Professional Documents
Culture Documents
PB 0783
Uploaded by
Mona HelouOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
PB 0783
Uploaded by
Mona HelouCopyright:
Available Formats
ACOG
PRACTICE
BULLETIN
CLINICAL MANAGEMENT GUIDELINES FOR
OBSTETRICIAN–GYNECOLOGISTS
NUMBER 78, JANUARY 2007
(Replaces Practice Bulletin Number 64, July 2005)
Hemoglobinopathies in
This Practice Bulletin was Pregnancy
developed by the ACOG Com- The hemoglobinopathies are a heterogeneous group of single-gene disorders
mittee on Practice Bulletins— that includes the structural hemoglobin variants and the thalassemias. More
Obstetrics with the assistance
than 270 million people worldwide are heterozygous carriers of hereditary dis-
of John Williams III, MD. The
orders of hemoglobin, and at least 300,000 affected homozygotes or compound
information is designed to aid
practitioners in making deci- heterozygotes are born each year (1). The purpose of this document is to review
sions about appropriate obstet- the most common hemoglobinopathies and to provide recommendations for
ric and gynecologic care. These screening and clinical management of hemoglobinopathies during pregnancy.
guidelines should not be con-
strued as dictating an exclusive
course of treatment or proce- Background
dure. Variations in practice may Hemoglobin Structure
be warranted based on the
needs of the individual patient, Hemoglobin consists of four interlocking polypeptide chains, each of which has
resources, and limitations an attached heme molecule. The polypeptide chains are called alpha (α), beta
unique to the institution or type (β), gamma (γ), delta (δ), epsilon (ε), and zeta (ζ). Adult hemoglobins consist
of practice of two α-chains and either two β-chains (hemoglobin A), two γ-chains (hemo-
globin F), or two δ-chains (hemoglobin A2). Hemoglobin F (fetal hemoglobin,
Reaffirmed 2015 Hb F) is the primary hemoglobin of the fetus from 12 to 24 weeks of gestation.
In the third trimester, production of Hb F decreases as production of β-chains
and Hb A begins. The genes that code for α-globin chains are located on the
short arm of chromosome 16, and the β-globin gene is located on the short arm
of chromosome 11.
Sickle Cell Disease
Sickle cell disease refers to a group of autosomal recessive disorders involving
abnormal hemoglobin (hemoglobin S). Hemoglobin S differs from the normal
Hb A because of a single nucleotide substitution of thymine for adenine in the
β-globin gene; this alteration causes a substitution of valine for glutamic acid in
the number six position of the β-globin polypeptide. Asymptomatic individuals
with heterozygous Hb S genotypes (carriers) are said to nosis of sickle cell disorders because they cannot distin-
have sickle cell trait. The most severe form of the disease, guish between the heterozygous AS and homozygous SS
Hb SS (homozygous Hb S), is called sickle cell anemia. genotypes. In addition, they fail to detect other patho-
Sickle cell disorders are found not only in patients logic variants such as Hb C trait, β-thalassemia trait,
who have the hemoglobin genotype SS, but also in those Hb E trait, Hb B trait, and Hb D trait.
who have Hb S and one other abnormality of β-globin
structure or β-globin production. The most common of The Thalassemias
these are Hb SC disease and Hb S/β-thalassemia. In Hb C, The thalassemias represent a wide spectrum of hemato-
the same nucleotide involved in the Hb S mutation is logic disorders that are characterized by a reduced syn-
altered with the substitution of adenine for guanine, thesis of globin chains, resulting in microcytic anemia.
which results in the amino acid substitution of lysine for Thalassemias are classified according to the globin chain
glutamic acid. This and other abnormal hemoglobins, affected, with the most common types being α-thal-
when inherited with Hb S, may cause clinically signifi- assemia and β-thalassemia. Many different molecular
cant vasoocclusive phenomena and hemolytic anemia mechanisms lead to thalassemia in populations from dif-
similar to Hb SS. ferent areas of the world (5).
Sickle cell disease occurs most commonly in people
of African origin. Approximately 1 in 12 African Ameri- Alpha-Thalassemia
cans has sickle cell trait (2). One in every 300 African- Alpha-thalassemia usually results from a gene deletion of
American newborns has some form of sickle cell disease, two or more copies of the four α-globin genes. Deletion
and approximately 1 in 600 has sickle cell anemia. Hemo- of one α-globin gene (α-/αα) is clinically unrecogniz-
globin S also is found in high frequency in other popula- able, and laboratory testing yields normal results.
tions such as Greeks, Italians (particularly Sicilians), Deletion of two α-globin genes causes α-thalassemia
Turks, Arabs, Southern Iranians, and Asian Indians (3). trait, a mild asymptomatic microcytic anemia. The dele-
The classical clinical feature of patients with sickle tions can be on the same chromosome or in cis (αα/--),
cell disease is seen under conditions of decreased oxygen or on each chromosome or in trans (α-/α-). Individuals
tension, in which the red blood cells become distorted with these chromosomal abnormalities are referred to as
into various shapes, some of which resemble sickles. The carriers and are at an increased risk for having a child
distorted red cells lead to increased viscosity, hemolysis, with a more severe form of thalassemia caused by dele-
and anemia and a further decrease in oxygenation. When tions of three or four copies of the α-globin gene (α-thal-
sickling occurs within small blood vessels, it can cause assemia major). The possible genetic combinations are
“logjams” that can interrupt blood supply to vital organs summarized in Table 1.
(vasoocclusive crisis). Repeated vasoocclusive crises Alpha-thalassemia trait (α-thalassemia minor) is
result in widespread microvascular obstruction with common among individuals of Southeast Asian, African,
interruption of normal perfusion and function of several and West Indian descent. It also is common in individuals
organs, including the spleen, lungs, kidneys, heart, and with Mediterranean ancestry. Individuals with Southeast
brain. Adults with Hb SS are functionally asplenic, hav- Asian ancestry are more likely to carry two gene dele-
ing undergone autosplenectomy by adolescence. Absence tions in cis or on the same chromosome (--/αα) and are
of the spleen contributes to the increased incidence and at an increased risk for offspring with Hb Bart’s or Hb H
severity of infection in patients with sickle cell disease. disease. Hemoglobin H disease, which is caused by the
The most significant threat to patients with sickle deletion of three α-globin genes, usually is associated
cell disease is acute chest syndrome. Chest syndrome is with mild to moderate hemolytic anemia. Alpha-thal-
characterized by a pulmonary infiltrate with fever that assemia major (Hb Bart’s) results in the absence of α-
leads to hypoxemia and acidosis. The infiltrates are not globin (--/--); this is associated with hydrops fetalis,
infectious in origin but rather are due to vasoocclusion intrauterine death, and preeclampsia (3).
from sickling or embolization of marrow from long In individuals of African descent, α-thalassemia usu-
bones affected by sickling (4). ally is due to a deletion of a single α-globin gene on each
The diagnosis of hemoglobinopathies, including chromosome 16 (α-/α-). This is in contrast to the com-
sickle cell disorders, is made by hemoglobin electro- mon Asian genotype, which is a deletion of both α-glo-
phoresis. In the homozygous form, nearly all the hemo- bin genes on one chromosome 16 (cis) (αα/--).
globin is Hb S with small amounts of Hb A2 and Hb F. Hemoglobin Bart’s disease does not typically develop in
Heterozygous sickle cell trait (Hb AS) is identified by a fetuses of α-thalassemia carriers of African origin.
larger percentage of Hb A and an asymptomatic course. Because Hb S results from an abnormality of the
Solubility tests (Sickledex) alone are inadequate for diag- β-chain, both heterozygous (AS) and homozygous (SS)
2 ACOG Practice Bulletin No. 78
Table 1. Classification of Alpha-Thalassemias
Number of Clinical
Globin Genes Genotype Description Features
4 αα/αα Normal Normal
3 α-/αα Heterozygous Asymptomatic
α+-thalassemia
2 α-/α- Homozygous Mild
α+-thalassemia anemia
αα/-- Heterozygous
αo-thalassemia
1 α-/-- α+-Thalassemia/ Hb H disease
αo-thalassemia hemolytic anemia
0 --/-- Homozygous Hb Bart’s disease
αo-thalassemia hydrops fetalis
forms can be inherited with heterozygous or homozy- are produced and, as a result, variable amounts of Hb A
gous α+-thalassemia. In individuals with sickle cell trait are produced. The genes for Hb S and β-thalassemia usu-
(Hb AS), α-thalassemia lowers the proportion of ally behave as alleles, with only one gene inherited from
Hb S, and in those with Hb SS, it lessens the severity of each parent. The expression of the resulting Hb S/β-thal-
sickle cell disease. assemia is determined by the type of β-thalassemia
Alpha-thalassemia also may occur as a result of a mutation (6).
gene mutation. In this case, the genes are present but not Beta-thalassemia minor, common in individuals of
functioning normally. This may result from mutation in Mediterranean, Asian, Middle Eastern, Hispanic, and West
the stop codon leading to synthesis of a longer and unsta- Indian descent, varies in severity of disease. Depending
ble α-chain (Hb Constant Spring), from substitutions on the amount of β-chain production, it usually is asso-
impairing αβ dimer formation (Hb Qong Sze), and from ciated with asymptomatic mild anemia. Beta-thal-
point substitutions in the poly A region at the 3' end of assemia minor often occurs in association with Hb S. In
the gene (αTSaudi). the most severe form, no normal β-globin chains are
produced. This results in a clinically severe syndrome
Beta-Thalassemia called sickle cell–β0-thalassemia, in which no Hb A is
Beta-thalassemia is caused by a mutation in the β-globin produced.
gene that causes deficient or absent β-chain production,
which results in absence of Hb A. Classification of
β-thalassemias is based on a description of the molecu- Clinical Considerations and
lar mutation or by clinical manifestations. Individuals
who are heterozygous for this mutation have β-thalas-
Recommendations
semia minor. Those who are homozygous have β-thal- Who should be screened for hemoglobinopa-
assemia major (Cooley’s anemia) or a milder form thies and how should this be accomplished?
called thalassemia intermedia. Beta-thalassemia major
is characterized by severe anemia with resultant Genetic screening can identify couples at risk for off-
extramedullary erythropoesis, delayed sexual develop- spring with hemoglobinopathies and allow them to make
ment, and poor growth. Elevated levels of Hb F in indi- informed decisions regarding reproduction and prenatal
viduals with β-thalassemia major partially compensate diagnosis (3). Individuals of African, Southeast Asian,
for the absence of Hb A; however, death usually occurs and Mediterranean ancestry are at a higher risk for being
by age 10 years unless treatment is begun early with carriers of hemoglobinopathies and should be offered
periodic blood transfusions. With transfusion, the severe carrier screening. Ethnic groups considered to be at low
anemia is reversed and extramedullary erythropoesis is risk for hemoglobinopathies include northern Euro-
suppressed. In homozygotes with the less severe β+-thal- peans, Japanese, Native Americans, Inuit (Eskimo), and
assemia mutations, often referred to as β-thalassemia Koreans. If both parents are determined to be carriers,
intermedia, variable but decreased amounts of β-chains genetic counseling is recommended. It should be noted
ACOG Practice Bulletin No. 78 3
that ethnicity is not always a good predictor of risk ous hemoglobinopathies, such as Hb S/β-thalassemia and
because individuals from at-risk groups may marry out- Hb SC disease. Solubility testing may be valuable, how-
side their ethnic group (3). ever, for rapid screening for sickling when this informa-
A combination of laboratory tests may be required to tion is critical for immediate patient care.
provide the information necessary to counsel couples Determination of mean corpuscular volume (MCV)
who are carriers of one of the thalassemias or sickle cell is recommended for patients who are at risk for α- or
disease (Fig. 1). To ensure accurate hemoglobin identifi- β-thalassemia. Patients who have a low MCV (less than
cation, which is essential for genetic counseling, a com- 80 fL) may have one of the thalassemia traits and are
plete blood count (CBC) is the appropriate initial candidates for hemoglobin electrophoresis. These indi-
laboratory test for individuals of non-African descent. In viduals also may have iron deficiency anemia, and
individuals of African descent, a hemoglobin elec- measurement of serum ferretin levels is recommended.
trophoresis should be performed in addition to a CBC. Beta-thalassemia is associated with elevated Hb F and
Several tests, including solubility testing such as a test for elevated Hb A2 levels (more than 3.5%). Neither hemo-
the presence of Hb S (Sickledex), isoelectric focusing, globin electrophoresis nor solubility testing can identify
and high-performance liquid chromatography (HPLC), individuals with α-thalassemia trait; only molecular
have been used for primary screening. However, solubil- genetic testing can identify this condition. If the MCV is
ity tests alone are inadequate for screening and fail to below normal, iron deficiency anemia has been excluded,
identify important transmissible hemoglobin gene abnor- and the hemoglobin electrophoresis is not consistent with
malities affecting fetal outcome (eg, Hb C trait, β-thal- β-thalassemia trait (ie, there is no elevation of Hb A2 or
assemia trait, Hb E trait, Hb B trait, Hb D trait). Many Hb F), then DNA-based testing should be used to detect
individuals with these genotypes are asymptomatic, but if α-globin gene deletions characteristic of α-thalassemia.
their partners have the sickle cell trait or other hemoglo- The hematologic features of some of the common
binopathies, they may produce offspring with more seri- hemoglobinopathies are shown in Table 2. If both part-
CBC and RBC indices
Patients of Southeast Asian or Mediterranean descent Patients of African descent
No abnormality Anemia (with reduced MCV
and normal iron status)
Hemoglobin electrophoresis
Normal Hb AS, AC, SS, SC, elevated A2, and
other abnormal hemoglobin
If Southeast Asian, evaluate for α-thalassemia
Not a carrier of Carrier of
α-thalassemia α-thalassemia
Offer testing of partner to assess reproductive risk
Figure 1. Specialized antepartum evaluation for hematologic assessment of patients of African,
Southeast Asian, or Mediterranean descent. Patients of Southeast Asian or Mediterranean descent
should undergo electrophoresis if their blood test results reveal anemia. Abbreviations: CBC, complete
blood count; Hb, hemoglobin; MCV, mean corpuscular volume; RBC, red blood cell.
4 ACOG Practice Bulletin No. 78
Table 2. Hematologic Features of Main Hemoglobinopathies
Disorder Heterozygous State Homozygous State DNA Analysis
α+ Thalassemia (-α) 0–2% Hb Bart’s at birth 5–10% Hb Bart’s in the neonatal S. blot: α-gene probe,
period, low MCV abnormal band with Bam H1
αo Thalassemia (--) 5–10% Hb Bart’s in the neonatal Hb Bart’s hydrops fetalis S. blot or PCR: absence of:
period, low MCV, normal Hb A2 α-gene band in homozygote
βo Thalassemia Low MCH & MCV, Hb A2 3.5–7.0% Thalassemia major: Hb F 98% PCR, ASO – dot blot, S. blot
Hb A2 2% β-gene probe
β+ Thalassemia (severe) Low MCH & MCV, Hb A2 3.5–7.0% Thalassemia major: Hb F 70–95% PCR, ASO – dot blot, S. blot
β-gene probe
β+ Thalassemia (mild) Low MCH & MCV, Hb A2 3.5–7.0% Thalassemia intermedia: PCR, ASO – dot blot, S. blot
Hb F 20–40% β-gene probe
Hb S Hb A, Hb S, Hb A2 Hb S, Hb F (1–15%), Hb A2 PCR: Dde 1 digestion
PCR, ASO – dot blot
Hb S/β-Thalassemia — If βo thalassemia, severe sickle PCR: Dde 1 digestion
cell anemia; if β+ thalassemia, PCR, ASO – dot blot
less severe
Hb E/β-Thalassemia — Thalassemia major or intermedia: PCR: Hb E by Mnl 1 digestion
Hb E 60–70%, Hb F 30–40%
Abbreviations: ASO, allele specific oligonucleotide; Hb, hemoglobin; MCH, mean corpuscular hemoglobin; MCV, mean corpuscular volume; PCR, polymerase chain
reaction; S. blot, Southern blot.
Modified from Milunsky, Aubrey, MB.B.Ch., D.Sc., F.R.C.P., F.A.C.M.G., D.C.H., ed. Genetic Disorders and the Fetus, fifth edition: Diagnosis, Prevention, and Treatment.
pp. 665, Table 19.1. © 2004 Aubrey Milunsky. Reprinted with permission of The Johns Hopkins University Press.
ners are identified as carriers of a gene for abnormal technology has been somewhat limited because of ethi-
hemoglobins, genetic counseling is recommended. cal, social, and cultural concerns. Prenatal diagnosis is
most commonly requested by families who have had a
For couples with an increased risk for having child with sickle cell disease and who wish to be certain
an affected offspring, what methods are that their next child is not affected. In many respects,
available for genetic diagnosis of the fetus or these families are “self-counseled.” The difficulty in
embryo? counseling families who have not had an affected child
lies in the variable severity of the disease and the inabil-
Couples at risk for having a child with a hemoglobinopa- ity to predict its course (6). One investigator found that
thy may benefit from genetic counseling to review the nearly 70% of families in whom prenatal diagnosis con-
natural history of these disorders, prospects for treatment firmed that the fetus was affected with Hb SS elected to
and cure, their risk, availability of prenatal genetic testing, continue the pregnancy (7).
and reproductive options. Prenatal diagnostic testing for
the single mutation responsible for sickle cell disease is How is sickle cell disease in pregnancy
widely available. Testing for α- and β-thalassemia is pos- managed?
sible if the mutations and deletions have been previously
identified in both parents. These DNA-based tests can be Pregnancy in women with sickle cell disease is associat-
performed using chorionic villi obtained by chorionic ed with an increased risk of morbidity and mortality
villus sampling (CVS) at 10–12 weeks of gestation or because of the combination of underlying hemolytic
using cultured amniotic fluid cells obtained by amnio- anemia and multiorgan dysfunction associated with this
centesis after 15 weeks of gestation. For some couples, disorder. Morbidity and mortality have decreased
preimplantation genetic diagnosis in combination with in markedly over the past 3 decades because of improve-
vitro fertilization may be a desirable alternative to avoid ments in general medical care for patients with sickle cell
termination of an affected pregnancy. Preimplantation disease, improvements in transfusion medicine, and
genetic diagnosis has been successfully performed for advancements in neonatal care (8, 9). In spite of the
sickle cell disease and most cases of β-thalassemia. decline in maternal and perinatal mortality rates, how-
Although the advances in prenatal diagnosis of ever, pregnancy is still a significant clinical risk for many
hemoglobinopathies have been impressive, use of the patients with sickle cell disease. The magnitude of the
ACOG Practice Bulletin No. 78 5
risk varies with genotype and severity of anemia. When What is the role of transfusion or prophylac-
compared with Hb AA patients, women with Hb SS have tic exchange transfusion for pregnancies
increased risk for maternal complications, such as pre- complicated by sickle cell anemia?
term labor, premature rupture of membranes, antepartum
hospitalization, and postpartum infection. In addition, Controversy exists regarding the role of prophylactic
patients with Hb SS are at higher risk for fetal complica- blood transfusion in the management of sickle cell dis-
tions, such as intrauterine growth restriction (IUGR), low ease in pregnancy (13–15). By limiting transfusion to
birth weight, and preterm delivery (9, 10). Patients with situations in which it is clinically indicated, patients are
Hb SC disease also are at risk for the aforementioned not subjected to the increased risk for alloimmunization
complications but to a lesser extent than patients with (16), viral infections, and iron overload. Major compli-
Hb SS disease (10). cations (eg, worsening anemia; intrapartum complica-
Pregnant patients with sickle cell disease need tions such as hemorrhage, septicemia, and cesarean
increased prenatal folic acid supplementation. The stan- delivery; painful crisis; and chest syndrome) may
dard 1 mg of folate in prenatal vitamins is not adequate require intervention with an exchange transfusion. There
for patients with hemoglobinopathies; 4 mg per day of is no consensus regarding the exact hematocrit value
folic acid should be prescribed because of the continual below which transfusion should be considered.
turnover of red blood cells. However, when a transfusion is clinically indicated in
Routine cesarean delivery for women with sickle cell the patient with sickle cell disease, the objective is to
disease is not indicated and should be performed only for lower the percentage of Hb S to approximately 40%
obstetric indications. Epidural analgesia usually is well while simultaneously raising the total hemoglobin con-
tolerated as long as care is taken to avoid hypotension centration to about 10 g/dL. Hemoglobin levels and the
and hypoxemia. Pregnant patients should, if possible, be percentage of Hb S should be monitored serially during
cared for at institutions that are able to manage both the the remainder of the pregnancy to determine the need for
complications of sickle cell disease and high-risk preg- subsequent transfusions.
nancies. They also should have regular prenatal care by Prophylactic exchange transfusion was first pro-
or in consultation with obstetricians who are experienced posed by Ricks in 1965, who recommended exchange
in the management of sickle cell disease. transfusion 4–6 weeks before the delivery date (17).
The most common cause of recurrent morbidity in Preliminary results appeared to show a benefit in that all
Hb SS disease is painful crisis. If possible, precipitating women and infants survived (18). Subsequently, several
factors, such as cold environment, heavy physical exer- studies have shown improvement in maternal and fetal
outcome with prophylactic transfusion (15, 19). How-
tion, dehydration, and stress, should be avoided. Hydroxy-
ever, the evidence is not conclusive that transfusion is
urea has been shown to reduce the frequency of painful
responsible for the improvement; similar improvement
crises in nonpregnant patients with severe sickle cell dis-
has been observed in programs that do not use prophy-
ease (11). However, the use of hydroxyurea is not recom-
lactic transfusion. In the only randomized controlled trial
mended during pregnancy because it is teratogenic.
published to date, prophylactic transfusion was associ-
Painful crises in pregnancy as well as in the non-
ated with a decreased risk for painful crisis and severe
pregnant patient are managed with rapid assessment of
anemia, but no difference was observed for pregnancy
the level of pain and prompt administration of analgesia.
outcome (14). It appears from the available evidence that
Pain, respiratory rate, and level of sedation should be
the reduction in morbidity and mortality of sickle cell
assessed until pain is controlled. Opiates can be given
disease in pregnancy is attributable to improvements in
orally or parenterally by the intravenous, intramuscular,
general management of pregnancy rather than prophy-
or subcutaneous route. Oxygen should be given if the O2
lactic transfusion per se.
saturation is less than 95% by pulse oximetry. The initial
clinical assessment also should focus on detection of Is fetal surveillance useful in pregnancies
serious medical complications requiring specific therapy,
complicated by sickle cell anemia?
such as acute chest syndrome (fever tachypnea, chest
pain, and hypoxia), infection, dehydration, severe ane- Pregnancies in women with sickle cell disease are at
mia, cholecystitis, and hypersplenism. A multidiscipli- increased risk for spontaneous abortion, preterm labor,
nary approach should be used involving obstetricians, IUGR, and stillbirth (20). For this reason, a plan for ser-
hematologists, and anesthesiologists (12). Painful crises ial ultrasound examinations and antepartum fetal testing
in the third trimester may have a prolonged course and is reasonable. Published data on antenatal fetal surveil-
may not resolve until after delivery. lance in women with sickle cell disease are limited. In a
6 ACOG Practice Bulletin No. 78
retrospective review of 58 pregnancies in women with Beta-thalassemia minor usually causes mild asympto-
sickle cell disease undergoing prophylactic transfusion, matic anemia. In the absence of documented iron defi-
no patients had a nonreactive nonstress test result or pos- ciency, replacement beyond prophylactic doses of iron is
itive contraction stress test result (21). All pregnancy not indicated. Studies involving fairly small numbers of
outcomes were normal. The investigators concluded that patients suggest that pregnancy outcome is favorable in
placental reserve and fetal reactivity were uncompro- women with β-thalassemia minor. A study of 261 pregnant
mised and that these tests were as sensitive for assess- women with β-thalassemia minor found a significantly
ment of fetal well-being in women with sickle cell higher rate of IUGR and oligohydramnios than is found in
disease as for women with other indications for antenatal nonthalassemic patients (26). No differences were noted in
testing. perinatal outcomes such as low Apgar scores, congenital
Because patients with sickle cell crisis usually malformations, or perinatal mortality (26).
require narcotics for pain control, the results of abnormal
antepartum testing should be interpreted with caution.
One small study has shown that nonstress test results and Summary of
biophysical profiles may be abnormal during an episode
of crisis but revert back to normal with resolution of the Recommendations and
episode (22). The clinical significance of this is unclear. Conclusions
How is thalassemia in pregnancy managed? The following recommendations are based on
good and consistent scientific evidence (Level A):
The course of pregnancy in women with the α-thalas-
semia trait is not significantly different from that of Individuals of African, Southeast Asian, and
women with normal hemoglobin. Pregnancy in women Mediterranean descent are at increased risk for
with Hb H disease has been reported, and with the being carriers of hemoglobinopathies and should be
exception of mild to moderate chronic anemia, outcomes offered carrier screening and, if both parents are
have been favorable. However, the number of reports is determined to be carriers, genetic counseling.
too few to draw definite conclusions regarding pregnan-
A complete blood count and hemoglobin electro-
cy outcome in all women with Hb H disease (23).
phoresis are appropriate laboratory tests for screen-
Until recently, pregnancy in women with β-thalas-
ing for hemoglobinopathies. Solubility tests alone
semia major was extremely rare. Initially, this was are inadequate for screening because they fail to
because delay of growth and sexual development and identify important transmissible hemoglobin gene
early death in untreated patients prevented reproduction. abnormalities affecting fetal outcome.
After the introduction of transfusion therapy in the 1960s,
pregnancy was still uncommon because of infertility Couples at risk for having a child with sickle cell
(secondary to hypothalamic dysfunction and anovulation disease or thalassemia should be offered genetic
caused by hemosiderin deposition). Since the introduc- counseling to review prenatal testing and reproduc-
tion of hypertransfusion and iron chelation therapy with tion options. Prenatal diagnosis of hemoglobin-
deferoxamine in the late 1970s, several reports and case opathies is best accomplished by DNA analysis of
series have documented favorable pregnancy outcomes in cultured amniocytes or chorionic villi.
women with β-thalassemia major (24, 25). Pregnancy in
women with β-thalassemia major is recommended only
for those with normal cardiac function who have had pro- References
longed hypertransfusion therapy to maintain hemoglobin 1. Angastiniotis M, Modell B. Global epidemiology of hemo-
levels at 10 g/dL and iron chelation therapy with defer- globin disorders. Ann N Y Acad Sci 1998;850:251–69.
oxamine (25). During pregnancy, hemoglobin levels (Level II-3)
should be maintained at or near 10 g/dL with transfu- 2. Motulsky AG. Frequency of sickling disorders in U.S.
sions. Deferoxamine usually is discontinued because the blacks. N Engl J Med 1973;288:31–3. (Level III)
safety of iron chelation therapy during pregnancy has not 3. Davies SC, Cronin E, Gill M, Greengross P, Hickman M,
been established. Fetal growth should be monitored with Normand C. Screening for sickle cell disease and thalas-
serial ultrasonography. In cases in which fetal growth is semia: a systematic review with supplementary research.
suboptimal, patients should have fetal surveillance. The Health Technol Assess 2000;4:i–v, 1–99. (Level III)
mode of delivery should be individualized, with cesarean 4. Duffy TP. Hematologic aspects of pregnancy. In: Burrow
delivery reserved for obstetric indications. GN, Duffy TP, Copel JA, editors. Medical complications
ACOG Practice Bulletin No. 78 7
during pregnancy. 6th ed. Philadelphia (PA): Elsevier patients with sickle cell hemoglobinopathies: benefit ver-
Saunders; 2004. p. 69–86. (Level III) sus risk. Obstet Gynecol 1980;56:274–80. (Level III)
5. Kazazian HH Jr. The thalassemia syndromes: molecular 16. Brumfield CG, Huddleston JF, DuBois LB, Harris BA Jr.
basis and prenatal diagnosis in 1990. Semin Hematol A delayed hemolytic transfusion reaction after partial
1990;27:209–28. (Level III) exchange transfusion for sickle cell disease in pregnancy:
a case report and review of literature. Obstet Gynecol
6. Serjeant GR, Serjeant BE. Sickle cell disease. 3rd ed. New 1984;63(suppl):13s–15s. (Level III)
York (NY): Oxford University Press; 2001. (Level III)
17. Ricks P Jr. Exchange transfusion in sickle cell anemia in
7. Alter BP. Prenatal diagnosis of hematologic diseases, pregnancy. Obstet Gynecol 1965;25:117–9. (Level III)
1986 update. Acta Haematol 1987;78:137–41. (Level II-3)
18. Ricks P Jr. Further experience with exchange transfusion
8. Smith JA, Espeland M, Bellevue R, Bonds D, Brown AK, in sickle cell anemia in pregnancy. Am J Obstet Gynecol
Koshy M. Pregnancy in sickle cell disease: experience of 1968;100:1087–90. (Level III)
the Cooperative Study of Sickle Cell Disease. Obstet 19. Morrison JC, Wiser WL. The use of prophylactic partial
Gynecol 1996;87:199–204. (Level II-2) exchange transfusion in pregnancies associated with sickle
9. Sun PM, Wilburn W, Raynor BD, Jamieson D. Sickle cell cell hemoglobinopathies. Obstet Gynecol 1976;48:516–20.
disease in pregnancy: twenty years of experience at Grady (Level III)
Memorial Hospital, Atlanta, Georgia. Am J Obstet 20. Serjeant GR, Loy LL, Crowther M, Hambleton IR, Thame
Gynecol 2001;184:1127–30. (Level II-2) M. Outcome of pregnancy in homozygous sickle cell dis-
10. Powars DR, Sandhu M, Niland-Weiss J, Johnson C, Bruce ease. Obstet Gynecol 2004;103:1278–85. (Level II–2)
S, Manning PR. Pregnancy in sickle cell disease. Obstet 21. Morrison JC, Blake PG, McCoy C, Martin JN Jr, Wiser
Gynecol 1986;67:217–28. (Level II-3) WL. Fetal health assessment in pregnancies complicated
by sickle hemoglobinopathies. Obstet Gynecol 1983;61:
11. Charache S. Mechanism of action on hydroxyurea in the 22–4. (Level III)
management of sickle cell anemia in adults. Semin
Hematol 1997;34(suppl 3):15–21. (Level I) 22. Anyaegbunam A, Morel MI, Merkatz IR. Antepartum
fetal surveillance tests during sickle cell crisis. Am J
12. Rees DC, Olujohungbe AD, Parker NE, Stephens AD, Obstet Gynecol 1991;165:1081–3. (Level II-2)
Telfer P, Wright J. Guidelines for the management of the
acute painful crisis in sickle cell disease. British 23. Ong HC, White JC, Sinnathuray TA. Haemoglobin H dis-
Committee for Standards in Haematology General ease and pregnancy in a Malaysian woman. Acta
Haematol 1977;58:229–33. (Level III)
Haematology Task Force by the Sickle Cell Working
Party. Br J Haematol 2003;120:744–52. (Level III) 24. Jensen CE, Tuck SM, Wonke B. Fertility in beta thalas-
semia major: a report of 16 pregnancies, preconceptual
13. Tuck SM, James CE, Brewster EM, Pearson TC, Studd evaluation and a review of the literature. Br J Obstet
JW. Prophylactic blood transfusion in maternal sickle cell Gynaecol 1995;102:625–9. (Level III)
syndromes. Br J Obstet Gynaecol 1987;94:121–5. (Level
III) 25. Aessopos A, Karabatsos F, Farmakis D, Katsantoni A,
Hatziliami A, Youssef J, et al. Pregnancy in patients with
14. Koshy M, Burd L, Wallace D, Moawad A, Baron J. well-treated beta-thalassemia: outcome for mothers and
Prophylactic red-cell transfusions in pregnant patients newborn infants. Am J Obstet Gynecol 1999;180:360–5.
with sickle cell disease. A randomized cooperative study. (Level III)
N Engl J Med 1988;319:1447–52. (Level I)
26. Sheiner E, Levy A, Yerushalmi R, Katz M. Beta-thalas-
15. Morrison JC, Schneider JM, Whybrew WD, Bucovaz ET, semia minor during pregnancy. Obstet Gynecol 2004;103:
Menzel DM. Prophylactic transfusions in pregnant 1273–7. (Level II-2)
ACOG Practice Bulletin No. 78 8
Copyright © January 2007 by the American College of Obste-
The MEDLINE database, the Cochrane Library, and tricians and Gynecologists. All rights reserved. No part of this
ACOG’s own internal resources and documents were used publication may be reproduced, stored in a retrieval system,
to conduct a literature search to locate relevant articles pub- posted on the Internet, or transmitted, in any form or by any
lished between January 1985 and March 2005. The search means, electronic, mechanical, photocopying, recording, or
was restricted to articles published in the English language. otherwise, without prior written permission from the publisher.
Priority was given to articles reporting results of original
research, although review articles and commentaries also Requests for authorization to make photocopies should be
were consulted. Abstracts of research presented at sympo- directed to Copyright Clearance Center, 222 Rosewood Drive,
sia and scientific conferences were not considered adequate Danvers, MA 01923, (978) 750-8400.
for inclusion in this document. Guidelines published by or- ISSN 1099-3630
ganizations or institutions such as the National Institutes of The American College of
Health and the American College of Obstetricians and Gy- Obstetricians and Gynecologists
necologists were reviewed, and additional studies were 409 12th Street, SW
located by reviewing bibliographies of identified articles. PO Box 96920
When reliable research was not available, expert opinions Washington, DC 20090-6920
from obstetrician–gynecologists were used.
Studies were reviewed and evaluated for quality according
to the method outlined by the U.S. Preventive Services Task Hemoglobinopathies in pregnancy. ACOG Practice Bulletin No. 78.
Force: American College of Obstetricians and Gynecologists. Obstet Gynecol
2007;109:229–37.
I Evidence obtained from at least one properly de-
signed randomized controlled trial.
II-1 Evidence obtained from well-designed controlled
trials without randomization.
II-2 Evidence obtained from well-designed cohort or
case–control analytic studies, preferably from more
than one center or research group.
II-3 Evidence obtained from multiple time series with or
without the intervention. Dramatic results in uncon-
trolled experiments also could be regarded as this
type of evidence.
III Opinions of respected authorities, based on clinical
experience, descriptive studies, or reports of expert
committees.
Based on the highest level of evidence found in the data,
recommendations are provided and graded according to the
following categories:
Level A—Recommendations are based on good and consis-
tent scientific evidence.
Level B—Recommendations are based on limited or incon-
sistent scientific evidence.
Level C—Recommendations are based primarily on con-
sensus and expert opinion.
9 ACOG Practice Bulletin No. 78
You might also like
- Thalassemias: Alissa Martin,, Alexis A. ThompsonDocument9 pagesThalassemias: Alissa Martin,, Alexis A. ThompsonAmada RosalesNo ratings yet
- HemoglobinopathiesDocument37 pagesHemoglobinopathiesBabak Nami100% (1)
- Thalasemia MedscapeDocument21 pagesThalasemia MedscapeFenty IswarNo ratings yet
- Background: Alpha ThalassemiaDocument24 pagesBackground: Alpha ThalassemiacristieristiieNo ratings yet
- Detection and Quantitation of Normal and Variant Haemoglobins: An Analytical ReviewDocument15 pagesDetection and Quantitation of Normal and Variant Haemoglobins: An Analytical ReviewAmanda MatthewsNo ratings yet
- Erythrocyte Disorders in The Perinatal Period in AdversePregnancy Outcome and The Fetus:NeonateDocument12 pagesErythrocyte Disorders in The Perinatal Period in AdversePregnancy Outcome and The Fetus:Neonatethanhhien900No ratings yet
- ThalassaemiasDocument8 pagesThalassaemiasSalim UddinkhanNo ratings yet
- ThalassemiaDocument3 pagesThalassemiaArmandoNo ratings yet
- ThalassaemiasDocument8 pagesThalassaemiasSalim UddinkhanNo ratings yet
- Thalassemia and Related HemoglobinopathiesDocument6 pagesThalassemia and Related HemoglobinopathiesMelly SyafridaNo ratings yet
- Thalassaemia: Definition, Classification, Pathogenesis and Complications of This DisorderDocument37 pagesThalassaemia: Definition, Classification, Pathogenesis and Complications of This DisorderSheila MichaelsNo ratings yet
- Introduction To Hemoglobinopathies Diagnostics On HPLC by P.C. GiordanoDocument4 pagesIntroduction To Hemoglobinopathies Diagnostics On HPLC by P.C. GiordanoUMMID WashimNo ratings yet
- Hemoglobin SynthesisDocument4 pagesHemoglobin Synthesismadison DeliNo ratings yet
- Hemoglobinopathies Hanna Waleed MohamedDocument10 pagesHemoglobinopathies Hanna Waleed Mohamedx8w6df2fxwNo ratings yet
- THALASSEMIADocument30 pagesTHALASSEMIAjismi vallachiraNo ratings yet
- Sickle Cell Anemia and Thalassemias: Paul R. EarlDocument21 pagesSickle Cell Anemia and Thalassemias: Paul R. EarlNavisatul MutmainahNo ratings yet
- Case Study - ThalassemiaDocument42 pagesCase Study - ThalassemiaROMER LOZADANo ratings yet
- Study On Hemoglobinopathies and G6PD Deficiency in Terai Districts of NepalDocument30 pagesStudy On Hemoglobinopathies and G6PD Deficiency in Terai Districts of NepalSaroj BhattaraiNo ratings yet
- Sickle Cell Diseases and Thalasemia Asma2Document60 pagesSickle Cell Diseases and Thalasemia Asma2Female calmNo ratings yet
- ThalassemiaDocument22 pagesThalassemiaturky hadiNo ratings yet
- Variable Clinical Phenotypes of α-Thalassemia Syndromes: The Scientific World Journal · February 2009Document12 pagesVariable Clinical Phenotypes of α-Thalassemia Syndromes: The Scientific World Journal · February 2009Minh Triết CochonNo ratings yet
- Thalassaemia S 1Document24 pagesThalassaemia S 1Nickesha MilletteNo ratings yet
- Hemoglobinopathies (Hemoglobin Disorders)Document18 pagesHemoglobinopathies (Hemoglobin Disorders)Bravan AliennNo ratings yet
- Thalassemia Case ReportDocument40 pagesThalassemia Case ReportZarvi Jane MangubatNo ratings yet
- Alpha and Beta ThalassemiaDocument6 pagesAlpha and Beta ThalassemiaSi vis pacem...100% (1)
- Thalassemia - StatPearls - NCBI BookshelfDocument10 pagesThalassemia - StatPearls - NCBI Bookshelfrsaurabh396No ratings yet
- Thalassemia An OverviewDocument4 pagesThalassemia An OverviewLink BuiNo ratings yet
- Sickle Cell Disease in PregnancyDocument18 pagesSickle Cell Disease in Pregnancyapi-370504667% (3)
- Thalassemia: Submitted By: Jovan Pierre C. Ouano Submitted To: Mark Gil T. DacutanDocument8 pagesThalassemia: Submitted By: Jovan Pierre C. Ouano Submitted To: Mark Gil T. DacutanJvnpierre AberricanNo ratings yet
- Alpha ThalassemiaDocument3 pagesAlpha ThalassemiaSravya PangaNo ratings yet
- Alpha-Thalassemia: Authors: Renzo Galanello, MD Antonio Cao, MDDocument31 pagesAlpha-Thalassemia: Authors: Renzo Galanello, MD Antonio Cao, MDKiran KumarNo ratings yet
- Automated Capillary Electrophoresis in The ScreeningDocument9 pagesAutomated Capillary Electrophoresis in The Screeningsomething privateNo ratings yet
- Resistencia Genética A La MalariaDocument6 pagesResistencia Genética A La MalariaJuan Diego García sicchaNo ratings yet
- Hemoglobin ElectrophoresisDocument22 pagesHemoglobin ElectrophoresisMohamed IbrahimNo ratings yet
- HemoglobinDocument41 pagesHemoglobinSri Ram 07No ratings yet
- Sickle Cell Disease and Other HemoglobinopathiesDocument5 pagesSickle Cell Disease and Other HemoglobinopathiesOkwukwe Dan-WachukuNo ratings yet
- HB H Disease Clinical Course and DiseaseDocument9 pagesHB H Disease Clinical Course and DiseaseLink BuiNo ratings yet
- Review Article Role Of Xmni Polymorphism In Hbf Induction In Hbe/Β And Β-Thalassaemia PatientsDocument10 pagesReview Article Role Of Xmni Polymorphism In Hbf Induction In Hbe/Β And Β-Thalassaemia PatientsRumana Mahtarin TrishaNo ratings yet
- Jbjba 73 S D7 WKNCQ MVF BGH 6 Zs TK SQformat PDFDocument8 pagesJbjba 73 S D7 WKNCQ MVF BGH 6 Zs TK SQformat PDFmaedasalih2002No ratings yet
- B-Talasemias. N Engl J Med 2021.Document17 pagesB-Talasemias. N Engl J Med 2021.VirginiaÁlvarezYepesNo ratings yet
- Hemoglobinopathies and Thalassemias Lin OswariDocument16 pagesHemoglobinopathies and Thalassemias Lin OswariNOVRILIANo ratings yet
- Hemoglobin Op A Thy Is A Kind of Genetic Defect That Results in Abnormal Structure of One of The Globin Chains of The Hemoglobin MoleculeDocument3 pagesHemoglobin Op A Thy Is A Kind of Genetic Defect That Results in Abnormal Structure of One of The Globin Chains of The Hemoglobin MoleculeIkram ShinwariNo ratings yet
- Novel Genetic Therapeutic Approaches For Modulating The Severity of Thalassemia (Review)Document11 pagesNovel Genetic Therapeutic Approaches For Modulating The Severity of Thalassemia (Review)drsourabhsinghNo ratings yet
- Аlpha-thalassemia A practical overviewDocument18 pagesАlpha-thalassemia A practical overvieweskandaronalabNo ratings yet
- Case Report Non-infection Unit Β-Major ThalassemiaDocument27 pagesCase Report Non-infection Unit Β-Major ThalassemiaimamkdNo ratings yet
- Hemoglobinopathies and ThalassemiasDocument10 pagesHemoglobinopathies and ThalassemiashartNo ratings yet
- Hemoglobinopathies & Thalasemia Learning ObjectivesDocument10 pagesHemoglobinopathies & Thalasemia Learning ObjectivesFatima AhmedNo ratings yet
- HB Bart Fact SheetDocument2 pagesHB Bart Fact Sheetstrawberry pieNo ratings yet
- Thalassemia Case ReportDocument40 pagesThalassemia Case ReportGracelia DamanikNo ratings yet
- 1.2 Thalasemmia BookDocument21 pages1.2 Thalasemmia BookRhoda Lom-ocNo ratings yet
- Alpha-Thalassemia Syndromes: From Clinical and Molecular Diagnosis To Bedside ManagementDocument12 pagesAlpha-Thalassemia Syndromes: From Clinical and Molecular Diagnosis To Bedside Managementmayro simanjuntakNo ratings yet
- Haemoglobinopathies - ThalassaemiaDocument49 pagesHaemoglobinopathies - ThalassaemiaRaymond LundaNo ratings yet
- Labmed44 0e72Document5 pagesLabmed44 0e72Firdaus Al HafizNo ratings yet
- Talasemias RevisionDocument17 pagesTalasemias Revisionrodolfo venegasNo ratings yet
- Abid 3 PDFDocument14 pagesAbid 3 PDFLuan MatosNo ratings yet
- A Model for Gene Therapy: Gene Replacement in the Treatment of Sickle Cell Anemia and ThalassemiaFrom EverandA Model for Gene Therapy: Gene Replacement in the Treatment of Sickle Cell Anemia and ThalassemiaNo ratings yet
- PB 1299Document17 pagesPB 1299Mona HelouNo ratings yet
- PB 082Document10 pagesPB 082Mona HelouNo ratings yet
- Septeper 2015 Recall 200 Sba Mrcog Part 1Document49 pagesSepteper 2015 Recall 200 Sba Mrcog Part 1VINOD GUPTA100% (2)
- No. 44. Neural Tube DefectsDocument11 pagesNo. 44. Neural Tube DefectsenriqueNo ratings yet
- PB 0533Document13 pagesPB 0533Mona HelouNo ratings yet
- ACOG Management of Stillbirth PDFDocument14 pagesACOG Management of Stillbirth PDFLêMinhĐứcNo ratings yet
- PB 172Document13 pagesPB 172Mona HelouNo ratings yet
- Passmrcog Pharma 2016Document150 pagesPassmrcog Pharma 2016Mona Helou100% (1)
- 190 - Gestational Diabetes Mellitus AgogDocument16 pages190 - Gestational Diabetes Mellitus Agogjorge vergara100% (2)
- PB 110Document13 pagesPB 110Mona HelouNo ratings yet
- Passmrcog Patho, Embryo 2016Document171 pagesPassmrcog Patho, Embryo 2016Mona HelouNo ratings yet
- Physiology Passmrcog 2016Document73 pagesPhysiology Passmrcog 2016Mona HelouNo ratings yet
- PB 114Document14 pagesPB 114Mona HelouNo ratings yet
- Barriers of Influenza Vaccination Intention and Behavior - A Systematic Review of Influenza Vaccine Hesitancy, 2005 - 2016Document46 pagesBarriers of Influenza Vaccination Intention and Behavior - A Systematic Review of Influenza Vaccine Hesitancy, 2005 - 2016Mona HelouNo ratings yet
- Patients' and Health Professionals' Use of Social Media in Health CareDocument6 pagesPatients' and Health Professionals' Use of Social Media in Health CareMona HelouNo ratings yet
- CDCDocument11 pagesCDCMona HelouNo ratings yet
- Prescribers Prefer People: The Sources of Information Used by Doctors For Prescribing Suggest That The Medium Is More Important Than The MessageDocument6 pagesPrescribers Prefer People: The Sources of Information Used by Doctors For Prescribing Suggest That The Medium Is More Important Than The MessageMona HelouNo ratings yet
- Randomized Controlled Trial On Promoting Influenza Vaccine in General Practice Waiting RoomsDocument8 pagesRandomized Controlled Trial On Promoting Influenza Vaccine in General Practice Waiting RoomsMona HelouNo ratings yet
- Intervention Effects From A Social Marketing Campaign To promoteHPV VaccinationDocument8 pagesIntervention Effects From A Social Marketing Campaign To promoteHPV VaccinationMona HelouNo ratings yet
- NIH Public Access: Author ManuscriptDocument8 pagesNIH Public Access: Author ManuscriptMona HelouNo ratings yet
- Albarqouni 2019Document6 pagesAlbarqouni 2019Mona HelouNo ratings yet
- Correlation EmpowermentDocument140 pagesCorrelation EmpowermentMona HelouNo ratings yet
- Harnessing Social Media For HealthDocument10 pagesHarnessing Social Media For HealthMona HelouNo ratings yet
- Social Media and Organ Donor RegistrationDocument7 pagesSocial Media and Organ Donor RegistrationMona HelouNo ratings yet
- Randomized Controlled Trial On Promoting Influenza Vaccine in General Practice Waiting RoomsDocument8 pagesRandomized Controlled Trial On Promoting Influenza Vaccine in General Practice Waiting RoomsMona HelouNo ratings yet
- Intervention Effects From A Social Marketing Campaign To promoteHPV VaccinationDocument8 pagesIntervention Effects From A Social Marketing Campaign To promoteHPV VaccinationMona HelouNo ratings yet
- CanadianDocument31 pagesCanadianMona HelouNo ratings yet
- Potential of Social Media in Promoting MentalDocument11 pagesPotential of Social Media in Promoting MentalMona HelouNo ratings yet
- CDCDocument11 pagesCDCMona HelouNo ratings yet
- A Study of PlacentaDocument9 pagesA Study of PlacentaDr. Zain FazalNo ratings yet
- Intussusception: Read By: Krisna (KNA)Document26 pagesIntussusception: Read By: Krisna (KNA)krisnaNo ratings yet
- Cefizox® FDADocument15 pagesCefizox® FDAMutiaraNo ratings yet
- Host Parasite InteractionDocument20 pagesHost Parasite InteractionRhomizal MazaliNo ratings yet
- q2 Health - 8 M 4 Revised PDFDocument24 pagesq2 Health - 8 M 4 Revised PDFGemarie CallosaNo ratings yet
- Episode ListDocument25 pagesEpisode ListhectorNo ratings yet
- Oxygen AdministrationDocument6 pagesOxygen AdministrationAsma SaleemNo ratings yet
- CBT Introductory WorkbookDocument18 pagesCBT Introductory WorkbookSohel AzamNo ratings yet
- Phenytoin Drug StudyDocument3 pagesPhenytoin Drug StudyCheezy Bread100% (1)
- Kine Assignment by Arsh NazDocument10 pagesKine Assignment by Arsh NazArsh NazNo ratings yet
- Atypical Extractions-Oral Surgery / Orthodontic Courses by Indian Dental AcademyDocument36 pagesAtypical Extractions-Oral Surgery / Orthodontic Courses by Indian Dental Academyindian dental academyNo ratings yet
- ANATOM 128 Brochure-ReDocument8 pagesANATOM 128 Brochure-ReAli MirzaNo ratings yet
- SMP 3510 Heller Chapter34Document48 pagesSMP 3510 Heller Chapter34Ari DewiyantiNo ratings yet
- Industrial Pharmacy Practice Notes-1Document4 pagesIndustrial Pharmacy Practice Notes-1Gerald Limo Arap ChebiiNo ratings yet
- Anti Human+HLA DR 174yb - 3174023DDocument1 pageAnti Human+HLA DR 174yb - 3174023DPaulo MattosNo ratings yet
- Catheter Care and MaintenanceDocument4 pagesCatheter Care and MaintenanceSha BtstaNo ratings yet
- Personal Data:: Curiculum VitaeDocument7 pagesPersonal Data:: Curiculum Vitaebudi darmantaNo ratings yet
- Epulis KongenitalDocument3 pagesEpulis KongenitalFriadi NataNo ratings yet
- Bacte01 STREPTOCOCCUS ENTEROCOCCUSDocument8 pagesBacte01 STREPTOCOCCUS ENTEROCOCCUSAngelic AngelesNo ratings yet
- Adenovirus DiseasesDocument44 pagesAdenovirus Diseasestummalapalli venkateswara rao100% (1)
- Sample: Reading Sub-Test - Text Booklet: Part ADocument24 pagesSample: Reading Sub-Test - Text Booklet: Part AAlwin BrightNo ratings yet
- Questionário Ii - Fundamentos Etimológicos Do InglêsDocument4 pagesQuestionário Ii - Fundamentos Etimológicos Do InglêsDébora Bandeira David100% (1)
- 69-Article Text-283-2-10-2022Document8 pages69-Article Text-283-2-10-2022EfanNo ratings yet
- Mya Harkness-Annotated Bibliography 1-12Document10 pagesMya Harkness-Annotated Bibliography 1-12api-403918901No ratings yet
- Cannabis Versus Rx-AntidepressantsDocument2 pagesCannabis Versus Rx-AntidepressantsDimitri HalleyNo ratings yet
- Split Technique 3Document13 pagesSplit Technique 3Alejandro RuizNo ratings yet
- Evaluation of Dysuria in AdultsDocument8 pagesEvaluation of Dysuria in AdultspapermintNo ratings yet
- A 55-Year-Old Woman With Shock and Labile Blood PressureDocument11 pagesA 55-Year-Old Woman With Shock and Labile Blood PressureMr. LNo ratings yet
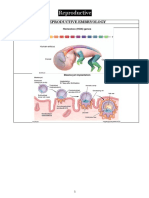
- Reproductive Arranged (MedicalBooksVN - Com)Document63 pagesReproductive Arranged (MedicalBooksVN - Com)Rabooh AyashiNo ratings yet
- What Is Mental Health?Document8 pagesWhat Is Mental Health?Sonal SahuNo ratings yet