Professional Documents
Culture Documents
Early Warning System for Pediatrics (EWS
Uploaded by
Yulia Derini0 ratings0% found this document useful (0 votes)
8 views15 pagesAn early warning system (EWS) uses vital sign scores to detect deterioration in pediatric patients' conditions before serious events occur. Key vital signs are assigned scores from 0-3, with 0 being normal and higher scores indicating issues. The total score determines the patient's color: green (0-2), yellow (3), orange (4), or red (5+). Higher scores require notification of supervising nurses and physicians and more frequent reassessment to address problems promptly. Properly using a pediatric early warning system through standardized screening and communication can help improve patient outcomes by reducing mortality and length of stay.
Original Description:
Ews
Original Title
Early-Warning-System-for-Pediatrics
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAn early warning system (EWS) uses vital sign scores to detect deterioration in pediatric patients' conditions before serious events occur. Key vital signs are assigned scores from 0-3, with 0 being normal and higher scores indicating issues. The total score determines the patient's color: green (0-2), yellow (3), orange (4), or red (5+). Higher scores require notification of supervising nurses and physicians and more frequent reassessment to address problems promptly. Properly using a pediatric early warning system through standardized screening and communication can help improve patient outcomes by reducing mortality and length of stay.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
8 views15 pagesEarly Warning System for Pediatrics (EWS
Uploaded by
Yulia DeriniAn early warning system (EWS) uses vital sign scores to detect deterioration in pediatric patients' conditions before serious events occur. Key vital signs are assigned scores from 0-3, with 0 being normal and higher scores indicating issues. The total score determines the patient's color: green (0-2), yellow (3), orange (4), or red (5+). Higher scores require notification of supervising nurses and physicians and more frequent reassessment to address problems promptly. Properly using a pediatric early warning system through standardized screening and communication can help improve patient outcomes by reducing mortality and length of stay.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 15
Early Warning System for
Pediatrics
REGIE A. BAUTISTA, RN, MN, EdD
Dean, College of Nursing
Systems Plus College Foundation
Angeles City, Philippines
How EWS works
An EWS is a physiologic scoring system typically
used in general medical-surgical units before
patients experience a catastrophic medical event.
This scoring is accompanied by a descriptive
step-by-step guide or algorithm of actions to take
based on the patient’s assessment score.
An EWS can add another layer of early detection
to the rapid response team system, helping staff
recognize high-risk patients before their condition
deteriorates.
Purpose
An Early Warning Score must be used for all
patients within a hospital setting when recording
observations/vital signs, to aide:
Early detection of detrimental changes
Safe, timely, effective management of care in response to a
patient’s deteriorating condition.
The EWS is required to be communicated
between staff when transferring patients between
areas and with requests for clinical assistance.
For a Pediatric patient the following observations/symptoms must
be completed on admission to obtain accurate PEWS. Subsequent
observation requirements are determined by the PEWS
management plan and/or the medical team.
Respiratory rate calculated over 1 minute
Respiratory distress score
Pulse oximetry
Heart rate for at least ½ minute
Blood pressure
Conscious level (using the AVPU)
Capillary refill time
Note whilst temperature is not included in the PEWS,
a baseline temperature recording is taken on
admission and four hourly thereafter for an inpatient.
Pediatric patients up to 15 years of age, use the age
appropriate Pediatric EWS (PEWS).
Scoring
The nurse scores each indicator according to a
specific behavior or range of vital signs. Each
physiologic indicator is assigned a score, ranging
from 0 to 3, depending on the assessment
outcome.
A score of 0 is considered normal or acceptable.
Scores ranging from 1 to 3 are considered
abnormal or unacceptable.
Scores for all indicators are added to create the
PEWS (Pediatric Early Warning System) score. The
total PEWS score is assigned a color based on the
sum of these numbers: a total of 0 to 2 is green, 3 is
yellow, 4 is orange, and 5 or higher is red.
Here are the actions mandated by
each color:
A yellow score:
Requires the reassessment of the patient by the
charge nurse on duty.
If the charge nurse confirms that the score is
accurate, he or she determines whether
intervention is required, documents assessment
and intervention in the medical record, and
reassesses the patient within 2 hours.
An orange score:
Requires reassessment by the charge nurse and
notification of the first- or second-year medical
resident. The resident alerts the senior resident
and attending healthcare provider of the change
in the patient’s medical condition, and medical
staff takes appropriate action. The direct care
nurse reassesses the patient within 1 hour.
A red score
Requires notification of the rapid response team
and resident. The resident alerts the senior
resident and attending healthcare provider, who
are all expected to respond to the patient’s
bedside. The rapid response team and primary
care team collaborate on the patient’s plan of
care. The direct care nurse reassesses the patient
within 1 hour.
Improving patient outcomes
A standardized acuity assessment and
communication method to recognize and avoid
patient decline may reduce patient mortality and
length of stay.
Standardization increases reliability and
decreases variation in the delivery of patient care.
Terima Kasih!
You might also like
- Consumer Reports Buying Guide 2021Document227 pagesConsumer Reports Buying Guide 2021fatso68100% (1)
- Icu NurseDocument3 pagesIcu NurseSherla Apple Oliveros RamosNo ratings yet
- ICU ProtocolsDocument35 pagesICU ProtocolsJohn Reynolds100% (6)
- The Electricity Wiring RegulationDocument239 pagesThe Electricity Wiring Regulationgodson50% (2)
- The COAT & Review Approach: How to recognise and manage unwell patientsFrom EverandThe COAT & Review Approach: How to recognise and manage unwell patientsRating: 5 out of 5 stars5/5 (1)
- Duties and Responsibilities of Icu Nurse RNDocument1 pageDuties and Responsibilities of Icu Nurse RNvalenzuelajrbenjamin100% (3)
- JCI PresentationDocument66 pagesJCI PresentationOsama MarzoukNo ratings yet
- PATIENT ASSESSMENT DEFINITIONS AND STEPSDocument15 pagesPATIENT ASSESSMENT DEFINITIONS AND STEPSDyah Arum KusumaningtyasNo ratings yet
- Nursing AssessmentDocument16 pagesNursing AssessmentJihan Novita100% (1)
- OnScreen B2 Quiz 2ADocument2 pagesOnScreen B2 Quiz 2ALaura B.100% (1)
- Patient Safety PlanDocument4 pagesPatient Safety PlanDhananjay SainiNo ratings yet
- Scope and Standards of Practice For The MedicalDocument10 pagesScope and Standards of Practice For The Medicalapi-239630424100% (1)
- Quality and Patient Safety ChecklistDocument7 pagesQuality and Patient Safety ChecklistKarl Roble100% (4)
- NICU Documentation: Gama Hospital Al Khobar K.S.ADocument8 pagesNICU Documentation: Gama Hospital Al Khobar K.S.ALucian CaelumNo ratings yet
- Patient Safety: Early Warning ScoreDocument50 pagesPatient Safety: Early Warning ScoreAiko himeNo ratings yet
- Assessing Pain Critically Ill AdultDocument7 pagesAssessing Pain Critically Ill AdultKitesaMedeksaNo ratings yet
- Ba GastrectomyDocument10 pagesBa GastrectomyHope3750% (2)
- Video Conferencing Lesson PlanDocument6 pagesVideo Conferencing Lesson PlanANN JILLIAN JOYCE MONDONEDO100% (1)
- Modified Early Warning System (Mews)Document6 pagesModified Early Warning System (Mews)ARDSNo ratings yet
- EWS for NewbornsDocument6 pagesEWS for NewbornsElizeus HaninditoNo ratings yet
- Early Warning Score RosalinaDocument18 pagesEarly Warning Score RosalinaRosalina LubisNo ratings yet
- Modified Early Warning Score (MEWS) Observation Chart: Clinical ProtocolDocument4 pagesModified Early Warning Score (MEWS) Observation Chart: Clinical ProtocolElena DolcanNo ratings yet
- Comprehensive Nursing Assessment GuidelineDocument10 pagesComprehensive Nursing Assessment GuidelineFrances Katherine I. GarciaNo ratings yet
- The Triage Process: Primary Survey Vs Primary Nursing AssessmentDocument13 pagesThe Triage Process: Primary Survey Vs Primary Nursing AssessmentPingkan MuntuanNo ratings yet
- Assesment Form': Sekolah Tinggi Ilmu Kesehatan Pemkab Jombang Program Studi D-Iii Keperawatan 2017 / 2018Document17 pagesAssesment Form': Sekolah Tinggi Ilmu Kesehatan Pemkab Jombang Program Studi D-Iii Keperawatan 2017 / 2018sindimei alvianiNo ratings yet
- Early Warning Score (EWS) clinical policiesDocument16 pagesEarly Warning Score (EWS) clinical policiesmiftachul munirohNo ratings yet
- Pain Management GuidelinesDocument3 pagesPain Management GuidelinesMr. BamsNo ratings yet
- ESI ER CompleteDocument45 pagesESI ER Completetammy2121No ratings yet
- Sample RRTEducation Training Packet CHIDocument13 pagesSample RRTEducation Training Packet CHIReza Badruun Syahrul HakimNo ratings yet
- Ews Workshop Jcca Nov 2016Document56 pagesEws Workshop Jcca Nov 2016rezaNo ratings yet
- Policy of Alergy and Adverse Drug ReactionDocument4 pagesPolicy of Alergy and Adverse Drug ReactiondmuscleNo ratings yet
- Early Warning SystemDocument7 pagesEarly Warning SystemajengsatyaNo ratings yet
- Principles of Monitoring Postoperative Patients: Oleh: Meity Sarah 2012610108Document8 pagesPrinciples of Monitoring Postoperative Patients: Oleh: Meity Sarah 2012610108Jefry ArieNo ratings yet
- Nurse-Administered Early Warning Score SystemDocument5 pagesNurse-Administered Early Warning Score SystemzakyNo ratings yet
- I PassDocument43 pagesI PassAnmol shresthaNo ratings yet
- Mews ScoreDocument13 pagesMews Score2009nicoleta100% (2)
- Chapter 2: Emergency Triage and Rapid AssessmentDocument6 pagesChapter 2: Emergency Triage and Rapid AssessmentsafwanNo ratings yet
- Adult Vital Sign ProtocolDocument10 pagesAdult Vital Sign ProtocolMegersa AleneNo ratings yet
- Asesment Conditional 06Document8 pagesAsesment Conditional 06Abdul WakhidNo ratings yet
- Triage System in Accident and EmergencyDocument8 pagesTriage System in Accident and EmergencySherry SinghNo ratings yet
- Moore RDocument7 pagesMoore RElaine IllescasNo ratings yet
- Eastern Health MET PolicyDocument6 pagesEastern Health MET Policyhamad abdulla mohamed abdullaNo ratings yet
- Transitions of CareDocument3 pagesTransitions of Caredelap05No ratings yet
- Early Warning System Lowers Mortality RateDocument9 pagesEarly Warning System Lowers Mortality RateAnasthasia hutagalungNo ratings yet
- Au Yit MoyDocument27 pagesAu Yit Moyasraf amirullahNo ratings yet
- Pediatric Early Warning ScorecardDocument1 pagePediatric Early Warning ScorecardMuh NatsirNo ratings yet
- Scoping Review of Pediatric Early Warning SystemsDocument29 pagesScoping Review of Pediatric Early Warning SystemsCantika SRNo ratings yet
- Children's Early Warning ToolDocument7 pagesChildren's Early Warning ToolYwagar YwagarNo ratings yet
- Experiment10 Adverse Drug Reaction MonitoringDocument3 pagesExperiment10 Adverse Drug Reaction MonitoringGelieNo ratings yet
- HuhuhuhDocument2 pagesHuhuhuhHAIDER JULAILINo ratings yet
- PALS UptodateDocument41 pagesPALS UptodateAnmol shresthaNo ratings yet
- NyeriDocument4 pagesNyeriRizka Yuliasih KussantyNo ratings yet
- ICU Nurse Job <40Document9 pagesICU Nurse Job <40Bruk AmareNo ratings yet
- Patient Assessment PolicyDocument7 pagesPatient Assessment Policysyed ishan ahmedNo ratings yet
- Early-Warning-Score (June 2013) PDFDocument8 pagesEarly-Warning-Score (June 2013) PDFluckyoluzNo ratings yet
- Qi-Project FinalDocument10 pagesQi-Project Finalapi-253211220No ratings yet
- SLR Ventilator Weaning Education PresentationDocument48 pagesSLR Ventilator Weaning Education Presentationfallenczar100% (1)
- Screening for Medical Referral in Physical TherapyDocument27 pagesScreening for Medical Referral in Physical Therapysaba ramzanNo ratings yet
- Lanjutan Chapter 2 SDocument2 pagesLanjutan Chapter 2 SGusna Khairani PanggabeanNo ratings yet
- Monitoring The Critically Ill PatientDocument4 pagesMonitoring The Critically Ill PatientAh ZhangNo ratings yet
- Chapter 2 PEY-Measurement of Outcomes - Pharma DostDocument50 pagesChapter 2 PEY-Measurement of Outcomes - Pharma DostKhadeer AG50% (2)
- CMRP0218Document14 pagesCMRP0218cherish60126No ratings yet
- Textbook of Urgent Care Management: Chapter 16, Urgent Care Duties, Staffing Mix and RatiosFrom EverandTextbook of Urgent Care Management: Chapter 16, Urgent Care Duties, Staffing Mix and RatiosNo ratings yet
- Hasil Output LengkapDocument9 pagesHasil Output LengkapYulia DeriniNo ratings yet
- Ska - Ah PDFDocument13 pagesSka - Ah PDFYulia DeriniNo ratings yet
- Lampiran Uji Valid Titik - 082926Document10 pagesLampiran Uji Valid Titik - 082926Yulia DeriniNo ratings yet
- Pelatihan Early Warning System (EWS)Document21 pagesPelatihan Early Warning System (EWS)Yulia DeriniNo ratings yet
- Surat UndanganDocument1 pageSurat UndanganYulia DeriniNo ratings yet
- Katalog Hard CoverrDocument16 pagesKatalog Hard CoverrYulia DeriniNo ratings yet
- Covid Severe PregnancyDocument7 pagesCovid Severe PregnancyYulia DeriniNo ratings yet
- Kayu Manis RT RW Kelurahan DataDocument48 pagesKayu Manis RT RW Kelurahan DataYulia DeriniNo ratings yet
- Webinar 13-14 Nov'2021Document4 pagesWebinar 13-14 Nov'2021Yulia DeriniNo ratings yet
- JADWAL PELAKSANAAN KEGIATAN BIAS DT & TD TINGKAT SD/MI UPT PUSKESMAS TAJURHALANG 2021Document2 pagesJADWAL PELAKSANAAN KEGIATAN BIAS DT & TD TINGKAT SD/MI UPT PUSKESMAS TAJURHALANG 2021Yulia DeriniNo ratings yet
- Webinar 13-14 Nov'2021Document4 pagesWebinar 13-14 Nov'2021Yulia DeriniNo ratings yet
- 3ms Squence 3 (Summary)Document3 pages3ms Squence 3 (Summary)toumi khadidjaNo ratings yet
- Australian Institute For Teaching and School Leadership - AITSLDocument5 pagesAustralian Institute For Teaching and School Leadership - AITSLYu LiNo ratings yet
- SP Manual Addendum For OS 3 - 03Document2 pagesSP Manual Addendum For OS 3 - 03kevmac88No ratings yet
- Tugas 3vDocument4 pagesTugas 3vRomie SyafitraNo ratings yet
- CEO Corner New Products Powerful Pocket SimulatorDocument23 pagesCEO Corner New Products Powerful Pocket SimulatorMOHAMMA MUSANo ratings yet
- Vernacular Terms in Philippine ConstructionDocument3 pagesVernacular Terms in Philippine ConstructionFelix Albit Ogabang IiiNo ratings yet
- MF ISIN CodeDocument49 pagesMF ISIN CodeshriramNo ratings yet
- 32 Productivity Increase in A PeirceSmith Convert 153013Document14 pages32 Productivity Increase in A PeirceSmith Convert 153013amirlpNo ratings yet
- Exercise 1: Chọn đáp án đúng:: Buổi 9: Động từ khuyết thiếu (Modal verb)Document6 pagesExercise 1: Chọn đáp án đúng:: Buổi 9: Động từ khuyết thiếu (Modal verb)Huyền HồNo ratings yet
- ES Model Question Paper With Solution KeyDocument10 pagesES Model Question Paper With Solution Keyvidhya_bineeshNo ratings yet
- C Pid3 009Document9 pagesC Pid3 009Youssef EBNo ratings yet
- Ultrasonic Couplant MSDSDocument2 pagesUltrasonic Couplant MSDSAnonymous uhqwokAeU0No ratings yet
- AP Poetry TermsDocument8 pagesAP Poetry TermsTEACHER BARAY LLCE ANGLAISNo ratings yet
- CPA Review Module on Accounting Standards and RegulationDocument13 pagesCPA Review Module on Accounting Standards and RegulationLuiNo ratings yet
- MJP Rate Schedule for Water Supply Pipeline ProjectDocument6 pagesMJP Rate Schedule for Water Supply Pipeline ProjectJalal TamboliNo ratings yet
- Investigation of Nursing Students Knowledge of and Attitudes About Problem Based LearningDocument4 pagesInvestigation of Nursing Students Knowledge of and Attitudes About Problem Based LearningasdasdasdasNo ratings yet
- Chapin - Advanced Tech For Modern Drummer - SAMPLEDocument5 pagesChapin - Advanced Tech For Modern Drummer - SAMPLEhokoNo ratings yet
- San Lam Stratus FundsDocument2 pagesSan Lam Stratus FundsTiso Blackstar GroupNo ratings yet
- Taxation Management AssignmentDocument11 pagesTaxation Management AssignmentniraliNo ratings yet
- 3M SS Filters Data SheetDocument4 pages3M SS Filters Data SheetbinnisfquoteNo ratings yet
- Contoh Skripsi Bahasa Inggris Case StudyDocument18 pagesContoh Skripsi Bahasa Inggris Case StudyRizki Fajrita100% (14)
- Korean Enthusiasm and PatriotismDocument68 pagesKorean Enthusiasm and PatriotismYukino Hera100% (1)
- Inv 069 1701757527Document1 pageInv 069 1701757527neetu9414576916No ratings yet
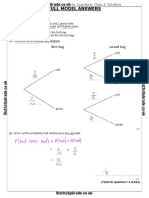
- Probability Tree Diagrams Solutions Mathsupgrade Co UkDocument10 pagesProbability Tree Diagrams Solutions Mathsupgrade Co UknatsNo ratings yet
- The 9 Building Blocks of Business ModelsDocument3 pagesThe 9 Building Blocks of Business ModelsTobeFrankNo ratings yet
- Document Revision TableDocument11 pagesDocument Revision Tableseva1969No ratings yet