Professional Documents
Culture Documents
Asthma 1
Asthma 1
Uploaded by
لوى كمال0 ratings0% found this document useful (0 votes)
6 views5 pagesCopyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
6 views5 pagesAsthma 1
Asthma 1
Uploaded by
لوى كمالCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 5
Asthma
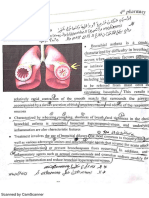
Asthma is a disease that affects the airways (bronchi) of the lungs.
Asthma is characterized by a predisposition to chronic airway inflammation and bronchoconstriction
The inflammation and bronchoconstriction cause airflow obstruction, which results in expiratory airflow
limitation (difficulty with exhalation).
This results in recurrent episodes of wheezing, breathlessness, chest tightness and coughing, which are the
classic symptoms of asthma
The inflammation and bronchoconstriction in asthma is reversible with medication (and sometimes
spontaneously).
The most common complication of asthma is exacerbations, which can range from mild to severe, and in
some cases can be fatal.
Diagnosis
Most types of asthma have activation of inflammatory mediators (e.g., histamine, leukotrienes, cytokines)
and an increase in inflammatory cells (e.g., mast cells, eosinophils) contributing to the disease
Some patients have a genetic predisposition to the development of severe allergic asthma, which is mediated
by immunoglobulin E (igE), or severe eosinophilic asthma
An asthma diagnosis is confirmed with spirometry and pulmonary function tests
These should be measured at the patient' s baseline, and after use of a short- acting bronchodilator (e.g.,
albuterol) to test for reversibility (i.e.,if the FEV1 increases by more than 12% with the use of bronchodilator).
Peak expiratory flow rate (PEFR) is measured using a peak flow meter. This is typically used for monitoring
asthma control as part of the asthma action plan, but it can be used at initial diagnosis to test for variability in
expiratory airflow limitation.
Patients will use the peak flow meter twice daily for a period of two weeks to check the PEFR;
if the average daily PEFR variability is greater than 10%, this suggests a diagnosis of asthma.
SPIROMETRY:TESTS LUNG FUNCTION (HOW WELL THE LUNGS WORK)
1. FEV1 How much air can be forcefully exhaled in one second.
2. FVC After taking a deep breath, the maximum volume of air that is exhaled (how much air is exhaled)
3. FEV1/FVC The percentage of total air capacity ("vital capacity") that can be forcefully exhaled in one
second (the speed of the exhale).
CLASSIFYING ASTHMA SEVERITY
Components of Severity Intermittent Persistent
Mild Moderate Sever
Daytime symptoms < 2 days/week > 2 days/week but not daily Daily Throughout the day
Nighttime awakenings < 2x/month 3-4x/month > lx/week but not Often (7x/week)
nightly
Rescue inhaler use < 2 days/week > 2 days/week ,but not daily Daily Several times per day
or >1x/day
Activity limitations None Minor limitation Some limitation Extremely limited
Lung function FEV1(% > 80% Normal > 80% Normal 60-80% Reduced 5% 60% Reduced 5%
predicted) FEV1/FVC
Recommended Step for Step 1 Step 2 Step 3 Step 4 or 5
Initiating Treatment
•Normal FEV1/FVC by age: 8-19 years. 85%; 20-39 years, 80%; 40-59 years. 75%; 60-80 years,70%
CONTROLLING RISK FACTORS
Patients with asthma should avoid exposure to tobacco smoke
An annual influenza vaccine is recommended in all patients with asthma > 6 months of age.
Patients age 2-64 years should receive one dose of the pneumococcal polysaccharide vaccine (PPSV23, Pneumovax 23)
Any patient with persistent asthma and a clear connection of symptoms with exposure to an allergen should have skin
or in vitro testing to assess sensitivity.
Treatment with subcutaneous allergen immunotherapy should be used, if indicated, based on the test results.
DRUG TREATMENT
Inhaled forms deliver drugs directly into the lungs, have reduced toxicity and are the preferred delivery vehicle.
Drugs used to treat asthma long-term are classified as relievers (rescue inhalers) or controllers (maintenance drugs)
Rescue inhalers can be used preventively for exercise-induced bronchospasm (EIB)
Relievers, or rescue inhalers, rapidly open airways within minutes of inhalation to make breathing easier.
Controllers, or maintenance inhalers, are taken on a chronic, daily basis to reduce inflammation and maintain asthma
Inhaled corticosteroids (ICS) are the mainstay of treatment for patients with asthma.
ASTHMA MEDICATION CLASS
Relievers (Rescue Drugs) Note
Inhaled low-dose ICS + formoterol Combines an inhaled corticosteroid (ICS) and a long-acting beta-2
agonist (LABA)
Used intermittently (as needed) for acute asthma symptoms
Combination proven to have reduced exacerbations over SABA alone
Inhaled short-acting beta-2 agonists (SABAs) Used intermittently (as needed) for acute asthma symptoms
Quickly reverse bronchoconstriction
Systemic steroids Injections: used during exacerbations
Oral: used during exacerbations or for severe asthma that is difficult to
control with other drug combinations
Inhaled epinephrine Available OTC, can be used for acute treatment of mild symptoms in
intermittent asthma only
Inhaled short-acting muscarinic antagonists Can be used in combination during exacerbations
Controllers (Maintenance Drugs) Note
Inhaled corticosteroids (ICS) First-line for all patients with persistent asthma;
Inhaled long-acting beta-2 agonists (LABAs) Used in combination with ICS (should never be used alone due to
increased risk of serious adverse outcomes)
Oral leukotriene receptor antagonists Alternative option to LABA in combination with ICS; can also be added
(LTRAs) to ICS/LABA treatment
Most commonly used in children
Theophylline (oral or IV) Least desirable option for add-on treatment due to significant adverse
effects, drug interactions and the need to monitor serum drug
concentrations
Inhaled long-acting muscarinic antagonists Can be used as add-on treatment in patients with a history of
(LAMAs) exacerbations despite ICS/ LABA treatment
Injectable monoclonal antibodies (SC or IV) Add-on treatment in persistent severe asthma of a specific type:
Omalizumab: for severe allergic asthma Mepolizumab, reslizumab,
benralizumab and dupilumab: for severe eosinophilic asthma
DETERMINE TREATMENT STEP BASED ON ASTHMA SEVERITY
Step 1 (Intermittent Asthma) As-needed low-dose ICS + formoterol or low-dose ICS taken whenever SABA is taken
Step 2 (Mild Persistent Asthma) Daily low-dose ICS or as-needed low-dose ICS + formoterol
Step 3 (Moderate Persistent Asthma) Low-dose ICS + LABA
Step 4 (Severe Persistent Asthma) Medium-dose ICS + LABA
Step 5 (Severe Persistent Asthma) High-dose ICS + LABA, refer for further assessment
BETA-2 AGONISTS
These medications bind to beta-2 receptors, causing relaxation of bronchial smooth muscle, which leads to
bronchodilation.
SABAs are used as needed (rescue therapy) for acute asthma symptoms.
LABAs are used as part of maintenance therapy beginning in Step 3 of treatment and only in combination with an ICS.
Short-Acting Beta-2 Agonists (SABAs)
Drugs Note
Albuterol SIDE EFFECTS
Levalbuterol Nervousness, tremor, tachycardia, palpitations, cough, hyperglycemia , decrease K
Racepinephrine MONITORING
Epinephrine Number of days of SABA use, symptom frequency, peak flow, pulmonary function tests, BP, HR,
blood glucose, K
NOTES
Levalbuterol contains R-isomer of albuterol
Epinephrine inhaler is FDA-approved for mild symptoms in intermittent asthma only. Not
discussed in guidelines.
Long-Acting Beta-2 Agonists (LABAs)
Salmetrol Increase risk of asthma-related deaths, should only be used in asthma patients who are currently
receiving but are not adequately controlled on a long-term asthma control medication (an inhaled
corticosteroid)
Increase risk of asthma-related hospitalizations in pediatric and adolescent patients I
Maintenance inhaler only; not for acute bronchospasm
INHALED CORTICOSTEROIDS
They block the late-phase reaction to the allergen, reduce airway hyper-responsiveness, and are potent and effective
anti-inflammatory medications.
ICSs reduce symptoms, increase lung function, improve quality of life and reduce the risk of exacerbations.
They are used as-needed in combination with formoterol for rescue treatment with acute symptoms, and individually
or in combination for maintenance/controller treatment.
DRUG Notes
Bedomethasone High doses for prolonged periods of time can cause adrenal suppression,I ncrease risk of fractures,
Budesonide growth retardation (in children) and immunosuppression
Fluticasone Cause Dysphonia (difficulty speaking), oral candidiasis (thrush), cough
Mometasone To prevent oral candidiasis, rinse mouth and throat with warm water and spit out after each use,
or use a spacer device if using a MDI
Budesonide is the only ICS available as a nebulized solution; used commonly in young children
LEUKOTRIENE MODIFYING AGENTS
Leukotriene receptor antagonists (LTRAs) inhibit leukotriene mediators of airway inflammation. This reduces airway
edema, constriction and inflammation.
Montelukast inhibits leukotriene D4 (LTD4)
Zafirlukast inhibits both LTD4 and LTE4.
Zileuton, a 5-lipoxygenase inhibitor, inhibits leukotriene formation
Drug Notes
Montelukast Warning
Zafirlukast Neuropsychiatric events; monitor for signs of aggressive behavior, hostility, agitation, hallucinations,
Zileuton depression, suicidal thinking
Monitor
LFTs (zafirlukast and zileuton), mood or behavior changes (montelukast)
Note
Zafirlukast: protect from moisture and light; dispense in original container
Montelukast 10 mg daily in the evening
Montelukast Age 6-14 years: 5 mg daily in the evening
Montelukast Age 1-5 years: 4 mg daily in the evening
THEOPHYLLINE
Theophylline blocks phosphodiesterase, causing an increase in cyclic adenosine monophosphate (cAMP) and release of
epinephrine from adrenal medulla cells.
This results in bronchodilation, but it also causes diuresis, CNS and cardiac stimulation and gastric acid secretion.
Use of theophylline is limited by decrease , effectiveness, drug interactions and adverse effects.
Theophylline Caution in patients with cardiovascular disease, hyperthyroidism, PUD and seizure disorder
Cause increase HR, insomnia, tremor and nervousness
Signs of toxicity: persistent vomiting, arrhythmias, seizures
Note
To convert aminophylline to theophylline, multiply by 0.8*; to convert theophylline to aminophylline,
divide by 0.8
Therapeutic range: 5-15 mcg/mL (measure peak level at steady state, after 3 days of oral dosing)
Active metabolites are caffeine and 3-methylxanthine
Aminophylline contains 80% theophylline
ANTICHOLINERGICS
Anticholinergics inhibit muscarinic cholinergic receptors and reduce the intrinsic vagal tone of the airway, leading to
bronchodilation.
Short-acting anticholinergics (e.g., ipratropium) are sometimes used in combination with SABAs in hospitalized patients
experiencing an acute exacerbation.
A long-acting anticholinergic, tiotropium is FDA-approved for asthma in patients 6 years of age and older with a history
of exacerbations despite ICS/LABA therapy
OMALIZUMAB
Omalizumab is a monoclonal antibody that inhibits IgE binding to the IgE receptor on mast cells and basophils.
It is indicated for moderate to severe persistent, allergic asthma in patients 6 years of age and older if a skin test to a
perennial allergen is positive and symptom control on inhaled corticosteroids is inadequate (Step 5 or 6 treatment).
Omalizumab Anaphylaxis has occurred as early as after the first dose but also has occurred beyond 1 year after
beginning treatment
Monitor Baseline IgE, FEV1, peak flow, s/sx of anaphylaxis and infection
Given SC every 2 or 4 weeks
INTERLEUKIN RECEPTOR ANTAGONISTS
Interleukin is a cytokine responsible for the growth, differentiation, recruitment, activation and survival of eosinophils
Monoclonal antibodies can be used to inhibit interleukin from binding to receptors.
Mepolizumab, reslizumab and benralizumab are IL-5 receptor antagonists, and dupilumab is an IL-4 and IL-3 receptor
antagonist.
All are indicated for management of severe asthma with an eosinophilic phenotype
Mepolizumab is indicated in patients > 12 years of age and given SC once every four weeks.
Reslizumab is indicated in adult patients only, and is given IV once every four weeks has a boxed warning for
anaphylaxis
Benralizumab is indicated for patients > 12 years of age and given SC once every four weeks x three doses, then every
eight weeks.
Dupilumab is indicated for patients > 12 years of age and given SC every other week.
SPECIAL SITUATIONS
EXERCISE-INDUCED BRONCHOSPASM
SABAs are preferred to prevent most EIB.
They are taken 5 - 15 minutes before exercise and last 2-3 hours.
If a longer duration ofsymptom control is needed, salmeterol (a LABA), can be taken 30 minutes before exercise.
If the patient is using a LABA for asthma maintenance, they should not use additional doses for EIB.
LABAs should never be used alone for persistent asthma.
Montelukast is taken two hours prior to exercise and lasts up to 24 hours.
PREGNANCY
A short-acting beta-agonist is a must.
ICS are preferred controllers, typically budesonide.
Important note
Different classes of controller medications for asthma and chronic obstructive pulmonary disease (COPD).
ICS and ICS/LABA combinations are preferred for asthma, whereas LABA, LAMA or LAMA/LABA combinations are
preferred for COPD.
Some ICS/LABA combinations are approved for COPD and can be used in select patients (see COPD chapter for
treatment recommendations).
Drugs that can increase theophylline levels due to CYP1A2 inhibition include: cimetidine, ciprofloxacin, fluvoxamine,
propranolol, zafirlukast and zileuton.
Drugs and conditions that can decrease theophylline levels: carbamazepine, fosphenytoin, phenobarbital, phenytoin,
primidone, rifampin, ritonavir, tobacco/marijuana smoking, St. John’s wort, levothyroxine, high-protein diet and
charbroiled meats.
Drugs that can increase theophylline levels due to CYP3A4 inhibition include: clarithromycin and erythromycin.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5814)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- أدوات الاستفهام فى اللغة الانجليزيةDocument21 pagesأدوات الاستفهام فى اللغة الانجليزيةلوى كمالNo ratings yet
- 700 سؤال مهمDocument114 pages700 سؤال مهملوى كمالNo ratings yet
- ملف غادة تصحيح منى نصر-1Document54 pagesملف غادة تصحيح منى نصر-1لوى كمالNo ratings yet
- 3) Cases ElnahdiDocument42 pages3) Cases Elnahdiلوى كمالNo ratings yet
- مبادئ الإحصاء الطبيDocument74 pagesمبادئ الإحصاء الطبيلوى كمالNo ratings yet
- اختبار صيدلة المجتمع النهائيDocument6 pagesاختبار صيدلة المجتمع النهائيلوى كمالNo ratings yet
- ChemotherpyDocument79 pagesChemotherpyلوى كمالNo ratings yet
- Hepatitis SummaryDocument3 pagesHepatitis Summaryلوى كمالNo ratings yet
- أدوية البرد والانفلونزاCold and Flu??Document57 pagesأدوية البرد والانفلونزاCold and Flu??لوى كمالNo ratings yet
- SPLE Group, Peptic UlcerDocument16 pagesSPLE Group, Peptic Ulcerلوى كمالNo ratings yet
- Orion - Mona NasrDocument169 pagesOrion - Mona Nasrلوى كمال100% (1)
- 876678Document10 pages876678لوى كمالNo ratings yet
- PhytomedicineDocument45 pagesPhytomedicineلوى كمالNo ratings yet
- Pharmaceutics &Document22 pagesPharmaceutics &لوى كمالNo ratings yet
- 4 5978807622374002235Document6 pages4 5978807622374002235لوى كمالNo ratings yet
- حل نموذج اختبار DdsDocument5 pagesحل نموذج اختبار Ddsلوى كمالNo ratings yet
- CeuticsDocument28 pagesCeuticsلوى كمالNo ratings yet
- 4 5854696639616257570Document16 pages4 5854696639616257570لوى كمالNo ratings yet
- 4 5965129697724468390Document12 pages4 5965129697724468390لوى كمالNo ratings yet
- Protocol 002Document21 pagesProtocol 002لوى كمالNo ratings yet
- PD (Sple Lec) 13.10.21Document48 pagesPD (Sple Lec) 13.10.21لوى كمالNo ratings yet
- Sterile and Non Sterile CompoundingDocument52 pagesSterile and Non Sterile Compoundingلوى كمالNo ratings yet