Professional Documents
Culture Documents
Compulsive Disorders Parkinson
Uploaded by
Paola Sofia CortesTamayoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Compulsive Disorders Parkinson
Uploaded by
Paola Sofia CortesTamayoCopyright:
Available Formats
Dopamine and Impulse Control Disorders in
Parkinson’s Disease
Daniel Weintraub, MD
There is an increasing awareness that impulse control disorders (ICDs), including compulsive gambling, buying, sexual behavior,
and eating, can occur as a complication of Parkinson’s disease (PD). In addition, other impulsive or compulsive disorders have
been reported to occur, including dopamine dysregulation syndrome (DDS) and punding. Case reporting and prospective
studies have reported an association between ICDs and the use of dopamine agonists (DAs), particularly at greater dosages,
whereas dopamine dysregulation syndrome has been associated with greater dosages of levodopa or short-acting DAs. Data
suggest that risk factors for an ICD may include male sex, younger age or younger age at PD onset, a pre-PD history of ICD
symptoms, personal or family history of substance abuse or bipolar disorder, and a personality style characterized by impulsive-
ness. Although psychiatric medications are used clinically in the treatment of ICDs, there is no empiric evidence supporting their
use in PD. Therefore, management for clinically significant ICD symptoms should consist of modifications to dopamine re-
placement therapy, particularly DAs, and there is emerging evidence that such management is associated with an overall im-
provement in ICD symptomatology. It is important that PD patients be aware that DA use may lead to the development of an
ICD, and that clinicians monitor patients as part of routine clinical care. As empirically validated treatments for ICDs are
emerging, it will be important to examine their efficacy and tolerability in individuals with cooccurring PD and ICDs.
Ann Neurol 2008;64 (suppl):S93–S100
As clinicians have become more successful at treating ICDs constitute a group of psychiatric disorders in
the motor symptoms of Parkinson’s disease (PD), the Diagnostic and Statistical Manual of Mental Disor-
many of the nonmotor symptoms, particularly cogni- ders, Fourth Edition, Text Revision (DSM-IV-TR),1
tive and neurobehavioral complications, are increas- and are characterized by a failure to resist an impulse,
ingly recognized as significant contributors to long- drive, or temptation to perform a typically pleasurable
term disability, impaired quality of life, and caregiver activity that is ultimately harmful to the person or to
distress. Although dementia and depression are the others because of its excessive nature. Pathological
most recognizable and common of the neurobehavioral gambling (PG) is the most common ICD, and other
manifestations of PD, psychosis, apathy, anxiety, im- ICDs without formal DSM-IV-TR diagnostic criteria
pulse control disorders (ICDs), and ICD-related disor- include compulsive sexual behavior and compulsive
ders also occur not frequently. ICDs are particularly buying.2,3 Binge eating disorder, classified as an eat-
important to recognize, because they can cause consid- ing disorder in the DSM-IV-TR, shares many of the
erable distress to the patient and caregiver, may have clinical features of ICDs. Recent observational studies
disastrous personal and financial consequences, and ap- suggest that a range of ICDs may occur4 at a greater
pear to be underreported. The recent awareness of frequency in PD than in the general population and
ICDs in PD has fueled the search for an increased un- may be associated with the use of dopamine agonists
derstanding of their epidemiology, the underlying neu- (DAs).
ral mechanisms, and the most effective treatment ap- Other related disorders reported to occur in PD
proaches. and characterized by repetitive, or compulsive, behav-
From the Department of Psychiatry, University of Pennsylvania Published online in Wiley InterScience (www.interscience.wiley.com).
School of Medicine, Parkinson’s Disease Research, Education and DOI: 10.1002/ana.21454
Clinical Center; and the Mental Illness Research, Education and
Clinical Center, Philadelphia Veterans Affairs Medical Center, Phil- Address correspondence to Dr Weintraub, Assistant Professor of
adelphia, PA. Psychiatry, University of Pennsylvania School of Medicine;
Received Mar 19, 2008, and in revised form May 28. Accepted for 3615 Chestnut St., #330, Philadelphia, PA 19104. E-mail:
publication Jun 2, 2008. weintrau@mail.med.upenn.edu
Potential conflicts of interest: This article is part of a supplement
sponsored by Boehringer Ingelheim (BI). D.W. has served as a con-
sultant to, has served on advisory boards for, and has received grant
support from BI. D.W. has also consulted for and served on advi-
sory boards for Novartis, Merck Serono, Brain Cells, and Osmotica
Pharmaceuticals.
© 2008 American Neurological Association S93
Published by Wiley-Liss, Inc., through Wiley Subscription Services
iors include: (1) dopamine dysregulation syndrome PD,15 and in a recent study, 10% of a sample of 50 consec-
(DDS) or hedonic homeostatic dysregulation,5 an utively evaluated PD patients met criteria for compulsive
addiction-like state marked by excessive dopaminergic buying and 10% for compulsive sexual behavior.16 In an-
medication usage, particularly L-dopa and short-acting other recent study,17 a total prevalence rate of 9% for com-
DAs (eg, subcutaneous apomorphine); (2) punding, pulsive gambling, buying, and sexual behaviors was reported.
Compulsive or binge eating has been reported in PD, but its
an intense fascination with meaningless movements or
prevalence in not known.5,18
activities (eg, collecting, arranging, or taking apart The results of two large studies that prospectively screened
objects)6; and (3) walkabout, defined as excessive, for ICDs in PD were published recently. In the first study,19
aimless wandering.5 297 patients with idiopathic PD at a tertiary clinic were
screened for PG with a modified version of the South Oaks
Epidemiology of Impulse Control Disorders in Gambling Scale.20 Lifetime and current (past 3 months) fre-
Parkinson’s Disease quencies of PG were 3.4% and 1.7%, respectively. In the
second study,21 272 patients with idiopathic PD at 2 move-
Nomenclature
ment disorders centers were screened for the presence of sev-
Multiple terms have been used to describe the clinical pre- eral ICDs (compulsive gambling, sexual behavior, and buy-
sentation of compulsive behaviors in PD. These terms in- ing). Those who screened positive for one or more ICDs
clude “dopamine dysregulation syndrome” (DDS),6 “hedo- during the course of PD were contacted by phone for
nistic homeostatic dysregulation,”5,7 “dopamimetic drug follow-up and administered a modified Minnesota Impulsive
addiction,”8 “compulsive behaviors,”9 “compulsive dopami- Disorders Interview,22 which includes queries for the pres-
nergic drug use,”10 and “repetitive behaviors.”11 DDS is de- ence of clinically significant compulsive gambling, sexual,
fined as compulsive use (eg, escalating daily dosages) of do- and buying behaviors. In this study, the frequency rates of at
pamine replacement therapy (DRT), but anecdotally, most least one active ICD or an ICD anytime during PD was 4.0
PD patients with an ICD do not report compulsive use of and 6.6%, respectively. Among active cases, compulsive sex-
DRT. ual behavior was as common as problem gambling (2.6 vs
Other psychiatric disorders or behaviors that share features 2.2%, respectively), and the frequency of compulsive buying
of ICDs have been reported to occur in PD in the context of was 0.4%.
DRT treatment. For instance, patients have been reported to DDS and other ICD-related disorders in PD have not
develop (hypo)mania,5 a mood disorder that can involve ex- been as well studied as the aforementioned ICDs. A total of
cessive involvement in pleasurable activities that have a high 15 DDS cases was reported in the original description of this
potential for painful consequences, with excessive use of syndrome in PD,5 but a cross-sectional or cumulative prev-
DRT. In addition, obsessive-compulsive disorder, an anxiety alence rate was not reported. Regarding punding, in one se-
disorder characterized by the repetition of nonharmful be- ries examining PD patients taking greater L-dopa–equivalent
haviors to reduce anxiety, may occur at an increased fre- daily dosages (LEDDs), 14% met criteria for punding,6 but
quency in PD, although it has not been reported in associ- another, larger study of unselected PD patients reported a
ation with DRT.11 As mentioned previously, punding and prevalence rate of 1.4%.23
walkabout are characterized by repetitive behaviors and poor Thus, preliminary prevalence (either current or anytime
impulse control, but the behaviors are typically nonpleasur- during PD) estimates for ICDs in PD patients overall are
able or low in risk-reward characteristics when compared approximately 2.0 to 6.0% for pathological or problem gam-
with ICD behaviors. Thus, ICDs may represent the severe bling, 2.0 to 10.0% for compulsive sexual behavior, and
end of a spectrum of behavioral disturbances in PD that are 0.4% to 2.0% for compulsive buying. These studies have
characterized by poorly or uncontrolled repetitive behaviors. also suggested that these ICDs may be more common in PD
For the purposes of this article, the term impulse control than in the general population24 –30 or in assessed healthy
disorder (ICD) is used (except when discussing DDS, which control subjects.31,32 However, the true prevalence of ICDs
is distinct from ICDs in many ways), because PG is consid- in PD is not known. First, most studies have focused only
ered to be an ICD in the psychiatric nomenclature, and this on gambling disorders, and other ICDs may be as common
and the other disorders discussed herein are characterized by as PG in PD. Second, the reported values for all disorders
a failure of impulse control that is not better explained by may underestimate the true frequencies, because some studies
another psychiatric condition. relied on information documented in charts during routine
clinical care, and in one of the aforementioned screening
Prevalence studies,21 active ICD cases were rarely documented in the
Driver-Dunckley and colleagues12 reviewed 1,884 charts at a clinical record. Third, patients may be reluctant to acknowl-
PD research center and identified 9 patients (0.5% of the edge ICD behaviors in the context of a research study.
sample) with documentation of PG. In a subsequent pro- It is not known whether ICDs are more common in PD
spective study using face-to-face interviews,13 the prevalences than in the general population because it is difficult to find
of PG in approximately 200 patients was reported to be 7% an appropriate comparison group. However, in a recent pro-
(12/188). In a recent prospective study, 4.4% (17/388) of spective study, PD patients were approximately 25 times
patients at 6 movement disorders centers met criteria for PG, more likely (odds ratio, 25.6) to have PG than an age- and
and the rate for patients on a DA was 8.0%.14 Regarding sex-matched control group.32 In addition, a recent case–con-
other ICDs, a cumulative incidence rate (after starting DRT) trol study found that new-onset “heightened interest in or
of 2.4% was reported for compulsive sexual behavior in drive” for gambling, shopping, eating, or sexual activity was
S94 Annals of Neurology Vol 64 (suppl) December 2008
reported in 14% of PD patients and in none of the age- and Other Clinical Correlates
sex-matched healthy control subjects.31 Among the published case reports, PD patients with ICDs
have disproportionately been younger male individu-
als,34,35,36 suggesting age and sex as potential risk factors for
Association with Dopamine Replacement Therapy the development of ICDs in this population. These findings
Case reports have implicated DAs (eg, pramipexole, ropini- are consistent with those from epidemiological and clinical
role, and pergolide), and less commonly L-dopa,33 as precip- studies that observe high rates of PG and compulsive sexual
itating PG in PD. In Driver-Dunckley and colleagues’12 case
behaviors in young male individuals in the general popula-
series, all nine patients were treated with a DA, including
tion and treatment settings.3
eight with pramipexole. In another case series, all 11 PD
In one of the aforementioned prospective studies,21 on
patients identified as having criteria for PG were taking a
DA, 9 of whom were taking pramipexole and 2 taking ropi- univariate analysis, younger age, longer duration of PD, and
nirole.34 In another study,13 all 14 subjects identified as hav- a history of ICD symptomatology before PD each were as-
ing PG were taking a DA. In the most recent case series, all sociated with the presence of an active ICD. Entering the
17 patients identified as having PG were taking a DA.14 aforementioned variables into a multivariate model, only a
Regarding other ICDs in PD, in a series of 15 patients history of ICD symptomatology before PD remained a sig-
with compulsive sexual behavior and either PD or multiple nificant predictor of an active ICD. In the other prospective
system atrophy, DA treatment was implicated in the emer- study,19 on univariate analysis, PG was associated with earlier
gence of the sexual behavior in 14 cases.35 This case report- PD onset. In addition, 60% of patients with a history of PG
ing suggests an association between DA use and ICDs, be- had either a premorbid personal or family history of alcohol
cause only approximately 50% of PD patients surveyed in use disorder, or a family history of bipolar disorder. Finally,
specialty care are taking a DA.19,21 In a case–control study of in a recent case–control study,31 PD patients with new-onset
PD patients and matched control subjects,31 longer duration heightened interest or drive for a range of ICD behaviors had
of DA treatment (vs never treated) was associated with the younger age at PD onset and were more likely to be male
new-onset heightened interest in or drive for gambling, shop- than unaffected PD patients.
ping, eating, or sexual activity. In some instances,12,34,35 substantial time elapsed between
In one of the aforementioned prospective screening stud- initiation of DA treatment and the onset of ICD behaviors
ies,19 PG was significantly more common in DA-treated pa- in PD patients. This delay could reflect either a priming ef-
tients than in those receiving L-dopa monotherapy. In the
fect, a threshold in the PD neurodegenerative process that
other prospective study,21 on univariate analysis use of a DA
must be crossed before ICD behavior manifests itself, or the
or amantadine, each was associated with the presence of an
active ICD, and a trend for greater total LEDD was ob- importance of escalating dosages over time and the need to
served. All active ICD cases were currently taking a DA. En- cross a necessary dosage threshold before becoming symp-
tering all the aforementioned variables into a multivariate tomatic.
model, only current DA use remained a significant predictor Although case reports have suggested that younger pa-
of an active ICD. No differences were observed between the tients are disproportionately affected, older patients are less
three DAs examined (pramipexole, ropinirole, and pergolide) likely to be treated with DAs because of concerns about ad-
in their association with ICDs. Examining only patients who verse events.21 Considering only patients taking a DA,
were taking a DA at the time of screening, an active ICD younger patients in one study21 were found to have been
was associated a greater mean daily DA dosage. treated with greater dosages. Thus, the previous reporting of
Thus, the pharmacotherapy risk associated with ICDs ap- younger PD patients being disproportionately affected with
pears to be specific to the DA medication class because no ICDs may, in part, reflect prescribing patterns.
association was found between daily L-dopa dosage or total There is controversy about whether certain personality
LEDD and the presence of an ICD.19,21 These results sug- traits or psychiatric disorders predispose to ICD development
gest a distinct mechanism of action, as opposed to an addi- in PD, as cross-sectional studies of patients symptomatic
tive effect, for DAs in the development of ICDs. In addition, with an ICD may confound “state” effects for “trait” effects.
a differential association between specific DAs and ICDs was That being said, greater scores on impulsivity and compul-
not supported in two larger studies,19,21 suggesting a class, as sivity inventories were reported in PD ICD patients com-
opposed to specific medication, effect. Finally, the finding
pared with PD control subjects in one study.16 In a study
that the greatest risk for development of an ICD with DA
focusing on psychiatric comorbidity, a range of ICDs were
treatment may involve doses at the high end of the thera-
associated with depressed mood, disinhibition, irritability,
peutic range is consistent with previous case reporting.12,34
By definition, DDS is associated with escalating dosages of and appetite disturbance.17
PD medications, typically L-dopa or short-acting DA medi- Regarding DDS, in one study, patients with DDS (more
cations (eg, subcutaneous apomorphine).5 In studies of than half of whom had one or more comorbid ICDs) had
punding, an association with DA treatment23 or greater younger age of PD onset and were more likely to have a
LEDDs6 has been reported, with the latter study concluding history of experimental drug use.10 Although there has been
that punding and DDS often co-occur. In a study of PD comparatively little research on punding, in a study of PD
patients unselected for an ICD diagnosis, greater scores on not selected for an ICD diagnosis, greater scores on the
the self-completed Punding Scale were associated with Punding scale was associated with younger age at PD onset
greater DA dosages.36 and greater impulsivity scores.36
Weintraub: Review of ICDs in PD S95
Neural Substrate of Impulse Control Disorders a pronounced depletion of dopamine in the nigrostri-
General Population atal pathway.47 This depletion influences dopaminergic
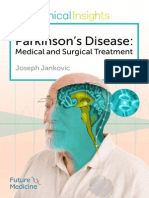
The pathophysiology of ICDs has been reported to in- cortical-subcortical circuits, leading to cognitive and
volve alterations in specific neurotransmitter systems, emotional impairment that may predispose to the de-
brain regions, and neural circuitry (Figure). Regarding velopment of numerous psychiatric and cognitive dis-
neurotransmitters, dopamine function, particularly orders, including ICDs.
within the mesocorticolimbic pathways, is critical in Second, PD patients, even those without dementia,
the mediation of reward and reinforcement behav- commonly display a range of impairment in executive
iors.38 The brain regions most implicated in ICDs in- abilities,48,49 which has been linked to degeneration in
clude the ventromedial39,40 and orbitofrontal regions41 the striatal-frontal tracts secondary to cell loss within
of the prefrontal cortex, the ventral striatum (particu- the substantia nigra.50,51 On a computerized gambling
larly the nucleus accumbens),38,42 and the amygda- task of theoretical relevance to ICD behaviors, PD pa-
la,43,44 all of which are thought to mediate aspects of tients were significantly more impaired than control
motivated behaviors underlying engagement in risky, subjects in performance (both number of disadvanta-
compulsive behaviors. Finally, data suggest that alter- geous choices and ability to use negative feedback for a
ations in cortico-striato-thalamo-cortical circuitry con- decision shift to an advantageous alternative), and task
tribute to ICD behaviors, with projections coursing impairment correlated with impairment on other exec-
through the more ventral component of the striatum utive measures.51 In a recent study52 that involved ad-
(including the nucleus accumbens) more implicated in ministration of computerized decision-making tasks to
urges and impulsive aspects, and those involving the PD patients on and off PD medications, the medicated
dorsal striatum more implicated in motoric habits and group showed impairment in the ability to learn from
compulsive aspects.45,46 This neurocircuitry involves negative decision outcomes, a psychological deficit that
additional brain regions (eg, the amygdala providing also may have relevance to the maintenance of ICD
affective salience, and the hippocampus contextual behaviors. Regarding differential effects of PD medica-
memories), with disruptions in one area having the po- tions, there is also some evidence that DA, but not
tential to influence function throughout the circuitry. L-dopa, treatment impairs executive abilities in patients
with early or mild PD.53
Parkinson’s Disease Third, DAs, compared with L-dopa, have signifi-
There are several plausible explanations for a possible cantly greater D3:D2 and D3:D1 striatal receptor ac-
association between ICDs in PD and treatment with tivation ratios.54 D1 and D2 receptors are located in
DRT, especially DAs. First, PD leads to a loss of do- the dorsal striatum, and their activation by different
paminergic neurons in the substantia nigra, resulting in PD pharmacotherapies is associated primarily with the
Fig. Main brain areas and neurotransmitter pathways implicated in reward processes. (Reproduced from Tomkins and Sellers,71 by
permission.)
S96 Annals of Neurology Vol 64 (suppl) December 2008
motor effects of the medications. In contrast, the D3 system.”59 This proposed neural substrate of disorders
receptor is concentrated in limbic areas of the brain, of addiction may be similar to the neural substrate of
including the ventral striatum, and may mediate psy- ICDs in PD.
chiatric manifestations of dopamine receptor stimula- In the only published study examining the neurobi-
tion.55 ology of any of the discussed disorders in PD,58 a small
Recent cognitive neuroscience studies in PD have fo- group of patients with and without active DDS under-
cused on differential neurodegeneration of the striatum went positron emission tomography scanning with the
in early or mild PD, with the dorsal striatum being D2/D3 receptor ligand 12C-raclopride before and after
more affected than the ventral striatum.56,57 This de- L-dopa oral challenge. PD patients with DDS exhibited
pletion differentially affects distinct cortical-basal enhanced L-dopa–induced ventral striatal dopamine re-
ganglia-thalamo-cortical circuits that subserve multiple lease compared with non-DDS patients. In addition,
processes, including motor, cognitive, and limbic func- the degree of sensitized striatal dopamine release corre-
tions. It has been proposed that in mild PD, dopami- lated with self-reported drug “wanting” but not “lik-
nergic stimulation of dopamine-deficient dorsal striatal ing.” The authors conclude that that compulsive med-
receptors is associated with cognitive enhancement on ication use in PD is associated with sensitization of
tasks that require activation of the dorsal striatum, ventral striatal circuitry.
whereas dopaminergic stimulation of the relatively in-
tact ventral striatal receptors is associated with impair- Clinical Assessment and Management
ment on cognitive tasks that depend on ventral striatal
activation (ie, dopaminergic “overdose” hypothesis in Screening and Assessment
PD). Of note, the cognitive tasks that rely on ventral The apparent underrecognition of ICDs in PD should
striatal activation include stimulus-outcome tasks, be addressed initially through a careful history and pa-
which involve the ability to modify behaviors by out- tient education before initiating DA treatment, and by
comes, an ability that is impaired at a clinical level in regular monitoring or screening for ICDs throughout
PD patients with ICDs. Thus, one hypothesis is that the course of treatment. Once the possible association
excessive, targeted dopamine stimulation of intact ven- between DRT (particularly DA treatment) and ICDs
tral striatal receptors in early or mild PD leads to an in PD has been introduced, clinicians should inquire
“overdose” of ventral striatal-cortical circuitry that can about ICD behaviors in the context of routine clinical
manifest itself in the clinical phenomenon of care.
impulsive-compulsive behaviors, including ICDs. Screening instruments that lend structure to the
These behaviors, similar to addictive disorders, initially questioning can assist in making a determination if a
may be maintained because of the pleasure feelings in- clinically significant problem exists. Unfortunately,
duced by the activities, but eventually they are experi- there is no single instrument that has been developed
enced as nonpleasurable, yet uncontrollable.58 The be- and validated in PD for the range of ICD and ICD-
haviors are maintained by ongoing dopaminergic related disorders that can occur in this population.
stimulation of a sensitized ventral striatal system, which One existing instrument is the Minnesota Impulsive
is manifested clinically as an increased drive for certain Disorders Interview,22 which queries for the presence
behaviors (ie, limbic system overactivation) and main- of some of the ICDs reported to occur in PD, includ-
tained by an inability to learn from negative decision ing compulsive gambling, buying, and sexual behav-
outcomes (ie, prefrontal cortex overactivation). iors. The South Oaks Gambling Screen is a more de-
Regarding the association between ICDs and a his- tailed instrument that is widely used to screen for PG
tory of ICD behavior or substance use disorders, dif- specifically.60 The Early Intervention Gambling Health
ferences in the neural substrate that predispose to the Test is a brief screen that has been validated in primary
development of ICD-related behaviors before PD onset care settings.61 If a clinician suspects the presence of an
may make patients more vulnerable to manifest similar ICD and needs assistance in the assessment and man-
behaviors during PD in the context of DA treatment. agement process, then the patient should be promptly
It has been proposed that addiction is “the product of referred to a psychiatrist for a comprehensive evalua-
an imbalance between two separate, but interacting, tion and ongoing care.
neural systems that control decision making: an impul-
sive, amygdala system for signaling pain or pleasure of Treatment
immediate prospects, and a reflective, prefrontal cortex Regarding the neurological management of ICDs in
system for signaling pain or pleasure of future pros- PD, case reporting and anecdotal experience suggest
pects. . .drugs can trigger bottom-up, involuntary sig- that ICD behaviors often resolve after reducing the
nals originating from the amygdala that modulate, bias dose of the existing DA, switching to a different ago-
or even hijack the goal-driven cognitive resources that nist, discontinuing DA treatment entirely, or perhaps
are needed for the normal operation of the reflective receiving counseling.12,34 In a recent publication that
Weintraub: Review of ICDs in PD S97
documented the long-term clinical outcomes of 15 Conclusions
ICD patients,62 80% of patients discontinued or sig- Mounting data, including from prospective studies,
nificantly decreased DA treatment, all of whom expe- suggest that DA treatment is associated with the devel-
rienced full or partial remission of ICD symptoms by opment of a variety of ICDs in a subset of PD pa-
self-report. On average, patients significantly decreased tients, particularly those with certain demographic or
their DA dosage and significantly increased their clinical characteristics, whereas greater dosages of
L-dopa dosage, with no change in total LEDD. In ad- L-dopa and short-acting DAs may be associated with
dition, there was no change in UPDRS motor scores DDS and punding. Given the potential substantial im-
over time. These results suggest that many ICD pa- pact of ICDs and related disorders on personal, famil-
tients can be adequately managed by making changes ial, social, and financial well-being, clinicians should
to their PD pharmacotherapy regimen. educate PD patients about and closely monitor for the
The relationship between deep brain stimulation occurrence of these disorders. Prevention and treat-
(DBS) and ICDs appears to be complex. On the one ment strategies involve appropriate patient education,
hand, chronic subthalamic nucleus DBS has been asso- clinical assessment (including questioning regarding
ciated with improvement in ICD symptoms in a small personal or family history of ICD or related behaviors),
careful DA dosing (using lowest effective dosages), and
case series, perhaps secondary to significant reductions
ICD symptom monitoring throughout treatment.
in DRT that occurred after surgery.63 However, there
Existing data suggest that clinical management of
is also anecdotal evidence that although ICDs may be-
clinically significant ICDs should involve serious con-
gin or worsen transiently immediately after subtha-
sideration of a prompt discontinuation or decrease in
lamic nucleus DBS.64 In addition a recent cognitive DA treatment. The risk/benefit ratio of continuing
neuroscience study of PD DBS patients without an with DA therapy should be evaluated for severity of
ICD found that patients were more impulsive in their parkinsonism, severity of ICD behaviors, and available
decision making when their stimulators were turned options for the treatment of both PD and ICDs. In
on.52 addition, empirically validated treatments are emerging
A range of psychiatric treatments, most commonly for ICDs and should be considered for patients with
selective serotonin reuptake inhibitors, have been used co-occurring PD and ICDs.
in the treatment of ICDs in PD, but there is only The association between DA treatment and ICDs in
mixed empirical evidence to support their use for this PD is understandable given existing knowledge regard-
indication in non-PD subjects,65 and no empirical ev- ing the importance of the dopamine system, executive
idence has been reported in PD patients. There are two impairment, and prefrontal cortex-ventral striatal cir-
case reports of successful treatment of PG in PD with cuitry in the development of ICDs. This association
either risperidone34 or quetiapine,66 although the only also offers an opportunity to improve our understand-
controlled study of an atypical antipsychotic drug ing of the neural substrate of a variety of ICDs, be-
(olanzapine) for PG in non-PD subjects was nega- cause discontinuation of DA treatment often leads to a
tive.65 In non-PD patients, recent research suggests prompt resolution of ICD behaviors. As a result, PD
that nalmefene and naltrexone, both opioid antago- patients with an ICD can be studied in both symptom-
nists, are efficacious in the treatment of PG.67,68 atic and asymptomatic states at two proximate time
Pharmacotherapy selection for treatment of ICDs in points, allowing determination of “state” versus “trait”
the general population currently is guided, in part, by neuropsychological and neurobiological correlates. This
cooccurring psychiatric disorders.60,69 However, the ex- may ultimately lead to improved recognition and treat-
tent to which the treatment of cooccurring psychiatric ment of ICDs not only in PD, but in the population
disorders (eg, depression or anxiety) in individuals with at large.
PD and ICDs influences ICD symptom severity is un-
known. Behavioral treatments (eg, cognitive behavioral
therapy and motivational interviewing) appear effective This work was supported by the NIH (National Institute of Mental
in specific groups of patients with PG,70 but their ef- Health, K23MH067894).
ficacy has not been examined in individuals with PD,
and one might predict that certain PD patients (eg,
those with executive impairment) might not respond as References
well to structured behavioral treatments. Similarly, al- 1. American Psychiatric Association. Diagnostic and statistical
though attendance at Gamblers Anonymous meetings manual of mental disorders, fourth edition, text revision. Wash-
ington, DC: American Psychiatric Association, 2000.
has been associated with better treatment outcome in 2. Grant JE, Levine L, Kim D, et al. Impulse control disorders in
non-PD samples,70 no studies have examined its effec- adult psychiatric inpatients. Am J Psychiatry 2005;162:
tiveness in individuals with PD and PG. 2184 –2188.
S98 Annals of Neurology Vol 64 (suppl) December 2008
3. Potenza MN, Hollander E. Pathological gambling and impulse 25. Stucki S, Rihs-Middel M. Prevalence of adult problem and
control disorders. In: Coyle JT, Nemeroff CB, Charney DS, et pathological gambling between 2000 and 2005: an update. J
al, eds. Neuropsychopharmacology: the 5th generation of Gambl Stud 2008;23:245–257.
progress. Baltimore: Lippincott Williams & Wilkins, 2002: 26. Volberg RA, Nysse-Carris KL, Gerstein DR. 2006 California
1725–1742. Problem Gambling Prevalence Survey. Chicago: National
4. Bonvin C, Horvath J, Christe B, et al. Compulsive singing: Opinion Research Center at the University of Chicago, 2006.
Another aspect of punding in Parkinson’s disease. Ann Neurol 27. Shaffer HJ, Hall MN, Vander J. Estimating the prevalence of
2007;62:525–528. disordered gambling behavior in the United States and Canada:
5. Giovannoni G, O’Sullivan JD, Turner K, et al. Hedonistic ho- a research synthesis. Am J Public Health. 1999;89:1369 –1376.
meostatic dysregulation in patients with Parkinson’s disease on 28. Black DW. A review of compulsive buying disorder. World
dopamine replacement therapies. J Neurol Neurosurg Psychia- Psychiatry 2007;6:14 –18.
try 2000;68:423– 428. 29. Lilenfeld LRR, Ringham R, Kalarchian MA, et al. A family
6. Evans AH, Katzenschlager R, Paviour D, et al. Punding in Par- history study of binge-eating disorder. Compr Psychiatry 2008;
kinson’s disease: its relation to the dopamine dysregulation syn- 49:247–254.
drome. Mov Disord 2004;19:397– 405.
30. Coleman E. Is your patient suffering from compulsive sexual
7. Pezzella FR, Di Rezze S, Chianese M, et al. Hedonistic homeo-
behavior? Psychiatr Ann 1992;22:320 –325.
static dysregulation in Parkinson’s disease: a short screening
31. Giladi N, Weitzman N, Schreiber S, et al. New onset height-
questionnaire. Neurol Sci 2003;24:205–206.
ened interest or drive for gambling, shopping, eating or sexual
8. Serrano-Dueñas M. Chronic dopamimetic drug addiction and
activity in patients with Parkinson’s disease: the role of dopa-
pathologic gambling in patients with Parkinson’s disease—pre-
sentation of four cases. German J Psychiatry 2002;5:62– 66. mine agonist treatment and age at motor symptoms onset.
9. Voon V. Repetition, repetition, and repetition: compulsive and J Psychopharmacol (Oxf) 2007;21:501–506.
punding behaviors in Parkinson’s disease. Mov Disord 2004;19: 32. Avanzi M, Baratti M, Cabrini S, et al. Prevalence of patholog-
367–370. ical gambling in patients with Parkinson’s disease. Mov Disord
10. Evans AH, Lawrence AD, Potts J, et al. Factors influencing 2006;21:2068 –2072.
susceptibility to compulsive dopaminergic drug use in Parkin- 33. Tyne HL, Medley G, Ghadiali E, Steigner MJ. Gambling in
son disease. Neurology 2005;65:1570 –1574. Parkinson’s disease. Mo Disord 2004;19(suppl 9):S195.
11. Kurlan R. Disabling repetitive behaviors in Parkinson’s disease. 34. Dodd ML, Klos KJ, Bower JH, et al. Pathological gambling
Mov Disord 2004;19:433– 437. caused by drugs used to treat Parkinson disease. Arch Neurol
12. Driver-Dunckley E, Samanta J, Stacy M. Pathological gambling 2005;62:1–5.
associated with dopamine agonist therapy in Parkinson’s dis- 35. Klos KJ, Bower JH, Josephs KA, et al. Pathological hypersexu-
ease. Neurology 2003;61:422– 423. ality predominantly linked to adjuvant dopamine agonist ther-
13. Lu C, Bharmal A, Suchowersky O. Gambling and Parkinson’s apy in Parkinson’s disease and multiple system atrophy. Parkin-
Disease. Arch Neuro. 2006;63:298. sonism Relat Disord 2005;11:381–386.
14. Grosset KA, Macphee G, Pal G, et al. Problematic gambling on 36. Lawrence AJ, Blackwell AD, Barker RA, et al. Predictors of
dopamine agonists: not such a rarity. Mov Disord 2006;21: punding in Parkinson’s disease: results from a questionnaire
2206 –2208. survey. Mov Disord 2007;22:2339 –2345.
15. Voon V, Hassan K, Zurowski M, et al. Prevalence of repetitive 37. Gallagher DA, O’Sullivan SS, Evans AH, et al. Pathological
and reward-seeking behaviors in Parkinson disease. Neurology gambling in Parkinson’s disease: risk factors and differences
2006;67:1254 –1257. from dopamine dysregulation. An analysis of published case se-
16 Isaias IU, Siri C, Cilia R, et al. The relationship between im- ries. Mov Disord 2007; 22:1757–1763.
pulsivity and impulse control disorders in Parkinson’s disease. 38. Hollander E, Evers M. New developments in impulsivity. Lan-
Mov Disord 2008;23:411– 415. cet 2001;358:949 –950.
17. Pontone G, Williams JR, Bassett SS, et al. Clinical features as- 39. Potenza MN, Leung H-C, Blumberg HP, et al. An fMRI
sociated with impulse control disorders in Parkinson disease. Stroop task study in ventromedial prefrontal cortical func-
Neurology 2006;67:1258 –1261. tion in pathological gamblers. Am J Psychiatry 2003;160:
18. Nirenberg MJ, Waters C. Compulsive eating and weight gain 1990 –1994.
related to dopamine agonist use. Mov Disord 2006;21:
40. Bechara A, Tranel D, Damasio H. Characterization of the
524 –529.
decision-making deficit of patients with ventromedial prefrontal
19. Voon V, Hassan K, Zurowski M, et al. Prospective prevalence
cortex lesions. Brain 2000;123:2189 –2202.
of pathological gambling and medication association in Parkin-
41. O’Doherty J, Kringelbach ML, Rolls ET, et al. Abstract reward
son disease. Neurology 2006;66:1750 –1752.
and punishment representations in the human orbitofrontal
20. Lesieur HR, Blume SB. The South Oaks Gambling Screen
(SOGS): a new instrument for the identification of pathological cortex. Nat Neurosci 2001;4:95–102.
gamblers. Am J Psychiatry 1987;144:1184 –1188. 42. Reuter J, Raedler T, Rose M. Pathological gambling is linked to
21. Weintraub D, Siderowf AD, Potenza MN, et al. Association of reduced activation of the mesolimbic reward system. Nat Neu-
dopamine agonist use with impulse control disorders in Parkin- rosci 2005;8:147–148.
son disease. Arch Neurol 2006;63:969 –973. 43. Bechara A, Damasio H, Damasio AR, et al. Different contribu-
22. Christenson GA, Faber RJ, deZwaan M. Compulsive buying: tions of the human amygdala and ventromedial prefrontal cor-
descriptive characteristics and psychiatric comorbidity. J Clin tex to decision-making. J Neurosci 1999;19:5473–5481.
Psychiatry 1994;55:5–11. 44. Chambers RA, Potenza MN. Neurodevelopment, impulsivity,
23. Miyasaki J, Hassan KL, Lang AE, et al. Punding prevalence in and adolescent gambling. J Gambl Stud 2003;19:53– 84.
Parkinson’s disease. Mov Disord 2007;22:1179 –1181. 45. Chambers RA, Taylor JR, Potenza MN. Developmental neuro-
24. Pietrzak RH, Morasco BJ, Blanco C, et al. Gambling level and circuitry of motivation in adolescence: a critical period of ad-
psychiatric and medical disorders in older adults: results from diction vulnerability. Am J Psychiatry 2003;160:1041–1052.
the National Epidemiologic Survey on Alcohol and Related 46. Yin HH, Knowlton BJ. The role of the basal ganglia in habit
Conditions. Am J Geriatr Psychiatry 2007;15:301–313. formation. Nat Rev Neurosci 2006;7:464 – 476.
Weintraub: Review of ICDs in PD S99
47. Bjarkam CR, Sørensen JC. Therapeutic strategies for neurode- 60. Pathological gambling: a clinical guide to treatment. Arlington,
generative disorders: emerging clues from Parkinson’s disease. VA: American Psychiatric Publishing, 2004.
Biol Psychiatry 2004;56:213–216. 61. Potenza MN, Fiellin DA, Heninger GR, et al. Gambling: an
48. Levin BE, Katzen HL. Early cognitive changes and nondement- addictive behavior with health and primary care implications.
ing behavioral abnormalities in Parkinson’s disease. In: Weiner J Gen Intern Med 2002;17:721–732.
WJ, Lang AE, eds. Behavioral neurology of movement disor- 62. Mamikonyan E, Siderowf AD, Duda JE, et al. Long-term
ders. New York: Raven Press, 1995:85–95. follow-up of impulse control disorders in Parkinson’s disease.
49. Green J, McDonald WM, Vitek JL, et al. Cognitive impair- Mov Disord 2008;23:75– 80.
ments in advanced PD without dementia. Neurology 2002;59:
63. Ardouin C, Voon V, Worbe Y, et al. Pathological gambling in
1320 –1324.
Parkinson’s disease improves on chronic subthalamic nucleus
50. Dubois B, Pillon B. Cognitive deficits in Parkinson’s disease.
stimulation. Mov Disord 2006;21:1941–1946.
J Neurol 1997;244:2– 8.
51. Brand M, Labudda K, Kalbe E, et al. Decision-making impair- 64. Smeding HMM, Goudriaan AE, Foncke EMJ, et al. Patholog-
ments in patients with Parkinson’s disease. Behav Neurol 2004; ical gambling after bilateral subthalamic nucleus stimulation in
15:77– 85. Parkinson disease. J Neurol Neurosurg Psychiatry 2007;78:
52. Frank JF, Samanta J, Moustafa AA, et al. Hold your horses: 517–519.
impulsivity, deep brain stimulation, and medication in parkin- 65. Grant JE, Potenza MN. Impulse control disorders: clinical
sonism. Science 2007;318:1309 –1312. characteristics and pharmacological management. Ann Clin
53. Brusa L, Bassi A, Stefani A, et al. Pramipexole in comparison to Psychiatry 2004;16:27–34.
l-dopa: a neuropsychological study. J Neural Transm 2003;110: 66. Sevincok L, Akoglu A, Akyol A. Quetiapine in a case with Par-
373–380. kinson disease and pathological gambling [letter]. J Clin Psy-
54. Gerlach M, Double K, Arzberger T, et al. Dopamine receptor chopharmacol 2007;27:107–108.
agonists in current clinical use: comparative dopamine receptor 67. Grant JE, Potenza MN, Hollander E, et al. Multicenter in-
binding profiles defined in the human striatum. J Neural vestigation of the opioid antagonist nalmefene in the treat-
Transm 2003;110:1119 –1127. ment of pathological gambling. Am J Psychiatry 2006;163:
55. Sokoloff P, Giros B, Martres MP, et al. Molecular cloning and 303–312.
characterization of a novel dopamine receptor (D3) as a target 68. Kim SW, Grant JE, Adson DE, et al. Double-blind naltrexone
for neuroleptics. Nature 1990;347:146 –151. and placebo comparison study in the treatment of pathological
56. Cools R. Dopaminergic modulation of cognitive function—im-
gambling. Biol Psychiatry 2001;49:914 –921.
plications for l-DOPA treatment in Parkinson’s disease. Neuro-
69. Potenza MN. Impulse control disorders and co-occurring
sci Biobehav Rev 2006;30:1–23.
disorders: dual diagnosis considerations. J Dual Diagn 2007;3:
57. Cools R, Altamirano L, D’Esposito M. Reversal learning in Par-
kinson’s disease depends on medication status and outcome va- 47–57.
lence. Neuropsychologia 2006;44:1663–1673. 70. Hodgins DC, Petry NM. Cognitive and behavioral treatments.
58. Evans AH, Pavese N, Lawrence AD, et al. Compulsive drug use In: Grant JE, Potenza MN, eds. Pathological gambling: a clin-
linked to sensitized ventral striatal dopamine transmission. Ann ical guide to treatment. Washington, DC: American Psychiatric
Neurol 2006;59:852– 858. Press, 2004:169 –188.
59. Bechara A. Decision making, impulse control and loss of will- 71. Tomkins DM, Sellers EM. Addiction and the brain: the role of
power to resist drugs: a neurocognitive perspective. Nat Neuro- neurotransmitters in the cause and treatment of drug depen-
sci 2005;8:1458 –1463. 60 dence. CMAJ 2001;164:817– 821.
S100 Annals of Neurology Vol 64 (suppl) December 2008
You might also like
- Fast Facts: Psychosis in Parkinson's Disease: Finding the right therapeutic balanceFrom EverandFast Facts: Psychosis in Parkinson's Disease: Finding the right therapeutic balanceNo ratings yet
- Jurnal ManduaDocument7 pagesJurnal ManduaMinorC3No ratings yet
- The Prevention and Treatment of Disease with a Plant-Based Diet Volume 2: Evidence-based articles to guide the physicianFrom EverandThe Prevention and Treatment of Disease with a Plant-Based Diet Volume 2: Evidence-based articles to guide the physicianNo ratings yet
- Impulse Control Disorders in Parkinson's Disease: Definition, Epidemiology, Risk Factors, Neurobiology and ManagementDocument5 pagesImpulse Control Disorders in Parkinson's Disease: Definition, Epidemiology, Risk Factors, Neurobiology and Managementkumaran5488No ratings yet
- Parkinsonism and Related Disorders: Dolores Vilas, Claustre Pont-Sunyer, Eduardo TolosaDocument5 pagesParkinsonism and Related Disorders: Dolores Vilas, Claustre Pont-Sunyer, Eduardo Tolosakumaran5488No ratings yet
- Farmacologia de Los Medicamentos Antipsicoticos en AmDocument9 pagesFarmacologia de Los Medicamentos Antipsicoticos en AmedgarmoncadaNo ratings yet
- Course of Psychiatric Symptoms and GlobalDocument8 pagesCourse of Psychiatric Symptoms and GloballoloasbNo ratings yet
- STEPPS Preliminary Report 2002Document11 pagesSTEPPS Preliminary Report 2002MARGARITA ALONSO ESCAMILLANo ratings yet
- Current Treatment of Behavioral and Cognitive Symptoms of Parkinson's DiseaseDocument9 pagesCurrent Treatment of Behavioral and Cognitive Symptoms of Parkinson's DiseasePriska AmeliaNo ratings yet
- Acn3 7 449Document13 pagesAcn3 7 449Elisa FioraNo ratings yet
- A Review of Bipolar Disorder Among Adults PDFDocument13 pagesA Review of Bipolar Disorder Among Adults PDFNadyaNo ratings yet
- JNeurosciRuralPract6165-7834297 214542Document12 pagesJNeurosciRuralPract6165-7834297 214542Edu SajquimNo ratings yet
- Personality Addiction Dopamine Insights From Parkinsons Disease DagherDocument9 pagesPersonality Addiction Dopamine Insights From Parkinsons Disease DagherSimon BrezovarNo ratings yet
- Management of Psychiatric Disorders in Children and Adolescents With Atypical AntipsychoticsDocument17 pagesManagement of Psychiatric Disorders in Children and Adolescents With Atypical Antipsychoticsnithiphat.tNo ratings yet
- Manejo Depresion 1Document10 pagesManejo Depresion 1Luis HaroNo ratings yet
- Park, 2019 - NEJM - DepressionDocument10 pagesPark, 2019 - NEJM - DepressionFabian WelchNo ratings yet
- 1 s2.0 S1353802013000746 Main PDFDocument9 pages1 s2.0 S1353802013000746 Main PDFkumaran5488No ratings yet
- PDpsychosisDocument8 pagesPDpsychosismyosotysNo ratings yet
- Seminar: Epidemiology, Comorbidity, and DiagnosisDocument11 pagesSeminar: Epidemiology, Comorbidity, and DiagnosisMartin GiraudoNo ratings yet
- Linehan 1991Document5 pagesLinehan 1991Ekatterina DavilaNo ratings yet
- Estudo. Espectro BipolarDocument9 pagesEstudo. Espectro BipolarGabriel LemosNo ratings yet
- Antipsychotic-Related Movement Disorders: Drug-Induced Parkinsonism vs. Tardive Dyskinesia-Key Differences in Pathophysiology and Clinical ManagementDocument16 pagesAntipsychotic-Related Movement Disorders: Drug-Induced Parkinsonism vs. Tardive Dyskinesia-Key Differences in Pathophysiology and Clinical ManagementudzmaNo ratings yet
- Caffeine and Risk of Parkinson's Disease in A Large Cohort of Men and WomenDocument7 pagesCaffeine and Risk of Parkinson's Disease in A Large Cohort of Men and WomenJenivia LulileloNo ratings yet
- Coffee and Tea Consumption and The Risk of Parkinson's DiseaseDocument7 pagesCoffee and Tea Consumption and The Risk of Parkinson's DiseaseJenivia LulileloNo ratings yet
- Ultra High Dilution of Zinc in The Management of Refractory Parkinson'S Disease-A Case ReportDocument10 pagesUltra High Dilution of Zinc in The Management of Refractory Parkinson'S Disease-A Case ReportTJPRC PublicationsNo ratings yet
- Severely Affected by Parkinson Disease: The Patient's View and Implications For Palliative CareDocument7 pagesSeverely Affected by Parkinson Disease: The Patient's View and Implications For Palliative CareLorenaNo ratings yet
- A Review of Bipolar DisorderDocument13 pagesA Review of Bipolar DisorderCharpapathNo ratings yet
- Depakote Child PsychiDocument12 pagesDepakote Child PsychiPaul BerndNo ratings yet
- Parkinson en Hombres y MujeresDocument15 pagesParkinson en Hombres y MujeresAbigail RamosNo ratings yet
- Neuroleptic DrugDocument7 pagesNeuroleptic DrugyunikNo ratings yet
- The Neuropsychiatry of Parkinson Disease: A Perfect Storm: SciencedirectDocument21 pagesThe Neuropsychiatry of Parkinson Disease: A Perfect Storm: SciencedirectroxanaNo ratings yet
- Comorbidity Between Substance Use Disorder and Severe Mental Illness: Dual DiagnosisDocument11 pagesComorbidity Between Substance Use Disorder and Severe Mental Illness: Dual DiagnosisJulián Alberto MatulevichNo ratings yet
- Psicosis en Adulto Mayor-3Document8 pagesPsicosis en Adulto Mayor-3Carolina JaramilloNo ratings yet
- A Case Study of A Mental DisorderDocument7 pagesA Case Study of A Mental DisorderMaurine TuitoekNo ratings yet
- Jurnal 3Document12 pagesJurnal 3Mega Cahya AlfiraNo ratings yet
- Parkinsonism and Related DisordersDocument7 pagesParkinsonism and Related DisordersnellieauthorNo ratings yet
- Parkinson's Disease: EpidemiologyDocument6 pagesParkinson's Disease: EpidemiologyCarlos MichasNo ratings yet
- Apatia e ParkinsonDocument11 pagesApatia e ParkinsonFernanda NascimentoNo ratings yet
- Mds 21803Document7 pagesMds 21803Elisa FioraNo ratings yet
- Impulse Control Disorders in Parkinson's Disease: Crossroads Between Neurology, Psychiatry and NeuroscienceDocument11 pagesImpulse Control Disorders in Parkinson's Disease: Crossroads Between Neurology, Psychiatry and NeuroscienceCarmen CiursaşNo ratings yet
- Diagnosis and Management of Depression in Primary CareDocument8 pagesDiagnosis and Management of Depression in Primary CareMaria Jose OcNo ratings yet
- Bipolar 2 PDFDocument3 pagesBipolar 2 PDFPrecious Ann ParelNo ratings yet
- Beitz 2014Document10 pagesBeitz 2014Anna Beatriz Silva EspindolaNo ratings yet
- Lino Palacios Cruz, Francisco Romo Nava, Luis Rodrigo Patiño Durán, Fernando Leyva Hernández, Eduardo Barragán Pérez, Claudia Becerra Palars, Francisco de La Peña OlveraDocument5 pagesLino Palacios Cruz, Francisco Romo Nava, Luis Rodrigo Patiño Durán, Fernando Leyva Hernández, Eduardo Barragán Pérez, Claudia Becerra Palars, Francisco de La Peña Olveraelchito1987No ratings yet
- ParkinsonDocument157 pagesParkinsonMassiel Alvarado100% (1)
- Suicide and Treatm EntDocument8 pagesSuicide and Treatm EntSourav DasNo ratings yet
- Dissociative Identity Disorder A Case of Three SelDocument2 pagesDissociative Identity Disorder A Case of Three SelMartín SalamancaNo ratings yet
- Ansiedade 04Document9 pagesAnsiedade 04Karina BorgesNo ratings yet
- Dialectical Behavior Therapy For Patients With Borderline Personality Disorder and Drug-DependenceDocument15 pagesDialectical Behavior Therapy For Patients With Borderline Personality Disorder and Drug-DependenceOsvaldoMuñozEspinozaNo ratings yet
- De Fining Atypical Anxiety in Parkinson's Disease: Clinical PracticeDocument11 pagesDe Fining Atypical Anxiety in Parkinson's Disease: Clinical PracticeketevanNo ratings yet
- TX No Farmacologico QX NeuropsiquiatricosDocument16 pagesTX No Farmacologico QX NeuropsiquiatricosCONSEJO R4No ratings yet
- Psychopharmacology of AutismDocument17 pagesPsychopharmacology of AutismMichelle2No ratings yet
- Bipolaridad 1Document12 pagesBipolaridad 1JambisNo ratings yet
- NIH Public Access: Sleep and Impulsivity in Parkinson's DiseaseDocument10 pagesNIH Public Access: Sleep and Impulsivity in Parkinson's DiseaseCarmen CiursaşNo ratings yet
- Babeo en El ParkinsonDocument3 pagesBabeo en El Parkinsonfernanda cespedesNo ratings yet
- Delirium: Robyn P. Thom, M.D., Nomi C. Levy-Carrick, M.D., M.Phil., Melissa Bui, M.D., David Silbersweig, M.DDocument9 pagesDelirium: Robyn P. Thom, M.D., Nomi C. Levy-Carrick, M.D., M.Phil., Melissa Bui, M.D., David Silbersweig, M.DfatinNo ratings yet
- Parkinson's Disease: A Treatment GuideDocument8 pagesParkinson's Disease: A Treatment GuideaimahNo ratings yet
- Journal ClubDocument63 pagesJournal Clubdrkadiyala2No ratings yet
- McIntyre, CANMAT Comorbidity - Metabolic, Ann Clin Psyt 2012Document13 pagesMcIntyre, CANMAT Comorbidity - Metabolic, Ann Clin Psyt 2012JESUS FRANCISCO SANCHEZ PATRICIONo ratings yet
- Comparative Analysis of Self-Injury in People With Psychopathology or Neurodevelopmental DisordersDocument13 pagesComparative Analysis of Self-Injury in People With Psychopathology or Neurodevelopmental Disordersme13No ratings yet
- Adhd Research Paper TopicsDocument4 pagesAdhd Research Paper Topicsfvffv0x7100% (1)
- Level 1 Manual Modules 16 PDFDocument215 pagesLevel 1 Manual Modules 16 PDFMaria Bagourdi100% (5)
- Factors Influencing Impulse BuyingDocument23 pagesFactors Influencing Impulse BuyingRafa CohenNo ratings yet
- Bedtime Procrastination Introducing A New Area of ProcrastinationDocument8 pagesBedtime Procrastination Introducing A New Area of ProcrastinationFercho MedNo ratings yet
- Telaah JurnalDocument7 pagesTelaah JurnalPramyta FirstNo ratings yet
- Petry, Nancy M - Behavioral Addictions - DSM-5 and Beyond-Oxford University Press (2016) PDFDocument257 pagesPetry, Nancy M - Behavioral Addictions - DSM-5 and Beyond-Oxford University Press (2016) PDFanang7No ratings yet
- Chapter 1-3 3is Grouop6Document23 pagesChapter 1-3 3is Grouop6LoeynahcNo ratings yet
- WSC-2024-General Knowledge Quiz-Nostradamus O, NostalgiaDocument9 pagesWSC-2024-General Knowledge Quiz-Nostradamus O, NostalgiayousuffateemaNo ratings yet
- Reflection-Communicating About Mental HealthDocument6 pagesReflection-Communicating About Mental HealthAshley KiddNo ratings yet
- IE y MFN - Rodriguez2018 PDFDocument10 pagesIE y MFN - Rodriguez2018 PDFnicole toroNo ratings yet
- Management of ADHD in Children and Young PeopleDocument52 pagesManagement of ADHD in Children and Young PeopleAna Santos0% (1)
- Tihitina GirmaDocument87 pagesTihitina GirmaDaveNo ratings yet
- Relation Between Time Perspective and Delay Discounting - A LiteraDocument20 pagesRelation Between Time Perspective and Delay Discounting - A LiteraCarlos FeratNo ratings yet
- Ce Lenk 2013Document4 pagesCe Lenk 2013RajabSaputraNo ratings yet
- Analysing Important Antecedents On Online Impulsive Buying Among MillennialDocument23 pagesAnalysing Important Antecedents On Online Impulsive Buying Among Millennialstfasinaga.urukNo ratings yet
- 2020 수능의 감잡기 변형문제 3강 (60문제) -편집가능 (Vvip)Document24 pages2020 수능의 감잡기 변형문제 3강 (60문제) -편집가능 (Vvip)1213wldorlaNo ratings yet
- University of NottinghamDocument119 pagesUniversity of NottinghamRini DasNo ratings yet
- Behavioural Brain Research: Jinjin Wang, Yuzhen Li, Siqi Wang, Wenmin Guo, Hang Ye, Jinchuan Shi, Jun LuoDocument8 pagesBehavioural Brain Research: Jinjin Wang, Yuzhen Li, Siqi Wang, Wenmin Guo, Hang Ye, Jinchuan Shi, Jun LuoElíasNo ratings yet
- PAP Convention - Abstracts 2017Document78 pagesPAP Convention - Abstracts 2017TinoRepaso50% (2)
- CRIM 3 Human Behavior VictimologyDocument4 pagesCRIM 3 Human Behavior VictimologyAero Eusheko Borja100% (1)
- Attention Resource HandbookDocument63 pagesAttention Resource Handbookapi-202351147No ratings yet
- Smeijsters, H. and Clever, G. (2006) - The Treatment of Aggression Using Arts Therapies in Forensi PDFDocument22 pagesSmeijsters, H. and Clever, G. (2006) - The Treatment of Aggression Using Arts Therapies in Forensi PDFaleksandra_radevicNo ratings yet
- Friendship Quality Emotion Understanding and Emotion Regulation of Children With and Without Attention Deficit Hyperactivity Disorder or SpecificDocument18 pagesFriendship Quality Emotion Understanding and Emotion Regulation of Children With and Without Attention Deficit Hyperactivity Disorder or SpecificÁgata Rodrigues da CâmaraNo ratings yet
- Recklessness To Calculated RisksDocument3 pagesRecklessness To Calculated RisksYungston100% (1)
- Mini Lesson Managing ImpulsivityDocument2 pagesMini Lesson Managing Impulsivityapi-378198603100% (1)
- Borderline and Histrionic Personality DisordersDocument38 pagesBorderline and Histrionic Personality DisordersSahel100% (1)
- 1 s2.0 S2451902222001471 MainDocument11 pages1 s2.0 S2451902222001471 MainAlejandro CabaNo ratings yet
- The Role of Fashion Orientated Involvement and Individual Mood On Impulse Buying in TabrizDocument7 pagesThe Role of Fashion Orientated Involvement and Individual Mood On Impulse Buying in TabrizShaifaliChauhanNo ratings yet
- Violence Assessment ToolDocument1 pageViolence Assessment ToolmahmoudNo ratings yet
- Online Reviews and Impulse Buying Behavior: The Role of Browsing and ImpulsivenessDocument24 pagesOnline Reviews and Impulse Buying Behavior: The Role of Browsing and Impulsivenessruby_evangelinNo ratings yet
- Allen Carr's Easy Way to Quit Vaping: Get Free from JUUL, IQOS, Disposables, Tanks or any other Nicotine ProductFrom EverandAllen Carr's Easy Way to Quit Vaping: Get Free from JUUL, IQOS, Disposables, Tanks or any other Nicotine ProductRating: 5 out of 5 stars5/5 (31)
- Alcoholics Anonymous, Fourth Edition: The official "Big Book" from Alcoholic AnonymousFrom EverandAlcoholics Anonymous, Fourth Edition: The official "Big Book" from Alcoholic AnonymousRating: 5 out of 5 stars5/5 (22)
- Healing Your Aloneness: Finding Love and Wholeness Through Your Inner ChildFrom EverandHealing Your Aloneness: Finding Love and Wholeness Through Your Inner ChildRating: 3.5 out of 5 stars3.5/5 (9)
- Breaking Addiction: A 7-Step Handbook for Ending Any AddictionFrom EverandBreaking Addiction: A 7-Step Handbook for Ending Any AddictionRating: 4.5 out of 5 stars4.5/5 (2)
- Stop Drinking Now: The original Easyway methodFrom EverandStop Drinking Now: The original Easyway methodRating: 5 out of 5 stars5/5 (29)
- Self-Love Affirmations For Deep Sleep: Raise self-worth Build confidence, Heal your wounded heart, Reprogram your subconscious mind, 8-hour sleep cycle, know your value, effortless healingsFrom EverandSelf-Love Affirmations For Deep Sleep: Raise self-worth Build confidence, Heal your wounded heart, Reprogram your subconscious mind, 8-hour sleep cycle, know your value, effortless healingsRating: 4.5 out of 5 stars4.5/5 (6)
- The Heart of Addiction: A New Approach to Understanding and Managing Alcoholism and Other Addictive BehaviorsFrom EverandThe Heart of Addiction: A New Approach to Understanding and Managing Alcoholism and Other Addictive BehaviorsNo ratings yet
- We Are the Luckiest: The Surprising Magic of a Sober LifeFrom EverandWe Are the Luckiest: The Surprising Magic of a Sober LifeRating: 5 out of 5 stars5/5 (183)
- Easyway Express: Stop Smoking and Quit E-CigarettesFrom EverandEasyway Express: Stop Smoking and Quit E-CigarettesRating: 5 out of 5 stars5/5 (15)
- Allen Carr's Easy Way to Quit Smoking Without Willpower: The best-selling quit smoking method updated for the 21st centuryFrom EverandAllen Carr's Easy Way to Quit Smoking Without Willpower: The best-selling quit smoking method updated for the 21st centuryRating: 5 out of 5 stars5/5 (47)
- Save Me from Myself: How I Found God, Quit Korn, Kicked Drugs, and Lived to Tell My StoryFrom EverandSave Me from Myself: How I Found God, Quit Korn, Kicked Drugs, and Lived to Tell My StoryNo ratings yet
- Allen Carr's Quit Drinking Without Willpower: Be a happy nondrinkerFrom EverandAllen Carr's Quit Drinking Without Willpower: Be a happy nondrinkerRating: 5 out of 5 stars5/5 (8)
- Guts: The Endless Follies and Tiny Triumphs of a Giant DisasterFrom EverandGuts: The Endless Follies and Tiny Triumphs of a Giant DisasterRating: 4 out of 5 stars4/5 (99)
- Twelve Steps and Twelve Traditions: The “Twelve and Twelve” — Essential Alcoholics Anonymous readingFrom EverandTwelve Steps and Twelve Traditions: The “Twelve and Twelve” — Essential Alcoholics Anonymous readingRating: 5 out of 5 stars5/5 (11)
- The Language of Letting Go: Daily Meditations on CodependencyFrom EverandThe Language of Letting Go: Daily Meditations on CodependencyRating: 4.5 out of 5 stars4.5/5 (18)
- Stop Smoking with Allen Carr: Includes 70 minute audio epilogue read by AllenFrom EverandStop Smoking with Allen Carr: Includes 70 minute audio epilogue read by AllenRating: 5 out of 5 stars5/5 (62)
- Alcoholics Anonymous: The Landmark of Recovery and Vital LivingFrom EverandAlcoholics Anonymous: The Landmark of Recovery and Vital LivingRating: 4.5 out of 5 stars4.5/5 (291)
- Drunk-ish: A Memoir of Loving and Leaving AlcoholFrom EverandDrunk-ish: A Memoir of Loving and Leaving AlcoholRating: 4 out of 5 stars4/5 (6)
- THE FRUIT YOU’LL NEVER SEE: A memoir about overcoming shame.From EverandTHE FRUIT YOU’LL NEVER SEE: A memoir about overcoming shame.Rating: 4 out of 5 stars4/5 (7)
- Intoxicating Lies: One Woman’s Journey to Freedom from Gray Area DrinkingFrom EverandIntoxicating Lies: One Woman’s Journey to Freedom from Gray Area DrinkingRating: 5 out of 5 stars5/5 (1)
- Allen Carr's Easy Way to Quit Cannabis: Regain your drive, health and happinessFrom EverandAllen Carr's Easy Way to Quit Cannabis: Regain your drive, health and happinessRating: 4.5 out of 5 stars4.5/5 (31)
- Total Dopamine Detox in 7 Easy Steps: Become the Master of Your Brain to Quit Your Phone Addiction, Porn Addiction, or Manage Your ADHDFrom EverandTotal Dopamine Detox in 7 Easy Steps: Become the Master of Your Brain to Quit Your Phone Addiction, Porn Addiction, or Manage Your ADHDRating: 4 out of 5 stars4/5 (8)
- Little Red Book: Alcoholics AnonymousFrom EverandLittle Red Book: Alcoholics AnonymousRating: 5 out of 5 stars5/5 (20)