Professional Documents
Culture Documents
Pyo Pneumothorax
Uploaded by
Sarah Dyaanggari Akip0 ratings0% found this document useful (0 votes)
5 views2 pagesThis document summarizes a case report of a rare case of necrotizing pneumonia complicated by pneumothorax in a 45-year-old male patient. The patient was intubated for hypoxemic respiratory failure and treated empirically with antibiotics. His condition deteriorated with septic shock. Imaging showed worsening right lower lobe infiltrates and a new right-sided pneumothorax. Klebsiella pneumoniae was isolated from tracheal aspirate. Despite iatrogenic pneumothorax being considered, serial imaging and exams ruled it out. This case describes the progression of necrotizing pneumonia to cavities, pleural abnormalities, and eventual pneumothorax, requiring special attention and treatment
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes a case report of a rare case of necrotizing pneumonia complicated by pneumothorax in a 45-year-old male patient. The patient was intubated for hypoxemic respiratory failure and treated empirically with antibiotics. His condition deteriorated with septic shock. Imaging showed worsening right lower lobe infiltrates and a new right-sided pneumothorax. Klebsiella pneumoniae was isolated from tracheal aspirate. Despite iatrogenic pneumothorax being considered, serial imaging and exams ruled it out. This case describes the progression of necrotizing pneumonia to cavities, pleural abnormalities, and eventual pneumothorax, requiring special attention and treatment
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
5 views2 pagesPyo Pneumothorax
Uploaded by
Sarah Dyaanggari AkipThis document summarizes a case report of a rare case of necrotizing pneumonia complicated by pneumothorax in a 45-year-old male patient. The patient was intubated for hypoxemic respiratory failure and treated empirically with antibiotics. His condition deteriorated with septic shock. Imaging showed worsening right lower lobe infiltrates and a new right-sided pneumothorax. Klebsiella pneumoniae was isolated from tracheal aspirate. Despite iatrogenic pneumothorax being considered, serial imaging and exams ruled it out. This case describes the progression of necrotizing pneumonia to cavities, pleural abnormalities, and eventual pneumothorax, requiring special attention and treatment
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 2
A46 INFECTIONS AND INFECTIOUS COMPLICATIONS IN THE ICU / Thematic Poster Session / Sunday, May 15/09:30 AM-03:45
PM / Area K, Hall F (North Building, Exhibition Level), Moscone Center
A Rare Case of Necrotizing Pneumonia Complicated with Pneumothorax
M. Al Khateeb1, M. Aldiabat2, Y. Al Jabiri1; 1Internal Medicine, NYCHHC Lincoln medical center,
Bronx, NY, United States, 2Internal Medicine, Lincoln Medical Center, Bronx, NY, United States.
Corresponding author's email: mohanadkhat@outlook.com
Introduction: Necrotizing pneumonia is an uncommon severe complication characterized by
inflammation, consolidation progressive peripheral necrosis of lung parenchyma, multiple small
cavities secondary to cytokines and toxins release; furthermore, it can cause vascular interruption
secondary to thrombus formation which favors uncontrolled bacterial growth, impaired antibiotic
delivery resulting in liquefaction and gangrene formation. Case Presentation: 45-year-old male was
found lying down with bizarre behavior. On presentation he was disheveled with poor hygiene and
food inside his mouth. Later, his clinical status deteriorated with tachypnea, tachycardia and
accessory muscle use, intubated due to hypoxemic respiratory failure. Chest radiograph on
admission showed right lower lobe infiltrate. He was started on ceftriaxone and azithromycin as an
empirical treatment, after obtaining blood and tracheal aspirate cultures. On the second day after
intubation, his hospital course was complicated with septic shock with drop in blood pressure, right
subclavian central line was placed to start vasopressors medications. Chest radiograph obtained
after insertion of central line confirmed central line placement without complications, also shows
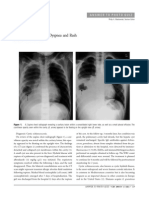
worsening of the infiltrate in the right lower lobe of the lung. On the 4th day, he spiked fever, with
drop in blood pressure requiring increase in the vasopressors with full ventilatory support. chest
radiograph showed new right sided pneumothorax portable chest x ray shows right lower lobe
infiltrates with pneumothorax on the right side. On that day, antibiotic therapy escalated to
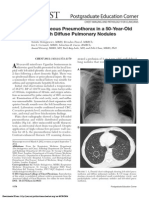
piperacillin tazobactam therapy. CT scan was done after placement of chest tube as in the attached
figure. Culture from tracheal aspiration came back positive for numerous Klebsiella pneumoniae.
Discussion: we describe a case of necrotizing pneumonia complicated with pneumothorax. The
consolidation with surrounding inflammation progressed to cavities and pleural abnormalities and
eventually pneumothorax. Iatrogenic pneumothorax from right subclavian central line placement
would be one of the causes of pneumothorax in this case, but it was ruled out with chest radiograph
confirmed placement 2 days prior to pneumothorax complication event and serial physical
examinations prior to the event of pneumothorax with confirmed bilateral air entry with crackles
bilaterally. Our case requires special attention to this rare but serious presentation, which can lead
to death if not appropriately evaluated with the pertinent treatments and interventions when needed.
To the best of our knowledge, necrotizing pneumonia has been described before as a rare
complication of pneumonia, but never described in similar presentation and complication.
This abstract is funded by: none
Am J Respir Crit Care Med 2022;205:A1623
Internet address: www.atsjournals.org Online Abstracts Issue
You might also like
- Inflammation - Case StudiesDocument55 pagesInflammation - Case StudiesDr Suvarna Nalapat100% (3)
- Vastu Diagnostic Software Ver 2Document115 pagesVastu Diagnostic Software Ver 2Jai Kishan Babani100% (1)
- Letter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationDocument3 pagesLetter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationfatimiahmastaNo ratings yet
- Organizing Pneumonia Following Covid19 PneumoniaDocument4 pagesOrganizing Pneumonia Following Covid19 PneumoniaKhangNo ratings yet
- Lesoes Cisticas HIVDocument5 pagesLesoes Cisticas HIVAndrey Barbosa PimentaNo ratings yet
- COP - Cryptogenic Organizing Pneumonia - StatPearls - NCBI BookshelfDocument7 pagesCOP - Cryptogenic Organizing Pneumonia - StatPearls - NCBI Bookshelfrbatjun576No ratings yet
- Necrotizing Pneumonia (Aetiology, Clinical Features and Management)Document8 pagesNecrotizing Pneumonia (Aetiology, Clinical Features and Management)pachomdNo ratings yet
- Lung QuizDocument14 pagesLung QuizConcepcion R. AquinoNo ratings yet
- Tubo Ovarian AbscessDocument4 pagesTubo Ovarian AbscessFitria RiaNo ratings yet
- Abses Paru JurnalDocument2 pagesAbses Paru JurnalAzha AzzunaNo ratings yet
- F - CMCRep 1 Assy Et Al - 1405Document2 pagesF - CMCRep 1 Assy Et Al - 1405faegrerh5ju75yu34yNo ratings yet
- Valente Acosta2020Document4 pagesValente Acosta2020Andres TameNo ratings yet
- Pulmonary Pseudotumoral Tuberculosis in An Old Man: A Rare PresentationDocument3 pagesPulmonary Pseudotumoral Tuberculosis in An Old Man: A Rare PresentationNurhasanahNo ratings yet
- A 28 Year Old Man With Chest Pain, Shortness of BRDocument4 pagesA 28 Year Old Man With Chest Pain, Shortness of BRagamerocallejasNo ratings yet
- Bronchitis Obliterans Due To Mycoplasma PneumoniaDocument7 pagesBronchitis Obliterans Due To Mycoplasma Pneumoniawawa chenNo ratings yet
- Chest: Recent Advances in Chest MedicineDocument9 pagesChest: Recent Advances in Chest MedicinesmansakobiNo ratings yet
- Jurding Bedah MuzzamilDocument16 pagesJurding Bedah MuzzamilunknownNo ratings yet
- Pulmonary Tuberculosis Presenting With Acute Respiratory Distress Syndrome (ARDS) : A Case Report and Review of LiteratureDocument5 pagesPulmonary Tuberculosis Presenting With Acute Respiratory Distress Syndrome (ARDS) : A Case Report and Review of LiteratureCimol AgustinaNo ratings yet
- Altenburg J Review Article Neth J Med 2015Document8 pagesAltenburg J Review Article Neth J Med 2015manalNo ratings yet
- 1752 1947 5 377 PDFDocument4 pages1752 1947 5 377 PDFBrian GreenNo ratings yet
- Medscape Infectious DiseaseDocument110 pagesMedscape Infectious DiseaseAnoop DSouzaNo ratings yet
- Acute Airway Compromise Due To Subcutaneus EmphysemaDocument5 pagesAcute Airway Compromise Due To Subcutaneus EmphysemaUssy TsnnnNo ratings yet
- Necrotizing PneumoniaDocument7 pagesNecrotizing PneumoniaMahdalenaSyahNo ratings yet
- A Case of Endobronchial Actinomycosis As A Challenging Cause of Lung AtelectasisDocument4 pagesA Case of Endobronchial Actinomycosis As A Challenging Cause of Lung AtelectasisNiatazya Mumtaz SagitaNo ratings yet
- Underdiagnosed and Potentially Lethal. Upper Extremity Deep Venous ThrombosisDocument6 pagesUnderdiagnosed and Potentially Lethal. Upper Extremity Deep Venous Thrombosischarlietuna1No ratings yet
- Neu Motor AxDocument6 pagesNeu Motor AxZay SiagNo ratings yet
- Surgical Treatment of Awn Aspiration Causing BroncDocument5 pagesSurgical Treatment of Awn Aspiration Causing BroncEasti EmoraNo ratings yet
- A 7-Year-Old Girl With Dyspnea and Rash: AnswertophotoquizDocument2 pagesA 7-Year-Old Girl With Dyspnea and Rash: AnswertophotoquizMateen ShukriNo ratings yet
- Staphy 2Document5 pagesStaphy 2Alexandra MariaNo ratings yet
- Computed Tomography Findings of Community-Acquired Immunocompetent Patient: A Case ReportDocument4 pagesComputed Tomography Findings of Community-Acquired Immunocompetent Patient: A Case ReportDenta HaritsaNo ratings yet
- 1 s2.0 S193004332100902X MainDocument6 pages1 s2.0 S193004332100902X MainFatimah AssagafNo ratings yet
- TMP 8 E70Document4 pagesTMP 8 E70FrontiersNo ratings yet
- Gharib2001 Radiologi Pneumonia-DikonversiDocument31 pagesGharib2001 Radiologi Pneumonia-Dikonversitsamara24_No ratings yet
- Diagnosis and Treatment Protocol For Novel Coronavirus PneumoniaDocument17 pagesDiagnosis and Treatment Protocol For Novel Coronavirus PneumoniaYaqeen MutanNo ratings yet
- (Materi Dr. Heny) PneumoniaDocument86 pages(Materi Dr. Heny) PneumoniaFathiyah SalsabilaNo ratings yet
- Treatment of Slowly Growing Mycobacteria: Julie V. Philley,, David E. GriffithDocument12 pagesTreatment of Slowly Growing Mycobacteria: Julie V. Philley,, David E. Griffiththanhnhat5521No ratings yet
- ccr3 4071Document3 pagesccr3 4071helamahjoubmounirdmoNo ratings yet
- Bacterial PneumoniaDocument6 pagesBacterial PneumoniaIrsa SevenfoldismNo ratings yet
- Neumonia NecrotizanteDocument8 pagesNeumonia Necrotizantearturo garciaNo ratings yet
- Case ReportDocument5 pagesCase ReportMax FaxNo ratings yet
- Pneumonitis Ec ChemotheraphyDocument5 pagesPneumonitis Ec ChemotheraphyNurafiat AntonNo ratings yet
- Primary Malignant Melanoma of The TracheDocument93 pagesPrimary Malignant Melanoma of The TracheMikmik bay BayNo ratings yet
- Pneumatocele: BackgroundDocument8 pagesPneumatocele: BackgroundSilmi Noor RachniNo ratings yet
- Severe TuberculosisDocument4 pagesSevere TuberculosisAdelia GhosaliNo ratings yet
- Pulmonary Pathology of Early-Phase 2019 Novel Coronavirus (COVID-19) Pneumonia in Two Patients With Lung CancerDocument5 pagesPulmonary Pathology of Early-Phase 2019 Novel Coronavirus (COVID-19) Pneumonia in Two Patients With Lung Cancermuhammad RidoNo ratings yet
- Simultaneous Bilateral Primary Spontaneous Pneumothorax (2019)Document7 pagesSimultaneous Bilateral Primary Spontaneous Pneumothorax (2019)sandi_prawira_yudhaNo ratings yet
- Case Report: A 75-Year-Old Female With Hemoptysis and Recurrent Respiratory InfectionsDocument4 pagesCase Report: A 75-Year-Old Female With Hemoptysis and Recurrent Respiratory InfectionsIRa SyalalaNo ratings yet
- Case Report: Hydropneumothorax in Children: A Rare Complication of A Bacterial PneumoniaDocument5 pagesCase Report: Hydropneumothorax in Children: A Rare Complication of A Bacterial PneumoniaNadya NovianiNo ratings yet
- Proptosis UnilateralDocument5 pagesProptosis UnilateralCarlos NiveloNo ratings yet
- A 65-Year-Old Man Came To The Emergency Department Via Ambulance - Relatives Accompanied The Patient and Described A 1-Day History of FeverDocument43 pagesA 65-Year-Old Man Came To The Emergency Department Via Ambulance - Relatives Accompanied The Patient and Described A 1-Day History of FeverandriopaNo ratings yet
- BrochiectasisDocument34 pagesBrochiectasisAndi Wija Indrawan PangerangNo ratings yet
- E.P.C.M.S.: A Case of Bronchiolitis Obliterans in A 21 Month Old InfantDocument3 pagesE.P.C.M.S.: A Case of Bronchiolitis Obliterans in A 21 Month Old InfantWelly ElvandariNo ratings yet
- Coronavirus (COVID-19) Outbreak: What The Department of Radiology Should KnowDocument5 pagesCoronavirus (COVID-19) Outbreak: What The Department of Radiology Should KnowrezaNo ratings yet
- Talcum Induced Pneumoconiosis Following Inhalation of Adulterated Marijuana, A Case ReportDocument6 pagesTalcum Induced Pneumoconiosis Following Inhalation of Adulterated Marijuana, A Case ReportRyl WonNo ratings yet
- Jnma00736 0021Document3 pagesJnma00736 0021talenticaxo1No ratings yet
- A Treacherous Course: Clinical Problem-SolvingDocument6 pagesA Treacherous Course: Clinical Problem-SolvingMorocco CandycatyNo ratings yet
- Case 1: Recurrent Pneumonia in A 15-Year-Old Girl: Article Figures & Data Info & Metrics CommentsDocument7 pagesCase 1: Recurrent Pneumonia in A 15-Year-Old Girl: Article Figures & Data Info & Metrics CommentsJoshua MendozaNo ratings yet
- Landouzy Septicemia (Sepsis Tuberculosa Acutissima) Due To Mycobacterium Microti in An Immunocompetent ManDocument4 pagesLandouzy Septicemia (Sepsis Tuberculosa Acutissima) Due To Mycobacterium Microti in An Immunocompetent Manreadyboy89No ratings yet
- Acute Bronchitis Case StudyDocument6 pagesAcute Bronchitis Case Studyulka0750% (2)
- CytomegaloDocument3 pagesCytomegaloYusi RizkyNo ratings yet
- Studies on Epidemic Influenza: Comprising Clinical and Laboratory InvestigationsFrom EverandStudies on Epidemic Influenza: Comprising Clinical and Laboratory InvestigationsNo ratings yet
- DLP-Bohol - Science9 Q1 W1 D1Document3 pagesDLP-Bohol - Science9 Q1 W1 D1Jen Lorejas100% (1)
- Blood Vessel and Lymphatic Lab OutputDocument12 pagesBlood Vessel and Lymphatic Lab OutputDayledaniel SorvetoNo ratings yet
- BIO MCQS by IlmiDocument67 pagesBIO MCQS by IlmiZee waqarNo ratings yet
- Reexpansion Pulmonary Edema : UpdateDocument6 pagesReexpansion Pulmonary Edema : UpdateWenny EudensiaNo ratings yet
- Animal Kingdom-Subphylum Vertebrata-Class IXDocument2 pagesAnimal Kingdom-Subphylum Vertebrata-Class IXMonika Mehan100% (2)
- Respiratory PathologyDocument42 pagesRespiratory PathologyMorgan PeggNo ratings yet
- A Doctor View of The CrucifixionDocument5 pagesA Doctor View of The CrucifixiontimothjohnNo ratings yet
- PneumoniaDocument4 pagesPneumoniaroscelle100% (1)
- Idiopathic Pulmonary Fibrosis NEWDocument34 pagesIdiopathic Pulmonary Fibrosis NEWrahayuNo ratings yet
- Transportation in Animals and PlantsDocument3 pagesTransportation in Animals and Plantsravilulla100% (1)
- San Beda Respiratory System 9-15Document68 pagesSan Beda Respiratory System 9-15conyxzNo ratings yet
- Mastering Running Cathy UtzschneiderDocument241 pagesMastering Running Cathy Utzschneidervirus100% (2)
- 10 Biology BitsDocument34 pages10 Biology BitsSuresh Raghava100% (1)
- Pulmonary Function TestsDocument1 pagePulmonary Function Testsprecious_n143No ratings yet
- A Case Presentation in Community Acquired PneumoniaDocument24 pagesA Case Presentation in Community Acquired PneumoniaMarineth O. LasicNo ratings yet
- Nyeri Dada Dalam EmergensiDocument18 pagesNyeri Dada Dalam EmergensiSyukran AbNo ratings yet
- Case Studies: Restrictive and Obstructive Respiratory Conditions Case Study # 1Document5 pagesCase Studies: Restrictive and Obstructive Respiratory Conditions Case Study # 1psyarjavierNo ratings yet
- CASE PDL RSMP Hana (Wecompress - Com) .Id - enDocument88 pagesCASE PDL RSMP Hana (Wecompress - Com) .Id - enHana SulistiaNo ratings yet
- Pulmonary EdemaDocument31 pagesPulmonary EdemaMourian Aman100% (1)
- How To Read Chest X RayDocument3 pagesHow To Read Chest X RayGeetha PuvanNo ratings yet
- Lung Examination: AbnormalDocument56 pagesLung Examination: AbnormalBECAREFUL89ANo ratings yet
- Chapter 53 - Introduction To The Respiratory SystemDocument13 pagesChapter 53 - Introduction To The Respiratory SystemJonathonNo ratings yet
- Core 2 PDHPE - Body in Motion Study NotesDocument43 pagesCore 2 PDHPE - Body in Motion Study Notesmarissa.makhNo ratings yet
- IRDSDocument17 pagesIRDSJustin Ahorro-DionisioNo ratings yet
- Chicken Anatomy and Physiology: Respiratory System: by Jacquie Jacob and Tony PescatoreDocument4 pagesChicken Anatomy and Physiology: Respiratory System: by Jacquie Jacob and Tony Pescatoreసాయిమహేష్రెడ్డిఆవులNo ratings yet
- Handout AtelectasisDocument14 pagesHandout AtelectasisSasha IfahmyNo ratings yet
- CSEC Biology June 2007 P1Document10 pagesCSEC Biology June 2007 P1Andre Pachico67% (3)
- Case Study For PneumothoraxDocument4 pagesCase Study For PneumothoraxGabbii CincoNo ratings yet
- Respiratory DisordersDocument15 pagesRespiratory Disordersmnlstr100% (5)