Professional Documents
Culture Documents
Elbow Total Elbow Arthroplasty BWH
Uploaded by
nurul ulyaniOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Elbow Total Elbow Arthroplasty BWH
Uploaded by
nurul ulyaniCopyright:
Available Formats
Department of Rehabilitation Services
Total Elbow Arthroplasty Protocol:
The intent of this protocol is to provide the clinician with a guideline of the
postoperative rehabilitation course of a patient that has undergone a total elbow
arthroplasty (TEA). It is not intended to be a substitute for appropriate clinical
decision-making regarding the progression of a patient’s postoperative course. The
actual post-surgical therapy management must be based on the surgical approach,
physical exam/findings, individual progress, and/or the presence of postoperative
complications. If a clinician requires assistance in the progression of a patient post-
surgery, s/he should consult with the referring surgeon.
The semi-constrained, hinged (linked) prosthesis is the most commonly used prosthesis.
This prosthesis is stable postoperatively. Patients are encouraged to do range of motion
exercises and use their elbow for activities of daily living as dictated by their pain level
and status of wound healing. Wound management is critical following TEA.
A posterior triceps–sparing approach, which preserves the continuity of the triceps, when
possible, is typically used. Postoperatively the therapist and patient need to respect the
integrity of the triceps and posterior incision when performing both active and passive
elbow flexion exercises and functional activities. The surgeon may choose to limit
flexion range of motion based on the intraoperative inspection of the triceps tendon.
Postoperative range of motion expectations are influenced by a number of factors:
• Presence of preoperative flexion contractures.
• Severity and chronicity of underlying disease process and tissue quality.
For the purpose of this protocol, functional range of motion of the elbow is defined as
30 to 120/130 degrees of flexion and 60 degrees of supination and 60 degrees of
pronation around a neutral axis.
PHASE I – IMMEDIATE POST SURGICAL PHASE:
Phase I Goals:
• Allow healing of soft tissue.
• Maintain integrity of replaced joint, triceps tendon, and ligamentous
reconstruction (if applicable).
• Gradually restore active range of motion (AROM) of cervical spine,
shoulder/wrist/hand as indicated.
• Gradually increase active assisted range of motion (AAROM) of the elbow and
forearm.
Total Elbow Arthroplasty Protocol 1
© 2010, Department of Rehabilitation Services, Brigham & Women’s Hospital, Boston,
MA
• Reduce/minimize pain and inflammation.
• Manage distal upper extremity swelling.
• Regain independence with activities of daily living (ADLs) with modifications.
Phase I Precautions:
• Elbow is positioned in a soft posterior elbow splint @ about 60 degrees of flexion,
unless otherwise specified. A sling is used for comfort only. (A hinged elbow
brace or hard posterior elbow splint may be used to minimize varus/valgus forces
of the elbow if the surgeon is concerned about the integrity of the soft tissues and
surgical construct.)
• Therapists should assess for signs of ulnar neuropathy during the rehabilitation
process and alert the orthpaedic team if present.
• No lifting of objects greater than 1 lb. with operated upper extremity.
• No excessive stretching or sudden movements (particularly extension).
• No forced flexion secondary to incision and triceps tendon integrity.
• Avoid varus/valgus stress to the elbow (i.e. avoid excessive reaching across the
body with ADLs).
• No upper extremity weight bearing with the involved side. No assistive device for
ambulation should be used with operative upper extremity. No upper extremity
pushing motions against resistance.
• No soaking for 2 weeks, or until staples/sutures are removed and incision is dry
and intact.
• Report to surgeon any signs of delayed wound healing, drainage, and/or infection.
Early Phase I: (Post-operative day 1-7)
• Out of Sling/elbow splint as tolerated.
• AROM cervical spine, shoulder, wrist, and hand.
• Gentle AAROM elbow extension and flexion exercises initiated with elbow held
close to the body (adducted position) with forearm in neutral to pronation bias.
• Gentle AAROM supination and pronation exercises initiated with elbow held
close to the body. Unless otherwise instructed, forearm rotations are to be
completed with the elbow held at the side at 90 degrees of flexion to minimize
strain on ligamentous structures.
• Gentle gravity-assisted elbow extension stretching to enhance extension ROM.
• Frequent cryotherapy for pain, swelling, and inflammation management.
• Compressive wrapping/garments for edema management as indicated.
• Patient education regarding proper positioning, ROM precautions, joint protection
techniques, and ADLs.
Late Phase I: (Post-operative day 8 thru post-operative week 6):
Total Elbow Arthroplasty Protocol 2
© 2010, Department of Rehabilitation Services, Brigham & Women’s Hospital, Boston,
MA
• Patients are typically weaned out of the elbow splint for daytime use during their
2rd postoperative week, unless otherwise specified. The splint is typically worn
only at night and during high-risk activity (to avoid full elbow extension and
supination for those who have had a resurfacing procedure).
• Continue above exercises.
• Progress AROM cervical spine, shoulder, wrist, and hand exercises, while
following applicable precautions.
• AAROM/AROM elbow extension, flexion, supination, and pronation to tolerance.
o No combined extension and supination for those with resurfacing
procedure.
o Unless otherwise instructed, forearm rotations are to be completed with
the elbow held at the side at 90 degrees of flexion to minimize strain on
ligamentous structures.
• Continue cryotherapy and edema management as needed for pain and
inflammation.
• Scar management upon suture/staple removal.
PHASE II –FUNCTIONAL ACTIVITY PHASE
(Not to begin before 6 Weeks post-surgery to allow for appropriate soft tissue
healing):
Phase II Goals:
• To encourage functional ROM and strength of the elbow for ADLs, while
protecting healing soft tissues.
• Minimize pain and inflammation.
• Re-establish dynamic elbow stability.
Phase II Precautions:
• No repetitive motions of more than 5 lbs. and no single lifts of more than 15 lbs.
with operated upper extremity.
• Those patients with a resurfacing procedure should not perform combined
repetitive extension/supination exercise or activity.
• No upper extremity weight bearing, pushing, or pulling with the involved side.
Early Phase II (6-12 Weeks postoperatively):
• Continue above previous exercises as indicated.
• Most strengthening gains will be achieved by the patient gradually progressing
their activity level. The need for a vigorous strengthening program is not
appropriate following total elbow arthroplasty.
Total Elbow Arthroplasty Protocol 3
© 2010, Department of Rehabilitation Services, Brigham & Women’s Hospital, Boston,
MA
• 6 weeks postop: Begin submaximal painfree elbow/forearm/wrist/hand isometrics
at mid range of available elbow range of motion (all planes).
• 8 weeks postop: Progress to submaximal painfree elbow/forearm/wrist/hand
isometrics at multiple angles of available elbow range of motion. Avoid
isometrics at end ranges of motions.
• 10-12 Weeks postop: Progress to sub maximal pain free shoulder and
elbow/wrist/hand isotonic strengthening as motor control improves. (No weights
or resistance greater than 5 lbs.)
o Initially single plane elbow movement, then progress to composite
movements as appropriate. Those patients with a resurfacing procedure
should not perform combined repetitive extension/supination exercise or
activity.
• If patient has not achieved functional elbow range of motion of at least 120
degrees flexion then consider the use of a dynamic or static progressive splint.
Consult with surgeon.
• Continue use of cryotherapy and edema management for pain and inflammation
as needed.
Late Phase II (12 weeks postoperatively on):
• Typically patients are on a home program at this point focused on maintaining a
pain free functional arc of elbow motion.
• Continue previous exercises 2-3 x/ week to maintain ROM, strength, and function
upon discharge from therapy.
• No heavy lifting of objects (no heavier than 15 lbs) for life.
• No tennis or throwing activities for life.
Authors: Reviewers:
Jen Sayles, OTL/R Gayle Lang, OTL/R
Reg B. Wilcox III, PT Tom S. Thornhill, MD
3/07
Updated: Reviewer:
Reg B. Wilcox III, PT Tom S. Thornhill, MD
9/2010
© 2010, Department of Rehabilitation Services, Brigham & Women’s Hospital, Boston,
MA
Total Elbow Arthroplasty Protocol 4
© 2010, Department of Rehabilitation Services, Brigham & Women’s Hospital, Boston,
MA
You might also like
- Tips for Everyday Life and Sports With an Artificial Joint: Expert guidebook for dealing with a prosthesis for patients with a new hip or knee jointFrom EverandTips for Everyday Life and Sports With an Artificial Joint: Expert guidebook for dealing with a prosthesis for patients with a new hip or knee jointNo ratings yet
- Tha Protocol THRDocument6 pagesTha Protocol THRNiña del Prado 4thNo ratings yet
- Reverse Total Shoulder Arthroplasty RehabDocument4 pagesReverse Total Shoulder Arthroplasty Rehabprwill00No ratings yet
- Brigham & Women's Hospital - Elbow & Hand Rehabilitation PT ProtocolsDocument25 pagesBrigham & Women's Hospital - Elbow & Hand Rehabilitation PT ProtocolsShrutiNo ratings yet
- Tha ProtocolDocument7 pagesTha ProtocolJosephine SaesariaNo ratings yet
- Total Elbow Arthroplasty and RehabilitationDocument5 pagesTotal Elbow Arthroplasty and RehabilitationMarina ENo ratings yet
- Achilies Tendon RepairDocument16 pagesAchilies Tendon Repairapi-611889946No ratings yet
- Distal Radius FractureDocument10 pagesDistal Radius Fracturemajiavik11No ratings yet
- Total Shoulder Arthroplasty Tsa 2Document15 pagesTotal Shoulder Arthroplasty Tsa 2api-550365743No ratings yet
- ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon GraftDocument6 pagesACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon GraftArun TamilvananNo ratings yet
- Arthroscopic Shoulder Anterior Stabilisation Rehabilitation Protocol by TENDAYI MUTSOPOTSI MSc. ORTHO-MEDDocument8 pagesArthroscopic Shoulder Anterior Stabilisation Rehabilitation Protocol by TENDAYI MUTSOPOTSI MSc. ORTHO-MEDPhysiotherapy Care SpecialistsNo ratings yet
- Rehabilitation Guidelines For Post Operative Shoulder Instability Repair Updated20june08 - 0Document11 pagesRehabilitation Guidelines For Post Operative Shoulder Instability Repair Updated20june08 - 0Florin Vasile BosiNo ratings yet
- Rehab Guidelines For Reverse Shoulder ArthroplastyDocument7 pagesRehab Guidelines For Reverse Shoulder Arthroplastydeepak100% (1)
- Reverse Total Shoulder ProtocolDocument2 pagesReverse Total Shoulder Protocolsurender_singh_43No ratings yet
- Postoperative protocol distal humerus ORIFDocument3 pagesPostoperative protocol distal humerus ORIFRahma HanifaNo ratings yet
- Shoulder Post-Operative Rehabilitation ProtocolsDocument6 pagesShoulder Post-Operative Rehabilitation ProtocolsShrutiNo ratings yet
- ReverseTotalShoulderArthroplastyDocument3 pagesReverseTotalShoulderArthroplastyTiberiu BondreaNo ratings yet
- Post-op shoulder rehab protocolDocument3 pagesPost-op shoulder rehab protocolUpender YadavNo ratings yet
- Acl Reconstruction ProtocolDocument8 pagesAcl Reconstruction ProtocolFahd AbdelazimNo ratings yet
- Total Shoulder Arthroplasty GuidelineDocument17 pagesTotal Shoulder Arthroplasty GuidelineMaria Luísa MirandaNo ratings yet
- Physiotherapy in AmputationsDocument6 pagesPhysiotherapy in Amputationskrissh20No ratings yet
- Acromioplasty Rehab ProtocolDocument3 pagesAcromioplasty Rehab ProtocolJay RammaNo ratings yet
- Patellar Tendon Rupture and RehabilitationDocument4 pagesPatellar Tendon Rupture and RehabilitationdedsnetNo ratings yet
- Brigham & Women's Hospital - Knee Rehabilitation PT ProtocolsDocument27 pagesBrigham & Women's Hospital - Knee Rehabilitation PT ProtocolsShrutiNo ratings yet
- Tendon Transfers - RehabilitationDocument4 pagesTendon Transfers - RehabilitationPankaj Malik100% (4)
- Review of Hand Rehabilitation Protocols After Flexor Tendon Injury RepairDocument47 pagesReview of Hand Rehabilitation Protocols After Flexor Tendon Injury RepairtesfahuntekletilahunNo ratings yet
- Rehabilitation Protocol For LatarjetDocument4 pagesRehabilitation Protocol For LatarjetalizzxNo ratings yet
- distal-radius-fracture-postop-hand-therapy-guidelineDocument4 pagesdistal-radius-fracture-postop-hand-therapy-guidelineKhyathi SriNo ratings yet
- Triangular Fibrocartilage Complex (TFCC) Repair and RehabilitationDocument5 pagesTriangular Fibrocartilage Complex (TFCC) Repair and RehabilitationmksayshiNo ratings yet
- 15hip TotalHipArthroplastyDocument4 pages15hip TotalHipArthroplastyudaysravsNo ratings yet
- Role of Physiotherapy in Management of Burns-HshDocument25 pagesRole of Physiotherapy in Management of Burns-HshChristopher Chibueze Igbo100% (1)
- Acl Reconstruction ProtocolDocument8 pagesAcl Reconstruction ProtocolMestereaga AlinNo ratings yet
- ASEST Rotator Cuff Repair Rehab Guide Phases 1-2Document9 pagesASEST Rotator Cuff Repair Rehab Guide Phases 1-2ProfPT44No ratings yet
- HSSRehabilitationClinicalGuidelines Knee MedialCollateralLigament MCL Sprain Non OperativeDocument12 pagesHSSRehabilitationClinicalGuidelines Knee MedialCollateralLigament MCL Sprain Non OperativeJo CacerNo ratings yet
- Lower Extremity Prosthesis Part IIDocument98 pagesLower Extremity Prosthesis Part IIsjs6r8wwv9No ratings yet
- RE 304600 19 - TotalKneeArthroplasty PDFDocument4 pagesRE 304600 19 - TotalKneeArthroplasty PDFtriaNo ratings yet
- Flexor Tendon Repair Zones I IV 05 13 2013Document2 pagesFlexor Tendon Repair Zones I IV 05 13 2013Manish KumarNo ratings yet
- Hip ArthroplastyDocument29 pagesHip ArthroplastyAmiraa IbrahiimmNo ratings yet
- Shoulder SurgeryDocument3 pagesShoulder SurgeryTirumala RaoNo ratings yet
- Ankle Brostrom Gould Repair For Lateral Ankle Instablility BWHDocument6 pagesAnkle Brostrom Gould Repair For Lateral Ankle Instablility BWHanujNo ratings yet
- PCL Reconstruction - 2023Document15 pagesPCL Reconstruction - 2023mohamedhelalptNo ratings yet
- Arthroscopic Rotator Cuff Repair Protocol:: Peter J. Millett, MD, MSCDocument4 pagesArthroscopic Rotator Cuff Repair Protocol:: Peter J. Millett, MD, MSCPhooi Yee LauNo ratings yet
- Hip Labral Repair PresentationDocument15 pagesHip Labral Repair Presentationapi-612728940No ratings yet
- Rehabilitation Protocol For Clavicle OrifDocument3 pagesRehabilitation Protocol For Clavicle OrifJaneNo ratings yet
- Q&A About Total Knee ReplacementDocument4 pagesQ&A About Total Knee ReplacementDrManoj JagarlamudiNo ratings yet
- TRACTION LavlyDocument9 pagesTRACTION Lavlylabsky_evol100% (1)
- Weaver-Dunn Rehabilitation Protocol BY TENDAYI MUTSOPOTSIDocument6 pagesWeaver-Dunn Rehabilitation Protocol BY TENDAYI MUTSOPOTSIPhysiotherapy Care Specialists100% (1)
- Posterior Cruciate Ligament (PCL) Reconstruction Clinical Practice GuidelineDocument12 pagesPosterior Cruciate Ligament (PCL) Reconstruction Clinical Practice GuidelineYafiahnaf FirdausNo ratings yet
- Total Hip ArthroplastyDocument15 pagesTotal Hip Arthroplastyapi-550438875No ratings yet
- Foot and Ankle RehabDocument4 pagesFoot and Ankle RehabNysm NydNo ratings yet
- Hamstring Exercise ProgressionDocument15 pagesHamstring Exercise ProgressionFrancisco De VelascoNo ratings yet
- Total Hip ArthroplastyDocument15 pagesTotal Hip ArthroplastyDestiny BonetaNo ratings yet
- Rehabilitation Protocol For ACLDocument9 pagesRehabilitation Protocol For ACLgb tradeNo ratings yet
- Flexor Tendon Repairs Zones I III 05-13-2013Document3 pagesFlexor Tendon Repairs Zones I III 05-13-2013Mihaela DoniciNo ratings yet
- Rehabilitation Protocol After Anterior Cruciate Ligament ReconstructionDocument3 pagesRehabilitation Protocol After Anterior Cruciate Ligament ReconstructionTirumala RaoNo ratings yet
- Rehabilitation Protocol For Patella Quad TendonDocument5 pagesRehabilitation Protocol For Patella Quad TendonYova TmbxNo ratings yet
- RomsDocument31 pagesRomsAhsen RazaNo ratings yet
- Achilles Repair Protocol 2019Document10 pagesAchilles Repair Protocol 2019dNo ratings yet
- Length Tension Testing Book 1, Lower Quadrant: A Workbook of Manual Therapy TechniquesFrom EverandLength Tension Testing Book 1, Lower Quadrant: A Workbook of Manual Therapy TechniquesRating: 3.5 out of 5 stars3.5/5 (3)
- Klasifikasi Impaksi Caninus Rahang Atas Pada Pemeriksaan Radiograf Panoramik Dan CBCT Sebagai Penunjang OdontomyDocument8 pagesKlasifikasi Impaksi Caninus Rahang Atas Pada Pemeriksaan Radiograf Panoramik Dan CBCT Sebagai Penunjang OdontomyRahmi WastriNo ratings yet
- Human Physiology From Cells To Systems Sherwood 9th Edition Test BankDocument25 pagesHuman Physiology From Cells To Systems Sherwood 9th Edition Test Bankkeithzunigakzpcfjgbaw100% (27)
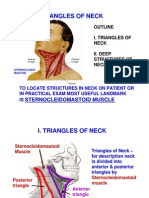
- Triangles of Neck: Sternocleidomastoid MuscleDocument28 pagesTriangles of Neck: Sternocleidomastoid MusclebibierabiaNo ratings yet
- Ankle&fEET Written Procedure-MagsombolDocument2 pagesAnkle&fEET Written Procedure-Magsombolhazell_aseronNo ratings yet
- Lab Worksheet 4 1 AnswersDocument5 pagesLab Worksheet 4 1 Answersjames bulawinNo ratings yet
- ANATOMY AND PHYSIOLOGY - HypokalemiaDocument2 pagesANATOMY AND PHYSIOLOGY - HypokalemiaJairah CandaoNo ratings yet
- Daftar Harga DiagnosaDocument9 pagesDaftar Harga DiagnosaIrpan FirmansyahNo ratings yet
- (Ebook PDF) Equine Ophthalmology 3Rd Edition by Brian C. GilgerDocument41 pages(Ebook PDF) Equine Ophthalmology 3Rd Edition by Brian C. Gilgerjessica.rohrbach136100% (46)
- Renal Ultrasound ProtocolDocument4 pagesRenal Ultrasound Protocolfouad tabetNo ratings yet
- Congenital Auricular Malformation: Dr. R. Isma Nurul A'IniDocument47 pagesCongenital Auricular Malformation: Dr. R. Isma Nurul A'Inithtkl irpNo ratings yet
- Occlusal Plane Change After Intrusion of Maxillary Posterior Teeth by Microimplants To Avoid Maxillary Surgery With Skeletal Class III Orthognathic SurgeryDocument10 pagesOcclusal Plane Change After Intrusion of Maxillary Posterior Teeth by Microimplants To Avoid Maxillary Surgery With Skeletal Class III Orthognathic SurgeryNg Chun HownNo ratings yet
- Review of Clinical EEGDocument200 pagesReview of Clinical EEGtuanamg66100% (10)
- Open Workout Plan 2Document2 pagesOpen Workout Plan 2SiddheshPatilNo ratings yet
- Hypothyroidism Case FileDocument2 pagesHypothyroidism Case Filehttps://medical-phd.blogspot.comNo ratings yet
- Case Management Physiotherapy Ischialgia Due to Lumbar Spondylosis L4 – L5Document15 pagesCase Management Physiotherapy Ischialgia Due to Lumbar Spondylosis L4 – L5Pantas SiburianNo ratings yet
- Word Search Muscles Bones and Joints-3Document4 pagesWord Search Muscles Bones and Joints-3api-308609686No ratings yet
- Neurological AssessmentDocument34 pagesNeurological Assessmentdrprasant100% (9)
- Qééçxé Kééiéñ: DR - Ganesh NaikDocument9 pagesQééçxé Kééiéñ: DR - Ganesh NaikkgnaikNo ratings yet
- CRANIAL BASE DEVELOPMENT STUDYDocument28 pagesCRANIAL BASE DEVELOPMENT STUDYPauly JinezNo ratings yet
- Major Human Body Organs for KidsDocument8 pagesMajor Human Body Organs for KidsRica Jean IbcasNo ratings yet
- Pituitary Adenoma FinalDocument44 pagesPituitary Adenoma FinalTuhinaRaj100% (1)
- Trauma Conclave 2021 - Agenda Without LinkDocument2 pagesTrauma Conclave 2021 - Agenda Without LinkDebangshu KumarNo ratings yet
- An - Sci 1 Intro To Animals Science 2Document98 pagesAn - Sci 1 Intro To Animals Science 2Ramil Jr. EntanaNo ratings yet
- Rectum Anus Anatomy 2009 11-3Document38 pagesRectum Anus Anatomy 2009 11-3Ditas ChuNo ratings yet
- Anatomical Terminology GuideDocument57 pagesAnatomical Terminology GuideAlicina DaleNo ratings yet
- The Stages of Puberty: Development in Girls and Boys: Tanner Stage 3Document3 pagesThe Stages of Puberty: Development in Girls and Boys: Tanner Stage 3Yuan LatNo ratings yet
- B.SC Radiology Imaging Technology 1 2 Sem. SyllabusDocument33 pagesB.SC Radiology Imaging Technology 1 2 Sem. Syllabusالمدرب عمر عادلNo ratings yet
- Enhancing Your Diagnostic Potential: Refurbished SolutionsDocument16 pagesEnhancing Your Diagnostic Potential: Refurbished SolutionsAhmed IsawiNo ratings yet
- Air Alert 2Document3 pagesAir Alert 2varunNo ratings yet