Professional Documents
Culture Documents
Access TSH (3rd IS) Instructions For Use Thyrotropin
Uploaded by
carineOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Access TSH (3rd IS) Instructions For Use Thyrotropin
Uploaded by
carineCopyright:
Available Formats
ACCESS
Immunoassay Systems
Access TSH (3rd IS)
Instructions For Use Thyrotropin
© 2022 Beckman Coulter, Inc. All rights reserved.
B63284
FOR PROFESSIONAL USE ONLY
PRINCIPLE
INTENDED USE
The Access TSH (3rd IS) assay is a paramagnetic particle, chemiluminescent immunoassay for the quantitative
determination of human thyroid-stimulating hormone (thyrotropin, TSH, hTSH) levels in human serum and plasma
using the Access Immunoassay Systems. This assay is capable of providing 3rd generation TSH results.
SUMMARY AND EXPLANATION
Human thyroid-stimulating hormone is a glycoprotein hormone consisting of two noncovalently-bound subunits: an
α subunit, which is nearly identical to the α subunits of human luteinizing hormone (hLH), human follicle-stimulating
hormone (hFSH), and human chorionic gonadotropin (hCG), and a β subunit, which is responsible for immunological
and biological specificity.1
TSH, released from the anterior pituitary, is the principal regulator of thyroid function, stimulating the synthesis and
release of thyroid hormones thyroxine (T4) and triiodothyronine (T3). T3 and T4 regulate biochemical processes that
are essential for normal metabolism. The synthesis and secretion of TSH is stimulated by thyrotropin-releasing hormone
(TRH), which is produced by the hypothalamus in response to low levels of circulating T3 and T4. In contrast, elevated
levels of T3 and T4 suppress the production of TSH. Collectively, this negative feedback system is referred to as the
hypothalamic-pituitary-thyroid axis. Any alteration in the function of this axis can influence the levels of TSH, T4, and T3
in circulation.1
The principal clinical use for TSH measurement is for the assessment of thyroid status. TSH is measured in conjunction
with thyroid hormones or antibodies to: 1) detect or exclude hypothyroidism or hyperthyroidism; 2) monitor T4
replacement treatment in hypothyroidism or antithyroid treatment in hyperthyroidism; 3) monitor TSH suppression in
thyroid cancer patients on thyroxine therapy; and 4) assess the response to TRH stimulation testing.2,3
Reference ranges for TSH may vary, depending on the method of analysis, and do not necessarily equate to cut-offs for
diagnosing thyroid dysfunction.
As methods achieving third-generation sensitivity have become available, TSH measurements are also used to identify
subclinical or latent hypothyroidism or hyperthyroidism. Third generation methods for TSH measurement are defined
as achieving a functional sensitivity of 0.01-0.02 µIU/mL (mIU/L) with an interassay %CV ≤ 20%.4,5 Clinical laboratories
may use these more sensitive and precise methods to distinguish different levels of TSH suppression associated with
Graves’ disease and subclinical hyperthyroidism and to assist in the diagnosis of gestational and postpartum thyroid
diseases.3,6,7
METHODOLOGY
The Access TSH (3rd IS) assay is a two-site immunoenzymatic (“sandwich”) assay. A sample is added to a reaction
vessel with mouse anti-hTSH-alkaline phosphatase conjugate, buffered protein solution and paramagnetic particles
coated with immobilized mouse monoclonal anti-hTSH antibody. The hTSH binds to the immobilized monoclonal
anti-hTSH antibody on the solid phase while the mouse anti-hTSH-alkaline phosphatase conjugate reacts with a
different antigenic site on the hTSH.
Instructions For Use B77706 P English Access TSH (3rd IS)
JUNE 2022 Page 1 of 13
After incubation in a reaction vessel, materials bound to the solid phase are held in a magnetic field while unbound
materials are washed away. Then, the chemiluminescent substrate is added to the vessel and light generated by the
reaction is measured with a luminometer. The light production is directly proportional to the concentration of TSH in the
sample. The amount of analyte in the sample is determined from a stored, multi-point calibration curve.
SPECIMEN
SPECIMEN COLLECTION AND PREPARATION
1. Serum (gel and no gel) and plasma (lithium heparin) are the recommended samples.
2. The role of preanalytical factors in laboratory testing has been described in a variety of published literature.8,9 To
minimize the effect of preanalytical factors observe the following recommendations for handling, processing, and
storing blood samples:8
• Collect all blood samples observing routine precautions for venipuncture.
• Allow serum samples to clot completely before centrifugation in a vertical, closure-up position.
- Nonanticoagulated tubes containing gel separator should be stored in an upright position as soon as the
mixing is complete.
- Precentrifugation serum/cells contact time is according to tube manufacturer’s recommendations. Clotting
may be slowed at cooler temperatures or if patient is on anticoagulant therapy.
• Keep tubes stoppered at all times.
• Physically separate serum or plasma from contact with cells as soon as possible. Tightly stopper the tube
immediately.
• Store samples tightly stoppered at room temperature (15 to 30°C) for up to 18 hours.
• If the assay will not be completed within 18 hours, refrigerate the samples at 2 to 8°C.
• If the assay will not be completed within seven days, freeze at -20°C or colder.
• Frozen specimens can be stored up to 90 days before testing.
• Do not thaw samples more than two times.
3. Use the following guidelines when preparing specimens:
• Ensure residual fibrin and cellular matter have been removed prior to analysis.
• Follow blood collection tube manufacturer's recommendations for centrifugation.
4. Each laboratory should determine the acceptability of its own blood collection tubes and serum separation products.
Variations in these products may exist between manufacturers and, at times, from lot-to-lot.
5. Avoid assaying lipemic or hemolyzed samples.
REAGENTS
PRODUCT INFORMATION
Access TSH (3rd IS) Reagent Pack
Ref. No. B63284: 200 determinations, 2 packs, 100 tests/pack
• Provided ready to use.
• Store upright and refrigerate at 2 to 10°C.
• Refrigerate at 2 to 10°C for a minimum of two hours before use on the instrument.
• Stable until the expiration date stated on the label when stored at 2 to 10°C.
Access TSH (3rd IS) English Instructions For Use B77706 P
Page 2 of 13 JUNE 2022
• Stable at 2 to 10°C for 63 days after initial use.
• Signs of possible deterioration are a broken elastomeric layer on the pack or quality control values out of range.
• If the reagent pack is damaged (e.g., broken elastomer), discard the pack.
R1a: Paramagnetic particles coated with mouse monoclonal anti-human TSH antibody suspended in
TRIS buffered saline, with surfactant, bovine serum albumin (BSA), < 0.1% sodium azide, and
0.1% ProClin* 300.
R1b: TRIS buffered saline with surfactant, BSA, protein (murine), < 0.1% sodium azide, and 0.1%
ProClin 300.
R1c: Mouse monoclonal anti-human TSH alkaline phosphatase conjugate in ACES buffered saline,
with surfactant, BSA matrix, protein (murine), < 0.1% sodium azide, and 0.25% ProClin 300.
R1d: Mouse monoclonal anti-human TSH alkaline phosphatase conjugate in ACES buffered saline,
with surfactant, BSA matrix, protein (murine), < 0.1% sodium azide, and 0.25% ProClin 300.
*ProClin™ is a trademark of The Dow Chemical Company (“Dow”) or an affiliated company of Dow.
WARNING AND PRECAUTIONS
• For in vitro diagnostic use.
• Patient samples and blood-derived products may be routinely processed with minimum risk using the procedure
described. However, handle these products as potentially infectious according to universal precautions and good
clinical laboratory practices, regardless of their origin, treatment, or prior certification. Use an appropriate disinfectant
for decontamination. Store and dispose of these materials and their containers in accordance with local regulations
and guidelines.
• For hazards presented by the product refer to the following sections: REACTIVE INGREDIENTS and GHS HAZARD
CLASSIFICATION.
REACTIVE INGREDIENTS
CAUTION
Sodium azide preservative may form explosive compounds in metal drain lines.
See NIOSH Bulletin: Explosive Azide Hazard (8/16/76).
To avoid the possible build-up of azide compounds, flush wastepipes with
water after the disposal of undiluted reagent. Sodium azide disposal must be in
accordance with appropriate local regulations.
GHS HAZARD CLASSIFICATION
TSH Particles (Compartment WARNING
R1a)
H316 Causes mild skin irritation.
H317 May cause an allergic skin reaction.
H412 Harmful to aquatic life with long lasting effects.
P273 Avoid release to the environment.
Instructions For Use B77706 P English Access TSH (3rd IS)
JUNE 2022 Page 3 of 13
P280 Wear protective gloves, protective clothing and eye/face
protection.
P332+P313 If skin irritation occurs: Get medical advice/attention.
P333+P313 If skin irritation or rash occurs: Get medical
advice/attention.
P362+P364 Take off contaminated clothing and wash it before use.
Tris(hydroxymethyl)– aminomethane 1 - 5%
reaction mass of: 5-chloro-2-methyl-4-isothiazolin -3-one
[EC# 247-500-7] and 2-methyl-4-isothiazolin-3-one [EC#
220-239-6](3:1) < 0.05%
TSH Ancillary (Compartment WARNING
R1b)
H316 Causes mild skin irritation.
H317 May cause an allergic skin reaction.
H412 Harmful to aquatic life with long lasting effects.
P273 Avoid release to the environment.
P280 Wear protective gloves, protective clothing and eye/face
protection.
P332+P313 If skin irritation occurs: Get medical advice/attention.
P333+P313 If skin irritation or rash occurs: Get medical
advice/attention.
P362+P364 Take off contaminated clothing and wash it before use.
Tris(hydroxymethyl)– aminomethane 1 - 5%
reaction mass of: 5-chloro-2-methyl-4-isothiazolin -3-one
[EC# 247-500-7] and 2-methyl-4-isothiazolin-3-one [EC#
220-239-6](3:1) < 0.05%
TSH Conjugate (Compartment WARNING
R1c)
H317 May cause an allergic skin reaction.
H412 Harmful to aquatic life with long lasting effects.
P273 Avoid release to the environment.
P280 Wear protective gloves, protective clothing and eye/face
protection.
P333+P313 If skin irritation or rash occurs: Get medical
advice/attention.
P362+P364 Take off contaminated clothing and wash it before use.
Access TSH (3rd IS) English Instructions For Use B77706 P
Page 4 of 13 JUNE 2022
reaction mass of: 5-chloro-2-methyl-4-isothiazolin -3-one
[EC# 247-500-7] and 2-methyl-4-isothiazolin-3-one [EC#
220-239-6](3:1) < 0.05%
TSH Conjugate (Compartment WARNING
R1d)
H317 May cause an allergic skin reaction.
H412 Harmful to aquatic life with long lasting effects.
P273 Avoid release to the environment.
P280 Wear protective gloves, protective clothing and eye/face
protection.
P333+P313 If skin irritation or rash occurs: Get medical
advice/attention.
P362+P364 Take off contaminated clothing and wash it before use.
reaction mass of: 5-chloro-2-methyl-4-isothiazolin -3-one
[EC# 247-500-7] and 2-methyl-4-isothiazolin-3-one [EC#
220-239-6](3:1) < 0.05%
Safety Data Sheet is available at beckmancoulter.com/techdocs
MATERIALS NEEDED BUT NOT SUPPLIED WITH REAGENT KIT
1. Access TSH (3rd IS) Calibrators
Provided at zero and approximately 0.050, 0.30, 3.0, 15.0 and 50.0 µIU/mL (mIU/L).
Ref. No. B63285
2. Quality Control (QC) materials: commercial control material.
3. Access Substrate
Ref. No. 81906
4. Access Wash Buffer II, Ref. No. A16792
UniCel DxI Wash Buffer II, Ref. No. A16793
EQUIPMENT AND MATERIALS
R1 Access TSH (3rd IS) Reagent Packs
CALIBRATION
CALIBRATION INFORMATION
An active calibration curve is required for all tests. For the Access TSH (3rd IS) assay, calibration is required every 63
days. Refer to the appropriate system manuals and/or Help system for information on calibration theory, configuring
calibrators, calibrator test request entry, and reviewing calibration data.
Instructions For Use B77706 P English Access TSH (3rd IS)
JUNE 2022 Page 5 of 13
QUALITY CONTROL
Quality control materials simulate the characteristics of patient samples and are essential for monitoring the system
performance of immunochemical assays. Because samples can be processed at any time in a "random access"
format rather than a "batch" format, quality control materials should be included in each 24-hour time period.10 Include
commercially available quality control materials that cover at least two levels of analyte. More frequent use of controls
or the use of additional controls is left to the discretion of the user based on good laboratory practices or laboratory
accreditation requirements and applicable laws. Follow manufacturer's instructions for reconstitution and storage. Each
laboratory should establish mean values and acceptable ranges to assure proper performance. Quality control results
that do not fall within acceptable ranges may indicate invalid test results. Examine all test results generated since
obtaining the last acceptable quality control test point for this analyte. Refer to the appropriate system manuals and/or
Help system for information about reviewing quality control results.
TESTING PROCEDURE(S)
PROCEDURAL COMMENTS
1. Refer to the appropriate system manuals and/or Help system for a specific description of installation, start-up,
principles of operation, system performance characteristics, operating instructions, calibration procedures,
operational limitations and precautions, hazards, maintenance, and troubleshooting.
2. Mix contents of new (unpunctured) reagent packs by gently inverting pack several times before loading on the
instrument. Do not invert open (punctured) packs.
3. Use fifty-five (55) µL of sample for each determination in addition to the sample container and system dead volumes
when requesting the assay (test name: TSH3). Use fifty (50) µL of sample in addition to the sample container and
system dead volumes for each determination run with the special dilution feature (test name: TSH3d). Refer to the
appropriate system manuals and/or Help system for the minimum sample volume required.
4. The system default unit of measure for sample results is µIU/mL. To change sample reporting units to the
International System of Units (SI units), mIU/L, refer to the appropriate system manuals and/or Help system. To
manually convert concentrations to the International System, multiply µIU/mL by multiplication factor 1.
PROCEDURE
Refer to the appropriate system manuals and/or Help system for information on managing samples, configuring tests,
requesting tests, and reviewing test results.
• Select TSH3 as the test name for assaying samples containing hTSH concentrations up to the concentration of the
Access TSH (3rd IS) S5 calibrator.
• Use the special dilution feature (test name: TSH3d) for assaying samples containing hTSH concentrations greater
than the Access TSH (3rd IS) S5 calibrator.
RESULTS INTERPRETATION
Test results are determined automatically by the system software. The amount of analyte in the sample is determined
from the measured light production by means of the stored calibration data. Test results can be reviewed using the
appropriate screen. Refer to the appropriate system manuals and/or Help system for complete instructions on reviewing
sample results.
REPORTING RESULTS
EXPECTED RESULTS
1. Each laboratory should establish its own reference intervals to assure proper representation of specific populations.
Access TSH (3rd IS) English Instructions For Use B77706 P
Page 6 of 13 JUNE 2022
2. Beckman Coulter conducted a multicenter prospective study across geographically diverse locations to establish
the central 97.5% reference interval in apparently healthy, euthyroid adults. Subjects with no known personal or
family thyroid disease, goiter, chronic disease (including cancer, diabetes, autoimmune disease, or cardiovascular
disease), acute bacterial or viral infection, or current use of prescription medication (excluding prenatal vitamins) or
aspirin were enrolled in the study, following the guidance of both the National Academy of Clinical Biochemistry’s
(NACB) Laboratory Medicine Practice Guideline, Laboratory Support for the Diagnosis and Monitoring of Thyroid
Disease, and the Third National Health and Nutrition Examination Survey (NHANES III). 3,11
The study included four populations: a general population of approximately equal numbers of males and
non-pregnant females between the ages of 18-88; and pregnant females with approximately equal distribution
across all three trimesters. Trimesters were defined according to American Congress of Obstetricians and
Gynecologists guidelines.12 Approximately four hundred (400) subjects were enrolled in each population.
After enrollment, subjects’ samples were screened for positive thyroid peroxidase antibody (TPOAb) and
thyroglobulin antibody (TgAb) using the Beckman Coulter Access TPO Antibody and Access Thyroglobulin
Antibody II assays prior to analyses. Samples with positive TPOAb or TgAb results (approximately 10%) were
excluded from analysis of the TSH reference intervals.
Serum samples were analyzed using multiple UniCel DxI 800 Access Immunoassay Systems with the Access
TSH (3rd IS) assay, following the CLSI EP28-A3c guideline.13 The observed non-parametric ranges of TSH
concentrations are shown below for each population tested.
Median 97.5% Reference Interval
Population Sample Size (µIU/mL) (µIU/mL)
General Population (males 393 1.45 0.38 - 5.33
and non-pregnant females,
aged 18-88)
Pregnant Females, 318 1.13 0.05 - 3.70
1st Trimester
Pregnant Females, 362 1.47 0.31 - 4.35
2nd Trimester
Pregnant Females, 335 1.61 0.41 - 5.18
3rd Trimester
3. For additional reference interval guidance, refer to the National Academy of Clinical Biochemistry (NACB)
publication, Laboratory Support for the Diagnosis and Monitoring of Thyroid Disease, and the Third National
Health and Nutrition Examination Survey (NHANES III).3,11
4. The evaluation of thyroid status should not depend on results from a single test. Complete thyroid status evaluation
should include other thyroid function tests, including evaluation of thyroid autoantibodies (useful in the diagnosis
of autoimmune thyroiditis), and the physician’s clinical evaluation.
PROCEDURAL NOTES
LIMITATIONS
1. Samples can be accurately measured within the analytical range of the Limit of Detection (LoD) and the highest
calibrator value (approximately 0.005 - 50.0 µIU/mL [mIU/L]).
• If a sample contains less than the lower Limit of Detection (LoD) for the assay, report the result as less than that
value (i.e., < 0.005 µIU/mL [mIU/L]).
Instructions For Use B77706 P English Access TSH (3rd IS)
JUNE 2022 Page 7 of 13
• If a sample contains more than the stated value of the highest Access TSH (3rd IS) Calibrator (S5), report the
result as greater than that value (i.e., > 50.0 µIU/mL [mIU/L]). Alternatively, dilute one volume of sample with 9
volumes of Access Wash Buffer II or UniCel DxI Wash Buffer II.
Refer to the appropriate system manuals and/or Help system for instructions on entering a sample dilution in a
test request. The system reports the results adjusted for the dilution.
Dil-TSH (3rd IS) Special Dilution Feature for use on Access 2 and UniCel DxI systems:
Samples containing hTSH concentrations greater than the concentration of the Access TSH (3rd IS) S5 calibrator
can be processed using the Special Dilution Feature. When TSH3d is requested, the system automatically
dilutes the sample using Wash Buffer II and reads the resulting dose off the TSH3 calibration curve.
Test Name Reportable Range (µIU/mL) Sample Volume Required
TSH3d 37.5 - 500 50 µL
2. For assays employing antibodies, the possibility exists for interference by heterophile antibodies in the patient
sample. Patients who have been regularly exposed to animals or have received immunotherapy or diagnostic
procedures utilizing immunoglobulins or immunoglobulin fragments may produce human anti-animal antibodies,
e.g. HAMA, that interfere with immunoassays.14,15 Such interfering antibodies may cause erroneous results.
Carefully evaluate the results of patients suspected of having these antibodies.
3. Other potential interferences in the patient sample could be present and may cause erroneous results in
immunoassays. Some examples that have been documented in literature include rheumatoid factor, endogenous
alkaline phosphatase, fibrin, and proteins capable of binding to alkaline phosphatase.16 Carefully evaluate results
if the sample is suspected of having these types of interferences.
4. The Access TSH (3rd IS) results should be interpreted in light of the total clinical presentation of the patient,
including: symptoms, clinical history, data from additional tests, and other appropriate information.
5. The Access TSH (3rd IS) assay does not demonstrate any “hook” effect up to 1,000 µIU/mL (mIU/L).
6. This assay is not validated for testing neonatal serum hTSH levels.
PERFORMANCE CHARACTERISTICS
PERFORMANCE CHARACTERISTICS
METHODS COMPARISON
Representative data for methods comparison are provided for illustration only. Performance obtained in individual
laboratories may vary.
A comparison of 207 samples using the Access TSH (3rd IS) assay on the UniCel DxI 800 Immunoassay System
and a commercially available immunoassay kit gave the following statistical data using Passing-Bablok regression and
Pearson’s correlation, following the CLSI EP9-A3 guideline:17
Range of Intercept Correlation
Observations† (µIU/mL) Slope Coefficient
n (µIU/mL) [95% CI] (95% CI) (r)
207 0.010 - 44.90 -0.04 [-0.05 - (-0.02)] 0.91 (0.88 - 0.92) 0.99
†Observed concentration range of the Access TSH (3rd IS) assay.
Access TSH (3rd IS) English Instructions For Use B77706 P
Page 8 of 13 JUNE 2022
LINEARITY
Representative data for linearity are provided for illustration only. Performance obtained in individual laboratories may
vary.
Based on CLSI EP6-A18, one high sample [approximately 50.0 µIU/mL (mIU/L)] and one low sample [< 0.005 µIU/mL
(mIU/L)] were mixed to make nine sample concentrations evenly distributed across the analytical measuring range. Four
replicates of the seven mixed samples, eight replicates of the low sample, and four replicates of the high sample were
tested on one UniCel DxI 800 Immunoassay System. The Access TSH (3rd IS) assay demonstrated acceptable linearity
throughout the analytical measuring range of 0.005 to approximately 50.0 µIU/mL (mIU/L).
DILUTION RECOVERY
Representative data for dilution recovery are provided for illustration only. Performance obtained in individual laboratories
may vary.
Four serum samples at concentrations above the Access TSH (3rd IS) S5 calibrator [approximately 50.0 µIU/mL (mIU/L)]
were diluted 1/10 with Wash Buffer II. Twenty-four replicates for each sample were measured on one UniCel DxI 800
Immunoassay System, providing the following data:
Target Concentration Dil-TSH (3rd IS) Sample Manual Dilution Sample
Sample (µIU/mL) Mean Recovery (%) Mean Recovery (%)
Sample 1 100 97 96
Sample 2 200 98 95
Sample 3 300 93 95
Sample 4 400 93 93
IMPRECISION
Representative data for imprecision are provided for illustration only. Performance obtained in individual laboratories
may vary.
The Access TSH (3rd IS) assay exhibits total imprecision ≤ 10% CV at concentrations > 0.02 µIU/mL (mIU/L) and total
standard deviation (SD) ≤ 0.0029 µIU/mL (mIU/L) at concentrations ≤ 0.02 µIU/mL (mIU/L).
One study, using four serum-based samples on one UniCel DxI 800 Immunoassay System, generating a total of 40
assays, two replicates per assay, over 20 days with two runs per day, provided the following data, calculated based on
the CLSI EP5-A319 guideline.
Total Imprecision
Within-Run (Within-Laboratory
(Repeatability) Between-Day Between-Run Precision)
Grand
Mean
(µIU/mL) SD SD SD SD
Sample (n=80) (µIU/mL) (%CV) (µIU/mL) (%CV) (µIU/mL) (%CV) (µIU/mL) (%CV)
Sample 1 0.02 0.0004 N/A 0.0008 N/A 0.0004 N/A 0.0010 N/A
Sample 2 0.37 0.006 2 0.010 3 0.006 2 0.013 3
Sample 3 4.71 0.13 3 0.11 2 0.008 0.2 0.17 4
Sample 4 38.76 1.36 4 1.80 5 0.49 1 2.31 6
Instructions For Use B77706 P English Access TSH (3rd IS)
JUNE 2022 Page 9 of 13
ANALYTICAL SPECIFICITY / INTERFERENCES
Representative data for analytical specificity/interferences are provided for illustration only. Performance obtained in
individual laboratories may vary.
Serum samples containing hTSH concentrations of approximately 0.30 µIU/mL and 5.0 µIU/mL were spiked with multiple
concentrations of the substances below and run on one UniCel DxI 800 Immunoassay System. Values were calculated
as described in CLSI EP7-A2.20 Interference was determined by testing controls (no interfering substance added) and
matched test samples (with interfering substance added). Of the compounds tested, none were found to cause significant
interference (as defined by a shift in dose greater than 10%) using the highest test concentrations indicated in the table
below.
Substance Highest Concentration Added
Acetaminophen 200 µg/mL
Acetylsalicylic acid 650 µg/mL
Bilirubin (conjugated) 450 µg/mL
Bilirubin (unconjugated) 400 µg/mL
Hemoglobin 10 mg/mL
Heparin (Sodium) 3 U/mL
hGH (Human Growth Hormone) 134 ng/mL
Human Serum Albumin (HSA) 60 mg/mL
Ibuprofen 500 µg/mL
Multivitamin 0.9% (v/v)
Triglycerides (Intra Lipid) 33 mg/mL
A study was performed to evaluate the potential cross-reactivity of the assay with other substances that are similar in
structure to hTSH. Serum samples containing hTSH concentrations of approximately 0.30 µIU/mL and 5.0 µIU/mL were
spiked with multiple concentrations of the substances below and run on one UniCel DxI 800 Immunoassay System.
Values were calculated as described in CLSI EP7-A2.20
Samples containing substances at the concentrations listed below do not affect the concentration of hTSH reported.
Highest Concentration Added Cross-reactivity
Substance (mIU/mL) (%)
hCG 1,000,000 < 0.010%
hFSH 1,000 < 0.10%
hLH 3,000 < 0.10%
Representative data for Limit of Blank, Limit of Detection and Limit of Quantitation are provided for illustration only.
Performance obtained in individual laboratories may vary.
LIMIT OF BLANK
The Access TSH (3rd IS) assay is designed to have a Limit of Blank (LoB) of < 0.005 µIU/mL (mIU/L). In one study,
LoB was tested using a protocol based on CLSI EP17-A2.21 A total of 360 replicates of four zero analyte samples were
measured in three runs using multiple reagent pack lots and one calibrator lot on multiple UniCel DxI 800 Immunoassay
Systems. This study determined the LoB for the Access TSH (3rd IS) assay to be 0.001 µIU/mL (mIU/L), which supports
the claim of < 0.005 µIU/mL (mIU/L).
Access TSH (3rd IS) English Instructions For Use B77706 P
Page 10 of 13 JUNE 2022
LIMIT OF DETECTION
The Access TSH (3rd IS) assay is designed to have a Limit of Detection (LoD) of ≤ 0.005 µIU/mL (mIU/L). In one study,
LoD was tested using a protocol based on CLSI EP17-A2.21 A total of 675 replicates from five low-level samples were
measured using multiple reagent pack lots and one calibrator lot in five runs on multiple UniCel DxI 800 Immunoassay
Systems. This study determined the LoD for the Access TSH (3rd IS) assay to be 0.001 µIU/mL (mIU/L), which supports
the claim of ≤ 0.005 µIU/mL (mIU/L).
LIMIT OF QUANTITATION
The Access TSH (3rd IS) assay is designed to have a Limit of Quantitation (LoQ) of ≤ 0.01 µIU/mL (mIU/L) at ≤ 10%
between-run CV. In one study, LoQ was tested using a protocol based on CLSI EP17-A2.21 A total of 945 replicates of
seven samples were measured using multiple reagent pack lots and one calibrator lot in five runs on one UniCel DxI
800 Immunoassay System. LoQ was determined as the lowest concentration with a between-run imprecision of 10%
CV. This study determined the LoQ for the Access TSH (3rd IS) assay to be 0.001 µIU/mL (mIU/L), which supports the
claim of ≤ 0.01 µIU/mL (mIU/L) at ≤ 10% between-run CV.
ADDITIONAL INFORMATION
Beckman Coulter, the stylized logo, and the Beckman Coulter product and service marks mentioned herein are
trademarks or registered trademarks of Beckman Coulter, Inc. in the United States and other countries.
May be covered by one or more pat. -see www.beckmancoulter.com/patents.
REVISION HISTORY
Revision K
IFU updated to add Dutch, Finnish, Macedonian, and Estonian
Revision L
Remove CE Mark, Update GHS Hazard Information and Website Address
Revision M
Updated French translation in the Expected Results section. Add CE Mark, Update GHS Hazard Information
Revision N
Updated Product Information and Calibration sections
Revision P
Remove CE Mark, Update GHS Hazard Information
SYMBOLS KEY
Glossary of Symbols is available at beckmancoulter.com/techdocs (document number C02724).
Instructions For Use B77706 P English Access TSH (3rd IS)
JUNE 2022 Page 11 of 13
REFERENCES
1. Larsen PR, Davies TF, and Hay, ID. The Thyroid Gland. In: Wilson JD, Foster, DW, Kronenberg HM, Larsen
PR, editors. Williams Textbook of Endocrinology. 9th ed. Philadelphia, PA: W.B. Saunders Company; c1998. p.
389-515.
2. Howanitz JH, Henry JB. Evaluation of Endocrine Function. In: Henry, JB, editor. Clinical Diagnosis and
Management by Laboratory Methods. 20th ed. Philadelphia, PA: W.B. Saunders Company; c2001. p. 304-334.
3. Demers, LM, Spencer, CA. Laboratory medicine practice guidelines: laboratory support for the diagnosis and
monitoring of thyroid disease. Washington, DC: National Academy of Clinical Biochemistry; 2002; 1-125.
4. Spencer CA, et al. Interlaboratory/intermethod differences in functional sensitivity of immunometric assays of
Thyrotropin (TSH) and impact on reliability of measurement of subnormal concentrations of TSH. Clin Chem 1995;
41/3, 367-374.
5. Spencer CA., Takeuchi M, and Kazarosyan M. Current status and performance goals for serum thyrotropin (TSH)
assays. Clinical Chemistry 42.1 (1996): 140-145.
6. National Comprehensive Cancer Network. NCCN Clinical practice guidelines in oncology: thyroid carcinoma.
Version 2.2014 (2014).
7. Stagnaro-Green A, et al. Guidelines of the American Thyroid Association for the diagnosis and management of
thyroid disease during pregnancy and postpartum. Thyroid 21.10 (2011): 1081-1125.
8. Approved Guideline - Procedures for the Handling and Processing of Blood Specimens for Common Laboratory
Tests, GP44-A4. 2010. Clinical and Laboratory Standards Institute.
9. Approved Standard - Sixth Edition, Procedures for the Collection of Diagnostic Blood Specimens by Venipuncture,
H3-A6. 2007. Clinical and Laboratory Standards Institute.
10. Cembrowski GS, Carey RN. Laboratory quality management: QC ⇌ QA. ASCP Press, Chicago, IL, 1989.
11. Hollowell JG, et al. Serum TSH, T4, and thyroid antibodies in the United States population (1988 to 1994): National
Health and Nutrition Examination Survey (NHANES III). The Journal of Clinical Endocrinology & Metabolism 87.2
(2002): 489-499.
12. Method for estimating due date. Committee Opinion No. 611. American College of Obstetricians and
Gynecologists. Obstet Gynecol 124.4 (2014): 863-6.
13. Approved Guideline - Defining, Establishing, and Verifying Reference Intervals in the Clinical Laboratory,
EP28-A3c. October 2010. Clinical and Laboratory Standards Institute.
14. Kricka L. Interferences in immunoassays - still a threat. Clin Chem 2000; 46: 1037-1038.
15. Bjerner J, et al. Immunometric assay interference: incidence and prevention. Clin Chem 2002; 48: 613-621.
16. Lingwood D, Ballantyne JS. Alkaline phosphatase-immunoglobulin conjugate binds to lipids in vitro, independent
of antibody selectivity. Journal of Immunological Methods 2006; 311: 174-177.
17. Approved Guideline – Measurement Procedure Comparison and Bias Estimation Using Patient Samples, EP9-A3.
2013. Clinical and Laboratory Standards Institute.
18. Approved Guideline - Evaluation of the Linearity of Quantitative Measurement Procedures: A Statistical Approach,
EP06-A. April 2003. Clinical and Laboratory Standards Institute.
Access TSH (3rd IS) English Instructions For Use B77706 P
Page 12 of 13 JUNE 2022
19. Approved Guideline – Evaluation of Precision of Quantitative Measurement Procedures, EP5-A3. 2014. Clinical
and Laboratory Standards Institute.
20. Approved Guideline - Interference Testing in Clinical Chemistry, EP7- A2. November 2005. Clinical and Laboratory
Standards Institute.
21. Approved Guideline - Evaluation of Detection Capability for Clinical Laboratory Measurement Procedures,
EP17-A2. June 2012. Clinical and Laboratory Standards Institute.
IMMUNOTECH SAS A Beckman Coulter Company, 130, Avenue de Lattre de Tassigny,
BP 177, 13276 Marseille Cedex 9, France, +(33) 4 91 17 27 27
www.beckmancoulter.com
Instructions For Use B77706 P English Access TSH (3rd IS)
JUNE 2022 Page 13 of 13
You might also like
- B77706K AccessTSH 3rdDocument13 pagesB77706K AccessTSH 3rdТатьяна ИсаеваNo ratings yet
- Access 3rd IS TSH - DXL9000Document13 pagesAccess 3rd IS TSH - DXL9000Chris ThomasNo ratings yet
- Package Insert - TSH3Document6 pagesPackage Insert - TSH3Kadek Ayang Cendana Prahayu100% (1)
- Thyroid Stimulating Hormone (TSH) CLIADocument2 pagesThyroid Stimulating Hormone (TSH) CLIAp11.sethiaNo ratings yet
- Enzyme Immunoassay For The Quantitative Determination of Triiodothyronine (T3) in Human SerumDocument10 pagesEnzyme Immunoassay For The Quantitative Determination of Triiodothyronine (T3) in Human SerumcitrahdynNo ratings yet
- SHBGDocument18 pagesSHBGcarineNo ratings yet
- Sensitive Thyroid Stimulating Hormone (S-TSH) Enzyme Immunoassay Test Kit Catalog Number: BC-1003Document4 pagesSensitive Thyroid Stimulating Hormone (S-TSH) Enzyme Immunoassay Test Kit Catalog Number: BC-1003Juan SánchezNo ratings yet
- Intended Use: Ichroma™ TSH Is A Fluorescence Immunoassay (FIA) ForDocument4 pagesIntended Use: Ichroma™ TSH Is A Fluorescence Immunoassay (FIA) ForFathi MesoNo ratings yet
- Rapid TSH Immulite - 230524111657469Document31 pagesRapid TSH Immulite - 230524111657469laboratorio almarNo ratings yet
- B29061KDocument13 pagesB29061KMeethuanNo ratings yet
- Lab Policies TSH - Cobas E411 Lab 1598Document5 pagesLab Policies TSH - Cobas E411 Lab 1598Bassam Alharazi100% (1)
- Can-Fte-260 - Free TestosteroneDocument2 pagesCan-Fte-260 - Free TestosteronevijayaNo ratings yet
- Free T3 - IMMULITE 2000 Systems - Rev 24 DXDCM 09017fe9802975f7-1538193198932Document36 pagesFree T3 - IMMULITE 2000 Systems - Rev 24 DXDCM 09017fe9802975f7-1538193198932Jorge Stban PerezNo ratings yet
- Instructions For Use TSHDocument12 pagesInstructions For Use TSHBenjamin MannNo ratings yet
- Testosterone ELISADocument16 pagesTestosterone ELISARichard Ortiz100% (1)
- KAQ0621 Rev1Document16 pagesKAQ0621 Rev124redred4578No ratings yet
- Package Insert - 07204 - I - en - 30403 T3 PDFDocument5 pagesPackage Insert - 07204 - I - en - 30403 T3 PDFadybaila4680No ratings yet
- TSI - IMMULITE 2000 Systems - Rev 12 2018Document35 pagesTSI - IMMULITE 2000 Systems - Rev 12 2018Mario Echeverria GonzalezNo ratings yet
- Anti-Thyroid Peroxidase Antibody (Anti-TPO) CLIA: 2 X 50 Test 52025070Document2 pagesAnti-Thyroid Peroxidase Antibody (Anti-TPO) CLIA: 2 X 50 Test 52025070p11.sethiaNo ratings yet
- Lab Policies Complete Blood Count of Whole Blood On The Sysmex KX 21N - RB Lab 1535Document20 pagesLab Policies Complete Blood Count of Whole Blood On The Sysmex KX 21N - RB Lab 1535tomNo ratings yet
- Total T3: For Use On The IMMULITE and Immulite 1000 SystemsDocument31 pagesTotal T3: For Use On The IMMULITE and Immulite 1000 SystemsEdgar Galván0% (1)
- 30 400 Vidas TSH: Summary and Explanation PrincipleDocument7 pages30 400 Vidas TSH: Summary and Explanation PrincipleWarda Niah100% (1)
- Ft3 IiiDocument4 pagesFt3 IiihairiNo ratings yet
- Salivary Cortisol: Expanded Range High SensitivityDocument21 pagesSalivary Cortisol: Expanded Range High Sensitivityerik gunawanNo ratings yet
- Biomérieux 30 400 Vidas TSH: Summary and Explanation PrincipleDocument7 pagesBiomérieux 30 400 Vidas TSH: Summary and Explanation Principlecass50% (2)
- TSH ImmuliteDocument35 pagesTSH ImmuliteEdgar Galván50% (2)
- Elecsys FT3Document4 pagesElecsys FT3Arnaz AdisaputraNo ratings yet
- Insert - Elecsys Anti-TSHR.08496633500.V4.enDocument5 pagesInsert - Elecsys Anti-TSHR.08496633500.V4.enVegha NedyaNo ratings yet
- Inserto T3Document2 pagesInserto T3cesiahdez0% (2)
- Neonatal TSH ELISA Screening TestDocument10 pagesNeonatal TSH ELISA Screening Testyandros666No ratings yet
- Package Insert - FT3 PDFDocument6 pagesPackage Insert - FT3 PDFKadek Ayang Cendana Prahayu0% (1)
- TSH 2017-05 v23Document3 pagesTSH 2017-05 v23Yaser MNo ratings yet
- Enzyme Immunoassay Test Kit Catalog Number: 10304: Thyroid Stimulating Hormone (TSH)Document2 pagesEnzyme Immunoassay Test Kit Catalog Number: 10304: Thyroid Stimulating Hormone (TSH)petertrungNo ratings yet
- TSH Accubind Elisa Rev 3Document0 pagesTSH Accubind Elisa Rev 3Rafael ZevallosNo ratings yet
- HBSAG Rapid Test 2Document6 pagesHBSAG Rapid Test 2Charlotte OhNo ratings yet
- Insert - Elecsys T3.ms - 11731360122.v26.enDocument4 pagesInsert - Elecsys T3.ms - 11731360122.v26.enGuneyden Guneyden100% (3)
- TSHDocument25 pagesTSHFlorea RodicaNo ratings yet
- TSH LiaisonDocument6 pagesTSH Liaisonsorayafathi90No ratings yet
- nbl-rna-prep-trizolDocument7 pagesnbl-rna-prep-trizolmannukr565No ratings yet
- Inserto TP Thromborel S SIEMENSDocument6 pagesInserto TP Thromborel S SIEMENSedson flores100% (2)
- E Anti-TSHR Ms en 9Document4 pagesE Anti-TSHR Ms en 9Hassan GillNo ratings yet
- Synchron System(s) Chemistry Information Sheet Gluh: GlucoseDocument16 pagesSynchron System(s) Chemistry Information Sheet Gluh: GlucosehongNo ratings yet
- TSH OrigeneDocument3 pagesTSH OrigeneAlejandro AlvaradoNo ratings yet
- PI e TCU 9Document1 pagePI e TCU 9Khuon BunthaNo ratings yet
- Lsab KitDocument9 pagesLsab KitnutjabberNo ratings yet
- FT3Document26 pagesFT3Florea RodicaNo ratings yet
- Free T4 - IMMUNOLITE 2000Document36 pagesFree T4 - IMMUNOLITE 2000pyx5pjqqx4No ratings yet
- ft4 III 2020-04 v3Document4 pagesft4 III 2020-04 v3Ismael CulquiNo ratings yet
- bc-1001 TSHDocument5 pagesbc-1001 TSHJuan SánchezNo ratings yet
- A46221DDocument15 pagesA46221DQuoctytranNo ratings yet
- 43 Hahhu E01Document8 pages43 Hahhu E01Cao Thi Le ChiNo ratings yet
- Lab Policies Sysmex XS 1000i Procedure Lab 1501 PDFDocument26 pagesLab Policies Sysmex XS 1000i Procedure Lab 1501 PDFakiNo ratings yet
- Ichroma Anti CCP Plus Rev.03Document4 pagesIchroma Anti CCP Plus Rev.03Laboratorio Medic BactLabNo ratings yet
- QualityDocument4 pagesQualityNIGHT tubeNo ratings yet
- Immunology and Serology Lab TestsDocument48 pagesImmunology and Serology Lab TestsKaycee Gretz LorescaNo ratings yet
- Sgot TestDocument2 pagesSgot TestShribagla MukhiNo ratings yet
- PI e TLN 8Document1 pagePI e TLN 8TRITEST TRITESTNo ratings yet
- A TpoDocument4 pagesA TpoJimboreanu György PaulaNo ratings yet
- 30 400-01 Vidas TSH: Summary and Explanation of The Test Principle of The ProcedureDocument9 pages30 400-01 Vidas TSH: Summary and Explanation of The Test Principle of The ProcedureAuxy MassandeNo ratings yet
- Asi RFDocument4 pagesAsi RFcarineNo ratings yet
- ASI Infectious MonoDocument4 pagesASI Infectious MonocarineNo ratings yet
- Aptima BVDocument34 pagesAptima BVcarineNo ratings yet
- En TriglyceridesDocument4 pagesEn TriglyceridesYến Minh NguyễnNo ratings yet
- Access 25 (OH) Vitamin D Assay Total IFUDocument16 pagesAccess 25 (OH) Vitamin D Assay Total IFUcarineNo ratings yet
- SHBGDocument18 pagesSHBGcarineNo ratings yet
- Apolipoprotein BDocument13 pagesApolipoprotein BcarineNo ratings yet
- Arpèges de Trois Notes: Arpeggios in TripletsDocument3 pagesArpèges de Trois Notes: Arpeggios in TripletspanapapakNo ratings yet
- Beef Steaks: MethodDocument2 pagesBeef Steaks: MethodGoshigoshi AkhtarNo ratings yet
- C42135AA Beckman Coulter ClearLLab 10C Casebook PDFDocument586 pagesC42135AA Beckman Coulter ClearLLab 10C Casebook PDFHam Bone100% (1)
- PariharaDocument2 pagesPariharahrvNo ratings yet
- Familiarization With Apparatus and Equipment Used in Testing of MaterialsDocument5 pagesFamiliarization With Apparatus and Equipment Used in Testing of MaterialsEmanoAce33% (6)
- Vaping in Preganacy A Systematic ReviewDocument8 pagesVaping in Preganacy A Systematic ReviewMia LouwNo ratings yet
- 6 Thinking Hats Detailed Model - UpdatedDocument32 pages6 Thinking Hats Detailed Model - Updatedgeetanshi mittalNo ratings yet
- Forum Ex 2 2Document5 pagesForum Ex 2 2Didan EnricoNo ratings yet
- Urbanclap 160731135642Document20 pagesUrbanclap 160731135642Kaustav Dey100% (1)
- TEFL I Course Prepares Students to Teach EnglishDocument8 pagesTEFL I Course Prepares Students to Teach EnglishErma DomosNo ratings yet
- Analog and Digital Communication Systems: The Transmission of Information Is Called CommunicationDocument71 pagesAnalog and Digital Communication Systems: The Transmission of Information Is Called Communication20-403 TejashwiniNo ratings yet
- 水印AMSCO® Advanced Placement® European History, 水印2nd Edition (Perfection Learning Authors)Document764 pages水印AMSCO® Advanced Placement® European History, 水印2nd Edition (Perfection Learning Authors)Cherry panNo ratings yet
- MdmedichaoiceDocument324 pagesMdmedichaoicelancastd54No ratings yet
- RSG 303Document196 pagesRSG 303Makinde TimiNo ratings yet
- Engine Technology Course A/F Control Classroom TrainingDocument14 pagesEngine Technology Course A/F Control Classroom Traininglongtrandang5867No ratings yet
- ES Model Question Paper With Solution KeyDocument10 pagesES Model Question Paper With Solution Keyvidhya_bineeshNo ratings yet
- SRV210 - 250TC Spare PartsDocument2 pagesSRV210 - 250TC Spare PartsEnzo SovittiNo ratings yet
- X-Plane Installer LogDocument3 pagesX-Plane Installer LogMarsala NistoNo ratings yet
- WEEK 7 ICPS - and - ICSSDocument31 pagesWEEK 7 ICPS - and - ICSScikguhafidzuddinNo ratings yet
- Saura, Jasmin E. - DVM - 2B Biochemistry (Activity 2)Document2 pagesSaura, Jasmin E. - DVM - 2B Biochemistry (Activity 2)Jasmin SauraNo ratings yet
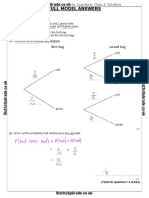
- Probability Tree Diagrams Solutions Mathsupgrade Co UkDocument10 pagesProbability Tree Diagrams Solutions Mathsupgrade Co UknatsNo ratings yet
- Certified Islamic Professional Accountant (Cipa) ProgramDocument13 pagesCertified Islamic Professional Accountant (Cipa) ProgramTijjani Ridwanulah AdewaleNo ratings yet
- Analgesia SystemDocument7 pagesAnalgesia SystemMudassar Roomi100% (1)
- Exercise 1: Chọn đáp án đúng:: Buổi 9: Động từ khuyết thiếu (Modal verb)Document6 pagesExercise 1: Chọn đáp án đúng:: Buổi 9: Động từ khuyết thiếu (Modal verb)Huyền HồNo ratings yet
- An Implementation of Illuminance Meter Using Light Dependent Resistor Integrated With Labview ProgramDocument11 pagesAn Implementation of Illuminance Meter Using Light Dependent Resistor Integrated With Labview ProgramAshraf YusofNo ratings yet
- Blackmores LTDDocument5 pagesBlackmores LTDEddy MusyokaNo ratings yet
- SampleContract ShuttleDocument10 pagesSampleContract ShuttleLJ BNo ratings yet
- Beowulf The Monsters and The Critics SevDocument20 pagesBeowulf The Monsters and The Critics SevNirmala GaneshNo ratings yet
- Photon BrochureDocument1 pagePhoton Brochureshwetha281889242No ratings yet
- Kristine Jane T. Zipagan Assignment: 1. Parts of InfographicsDocument2 pagesKristine Jane T. Zipagan Assignment: 1. Parts of InfographicsChristyNo ratings yet