Professional Documents
Culture Documents
Path4 5a
Uploaded by
Abid KhanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Path4 5a
Uploaded by
Abid KhanCopyright:
Available Formats
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
TOPIC 4: CHRONIC INFLAMMATION
SUMMARY OF CASE SCENARIOS
4.1 HAEMATEMESIS IN A 45-YEAR-OLD MAN .......................................................................................... 116
4.2 BLOODY DIARRHOEA IN A 39-YEAR-OLD WOMAN ........................................................................... 119
4.3 JOINT PAIN, FEVER AND STUPOR IN A 58-YEAR-OLD WOMAN...................................................... 122
4.4 HEADACHE, VOMITING AND FEVER IN A 7-YEAR-OLD GIRL........................................................... 125
4.5 RENAL FAILURE IN A 61-YEAR-OLD MAN........................................................................................... 130
Ó Royal Australasian College of Surgeons – December 2000 Page 110 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CHRONIC INFLAMMATION
GOALS AND OBJECTIVES
At the end of this topic you should be able to demonstrate an understanding of:
· structural and functional changes involved in the reactions of the defence and healing processes of
immune reactivity, acute and chronic (including granulomatous) inflammation, regeneration and fibrous
repair; this should include an ability to demonstrate understanding of the molecular/pharmacological
mechanisms which bring about these reactions, how they are endogenously modulated and how they
interact and are modified by pharmacological manipulation. An appreciation of both the beneficial and
harmful effects of these reactions should be able to be delineated, demonstrating an understanding of
the pathogenesis and pathology of aberrant defence reactions of importance in surgical practice (such as
inflammatory bowel disease, systemic vasculitis, rheumatoid disease);
· pathways by which chronic inflammation may arise, and give examples of each;
· the gross and histological features of chronic inflammation;
· complications of chronic inflammation, with examples of each;
· why some chronic inflammatory responses result in granuloma formation;
· the causes of granulomatous inflammation and their microscopic features.
REFERENCE SUBSECTIONS
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
Chapter 3, Chronic Inflammation and Healing
Ó Royal Australasian College of Surgeons – December 2000 Page 111 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Chronic Inflammation
Description - co-existing:
1. Acute inflammation (cellular and fluid exudate – variable extent)
2. Healing (‘frustrated’) – granulation and productive fibrosis
3. Lymphocytes, plasma cells, eosinophils
4. Monocyte derivatives – macrophages (+/- epithelioid cells) +/- giant cells. Epithelioid cells only in
‘immune’ CI (Tb, sarcoidosis etc)
5. Tissue destruction
Granulomatous Inflammation
"A highly cellular form of chronic inflammation, the predominant cells of which are monocytes and
their derivatives, macrophages, epithelioid cells and giant cells”.
The inciting agent is usually particulate, poorly soluble and persistent, either bland or antigenically active.
The section on granulomatous inflammation is somewhat confusing in Chapter 3 of Robbins. What is most
important is that there are distinct types of granulomatous inflammation:
1. Foreign body granuloma
This is an innate (non-immune) reaction where the recruited monocytes (from the blood) react to the
foreign (particulate and persisting) material by forming macrophages and, with large particles, foreign
body giant cells.
Despite the statement on page 83 of Robbins, epithelioid cells do not form in this ‘innate’ , non-immune,
foreign body granuloma – purely phagocytic (see EC function below)
2. Immune or epithelioid granuloma
In this reaction, an immune stimulus causes lymphocyte-mediated recruitment and differentiation of
blood-derived monocytes to epithelioid cells – these are not phagocytic; they are synthetic (lots of RER)
and secretory. They ‘wall-off’ the (infected) site and their secretions are presumed to be fibrogenic
cytokines (not yet characterised). The granuloma is avascular. Granulomatous immunity in
tuberculosis is accompanied by TH1 cell activation which induces the accompanying macrophages (yes,
both epithelioid cells and macrophages interact, the former directed by immunocyte [T-lymphocytes]
secretions, in particular g-interferon). Caseous necrosis is characteristic of infective immune
granulomas – tuberculosis in particular – presumed to be immune-mediated - ? Tc cell action.
Ó Royal Australasian College of Surgeons – December 2000 Page 112 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Morphological Patterns In Inflammation
· Serous
· Fibrinous
· Suppurative / purulent
· Necrotising
· Ulcerative
Systemic Effects
Acute phase reaction (note that this is prolonged in CI of any cause)
1. Fever
2. Serum protein changes
CRP, SAA, SAP
procoagulation Il-1 / TNF; IL-6
WBC / platelet other mediators
Autonomic
Behaviour
3. Cachexia, shock
4. Amyloidosis
Tuberculosis
M. tuberculosis and subtypes
· Not killed by non-immune host – resides in macrophage phagosomes
· Induces immune reaction
· Humoral –immune complex effects (eg ? erythema nodosum). No healing effect
· CMI – TH1, lymphokine-producing lymphocyte - Ý vascular effects; kills bacteria
· Granulomatous immunity - ? mediators – sequesters infection, induces fibrogenesis
Primary Infection
· Initial non-immune spreading state – Ghon focus and complex
· Immune state - halts spread, kills organisms, induces fibrous healing if successful
Ó Royal Australasian College of Surgeons – December 2000 Page 113 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Progressive Primary Tuberculosis
· Ineffectual immune response/overwhelming dose
· Progressive growth of primary focus and spread in regional nodes
· Vascular dissemination – via thoracic duct (miliary lung); pulmonary vein (miliary systemic)
Secondary/Reactivation Tuberculosis
· ‘Seeding’ during primary infection
· Predisposing causes to reactivation – age; immune breakdown etc.
Morphology
See also specific disease processes in case studies
Rheumatoid arthritis; inflammatory bowel disease; osteomyelitis; peptic ulcer etc.
Healing
Control of Normal Cell Growth
This introduction (pp 90-98) is also an excellent preliminary to the section on abnormal growth in neoplasia.
It is not clear exactly how much detail of the molecular events you need to know. The principles are
absolutes in that you must understand the cell cycle and signal methods (figs 4-2; 4-3), growth factors,
receptors and their types, transduction systems and transcription. You would be well advised to know of the
different types of cell surface receptors, as well as the common growth factors. A nodding acquaintance with
the cyclin system and apoptosis control would be wise.
The section on growth factors pp 97-98 and Table 4-1 is about right, but exquisite detail on what cytokine
controls precisely what ‘switch on, switch-off’ function is not required.
Extracellular Matrix and Matrix Interactions
This is becoming important in both healing and neoplasia.
The section in pp 98-102 is clear and requires no summary.
Repair by Connective Tissue
Repair follows injury and the sequence is:
(a) damage (necrosis, haematoma, abscess etc.);
(b) acute inflammation;
(c) demolition (macrophage influx and phagocytosis);
(d) Granulation tissue ingrowth (angiofibrogenesis) with fibrogenesis;
(e) matrix deposition (maximal collagen is laid down swiftly);
(f) remodelling (realignment of extracellular matrix – collagen, by removal of ‘haphazard’ matrix and
replacement along lines of stress – the amount of collagen does not increase; its strength does).
Ó Royal Australasian College of Surgeons – December 2000 Page 114 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
This same time sequence is seen, and the sequence reflected in the histology layering in – peptic ulcer;
abscess wall; haematoma; healing myocardial infarct etc.
The points to be familiar with are:
1. Angiogenesis and the likely mediators (growth, migration, tube formation etc).
2. Fibroplasia and the likely mediators
3. Remodelling and the likely mediators
Wound Healing
The healing process is identical in so-called primary and second intention.
The process is well described in Robbins except for wound contraction, which is an extremely important
phenomenon, dealt with briefly on p 109.
Local and Systemic Factors
· Nutrition
· Diabetes - both in the inflammation (neutrophil) defect and in blood supply problems
· Blood supply - age and / or diabetes mellitus
· Hormones
· Infection
· Foreign bodies, etc
Pathological Repair
Note the principles:
· Deficient scar
· Too much scar (keloid / hypertrophic scar)
· Contracture
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
Chapter 3, pages 79-87, See also specific disease references
Chapter 4
Ó Royal Australasian College of Surgeons – December 2000 Page 115 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 4.1
HAEMATEMESIS IN A 45-YEAR-OLD MAN
This 45-year-old man had experienced intermittent episodes of gnawing epigastric pain for many
years. The pain seemed to occur in bouts, with pain every day for a few weeks followed by many
months during which he was pain free. The pain typically came on 30 to 90 minutes after a meal
and was partially relieved by taking antacids or milk.
A year before admission he had a more prolonged bout with pain every day for a month. This had
occurred while he was on an rugby supporters’ tour of France. He had sprained his ankle and been
given a course of ibuprofen. On his return he saw his general practitioner who had referred him for
barium meal examination. He was given a course of ranitidine, stopped smoking and his symptoms
resolved.
In the ten weeks prior to admission to hospital, his symptoms recurred. He attributed this to stress
in his job in the ‘Human Resources Department’ of a large enterprise. He had also started smoking
again. On the evening of his admission he was watching TV when he suddenly felt faint and
vomited a large amount of bright red blood. An ambulance was called and he was taken to hospital.
On admission he was found to have a blood pressure of 80/50 mmHg and a pulse of 120/min.
Blood samples for urgent cross match and baseline laboratory data was taken and he was
resuscitated with IV fluids. An urgent gastroscopy showed continuing bleeding in the stomach.
Sclerotherapy was attempted but was unsuccessful. He was taken to the operating theatre and the
ulcer was oversewn. He had no further bleeding and made an uneventful recovery.
Ó Royal Australasian College of Surgeons – December 2000 Page 116 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 4.1
“Wherever they occur, chronic peptic ulcers have a fairly standard, virtually diagnostic gross and
microscopic appearance.” (Robbins)
1. What are the characteristic gross appearances and sites of chronic peptic ulcers in:
(a) the stomach?
(b) the duodenum?
2. What are the characteristic gross features of acute gastric ulcers?
3. How may Helicobacter pylori colonisation (previously Campylobacter pylori) lead to damage of gastric
mucosa?
4. Figure 4-1A shows the barium meal examination of the man in the clinical history.
(a) Describe/draw the features seen.
(b) What is your diagnosis? Explain your reasoning.
(c) Would there have been any advantage in investigating this man by endoscopy, rather than by a
barium meal at this time? Explain your reasoning.
Refer to Resource Unit General Principles of Pathology Figure 4-1A
http://www.bst.racs.edu.au/racs/servlet/disp/16497?
5. Figure 4-1B shows a partial gastrectomy specimen from a patient with the same history as the man in
the clinical history. Describe/draw the specimen and make a diagnosis of the changes seen in the ulcer
and the adjacent stomach.
Refer to Resource Unit General Principles of Pathology Figure 4-1B
http://www.bst.racs.edu.au/racs/servlet/disp/16498?
6. Figures 4-1C(i) shows the histology seen in a section taken through the ulcer. Figure
4-1C(ii) shows the histology of the ulcer base, and Figure 4-1C(iii) shows tissue just deep to the ulcer
base at higher magnification. Is this an acute or a chronic ulcer? Explain your reasoning.
Refer to Resource Unit General Principles of Pathology Figure 4-1C (I)
http://www.bst.racs.edu.au/racs/servlet/disp/16499?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-C (ii)
http://www.bst.racs.edu.au/racs/servlet/disp/16499?
Scroll down to thumbnails and select the appropriate image
Ó Royal Australasian College of Surgeons – December 2000 Page 117 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Refer to Resource Unit General Principles of Pathology Figure 4–C (iii)
http://www.bst.racs.edu.au/racs/servlet/disp/16499?
Scroll down to thumbnails and select the appropriate image
7. Histology slide Figure 4-1D shows a gastric biopsy.
(a) Describe the changes seen.
(b) What is your diagnosis?
(c) What is the relevance of this finding in a patient with a chronic peptic ulcer?
Refer to Resource Unit General Principles of Pathology Figure 4-1D
http://www.bst.racs.edu.au/racs/servlet/disp/16500?
8. (a) Describe/draw the appearances seen in Figures 4-1E and 4-1F.
(b) What is your diagnosis for each of Figures 4-1E and 4-1F? Explain your reasoning.
Refer to Resource Unit General Principles of Pathology Figure 4-1E
http://www.bst.racs.edu.au/racs/servlet/disp/16501?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-1F
http://www.bst.racs.edu.au/racs/servlet/disp/16501?
Scroll down to thumbnails and select the appropriate image
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 791-793, Gastritis
pages 486-490, Peptic ulcer
Ó Royal Australasian College of Surgeons – December 2000 Page 118 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 4.2
BLOODY DIARRHOEA IN A 39-YEAR-OLD WOMAN
This 39-year-old woman presented with an episode of bloody diarrhoea and anal pain. She had had
a previous episode six months ago, but had otherwise been in good health. Following hospital
admission for investigation, she was diagnosed as having proctitis and treated with topical steroids.
The condition did not respond to this treatment and over the next two years severe diarrhoea
persisted, with up to 8 to 10 loose bowel motions a day. Further treatment with systemic
prednisone, predsol enemas and azathioprine did not control the disease.
The patient developed severe lassitude and weight loss and suffered from intermittent arthralgia
involving the knees and ankles. Iritis recurred and cutaneous lesions of erythema nodosum
developed. The disease also involved the perineum with the development of numerous fissures
and fistulae.
Three and a half years after the initial development of the bowel symptoms, she presented with a
bowel obstruction requiring surgical treatment.
Ó Royal Australasian College of Surgeons – December 2000 Page 119 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 4.2
1. What is the differential diagnosis of bloody diarrhoea as given in this case? What is your preferred
diagnosis? Explain your reasoning.
2. What is the rationale of the therapy given for the bowel symptoms?
3. What is granulomatous chronic inflammation and how does it arise?
4. Figure 4-2A shows the barium enema of the patient in the clinical history. Describe the changes seen
and compare the abnormal with the normal zones of the colon visible.
Refer to Resource Unit General Principles of Pathology Figure 4-2A
http://www.bst.racs.edu.au/racs/servlet/disp/16506?
5. Figures 4-2B(i) and 4-2B(ii) are low and medium power photomicrographs from the colon of one patient,
while Figures 4-2C(i) and 4-2C(ii) are from another patient - one shows the type of changes seen in the
bowel of the patient in the clinical history and the other is from a patient with a similar history.
Photomicrographs 4-2C(ii) is high power of the arrowed area of Figure 4-2C(i).
(a) Describe the features seen.
(b) Discuss the findings in the sections under the headings:
i) types of inflammatory cells
ii) depth of involvement
iii) fissures
iv) crypt abscesses
v) granulomata
vi) pseudopolyps
vii) diagnosis
Refer to Resource Unit General Principles of Pathology Figure 4-2B(i)
http://www.bst.racs.edu.au/racs/servlet/disp/16507?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-2B(ii)
http://www.bst.racs.edu.au/racs/servlet/disp/16507?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-2C(i)
http://www.bst.racs.edu.au/racs/servlet/disp/16507?
Scroll down to thumbnails and select the appropriate image
Ó Royal Australasian College of Surgeons – December 2000 Page 120 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Refer to Resource Unit General Principles of Pathology Figure 4-2C(ii)
http://www.bst.racs.edu.au/racs/servlet/disp/16507?
Scroll down to thumbnails and select the appropriate image
6. Which histology slide shows the features you would expect to see in the bowel of the woman in the
clinical history in Case Scenario 4.2? Explain your reasoning.
7. Figures 4-2D and 4-2E show the corresponding gross appearances of the colon in each of the two
conditions seen in the photomicrographs (Figures 4-2B(i) and (ii); Figures 4-2C(i) and (ii)). Make a
diagnosis and explain your reasoning. The important difference between the two is in the distribution of
pathology along the bowel length and through the wall layers.
Refer to Resource Unit General Principles of Pathology Figure 4-2D
http://www.bst.racs.edu.au/racs/servlet/disp/16509?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-2E
http://www.bst.racs.edu.au/racs/servlet/disp/16509?
Scroll down to thumbnails and select the appropriate image
8. Summarise the characteristic gross and microscopic appearances seen in the two types of inflammatory
bowel disease you have seen in the tutorial.
9. Figure 4-2F shows an electronmicrograph of a chronic inflammatory cell. Identify the organelles
indicated by the labels a, b, c and d. What function do these perform in this cell?
Refer to Resource Unit General Principles of Pathology Figure 4-2F
http://www.bst.racs.edu.au/racs/servlet/disp/16624?
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 815-820, Inflammatory bowel disease – Ulcerative colitis and Crohn’s disease
pages 820-822, Ischaemic bowel disease
Ó Royal Australasian College of Surgeons – December 2000 Page 121 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 4.3
JOINT PAIN, FEVER AND STUPOR IN A 58-YEAR-OLD WOMAN
At the age of 22 years, this woman presented to her doctor with 6 week history of pain, tenderness
and swelling in the joints of both hands and feet. She had also noticed stiffness of these joints in
the morning, and said that it took over an hour some days for her to loosen up. She had been
feeling generally unwell for some weeks, with loss of appetite and poor energy. On examining her
joints, her doctor noted swelling, tenderness and some decreased movement in the proximal
interphalangeal, metacarpophalangeal and metatarsophalangeal joints.
Blood tests were taken. The blood screen result is shown below. Tests for rheumatoid factor
were strongly positive and she had a weakly positive test for anti-nuclear antibody. She was
initially treated with aspirin, with good relief of her symptoms.
The condition rapidly progressed however, and within a few years came to involve her wrists,
elbows, ankles and knees. She was severely affected by stiffness and pain in her joints and was
treated with anti-inflammatory drugs and steroids. A synovectomy was performed in the left knee
at age 42.
At age 52 her blood urea was noted on routine testing to be slightly raised and a urine test showed
proteinuria.
Her final hospital admission was at the age of 58. She was found in a confused state at home by
her daughter. Her daughter said that her mother had been off colour for the previous couple of
days and had complained that her ‘left knee was playing up again’. On admission, she was
stuporous and responding to painful stimuli but not commands. Her temperature was 39oC, pulse
95/min, respiratory rate 26/min and she was clinically dehydrated. Her left knee was hot and
markedly swollen. Aspiration of the knee joint yielded turbid fluid. Microscopy showed Gram
positive cocci and 80 x 106 /L leukocytes, predominantly neutrophils. Blood tests, including blood
cultures were taken and she was commenced on intravenous fluids and antibiotics. She
continued to deteriorate and died the next day.
Haematology - Blood Screen
Test Age 22 yrs Age 58 yrs Ref Range Units
Haemoglobin 110 108 115 - 165 g/L
Haematocrit 0.34 0.33 0.37 - 0.47
MCV 81 79 76 - 96 fL
MCH 28 26 27 - 32 pg
9
Platelets 360 440 150 - 400 x10 /L
9
Leucocytes 8.5 11.3 4.0 - 11.0 x10 /L
9
Metamyelocytes 0.6 x10 /L
9
Neutrophils 6.3 9.1 2.0 - 7.5 x10 /L
9
Lymphocytes 1.8 1.0 1.5 - 4.0 x10 /L
9
Monocytes 0.3 0.3 0.2 - 0.4 x10 /L
9
Eosinophils 0.1 0.3 0.04 - 0.4 x10 /L
ESR 45 120 mm/hr
Ó Royal Australasian College of Surgeons – December 2000 Page 122 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 4.3
1. What is rheumatoid factor and how may it be involved in the pathogenesis of rheumatoid arthritis?
2. List the mechanisms by which corticosteroid treatment may modify the effects of rheumatoid arthritis.
3. What are the undesirable effects of long term corticosteroid treatment on the body’s defences?
4. List the abnormalities in the bloodscreen of this woman just before her death. Explain the basis of these
changes.
5. Histology slides Figures 4-3A and 4-3B(i)(ii)(iii) show synovium from two patients. One shows the type
of changes seen in the synovectomy specimen of the patient in the clinical history. The other is from the
hip joint of a child with a 6-week history of a pain in the hip.
(a) Describe or draw the features seen in each.
(b) What is your diagnosis for each?
Refer to Resource Unit General Principles of Pathology Figure 4-3A
http://www.bst.racs.edu.au/racs/servlet/disp/16515?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-3B(i)
http://www.bst.racs.edu.au/racs/servlet/disp/16515?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-3B(ii)
http://www.bst.racs.edu.au/racs/servlet/disp/16515?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-3B(iii)
http://www.bst.racs.edu.au/racs/servlet/disp/16515?
Scroll down to thumbnails and select the appropriate image
A slide of normal histology is not available - it would show 1-4 layers of synovial cells overlying a
relatively thin layer of fibrovascular tissue in which there are occasional mononuclear cells - a few
macrophages and mast cells.
6. Explain the possible roles of the different cells present in the synovium of Figure 4-3A and 4-3B(i)-(iii) in
the pathogenesis of the condition seen in each.
Ó Royal Australasian College of Surgeons – December 2000 Page 123 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
7. Figure 4-3C shows the tibial surface of the right knee and the synovium from the right knee of the patient
in the clinical history.
(a) Describe the changes seen in each photograph (knee joint and synovium) and explain the
pathogenesis of the changes.
(b) It was noted that there had been increasing laxity of this joint on examination over the last 30 years.
What was the underlying pathologic basis of this?
Refer to Resource Unit General Principles of Pathology Figure 4-3C
http://www.bst.racs.edu.au/racs/servlet/disp/16517?
8. The histology slide Figure 4-3D shows a section of kidney taken at postmortem from the patient in the
clinical history.
(a) Describe the abnormalities seen and explain the abnormalities of the patient’s renal function as
noted in the history.
Refer to Resource Unit General Principles of Pathology Figure 4-3D
http://www.bst.racs.edu.au/racs/servlet/disp/16518?
Scroll down to thumbnails and select the appropriate image
(b) Photomicrograph set Figure 4-3E is a Congo red stain. What is the Congo red stain used to
demonstrate? What is the diagnosis?
Refer to Resource Unit General Principles of Pathology Figure 4-3E
http://www.bst.racs.edu.au/racs/servlet/disp/16518?
Scroll down to thumbnails and select the appropriate image
9. Draw a flow chart summarising the different factors that contributed to this woman's death.
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 211-216, Autoimmunity – mechanisms in autoimmune disease
pages 251-257, Amyloidosis
pages 1248-1251, Rheumatoid arthritis
pages 1253, Infectious arthritis
Ó Royal Australasian College of Surgeons – December 2000 Page 124 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 4.4
HEADACHE, VOMITING AND FEVER IN A 7-YEAR-OLD GIRL
This 7-year-old girl developed persisting severe headache and attacks of recurrent vomiting,
becoming febrile after having had these symptoms for a couple of weeks. She had complained
repeatedly of tiredness, and her mother had noted her to be apathetic and to have a decreased
appetite. Her mother also said that the child had had the flu about one month earlier.
She became delirious and was admitted to hospital where she was described as being dehydrated
with a pulse rate of 50. Her temperature was normal. She was irritable, photophobic and had
fluctuating drowsiness. Minimal neck stiffness was present and Kernig’s sign was positive. She
was able to move all four limbs voluntarily. The plantar responses were flexor. The optic fundi
showed mild papilloedema.
A lumbar puncture was performed soon after admission. Antibiotic therapy for an acute bacterial
meningitis was commenced together with a regime to prevent cerebral swelling. Over the following
two days she developed signs of a divergent squint and right pupillary dilatation, which did not
respond well to light, right sided weakness and a right extensor plantar response. Two further
lumbar punctures were performed.
She continued to deteriorate, developed a fever and suffered two grand-mal type seizures. Her
respirations were slow and irregular and on her fourth hospital she died following the development
of respiratory failure.
Haematology - Blood Screen
Test Admission Ref - range Units
Haemoglobin 122 115 - 165 g/L
MCV 79 76 - 96 fL
9
Leucocytes 9.4 4.0 - 11.0 x10 /L
9
Neutrophils 6.9 2.0 - 7.5 x10 /L
9
Lymphocytes 1.8 1.5 - 4.0 x10 /L
9
Monocytes 0.3 0.2 - 0.4 x10 /L
9
Eosinophils 0.3 0.04 - 0.4 x10 /L
ESR 91 4-7 mm/hr
Ó Royal Australasian College of Surgeons – December 2000 Page 125 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CSF Results
CSF Chemistry 1 2 3 Ref Range
Total protein 1.2 1.0 0.4 0.2 - 0.4 g/L
Glucose 0.8 0.2 0.5 2.2 - 4.4 mmol/L
CSF Microbiology
WBC 32 35 87 0 - 6 / ml
WBC differential 90% lymphocytes All mononuclears
RBC 0 0 245 0
Gram stain No organisms No organisms No organisms
Culture No growth No growth No growth
Other ZN stain negative
Ó Royal Australasian College of Surgeons – December 2000 Page 126 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 4.4
1. Explain the cerebrospinal fluid and blood screen laboratory results.
2. What organ was initially involved in this case? What other organs may be involved and how do they
become involved?
3. What is granulomatous chronic inflammation and how does it arise?
4. Histology slides Figures 4-4A and 4-4B are from two different patients. One slide shows the changes
seen in the patient in the clinical history.
(a) Describe what you see.
(b) Make a diagnosis and indicate which is from the patient in Case Scenario 4.4.
Refer to Resource Unit General Principles of Pathology Figure 4-4A
http://www.bst.racs.edu.au/racs/servlet/disp/16524?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-4B
http://www.bst.racs.edu.au/racs/servlet/disp/16524?
Scroll down to thumbnails and select the appropriate image
Figures 4-4C and 4-4D each correspond to one of the photomicrographs. Match these with the
histology slides and indicate which pair correlate best with the clinical history.
Refer to Resource Unit General Principles of Pathology Figure 4-4C
http://www.bst.racs.edu.au/racs/servlet/disp/16524?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-4D
http://www.bst.racs.edu.au/racs/servlet/disp/16524?
Scroll down to thumbnails and select the appropriate image
Ó Royal Australasian College of Surgeons – December 2000 Page 127 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
5. Figure 4-4E shows the chest x-ray of this patient. Describe the changes seen. Figure 4-4E[normal] is a
normal chest x-ray for comparison.
Refer to Resource Unit General Principles of Pathology Figure 4-4E
http://www.bst.racs.edu.au/racs/servlet/disp/16525?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-4E[normal]
http://www.bst.racs.edu.au/racs/servlet/disp/16525?
Scroll down to thumbnails and select the appropriate image
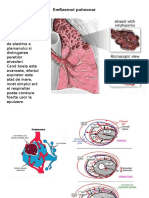
6. (a) Describe/draw the appearances of the lungs seen in Figures 4-4F and 4-4G.
(b) Which shows the type of changes you would expect to see in the patient in the clinical history?
Explain your reasoning.
(c) What is the diagnosis for each?
(d) Describe the pathogenesis and development for each.
Refer to Resource Unit General Principles of Pathology Figure 4-4F
http://www.bst.racs.edu.au/racs/servlet/disp/16526?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-4G
http://www.bst.racs.edu.au/racs/servlet/disp/16526?
Scroll down to thumbnails and select the appropriate image
7. Describe/draw the changes seen in Figures 4-4H(i) and 4-4H(ii) (high magnification). Explain the
pathogenesis of the changes.
Refer to Resource Unit General Principles of Pathology Figure 4-4H(i)
http://www.bst.racs.edu.au/racs/servlet/disp/16527?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-4H(ii)
http://www.bst.racs.edu.au/racs/servlet/disp/16527?
Scroll down to thumbnails and select the appropriate image
Ó Royal Australasian College of Surgeons – December 2000 Page 128 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 83-84, Granulomatous inflammation
pages 349-352, Tuberculosis
pages 1316-1317, Tuberculous mengitis
Ó Royal Australasian College of Surgeons – December 2000 Page 129 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 4.5
RENAL FAILURE IN A 61-YEAR-OLD MAN
A 61-year-old man was admitted to hospital for investigation of progressive renal failure, discovered
incidentally when his blood urea and creatinine were found to be mildly raised three months
previously during a routine follow-up investigation during ongoing treatment for hypertension, found
eight years previously.
On physical examination his pulse rate was 88/minute and regular, blood pressure was 200/100
mmHg, there was mild ankle oedema and crepitations in both lung fields. A chest X-ray confirmed
the enlarged heart and early evidence of pulmonary oedema. Autoantibody screening tests were all
negative. Laboratory tests were as follows:
Blood screen
Test Result Normal range Units
Haemoglobin 83 130-165 g/L
Total leukocytes 13.0 4.0-11.0 x109/L
Metamyelocytes 0.8 0 x109/L
Neutrophils 9.3 4.0-7.5 x109/L
lymphocytes 1.9 1.5-4.0 x109/L
Monocytes 1.0 0.2-0.4 x109/L
Sedimentation rate 136 4-7 mm in 1hr
Electrolytes
Urea 26.3 4.6-6.8 mmol/L
Creatinine 240 50-110 mmol/L
Ó Royal Australasian College of Surgeons – December 2000 Page 130 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Needle biopsy of his kidney showed histological features of severe glomerulonephritis with
extensive and apparently progressive kidney damage; immunofluorescent studies showed the
pattern seen in Figure 4-5A.
Because of the severity of the kidney damage, it was decided to attempt to reduce this by treating
the patient with very high dose immunosuppression (corticosteroids plus cyclophosphamide), and
his high blood pressure was also treated.
His renal function stabilised, but less than six weeks later he was having fever, rigors, and severe
shortness of breath, but no pain. A diagnosis of pulmonary embolism was made, and he was
readmitted, treated with anticoagulants and antibiotics, improved and was sent home. Treatment
with high dose immune suppressant therapy was continued, but a further six weeks later, severe
breathlessness recurred requiring his admission to hospital and oxygen therapy because of severe
hypoxaemia.
Chest x-ray at this time showed irregular consolidation of both lung fields. His renal function had
deteriorated only slightly, but by this time his haemoglobin had fallen to 75 g/l and his total leukocyte
count was 3.3x109/L, with 55% neutrophils. Repeated sputum examinations did not yield any
pathogenic organisms, but it was assumed that he had a pulmonary infection. He refused to have a
needle biopsy of his lung to confirm this. Despite use of artificial ventilation and antiprotozoal drugs,
his condition continued to deteriorate and he died with progressive respiratory failure.
This patient did not have HIV infection.
Ó Royal Australasian College of Surgeons – December 2000 Page 131 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 4.5
1. What was the likely pathogenesis of this man's glomerulonephritis?
2. Figure 4-5A is a photomicrograph of an immunofluorescent study of a glomerulus giving a linear
capillary wall staining for the presence of IgG (ie anti-IgG-antibody stain), and the same pattern was seen
for complement components C1q and C3c.
(a) What type of immunopathology does this indicate?
(b) What is the likely disease process?
Refer to Resource Unit General Principles of Pathology Figure 4-5A
http://www.bst.racs.edu.au/racs/servlet/disp/16530?
3. What could be the justification for using such dangerous immune suppressant treatment in this patient?
4. (a) What lung infection do you think that the medical team assumed this man to have?
(b) Why would the medical team have wanted to do a lung biopsy? Surely this is a bit radical to use as a
routine diagnostic technique for pulmonary infections!
5. Figure 4-5B is a photomicrograph of an HE stain of his lung biopsy; the capillary walls are readily
identified as well as foamy, granular material in alveolar spaces. Figure 4-5B[silver] is a Grocott-
Gomori methenamine silver stain at about double magnification of the HE figure. Fungi stain black with
GGMS. What is the organism and what is its significance?
Refer to Resource Unit General Principles of Pathology Figure 4-5B
http://www.bst.racs.edu.au/racs/servlet/disp/16533?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 4-5B[silver]
http://www.bst.racs.edu.au/racs/servlet/disp/16533?
Scroll down to thumbnails and select the appropriate image
6. What other lung infections would this man be particularly susceptible to?
7. (a) What risk factors did this man have for the development of the infection which you suggest?
(b) How do these risk factors cause the increased susceptibility to infection?
Ó Royal Australasian College of Surgeons – December 2000 Page 132 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 381-382, Pneumocystis pneumonia (note also in this section, other ‘opportunistic’ organisms
active in the immunocompromised individual)
Ó Royal Australasian College of Surgeons – December 2000 Page 133 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
MULTIPLE CHOICE QUESTIONS
TYPE X (MULTIPLE TRUE-FALSE)
Q1 Chronic colitis is more likely to be due to Crohn disease if
1. epithelial cell dysplasia is present out of proportion to the degree of inflammation in that area of
mucosa
2. submucosal oedema and lymphocytic infiltrate are prominent
3. multiple biopsies show progressive distal increase in mucosal disease severity
4. colonoscopic biopsy shows focal epithelioid cell granulomas
Q2 Granulomatous inflammation may be composed of
1. a compact mass of immature granulation tissue
2. a compact mass of lymphocytes and plasma cells
3. a mass of macrophages and giant cells
4. a mass of epithelioid cells and giant cells
TYPE B (RELATIONSHIP-ANALYSIS)
Q3 Epithelial metaplasia in considered to be an adaptive response to a change in the cell environment
because
epithelial metaplasia does not revert to normal morphology following cessation of the causal injury
TYPE X (MULTIPLE TRUE-FALSE)
Q4 Fibroblasts proliferate and migrate during the healing process in response to the direct action of
1. cytokines
2. expression of adhesion molecules on endothelial cells
3. leukotrienes
4. platelet activating factor (PAF)
Q5 Myofibroblasts in granulation tissue
1. cause wound contraction
2. contain contractile cytoplasmic filaments
3. secrete collagen
4. develop from fibroblast progenitor cells
Ó Royal Australasian College of Surgeons – December 2000 Page 134 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Q6 New blood vessel formation (angiogenesis) is a feature of
1. chronic inflammation
2. metastatic spread of cancer
3. tuberculous granuloma formation
4. pulmonary silicosis
Q7 Resolution of inflammation and regeneration lead to complete restoration of normal structure and
function following healing of
1. renal papillary necrosis
2. acute viral hepatitis
3. hypovolaemic acute renal tubular necrosis
4. liver abscess
Ó Royal Australasian College of Surgeons – December 2000 Page 135 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Answers and Commentaries
A1 Chronic colitis is more likely to be due to Crohn disease if
1. epithelial cell dysplasia is present out of proportion to the degree of inflammation in that area of
mucosa
2. submucosal oedema and lymphocytic infiltrate are prominent
3. multiple biopsies show progressive distal increase in mucosal disease severity
4. colonoscopic biopsy shows focal epithelioid cell granulomas
2, 4 True; 1 3 False
Non-inflammatory epithelial dysplasia is said to be the hallmark of developing carcinoma in long-
standing active ulcerative colitis - cancer incidence is probably increased in all long-standing IBD, but
this is disproportionately so in UC. Mucosal inflammation is present in involved zones in both UC and
Crohn disease and there may be some superficial submucosal lymphocytic infiltration in UC, but
prominent submucosal lymphocytic infiltration and oedema are strong hallmarks of Crohn disease.
Crohn's disease is random and discontinuous; UC involvement is progressively distally severe.
Granulomas are regarded as a virtually pathognomonic diagnostic feature of Crohn disease.
A2 Granulomatous inflammation may be composed of
1. a compact mass of immature granulation tissue
2. a compact mass of lymphocytes and plasma cells
3. a mass of macrophages and giant cells
4. a mass of epithelioid cells and giant cells
3, 4 True; 1, 2 False
The clear distinction between epithelioid cells and macrophages and the clear implications of their
different morphologies and functions is poorly dealt with in Robbins. Nevertheless, at least the book
makes it clear that there are both innate (non-immune - characterised by macrophages, ie. phagocytic)
and immune (characterised by epithelioid cells - which are not phagocytic, but are synthetic and
secretory and probably also fulfil a ‘barrier’ function before fibrosis). Granulomas are not composed of
granulation tissue, not primarily made up of immunocytes (lymphocytes and plasma cells), though both
may be present.
Ó Royal Australasian College of Surgeons – December 2000 Page 136 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A3 Epithelial metaplasia in considered to be an adaptive response to a change in the cell
environment because epithelial metaplasia does not revert to normal morphology following cessation of
the causal injury.
Answer: C (Correct - Incorrect)
Metaplasia is an adaptive response to chronic cell injury. Moreover, influences predisposing to such
metaplasia, if persistent, may induce cancerous transformation in the metaplastic epithelium.
Metaplasia is thought to be caused by the environmental change inducing, in differentiating progeny of
‘stem cells’, expression of different genes, thus resulting in a different phenotypic expression (ie a
different adult cell). With removal of the environmental injury, metaplastic cells die off and the stem
cells regenerate under the now normal environmental situation - usually back to normal.
A4 Fibroblasts proliferate and migrate during the healing process in response to the direct action of
1. cytokines
2. expression of adhesion molecules on endothelial cells
3. leukotrienes
4. platelet activating factor (PAF)
1 True; 2, 3, 4 False
Fibroblast proliferation and differentiation appears to be largely under the control of growth-promoting
and growth-controlling cytokines. The influence of other factors such as extracellular matrix products
(particularly fibronectin, laminin, etc and fibrino-peptides), although persuasive, is still equivocal. The
endothelial adhesion molecules include members of the immunoglobulin family of proteins - they have
no known influence on fibroblast ( or other ECM cell ) activity and the same goes for the two cell
membrane phospholipid derivatives LT and PAF.
A5 Myofibroblasts in granulation tissue
1. cause wound contraction
2. contain contractile cytoplasmic filaments
3. secrete collagen
4. develop from fibroblast progenitor cells
1, 2, 3, 4 True
Myofibroblasts are important cells in wound healing and variants of this (chronic inflammation, tumour
fibroplasia etc). In all of these , ‘wound contraction’ leads to a scar which, in uncomplicated healing, is
smaller than the original tissue it replaces; in other circumstances, this leads to such problems as
bowel obstruction in cancer, Crohn disease etc. All of the suggested functions and the cell origin are
true. ‘Wound contraction’ is common and important - that message does not come through clearly in
Ó Royal Australasian College of Surgeons – December 2000 Page 137 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Robbins, but the gist of the phenomenon and its importance is clear - where there is granulation tissue,
there is wound contraction, occurring early in connective tissue healing.
A6 New blood vessel formation (angiogenesis) is a feature of
1. chronic inflammation
2. metastatic spread of cancer
3. tuberculous granuloma formation
4. pulmonary silicosis
1, 2 True; 3, 4 False
Chronic inflammation is a continuing attempted healing which never completes itself unless/until the
damaging agent is removed. Continuous granulating scar formation is characteristic of this process - ie.
angiogenesis. Likewise, metastatic cancer foci can not establish a separate existence without
establishing a microvasculature for supply of nutrients, including oxygen.
Tubercles and silicotic nodules are generally described as 'avascular' - this may or may not be
absolutely true but overt granulation tissue formation with angiogenesis is not a feature of either.
A7 Resolution of inflammation and regeneration lead to complete restoration of normal structure and
function following healing of
1. renal papillary necrosis
2. acute viral hepatitis
3. hypovolaemic acute renal tubular necrosis
4. liver abscess
2, 3 True; 1, 4 False
Renal papillary necrosis and liver abscess both result in total destruction of the ‘framework’ of the tissue
involved - healing by scarring is the best possible outcome here. In acute viral hepatitis (apoptotic cell
death, not necrosis), cells regenerate along the intact basement membrane framework as they also do
following acute renal tubular necrosis. Although oliguric renal failure caused by hypovolaemic shock is
a hazardous disorder, when recovery occurs without complications (eg infection etc), eventual complete
restoration of ‘pre-injury’ renal structure and function occurs.
Ó Royal Australasian College of Surgeons – December 2000 Page 138 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
TOPIC 5: NEOPLASIA
SUMMARY OF CASE SCENARIOS
5.1 BACK PAIN AND SMOKER’S COUGH IN A 62-YEAR-OLD MAN ........................................................ 145
5.2 ABNORMAL CERVICAL SMEAR IN A 51-YEAR-OLD WOMAN ........................................................... 149
5.3 HEADACHE AND TIREDNESS IN A 39-YEAR-OLD MAN .................................................................... 153
5.4 A 44-YEAR-OLD MAN WITH MALIGNANT MELANOMA ...................................................................... 157
5.5 RECURRENT ABDOMINAL PAIN IN A 60-YEAR-OLD MAN ................................................................ 160
5.6 TIREDNESS AND PALLOR IN A 55-YEAR-OLD WOMAN.................................................................... 163
Ó Royal Australasian College of Surgeons – December 2000 Page 139 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
NEOPLASIA
GOALS AND OBJECTIVES
At the end of this topic you should be able to demonstrate an understanding of:
· characteristics of benign and malignant neoplasms including: their general gross and microscopic
appearances and their biological behaviour, growth and methods of spread including expansion,
invasion and metastasis;
· the basis of classification of neoplasms according to their differentiation, the relationship of
morphological characteristics to likely behaviour and the implications of these characteristics in regard to
the likely biology and response to therapy;
· the molecular basis of neoplasia, genetic and environmental causes of neoplasms and the basis of
progressive aggression of malignant neoplasms which reflects their acquired genetic instability;
· the progressive and multi-step nature of neoplastic induction and progression, and how this is reflected
in the nature of 'precancer' and precancerous conditions;
· the growth cycle, the molecular basis for this and the mediation and modulation of cell growth through
ligand-receptor interactions; how these normal interactions are disorganised in neoplasia, and how the
factors co-ordinating normal cell growth (both DNA and protein/polypeptide 'growth factors') engage
inappropriately in neoplastic growth mediation; this includes factors influencing the progressive and
relentlessly increasing mass of neoplastic tissue and its invasive and destructive biology;
· the range of possible clinical effects and complications of neoplasms on the host, including those effects
which are predictable as well as those related to tumour secretions producing systemic effects such as
cachexia, and paraneoplastic syndromes;
· morphological and behavioural characteristics of common and clinically important neoplasms including
prognosis, principles of treatment, the laboratory manifestations and investigations of neoplasms
(particularly lung; breast; large bowel; prostate; solar skin cancers);
· examples of malignancies associated with known premalignant lesions, and current techniques for the
early detection and treatment of such lesions.
· examples of malignancies in which radiation, chemicals or viruses are thought to be aetiologically
implicated.
Ó Royal Australasian College of Surgeons – December 2000 Page 140 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
Chapter 8, pages 260-325, Neoplasia
pages 650-686, Lymphomas and leukaemias
pages 741-749, Lung tumours (also pages 751-752 – mesothelioma)
pages 769-773, Salivary gland tumours
pages 783-787; 798-801; 826-838, Oesophagus; Stomach; Small and large intestine
pages 899-900; 910-911, Gallbladder and bile ducts; Pancreas
pages 991-994; 1003-1008, Kidney; Urothelial neoplasms
pages 1017-1024; 1029-1033, Testis; Prostate
pages 1048-1053; 1102-1117, Cervix; Breast
pages 1140-1147; 1166-1167, Thyroid; Multiple endocrine neoplasia
pages 1174-1179; 1184-1188, Naevi and melanoma; Epidermal tumours
pages 1236-1237, Osteosarcoma
pages 1343-1345; 1350-1351; 1354, Glioma; Meningioma; Neurofibromatosis
Ó Royal Australasian College of Surgeons – December 2000 Page 141 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
REFERENCE SUBSECTION
th
Robbins Pathologic Basis of Disease, 6 Ed, Chapters 8, 12, 13, 16.
Neoplasia
1. Introduction
· This is standard material, but it is important and worth your thorough understanding
pages 260-276.
· Molecular basis of cancer, summary Figure 8-36, page 299.
· Non-lethal genetic damage, inherited and/or acquired Figure 8-24, page 278.
· Multistep process involving aberrations of both growth-promoting and growth-suppressing genes.
2. Oncogenes and Cancer (‘dominant’)
Oncogenesis is growth induction by abnormal activation of a (normal) proto-oncogene. Just as proto-
oncogenes encode normal growth proteins, oncogenes encode growth factors which are
uncontrolled; or encodement may be for a growth factor receptor, either through mutation or
overexpression.
The oncogene may encode for a signal-transducing protein (‘intracellular messenger’). Encodement
may be for nuclear transcription proteins which control mitosis.
PROTO-ONCOGENES CELLULAR ONCOGENES (cancer) Example
(normal)
Growth factor synthesis Continuous autocrine GF stimulus sis/PDGF
GF receptor synthesis Defective receptor erb-B1/EGF receptor
(mimics continuous stimulus)
Cytoplasmic messenger Defective message ras/GTP binding
synthesis (mimics continuous stimulus)
Nuclear protein synthesis Abnormal 'competence' / 'progress' stimulus myc (N-myc, L-myc)
Cell cycle regulators Cyclins and cyclin-dependent kinases Cyclin D/CDK4
Activation of oncogenes:
· Point mutation (activates oncogene, or removes control mechanisms)
· Chromosome rearrangement (oncogene near stimulator or distant from control)
· Gene amplification
Ó Royal Australasian College of Surgeons – December 2000 Page 142 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
3. Cancer Suppressor Genes (‘recessive’)
· Rb gene
· p53 gene - very common mutation in human cancers. Involved in mitosis arrest (DNA repair) – also
in apoptosis (later)
· APC gene - germline mutation in one gene Þ FAP/colon cancer
· BRCA-1 and BRCA-2 mutations common in familial breast cancer
· NF-1 gene mutation Þ neurofibromatosis, type 1 (and AML)
· Tumour suppressor function in signal transduction, regulation of cell surface receptor function
4. Genes Regulating Apoptosis
Successful outcome following potentially oncogenic DNA mutation in a cell involves mitosis arrest
allowing time for DNA repair and if this is unsuccessful, destruction of the cell through induction of
apoptosis (‘benevolent suicide’).
Within this system there are:
· Gene products which inhibit apoptosis (pro-cancer in some circumstance – bcl-2)
· Gene products favouring apoptosis – bax; bad etc. p53 influences apoptosis (promoting it) by
up-regulating bax
5. Genes Regulating DNA Repair
Examples:
· Xeroderma pigmentosum (premature skin cancers of all types)
· Hereditary non-polyposis colon cancer (HNPCC)
· Ataxia telangiectasia
6. Telomeres and Cancer
Interesting, but no hard data and nothing to ask
7. Molecular Basis of Multistep Carcinogenesis
See Figure 8-24, page 278 and Figure 8-34, page 297
8. Biology of Tumour Growth
Kinetics - The theory is OK, but there are no clear rules and ‘excess of cell production over cell loss’
9. Tumour Angiogenesis
Ó Royal Australasian College of Surgeons – December 2000 Page 143 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
10. Tumour Progression and Tumour Heterogeneity
Tumour progression results from genetic instability of the neoplastic cells, which results in
permanent, irreversible, qualitative change. Subset survival depends on innate and immune host
reactions to each subset, which favour the 'survivors' - generally biologically aggressive cells.
11. Invasion and Metastasis
This is elegantly described and illustrated in Robbins, pages 302-305. Chemicals that attach neoplastic
cells to matrix components or degrade matrix, favour metastasis.
12. Carcinogenic Agents
· Chemical
· Radiation
· Viral and microbial
This is elegantly described and illustrated in Robbins, pages 305-315.
13. Host defence – Tumour Immunity
The best defence is mutation recognition, mitosis arrest, DNA repair or apoptosis. It only gets this far if
these mechanisms fail. Elegant summary – Figures 8-45; 8-46, pages 316 and 318.
14. Clinical Features - Important Concepts
· Local and hormonal effects
· It only gets to involve immune defences if mutation recognition and repair (or apoptosis) fail
· Paraneoplastic syndromes endocrine, osteoarthropathy, venous thrombosis
15. Grading and Staging
16. Laboratory Diagnosis
Specific Neoplasms
See references
Ó Royal Australasian College of Surgeons – December 2000 Page 144 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 5.1
BACK PAIN AND SMOKER’S COUGH IN A 62-YEAR-OLD MAN
This 62-year-old man was admitted to hospital with a one month history of thoracic back pain. The
pain was continuous and throbbing and was made worse by coughing. It dated from an accident
when he had fallen backwards and landed on his back and shoulders. Recently he had also noted
increasing cough. He had a longstanding smoker’s cough, having been a smoker for 40 years. On
a few occasions in the previous month there had been some blood in his sputum.
He also said that he had felt generally unwell with persisting tiredness and weakness for the last
two months. He had lost his appetite and had noted a recent weight loss of 5 or 6 kilos.
On examination there was marked tenderness over the 7th and 9th thoracic vertebrae.
Radiographs showed compression fractures of the 7th and 9th thoracic vertebrae. A chest x-ray
showed a mass in the right hilar region. The striking abnormality on his blood tests was marked
hypercalcaemia.
Treatment with intravenous fluids, frusemide and corticosteroids was started for his
hypercalcaemia. A bronchoscopy was performed and a mass was seen in a right upper lobe
bronchus. Cytology and histology samples were taken.
As a result of treatment his serum calcium slowly decreased. He was referred for radiotherapy. A
day before he was due to start radiotherapy he developed a fever and a productive cough.
Treatment with AugmentinÒ was started with some improvement, however he was found dead in
bed two days later.
Ó Royal Australasian College of Surgeons – December 2000 Page 145 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 5.1
1. What is the evidence for a positive relationship between tobacco smoking and lung cancer?
2. What does the ‘differentiation’ of a tumour refer to?
3. What secondary pathologies may be seen in the lung as complications of lung cancer?
4. List the commoner ‘paraneoplastic syndromes’ that may be seen in patients with lung cancer.
5. What factors may be contributing to the hypercalcaemia in this man?
Ó Royal Australasian College of Surgeons – December 2000 Page 146 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
6. Figure 5-1A shows similar changes to those seen at autopsy in the lung of the patient in the clinical
history.
(a) Describe/draw what you see.
(b) Make a diagnosis for each of the changes.
(c) Explain the pathogenesis of each diagnosis.
Refer to Resource Unit General Principles of Pathology Figure 5-1A
http://www.bst.racs.edu.au/racs/servlet/disp/16548?
7. Figure 5-1B shows the left upper and lingula lobectomy specimen of a patient who had surgery following
investigation for an unresolving right middle lobe pneumonia.
(a) Describe/draw what you see.
(b) Make a diagnosis for each of the changes.
(c) Explain the pathogenesis of each diagnosis.
Refer to Resource Unit General Principles of Pathology Figure 5-1B
http://www.bst.racs.edu.au/racs/servlet/disp/16549?
8. Figure 5-1C shows the cytology sample taken at bronchoscopy of the patient in the clinical history.
There are both abnormal cells and normal bronchial epithelium provided for comparison.
(a) Describe the cells in Figure 5-1C.
(b) What is your diagnosis? Explain your reasoning.
Refer to Resource Unit General Principles of Pathology Figure 5-1C
http://www.bst.racs.edu.au/racs/servlet/disp/16550?
Ó Royal Australasian College of Surgeons – December 2000 Page 147 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
9. Photomicrograph Figures 5-1D and 5-1E are from different patients. One slide shows the type of
tumour seen in the patient in the clinical history and also in the resected lung seen in Figure 5-1B. The
other slide shows a primary lung tumour in another patient who was treated with chemotherapy and who
died a year later.
(a) Describe the tumour in each slide and make a diagnosis.
(b) Note other pathology in these lungs.
(c) Match the tumour types to the patients
(d) Note the type of treatment instituted in each tumour case.
Refer to Resource Unit General Principles of Pathology Figure 5-1D
http://www.bst.racs.edu.au/racs/servlet/disp/16551?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-1E
http://www.bst.racs.edu.au/racs/servlet/disp/16551?
Scroll down to thumbnails and select the appropriate image
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 741-749, Lung tumours
pages 264-268, Benign & malignant tumours – Table 8.2
pages 269-271, Pathways of spread
pages 302-305, Mechanisms of invasion and metastasis
pages 305-309, Mechanisms in carcinogenesis – chemical carcinogenesis (summary page 307)
pages 319-321, Effects of tumour on host
Ó Royal Australasian College of Surgeons – December 2000 Page 148 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 5.2
ABNORMAL CERVICAL SMEAR IN A 51-YEAR-OLD WOMAN
At the age of 30 this woman had her first cervical smear, which was normal. A repeat smear one
year later and a routine smear three years after that were also normal. She did not have another
smear until she consulted her doctor about perimenopausal symptoms at the age of 51 years. At
the time of taking the smear her doctor noted that the cervix appeared healthy to visual inspection.
The smear was reported as showing:
" ... a high grade squamous intraepithelial lesion. Abnormal squamous epithelial cells
are present indicating a lesion in the severe dysplasia/carcinoma in situ class (CIN 3),
with coexisting wart virus (HPV) infection ..."
At colposcopy, a large intraepithelial lesion with features of CIN 3 was seen extending almost
circumferentially around the transformation zone. Multiple biopsies were taken which confirmed a
high grade squamous intraepithelial lesion with features of CIN 3. Changes of HPV infection were
also seen in the squamous epithelium. There was no evidence of invasion in the biopsies.
Due to domestic problems, she suddenly moved overseas and was lost to follow-up. Five years
later, having returned to Australia, she consulted her doctor about postcoital bleeding that she had
noticed for the previous six weeks. Inspection of the cervix showed an ulcerated tumour. She was
immediately referred to a gynaecologist who took a cervical biopsy. On the basis of the biopsy
result and the findings on further clinical workup this woman underwent a course of radiotherapy
and then had a total hysterectomy and pelvic lymphadenectomy.
Ó Royal Australasian College of Surgeons – December 2000 Page 149 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 5.2
1. What is cervical intraepithelial neoplasia (CIN)?
2. What is the relationship of CIN to invasive cervical cancer?
3. What are known risk factors for cervical cancer?
4. What agents are thought to be involved in the pathogenesis of cervical cancer, and what are the
postulated mechanisms of their action?
5. Describe ways to reduce the incidence of invasive cervical cancer in Australasia.
6. Histology slides Figures 5-2A and 5-2B the type of changes seen in the two biopsies, taken five years
apart, from cervix of the woman in the clinical history. Describe the changes seen in each under the
headings below and make a diagnosis:
(a) Surface epithelium:
i) nuclei
ii) mitosis
iii) ration of nuclear to cytoplasmic area (N:C ratio)
iv) organisation and maturation of cells
(b) Invasion
Refer to Resource Unit General Principles of Pathology Figure 5-2A
http://www.bst.racs.edu.au/racs/servlet/disp/16985?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-2B
http://www.bst.racs.edu.au/racs/servlet/disp/16985?
Scroll down to thumbnails and select the appropriate image
7. (a) What is the treatment for the lesion seen in Figure 5-2A, and what is the rationale for this
treatment?
(b) How may this type of lesion be detected, other than by biopsy?
Ó Royal Australasian College of Surgeons – December 2000 Page 150 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
8. Figures 5-2C and 5-2D show representative areas from routine cervical smears from two women. Both
smears show an intraepithelial lesion. Neither woman had had a previous abnormal smear. Normal
squamous epithelial cells as well as abnormal squamous cells are seen in each.
(a) Describe the abnormal cells.
(b) What would you advise each of these women?
Refer to Resource Unit General Principles of Pathology Figure 5-2C
http://www.bst.racs.edu.au/racs/servlet/disp/16990?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-2D
http://www.bst.racs.edu.au/racs/servlet/disp/16990?
Scroll down to thumbnails and select the appropriate image
9. Figure 5-2E shows the uterus, kidneys and lower aorta of a 53-year-old woman who died of renal failure.
She had been treated with radiotherapy for a squamous cell carcinoma of the cervix. At autopsy an
occlusive thrombus was found at the origin of the left renal artery.
(a) Describe the changes seen in the right kidney and explain the likely pathogenesis of the changes
(photograph is orientated so right kidney is on the right side of the photograph).
Refer to Resource Unit General Principles of Pathology Figure 5-2E
http://www.bst.racs.edu.au/racs/servlet/disp/16993?
(b) Describe other complications of advanced invasive cervical carcinoma that are not seen in this
photograph.
This woman had had a single previous cervical smear 13 years before her death, which had been
reported as showing no abnormal cells. The smear showed much fresh blood, as it had been taken at
the time of withdrawal bleeding following cessation of oral contraceptives. On review 13 years later it
was thought that there were small numbers of abnormal cells obscured by the blood, that probably
represented CIN.
(c) List ways to try and prevent the tragic outcome seen in this woman.
10. Figures 5-2F and 5-2G show uterus and cervix from two hysterectomies. Match the appearances of
each cervix (allowing for different specimen preparation) with histology Figures 5-2A or 5-2B and
corresponding cytology Figures 5-2C or 5-2D. Figure 5-2G also shows multiple small tumours of
smooth muscle in the body of the uterus. Figures 5-2H and 5-2I show two smooth muscle tumours.
Describe each of these and make a diagnosis for each.
Ó Royal Australasian College of Surgeons – December 2000 Page 151 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Refer to Resource Unit General Principles of Pathology Figure 5-2F
http://www.bst.racs.edu.au/racs/servlet/disp/16995?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-2G
http://www.bst.racs.edu.au/racs/servlet/disp/16995?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-2H
http://www.bst.racs.edu.au/racs/servlet/disp/16995?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-2I
http://www.bst.racs.edu.au/racs/servlet/disp/16995?
Scroll down to thumbnails and select the appropriate image
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 311-315, Viral and microbial carcinogenesis
pages 1048-1053, Intraepithelial and invasive cervical squamous-neoplasia
Ó Royal Australasian College of Surgeons – December 2000 Page 152 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 5.3
HEADACHE AND TIREDNESS IN A 39-YEAR-OLD MAN
This 39-year-old farmer consulted his GP with a history of six months of tiredness, weakness
and persisting headache. He had previously been in good health and had not seen his doctor
for over five years. His GP noted a 7 kg weight gain since the patient’s previous visit. He also
thought that there had been a change, other than just aging, in the patient’s appearance - he
remembered the patient well as they had played rugby together some years previously.
On examination the patient appeared fit and strongly built. He was sweating, despite the
coolness of the surgery, and had a blood pressure of 150/100 mm Hg. Nothing else was noted
on physical examination. His blood pressure was checked after a further 10 minutes of sitting
and found to be 145/100 mm Hg.
Blood tests were taken and the patient was asked to return in a week. He was asked to bring
some photographs of himself from 5 to 10 years previously. When he returned a week later, the
patient said that both he and his wife were surprised at how much his facial features had
changed over the last 10 years. His wife had also noticed a change in his voice. On questioning
the patient recalled that his shoe size had increased twice in the last 10 years.
Visual field examination was performed - the results of this are provided. The patient was
referred to outpatients’ clinic for specialist consultation.
Ó Royal Australasian College of Surgeons – December 2000 Page 153 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 5.3
1. List the likely changes in this man's appearance over the last 5-10 years. Explain the pathophysiologic
basis.
2. Explain the abnormalities of his visual fields.
3. List the complications of a benign neoplasm seen in this man.
4. List general complications of benign neoplasms; include consideration of neoplasms arising in the cranial
cavity.
5. Figures 5-3A and 5-3[normal] show two CT scans - the plane of section is indicated on each by the
small inset. One scan shows a normal pituitary fossa and the other is from the patient.
(a) Identify the pituitary fossa in each CT scan.
(b) Describe the lesion seen in the CT scan of the patient.
(c) What is the pattern of growth of this lesion?
Refer to Resource Unit General Principles of Pathology Figure 5-3A
http://www.bst.racs.edu.au/racs/servlet/disp/16558?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-3[normal] Pituitary fossa
http://www.bst.racs.edu.au/racs/servlet/disp/16558?
Scroll down to thumbnails and select the appropriate image
6. Growth hormone levels were measured in this patient during a 75 g glucose tolerance test. Normal
fasting levels of growth hormone (GH) are < 5 ng/ml.
(a) What do these results indicate about the source of the GH?
(b) Do you have any other comments about the test?
7. The patient underwent trans-sphenoidal hypophysectomy.
(a) What non-routine blood test(s) should be done before surgery in this patient? Explain your
reasoning.
Review the histologic features of the normal pituitary gland provided, Figure 5-3B[normal]. On this
PAS-OG stain basophilic cells are purple, acidophilic cells are orange and chromophobe cells are
weakly staining.
Ó Royal Australasian College of Surgeons – December 2000 Page 154 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Figure 5-3B shows one of the fragments removed at hypophysectomy. Fragments of both normal
pituitary and tumour are seen.
(b) Identify the fragment(s) of tumour and describe the features seen in the tumour.
(c) What features indicate that this represents tumour?
(d) Comment on the differentiation of the tumour cells.
(e) What is your diagnosis? Summarise the features of the various tests that lead to this diagnosis
under the following headings:
i) CT scan
ii) GTT
iii) Histology
Refer to Resource Unit General Principles of Pathology Figure 5-3B
http://www.bst.racs.edu.au/racs/servlet/disp/16560?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-3B[normal] PAS-orange G
http://www.bst.racs.edu.au/racs/servlet/disp/16560?
Scroll down to thumbnails and select the appropriate image
8. List the complications that may occur from the continued growth of this neoplasm.
9. Figures 5-3C(i) and 5-3C(ii) (outer and cut surface) shows an intracranial tumour from a patient who
had an 8-year history of fits. Describe the gross and microscopic appearances and make a diagnosis.
Refer to Resource Unit General Principles of Pathology Figure 5-3C(i)
http://www.bst.racs.edu.au/racs/servlet/disp/16562?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-3C(ii)
http://www.bst.racs.edu.au/racs/servlet/disp/16562?
Scroll down to thumbnails and select the appropriate image
Ó Royal Australasian College of Surgeons – December 2000 Page 155 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
10. Compare and contrasting benign and malignant neoplasms.
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 1123-1127, Hyperpituitarism
pages 1297-1299, Increased intracranial pressure
pages 1350-1351, Meningioma
page 319, Clinical effects - general
Ó Royal Australasian College of Surgeons – December 2000 Page 156 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 5.4
A 44-YEAR-OLD MAN WITH MALIGNANT MELANOMA
This 44-year-old man consulted his doctor about an enlarging mole on the back of his left leg. He
thought that it had grown slowly over many months, but he had not paid much attention to it.
Recently it had developed a raised area which had bled when drying himself with a towel. On
examination the doctor noted an irregularly outlined, irregularly pigmented zone 1 cm in diameter,
which was predominantly flat with a nodular raised area near one edge. An excision biopsy was
performed and the tissue was sent to the laboratory for histologic examination. Subsequently a
wider excision of skin around the biopsy site was carried out.
Approximately one year later he represented with enlarged lymph nodes in the left groin which
were excised and found to contain metastatic malignant melanoma.
Eighteen months later he was admitted acutely following a grand mal seizure. On questioning he
admitted to having had ‘funny turns’ over the six months prior to admission. A CT scan of his head
was undertaken following which he was treated with radiotherapy.
He was discharged home but over a three month period became increasingly weak and debilitated.
He also developed right sided weakness.
He was finally admitted for terminal care because of increasing frequency of seizures and
persisting headache. On admission he was drowsy and had bilateral papilloedema. His abdomen
was distended, and he had a grossly enlarged liver. He was treated symptomatically, with good
relief of his symptoms, although he remained drowsy. In the days before his death he developed a
fever and a chesty cough. He was kept comfortable and died in his sleep.
Ó Royal Australasian College of Surgeons – December 2000 Page 157 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 5.4
1. Describe features that should raise suspicion about the nature of a pigmented skin lesion.
2. Summarise current information about the relationship of sun exposure and the risk of developing
malignant melanoma.
3. "The principle of tumour progression is elegantly illustrated by the events of human melanocytic
neoplasia." (Rubin and Farber, 1st Ed., page 1242). Describe the stages of tumour progression seen in
development of many malignant melanomas.
4. Figure 5-4A shows a pigmented skin lesion.
(a) Describe/draw what you see and make a diagnosis.
(b) What changes would you have expected to have seen in this lesion in the months prior to excision?
Explain your reasoning.
(c) Do you expect a lesion like this to have metastatic potential? Explain your reasoning.
Refer to Resource Unit General Principles of Pathology Figure 5-4A
http://www.bst.racs.edu.au/racs/servlet/disp/16570?
Scroll down to thumbnails and select the appropriate image
5. Figure 5-4B shows the type of changes seen histologically in a cross-section of a lesion like
Figure 5-4A.
(a) Describe the findings and make a diagnosis, explaining your reasoning.
(b) In which part of the lesion seen in Figure 5-4A would a cross-section show these histologic
features?
(c) What is the prognosis for this patient? Explain your reasoning.
Refer to Resource Unit General Principles of Pathology Figure 5-4B
http://www.bst.racs.edu.au/racs/servlet/disp/16572?
Scroll down to thumbnails and select the appropriate image
Ó Royal Australasian College of Surgeons – December 2000 Page 158 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
6. Figures 5-4C and 5-4D show the type of changes seen grossly at autopsy examination. Figure 5-4E
shows histologic changes from specimen Figure 5-4C.
(a) What is your diagnosis of these lesions?
(b) List characteristic features of these lesions.
(c) Describe/draw a flow chart of the sequence of events that have lead to the development of these
lesions.
Refer to Resource Unit General Principles of Pathology Figure 5-4C
http://www.bst.racs.edu.au/racs/servlet/disp/16574?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-4D
http://www.bst.racs.edu.au/racs/servlet/disp/16574?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-4E
http://www.bst.racs.edu.au/racs/servlet/disp/16574?
Scroll down to thumbnails and select the appropriate image
7. List ways to decrease the mortality from malignant melanoma.
8. Figure 5-4F show the type of changes seen at autopsy in the lower part of both lungs of the patient in
the clinical history.
(a) Describe the findings. What is your diagnosis?
(b) What is the pathogenesis of these changes?
(c) What predisposed this man to develop this lung condition?
Refer to Resource Unit General Principles of Pathology Figure 5-4F
http://www.bst.racs.edu.au/racs/servlet/disp/16579?
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 309-311, Radiation carcinogenesis
pages 1179-1179, Naevi and melanoma
Ó Royal Australasian College of Surgeons – December 2000 Page 159 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 5.5
RECURRENT ABDOMINAL PAIN IN A 60-YEAR-OLD MAN
A sixty-year-old man consulted his family doctor because of recurrent ‘vague, gnawing’ abdominal
pain which he described as deep and poorly localised, but very debilitating. There were no other
significant symptoms and the physical examination showed no abnormal findings. At this stage an
ultrasound examination of the abdomen and retroperitoneal region gave no diagnostic assistance.
Panadol was prescribed.
He returned two weeks later having had no relief; if anything the pain had become more persistent.
His doctor noted that he showed obvious signs of recent weight loss to a degree that made him
highly suspicious of some occult malignant process. A number of further investigations were
undertaken, this time including computerised axial tomography to visualise the kidneys and
retroperitoneal structures.
An abnormal density was present in the body of the pancreas, with enlargement of the
peripancreatic lymph nodes.
After discussion with the patient, it was decided not to proceed with an operation to remove the
presumed cancer. However, to ensure that the diagnosis was correct, a needle biopsy was
obtained under radiological guidance. This gave a diagnosis of ‘poorly differentiated
adenocarcinoma’.
He returned to Oncology Day Clinic for the first three weeks for treatment; there was no apparent
improvement in his clinical condition. Home management was accomplished with suitable nursing
and emotional support and adequate pain relief through a ‘demand infusion’ apparatus. He was
visited regularly by his family doctor who said he ‘seemed to melt away visibly each day’ with
profound progressive weight loss to the point of profound emaciation.
Eight weeks after first consulting his doctor, he developed a weak ‘rattly’ cough with fever,
gradually became obtunded and then comatose. No active treatment was undertaken; he died a
few hours later.
Ó Royal Australasian College of Surgeons – December 2000 Page 160 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 5.5
1. Figure 5-5A shows the cut surface of the pancreatic mass found at autopsy.
(a) How does this appearance differ from Figure 5-5A[normal]?
(b) The main pancreatic duct has been obstructed by the tumour. What changes would you expect to
ultimately occur distal to the tumour:
i) in the exocrine lobules?
ii) in the endocrine islets?
Refer to Resource Unit General Principles of Pathology Figure 5-5A
http://www.bst.racs.edu.au/racs/servlet/disp/16582?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-5A[normal]
http://www.bst.racs.edu.au/racs/servlet/disp/16582?
Scroll down to thumbnails and select the appropriate image
2. Figure 5-5B shows the histology of this pancreatic carcinoma. What feature(s) indicating malignancy
is/are shown?
Refer to Resource Unit General Principles of Pathology Figure 5-5B
http://www.bst.racs.edu.au/racs/servlet/disp/16585?
3. Figure 5-5C is of a patient in the terminal phases of inoperable pancreatic cancer.
(a) What immediately striking clinical feature is apparent?
(b) What is the usual clinical term for this syndrome?
(c) What is thought to be the pathogenesis of this syndrome?
(d) The effects of these cytokines are dose-related and may be local or systemic. The pathological
effects are:
i) low dose – local, acute?
ii) low dose – systemic, acute?
iii) ‘medium’ dose – systemic, subacute, result – cancer cachexia
iv) ‘high’ dose – systemic, acute?
Refer to Resource Unit General Principles of Pathology Figure 5-5C
http://www.bst.racs.edu.au/racs/servlet/disp/16586?
Ó Royal Australasian College of Surgeons – December 2000 Page 161 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
page 319, Cancer cachexia
pages 910-911, Carcinoma of the pancreas
Ó Royal Australasian College of Surgeons – December 2000 Page 162 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
CASE SCENARIO 5.6
TIREDNESS AND PALLOR IN A 55-YEAR-OLD WOMAN
Mrs VR aged 55, a part-time secretary, consulted her family doctor about tiredness and occasional
attacks of 'palpitations'. These symptoms had come on gradually during the previous two to three
months. A friend at work had recently told her she 'looked pale'. She said her appetite was good
and her weight was steady although she had always thought she was 'thin for her height'.
Mrs VR had suffered no serious illness in the past and she had passed the menopause
uneventfully at the age of 50. She had three children (a son aged 27 and two daughters aged 25
and 23) who were well. Her husband, a carpenter, was fit and her mother was alive and well at the
age of 82. Her father had died aged 70, shortly after a 'heart attack'. An aunt on her mother's side
of the family had died aged 49 from rectal cancer.
On examination, oral mucosa and conjunctivae were pale and her tongue looked somewhat
smooth and shiny, with loss of papillae. Her blood pressure (lying) was 155/75 mmHg and her
radial pulse was 92/min and regular in rhythm. The apex beat was in the fifth left intercostal space,
in the mid-clavicular line. The heart was clinically normal. No abnormalities were detected in the
abdomen, except for some slight tenderness to palpation in the epigastrium. Nothing abnormal
was found on rectal examination. An ECG was normal.
The doctor sent Mrs VR for blood tests. The results of these tests were as follows.
Ó Royal Australasian College of Surgeons – December 2000 Page 163 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Blood Screen
Test Result Normal Range Units
Blood Haemoglobin concentration 73 115 - 165 g/l
12
Red cell count 3.6 3.8 - 5.8 x10 /l
Haematocrit 0.25 0.37 - 0.47
Mean cell haemoglobin 20 27 - 32 pg
Mean cell volume 69 76 - 96 fL
Mean cell haemoglobin conc 292 300 - 350 g/l
9
Reticulocyte count 40 24 - 84 x10 /l
9
White cell count 12.1 4 - 11 x10 /l
9
Differential count x10 /l
Neutrophils 9.1 2.0 - 7.5
Lymphocytes 2.5 1.5 - 4.0
Monocytes 0.4 0.2 - 0.8
Eosinophils 0.07 0.04 - 0.4
Basophils 0.03 0-0.1
9
Platelet count 440 150 - 400 x10 /l
Serum Iron 5 10 - 30 µmol/l
TIBC 95 40 - 75 µmol/l
Ferritin 8 40 - 340 µg/l
Blood film: The red cells are hypochromic and microcytic, with pencil-shaped
poikilocytes. Anisocytosis ++ , poikilocytosis ++.
After discussing these results with Mrs VR, her family doctor prescribed tablets of dried ferrous
sulphate 200 mg, one tablet to be taken three times a day. Follow-up blood tests (haemoglobin
and reticulocyte counts) were as follows. (Day 0 was when the patient started taking iron tablets).
Test Day 0 Day 7 Day 14 Day 21 Ref Range Units
Haemoglobin 74 77 82 84 115 - 165 g/l
Reticulocytes 41 130 110 80 24 - 84 x109/l
Ó Royal Australasian College of Surgeons – December 2000 Page 164 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Mrs VR was then referred to a surgeon and admitted to hospital for further investigations. Barium
enema x-ray indicated the presence of a large mass in the right colon near the caecum. At
operation, a large tumour was resected. The surgeon reported in the operating notes that the
tumour seemed to be confined to the wall of the colon but regional lymph nodes appeared to be
involved. This statement was confirmed by a subsequent pathology report. She recovered
uneventfully and was discharged from hospital.
Fifteen months later, Mrs VR called to make an appointment with her family doctor because of
recent onset of headaches which ‘woke her in the morning’. On the morning of the day when
scheduled to keep her appointment, she had a grand mal seizure and was admitted directly to
hospital. When she was examined it was apparent that:
· Her memory for recent events was faulty
· She had a slight but definite weakness of the right side of her body
· Her visual acuity was impaired, without a local defect
· She had bilateral papilloedema
OBJECTIVES
By the end of this case study you should be able to:
1. Describe the gross and microscopic features of colonic adenomas and colonic adenocarcinomas.
2. Explain the concept of the colonic ‘adenoma-carcinoma sequence’ and the evidence for this.
3. Describe the common complications of colonic adenomas and colonic adenocarcinomas.
Ó Royal Australasian College of Surgeons – December 2000 Page 165 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
SELF-TEST TASK 5.4
1. Figures 5-6A(i) and 5-6A(ii) [mucosal and serosal surfaces] show changes similar to those found in
the right colon of this patient. Describe or draw the changes seen. List your diagnoses - make sure
that you inspect the whole of the mucosal surface and the serosal surface.
Refer to Resource Unit General Principles of Pathology Figure 5-6A(i)
http://www.bst.racs.edu.au/racs/servlet/disp/16589?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-6A(ii)
http://www.bst.racs.edu.au/racs/servlet/disp/16589?
Scroll down to thumbnails and select the appropriate image
2. Explain the anaemia noted in the woman in the case history.
3. Figures 5-6B and 5-6C show two tumours of the type found in Figures 5-6A(i) and 5-6(ii). Each one
shows areas of normal epithelial pattern and of neoplasia.
(a) Describe or draw and label each, contrasting normal and abnormal patterns of growth and
cytological features.
(b) Match each to a corresponding area on Figure 5-6A(i) and 5-6A(ii).
(c) Allowing that one only of these corresponds to the large lesion in Figure 5-6A(i), give a diagnosis.
Refer to Resource Unit General Principles of Pathology Figure 5-6B
http://www.bst.racs.edu.au/racs/servlet/disp/16593?
Scroll down to thumbnails and select the appropriate image
Refer to Resource Unit General Principles of Pathology Figure 5-6C
http://www.bst.racs.edu.au/racs/servlet/disp/16593?
Scroll down to thumbnails and select the appropriate image
4. What risk factors appear to predispose to the development of these lesions of the colon?
5. Figure 5-6D shows the histological appearances of a mesenteric lymph node examined from the
resected material.
(a) What do you see and what is the pathogenesis of this development?
(b) What is your diagnosis?
(c) What are the prognostic implications of this finding?
(d) What other sites of intra-abdominal involvement would the surgeon have looked for during surgery?
(e) What are the possible routes of spread?
Ó Royal Australasian College of Surgeons – December 2000 Page 166 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Refer to Resource Unit General Principles of Pathology Figure 5-6D
http://www.bst.racs.edu.au/racs/servlet/disp/16597?
REFERENCE
th
Cotran R, Kumar V, Collins T, Robbins Pathologic Basis of Disease, W B Saunders Co, 6 Ed,
1999;
pages 275-276, Heredity and cancer
pages 276-294, Molecular basis of cancer
pages 296-297, Molecular basis of multistep carcinogenesis
pages 827-835, Carcinoma of colon and rectum
Ó Royal Australasian College of Surgeons – December 2000 Page 167 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
MULTIPLE CHOICE QUESTIONS
TYPE A (ONE OF FIVE)
Q1 The closest association between development of malignancy and radiation is seen with
A. thyroid
B. salivary gland
C. bone
D. leukaemia
E. breast
Q2 In the following sequential developments in the 'metastatic cascade' the second event to occur is
A. degradation of collagen and other matrix components
B. tumour embolisation
C. extravasation
D. carcinogenic cell transformation
E. tumour cell interaction with platelets
Q3 Each of the following is true of carcinogenic initiation, except
A. effects are rapid
B. effects are reversible
C. induces DNA alteration
D. has ‘memory’
E. can be active when given in divided doses
Q4 In the following steps in the ‘metastatic cascade’, the second occurrence is
A. development of a ‘metastatic subclone’
B. extravasation
C. clonal expansion, growth and diversification
D. passage through extracellular matrix
E. tumour cell embolus
Q5 The best survival with thyroid neoplasia is seen with
A. sporadic (non-familial) medullary carcinoma
B. giant cell carcinoma
C. follicular carcinoma
D. papillary carcinoma
E. small cell carcinoma
Ó Royal Australasian College of Surgeons – December 2000 Page 168 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
TYPE X (MULTIPLE TRUE-FALSE)
Q6 The human papilloma virus (HPV) has been causally implicated in the genesis of
1. nasopharyngeal cancer
2. cancer of the uterine cervix
3. Hodgkin's disease, nodular sclerosing type
4. skin cancer in individuals with inherited or induced (renal transplant) cell-mediated immune
defects
Q7 Cushing's syndrome may be caused by neoplasms originating in
1. bronchus
2. pituitary
3. oesophagus
4. breast
Q8 Using a standard accepted model of theoretical growth of a cancer clone (30 doublings =
9
1 x 10 cells = 1 gram), this potential is never achieved because cells are lost to the proliferative pool
when they
1. enter the Go phase
2. are in the G1 phase
3. enter the G2 phase
4. differentiate
Q9 There is a positive experimental and/or clinical correlation between metastatic potential of cancer cells
and their
1. elaboration of plasminogen activator
2. blockade of fibronectin receptors on tumour cells
3. secretion of type IV collagenase
4. density of laminin receptors
Q10 Extracellular matrix degradation by tumour cells, together with the products of such matrix breakdown,
gives rise to
1. angiogenesis factors
2. chemotaxis factors
3. growth factors
4. a physical passage for tumour cell migration
Ó Royal Australasian College of Surgeons – December 2000 Page 169 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Q11 Laminin in basement membranes has binding sites for
1. macrophage Fc receptors
2. epithelial cell membrane receptors
3. proteoglycan
4. collagen type IV
Q12 When complicated by extensive metastatic spread, the following cancers characteristically cause
hypercalcaemia
1. kidney
2. lung
3. breast
4. prostate
Q13 Choriocarcinoma of gestational origin
1. if untreated, parallels the behaviour of primary ovarian choriocarcinoma
2. metastasises early and widely
3. has a generally good prognosis with chemotherapy
4. can be monitored clinically by plasma gonadotrophin (HCG) levels
Q14 Neuroblastoma of the adrenal
1. commonly matures spontaneously to form a ganglioneuroma
2. is a cancer of childhood
3. commonly causes hypertension
4. has often metastasised by the time of diagnosis
Q15 Carcinoma of the bronchus may cause
1. hypocalcaemic syndrome of pseudohypoparathyroidism
2. Cushing's syndrome
3. hyponatraemia
4. inappropriate secretion of norepinephrine
Q16 Carcinoid tumours
1. are most commonly found incidentally at surgery or autopsy
2. show neuroendocrine differentiation
3. are clinically innocuous neoplasms
4. most commonly grow ‘within the range of the competent sigmoidoscopist’
Ó Royal Australasian College of Surgeons – December 2000 Page 170 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Q17 In human cancers research suggests that , when compared with normal tissues derived from labile cell
populations, cancer cells
1. have a higher percentage of terminally maturing cells
2. do not have a shorter cell cycle time
3. have a greater proportion of cells in the replication cycle
4. replicate at a rate in excess of most labile cell populations
Q18 Colonic carcinoma has an increased incidence in individuals with
1. hyperplastic polyps
2. Peutz-Jegher's syndrome
3. tubular adenomas
4. chronic ulcerative colitis
Q19 Malignant melanoma
1. is usually uniformly either black or amelanotic
2. may arise in diverse mucosal sites
3. usually has irregular ‘notched’ borders
4. prognosis is predicted most accurately by the mitotic rate
Q20 Dysplastic melanocytic naevi
1. very seldom occur on other than sun-exposed skin
2. usually have pale edges with a uniform central 'salmon pink' papule
3. most develop into malignant melanoma within two decades if not ablated
4. show melanocytic atypia and superficial dermal lymphocytic infiltrate
Q21 Merkel cell carcinoma of the skin
1. is an indolent ‘adnexal’ tumour resembling basal cell carcinoma in behaviour
2. histologically resembles ‘oat cell’ bronchial carcinoma
3. most commonly arises in axillae, groins or midline anterior abdominal skin
4. shows both neuroendocrine and epithelial differentiation by cell marker studies
Q22 Kaposi's sarcoma
1. arises in skin and usually remains confined to skin and subcutaneous tissue
2. is less biologically aggressive when it occurs in HIV-positive individuals
3. presents as reddish, spreading and merging papules and plaques in the skin
4. is a suppressor T lymphoproliferative disorder
Ó Royal Australasian College of Surgeons – December 2000 Page 171 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Q23 Multiple endocrine neoplasia syndromes may threaten life because they may cause
1. hypertension
2. inappropriate ADH secretion
3. relentless peptic ulcer syndrome
4. 'malignant' thyrotoxicosis (thyrotoxic storm)
Q24 Carcinogenesis induced by DNA viruses
1. is usually a single step (‘single hit’) process
2. may act by neutralising growth-inhibiting molecules
3. may involve incorporation of viral oncogene into host DNA
4. may cause stimulation of function of growth-promoting protein(s)
Q25 In follow-up of asymptomatic family members of a patient with medullary thyroid carcinoma associated
with multiple endocrine neoplasia syndrome (MEN II), effective screening tests include
1. plasma calcitonin levels
2. urinary catecholamine estimation
3. plasma calcium estimation
4. serum ionised calcium/phosphate ratio
Q26 Papillary carcinoma of the thyroid
1. can be the result of childhood thyroid irradiation
2. may have lung metastases for many years
3. commonly presents clinically because of metastases
4. is biologically more aggressive, when the histology shows an admixture of papillary and follicular
growth patterns
Q27 RNA oncogenic viruses
1. have been shown to be causally involved in the genesis of many human cancers
2. can convert normal host cell proto-oncogenes into oncogenes (c-oncogenes)
3. form templates for DNA transcription within the host cell
4. usually splice directly into the host genome before activation
Ó Royal Australasian College of Surgeons – December 2000 Page 172 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Q28 Proto-oncogenes
1. are rendered incapable of transcribing growth-related proteins following chromosomal
translocation
2. are, in the normal cell, inactive DNA sequences without physiological action
3. may be activated into functional oncogenes (c-onco-genes) by mutation of a specific gene site
4. may be activated by destruction of adjacent controller genes, which normally suppress their
action
Q29 Familial retinoblastoma
1. is always a congenital neoplasm
2. is activated by chromosomal translocation
3. has an inheritance pattern which is autosomal recessive
4. develops only in a retinoblast which has the appropriate DNA defect in both of the paired
chromosomes
Ó Royal Australasian College of Surgeons – December 2000 Page 173 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
TYPE B (RELATIONSHIP-ANALYSIS)
Q30 Carcinogenic initiating agents are thought to produce their actions by their mutagenic effects
because
carcinogenic initiation produces irreversible alterations in DNA chemistry in target cells.
Q31 DNA damage by chemicals is not necessarily carcinogenic
because
DNA damage can be repaired by cellular enzyme systems.
Q32 The effects of carcinogenic promoters are thought to be potentially reversible
because
tumours do not eventuate if the 'promoter-effective' dose is applied prior to the application of the
appropriate initiator.
Q33 The effects of carcinogenic initiators on DNA chemistry are reversible
because
tumours do not eventuate if the subsequent promoter application is delayed.
Q34 Karyotype/chromosomal abnormalities are thought to be a primary event in development of many
human neoplasms
because
in certain types of human neoplasia, karyotype abnormality is non-random and common in that tumour
type.
Q35 Major karyotype/chromosomal abnormalities are not thought to be a primary event in human
neoplasms
because
in human neoplasms, any karyotype abnormalities are uncommon and always variable within the
same tumour type.
Q36 Gardner's syndrome is a clinically more sinister variant of familial polyposis coli (FPC)
because
in Gardner's syndrome, colonic malignancies occur, on average, about one decade earlier than when
FPC occurs alone.
Q37 Gardner's syndrome is a clinically more sinister variant of familial polyposis coli (FPC)
because
aggressive neoplasms, other than colonic carcinoma, may determine mortality in Gardner's syndrome.
Ó Royal Australasian College of Surgeons – December 2000 Page 174 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
TYPE X (MULTIPLE TRUE-FALSE)
Q38 Testicular seminoma
1. when dissemination occurs, is usually first manifest by blood stream spread
2. is highly radiosensitive
3. when associated with raised plasma human chorionic gonadotrophin (HCG), shows no different
clinical behaviour
4. is the least aggressive of the testicular germ cell neoplasms
Q39 Likelihood of infections in advanced, untreated myeloma is contributed to by
1. reduced levels of normal (non-myeloma) immunoglobulins
2. high rate of infection by low-grade ('opportunistic') pathogens
3. depression of cellular (T cell) immunity
4. progressive, unrelenting viral infections
Q40 Precursor lesions of colonic adenocarcinoma include
1. hyperplastic polyps
2. Peutz-Jegher polyps
3. adenomatous polyps
4. juvenile polyps
Q41 Colonic epithelial neoplasia is considered as not having significant metastatic potential if adequate
histological examination shows
1. adenoma with carcinoma in situ
2. adenoma showing severe epithelial dysplasia with focal intramucosal carcinoma
3. adenocarcinoma, invasive into submucosa only
4. invasive adenocarcinoma to superficial muscularis propria, without demonstrable vascular or
lymphatic permeation
Q42 Most colorectal carcinomas
1. arise within pre-existing adenomas
2. occur in the absence of pre-existing ulcerative colitis or familial adenomatous polyposis syndrome
3. present clinically in individuals under age 55 years
4. arise in the distal 15 cm of colon/rectum
Ó Royal Australasian College of Surgeons – December 2000 Page 175 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Q43 Most carcinomas of the gallbladder
1. are squamous or adenosquamous carcinomas
2. present clinically with pain plus an enlarged gallbladder
3. have invaded the liver at the time of operation
4. are always associated with presence of gall bladder calculi
Q44 Carcinoma of the extrahepatic bile ducts
1. in most cases does not cause palpable gallbladder enlargement
2. has a prognostic outlook similar to that of colonic carcinoma
3. is curably resectable in most instances
4. commonly causes obstructive jaundice
Q45 Clinical manifestations/complications of renal adenocarcinoma may include
1. amyloidosis
2. polycythaemia
3. fever and cachexia
4. hypercalcaemia
Q46 With adenocarcinoma of the prostate
1. there is good correlation between tumour differentiation and prognosis
2. early haematogenous visceral metastatic dissemination is common
3. lymph node metastases are unusual
4. local extension commonly involves seminal vesicles
Q47 In cases of prostatic carcinoma
1. raised plasma prostate-specific antigen (PSA) level is a reliable marker for disease in
asymptomatic men
2. plasma prostate-specific antigen (PSA) levels correlate well with total tumour volume
3. most patients, at presentation with symptomatic disease, have carcinoma which is localised within
the gland
4. haematogenous spread occurs chiefly to bone
Ó Royal Australasian College of Surgeons – December 2000 Page 176 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
TYPE B (RELATIONSHIP-ANALYSIS)
Q48 Carcinomas develop through ‘dedifferentiation’ of normal, differentiated, cells
because
carcinomas result from repression of normal gene activity in differentiated, mature cells which revert
to ‘immature’ cells.
Q49 Genes controlling apoptosis such as p53 are believed to be important in controlling/preventing growth
of potential cancer cells
because
‘apoptosis genes’ arrest the mitotic process of cells with DNA damaged by mutagenic agents which
allows time for DNA repair or, if repair does not occur, induces cell autodestruction.
Q50 Oncogenic viruses all contain oncogenes which are virtually or actually identical with proto-oncogenes
present in normal cells
because
cancer-causing viruses are oncogenic only because of the actions of proto-oncogene- homologous
DNA.
Q51 Oncogenesis probably involves multiple sequential DNA mutations before neoplastic behaviour
develops
because
all human cancers which have been analysed in detail have been found to have mutations which
involve both activation of promoter genes and loss of cancer suppressor genes.
Q52 Acquisition of the characteristics of ability to metastasise by cancer cells is presumed to be dependent
on multiple different mutations in the cells
because
no single gene has thus far been discovered which appears to code for metastasising behaviour by
neoplastic cells.
TYPE A (ONE OF FIVE)
Q53 The commonest cause of death in multiple myeloma is
A. renal failure
B. amyloid-related multiple organ failure
C. intestinal infarction due to hyperviscosity syndrome
D. infections by pyogenic bacteria
E. cardiac arrhythmia due to hypercalcaemia
Ó Royal Australasian College of Surgeons – December 2000 Page 177 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
Answers and Commentaries
A1 The closest association between development of malignancy and radiation is seen with
A. thyroid
B. salivary gland
C. bone
D. leukaemia
E. breast
Answer D
Thyroid papillary cancer is a major risk following childhood head and neck radiation, often for trivial
problems. The story of bone cancer following repeated ingestion of radium in young women who
painted watch dials is (in)famous (they 'pointed' their brushes by moistening them with their tongues!).
Leukaemia > thyroid > breast, lungs, salivary gland > skin, bone, G-I oncogenesis is the hierarchy
experience of fluoroscopy, and post-Hiroshima, Nagasaki, Marshall Islands and Chernobyl epidemics.
CML does not share the radiation risk seen with other leukaemias.
A2 In the following sequential developments in the 'metastatic, cascade' the second event to occur is
A. degradation of collagen and other matrix components
B. tumour embolisation
C. extravasation
D. carcinogenic cell transformation
E. tumour cell interaction with platelets
Answer: A
The ‘metastatic cascade’ concept is a useful one, in that it takes the whole process and itemises the
steps in sequence from cancer cell ‘initiation’ through the concepts of genetic instability, selection of
‘metastatic subclones’, the necessity for acquisition of new characteristics of cells to break down
extracellular matrix and so on. Detailed consideration of each of these areas is considered in
preceding or following sections of the same chapter.
Ó Royal Australasian College of Surgeons – December 2000 Page 178 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A3 Each of the following is true of carcinogenic initiation, except
A. effects are rapid
B. effects are reversible
C. induces DNA alteration
D. has ‘memory’
E. can be active when given in divided doses
Answer: B
This deals with oncogenic initiation and promotion. It relates to chemical carcinogenesis but is
applicable, with modification, to radiation and viral oncogenesis. Rigid classification as 'complete'
carcinogens (oncogens, but not oncogenes), initiators and promoters is conceptually useful, but not
always easy. The concept is that initiators damage DNA in a fashion which is not susceptible to repair
(either widely, or in individuals with genetic defect in DNA repair capability). Promoters then apparently
‘push’ the cell the extra step(s) to uncontrolled growth. This is central to understanding oncogenesis.
A4 In the following steps in the ‘metastatic cascade’, the second occurrence is
A. development of a ‘metastatic subclone’
B. extravasation
C. clonal expansion, growth and diversification
D. passage through extracellular matrix
E. tumour cell embolus
Answer: A
The concept is, that before cancer cells can invade (or metastasise), there has to be: (1) initiation, (2)
promotion, (3) proliferation (clonal expansion, growth) and diversification through subclone selection;
via the inherent genetic instability of cancer cells, (4) selection of a ‘metastatic subclone’ (requires eg
laminin and fibronectin receptor elaboration, ECM protease synthesis etc, locomotion capability and
perhaps chemotaxis), before any of the possible responses (D), (E) or (B) come onto the scene (these
last three are in that order of events).
Ó Royal Australasian College of Surgeons – December 2000 Page 179 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A5 The best survival with thyroid neoplasia is seen with
A. sporadic (non-familial) medullary carcinoma
B. giant cell carcinoma
C. follicular carcinoma
D. papillary carcinoma
E. small cell carcinoma
Answer: D
Papillary cancer of the thyroid has a very good medium and even long term outlook, even in the
presence of disseminated disease. Familial medullary cancer also has an excellent prognosis; this is
not shared by the sporadic (non-familial) form of medullary cancer, which also has marked differences
in clinical presentation. Follicular cancer has an outlook somewhere between papillary/familial
medullary and the highly malignant giant and small cell (collectively ‘undifferentiated’) forms.
A6 The human papilloma virus (HPV) has been causally implicated in the genesis of
1. nasopharyngeal cancer
2. cancer of the uterine cervix
3. Hodgkin's disease, nodular sclerosing type
4. skin cancer in individuals with inherited or induced (renal transplant) cell-mediated
immune defects
2, 4 True; 1, 3 False
There is close association of HPV (types 16, 18 and 31) with anogenital cancers (especially cervix).
HPV (multiple strains) causes venereally acquired condyloma acuminatum. High risk HPV strains
(16, 18 and 31):
(a) Often become incorporated in the host genome
(b) Co-operate in cultured cells with the ras oncogene to form tumourigenic foci; and
(c) The probable transforming sequences of HPV are consistently/mostly found in cancer cells from
clinical CIN and invasive cancer. Defective cell-mediated immunity - CMI (hereditary, renal
transplant immunosuppression), HPV (5, 8, 14) and sunlight appear to interplay in formation of
skin cancer.
Ó Royal Australasian College of Surgeons – December 2000 Page 180 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A7 Cushing's syndrome may be caused by neoplasms originating in
1. bronchus
2. pituitary
3. oesophagus
4. breast
1, 2 True; 3, 4 False
Responses 1 and 2 are straightforward (pituitary as a ‘normal’ producer; bronchus as an
‘inappropriate’ producer). While oesophageal squamous cell carcinoma occasionally is associated
with ‘inappropriate hyperparathyroid’ state, it does not cause Cushing’s syndrome. Nor has breast
cancer been documented as a cause of ‘inappropriate ACTH production’.
9
A8 Using a standard accepted model of theoretical growth of a cancer clone (30 doublings = 1 x 10 cells
= 1 gram), this potential is never achieved because cells are lost to the proliferative pool when they
1. enter the Go phase
2. are in the G1 phase
3. enter the G2 phase
4. differentiate
1, 4 True; 2, 3 False
9 12
The ‘30 doublings = 10 cells = 1 gram; 10 more doublings = 10 = 1 kg = maximum possible tumour
burden’ concept is alive and well! The question asks for the reason(s) why that model is not
applicable to clinical cancer. Cells in any of the G1, S, G2 or M phases of the cell cycle are
considered to be in the ‘proliferative pool’ by definition; in clinical cancer, cells are lost to the
proliferative pool for many reasons and cell proliferation is not synchronous. Much of theoretical
oncology deals with ‘models’ - try ‘Gompertzian growth curve’!
A9 There is a positive experimental and/or clinical correlation between metastatic potential of cancer cells
and their
1. elaboration of plasminogen activator
2. blockade of fibronectin receptors on tumour cells
3. secretion of type IV collagenase
4. density of laminin receptors
1, 3, 4 True; 2 False
Responses 2 and 4 (pages 303-4) relate to the important capacity of tumour cells to bind to collagen
of basement membrane (type IV - laminin) and interstitium (type I - fibronectin). Blockade of
receptors will decrease metastatic potential (response 2); 1 and 3 refer to breakdown of intercellular
Ó Royal Australasian College of Surgeons – December 2000 Page 181 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
matrix, which creates space for cancer cell invasion and probably also growth and chemotactic stimuli
(for stromal and perhaps also cancer cells). Experimental fibronectin receptor blockade (using an
analogue which occupies the receptor sites for laminin on tumour cells) inhibits lung metastases.
A10 Extracellular matrix degradation by tumour cells, together with the products of such matrix breakdown,
gives rise to
1. angiogenesis factors
2. chemotaxis factors
3. growth factors
4. a physical passage for tumour cell migration
1, 2, 3, 4 True
The discussion is the same as for the previous question: any increase in matrix/tumour cell binding;
anything which increases matrix destruction (response 2); any factor which makes space or growth
factors or chemotactic factors, will increase the invasion/metastatic potential of a malignant neoplasm.
There is excellent, and increasing, evidence that matrix breakdown products are very active in all of
these areas for neoplasia (and for the pathophysiological counterpart - wound healing).
A11 Laminin in basement membranes has binding sites for
1. macrophage Fc receptors
2. epithelial cell membrane receptors
3. proteoglycan
4. collagen type IV
2, 3, 4 True; 1 False
Explanation as for the previous two questions. Laminin is not a ligand for Fc receptors.
A12 When complicated by extensive metastatic spread, the following cancers characteristically cause
hypercalcaemia
1. kidney
2. lung
3. breast
4. prostate
1, 2, 3 True; 4 False
Hypercalcaemia is probably the commonest paraneoplastic syndrome. In some cancers, this is simply
a calcaemic effect of rapid osteolysis; in others the elaboration of a calcaemic tumour secretion (PTH-
like; TNF-a) is either known or assumed to cause raised plasma calcium - in such discussions, the
Ó Royal Australasian College of Surgeons – December 2000 Page 182 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
question of why some cancers cause rapid bone destruction obviously raises the same possibilities!
With tumours 1, 2 and 3, both mechanisms are thought to be active. Bone lysis is the exception in
prostatic cancer, as is the corresponding (presumably) hypercalcaemia.
A13 Choriocarcinoma of gestational origin
1. if untreated, parallels the behaviour of primary ovarian choriocarcinoma
2. metastases early and widely
3. has a generally good prognosis with chemotherapy
4. can be monitored clinically by plasma gonadotrophin (HCG) levels
1, 2, 3, 4 True
This cancer is one of the success stories of modern systemic chemotherapy. It contrasts markedly
with the still formidable mortality of non-gestational choriocarcinoma, despite the fact that both
neoplasms share the same morphology, cell markers, HCG elaboration etc.
A14 Neuroblastoma of the adrenal
1. commonly matures spontaneously to form a ganglioneuroma
2. is a cancer of childhood
3. commonly causes hypertension
4. has often metastasised by the time of diagnosis
2, 4 True; 1, 3 False
Neuroblastoma has been documented to mature to ganglioneuroma - to find out why is currently akin
to the quest for the holy grail! This type of regression/maturation is rare. More than 90% of adrenal
neuroblastomas secrete catecholamines, but hypertension is rare.
A15 Carcinoma of the bronchus may cause
1. hypocalcaemic syndrome of pseudohypoparathyroidism
2. Cushing's syndrome
3. hyponatraemia
4. inappropriate secretion of norepinephrine
2, 3 True; 1, 4 False
I am unaware of the occurrence of either syndrome 1 or 4 in neoplasia as a ‘para’ neoplastic
syndrome (epinephrine secretion in phaeochromocytoma, for instance, is predictable). Options 2 and
3 are common in lung cancer.
Ó Royal Australasian College of Surgeons – December 2000 Page 183 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A16 Carcinoid tumours
1. are most commonly found incidentally at surgery or autopsy
2. show neuroendocrine differentiation
3. are clinically innocuous neoplasms
4. most commonly grow ‘within the range of the competent sigmoidoscopist’
1, 2 True; 3, 4 False
Options 1 and 2 are clearly correct. However, despite the truth of option 1, carcinoids presenting with
symptoms referable to the presence of the tumour (either its mass effect or due to its secretory
products) present a formidable problem thereafter. Obstructing gut carcinoids usually eventually
metastasise and bronchial carcinoids are “… often locally invasive or occasionally capable of
metastasis”. Option 4 is wildly optimistic, even for exhibitionists!
A17 In human cancers research suggests that, when compared with normal tissues derived from labile cell
populations, cancer cells
1. have a higher percentage of terminally maturing cells
2. do not have a shorter cell cycle time
3. have a greater proportion of cells in the replication cycle
4. replicate at a rate in excess of most labile cell populations
2 True; 1, 3, 4 False
This is a difficult concept - as discussed in any treatise on neoplasia with which I am familiar. The
points are valid - responses 1, 3 and 4 are false and 2 is correct - the explanations for continued
growth are, however, not explored in depth and the bland statement “... there is an imbalance between
cell production and cell loss …” is meant to explain it all! Perhaps a major factor here is that in normal
epithelia (for example), mitosing cells are present only in basal layers (skin or gut crypt) and the bulk
of the epithelial cells are terminally maturing. In CIN, for example, mitoses are present at all layers of
dysplastic epithelium - I suspect that the cells being included for defining the ‘proliferative pool’ stacks
the result. Perhaps more importantly, labile cells such as granulocytes and gut epithelia have a very
short life span - cancer cells may well be more robust!
Ó Royal Australasian College of Surgeons – December 2000 Page 184 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A18 Colonic carcinoma has an increased incidence in individuals with
1. hyperplastic polyps
2. Peutz-Jegher's syndrome
3. tubular adenomas
4. chronic ulcerative colitis
3, 4 True; 1, 2 False
Chronic ulcerative colitis is the most significant non-neoplastic precursor of carcinoma and the debate
over whether or not adenomas (tubular or villous) are precancerous has long been settled!
Hyperplastic polyps are generally agreed to have no premalignant potential in their own makeup, but
may be admixed with adenoma whereupon the lesion takes on the premalignant mantle of the
adenoma. Peutz-Jegher's polyps are considered to be hamartomas with no innate premalignant
potential. The syndrome is, however, associated with an increased incidence of cancers of other
sites.
A19 Malignant melanoma
1. is usually uniformly either black or amelanotic
2. may arise in diverse mucosal sites
3. usually has irregular ‘notched’ borders
4. prognosis is predicted most accurately by the mitotic rate
2, 3 True; 1, 4 False
The points highlighted here are that malignant melanoma is characterised by irregularity of colour
within individual lesions and usually an irregular outline. There are many factors being investigated as
to relevance in terms of prognosis; the “… nature and extent of the vertical growth phase, however,
determines the biologic behaviour …”. Melanomas occur in a variety of sites other than skin (including
virtually every mucosa).
A20 Dysplastic melanocytic naevi
1. very seldom occur on other than sun-exposed skin
2. usually have pale edges with a uniform central 'salmon pink' papule
3. most develop into malignant melanoma within two decades if not ablated
4. show melanocytic atypia and superficial dermal lymphocytic infiltrate
4 True; 1, 2, 3 False
Unlike ordinary moles, dysplastic naevi are common on sun-protected skin. Like malignant
melanoma, they are larger than moles, irregular in both outline and colour, but lack the distinct nodular
Ó Royal Australasian College of Surgeons – December 2000 Page 185 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
development seen in MM (unless they themselves develop a focus of malignant degeneration), being
macular (flat) or slightly raised (papular). Dysplastic naevi do show melanocytic dysplasia, and upper
dermal lymphocytosis, do have a very significant premalignant potential; nevertheless, the majority of
dysplastic naevi are stable lesions.
A21 Merkel cell carcinoma of the skin
1. is an indolent ‘adnexal’ tumour resembling basal cell carcinoma in behaviour
2. histologically resembles ‘oat cell’ bronchial carcinoma
3. most commonly arises in axillae, groins or midline anterior abdominal skin
4. shows both neuroendocrine and epithelial differentiation by cell marker studies
2, 4 True; 1, 3 False
Robbins pays this cancer scant attention and considers it to be rare. Not in our experience - unusual
perhaps. It has a formidably aggressive biology, and morphologically resembles neuroendocrine
cancers elsewhere in the body (‘oat cell’ cancer, carcinoids in various sites, islet cell tumour etc). It is
most commonly present in head and neck (and extremities).
A22 Kaposi's sarcoma
1. arises in skin and usually remains confined to skin and subcutaneous tissue
2. is less biologically aggressive when it occurs in HIV-positive individuals
3. presents as reddish, spreading and merging papules and plaques in the skin
4. is a suppressor T lymphoproliferative disorder
3 True; 1, 2, 4 False
This tumour is of as yet undefined histogenesis. As seen up until about two decades ago in USA, this
was an indolent tumour of ageing men of Mediterranean origin. As part of the AIDS syndrome, it is an
aggressive skin neoplasm which fairly rapidly disseminates to the viscera. It is almost certainly an
endothelial sarcoma of some sort; certainly not a T lymphoma.
A23 Multiple endocrine neoplasia syndromes may threaten life because they may cause
1. hypertension
2. inappropriate ADH secretion
3. relentless peptic ulcer syndrome
4. 'malignant' thyrotoxicosis (thyrotoxic storm)
1, 3 True; 2, 4 False
Phaeochromocytoma is part of the variations on the theme of MEN II. Zollinger-Ellison syndrome is
part of MEN I. Inappropriate ADH secretion is seen with bronchial cancer (usually ‘oat cell’ or a
Ó Royal Australasian College of Surgeons – December 2000 Page 186 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
variant) or with hypothalamic pathology. Life-threatening thyrotoxicosis is seen only in Graves'
disease, which is not part of MEN.
A24 Carcinogenesis induced by DNA viruses
1. is usually a single step (‘single hit’) process
2. may act by neutralising growth-inhibiting molecules
3. may involve incorporation of viral oncogene into host DNA
4. may cause stimulation of function of growth-promoting protein(s)
2, 3, 4 True; 1 False
Each of items 2, 3 and 4 is correct under different circumstances and with various viruses. However
“… studies provide firm evidence that cancer, even when caused by highly oncogenic viruses, is a
multistep process”. This section of Robbins also deals with other important concepts of viral
oncogenesis eg the cell must survive the infection; early transcribed genes are essential for oncogenic
transformation, they are incorporated stably into the host cell genome (and subsequent generations)
and they interrupt the subsequent replication of the late viral genes, thus preventing assembly of the
complete virus.
A25 In follow-up of asymptomatic family members of a patient with medullary thyroid carcinoma associated
with multiple endocrine neoplasia syndrome (MEN II), effective screening tests include
1. plasma calcitonin levels
2. urinary catecholamine estimation
3. plasma calcium estimation
4. serum ionised calcium/phosphate ratio
1, 2 True; 3, 4 False
Despite the theoretical action of calcitonin on plasma ionised calcium, plasma calcium and phosphate
levels are normal in this syndrome, even in the presence of a calcitonin-secreting medullary cancer of
the thyroid with metastases. Urinary catecholamine determinations, on the other hand, will often
unearth an early phaeochromocytoma.
Ó Royal Australasian College of Surgeons – December 2000 Page 187 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A26 Papillary carcinoma of the thyroid
1. can be the result of childhood thyroid irradiation
2. may have lung metastases for many years
3. commonly presents clinically because of metastases
4. is biologically more aggressive, when the histology shows an admixture of papillary and follicular
growth patterns
1, 2, 3 True; 4 False
Papillary cancer follows childhood radiation like bills follow credit cards. There is no reason to feel
confident that this will not continue. This is an indolent cancer which has been likened in behaviour to
endometriosis; metastatic spread is extremely common, sometimes widespread (even to lungs, brain!
for many years) with minimal deterioration - however, needless to say, overall these are markers for
poorer prognosis. Over half of papillary carcinomas have admixtures of follicular growth. However,
long-term follow-up shows that ”… regardless of precise proportions, all neoplasms containing some
papillary areas have identical biologic behaviour …".
A27 RNA oncogenic viruses
1. are causally involved in the genesis of many human cancers
2. can convert normal host cell proto-oncogenes into oncogenes (c-oncogenes)
3. form templates for DNA transcription within the host cell
4. usually splice directly into host genome before activation
2, 3 True; 1, 4 False
Only human T cell leukaemia virus (HTLV-1) which is, like HIV, strongly tropic for T4/TH cells, has
been implicated in causing human cancer, although there are heaps of animal counterparts. They act
as oncogenic viruses by incorporating a copy DNA (ie. mirror image of virus RNA structure [response
3, but not 4]) into host genome. They can (indirectly) then activate host proto-oncogenes =
> c-oncogenes or possibly splice in a DNA copy identical to a host proto-oncogene into the wrong
place where it acts as a c-oncogene (eg too near an ‘activator’ gene or too distant from a
‘controller/suppressor’ gene).
Ó Royal Australasian College of Surgeons – December 2000 Page 188 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A28 Proto-oncogenes
1. are rendered incapable of transcribing growth-related proteins following chromosomal
translocation
2. are, in the normal cell, inactive DNA sequences without physiological action
3. may be activated into functional oncogenes (c-onco-genes) by mutation of a specific gene
site
4. may be activated by destruction of adjacent controller genes, which normally suppress
their action
3, 4 True; 1, 2 False
Response 1 is false; gene sequences may be activated (removed from a ‘suppressor’ or inserted near
an ‘activator’) by translocation. For response 2, proto-oncogenes are, in the normal cell, the activators
and switches (‘on’ and ‘off’) for normal growth. Responses 3 and 4 outline two of the ways in which
normal proto-oncogenes may be influenced to become oncogenes (also referred to as c-oncogenes).
[Cellular] oncogenes are perverted proto-oncogenes (growth genes).
A29 Familial retinoblastoma
1. is always a congenital neoplasm
2. is activated by chromosomal translocation
3. inheritance pattern is autosomal recessive
4. develops only in a retinoblast which has the appropriate DNA defect in both of the paired
chromosomes
4 True; 1, 2, 3 False
Familial retinoblastoma is inherited, but not necessarily congenital. The inheritance genetics is of a
single defective gene, which is protected by the paired gene in each retinoblast cell. However, all of
the retinoblasts are ‘primed’ by having one defective gene - mutation of the other gene in just one
retinoblast, removes all of that suppressor gene activity from that cell. If that retinoblast is still in the
‘replication pool’, retinoblastoma ensues; if that cell has matured to join the ranks of permanent cells
(differentiated), presumably cancer does not ensue.
Ó Royal Australasian College of Surgeons – December 2000 Page 189 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A30 Carcinogenic initiating agents are thought to produce their actions by their mutagenic effects
because carcinogenic initiation produces irreversible alterations in DNA chemistry in target
cells.
Answer: A (True; True; related)
Whether they act as complete, direct or indirect initiators, the action of carcinogenic initiators is
presumed to be because they cause permanent alteration to the DNA, by an action which is rapid and
irreversible. It also has ‘memory’, in that a threshold dose is effective when given either in a single
dose or as divided doses.
A31 DNA damage by chemicals is not necessarily carcinogenic because DNA damage can be
repaired by cellular enzyme systems.
Answer: A (True; True; related)
The written evidence for this statement and reason is, perhaps, not as direct as I would like. The
evidence for repair of DNA following radiation injury is very strong. Single strand breaks are rapidly
repaired (within minutes) and double strand breaks may also be repaired, usually less promptly.
Some are irreparable - these may lead to cell death or become the initial steps of oncogenesis. By
implication, the same should be true for chemicals, but a direct and definitive statement to this effect
cannot be found in Robbins.
A32 The effects of carcinogenic promoters are thought to be potentially reversible because
tumours do not eventuate if the ‘promoter-effective’ dose is applied prior to the application of
the appropriate initiator.
Answer: A (True; True; related)
Promoters are not electrophilic compounds and do not damage DNA. They induce clonal proliferation
of initiated cells and influence their differentiation programmes. They appear to bring about these
changes by the use of existing normal growth-promoting physiologic transduction pathways, not by
inducing new ones.
A33 The effects of carcinogenic initiators on DNA chemistry are reversible because tumours do not
eventuate if the subsequent promoter application is delayed.
Answer: E (False - False)
This is central to the ‘initiator’ and ‘promoter’ model. Initiation is rapid, irreversible and has ‘memory’:
ie application of the promoter by appropriate method and amount is equally effective whether it follows
Ó Royal Australasian College of Surgeons – December 2000 Page 190 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
application of the initiator immediately, or after a delay. The action of the promoter is, however,
potentially reversible as shown by the fact that divided doses of promoter cannot be separated by too
long an interval, or the promoter effect is lost: ie some form of repair has occurred between
applications of the promoter.
A34 Karyotype/chromosomal abnormalities are thought to be a primary event in development of
many human neoplasms because in certain types of human neoplasia, karyotype abnormality
is non-random and common in that tumour type.
Answer: A (True; True; related)
“ …Nonlethal genetic damage lies at the heart of carcinogenesis.” Robbins 6th Ed Chapter 8, page
277.
“ ... karyotypic alterations ... are found in many ... cancerous cells ... are gene changes present in all ?
...With each passing year, it becomes more certain that the malignant cells of most types of human
cancers have chromosomal abnormalities and ... defects are consistent … ”
The most common types of nonrandom structural abnormalities in tumour cells are:
(a) balanced translocations,
(b) chromosomal deletions, and
(c) cytogenetic manifestations of gene amplification.
Robbins 5th Edition, Chapter 7, page 258.
A35 Major karyotype/chromosomal abnormalities are not thought to be a primary event in human
neoplasms because in human neoplasms, any karyotype abnormalities are uncommon and always
variable within the same tumour type.
Answer: E (False - False)
See previous discussions.
A36 Gardner's syndrome is a clinically more sinister variant of familial polyposis coli (FPC)
because in Gardner's syndrome, colonic malignancies occur, on average, about one decade earlier
than when FPC occurs alone.
Answer: C (True - False)
Ó Royal Australasian College of Surgeons – December 2000 Page 191 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A37 Gardner's syndrome is a clinically more sinister variant of familial polyposis coli (FPC)
because aggressive neoplasms, other than colonic carcinoma, may determine mortality in
Gardner's syndrome.
Answer: A (True; True; related)
Because of co-existence of other ‘tumours’, Gardner’s syndrome has a deservedly sinister reputation.
The fatal problem in many of these patients becomes intra-abdominal fibromatosis which often follows
surgery for polyposis and may not be clinically obvious before this. Regarding the time onset of the
malignancies, there is no difference between those with and those without extra-colonic
manifestations.
A38 Testicular seminoma
1. when dissemination occurs, is usually first manifest by blood stream spread
2. is highly radiosensitive
3. when associated with raised plasma human chorionic gonadotrophin (HCG), shows no
different clinical behaviour
4. is the least aggressive of the testicular germ cell neoplasms
2, 3, 4 True; 1 False
Seminoma and ‘non-seminomatous germ cell tumours’ (NSGCT) are the clinically important testicular
tumours. Seminomas remain confined to the testis longer and typically metastasise to lymph nodes,
with blood spread occurring (when it does) as a later phenomenon. NSGCT metastasise earlier and
more frequently by blood stream. Seminomas are extremely radiosensitive whereas NSGCT are
radio-resistant. Significance of a positive HCG in some seminoma patients is unknown; it does not
alter the generally good prognosis for seminoma.
A39 Likelihood of infections in advanced, untreated myeloma is contributed to by
1. reduced levels of normal (non-myeloma) immunoglobulins
2. high rate of infection by low-grade ('opportunistic') pathogens
3. depression of cellular (T cell) immunity
4. progressive, unrelenting viral infections
1 True; 2, 3, 4 False
The raised total level of plasma immunoglobulins is predominantly due to the monoclonal tumour-
manufactured Ig (which is, protectively speaking, 'nonsense Ig'). The infections which pose the threat
to life are, therefore, the 'usual' pyogenic infections for which adequate protection is lost. T-cell
Ó Royal Australasian College of Surgeons – December 2000 Page 192 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
immunity is well conserved and so the relentlessly progressive viral infections which are characteristic
of depressed T-cell function are not a feature of myeloma.
A40 Precursor lesions of colonic adenocarcinoma include
1. hyperplastic polyps
2. Peutz-Jegher polyps
3. adenomatous polyps
4. juvenile polyps
3 True; 1, 2, 4 False
The usual small hyperplastic polyp has virtually no malignant potential. Large hyperplastic polyps
occasionally contain foci of admixed adenoma - as may any part of the colonic mucosa; the
‘hyperplastic’ component is considered to be innocuous. Adenomatous polyps are on the ‘normal
mucosa to adenoma to carcinoma’ trail and have already undergone the initial mutation(s) which will
occur progressively if carcinoma is to eventually develop. The other two polyps are examples of
hamartoma (responses 2 and 4) and have no known pre-malignant potential.
A41 Colonic epithelial neoplasia is considered as not having significant metastatic potential if adequate
histological examination shows
1. adenoma with carcinoma in situ
2. adenoma showing severe epithelial dysplasia with focal intramucosal carcinoma
3. adenocarcinoma, invasive into submucosa only
4. invasive adenocarcinoma to superficial muscularis propria, without demonstrable vascular or
lymphatic permeation
1, 2 True; 3, 4 False
Carcinoma in situ is still, for pragmatic purposes, a benign lesion. It has not yet acquired the attributes
which will cause metastasis. Because lymphatic channels are largely absent from colonic mucosa,
intramucosal carcinoma is regarded as having little or no metastatic potential. Invasion into
submucosa indicates adenocarcinoma which has now acquired metastatic potential - real in all cases.
Likewise for response (4).
Ó Royal Australasian College of Surgeons – December 2000 Page 193 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A42 Most colorectal carcinomas
1. arise within pre-existing adenomas
2. occur in the absence of pre-existing ulcerative colitis or familial adenomatous polyposis
syndrome
3. present clinically in individuals under age 55 years
4. arise in the distal 15 cm of colon/rectum
1, 2 True; 3, 4 False
Colonic adenomas are premalignant and most adenocarcinomas arise from pre-existing adenomas -
the larger the adenoma, the greater the risk that adenocarcinoma has developed in it. Less than 5%
of cases of colorectal cancer arise in the setting of pre-existing familial adenomatous polyposis or
inflammatory bowel disease - responses (1 and 2) are correct. Peak incidence for colorectal
carcinoma is 60-70 years ie the incidence increases with increasing age. Less than 25% are located
in the rectosigmoid and this trend of higher incidence of proximal involvement is more prevalent in
Australasia.
A43 Most carcinomas of the gallbladder
1. are squamous or adenosquamous carcinomas
2. present clinically with pain plus an enlarged gallbladder
3. have invaded the liver at the time of operation
4. are always associated with presence of gall bladder calculi
3 True; 1, 2, 4 False
Most cancers of the gallbladder are adenocarcinomas. Clinical presentation is typically insidious and
indistinguishable from the symptoms and signs of benign gallbladder disease - palpable enlargement
of the gallbladder is distinctly unusual. According to Robbins, 60-90% of carcinoma of the gallbladder
is associated with gallstones - the point is that there is a very significant incidence of cases occurring
without gallstones and the overall incidence of gallbladder carcinoma in patients with gallstones is so
low that prophylactic cholecystectomy for gallstones is considered unjustified. By the time these
cancers are discovered, most have invaded the liver.
Ó Royal Australasian College of Surgeons – December 2000 Page 194 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
A44 Carcinoma of the extrahepatic bile ducts
1. in most cases does not cause palpable gallbladder enlargement
2. has a prognostic outlook similar to that of colonic carcinoma
3. is curably resectable in most instances
4. commonly causes obstructive jaundice
1, 4 True; 2, 3 False
Only approximately 25% of patients have palpable gallbladder, but obstructive jaundice is the rule,
often with stool decolourisation. The majority of ductal cancers are not resectable at the time of
diagnosis, despite their small size; mean survival times range from 6 to 18 months, no matter what the
treatment given; this is in sharp contrast to the considerably superior survival rates for colonic cancer.
A45 Clinical manifestations/complications of renal adenocarcinoma may include
1. amyloidosis
2. polycythaemia
3. fever and cachexia
4. hypercalcaemia
1, 2, 3, 4 True
Renal adenocarcinoma is a rich source of ‘paraneoplastic’ syndromes and of syndromes relating more
directly to some of the legitimate endocrine functions of the kidney. Polycythaemia is a classical
association with renal carcinoma (5-10% incidence) and this neoplasm is one of the group which
produces hypercalcaemia (even in the absence of bone metastases at times, but particularly in
association with tumour osteolysis). It is one of the classical causes of ‘pyrexia of uncertain cause’
and is the major cancer apart from myeloma which causes amyloidosis (but of the AA type, not AL).
A46 With adenocarcinoma of the prostate
1. there is good correlation between tumour differentiation and prognosis
2. early haematogenous visceral metastatic dissemination is common
3. lymph node metastases are unusual
4. local extension commonly involves seminal vesicles
1, 4 True; 2, 3 False
The Gleason staging system is best known; in prostatic carcinoma there is generally fairly good
correlation between prognosis and degree of differentiation; grading is therefore considered to be of
considerable importance. Local extension to involve seminal vesicles and base of bladder is common.
Lymph node metastases are common and often this mode of dissemination precedes spread to the
Ó Royal Australasian College of Surgeons – December 2000 Page 195 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
bones. When haematogenous spread occurs, it is very commonly confined at first to the axial
skeleton. Massive visceral dissemination is unusual.
A47 In cases of prostatic carcinoma
1. raised plasma prostate-specific antigen (PSA) level is a reliable marker for disease in
asymptomatic men
2. plasma prostate-specific antigen (PSA) levels correlate well with total tumour volume
3. most patients, at presentation with symptomatic disease, have carcinoma which is localised within
the gland
4. haematogenous spread occurs chiefly to bone
2, 4 True; 1, 3 False
PSA is of value in diagnosis and management of prostatic cancer. PSA levels correlate well with total
tumour volume. However, PSA levels are also raised in prostatic hyperplasia and, because of overlap
between levels found in hyperplasia and in early and localised cancer, PSA alone cannot be used for
the reliable detection of early cancer. More than 75% of patients have advanced prostatic cancer
when diagnosed. When haematogenous spread occurs, it is chiefly to the axial skeleton and
produces predominantly osteoblastic metastases.
A48 Carcinomas develop through ‘dedifferentiation’ of normal, differentiated, cells because carcinomas
result from repression of normal gene activity in differentiated, mature cells which revert to ‘immature’
cells.
Answer: E (Incorrect - Incorrect)
Cancers arise from mutations in the DNA of cells. Such mutations will not induce growth in terminally
differentiated cells which are not undergoing proliferation (ie are not dividing). There is general
agreement that most, if not all, clinical cancers are the result of multiple mutations occurring
sequentially in a clone of proliferating cells ie stem cells from which the resident cell population of the
particular tissue derives its adult cell population.
A49 Genes controlling apoptosis such as p53 are believed to be important in controlling/preventing
growth of potential cancer cells because ‘apoptosis genes’ arrest the mitotic process of cells
with DNA damaged by mutagenic agents which allows time for DNA repair or, if repair does not
occur, induces cell autodestruction.
Answer: A (Correct - Correct - related)
There is no evidence that p53 gene expression is necessary for normal cell division. Once cells are
exposed to mutagenic agents such as chemicals or radiation, the p53 protein (normally with very short
Ó Royal Australasian College of Surgeons – December 2000 Page 196 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
half-life) is stabilised and accumulates in the nucleus, where it binds to DNA, causing cells to arrest in
the G1 phase. This allows time for DNA repair mechanisms to work. If this does not occur, the cell
undergoes apoptotic death. p53 is widely active and has been dubbed ‘guardian of the genome’.
A50 Oncogenic viruses all contain oncogenes which are virtually or actually identical with proto-oncogenes
present in normal cells because cancer-causing viruses are oncogenic only because of the actions of
proto-oncogene- homologous DNA.
Answer: E (Incorrect - Incorrect)
Some oncogenic DNA viruses do contain DNA sequences which have close homology with normal
proto-oncogenes. However, there are other ways by which oncogenic viruses influence the
proliferative activity of the cell. For example, translocation may separate a proto-oncogene from its
controlling suppressor gene or may relocate a proto-oncogene gene (usually normally controlled)
adjacent to a promoter gene (eg EBV in causation of lymphoma). RNA viruses do not contain DNA
and so cannot ‘contain’ oncogenes per se! It is true that they cause transcription of cDNA which may
function as a c-oncogene.
A51 Oncogenesis probably involves multiple sequential DNA mutations before neoplastic
behaviour develops because all human cancers which have been analysed in detail have been
found to have mutations which involve both activation of promoter genes and loss of cancer
suppressor genes.
Answer: A (Correct - Correct - related)
“Every human cancer that has been analysed reveals multiple genetic alterations involving activation
of several oncogenes and loss of two or more cancer suppressor genes. Each of these alterations
represents a crucial step in the progression from a normal cell to a malignant tumour.” - Robbins.
Robbins also quotes the evidence relating to one or more ‘master mutator genes’ which may point to
some overall control (or, more specifically, its loss) of mutation. Note here the APC gene which
appears to regulate or influence mutations at hundreds (at least) of other loci.
A52 Acquisition of the characteristics of ability to metastasise by cancer cells is presumed to be
dependent on multiple different mutations in the cells because no single gene has thus far
been discovered which appears to code for metastasising behaviour by neoplastic cells.
Answer: A (Correct - Correct - related)
At present, no single ‘metastasis gene’ has been discovered. It is thought that such a ‘master gene’
influencing metastatic (or, indeed, invasive) behaviour is unlikely, because each of these activities
Ó Royal Australasian College of Surgeons – December 2000 Page 197 of 198
STEM MODULE: GENERAL PRINCIPLES OF PATHOLOGY
involves multiple, apparently individual, processes (eg adhesion, secretion of extracellular matrix-
digesting enzymes, locomotion etc). However, some experimental evidence does exist that some
genes act to specifically suppress one or more properties which are essential for metastasis. There is
some tantalising evidence that one such gene may operate in modulating metastasis behaviour in
human breast cancer.
Q53 The commonest cause of death in multiple myeloma is
A. renal failure
B. amyloid-related multiple organ failure
C. intestinal infarction due to hyperviscosity syndrome
D. infections by pyogenic bacteria
E. cardiac arrhythmia due to hypercalcaemia
Answer: D True
What’s to add? The specific immunoglobulin lack (not only the lack of ability to make ‘new’
immunoglobulins to combat infections with ‘new’ invaders, but loss of adequate levels from previous
infections) leads to particular susceptibility to infections with encapsulated bacteria (eg pneumococci).
All of the others are hazards for patients with multiple myeloma, but pyogenic infections are the
commonest killer.
Ó Royal Australasian College of Surgeons – December 2000 Page 198 of 198
You might also like
- Mechanisms of Inflammation I, II, and III LOsDocument9 pagesMechanisms of Inflammation I, II, and III LOsAndrew SagalovNo ratings yet
- Inflammation and RepairDocument21 pagesInflammation and RepairlolNo ratings yet
- Abd 91 05 0614Document7 pagesAbd 91 05 0614Selvy Anriani GasperszNo ratings yet
- 4 Chronic Inflammation IDocument38 pages4 Chronic Inflammation IAlex XanderNo ratings yet
- Acute and Chronic Inflammation: Yacob Alemu (MD) May 2021Document89 pagesAcute and Chronic Inflammation: Yacob Alemu (MD) May 2021Tazeb AyeleNo ratings yet
- InflammationDocument85 pagesInflammationUmmi Rinandari100% (2)
- Inflammation (Acute and Chronic) - StudentDocument61 pagesInflammation (Acute and Chronic) - StudentSaubie AslamiahNo ratings yet
- Ackerman, 2017Document1 pageAckerman, 2017intansofiairsaNo ratings yet
- Glomerulonephritis Guide for International StudentsDocument43 pagesGlomerulonephritis Guide for International StudentsNosirova ManijaNo ratings yet
- Path1 3Document109 pagesPath1 3Abid KhanNo ratings yet
- Sterile Inflammation - Sensing andDocument12 pagesSterile Inflammation - Sensing andJOHN HELIBERTH ANDREY TORRES GRANADOSNo ratings yet
- Markers of Inflammation: Dori R. Germolec, Kelly A. Shipkowski, Rachel P. Frawley, and Ellen EvansDocument23 pagesMarkers of Inflammation: Dori R. Germolec, Kelly A. Shipkowski, Rachel P. Frawley, and Ellen EvansTiến Đạt NguyễnNo ratings yet
- Session 2Document65 pagesSession 2kasper mkNo ratings yet
- Basic PathologyDocument71 pagesBasic Pathologycocopandanenak100% (1)
- The Roles of in Ammation in Keloid and Hypertrophic ScarsDocument10 pagesThe Roles of in Ammation in Keloid and Hypertrophic ScarsireneardianiNo ratings yet
- Suptipos de SepsisDocument17 pagesSuptipos de SepsisoswaldoninaNo ratings yet
- Patologis Radang Akut Dan KronikDocument13 pagesPatologis Radang Akut Dan Kronikwiena nadellaNo ratings yet
- Chronic Inflammation 1: DR Nahiid StephensDocument46 pagesChronic Inflammation 1: DR Nahiid Stephensmelinda0% (1)
- Wound Healing and Its Impairment in The Diabetic Foot: ReviewDocument9 pagesWound Healing and Its Impairment in The Diabetic Foot: ReviewJoey TsaiNo ratings yet
- 1 s2.0 S0749070421001019 MainDocument17 pages1 s2.0 S0749070421001019 MainEliseu AmaralNo ratings yet
- Acute appendicitis, pneumonia, tuberculosis and other medical quiz diagnosesDocument23 pagesAcute appendicitis, pneumonia, tuberculosis and other medical quiz diagnoses182 ROHIL HNo ratings yet
- Surgery I Block 4 Super Reviewer PDFDocument14 pagesSurgery I Block 4 Super Reviewer PDFlems9No ratings yet
- BR J Dermatol - 2022 - Dissemond - Inflammatory Skin Diseases and WoundsDocument11 pagesBR J Dermatol - 2022 - Dissemond - Inflammatory Skin Diseases and Woundsวสุชล ชัยชาญNo ratings yet
- T Lymphocyte Exhaustion During Human and Experimental Visceral LeishmaniasisDocument15 pagesT Lymphocyte Exhaustion During Human and Experimental Visceral LeishmaniasisLuis Carlos Calvanapon TerronesNo ratings yet
- L08: Inflammation (Acute and Chronic), Healing, Repair and OsteomyelitisDocument9 pagesL08: Inflammation (Acute and Chronic), Healing, Repair and Osteomyelitishstest842No ratings yet
- Chapter 6 - Inflammation, Tissue Repair & FeverDocument8 pagesChapter 6 - Inflammation, Tissue Repair & FeverChrista CastorNo ratings yet
- Inflammation and Repair: Definition of Inflammation Acute Inflammation Vascular Events in InflammationDocument35 pagesInflammation and Repair: Definition of Inflammation Acute Inflammation Vascular Events in InflammationSoji AdimulaNo ratings yet
- Journal of International Medical Research-2009-Velnar-1528-42Document16 pagesJournal of International Medical Research-2009-Velnar-1528-42angelica najeraNo ratings yet
- Inflammasi - 2: Nunuk Purwanti Biomedika Kedokteran GigiDocument41 pagesInflammasi - 2: Nunuk Purwanti Biomedika Kedokteran GigiMonica Abigail Wohing AtiNo ratings yet
- Robbins & Cotran Pathologic Basis of Disease - With STUDENT CONSULT Online Access, 8e (PDFDrive - Com) - 89-105Document17 pagesRobbins & Cotran Pathologic Basis of Disease - With STUDENT CONSULT Online Access, 8e (PDFDrive - Com) - 89-105bgfhnfgNo ratings yet
- Immunology of Periodontal DiseasesDocument9 pagesImmunology of Periodontal DiseasesoladunniNo ratings yet
- Unit 4.1Document8 pagesUnit 4.1Bloody MarieNo ratings yet
- 2019 - Malignant Transformation in Diabetic Foot UlcersDocument14 pages2019 - Malignant Transformation in Diabetic Foot UlcersAnca Catalina MunteanuNo ratings yet
- (24508608 - Journal of Veterinary Research) Mechanisms of Tumour Escape From Immune SurveillanceDocument8 pages(24508608 - Journal of Veterinary Research) Mechanisms of Tumour Escape From Immune Surveillancekalppena naiduNo ratings yet
- Inflammation Repair PTDocument41 pagesInflammation Repair PTMarili Camille CoquiaNo ratings yet
- Cellular Responses to InjuryDocument110 pagesCellular Responses to InjuryJustine Nicole Clavel LachicaNo ratings yet
- Referat - CHRONIC WOUNDDocument19 pagesReferat - CHRONIC WOUNDAfifah Syifaul UmmahNo ratings yet
- Inflammation and Chemical MediatorDocument58 pagesInflammation and Chemical MediatorMadhura ShekatkarNo ratings yet
- Inflammation and RepairDocument77 pagesInflammation and RepaironyekaNo ratings yet
- Introduction to Cellular PathologyDocument11 pagesIntroduction to Cellular PathologyPhil HuseyNo ratings yet
- Module 4 Chronic InflammationDocument34 pagesModule 4 Chronic InflammationAllan SigangaNo ratings yet
- Immune Response in The Skin of AgingDocument7 pagesImmune Response in The Skin of AgingInmunoBlogNo ratings yet
- Inflammation Seminar OverviewDocument19 pagesInflammation Seminar OverviewDrGurinder Kanwar100% (1)
- Pathology InflammationDocument111 pagesPathology InflammationAlyssa ArroyoNo ratings yet
- WOUND HEALING: A COMPLEX PROCESSDocument35 pagesWOUND HEALING: A COMPLEX PROCESSGayathri MaigandanNo ratings yet
- Summer of Patho.t PDFDocument10 pagesSummer of Patho.t PDFحسن محمد سعيد جاسمNo ratings yet
- InflammationDocument35 pagesInflammationSajjad AliNo ratings yet
- Chronic Inflammation Causes, Features and EffectsDocument24 pagesChronic Inflammation Causes, Features and EffectsTommys100% (1)
- Chronic Inflammation 1Document14 pagesChronic Inflammation 1Nayela AkramNo ratings yet
- Tissue Injury and Healing: Brent Kincaid, DDS, John P. Schmitz, DDS, PHDDocument10 pagesTissue Injury and Healing: Brent Kincaid, DDS, John P. Schmitz, DDS, PHDAmith HadhimaneNo ratings yet
- Jcad 13 2 33Document11 pagesJcad 13 2 33ntnquynhproNo ratings yet
- Immune Complex Diseases PathogenesisDocument11 pagesImmune Complex Diseases PathogenesisBryan AmataNo ratings yet
- Management of Head and Neck Infections in The PDFDocument8 pagesManagement of Head and Neck Infections in The PDFVijay TiwariNo ratings yet
- Multiple Organ Dysfunction SyndromeDocument21 pagesMultiple Organ Dysfunction SyndromeRo-Anne LozadaNo ratings yet
- Patho 4Document9 pagesPatho 4ambiliNo ratings yet
- Acute InflammationDocument71 pagesAcute Inflammationsi_miaomiao100% (1)
- Cell Stress, Inflammatory Responses and Cell Death: SynopsisDocument29 pagesCell Stress, Inflammatory Responses and Cell Death: SynopsisSasa PuiuNo ratings yet
- Fibrosis Hepática e InflamaciónDocument5 pagesFibrosis Hepática e InflamaciónMartha Antoane Orbegoso GamonalNo ratings yet
- Guideline For Emergency Oxygen Use in Adult Patients: Executive SummaryDocument12 pagesGuideline For Emergency Oxygen Use in Adult Patients: Executive SummaryAnne MarieNo ratings yet
- Year 3 OSCE ProcedureDocument2 pagesYear 3 OSCE ProcedureAbid KhanNo ratings yet
- GAMSAT Information Booklet SepDocument40 pagesGAMSAT Information Booklet SepAbid KhanNo ratings yet
- Examination of Sensory TestingDocument2 pagesExamination of Sensory TestingAbid KhanNo ratings yet
- 2015 - Topic Notes Mol Genetics 141 PagesDocument165 pages2015 - Topic Notes Mol Genetics 141 PagesAbid KhanNo ratings yet
- MicrobiologyDocument5 pagesMicrobiologyAbid KhanNo ratings yet
- Organic Chemistry ReactionsDocument21 pagesOrganic Chemistry ReactionsAbid KhanNo ratings yet
- Discussion of Microbiological TestingDocument4 pagesDiscussion of Microbiological TestingAbid Khan100% (1)
- T3 ExamDocument2 pagesT3 ExamAbid KhanNo ratings yet
- Organic Chemistry ReactionsDocument21 pagesOrganic Chemistry ReactionsAbid KhanNo ratings yet
- Goldfinger Human Anatomy For Artists PDFDocument4 pagesGoldfinger Human Anatomy For Artists PDFSamuelNo ratings yet
- VPB 111Document3 pagesVPB 111Dr-Ashok KeerNo ratings yet
- Histology - The Microscopic Anatomy and Function of Tissues and OrgansDocument423 pagesHistology - The Microscopic Anatomy and Function of Tissues and Organsdorina0101100% (1)
- The Cardiovascular System: Lecture Presentation by Patty Bostwick-Taylor Florence-Darlington Technical CollegeDocument124 pagesThe Cardiovascular System: Lecture Presentation by Patty Bostwick-Taylor Florence-Darlington Technical Collegelourd nabNo ratings yet
- Laennecs Cirrhosis PathophysiologyDocument2 pagesLaennecs Cirrhosis PathophysiologyTrixie Al Marie100% (3)
- Medical Terminology Roots and SuffixesDocument7 pagesMedical Terminology Roots and SuffixesJessiree Joyce Layosa RaganitNo ratings yet
- Reading-The Human HeartDocument4 pagesReading-The Human HeartMichelle ViafaraNo ratings yet
- EmfizemulDocument19 pagesEmfizemulMirela IoanaNo ratings yet
- HepatoblastomaDocument6 pagesHepatoblastomaNurul IzzatiNo ratings yet
- Bone Patology PDFDocument12 pagesBone Patology PDFLuis Humberto Padilla VazquezNo ratings yet
- Vpat 101:: Veterinary General PathologyDocument4 pagesVpat 101:: Veterinary General PathologyHarleanne ParkNo ratings yet
- Detailed Lesson Plan Reproductive SystemDocument12 pagesDetailed Lesson Plan Reproductive SystemMau Acusa100% (1)
- Shivanshu Gangwar M. Pharma (Pharmaceutics)Document16 pagesShivanshu Gangwar M. Pharma (Pharmaceutics)Shibbu GangwarNo ratings yet
- Unit I - Lecture Notes - Body OrganizationDocument8 pagesUnit I - Lecture Notes - Body OrganizationSteve Sullivan100% (3)
- Eczema - Final Thesis Edited 22.8.09Document152 pagesEczema - Final Thesis Edited 22.8.09579Rishikesh SavardekarNo ratings yet
- Anatomy & Physiology 1 Chapter 9 The Nervous System Flashcards - QuizletDocument7 pagesAnatomy & Physiology 1 Chapter 9 The Nervous System Flashcards - Quizletmalenya1100% (1)
- MB115 2020 Final Exam 2020Document26 pagesMB115 2020 Final Exam 2020Milimo MweembaNo ratings yet
- 10 Science Imp ch6 Mix2Document5 pages10 Science Imp ch6 Mix2Anush ShettigarNo ratings yet
- Cleavage: Types and PatternsDocument15 pagesCleavage: Types and PatternstrivikramraoNo ratings yet
- Blood Grouping Reagents and Anti Human Globulin Reagents - Seraclone - Package Insert - Ani IgGDocument2 pagesBlood Grouping Reagents and Anti Human Globulin Reagents - Seraclone - Package Insert - Ani IgGأنا الجفاNo ratings yet
- Instruments Tajimaco CatalogDocument4 pagesInstruments Tajimaco CatalogFandi AhmadNo ratings yet
- Pathology INI CET 2020Document35 pagesPathology INI CET 2020pathikNo ratings yet
- Coordination and Control in the Human BodyDocument37 pagesCoordination and Control in the Human Bodywardah nooriNo ratings yet
- NEET Chemical Control and Coordination Important QuestionsDocument14 pagesNEET Chemical Control and Coordination Important QuestionsAditiNo ratings yet
- Pathophysiology of Hansen's DiseaseDocument1 pagePathophysiology of Hansen's DiseaseGrace Lyn Borres ImpasNo ratings yet
- Lymphatics of ThoraxDocument29 pagesLymphatics of ThoraxconovastyleNo ratings yet
- Sympathetic Receptors and Their ResponsesDocument3 pagesSympathetic Receptors and Their Responsesjulinka beyla yansonNo ratings yet
- Pregnancy Doubles (Gemelli)Document15 pagesPregnancy Doubles (Gemelli)Hengky HanggaraNo ratings yet
- Osmosis 41Document1 pageOsmosis 41Sarawini KosolsombatNo ratings yet
- Glomerular DiseasesDocument211 pagesGlomerular DiseasesAdrián Beltrán67% (3)