Professional Documents
Culture Documents
Comparison of The Efficacy and Safety
Uploaded by
yun baiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Comparison of The Efficacy and Safety
Uploaded by
yun baiCopyright:
Available Formats
Zeitschrift für
Rheumatologie
Originalien
Z Rheumatol
https://doi.org/10.1007/s00393-022-01315-0
Accepted: 12 December 2022
Comparison of the efficacy and
© The Author(s), under exclusive licence to safety of tocilizumab, sarilumab,
Springer Medizin Verlag GmbH, ein Teil von
Springer Nature 2023 and olokizumab in patients with
Redaktion
Ulf Müller-Ladner, Bad Nauheim
Uwe Lange, Bad Nauheim
active rheumatoid arthritis:
a network meta-analysis of
randomized controlled trials
Young Ho Lee1,2 · Gwan Gyu Song1
1
Department of Rheumatology, Korea University College of Medicine, Seoul, Korea (Republic of)
2
Division of Rheumatology, Department of Internal Medicine, Korea University Anam Hospital, Korea
University College of Medicine, Seongbuk-gu, Korea (Republic of)
Abstract
Objective: This study compared the relative efficacy and safety of olokizumab,
tocilizumab, and sarilumab in rheumatoid arthritis (RA) patients who were intolerant
or responding inadequately to methotrexate (MTX).
Methods: We performed a Bayesian network meta-analysis to combine direct and
indirect evidence from randomized controlled trials (RCTs) to examine the efficacy and
safety of olokizumab, tocilizumab, and sarilumab in RA patients who were intolerant or
responding inadequately to MTX.
Results: Six RCTs comprising 4439 patients met the inclusion criteria. Tocilizumab,
sarilumab, olokizumab, and adalimumab treatments achieved a significant American
College of Rheumatology 20% (ACR20) response rate compared with placebo. However,
tocilizumab was associated with the most favorable surface area using the cumulative
ranking curve (SUCRA) for the ACR20 response rate. The ranking probability based
on the SUCRA indicated that tocilizumab treatment had the highest probability of
providing the best ACR20 response rate, followed by sarilumab, olokizumab every
2 weeks (Q2W), olokizumab Q4W, adalimumab 40 mg, and placebo. The ACR50 and 70
response rates showed a distribution pattern similar to that of the ACR20 response rate.
However, olokizumab Q4W had a higher ranking probability than olokizumab Q2W.
The SUCRA rating showed that the placebo was the best intervention with the least
adverse events (AEs) and withdrawal due to AEs, followed by interleukin-6 inhibitors.
Conclusion: Tocilizumab, sarilumab, and olokizumab are more effective than
adalimumab and have similar efficacy and safety in RA patients with inadequate
responses to MTX.
Keywords
Tocilizumab · Sarilumab · Olokizumab · Rheumatoid arthritis · Network meta-analysis
Scan QR code & read article online
Zeitschrift für Rheumatologie 1
Originalien
Table 1 Characteristics of the individual studies included in the network meta-analysis
Study Subjects Total Drugs No. of No. No. No. No. of seri- No. of withl
number patients achieving achieving achieving ous adverse drawal due to
ACR20 ACR50 ACR70 events adverse events
A. Olokizumab
Smolen MTX-IRa 1648 Olokizumab Q2W 464 344 234 133 324 21
2022 [30] Olokizumab Q4W 479 342 240 129 338 30
Adalimumab 462 319 214 119 302 26
Placebo 243 113 55 27 154 9
Nasonov MTX-IRa 428 Olokizumab Q2W 143 98 61 28 83 7
2022 [24] Olokizumab Q4W 142 101 69 32 81 5
Placebo 143 49 11 3 62 1
B. Tocilizumab
Yazici 2012 DMARD-IR 614 Tocilizumab 409 184 123 65 290 27
[35] Placebo 205 52 23 4 122 8
Nishimoto MTX-IRa 125 Tocilizumab 61 49 30 18 37 2
2009 [25] Placebo 64 16 7 4 17 3
Smolen MTX-IRa 409 Tocilizumab 205 120 90 45 143 16
2008 [29] Placebo 204 54 22 4 129 13
Genovese DMARD-IR 1216 Tocilizumab 803 488 302 165 584 31
2008 [12] Placebo 413 101 37 12 253 8
C. Sarilumab
Bumester MTX-IR 597 Sarilumab 200 mg 184 132 84 43 9 11
2016 [4] Adalimumab 185 108 55 22 12 13
Placebob 398a 133 68 28 23 20
Fleischmann TNF 365 Sarilumab 200 mg 184 265 75 100 48 17
2016 [9] blocker-IR Placebo 181 133 33 28 23 8
Genovese MTX-IR 797 Sarilumab 200 mg 399 112 184 30 10 59
2015 [11] Placebo 398 61 68 13 6 20
Huizinga MTX-IR 104 Sarilumab 200 mg 52 34 21 9 0 4
2014 [15] Placebo 52 24 8 1 2 2
ACR20, 50, 70 American College of Rheumatology 20%, 50%, or 70% response rate, MTX methotrexate, IR incomplete response, Q2W Every 2 weeks,
Q4W Every 4 weeks, DMARD disease-modifying anti-rheumatic drug
a
An inadequate response to MTX or intolerant to or inappropriate for MTX. All patients received conventional synthetic DMARD(s)
b
For network meta-analysis, data of placebo plus MTX was included from the study by Genovese et al. [11]
Table 2 Study numbers of biological
agents Introduction Notably, interleukin-6 (IL-6) is over-
Treatment Study Number of expressed in RA-affected tissues [26].
number patients Rheumatoid arthritis (RA) is a systemic Elevated IL-6 levels in the blood and syn-
Placebo 11 2381 autoimmune disease that causes persis- ovial fluid have been linked to synovitis,
Olokizumab Q2W 2 607 tent synovial joint inflammation, resulting systemic inflammation, bone metabolism,
Olokizumab Q4W 2 621 in disability and a poorer quality of life and joint deterioration [32]. Tocilizumab,
Tocilizumab 4 1478 [16, 18]. Conventional synthetic disease- a humanized anti-human IL-6 receptor
Adalimumab 2 647 modifying antirheumatic medications monoclonal antibody, is used to treat
Sarilumab 200 mg 5 899 (csDMARDs), such as methotrexate (MTX), individuals who have not responded to
are used to treat RA. Although MTX is tumor necrosis factor inhibitors or MTX.
Q2W every 2 weeks, Q4W every 4 weeks
a successful DMARD [8, 17], not all pa- It is used either alone or in combination
tients respond to this drug and 30% quit with MTX [29]. Sarilumab is a fully human,
treatment within a year of starting it, anti-IL-6 receptor α (IL-6Rα) monoclonal
often due to a lack of effectiveness or antibody that binds specifically to both
unacceptable side effects [2]. Patients soluble and membrane-bound IL-6 recep-
who do not respond to MTX are treated tors [10]. Olokizumab, a novel humanized
with biological DMARDs (bDMARDs). monoclonal antibody specific for IL-6, has
been developed to treat RA [9]. It binds
2 Zeitschrift für Rheumatologie
Table 3 Network meta-analysis of the efficacy of all comparators along with odds ratios (upper number in each cell) and 95% credible interval (range)
A. ACR20. OR > 1 signifies that the treatment in the top left is better
Tocilizumab – – – – –
1.01 (0.77–1.32) Sarilumab 200 mg – – – –
1.16 (0.84–1.59) 1.15 (0.84–1.57) Olokizumab Q2W – – –
1.25 (0.91–1.71) 1.24 (0.91–1.68) 1.08 (0.84–1.39) Olokizumab Q4W – –
1.51 (1.12–2.02) 1.50 (1.13–1.97) 1.30 (1.01–1.68) 1.20 (0.94–1.55) Adalimumab –
4.12 (3.42–4.97) 4.09 (3.38–4.95) 3.55 (2.76–4.60) 3.29 (2.56–4.24) 2.74 (2.18–3.42) Placebo
B. ACR50
Tocilizumab – – – – –
1.24 (0.90–1.71) Sarilumab 200 mg – – – –
1.40 (0.97–2.01) 1.13 (0.82–1.55) Olokizumab Q4W – – –
1.46 (1.02–2.10) 1.18 (0.86–1.62) 1.04 (0.83–1.31) Olokizumab Q2W – –
1.89 (1.34–2.69) 1.53 (1.14–2.04) 1.36 (1.07–1.72) 1.30 (1.02–1.64) Adalimumab –
5.53 (4.34–7.13) 4.47 (3.64–5.51) 3.97 (3.04–5.17) 3.80 (2.91–4.95) 2.93 (2.29–3.72) Placebo
C. ACR70
Tocilizumab – – – – –
2.34 (1.45–3.82) Sarilumab 200 mg – – – –
3.03 (1.79–5.16) 1.29 (0.85–1.95) Olokizumab Q2W – – –
3.13 (1.85–5.29) 1.33 (0.88–2.02) 1.04 (0.80–1.33) Olokizumab Q4W – –
3.78 (2.26–6.32) 1.61 (1.10–2.36) 1.25 (0.95–1.65) 1.20 (0.92–1.59) Adalimumab –
10.16 (7.01–15.12) 4.34 (3.25–5.82) 3.36 (2.40–4.79) 3.25 (2.32–4.62) 2.70 (1.96–3.74) Placebo
to the IL-6 receptor site 3 and blocks the Methods (3) the study included patients diagnosed
interaction of IL-6 and IL-6 receptor dimer with RA based on the ACR criteria for
with the signal-transducing β-receptor Identification of eligible studies and RA [14] or the 2010 ACR/EULAR classifi-
subunit glycoprotein 130 of the receptor data extraction cation criteria [1]. The exclusion criteria
complex [28]. Olokizumab was shown were as follows: (1) studies that included
to be considerably more effective than We searched for studies that examined duplicate data and (2) studies that did
placebo in clinical studies of RA [24, 30]. the efficacy and safety of olokizumab, not contain adequate data for inclusion.
Olokizumab, similar to tocilizumab, sarilumab, and tocilizumab in patients The primary endpoint for efficacy was the
is an effective therapeutic drug in trials with active RA who had an inadequate number of patients who achieved an ACR
of individuals with RA with an insuffi- response to MTX or were intolerant to 20% (ACR20) response rate as a preferred
cient response to MTX. However, the MTX. A literature search was performed outcome measure for testing efficacy.
head-to-head effectiveness and safety of using MEDLINE, EMBASE, the Cochrane The primary safety outcome crucial for
tocilizumab, sarilumab, and olokizumab Controlled Trials Register, and the Ameri- assessing risks was the number of patients
has not been determined in these patients. can College of Rheumatology (ACR) and with serious adverse events (AEs). The
In the absence of direct comparison trials the European League Against Rheuma- secondary endpoint for efficacy was the
of the relevant comparators [12, 24, 25, tism (EULAR) conference proceedings to number of patients who achieved an ACR
29, 30, 35], information from random- identify available articles (up to Septem- 50% (ACR50) or 70% (ACR70) response
ized controlled trials (RCTs) of various ber 2022). The following keywords and rate. Data were extracted from the original
therapies must be combined to evaluate subject terms were used: “olokizumab,” studies by two independent reviewers.
the impact of different therapies. Using “tocilizumab,” “sarilumab,” and “RA.” All The secondary endpoint for efficacy was
a network meta-analysis, the current study references cited in the studies were re- the number of patients who withdrew
assessed the effectiveness and safety of viewed to identify additional reports owing to AEs. Any discrepancies between
tocilizumab, sarilumab, and olokizumab excluded from electronic databases. The reviewers were resolved by consensus.
in patients with active RA and insufficient inclusion criteria for RCTs in the present The following information was extracted
response to MTX. study were as follows: (1) the study from each study: first author; year of
compared olokizumab, tocilizumab, or publication; country of the study; doses
sarilumab with a placebo to treat active of IL-6 inhibitors and adalimumab; time
RA that inadequately responded to MTX; of outcome evaluation; and efficacy and
(2) the study provided endpoints for the safety outcomes at 12–24 weeks. We
clinical efficacy and safety of olokizumab, quantified the methodological qualities
tocilizumab, or sarilumab at 12–24 weeks; of the three included studies using Jadad
Zeitschrift für Rheumatologie 3
Originalien
ond best, and so on, or into a ranking for
each treatment called the “surface under
the cumulative ranking curve” (SUCRA)
[27]. SUCRA is expressed as a percentage
(e.g., a value of 100% for SUCRA would be
obtained when a particular treatment is
guaranteed to be the best, and a value of
0% would guarantee that it is the worst
treatment). League tables were used to
organize summary estimates by ranking
treatments according to the strength of
their impact on the outcome based on
their respective SUCRA values [27]. We
reported the pairwise odds ratio (OR)
and 95% credible interval (CrI or Bayesian
CI) and adjusted them for multiple-arm
trials. Pooled results were considered
statistically significant when the span of
the 95% CrI did not include 1.
Test for inconsistency
Inconsistency is the disagreement be-
tween direct and indirect evidence [7].
Therefore, an assessment of inconsistency
is crucial when conducting a network
meta-analysis [13]. To assess the network
inconsistency between the direct and in-
direct estimates in each loop, we plotted
the posterior mean deviance of individual
data points in the inconsistency model
against their posterior mean deviance in
the consistency model [34].
Results
Studies included in the meta-
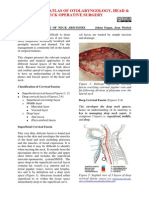
Fig. 1 8 Bayesian network meta-analysis of randomized controlled trials examining relative effec- analysis
tiveness according to the number of patients achieving the American College of Rheumatology 20%
response rate (ACR20) A total of 1005 studies were identified
through electronic or manual searches;
scores, with the quality classified as high the different arms were arranged based 33 were selected for a full-text review
(score of 3–5) or low (score of 0–2), and on the probability of the treatment to based on the title and abstract details.
conducted a network meta-analysis fol- be ranked as the best-performing regi- However, 23 studies were excluded be-
lowing the guidelines provided by the men. We adopted a Bayesian fixed-effects cause they were duplicates or irrelevant.
PRISMA statement [23]. model for network meta-analysis using Thus, 10 RCTs met the inclusion criteria [4,
NetMetaXL [3] and WinBUGS statistical 9, 11, 12, 15, 24, 25, 29, 30, 35]. The search
Evaluation of statistical associations analysis program, version 1.4.3 (MRC Bio- results contained ten pairwise compar-
for network meta-analysis statistics Unit, Institute of Public Health, isons, including seven direct comparisons,
Cambridge, UK). We used the Markov and five interventions. Various dosages of
The results from different arms were chain Monte Carlo method to obtain the the biologics were reported: olokizumab
analyzed simultaneously for RCTs that pooled effect sizes [5]. All chains were run at a dose of 64 mg was administered intra-
compared multiple doses of olokizumab, with 10,000 burn-in iterations followed by venously every 2 or 4 weeks (QW2, QW4);
tocilizumab, sarilumab, and placebo in 10,000 monitoring iterations. The relative tocilizumab at 8 mg/kg was administered
different arms. The efficacy and toler- effects were converted into a probability intravenously every 4 weeks; sarilumab
ability of the biologics and placebo in that a particular treatment was best, sec- 200 mg was administered subcutaneously
4 Zeitschrift für Rheumatologie
every 2 weeks; and adalimumab 40 mg
was administered subcutaneously every
2 weeks. The Jadad scores of the studies
were between 3 and 5, indicating high-
quality studies (. Tables 1 and 2). The rel-
evant features of the studies included in
the meta-analysis are listed in . Tables 1
and 2.
Network meta-analysis of the
efficacy of tocilizumab, sarilumab,
and olokizumab in RCTs
Tocilizumab is listed at the top left of the
diagonal of the league table (. Table 3) be-
causeitwas associated withthemostfavor-
able SUCRA for the ACR20 response rate.
Tocilizumab showed a significantly higher
ACR20 response rate compared with adal-
imumab or placebo (. Table 3; . Fig. 1).
Tocilizumab, sarilumab, olokizumab, and
adalimumab treatments achieved a signifi-
cant ACR20 response compared to placebo
(. Tables 3 and 4; . Fig. 1). SUCRA simpli-
fies information on the effect of each treat-
ment into a single number to guide the de-
cision-making process. The ranking prob-
ability based on the SUCRA indicated that
tocilizumab had the highest probability of
being considered the best treatment op-
tion for achieving the ACR20 response rate,
followed by sarilumab, olokizumab Q2W,
olokizumab Q4W, adalimumab 40 mg, and
placebo (. Table 5). The ACR50 and 70 re-
sponse rates showed a distribution pattern
similar to that of the ACR20 response rate,
except for olokizumab Q4W, which had
Fig. 1 8 (continued) Bayesian network meta-analysis of randomized controlled trials examining rela- a higher ranking probability than olok-
tive effectiveness according to the number of patients achieving the American College of Rheumatol- izumab Q2W (. Table 3).
ogy 50% response rate (ACR50)
Network meta-analysis of the safety
of tocilizumab, sarilumab, and
olokizumab in RCTs
Concerning AEs and withdrawal due to
AEs, the SUCRA rating likelihood showed
that placebo was the best intervention, fol-
lowed by IL-6 inhibitors (. Tables 4 and 6).
Olokizumab was associated with fewer
AEs than tocilizumab, while tocilizumab
was associated with fewer withdrawals
than olokizumab; the difference was not
statistically significant based on SUCRA
(. Table 6; . Fig. 2).
Zeitschrift für Rheumatologie 5
Originalien
Inconsistency and sensitivity
analysis
Inconsistency plots were used to assess
network inconsistencies between direct
and indirect estimates, revealing a low pos-
sibility of inconsistencies that might sig-
nificantly affect the network meta-analysis
results. This was confirmed using random-
and fixed-effects models, indicating that
the results of this network meta-analysis
were robust (. Fig. 1).
Discussion
We performed a network meta-analysis
to assess the effectiveness and safety of
tocilizumab, sarilumab, and olokizumab
in patients with active RA showing an
unsatisfactory response to MTX. Based
on ACR20 responses, our network meta-
analysis found that tocilizumab was the
most effective therapy for active RA that
did not respond well to MTX, followed by
sarilumab, olokizumab Q2W, olokizumab
Q4W, adalimumab 40 mg, and placebo.
The ACR50 and 70 response rates followed
a pattern similar to that of the ACR20 re-
sponse rate. No significant differences in
AEs or withdrawals due to AEs were iden-
tified among tocilizumab, sarilumab, and
olokizumab, indicating that both biologi-
cals had a comparable profile.
IL-6 binds to IL-6R to exert biological
effects; once this complex is established,
signaling pathways in the target cell may
be triggered [33]. Direct targeting of the
Fig. 1 8 (continued) Bayesian network meta-analysis of randomized controlled trials examining rela- cytokine or its receptor is a particular in-
tive effectiveness according to the number of patients achieving the American College of Rheumatol- hibitory mechanism of IL-6-blocking bi-
ogy 70% response rate (ACR70) ologics. Effective treatment of RA with
tocilizumab has led to developing new bi-
ologics targeting IL-6 or IL-6R. Different IL-
6 inhibitor, such as anti-IL-6R (sarilumab),
is effective in treating RA, regardless of
whether the specific inhibitory mechanism
involves direct cytokine or receptor target-
ing. Olokizumab is a direct inhibitor of the
IL-6 ligand, which distinguishes it from
already licensed IL-6 receptor inhibitors
[28]. Several antibodies targeting the IL-6
pathway have been developed in addition
to olokizumab [6, 22]. Targeted proteins
(IL-6 or IL6R), the targeted phase of the
IL-6 signaling complex cascade, method
of administration, immunoglobulin type,
6 Zeitschrift für Rheumatologie
Table 4 Network meta-analysis of the safety of all comparators along with odds ratios (upper number in each cell) and 95% credible interval (range)
A. Serious adverse events. OR < 1 signifies that the treatment at the top left is better
Olokizumab Q4W – – – – –
0.89 (0.46–1.69) Placebo – – – –
0.87 (0.47–1.63) 0.99 (0.53–1.86) Olokizumab Q2W – – –
0.71 (0.40–1.25) 0.80 (0.49–1.32) 0.82 (0.46–1.41) Adalimumab – –
0.61 (0.30–1.25) 0.69 (0.48–0.98) 0.70 (0.34–1.41) 0.86 (0.48–1.52) Sarilumab 200 mg –
0.59 (0.27–1.29) 0.66 (0.42–1.02) 0.67 (0.31–1.45) 0.83 (0.43–1.60) 0.96 (0.55–1.68) Tocilizumab
B. Withdrawal due to adverse events
Placebo – – – – –
0.64 (0.41–0.96) Tocilizumab – – – –
0.55 (0.29–1.02) 0.86 (0.40–1.84) Olokizumab Q2W – – –
0.48 (0.29–0.79) 0.75 (0.39–1.46) 0.87 (0.51–1.47) Adalimumab – –
0.44 (0.24–0.80) 0.69 (0.33–1.46) 0.81 (0.48–1.35) 0.92 (0.56–1.54) Olokizumab Q4W –
0.43 (0.30–0.60) 0.67 (0.39–1.18) 0.78 (0.40–1.54) 0.90 (0.52–1.56) 0.98 (0.51–1.87) Sarilumab 200 mg
Table 5 Rank probability of efficacy of Table 6 Rank probability ofsafety ofolok- and/or antibody design are all potential
olokizumab, tocilizumab, and sarilumab izumab, tocilizumab, and sarilumab based distinguishing criteria for these antibodies.
based on the number of patients who on the number of patients who experienced As the current investigation has several
achieved an ACR20, ACR50, and ACR70 re- serious adverse events and withdrawal due
limitations, our results should be inter-
sponse to adverse events
preted with caution. First, a 6-month fol-
Treatment SUCRA Treatment SUCRA
low-up of the safety profile of IL-6-blocking
A. ACR20 A. Adverse events
biologics was inadequate for determining
Tocilizumab 0.851 Olokizumab Q4W 0.802
all relevant safety issues connected with
Sarilumab 200 mg 0.841 Placebo 0.7269 biologicals, particularly for evaluating un-
Olokizumab Q2W 0.615 Olokizumab Q2W 0.654 common occurrences or events requiring
Olokizumab Q4W 0.474 Adalimumab 0.394 longer exposure durations. Second, the
Adalimumab 0.220 Sarilumab 200 mg 0.224 included studies varied in terms of design
Placebo 0.000 Tocilizumab 0.200 and clinical aspects. As a result, these inter-
B. ACR50 B. Withdrawal due to adverse events study differences may have affected our
Tocilizumab 0.970 Placebo 0.990 results. Third, this investigation did not
Sarilumab 200 mg 0.741 Tocilizumab 0.643 thoroughly discuss the effectiveness and
Olokizumab Q4W 0.582 Olokizumab Q2W 0.523 safety of the biologicals. Notably, because
Olokizumab Q2W 0.5027 Adalimumab 0.3543 of the low incidence of AEs, the number of
Adalimumab 0.205 Olokizumab Q4W 0.258 withdrawals due to AEs was insufficient to
Placebo 0.000 Sarilumab 200 mg 0.232 evaluate safety. Fourth, this meta-analysis
included only a limited number of studies.
C. ACR70 SUCRA surface under the cumulative rank-
ing curve, Q2W every 2 weeks, Q4W every This study had insufficient power to inves-
Tocilizumab 1.000
4 weeks tigate biologics’ relative effectiveness and
Sarilumab 200 mg 0.758
safety.
Olokizumab Q2W 0.533 However, this meta-analysis does offer
Olokizumab Q4W 0.479 meaningful information. First, the RCTs
Adalimumab 0.231 employed in this network meta-analysis
Placebo 0.000 were of good quality, with credible find-
ACR20 American College of Rheumatol- ings. Second, the number of patients in
ogy 20% response, ACR50 50% response, each sample ranged from 125 to 1648,
ACR70 70% response, SUCRA surface under
the cumulative ranking curve, Q2W every
with 4439 patients in this study. Third, net-
2 weeks, Q4W every 4 weeks work meta-analysis combines all relevant
data to enable simple head-to-head com-
parisons of various treatment approaches.
Finally, in contrast to individual tests, more
trustworthy and high-resolution findings
have been produced using statistical analy-
sis and by pooling separate research data
[19–21, 31]. To our knowledge, this is
Zeitschrift für Rheumatologie 7
Originalien
Fig. 2 8 Bayesian network meta-analysis of randomized controlled trials examining relative safety
according to the number of serious adverse events
8 Zeitschrift für Rheumatologie
Declarations
Conflict of interest. Y. Ho Lee and G. Gyu Song
declare that they have no competing interests.
For this article no studies with human participants
or animals were performed by any of the authors. All
studies mentioned were in accordance with the ethical
standards indicated in each case.
References
1. Aletaha D, Landewe R, Karonitsch T et al (2008)
Reporting disease activity in clinical trials of
patients with rheumatoid arthritis: EULAR/ACR
collaborative recommendations. Arthritis Care Res
59(10):1371–1377
2. Aletaha D, Smolen JS (2002) The rheumatoid
arthritis patient in the clinic: comparing more than
1,300 consecutive DMARD courses. Rheumatology
41(12):1367–1374
3. Brown S, Hutton B, Clifford T et al (2014)
A Microsoft-Excel-based tool for running and
critically appraising network meta-analyses—an
overview and application of NetMetaXL. Syst Rev
3(1):110
4. Burmester GR, Lin Y, Patel R et al (2016) Efficacy
and safety of sarilumab monotherapy versus
adalimumab monotherapy for the treatment
of patients with active rheumatoid arthritis
(MONARCH): arandomised, double-blind, parallel-
group phase III trial. Ann Rheum Dis. https://doi.
org/10.1136/annrheumdis-2016-210310
5. Caldwell DM, Ades A, Higgins J (2005) Simul-
taneous comparison of multiple treatments:
combining direct and indirect evidence. BMJ
331(7521):897
6. De Bruyn S, Gachalyi B, Rojkovich B et al (2012)
Anti-IL-6 receptor Nanobody (ALX-0061) seamless
“first-in-human” phase I/II POC study in patients
with active RA on stable MTX treatment. In:
Arthritis And Rheumatism. Wiley-Blackwell,
Hoboken
7. Dias S, Welton NJ, Sutton AJ et al (2013) Evidence
synthesis for decision making 4 inconsistency
in networks of evidence based on randomized
controlled trials. Med Decis Making 33(5):641–656
Fig. 2 8 (continued) Bayesian network meta-analysis of randomized controlled trials examining rela- 8. Felson DT, Anderson JJ, Meenan RF (1990) The
tive safety according to the number of withdrawals due to adverse events comparative efficacy and toxicity of second-line
drugs in rheumatoid arthritis. Results of two
metaanalyses. Arthritis Rheum 33(10):1449–1461
the first Bayesian network meta-analysis to who did not respond to MTX. Long-term 9. Fleischmann R, van Adelsberg J, Lin Y et al (2016)
systematically and concurrently examine trials involving a large number of patients Sarilumab and non-biologic disease-modifying
antirheumatic drugs in patients with active RA
tocilizumab, sarilumab, and olokizumab with active RA who do not respond effec- and inadequate response or intolerance to TNF
in patients with active RA intolerant to or tively to MTX are required to assess the inhibitors. Arthritis Rheumatol. https://doi.org/10.
not responding well to MTX. Until further relative effectiveness and safety of these 1002/art.39944
10. Genovese M, Fleischmann R, Fiore S et al
RCTs are conducted, this may be the best IL-6 inhibitors. (2013) SAT0117 sarilumab, a subcutaneously-
evidence available on this issue. administered, fully-human monoclonal antibody
inhibitor of the IL-6 receptor: relationship between
Corresponding address
eular responses and change from baseline of
Conclusion Young Ho Lee, MD, PhD selected clinical parameters. Ann Rheum Dis
Division of Rheumatology, Department of 72(Suppl 3):A620–A620
This Bayesian network meta-analysis 11. Genovese MC, Fleischmann R, Kivitz AJ et al
Internal Medicine, Korea University Anam
(2015) Sarilumab plus methotrexate in patients
demonstrated that tocilizumab, sarilumab, Hospital, Korea University College of Medicine with active rheumatoid arthritis and inadequate
and olokizumab are more efficacious than 73, Goryeodae-ro, 02841 Seongbuk-gu, Seoul, response to methotrexate: results of a phase III
Korea (Republic of) study. Arthritis Rheum 67(6):1424–1437
adalimumab. Further, tocilizumab, sar-
lyhcgh@korea.ac.kr 12. Genovese MC, McKay JD, Nasonov EL et al
ilumab, and olokizumab have comparable (2008) Interleukin-6 receptor inhibition with
efficacy and safety in patients with RA tocilizumabreducesdiseaseactivityinrheumatoid
Zeitschrift für Rheumatologie 9
Zusammenfassung
arthritis with inadequate response to disease-
modifyingantirheumaticdrugs: theTocilizumabin Vergleich der Wirksamkeit und Sicherheit von Tocilizumab, Sarilumab
Combination With Traditional Disease-Modifying und Olokizumab bei Patienten mit aktiver rheumatoider Arthritis:
Antirheumatic Drug Therapy study. Arthritis
Rheumatol 58(10):2968–2980 Netzwerk-Metaanalyse von randomisierten kontrollierten Studien
13. Higgins J, Jackson D, Barrett J et al (2012)
Consistency and inconsistency in network meta- Ziel: In der vorliegenden Studie wurde die relative Wirksamkeit und Sicherheit von
analysis: concepts and models for multi-arm Olokizumab, Tocilizumab und Sarilumab bei Patienten mit rheumatoider Arthritis (RA)
studies. Res Synth Methods 3(2):98–110 verglichen, bei denen eine Unverträglichkeit und unzureichende Therapieantwort auf
14. Hochberg MC, Chang RW, Dwosh I et al (1992) The
Methotrexat (MTX) bestand.
American College of Rheumatology 1991 revised
criteria for the classification of global functional Methoden: Es wurde eine Bayes-Netzwerk-Metaanalyse durchgeführt, um direkte und
status in rheumatoid arthritis. Arthritis Rheum indirekte Evidenz aus randomisierten kontrollierten Studien (RCT) für die Untersuchung
35(5):498–502 der Wirksamkeit und Sicherheit von Olokizumab, Tocilizumab und Sarilumab bei
15. HuizingaTW,FleischmannRM,JassonMetal(2014)
Sarilumab, a fully human monoclonal antibody
RA-Patienten zu kombinieren, bei denen eine Unverträglichkeit und unzureichende
againstIL-6Rα inpatientswithrheumatoidarthritis Therapieantwort auf Methotrexat (MTX) bestand.
and an inadequate response to methotrexate: Ergebnisse: Die Einschlusskriterien wurden von 6 RCT mit 4439 Patienten erfüllt.
efficacy and safety results from the randomised Unter Therapie mit Tocilizumab, Sarilumab, Olokizumab und Adalimumab wurde
SARIL-RA-MOBILITY part A trial. Ann Rheum Dis
73(9):1626–1634
eine signifikante ACR20-Responserate (American College of Rheumatology 20 %) im
16. Kim H, Sung Y-K (2021) Epidemiology of rheuma- Vergleich mit Placebo erzielt. Jedoch ging Tocilizumab mit der günstigsten SUCRA
toid arthritis in Korea. J Rheum Dis 28(2):60–67 („surface area using the cumulative ranking curve“) für die ACR20-Responserate einher.
17. Kremer JM (2004) Toward a better under- Die Rankingwahrscheinlichkeit auf Grundlage der SUCRA zeigte, dass die Therapie
standing of methotrexate. Arthritis Rheum
50(5):1370–1382 mit Tocilizumab die höchste Wahrscheinlichkeit für die beste ACR20-Responserate
18. Lee Y-K, Bae S-C (2021) Mortality in Korean aufwies, es folgten Sarilumab, Olokizumab alle 2 Wochen (Q2W), Olokizumab
patients with rheumatoid arthritis. J Rheum Dis Q4W, Adalimumab 40 mg und Placebo. Die ACR50- und ACR70-Responseraten
28(3):113–118
wiesen ein Verteilungsmuster auf, das dem der ACR20-Responserate ähnlich war.
19. Lee YH, Bae SC, Choi SJ et al (2012) Associations
between interleukin-10 polymorphisms and Allerdings bestand für Olokizumab Q4W eine höhere Rankingwahrscheinlichkeit als für
susceptibility to rheumatoid arthritis: a meta- Olokizumab Q2W. Das SUCRA-Rating ergab, dass Placebo die beste Intervention mit
analysis. Mol Biol Rep 39(1):81–87 den wenigsten unerwünschten Ereignissen (AE) und Therapieabbruch aufgrund von
20. Lee YH, Bae SC, Song GG (2011) The efficacy and
safety of rituximab for the treatment of active
AE war, es folgten Interleukin(IL)-6-Inhibitoren.
rheumatoid arthritis: a systematic review and Schlussfolgerung: Tocilizumab, Sarilumab und Olokizumab sind wirksamer als
meta-analysis of randomized controlled trials. Adalimumab und weisen eine ähnliche Wirksamkeit und Sicherheit bei RA-Patienten
Rheumatol Int 31(11):1493–1499 mit unzureichender Therapieantwort auf MTX auf.
21. Lee YH (2018) An overview of meta-analysis for
clinicians. Korean J Intern Med 33(2):277–283
22. Mease P, Strand V, Shalamberidze L et al (2012) Schlüsselwörter
A phase II, double-blind, randomised, placebo- Tocilizumab · Sarilumab · Olokizumab · Rheumatoide Arthritis · Netzwerk-Metaanalyse
controlled study of BMS945429 (ALD518) in
patients with rheumatoid arthritis with an
inadequate response to methotrexate. Ann
Rheum Dis 71(7):1183–1189 28. Shaw S, Bourne T, Meier C et al (2014) Discovery 35. Yazici Y, Curtis JR, Ince A et al (2012) Efficacy
23. Moher D, Liberati A, Tetzlaff J et al (2009) Preferred and characterization of olokizumab: a humanized of tocilizumab in patients with moderate to
reporting items for systematic reviews and meta- antibody targeting interleukin-6 and neutralizing severe active rheumatoid arthritis and a previous
analyses: the PRISMA statement. Ann Intern Med gp130-signaling. In: MAbs. Taylor & Francis, pp inadequate response to disease-modifying an-
151(4):264–269 773–781 tirheumatic drugs: the ROSE study. Ann Rheum Dis
24. Nasonov E, Fatenejad S, Feist E et al (2022) 29. Smolen JS, Beaulieu A, Rubbert-Roth A et al 71(2):198–205
Olokizumab, a monoclonal antibody against (2008) Effect of interleukin-6 receptor inhibition
interleukin 6, in combination with methotrexate with tocilizumab in patients with rheuma-
in patients with rheumatoid arthritis inadequately toid arthritis (OPTION study): a double-blind,
controlled by methotrexate: efficacy and safety placebo-controlled, randomised trial. Lancet
results of a randomised controlled phase III study. 371(9617):987–997
Ann Rheum Dis 81(4):469–479 30. Smolen JS, Feist E, Fatenejad S et al (2022)
25. Nishimoto N, Miyasaka N, Yamamoto K et al Olokizumab versus placebo or adalimumab in
(2009) Study of active controlled tocilizumab rheumatoid arthritis. N Engl J Med 387(8):715–726
monotherapy for rheumatoid arthritis patients 31. Song GG, Bae SC, Lee YH (2014) Association
with an inadequate response to methotrexate of the MTHFR C677T and A1298C polymor-
(SATORI): significant reduction in disease activity phisms with methotrexate toxicity in rheumatoid
and serum vascular endothelial growth factor by arthritis: a meta-analysis. Clin Rheumatol
IL-6 receptor inhibition therapy. Mod Rheumatol 33(12):1715–1724
19(1):12–19 32. Srirangan S, Choy EH (2010) The role of interleukin
26. Nurnberg W, Haas N, Schadendorf D et al (1995) 6 in the pathophysiology of rheumatoid arthritis.
Interleukin-6 expressionintheskinofpatientswith Ther Adv Musculoskelet Dis 2(5):247–256
lupus erythematosus. Exp Dermatol 4(1):52–57 33. Tanaka T, Narazaki M, Kishimoto T (2014) IL-6 in
27. Salanti G, Ades A, Ioannidis JP (2011) Graphical inflammation, immunity, and disease. Cold Spring
methods and numerical summaries for presenting Harb Perspect Biol 6(10):a16295
results from multiple-treatment meta-analysis: 34. Valkenhoef G, Lu G, Brock B et al (2012) Automating
an overview and tutorial. J Clin Epidemiol network meta-analysis. Res Synth Methods
64(2):163–171 3(4):285–299
10 Zeitschrift für Rheumatologie
You might also like
- MSE Psychiatric InterviewingDocument26 pagesMSE Psychiatric InterviewingZonny PatelNo ratings yet
- DR Thomas Brown PH D Attention Deficit Disorder The Unfocused Mind in Children and AdultsDocument191 pagesDR Thomas Brown PH D Attention Deficit Disorder The Unfocused Mind in Children and AdultsjenNo ratings yet
- Radiation Safety in Nuclear Medicine: A Practical, Concise GuideFrom EverandRadiation Safety in Nuclear Medicine: A Practical, Concise GuideNo ratings yet
- Demonstrate Knowledge of The Stages of Child DevelopmentDocument64 pagesDemonstrate Knowledge of The Stages of Child DevelopmentAvaNo ratings yet
- Fetal Macrosomia ArtDocument14 pagesFetal Macrosomia Artanyka2No ratings yet
- Vertigo Physiology and Clinical AssessmentDocument63 pagesVertigo Physiology and Clinical AssessmentdraseemmishraNo ratings yet
- The Secret of Being HappyDocument282 pagesThe Secret of Being Happylcs1234678100% (3)
- The Skeletal SystemDocument5 pagesThe Skeletal Systemeducguide100% (1)
- 11.1 Multiple Choice Part I Questions: Chapter 11 The Cardiovascular SystemDocument33 pages11.1 Multiple Choice Part I Questions: Chapter 11 The Cardiovascular SystemmuryumNo ratings yet
- Adamgammadex Mai Bun Ca SugammadexDocument6 pagesAdamgammadex Mai Bun Ca SugammadexAdi CărbunaruNo ratings yet
- Slides - Lung-MAP & S1900E Webinar - FOR WEB - 10.26.20Document77 pagesSlides - Lung-MAP & S1900E Webinar - FOR WEB - 10.26.20gurjeetwadiaNo ratings yet
- Notes On Radiographic Contrast Agents: Basic PrinciplesDocument11 pagesNotes On Radiographic Contrast Agents: Basic PrinciplesHarsha Vijaykumar100% (1)
- Results of Treatment For Low-Grade Gliomas: Select Randomized TrialsDocument46 pagesResults of Treatment For Low-Grade Gliomas: Select Randomized Trialsana claraNo ratings yet
- A Novel Neuromuscular Blocker Binding AgentDocument9 pagesA Novel Neuromuscular Blocker Binding AgentMarius PapuricaNo ratings yet
- Davis Symposium AdvancesInSarcomaDocument55 pagesDavis Symposium AdvancesInSarcomaFernando SilalahiNo ratings yet
- Antiplatelet Pada ACSDocument22 pagesAntiplatelet Pada ACSRidyah Ning TyasNo ratings yet
- The Radiolytic Studies of Ceftriaxone in The Solid State: AbstractDocument6 pagesThe Radiolytic Studies of Ceftriaxone in The Solid State: AbstractWinona DavinaNo ratings yet
- Aac 35 7 1309Document6 pagesAac 35 7 1309Razaz FarougNo ratings yet
- Acs Jcim 0c00171Document61 pagesAcs Jcim 0c00171mnjagaNo ratings yet
- Stromectol PiDocument7 pagesStromectol PiZainul AnwarNo ratings yet
- Ling Et Al 2003 Mutations in Topoisomerase Genes of Fluoroquinolone Resistant Salmonellae in Hong KongDocument7 pagesLing Et Al 2003 Mutations in Topoisomerase Genes of Fluoroquinolone Resistant Salmonellae in Hong Kongren renNo ratings yet
- Drug Development and Industrial Pharmacy: Please Scroll Down For ArticleDocument7 pagesDrug Development and Industrial Pharmacy: Please Scroll Down For Articleapi-19973331No ratings yet
- Jurnal 3Document6 pagesJurnal 3sri AdhayaniNo ratings yet
- Types of BlottingDocument7 pagesTypes of Blottingporkodi sudhaNo ratings yet
- American J Hematol - 2023 - JoinerDocument4 pagesAmerican J Hematol - 2023 - Joinersalman mehriNo ratings yet
- SHENDU JAMAN IMRAN Barnabas2022 - Article - DevelopmentAndValidationOfStabDocument15 pagesSHENDU JAMAN IMRAN Barnabas2022 - Article - DevelopmentAndValidationOfStabLODH HITESHNo ratings yet
- Elecsyscyfra211 11820966122 en CanDocument5 pagesElecsyscyfra211 11820966122 en CanAgus SunardiNo ratings yet
- Aptamer Based Fluorometric Sulfamethazine Assay Based On The Use of Graphene Oxide Quantum Dots NO ADVDocument8 pagesAptamer Based Fluorometric Sulfamethazine Assay Based On The Use of Graphene Oxide Quantum Dots NO ADVNikola MicicNo ratings yet
- Terminalia Arjuna, A Herbal Remedy Against Environmental Carcinogenicity: An in Vitro and in Vivo StudyDocument7 pagesTerminalia Arjuna, A Herbal Remedy Against Environmental Carcinogenicity: An in Vitro and in Vivo StudyMahnoorNo ratings yet
- Zhang 2021Document8 pagesZhang 2021Magna Fitriani HutasuhutNo ratings yet
- Feline Non-Regenerative Immune-Mediated Anaemia: Features and Outcome in 15 CasesDocument7 pagesFeline Non-Regenerative Immune-Mediated Anaemia: Features and Outcome in 15 CasesTORRES GUTIERREZ JOYNY RAQUEL catedraticoNo ratings yet
- WHO Living Guideline Son Antivirals For COVID-19 Are Evidence Based - 2022Document3 pagesWHO Living Guideline Son Antivirals For COVID-19 Are Evidence Based - 2022GlauciaNo ratings yet
- Dosing Eculizumab For Antibody-Mediated Rejection in Kidney Transplantation: A Case ReportDocument7 pagesDosing Eculizumab For Antibody-Mediated Rejection in Kidney Transplantation: A Case Reportgoolpoll hieNo ratings yet
- Lauracornacchia TesiDocument106 pagesLauracornacchia Tesikedeng1307No ratings yet
- 107.11.1 GlycopeptidePK - 20181101 - GIOCP - Case - Part2Document4 pages107.11.1 GlycopeptidePK - 20181101 - GIOCP - Case - Part2ft84nzzc92No ratings yet
- Cefiderocol Resistance in Acinetobacter BaumanniiDocument4 pagesCefiderocol Resistance in Acinetobacter Baumanniiczikkely23No ratings yet
- 32817358: Efficacy and Safety of Adjunctive Lacosamide in The Treatment of Primary Generalised Tonic-Clonic Seizures A Double-Blind, Randomised, Placebo-Controlled TrialDocument9 pages32817358: Efficacy and Safety of Adjunctive Lacosamide in The Treatment of Primary Generalised Tonic-Clonic Seizures A Double-Blind, Randomised, Placebo-Controlled TrialEva Bastida MercadoNo ratings yet
- CV 20240403 JCC-14-1693Document30 pagesCV 20240403 JCC-14-1693Nejc KovačNo ratings yet
- Keaa 823Document7 pagesKeaa 823Andres CasteloNo ratings yet
- Comment: The Lancet OncologyDocument2 pagesComment: The Lancet OncologyRaul Matute MartinNo ratings yet
- Product Information: Adriamycin Solution For InjectionDocument18 pagesProduct Information: Adriamycin Solution For InjectionArya GuganNo ratings yet
- Antiplatelet Therapy September 2013Document31 pagesAntiplatelet Therapy September 2013Randilufti SantosoNo ratings yet
- Cancer Sarcoma Chemotherapy Regimen V2.1 May 2012Document75 pagesCancer Sarcoma Chemotherapy Regimen V2.1 May 2012Niken AmritaNo ratings yet
- Journal Terapi UTIDocument6 pagesJournal Terapi UTIprogiezNo ratings yet
- 542fa5ce-43f5-4f84-a986-20ac2f0fadb8Document7 pages542fa5ce-43f5-4f84-a986-20ac2f0fadb8ShresthNo ratings yet
- Mechanism-Based Inhibition of Cytochrome P450 3A4 by Therapeutic DrugsDocument26 pagesMechanism-Based Inhibition of Cytochrome P450 3A4 by Therapeutic DrugsAndzar Fikranus SNo ratings yet
- L12 - Cholinergics IIDocument24 pagesL12 - Cholinergics IIyasaira707No ratings yet
- Xofigo: Product MonographDocument29 pagesXofigo: Product Monographjuan_2234No ratings yet
- Pharmacology of Antithrombotic DrugsDocument58 pagesPharmacology of Antithrombotic DrugsSoda SodaNo ratings yet
- Computational Drug Repurposing Study Elucidating Simultaneous Inhibition of Entry and Replication of Novel Corona Virus by GrazoprevirDocument11 pagesComputational Drug Repurposing Study Elucidating Simultaneous Inhibition of Entry and Replication of Novel Corona Virus by GrazoprevirAlok JainNo ratings yet
- EANM Practice Guideline SNMMI Procedure Standard For RAIU and Thyroid ScintigraphyDocument12 pagesEANM Practice Guideline SNMMI Procedure Standard For RAIU and Thyroid ScintigraphyArif SatriaNo ratings yet
- Advanced Powder Technology: Kandasamy Saravanakumar, Myeong-Hyeon WangDocument9 pagesAdvanced Powder Technology: Kandasamy Saravanakumar, Myeong-Hyeon WangsilviaNo ratings yet
- Radio PharmaceuticalsDocument48 pagesRadio PharmaceuticalsKris Joy EbonNo ratings yet
- Effect of Omeprazole On The Metabolism of Cilostazol: Ajit Suri and Steven L. BramerDocument7 pagesEffect of Omeprazole On The Metabolism of Cilostazol: Ajit Suri and Steven L. BramerNurul Kamilah SadliNo ratings yet
- Insert - Elecsys CYFRA 21-1.07299966500.v7.enDocument5 pagesInsert - Elecsys CYFRA 21-1.07299966500.v7.enVegha NedyaNo ratings yet
- EtoricoxibDocument15 pagesEtoricoxibSree BanNo ratings yet
- Investigation of Dosimetric Parameters of HDR Cobalt60 Afterloadingbrachytherapy Source Using Monte Carlo Fluka Code 2155 9619 1000366Document6 pagesInvestigation of Dosimetric Parameters of HDR Cobalt60 Afterloadingbrachytherapy Source Using Monte Carlo Fluka Code 2155 9619 1000366orlando durandNo ratings yet
- 3D-QSAR and Docking Studies On PyrimidineDocument15 pages3D-QSAR and Docking Studies On PyrimidineLuis MartinezNo ratings yet
- 1 s2.0 S0969805119301076 MainDocument7 pages1 s2.0 S0969805119301076 Mainarifudin_achmadNo ratings yet
- Carole Mitnick EndtbDocument15 pagesCarole Mitnick Endtbeko kartiniNo ratings yet
- Pezaro 2014Document7 pagesPezaro 2014eir235dNo ratings yet
- SugammadexDocument18 pagesSugammadexSuresh KumarNo ratings yet
- 2460 Samanta 2021Document2 pages2460 Samanta 2021Aiswarya ShreeNo ratings yet
- Attack Journal Club PowerpointDocument18 pagesAttack Journal Club Powerpointapi-734449276No ratings yet
- Blood Transfusion Management For Patients Treated With Anti-CD38 Monoclonal AntibodiesDocument8 pagesBlood Transfusion Management For Patients Treated With Anti-CD38 Monoclonal AntibodiesenglaNo ratings yet
- 9th JC Paper - Katoh Et Al. Cardiovascular Safety of Mirabegron Add-On Therapy To Tamsulosin For The Treatment of Overactive Bladder in Men WithDocument10 pages9th JC Paper - Katoh Et Al. Cardiovascular Safety of Mirabegron Add-On Therapy To Tamsulosin For The Treatment of Overactive Bladder in Men WithWai Kit CheongNo ratings yet
- Applications of Zeeman Graphite Furnace Atomic Absorption Spectrometry in the Chemical Laboratory and in ToxicologyFrom EverandApplications of Zeeman Graphite Furnace Atomic Absorption Spectrometry in the Chemical Laboratory and in ToxicologyC. MinoiaNo ratings yet
- Protocols For The Analytical Characterization of Therapeutic Monoclonal Antibodies. I - Non-Denaturing Chromatographic Techniques PDFDocument15 pagesProtocols For The Analytical Characterization of Therapeutic Monoclonal Antibodies. I - Non-Denaturing Chromatographic Techniques PDFyun baiNo ratings yet
- Mass Spectrometry-Based Glycoprofiling of Biopharmaceuticals by Using An Automated Data Processing Tool - SimGlycan®Document10 pagesMass Spectrometry-Based Glycoprofiling of Biopharmaceuticals by Using An Automated Data Processing Tool - SimGlycan®yun baiNo ratings yet
- Multi Attribute Method Implementation Using A High Resolution Mass Spectrometry PlatformDocument22 pagesMulti Attribute Method Implementation Using A High Resolution Mass Spectrometry Platformyun baiNo ratings yet
- Cost-Effective and Disposable Label-Free Voltammetric Immunosensor For Sensitive Detection of Interleukin-6Document7 pagesCost-Effective and Disposable Label-Free Voltammetric Immunosensor For Sensitive Detection of Interleukin-6yun baiNo ratings yet
- 365 Ways To Dispose of Barney The Purple Toliet DinosaurDocument27 pages365 Ways To Dispose of Barney The Purple Toliet DinosaurEmmanuel Rei ZamoraNo ratings yet
- Cology of Pediatrics N GeriatricsDocument41 pagesCology of Pediatrics N GeriatricsGANESH KUMAR JELLA100% (1)
- Origen HipotoniaDocument7 pagesOrigen HipotoniaPablo Hernández MaripillánNo ratings yet
- Stress Dose SteroidsDocument4 pagesStress Dose SteroidsTitien fitria sholihati100% (1)
- Surgical Drainage of Deep Neck AbscessesDocument27 pagesSurgical Drainage of Deep Neck AbscessesIrma DamayantiNo ratings yet
- Medicine: Primary Testicular T-Lymphoblastic Lymphoma in A ChildDocument5 pagesMedicine: Primary Testicular T-Lymphoblastic Lymphoma in A ChildgalalNo ratings yet
- Pharmacology Respiratory DrugsDocument2 pagesPharmacology Respiratory DrugsM Youssif Elkady100% (1)
- Postpartum Depression: Beyond The BluesDocument33 pagesPostpartum Depression: Beyond The Bluesrevathidadam55555No ratings yet
- Striped Cucumber Beetle and Bacterial Wilt Management in Vine CropsDocument3 pagesStriped Cucumber Beetle and Bacterial Wilt Management in Vine CropsHasbi Yusuf Abu ZakiNo ratings yet
- Microcarrier Cell Culture ScaleUp Procedures HandbookDocument32 pagesMicrocarrier Cell Culture ScaleUp Procedures HandbookDolphingNo ratings yet
- Research Paper Topics Neonatal NursingDocument4 pagesResearch Paper Topics Neonatal Nursingzufehil0l0s2100% (1)
- Reviewer Hema LabDocument12 pagesReviewer Hema LabPatricia Jean RodriguezNo ratings yet
- Cross ReactivityDocument40 pagesCross ReactivityjanieinMNNo ratings yet
- ERCP CurriculumDocument17 pagesERCP CurriculumEvangelosNo ratings yet
- Scientific Writing, July 2012Document1 pageScientific Writing, July 2012Rahmat KurniawanNo ratings yet
- Impact of Covid-19Document9 pagesImpact of Covid-19adane yehualawNo ratings yet
- Components of CSHP: Polangui Community CollegeDocument9 pagesComponents of CSHP: Polangui Community CollegeJohn Albert AlejandrinoNo ratings yet
- San Joaquin Resources 2013-2014Document466 pagesSan Joaquin Resources 2013-2014api-22559015No ratings yet
- Table of ContentsDocument4 pagesTable of Contentssharmainerose17No ratings yet
- Reviews/Analyses: Iodine Deficiency Disorders in EuropeDocument9 pagesReviews/Analyses: Iodine Deficiency Disorders in EuropeSeta FadilaNo ratings yet
- 1 s2.0 S0928493122000443 MainDocument13 pages1 s2.0 S0928493122000443 MainmrshirafatimaNo ratings yet
- Protac 2Document14 pagesProtac 2muruganvvkNo ratings yet