Professional Documents
Culture Documents
+lymphoedema 150118110815 Conversion Gate02
Uploaded by
Oussama A0 ratings0% found this document useful (0 votes)
8 views24 pages+lymphoedema
Original Title
+lymphoedema-150118110815-conversion-gate02
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document+lymphoedema
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
8 views24 pages+lymphoedema 150118110815 Conversion Gate02
Uploaded by
Oussama A+lymphoedema
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 24
LYMPHOEDEMA
• Lymphoedema may be defined as
abnormal limb swelling caused by the
accumulation of increased amounts of
high protein ISF secondary to defective
lymphatic drainage in the presence of
(near) normal net capillary filtration.
Risk factors:
Upper limb/trunk lymphoedema
• Surgery for lymph node dissection. Breast surgey.
• Radiotherapy to breast or to axilary, im or subclaviclar
lymph nodes.
• Wound complications
• Cancer
• Obesity
• Hypertension
• Chronic skin disorders
• Air travel
• Congenital predisposition
Lower limb lymphoedema
• Obesity
• Varicose vein stripping
• Advance cancer
• Orthopedic surgery
• Surgery with inguinal lymph node dissection
• Postoperative pelvic radiotherapy
• Genetic predisposition/family history of chronic
oedema
• Thrombophlebitis and chronic venous
insufficiency
Symptoms and signs
• Constant dull ache, even severe pain
• Burning and bursting sensations
• General tiredness and debility
• Sensitivity to heat
• ‘Pins and needles’
• Cramp
• Skin problems including flakiness, weeping, excoriation
and breakdown
• Immobility, leading to obesity and muscle wasting
• Backache and joint problems
• Athlete’s foot
• Acute infective episodes
• Toes become “square” shaped
• Stemmer’s sign
Classification
• Primary lymphoedema, in which the cause
is unknown (or at least uncertain and
unproven); it is thought to be caused by
‘congenital lymphatic dysplasia’
• Secondary or acquired lymphoedema, in
which there is a clear underlying cause.
Clinical classification
PRIMARY LYMPHOEDEMA
• all cases of primary lymphoedema are due
to an inherited abnormality of the
lymphatic system, sometimes termed
‘congenital lymphatic dysplasia’.
• Primary lymphoedema is much more
common in the legs than the arms.
Classification
• Congenital (onset < 2 years old): sporadic;
familial (Nonne–Milroy’s disease)
• Praecox (onset 2–35 years old): sporadic;
familial (Letessier–Meige’s disease)
• Tarda (onset after 35 years old)
SECONDARY LYMPHOEDEMA
• This is the most common form of
lymphoedema. There are several well-
recognised causes including infection,
inflammation, neoplasia and trauma
INVESTIGATION OF
LYMPHOEDEMA
• ‘Routine’ tests
• Lymphangiography
• Isotope lymphoscintigraphy
• Computerised tomography
• Magnetic resonance imaging
• Ultrasound
• Pathological examination
MANAGEMENT OF LYMPHOEDEMA
Initial evaluation of the patient with lymphoedema
• History (age of onset, location, progression, exacerbating
and relieving features)
• Past medical history including cancer history
• Family history
• Obesity
• Complications (venous, arterial, skin, joint, neurological,
malignant)
• Assessment of physical, emotional and psychosocial
symptoms
• Social circumstances (mobility, housing, education, work)
• Special needs (footwear, clothing, compression garments)
• Previous and current treatment
• Pain control
• Compliance with therapy and ability to self-care
• Relief of pain
• Control of swelling
– Decongestive lymphoedema therapy (DLT),
• Intensive phase :
– Skin care
– Manual lymphatic drainage
– Multilayer lymphoedema bandaging and
compression garments
– Exercise
• Maintainence phase
Surgery
• Only a small minority of patients with lymphoedema
benefit from surgery. Operations fall into two categories:
• Bypass procedures
– The rare patient with proximal ilioinguinal lymphatic
obstruction and normal distal lymphatic channels
might benefit, at least in theory, from lymphatic
bypass.
• Limb Reduction procedures.
– Sistrunk
– Homans
– Thompson
– Charles
You might also like
- Lymphedema 13Document16 pagesLymphedema 13Iqra RazzaqNo ratings yet
- Surgery Seminar-2: Serial Numbers: 132,148,190Document38 pagesSurgery Seminar-2: Serial Numbers: 132,148,190Arhaan MohammedNo ratings yet
- Emily Iker, MD: LymphedemaDocument37 pagesEmily Iker, MD: LymphedemaJustin HarperNo ratings yet
- Lymphatic Disorders: DR - Rehab GwadaDocument30 pagesLymphatic Disorders: DR - Rehab GwadaMohamed ElMeligieNo ratings yet
- Disorders of The Lymphatic SystemDocument37 pagesDisorders of The Lymphatic SystemJSeasharkNo ratings yet
- Limfoma PPT MonceDocument65 pagesLimfoma PPT MonceSylvia PertiwiNo ratings yet
- Nicole Baldridge, PT, DPT, CLTDocument76 pagesNicole Baldridge, PT, DPT, CLTAan AlawiyahNo ratings yet
- Lymphedema Lecture - PowerPoint.keyDocument59 pagesLymphedema Lecture - PowerPoint.keyCristina Klymasz100% (1)
- Penyakit VenaDocument37 pagesPenyakit VenaSarah JR Nur AzizahNo ratings yet
- Idk 9 LimfademaDocument16 pagesIdk 9 LimfademaKartika YuliantiNo ratings yet
- Vascular Diseases: Kibrom Gebreselassie, MD, FCS-ECSA Cardiovascular and Thoracic SurgeonDocument57 pagesVascular Diseases: Kibrom Gebreselassie, MD, FCS-ECSA Cardiovascular and Thoracic SurgeonVincent SerNo ratings yet
- Pediatric Ent MalignanciesDocument69 pagesPediatric Ent MalignanciesKita kitaNo ratings yet
- Lymphedema IngDocument63 pagesLymphedema IngRio PotterNo ratings yet
- Unilateral Leg Swelling 1Document67 pagesUnilateral Leg Swelling 1maryam tariqNo ratings yet
- Week 3- Breast Cancer and LymphedemaDocument75 pagesWeek 3- Breast Cancer and Lymphedemamemoona kaleemNo ratings yet
- DermatologyDocument223 pagesDermatologySahan EpitawalaNo ratings yet
- Oedema PathophysiologyDocument10 pagesOedema PathophysiologyAudrey100% (6)
- The Skin in commonly encountered systemic diseasesDocument42 pagesThe Skin in commonly encountered systemic diseasesrainmaker77771121No ratings yet
- Listeriosis - O&G SeminarDocument17 pagesListeriosis - O&G SeminarFaris Mohd NasirNo ratings yet
- Overview of LymphomasDocument44 pagesOverview of LymphomasHarsha MaheshwariNo ratings yet
- Vitamin B12 or folate deficiencyDocument86 pagesVitamin B12 or folate deficiencyShaun TanNo ratings yet
- Blood Disorders - LeukemiaDocument24 pagesBlood Disorders - LeukemiaanreilegardeNo ratings yet
- SarcoidosisDocument95 pagesSarcoidosisvnybhagat100% (2)
- Lymphadenopathy OmfsDocument17 pagesLymphadenopathy OmfsAnirutha AnnaduraiNo ratings yet
- Lesson 3 Organ Speecific CancersDocument78 pagesLesson 3 Organ Speecific Cancersmaryelle conejarNo ratings yet
- Vulvar Disease Classification and Treatment GuideDocument28 pagesVulvar Disease Classification and Treatment GuideHervis FantiniNo ratings yet
- Perioperative Care 2Document28 pagesPerioperative Care 2Worku KifleNo ratings yet
- Leukocyte DisordersDocument55 pagesLeukocyte DisordersSherlyn Yee100% (1)
- Infectious Disease: Syphilis: Dessa AlbaricoDocument25 pagesInfectious Disease: Syphilis: Dessa AlbaricoAnnbe BarteNo ratings yet
- Alterations in Hematologic System Health: Lymphoma, Hodgkin's LymphomaDocument12 pagesAlterations in Hematologic System Health: Lymphoma, Hodgkin's LymphomaKelly HollenbeakNo ratings yet
- Teaching Case Presentation 2Document20 pagesTeaching Case Presentation 2api-347034408No ratings yet
- Neoplastic White Blood Cell Disorders: Leukemias, Lymphomas and MyelomaDocument45 pagesNeoplastic White Blood Cell Disorders: Leukemias, Lymphomas and MyelomayalahopaNo ratings yet
- Understanding Lymphoma: Causes, Types, Symptoms and TreatmentDocument46 pagesUnderstanding Lymphoma: Causes, Types, Symptoms and Treatmentshapan biswaNo ratings yet
- Differential Diagnosis of Lymphadenopathy in ChildrenDocument21 pagesDifferential Diagnosis of Lymphadenopathy in ChildrenAnaNo ratings yet
- Deep Venous Thrombosis: Farouq Muhammad 6-10-11Document59 pagesDeep Venous Thrombosis: Farouq Muhammad 6-10-11farouqmuhdNo ratings yet
- Lymphomas: Dr. Y.A. AdelabuDocument28 pagesLymphomas: Dr. Y.A. Adelabuadamu mohammadNo ratings yet
- Varicose Veins Treatment OptionsDocument49 pagesVaricose Veins Treatment OptionsYuli Setio Budi PrabowoNo ratings yet
- Lymphadenopathy in Children: Diagnosis and Treatment ApproachDocument45 pagesLymphadenopathy in Children: Diagnosis and Treatment ApproachmiauNo ratings yet
- LYMPHEDEMADocument4 pagesLYMPHEDEMAFrnz RiveraNo ratings yet
- 9475-Jurnal Keperawatan Terapan Vol 2 No 2 September 2016 Pengaruh Batik EfektifDocument8 pages9475-Jurnal Keperawatan Terapan Vol 2 No 2 September 2016 Pengaruh Batik EfektifNYONGKERNo ratings yet
- The Skin and Systemic DiseaseDocument36 pagesThe Skin and Systemic DiseaseAhmad AltarefeNo ratings yet
- Peripheral Vascular DiseaseDocument32 pagesPeripheral Vascular DiseaseShy PatelNo ratings yet
- Hodgkin LymphomaDocument34 pagesHodgkin Lymphomaroohi khanNo ratings yet
- Cardiomyopathy & Lvad: Presenter: Ms Elby JohnDocument43 pagesCardiomyopathy & Lvad: Presenter: Ms Elby JohnajishNo ratings yet
- Blood Analysis NormalDocument3 pagesBlood Analysis NormalearNo ratings yet
- (K25) Path - Musculosceletal FK Part 2Document69 pages(K25) Path - Musculosceletal FK Part 2Virginia JawaNo ratings yet
- GangreneDocument44 pagesGangreneAkshat SrivastavaNo ratings yet
- Lymphoreticular FinalDocument42 pagesLymphoreticular FinalNafis Fuad SheikhNo ratings yet
- Arterial Disease SurgicalDocument43 pagesArterial Disease SurgicalWahid SyedNo ratings yet
- Onco Emergency and MCHDocument51 pagesOnco Emergency and MCHJosephin dayanaNo ratings yet
- Connective Tissue Disorders: DR Josephine Ojoo MBCHB FRCP CCST (Resp) Dip Hiv Med Senior Lecturer Maseno UniversityDocument70 pagesConnective Tissue Disorders: DR Josephine Ojoo MBCHB FRCP CCST (Resp) Dip Hiv Med Senior Lecturer Maseno UniversityMalueth AnguiNo ratings yet
- Derma Quiz 2 NotesDocument9 pagesDerma Quiz 2 NotesJolaine ValloNo ratings yet
- Phlebitis and ThrombophlebitisDocument27 pagesPhlebitis and ThrombophlebitisMaría Fernanda RíosNo ratings yet
- Skin PathologyDocument55 pagesSkin PathologyJhost Clinton PurbaNo ratings yet
- Lymphadenopathy: Clinical ApproachDocument31 pagesLymphadenopathy: Clinical ApproachPooja ShashidharanNo ratings yet
- DVTDocument20 pagesDVTNachiket Vijay PotdarNo ratings yet
- Postoperative Surgical ComplicationDocument27 pagesPostoperative Surgical ComplicationdfdxgfcvhbNo ratings yet
- Thyroid & Lymph NodesDocument44 pagesThyroid & Lymph NodesSarah CornerNo ratings yet
- 2 - Lymphoma Lecture by Dr. M T - PresentationDocument40 pages2 - Lymphoma Lecture by Dr. M T - Presentationsohilaw210No ratings yet
- The Ideal Lymphedema Diet Cookbook; The Superb Diet Guide For Effective Lymphedema Management And Treatment With Nutritious RecipesFrom EverandThe Ideal Lymphedema Diet Cookbook; The Superb Diet Guide For Effective Lymphedema Management And Treatment With Nutritious RecipesNo ratings yet
- +oleksandr Chaika Theme 16 Thrombosis of The Main VeinsDocument22 pages+oleksandr Chaika Theme 16 Thrombosis of The Main VeinsOussama ANo ratings yet
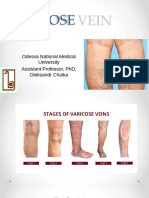
- +oleksandr Chaika Theme 15 Varicose Veins.Document19 pages+oleksandr Chaika Theme 15 Varicose Veins.Oussama ANo ratings yet
- +oleksandr Chaika Theme 17 Postthrombophlebetic Syndrome.Document11 pages+oleksandr Chaika Theme 17 Postthrombophlebetic Syndrome.Oussama ANo ratings yet
- Clinical Anatomy 1Document4 pagesClinical Anatomy 1Oussama ANo ratings yet
- Syllabus Obs - Gyn 2022 MedicineDocument8 pagesSyllabus Obs - Gyn 2022 MedicineOussama ANo ratings yet
- Lection 10. Diseases of IntestineDocument23 pagesLection 10. Diseases of IntestineOussama ANo ratings yet
- Lection 6. Acute PeritonitisDocument12 pagesLection 6. Acute PeritonitisOussama ANo ratings yet
- Food Allergy GuideDocument3 pagesFood Allergy GuideJamani Pritchett-SinegalNo ratings yet
- NCP Activity IntoleranceDocument1 pageNCP Activity IntoleranceBen David100% (2)
- Clinical and Dermoscopic Features of Seborrheic KeratosisDocument1 pageClinical and Dermoscopic Features of Seborrheic KeratosisRicky SetiawanNo ratings yet
- Final Test FK - 1 - Ang - 2019 - Juli 2020Document3 pagesFinal Test FK - 1 - Ang - 2019 - Juli 2020CahayaNo ratings yet
- CellulitisDocument3 pagesCellulitisAllen MallariNo ratings yet
- 35 - Eposter - Subhenjit Ray.Document1 page35 - Eposter - Subhenjit Ray.Subhenjit RoyNo ratings yet
- Hepatitis in ChildrenDocument2 pagesHepatitis in ChildrenShilpi SinghNo ratings yet
- Mini OSCE Surgery-Group A - Soul 2014Document18 pagesMini OSCE Surgery-Group A - Soul 2014Hasan H.No ratings yet
- Optimal Antibiotic Therapy for UTIDocument3 pagesOptimal Antibiotic Therapy for UTIGokull ShautriNo ratings yet
- HypertensionDocument14 pagesHypertensionChucky Vergara100% (2)
- Resume Tutorial A Skenario 1 Blok 14Document74 pagesResume Tutorial A Skenario 1 Blok 14Istaz MaulanaNo ratings yet
- DR Paul Harijanto - WS MALARIA-PIN PAPDI-19 PDFDocument33 pagesDR Paul Harijanto - WS MALARIA-PIN PAPDI-19 PDFMukhammadBurhanuddinNo ratings yet
- R.A. 11332 Mandatory Reporting of DiseasesDocument4 pagesR.A. 11332 Mandatory Reporting of Diseasespaolo llegoNo ratings yet
- HerniaDocument6 pagesHerniahani alzo3bi100% (7)
- Syllabus EpidemiologyDocument10 pagesSyllabus EpidemiologyHaris PapadopoulosNo ratings yet
- History of Polio-1Document21 pagesHistory of Polio-1world photocopyNo ratings yet
- Vaccine Friendly PlanDocument4 pagesVaccine Friendly PlanAna Sampaio89% (9)
- Molecular Biology: Test Name Result Reference Value/ Specimen Units Method Prev ResultDocument1 pageMolecular Biology: Test Name Result Reference Value/ Specimen Units Method Prev ResultPrasanna Das RaviNo ratings yet
- Atienza Vs Orophil GR. 191049Document1 pageAtienza Vs Orophil GR. 191049Crizedhen VardeleonNo ratings yet
- Upper Gastrointestinal BleedingDocument24 pagesUpper Gastrointestinal BleedingDr.Sathaporn Kunnathum100% (1)
- Family Community Society: 1. Health-Illness Continuum ModelDocument14 pagesFamily Community Society: 1. Health-Illness Continuum ModelJohn kananamanNo ratings yet
- An Overview of Inclusion Body Hepatitis-Hydropericardium Syndrome (IBH-HPS)Document26 pagesAn Overview of Inclusion Body Hepatitis-Hydropericardium Syndrome (IBH-HPS)kedar karkiNo ratings yet
- Ovarian Cancer NCPDocument7 pagesOvarian Cancer NCPAsterlyn Coniendo100% (1)
- Lymphadenopathy: Soheir Adam, MD, MSC, MrcpathDocument34 pagesLymphadenopathy: Soheir Adam, MD, MSC, MrcpathWilly OematanNo ratings yet
- Hand and Wrist PathwayDocument2 pagesHand and Wrist PathwaydrsadafrafiNo ratings yet
- Community health nursing exam questionsDocument10 pagesCommunity health nursing exam questionsCiena MaeNo ratings yet
- Psychotic Disorder Case Linked to Dengue FeverDocument4 pagesPsychotic Disorder Case Linked to Dengue FeverHoney SarmientoNo ratings yet
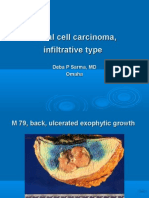
- Basal Cell Carcinoma, Infiltrative TypeDocument8 pagesBasal Cell Carcinoma, Infiltrative TypeDeba P SarmaNo ratings yet
- Clinical Efficacy of Placentrex for Pelvic Inflammatory DiseaseDocument3 pagesClinical Efficacy of Placentrex for Pelvic Inflammatory DiseaseGaneshkumar SarvesanNo ratings yet
- Bipolar DisorderDocument24 pagesBipolar DisorderJamie PilloffNo ratings yet