Professional Documents
Culture Documents
Gastropleural Fistula An Unusual Cause Of.34
Uploaded by
Betet AingOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Gastropleural Fistula An Unusual Cause Of.34
Uploaded by
Betet AingCopyright:
Available Formats
Gastropleural Fistula: An Unusual Cause of Intractable
Postoperative Nausea and Vomiting
Iqbal H. Biswas, MD*, Chitra Raghavan, MDt, and Ludovit Sevcik, MDt
*Critical Care Medicine, Mayo Clinic, Rochester, Minnesota, and tDepartment of Clinical Anesthesia, St. Agnes Hospital,
White Plains, New York
Downloaded from http://journals.lww.com/anesthesia-analgesia by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3i3D0OdRyi7TvSFl4Cf3VC4/OAVpDDa8KKGKV0Ymy+78= on 07/01/2021
G
astropleural fistula is an uncommon finding (1). On physical examination, her temperature was 38”C,
Gastropleural fistulae have been reported after heart rate 96 bpm, and arterial blood pressure 100/80 mm
pulmonary resection (l), perforated paraesoph- Hg. Breath sounds were decreased in the lower left lung
field. Pulse oximetry was 90%. White blood cell count was
ageal hernia (2), perforated malignant gastric ulcer at
16,000/mm3. Infiltrates and consolidation of the left lower
the fundus, and gastric bypass operation for morbid lobe were evident on chest radiograph (Fig. 2). Electro-
obesity. We present a case of gastropleural fistula that cardiogram, ventilation perfusion scan, and cardiac iso-
resulted acutely from intractable postoperative nausea enzymes were within normal limits. Bilateral lower ex-
and vomiting after ambulatory knee arthroscopic sur- tremity Doppler studies were normal. A presumptive
gery under general anesthesia. diagnosis of pneumonia was made, and treatment with
antibiotics was started.
The patient continued to have chest pain and fever, and
pulmonary consultation was requested. Contrast computed
axial tomography of the chest revealed massive pleural ef-
Case Report fusion with hydropneumothorax. Thoracocentesis revealed
A 67-yr-old female underwent arthroscopy of the right knee a turbid brownish acidic fluid with no odor and with many
and debridement of the right femoral condyle for chondro- white blood cells. A 32 Fr chest tube placed via the left sixth
malacia. Her past medical history was significant for left intercostal space drained 1.5 L of turbid fluid.
thoracotomy and segmental lung resection for multiple be- Antibiotic therapy was continued. The next day, i.e., the
nign lesions (hamartomas) 4 yr previously. She had also third postoperative day, a barium swallow study revealed a
smoked heavily until that time. Exercise tolerance was nor- perforated fundus of the stomach with a fistulous connec-
mal for her age and she had no residual signs or symptoms tion to the left pleural space (Fig. 3). Exploratory laparotomy
of pulmonary disease. Laboratory data including chest was performed. The perforated area of the gastric fundus
radiography (Fig. 1) and electrocardiogram were within nor- had incarcerated through a 3 X 3 cm hernia in the tendinous
mal limits. portion of the diaphragm. The diaphragmatic hernia was
Anesthesia was induced with thiopental 4 mg/kg, mi- repaired and the fundus and part of the stomach resected.
dazolam 1 mg, and fentanyl 2 ,ug/kg. Endotracheal intu- Histologic examination of the specimen showed the stomach
bation was facilitated by administration of atracurium with perforation, acute peritonitis, and acutely inflamed
0.4 mg/kg and was accomplished atraumatically. General granulation tissue. The remainder of the stomach showed
anesthesia was maintained with nitrous oxide, oxygen, marked mucosal and submucosal congestion and edema.
and isoflurane. Neuromuscular blockade was reversed The patient tolerated the procedure well. She was admitted
with 0.4 mg of atropine and 30 mg of edrophonium and to the intensive care unit postoperatively and recovered
tracheal extubation was performed smoothly. The proce- uneventfully. She was discharged home 7 days after
dure lasted less than 1 h. surgery.
Postoperatively the patient complained of nausea. She was
medicated with prochlorperazine 5 mg intravenously (IV).
Nausea and vomiting persisted but IV ondansetron 8 mg
brought satisfactory relief. The patient was discharged from Discussion
the same-day surgery unit to her home 6 h after the com- Markowitz and Herter (2) noted that gastropleural
pletion of surgery. That night she vomited violently several fistulae may arise from different pathologic condi-
times after drinking clear liquids. The vomiting subsided the
tions: perforation of the intrathoracic portion of the
next day but she developed a sudden pain in the midaxillary
line on the left side. The pain persisted, so she returned to stomach in an esophageal hiatal hernia, trauma result-
the emergency room on the second postoperative day. ing in immediate formation of a gastropleural fistula
or formation of a diaphragmatic hernia with a subse-
quent perforation of the intrathoracic portion of the
Accepted for publication March 20, 1996.
Address correspondence to Iqbal H. Biswas, MD, Critical Care stomach, and, lastly, erosion of an intraabdominal
Service, St. Mary’s Hospital, Alfred 4-440, Rochester, MN 55905. abscess through the diaphragm.
01996 by the International Anesthesia Research Society
186 Anesth Analg 1996;3:186-8 0003.2999/96/$5.00
ANESTH ANALG CASE REPORTS 187
1996;3:186-8
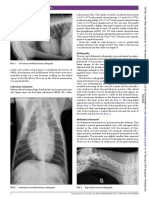
Figure 3. Barium swallow showing a perforated fundus of the
stomach with fistulous connection to the left pleural space.
Figure 1. The preoperative chest radiograph.
may later have incarcerated and perforated resulting
in the development of a gastropleural fistula.
Nausea and vomiting is a common postoperative
complication (3). Zuurmond and VanLeeuwen (4)
found an increased incidence of postoperative nausea
and vomiting in patients undergoing knee arthros-
copy under nitrous oxide, oxygen, and sufentanyl an-
esthesia compared to nitrous oxide, oxygen, and
isoflurane. There is an increased incidence of postop-
erative nausea and vomiting in female patients after
abdominal and orthopedic surgeries, under balanced
anesthesia, and during long procedures (5). Cardosa et
al. (6) found an 11.5% incidence of postoperative nau-
sea and vomiting after knee arthroscopy performed
under general anesthesia. Same-day surgical patients
may experience postoperative nausea and vomiting
for as long as 1.7 days after discharge (7). There were
Figure 2. Infiltration and consolidation of left lower lobe of lung.
thus several factors that placed our patient at greater
risk of vomiting.
In conclusion, in a patient with a history of pulmo-
In our patient, there was no history of hiatal hernia nary resection, especially the lower lobe, esophageal
or trauma, nor were there any symptoms suggestive of surgery, gastric bypass operation or gastric ulcer, the
abdominal abscess or hiatal hernia. The only signifi- possibility of a diaphragmatic hernia or hiatal hernia
cant medical history was left thoracotomy and seg- should be considered. Measures should be taken to
mental lung resection for multiple hamartomas four avoid postoperative nausea and vomiting, especially if
years previously. Review of the operative report of the other risk factors for increased nausea and vomiting
above surgery showed that the patient had a small are present. Several drugs have been used to prevent
lesion at the junction of the diaphragm and the lower and treat postoperative nausea and vomiting. Newer anti-
lobe of the left lung which was excised and oversewn. emetics which selectively antagonize 5-hydroxytryptamine
This procedure may have created a weak area in the type 3 receptors, like ondansetron 4 mg IV (8) and
diaphragm contributing to the development of a granisetron 20 pg/kg IV (9) are effective and well
small, asymptomatic, diaphragmatic hernia. Episodes tolerated in the treatment and prevention of postop-
of postoperative retching may have contributed to erative nausea and vomiting. Also, if postoperative
herniation of the fundus of stomach through the pre- nausea and vomiting is prolonged and intractable in
existing diaphragmatic hernia and prolonged nausea spite of apparently adequate pharmacotherapy, other
and vomiting. The herniated portion of the stomach causes should be sought.
188 CASE REPORTS ANESTH ANALG
1996;3:186-8
5. Larson S, Lundberg D. A prospective survey of postoperative
The authors would like to thank Dr. Elizabeth A. M. Frost for her nausea and vomiting with special regard to incidence and rela-
editorial contribution and Mrs. Beverley Pipolo for her secretarial tions to patient characteristics, anesthetic routines and surgical
skills. procedures. Acta Anesthesiol Stand 1995;39:539-45.
6. Cardosa M, Rudkin GE, Osborne GA. Outcome from day-case
knee arthroscopy in a major teaching hospital. Arthroscopy
1994;10:624-9.
7. Carrol NV, Miederhoff I’, Cox FM, et al. Postoperative nausea
References and vomiting after discharge from outpatient surgery centers.
1. O’Keefe PA, Goldstraw P. Gastropleural fistula following pul- Anesth Analg 1995;80:903-9.
monary resection. Thorax 1993;48:1278-9. 8. Paxton LD, McKay AC, Mirakhur RK. Prevention of nausea and
2. Markowitz AM, Herter FP. Gastropleural fistula as a complica- vomiting after day case gynaecological laparoscopy. A compar-
tion of esophageal hiatus hernia. Ann Surg 1960;152:129-34. ison of ondansetron, droperidol, metoclopramide and placebo.
3. Muir JJ, Warner MA, Offord KP, et al. Role of nitrous oxide and Anaesthesia 1995;50:403-6.
other factors in postoperative nausea and vomiting: a random-
9. Mikawa K, Takao Y, Nishina K, et al. The antiemetic efficacy of
ized and blinded prospective study. Anesthesiology 1987;67:
granisetron in gynecologic surgery. Anesth Analg 1995;80:
513-8.
970-4.
4. Zuurmond WW, VanLeeuwen L. Recovery from sufentanil an-
esthesia for outpatient arthroscopy: a comparison with isoflu-
rane. Acta Anesthesiol Stand 1987;31:154-6.
You might also like
- Obstetric History Taking OSCE GuideDocument17 pagesObstetric History Taking OSCE GuideSYDNIKA AIRA CARBONILLANo ratings yet
- Modern Anaesthesia:: A Concise Guide to the Study and Practice of Anaesthesia.From EverandModern Anaesthesia:: A Concise Guide to the Study and Practice of Anaesthesia.No ratings yet
- Surgical TechniquesDocument32 pagesSurgical TechniquesJackson Souza100% (1)
- Hyperemesis Gravidarum GuideDocument5 pagesHyperemesis Gravidarum GuideGladys Ocampo100% (5)
- National Geographic USA - January 2016Document148 pagesNational Geographic USA - January 2016stamenkovskib100% (4)
- SbarDocument3 pagesSbarCharlie65129No ratings yet
- DRUG-STUDY OmeprazoleIV AngelicaRonquilloDocument4 pagesDRUG-STUDY OmeprazoleIV AngelicaRonquillokarl eiron delos santosNo ratings yet
- Anesthesiaforpituitary Surgery: Jinu Kim,, Ross Scott-MillerDocument10 pagesAnesthesiaforpituitary Surgery: Jinu Kim,, Ross Scott-MillerJose Miguel CastellonNo ratings yet
- Pneumoperitoneum Signs on Supine X-rayDocument4 pagesPneumoperitoneum Signs on Supine X-rayDaniel DerianNo ratings yet
- Pyloric BandDocument6 pagesPyloric BandRia RfNo ratings yet
- Dystrophia Myotonica and Atracurium Case ReportDocument5 pagesDystrophia Myotonica and Atracurium Case Reportmohamed alshoshanNo ratings yet
- Focsaneanu2018 (2 4)Document3 pagesFocsaneanu2018 (2 4)Kollinz ZfNo ratings yet
- An Unusual Source of Tension - ChestDocument5 pagesAn Unusual Source of Tension - ChestKaran KalraNo ratings yet
- Postural Hypotension With Bradycardia PDFDocument3 pagesPostural Hypotension With Bradycardia PDFAnonymous HwO3MTmftNo ratings yet
- Beyond The Boundaries: Enigma of Distinguishing Exophytic Upper Pole Renal Cell Carcinoma From An Adrenal MassDocument4 pagesBeyond The Boundaries: Enigma of Distinguishing Exophytic Upper Pole Renal Cell Carcinoma From An Adrenal MassAyush JainNo ratings yet
- Laparoscopic Excision of A Renal Subcapsular Abscess Presenting As A Subcapsular HaematomaDocument3 pagesLaparoscopic Excision of A Renal Subcapsular Abscess Presenting As A Subcapsular HaematomaDavid MorgNo ratings yet
- Bile Leak CaseDocument6 pagesBile Leak CaseDimas ErlanggaNo ratings yet
- Cardiac Arrest Post Tourniquet ReleaseDocument2 pagesCardiac Arrest Post Tourniquet ReleaseaksinuNo ratings yet
- S2116 Novel Presentation of Rectal Granular Cell.2116Document2 pagesS2116 Novel Presentation of Rectal Granular Cell.2116dianisaindiraNo ratings yet
- MY MAXICARE (Brochure) PDFDocument16 pagesMY MAXICARE (Brochure) PDFFeedLab CARNo ratings yet
- Anesthetic Management of A Patient of Valvular Heart Disease Posted For Inguinal Hernioplasty A Case ReportDocument3 pagesAnesthetic Management of A Patient of Valvular Heart Disease Posted For Inguinal Hernioplasty A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Anaesthetic Management of Abdominal Aorta AneurysmDocument4 pagesAnaesthetic Management of Abdominal Aorta Aneurysmaswin febriaNo ratings yet
- BoerhaaveDocument3 pagesBoerhaaveMartu EilertNo ratings yet
- CIRCULATIONDocument2 pagesCIRCULATIONRVDNo ratings yet
- Urologie - Bencherki Youssef - Giant Abscessed Urachal in AdultDocument1 pageUrologie - Bencherki Youssef - Giant Abscessed Urachal in AdultYoussef BencherkiNo ratings yet
- 2023 Hiatal Hernia The Great Masquerade in TheDocument4 pages2023 Hiatal Hernia The Great Masquerade in ThekueputuNo ratings yet
- Jurnal Hernia UmbicalDocument3 pagesJurnal Hernia UmbicaltutiNo ratings yet
- Guyons CanalDocument9 pagesGuyons CanalanindyaNo ratings yet
- Primary Review: Psoas Abscess: Case of The LiteratureDocument3 pagesPrimary Review: Psoas Abscess: Case of The LiteratureDung Tran HoangNo ratings yet
- Heart Rate Control during Experimental Sepsis in Mice: Comparison of Ivabradine and β-BlockersDocument9 pagesHeart Rate Control during Experimental Sepsis in Mice: Comparison of Ivabradine and β-BlockersCostina BbNo ratings yet
- The Snapping Hip SyndromeDocument6 pagesThe Snapping Hip SyndromeFlorin MacarieNo ratings yet
- Case 4-1999Document10 pagesCase 4-1999K. O.No ratings yet
- Prolonged Post-Spinal ParalysisDocument3 pagesProlonged Post-Spinal ParalysisNurul FajriNo ratings yet
- Drug Fever in An Elderly Patient After Pacemaker ImplantationDocument4 pagesDrug Fever in An Elderly Patient After Pacemaker ImplantationSurjeetNo ratings yet
- Quick 1978Document4 pagesQuick 1978RENAULTNo ratings yet
- Cancer - June 1979 - Diasio - Adenocarcinoma of The Pancreas Associated With Hypoglycemia Case Report and Review of TheDocument8 pagesCancer - June 1979 - Diasio - Adenocarcinoma of The Pancreas Associated With Hypoglycemia Case Report and Review of Theabdullah shamshirNo ratings yet
- Gastric Perforation by Fish Bone Case: © All Rights Are Reserved by Pedro MonsalveDocument5 pagesGastric Perforation by Fish Bone Case: © All Rights Are Reserved by Pedro MonsalveMuhamad Chairul SyahNo ratings yet
- Faustinella 1997 Glomerulomegaly and Proteinuria in A Patient With Idiopathic Pulmonary HypertensionDocument5 pagesFaustinella 1997 Glomerulomegaly and Proteinuria in A Patient With Idiopathic Pulmonary HypertensionPaul SimononNo ratings yet
- Oesophagus - Lecture (1 & 2) SurgeryDocument27 pagesOesophagus - Lecture (1 & 2) Surgeryhussain AltaherNo ratings yet
- Esophagus - 1Document27 pagesEsophagus - 1hussain AltaherNo ratings yet
- Postoperative Atrial Fibrillation: The Role of The Inflammatory ResponseDocument9 pagesPostoperative Atrial Fibrillation: The Role of The Inflammatory ResponseHendrik AbrahamNo ratings yet
- 09 - 211acute Limb Ischaemia-Case Report PDFDocument4 pages09 - 211acute Limb Ischaemia-Case Report PDFKarimah NasarNo ratings yet
- Acute Mesenteric Ischaemia on Unenhanced CTDocument7 pagesAcute Mesenteric Ischaemia on Unenhanced CTmike_lavaresNo ratings yet
- Postoperative Urinary Retention: Anesthetic and Perioperative ConsiderationsDocument19 pagesPostoperative Urinary Retention: Anesthetic and Perioperative Considerationspooria shNo ratings yet
- Acute Mesenteric Ischemia: A Challenging Diagnostic Disease-Four Cases Reports and Literature Review (AMI)Document10 pagesAcute Mesenteric Ischemia: A Challenging Diagnostic Disease-Four Cases Reports and Literature Review (AMI)rahmatobineNo ratings yet
- Lapsus Retained Catheter Epidural UndipmteDocument7 pagesLapsus Retained Catheter Epidural UndipmtewindyNo ratings yet
- Fistula broncobiliarDocument3 pagesFistula broncobiliarsamuelfdiaz.0103No ratings yet
- Laparoscopic Heller Myotomy For Achalasia: Robert N. Cacchione, M.D., Dan N. Tran, M.D., Diane H. Rhoden, M.DDocument5 pagesLaparoscopic Heller Myotomy For Achalasia: Robert N. Cacchione, M.D., Dan N. Tran, M.D., Diane H. Rhoden, M.Dgabriel martinezNo ratings yet
- Case Report: A Case of Traumatic Asphyxia Due To Motorcycle AccidentDocument4 pagesCase Report: A Case of Traumatic Asphyxia Due To Motorcycle AccidentAgus MarkembengNo ratings yet
- Thoracic Epidural For Modified Radical Mastectomy in A High-Risk PatientDocument2 pagesThoracic Epidural For Modified Radical Mastectomy in A High-Risk PatientBianca CaterinalisendraNo ratings yet
- 480 FullDocument6 pages480 FullStamenko S. SusakNo ratings yet
- AAA Case ReportDocument6 pagesAAA Case Reportfelix_3264_hariantoNo ratings yet
- Fistula BroncopleuralDocument4 pagesFistula BroncopleuralKimberly Solange Holguin MedinaNo ratings yet
- Case 126:: Extramedullary HematopoiesisDocument4 pagesCase 126:: Extramedullary HematopoiesisVo VũNo ratings yet
- Canine InsulinomaDocument5 pagesCanine Insulinomasoff4ikaNo ratings yet
- Kateter Epidural Terputus Saat Dipasang: Epidural Catheter Breakage During InsertionDocument7 pagesKateter Epidural Terputus Saat Dipasang: Epidural Catheter Breakage During InsertionYani SudiarsoNo ratings yet
- Anaesthesia Management in Endoscopic Ultrasound Guided Lung BiopsyDocument2 pagesAnaesthesia Management in Endoscopic Ultrasound Guided Lung BiopsyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 1 s2.0 S0929644112000057 MainDocument4 pages1 s2.0 S0929644112000057 MainAisahNo ratings yet
- ZZ - 1977-09 - Spontaneous Hemorrhage Due To Pseudocysts of The PancreasDocument3 pagesZZ - 1977-09 - Spontaneous Hemorrhage Due To Pseudocysts of The PancreasNawzad SulayvaniNo ratings yet
- Atraumatic Acute Forearm Compartment Syndrome Due To Systemic HeparinDocument2 pagesAtraumatic Acute Forearm Compartment Syndrome Due To Systemic HeparinRaymond WinNo ratings yet
- Acodaduras Ureterales (Kinking)Document7 pagesAcodaduras Ureterales (Kinking)Clínica CIPRONo ratings yet
- Acta Anaesthesiologica Taiwanica: Takeshi MurouchiDocument2 pagesActa Anaesthesiologica Taiwanica: Takeshi MurouchiShuaib AhmedNo ratings yet
- Tuberous Sclerosis Complex. Forty-Years of Follow-Up of A Patient AffectedDocument3 pagesTuberous Sclerosis Complex. Forty-Years of Follow-Up of A Patient AffectedLilik FitrianaNo ratings yet
- Treatment Cysts: Thoracoscopic PleuropericardialDocument8 pagesTreatment Cysts: Thoracoscopic PleuropericardialJuhi SahajwaniNo ratings yet
- Anticholinergic: Classification Generic Name Brand NameDocument6 pagesAnticholinergic: Classification Generic Name Brand NameKarina MadriagaNo ratings yet
- OtcDocument9 pagesOtcChrissie100% (1)
- Nausea and Vomiting: Key ConceptsDocument35 pagesNausea and Vomiting: Key ConceptsMila ErnilaNo ratings yet
- CYPERMETHRINDocument7 pagesCYPERMETHRINJurgen SchirmacherNo ratings yet
- Chapter 6 Diagnostic EnzymologyDocument81 pagesChapter 6 Diagnostic EnzymologyFathimathNo ratings yet
- Cefuroxime, Albendazole, NyastatinDocument4 pagesCefuroxime, Albendazole, NyastatinMAE THERESE MONICITNo ratings yet
- Patient Medical RecordDocument1 pagePatient Medical RecordKyla Barrera TabungarNo ratings yet
- Tolak Angin TranslatedDocument3 pagesTolak Angin TranslatedWadz MuharNo ratings yet
- Gastrointestinal System Template ExaminationDocument5 pagesGastrointestinal System Template ExaminationSaraNo ratings yet
- Xoswego 401-303 StudentDocument12 pagesXoswego 401-303 StudentJocelin LedesmaNo ratings yet
- Amoxicillin and Other Common AntibioticsDocument21 pagesAmoxicillin and Other Common AntibioticsAdeel ur RahmanNo ratings yet
- Myoma Pathophysio, Gordon's NCPDocument13 pagesMyoma Pathophysio, Gordon's NCPicesexy100% (1)
- AmphetwdrlscaleDocument4 pagesAmphetwdrlscaleAstrid WardhaniNo ratings yet
- Red Flags of The Shoulder and NeckDocument5 pagesRed Flags of The Shoulder and NecksugoimanNo ratings yet
- A&B-WPS OfficeDocument9 pagesA&B-WPS OfficeDianne LabisNo ratings yet
- PancreatitisDocument12 pagesPancreatitisjhodane100% (4)
- Calcium Gluconate Drug Classification, Dosage and Side EffectsDocument4 pagesCalcium Gluconate Drug Classification, Dosage and Side EffectsStacy MC PelitoNo ratings yet
- Effects of Benson's Relaxation Technique On Nausea in Patients With Chronic Kidney Disease Undergoing HemodialysisDocument10 pagesEffects of Benson's Relaxation Technique On Nausea in Patients With Chronic Kidney Disease Undergoing HemodialysisendroNo ratings yet
- Afina Fitra Firdaus Ppds Ipd 50Document30 pagesAfina Fitra Firdaus Ppds Ipd 5050Afina Fitra FirdausNo ratings yet
- Biochemic MedicineDocument748 pagesBiochemic MedicineManeesh YadavNo ratings yet
- Soal Bahasa Inggris 1 - AtmaDocument20 pagesSoal Bahasa Inggris 1 - Atmarumanimalis YTNo ratings yet
- Daftar Pustaka HEGDocument2 pagesDaftar Pustaka HEGJennifer BrockNo ratings yet
- Natural Substances NutmegDocument4 pagesNatural Substances NutmegtheoNo ratings yet
- Bulk Stimulants Lubricants Other Laxatives GI StimDocument5 pagesBulk Stimulants Lubricants Other Laxatives GI Stimrosita d. ramosNo ratings yet
- MotiliumDocument5 pagesMotiliumAkram KhanNo ratings yet