Professional Documents
Culture Documents
Clinical Management of Inflammatory Bowel Disease in The Organ Recipient
Uploaded by
William Alexander Guzman MartinOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Clinical Management of Inflammatory Bowel Disease in The Organ Recipient
Uploaded by
William Alexander Guzman MartinCopyright:
Available Formats
Online Submissions: http://www.wjgnet.
com/esps/ World J Gastroenterol 2014 April 7; 20(13): 3525-3533
bpgoffice@wjgnet.com ISSN 1007-9327 (print) ISSN 2219-2840 (online)
doi:10.3748/wjg.v20.i13.3525 © 2014 Baishideng Publishing Group Co., Limited. All rights reserved.
TOPIC HIGHLIGHT
WJG 20th Anniversary Special Issues (3): Inflammatory bowel disease
Clinical management of inflammatory bowel disease in the
organ recipient
Amedeo Indriolo, Paolo Ravelli
Amedeo Indriolo, Paolo Ravelli, Digestive Endoscopy Unit, annual program of endoscopic surveillance with serial
Department of Gastroenterology, Papa Giovanni XXIII Hospital, biopsies for CRC is recommended. A prophylactic col-
24127 Bergamo, Italy ectomy in selected IBD/PSC patients with CRC risk fac-
Author contributions: Indriolo A and Ravelli P solely contrib- tors could be a good management strategy in the CRC
uted to this paper.
prevention, but it is used infrequently in the majority of
Correspondence to: Amedeo Indriolo, MD, Digestive Endos-
copy Unit, Department of Gastroenterology, Papa Giovanni XXIII LT centers. About 30% of patients develop multiple IBD
Hospital, Piazza OMS, 1, 24127 Bergamo, recurrence and 20% of patients require a colectomy
Italy. amedeo.indriolo@gmail.com after renal transplantation. Like in the liver transplanta-
Telephone: +39-35-2673407 Fax: +39-35-2674837 tion, anti-TNFα therapy could be an effective treatment
Received: September 28, 2013 Revised: November 6, 2013 in IBD patients with conventional refractory therapy
Accepted: January 19, 2014 after renal or heart transplantation. A large number
Published online: April 7, 2014 of patients are needed to confirm the preliminary ob-
servations. Regarding the higher clinical complexity of
this subgroup of IBD patients, a close multidisciplinary
approach between an IBD dedicated gastroenterologist
Abstract and surgeon and an organ transplantation specialist is
necessary in order to have the best clinical manage-
There was estimated a higher incidence of de novo
ment of IBD after transplantation.
inflammatory bowel disease (IBD) after solid organ
transplantation than in the general population. The
© 2014 Baishideng Publishing Group Co., Limited. All rights
onset of IBD in the organ transplant recipient popula-
reserved.
tion is an important clinical situation which is associ-
ated to higher morbidity and difficulty in the medical
therapeutic management because of possible interac- Key words: Inflammatory bowel disease; Ulcerative coli-
tion between anti-reject therapy and IBD therapy. IBD tis; Crohn’s disease; Primary sclerosing cholangitis; Liver
course after liver transplantation (LT) is variable, but transplantation; Heart transplantation; Renal transplan-
about one third of patients may worsen, needing an in- tation; Anti-tumor necrosis factor alpha therapy
crease in medical therapy or a colectomy. Active IBD at
the time of LT, discontinuation of 5-aminosalicylic acid Core tip: Inflammatory bowel disease (IBD) in the
or azathioprine at the time of LT and use of tacrolimus- organ transplant recipient population is an important
based immunosuppression may be associated with an clinical situation which is associated to higher morbidity
unfavorable outcome of IBD after LT. Anti-tumor necro- and difficulty in the medical therapeutic management
sis factor alpha (TNFα) therapy for refractory IBD may because of possible interaction between anti-reject
be an effective and safe therapeutic option after LT. therapy and IBD therapy. IBD course after liver trans-
The little experience of the use of biological therapy in plantation is variable, but about one third of patients
transplanted patients, with concomitant anti-rejection may worsen, needing an increase in medical therapy or
therapy, suggests there be a higher more careful sur- a colectomy. About 30% of patients develop multiple
veillance regarding the risk of infectious diseases, auto- IBD recurrence and 20% of patients require colectomy
immune diseases, and neoplasms. An increased risk of after renal transplantation. Like in the liver transplanta-
colorectal cancer (CRC) is present also after LT in IBD tion, anti-tumor necrosis factor alpha therapy could be
patients with primary sclerosing cholangitis (PSC). An an effective treatment in IBD patients with conventional
WJG|www.wjgnet.com 3525 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
refractory therapy after renal or heart transplantation. need of colectomy for acute IBD refractory to medical
therapy is nearly 9% (range, 0%-21%)[2-6]. Dvorchik et al[7]
observed a significant 3.1-fold increased risk of colec-
Indriolo A, Ravelli P. Clinical management of inflammatory tomy due to severe IBD flare up or medically refractory
bowel disease in the organ recipient. World J Gastroenterol 2014; disease after LT compared to IBD patients who did not
20(13): 3525-3533 Available from: URL: http://www.wjgnet. require LT.
com/1007-9327/full/v20/i13/3525.htm DOI: http://dx.doi.
org/10.3748/wjg.v20.i13.3525
De novo IBD
Wörns et al[8] evaluated 44 patients with IBD after solid
organ transplant (SOT) and reported the de novo disease:
38 of 44 (86%) cases occurred following LT (23) or
INTRODUCTION combined liver/kidney transplantation (15), 4 (9%) after
Inflammatory bowel disease (IBD) is a complex chronic heart transplantation, and 2 (5%) after kidney transplan-
inflammatory intestinal disease with a prevalence steadily tation. Riley et al[9] identified 14 patients who developed
increasing during the recent years. The management of de novo IBD in 6800 cases after liver and kidney transplan-
IBD is leaning towards more complex clinical situations, tation. Twelve (86%) of the patients developed IBD post
with possible interactions between the intestinal disease liver transplant and two (14%) were detected post kidney
and others organ diseases. The organ recipient popula- transplant. The authors estimated a higher incidence of de
tion is constantly increasing in the medical specialized novo IBD after SOT than in the general population (206 vs
centers in the world and it can happen that a patient with 20 cases per 100000 persons-year. The higher prevalence
a solid organ transplantation has a recurrence of IBD. of IBD post LT in the SOT patients can be related to the
This is particularly important in the liver transplantation strong association between PSC and UC. In these patients,
(LT) because there is a close pathophysiological correla- the 10-year risk of de novo IBD after LT is estimated to be
tion between primary sclerosing cholangitis (PSC) and 14%-30%, with median time to development of approxi-
ulcerative colitis (UC) before the transplant. De novo IBD mately 4 years (range, 1.1-7.1 years)[2-4]. After a median fol-
has been reported after solid organ transplantation, with low-up of 4 years 18/86 (21%) patients who underwent LT
an incidence estimated ten times higher with respect to for PSC developed IBD. Verdonk et al[3] observed that the
the expected incidence of IBD in the general population. de novo IBD patients tended to develop disease later in post-
Therefore, the organ recipient patient may be a new clini- transplant period than the patients with pre-existing IBD.
cal “scenario” for IBD management. Moreover, the patients with de novo IBD after LT respond
The first objective of this review was to examine better to medical therapy and none required colectomy.
the studies present in the English literature (PubMed)
about the natural history in organ recipient patients.In
RISK FACTORS FOR IBD AFTER LIVER
particular, we have evaluated: (1) risk of recurrent IBD;
(2) risk of de novo IBD; (3) need for colectomy; (4) risk of TRANSPLANTATION
pouchitis; and (5) risk of colorectal cancer. The second Clinical activity of IBD
objective was to examine the medical therapy for active The clinical activity of IBD at the time of LT may be a
IBD after organ transplantation. risk factor for worsening the intestinal disease after LT.
We have more knowledge of IBD clinical manage- In fact, a three-fold higher risk of IBD flare up after LT
ment after LT, but in this review we have evaluated the in patients with active IBD at the time of LT it was ob-
IBD studies after heart, renal, lung, and intestinal trans- served[3].
plantation.
Smoking
EPIDEMIOLOGY AND CLINICAL FEATURE Joshi et al[4] evaluated 110 patients underwent LT for PSC.
In the multivariate analysis, active smoking at the time of
OF IBD AFTER LIVER TRANSPLANTATION transplant was the only significant risk factor for flare up
Recurrent IBD of IBD post-transplantation (HR = 17; 95%CI: 2-180).
Singh et al[1] has recently examined the studies on the
natural history of IBD after LT for PSC, reporting 609 Cytomegalovirus
patients in 14 studies, followed approximately 4.8 years Cytomegalovirus (CMV) mismatch (seropositive donor,
after LT (range, 1.8-7.2 years), about 31% of patients seronegative recipient and CMV infection) have not been
have improvement of IBD activity, 39% of patients do associated with the recurrence of IBD after LT[4,10,11].
not have a significant change in IBD activity, and 30% of CMV mismatch was associated with a 4.5-fold higher risk
patients develop worsening IBD, requiring intensification of de novo IBD after LT, but CMV infection is not related
of medical therapy and/or surgery. The estimated risk to de novo IBD post LT[11].
of severe IBD flare up at 5 and 10 years after LT ranged
from 39% to 63% and 39% to 98%, with a median time Therapy of IBD after LT
of a flare up around 1 year (range, 0.3-8.6 years)[2-4]. The The therapy with proven efficacy for active IBD may re-
WJG|www.wjgnet.com 3526 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
Table 1 Interaction between inflammatory bowel disease
safety of anti-TNFα therapy in patients with refractory
therapy and anti-reject therapy in inflammatory bowel disease IBD following LT, but larger studies are needed to evalu-
patients after liver transplantation ate the safety profile of biological therapy combined with
anti rejection treatment.
Drug Efficacy Ref.
IBD therapy Anti-reject therapy
Anti-reject therapy
5-ASA + [3]
[12] Tracrolimus is the principal immunosuppresive agent in
Prednisone + + [12] SOT, but it has been observed, in retrospective studies,
[21] that it may be associated with a four-fold higher risk of
Azathioprine + + [2] post-LT IBD relapse[2,3]. In patients with tacrolimus for
Anti-TNFα + [15]
[16]
transplant-related immunosuppression, Dvorchik et al[7]
[13] found that the risk of relapse of IBD at 1- and 5-year
[14] was 13% and 64%, respectively; while, in patients with
[18] tacrolimus-free regimens, the risk of IBD was 4% and
Tacrolimus - + [2] 10%, respectively. The cause of a possible relationship
[3]
Cyclosporine + + [3]
between tacrolimus and IBD flare up after transplant is
Mycophenolate - + [22] not known. IBD results from inappropriate and ongoing
Mofetil [23] activation of the mucosal immune system in the presence
of normal luminal flora. Immunosuppression agents
TNFα: Tumor necrosis factor alpha; IBD: Inflammatory bowel disease; may promote infections which may lead to the change
5-ASA: 5-aminosalicylates. bacterial gut flora and decrease the intestinal barrier
function[19]. Moreover, tacrolimus is a strong inhibitor of
duce the risk of disease exacerbation post-LT (Table 1). interleukin-2 production. Deficiency of interleukin-2 can
result in T-cell dysregulation, leading to the development
5-aminosalicylates (5-ASA) therapy after LT appears
of intestinal chronic inflammation[2,4].
to be protective against the worsening disease activity of
Cyclosporine, like anti-TNFα, is the chosen drug
IBD, decreasing the flare up and/or colectomy risk about
in severe steroid refractory UC. Cyclosporine does not
80%[3,12]. seem to worsen the course of IBD after transplant[3,10].
Azathioprine may reduce the risk of active IBD after In contrast with tacrolimus, the frequency of interleukin-
transplant. In the study’s Haagsma et al[2], a comparison 2-expressing T cells was significantly higher with cyclo-
between 55 patients who received azathioprine with the sporine in renal transplant patients[20]. This may explain
23 patients did not receive azathioprine, was performed in part the different effect of ciclosporine and tacrolimus
and this showed a significantly higher IBD-free survival on IBD course after transplant.
for azathioprine group. In particular, at 1, 3 and 5 years Corticosteroids are effective in acute and chronic
after LT, the IBD-free survival rates in patients receiving prevention of SOT rejection as well as in inducing clinical
azathioprine were 96%, 96% and 88%, respectively; while remission in IBD. Moncrief et al[21] and Navaneethan et al[12]
in patients not receiving azathioprine, these value were observed that prednisone therapy may favorably modify
87%, 63% and 54%, respectively. the course of IBD after LT, but this therapeutic regime is
We have little knowledge about the use of anti-tumor associated to important side effects.
necrosis factor alpha (TNF α) therapy for refractory Mycophenolate mofetil (MMF) has proven efficacy in
IBD after transplant. To date, there have been only 22 SOT, but its role in IBD is not clear[22,23]. Moreover, MMF
patients treated with anti-TNF for relapsing IBD follow- is associated with enterocolitis, which can mimic a IBD
ing LT; this number includes patients with UC, Crohn’s flare up.
disease, indeterminate colitis and pouchitis, treated with
infliximab or adalimumab (Table 2)[13-18]. In our study, we
COLECTOMY POST-LIVER
evaluated the efficacy and safety of infliximabtherapy in a
homogeneous series of four patients with refractory UC TRANSPLANTATION
following LT, followed for a median time of 18 mo. At Ho et al[24] observed a prevalence of colectomy after LT
week 54, three patients (75%) experienced sustained im- about 35%. In this Scottish study 7 of 20 patients under-
provement of IBD. Complete mucosal healing (defined as went colectomy with a median time of 3.4 years (range
absence of lesions) was observed in one of three patients 1.5-6.3 years) following LT[24]. The indication for colec-
(33%). Steroid treatment was successfully withdrawn tomy was chronically active severe UC in three patients
during infliximab therapy in all patients. Adverse events (43%), colonic dysplasia or colorectal cancer in three pa-
included only one infection by Molluscum contagiosum, tients (43%) and benign stricture of colon in one patient
which resolved without sequelae. No malignancies were (14%).The study in Cleveland compared 86 patients with
observed in any patient following infliximab therapy. No UC and LT for PSC with 81 patients with UC and PSC
cases of hepatic rejection were documented. Our results who did not require LT[25]. The necessity of colectomy
are in line with others studies about the efficacy and was significantly more frequently in the non-LT group
WJG|www.wjgnet.com 3527 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
Table 2 Anti-tumor necrosis factor alpha therapy for management of refractory inflammatory bowel disease after liver transplantation
Author Number LT patients Clinical outcome Endoscopic outcome Adverse events
Sandhu et al[13] 6 Response: 67% - Systemic lupus erythematosus
Colorectal cancer
Mohabbat et al[14] 8 Response: 87.5% Mucosal healing: 42.9% Oral candidiasis
Clostridium difficile colitis
Bacterial pmeumonia
Cryptosporidiosis
Post-tansplant lympho-proliferative disorder
Lal et al[15] 1 Response: 100% Improvement: 100% No
El-Nachef et al[16] 2 Response: 100% - No
Indriolo et al[18] 4 Response: 75% Mucosal healing: 33% Molluscum contagiosum
than the LT group (76.5% vs 34.9%). The percentage of fore, the combination of IBD and PSC after LT leads the
patients which underwent colectomy for steroid depen- patient to a higher risk in developing CRC.
dent/refractory disease was lower in the LT group than Moreover, the CRC risk is increased in patients with
patients in the non-LT group (39.9% vs 48.4%). Regard- long-standing IBD, long-standing LT and extensive colon-
ing the possible difficulties to surgically pack the J pouch ic involvement[32,35,45]. In fact, it was observed at 1-, 5- and
in patients who underwent LT and Roux-en-Y biliary- 10-year, a cumulative incidence of CRC of 3.3%, 6.7%,
jejunal reconstruction, Mathis et al[26] did not encounter and 11.8%, respectively, after LT. Regarding the colorectal
any problems in the 13 patients operated on. cancer location, similarly to IBD/PSC patients before LT,
the right-side colon is more frequently affected[39]. There
is no clear evidence if the age of the patients at the time
POUCHITIS POST-LIVER of LT is associated with CRC risk[7,33,35,45]. No significant
TRANSPLANTATION association between clinical severity IBD and CRC risk
after LT was observed[39,45]. Regarding the use of 5-ASA
The risk of acute pouchitis after LT for PSC ranged from
or ursodeoxycholic acid in the chemoprevention of CRC,
14% to 66%[26-28]. The risk of chronic pouchitis ranged
it seems that they don’t change the cancer risk[33,39].
from 9.1% to 73.7%[26-30]. Freeman et al[29] observed that
the risk of chronic refractory pouchitis was comparable
Risk factors
in patients who underwent LT and those who did not.
The risk of CRC may increase after LT because of errors
Therefore, it seems that LT does not increase the risk of
in mucosa sampling during colonoscopy or perhaps due
pouchitis. With regard to the therapy of pouchitis after
to the immunosuppression treatment of anti-reject thera-
LT, Mathis et al[26] evaluated 32 patients who underwent
py. Loftus et al[42] observed that the CRC rate was 4.4-fold
ileal pouch-anal anastomosis (IPAA) for UC and LT for
higher after LT, as compared to a historical cohort patient
PSC (in 13 patients IPAA followed by OLT). Two-thirds
with PSC/IBD who did not undergo LT. However, the
of the patients had pouchitis during follow-up, about
role of LT in the risk of CRC in IBD/PSC patients still
half developed a chronic pouchitis that required daily an-
isn’t clear. In fact, while Dvorchik found that LT did not
tibiotic therapy. Only one patient needed a defunctioning
significantly influence the risk of CRC, it was observed
ileostomy. Anti-TNFα therapy was used in only four IBD
that LT may be an independent risk factor for CRC in
patients in three studies for refractory pouchitis after LT
other studies[7,35,42,45].
for PSC[13,14,18]. Even though a clinical improvement was
observed, the little data available does not allow us to
Surveillance
extrapolate any conclusions about the efficacy and safety
A program of endoscopic surveillance with serial biop-
of biological therapy in patients with chronic refractory
sies for CRC is recommended by the European Associa-
pouchitis after LT.
tion for the Study of Liver[49]. A colonoscopy is suggested
every year in IBD/PSC patients after LT. If dysplasia
COLORECTAL CANCER POST-LIVER colonic mucosa is found, a colectomy is advised. It has
been shown to be a relatively safe procedure in special-
TRANSPLANT ized surgical centers[45,46].
Epidemiology
A large range with rates of risk of colorectal cancer after Management
LT for PSC, from 0 to 31.5 per 1000 person/year, is pres- Adjuvant pharmacotherapy with drugs like oxaliplatin
ent in literature in recent years[4,7,21,25,31-48]. Watt et al[31], re- has also been shown to be well tolerated in patients post-
ported a cumulative incidence of colorectal cancer (CRC) LT and hepatic graft dysfunction was not documented[50].
at 10-years post LT for PSC of 8.2% as compared to 2.6% Prophylactic colectomy in selected IBD/PSC patients
after LT for non-PSC patients. The CRC risk in PSC with CRC risk factors could be a good management strat-
patients without IBD after LT is 2.8% at 10-years. There- egy in the CRC prevention, but it is used infrequently in
WJG|www.wjgnet.com 3528 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
IBD/PSC
1 Adequate treatment of IBD in active flare up and in remission
period.
2 Annual colonoscopic surveillance program with serial biopsies for
Before LT dysplasia/CRC screening. Colectomy is indicated in patients with
dysplasia/CRC.
3 Evaluate indication for colectomy in selected patients with
medically refractory IBD or frequent relapse before the PSC patient
develops cirrhosis and liver disfunction.
1 Clinical remission of IBD patient is necessary at the time of LT.
At the time of LT 2 Don't interrupt the 5-ASA and/or azathioprin therapy.
3 Don’t smoke at the time of transplant because it may be a risk
factor for flare up of IBD post-transplantation.
1 Evaluate the possibility of substituting tacrolimus with other
drugs, like ciclosporine for anti-reject immunosuppressive therapy.
2 Avoid mycophenolate mofetil in the anti-reject immunosuppressive
therapy for its possible side effects (enterocolitis).
3 Exclude opportunistic intestinal infections (like CMV and clostridium
difficile ) or consider the possibility that diarrhea is induced by the
drugs.
4 Add azathioprine to therapy if the patient presents an IBD
After LT recurrence.
5 Anti-TNFα therapy seems effective and safe in refractory to
conventional therapy IBD patients. The combination of biological
therapy with anti-reject therapy needs a careful monitoring
program for infections, autoimmune diseases and neoplasms.
6 An annual colonoscopic surveillance program with serial biopsies
for dysplasia/CRC screening is necessary. Colectomy is indicated
in patients with dysplasia/CRC or refractory medical therapy of
recurrence/de novo IBD.
7 Adjuvant pharmacotherapy seems to be well tolerated in CRC
patients.
8 Chronic refractory pouchitis is treated according to guidelines.
Figure 1 Clinical management of inflammatory bowel disease/primary sclerosing cholangitis patients before and after liver transplantation. TNFα: Tumor
necrosis factor alpha; IBD: Inflammatory bowel disease; LT: Liver transplantation; PSC: Primary sclerosing cholangitis; CRC: Colorectal cancer; CMV: Cytomegalovi-
rus; 5-ASA: 5-aminosalicylates.
the majority of LT centers[45,51]. tridium difficile), or consider the possibility that diarrhea may
be caused by the drugs (Figure 1). If the symptoms of ac-
tive IBD are confirmed from a colonoscopy and a histo-
CLINICAL MANAGEMENT OF ACTIVE IBD logical exam, the patient starts the IBD therapy. The plan
of IBD therapy in the patient who underwent transplant,
AFTER LT is similar to the therapy plan before the transplant. 5-ASA
Patients who underwent LT can develop diarrhea and it is at a dose of 2.4 g per day is indicated in induction and in
very important exclude an intestinal infection (CMV, Clos- maintenance in the mild-to-moderate UC patients. Topical
WJG|www.wjgnet.com 3529 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
therapy with 5-ASA and/or beclomethasone dipropionate 11 studies were reported[9,16,54-63]. One patient presented
can be useful in distal UC. Budesonide or systemic ste- erythema nodosum associated to IBD[60], one patient de-
roids are indicated in patients with mild Crohn’s disease. veloped colonic cancer with liver metastasis 2 years later
In moderate-to-severe IBD patients the use of oral or iv and died[60], thirteen (50%) patients were treated with
corticosteroids are necessary. Prednisone at a dose of 50 conventional medical IBD therapy (mesalazine, cortico-
mg per day or prednisolone at a dose of 40-60 mg per day steroids, and azathioprine), achieving a clinical remission.
based on the patient’s body weight (60-80 kg) may be used Significant clinical improvement of IBD was observed
in clinical practice. A gradual tapering of corticosteroids with anti-TNFα therapy in three (11.5%) patients. No
is recommended, for example 5 mg every week in predni- severe infections or graft reject were documented after
sone therapy. Maintenance immunosuppression therapy biological therapy[22,61]. Five (19.2%) patients with Crohn’
with azathioprine at a dose of 2.0-2.5 mg/kg body weight s disease continued to have flare up despite treatment[9].
per day is effective after the corticosteroid therapy. Anti- Five (19.2%) UC patients were refractory to therapy and
TNFα treatment could be effective and safe in refractory required a colectomy[9,55,56,62].
to conventional therapy IBD[13,14,18]. The little experience
of the use of biological therapy in transplanted patients,
IBD AFTER LUNG AND INTESTINAL
with concomitant anti-rejection therapy, suggests there
be a higher and more careful surveillance regarding the TRANSPLANTATION
risk of infectious diseases, autoimmune diseases, and neo- The number of patients who underwent lung or intesti-
plasms. nal transplantation is significantly lower than the patients
It is very important to consider the possibility of who underwent liver, heart, and renal transplantation.
surgical treatment in patients with moderate-to-severe This could probably be explained because no IBD cases
IBD after LT for PSC and even more so, because of the were reported after lung and intestinal transplantation.
higher colorectal cancer risk. Proctocolectomy with IPAA
is feasible and safe in dedicated surgical centers[26,27].
CLINICAL MANAGEMENT OF IBD
IBD AFTER HEART TRANSPLANTATION PATIENTS AFTER HEART AND RENAL
Three cases of de novo IBD after heart transplantation TRANSPLANTATION
have been reported in 3 studies: two cases of Crohn’s The concomitant anti-reject immunosuppressive therapy
disease and one case of UC[52-54]. The onset of IBD has can increase the risk of infectious diseases in transplanted
been observed in pediatric age in two of three patients. patients. Therefore, in patients who develop diarrhea, it
Rakhit et al[52] reported one case of Crohn’s disease in 104 is very important to exclude an intestinal infection (CMV,
post-orthotopic heart transplant children. The patient Clostridium difficile). It is also necessary to exclude that di-
developed diarrhea and rectal bleeding immediately after arrhea may be induced by the drugs. The onset of IBD
the transplant and IBD was diagnosed after one year. after heart or renal transplantation could lead to a severe
The patient continued to have flares despite immunosup- clinical situation for the transplanted patient. In fact, in
pressive therapy. Harms et al[53] reported a 15-year-old about half of the patients, conventional IBD therapy
girl developed IBD 10 years after cardiac transplantation combined with anti-reject therapy, can be non-effective.
and presented a severe growth failure and delayed onset Nineteen percent of patients developed multiple recur-
of puberty. The patient was found to have pan-enteric rence on IBD in the renal transplantation group. Eleven
Crohn’s disease and has done remarkably well following a percent of patients required anti-TNFα therapy in order
nutritional therapy. Jüngling et al[54] reported a 53-year-old to have clinical remission and in about 20% of patients
patient who developed distal UC 2 years after heart trans- required a colectomy. The LT model suggests that anti-
plantation. In spite of high-dose treatment with prednis- TNFα therapy combined with anti-reject therapy could
olone the patient’s clinical situation worsened with a pro- be useful in selected IBD patients with refractory to
gression of inflammation in the entire colon. Colectomy conventional therapy after heart or renal transplantation.
with ileostomy was necessary to obtain a good state of Like in the LT, it is very important that there be a higher
health. Three IBD cases have been observed after heart more careful surveillance regarding the risk of infectious
transplantation in spite of immunosuppresive therapy. diseases, autoimmune diseases, and neoplasms after bio-
Two of them have been treated with conventional medi- logical therapy in heart and renal transplanted patients.
cal therapy with success, whereas one IBD case required The surgical option remains an essential treatment in
surgery with colectomy and ileostomy. No IBD patient complicated IBD cases which are refractory to the inten-
was treated with anti-TNFα therapy. sive medical therapy.
IBD AFTER RENAL TRANSPLANTATION CONCLUSION
A total of about of twenty-seven de novo IBD patients (15 There is estimated a higher incidence of de novo IBD after
UC and 11 Crohn’s disease) after renal transplantation in solid organ transplantation than in the general popula-
WJG|www.wjgnet.com 3530 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
tion. The onset of IBD in the organ transplant recipi- plant 2006; 6: 1422-1429 [PMID: 16686766 DOI: 10.1111/
ent population is an important clinical situation which j.1600-6143.2006.01333.x]
4 Joshi D, Bjarnason I, Belgaumkar A, O’Grady J, Suddle
is associated with higher morbidity and difficulty in the A, Heneghan MA, Aluvihare V, Rela M, Heaton N, Agar-
medical therapeutic management because of the possible wal K. The impact of inflammatory bowel disease post-
interaction between anti-reject therapy and IBD therapy. liver transplantation for primary sclerosing cholangitis.
IBD course after LT is variable, but about one third of Liver Int 2013; 33: 53-61 [PMID: 22103794 DOI: 10.1111/
patients may worsen, needing increased medical therapy j.1478-3231.2011.02677.x]
5 Befeler AS, Lissoos TW, Schiano TD, Conjeevaram H, Das-
or a colectomy. Active IBD at the time of LT, discontinu- gupta KA, Millis JM, Newell KA, Thistlethwaite JR, Baker
ation of 5-ASA or azathioprine at the time of LT and AL. Clinical course and management of inflammatory bowel
use of tacrolimus-based immunosuppression may be as- disease after liver transplantation. Transplantation 1998; 65:
sociated with an unfavorable outcome of IBD after LT. 393-396 [PMID: 9484758]
Anti-TNF therapy for refractory IBD may be an effective 6 MacLean AR, Lilly L, Cohen Z, O’Connor B, McLeod RS.
Outcome of patients undergoing liver transplantation for
and safe therapeutic option after LT. The little experience
primary sclerosing cholangitis. Dis Colon Rectum 2003; 46:
of the use of biological therapy in transplanted patients, 1124-1128 [PMID: 12907911]
with concomitant anti-rejection therapy, suggests there be 7 Dvorchik I, Subotin M, Demetris AJ, Fung JJ, Starzl TE,
a higher more careful surveillance regarding the risk of Wieand S, Abu-Elmagd KM. Effect of liver transplantation
infectious diseases, autoimmune diseases, and neoplasms. on inflammatory bowel disease in patients with primary
sclerosing cholangitis. Hepatology 2002; 35: 380-384 [PMID:
Therefore, it is very important to consider the possibil-
11826412 DOI: 10.1053/jhep.2002.30695]
ity of a surgical treatment in refractory severe IBD after 8 Wörns MA, Lohse AW, Neurath MF, Croxford A, Otto G,
LT. An increased risk of colorectal cancer is also present Kreft A, Galle PR, Kanzler S. Five cases of de novo inflam-
after LT in IBD/PSC patient. An annual program of matory bowel disease after orthotopic liver transplantation.
endoscopic surveillance with serial biopsies for CRC is Am J Gastroenterol 2006; 101: 1931-1937 [PMID: 16790037
DOI: 10.1111/j.1572-0241.2006.00624.x]
recommended. If dysplasia colonic mucosa is found, a
9 Riley TR, Schoen RE, Lee RG, Rakela J. A case series of
colectomy with IPAA is advised. It has been shown to be transplant recipients who despite immunosuppression
a relatively safe procedure in the specialized surgical cen- developed inflammatory bowel disease. Am J Gastroenterol
ters. Adjuvant pharmacotherapy has been shown to be 1997; 92: 279-282 [PMID: 9040206]
well tolerated in patients post-LT. Hepatic graft dysfunc- 10 Cholongitas E, Papatheodoridis GV, Zappoli P, Gianna-
kopoulos A, Patch D, Marelli L, Shusang V, Kalambokis G,
tion has not been documented after adjuvant pharmaco-
Shirling G, Rolando N, Burroughs AK. Combined HLA-DR
therapy. A prophylactic colectomy in selected IBD/PSC and -DQ disparity is associated with a stable course of ulcer-
patients with CRC risk factors could be a good man- ative colitis after liver transplantation for primary sclerosing
agement strategy in the CRC prevention, but it is used cholangitis. Liver Transpl 2007; 13: 552-557 [PMID: 17394153
infrequently in the majority of LT centers. About 30% DOI: 10.1002/lt.21077]
of patients developed multiple recurrences of IBD and 11 Verdonk RC, Haagsma EB, Van Den Berg AP, Karrenbeld
A, Slooff MJ, Kleibeuker JH, Dijkstra G. Inflammatory bowel
20% of patients required a colectomy after renal trans- disease after liver transplantation: a role for cytomegalovi-
plantation. Like in the LT, anti-TNFα therapy could be rus infection. Scand J Gastroenterol 2006; 41: 205-211 [PMID:
an effective treatment in IBD patients with conventional 16484126 DOI: 10.1080/00365520500206293]
refractory therapy after renal or heart transplantation. A 12 Navaneethan U, Choudhary M, Venkatesh PG, Lashner
large number of patients are needed to confirm the pre- BA, Remzi FH, Shen B, Kiran RP. The effects of liver trans-
plantation on the clinical course of colitis in ulcerative colitis
liminary observations.
patients with primary sclerosing cholangitis. Aliment Phar-
Regarding the higher clinical complexity of this sub- macol Ther 2012; Epub ahead of print [PMID: 22428731 DOI:
group of IBD patients, a close multidisciplinary approach 10.1111/j.1365-2036.2012.05067.x]
between an IBD dedicated gastroenterologist and sur- 13 Sandhu A, Alameel T, Dale CH, Levstik M, Chande N.
geon and an organ transplantation specialist is necessary The safety and efficacy of antitumour necrosis factor-
alpha therapy for inflammatory bowel disease in patients
in order to have the best clinical management of IBD
post liver transplantation: a case series. Aliment Pharmacol
after transplantation. Ther 2012; 36: 159-165 [PMID: 22616981 DOI: 10.1111/
j.1365-2036.2012.05141.x]
14 Mohabbat AB, Sandborn WJ, Loftus EV, Wiesner RH, Bru-
REFERENCES ining DH. Anti-tumour necrosis factor treatment of inflam-
1 Singh S, Loftus EV, Talwalkar JA. Inflammatory bowel matory bowel disease in liver transplant recipients. Aliment
disease after liver transplantation for primary sclerosing Pharmacol Ther 2012; 36: 569-574 [PMID: 22779779 DOI:
cholangitis. Am J Gastroenterol 2013; 108: 1417-1425 [PMID: 10.1111/j.1365-2036.2012.05217.x]
23896954 DOI: 10.1038/ajg.2013.163] 15 Lal S, Steinhart AH. Infliximab for ulcerative colitis follow-
2 Haagsma EB, Van Den Berg AP, Kleibeuker JH, Slooff MJ, ing liver transplantation. Eur J Gastroenterol Hepatol 2007; 19:
Dijkstra G. Inflammatory bowel disease after liver transplan- 277-280 [PMID: 17301656]
tation: the effect of different immunosuppressive regimens. 16 El-Nachef N, Terdiman J, Mahadevan U. Anti-tumor ne-
Aliment Pharmacol Ther 2003; 18: 33-44 [PMID: 12848624 DOI: crosis factor therapy for inflammatory bowel disease in the
10.1046/j.1365-2036.2003.01613.x] setting of immunosuppression for solid organ transplanta-
3 Verdonk RC, Dijkstra G, Haagsma EB, Shostrom VK, Van tion. Am J Gastroenterol 2010; 105: 1210-1211 [PMID: 20445523
den Berg AP, Kleibeuker JH, Langnas AN, Sudan DL. In- DOI: 10.1038/ajg]
flammatory bowel disease after liver transplantation: risk 17 Indriolo A, Fagiuoli S, Pasulo L. Infliximab in patients with
factors for recurrence and de novo disease. Am J Trans- ulcerative colitis and primary sclerosing cholangitis before
WJG|www.wjgnet.com 3531 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
and after liver transplantation. J Crohns Colitis 2012; 6 Suppl 1: 10.1136/gut.37.6.845]
S117 31 Watt KD, Pedersen RA, Kremers WK, Heimbach JK, Sanchez
18 Indriolo A, Fagiuoli S, Pasulo L, Fiorino G, Danese S, Ravelli W, Gores GJ. Long-term probability of and mortality from
P. Letter: infliximab therapy in inflammatory bowel disease de novo malignancy after liver transplantation. Gastroenter-
patients after liver transplantation. Aliment Pharmacol Ther ology 2009; 137: 2010-2017 [PMID: 19766646 DOI: 10.1053/
2013; 37: 840-842 [PMID: 23496317 DOI: 10.1111/apt.12256] j.gastro.2009.08.070]
19 Gabe SM, Bjarnason I, Tolou-Ghamari Z, Tredger JM, 32 Fabia R, Levy MF, Testa G, Obiekwe S, Goldstein RM, Hus-
Johnson PG, Barclay GR, Williams R, Silk DB. The effect of berg BS, Gonwa TA, Klintmalm GB. Colon carcinoma in pa-
tacrolimus (FK506) on intestinal barrier function and cellular tients undergoing liver transplantation. Am J Surg 1998; 176:
energy production in humans. Gastroenterology 1998; 115: 265-269 [PMID: 9776156]
67-74 [PMID: 9649460] 33 Hanouneh IA, Macaron C, Lopez R, Zein NN, Lashner
20 Rostaing L, Puyoo O, Tkaczuk J, Peres C, Rouzaud A, Cis- BA. Risk of colonic neoplasia after liver transplantation for
terne JM, de Preval C, Ohayon E, Durand D, Abbal M. Dif- primary sclerosing cholangitis. Inflamm Bowel Dis 2012; 18:
ferences in Type 1 and Type 2 intracytoplasmic cytokines, 269-274 [PMID: 21425212]
detected by flow cytometry, according to immunosuppres- 34 Albright JB, Bonatti H, Stauffer J, Dickson RC, Nguyen
sion (cyclosporine A vs. tacrolimus) in stable renal allograft J, Harnois D, Jeanpierre C, Hinder R, Steers J, Chua H,
recipients. Clin Transplant 1999; 13: 400-409 [PMID: 10515221 Aranda-Michel J. Colorectal and anal neoplasms following
DOI: 10.1034/j.1399-0012.1999.130506.x] liver transplantation. Colorectal Dis 2010; 12: 657-666 [PMID:
21 Moncrief KJ, Savu A, Ma MM, Bain VG, Wong WW, Tandon 19508543 DOI: 10.1111/j.1463-1318.2009.01840.x]
P. The natural history of inflammatory bowel disease and 35 Bleday R, Lee E, Jessurun J, Heine J, Wong WD. Increased
primary sclerosing cholangitis after liver transplantation--a risk of early colorectal neoplasms after hepatic transplant in
single-centre experience. Can J Gastroenterol 2010; 24: 40-46 patients with inflammatory bowel disease. Dis Colon Rectum
[PMID: 20186355] 1993; 36: 908-912 [PMID: 8404380]
22 Neurath MF, Wanitschke R, Peters M, Krummenauer F, Meyer 36 Higashi H, Yanaga K, Marsh JW, Tzakis A, Kakizoe S, Starzl
zum Büschenfelde KH, Schlaak JF. Randomised trial of myco- TE. Development of colon cancer after liver transplantation
phenolate mofetil versus azathioprine for treatment of chronic for primary sclerosing cholangitis associated with ulcerative
active Crohn’s disease. Gut 1999; 44: 625-628 [PMID: 10205197] colitis. Hepatology 1990; 11: 477-480 [PMID: 2312061]
23 Fellermann K, Steffen M, Stein J, Raedler A, Hämling J, Lud- 37 Jonas S, Rayes N, Neumann U, Neuhaus R, Bechstein WO,
wig D, Loeschke K, Stange EF. Mycophenolate mofetil: lack Guckelberger O, Tullius SG, Serke S, Neuhaus P. De novo
of efficacy in chronic active inflammatory bowel disease. Ali- malignancies after liver transplantation using tacrolimus-
ment Pharmacol Ther 2000; 14: 171-176 [PMID: 10651657 DOI: based protocols or cyclosporine-based quadruple immu-
10.1046/j.1365-2036.2000.00695.x] nosuppression with an interleukin-2 receptor antibody or
24 Ho GT, Seddon AJ, Therapondos G, Satsangi J, Hayes PC. antithymocyte globulin. Cancer 1997; 80: 1141-1150 [PMID:
The clinical course of ulcerative colitis after orthotopic liver 9305716]
transplantation for primary sclerosing cholangitis: further 38 Johnson EE, Leverson GE, Pirsch JD, Heise CP. A 30-year
appraisal of immunosuppression post transplantation. Eur J analysis of colorectal adenocarcinoma in transplant recipi-
Gastroenterol Hepatol 2005; 17: 1379-1385 [PMID: 16292093] ents and proposal for altered screening. J Gastrointest Surg
25 Navaneethan U, Venkatesh PG, Mukewar S, Lashner BA, 2007; 11: 272-279 [PMID: 17458597]
Remzi FH, McCullough AJ, Kiran RP, Shen B, Fung JJ. 39 Jørgensen KK, Lindström L, Cvancarova M, Castedal M, Fri-
Progressive primary sclerosing cholangitis requiring liver man S, Schrumpf E, Foss A, Isoniemi H, Nordin A, Holte K,
transplantation is associated with reduced need for colec- Rasmussen A, Bergquist A, Vatn MH, Boberg KM. Colorectal
tomy in patients with ulcerative colitis. Clin Gastroenterol neoplasia in patients with primary sclerosing cholangitis un-
Hepatol 2012; 10: 540-546 [PMID: 22245961 DOI: 10.1016/ dergoing liver transplantation: a Nordic multicenter study.
j.cgh.2012.01.006] Scand J Gastroenterol 2012; 47: 1021-1029 [PMID: 22577871
26 Mathis KL, Dozois EJ, Larson DW, Cima RR, Sarmiento JM, DOI: 10.3109/00365521.2012.685754]
Wolff BG, Heimbach JK, Pemberton JH. Ileal pouch-anal 40 Kelly DM, Emre S, Guy SR, Miller CM, Schwartz ME, Shein-
anastomosis and liver transplantation for ulcerative colitis er PA. Liver transplant recipients are not at increased risk for
complicated by primary sclerosing cholangitis. Br J Surg nonlymphoid solid organ tumors. Cancer 1998; 83: 1237-1243
2008; 95: 882-886 [PMID: 18496886 DOI: 10.1002/bjs.6210] [PMID: 9740091]
27 Cho CS, Dayton MT, Thompson JS, Koltun WA, Heise CP, 41 Knechtle SJ, D’Alessandro AM, Harms BA, Pirsch JD, Belzer
Harms BA. Proctocolectomy-ileal pouch-anal anastomosis FO, Kalayoglu M. Relationships between sclerosing chol-
for ulcerative colitis after liver transplantation for primary angitis, inflammatory bowel disease, and cancer in patients
sclerosing cholangitis: a multi-institutional analysis. J Gas- undergoing liver transplantation. Surgery 1995; 118: 615-619;
trointest Surg 2008; 12: 1221-1226 [PMID: 18449613 DOI: discussion 619-620 [PMID: 7570313]
10.1007/s11605-008-0528-5] 42 Loftus EV, Aguilar HI, Sandborn WJ, Tremaine WJ, Krom
28 Zins BJ, Sandborn WJ, Penna CR, Landers CJ, Targan SR, RA, Zinsmeister AR, Graziadei IW, Wiesner RH. Risk of
Tremaine WJ, Wiesner RH, Dozois RR. Pouchitis disease colorectal neoplasia in patients with primary sclerosing chol-
course after orthotopic liver transplantation in patients angitis and ulcerative colitis following orthotopic liver trans-
with primary sclerosing cholangitis and an ileal pouch-anal plantation. Hepatology 1998; 27: 685-690 [PMID: 9500695]
anastomosis. Am J Gastroenterol 1995; 90: 2177-2181 [PMID: 43 Narumi S, Roberts JP, Emond JC, Lake J, Ascher NL. Liver
8540511] transplantation for sclerosing cholangitis. Hepatology 1995;
29 Freeman K, Shao Z, Remzi FH, Lopez R, Fazio VW, Shen B. 22: 451-457 [PMID: 7635412]
Impact of orthotopic liver transplant for primary sclerosing 44 Sint Nicolaas J, Tjon AS, Metselaar HJ, Kuipers EJ, de Man
cholangitis on chronic antibiotic refractory pouchitis. Clin RA, van Leerdam ME. Colorectal cancer in post-liver trans-
Gastroenterol Hepatol 2008; 6: 62-68 [PMID: 18065274 DOI: plant recipients. Dis Colon Rectum 2010; 53: 817-821 [PMID:
10.1016/j.cgh.2007.09.018] 20389217 DOI: 10.1007/DCR.0b013e3181cc90c7]
30 Rowley S, Candinas D, Mayer AD, Buckels JA, McMaster P, 45 Vera A, Gunson BK, Ussatoff V, Nightingale P, Candinas D,
Keighley MR. Restorative proctocolectomy and pouch anal Radley S, Mayer A, Buckels JA, McMaster P, Neuberger J,
anastomosis for ulcerative colitis following orthotopic liver Mirza DF. Colorectal cancer in patients with inflammatory
transplantation. Gut 1995; 37: 845-847 [PMID: 8537060 DOI: bowel disease after liver transplantation for primary scleros-
WJG|www.wjgnet.com 3532 April 7, 2014|Volume 20|Issue 13|
Indriolo A et al . Clinical management of IBD
ing cholangitis. Transplantation 2003; 75: 1983-1988 [PMID: 55 Hibbs AM, Bznik-Cizman B, Guttenberg M, Goldberg B,
12829898] Meyers K. Ulcerative colitis in a renal transplant patient
46 Goss JA, Shackleton CR, Farmer DG, Arnaout WS, Seu P, with previous Goodpasture disease. Pediatr Nephrol 2001; 16:
Markowitz JS, Martin P, Stribling RJ, Goldstein LI, Busuttil 543-546 [PMID: 11465800]
RW. Orthotopic liver transplantation for primary sclerosing 56 Nagai H, Matsumaru K, Shiozawa K, Momiyama K, Wakui
cholangitis. A 12-year single center experience. Ann Surg N, Shinohara M, Watanabe M, Ishii K, Nonaka H, Hasegawa
1997; 225: 472-481; discussion 481-483 [PMID: 9193175] A, Teramoto T, Yamamuro W, Sumino Y, Miki K. Disap-
47 Jain AB, Yee LD, Nalesnik MA, Youk A, Marsh G, Reyes J, pearance of HCV after cessation of immunosuppression in
Zak M, Rakela J, Irish W, Fung JJ. Comparative incidence of a patient with ulcerative colitis and renal transplantation. J
de novo nonlymphoid malignancies after liver transplan- Gastroenterol 2005; 40: 848-853 [PMID: 16143892]
tation under tacrolimus using surveillance epidemiologic 57 Halim MA, Said T, Nair P, Schmidt I, Hassan A, Johny KV,
end result data. Transplantation 1998; 66: 1193-1200 [PMID: Al-Muzairai I, Samhan M, Nampoory MR, Al-Mousawi
9825817] M. De novo Crohn’s disease in a renal transplant recipient.
48 Koornstra JJ, Wesseling J, de Jong AE, Vasen HF, Kleibeuker Transplant Proc 2007; 39: 1278-1279 [PMID: 17524953 DOI:
JH, Haagsma EB. Increased risk of colorectal neoplasia in as- 10.1016/j.transproceed.2007.03.045]
ymptomatic liver-transplant recipients. Gut 2007; 56: 892-893 58 Stewart IJ, Gallagher JP, Dahms WJ. A case of new onset
[PMID: 17519499 DOI: 10.1136/gut.2007.120121] Crohn’s disease after renal transplantation. Gastroenterol
49 European Association For The Study Of The Liver. EASL Hepatol (N Y) 2008; 4: 877-878 [PMID: 21904480]
Clinical Practice Guidelines: management of cholestatic liver 59 Kourda N, Bettaïeb I, Blel A, Zoghlami A, Bedoui R, Najah N,
diseases. J Hepatol 2009; 51: 237-267 [PMID: 19501929 DOI: Ben Jilani SB, Zermani R. An aggressive course of de novo
10.1016/j.jhep.2009.04.009] ulcerative colitis after renal transplantation: colonic adeno-
50 Doroshow JH, Synold TW, Gandara D, Mani S, Remick SC, carcinoma with choriocarcinomatous differentiation. Tunis
Mulkerin D, Hamilton A, Sharma S, Ramanathan RK, Lenz Med 2009; 87: 359-361 [PMID: 19927772]
HJ, Graham M, Longmate J, Takimoto CH, Ivy P. Pharma- 60 Gheith O, Al-Otaibi T, Tawab KA, Said T, Balaha MA,
cology of oxaliplatin in solid tumor patients with hepatic Halim MA, Nair MP, Nampoory MR. Erythema nodosum in
dysfunction: a preliminary report of the National Cancer renal transplant recipients: multiple cases and review of lit-
Institute Organ Dysfunction Working Group. Semin Oncol erature. Transpl Infect Dis 2010; 12: 164-168 [PMID: 20002354
2003; 30: 14-19 [PMID: 14523790] DOI: 10.1111/j.1399-3062.2009.00474.x]
51 Levin B. Risk of cancer in ulcerative colitis. Gastrointest En- 61 Temme J, Koziolek M, Bramlage C, Schaefer IM, Füzesi
dosc 1999; 49: S60-S62 [PMID: 10049450] L, Ramadori G, Müller GA, Schwörer H. Infliximab as
52 Rakhit A, Nurko S, Gauvreau K, Mayer JE, Blume ED. therapeutic option in steroid-refractory ulcerative coli-
Gastrointestinal complications after pediatric cardiac trans- tis after kidney transplantation: case report. Transplant
plantation. J Heart Lung Transplant 2002; 21: 751-759 [PMID: Proc 2010; 42: 3880-3882 [PMID: 21094876 DOI: 10.1016/
12100901] j.transproceed.2010]
53 Harms B, Bremner AR, Mulligan J, Fairhurst J, Griffiths DM, 62 Parameswaran S, Singh K, Nada R, Rathi M, Kohli H, Jha V,
Salmon T, Beattie RM. Crohn’s disease post-cardiac trans- Gupta K, Sakhuja V. Ulcerative colitis after renal transplan-
plantation presenting with severe growth failure and delayed tation: A case report and review of literature. Indian J Nephrol
onset of puberty. Pediatr Allergy Immunol 2004; 15: 186-189 2011; 21: 120-122 [DOI: 10.4103/0971-4065.78063]
[PMID: 15059198 DOI: 10.1046/j.1399-3038.2003.00130.x] 63 Azevedo P, Freitas C, Aguiar P, Silva H, Santos T, Farrajota P,
54 Jüngling B, Kindermann I, Moser C, Püschel W, Ecker KW, Almeida M, Pedroso S, Martins LS, Dias L, Vizcaíno R, Hen-
Schäfers HJ, Böhm M, Zeuzem S, Giese T, Stallmach A. De- riques AC, Cabrita A. A case series of de novo inflammatory
velopment of ulcerative colitis after heart transplantation bowel disease after kidney transplantation. Transplant Proc
during immunosuppressive therapy. Z Gastroenterol 2005; 43: 2013; 45: 1084-1087 [PMID: 23622632 DOI: 10.1016/j.transpro-
195-199 [PMID: 15700214 DOI: 10.1055/s-2004-813743] ceed.2013.03.008]
P- Reviewers: Bonaz BL, Liu ZJ S- Editor: Gou SX
L- Editor: A E- Editor: Wu HL
WJG|www.wjgnet.com 3533 April 7, 2014|Volume 20|Issue 13|
Published by Baishideng Publishing Group Co., Limited
Flat C, 23/F., Lucky Plaza,
315-321 Lockhart Road, Wan Chai, Hong Kong, China
Fax: +852-65557188
Telephone: +852-31779906
E-mail: bpgoffice@wjgnet.com
http://www.wjgnet.com
I S S N 1 0 0 7 - 9 3 2 7
1 3
9 7 7 1 0 0 7 9 3 2 0 45
© 2014 Baishideng Publishing Group Co., Limited. All rights reserved.
You might also like
- The Somatic Nervous System The Autonomic Nervous System - The Enteric Nervous SystemDocument5 pagesThe Somatic Nervous System The Autonomic Nervous System - The Enteric Nervous SystemMarissa AsimNo ratings yet
- Peripheral Vascular DiseasesDocument25 pagesPeripheral Vascular DiseasesShruthi Arun100% (1)
- Music Therapy ResearchDocument7 pagesMusic Therapy ResearchALEXNo ratings yet
- Proteins in Serum & UrineDocument66 pagesProteins in Serum & Urinekiedd_04100% (1)
- Nutrition-Based Management of Inflammaging in CKDDocument17 pagesNutrition-Based Management of Inflammaging in CKDAndrés ZapataNo ratings yet
- UrologyDocument35 pagesUrologymiansk100% (1)
- Vascular Dementia (Case Study)Document22 pagesVascular Dementia (Case Study)Coleen Mae CamaristaNo ratings yet
- Gastrointestinal Complications After Kidney TransplantationDocument16 pagesGastrointestinal Complications After Kidney TransplantationNatalyFuertesNo ratings yet
- Editorial Commentary On The Indian Journal of Gastroenterology May-June 2020Document3 pagesEditorial Commentary On The Indian Journal of Gastroenterology May-June 2020sivagiri.pNo ratings yet
- Medical Nutritional Therapy For Renal Transplantation in The COVID-19Document9 pagesMedical Nutritional Therapy For Renal Transplantation in The COVID-19Magaly LizaolaNo ratings yet
- Liver Intensive CareDocument3 pagesLiver Intensive CareSureddi KumarNo ratings yet
- Wjgo 11 1161Document12 pagesWjgo 11 1161davidgalcantaraNo ratings yet
- Acute Sever UCDocument11 pagesAcute Sever UClunaTSNo ratings yet
- Critically-Ill Patients With Biliary Obstruction and Cholangitis: Bedside Fluoroscopic-Free Endoscopic Drainage Versus Percutaneous DrainageDocument10 pagesCritically-Ill Patients With Biliary Obstruction and Cholangitis: Bedside Fluoroscopic-Free Endoscopic Drainage Versus Percutaneous DrainageAgung KaryawinaraNo ratings yet
- Management of Patients With Hepatitis C Infection and Renal DiseaseDocument14 pagesManagement of Patients With Hepatitis C Infection and Renal DiseaseAstri Arri FebriantiNo ratings yet
- Breakthroughs in Hepatology JhepatDocument2 pagesBreakthroughs in Hepatology JhepatCláudia SilvaNo ratings yet
- 10.1007@s00384 019 03481 1Document11 pages10.1007@s00384 019 03481 1Bernadett FarkasNo ratings yet
- 10.1053@j.gastro DiverticulitisDocument20 pages10.1053@j.gastro DiverticulitisCarlos CaicedoNo ratings yet
- WJG 29 241Document17 pagesWJG 29 241HICHAM WAHNOUNo ratings yet
- Gastroenterology: World Journal ofDocument13 pagesGastroenterology: World Journal ofdrcafemanNo ratings yet
- Renal Cell Carcinoma A Case Series With Integrative Treatment 2329 6771 S1 002Document5 pagesRenal Cell Carcinoma A Case Series With Integrative Treatment 2329 6771 S1 002VanroNo ratings yet
- Jyoti Bansode-Feb-26Document5 pagesJyoti Bansode-Feb-26Putu juni wulandariNo ratings yet
- Evaluation of The Renal Transplant Recipient in The Emergency DepartmentDocument27 pagesEvaluation of The Renal Transplant Recipient in The Emergency DepartmentMauricio RiveraNo ratings yet
- Original Article: Key WordsDocument9 pagesOriginal Article: Key WordsykommNo ratings yet
- Journal of Pediatric Surgery: Wendy K. Fujioka, Robert A. CowlesDocument3 pagesJournal of Pediatric Surgery: Wendy K. Fujioka, Robert A. CowlesVmiguel LcastilloNo ratings yet
- tmp20EE TMPDocument9 pagestmp20EE TMPFrontiersNo ratings yet
- Antibiotics 10 00139Document12 pagesAntibiotics 10 00139Kieth Roland PalosoNo ratings yet
- Diverticulitis 2021 UptodateDocument23 pagesDiverticulitis 2021 UptodateEgdar Allan PoeNo ratings yet
- Venter, Willem D. F., Et Al.2018Document8 pagesVenter, Willem D. F., Et Al.2018priya panaleNo ratings yet
- Hep C en WercDocument7 pagesHep C en WerchidrogiriumNo ratings yet
- Total Joint Arthroplasty Should Not Be Delayed in Hepatitis C - 2022 - ArthroplDocument7 pagesTotal Joint Arthroplasty Should Not Be Delayed in Hepatitis C - 2022 - ArthroplSanty OktavianiNo ratings yet
- Approach To The Management of Recently Diagnosed IDocument19 pagesApproach To The Management of Recently Diagnosed IdudinkarulesNo ratings yet
- Wjgo 14 1199Document12 pagesWjgo 14 1199juan uribeNo ratings yet
- Responding To Organ Failure in HIV-Infected Patients: Volume 348:2279-2281 June 5, 2003 Number 23Document4 pagesResponding To Organ Failure in HIV-Infected Patients: Volume 348:2279-2281 June 5, 2003 Number 23Andrie WigunaNo ratings yet
- Absceso Hepatico 2Document7 pagesAbsceso Hepatico 2Astrid MendezNo ratings yet
- Complicationsafter Pancreaticoduodenectomy: Robert SimonDocument10 pagesComplicationsafter Pancreaticoduodenectomy: Robert SimonŞükriye AngaNo ratings yet
- Pi Is 1089326121000039Document20 pagesPi Is 1089326121000039Muzaffar MehdiNo ratings yet
- Acute Appendicitis in Patients With End-Stage Renal Disease: Original ArticleDocument7 pagesAcute Appendicitis in Patients With End-Stage Renal Disease: Original ArticleUkh ChyNo ratings yet
- Articulo ADocument8 pagesArticulo AJaver Andres HernandezNo ratings yet
- Complications of Pancreatic SurgeryDocument5 pagesComplications of Pancreatic Surgeryhenok seifeNo ratings yet
- Consensus Statement Management of Drug-Induced LivDocument8 pagesConsensus Statement Management of Drug-Induced LivShannon Marcella EvangelinaNo ratings yet
- DOACs in Cirrhotic Patients With Portal Vein Thrombosis - The EvidenceDocument15 pagesDOACs in Cirrhotic Patients With Portal Vein Thrombosis - The EvidencelabertoNo ratings yet
- Liver Abscess ThesisDocument7 pagesLiver Abscess Thesisjenniferalexanderfortlauderdale100% (1)
- 2014 Article 639Document8 pages2014 Article 639Anida HasnaNo ratings yet
- Clinical Outcomes of Esophagogastroduodenoscopy In.27Document6 pagesClinical Outcomes of Esophagogastroduodenoscopy In.27Agung KaryawinaraNo ratings yet
- Literature Review of Liver AbscessDocument4 pagesLiterature Review of Liver Abscessc5ng67v1100% (1)
- ESC Heart Failure - 2022 - Liu - Prevalence and Impact of Malnutrition On Readmission Among Hospitalized Patients WithDocument10 pagesESC Heart Failure - 2022 - Liu - Prevalence and Impact of Malnutrition On Readmission Among Hospitalized Patients WithGilmara12No ratings yet
- Abdominal Sepsis Prognostic FactorDocument6 pagesAbdominal Sepsis Prognostic FactorPrasojo JojoNo ratings yet
- Review of Early Immune Response To Sars-Cov-2 Vaccination Among Patients With CKDDocument13 pagesReview of Early Immune Response To Sars-Cov-2 Vaccination Among Patients With CKDVivi Permana SarieNo ratings yet
- Effect of Nursing Intervention Program On Interferone Side Effects Among Hepatitis C PatientsDocument9 pagesEffect of Nursing Intervention Program On Interferone Side Effects Among Hepatitis C PatientsNovi Trisnawati 16040073501No ratings yet
- Abdominal Sepsis.15Document8 pagesAbdominal Sepsis.15Dario Xavier Achachi MelendezNo ratings yet
- Acute-On-Chronic Liver Failure - Controversies and ConsensusDocument10 pagesAcute-On-Chronic Liver Failure - Controversies and ConsensusPhan Nguyễn Đại NghĩaNo ratings yet
- Peritoneal Tuberculosis Mimiking Gastrointestinal Stromal TumorDocument3 pagesPeritoneal Tuberculosis Mimiking Gastrointestinal Stromal TumorIJAR JOURNALNo ratings yet
- Can Radioiodine Be Administered Effectively and Safely To A Patient With Severe Chronic Kidney Disease?Document6 pagesCan Radioiodine Be Administered Effectively and Safely To A Patient With Severe Chronic Kidney Disease?Mariano CadeNo ratings yet
- Scar Pigna To 2010Document32 pagesScar Pigna To 2010anon_535071452No ratings yet
- The Patient With Cirrhosis in TheDocument9 pagesThe Patient With Cirrhosis in TheJoseph Antonio Apaza GómezNo ratings yet
- Study of Clinical Profile of Patient With Acute Kidney DiseaseDocument7 pagesStudy of Clinical Profile of Patient With Acute Kidney DiseaseIJAR JOURNALNo ratings yet
- Covid-19 domID StatinDocument6 pagesCovid-19 domID StatinAcinetobacter BaumemmeeNo ratings yet
- Anaesthesiology For Pancreatic CancerDocument18 pagesAnaesthesiology For Pancreatic CancerAnggi CalapiNo ratings yet
- Ten Major Concerns About Antibiotic Use in Acute PancreatitisDocument9 pagesTen Major Concerns About Antibiotic Use in Acute PancreatitislakshitNo ratings yet
- Antiviral Therapy For Chronic Hepatitis B in China: Xin Zheng Junzhong Wang Dongliang YangDocument6 pagesAntiviral Therapy For Chronic Hepatitis B in China: Xin Zheng Junzhong Wang Dongliang Yangapi-206282033No ratings yet
- Telemedicine in The COVID-19 Era For Liver Transplant Recipients: An Italian Lockdown Area ExperienceDocument8 pagesTelemedicine in The COVID-19 Era For Liver Transplant Recipients: An Italian Lockdown Area ExperienceMayank AhujaNo ratings yet
- Zalavras 2009Document6 pagesZalavras 2009Mohamed GoudaNo ratings yet
- 1 s2.0 S2049080122000279 MainDocument4 pages1 s2.0 S2049080122000279 MainAfniNo ratings yet
- Peritonitis Clinical Pathway PDFDocument4 pagesPeritonitis Clinical Pathway PDFIndah95No ratings yet
- ERCP - and Endoscopic Sphincterotomy-Induced PancreatitisDocument18 pagesERCP - and Endoscopic Sphincterotomy-Induced PancreatitisWilliam Alexander Guzman MartinNo ratings yet
- INGLES - Active Transcutaneous Bone Conduction Hearing ImplantsDocument19 pagesINGLES - Active Transcutaneous Bone Conduction Hearing ImplantsWilliam Alexander Guzman MartinNo ratings yet
- INGLES - Medical, Technical and Audiological Outcomes of Hearing RehabilitationDocument9 pagesINGLES - Medical, Technical and Audiological Outcomes of Hearing RehabilitationWilliam Alexander Guzman MartinNo ratings yet
- Sedation and Monitoring For Gastrointestinal Endoscopy - 2013 PDFDocument9 pagesSedation and Monitoring For Gastrointestinal Endoscopy - 2013 PDFWilliam Alexander Guzman MartinNo ratings yet
- Bahan Tutor Skenario 3Document5 pagesBahan Tutor Skenario 3Azka MuflihaNo ratings yet
- Balanitis: Pathophysiology Incubation PeriodDocument2 pagesBalanitis: Pathophysiology Incubation PeriodIzhra MargateNo ratings yet
- Oral Manifestations of Thyroid Disorders and Its MDocument4 pagesOral Manifestations of Thyroid Disorders and Its MNike WijayaNo ratings yet
- Visudyne (Verteporfin For Injection) : Adverse Reactions (6) )Document2 pagesVisudyne (Verteporfin For Injection) : Adverse Reactions (6) )Upik MoritaNo ratings yet
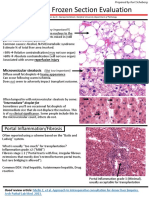
- Donor Liver and Kidney Frozen Section Evaluation CriteriaDocument7 pagesDonor Liver and Kidney Frozen Section Evaluation CriteriaJose SirittNo ratings yet
- 2002 Magnetom Flash 3Document104 pages2002 Magnetom Flash 3Herick Savione100% (3)
- 2 ApikDocument5 pages2 ApikAhmad Syauqie Al MuhdarNo ratings yet
- Autoimmune Hemolytic AnemiasDocument13 pagesAutoimmune Hemolytic Anemiasb101103139No ratings yet
- Atorvastatin Nursing ConsiderationsDocument11 pagesAtorvastatin Nursing ConsiderationsClaire M. AuditorNo ratings yet
- Fluids and Electrolytes: Epidemiology/PathophysiologyDocument27 pagesFluids and Electrolytes: Epidemiology/PathophysiologyManna YankiNo ratings yet
- Management Pancreas and GallbladderDocument21 pagesManagement Pancreas and Gallbladderapi-19790126No ratings yet
- Veljko Vlaisavljević, Marko Došen, Borut Kovačic ̌ - Embryo Quality and Pregnancy Outcome in Infertile Patients With Endometriosis - Intech (2012) PDFDocument500 pagesVeljko Vlaisavljević, Marko Došen, Borut Kovačic ̌ - Embryo Quality and Pregnancy Outcome in Infertile Patients With Endometriosis - Intech (2012) PDFRoxana DalioNo ratings yet
- Pathophysiology of Type 1 DiabetesDocument14 pagesPathophysiology of Type 1 DiabetesBoNo ratings yet
- Neonatal Respiratory System Updates 2020Document824 pagesNeonatal Respiratory System Updates 2020link_wolfloboNo ratings yet
- 4th Edition World Health Organization Classification For Thyroid Tumors, Asian PerspectivesDocument24 pages4th Edition World Health Organization Classification For Thyroid Tumors, Asian PerspectivesbeosroNo ratings yet
- Disorders of Red Blood CellsDocument27 pagesDisorders of Red Blood Cellskirti sharmaNo ratings yet
- Hemodialysis Case PresentationDocument25 pagesHemodialysis Case Presentationapi-590340413No ratings yet
- Paget's Disease of BonesDocument40 pagesPaget's Disease of BonesOlga GoryachevaNo ratings yet
- Case Study Obstetric PatientDocument19 pagesCase Study Obstetric PatientPrinz Lozano100% (1)
- Test Bank For Introduction To Critical Care Nursing 6th Edition Mary Lou SoleDocument8 pagesTest Bank For Introduction To Critical Care Nursing 6th Edition Mary Lou SoleJessica Smith100% (31)
- Ayurved TerminologiesDocument30 pagesAyurved TerminologiesVipul RaichuraNo ratings yet
- BilirubinDocument3 pagesBilirubinIkhza LastPandawaNo ratings yet
- Danger Signs in Newborn DR Varsha Atul ShahDocument22 pagesDanger Signs in Newborn DR Varsha Atul ShahRSU ALFUADI BINJAINo ratings yet
- Indications For TetracyclineDocument135 pagesIndications For TetracyclinemariobbsNo ratings yet