Professional Documents
Culture Documents
Uchida 2010
Uploaded by
al qurtubi al andalusiOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Uchida 2010
Uploaded by
al qurtubi al andalusiCopyright:
Available Formats
486 Letters to the editor / Joint Bone Spine 77 (2010) 482–491
Table 1
Blood chemical values during a 5-year follow-up.
Parameter RL 11/04 05/05 03/07 10/07 01/08 05/08 03/09 05/09 10/09
Steroid in mg 0 2.5§ 2.5§ 0 0 0 40$ 10$ 4$
AZT in mg 0 0 0 0 0 0 100 50# 0
BSR < 10/< 20 mm/ 93/115 75/104 61/92 77/101 49/80 52/77 108/128 na na
CK 172U/L 749 na 432 160 135 169 4569 62 953
Sodium 132–146mmol/L 130 na 136 132 136 143 127 136 137
␥-globulins 10–19% 29.9 na na 24.8 23.8 20.5 28.5 na 27.6
Eos 1–4% 1.4 na na 10.1 15.1 11.1 0.4 2.1 na
LYC 20–40% 16.7 na na 32.6 na na 17.0 26.7 na
HbA1c < 6% 7.2 7.2 7.8 7.9 7.7 na 8.1 8.4 na
RL: reference limits, Steroid: steroid dosage, AZT: azathioprin dosage, BSR: blood sedimentation rate, CK: creatine-kinase, Eos: eosinophils, LYC: lymphocyte count, §:
prednisolone, $: methyl-prednisolone started in 2/09 at a dosage of 80 mg, na: not available, #: AZT was discontinued after 3 months because of elevated liver function
parameters.
References
[1] Kocaaga Z, Bal S, Turan Y, et al. Camptocormia and dropped head syndrome as
a clinic picture of myotonic myopathy. Joint Bone Spine 2008;75:730–3.
[2] Leano AM, Miller K, White AC. Chronic graft-versus-host disease-related
polymyositis as a cause of respiratory failure following allogeneic bone marrow
transplant. Bone Marrow Transplant 2000;26:1117–20.
[3] Slobodin G, Rozenbaum M, Weller B, et al. Dropped head: an unusual presen-
tation of dermatomyositis. J Rheumatol 2005;32:1174–5.
[4] Kastrup A, Gdynia HJ, Nägele T, et al. Dropped-head syndrome due to steroid
responsive focal myositis: a case report and review of the literature. J Neurol
Sci 2008;267:162–5.
[5] Gaeta M, Mazziotti S, Toscano A, et al. Dropped-head” syndrome due to
isolated myositis of neck extensor muscles: MRI findings. Skeletal Radiol
2006;35:110–2.
[6] Bahnof R. The dropped head syndrome: rehabilitation of cervical focal myositis.
Disabil Rehabil 1999;21:563–5.
[7] Biran I, Cohen O, Diment J, et al. Focal, steroid responsive myositis causing
Fig. 1. Presented patient with dropped head syndrome due to polymyositis before dropped head syndrome. Muscle Nerve 1999;22:769–71.
(left panel) and 2 months after re-starting steroids (right panel). [8] Dalakas MC, Hohlfeld R. Polymyositis and dermatomyositis. Lancet
2003;362:971–82.
[9] Finsterer J. Dropped head syndrome in mitochondriopathy. Eur Spine J
myocardial thickening. Cerebral CT showed basal ganglia calcifi- 2004;13:652–6.
cation bilaterally, discrete diffuse atrophy, and lacunas. Cerebral [10] Rahim F, Gupta D, Bertorini TE, et al. Dropped head presentation of mitochon-
drial myopathy. J Clin Neuromuscul Dis 2003;5:108–14.
MRI revealed multiple glial spots exclusively. MRI of the cervical
spine was normal.
Josef Finsterer ∗
Since DHS was attributed to a relapse of PM, methyl-
Krankenanstalt Rudolfstiftung, Postfach 20,
prednisolone (80 mg/d) was restarted. Additionally, azathioprin
1180 Vienna, Austria
(100 mg/d) was given. Under this regimen, DHS improved by
60–70% within 2 months. Methyl-prednisolone was tapered down
Marlies Frank
to 4 mg within 8 months. Azathioprin had to be discontinued
Elisabeth Krexner
after 3 months because of hepatopathy. At the last follow-up,
First Medical Department, Krankenanstalt
8 months after re-starting steroids, his neurological condition was
Rudolfstiftung, Vienna, Austria
unchanged.
Arguments for a causative role of PM are that DHS has been ∗ Corresponding author. Tel.: +43 1 71165 92085;
previously described in PM [2], dermatomyositis [3], and as focal
fax: +43 1 4781711.
myositis of the extensor neck muscles [4,5,6,7,8], and that DHS
E-mail address: fifigs1@yahoo.de
responded well to steroids. Arguments for a mitochondrial disorder
(J. Finsterer).
(MID) are that there was basal ganglia calcification, hypoacu-
sia, diabetes, short stature, osteoporosis, recurrent hyponatremia,
10 February 2010
hyperlipidemia, myocardial thickening despite normal blood pres-
sure and short stature and hypoacusis in his mother, albinism, Available online18 May 2010
visual impairment, nystagmus and hypothyroidism in his daugh- doi:10.1016/j.jbspin.2010.02.028
ter, and that MID has been previously reported to cause DHS
[9,10]. Steroid-myopathy was excluded since DHS improved Unusual foreign body granuloma (gauzoma) found 46 years
under steroids and since DHS developed without taking steroids. after open reduction and fixation surgery for femoral shaft frac-
Chemotherapy was excluded for the long interval between ture
chemotherapy and occurrence of DHS. The most likely cause of DHS
in the presented patient is involvement of the neck extensor mus- Keywords:
Gauzoma
cles in PM, although the clinical picture additionally suggests an Foreign body granuloma
underlying MID. Soft tissue tumor
This case shows that DHS may be a feature of PM and responds
favorable to steroids.
Foreign body granuloma caused by retained surgical gauze
Conflict of interest statement
is synonymously described as gossypiboma, cottonballoma, tex-
There are no conflicts of interest tiloma or gauzoma [1,2]. Such granulomas are rarely in the soft
Letters to the editor / Joint Bone Spine 77 (2010) 482–491 487
in the center of the mass, showing a ring-shaped appearance
[8].
Pathologically, there are two types of foreign body reactions.
One is an aseptic fibrinous reaction that results in adhesion and
encapsulation, with the ultimate formation of a foreign-body gran-
uloma in an otherwise asymptomatic patient. The other variety of
response is an exudative reaction leading to abscess formation or
fluid collection [6,8]. One previous report also described sarcoma-
tous changes in gauzoma after a period of retention exceeding 20
years [2].
Even in the modern era, one should be aware of retained surgi-
cal gauzes at previously operated sites that might cause tumor-like
granuloma with extensive tissue damage in the vicinity of the
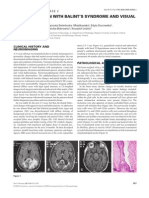
Fig. 1. (a) Anteroposterior radiograph showed bony fusion with deformation after retained material.
femoral shaft fracture and a slightly osteolytic lesion (scalloping) of the left femur
(arrows). (b) A transaxial high-resolution CT following contrast administration
showed a soft tissue mass with low density in the left adductor muscle and erosive Conflict of interest statement
femoral cortical bone without destructive or invasive changes. (c) A T2-weighted
transaxial MR image showed admixture of high- and low-signal mass in the left The authors declare no conflict of interest.
adductor muscle. (d) A T2-weighted sagittal MR image showed a heterogeneous
and high- to low-signal intensity mass in the center of the left thigh. (e) 18 FDG-PET
showed a slightly round ring-like shaped uptake in the medial side of the left thigh. Appendix A. Supplementary material
Supplementary material (Fig. S1) associated with this article can
be found, in the online version, at doi:10.1016/j.jbspin.2010.02.015.
tissues of the musculoskeletal system probably due to the lack of
space available in the regions [3,4]. References
A 66-year-old man noticed a painless soft tissue mass on
the medial side of the left thigh. The past history included [1] Chambi I, Tasker RR, Gentili F, et al. Gauze-induced granuloma (“gauzoma”): an
uncommon complication of gauze reinforcement of berry aneurysms. J Neuro-
open reduction and external traction for a comminuted proximal
surg 1990;72:163–70.
femoral shaft fracture at the age of 20, which were conducted [2] Sakayama K, Fujibuchi T, Sugawara Y, et al. A 40-year-old gossypiboma (foreign
at another hospital. A plain radiograph (Fig. 1a) showed a pic- body granuloma) mimicking a malignant femoral surface tumor. Skeletal Radiol
ture of “deformed union” of the proximal femoral shaft without 2005;34:221–4.
[3] Kominami M, Fujikawa A, Tamura T, et al. Retained surgical sponge in the
bony or cortical erosion or periosteal reaction. A high-resolution thigh: report of the third known case in the limb. Radiat Med 2003;21:
transaxial CT scan (Fig. 1b) showed a low-density round tumor- 220–2.
ous mass without contrast enhancement. MRIs showed the mass [4] Nakamura T, Kusuzaki K, Matsubara T, et al. Foreign-body granulomas in the
trunk and extremities may simulate malignant soft tissue tumors: report of three
was predominantly of low signal intensity on T1-weighted images cases. Acta Radiol 2008;49:80–3.
and admixture of high and low signal intensity on T2-weighted [5] Gawande AA, Studdert DM, Orav EJ, et al. Risk factors for retained instruments
images (Fig. 1c, d). 18 F-fluorodeoxyglucose (FDG)-positron emis- and sponges after surgery. N Engl J Med 2003;348:229–35.
[6] Zbar AP, Agrawal A, Saeed IT, et al. Gossypiboma revisited: a case report and
sion tomography (PET) (Fig. 1e) showed strong FDG uptake at the review of the literature. J R Coll Surg Edinb 1998;43:417–8.
periphery without FDG utilization in the middle portion of the [7] Aydogan M, Mirzanli C, Ganiyusufogle K, et al. A 13-year-old textiloma (gossyp-
mass. iboma) after discectomy for lumbar disc herniation: a case report and review of
the literature. Spine J 2007;7:618–21.
Histopathological examination of an open biopsy excluded
[8] Nakajo M, Jinnouchi S, Tateno R, et al. 18F-FDG PET/CT findings of a right sub-
hematoma, fibromatosis, schwannoma, malignant fibrous phrenic foreign-body granuloma. Ann Nucl Med 2006;20:553–6.
histiocytoma and other malignancies. Marginal excision dis- [9] Lo CP, Hsu CC, Chang TH. Gossypiboma of the leg: MR imaging characteristics. A
case report. Korean J Radiol 2003;4:191–3.
closed the lesion as necrotized granuloma around sheets of
gauze. Histopathological examination (Fig. S1; see the Sup-
plementary Material associated with this article online) Kenzo Uchida
revealed that the mass contained necrotic tissue with a Hideaki Nakajima ∗
mixture of fibrous tissue, lymphocytes, and foreign body Takafumi Yayama
giant cells clustered around barely perceptible foreign mate- Takayuki Hirai
rial. Kebing Chen
Gawande et al. [5] used multivariate analysis to determine the Alexander Rodriguez Guerrero
factors associated with a significantly increased risk of retention of Hisatoshi Baba
a foreign body during surgery. Their results showed that emergency Department of Orthopaedics and Rehabilitation
surgery, unplanned change in the operation, and body-mass index Medicine, Fukui University Faculty of Medical
were significant risk factors [5]. Sciences, Matsuoka-Shimoaizuki 23-3, Eiheiji, Fukui
Retained surgical gauzes could be suspected by ultrasonog- 910-1193, Japan
raphy in the presence of bright echogenic wavy structures in a ∗ Corresponding
cystic mass [6]. On CT scan, the typical feature is a spongiform author. Tel.: +81 776 61 8383;
pattern formed by gas bubbles or an inhomogeneous dense mass, fax: +81 776 61 8125.
low-density mass with a high-density fine capsule containing the E-mail address: nhideaki@u-fukui.ac.jp
contrast material [7,8]. In MR images, the wavy, low-signal inten- (H. Nakajima).
sity stripes seen on T2 weighted image, which represent gauze
fibers, are not apparent in other soft tissue tumors and could 10 February 2010
be characteristic of gauzoma [7,9]. 18 FDG-PET images showed Available online15 May 2010
intense FDG uptake in the hypodense rim and little FDG uptake doi:10.1016/j.jbspin.2010.02.015
You might also like
- Case Report: Characteristics and Treatment Results of 5 Patients With Fibrous Dysplasia and Review of The LiteratureDocument8 pagesCase Report: Characteristics and Treatment Results of 5 Patients With Fibrous Dysplasia and Review of The Literaturesolikin ikinNo ratings yet
- Turaka-2012-Does Fingolimod in Multiple ScleroDocument3 pagesTuraka-2012-Does Fingolimod in Multiple Sclerodr_jrcNo ratings yet
- A 10-Year Old Girl With Neck Pain: Clinical HistoryDocument4 pagesA 10-Year Old Girl With Neck Pain: Clinical HistorywillygopeNo ratings yet
- LED 660nm Celulas Tronco Do Cerebro Cells-10-01664Document15 pagesLED 660nm Celulas Tronco Do Cerebro Cells-10-01664andre.ramosNo ratings yet
- Unusual Intraconal Localization of Orbital Giant Cell AngiofibromaDocument4 pagesUnusual Intraconal Localization of Orbital Giant Cell AngiofibromaKezia TindasNo ratings yet
- 31-Year-Old Man With Balint'S Syndrome and Visual Problems: Clinical History and NeuroimagingDocument4 pages31-Year-Old Man With Balint'S Syndrome and Visual Problems: Clinical History and NeuroimagingwillygopeNo ratings yet
- Magnetic Resonance Imaging - 2023 - Shaikh - Editorial For Preliminary Study of Confounder Corrected Fat Fraction and R2Document2 pagesMagnetic Resonance Imaging - 2023 - Shaikh - Editorial For Preliminary Study of Confounder Corrected Fat Fraction and R2MarcNo ratings yet
- (10920684 - Neurosurgical Focus) Vision Loss After Spine Surgery - Review of The Literature and RecommendationsDocument9 pages(10920684 - Neurosurgical Focus) Vision Loss After Spine Surgery - Review of The Literature and RecommendationsjoshbakhNo ratings yet
- Canine Snake-Eye Myelopathy: Clinical, Magnetic Resonance Imaging, and Pathologic Findings in Four CasesDocument9 pagesCanine Snake-Eye Myelopathy: Clinical, Magnetic Resonance Imaging, and Pathologic Findings in Four CasesAlejandro Estrada RiosNo ratings yet
- Abnormalities of Neuromuscular Transmission in Patients With Miller-Fisher SyndromeDocument3 pagesAbnormalities of Neuromuscular Transmission in Patients With Miller-Fisher SyndromearaliNo ratings yet
- Introduction To Epigenetic Effects and Ionising Radiation Munira KadhimDocument45 pagesIntroduction To Epigenetic Effects and Ionising Radiation Munira KadhimFernando Castro EchavezNo ratings yet
- 0709 Case 2Document4 pages0709 Case 2willygopeNo ratings yet
- 1109 Case 2Document4 pages1109 Case 2willygopeNo ratings yet
- Differential interaction with TREM2 modulates microglial uptake of modified A β speciesDocument16 pagesDifferential interaction with TREM2 modulates microglial uptake of modified A β speciesericNo ratings yet
- Art 21377 PDFDocument12 pagesArt 21377 PDFlubna aloshibiNo ratings yet
- 10.1016/j.pnpbp.2016.11.005: Progress in Neuropsychopharmacology & Biological PsychiatryDocument42 pages10.1016/j.pnpbp.2016.11.005: Progress in Neuropsychopharmacology & Biological PsychiatryGustavo EspíndolaNo ratings yet
- Banwell 2003Document5 pagesBanwell 2003JAVIERA NAVARRETE VIONo ratings yet
- Heterogeneity of T1DM Raises Questions For Therapy: Paolo PozzilliDocument3 pagesHeterogeneity of T1DM Raises Questions For Therapy: Paolo PozzilliHovhannes SahakyanNo ratings yet
- Kebijakan Penggunaan ApronDocument61 pagesKebijakan Penggunaan ApronMeutia sariNo ratings yet
- Microsatellite Plots in SOD-1 Gene With Mutations and Predicted Domains Reveals A Possible Role of MutagenesisDocument6 pagesMicrosatellite Plots in SOD-1 Gene With Mutations and Predicted Domains Reveals A Possible Role of Mutagenesisvamsidhar2008No ratings yet
- Dr. Lakshmi Narayana Malabar Cancer CentreDocument81 pagesDr. Lakshmi Narayana Malabar Cancer Centresherani999No ratings yet
- Akita Inu: Ecvo Manual: Breeds 2017Document3 pagesAkita Inu: Ecvo Manual: Breeds 2017Павел ТопалоNo ratings yet
- Articulometodos 1Document19 pagesArticulometodos 1Sadness NeededNo ratings yet
- Degenerative Cervical Myelopathy: Clinical Presentation, Assessment, and Natural HistoryDocument12 pagesDegenerative Cervical Myelopathy: Clinical Presentation, Assessment, and Natural HistorySurya PangeranNo ratings yet
- A 45-Year Old Male With Left-Sided Hemihypesthesia: Clinical HistoryDocument4 pagesA 45-Year Old Male With Left-Sided Hemihypesthesia: Clinical HistorywillygopeNo ratings yet
- Fnins 14 00705Document11 pagesFnins 14 00705ryahrooNo ratings yet
- Duchenne Muscular Dystrophy - ppt-2010213558Document12 pagesDuchenne Muscular Dystrophy - ppt-2010213558Nadilla De PutriNo ratings yet
- حل اسئلة العملي-1Document91 pagesحل اسئلة العملي-1حسام الوجيهNo ratings yet
- Rheumatology Key MessageDocument3 pagesRheumatology Key MessagePrima YogiNo ratings yet
- Merrick2005 CCDocument11 pagesMerrick2005 CCantoine ailloudNo ratings yet
- Pterigium 4Document2 pagesPterigium 4adnanalikhan72No ratings yet
- GeneticsDocument20 pagesGeneticsAndriNo ratings yet
- 1208 Case 2Document4 pages1208 Case 2willygopeNo ratings yet
- 0909 Case 2Document2 pages0909 Case 2willygopeNo ratings yet
- Fnins 14 00824Document8 pagesFnins 14 00824Guillaume WurtzNo ratings yet
- 2020 - The Fate and Function of Oligodendrocyte Progenitor Cells After Traumatic Spinal Cord InjuryDocument19 pages2020 - The Fate and Function of Oligodendrocyte Progenitor Cells After Traumatic Spinal Cord InjuryMariana NannettiNo ratings yet
- Secondary Syphilis Presenting As Diffused Folliculitis: ReferencesDocument3 pagesSecondary Syphilis Presenting As Diffused Folliculitis: ReferencesNazihan Safitri AlkatiriNo ratings yet
- The Effect of Inflammation On BoneDocument14 pagesThe Effect of Inflammation On BoneKelas CNo ratings yet
- CT and MRI Contrast MediaDocument14 pagesCT and MRI Contrast MediadregleavNo ratings yet
- Bifascicular Block Revealing Steinerts Myotonic DystrophyDocument8 pagesBifascicular Block Revealing Steinerts Myotonic DystrophyIJAR JOURNALNo ratings yet
- Zaman Muscle PathologyDocument14 pagesZaman Muscle PathologyartikslennonNo ratings yet
- Low Laser TherapyDocument2 pagesLow Laser TherapySuzana PoloncaNo ratings yet
- Toronto Study in TBIDocument10 pagesToronto Study in TBICarlos Esteban Lopez GocheNo ratings yet
- Animal Husbandry Congenital Defects of Beef Cattle Breeds and General Principles of Their PreventionDocument5 pagesAnimal Husbandry Congenital Defects of Beef Cattle Breeds and General Principles of Their Preventionrana adnan ejazNo ratings yet
- Management of Degenerative Cervical Disc DiseaseDocument8 pagesManagement of Degenerative Cervical Disc DiseasefromneptuneNo ratings yet
- ElMofty FibroOsseous Lesions of The Craniofacial SkeletonDocument13 pagesElMofty FibroOsseous Lesions of The Craniofacial Skeletonfabiana vasquezNo ratings yet
- Severe Plasmodium Falciparum Malaria Complicated by Acute Myocarditis (Case Report)Document4 pagesSevere Plasmodium Falciparum Malaria Complicated by Acute Myocarditis (Case Report)IJAR JOURNALNo ratings yet
- The Dowager's Hump: An Early Start?: Clinical Section / Short CommunicationDocument4 pagesThe Dowager's Hump: An Early Start?: Clinical Section / Short CommunicationHERNAN PIZARRONo ratings yet
- 2022 Article 1425Document14 pages2022 Article 1425Uma DatarNo ratings yet
- Mammalian Cell Membranes: Volume 2: The Diversity of MembranesFrom EverandMammalian Cell Membranes: Volume 2: The Diversity of MembranesG. A. JamiesonNo ratings yet
- Toxicologic Emergencies, 11th Goldfrank's 2019Document10 pagesToxicologic Emergencies, 11th Goldfrank's 2019RenéNo ratings yet
- Baraitser-Winter CerebrofrontofacialDocument7 pagesBaraitser-Winter Cerebrofrontofacialthaismartins023No ratings yet
- DR. PAUL REGANIT - Nutrition Lecture March 1Document49 pagesDR. PAUL REGANIT - Nutrition Lecture March 1Sophie RoseNo ratings yet
- Novel Mutations HMDocument9 pagesNovel Mutations HMSitipradyta KasimNo ratings yet
- Alzheimer Mechanisms and Therapeutic StrategiesDocument19 pagesAlzheimer Mechanisms and Therapeutic StrategiesArtemis LiNo ratings yet
- R. Ricciarell 2007Document16 pagesR. Ricciarell 2007lucia coronaNo ratings yet
- Mutation of A TADRDocument23 pagesMutation of A TADRbagusdanuhNo ratings yet
- Nephrocalcinosis in CretinismDocument4 pagesNephrocalcinosis in CretinismoccuNo ratings yet
- Lamperti 2010Document10 pagesLamperti 2010Marina GomesNo ratings yet
- Suh 2009Document4 pagesSuh 2009al qurtubi al andalusiNo ratings yet
- Sakayama 2004Document4 pagesSakayama 2004al qurtubi al andalusiNo ratings yet
- WJG 11 4927Document3 pagesWJG 11 4927al qurtubi al andalusiNo ratings yet
- Skeletal GB Mimant SarcomeDocument7 pagesSkeletal GB Mimant Sarcomeal qurtubi al andalusiNo ratings yet
- Mercier 2016Document6 pagesMercier 2016al qurtubi al andalusiNo ratings yet
- Bevernage 2006Document3 pagesBevernage 2006al qurtubi al andalusiNo ratings yet
- Lo 2003Document3 pagesLo 2003al qurtubi al andalusiNo ratings yet
- Hisams Ibraham Evidence For A Canonical Quranic Reading Based On The RasmDocument20 pagesHisams Ibraham Evidence For A Canonical Quranic Reading Based On The Rasmal qurtubi al andalusiNo ratings yet
- Class Notes OrthoDocument7 pagesClass Notes OrthoNikhil junejaNo ratings yet
- Anatomy L4 Gluteal RegionDocument40 pagesAnatomy L4 Gluteal RegionsmhhjjyNo ratings yet
- Femoral Neck FractureDocument19 pagesFemoral Neck FractureTabita P SNo ratings yet
- A New Species of SteneotarsonemusDocument9 pagesA New Species of SteneotarsonemusRodrigo ChangNo ratings yet
- Mrcs Ana 3Document136 pagesMrcs Ana 3Shahriar SakibNo ratings yet
- Intramedullary Nailing For Femur Fracture Web Version EnglishDocument6 pagesIntramedullary Nailing For Femur Fracture Web Version EnglishCarima JatnoNo ratings yet
- Rajesh K Kaushal - Self Assessment and Review of AnatomyDocument1,000 pagesRajesh K Kaushal - Self Assessment and Review of AnatomyRavi Raj100% (1)
- HUMAN BIOmuscles Origin Insertion ActionDocument3 pagesHUMAN BIOmuscles Origin Insertion ActionandrealohrNo ratings yet
- Aaos PDFDocument4 pagesAaos PDFWisnu CahyoNo ratings yet
- BookDocument171 pagesBookdrgouldlibraNo ratings yet
- Vanguard Complete Knee System Design RationaleDocument40 pagesVanguard Complete Knee System Design RationaleLenci MuratiNo ratings yet
- 12 0001736 Rev A - Knee - Truliant Porous Design Rationale - WebDocument12 pages12 0001736 Rev A - Knee - Truliant Porous Design Rationale - WebValaMelkorNo ratings yet
- Hip Syndromes - Shirley SahrmanDocument17 pagesHip Syndromes - Shirley SahrmanSonia LvNo ratings yet
- Mhdpow PDFDocument95 pagesMhdpow PDFGana PathiNo ratings yet
- Treatment of Diaphyseal Femoral Fractures With Ilizarov Frame. Maurizio A. Catagni and Francesco GuerreschiDocument4 pagesTreatment of Diaphyseal Femoral Fractures With Ilizarov Frame. Maurizio A. Catagni and Francesco GuerreschiNuno Craveiro LopesNo ratings yet
- Advanced Orthopaedics - Principles and Techniques-Ruben P. Arafiles, MD (2013)Document235 pagesAdvanced Orthopaedics - Principles and Techniques-Ruben P. Arafiles, MD (2013)Heber Avitia100% (1)
- AO Surgery ReferenceDocument4 pagesAO Surgery Referencemetal_moggleNo ratings yet
- Traction Then and Now: Fran Pearce Education Coordinator Austin HealthDocument42 pagesTraction Then and Now: Fran Pearce Education Coordinator Austin HealthSalman KhanNo ratings yet
- 006 KAFO - Biomechanics LECTURE-1Document23 pages006 KAFO - Biomechanics LECTURE-1Alfred JacksonNo ratings yet
- American Board of Orthopaedic Surgery: Acceptable CPT Codes For Orthopaedic Sports Medicine Subspecialty Case ListDocument13 pagesAmerican Board of Orthopaedic Surgery: Acceptable CPT Codes For Orthopaedic Sports Medicine Subspecialty Case ListKrishna KumarNo ratings yet
- Hip Examination - FinalDocument18 pagesHip Examination - Finalcmonman100% (1)
- Trauma OITE - 2012 2013 2014Document543 pagesTrauma OITE - 2012 2013 2014ICH KhuyNo ratings yet
- Skeletal SystemDocument54 pagesSkeletal Systemanurag.dNo ratings yet
- Z Effect & Reverse Z Effect in PFNDocument7 pagesZ Effect & Reverse Z Effect in PFNNandan SurNo ratings yet
- Implant Related Fractures of The Femur Following.4Document7 pagesImplant Related Fractures of The Femur Following.4ANA MARIA ROCIO HURTADO ORTEGANo ratings yet
- HIP JOINT PresentationDocument16 pagesHIP JOINT PresentationAreeha KhanNo ratings yet
- What Is Femoral Offset - Bone and SpineDocument2 pagesWhat Is Femoral Offset - Bone and SpineChethan K NarayanNo ratings yet
- Pelvis (Summary)Document6 pagesPelvis (Summary)Michaella SangcapNo ratings yet
- Chapmans ReflexesDocument10 pagesChapmans ReflexesNickosteo100% (9)
- Splints and Traction: DR Digvijay Agarwal Assistant ProfessorDocument44 pagesSplints and Traction: DR Digvijay Agarwal Assistant ProfessorMrinali VatsaNo ratings yet