorously, inversion is
○ Can suspect deep placental implantation
possible
○ If D&C or manual is not effective, hysterectomy will be
● Placental delivery
the last resort
○ Placental is still attached and traction is already
● Depending on the amount of retained fragments
applied, uterus may be inverted
○ Can be early or late postpartum hemorrhage
● Uterine massage
depending on the amount
○ When you do the
○ Large tissues = usually early
uterine massage,
○ Small tissues = usually late
the nondominant
hand should be
● We should wait for signs of placental separation before we do
placed above the
the CCT with CT (controlled cord traction with countertraction)
symphysis to
● We have to make sure that the placenta has detached from the
avoid inversion
decidua before we deliver the placenta
● If we pull the placenta forcefully, it may not be removed totally
6 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
NOTE: Manual repositioning may be tried by the doctor; Tocolytics will be Perineal Hematoma
used to make it easier ● Very common after the delivery especially
● If not effective, last resort is hysterectomy if
a. The woman has very effective
Disseminated Intravascular Coagulation contraction but the secondary
● PROM, miscarriage, or IUFD power is not good (bearing
● When the woman is bleeding profusely and the body reacts by down power)
activating the thrombin, clotting factors and platelets → clot ○ The head of the baby
formation → if bleeding persists, thrombin, clotting factors are causes a lot of pressure →
used up → thrombocytopenia → diminished clotting factors → edematous → can bleed
bleeding somewhere → clot → hematoma
● Clot, bleed, clot, bleed, clot bleed b. When you keep doing internal exam
○ Traumatizes the tissue and makes a woman
more prone to infections
● Subcutaneous, purplish discoloration with swelling, firm globe
and tender, severe perineal pain (3-4 days absorbed)
○ We usually wash with cold water
○ To lessen inflammation and plainand to stop
bleeding
○ Antibiotics may be prescribed as well for possible
infections
● Rapid birth, perineal varicosities, lacerations
MANAGEMENT
MANAGEMENT ● Mild analgesic
● Transfusion ○ To lessen pain
● Avoid trauma or cutting the patient ● Ice pack (thermal injury)
○ Has an anesthetic effect
Subinvolution ○ Prevents further bleeding on the 1st 24 hrs
● Late postpartum hemorrhage cause ● Ligation with local anesthesia
● Involution process ○ To stop bleeding
○ Return of the uterus to its pre-pregnancy state
● Subinvolution - failing of the uterus to go back to its normal PUERPERAL INFECTION
position ● Infection of the reproductive tract in the postpartum period is
○ Malaki and mataas pa rin another major cause of maternal mortality
○ Not well-contracted ● Usually begins as local infection but could spread into the
○ Did not go back to its normal status peritoneum and/or circulatory system
● Retained fragments, mild endometritis, myoma ○ This is why it is important to assess the patient
○ Myoma prevents it from contracting well properly to discover the symptoms early on and
○ Abnormal tissue may inhibit contraction prevent further systemic complications
○ Retained fragments should be removed ○ Once it reaches the circulatory system, it would be
● Can also be due to infection very difficult to treat the patient already
○ Early assessment and early detection is very crucial for
clients at risk for infection
● Grp. B streptococci, staphylococci, and E. coli commonly
causes infections postpartum
● REMEMBER: during pregnancy, the contents of the uterus are
sterile (the fetus, the amniotic fluid, the placenta, the amnion and
chorion)
● Infection usually occurs because of the breakage of the amniotic
MANAGEMENT
sac (bag of water) that opens the intrauterine cavity to the
● Methylergonovine
pathogens present in the vaginal canal, perineum and these
○ Promote uterine contraction
pathogens can take advantage of it and invade the intrauterine
○ uterotonic
area. They can infect not only the mother but also the fetus
● Antibiotic
especially if the amniotic sac has already ruptured for a long time
○ For infections such as endometritis
before they give birth.
7 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
PROGNOSIS ○ Anything foreign that is introduced into the vaginal canal
● Women's general health raises the risk of acquiring infection
○ If they are not healthy to begin with (ex: with anemia → ○ Despite disinfecting the instruments prior to inserting it into
deficient blood components to help heal with whatever the vaginal canal, there can be no guarantee that it 100%
could go wrong with the body) If an infection happens, it won’t carry any pathogens
would take a longer time and more effort to recuperate
● Virulence of pathogen
○ Virulence - the ability of the pathogen to cause harm
○ The treatment would depend on the virulence of the
pathogen which would be discovered through the culture
and sensitivity test
● Portal of entry ● Internal fetal heart monitor
○ Where the infection came form and what part of the body ○ A little bit more accurate compared to the external fetal
it infected heart monitor but it is more invasive
○ The larger the infected part is, the more difficult it is to treat ○ The probes used to detect the status of the fetus and the
uterine contractions will be inserted into the vagianl canal
RISK FACTORS (p. 656 box 25.5) which makes this procedure invasive
● Postpartal hemorrhage ○ Even if these probes are sterile, you cannot guarantee there
● Preexisting anemia there will be no microorganisms that will be introduced into
○ Deficiency in oxygen and nutrient carriers in your body → the vaginal canal
difficulty in fighting invading pathogens and
microorganisms → ↑ risk of developing infection
● Ruptured membranes >24 hrs
○ The intrauterine cavity is sterile especially if the amniotic sac
is still intact. Once it is ruptured, pathogens may enter and
would be more prone to infection if the exposure is longer.
● Vaginal infection at time of birth
○ Due to the proximity of the cervix and the vaginal canal. If
there is a presence of infection at the vaginal canal, it could
easily ascend into the cervix and infect the intrauterine
lining.
● Retained placental fragments ○ Present infection can cause further infection at the
○ The placental fragments are treated by the body as a postpartum period
foreign material and when they are in the process of
necrosis, they are a very good source or medium for
bacterial growth.
○ If the cervical opening is exposed, pathogens may enter
and they may reside in the placental fragments as they
serve as a very good medium for bacterial growth → px may
show symptoms of infection any time ● Uterine exploration
○ It is important to remember that one of our nursing ○ Digital exploration of the uterus
responsibilities is to check for the completeness of the ○ Removal of retained membranes and
placenta when we deliver them to prevent infection. placental fragments
○ If there are retained fragments such as in the picture, report ○ To remove the retained placental
it immediately to the physician to make sure that there fragments, the doctors wrap a gauze on
won’t be any retained fragments. their gloved hand and insert that gloved
hand inside the uterus to manually
explore and scrape the retained
placental fragments
○ You have introduced something foreign into the uterine
cavity therefore we cannot exclude the possibility that it can
have a microorganism that has been introduced to it. With
this, there is a higher risk for the client to have a postpartum
● Prolonged and difficult labor
infection.
○ Prolonged and difficult labor that would already require the
assistance of instruments
8 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
NURSING DIAGNOSIS When she develops the infection, then everybody is not allowed
1. Risk for infection related to loss of uterine sterility with childbirth to go near her as she might be having an infection that can be
● Prioritize our care to prevent infection from occurring to our easily passed on to someone and even the infant.
client ● Make her know the situation and make sure that she follows the
● Goal: Patient will be free from any signs of infection (increase protocols of the institution to make the people around her safe
in temp after 24 hours, foul smelling lochia) from infection until the cause of infection is is discovered
● We consider infection if the elevation of the temp of the client ● Goal: Patient will acknowledge and will be willing to comply to
occurs after the first 24 hours of childbirth because the first 24 agency policy to protect others from microorganisms (Patient’s
hours postpartum, it is expected that the client will have temp >38 C for 2 consecutive 24 hours, infant is placed in
dehydration because of the process of labor therefore their CLOSED incubator in patient’s room until source of infection is
temperature may rise a bit. identified)
● Foul smelling lochia is an evidence that there is already a ● Once the source of infection is identified and is not contagious
bacterial infection in the intra uterus of the client or not an infection of the respiratory if GI system that can be
● Interventions: easily passed onto another person, the infant can now be
○ Maintain sterility of all equipments that will be removed from the enclosed incubator
introduced in the vaginal canal - prepare sterile ● Interventions:
gloves to be used ○ Explain to patients that if infection is not
○ Teach patient about proper perineal care and transmittable, she may be allowed to hold her
importance of handwashing - When you wash the newborn but the importance of handwashing must
perineum, wipe from front to back so that any be emphasized - e.g. if the infection is just an infection
microorganism from the rectal area, it will not be of the perineum which is not contagious, but
brought upwards to the vaginal opening or urethra. everytime that she washes her perineum which is
Handwashing should be done before and after the infected by the microorganism, then she has to wash
perineal care. her hands before touching the infant to make sure that
○ Instruct clients about important information on she doesn’t pass on the microorganisms that are
antibiotic therapy present in her discharges.
○ During postpartum, it is a protocol to give antibiotics ○ If patient needs to be isolated from the newborn,
as a prophylactic treatment because you want to provide emotional support - there are times there are
prevent infection because there is a high risk to mothers that are infected with disease that can be
develop infection esp if the client has an episiotomy transmittable and they have to be separated, the other
or undergone C-section where there is a chance for ill be devastated therefore you have to provide
the microorganisms to migrate. support, explain, let them verbalize, and be there for
■ She must finish the whole course them until they are allowed to hold their newborn.
■ Prescribed antibiotics must be
compatible to breast feeding - there are Endometritis
times that antibiotics may harm the baby. ● Inflammation and infection of the endometrium (the lining of the
Watch out for white plaques or thrush in uterus)
mouth (signs that it has passed through the ● Usually associated with CS or Chorioamnionitis
breast milk and there is already fungal ○ During CS, instruments are used. There is a presence
infection) or easy bruising in infants (this of incision. The intrauterine lining is really exposed
will be a manifestation that the production and there is a high risk that a microorganism is
of Vitamin K is already affected because of introduced to this area.
the ingestion of the infant of antibiotic ○ Chroioamnionitis is the infection of the chorion and
through the breast milk because Vit K is an amnion. It can be infected if the bag of water is
important part of the production of clotting ruptured greater than 24hrs before the patient
factors, if it is deficient, the the baby may delivers. It is more exposed to pathogens. If the px has
be prone to bleeding and bruising). this condition, it means that there was already an
2. Social isolation related to precautions necessary to protect baby infection that happened to the patient because of the
and others from exposure to infectious microorganisms opening that was due to the rupture of the amniotic
● If the client is with infection already sac.
● Most common problem that arises
● In some institutions, if the client has been discovered that she has
s/sx of infection, unless it is a condition that can be easily
contagious for others, then she will be isolated from everyone,
even her infant. This is a problem because the expectation of all
postpartum clients is that after delivery, it is a happy moment that
she will be together with her baby and relatives could visit them.
9 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
ASSESSMENT ● Analgesics
● Temperature elevation of over 38℃ for at least 2 consecutive ○ Client has an inflammatory process going on the
24 hrs starting on the 3rd or 4th day PP endometrium which is painful, and making it contract
NOTE: will add to the pain.
• WBC NORMALLY increases during postpartum due to stress
therefore elevated WBC will not be conclusive of presence of NON-PHARMACOLOGIC MANAGEMENT
infection. ● Increase fluid intake
• Breast filling causes elevation of temperature and also happens on ○ To help with the symptoms of fever and lower it down
the 3rd or 4th day PP a bit
o Chills, loss of appetite, body malaise ● Semi fowlers
o Uterus: note well contracted and painful to touch ○ Head of the bed raised
o The inflammation of the endometrial lining causes ● Ambulation (if tolerated)
pain when touched ○ This will drain the lochia that is infected by bacteria.
o Lochia: dark brown, foul smelling When it is expelled from the uterus, the uterus will
o NR: Give patient health teaching that on the 3rd and 4th day of now have a faster healing process (also putting in
PP , if their temp. increases over 38℃ they should not dismiss semi fowlers)
this as a side effect of lactation. Remind them to monitor ● Hand washing
themselves as well and let you know if they have a fever and other
s/sx that could indicate that the patient has endometritis. COMPLICATION
● Usually lasts for 7-10 days if infection is limited to endometrium
MANAGEMENT ○ If a client was not diagnosed with endometritis and it
Vaginal discharge culture is not a complicated case, it will be gone by 7-10 days.
● Use sterile swab The infection in the intrauterine lining if not detected
○ Sterile equipment (cotton early can spread and have an effect on the fallopian
applicator) tubes.
○ Provided with test tube that is ● Can lead to tubal scarring and infertility
also sterile where you will place ○ If the fallopian tubes are affected even if the client
your sample recovers, it could lead to scarring which narrows the
● Obtain sample from the vagina tube and causes infertility or fertility problems.
○ Nurses should collect the discharge from the vaginal ○ Give health teachings to the client about this possible
discharge directly from the vaginal canal to be sure complication especially if they have a complicated
that you are getting the microorganism that is actually type of endometritis
causing the infection, not from the perineal pad of the
client because it is not sterile and can be exposed to WHO IS AT RISK?
anything, and it may already have other ● Women with suture line in the perineum from episiotomy or
microorganisms and not the one that causes the repair of laceration
infection in the client ○ Wound or opening in the skin at the perineum
NOTE: Before the doctors could give the appropriate antibiotics, there
would be a culture and sensitivity test. ASSESSMENT
● Pain
PHARMACOLOGIC MANAGEMENT
○ Pains seems to
● Clindamycin (Cleocin) as usually determined by culture and increase by the hour
sensitivity over the area of the
○ Usually the microorganisms that are tested, are repaired laceration or
sensitive to clindamycin. Most of the time, expect that episiotomy
this would be the drug of choice for clients with ● Heat
endometritis ○ Warmth over the area
● Oxytocic agent to encourage uterine contractions ● Feeling of pressure at the suture line
○ Methergine - for patients that have already been sent ○ Building pressure over the area
home since it happens during the 3rd or 4th day ● Fever if the infection has a systemic effect
○ Oxytocin drip - if client still has IV ○ If the microorganism has affected the blood vessels
○ NOTE: Aside from the process of infection, the already
relaxed uterus could cause another problem which is ○ Not so much if the infection if localized at the perineal
bleeding. The non-contracted uterus should be dealt area only
with also during the course of endometritis ● Inflamed suture line
10 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
○ Reddened and if it is already days old, then there ○ Patient placed in a lithotomy
would be a discharge that is foul smelling, coming position, legs are raised using
from the wound itself and not the lochia stirrups which can impede the
circulation or flow at the popliteal
MANAGEMENT area. When the blood flow is
● Culture and sensitivity impeded and becomes stagnant,
○ The discharge at the area of affectation to know which it can lead to blood clot.
is the proper antibiotic to be used ● Inactivity during pregnant
● Antibiotics ○ The ones who have complications or problems with
● Drainage of wound weight (obese patients) they cannot walk for a very
○ Especially if there is already development of abscess long time because the pain is more severe in the hip
○ Sometimes the doctors would remove the stitches to area and heel, then there is an added weight of the
let the wound dry growing fetus, therefore they have a tendency to be
● Sitz bath inactive and have a sedentary lifestyle
○ Let patient sit over the sitz ● With pre existing varicose veins
bath ● With postpartum infections
● Hubbard Tank ● Older than 35
○ Submerge the greater part ● History: thrombophlebitis, smokers
of the body in water ○ Smoking decreases the diameter of the blood vessels,
● Change the perineal pads frequently therefore it will become easily irritated even if small
○ To help in the elimination of the microorganism clots will be formed
● Proper perineal care
Femoral Thrombophlebitis
Thrombophlebitis ● It happens usually in the greater saphenous vein, popliteal vein,
Phlebitis and femoral vein
● Inflammation of the lining of the blood
vessel
● In intravenous cannulation or therapy
Thrombophlebitis
● Inflammation with formation of blood clots
● Blood clots inflamed and irritated the
blood vessel wall
● Superficial vein thrombosis - you can see the ● Arterial circulation also diminished
blood vessel infected ○ It is not just the venous circulation that is affected
○ Usually seen on the veins on the ● Edema
upper extremities or the foot ● Pallor of affected leg
● Deep vein thrombophlebitis - affects the larger ○ Because of the affectation,
veins there is a significant pallor
when you compare it to an
WHY ARE POSTPARTUM AT RISK? unaffected leg
● Elevated fibrinogen level
○ Makes blood clot more easily which is true for all PREVENTION
pregnant clients ● Ambulation
○ Once they delivered, it does not automatically go ○ One of the risk factors for thrombophlebitis is
away inactivity
● Lower extremity veins are dilated ○ Encourage the client to do early ambulation as
○ Because of the pressure of the presenting part, usually tolerated and as permitted by the health care
the head of the baby, over the lower pelvic cavity of provider
the patient ● Limit stirrup time
○ During labor and delivery
WHO ELSE IS AT RISK? ○ Only place the client on stirrups if there is a need to
● Inactive women during labor and early postpartum inspect the perineum, or to do perineal care
○ Those who are bed-bound, not allowed to ambulate, ○ After that, if not necessary, remove client’s leg from
to walk, or to turn, and stagnant in their position the stirrups
therefore they are more prone to blood clots that can ● Support stockings on first 2 weeks for those with
irritate the lining of the blood vessel varicosities
● Prolonged time leg is in stirrups for a long time ○ We have to emphasize to them that it is not the
11 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
pantyhose type. of milk that can be consumed by the baby
○ Medical support stocking after the coumadin therapy
- it is only up until the area ● Assess for signs of bleeding and increase in lochial
below the knee, it will discharge
support the blood vessel ○ With a previous implantation sita of the placenta at
so that the circulation will the uterus - The anticoagulant therapy could increase
get better. the bleeding or lochial discharge
○ Advise the client to wear it ○ Teach the client to monitor and report the lochial
before getting up from discharge if she notices that it becomes a clotted
bed so that the blood vessels will not be filled yet blood or heavier to the point that she is showing
with blood and there would not be an accumulation signs of deficient blood volume (dizzy, more pale),
of blood. When they stand up, the flow of blood to advice to tell her doctor right away
the blood vessels of the lower extremities will be
controlled and it will not cause stagnation or cause Mastitis
any development of blood clots ● Infection of the breast
ASSESSMENT
NOTE: Symptoms usually occur 10 days postpartum (client will already be
at home)
● Doppler ultrasound confirms diagnosis
● Localized redness, swelling, warmth
● Hard, inflamed vessel in affected leg
● Positive Homan’s Sign
○ Will elicit pain when you dorsiflex the foot of the • Normally for a healthy breast (left picture) - duct will contain the
client milk and there would be no problem, milk supply is okay, the
client reports that she is lactating well
TREATMENT ● For clients with mastitis (middle and right picture) - the
● Application of moist heat pathogens have entered through breakage in the skin, it can
● Bed rest inflame the lobes and will now cause the breast milk to
● Elevation of affected leg decrease and cause signs of infection such as inflammation,
● Mild anticoagulants (Aspirin) skin redness and pain
● Antibiotics if with infection ● Usually caused by the entrance of the microorganism in the
● NEVER massage over the clotted area because this could breakage in the skin of the nipples of the client
loosen the clot and cause pulmonary or cerebral embolism ● Nosocomial infection
○ Once the affected part is identified (e.g. popliteal), ○ There are times that it is caused by the infant, if the
never massage because it might dislodge the blood infant acquired an infection caused by
clot staphylococcus aureus or worse by the methicillin
○ Pulmonary or cerebral embolism is very fatal to the resistant staphylococcus aureus (MRSA) and will have
client nasal discharge and suck on the breast of the
● Anticoagulant Therapy mother, the infant could transfer the pathogen to the
○ Heparin mother.
■ Can be continued until symptoms resolve ● Epidemic mastitis
■ Safe during breastfeeding ○ If the mother got the mastitis through that route, she
■ Subcutaneous injection - teach the client can spread it to other breastfeeding mothers
how to self-inject this to continue her
treatment at home PREVENTION OF NIPPLE CRACKING OR FISSURES
○ Coumadin ● Correct latching
■ Are passed in breast milk ○ Good latch - Lip is
■ Discontinue BF while on this medication protruded outward
■ PUMP and DUMP - if the client still wants and attached to the
to continue breastfeeding after the breast of the mother
coumadin therapy - teach or encourage ○ Bad latch - Lower lip
them to empty the breast by pumping and is pushed inward
expressing the milk and then throwing it while it was attached
away (not given to the baby to consume) to the breast of the mother and will cause abrasion
just to maintain the supply of milk in the on the nipple of the mother and become a crack
breast so that there is a sufficient amount overtime.
12 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN POSTPARTUM CONDITIONS
● Correct nipple release ● Continue breastfeeding or maternal expression
○ If the mother have to remove the infant from the ○ Continue breastfeeding - if there is no abscess
breast in the middle of breastfeeding, it is not right ○ Manual expression and dumping or throwing away
to just pull the infant away from the breast the breast milk - if there is an abscess
○ Push the chin downwards so the mouth will be open ● Cold or hot compress
and the suction from the breast will be release and ● Good supportive bra
then she can now remove the infant from the breast ○ With thick straps which decreases discomfort during
● Hand washing mastitis
● Exposing to air
○ For a few hours each day so that it is not constantly COMPLICATION
wet that it can be macerated and be prone to
breakage
● Vitamin E ointments
○ Lanolin cream - contains vitamin E to make sure that
the nipple won’t dry and crack easily
● PUMP and DUMP - if abscess is present (no breastfeeding)
● Unaffected breast when infant sucks forcefully
● Treated by incision and drainage - It will not heal unless the
○ If there is already starting cracking or soreness on
incision is drained
one breast, advice to breastfeed initially on the
● Sometimes the abscess formation and mastitis is treated late
unaffected breast to prevent further development of
that it already caused breakage in the skin even w/o incision
cracking or fissures
and drainage, there is already necrosis seen at the area that is
○ Initial breastfeeding - the infant is very hungry so
affected
they would suck forcefully and could worsen the
beginning crack or fissure and open up and become
a wound
○ If the infant is already sucking normally and not
forcefully sucking, then breastfeeding can be
continued on the affected breast
ASSESSMENT
● Usually unilateral pain, redness, swelling of breast
○ It is very rare that both breast are affected with
mastitis
○ Swelling is localized over one area of one breast,
only that part that is painful and reddened
● Fever
● Scanty milk
○ The ducts are inflamed and cannot express the milk
that it is holding
● Sonogram to make sure breast abscess is not present
○ If an abscess is suspected because there will be a
different treatment for these clients
MANAGEMENT
● Antibiotics
○ For penicillin resistant organisms (or MRSA):
dicloxacillin or cephalosporin
○ Effects usually at 3rd day
■ Advise the client to finish the whole
course of antibiotics until 7 days usually
and not until the symptoms subside or no
longer there
13 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
GYNECOLOGIC DISORDERS TYPES
● Primary
MENSTRUAL DYSFUNCTIONS
● Relative or secondary – inability to conceive following the birth
A. Amenorrhea - absence of menstruation anytime between puberty
of a child or difficulty in achieving another pregnancy after a
and menopause (not a disease but a symptom)
previous conception
1. Primary - failure of menstruation to appear initially at puberty
● Absolute – pregnancy in forever impossible
2. Secondary – cessation of menstruation after menarche
a. Physiologic – normal absence before puberty,
during pregnancy, lactation and menopause ETIOLOGY
b. Cryptomenorrhea or Pseudomenorrhea – Causes in the Male (40%)
menstruation occurs but does not appear externally 1. Infection which may obliterate the main sex ducts
because of obstruction in the lower genital organs 2. Trauma or injury – which may close the ducts
c. Pathological – due to some pathological diseases of 3. Toxic conditions – which may devitalize the germ cell
the reproductive system 4. Severe illness – leading to physical exhaustion and impotence
B. Oligomenorrhea - reduction in frequency of menstruation of 5. Insufficient sperm count – caused by:
prolongation of interval abnormally, usually from 38 days to 3 months ○ Disease like orchitis- a complication of mumps
C. Polymenorrhea - interval is shortened or more frequent occurrence ○ Anomalies of reproductive tract
of menses, usually every 20 days ○ Idiopathic tubular atrophy – leading to
D. Hypomenorrhea – scanty menstrual flow without relation to azoospermia
frequency 6. Impotence and premature of ejaculation – which may
E. Hypermenorrhea or Menorrhagia – excessive menstrual flow interfere with the deposition of the sperms in the vaginal canal
F. Metrorrhagia – bleeding or spotting without obvious relation to 7. Accidental division of the spermatic cord – as what may
menstrual cycle. Also known as intermenstrual bleeding interfere in surgeries like herniorrhaphy
G. Dysmenorrhea – painful menstruation with spastic, crampy and 8. Faulty diet – especially deficiency in Vitamin C and E
congestive pains
SPERM ANALYSIS
POSSIBLE CAUSES OF MENSTRUAL DYSFUNCTIONS The sperm can be examined on the basis of:
● Neurogenic – organic lesion or idiopathic hypothalamic 1. Quality in terms of content
dysfunction 2. Ease at which conception is attained
● Pituitary – insufficiency of hormones, tumors or congenital
defect Quality is good if:
● Psychogenic – minor or major psychosis ● Volume/ejaculation – 3-5 ml
● Chronic illness ● Number of sperms/ml – 60-120 Million
● Metabolic diseases of the pancreas, thyroid and adrenals ● 60-80% are actively motile a two hour interval
● Nutritional disturbances like malnutrition ● 85% sperm cells/ ejaculation are normal in form
● Ovarian – as in tumors or congenital defects
● Congenital defects – like imperforate hymen, absence of CAUSES IN FEMALE (60%)
vaginal septum (gynatresis) 1. Infection like endometritis which may obstruct the tubes
● Traumatic – like stenosis of vagina or cervix due to trauma 2. Immaturity of the reproductive organs
3. Anomalies of the reproductive organs like:
GENERAL METHODS OF TREATMENT ● Imperforate hymen
Each patient must be treated according to etiologic factor ● Absence of vagina
1. Steroid therapy – designed to etiologic factor ● Tumors
2. Gonadotropic therapy – designed to replace pituitary ● Uterine displacement
hormones ● General debility like renal and cardiac disease
3. Clomiphene therapy – stimulate pituitary activity through the ● Disturbed endocrine functions
hypothalamus ● Faulty diet – Vitamin C and E
4. Hypothalamic hormone stimulation which directly stimulate
synthesis and release of pituitary gonadotropins (under DIAGNOSIS
research) ● Thorough history including marital history
5. Good nutrition ● Complete physical exam of both husband and wife
● Assessment of ovulation
Infertility ○ BBT
● failure to conceive after 1 year of unprotected sex. ○ Spinnbarkeit
● Sterility – term used only for individual who has some absolute ● Urine test for adequate levels of pituitary gonadotropins (FSH
factor preventing procreation and estriol)
1 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
● Endometrial biopsy done on the 21st day of the menstrual ● Terminated with the completion of menopause or
cycle to determine if the secretory phase is occurring climacterium
● Rubin’s test to check for tubal patency ● Physiological changes that are notable are related to
● Hysterosalpingogram vasomotor instability
○ temperature regulating system is affected → hot
MENOPAUSE flashes (feeling that upper body is warm while
Gynecologic geriatrics - refers to changes in the reproductive organs due extremities are cold), night sweats
to aging ○ More irritable, moody
● Estrogen levels go down
REPRODUCTIVE CYCLE ● Ends when the menstruation stops
● Menarche - beginning of reproductive cycle; start of menses 3. Menopause
● Reproductive period - approximately 35 years ● It is the end of menstruation
● Menopause - end of reproductive cycle ○ Some may think their menses are over but it is only
● Onset of women’s reproductive period is when they are able to confirmed if 12 months have passed without menses
mature and release the eggs (time they can get pregnant) ○ Menopausal pregnancies - woman doesn’t know
● Ovaries already formed the eggs ever when we were still in the that she still has few eggs left → sexual intercourse →
womb; when girls are born, they already have egg cells in their possibility to get pregnant
ovaries ■ Dangerous pregnancy because complications
○ Around 400,000 immature eggs (primordial) may arise due to risk factors (age & unbalanced
○ At 7 years old, half of these egg cells have died hormones)
○ By the time we reach the age when we start maturing ● The age of menopause ranges between 45-55 years old
& releasing the eggs, we lose most of them until such ● Average being 50 years
time when there’s no more egg left in the ovaries 4. Post Menopause
● In males, they start maturing sperms during puberty and ● The time after which a woman has experienced 12
continue producing healthy sperms until they get old; can still consecutive months of amenorrhea
have children even after 50 years old ● No need to use birth control
Menopause - from the Greek word ‘mens’ meaning “monthly” and ‘pausis’ Physical Changes
meaning “cessation”; cessation of monthly periods/menstruation Decrease in estrogen causes:
● Part of a woman’s natural aging process when her ovaries ● Gradual atrophy of the reproductive tract
produce lower level of the estrogen and progesterone ○ Estrogen is needed for the growth of reproductive
● She can no longer become pregnant organs
● Also called as “Empty Nest Syndrome” ○ No baby will pass through anymore → reproductive
● Women find it hard to adapt initially organs needs to rest
● Change in life of a woman ● Vulva loses contour and tumescence
● Grand climacteric ● Labia shrinks
● Usual age of menopause: age 40 ● Labia thin and pale
○ Women starts to see signs ● Vaginal mucosa becomes thinner and smooth
● Average age for natural menopause: 51.5 ● Vaginal atrophy / Decrease in vaginal secretions → prone to
○ Time menses stops atrophic vaginitis
● Surgical menopause - effect of radiation, removal of ovaries ○ Vagina becomes dry → frequent infections
○ Removal of ovaries → no more supply of estrogen & ● Uterus gets smaller and firm
progesterone hormones ● Breasts lose fullness and reveals atrophy and shrinkage
○ Hysterectomy (removal of uterus) → woman still has ○ Tendency of breasts to sag if not supported when
ovaries → will not menstruate → but not yet surgically younger → change in body image
menopause because she still has ovaries supplying ● Decrease breast size
her with estrogen & progesterone ● Ovaries become small, firm, and atrophic
○ Radiation treatment can alter the normal functioning ● Uterine atrophy
of ovaries ○ Decrease in uterine tone
○ May cause prolapse of the uterus
PHASES OF MENOPAUSE ■ Uterus is held in place by ligaments →
ligaments get weaker as woman ages →
1. Pre-menopause
● Initial or beginning uterus has tendency to go down and enter
2. Perimenopause vaginal canal
● Changes are observable ○ May have pessary (supportive device) or
● Physiological changes associated with the end of hysterectomy
reproduction capacity
2 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
■ Pessary can be used to hold the uterus if ○ Curvature in the spine (wedged upper vertebrae or
the prolapse is inside the vagina kyphosis “kuba”) due to the loss of bone density
■ If the prolapse is out of the vagina → needs 3. Bone mineral analysis (Vitamin D, Calculated calcium levels)
to be removed through hysterectomy ● To know if there is calcium and Vit D retained in the bones
4. Bone density scan (DEXA scan)
Changes in Metabolism ● To determine the degree of osteoporosis
● Increase on low density lipoprotein (LDL) → increased
cholesterol levels MEDICAL TREATMENT
● Decrease in high density lipoprotein (HDL) which carries ● Allendronate (Fosamax)- prevents bone resorption
cholesterol to liver for excretion ○ Take in the morning with plenty of water, 30 minutes
○ Estrogen helps in keeping the good cholesterol (HDL) before eating breakfast
high and bad cholesterol (LDL) low ○ Instruct patient to stay upright for 30 minutes after
● Hyperlipidemia - lead to gradual rise in the risk of heart disease taking to avoid reflux and other GI symptoms
and stroke after menopause ■ Possibility to have acid formation if person
○ Since LDL is higher than HDL → clogging of arteries have taken medicine w/o food → if person
or atherosclerosis → woman is more prone to lies down immediately without staying
problems of heart disease and stroke upright for 30 mins → acid reflux →
discomfort
Psychosocial Changes ● Calcitonin - allows calcium to go to the bones
● Grieving over the end of childbearing years ● Estrogen replacement - 0.625 mg daily; not used in the past
○ Especially if the woman has not given birth ○ Not used continuously; hormone therapy not used
● Aging issues unless really needed
● New role as a grandmother ● Calcium - 1500mg daily
○ Some may want to just rest at this moment in their life ○ Double the dose of calcium supplements since no
rather than take care of grandchildren → depression, matter how much the woman takes, she is not able to
mood swings, problem in contentment retain a lot
● Depression, mood swings, or contentment ○ Normally, the body only needs ~800 mg/day
● New sense of vitality and increase in libido ○ Best time to take calcium is at night because it can
○ Desire to have sex increases since they are not afraid cause muscles to relax → sleep better
to get pregnant anymore ○ Drink lots of water for better absorption
○ But due to changes in the vagina (dryness) → ● Vitamin D - 400 to 800 units daily
dyspareunia or pain during coitus ○ Can get in form of supplements
○ NR: Advise the woman to use water-based lubricant ○ Good way to utilize it is to expose self to sunlight
to lubricate the vagina if they tell you that they want to
have sex but are afraid to do so because of the pain NURSING DIAGNOSES RELATED TO OSTEOPOROSIS
● Risk for injury (fractures, complications) related to lack of
Psychological Changes knowledge about causes, prevention, and treatment for
● Frequent headache, irritability, fatigue, depression, insomnia osteoporosis
● Although these are often said to be due to changes in the ○ Usually smaller bones
hormonal levels, they are more likely to be related to the loss of ○ Worst kind of fracture: pelvic fracture since the bone
sleep due to night sweats won’t heal anymore so the woman will not be able to
● Diminished interest in sex may be due to emotional upset or walk without the help of a wheelchair
may be secondary to painful intercourse due to dry vagina ○ Advise them to be accompanied by somebody when
they have to move about or to use a walker to support
Risk of Osteoporosis them when they walk
● Loss of bone density → bones become more brittle ■ Walker is better than a cane since it has 4
● Estrogen helps in calcium absorption and retention in the bones wheels while a cane can still cause
→ when estrogen levels drop, there is decreased ability to retain imbalance
calcium and Vit D ○ Avoid any kind of exercise that can make them
accident or injury-prone (no contact sports, no
DIAGNOSIS jumping)
1. History ■ Example of possible activities: walking,
2. Physical Exam swimming, light aerobic activities, dancing
● Check patient’s height ● Impaired physical mobility related to fractures or fear of
○ It will reveal a decrease in height because there is a fractures with bone loss
curvature of the spine ○ Sometimes there is pain on their back and hip when
● Difference in posture they stand up → they will fear standing up and walking
3 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
○ Impaired physical mobility → risk of poor circulation result to problems in the uterus → can lead
→ thrombus to uterine cancer
○ Advise that when they have to move, make sure that ○ Contraindicated in patients with thromboembolitic
they are able to support themselves with handrails or disease, undiagnosed vaginal bleeding, pregnancy,
handles that they can hold on to lactation
○ When they stand up, they should wait for a while ○ Use of estrogen only increases risk for cancers
before attempting to walk and stretch first influenced by hormones (breast, ovarian, cervical)
○ Do not make old people walk fast because greater risk ● Patient Education
for accident ○ Take medication with meals to prevent nausea
○ Don’t attempt to push them since they can easily lose ○ If missed dose do not double the dose
balance ○ Withdrawal bleeding when meds are d/c
● Altered nutrition: less than body requirements for calcium ○ Report unexplained bleeding
related to age and adequate intake of calcium ○ No smoking
● Knowledge deficit related to causes, prevention, and ○ Use sunscreen with SPF of at least 15
treatment of osteoporosis ○ Compliance with follow up care
○ Advise to quit smoking since it can cause vasospasm 3. Medroxyprogesterone
& vasoconstriction → diminished blood flow to organs ● Provera, Cycrin, Amen
→ further delay transport of minerals including
calcium in the bones ALTERNATIVE TREATMENT
○ Avoid alcohol (toxic substance), caffeinated ● Vitamin E, ginseng, dong quai, and other complementary
beverages (has diuretic effect → loses calcium) supplements decrease hot flashes
■ As much as possible decaffeinated or only ● Water soluble lubricant
1 cup of coffee per day ● Kegel exercises
● Hydration - 8 glasses of water daily
NURSING INTERVENTIONS FOR OSTEOPOROSIS ● Wild yam cream topically
● Weight bearing exercises which increase lumbar bone density
○ Exercises for lower body NURSING DIAGNOSIS FOR MENOPAUSE
○ Ex. walking, hiking, stair climbing, dancing NOTE: The nurse can play an important role in helping women cope with
○ No jumping and jogging the symptoms of menopause; Teaching and counseling about
● Avoid high impact exercise menopause, its symptoms, and medical and alternative therapies are
● Diet: high calcium diet foremost in the arsenal of interventions available to nurses in this area
● Anticipatory grieving related to loss of childbearing ability
NURSING INTERVENTIONS FOR MENOPAUSE ○ Let them verbalize their concern, they may need help
1. Explain all changes and s/sx (counseling, psychotherapy)
2. Hormone Replacement Therapy (HRT) ● Self-esteem disturbance related to physical and emotional
● In cases where patient has life threatening conditions (e.g. heart changes associated with menopause
disease) ○ Low self-esteem → not able to solve own problems,
● Not everyone needs it; only given if very serious becomes more depressed
● More likely estrogen replacement ○ It is important that they understand their own changes
● Estrogen with or without progestin is given for a short period of and be able to deal with them
time to relieve vasomotor symptoms (hot flashes) ○ Ex. feel hot/cold - adjust room temperature; wear
● Has been used in the past as protection from bone loss and appropriate clothes; insomnia - find relaxation
osteoporosis exercises (listening to radio)
● Ex. Estrace, Premarin, Ogen are all used as conjugated ● Knowledge deficit related to normal changes and symptoms
estrogens, jasmine ○ Provide them information that is necessary to make
● Nursing Considerations them understand that these changes are part of the
○ Assess VS prior to and during therapy aging process
■ To compare baseline ● Altered sexuality patterns related to hormonal changes and
○ Protect skin from direct sunlight decreased vaginal lubrication
■ Skin is extra sensitive due to loss of
estrogen → skin can easily burn
■ Use sunscreen, sunblock, and avoid skin
exposure to sun
○ Assess for increase or decrease in vaginal bleeding
■ Any signs of vaginal bleeding is an
indication that the hormone given can
trigger abnormal lining of the uterus → can
4 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
SEXUALLY TRANSMITTED INFECTIONS SYMPTOMS
Something nurses should be aware of so that we can do some interventions ● Thick, curdy vaginal discharge - thick and whitish
to help our patient and to prevent transmission from one infected person to ● Severe itching - since it is a fungal infection, pruritus (itchiness of
the next. vagina) is very common, also felt in the vaginal canal (it is
irritated)
RISK FACTORS ● Dysuria (pain during urination) - urinary system is affected
1. Age because infection can go upwards
● The younger the person is, the more sexually active a person is, ● Dyspareunia (pain during sex) - during sexual activity, inflamed
the more likely she will be exposed to these risks of sexually vagina causes irritation → woman feels pain during sex
transmitted infections
● Sometimes young people are not afraid to get sick → risky PHYSICAL EXAM
behavior → put themselves in a greater chance of developing ● Labia may be swollen
the disease ● Speculum exam reveals thick, white
tenacious cheese like patches adhering
2. Multiple partners to the vaginal mucosa
● Put women at risk for infections
● The more partners you have → likelihood of getting infected is TREATMENT (PREGNANT)
greater ● Intravaginal insertion of Miconazole, Butoconazole or other
● If one person is infected → transfer it to multiple partners → topical azole preparations for 7 days
transmission that can go to a lot of people ○ Antifungal
● Epidemiology and case finding - if you reported one infected ● Clotrimazole suppositories at bedtime for 1 week
person, they will trace the contacts and from there they can test ○ Combination of Miconazole and Clotrimazole for
to know who is infected because they do not want to spread it all treatment
over the place (E.g. Trichomonas Vaginalis) ● Cream may be prescribed for topical application on the
● Some people are asymptomatic vulva (on the outside surface) if necessary
3. Oral contraceptives ○ First thing they can do
● Can change the vaginal environment → making the vagina more ○ The area that has an irritation is very raw and can also
susceptible to overgrowth of microorganisms that are already have openings that create more problems for the
there (opportunistic microorganisms) woman
● Vaginal condition is altered by hormones (synthetic ● Oral medications as antifungal agents used for treatment are not
hormones/drugs that act like hormones) that are taken orally → safe during pregnancy
make one more prone to develop infections
FETAL-NEONATAL RISKS
Vulvo Vaginal Candidasis ● Thrush if delivered vaginally
● Moniliasis or yeast infection
○ If the vagina has the infection and she is having
● Causative organism: Candida albicans
discharge during pregnancy and the baby passes
○ Common organism in our vagina
through the infected birth canal, the baby can have
○ Opportunistic (waiting for a chance to multiply)
the infection → baby’s mouth → oral thrush or oral
candidiasis (white patches on the tongue and very
CONTRIBUTING FACTORS painful) → nahihirapan mag breastfeed due to lesions
● Oral contraceptives - alterations of the condition of vagina can brought about by the infection
help them grow ○ That’s why treatment should be done early
● Immunosuppressants
● Antibiotics - when you use this to kill bacteria in your body it can
NURSING INTERVENTIONS
also kill the good bacteria that are protecting the vagina →
1. Avoid douching
normal flora
2. Wear cotton underwear - she has to wear something that can
● Frequent douching - vagina is cleansed internally using
absorb the discharge, don’t wear anything that can trap moisture
solutions → alter the vaginal pH → more prone to overgrowth of
(e.g. underwear with lycra material) → moisture can be a good
candida
medium for the growth of organism
● Pregnancy - high glycogen content of vagina brought by
3. Clean perineal area from front to back
hormonal changes → vagina becomes a good medium for the
4. Use condoms - if the woman is infected use condoms to avoid
growth of this organism
transmission, contamination or infection of the partner
● DM - has a lot of glycogen that makes the vagina a good medium
for growth of candida
5 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
Trichomoniasis ● Avoid drinking alcohol (with Flagyl)
● Something you don’t want to have ○ Avoid anything with alcohol
because it stays in the body for a ○ If alcohol enters her system while taking this
while medication → her body will react with vomiting
● Causative organism: Trichomonas (similar to the effect of antabuse → drug for alcoholics
vaginalis to prevent them for drinking because when they take
○ An anaerobic (organism this they will vomit)
that will not survive in the presence of oxygen) ○ Mouthwash with alcohol - you may ingest the alcohol
protozoa that lives in an alkaline environment kasi minsan di mo nalalabas lahat and nalulunok →
○ If the vagina is naturally an acidic environment, it will triggers vomiting
die ● Can give vinegar douche if pregnant or if adolescent
○ During pregnancy, vaginal pH is altered → risk for ○ You alter the vaginal environment to kill the organism
Trichomoniasis ○ Vinegar douche when pregnant, because
● Most infections are acquired through sexual intimacy Metronidazole cannot be given (teratogenic)
○ When males are infected, they don't show signs or ● Treatment of the sexual partner
symptoms because the organism can hide in their ● Use only Metronidazole during first trimester because it is
prostate gland teratogenic
○ Example: the woman is positive for the infection
because she has signs and symptoms but her infected IMPLICATIONS FOR PREGNANCY
husband has no manifestations → hindi gagamutin → ● Increased risk for PROM, preterm birth and LBW
the woman is treated but when they resume sexual
activity → husband can reinfect the wife → “pingpong Bacterial Vaginosis
effect” ● Usually caused by Gardinella vaginalis found in the normal
○ When a woman is diagnosed, partner should also be vagina
screened and identified so he will also be treated → ● Formerly referred to as nonspecific vaginitis or Gardnerella
no risk for reinfection vaginalis
NOTE: Discharge is different from Moniliasis ● Causative organism: Garderella, mycoplasmas, anaerobes
SYMPTOMS CONTRIBUTING FACTORS
● Yellow-green frothy, odorous discharge ● Tissue trauma
○ Sometimes grayish ● Sexual intercourse
○ Frothiness/foamy characteristic sign ● Tissue trauma brought about by sexual intercourse
○ When organism is exposed to the environment and it
has oxygen, it causes the change in the characteristic
SYMPTOMS
of the discharge
● Excessive amount of thin, watery, white or gray vaginal
○ Foul smelling discharge
discharge with a foul odor (“fishy” → dead fish)
○ It has been there for a long time to produce that kind
○ Similar to the discharge being passed out after our
of discharge
period but our mucus is clear
● Inflammation of vagina and cervix
○ Regular discharge is clear and watery
● Vulvar itching
○ Smell is also different
● Dysuria
○ Normal: fleshy smell (malansa) but not malodorous
● Dyspareunia - causes pain due to inflammation and irritation
○ Fishy smell (parang nabubulok na fish)
● Strawberry patches may be visible on vaginal walls or cervix
● Vaginal pH is usually > 4.5
○ Most likely what would tell the doctor that the patient
● To diagnose: wet-mount preparation reveals “clue cells”,
has Trichomoniasis
application of potassium hydroxide (KOH) to a specimen of
● Not transmitted across the placental barrier
vaginal secretions produced a pronounced fishy odor (checking
○ When the woman is pregnant, the infection stays in
the response of discharge to KOH)
the vagina
○ But if the baby passes through the infected birth
IMAGE NOTE: Thin whitish discharge, swollen
canal, the baby can get the infection
labia
○ Baby may get neonatal sepsis
○ If the woman has this infection and is not treated, she
may deliver via CS
INTERVENTIONS
● Assist with saline wet mount prep slide
TREATMENT
● Administer and teach client regarding the use of
● Single 2 g dose of Metronidazole orally
Metronidazole (for treatment)
○ Generic name (Flagyl is the brand name)
6 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
● Clindamycin cream or Metronidazole vaginal gel can be used ○ They should be treated and everything is done to
during the first trimester prevent risk of PID (Pelvic Inflammatory Disease)
○ For the redness caused by irritation NOTE: Infants born to mothers with Chlamydia may have pneumonia or
○ Can be used if the patient is still having her baby conjunctivitis. This cannot be transferred transplacentally but when the
developed because Metronidazole (oral) is baby passes through the infected birth canal, the baby is at risk for having
teratogenic infection in the EYES (OPHTHALMIA NEONATORUM) - only 2 organisms
○ When teratogenicity is not there anymore, that can cause this in the newborn baby (either chlamydia or gonorrhea)
Metronidazole can be used NOTE: If the baby is infected, the baby may die of pneumonia at birth due
to the infection
Chlamydia
● Most common STD in the western countries (United States) LABORATORY DETECTION
● Caused by gram-negative bacteria Chlamydia trachomatis ● Antigen detection
● DNA Probe assays, polymerase chain reaction (PCR Tests)
TREATMENT
● Erythromycin or Amoxicillin followed by repeat culture in 3
weeks
NOTE: Manifestations are the same with gonorrhea in terms of the color of
discharge (mucopurulent → greenish yellow discharge) Difference is that IMPLICATIONS FOR PREGNANCY
sa chlamydia konti lang, sa gonorrhea mas maraming discharge. Pic: The ● If untreated, infant may develop newborn conjunctivitis which is
infection that started from the vagina can go upwards and all the way to the treated with Erythromycin ointment
tubes (fallopian tube infection = pelvic inflammatory disease) ○ To prevent risk of ophthalmia, we apply crede’s eye
prophylaxis to the newborns
SYMPTOMS
● Thin, purulent discharge (yellowish greenish in color but thinner Gonorrhea
and konti lang) ● If you have Gonorrhea, then you most likely also have Chlamydia
● Burning and frequency of urination ● Causative organism: Neisseria gonorrhoeae
○ Possible urinary tract infection that can go with this ● Majority of women are asymptomatic
STD kasi madaling mag ascend yung organism sa
urethra → inflamed urethra SYMPTOMS
● Lower abdominal pain ● Purulent, greenish yellow discharge
○ Due to inflammatory process that goes to the uterus, ● Dysuria
patient feels heaviness or fullness of the lower ● Urinary frequency
abdominal area ● Inflammation and swelling of the vulva
ASSESSMENT ASSESSMENT
● Female: no s/sx or may have heavy yellowish discharge or ● Female: may be asymptomatic or may have purulent vaginal
painful urination discharge, dysuria, they may have inflamed and painful
○ Sometimes they may have no s/sx during the Bartholin’s glands (infected from outside going inside)
beginning of infection but later on it will progress with ● Male: Urethritis (pain on urination and frequency of urination),
symptoms may also have urethral discharge
● Male: non specific urethritis ○ Usually goes to a doctor because they have difficulty
○ When the organism enters to their body through the of urinating & their passing out may pass out like
urethra, it will make the urethra experience the discharge
inflammatory process → urethritis ● Gonorrhea has heavier discharge compared to Chlamydia
○ This can cause infection of the urine
● May lead to infertility and ectopic pregnancy
TREATMENT
○ In females, since it can ascend all the way to the
● Non-pregnant women: Cefixime orally or Ceftriaxone IM +
fallopian tube, pelvic inflammatory disease may be
Doxycycline
resolved but there is possibility that the tubes can
○ Whatever is going to work on the organism
become smaller or have adhesions due to
○ Because some patient may already have resistance to
inflammatory process → big possibility that they are
certain antibiotics
are at risk for ectopic pregnancy
● Pregnant women: Ceftriaxone IM or Cefixime orally combined
○ Worst: totally magclose yung tube → when the tube
with Erythromycin or Azithromycin to address risk of co-infection
is blocked and closed → no chance of pregnancy
with chlamydia
7 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
FETAL-NEONATAL RISKS ○ Not painful
● Infection at time of birth may cause ophthalmia neonatorum in ● Chronic sore throat with hoarseness
the newborn
○ Preventive measure: crede’s eye prophylaxis Tertiary Stage
● Heart involvement, CVS, CNS -paralysis
INTERVENTION ● Congenital Syphilis
○ Enlarged liver, spleen
● Assist with culture
○ Skin lesions
● Administer and teach Cefixime, Ceftriaxone plus Doxycycline
○ Pneumonia
● Teach that if untreated or treatment incomplete it may lead to
○ Hepatitis
PID and infertility for female and may lead to permanent sterility
for female
● Treat partner DIAGNOSTIC TESTS
● All infants are treated with Erythromycin eye ointment ● Blood tests - VDRL, RPR, FTA, ABS
● Dark-field examination of spirochetes
ULCERS AND VAGINAL LESIONS
● Easy to distinguish TREATMENT
Syphilis ● For pregnant and nonpregnant with Syphilis of less than 1 year:
● Causative organism: Treponema Pallidum (spirochete) 2.4 million units of Benzathine penicillin G IM single dose
● Acquired through transplacental inoculation (fetus); results from ○ Safe to give during pregnancy
maternal exposure to infected exudate during sexual contact ○ Anything penicillin-based is safe to give during
● Divided into 3 stages (Primary, Secondary, Tertiary) pregnancy
● Transmitted by sexual contract with a person who has an active ○ Treatment should be started early in the pregnancy
spirochete lesion because the infection of the mother will not transfer
● Can cross placental barrier to the placenta yet
● Incubation period is 10 to 90 days before first symptom appears ○ May start to transfer through placenta starting the 4th
○ Upon exposure, the patient can be harboring the month
organism but does not show anything up to 90 days ○ While the layers of the placenta (syncytiotrophoblast
& cytotrophoblast) are present the organism cannot
Primary Stage pass through
● Painless chancre on genitalia, anus and/or mouth
○ Wart-like appearance FETAL-NEONATAL RISKS
● Stage I - Primary: chancre appears (lasts about 6 weeks then ● Can be passed transplacentally to the fetus. If untreated, one of
disappears) with slight fever, weight loss, malaise the following can occur:
● Lymphadenopathy - may not be noticed ○ 2nd trimester abortion
○ Stillborn infant at term
○ Congenitally infected infant
○ Uninfected live infant
Herpes Genitalis
● Caused by Herpes Simplex Virus II (HSV II)
● Transmission occurs by direct contact with the infected person
ASSESSMENT
Secondary Stage ● Vesicles on the genitalia appear 2 to 20 days after exposure
● 2-4 weeks after primary chancre disappears, there will be ● Clusters on vulva, perineum or perineal area
presence of generalized macular copper-colored rash ● Painful lesions
● Rash will also affect soles of feet and palms of hands ● Flu like symptoms during initial exposure
● Serologic test will be positive ● Recurring episodes during stress, fever, menstruation
● Hepatosplenomegaly ○ The organism will not leave the body, it only stays
● Headache quietly in the nerves until the person becomes
● Anorexia stressed or triggered because of certain factors such
● Condylomata lata on vulva as pregnancy
○ Lesions found on the vulva
INTERVENTIONS
● “Wart-like plaques”
● Assist with culture
● Acute arthritis
● Acyclovir PO reduces or suppressed S/Sx
● Enlargement of liver and spleen
● Abstain from sexual contract while lesions are present
● Nontender enlarged lymph nodes
8 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
● Vaginal delivery is contraindicated for mothers with active TREATMENT (mother)
lesions ● Combination of antiparasitic drugs Sulfadiazine and
Condylomata Acuminata Pyrimethamine
● Genital or venereal warts ● Spiramycin in Europe
● Caused by Human Papilloma Virus
● May be a precursor of cervical cancer TREATMENT (newborn)
● Relatively a common sexually transmitted condition ● Combination of Sulfadiazine, Pyrimethamine, Leucovorin for 1
year
SIGNS & SYMPTOMS
● Soft, grayish pink lesions on the vulva, vagina, cervix or anus Cytomegalovirus (CMV)
● Belongs to the herpes virus group and causes both congenital
INTERVENTIONS and acquired infections referred to as cytomegalic inclusion
● Weekly applications of 85% Bi or Trichloroacetic acid disease (CID)
● Cryotherapy, electrocautery or laser therapy ● Transmission: placenta, cervical route during birth, through
● Skin care body fluids; between human by any close contact e.g. kissing,
● Podophyllin - apply then wash off breastfeeding, and sexual intercourse
● If the mother was infected while she is pregnant, it may cause
TREATMENT multi organ defects to the baby, and the baby might not survive
Based on client preference, available resources, and experience of once he/she comes out because hepatosplenomegaly →
healthcare provider bleeding such as melena
● Client-applied therapies: Podofilox solution or gel or
Imiquimod cream (not used during pregnancy) DIAGNOSIS
● Provider-administered therapy: Cryotherapy with liquid ● Accurate dx in pregnant women: depends on the presence of
nitrogen or cryoprobe CMV in the urine, rise in IgM levels and identification of the CMV
○ Topical podophyllin, trichloroacetic acid (TCA), antibodies within the serum IgM fraction
bichloroacetic acid (BCA), intralesional interferon
○ Surgical removal by tangential scissor excision GENITAL ANOMALIES
○ Shave excision External Genitalia
○ Curettage Variation in Size of Labia Minora
○ Electrosurgery ● One labium is larger than the other
○ Laser surgery ● There are certain situations where you will find abnormalities in
the size of labia minora
IMPLICATIONS ● Labia majora is the external covering of the female, where the
● Large doses of Podophyllin have been associated with fetal labia minora is just beside it.
death ● When you see labia minora hiding behind the labia majora it is
because labia minora is a very sensitive structure.
Torch Syndrome ● Labia minora is made up of erectile tissue → needs to be
● Can lead to fetal abnormalities or deformities such as protected and covered, but what if you see a variation in the size
Toxoplasmosis → one labium is larger than the other → congenital defect of the
● Causative organism: Toxoplasma gondii (protozoan) external genitalia
● May contract organism by eating raw or undercooked meat,
drinking unpasteurized goat’s milk, contact with feces of Agglutination of the Labia
infected cats ● Labia minora and labia majora are held together in the midline
by dense adhesions.
FETAL-NEONATAL RISKS ● “Fused labia”
● Inflammation of the retina, blindness, deafness, severe ● Can either be complete or incomplete (synechia vulvae)
retardation ● But regardless whether it is complete or incomplete, it may be
● Severe disorders → convulsion, coma, microcephaly, related to low levels of estrogen in young girls (common)
hydrocephalus ○ That is why they don’t usually do any treatment until
the girl reaches puberty where she will have more and
more hormones which her body will naturally secrete
ASSESSMENT
and the problem can be corrected.
● IgG and IgM fluorescent antibody tests (IFA)
○ If not possible → resort to surgery
● Indirect hemagglutination antibody (IHAT)
● May resolve on its own or with treatment, or surgery
● Sabin-Feldman dye test
● Ultrasound to detect fetal infection
9 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
Vagina ● Very rigid, meaning masyadong matigas
Congenital Absence of the Vagina ● It can be a problem during coitus because this can lead to
● Usually associated with the absence of the uterus and with dyspareunia or painful sexual contact because the hymen does
anomalies of the urinary tracts not open up enough to give opening → disturbance or a
● Also termed “Agenesis of the Vagina” → absence of the problem to women
vaginal opening
● Quite rare Uterus and Fallopian Tubes
Vaginal Anus or “Atresia Ani Vaginalis” ● Certain problems can be found in the uterus
● Anus and the bowels open into the vagina ● Normal uterus has a cavity and there is a portion
○ Consequence → bowels open up into the vaginal that is connected to the fallopian tubes. There is
canal → there is a chance of contamination → risk of also a cervical portion
an infection
● Surgical correction is necessary
Septate Vagina Absence of the Uterus
● Separation of the canal of the vagina into two ● Occurs with absence of the vagina
where there is a presence of a septum that divides ● Absence of the uterus is also noted where you have absence of
the canal into two → double vagina the vagina
● This becomes a problem only if the woman starts ● If there is an agenesis of the vagina → possibility of absence of
to have sex and starts to have a baby because the uterus
when she gets pregant and its time for her to Infantile Uterus
deliver the baby → problem of the vagina where ● Presence of immature uterus
there are two compartments ● Also known as uterine hypoplasia
● One is usually bigger than the other compartment ● Due to pubertal failure/hypogonadism
● It is hope that in the later part of life → result in fusion that’s look ○ Gonads have a problem.
like isa nalang ang natira despite the presence of the septum ○ It does not develop and because of that, there are
● Female reproductive organs do not fully develop times that they wait for a time for the girl having
● Vagina is divided longitudinally to create double vagina developmental milestones and she has enough
stimulation for the infantile uterus to become normal
Hymen Abnormalities → quite rare that it’s going to be corrected and
● Hymen is covering the vagina, but it does sometimes it could be a reason for the female patients
not really ully cover the surface of the not to have baby (infantile, underdeveloped)
vagina. It is just there to cover it but Unicornuate Uterus
definitely when women menstruate → ● Uterus has only one horn or opening into
something passes to the vaginal canal → fallopian tubes caused by the development of
hymen is more on a crescent shape or like only one mullerial tube.
the shape of a doughnut that has hole in ● Ability to conceive depends upon the maturity
the middle. Sometimes even the use of of the unicornuate uterus
tampons, can change the actual shape of the hymen ● There is only one horn that open up to the
● With sexual activities → hymen will eventually open wider → a uterus, meaning one horn of the fallopian tube
lot of people have the myth that the only time that the hymen will has opening to the uterus
open is during sex but not 100% of time. There are some cases ● Although this is a problem in pregnancy, there is a chance that
that the hymen will open fully during coitus or first time that they this can have a baby for as long as the tube will mature. Even with
have sex and bleed a little bit, but in majority of cases the hymen one horn or tube, the will possibly allow pregnancy, as long as it
is no longer intact. Sometimes even the stretching activities, used will develop → chance of having a baby
of tampons → slightly open it up at the center
Uterus Didelphys
Imperforate Hymen ● Or double uterus, cervix, and vagina due to the
● Absence of hymenal opening presence of a complete septum in the midline
● This is usually treated with incision of the hymen under the ● Kind of uterus that is very very rare because it's
general anesthesia the uterus that is divided into two all the way
● It can’t open up → can be open up by surgical interventions down to the cervix and even up to the vaginal
● An opening is made surgically and they use general anesthesia. area sometimes
It is not painful but the person should not move during the ● Consequence: probably say that this can be a
surgery because there is a possibility of tissue problems if errors problem in having a baby because there is a septum that
are made separates in the midline
Rigid Hymen
● The hymenal opening is normal but the membrane is usually
firm giving rise to dyspareunia
10 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
Bicornuate Uterus Retrodisplacement
● The upper portion of fundus of the uterus is ● Backward displacement of the uterus
divided into two separate horns
● the lower fused to form only one cervix Retroflexion
● Has a two horns and this can be a problem ● Backward bending of the uterus with the cervix
because they are separated but at least they are in usual position
fused at the area of the cervix
Retroversion
● Uterus is tilted backward on its transverse axis
● A greater or less degree with forward rotation of
the cervix
● This will create certain symptoms that will tell you
that something is wrong with the uterus. Normally,
ante (facing front), but in retro, facing back
CAUSES OF RETRODISPLACEMENTS
Uterine Displacements
● Has something to do with the positioning of the 1. Congenital
uterus. ● Observed in uterus of very young girls
● This is because the person could be born with a problem in the
positioning especially seen in the uterus of very young girls
2. Acquired
● Puerperal
○ Due to increased strain on supporting ligaments that
NORMAL ASSESSMENTS
when the uterus involutes, the overstretched
● The uterus has central position in the pelvic
ligaments can no longer maintain it in normal
● The internal os is at the level of the ischial spine
position
● It is either ante verted or ante flexed
○ Puerperal → after birth of the baby
● Anteverted
○ The strain in the ligament that supports the uterus
○ Angle between axis of the cervix and
caused by the pregnancy, and all the even the took
vertical axis of female
place during the delivery, the overstretching of those
○ Angle of the cervix in reference to the
ligaments → it cannot hold the uterus in its normal
axis of the female
position → retroverted
● Ante flexed
● Adrenal diseases
○ Angle between the axis of the uterine body and axis
○ Like inflammatory or endometriosis
of the cervix
○ An inflammation or there could be an abnormal lining
○ The axis of the uterus in reference to the cervix (flexed)
in cases of endometriosis
● Neoplasms
Anteflexion
○ As in large uterine myomas which pushes the uterus
● Bending forward of the body of the uterus
backward or in ovarian tumor located over the
usually seen in small underdeveloped organ
uterine body
● Anterior tilt of the cervix is severe resulting in a
○ New growth; could be benign or something else
much greater forward flexing of the uterus
○ It is most commonly seen in cases of fibroid like
myomas and this could bring normal backward tilting
CAUSE of the uterus because of a presence of a growth, either
● Gonadal deficiency a tumor in the ovary or uterus that is going to cause it
○ Or hypogonadism to have an abnormal placement
● History of Pelvic Surgery
SIGNS AND SYMPTOMS ● History of prior pregnancy
● Crampy dysmenorrhea ○ Ligaments holding the uterus in place become
● Sterility overstretched during pregnancy
● Delayed menarche
SYMPTOMS
MANAGEMENT ● Backache
● Stimulation of growth of the uterus, dilatation of cervical canal ● Dysmenorrhea
and curettage (to be able to facilitate correction)
11 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
○ Become more intense during the period because the ● Overstretching of the pelvic floor especially of the cardinal
uterus cannot contract normally since it is not correctly ligaments which causes vaginal relaxation
positioned ○ When the vagina is relaxed and open → anything up
● Fatigue there can enter it that’s why uterus can enter the
○ Experience greater fatigue during the period vagina
● Bladder irritation - mild incontinence ○ May be due to multiple pregnancy delivery that is
○ Bladder can become irritable where the patient can vaginal
have an infrequency of urination or incontinence of
urination DEGREE OF UTERINE PROLAPSE
○ Because of the urinary symptoms → more prone to NOTE: Depends on where the location is
have infection of the urine 1. First Degree
● Constipation ● When the cervix of the uterus points in the axis of the vagina
○ Due to abnormal position ● Bumaba lang ng kaunti
NOTE: All of that could be really disturbing to someone who needs to have ● Can be managed by nonsurgical intervention
comfort during their cycles 2. Second Degree
● The cervix is at or near the introitus
TREATMENT ● Malapit sa opening pero hindi pa lumalabas
● Postural (positional) 3. Third Degree
○ Knee-chest position which causes air to distend the ● “Procedentia uteri”
vaginal to allow the freely movable uterus to all ● Cervix protrudes well beyond the vaginal surface
towards the front ● Lumabas na; nakikita na sa vaginal opening
○ Usually with dysmenorrhea, knee-chest position is the ● Can be managed by surgical intervention because it is already
recommended position to allow the uterus to assume out
a normal ante verted or anteflexed position
● Exercise SYMPTOMS
○ Pelvic contraction are used to strengthen the muscles ● Discomfort due to mechanical protrusion of the uterus
● Bimanual position and maintained afterwards with pessary ○ Due to protrusion that is felt by the woman; something
● Surgical na parang nakalabas
○ Shortening of the round and sacrouterine ligaments ● Some degree of bearing down and heaviness in the lower
○ Last resort abdomen and backache due to traction on the uterine
○ Usually done under laparoscopy and the surgery ligaments as well as venous congestion produced by the
sometimes involve the shortening of the round and prolapsed
sacrouterine ligaments ○ All of this is obviously because there is something that
■ Shortens → parang ihohold ang uterus in already went down and compressing the lower part
its normal position of the body → discomfort
○ On the other hand, the portion of the uterus that is
Prolapse of the Uterus prolapsed → compression of the blood supply →
● The uterus went down into the vaginal area venous congestion
● This is more frequently found in elderly woman (everything is ● Urinary incontinence
loose and weak → ligaments became weak) than in young ○ It’s affect the way the person voids
patients ● Pelvic drag (or pelvic heaviness)
● Normally the uterus is inside but with a prolapsed uterus, it went ● Constipation
down to vagina and the worst is, it is not only in the vaginal ○ If the uterus is affected, both bladder and bowel are
opening but also all the way down to the vaginal cavity (severe affected because the uterus is between the midway
type of prolapse) bladder anteriorly and posteriorly is the rectum
● General Fatigue
TREATMENT WILL DEPEND UPON:
● Age
○ If the patient is still young, they may perform
correction
○ If the patient is already old, surgery is dangerous →
CAUSES
conservative approach unless there is no other option
● Increasing laxity and atony of muscular structures in later
other than removing it
life
● Marital status
○ Normal aging process
○ Because they are still sexually active so we have to do
something for them to allow normal sexual activity
12 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
○ When they use a pessary or something that will Cube Pessary
prevent the uterus from further collapsing, it is good ● Easy to insert/remove
for first degree prolapse. Kung medyo baba → can ● Must remove regularly (every 1-3 days)
interfere with coitus ○ Remove and clean it
● General health ● Suctions to wall of vagina (strong)
● Degree of prolapse ● Can often work if ____ weak PF or avulsion _____
● Presence or absence of associated pathological conditions (natakpan :))
NOTE: This will be a guideline for determining what is the safest and the CARE OF PESSARY PRIOR TO USE (especially the removable ones)
best treatment ● Wash with soap and water, soak in antiseptic solution for 1 hour
○ it is going to be inserted in the vagina and we don’t
SURGICAL TREATMENT want it to be contaminated because it can result to an
1. Vaginal Hysterectomy infection
● Suitable for almost massive degree of prolapsed ● Doctor should assess condition of patient before its insertion
● Removal of uterus through vaginal entry ○ Before the insertion, the doctor will determine it first if
○ Nakababa na → cut the remaining ligaments that are it is going to be fitted and the doctor will see if the
attached condition of the vagina is okay for the insertion of the
2. Manchester operation pessary
● Done for a lesser degree of prolapsed especially those
associated with large cystoceles. PESSARY CARE DURING ITS USE
● This involves cervical amputation ● The patient should be aware that it produces an increase in
3. Colpocleisis (Le fort operation) vaginal discharge and asymptomatic irritation
● Closing the vaginal in occasional cases for massive procedentia. ○ Due to vaginal discharge → asymptomatic irritation
○ Yung talagang nakababa na → isasara na (hindi niya alam)
● This is performed only in the elderly or widow ○ More prone to definitely infection
○ Elderly and widows who are not sexually active ● Daily cleansing vaginal douche is required
● Preceded by vaginal hysterectomy. ○ Instead of just washing outside, the vaginal douche is
● Usually done as a last resort supposed to be irrigating the insides of the vagina
using a douching apparatus or a solution is placed in
NON-SURGICAL TREATMENT a douching apparatus which has a nozzle.
Pessary treatment ○ Place the nozzle inside the vaginal canal and squeeze
● Made of plastic soft, hand rubber coming in different shapes to the solution by using negative pressure.
fit the needs of the patient ○ whatever is inside the douchung container → squeeze
● A removable device placed into the vagina it → everything inside is going to be pushed out at
● It is designed to support areas of pelvic organ prolapse great force to clean the vagina.
● Usually fitted by gynaecologists, and some physiotherapist’s are ○ It’s require to clean the vagina all the time
trained to fit ● The patient should return to the doctor after one week for re-
● It must be fitted to prevent the further descent of the prolapse evaluation. If found fit, the doctor will let the patient wear it
uterus and it can hold it in place continuously and tell her to return again for regular check-up
● A temporary intervention ○ The doctor wants to know if the patient has adapted
with the use of pessary
TYPES OF PESSARIES ● In elderly woman, when operation is not feasible, the use of
Ring Pessary pessary may be desirable for an indefinite period of time
● Easy to insert and remove ○ Elderly ones who are not feasible for operation will
● Can remain in site for 3-6/12 (3-6 months) benefit from pessary, but remember, it must be used
● Very effective for ant and uterine prolapse with care
● Requires reasonable PF tone ● In young woman, use of pessary usually is a temporary measure
Gellhorn Pessary ○ Other measures have to be done to help the person
● Can only be removed by health professional who is a little bit young and might be sexually active
○ Once inserted, can only be removed
by physician or doctor or other health
professionals
● Unable to have intervcourse
○ Very very effective but will not allow
the patient to have an intercourse
● Stronger than ring (can anchor to uterus or sit on levator hiatus)
13 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
ANNE MARIS L. RELLAMA, RN, MAN GYNECOLOGIC CONDITIONS
Associated Anomalies with Prolapse TREATMENT
Retrocele Colpoperineorrhaphy
● This results from similar mechanism involving ● Anterior - for cystocele
the pararectal fascia with a deep posterior ● Posterior - for rectocele
fascia which may be drawn farther downward ● Colpo = vagina; perineorrhaphy = perineal repair
along the anterior surface of the rectum ○ Vaginal perineal repair
○ In short, it is the one that involves the
pararectal fascia with posterior Hermaphroditism
fascia which may be drawn ● Hermaphrodite → person is carrying or having both genital traits
downwards of both male and female
● Posterior vaginal wall prolapse ● Two types: pseudohermaphroditism and hermaphroditism
● Dropping of rectum forward and downward against posterior
wall of vagina Pseudo Hermaphroditism
● The portion of the rectum is having a downward pouching into ● Not real / fake hermaphrodite
the canal of the vagina
1. Female
SYMPTOMS ● Essential sex glands are the ovaries but the external
● Vaginal mass/fullness genitalia resemble that of the male due to abnormal
○ Nararamdaman na naka-protrude development
● Sensation of stool becoming ‘stuck’ as it moves through rectum ● Clitoris is hypertrophied and looks like the male penis,
○ Even if it is moving downward, it cannot pass through secondary sex characteristics and maternal attitude is that of
because there is an obstruction the male
○ Even if the person is able to defecate, di mailabas ○ Hindi talaga pang male yun kasi meron siyang
lahat → feeling of inadequate evacuation female gonads na ovaries
● Incomplete evacuation 2. Male
● Digital splinting to assist evacuation ● More frequent essential sex organs and the testes but the
NOTE: the person need intervention otherwise, the obstruction staying secondary sex characteristics and attitude are that of the
there for a long time and not treated, an obstruction constipation can female
happen anytime and can really have an obstruction of feces or stools in the ● All sex organs are relate to male characteristics but the
area attitude and everything else is that of the female
NOTE: the true sex cannot be easilty determined except through a nuclear
Cystocele sex chromatic pattern observed in the smear of cells taken from the
● The opposite of rectocele; for the bladder epithelium of the mouth, vagina or skin sained by the Pap’s smear
● The bladder is the one having protrusion technique; the only way to determine the true gender is to a test of the cells
● This occurs as a result of a defect in the (chromosomal pattern)
pubocervical fiscial plane which supports the
bladder anteriorly and tends to permit the Hermaphroditism
bladder to sag down and beyond the uterus ● Real hermaphrodite
and sometimes out of the vagina ● Combined existence in the same person of both the female and
○ The bladder weakens and prolapse male sex glands commonly associated with malformations of
● Anterior vaginal wall prolapse the reproductive organs
● Dropping of bladder base down and backward against anterior
vaginal wall FEMINIZING CHARACTERISTICS
○ Bladder is protruded ● A male but has an ovaries, uterus → true hermaphrodite
● Rudimentary vagina and uterus and presence of ovarian tissue
SYMPTOMS ● This is rare
● Vaginal mass/ fullness
○ Instead of constipation, will experience incomplete MASCULINIZING INFLUENCE
emptying when voiding (incontinence) ● Hypertrophied clitoris (extended; parang may penis), musculine
● Recurrent UTI secondary to incomplete emptying distribution of body hair (hirsutism), musculine type of body
● Lower abdomen dragging / discomfort configuration and low voice
● Obstructive / irritable voiding symptoms ● Has an ovaries but has a characteristics that is similar for male
○ Hesitancy, straining to void, slow flow, incomplete
emptying, double voiding, post void dribble,
learning forward to void
14 SACRAMENTO | SALUD | SANTOS, C. | SANTOS, Z | SAPALO | SAUL | SERRANO | SUMABAT
You might also like
- Anomalies of The Placenta and CordDocument2 pagesAnomalies of The Placenta and CordLuiciaNo ratings yet
- 04 Third Trimester ConditionsDocument11 pages04 Third Trimester ConditionsJAN CAMILLE LENONNo ratings yet
- Hemorrhagic Conditions of Late Pregnancy Other Related Problems 1Document5 pagesHemorrhagic Conditions of Late Pregnancy Other Related Problems 1imnasNo ratings yet
- 10.disorders of LaborDocument8 pages10.disorders of LaborWoo Rin ParkNo ratings yet
- Perdarahan Antepartum - EmiliaDocument26 pagesPerdarahan Antepartum - EmiliaEmilia NazmaNo ratings yet
- Placental Abnormalities Normal Placenta: © Mary Andrea G. Agorilla, Ust-Con 2021 - 1Document3 pagesPlacental Abnormalities Normal Placenta: © Mary Andrea G. Agorilla, Ust-Con 2021 - 1Mary AgorillaNo ratings yet
- Pedia Gi-GuDocument16 pagesPedia Gi-GuZhantelle A. Santos100% (1)
- OB 1.05 Late HemorrhageDocument15 pagesOB 1.05 Late HemorrhageMaikka IlaganNo ratings yet
- Abnormal Labour: Perceptor: Dr. Nurul Islamy, M. Kes., Sp. OGDocument54 pagesAbnormal Labour: Perceptor: Dr. Nurul Islamy, M. Kes., Sp. OGramadhiena destia100% (1)
- Abnormal LaborDocument21 pagesAbnormal LaborCharisse Aser Flores AquinoNo ratings yet
- Bleeding in The Second Half of PregnancyDocument33 pagesBleeding in The Second Half of PregnancyMara Medina - BorleoNo ratings yet
- Clin TG Abnormalities of The Placenta & CordDocument13 pagesClin TG Abnormalities of The Placenta & CordTami Selvi100% (2)
- Abnormalities of PlacentaDocument9 pagesAbnormalities of PlacentaprembarnabasNo ratings yet
- Umbilical Cord AccidentsDocument16 pagesUmbilical Cord Accidentschebetnaomi945No ratings yet
- Anomalies of The Placenta and The CordDocument38 pagesAnomalies of The Placenta and The CordDN Sly Litang DumangasNo ratings yet
- Anomalies of The Placenta and CordDocument17 pagesAnomalies of The Placenta and CordSheniel VariacionNo ratings yet
- E. DR David - Ruptur Serviks Kelompok 30Document25 pagesE. DR David - Ruptur Serviks Kelompok 30wawan saifullahNo ratings yet
- Placenta and Placental ProblemsDocument13 pagesPlacenta and Placental ProblemsLuvita Ronteltap100% (1)
- Placenta Previa: Case 4 RPS I - Low Lying Placenta Source: Williams Obstetrics 24e, Chapter 41Document20 pagesPlacenta Previa: Case 4 RPS I - Low Lying Placenta Source: Williams Obstetrics 24e, Chapter 41Michael Nobel SimanjuntakNo ratings yet
- Obstetric & Gynecology Health Care Center by SlidesgoDocument64 pagesObstetric & Gynecology Health Care Center by SlidesgoShane mNo ratings yet
- Abnormal LaborDocument26 pagesAbnormal LaborShane mNo ratings yet
- Female Reproductive System TransesDocument9 pagesFemale Reproductive System TransesReign SaplacoNo ratings yet
- Problem With The PassageDocument3 pagesProblem With The PassageLuiciaNo ratings yet
- Assessment of PlacentaDocument21 pagesAssessment of PlacentaAarti RajputNo ratings yet
- Placental Abormalities (Tables)Document5 pagesPlacental Abormalities (Tables)icNo ratings yet
- Placenta Previa (No Animation)Document12 pagesPlacenta Previa (No Animation)Jhong XyrusNo ratings yet
- MCN Lect Module 2.5 Complications of Labor and Birth 4Document6 pagesMCN Lect Module 2.5 Complications of Labor and Birth 4AmethystNo ratings yet
- Umbilical HerniaDocument19 pagesUmbilical HerniabonopazioNo ratings yet
- Placenta ExaminationDocument18 pagesPlacenta ExaminationAbi RajanNo ratings yet
- Placental AbnormalitiesDocument5 pagesPlacental AbnormalitiesNica Lopez FernandezNo ratings yet
- Williams Obstertics, Twenty-Second Edition - Page 619 630Document57 pagesWilliams Obstertics, Twenty-Second Edition - Page 619 630Bharat ThapaNo ratings yet
- Face PresentationDocument4 pagesFace PresentationRose Ann HajironNo ratings yet
- Lec01 - Assessing Male and Female GenitaliaDocument13 pagesLec01 - Assessing Male and Female GenitaliaIRISH MANIAGONo ratings yet
- Placenta Types and GradingDocument37 pagesPlacenta Types and GradingNishant RajNo ratings yet
- Pha618 Lab - Female Reproductive SystemDocument18 pagesPha618 Lab - Female Reproductive SystemKirsten Shayne ManingasNo ratings yet
- Umbilical Cord Accidents-1Document16 pagesUmbilical Cord Accidents-1chebetnaomi945No ratings yet
- Clinical Anatomy 5: Breast, Pectoral, and AxillaDocument3 pagesClinical Anatomy 5: Breast, Pectoral, and AxillaJohn DoeNo ratings yet
- 2C Orev Compilation TopicDocument56 pages2C Orev Compilation TopicPaolo AntonioNo ratings yet
- Placenta Previa OutlineDocument2 pagesPlacenta Previa Outlineyxly imperialNo ratings yet
- Trainee EvaluationDocument53 pagesTrainee EvaluationdeevoncNo ratings yet
- ReadingsDocument3 pagesReadingsYori Nicole Martine CuyosNo ratings yet
- Placental AbnormalitiesDocument7 pagesPlacental AbnormalitiesLrak SiaNo ratings yet
- Intra ReviewerDocument11 pagesIntra ReviewerDIAZ, GIANNA D.No ratings yet
- Lec 3Document9 pagesLec 3ibrahim.21hm32No ratings yet
- Module 4F Operative Obstetrics PDFDocument11 pagesModule 4F Operative Obstetrics PDFYori Nicole Martine CuyosNo ratings yet
- Complications of Pregnancy 2Document4 pagesComplications of Pregnancy 2MENDIETA, JACQUELINE V.No ratings yet
- NCM109 Maternal - Child Nursing (A-C) - Module 5Document6 pagesNCM109 Maternal - Child Nursing (A-C) - Module 5iratsyukieNo ratings yet
- Examination of The Placenta - AAFPDocument22 pagesExamination of The Placenta - AAFPEi Ei MyoNo ratings yet
- Multiple Gestation: Complications of Labor and Birth Problems With The PassengerDocument4 pagesMultiple Gestation: Complications of Labor and Birth Problems With The PassengerAmethystNo ratings yet
- Obstructed LaborDocument4 pagesObstructed Laborkhadzx100% (2)
- Labor and DeliveryDocument56 pagesLabor and DeliveryBernardo AntonioNo ratings yet
- Review of Placenta DeliveryDocument3 pagesReview of Placenta DeliverygitapramodhaNo ratings yet
- CPD, Obstructed Labour, Ruptured UterusDocument47 pagesCPD, Obstructed Labour, Ruptured UterusMax ZealNo ratings yet
- Week 11 - Assessment of Breast and Lymphatic SystemDocument5 pagesWeek 11 - Assessment of Breast and Lymphatic SystemJuan Miguel TevesNo ratings yet
- Obstructed Labour FDocument53 pagesObstructed Labour FMax ZealNo ratings yet
- 05.2 Problems of The PassageDocument5 pages05.2 Problems of The PassageJAN CAMILLE LENONNo ratings yet
- NCM 109 Midterms - Postpartal Complications L1Document7 pagesNCM 109 Midterms - Postpartal Complications L1Leigh Angelika Dela CruzNo ratings yet
- Intra ReviewerDocument10 pagesIntra ReviewerL Rean Carmelle MAGALLONESNo ratings yet
- Observations on Abortion: Containing an account of the manner in which it is accomplished, the causes which produced it, and the method of preventing or treating itFrom EverandObservations on Abortion: Containing an account of the manner in which it is accomplished, the causes which produced it, and the method of preventing or treating itNo ratings yet
- Pedia Cardio-DisordersDocument14 pagesPedia Cardio-DisordersZhantelle A. SantosNo ratings yet
- Pedia Gi-GuDocument16 pagesPedia Gi-GuZhantelle A. Santos100% (1)
- Pedia April30Document8 pagesPedia April30Zhantelle A. SantosNo ratings yet
- Neural Tube DefectsDocument8 pagesNeural Tube DefectsZhantelle A. Santos100% (1)
- Pedia SeizuresDocument2 pagesPedia SeizuresZhantelle A. SantosNo ratings yet
- Nursing Care of A Family Experiencing A Complication of Labor or BirthDocument25 pagesNursing Care of A Family Experiencing A Complication of Labor or BirthZhantelle A. SantosNo ratings yet
- LECTURE BY: Asst. Prof. Margaret M. Natividad, Ed.D., RN ImmunologyDocument21 pagesLECTURE BY: Asst. Prof. Margaret M. Natividad, Ed.D., RN ImmunologyZhantelle A. SantosNo ratings yet
- LECTURE BY: Asst. Prof. Margaret M. Natividad, Ed.D., RN Care of Client With Peripheral Vascular DisordersDocument8 pagesLECTURE BY: Asst. Prof. Margaret M. Natividad, Ed.D., RN Care of Client With Peripheral Vascular DisordersZhantelle A. SantosNo ratings yet
- Labor WatchDocument35 pagesLabor WatchLawrence Steve Beronio MapaNo ratings yet
- Idiopathic Central Precocious Puberty A Case ReportDocument8 pagesIdiopathic Central Precocious Puberty A Case ReportCarolyn CapisnonNo ratings yet
- Meri 3 Khalian StoryDocument14 pagesMeri 3 Khalian StorylaltaputunnnsNo ratings yet
- Physiologic Obstetrics by APMCDocument1,091 pagesPhysiologic Obstetrics by APMCKatrina Cajigal100% (8)
- Ebook Manfaat ASI EksklusifDocument2 pagesEbook Manfaat ASI EksklusifwishingbabyNo ratings yet
- Bishop Score - StatPearls - NCBI BookshelfDocument3 pagesBishop Score - StatPearls - NCBI BookshelfDewa ayu NarheswariNo ratings yet
- RH LawDocument30 pagesRH LawElizar Vince Cruz100% (1)
- Case Scenarios-NRCMDocument3 pagesCase Scenarios-NRCMMarielle CatainaNo ratings yet
- Your Hormone Blueprint QuestionnaireDocument4 pagesYour Hormone Blueprint QuestionnaireAndreea CiausNo ratings yet
- A Two-Part Critique of The RH LawDocument13 pagesA Two-Part Critique of The RH LawCarlos Antonio P. Palad100% (1)
- Parturition Related Disorders in Sheep and Goat: G.N.PurohitDocument36 pagesParturition Related Disorders in Sheep and Goat: G.N.PurohitgnpobsNo ratings yet
- IUGRDocument11 pagesIUGRAnastasiafynnNo ratings yet
- Teenage Pregnancy Thesis - 01Document15 pagesTeenage Pregnancy Thesis - 01Jacob Christian75% (44)
- NP IiDocument11 pagesNP IiOlivia LowellNo ratings yet
- 3-Psychological Factors of Menarche, Sexual and Reproductive DevelopmentDocument19 pages3-Psychological Factors of Menarche, Sexual and Reproductive DevelopmentIzzah KhurramNo ratings yet
- Intimate Partner Violence During PregnancyDocument13 pagesIntimate Partner Violence During PregnancyAnita BarríaNo ratings yet
- Maternal and Child NursingDocument30 pagesMaternal and Child NursingJack Bisarra Sanchez0% (1)
- ANC ModuleDocument103 pagesANC ModulePreeti ChouhanNo ratings yet
- Talis Sharma +2k Birth ControlDocument29 pagesTalis Sharma +2k Birth ControlTalis SharmaNo ratings yet
- Nursing Diagnosis: Related To Obstetrical Situations Prepared by Richard Benedict S. Roxas, RN, MDDocument26 pagesNursing Diagnosis: Related To Obstetrical Situations Prepared by Richard Benedict S. Roxas, RN, MDRichard S. RoxasNo ratings yet
- Oral SexDocument18 pagesOral SexVerlana Garcia100% (1)
- Maternity QuestionsDocument49 pagesMaternity Questionsdeb100% (17)
- Case Study Sry Not SryDocument13 pagesCase Study Sry Not Sryapi-357511225No ratings yet
- Kebidanan Komplementer: Pengurangan Nyeri Persalinan Dengan Latihan Birth BallDocument6 pagesKebidanan Komplementer: Pengurangan Nyeri Persalinan Dengan Latihan Birth BallnurayuNo ratings yet
- Debate For Abortion To Be LegalizedDocument11 pagesDebate For Abortion To Be LegalizedKyria JeremiahNo ratings yet
- RRL Local and ForeignDocument13 pagesRRL Local and ForeignDick Jefferson Ocampo Pating100% (1)
- Biostat&Epi Discussion Week 3Document17 pagesBiostat&Epi Discussion Week 3Bella VengcoNo ratings yet
- XaxaxDocument3 pagesXaxaxDarren BalbasNo ratings yet
- Pornografía en República ChecaDocument7 pagesPornografía en República ChecaCamilo BohórquezNo ratings yet
- HysterosDocument12 pagesHysterosAshraf Mohamad100% (1)