Professional Documents
Culture Documents
I RECOVER Long COVID Protocol 1 - 230430 - 232114 PDF
Uploaded by
elfriadiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
I RECOVER Long COVID Protocol 1 - 230430 - 232114 PDF
Uploaded by
elfriadiCopyright:
Available Formats
Table of Contents
Disclaimer ...................................................................................................................................................... 3
About Long COVID ......................................................................................................................................... 3
Theories for why long COVID occurs ............................................................................................................. 3
Groups of symptoms...................................................................................................................................... 4
Initial screening tests for long COVID ........................................................................................................ 5
Approach to treatment .............................................................................................................................. 5
References .................................................................................................................................................... 7
I-RECOVER: Long COVID Treatment 2/3/2023 2
Disclaimer
The information in this document is our recommended approach based on the best (and most recent)
literature. It is provided as guidance to healthcare providers worldwide. Our guidance should only be
used by medical professionals in formulating their approach to patients. Patients should always consult
with their provider before starting any medical treatment.
As this is a highly dynamic topic, we will update these guidelines as new information emerges. Please
check to ensure you are using the latest version of this protocol.
About Long COVID
Due to the marked overlap between long COVID and post-vaccine syndrome, please refer to the
I-RECOVER Post-Vaccine Treatment protocol for detailed treatment strategies. This document highlights
the differences between these two syndromes.
Long COVID, also known as Long Haul COVID Syndrome (LHCS) and more recently by the terminology
“Post-acute sequelae of COVID-19 (PASC), is a heterogenous syndrome characterized by prolonged
malaise, headaches, generalized fatigue, sleep difficulties, hair loss, smell disorder, decreased appetite,
painful joints, dyspnea, chest pain, and cognitive dysfunction. [1-13]
Up to 80% of patients experience prolonged illness after COVID-19. Furthermore, many of the symptoms
of are common to COVID-19 vaccine-injured patients; indeed, both disorders are considered
manifestations of “spike protein-related disease,” with a significant overlap in symptoms, pathogenesis,
and treatment.
To complicate this issue further, many long COVID patients are vaccinated, and the symptomatology of
vaccine-injured patients is often exacerbated by an acute COVID-19 infection.
Long COVID may persist for months after the acute infection and almost half of patients report reduced
quality of life. Patients may suffer prolonged neuropsychological symptoms, including multiple domains
of cognition. [10;14] A puzzling feature of long COVID is that it is not predicted by initial disease severity;
long COVID frequently occurs in people who had mild-to-moderate cases and in younger adults who did
not require respiratory support or intensive care. [12]
The symptom set of long COVID is, in the majority of cases, very similar to chronic inflammatory
response syndrome (CIRS)/myalgic encephalomyelitis/chronic fatigue syndrome. [12] An important
differentiating factor from CIRS is the observation that long COVID continues to improve on its own,
albeit slowly in the majority of cases. Another important observation is that long COVID includes more
young people compared to severe COVID, which affects older people or persons with comorbidities.
Furthermore, the similarity between mast cell activation syndrome (MCAS) and long COVID has been
observed, and many consider long COVID to be a variant of MCAS. [15]
Theories for why long COVID occurs
Long COVID is highly heterogeneous and likely results from a variety of pathogenetic mechanisms.
Furthermore, it is likely that delayed treatment in the early symptomatic phase results in a high viral
I-RECOVER: Long COVID Treatment 2/3/2023 3
load (high spike protein load), which increases the risk and severity of long COVID. The following
theories have been postulated to explain long COVID: [12]
1. Ongoing respiratory symptoms (shortness of breath, cough, reduced effort tolerance) may be
related to unresolved organizing pneumonia (activated pulmonary macrophages).
2. Monocyte and microglia activation. Persistence of Spike protein in monocytes, macrophages,
pericytes and microglia results in an ongoing inflammatory response in an attempt by the
immune system to clear the offending protein(s) and viral RNA fragments.
3. The neurological symptoms may be related to micro- and/or macrovascular thrombotic disease,
which appears to be common in severe COVID-19 disease. [16] The brain microvasculature
expresses ACE-2 receptors and SARS-CoV-2 “pseudovirions” may bind to the microvascular
endothelium causing cerebral microvascular inflammation and clotting. [17] Brain MRIs 3
months post-infection demonstrated microstructural changes in 55% of patients. [18]
4. Due to molecular mimicry, the spike protein results in a vast spectrum of autoantibodies, many
of which are associated with neurological complications. In particular, features of
encephalopathy may be related to encephalitis and auto-reactive brain antibodies. [19] Small
fiber neuropathy and autonomic neuropathy (POTS) are directly associated with the presence of
autoantibodies. Antibodies against the ACE2 receptor and G-coupled membrane receptors are
commonly found in long COVID patients. [20-22]
5. An unmasking or triggering of MCAS. Mast cells are present in the brain, especially in the
median eminence of the hypothalamus, where they are located perivascularly close to nerve
endings positive for corticotropin-releasing hormone. [23] Following stimulation, mast cells
release proinflammatory mediators such as histamine, tryptase, chemokines, and cytokines,
which may result in neurovascular inflammation. [23] The “brain fog,” cognitive impairment and
general fatigue reported in long COVID may be due to mast cell-related neurovascular
inflammation.
6. Immune suppression with reactivation of dormant viruses and/or reactivation of chronic
bacterial infections (i.e., Lyme disease, etc.).
Groups of symptoms
Further, the clinical signs and symptoms can be grouped into the following clusters. The reason for this
grouping is to allow organ-specific targeted therapy or individualized therapy:
1. Respiratory: shortness of breath, congestion, persistent cough, etc.
2. Neurological/psychiatric: brain fog, malaise, tiredness, headaches, migraines, depression,
inability to focus or concentrate, altered cognition, insomnia, vertigo, panic attacks, tinnitus,
anosmia, phantom smells, etc.
3. Musculoskeletal: myalgias, fatigue, weakness, joint pains, inability to exercise, post-exertional
malaise, inability to perform normal activities of daily life
4. Cardiovascular: Palpitations, arrhythmias, Raynaud-like syndrome, hypotension, and tachycardia
on exertion
5. Autonomic: Postural tachycardia syndrome (POTs), abnormal sweating
6. Gastrointestinal disturbance: anorexia, diarrhea, bloating, vomiting, nausea, etc.
I-RECOVER: Long COVID Treatment 2/3/2023 4
7. Dermatologic: itching, rashes, dermatographia
8. Mucus membranes: running nose, sneezing, burning and itchy eyes
Initial screening tests for long COVID
Many patients undergo a vast array of diagnostic tests including cytokines and chemokines,
autoantibodies, and toxicological studies. These tests are expensive, have very little clinical relevance,
and only complicate the management of these patients.
The following basic tests are recommended:
• CBC with lymphocyte count and CD8+ count
• Chemistry with liver function tests
• CRP (inflammation)
• Ferritin (macrophage activation)
• D-dimer
• Early morning cortisol
• Thyroid function tests
• HbA1C—long COVID patients are at an increased risk of developing diabetes
• Autoantibodies: antiphospholipid antibody and ANA
• In patients with allergic features or those who experienced an acute reaction to the vaccine, the
following tests may be helpful: eosinophil count; IgE levels, RAST testing and/or skin testing.
Serum tryptase, serum histamine and/or 24-h urine N-methylhistamine should be considered in
MCAS. [24]
• Reactivated viruses: Antibodies/PCR against EBV Herpes I/II and CMV
• Vitamin D level
Specific Phenotypic tests
• CXR / chest CT with contrast
• Brain MRI
• ECHO
Approach to treatment
Healthcare providers are referred to I-RECOVER: Post-Vaccine Treatment protocol for specific guidance
regarding the treatment of long COVID. This document outlines the major differences between the
management of long COVID and vaccine injury, namely ongoing organizing pneumonia.
Furthermore, although numerous reports describe the epidemiology and clinical features of long COVID,
[1-11] studies evaluating treatment options are glaringly sparse. [25] Indeed, the NICE guidelines for
managing the long-term effects of COVID-19 provide no specific pharmacologic treatment
recommendations. [26] Patients with long COVID should be managed by clinicians who have experience
treating this troublesome disorder.
The treatment approach should be individualized according to the grouping of clinical signs and
symptoms. However, in general, it is likely that patients who did not receive adequate antiviral
treatment (e.g., ivermectin, etc.) and adequate anti-inflammatory/macrophage repolarization treatment
during the acute symptomatic phase of COVID-19 are more likely to develop long COVID.
I-RECOVER: Long COVID Treatment 2/3/2023 5
The major difference between long COVID and post-vaccine syndrome patients is unresolved organizing
pneumonia with persistent respiratory symptoms. Therefore, chest imaging is suggested in patients with
ongoing respiratory symptoms (preferably a chest CT scan).
Those with unresolved pulmonary inflammation (organizing pneumonia with ground glass opacification)
should be treated with a course of corticosteroids. Low-dose prednisolone/methylprednisolone (10
mg/day) for six weeks is suggested. [27] However, the patients’ symptoms and CRP should be followed
closely, as a dose escalation may be required in those who respond poorly.
An unknown number of patients who have recovered from COVID-19 organizing pneumonia will develop
pulmonary fibrosis with associated limitation of activity. Pulmonary function testing demonstrates a
restrictive type pattern with decreased residual volume and DLCO. [7] These patients should be referred
to a pulmonologist with expertise in pulmonary fibrosis. Anti-fibrotic therapy may have a role in these
patients, [28-31] however additional data is required before this therapy can be more generally
recommended. The serotonin receptor blocker cyproheptadine may reduce the risk of pulmonary
fibrosis. [32]
I-RECOVER: Long COVID Treatment 2/3/2023 6
References
1. Carfi A, Bernabei R, Landi F. Persistent symptoms in patients after acute COVID-19. JAMA 2020.
2. Prescott HC, Girard TD. Recovery from Severe COVID-19. Leveraging the lessons of survival from
sepsis. JAMA 2020.
3. Greenhalgh T, Knight M, A'Court C, Buxton M, Husain L. Management of post-acute Covid-19 in
primary care. BMJ 2020.
4. Chopra V, Flanders SA, O'Malley M. Sixty-day outcomes among patients hospitalized with
COVID-19. Ann Intern Med 2020.
5. Mandal S, Barnett J, Brill SE, Brown JS, Hare SS. 'Long-COVID': a cross-sectional study of
persisting symptoms, biomarker and imaging abnormalities following hospitalization for COVID-
19. Thorax 2020.
6. Michelen M, Manoharan L, Elkheir N, Cheng V, Dagens D, Hastie C. Characterising long-term
covid-19: a rapid living systematic review. medRxiv 2020.
7. Huang C, Huang L, Wang Y, Li X, Ren L, Gu X. 6-month consequences of COVID-19 in patients
discharged feom hospital: a cohort study. Lancet 2021.
8. Logue JK, Franko NM, McCulloch DJ, McDonald D. Sequelae in adults at 6 months after COVID-19
infection. JAMA Network Open 2021; 4:e210830.
9. Janiri D, Carfi A, Kotzalidis GD, Bernabei R. Posttraumatic stress disorder in patients after severe
COVID-19 infection. JAMA Psychiatry 2021.
10. Voruz P, Allali G, Benzakour L, Jacot I, Pierce J. Long COVID neuropsychological deficits after
severe, moderate or mild infection. medRxiv 2021.
11. Al-Aly Z, Xie Y, Bowe B. High-dimensional characterization of post-acute sequalae of COVID-19.
Nature 2021.
12. Yong SJ. Long-haul COVID-19: Putative pathophysiology, risk factors, and treatments. medRxiv
2020.
13. Bek LM, Berentschot JC, Huijts S, Vlake JH, Aerts JG. Symptoms persisting after hospitalization
for COVID-19: 12 month interim results of the COFLOW study. medRxiv 2021.
14. Taquet M, Geddes JR, Husain M, Luciano S, Harrison PJ. 6-month neurological and psychiatric
outcomes in 236 379 survivors of COVID-19: a retrospective cohort study using electronic health
records. Lancet Psychiatry 2021.
15. Afrin LB, Weinstock LB, Molderings GJ. COVID-19 hyperinflammation and post-Covid-19 illness
may be rooted in mast cell activation syndrome. Int J Infect DIs 2020.
16. Bryce C, Grimes Z, Pujadas E, Ahuja S, Beasley MB, Albrecht R et al. Pathopysiology of SARS-CoV-
2: targeting of endothelial cells renders a complex disease with thrombotic microangiopathy and
aberrant immune response. The Mount Sinai COVID-19 autopsy experience. medRxiv 2020.
17. Magro CM, Mulvey JJ, Laurence J, seshan S, Crowson AN, Harp J. Docked severe acute
respiratory syndrome coronavirus 2 proteins within the cutaneous and subcutaneous
microvasculature and their role in the pathogenesis of severe coronavirus disease 2019. Human
Pathology 2020; 106:106-116.
18. Lu Y, Li X, Geng D, Mei N, Wu PY, Huang CC. Cerebral micro-structutal changes in COVID-19
patients - An MRI-based 3-month follow-up study. EClinicalMedicine 2020.
19. Franke C, Ferse C, Kreye J, Rocco A, Hosp J. High frequency of cerebrospinal fluid autoantibodies
in COVID-19 patients with neurological symptoms. Brain,Behavor, and Immunity 2021.
20. Arthur JM, Forrest JC, Boehme KW, Kennedy JL, Owens S, Liu J. Development of ACE2
autoantibodies after SARS-CoV-2 infection. PloS ONE 2021; 16:e0257016.
21. Cabral-Marques O, Halpert G, Schimke LF, Ostrinski Y, Vojdani A, Lattin MT. Autoantibodies
targeting GPCRs and RAS-related molecules associated with COVID-19 severity. Nature
Communications 2022; 13:1220.
I-RECOVER: Long COVID Treatment 2/3/2023 7
22. Wallukat G, Hohberger B, Wenzel K, Furst J, Wallukat A. Functional autoantibodies against G-
protein coupled receptors in patients with persistent Long-Covid-19 symptoms. Journal of
Translational Autoimmunity 2021; 4:100100.
23. Theoharides TT, Cholevas C, Polyzoidis K, Poliotis A. Long-COVID syndrome-associated brain fog
and chemofog: Luteolin to the rescue. Biofactors 2021; 47:232-241.
24. Theoharides TC, Tsilioni I, Ren H. Recent advances in our understanding of mast cell activation-
or should it be mast cell mediator disorders? Expert Rev Clin Immunol 2019; 15:639-656.
25. Zilberman-Itskovich S, Catalogna M, Sasson E, Hadanny A, Lang E, Finci S et al. Hyperbaric
oxygen therapy improves neurocognitive functions and symptoms of post-COVID condition:
randomized controlled trial. Scientific Reports 2022; 12:11252.
26. COVID-19 rapid guideline: managing the long-term effects of COVID-19. www nice org
uk/guidance/ng188 [ 2020 [cited 2021 Apr. 26];
27. Dhooria S, Chaudhary S, Sehgal IS, Agarwal R, Arora S. High-dose versus low-dose prednisolone
in symptomatic patients with post-COVID-19 diffuse parenchymal lung abnormalities: an open-
label, randomised trial (COLDSTER). Eur Respir J 2021.
28. Seifirad S. Pirfenidone: A novel hypothetical treatment for COVID-19. Medical Hypotheses 2020;
144:11005.
29. Saba A, Vaidya PJ, Chavhan VB, Achlerkar A, Leuppi J. Combined pirfenidone, azithromycin and
prednisolone in post-H1N1 ARDS pulmonary firbosis. Sarcoidosis Vasc Diffuse Lung Dis 2018;
35:85-90.
30. Spagnolo P, Balestro E, Aliberti S, Cocconcelli E, Biondini D, Casa GD. Pulmonary fibrosis
secondary to COVID-19: a call to arms? Lancet Resp Med 2020; 8:750-752.
31. George PM, Wells AU, Jenkins RG. Pulmonary fibrosis and COVID-19: the potential role for
antibibrotic therapy. Lancet Resp Med 2020; 8:807-815.
32. Skurikhin EG, Andreeva TV, Khnelevskaya ES, Ermolaeva LA, Pershina OV, Krupin VA. Effect of
antiserotonin drug on the development of lung fibrosis and blood system reactions after
intratracheal administration of bleomycin. Bull Exp Biol Med 2012; 152:519-523.
I-RECOVER: Long COVID Treatment 2/3/2023 8
You might also like
- Long Covid - The Long Covid Book for Clinicians and Sufferers - Away from Despair and Towards UnderstandingFrom EverandLong Covid - The Long Covid Book for Clinicians and Sufferers - Away from Despair and Towards UnderstandingNo ratings yet
- Post COVID 19 Long Hauler Symptoms Diagnosis & Management Handbook & Mobile Application: Physician and Patient Assistance Handbook to Distinguish Between Chronic Illness or COVID related IllnessFrom EverandPost COVID 19 Long Hauler Symptoms Diagnosis & Management Handbook & Mobile Application: Physician and Patient Assistance Handbook to Distinguish Between Chronic Illness or COVID related IllnessNo ratings yet
- Long COVID A Cytokine-Based Model For The Pathophysiology oDocument47 pagesLong COVID A Cytokine-Based Model For The Pathophysiology oIchlasul MadriddistaNo ratings yet
- Long Covid 1Document5 pagesLong Covid 1lakshminivas PingaliNo ratings yet
- Preprints202307 1081 v1Document19 pagesPreprints202307 1081 v1goyapatez2No ratings yet
- Clinical Management of Persons Admitted To Hospita v1 19 March 2020 PDFDocument13 pagesClinical Management of Persons Admitted To Hospita v1 19 March 2020 PDFAndreea DobreNo ratings yet
- Manajemen Klinis Rumah Sakit Bagi Pasien Dengan Dugaan Terkena COVID-19 (Bahasa Inggris)Document13 pagesManajemen Klinis Rumah Sakit Bagi Pasien Dengan Dugaan Terkena COVID-19 (Bahasa Inggris)PERDHAKINo ratings yet
- Management Booklet Coronavirus Disease MOHP - 2019 - 28marchDocument22 pagesManagement Booklet Coronavirus Disease MOHP - 2019 - 28marchSanaa SbdelghanyNo ratings yet
- CAP+Clinical+Guideline+ (Adults) v2 FINAL Jan2021+Document11 pagesCAP+Clinical+Guideline+ (Adults) v2 FINAL Jan2021+Tuna AhsanNo ratings yet
- Management Booklet Coronavirus Disease 2019 - 28marchDocument22 pagesManagement Booklet Coronavirus Disease 2019 - 28marchEzz123456789No ratings yet
- Adverse Effects of COVID-19 Vaccines - 2022-06-05Document3 pagesAdverse Effects of COVID-19 Vaccines - 2022-06-05A. Jaime OptimaNo ratings yet
- COVID-19: A Recommendation To Examine The Effect of Hydroxychloroquine in Preventing Infection and ProgressionDocument4 pagesCOVID-19: A Recommendation To Examine The Effect of Hydroxychloroquine in Preventing Infection and ProgressionDaniel ChávezNo ratings yet
- Long Covid Syndrome-Associated Brain Fog and ChemofogDocument10 pagesLong Covid Syndrome-Associated Brain Fog and ChemofogindanazulfaaNo ratings yet
- IM GRP 3Document11 pagesIM GRP 3Dale Maninantan De DiosNo ratings yet
- Math A Guide To Managing The HospitalizedDocument43 pagesMath A Guide To Managing The HospitalizedAjla SalihovicNo ratings yet
- COVID-19 A Recommendation To ExamineDocument4 pagesCOVID-19 A Recommendation To ExamineDayalisis E. RodriguezNo ratings yet
- Causes and Treatments For Long Haul CovidDocument4 pagesCauses and Treatments For Long Haul Covidandrogynus100% (1)
- METHAMEDICINDocument21 pagesMETHAMEDICINRobert ManriqueNo ratings yet
- Acute Disseminated Encephalomyelitis Post Sars-Cov-2 VaccinationDocument4 pagesAcute Disseminated Encephalomyelitis Post Sars-Cov-2 VaccinationIJAR JOURNALNo ratings yet
- Early ViewDocument34 pagesEarly Viewyesid urregoNo ratings yet
- OutDocument22 pagesOutANITA HUTAURUKNo ratings yet
- Long-COVID: An Evolving Problem With An Extensive Impact: Clinical UpdateDocument3 pagesLong-COVID: An Evolving Problem With An Extensive Impact: Clinical UpdateArif wicaksonoNo ratings yet
- Long Covid CDCDocument4 pagesLong Covid CDCXiaowei ZhongNo ratings yet
- "LONG COVID": An InsightDocument17 pages"LONG COVID": An InsightsilentluciditysfNo ratings yet
- Jurnal Kel3 Fiks BGTDocument14 pagesJurnal Kel3 Fiks BGTIntanAsmarani OfficialNo ratings yet
- 2020 REPORT: Global Strategy For The Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary DiseaseDocument53 pages2020 REPORT: Global Strategy For The Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary DiseaseManoj GhimireNo ratings yet
- Cells 12 00816 v2Document24 pagesCells 12 00816 v2Fernando ErnestoNo ratings yet
- Triage de HipoxiaDocument5 pagesTriage de HipoxiaMardithaNo ratings yet
- 05june2020 20200106 Clinical Management Guidelines For COVID-19 Infection v2Document13 pages05june2020 20200106 Clinical Management Guidelines For COVID-19 Infection v2Murtaza HasanNo ratings yet
- Possible Role of P-SelectinDocument30 pagesPossible Role of P-SelectinIoanna Bianca HNo ratings yet
- Anesthaesia and Intensive CareDocument139 pagesAnesthaesia and Intensive CareIvan Kurniadi100% (2)
- Clase 1. COVID-19 - Management in Hospitalized AdultsDocument44 pagesClase 1. COVID-19 - Management in Hospitalized AdultsJose OrtizNo ratings yet
- COVID 19 Management-Pocket Notes: Department of Critical Care Medicine, Bharati Vidyapeeth (DTU) Medical College, PuneDocument24 pagesCOVID 19 Management-Pocket Notes: Department of Critical Care Medicine, Bharati Vidyapeeth (DTU) Medical College, PunedrvinitaNo ratings yet
- Anakinra TheraphyDocument16 pagesAnakinra TheraphyNi Made Ari PramitaNo ratings yet
- Immune Reconstitution InflammatoryDocument10 pagesImmune Reconstitution InflammatoryBhanu KumarNo ratings yet
- Diagnosis and Treatment Protocol For COVID-19 Patients: (Trial Version 8)Document32 pagesDiagnosis and Treatment Protocol For COVID-19 Patients: (Trial Version 8)Fernando Ruben Rivera CastilloNo ratings yet
- Main PDFDocument4 pagesMain PDFRSDC Tower 5No ratings yet
- Assessment of Chronic Cough - BMJDocument84 pagesAssessment of Chronic Cough - BMJqayyum consultantfpscNo ratings yet
- AnnalsATS 202003-233PSDocument4 pagesAnnalsATS 202003-233PSambitiousamit1No ratings yet
- Overview of Neutropenic Fever SyndromesDocument16 pagesOverview of Neutropenic Fever Syndromesnon_zenseNo ratings yet
- Marco Cascella, Elvio de Blasio - Features and Management of Acute and Chronic Neuro-Covid-Springer (2021)Document172 pagesMarco Cascella, Elvio de Blasio - Features and Management of Acute and Chronic Neuro-Covid-Springer (2021)bbadoNo ratings yet
- Recurrent MeningitisDocument14 pagesRecurrent Meningitisidno1008No ratings yet
- Long COVID Guidelines Need To Reflect Lived Experience: CommentDocument3 pagesLong COVID Guidelines Need To Reflect Lived Experience: CommentAlexandra PimentaNo ratings yet
- National Comprehensive Guidelines For Management of Post-Covid SequelaeDocument36 pagesNational Comprehensive Guidelines For Management of Post-Covid SequelaeGaurav NandaNo ratings yet
- JMedLife 16 195Document8 pagesJMedLife 16 195Victoria VelardeNo ratings yet
- Covid19 HypercoagulabilityDocument22 pagesCovid19 Hypercoagulability陳瑞豐No ratings yet
- Novel CoronavirusDocument7 pagesNovel CoronavirusMustafa KhudhairNo ratings yet
- Immediate and Long-Term Consequences of COVID-19 Infections For The Development of Neurological DiseaseDocument3 pagesImmediate and Long-Term Consequences of COVID-19 Infections For The Development of Neurological DiseaseMaca Martínez-CuitiñoNo ratings yet
- Example of A Case Report-Cryptococcoal and IRISDocument5 pagesExample of A Case Report-Cryptococcoal and IRISTorgbui Gorni Treve IVNo ratings yet
- Overview of Neutropenic Fever SyndromesDocument30 pagesOverview of Neutropenic Fever SyndromesAna María Díaz MedinaNo ratings yet
- CACHEXIA J Cachexia Sarcopenia Muscle - 2022 - Rodriguez - Development and Early Diagnosis of Critical Illness Myopathy in COVID 19 22Document13 pagesCACHEXIA J Cachexia Sarcopenia Muscle - 2022 - Rodriguez - Development and Early Diagnosis of Critical Illness Myopathy in COVID 19 22ediNo ratings yet
- Anaesthesia & Intensive Care: For Fcai, Frca EdaicDocument139 pagesAnaesthesia & Intensive Care: For Fcai, Frca EdaicMuhammad Farid100% (2)
- Sepsis 2023 What Works and What Doesnt Judge Notes For DistributionDocument15 pagesSepsis 2023 What Works and What Doesnt Judge Notes For Distributionsansanee.sucNo ratings yet
- CONTINUATIONDocument6 pagesCONTINUATIONBHAVANA VNNo ratings yet
- Treating Long Haul Syndrome PDFDocument9 pagesTreating Long Haul Syndrome PDFNICOLAE100% (1)
- Chapter 2Document14 pagesChapter 2rahayusri yayuNo ratings yet
- Bahasa Inggris Keolompok 2Document17 pagesBahasa Inggris Keolompok 2Navi MayNo ratings yet
- Coronavirus, Enfoque Actual, Tratamiento FarmacologicoDocument15 pagesCoronavirus, Enfoque Actual, Tratamiento FarmacologicoEvanns Vela RuizNo ratings yet
- Aspectos Autonómicos Post CovidDocument7 pagesAspectos Autonómicos Post Covidtavo570No ratings yet
- Cvac 115Document21 pagesCvac 115Theofana MihailaNo ratings yet
- Form 9 Harian Ga Jan 2019 20Document24 pagesForm 9 Harian Ga Jan 2019 20elfriadiNo ratings yet
- Form 9 Harian Ga Jan 2019 16Document20 pagesForm 9 Harian Ga Jan 2019 16elfriadiNo ratings yet
- Form 9 Harian Ga December 2019Document24 pagesForm 9 Harian Ga December 2019elfriadiNo ratings yet
- Form 9 Harian QG Jan 2022Document25 pagesForm 9 Harian QG Jan 2022elfriadiNo ratings yet
- Form 9 Harian QG Jan 2022Document15 pagesForm 9 Harian QG Jan 2022elfriadiNo ratings yet
- Form 9 Harian QG Jan 2022Document55 pagesForm 9 Harian QG Jan 2022elfriadiNo ratings yet
- Form 9 Harian QG Jan 2022Document30 pagesForm 9 Harian QG Jan 2022elfriadiNo ratings yet
- Form 9 Harian Ga Jan 2019Document4 pagesForm 9 Harian Ga Jan 2019elfriadiNo ratings yet
- Form 9 Harian Ga Jan 2022...Document5 pagesForm 9 Harian Ga Jan 2022...elfriadiNo ratings yet
- Form 9 Harian QG Jan 2022Document25 pagesForm 9 Harian QG Jan 2022elfriadiNo ratings yet
- 1 Form 9 Charter Flight Travira Feb 2022Document5 pages1 Form 9 Charter Flight Travira Feb 2022elfriadiNo ratings yet
- Form 9 Harian QG Jan 2022Document5 pagesForm 9 Harian QG Jan 2022elfriadiNo ratings yet
- 01 Agustus 2018 MalindoDocument2 pages01 Agustus 2018 MalindoelfriadiNo ratings yet
- 01 Juli 2018 MalindoDocument2 pages01 Juli 2018 MalindoelfriadiNo ratings yet
- 01 Oktober 2018 LionDocument4 pages01 Oktober 2018 LionelfriadiNo ratings yet
- Form 9 Harian Ga Jan 2019Document4 pagesForm 9 Harian Ga Jan 2019elfriadiNo ratings yet
- 01 Oktober 2018 BatikDocument6 pages01 Oktober 2018 BatikelfriadiNo ratings yet
- 01 Juli 2018 WingsDocument2 pages01 Juli 2018 WingselfriadiNo ratings yet
- 01 Juni 2018 BatikDocument6 pages01 Juni 2018 BatikelfriadiNo ratings yet
- 01 Juli 2018 LionDocument4 pages01 Juli 2018 LionelfriadiNo ratings yet
- 01 Agustus 2018 WingsDocument2 pages01 Agustus 2018 WingselfriadiNo ratings yet
- 01 Agustus 2018 Wings PostponeDocument2 pages01 Agustus 2018 Wings PostponeelfriadiNo ratings yet
- 01 Agustus 2018 WingsDocument2 pages01 Agustus 2018 WingselfriadiNo ratings yet
- Rekapitulasi Penerbitan Laik Terbang 241122 Batch 1Document48 pagesRekapitulasi Penerbitan Laik Terbang 241122 Batch 1elfriadiNo ratings yet
- 01 Agustus 2018 LionDocument4 pages01 Agustus 2018 LionelfriadiNo ratings yet
- 01 Agustus 2018 BatikDocument6 pages01 Agustus 2018 BatikelfriadiNo ratings yet
- Misasmatic PrescribingDocument28 pagesMisasmatic PrescribingAli AkbarNo ratings yet
- ENT Deferential Diagnosis MEDADDocument22 pagesENT Deferential Diagnosis MEDADReham AshourNo ratings yet
- About Pancreatic Cancer - A Quick GuideDocument4 pagesAbout Pancreatic Cancer - A Quick Guide085857173575No ratings yet
- QCGH Appendicitis ReportDocument48 pagesQCGH Appendicitis ReportIsabel ArcangelNo ratings yet
- High Risk PregnancyDocument12 pagesHigh Risk Pregnancyggrrk7100% (2)
- The Technique: of ThyroidectomyDocument5 pagesThe Technique: of Thyroidectomyعمر كمالNo ratings yet
- Hypertensive EmergencyDocument17 pagesHypertensive EmergencyNhã PhạmNo ratings yet
- RLE III - A ENT MED Day 1Document7 pagesRLE III - A ENT MED Day 1Kristian Karl Bautista Kiw-isNo ratings yet
- Myasthenia Gravis Case Study 2Document2 pagesMyasthenia Gravis Case Study 2PJHGNo ratings yet
- Cardio WorkbookDocument5 pagesCardio WorkbookZhy Caluza100% (1)
- Acquired CataractDocument39 pagesAcquired CataractRaja Taha Yaseen KhanNo ratings yet
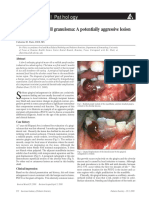
- Peripheral Giant Cell Granuloma: A Potentially Aggressive Lesion in ChildrenDocument2 pagesPeripheral Giant Cell Granuloma: A Potentially Aggressive Lesion in ChildrenYeni PuspitasariNo ratings yet
- Liver Cirrhosis: DR Alex MogereDocument51 pagesLiver Cirrhosis: DR Alex MogereGladys Maina100% (1)
- 10 Diagnosa Terbanyak FKTPDocument3 pages10 Diagnosa Terbanyak FKTPtandun nlmNo ratings yet
- Which Is Not True of Cardiopulmonary Resuscitation (CPR) ?Document241 pagesWhich Is Not True of Cardiopulmonary Resuscitation (CPR) ?Mostafa Kamel TemrazNo ratings yet
- The Content of This Leaflet Was Updated According To The Guidelines of The Ministry of Health in September 2017Document14 pagesThe Content of This Leaflet Was Updated According To The Guidelines of The Ministry of Health in September 2017ddandan_2No ratings yet
- Conversion Disorder, Functional Neurological Symptom Disorder, and Chronic Pain - Comorbidity, Assessment, and TreatmentDocument10 pagesConversion Disorder, Functional Neurological Symptom Disorder, and Chronic Pain - Comorbidity, Assessment, and TreatmentViviana CalderónNo ratings yet
- Nasal Polyps: MR Stephen O'HanlonDocument32 pagesNasal Polyps: MR Stephen O'HanlonAkhnal SyaputraNo ratings yet
- Homoeopathy Treatment of Vitreous OpacitiesDocument4 pagesHomoeopathy Treatment of Vitreous OpacitiesVitorio VenturiniNo ratings yet
- Psychiatric Nursing p.213-231Document20 pagesPsychiatric Nursing p.213-231hurrikhen100% (1)
- MCQsin ENTwith Explanations Module 2 OtologyDocument7 pagesMCQsin ENTwith Explanations Module 2 OtologyFatina AryanNo ratings yet
- Patho SGD 1 PDFDocument5 pagesPatho SGD 1 PDFOella CabangonNo ratings yet
- Neurofibromatosis Type 1Document4 pagesNeurofibromatosis Type 1Adam LechnerNo ratings yet
- College FormularyDocument142 pagesCollege FormularymarcuscainedNo ratings yet
- TungDocument203 pagesTungValdemar Caumo Junior100% (5)
- Salivary Gland Tumors: 1. AdenomasDocument18 pagesSalivary Gland Tumors: 1. AdenomasMahammed Ahmed BadrNo ratings yet
- Randa Al-Harizy Prof of Internal MedicineDocument40 pagesRanda Al-Harizy Prof of Internal MedicinerafikaNo ratings yet
- Botulism: Sabari Krishnan B. B. RA1711014010088Document16 pagesBotulism: Sabari Krishnan B. B. RA1711014010088Sabari Krishnan B BNo ratings yet
- Drug Guideline For Iron Polymaltose InjectionDocument7 pagesDrug Guideline For Iron Polymaltose Injectionmirza_baig_46No ratings yet
- Augmentin DdsDocument12 pagesAugmentin DdsQureshi imtiyazNo ratings yet