Professional Documents
Culture Documents
ML 10 2 120
Uploaded by
Gusti Ayu Sattwika PramitaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
ML 10 2 120
Uploaded by
Gusti Ayu Sattwika PramitaCopyright:
Available Formats
Case Report
Med Laser 2021;10(2):120-122
https://doi.org/10.25289/ML.2021.10.2.120
pISSN 2287-8300ㆍeISSN 2288-0224
Partial Unilateral Lentiginosis Successfully Treated with a
High-fluence 1,064-nm Q-switched Neodymium:Yttrium-
aluminum-garnet Laser
Jun Ki Hong Partial unilateral lentiginosis (PUL) is an unusual pigmentary disorder
Hye Sung Han characterized by numerous lentigines on the skin, with onset usually
Sun Hye Shin during early childhood. It is characterized by unilateral segmental dis
Kwang Ho Yoo tribution with sharp margins in one or more dermatomes. Conventional
laser treatments result in several adverse effects, such as mottled
pigmentary changes (hyper or hypopigmentation), especially in people of
Department of Dermatology, Chung-Ang
Asian descent. A 57-year-old man with PUL on the neck was treated with
University Hospital, Seoul, Korea a high-fluence 1,064-nm Q-switched (QS) neodymium-doped yttrium-
aluminum-garnet (Nd:YAG) laser. After 20 treatment sessions, the
lesions markedly improved without adverse effects or recurrence. We
suggest that high-fluence 1,064-nm QS Nd:YAG laser treatment is an
effective and safe modality for PUL.
Key words
Partial unilateral lentiginosis; Neodymium:yttrium-aluminum-garnet laser
Received March 15, 2021
Accepted April 19, 2021
Correspondence
Kwang Ho Yoo
Department of Dermatology, Chung-Ang
University Hospital, 102 Heukseok-ro,
Dongjak-gu, Seoul 06973, Korea
Tel.: +82-2-6299-3179
Fax: +82-2-6299-1718
E-mail: psyfan9077@naver.com
C Korean Society for Laser Medicine and Surgery
CC This is an open access article distributed under the
terms of the Creative Commons Attribution Non-
Commercial License (http://creativecommons.org/
licenses/by-nc/4.0) which permits unrestricted non-
commercial use, distribution, and reproduction in any
medium, provided the original work is properly cited.
120 Medical Lasers; Engineering, Basic Research, and Clinical Application
PUL Treated with Nd:YAG Laser
Jun Ki Hong, et al.
Case Report
INTRODUCTION and histo-pathologically diagnosed as PUL, and high-
fluence 1,064-nm QS Nd:YAG laser treatments were per-
Partial unilateral lentiginosis (PUL) is a rare pigmentary formed. Before the laser treatment, a topical anesthetic
disorder characterized by multiple lentigines on the skin (EMLA cream 5%; AstraZeneca AB, Sodertalje, Sweden)
and unilateral segmental distribution with sharp margins was applied for 30 minutes under occlusion. The patient
in the midline in one or more dermatomes.1 The lesions underwent 20 sessions of 1,064-nm QS Nd:YAG laser
almost always first appear during early childhood. PUL (SPECTRA; Lutronic Corp., Goyang, Korea) treatment at
can occur anywhere on the body, including the face, neck, 2-week intervals, using 2–3 sliding-stacking passes with
trunk, and upper and lower extremities. For cosmetic appropriate overlap and a spot size of 7 mm, fluence of 2.4
reasons, various conventional lasers have been utilized J/cm2, and pulse rate of 10 Hz, to achieve mild erythema.
to remove PUL; however, the treatment outcomes are The treated area was cooled with gauze, which had been
often unsatisfactory and adverse effects such as mottled soaked in normal saline for 10 minutes, immediately after
pigmentary changes (hyper or hypopigmentation) may each laser treatment session. Most of the pigmented le-
occur.2,3 Herein, we report a case of PUL on the neck that sions disappeared after 20 sessions of treatment (Fig. 1C).
was successfully treated with a high-fluence 1,064-nm No mottled pigmentary changes (hyper or hypopigmenta-
Q-switched (QS) neodymium-doped yttrium-aluminum- tion) were observed until the 6-month follow-up (Fig. 1D).
garnet (Nd:YAG) laser without recurrence. We suggest
that this treatment could be applicable to patients with DISCUSSION
other lentiginous disorders as well because their clinical
and histological findings are similar to those of PUL. Various types of laser devices, including the 532-nm
Nd:YAG laser, ruby laser, 755-nm alexandrite laser, and
CASE REPORT intense pulsed light, have been used to treat pigmentary
disorders.4-6 However, no standard treatment has been
A 57-year-old man presented to our clinic with unilater- established for PUL because treatment outcomes are
ally distributed brownish patches greater than 10 × 15 cm variable, and adverse effects such as mottled pigmentary
in diameter, with sharply demarcated borders, on the left changes (hyper or hypopigmentation) are common. Hy-
posterior neck. The patches were shown in Fig. 1A. He perpigmentation may occur when cytokines and inflam-
reported that the lesions had first appeared during early matory mediators, secreted by damaged keratinocytes,
childhood. Prior to his visit, he had been treated with vari- activate melanocytes and increase melanin synthesis.7,8
ous laser devices at other clinics. However, the outcomes Other damaged perilesional melanocyte cells also induce
were unsatisfactory because the lesions recurred a few unwanted hypopigmentation.4
months after the treatments, following partial resolution. To achieve successful outcomes, it is necessary to
Skin biopsy revealed increased melanin pigmentation in optimize the delivery of laser energy to the pigmentary
the basal layer, which is the typical histological finding lesions, while sparing the perilesional cells as much as
of lentigo simplex. The pigmented lesions were clinically possible. In this study, the delivery of laser energy to the
A B C D
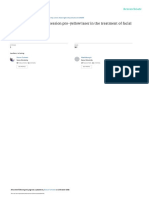
Fig. 1. Clinical manifestations and treatment response of a 57-year-old Korean man with partial unilateral lentiginosis on the right posterior neck.
(A) At baseline, (B) after 10 sessions of treatment (20 weeks after baseline), and (C) after 20 sessions of treatment (40 weeks after baseline). (D) At
6 months after the last treatment session.
VOLUME 10 NUMBER 2 June 2021 121
PUL was optimized to avoid permanent adverse effects, with low-fluence 1,064 nm Q-switched neodymium-doped yt-
while preventing recurrence. The 1,064-nm QS Nd:YAG trium aluminum garnet laser. Case Rep Dermatol 2017;9:30-4.
laser has been suggested to cause degradation of mela- 3. Pickering JG. Partial unilateral lentiginosis with associated de-
nin granules. A low-fluence 1,064-nm QS Nd:YAG laser velopmental abnormalities. Guys Hosp Rep 1973;122:361-70.
has been widely used for treating many pigmentary dis- 4. Baek JO, Park IJ, Lee KR, Ryu HR, Kim J, Lee S, et al. High-
orders; however, many Korean patients with pigmentary fluence 1064-nm Q-switched Nd:YAG laser: safe and effective
lesions are reported to be at a high risk of recurrence.9 treatment of café-au-lait macules in Asian patients. J Cosmet
In the present case, the high-fluence 1,064-nm Nd:YAG Dermatol 2018;17:380-4.
laser yielded satisfactory and long-lasting therapeutic 5. Kim HR, Ha JM, Park MS, Lee Y, Seo YJ, Kim CD, et al. A low-
outcomes by causing sufficient damage to the target cells fluence 1064-nm Q-switched neodymium-doped yttrium alu-
and preserving the perilesional normal tissue. After each minium garnet laser for the treatment of café-au-lait macules.
session of treatment, we closely observed the occurrence J Am Acad Dermatol 2015;73:477-83.
of side effects to decrease the risk of laser-induced hyper 6. Kim J, Hur H, Kim YR, Cho SB. Treatment of café-au-
or hypopigmentation. Only mild erythema was observed, lait macules with a high-fluenced 1064-nm Q-switched
so we continued the treatment with this treatment regi- neodymium:yttrium aluminum garnet laser. J Cosmet Laser
men. This approach can prevent laser-induced mottled Ther 2018;20:17-20.
pigmentary changes (hyper or hypopigmentation) and 7. Okazaki M, Yoshimura K, Suzuki Y, Uchida G, Kitano Y, Harii K,
reduce the risk of recurrence through adjustment of the et al. The mechanism of epidermal hyperpigmentation in café-
parameters of the laser device. au-lait macules of neurofibromatosis type 1 (von Reckling-
In conclusion, we experienced that high-fluence 1064- hausen's disease) may be associated with dermal fibroblast-
nm QS Nd:YAG laser treatment, using a spot size of 7 derived stem cell factor and hepatocyte growth factor. Br J
mm, fluence of 2.4 J/cm2, and pulse rate of 10 Hz with 2–3 Dermatol 2003;148:689-97.
sliding-stacking passes, is effective and safe for PUL. The 8. Okazaki M, Yoshimura K, Uchida G, Suzuki Y, Kitano Y, Harii K.
parameters were effective for preventing complications Epidermal hyperpigmentation in non-syndromic solitary cafe-
and recurrences after treatment. As our outcome analy- au-lait macules may be associated with increased secretion of
sis was limited to only one case, further investigations will endothelin-1 by lesional keratinocytes. Scand J Plast Reconstr
be needed for providing optimize the parameters. Surg Hand Surg 2005;39:213-7.
9. Kim MJ, Kim JS, Cho SB. Punctate leucoderma after melasma
CONFLICT OF INTEREST treatment using 1064-nm Q-switched Nd:YAG laser with low
pulse energy. J Eur Acad Dermatol Venereol 2009;23:960-2.
The authors declare no conflicts of interest.
How to cite this article: Hong JK, Han HS, Shin SH, Yoo
REFERENCES KH. Partial unilateral lentiginosis successfully treated with
a high-fluence 1,064-nm Q-switched neodymium:yttrium
1. Trattner A, Metzker A. Partial unilateral lentiginosis. J Am Acad
aluminum garnet laser. Med Laser 2021;10:120-122. https://doi.
Dermatol 1993;29(5 Pt 1):693-5.
org/10.25289/ML.2021.10.2.120
2. Kim EH. A case of facial partial unilateral lentiginosis treated
122 Medical Lasers; Engineering, Basic Research, and Clinical Application
You might also like
- ML010 02 120Document3 pagesML010 02 120Trần Hồng MyNo ratings yet
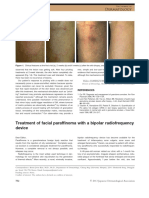
- Treatment of Epidermal Pigmented Lesions With 578 NM Yellow LaserDocument4 pagesTreatment of Epidermal Pigmented Lesions With 578 NM Yellow LaserArismunandar SosiloNo ratings yet
- Ad 29 427Document6 pagesAd 29 427hadi firmanNo ratings yet
- Treatment of Xanthelasma Palpebrarum by The Pinhole MethodDocument3 pagesTreatment of Xanthelasma Palpebrarum by The Pinhole MethodАркадий ЖивицаNo ratings yet
- RepigmentationDocument4 pagesRepigmentationMariyaNo ratings yet
- Bilateral Nevus of Ota Treated With Combination of CO Fractional Laser and 1064 NM Nd:YAG LaserDocument10 pagesBilateral Nevus of Ota Treated With Combination of CO Fractional Laser and 1064 NM Nd:YAG LaserNur CameliaNo ratings yet
- A 1064 NM Long-Pulsed Nd:YAG Laser For Treatment of Diverse Vascular DisordersDocument5 pagesA 1064 NM Long-Pulsed Nd:YAG Laser For Treatment of Diverse Vascular DisordersIngook SongNo ratings yet
- AlexandriteDocument4 pagesAlexandriteHong Nguyen ThiNo ratings yet
- SAMPLE CASE REPORT - Efficacy of Q-Switched ND YAG Laser in The Treatment of Freckles (ABNOM)Document9 pagesSAMPLE CASE REPORT - Efficacy of Q-Switched ND YAG Laser in The Treatment of Freckles (ABNOM)dnaielNo ratings yet
- Efficacy and Safety of A Novel 785 NM Picosecond Neodymium-Doped Yttrium Aluminum Garnet Laser For The Treatment of Facial Benign Pigmented Lesions inDocument6 pagesEfficacy and Safety of A Novel 785 NM Picosecond Neodymium-Doped Yttrium Aluminum Garnet Laser For The Treatment of Facial Benign Pigmented Lesions inNileena HydroseNo ratings yet
- Pigmentary Disorders in Asian Skin Treatment With Laser and Intense Pulsed Light SourcesDocument8 pagesPigmentary Disorders in Asian Skin Treatment With Laser and Intense Pulsed Light SourcesLutfi MKNo ratings yet
- LLL EyeDocument5 pagesLLL EyeNoura RoseNo ratings yet
- Treatment of Xanthelasma Palpebrarum by Fractional Carbon Dioxide LaserDocument1 pageTreatment of Xanthelasma Palpebrarum by Fractional Carbon Dioxide LaserАркадий ЖивицаNo ratings yet
- Clinical Effectiveness of Low-Fluence 585 NM Q-Switched NdYAG Laser Treatment On Persistent FacDocument6 pagesClinical Effectiveness of Low-Fluence 585 NM Q-Switched NdYAG Laser Treatment On Persistent FacBen BVHNo ratings yet
- Low-Fluence 1,064-nm Laser Hair Reduction For Pseudofolliculitis Barbae in Skin Types IV, V, and VIDocument10 pagesLow-Fluence 1,064-nm Laser Hair Reduction For Pseudofolliculitis Barbae in Skin Types IV, V, and VIRada TrifonovNo ratings yet
- Laser Hemangiomas 2023Document16 pagesLaser Hemangiomas 2023YosiNo ratings yet
- Review Skin Rejuvenation Qswitched NdyagDocument4 pagesReview Skin Rejuvenation Qswitched NdyagMaestro JadNo ratings yet
- Pavlidis 2016Document14 pagesPavlidis 2016igorfragaNo ratings yet
- Bromhidrosis NdyagDocument5 pagesBromhidrosis Ndyagika_anggrainiNo ratings yet
- Tàn NhangDocument8 pagesTàn NhangHong Nguyen ThiNo ratings yet
- Treatment of Verrucous Epidermal NevusDocument16 pagesTreatment of Verrucous Epidermal NevusCat FishNo ratings yet
- Laser Treatment of Glaucoma AscheDocument63 pagesLaser Treatment of Glaucoma AscheAschalew MulugetaNo ratings yet
- Laha2020 Chua OnlinefirstDocument4 pagesLaha2020 Chua OnlinefirstBrian BeeNo ratings yet
- Neodymium-YAG Iridotomy in Closure Glaucoma: Preliminary StudyDocument5 pagesNeodymium-YAG Iridotomy in Closure Glaucoma: Preliminary StudyWalida FadillahNo ratings yet
- 921-0398-000 r1 RevLiteWP Small PDFDocument6 pages921-0398-000 r1 RevLiteWP Small PDFika_anggrainiNo ratings yet
- Carbon Peel Laser Technique To Improve Skin QualitDocument2 pagesCarbon Peel Laser Technique To Improve Skin QualitSarah Albaladejo VerezNo ratings yet
- The Use of Er:YAG, Nd:YAG and Ga-Al-As Lasers in Periapical Surgery: A 3-Year Clinical StudyDocument6 pagesThe Use of Er:YAG, Nd:YAG and Ga-Al-As Lasers in Periapical Surgery: A 3-Year Clinical StudyTôn Thất Đam TriềuNo ratings yet
- Argon Laser Trabeculoplasty in Narrow Angle GlaucomaDocument10 pagesArgon Laser Trabeculoplasty in Narrow Angle GlaucomaBery Decky SaputraNo ratings yet
- Theefficacyofasingle Sessionpro YellowlaserinthetreatmentDocument7 pagesTheefficacyofasingle Sessionpro YellowlaserinthetreatmentRiyena ClinicNo ratings yet
- Lasers in Urology DR BiokuDocument33 pagesLasers in Urology DR BiokumbiokuNo ratings yet
- Therapeutic Efficacy and Safety of Invasive Pulsed-Type Bipolar Alternating Current Radiofrequency On Melasma and Rebound HyperpigmentationDocument7 pagesTherapeutic Efficacy and Safety of Invasive Pulsed-Type Bipolar Alternating Current Radiofrequency On Melasma and Rebound HyperpigmentationLillian Floresta HajuNo ratings yet
- Yeo 2013Document2 pagesYeo 2013Patrick KimNo ratings yet
- Al Dhalimi2013Document6 pagesAl Dhalimi2013deltanueveNo ratings yet
- Laser Treatment Postacne Scars1Document14 pagesLaser Treatment Postacne Scars1Stanca NicolaeNo ratings yet
- CASE REPORT: Treatment of Acne Vulgaris With Long-Pulsed 1064 NM Nd:YAG LaserDocument4 pagesCASE REPORT: Treatment of Acne Vulgaris With Long-Pulsed 1064 NM Nd:YAG LaserjeannchristyNo ratings yet
- 15) Refractory Open-Angle Glaucoma After Neodymium - Yttrium-Aluminum-Garnet Laser Lysis of Vitreous FloatersDocument6 pages15) Refractory Open-Angle Glaucoma After Neodymium - Yttrium-Aluminum-Garnet Laser Lysis of Vitreous FloatershasdiniNo ratings yet
- Dosimetric Evaluation of Anterior Visual Pathway Structures I.E Optic Nerve and Chiasma in Adjuvant Radiation Therapy of Glial Tumors Treated Using Intensity Modulated Radiation TherapyAn Observational StudyDocument3 pagesDosimetric Evaluation of Anterior Visual Pathway Structures I.E Optic Nerve and Chiasma in Adjuvant Radiation Therapy of Glial Tumors Treated Using Intensity Modulated Radiation TherapyAn Observational StudyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Effectiveness of Short-Pulse Width NdYAG in Laser Hair Jane2018Document7 pagesEffectiveness of Short-Pulse Width NdYAG in Laser Hair Jane2018MACPANAMERANo ratings yet
- Therapeutic Application of Lasers in OphthalmologyDocument5 pagesTherapeutic Application of Lasers in OphthalmologyKashif RazaNo ratings yet
- Seunglee 2008Document5 pagesSeunglee 2008dl qiuNo ratings yet
- Suh 2019Document23 pagesSuh 2019Andrean LinataNo ratings yet
- Evaluation of An Ablative and Non-Ablative Laser Procedure in The Treatment of Striae Distensae 2014Document6 pagesEvaluation of An Ablative and Non-Ablative Laser Procedure in The Treatment of Striae Distensae 2014Paula GuimaNo ratings yet
- Nevus BeckerDocument7 pagesNevus BeckerMarcelo Ortiz ValenzuelaNo ratings yet
- Duca2020 Ndyag Nevus OtaDocument4 pagesDuca2020 Ndyag Nevus OtaErnawati HidayatNo ratings yet
- A Review of The Adverse Effects of Laser Hair RemovalDocument5 pagesA Review of The Adverse Effects of Laser Hair RemovalSimão NóbregaNo ratings yet
- Scalpel Versus Diode Laser For Gingival Depigmentation: A Case ReportDocument8 pagesScalpel Versus Diode Laser For Gingival Depigmentation: A Case ReportIJAR JOURNALNo ratings yet
- WS PQX SemarangDocument33 pagesWS PQX SemarangKharmijyNo ratings yet
- Managing Burn Scar With A Combination Therapy of Long Pulsed 1064 NM ND YAG LPND Laser Topical Tretinoin and HydroquinoneDocument5 pagesManaging Burn Scar With A Combination Therapy of Long Pulsed 1064 NM ND YAG LPND Laser Topical Tretinoin and HydroquinoneMikail Ahmad FawzyNo ratings yet
- Carbon Activado 1Document9 pagesCarbon Activado 1Jefersson TiqueNo ratings yet
- Effective Treatment of Rosacea Using Intense Pulsed LightDocument5 pagesEffective Treatment of Rosacea Using Intense Pulsed LightVo Ha Phuong NguyenNo ratings yet
- Photodynamic Therapy As Adjuvant Treatment of Extensive Basal Cell Carcinoma Treated With Mohs Micrographic SurgeryDocument19 pagesPhotodynamic Therapy As Adjuvant Treatment of Extensive Basal Cell Carcinoma Treated With Mohs Micrographic SurgerydocanggunNo ratings yet
- Early Postoperative Treatment of Thyroidectomy Scars UsingDocument7 pagesEarly Postoperative Treatment of Thyroidectomy Scars UsingАркадий ЖивицаNo ratings yet
- Unusual Adverse Reaction in A Patient Sensitized With Photosan 3Document2 pagesUnusual Adverse Reaction in A Patient Sensitized With Photosan 3Dayse CSMNo ratings yet
- Vascular MalformationsDocument15 pagesVascular MalformationsMahmoud MuhamedNo ratings yet
- IPL - Photo Rejuvenation Seminars - SADICK & WEISSDocument8 pagesIPL - Photo Rejuvenation Seminars - SADICK & WEISSLarissa LopesNo ratings yet
- Managing Complications in Glaucoma SurgeryDocument121 pagesManaging Complications in Glaucoma Surgeryshetya_8212No ratings yet
- Photoderm Photoimm Photomed - 2008 - Anbar - Effect of One Session of ER YAG Laser Ablation Plus Topical 5fluorouracil OnDocument8 pagesPhotoderm Photoimm Photomed - 2008 - Anbar - Effect of One Session of ER YAG Laser Ablation Plus Topical 5fluorouracil OnMostafa EidNo ratings yet
- Surgical Pearl: Ligation of The Base of Pyogenic Granuloma-An Atraumatic, Simple, and Cost-Effective ProcedureDocument2 pagesSurgical Pearl: Ligation of The Base of Pyogenic Granuloma-An Atraumatic, Simple, and Cost-Effective ProceduregabbynengNo ratings yet
- Laser Treatment For Post Acne Scars - A ReviewDocument6 pagesLaser Treatment For Post Acne Scars - A ReviewAryantii AntyNo ratings yet
- Target Volume Delineation and Field Setup: A Practical Guide for Conformal and Intensity-Modulated Radiation TherapyFrom EverandTarget Volume Delineation and Field Setup: A Practical Guide for Conformal and Intensity-Modulated Radiation TherapyNo ratings yet
- Experimental Dermatology - 2012 - Reddy - Bioactive Oligopeptides in Dermatology Part IDocument6 pagesExperimental Dermatology - 2012 - Reddy - Bioactive Oligopeptides in Dermatology Part IGusti Ayu Sattwika PramitaNo ratings yet
- User Manual: Caution Before UseDocument2 pagesUser Manual: Caution Before UseGusti Ayu Sattwika PramitaNo ratings yet
- Kurva NailhouseDocument1 pageKurva NailhouseGusti Ayu Sattwika PramitaNo ratings yet
- Gambar Hand RejuvenationDocument4 pagesGambar Hand RejuvenationGusti Ayu Sattwika PramitaNo ratings yet
- Recommendations For The Treatment of Tear Trough DDocument12 pagesRecommendations For The Treatment of Tear Trough DGusti Ayu Sattwika PramitaNo ratings yet
- Shake SpareDocument2 pagesShake SpareGusti Ayu Sattwika PramitaNo ratings yet
- Gambar UroDocument2 pagesGambar UroGusti Ayu Sattwika PramitaNo ratings yet
- A Fairy SongDocument1 pageA Fairy SongGusti Ayu Sattwika PramitaNo ratings yet
- A Fairy SongDocument1 pageA Fairy SongGusti Ayu Sattwika PramitaNo ratings yet
- Nutrilon PoemDocument1 pageNutrilon PoemGusti Ayu Sattwika PramitaNo ratings yet
- Nutrilon PoemDocument1 pageNutrilon PoemGusti Ayu Sattwika PramitaNo ratings yet
- Skin CancerDocument14 pagesSkin CancerGusti Ayu Sattwika PramitaNo ratings yet
- Fundamentals of Designing Relative Strength ProgramsDocument35 pagesFundamentals of Designing Relative Strength ProgramsFlorian WolfNo ratings yet
- B2 Practice ListeningDocument2 pagesB2 Practice ListeningDavy EverhartNo ratings yet
- International Journal of Trend in Scientific Research and Development (IJTSRD)Document4 pagesInternational Journal of Trend in Scientific Research and Development (IJTSRD)Editor IJTSRDNo ratings yet
- Bylaws-Craigs Mill Hoa 2013Document10 pagesBylaws-Craigs Mill Hoa 2013api-243024250No ratings yet
- Aliyani Association Between Vitamin D Deficiency and Psoriasis A CasecontrolstudyDocument5 pagesAliyani Association Between Vitamin D Deficiency and Psoriasis A CasecontrolstudyAzmi FadhlihNo ratings yet
- Oedipus SummaryDocument1 pageOedipus SummaryReynold FrancoNo ratings yet
- Invoice, packing list mẫuDocument2 pagesInvoice, packing list mẫuPHI BUI MINHNo ratings yet
- Accessing The Healing Power of The Vagus NerveDocument9 pagesAccessing The Healing Power of The Vagus NerveShubham Doshi33% (3)
- Midterm Requirement-Green BuildingDocument7 pagesMidterm Requirement-Green BuildingJo-anne RiveraNo ratings yet
- Chennai City Disaster Management Plan GCC 2021Document772 pagesChennai City Disaster Management Plan GCC 2021Disability Rights AllianceNo ratings yet
- Comparative Study For Determination of Atracurium Besilate in Presence of Its Toxic Degradant (Laudanosine) by Reversed Phase HPLC and by TLC DensitometryDocument11 pagesComparative Study For Determination of Atracurium Besilate in Presence of Its Toxic Degradant (Laudanosine) by Reversed Phase HPLC and by TLC DensitometrySabrina JonesNo ratings yet
- Mercaptans Removal From Gases by Absorption Into Amines and CausticDocument8 pagesMercaptans Removal From Gases by Absorption Into Amines and Causticgopal100% (1)
- Climate Responsive ArchitectureDocument32 pagesClimate Responsive ArchitectureNikhila CherughattuNo ratings yet
- Account Transfer Form: Fax Cover SheetDocument6 pagesAccount Transfer Form: Fax Cover SheetJitendra SharmaNo ratings yet
- Unit 2 Lesson 1 Chlor-Alkali IndustryDocument16 pagesUnit 2 Lesson 1 Chlor-Alkali IndustryGreen JeskNo ratings yet
- CHEM 333: Lab Experiment 5: Introduction To Chromatography : Thin Layer and High Performance Liquid ChromatographyDocument5 pagesCHEM 333: Lab Experiment 5: Introduction To Chromatography : Thin Layer and High Performance Liquid ChromatographymanurihimalshaNo ratings yet
- Spoilage of Frozen Chicken Nuggets by Toxigenic Psycrophilic FungiDocument16 pagesSpoilage of Frozen Chicken Nuggets by Toxigenic Psycrophilic FungiNIDHI BARINo ratings yet
- PGS 504 Notes Part IIDocument3 pagesPGS 504 Notes Part IISejal PriyaNo ratings yet
- 2019 PSRANM Conference Program FinalDocument24 pages2019 PSRANM Conference Program FinalKimmie JordanNo ratings yet
- ACS AMI FacilitatorDocument21 pagesACS AMI FacilitatorPaul Zantua57% (7)
- Name of Learner: Section: Subject Teacher: Date:: Practical Research 2Document4 pagesName of Learner: Section: Subject Teacher: Date:: Practical Research 2J-heart Basabas Malpal100% (6)
- Odontektomi Bahan Diskusi Od KoasDocument51 pagesOdontektomi Bahan Diskusi Od Koaspanjidrg100% (1)
- Formulating A Dental Treatment Plan: DR Tashnim BagusDocument33 pagesFormulating A Dental Treatment Plan: DR Tashnim BagustarekrabiNo ratings yet
- Substation Off Line and Hot Line CommissioningDocument3 pagesSubstation Off Line and Hot Line CommissioningMohammad JawadNo ratings yet
- Syntheis Writing 2 How Do Fear and Desire For Personal Acceptance Influence Human BehaviorDocument2 pagesSyntheis Writing 2 How Do Fear and Desire For Personal Acceptance Influence Human Behaviorapi-463684021No ratings yet
- Escape From The Western Diet Summary RevisedDocument3 pagesEscape From The Western Diet Summary Revisedapi-385530863100% (1)
- Case Study NCP ActualDocument3 pagesCase Study NCP Actualdhamy florNo ratings yet
- E 23 Fuel System Schaffer 4350ZDocument3 pagesE 23 Fuel System Schaffer 4350ZSergeyNo ratings yet
- Chapter 10 Fitness Training PrinciplesDocument80 pagesChapter 10 Fitness Training Principlesapi-115744109No ratings yet
- ASTM C309: Do Liquid Hardeners Meet This Standard?Document2 pagesASTM C309: Do Liquid Hardeners Meet This Standard?Kishore Nayak kNo ratings yet