Professional Documents
Culture Documents
Iglay 2007
Uploaded by
壮Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Iglay 2007
Uploaded by
壮Copyright:
Available Formats
Resistance training and dietary protein: effects on glucose tolerance
and contents of skeletal muscle insulin signaling proteins in older
persons1–3
Heidi B Iglay, John P Thyfault, John W Apolzan, and Wayne W Campbell
ABSTRACT Most (7–11), but not all (12, 13), researchers report that resis-
Background: Resistance training (RT) and dietary protein indepen- tance training improves glucose tolerance and insulin action in
dently influence indexes of whole-body glucose control, though older persons. Resistance training decreases fat mass and in-
their synergistic effects have not yet been documented. creases fat-free mass (14, 15); both are associated with positive
Objective: This study assessed the influence of dietary protein changes in the control of blood glucose (16). Although chronic
intake on RT-induced changes in systemic glucose tolerance and the resistance training often improves both body composition and
contents of skeletal muscle insulin signaling proteins in healthy older glucose control (10, 11), an acute bout of resistance training also
persons. improves glucose control (17). This indicates that factors other
Design: Thirty-six older men and women (age: 61 앐 1 y) performed than body composition influence the resistance training–induced
RT (3 times/wk for 12 wk) and consumed either 0.9 g improvement in glucose tolerance (4). Skeletal muscle insulin
protein 䡠 kgҀ1 䡠 dҀ1 [lower-protein (LP) group; 앒112% of the Rec- receptor and Akt contents increased with single leg resistance
ommended Dietary Allowance (RDA)] or 1.2 g protein 䡠 kgҀ1 䡠 dҀ1 training in both healthy and diabetic older men (18), suggesting
[higher-protein (HP) group; 앒150% of the RDA]; the HP group that resistance training positively alters the skeletal muscle in-
consumed more total, egg, and dairy proteins. sulin signaling pathway. To our knowledge, the influence of
Results: After RT, body weight was unchanged; whole-body pro- whole-body resistance training on these variables has not been
tein and water masses increased, and fat mass decreased with no assessed in healthy older men and women.
significantly different responses observed between the LP and HP During a period of resistance training, appropriate energy and
groups. The RT-induced improvement in oral glucose tolerance (de- macronutrient intakes are necessary to promote performance and
creased area under the curve, AUC) was not significantly different body-composition changes (15). Dietary protein requirements
between the groups (LP: Ҁ28%; HP: Ҁ25%). The insulin (Ҁ21%) may increase with physical activity (19), though this has been
and C-peptide (Ҁ14%) AUCs decreased in the LP group but did not documented primarily in athletes. The preferred protein intake
change significantly in the HP group. Skeletal muscle insulin recep- during a resistance training program is currently undefined in
tor, insulin receptor substrate-1, and Akt contents were unchanged, older people, though it would permit maximal fat-free mass gains
and the amount of atypical protein kinase C / (aPKC /), a protein during resistance training. Some (20, 21), but not all (15), re-
involved with insulin signaling, increased 56% with RT, indepen- searchers have reported that protein intake influences resistance
dent of protein intake. training–induced improvement in body composition. A higher
Conclusion: These results support the hypothesis that older persons protein intake during resistance training may enhance improve-
who consume adequate or moderately high amounts of dietary pro- ments in whole-body glucose tolerance and metabolism by
tein can use RT to improve body composition, oral glucose toler- optimizing gains in muscle mass, the primary target of insulin-
ance, and skeletal muscle aPKC / content without a change in body stimulated glucose uptake (22). Chronic high protein intake in
weight. Am J Clin Nutr 2007;85:1005–13. subjects with type 2 diabetes improved glucose tolerance (23) but
is associated with worsened glucose control in healthy subjects
KEY WORDS Protein, diet, resistance training, skeletal mus-
cle insulin signaling, elderly, glucose tolerance 1
From the Department of Foods and Nutrition, Purdue University, West
Lafayette, IN (HBI, JWA, and WWC), and the Departments of Nutritional
Sciences and Internal Medicine, University of Missouri & Harry S Truman
INTRODUCTION
VA Hospital, Columbia, MO (JPT).
2
Even in healthy older adults, glucose tolerance decreases with Supported by the American Egg Board–Egg Nutrition Center. Additional
age (1). This age-associated decrease in glucose tolerance may be support was provided by Agriculture Research Program, Lynn and Bisland
caused by altered body composition (2, 3), decreased physical graduate student fellowships at Purdue University, graduate student support
activity (3, 4), decreased tissue sensitivity to insulin (5), or a funds from Experimental & Applied Sciences, Inc, and Phyllis Izant gift
funds to Purdue University.
combination of these factors. Although 7% of the general Amer- 3
Reprints not available. Address correspondence to WW Campbell, De-
ican population has diabetes, 21% of Americans (10.3 million
partment of Foods and Nutrition, Purdue University, 700 West State Street,
people) aged 욷60 y have diabetes (6). Safe and effective thera- West Lafayette, IN 47907-2059. E-mail: campbellw@purdue.edu.
pies are needed to improve glucose tolerance and decrease the Received September 11, 2006.
risk of developing type 2 diabetes mellitus in older persons. Accepted for publication December 1, 2006.
Am J Clin Nutr 2007;85:1005–13. Printed in USA. © 2007 American Society for Nutrition 1005
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
1006 IGLAY ET AL
(24, 25). Acute protein intake is associated with a minimal rise in were asked to continue habitual medication and supplement use
blood glucose concentration (26), though when consumed to- during the study and agreed not to change this routine or add
gether, protein increases the insulin response to glucose in indi- medications, drugs, or supplements. The subjects were also in-
viduals with type 2 diabetes (27). The disparate results indicate structed to maintain habitual activity levels unrelated to the re-
that this topic should be further studied. sistance training intervention.
The objective of the present study was to determine the influ- At the time of the study design, we were unaware of any
ence of resistance training combined with a lower or higher published research study that had evaluated the combined effects
dietary protein intake on improvements in glucose tolerance in of dietary protein and resistance training on glucose tolerance.
older people. We hypothesized that resistance training would We determined that 36 total subjects—18 subjects in each of the 2
increase the content of skeletal muscle insulin signaling proteins diet groups—was sufficient to test the main effect of time (ie, resis-
and that when compared with consumption of a lower protein tance training) and the group-by-time interaction (ie, differential
diet, resistance training and a higher protein diet would further response of protein intake during resistance training) (7, 29).
improve glucose tolerance.
Exercise intervention
SUBJECTS AND METHODS The subjects were familiarized with the resistance training
equipment and procedures before the intervention. All resistance
Subjects
training sessions were completed in the Exercise Research Fa-
Because older persons are at greater risk for developing im- cility at Purdue University with the use of pneumatic resistance
paired glucose metabolism and tolerance than are young persons exercise equipment (Keiser Sports Health Equipment Company,
(1), we chose to study healthy, older adults. We selected nondi- Fresno, CA). The subjects trained 3 d/wk during weeks 3–14.
abetic subjects rather than diabetic subjects because we wanted Before each exercise session, the subjects completed a preexer-
to focus on prevention or delay of problems in glucose control. cise questionnaire designed to assess their current health and
Fifty men and women from the greater Lafayette, IN, area ability to safely complete a resistance training session. Each
were recruited to participate in the study. Recruitment criteria training session lasted 앒1.25 h and included warm-up and cool-
included the following: 1) age range: 50 – 80 y; 2) body mass down periods and 2 sets of 8 repetitions plus a third set to vol-
index (BMI; in kg/m2) of 20 to 35 (28); 3) nondiabetic and not on untary failure at 80% of the measured 1-repetition maximum for
insulin replacement therapy; 4) clinically normal kidney, liver, 8 exercises. An upper back seated row, leg extension, chest press,
and cardiac functions; 5) not currently using antiinflammatory leg curl, latissimus dorsi pull down, and double leg press were
steroid medications; 6) no hip replacement; 7) no habitual resis- performed during each training session. The shoulder raise and
tance training in the past 6 mo; and 8) women were 욷2 y post- seated calf press were alternated with hip adductor and hip ab-
menopausal. Potential subjects completed a screening evaluation ductor exercises and were performed during every other training
that included a medical history, resting electrocardiogram, rest- session, so that subjects completed 6 primary exercises and 2
ing blood pressure, and routine blood and urine chemistries. The additional exercises for a total of 8 exercises per training session.
subjects were approved by the study physician before starting the All exercises were performed in a slow uniform fashion, giving
protocol. After both written and verbal explanations were pro- equal time to the concentric and eccentric portions (6 – 8 s per
vided, the subjects signed an informed consent agreement. The repetition). The subjects rested for 1 min between sets. On the
Purdue University Institutional Review Board reviewed and ap- third set of each exercise, the subjects exercised until voluntary
proved the informed consent agreement and the study protocol. fatigue, with a maximum of 12 repetitions performed. If the
A monetary stipend was provided to the subjects. subjects reached 12 repetitions, the resistance was increased by
Thirty-six of the fifty subjects completed the study protocol. 5% for that exercise at the next training session.
The timing of dropout and reason for leaving varied among the The training stimulus was periodically adjusted to maintain an
subjects. During baseline measurements, subjects left the study intensity of 80% of maximum strength, as assessed by the
due to the time commitment [n ҃ 3 in the higher-protein (HP) 1-repetition maximum test taken at baseline, twice during inter-
group], a fear of needles [n ҃ 1 in the lower-protein (LP) group], vention, and at the end of the study. Maximum strength was
and unknown reasons (n ҃ 1 in the LP group and 1 in the HP assessed on 5 core pieces of equipment (upper back seated row,
group). During the intervention period, subjects left the study due leg extension, chest press, leg curl, and leg press). A whole-body
to the time commitment (n ҃ 2 in the LP group and 1 in the HP strength summary was calculated as the sum of the 1-repetition
group), a dislike of the study diet (n ҃ 1 in the LP group and 1 in maximum results for these 5 exercises. A moderate resistance
the HP group), and health reasons unrelated to the study (n ҃ 2 training program was used in concurrence with current recom-
in the LP group and 1 in the HP group). mendations for the inclusion of resistance training for healthy
living (8, 30).
Experimental design
The 14-wk protocol was conducted on the Purdue University
campus. The subjects were randomly assigned to 1 of 2 diet Energy expenditure of physical activity
groups based on entry date into the study. Preintervention mea- The Yale Physical Activity Questionnaire was used to assess
surements were taken during weeks 1 and 2, while the subjects the subjects’ average energy expenditure and habitual activity at
continued habitual diet and activity. Dietary protein intake and baseline and the end of the study (31). As calculated in accor-
resistance training intervention followed in weeks 3–14, and dance with this questionnaire, habitual activity is reported in
postintervention measurements were taken during week 14 (di- units per week and reflects a weighted composite of vigorous
etary control and resistance training continued). The subjects activity, walking, moving, sitting, and standing (31).
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
EXERCISE, PROTEIN, AND GLUCOSE TOLERANCE 1007
Dietary intervention 3000 ҂ g (collected in vials containing serum separator and silica
The subjects were instructed to maintain body weight and were clot activator; BD Vacutainer Brand; Benton, Dickinson and Co,
counseled to habitually consume 1 of 2 diets throughout the Franklin Lakes, NJ). Serum samples were separated into plastic
intervention period. The LP group was counseled to consume storage vials and stored frozen at Ҁ80 °C until analysis. To
0.8 g protein 䡠 kgҀ1 䡠 dҀ1, the Recommended Dietary Allow- assess if a diet high in animal proteins altered the lipid profile
ance (RDA) for protein, with egg, striated tissue (beef, poultry, (34), total cholesterol concentrations, HDL-cholesterol concen-
pork, or fish), and dairy proteins as 5%, 25%, and 15% of total trations, and triacylglycerol concentrations were measured, and
protein intake, respectively. The subjects in the HP group were LDL was calculated by COBAS MIRA PLUS as LDL choles-
counseled to consume 1.6 g protein 䡠 kgҀ1 䡠 dҀ1, with egg, stri- terol ҃ total cholesterol – HDL ѿ 0.2 ҂ triacylglycerol (ana-
ated tissue, and dairy proteins as 25%, 20%, and 15% of total lyzed on COBAS Mira Plus; Roche Diagnostic Systems, India-
protein intake, respectively. The higher total protein intake of the napolis, IN). A standard clinical chemistry profile was measured
HP group was achieved via the consumption of larger quantities on one day to assess normative values (blood urea nitrogen,
of egg, striated tissue, and dairy proteins than those the subjects albumin, complete blood count, and electrolytes; analyzed by
in LP group consumed. The subjects in the HP group were coun- Mid America Clinical Laboratories, Indianapolis, IN).
seled to consume a higher percentage of protein from egg than Body-composition assessment
from other proteins because eggs are a readily available high-
quality protein source with a true digestibility score 욷97%. Each To monitor body weight stability, clothed body weight was
individualized diet was designed to provide 1.5 times the basal measured immediately before each exercise session (3 times/
energy requirement, as calculated by sex-specific Harris-Benedict wk). If body weight fluctuated by 쏜2 kg from baseline on 욷3
equations (32). All dietary counseling (verbal and written) was consecutive sessions, the subject’s diet was adjusted accordingly
based on the American Diabetes Association–American Dietetic to encourage a return to and maintenance of baseline body
Association Exchange Lists for Weight Management (33). Written weight. At baseline and the end of the study, whole-body com-
instructions, detailing the number of food exchanges each sub- position was assessed in the fasting state with a 4-compartment
ject was to consume daily, a tracking sheet, guidelines on how to model (fat mass, water mass, protein mass, and mineral mass)
appropriately measure food selections, a list of common serving (35). All measurements were completed within the same morn-
sizes, and a scale to weigh portion sizes were provided. ing. Total body water was measured via the deuterium oxide
Food records collected for 7 consecutive d at baseline (weeks dilution technique (deuterium, 99.9%; Cambridge Isotope Lab-
1–2), at the start of dietary control (weeks 3– 4), middle of dietary oratory, Woburn, MA) (36). All urine was collected before oral
control (weeks 9 –10), and at the end of intervention (weeks consumption of a preweighed amount of deuterium oxide, and 3
13–14) were analyzed for energy and macronutrient content (Nu- timed collections were taken at 2, 3, and 4 h after consumption.
tritionist Pro, N-squared computing; First DataBank version The total volume of each sample was recorded, and aliquots were
1.3.36, San Bruno, CA). Food records that were not returned to stored frozen at Ҁ20 °C for duplicate analysis of deuterium oxide
the study site or were incomplete were excluded from analysis. concentration with the use of an infrared spectrophotometer
Food records were deemed incomplete if the average energy (AVATAR 360 ESP FT-IR Spectrometer System; Thermo Nico-
intake over 7 d was not greater than or equal to the subject’s Harris- let Corporation, Madison, WI). Whole-body bone mineral, fat,
Benedict predicted basal energy requirement. A total of 56 food and lean tissue masses were measured via dual-energy X-ray
records (78% of a possible 72) were included in analysis of dietary absorptiometry (DXA; GE Lunar Prodigy with EnCORE soft-
change from baseline, and a total of 100 food records (69% of a ware version 5.60, Madison, WI) (37). The subjects wore loose
possible 144) were included in analysis of all food records. metal free clothing and remained in a supine position while
scanning was completed. Body weight and whole-body density
Urine analyses were assessed via whole-body plethysmography (BodPod; Life
Measurement Instruments Inc, Concord, CA). The subjects wore
The subjects completed 2 consecutive 24-h urine collections in minimal tight-fitting metal-free clothing and completed tripli-
wk 1, 5, 10, and 14. Total volume was calculated as mass of the cate tests. Tidal lung volume was measured within each test.
entire 24-h sample divided by the average of 3 measurements of Body circumference measurements were taken at the natural
specific gravity (Digital Probe Refractometer; Misco Products waist, umbilicus, and hip (widest girth below natural waist and
Division, Cleveland, OH). Samples were processed, stored fro- umbilicus) with a fiberglass spring tape measure. Height was
zen at Ҁ20 °C, and later analyzed for urinary urea nitrogen (the measured at the beginning of the study with a wall-mounted
primary nitrogenous component of urine) to help assess dietary stadiometer (Holtain Ltd, Crymych, Wales, United Kingdom).
protein intake before, during, and at the end of the period of
intervention and for measurement of urinary creatinine, as a Glucose tolerance assessment
marker of muscle mass (Cobas Mira Plus; Roche Diagnostic The subjects completed an oral-glucose-tolerance test
Systems, Indianapolis, IN). (OGTT) before and after intervention to measure blood glucose,
insulin, and C-peptide responses to drinking a sugar solution that
Blood analyses contained 75 g dextrose. The poststudy OGTT occurred one (n ҃
Fasting-state blood samples were obtained on 2 nonconsecu- 4 in the LP group and 4 in the HP group) to 2 (n ҃ 13 in the LP
tive days at baseline and the end of intervention. Poststudy col- group and 15 in the HP group) d after a resistance training ses-
lection occurred 1–2 d after a resistance training session (12– 48 sion. The day of testing did not affect the results (P 쏜 0.05).
h). Immediately after collection, vials were inverted 7 times, Blood samples were collected at 0, 15, 30, 45, 60, 90, and 120
maintained at room temperature for 45 min to allow clotting, and min (BD Vacutainer Brand; Becton Dickinson and Co). Collec-
then kept on ice until they were centrifuged at 4 °C for 10 min at tion vials contained either lithium heparin (for future glucose and
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
1008 IGLAY ET AL
insulin analyses) or EDTA and aprotinin (for C-peptide analysis; 3-factor ANOVA with time as a repeated measure. The main
85 L aprotinin was added to reduce cleaving, Sigma A-6012 effect of time was considered to be the effect of resistance train-
aprotinin from bovine lung; Sigma-Aldrich Corp, St Louis, MO). ing. Although the study was not powered to test sex differences,
Samples were inverted 7 times and kept on ice until they were certain data are presented within both group and sex. The change
centrifuged at 4 °C for 10 min at 3000 ҂ g. The plasma was from baseline was defined as the postintervention value minus
separated into plastic storage vials and stored frozen at Ҁ80 °C the baseline value. The degree of linear association between the
until further analysis. Samples were analyzed for glucose (oxi- variables of interest was determined by using either the Pearson
dase method; COBAS Mira Plus; Roche Diagnostic Systems) product-moment correlation or the Spearman rho nonparametric
(9), insulin (EIA; ALPCO diagnostics 1–2-3 Human Insulin EIA, ranked correlation, as appropriate. Statistical significance was
Windham, NH), and C-peptide (EIA; ALPCO diagnostics assigned if P 쏝 0.05. Data were not included in analysis if they
C-peptide EIA) concentrations. The 120-min integrated AUC were missing (ie, unable to obtain anthropometric measurements
for glucose, insulin, and C-peptide was determined by using on one subject), outliers (앐3 SDs), or physiologically improba-
the trapezoidal method (38). Hepatic insulin sensitivity and ble (ie, total body water measurement was far too low for 1
whole-body (composite) insulin sensitivity were calculated as subject). Data processing and statistical evaluations were com-
follows (39): pleted by using SPSS version 12.0 for WINDOWS (SPSS Inc,
Chicago, IL).
ISI(HOMA) ⫽ k/(FPI ⫻ FPG) (1)
ISI (composite) ⫽ 10 000/ 冑(FPG ⫻ FPI) ⫻ (G
⫻ Ī) RESULTS
(2) Subjects
where ISI is the insulin sensitivity index, HOMA is the homeo- At baseline, subjects were between 50 and 80 y old (range:
static model assessment, k ҃ 22.5 ҂ 18, FPI is fasting plasma 50 – 80 y for the LP group, 50 –75 y for the HP group) and BMI
insulin (in U/mL), FPG is fasting plasma glucose (in mg/dL), G ranged from 20 to 32 in the LP group and 21 to 35 in the HP group.
is the mean plasma glucose concentration during the OGTT Primary outcome measurements were not significantly different
(mg/dL), and I is the mean plasma insulin concentration during between the groups at baseline (Table 1).
the OGTT (in U/mL).
Fasting blood samples were analyzed for fructosamine (CO- Exercise intervention
BAS Mira Plus; Roche Diagnostic Systems) and glycated hemo- With intervention, composite maximum strength increased
globin (Hb A1c), which are markers of shorter (2–3 wk) and significantly (P 쏝 0.05) in both groups (LP group: 28 앐 4%; HP
longer-term (2–3 mo) glycemic control, respectively (40). group: 34 앐 5%; Table 1). Both habitual activity and average
energy expenditure outside of the laboratory were not signifi-
Skeletal muscle insulin signaling proteins cantly (P 쏜 0.05) changed from baseline (change from baseline:
At baseline and postintervention, a muscle biopsy sample was Ҁ3 앐 5 units/wk, 1215 앐 812 kcal/wk, 앒174 kcal/d in the LP
obtained in the fasting state from the vastus lateralis of the dom- group; Ҁ6 앐 4 units/wk, Ҁ1262 앐 1466 kcal/wk, 앒Ҁ180 kcal/d
inant leg by using a punch biopsy technique (41). Each biopsy in the HP group).
sample was divided into 30 –50-mg pieces and stored in liquid-
nitrogen for later analysis. Muscle was analyzed for changes in Dietary intervention
content of the proteins involved in the insulin signaling pathway, At baseline, as a percentage of average total daily energy
including insulin receptor (IR), insulin receptor substrate 1 (IRS- intake, the subjects’ diets were composed of 34% fat, 50% car-
1), Akt, and atypical protein kinase C / (aPKC /) protein bohydrate (includes 3% alcohol), and 16% protein. The macro-
content with homogenization and Western blotting (42) (all an- nutrient content of average daily intake was not significantly
tibodies purchased from Santa Cruz Biotechnology, Santa Cruz, different between the groups. At baseline and throughout the
CA). Because IR and IRS-1 have not previously been shown to intervention, the men consumed more energy, protein, carbohy-
be influenced by resistance training, a subset of these samples drates, and fat than did the women (data not shown). Protein
were analyzed (n ҃ 20 and 15, respectively) to assess changes. intake changed over time, and the subjects in the HP group
Protein contents of IR or IRS-1 did not significantly change in consumed more protein than did those in the LP group at the end
this subset so further analysis of these proteins was not completed of intervention (Table 2).
because of limited sample size. Western blot images were The average daily protein intake at baseline was 1.1 앐 0.1 g
scanned and band densitometry was assessed with Gel Pro An- protein 䡠 kgҀ1 䡠 dҀ1. An analysis of food records completed dur-
alyzer software (Media Cybernetics, Silver Spring, MD). Band ing the last week of intervention indicated that the subjects in the
density is in arbitrary units. A sample from each group was run LP group consumed 0.9 앐 0.1 g protein 䡠 kgҀ1 䡠 dҀ1 and the
on each blot, and blots were made relative by using a blot average subjects in the HP group consumed 1.2 앐 0.0 g
technique, which divides each band density by the average den- protein 䡠 kgҀ1 䡠 dҀ1 (significant group ҂ time interaction, P 쏝
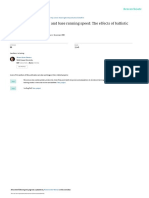
sity of all the bands on the blot. 0.05). Total, egg, and dairy protein intakes were different be-
tween the groups during the intervention (Figure 1). Total meat
Statistical analyses intake did not differ significantly between the groups. Urinary
All data are reported as means 앐 SEMs. Baseline group and urea nitrogen excretion (UUN) during the intervention was
sex differences were assessed with 2-factor analysis of variance higher in the HP group than in the LP group, consistent with the
(ANOVA) and the main effects of time, protein intake and sex, group difference in dietary protein intake (significant group dif-
and their interactions on dependent variables were assessed via ference at postintervention and significant group ҂ resistance
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
EXERCISE, PROTEIN, AND GLUCOSE TOLERANCE 1009
TABLE 1
Characteristics of the subjects in the lower-protein (LP) and higher-protein (HP) groups1
LP group HP group
Baseline After intervention Baseline After intervention
Subjects
Age (y)2 62 앐 2 61 앐 2
BMI (kg/m2)2 25.6 앐 0.8 25.6 앐 0.8 26.7 앐 0.9 26.8 앐 0.9
Exercise intervention
Composite 1RM (kg)3 397 앐 40 500 앐 454 409 앐 37 531 앐 414
Energy expenditure of physical activity (kcal/d)5 958 앐 109 1132 앐 155 1412 앐 189 1232 앐 134
Habitual activity (U)5 57 앐 7 54 앐 6 55 앐 7 50 앐 6
Serum and urine analyses
HDL (mg/dL)6 51 앐 2 51 앐 2 53 앐 3 53 앐 4
LDL (mg/dL)6 117 앐 7 111 앐 74 124 앐 6 120 앐 74
Triacylglycerol (mg/dL)6 111 앐 10 106 앐 11 90 앐 7 96 앐 6
Total cholesterol (mg/dL)6 190 앐 9 182 앐 84 195 앐 7 192 앐 84
Urinary creatinine/body weight (mg 䡠 kgҀ1 䡠 dҀ1)2 10.4 앐 0.6 11.0 앐 0.64 10.6 앐 0.8 12.5 앐 0.84
Urinary urea nitrogen/body weight (mg 䡠 kgҀ1 䡠 dҀ1)2 87.1 앐 5.2 74.0 앐 4.37 88.6 앐 7.4 104.8 앐 7.37,8
Body composition
Body fat (kg)6 26.4 앐 2.2 24.6 앐 2.54 27.0 앐 1.8 25.0 앐 1.94
Body weight (kg)2 74.8 앐 3.6 74.7 앐 3.6 78.2 앐 3.1 78.6 앐 3.2
Hip circumference (cm)9 100.3 앐 1.7 100.0 앐 1.8 101.9 앐 1.6 101.9 앐 1.5
Mineral mass (kg)6 3.4 앐 0.2 3.4 앐 0.2 3.8 앐 0.28 3.8 앐 0.28
Protein mass (kg)6 7.6 앐 0.7 7.8 앐 0.74 8.3 앐 0.6 9.0 앐 0.84
Total body water (L)6 36.4 앐 2.4 37.9 앐 1.94 39.2 앐 2.0 40.1 앐 2.04,8
Waist circumference (cm)9 84.8 앐 2.9 83.5 앐 3.04 84.8 앐 3.1 83.5 앐 2.94
Waist:hip9 0.84 앐 0.02 0.83 앐 0.024 0.83 앐 0.03 0.82 앐 0.024
1
All values are x 앐 SEM. Mineral mass differed significantly between groups at baseline, P 쏝 0.05. No other significant group differences were observed
at baseline, P 쏜 0.05.
2
LP: n ҃ 9 men and 9 women; HP: n ҃ 8 men and 10 women.
3
LP: n ҃ 7 men and 7 women; HP: n ҃ 8 men and 10 women.
4
Significant effect of resistance training, independent of group (P 쏝 0.05).
5
LP: n ҃ 9 men and 9 women; HP: n ҃ 8 men and 9 women.
6
LP: n ҃ 8 men and 9 women; HP: n ҃ 8 men and 10 women.
7
Significant time ҂ group interaction, P 쏝 0.05.
8
Significantly different from LP group at same time point, P 쏝 0.05.
9
LP: n ҃ 9 men and 8 women; HP: n ҃ 7 men and 9 women.
training interactions, P 쏝 0.05 for both; Table 1). Changes in HDL cholesterol and triacylglycerol were not significantly
protein intake and UUN were positively correlated (r ҃ 0.428, P changed (0 앐 1 mg/dL and 0 앐 4 mg/dL, respectively; P 쏜 0.05)
쏝 0.05). with intervention, independent of diet and sex (Table 1).
Blood lipid-lipoprotein profile Body composition
Total and LDL cholesterol decreased (Ҁ5 앐 3 mg/dL and Ҁ6 Body weight remained stable, total body water and protein
앐 2 mg/dL, respectively; P 쏝 0.05, all subjects combined) and mass increased, and fat mass decreased with resistance training,
TABLE 2
Dietary intakes in the lower-protein (LP) and higher-protein (HP) groups1
LP group HP group
Baseline After intervention Baseline After intervention
Energy (kcal/d) 1973 앐 120 2079 앐 137 1956 앐 108 2099 앐 134
Protein (g/d) 80 앐 5 64 앐 42 82 앐 5 88 앐 52,3
Carbohydrate (g/d) 242 앐 18 274 앐 184 228 앐 20 264 앐 234
Fat (g/d) 71 앐 6 78 앐 7 80 앐 5 77 앐 6
Alcohol (g/d) 14 앐 5 13 앐 5 4앐3 4앐2
Dietary fiber (g/d) 21 앐 2 25 앐 24 19 앐 2 22 앐 24
1
All values are x 앐 SEM. LP: n ҃ 8 men and 8 women; HP: n ҃ 3 men and 9 women. The groups did not differ significantly at baseline, P 쏜 0.05.
2
Significant time ҂ group interaction, P 쏝 0.05.
3
Significantly different from LP group at the same time point, P 쏝 0.05.
4
Significant effect of time, independent of group (P 쏝 0.05).
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
1010 IGLAY ET AL
125 DISCUSSION
Protein intake (g/d)
Lower-protein group
100 Higher-protein group The 25–28% decrease in plasma glucose AUC during the
75
OGTT observed after the 12-week period of resistance training
50
25
supports the effectiveness of this mode of exercise to positively
0 impact oral glucose tolerance in older, weight-stable people. This
Total* Other Egg* Meat Dairy* robust response contrasts with previous research that docu-
FIGURE 1. Mean (앐SEM) protein intake from targeted foods during mented that although glucose metabolism improves with resis-
intervention in the lower-protein group (n ҃ 16) and in the higher-protein tance training (8), the glucose response to an OGTT is not im-
group (n ҃ 12). “Other” represents protein from all sources except egg, meat,
and dairy products. *Significant group difference, P 쏝 0.05. proved (9 –11, 38, 43). The resistance training–induced decrease
in glucose AUC during the OGTT in the present study may be
caused by several factors, including an exercise-associated in-
independent of group and sex (Figure 2). Urinary creatinine crease in glucose clearance (44) or an improvement in body
excretion increased significantly (P 쏝 0.05) with intervention composition (16). Because all OGTTs were conducted within
(change from baseline: 0.6 앐 0.2 mg Ucreatinine 䡠 kgҀ1 䡠 dҀ1 in the 48 h of the last exercise session, it is possible that the decrease in
LP group compared with 1.9 앐 0.2 mg Ucreatinine 䡠 kgҀ1 䡠 dҀ1 in glucose AUC and alterations in insulin and C-peptide AUC were
the HP group; Table 1). caused by the recent exercise session and not by chronic training
(8, 44, 45).
Glucose tolerance
Fasting plasma glucose (9), insulin (7, 10, 11), and C-peptide
All OGTTs were completed within 48 h of a resistance training and insulin response to an OGTT (7, 9 –11) have been docu-
session, and the timing of the OGTT (ie, within 24 or 48 h) did not mented to decrease with chronic resistance training, although
significantly influence the results. The glucose AUC in response improvements were not documented with a shorter intervention
to an oral glucose challenge decreased with the intervention, period (4 wk compared with 12 wk). In resistance training pro-
independent of group and sex. Insulin and C-peptide AUC re- grams similar to that of the current study, insulin response to an
sponses were influenced by protein intake during resistance oral glucose challenge decreased by 19% and 33% (9, 43),
training (significant group ҂ resistance training interactions,
whereas glucose (10, 38, 43) and C-peptide (9) responses were
P 쏝 0.05; Figure 3). Both insulin and C-peptide AUCs de-
unchanged after resistance training in older subjects.
creased in the LP group (P 쏝 0.05) but did not significantly
The synergistic effect of protein intake and resistance training
change in the HP group (P 쏜 0.05). Fasting plasma glucose,
insulin, and C-peptide did not significantly change with resis- on glucose tolerance has not been previously studied. Chronic
tance training and were not influenced by protein intake (Figure higher protein intake has been associated with improved glucose
3). No significant changes were observed in fructosamine, metabolism in type 2 diabetics (46) and increased glucose stim-
HbA1c, HOMA, or composite insulin sensitivity with resistance ulated insulin secretion in nondiabetic individuals (25). Other
training or due to diet (P 쏝 0.05; Table 3). researchers have suggested that diet is not independently asso-
ciated with insulin sensitivity or secretion in older women (47).
Skeletal muscle insulin signaling proteins The present findings that insulin and C-peptide responses to the
Analysis of a subset of samples indicated no significant change oral glucose stimulus decreased after resistance training only in
in IR or IRS-1 content with the intervention (n ҃ 15 and 20, the LP group implicates diet as an important factor influencing
respectively). An analysis of all samples (n ҃ 32) indicated that the hormonal control of oral glucose tolerance in conjunction
Akt was not significantly changed and that aPKC / increased with resistance training. How or why this occurred was not mea-
with intervention, independent of group and sex (significant ef- sured within the current study. This difference does not appear to
fect of resistance training, P 쏝 0.05; Table 4). be caused by either body-composition or skeletal muscle insulin
signaling protein contents, because the responses in the LP and
Correlations HP groups were not significantly different. Perhaps the change in
Changes in body composition were not correlated with habitual protein intake (change from baseline: Ҁ0.2 g
changes in glucose, insulin, or C-peptide AUCs during the protein 䡠 kgҀ1 䡠 dҀ1 in the LP group compared with 0.1 g
OGTT or to changes in aPKC / (data not shown). protein 䡠 kgҀ1 䡠 dҀ1 in the HP group) in addition to the actual
level of protein intake influenced glucose tolerance (48), though
this cannot be assessed within the confines of the current project.
4
Lower-protein group Although confirmed by both diet records and UUN (49, 50), the
Higher-protein group relatively small change in protein intake from baseline may have
Change (kg)
2
limited the ability to detect group-specific differences in re-
0 sponse. Interestingly, despite the group difference in insulin and
C-peptide responses, insulin sensitivity as estimated from the
-2 OGTT was not significantly changed. Because average plasma
insulin during the OGTT is the only variable of 4 included in the
-4 composite insulin sensitivity index (39) that was differentially
Whole body Fat* Mineral Protein* Water*
affected by diet, the overall alteration in insulin sensitivity was
FIGURE 2. Changes in body weight and composition during intervention
in the lower-protein group (n ҃ 17) and in the higher-protein group (n ҃ 18). likely too small to detect. The lack of difference in insulin AUC
*
Significant effect of time (ie, resistance training), P 쏝 0.05. responses between the groups at the end of the intervention
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
EXERCISE, PROTEIN, AND GLUCOSE TOLERANCE 1011
10 400
Glucose (mmol/L)
(pmol ·120 min/L)
8 -56 ± 26*
Glucose AUC
300
-54 ± 19*
6
200
4
100
2
0 0
0 30 60 90 120 LP HP
Time (min)
500 60 000
Insulin (pmol/L)
(pmol ·120 min/L)
400 -7164 ± 2922†,‡
Insulin AUC
40 000 3550 ± 3198†
300
200
20 000
100
0 0
0 30 60 90 120 LP HP
Time (min)
(pmol ·120 min/L)
3000 300 000
C-peptide AUC
C-peptide (pmol/L)
-24472 ± 11045†,‡
2000 200 000 13515 ± 9419†
1000 100 000
0 0
0 30 60 90 120 LP HP
Time (min)
FIGURE 3. Glucose, insulin, and C-peptide concentrations and areas under the curve (AUCs) in response to a 75-g oral glucose challenge before and at
the end of intervention in the lower-protein (LP; n ҃ 8 men and 7 women) and higher-protein (HP; n ҃ 8 men and 9 women) groups. Numbers above brackets
indicate the mean (앐SEM) change within each group from baseline measurements. ■, LP group at baseline; 䊐, LP group after intervention; Œ, HP group at
baseline; ‚, HP group after intervention. *Significant effect of time (ie, resistance training, RT) for both groups combined, P 쏝 0.05. †Significant resistance
training ҂ group interaction, P 쏝 0.05. ‡Significant effect of time within a group, P 쏝 0.05.
period provides further caution as to whether the modest differ- and protein mass during weight maintenance suggest that skel-
ences in protein intake achieved in the present study differen- etal muscle mass increased during the study (35). The increase in
tially affected the insulin-mediated control of oral glucose tol- urinary creatinine excretion further supports an increase in skel-
erance. etal muscle mass with resistance training (51). Given that skeletal
Although the improvements in body composition were not muscle is the primary site of glucose uptake (22), this increase in
significantly associated with improvements in glucose tolerance, skeletal muscle mass likely contributed to the improvement in
they may have influenced these changes, because body fat has glucose tolerance (4). The minimal change in fat-free mass (1.2
been shown to predict insulin sensitivity in older people (2). The kg) but large decrease in insulin during the OGTT (1.9% increase
decrease in fat mass combined with increases in total body water in fat-free mass compared with 35% decrease in plasma insulin
TABLE 3
Changes in glycemic control and insulin sensitivity indexes in the lower-protein (LP) and higher-protein (HP) groups after 12 wk of progressive resistance
training1
LP group HP group
Baseline Change Baseline Change
Fructosamine (mol/L) 2
222 앐 4 Ҁ5 앐 3 231 앐 2 Ҁ1 앐 3
Hb A1c (%)3 5.1 앐 0.1 0.0 앐 0.0 5.3 앐 0.1 0.0 앐 0.0
ISI composite (dL2/mg2)3,4 8.9 앐 2.0 1.1 앐 0.7 9.8 앐 1.6 Ҁ0.2 앐 1.3
HOMA (dL2/mg2)3,5 1.2 앐 0.2 0.0 앐 0.1 1.4 앐 0.2 0.2 앐 0.1
1
All values are x 앐 SEM. The groups did not differ significantly at baseline, P 쏜 0.05. ISI, insulin sensitivity index; Hb A1c, glycated hemoglobin; HOMA,
homeostatic model assessment.
2
LP: n ҃ 7 men and 7 women; HP: n ҃ 8 men and 9 women.
3
LP: n ҃ 8 men and 7 women; HP: n ҃ 8 men and 9 women.
4
Whole-body insulin sensitivity.
5
Hepatic insulin sensitivity.
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
1012 IGLAY ET AL
TABLE 4 In conclusion, these data indicate that 12 wk of progressive
Skeletal muscle insulin signaling protein content in the lower-protein (LP) resistance training is an effective stimulus for older, weight-
and higher-protein (HP) groups1 stable persons to achieve an improvement in oral glucose toler-
LP group HP group ance. The unchanged compared with decreased insulin and
C-peptide responses in the HP and LP groups, respectively, after
After After the ingestion of glucose suggests that dietary protein intake in-
Baseline intervention Baseline intervention fluences how the improvement in glucose control was achieved.
IR2 0.90 앐 0.19 1.08 앐 0.21 1.09 앐 0.14 0.97 앐 0.18 Results from the present study also showed that resistance train-
IRS-13 1.10 앐 0.27 1.32 앐 0.19 0.97 앐 0.18 0.77 앐 0.19 ing increases skeletal muscle aPKC / content, a newly emerg-
Akt4 0.90 앐 0.09 0.92 앐 0.08 0.92 앐 0.07 1.09 앐 0.09 ing component of the insulin signaling pathway.
aPKC4 0.69 앐 0.09 0.98 앐 0.115 0.73 앐 0.11 1.23 앐 0.155
We thank the volunteers for their time and dedication to the project. We
1
All values are x 앐 SEM. IR, insulin receptor; IRS-1, IR substrate 1; thank WWC’s Nutrition, Fitness, and Aging research staff for their assistance
aPKC, atypical protein kinase C zeta/lambda (/). The groups did not differ as well.
significantly at baseline, P 쏜 0.05. HBI and WWC conceived and designed the experiment. HBI, JWA, and
2
LP: n ҃ 5 men and 4 women; HP: n ҃ 5 men and 6 women. WWC conducted the clinical portion of this study. HBI, JPT, JWA,
3
LP: n ҃ 3 men and 4 women; HP: n ҃ 4 men and 4 women. and WWC participated in sample analysis and data processing. HBI, JPT, and
4
LP: n ҃ 7 men and 7 women; HP: n ҃ 7 men and 8 women. WWC were involved in data interpretation. HBI, JPT, and WWC wrote the
5
Significant effect of time (ie, resistance training), independent of manuscript. None of the authors had any personal or financial conflicts of
group (P 쏝 0.05). interest.
REFERENCES
during the OGTT) previously documented after 16 wk of resis- 1. DeFronzo RA. Glucose intolerance and aging. Diabetes Care 1981;4:
tance training (10) suggests that it is not just a mass effect, but that 493–501.
skeletal muscle is more insulin sensitive after resistance training. 2. Boden G, Chen X, DeSantis RA, Kendrick Z. Effects of age and body fat
Resistance training improves insulin signaling in muscle from on insulin resistance in healthy men. Diabetes Care 1993;16:728 –33.
rodent models but has not been investigated in human models 3. Coon PJ, Rogus EM, Drinkwater D, Muller DC, Goldberg AP. Role of
body fat distribution in the decline in insulin sensitivity and glucose
(52). Because we performed OGTT measurements, we were tolerance with age. J Clin Endocrinol Metab 1992;75:1125–32.
unable to measure the stimulation of the insulin signaling cas- 4. Ryan AS. Insulin resistance with aging: effects of diet and exercise.
cade; however, we did measure the skeletal muscle content of IR, Sports Med 2000;30:327– 46.
IRS-1, Akt, and aPKC /, which play important roles in the 5. Pagano G, Cassader M, Cavallo-Perin P, et al. Insulin resistance in the
aged: a quantitative evaluation of in vivo insulin sensitivity and in vitro
insulin activation of glucose transport. Previous research has glucose transport. Metabolism 1984;33:976 – 81.
indicated that aerobic (53, 54) and resistance (18, 55) training 6. American Diabetes Association. Total prevalence of diabetes & pre-
increase the skeletal muscle content of insulin signaling proteins, diabetes. 2005. Internet: http://www.diabetes.org/diabetes-statistics/
though research in older persons is limited. To our knowledge, prevalence.jsp (accessed 15 November 2005).
only one study has documented an increase in skeletal muscle 7. Hurlbut DE, Lott ME, Ryan AS, et al. Does age, sex, or ACE genotype
affect glucose and insulin responses to strength training? J Appl Physiol
insulin signaling proteins (IR, Akt ␣/, glycogen synthase, and 2002;92:643–50.
glycogen synthase activity) with resistance training in older per- 8. Albright A, Franz M, Hornsby G, et al. American College of Sports
sons, though resistance training was limited to one-legged exer- Medicine position stand. Exercise and type 2 diabetes. Med Sci Sports
cise and the subjects were all men (18). One recent study in both Exerc 2000;32:1345– 60.
9. Joseph LJ, Farrell PA, Davey SL, Evans WJ, Campbell WW. Effect of
diabetic and nondiabetic individuals found that endurance train-
resistance training with or without chromium picolinate supplementa-
ing caused an increase in GLUT4 protein content and Akt ex- tion on glucose metabolism in older men and women. Metabolism 1999;
pression in both diabetic and nondiabetic individuals but that 48:546 –53.
IRS-1 and PI3-kinase were unaffected (54). The authors sug- 10. Miller JP, Pratley RE, Goldberg AP, et al. Strength training increases
gested that exercise improves insulin-stimulated glucose dis- insulin action in healthy 50- to 65-yr-old men. J Appl Physiol 1994;77:
1122–7.
posal by increasing skeletal muscle GLUT4 expression and does 11. Miller WJ, Sherman WM, Ivy JL. Effect of strength training on glucose
not influence the proximal signaling pathway (54). Similarly, in tolerance and post-glucose insulin response. Med Sci Sports Exerc 1984;
the subset of samples analyzed for IR and IRS-1, we found no 16:539 – 43.
significant change with resistance training, suggesting that re- 12. Ryan AS, Hurlbut DE, Lott ME, et al. Insulin action after resistive
sistance training does not influence this portion of the insulin training in insulin resistant older men and women. J Am Geriatr Soc
2001;49:247–53.
signaling pathway. However, we did find a robust increase in 13. Joseph LJ, Trappe TA, Farrell PA, et al. Short-term moderate weight loss
aPKC / content after resistance training, which has not been and resistance training do not affect insulin-stimulated glucose disposal
shown before. Atypical PKC / has recently emerged as an in postmenopausal women. Diabetes Care 2001;24:1863–9.
integral component of insulin signaling to glucose transport (56). 14. Hunter GR, McCarthy JP, Bamman MM. Effects of resistance training
on older adults. Sports Med 2004;34:329 – 48.
Furthermore, aPKC / content is reduced in skeletal muscle of 15. Campbell WW, Crim MC, Young VR, Evans WJ. Increased energy
humans with obesity and type 2 diabetes (57). An increase in requirements and changes in body composition with resistance training
aPKC / protein content appears to occur only after chronic in older adults. Am J Clin Nutr 1994;60:167–75.
resistance training; a previous study showed no difference in 16. Kahn SE, Schwartz RS, Porte D Jr, Abrass IB. The glucose intolerance
aPKC / content between endurance trained and sedentary in- of aging. Implications for intervention. Hosp Pract (Off Ed) 1991;26:
29 –38.
dividuals (58). Interestingly, aPKC / may also play a role in 17. King DS, Feltmeyer TL, Baldus PJ, Sharp RL, Nespor J. Effects of
protein synthesis pathways, because it has been shown to asso- eccentric exercise on insulin secretion and action in humans. J Appl
ciate with p70S6k, a key protein in muscle hypertrophy (59). Physiol 1993;75:2151– 6.
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
EXERCISE, PROTEIN, AND GLUCOSE TOLERANCE 1013
18. Holten MK, Zacho M, Gaster M, Juel C, Wojtaszewski JF, Dela F. 40. Osei K, Rhinesmith S, Gaillard T, Schuster D. Is glycosylated hemoglo-
Strength training increases insulin-mediated glucose uptake, GLUT4 bin A1c a surrogate for metabolic syndrome in nondiabetic, first-degree
content, and insulin signaling in skeletal muscle in patients with type 2 relatives of African-American patients with type 2 diabetes? J Clin
diabetes. Diabetes 2004;53:294 –305. Endocrinol Metab 2003;88:4596 – 601.
19. Lemon PW. Effects of exercise on dietary protein requirements. Int 41. Evans WJ, Phinney SD, Young VR. Suction applied to a muscle biopsy
J Sport Nutr 1998;8:426 – 47. maximizes sample size. Med Sci Sports Exerc 1982;14:101–2.
20. Campbell WW, Trappe TA, Jozsi AC, Kruskall LJ, Wolfe RR, Evans 42. Passonneau JV, Lauderdale VR. A comparison of three methods of
WJ. Dietary protein adequacy and lower body versus whole body resis- glycogen measurement in tissues. Anal Biochem 1974;60:405–12.
tive training in older humans. J Physiol 2002;542:631– 42. 43. Craig BW, Everhart J, Brown R. The influence of high-resistance train-
21. Campbell WW, Barton ML Jr, Cyr-Campbell D, et al. Effects of an ing on glucose tolerance in young and elderly subjects. Mech Aging Dev
omnivorous diet compared with a lactoovovegetarian diet on resistance- 1989;49:147–57.
training-induced changes in body composition and skeletal muscle in 44. Schneider SH, Amorosa LF, Khachadurian AK, Ruderman NB. Stud-
older men. Am J Clin Nutr 1999;70:1032–9. ies on the mechanism of improved glucose control during regular
22. Elahi D, Muller DC. Carbohydrate metabolism in the elderly. Eur J Clin exercise in type 2 (non-insulin-dependent) diabetes. Diabetologia
Nutr 2000;54(suppl):S112–20.
1984;26:355– 60.
23. Gannon MC, Nuttall FQ, Saeed A, Jordan K, Hoover H. An increase in
45. Goulet ED, Melancon MO, Dionne IJ, Leheudre MA. No sustained
dietary protein improves the blood glucose response in persons with type
effect of aerobic or resistance training on insulin sensitivity in nonobese,
2 diabetes. Am J Clin Nutr 2003;78:734 – 41.
24. Linn T, Geyer R, Prassek S, Laube H. Effect of dietary protein intake on healthy older women. J Aging Phys Act 2005;13:314 –26.
insulin secretion and glucose metabolism in insulin-dependent diabetes 46. Gannon MC, Nuttall FQ. Effect of a high-protein, low-carbohydrate diet
mellitus. J Clin Endocrinol Metab 1996;81:3938 – 43. on blood glucose control in people with type 2 diabetes. Diabetes 2004;
25. Linn T, Santosa B, Gronemeyer D, et al. Effect of long-term dietary 53:2375– 82.
protein intake on glucose metabolism in humans. Diabetologia 2000;43: 47. Larsson H, Elmstahl S, Berglund G, Ahren B. Habitual dietary intake
1257– 65. versus glucose tolerance, insulin sensitivity and insulin secretion in
26. Franz MJ. Protein: metabolism and effect on blood glucose levels. Di- postmenopausal women. J Intern Med 1999;245:581–91.
abetes Educ 1997;23:643– 6, 648, 650 –1. 48. Wolever TM, Hamad S, Gittelsohn J, et al. Low dietary fiber and high
27. Nuttall FQ, Mooradian AD, Gannon MC, Billington C, Krezowski P. protein intakes associated with newly diagnosed diabetes in a remote
Effect of protein ingestion on the glucose and insulin response to a aboriginal community. Am J Clin Nutr 1997;66:1470 – 4.
standardized oral glucose load. Diabetes Care 1984;7:465–70. 49. Isaksson B. Urinary nitrogen output as a validity test in dietary surveys.
28. Medicine ACoS. ACSM’s guidelines for exercise testing and prescrip- Am J Clin Nutr 1980;33:4 –5.
tion. 7th ed. Philadelphia, PA: Lippincott Williams & Wilkons, 2006. 50. Bingham SA, Williams R, Cole TJ, Price CP, Cummings JH. Reference
29. Farnsworth E, Luscombe ND, Noakes M, Wittert G, Argyiou E, Clifton values for analytes of 24-h urine collections known to be complete. Ann
PM. Effect of a high-protein, energy-restricted diet on body composi- Clin Biochem 1988;25:610 –9.
tion, glycemic control, and lipid concentrations in overweight and obese 51. Heymsfield SB, Arteaga C, McManus C, Smith J, Moffitt S. Measure-
hyperinsulinemic men and women. Am J Clin Nutr 2003;78:31–9. ment of muscle mass in humans: validity of the 24-hour urinary creati-
30. USDA. United States Department of Agriculture: Dietary Guidelines for nine method. Am J Clin Nutr 1983;37:478 –94.
Americans, 2005. 52. Krisan AD, Collins DE, Crain AM, et al. Resistance training enhances
31. Dipietro L, Caspersen CJ, Ostfeld AM, Nadel ER. A survey for assessing components of the insulin signaling cascade in normal and high-fat-fed
physical activity among older adults. Med Sci Sports Exerc 1993;25: rodent skeletal muscle. J Appl Physiol 2004;96:1691–700.
628 – 42. 53. Cox JH, Cortright RN, Dohm GL, Houmard JA. Effect of aging on
32. Harris JA, Benedict FG. A biometric study of human basal metabolism. response to exercise training in humans: skeletal muscle GLUT-4 and
Proc Natl Acad Sci U S A 1918;4:370 –3. insulin sensitivity. J Appl Physiol 1999;86:2019 –25.
33. American Diabetes Association and the American Dietetic Association. 54. Christ-Roberts CY, Pratipanawatr T, Pratipanawatr W, et al. Exercise
Exchange lists meal planning. Arlington, VA and Chicago, IL: American
training increases glycogen synthase activity and GLUT4 expression but
Diabetes Association and American Dietetic Association, 2003.
not insulin signaling in overweight nondiabetic and type 2 diabetic
34. Weggemans RM, Zock PL, Katan MB. Dietary cholesterol from eggs
subjects. Metabolism 2004;53:1233– 42.
increases the ratio of total cholesterol to high-density lipoprotein cho-
55. Tabata I, Suzuki Y, Fukunaga T, Yokozeki T, Akima H, Funato K.
lesterol in humans: a meta-analysis. Am J Clin Nutr 2001;73:885–91.
35. Baumgartner RN, Heymsfield SB, Lichtman S, Wang J, Pierson RN Jr. Resistance training affects GLUT-4 content in skeletal muscle of
Body composition in elderly people: effect of criterion estimates on humans after 19 days of head-down bed rest. J Appl Physiol 1999;
predictive equations. Am J Clin Nutr 1991;53:1345–53. 86:909 –14.
36. Lukaski HC, Johnson PE. A simple, inexpensive method of determining 56. Farese RV. Function and dysfunction of aPKC isoforms for glucose
total body water using a tracer dose of D2O and infrared absorption of transport in insulin-sensitive and insulin-resistant states. Am J Physiol
biological fluids. Am J Clin Nutr 1985;41:363–70. Endocrinol Metab 2002;283:E1–11.
37. Bolanowski M, Nilsson BE. Assessment of human body composition 57. Kim YB, Kotani K, Ciaraldi TP, Henry RR, Kahn BB. Insulin-stimulated
using dual-energy x-ray absorptiometry and bioelectrical impedance protein kinase C lambda/zeta activity is reduced in skeletal muscle of
analysis. Med Sci Monit 2001;7:1029 –33. humans with obesity and type 2 diabetes: reversal with weight reduction.
38. Fluckey JD, Hickey MS, Brambrink JK, Hart KK, Alexander K, Craig Diabetes 2003;52:1935– 42.
BW. Effects of resistance exercise on glucose tolerance in normal and 58. Nielsen JN, Frosig C, Sajan MP, et al. Increased atypical PKC activity in
glucose-intolerant subjects. J Appl Physiol 1994;77:1087–92. endurance-trained human skeletal muscle. Biochem Biophys Res Com-
39. Matsuda M, DeFronzo RA. Insulin sensitivity indices obtained from oral mun 2003;312:1147–53.
glucose tolerance testing: comparison with the euglycemic insulin 59. Hirai T, Chida K. Protein kinase Czeta (PKCzeta): activation mecha-
clamp. Diabetes Care 1999;22:1462–70. nisms and cellular functions. J Biochem (Tokyo) 2003;133:1–7.
Downloaded from https://academic.oup.com/ajcn/article-abstract/85/4/1005/4648965
by guest
on 05 June 2018
You might also like
- Devitt AA Et Al. J Diabetes Res Clin Metab. 2012 1 20Document9 pagesDevitt AA Et Al. J Diabetes Res Clin Metab. 2012 1 20Teresa100% (1)
- NICE Gestational Diabetes - 2021Document10 pagesNICE Gestational Diabetes - 2021Sajedah MahdiNo ratings yet
- Nutrition Through The Life Cycle 6th Edition Brown Solutions Manual 1Document10 pagesNutrition Through The Life Cycle 6th Edition Brown Solutions Manual 1matthew100% (55)
- Calorie Restriction With or Without Exercise On Insulin Sensitivity Beta Cell Functions Ectopic LipidDocument8 pagesCalorie Restriction With or Without Exercise On Insulin Sensitivity Beta Cell Functions Ectopic Lipidadibahfauzi85No ratings yet
- 2015 AjcnDocument8 pages2015 Ajcnseb2008No ratings yet
- Sự Gia Tăng Protein Trong Chế Độ Ăn Uống Giúp Cải Thiện Phản Ứng Đường Huyết ở Những Người Mắc Bệnh Tiểu Đường Loại 2Document8 pagesSự Gia Tăng Protein Trong Chế Độ Ăn Uống Giúp Cải Thiện Phản Ứng Đường Huyết ở Những Người Mắc Bệnh Tiểu Đường Loại 2Cao Phát ĐạtNo ratings yet
- Jur EngDocument8 pagesJur Engmeiimei meilienhaNo ratings yet
- Verreijen Et Al, 2017 - BIOACTIVE PROTEINDocument8 pagesVerreijen Et Al, 2017 - BIOACTIVE PROTEINAini MahmudahNo ratings yet
- Dietary Fat Modifies The Effects of FTO Genotype On Changes in Insulin Sensitivity.Document6 pagesDietary Fat Modifies The Effects of FTO Genotype On Changes in Insulin Sensitivity.Christian Jovanni Flores SolisNo ratings yet
- Two larger meals more effective than six smaller meals for type 2 diabetesDocument9 pagesTwo larger meals more effective than six smaller meals for type 2 diabetesHayna VieiraNo ratings yet
- The Effects of Fat and Protein on Glycemic ResponsesDocument6 pagesThe Effects of Fat and Protein on Glycemic ResponsesRavi kumarNo ratings yet
- Dietary Protein Effect On Body CompositionDocument8 pagesDietary Protein Effect On Body CompositionAllisa RufaedahNo ratings yet
- Rol Van Voedingsinterventie Bij CachexieDocument6 pagesRol Van Voedingsinterventie Bij CachexieKarunia Putri AmaliaNo ratings yet
- JCSM 12 2022Document12 pagesJCSM 12 2022Henrique OtavioNo ratings yet
- Gosby2013 - Protein Leverage and Energy IntakeDocument9 pagesGosby2013 - Protein Leverage and Energy IntakeDiego TenorioNo ratings yet
- 879 FullDocument7 pages879 FullAhsan Tanio DaulayNo ratings yet
- Neuhouser 2011Document6 pagesNeuhouser 2011Luii GomezNo ratings yet
- Proteina Peq Almoço Am J Clin Nutr-2013-Leidy-677-88Document12 pagesProteina Peq Almoço Am J Clin Nutr-2013-Leidy-677-88Daniee06No ratings yet
- The Effect of Breakfast vs Fasting on Energy Balance and Health in Obese AdultsDocument10 pagesThe Effect of Breakfast vs Fasting on Energy Balance and Health in Obese AdultsRizky LumalessilNo ratings yet
- SatietyDocument9 pagesSatietyfindasiftidewi_86391No ratings yet
- Effects of Exercise Modality On Insulin Resistance and Ectopic Fat in Adolescents With Overweight and Obesity A Randomized Clinical Trial - PMCDocument19 pagesEffects of Exercise Modality On Insulin Resistance and Ectopic Fat in Adolescents With Overweight and Obesity A Randomized Clinical Trial - PMCKevin TorresNo ratings yet
- hevia-larraín2021 (1)Document14 pageshevia-larraín2021 (1)Lucas Contreras RadaNo ratings yet
- DANTAS 2020 Exercise-Induced Increases in Insulin Sensitivity After Bariatric Surgery Are Mediated by Muscle Extracellular Matrix RemodelingDocument17 pagesDANTAS 2020 Exercise-Induced Increases in Insulin Sensitivity After Bariatric Surgery Are Mediated by Muscle Extracellular Matrix RemodelingCris AquinoNo ratings yet
- ARTIGO - Ovos e Risco CardiovascularDocument9 pagesARTIGO - Ovos e Risco Cardiovascularpaolla_ryenneNo ratings yet
- Physical Fitness and Vegetarian Diets: Is There A Relation?: David C NiemanDocument6 pagesPhysical Fitness and Vegetarian Diets: Is There A Relation?: David C Niemanyusi indiatiNo ratings yet
- Am J Clin Nutr 2008 Paddon Jones 1562S 6SDocument5 pagesAm J Clin Nutr 2008 Paddon Jones 1562S 6ScintaNo ratings yet
- 1602350a pdf751186925Document6 pages1602350a pdf751186925Nutricionista Nixa RamírezNo ratings yet
- 6 Carbohydrate Intake and ObesityDocument25 pages6 Carbohydrate Intake and ObesitymariaNo ratings yet
- Appetitive Dietary and Health Effects of Almonds CDocument10 pagesAppetitive Dietary and Health Effects of Almonds CPaula GarateNo ratings yet
- Case study 1.2. Experimental studyDocument8 pagesCase study 1.2. Experimental studyvulediemkhanhNo ratings yet
- Research Article: The Effect of Oral Leucine On Protein Metabolism in Adolescents With Type 1 Diabetes MellitusDocument6 pagesResearch Article: The Effect of Oral Leucine On Protein Metabolism in Adolescents With Type 1 Diabetes MellitushartithpNo ratings yet
- Art 3A10.1186 2Fs40795 017 0152 4Document9 pagesArt 3A10.1186 2Fs40795 017 0152 4NurfadhilahNo ratings yet
- Arad Et Al., 2015Document11 pagesArad Et Al., 2015Irene Chrysovalanto ThemistocleousNo ratings yet
- A Lower-Carbohydrate, Higher-Fat Diet Reduces Abdominal and Intermuscular Fat and Increases Insulin Sensitivity in Adults at Risk of Type 2 DiabetesDocument7 pagesA Lower-Carbohydrate, Higher-Fat Diet Reduces Abdominal and Intermuscular Fat and Increases Insulin Sensitivity in Adults at Risk of Type 2 DiabetesAureliaIstiQomahNo ratings yet
- JN 254532Document10 pagesJN 254532Conciencia CristalinaNo ratings yet
- 1 s2.0 S0002916522004385 MainDocument11 pages1 s2.0 S0002916522004385 Maincarlos santamariaNo ratings yet
- Mccann2015 Chori BarDocument15 pagesMccann2015 Chori BarMarko BrzakNo ratings yet
- Increased Consumption of Dairy Foods and Protein During Diet - and Exercise-Induced Weight Loss Promotes Fat Mass Loss and Lean Mass Gain in Overweight and Obese Premenopausal WomenDocument9 pagesIncreased Consumption of Dairy Foods and Protein During Diet - and Exercise-Induced Weight Loss Promotes Fat Mass Loss and Lean Mass Gain in Overweight and Obese Premenopausal Womenines.queiros.nutricionistaNo ratings yet
- Protein Supplement - Pros and Cons ReviewDocument8 pagesProtein Supplement - Pros and Cons Reviewleul amlekeNo ratings yet
- Clinical Nutrition: Randomized Control TrialsDocument7 pagesClinical Nutrition: Randomized Control Trialsteuku fahrilNo ratings yet
- Nqy 192Document17 pagesNqy 192Helena RahmaraniNo ratings yet
- Nxy 263Document10 pagesNxy 263Conciencia CristalinaNo ratings yet
- Nutrients 15 00332 v2Document17 pagesNutrients 15 00332 v2koehler.thereseNo ratings yet
- Enteral Nutrition in The Critically Ill Myths And.24Document8 pagesEnteral Nutrition in The Critically Ill Myths And.24adinacomNo ratings yet
- Nutrients 16 00419 v2Document22 pagesNutrients 16 00419 v2ela.sofiaNo ratings yet
- Effect of Diets Enriched in Almonds On Insulin Action and Serum Lipids in Adults With Normal Glucose Tolerance or Type 2 DiabetesDocument7 pagesEffect of Diets Enriched in Almonds On Insulin Action and Serum Lipids in Adults With Normal Glucose Tolerance or Type 2 DiabetesLyly SelenaNo ratings yet
- Jurnal FisikaDocument7 pagesJurnal FisikaKezia HanaraNo ratings yet
- 2 Year Paleo TrialDocument8 pages2 Year Paleo TrialOfer KulkaNo ratings yet
- Effects of A High-Protein Ketogenic Diet On Hunger, Appetite, and Weight Loss in Obese Men Feeding Ad Libitum-Am J Clin Nutr-2008-Johnstone-44-55Document12 pagesEffects of A High-Protein Ketogenic Diet On Hunger, Appetite, and Weight Loss in Obese Men Feeding Ad Libitum-Am J Clin Nutr-2008-Johnstone-44-55Ivonne BarrazaNo ratings yet
- Aging V14i1 203821Document15 pagesAging V14i1 203821DAINER ERNESTO MONTOYA LENISNo ratings yet
- Evidencia Científica de Dietas para Bajar de Peso Diferente Composición de Macronutrientes, Ayuno Intermitente y Dietas PopularesDocument35 pagesEvidencia Científica de Dietas para Bajar de Peso Diferente Composición de Macronutrientes, Ayuno Intermitente y Dietas PopularesCesar Flores ValleNo ratings yet
- Fructose increases visceral fat and lipids more than glucoseDocument13 pagesFructose increases visceral fat and lipids more than glucoseNur Ahmad HabibiNo ratings yet
- Cocca 29 101Document7 pagesCocca 29 101Rasime Sevgi CenanNo ratings yet
- A Ingestão de Proteína e Exercício para A Função Muscular IdealDocument8 pagesA Ingestão de Proteína e Exercício para A Função Muscular IdealCinthia Domingos BarbosaNo ratings yet
- Artigo - Metabolic ImpactsDocument11 pagesArtigo - Metabolic ImpactsRaissa Porta da Cruz RaissaNo ratings yet
- Plasma Ghrelin LevelDocument8 pagesPlasma Ghrelin Levelmilenerato2240No ratings yet
- Effect of A High-Protein Diet On Maintenance of Blood Pressure Levels Achieved After Initial Weight Loss: The Diogenes Randomized StudyDocument6 pagesEffect of A High-Protein Diet On Maintenance of Blood Pressure Levels Achieved After Initial Weight Loss: The Diogenes Randomized StudyDevi C'chabii ChabiiNo ratings yet
- Intermittent Fasting Promotes Adipose Thermogenesis and Metabolic Homeostasis Via VEGF-mediated Alternative Activation of MacrophageDocument18 pagesIntermittent Fasting Promotes Adipose Thermogenesis and Metabolic Homeostasis Via VEGF-mediated Alternative Activation of MacrophageNathália CristimannNo ratings yet
- Diabetes MellitusDocument8 pagesDiabetes Mellitusi_anitaNo ratings yet
- Los Carbohidratos No Digeribles Afectan La Salud Metabólica y La Microbiota Intestinal en Adultos Con Sobrepeso Después de La Pérdida de PesoDocument12 pagesLos Carbohidratos No Digeribles Afectan La Salud Metabólica y La Microbiota Intestinal en Adultos Con Sobrepeso Después de La Pérdida de PesoOrihuela Iparraguirre JuanaNo ratings yet
- Imun 2Document12 pagesImun 2kadekapiklestariNo ratings yet
- 107 Jls s4 109 Heidar Comparing PDocument8 pages107 Jls s4 109 Heidar Comparing P壮No ratings yet
- Research ArticleDocument11 pagesResearch Article壮No ratings yet
- A Comparison of The Kinematics, Kinetics and Muscle Activity Between Pneumatic and Free Weight ResistanceDocument20 pagesA Comparison of The Kinematics, Kinetics and Muscle Activity Between Pneumatic and Free Weight Resistance壮No ratings yet
- Research Article Prevention of Physical Risk and Rehabilitation of Muscle Injury in Sanda CompetitionDocument9 pagesResearch Article Prevention of Physical Risk and Rehabilitation of Muscle Injury in Sanda Competition壮No ratings yet
- Research Article Multimedia Based Medical Big Data Analysis of Leg Swing Strike Effect in Wushu Sanda SportsDocument12 pagesResearch Article Multimedia Based Medical Big Data Analysis of Leg Swing Strike Effect in Wushu Sanda Sports壮No ratings yet
- Neuromuscular Responses To Different Resistance Loading Protocols Using Pneumatic and Weight Stack DevicesDocument7 pagesNeuromuscular Responses To Different Resistance Loading Protocols Using Pneumatic and Weight Stack Devices壮No ratings yet
- Validity of Force-Velocity Profiling Assessed With A Pneumatic Leg Press DeviceDocument21 pagesValidity of Force-Velocity Profiling Assessed With A Pneumatic Leg Press Device壮No ratings yet
- 1322 Jaric - InddDocument8 pages1322 Jaric - Indd壮No ratings yet
- 6330 Article - Text 29296 1 10 20210209Document11 pages6330 Article - Text 29296 1 10 20210209壮No ratings yet
- Patent for Exercise Device with Linkage to Control Muscle ExertionDocument10 pagesPatent for Exercise Device with Linkage to Control Muscle Exertion壮No ratings yet
- 飞轮离心超负荷训练应用研究进展 苏玉莹Document10 pages飞轮离心超负荷训练应用研究进展 苏玉莹壮No ratings yet
- Validity and Reliability of A Controlled Pneumatic Resistance Exercise DeviceDocument6 pagesValidity and Reliability of A Controlled Pneumatic Resistance Exercise Device壮No ratings yet
- The Effects of Combined Weight and Pneumatic Training To Enhance Power Endurance in Tennis PlayersDocument9 pagesThe Effects of Combined Weight and Pneumatic Training To Enhance Power Endurance in Tennis Players壮No ratings yet
- Peak Lifting Velocities of Men and Women For The Reduced Inertia Squat Exercise Using Force ControlDocument7 pagesPeak Lifting Velocities of Men and Women For The Reduced Inertia Squat Exercise Using Force Control壮No ratings yet
- Optimizing Post Activation Potentiation For Explosive Activities in Competitive SportsDocument12 pagesOptimizing Post Activation Potentiation For Explosive Activities in Competitive Sports壮No ratings yet
- Pneumatic Resistance Machines Can Provide.29Document2 pagesPneumatic Resistance Machines Can Provide.29壮No ratings yet
- Loads and Movement Speeds Dictate Differences in Power Output During Circuit TrainingDocument38 pagesLoads and Movement Speeds Dictate Differences in Power Output During Circuit Training壮No ratings yet
- Sayers 2010Document12 pagesSayers 2010壮No ratings yet
- Jidovtseff ICST2016 PneumaticPPTDocument8 pagesJidovtseff ICST2016 PneumaticPPT壮No ratings yet
- Changes in Maximal Strength, Velocity, and Power After 8 Weeks of Traning With Pneumatic or Free Weight ResistanceDocument11 pagesChanges in Maximal Strength, Velocity, and Power After 8 Weeks of Traning With Pneumatic or Free Weight Resistance壮No ratings yet
- Influence of Isoinertial-Pneumatic Mixed Resistances On Force-Velocity RelationshipDocument22 pagesInfluence of Isoinertial-Pneumatic Mixed Resistances On Force-Velocity Relationship壮No ratings yet
- Abosolute and Relative Peak Power During Pneumatic Squat Exercise Using Different Percentages of Load in Elite Soccer PlayersDocument7 pagesAbosolute and Relative Peak Power During Pneumatic Squat Exercise Using Different Percentages of Load in Elite Soccer Players壮No ratings yet
- Comparison of Three Baseball-Specific 6-Week Training Programs On Throwing Velocity in High School Baseball PlayersDocument15 pagesComparison of Three Baseball-Specific 6-Week Training Programs On Throwing Velocity in High School Baseball Players壮No ratings yet
- Comparison of Flywheel and Pneumatic Training On Hypertrophy, Strength, and Power in Professional Handball PlayersDocument17 pagesComparison of Flywheel and Pneumatic Training On Hypertrophy, Strength, and Power in Professional Handball Players壮No ratings yet
- Baseball Throwing Speed and Base Running Speed TheDocument7 pagesBaseball Throwing Speed and Base Running Speed The壮No ratings yet
- Piirainen 2014Document7 pagesPiirainen 2014壮No ratings yet
- Comparison of Different Functional Tests For Leg Power and Normative Bilateral Asymmetry Index in Healthy Collegiate AthletesDocument10 pagesComparison of Different Functional Tests For Leg Power and Normative Bilateral Asymmetry Index in Healthy Collegiate Athletes壮No ratings yet
- Pojednic 2012Document6 pagesPojednic 2012壮No ratings yet
- Rouben Off 2001Document7 pagesRouben Off 2001壮No ratings yet
- Paul 2013Document14 pagesPaul 2013壮No ratings yet
- Screening and Diagnostic Tests TutorialDocument9 pagesScreening and Diagnostic Tests TutorialInriza RenzaNo ratings yet
- Diabetes Phils ReportDocument89 pagesDiabetes Phils ReportRold Brio SosNo ratings yet
- Gestational Diabetes Mellitus: Causes, Screening, and TreatmentDocument21 pagesGestational Diabetes Mellitus: Causes, Screening, and TreatmentGlen Jacobs SumadihardjaNo ratings yet
- Lec Framework Care of MotherDocument27 pagesLec Framework Care of MotherRica ParcasioNo ratings yet
- Gestational Diabetes MellitusDocument69 pagesGestational Diabetes MellitusStephen BakingNo ratings yet
- Presented By-Kamini SinghDocument52 pagesPresented By-Kamini SinghSupriyati RahayuNo ratings yet
- DM GestasionalDocument22 pagesDM GestasionalAditya Arya PutraNo ratings yet
- Glycosuria Diagnosis and TreatmentDocument6 pagesGlycosuria Diagnosis and TreatmentMuthuvel ShanmugasundaramNo ratings yet
- Diabetes Manual - A Guide To Diabetes ManagementDocument243 pagesDiabetes Manual - A Guide To Diabetes ManagementDrsarfaraz SiddiquiNo ratings yet
- Gestational Diabetes Mellitus Update and Review of Literature 2161 038X.S2 008 PDFDocument6 pagesGestational Diabetes Mellitus Update and Review of Literature 2161 038X.S2 008 PDFBuluan Mps McadNo ratings yet
- Control Your DiabetesDocument161 pagesControl Your DiabetesemanvitoriaNo ratings yet
- (2016) Roval - Resistência Insulínica - Leandro MedeirosDocument56 pages(2016) Roval - Resistência Insulínica - Leandro MedeirosAna Sara ZiniNo ratings yet
- Module 17 Part 2 Ratio 19 22 EndoDocument102 pagesModule 17 Part 2 Ratio 19 22 EndoLA BriguelaNo ratings yet
- Worksheet Hp04Document17 pagesWorksheet Hp04Andika Indra Purwantoro100% (1)
- Antidiabetic, Antihyperlipidemic and Antioxidant Properties of Roots of Ventilago Maderaspatana Gaertn. On StreptozotocinInduced Diabetic RatsDocument10 pagesAntidiabetic, Antihyperlipidemic and Antioxidant Properties of Roots of Ventilago Maderaspatana Gaertn. On StreptozotocinInduced Diabetic RatsIOSRjournalNo ratings yet
- Diagnostic Test For Endocrine DisordersDocument4 pagesDiagnostic Test For Endocrine DisordersjesperdomincilbayauaNo ratings yet
- Current Trends in The Diagnosis and Management ofDocument42 pagesCurrent Trends in The Diagnosis and Management ofseun williamsNo ratings yet
- Pedia NotesDocument36 pagesPedia NotesmelNo ratings yet
- DM and GlucoseDocument1 pageDM and GlucoseibunaraNo ratings yet
- DCMNT PDFDocument36 pagesDCMNT PDFOh HudaNo ratings yet
- M1.U3 Screening and Diagnosis in Public Health Students 2023Document11 pagesM1.U3 Screening and Diagnosis in Public Health Students 2023Raja RafianNo ratings yet
- Diabetes Mellitus in Children (Pedi Clinics of N. America Vol 52, No 6) WW PDFDocument275 pagesDiabetes Mellitus in Children (Pedi Clinics of N. America Vol 52, No 6) WW PDFEliMihaelaNo ratings yet
- Diabetes PPT FianlDocument31 pagesDiabetes PPT FianlUqba MishalNo ratings yet
- Suspected Postprandial Hypoglycemia Is Associated With ,&adrenergic Hypersensitivity and Emotional DistressDocument6 pagesSuspected Postprandial Hypoglycemia Is Associated With ,&adrenergic Hypersensitivity and Emotional Distresslasith123No ratings yet
- Clinical Presentation and Diagnosis of Diabetes Mellitus in AdultsDocument16 pagesClinical Presentation and Diagnosis of Diabetes Mellitus in AdultsjjjkkNo ratings yet
- A 34-Year-Ol... y at 24 Weeks GestationDocument4 pagesA 34-Year-Ol... y at 24 Weeks Gestationblndffl100% (1)
- Documents and RecordsDocument161 pagesDocuments and RecordsSaravnan Rajendran100% (2)
- Assay of Glucose 3 PDFDocument11 pagesAssay of Glucose 3 PDFrahma kaggwaNo ratings yet