Professional Documents
Culture Documents
Incidental Zinner Syndrome in Nigeria A Case Report
Uploaded by
kshwel.pOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Incidental Zinner Syndrome in Nigeria A Case Report
Uploaded by
kshwel.pCopyright:
Available Formats
Case Report
Incidental Zinner Syndrome in Nigeria:
A Case Report
Authors: *A.O. Takure,1,2 B.A. Adewumi,3 O.E. Fatade,4 A.O. Adeyinka4,5
1. Department of Surgery, College of Medicine, University
of Ibadan, Nigeria
2. Division of Urological Surgery, Department of Surgery,
University College Hospital (UCH), Ibadan, Nigeria
3. Department of Obstetrics and Gynaecology, University College
Hospital (UCH), Ibadan, Nigeria
4. Department of Radiology, University College Hospital (UCH),
Ibadan, Nigeria
5. Department of Radiology, College of Medicine, University of
Ibadan, Nigeria
*Correspondence to augusturoendo@gmail.com
Disclosure: The authors have declared no conflicts of interest.
The authors report that informed written consent has been
obtained from the patient for publication of this case report
and any accompanying images.
Received: 05.06.23
Accepted: 15.01.24
Keywords: Asymptomatic, case report, hepatitis, Nigeria, Zinner syndrome (ZS).
Citation: EMJ Urol. 2024; DOI/10.33590/emjurol/11000010.
https://doi.org/10.33590/emjurol/11000010.
Abstract
Zinner syndrome (ZS) is a rare urogenital condition characterised by the triad of
unilateral renal agenesis, ipsilateral seminal vesicle cyst, and ipsilateral ejaculatory
duct obstruction, resulting from malformation during early embryogenesis of the
mesonephric (Wolffian) duct.
The authors present a 35-year-old male who was being evaluated for chronic
hepatitis B virus infection. He was referred to the urology outpatient clinic on
account of incidental ultrasound finding of solitary right kidney. General physical
examination revealed a healthy-looking young male with a flat abdomen and no
palpable enlarged organs. Digital rectal examination revealed normal sized prostate
with no palpable pararectal masses. MRI of the pelvis revealed a triad of unilateral
renal agenesis, ipsilateral seminal vesicle cyst, and ipsilateral ejaculatory duct
obstruction.
The clinical diagnosis was asymptomatic ZS. He is on yearly follow-up at the urology
outpatient clinic for lower urinary tract symptoms, pelvic pain, painful ejaculation,
features of infertility, and pelvic ultrasound. If any of these symptoms occur, he will
be treated with an α-adrenergic receptor blocker, drainage of the seminal vesicle
cyst, and appropriate treatment for infertility. He is also on active surveillance for
viral hepatitis by the gastroenterology team.
Creative Commons Attribution-Non Commercial 4.0 ● February 2024 ● Urology ●
Case Report
In conclusion, prompt referral and comprehensive radiological imaging investigations
of patients with unilateral agenesis of the kidney will lead to increased identification
and report of patients with ZS. There is paucity of literature reports on ZS in the
authors’ environment, and this case report, to the best of the authors’ knowledge,
is the first from Nigeria.
Key Points
1. The presence of a solitary kidney on incidental ultrasound evaluation should raise a high index of
suspicion for Zinner syndrome (ZS).
2. CT scan and MRI are very important in establishing the diagnosis of ZS.
3. The association of infertility and ZS is not fully understood. Further study with close monitoring of ZS
is likely to identify the exact cause of infertility, to provide appropriate pre-emptive treatment.
INTRODUCTION outpatient clinic of the University College
Hospital (UCH), Ibadan, Nigeria. He was the third
Zinner syndrome (ZS) is a rare urogenital of three children in a monogamous family setting.
anomaly characterised by a triad of unilateral There was no family history of a similar medical
renal agenesis, ipsilateral seminal vesicle cyst, condition, and he did not smoke or drink alcohol.
and ipsilateral ejaculatory duct obstruction,
which was first described in 1914 by Zinner.1 The patient was referred to Urology for
It arises from the abnormal embryological evaluation of an incidentally noted congenital
development of the mesonephric ducts occurring solitary right kidney during ultrasound evaluation
during the first trimester, and usually presents of the liver, for the workup of chronic HB.
between the second and fourth decade of
life, when there is an increase in the size of At the presentation, there were no upper or lower
the seminal vesicle.2,3 Symptomatic patients urinary tract symptoms, nor deep pelvic pain.
often respond well to open surgical excision, There was no history suggestive of hypertension,
transurethral deroofing, or laparoscopic excision diabetes, peptic ulcer, or bronchial asthma.
of the seminal vesicles.4,5 There was no history of previous surgery and
blood transfusion. He had been a patient of the
The literature search did not reveal any Gastroenterology unit for 12 years on account
publication from the authors’ environment; of incidental HB surface antigen detection
hence, the authors present this case report of during a screening in school. He had remained
asymptomatic ZS discovered in an asymptomatic asymptomatic on follow-up. HB e-antigen, HB
chronic hepatitis B (HB) virus infection in a young e-antibody, and HB core immunoglobin M were
male Nigerian, which, in the course of evaluating all negative, and liver function test results were
the liver by ultrasound, revealed a solitary right within normal limits.
kidney. MRI further identified ipsilateral renal
agenesis, ipsilateral cystic seminal vesicle, and Examination revealed a young man who was
ipsilateral ejaculatory duct cyst. In addition, afebrile, not pale, anicteric, well hydrated, and
teratozoospermia was observed in the seminal with no demonstrable pitting pedal oedema.
fluid analysis. Vital signs were within normal limits. Chest,
cardiovascular, abdominal, and external genitalia
examinations were essentially normal. The digital
PATIENT INFORMATION rectal examination revealed a normal-sized
prostate, and no other extra-rectal masses
The patient was a 35-year-old, single factory were felt.
worker, who first presented to the Urology
● Urology ● February 2024 ● Creative Commons Attribution-Non Commercial 4.0
Case Report
The complete blood count, electrolyte urea, The abdominopelvic ultrasound scan showed
creatinine, and liver function tests were a normal urinary bladder and prostate, with
essentially normal. However, the semen analysis dilatation of both the left ejaculatory duct and left
revealed teratozoospermia. seminal vesicle (Figure 1).
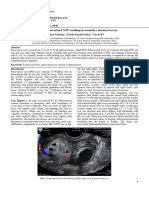
Figure 1: B-mode ultrasound images of patient with asymptomatic Zinner syndrome, showing left dilated
ejaculatory duct and left seminal vesicle.
The abdominal axial and coronal T1-weighted The patient expressed surprise and was happy
(T1W) MRI Fast Imaging Employing Steady-state that his clinical diagnosis was identified, and
Acquisition (FIESTA) images showed a normally promised to keep his appointment at the urology
located right kidney, and absent left kidney. outpatient surgical clinic.
The intestine was in the left renal bed, with the
psoas muscle seen (Figure 2). Both pelvic axial
T1W MRI and T2-weighted (T2W) MRIs showed DISCUSSION
cystic left seminal vesicles and a dilated left
ejaculatory duct that were hyperintense on The triad of unilateral renal agenesis, ipsilateral
T1W images, and hypointense on T2W images, obstruction of the ejaculatory duct, and ipsilateral
respectively (Figure 3). seminal vesicle cyst, is referred to as ZS.
The incidence of ZS is low. Sheih et al.6 reported
The patient has remained asymptomatic and that the incidence of seminal vesicle cystic
is currently on yearly follow-up with pelvic dilatations in patients with ipsilateral renal
ultrasound to assess the growth rate of the agenesis or dysplasia was 0.0046% (13 in 28,000)
seminal vesicle, as well as seminal fluid analysis among children in Taipei. Furthermore, van den
for his fertility status. Ouden et al.4 reported a pooled case of 52 cases
of ZS before 1998.
Creative Commons Attribution-Non Commercial 4.0 ● February 2024 ● Urology ●
Case Report
Figure 2: Fast Imaging Employing Steady-state Acquisition (FIESTA) MRI sequences.
A B
A) Axial
B) Coronal
Scans show a normally sited right kidney with empty left renal bed; a bowel loop is noted as hyperintense
structure surrounded by fat, just lateral to the left psoas muscle.
Figure 3: Pelvic axial MRI of dilated structure and adjacent beaded structures posterior to the
urinary bladder.
A B
A) T1W MRI showing hyperintense dilated structure and adjacent beaded structures posterior to the urinary
bladder, all consistent with seminal vesicle cyst and ejaculatory duct dilatation.
B) T2W MRI showing the same structures, now hypointense.
In a systematic review of 214 cases of ZS ZS is very rare among Africans. In their pooled
between 1999–2020, Liu et al.7 reported that study, van den Ouden et al.4 reported that only
80.8% of patients were symptomatic, with equal two patients (4%) were African. It is not surprising
prevalence of right and left renal agenesis. that only two cases have been reported from
Africa to date.8,9
● Urology ● February 2024 ● Creative Commons Attribution-Non Commercial 4.0
Case Report
From these reports, it seems that there are and obstruction of the ejaculatory duct on the
racial differences in the reported incidence of affected side.4,11
ZS. In Ethiopia, Beyene et al.9 reported that a
heightened sexual activity may have contributed The clinical presentations of ZS are variable
to presentation in their case report. This has not and non-specific, often leading to diagnostic
been corroborated by other authors. The authors challenges.10,12 Many patients tend to become
need to investigate this further in any new cases symptomatic between the second and fourth
of ZS in Africa. decade of life, when there is an increase in
the size of the seminal vesicle to >5 cm.3
This geographical question could be answered Some common presentations in ZS include
by screening preschool children and adults lower urinary tract symptoms, such as urinary
for renal agenesis with abdominal ultrasound, frequency and pelvic pain.12,13 The indications
before entry into secondary schools or tertiary for surgical intervention are recurrent urinary
institutions. This may likely increase the reporting tract infections,14 and haematospermia.15 ZS is a
of ZS in Nigeria, and across Africa. Of note is the recognised cause of painful ejaculation and male
presentation of incidental solitary right kidney in infertility.16,17 The patient in this case report had a
this case report, picked up on ultrasound. This significant percentage of abnormal sperm cells,
is the first case report from Nigeria that was despite good sperm concentration and motility;
asymptomatically discovered while evaluating therefore, he should be closely monitored.18
this index patient for asymptomatic chronic The complete blood count, electrolytes, urea,
HB infection. Further evaluation of the patient and creatinine, as well as liver function test,
was based on a high index of suspicion for ZS. and serum prostate-specific antigen, were
With this case report from Nigeria, the authors essentially normal.
hope to raise clinicians’ level of awareness, and
encourage them to thoroughly evaluate any case MRI is the gold standard in the diagnosis of ZS. It
of ipsilateral renal agenesis in order to identify is often performed in the coronal and transverse
the full spectrum of congenital anomalies in such plane without contrast. The protocol commonly
patients. This may translate into higher incidence used is T1W turbo spine-echo (TSE), T2W TSE,
of a condition that has seemingly been under- and a T1W TSE fat-saturation. It often shows
reported or misdiagnosed in Nigeria. a multiloculated seminal vesicle cyst that is
hypointense on T1W images, and appears bright
A study in China, where ZS is also rare, on T2W images. The MRI features are renal
discovered genetic features in the 14 cases agenesis and occasional situs inversus viscerum,
reported. The mutated genes were BMP4, as well as lobulated multiloculated cystic lesion of
RPGRIP1L, SEC63, SETD2, AGFG1, FLT1, and the seminal vesicle with saccular dilated enlarged
ZNF141.10 The authors cannot categorically state ectopic ureter that opens into the cystic seminal
that there is a genetic impact on ZS from this vesicle. This is well appreciated in the T1W
case report. However, they could explore this coronal view.19,20
possibility by screening for the mutated genes
in their patient, to determine genetic features in Contrast-enhanced axial CT of the abdomen
patients with ZS in Africa. with coronal reconstruction shows ipsilateral
renal agenesis, and lobulated multiloculated
The aetiology of ZS is believed to result from cystic seminal vesicle with saccular dilated, with
the developmental arrest of the mesonephric or without enlarged ectopic ureter, that opens
(Wolffian) ducts during the fifth week of into the cystic seminal vesicle. The dilated
embryogenesis. This is particularly obvious since seminal vesicle does not demonstrate contrast
the mesonephric duct in males develops to form enhancement, which is in keeping with non-
half of the trigone, the urinary bladder neck, malignant cyst.19,20
urethra, seminal vesicle, vas deferens, epididymis,
and epididymal heads, under the influence of Abdominal ultrasound shows solitary kidney
testosterone and Müllerian duct inhibitory factor. and empty contralateral renal bed with a
Thus, the outcome of such disturbances includes retrovesical liquid mass. Transrectal ultrasound
ipsilateral renal agenesis, dilatation of the distal visualises retrovesical hypoechoic cyst with
ureter, cystic dilatation of the seminal vesicle, posterior enhancement and impure content
Creative Commons Attribution-Non Commercial 4.0 ● February 2024 ● Urology ●
Case Report
that compresses the urinary bladder, and increased seminal vesicle cyst. Other available
protrudes into the bladder lumen.14,21 However, in treatment options of seminal vesicle cysts include
environments with limited resources, abdominal open or robotic excision of the cysts.25,26
CT or ultrasound scan are suitable alternatives
to MRI.14,20 In cases with infertility and painful ejaculation,
transurethral resection of ejaculatory ducts
Seminal fluid analysis is also an important aid resolution of symptoms, and improve
investigation in ZS, as about 45% of cases are semen characteristics.4
documented with infertility.22 In some cases,
cystoscopy may be necessary to exclude
ipsilateral ejaculatory duct causing bladder outlet CONCLUSION
obstruction, as this may require aspiration.23
This case report from Nigeria will increase the
Observation with close follow-up is advocated level of suspicion from ultrasound screening,
for those who are asymptomatic, as in this case encourage thorough evaluation of patients with
report. The duration of follow-up needed is solitary kidney, and reduce misdiagnosis and
variable, and the longest documented follow-up under-reporting of ZS. Asymptomatic patients
is that reported by Kelly et al.,24 where the patient should be closely followed up with imaging
was followed up for 14 years, and eventually studies and laboratory tests, and appropriately
had a successful laparoscopic excision of his treated when symptomatic.
References 10. Dai R et al. Clinicopathological role of imaging to identify and
and genetic features of Zinner’s evaluate the uncommon variation
1. Zinner A. Ein fall von intravesikaler
syndrome: two case reports and in development of the male
Samenblasenzyste. Wien Med
review of literature. Front Urol. genital tract. Radiol Case Rep.
Wochenshr. 1914;64:605.
2023;3:1257368. 2016;12(1):54-8.
2. Hevia Palacios M et al. Zinner
11. Hannema SE, Hughes IA. Regulation 20. Alarifi M et al. The association
syndrome with ectopic ureter
of Wolffian duct development. Horm of renal agenesis and ipsilateral
emptying into seminal vesicle.
Res. 2007;67(3):142-51. seminal vesicle cyst: Zinner
Case Rep Urol. 2021;2021:8834127.
syndrome case report. Case Rep
12. Sada F et al. Challenging clinical Urol. 2019;2019:1242149.
3. Bearrick EN, Husmann DA.
presentation of Zinner syndrome.
Screening for Zinner syndrome in
Radiol Case Rep. 2023;18(1):256-9. 21. Farooqui A et al. Massive seminal
patients with a congenitally solitary
vesicle cyst with ipsilateral renal
kidney: lessons learned. J Urol. 13. Pina-Vaz T et al. Zinner’s syndrome, agenesis – Zinner syndrome
2023;210(6):888-98. a retrospective series of three in Saudi patient. Urol Ann.
cases: different strategies to the 2018;10(3):333-5.
4. van den Ouden D et al. Diagnosis
same problem. BMJ Case Rep.
and management of seminal vesicle
2021;14(10):e242757. 22. Ostrowska M et al. Zinner
cysts associated with ipsilateral
syndrome–a rare cause of recurrent
renal agenesis: a pooled analysis 14. Ibrahim A et al. Zinner’s syndrome: epididymitis and infertility.
of 52 cases. Eur Urol. a rare diagnosis of dysuria based Clin Pract. 2021;11(4):942-6.
1998;33(5):433-40. on imaging. Case Rep Urol.
2020;2020:8826664. 23. Kori R et al. Zinner syndrome
5. Seo Y et al. Congenital seminal
mimicking bladder outlet
vesicle cyst associated with 15. Canales-Casco N et al. obstruction managed
ipsilateral renal agenesis. Hematospermia as a rare form of with aspiration. Urol Ann.
Yonsei Med J. 2009;50(4):560-3. presentation of Zinner syndrome. 2019;11(4):449-52.
Urology. 2017;99:e15-6.
6. Sheih CP et al. Cystic dilatations
24. Kelly NP et al. Long-term
within the pelvis in patients 16. Rahoui M et al. An unusual cause surveillance and laparoscopic
with ipsilateral renal agenesis or of painful ejaculation in a young management of Zinner syndrome.
dysplasia. J Urol. 1990;144 patient: Zinner syndrome. Ann Med Case Rep Urol. 2021;2021:6626511.
(2 Pt 1):324-7. Surg (Lond). 2022;10:79:103982.
25. Govorov A et al. Treatment of
7. Liu T et al. Zinner syndrome: an 17. Hofmann A et al. Zinner syndrome Zinner syndrome with robot-
updated pooled analysis based and infertility–a literature review assisted surgery. Eur Urol Open Sci.
on 214 cases from 1999 to 2020: based on a clinical case. Int J Impot 2022;44(Suppl 4):S282.
systematic review. Ann Palliat Med. Res. 2021;33(2):191-5.
2021;10(20):2271-82. 26. Lim CY, Liu CL, Huang SK.
18. Almuhanna AM et al. Zinner’s Laparoscopic excision of huge
8. Abakar D et al. Zinner syndrome. syndrome: case report of a rare seminal vesicle cyst in Zinner
Eur J Case Rep Intern Med. maldevelopment in the male syndrome. Radiol Case Rep.
2021;8(7):002628. genitourinary tract. Urol Case Rep. 2023;18(6):2172-5.
2021;39:101839.
9. Beyene E et al. Zinner syndrome:
a first case report from Ethopia. 19. Fiaschetti V et al. Zinner syndrome
Radiol Case Rep. 2023;18(1):86-90. diagnosed by magnetic resonance
imaging and computed tomography:
● Urology ● February 2024 ● Creative Commons Attribution-Non Commercial 4.0
You might also like
- Anorectal MalformationDocument4 pagesAnorectal MalformationFawzia Haznah Nurul ImaniNo ratings yet
- The Good News About Nuclear Destruction!Document7 pagesThe Good News About Nuclear Destruction!Ven GeanciaNo ratings yet
- Caregiving Elderly Care TRDocument170 pagesCaregiving Elderly Care TRRodolfo Corpuz67% (3)
- Capstone ReportDocument39 pagesCapstone ReportSai MaheshNo ratings yet
- Addison's DiseaseDocument17 pagesAddison's DiseaseMah Jezthy100% (1)
- Scrotal Abscess With A Rare Cause: Ase EportDocument3 pagesScrotal Abscess With A Rare Cause: Ase EportTeja Laksana NukanaNo ratings yet
- Case Report: Frican Medical JournalDocument6 pagesCase Report: Frican Medical JournalArief AdamaNo ratings yet
- International Archives of Urology and Complications Iauc 8 086Document6 pagesInternational Archives of Urology and Complications Iauc 8 086Ikhsan PrialaksanaNo ratings yet
- La Importancia de La Urografía Por TC en El Diagnóstico Precoz de Variaciones Anatómicas Del Tracto Urogenital Presentación de CasoDocument5 pagesLa Importancia de La Urografía Por TC en El Diagnóstico Precoz de Variaciones Anatómicas Del Tracto Urogenital Presentación de Casojose luis ramirez espinosaNo ratings yet
- Nyacp 2015 ConftracheomalaciaposterDocument92 pagesNyacp 2015 ConftracheomalaciaposterParth VinaypatilNo ratings yet
- Case StudiesDocument6 pagesCase StudiesPatricia CruzNo ratings yet
- True Hermaphroditism With Seminoma, Case ReportDocument4 pagesTrue Hermaphroditism With Seminoma, Case ReportJesahias Trejo MartínezNo ratings yet
- Jejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of LiteratureDocument6 pagesJejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of Literatureellya theresiaNo ratings yet
- Tuberculous Endometritis Presenting As A LeiomyomaDocument4 pagesTuberculous Endometritis Presenting As A LeiomyomaKoyel Sreyashi BasuNo ratings yet
- Ayoob 2019Document4 pagesAyoob 2019ManuelEduardoSanchezSotoNo ratings yet
- Non-Traumatic Rupture of Spleen Can Splenectomy BeDocument3 pagesNon-Traumatic Rupture of Spleen Can Splenectomy Beysh_girlNo ratings yet
- Situs Inversus Totalis in A 72-Year-Old Man WestAfrJRadiolDocument4 pagesSitus Inversus Totalis in A 72-Year-Old Man WestAfrJRadiolAnonymous 9QxPDpNo ratings yet
- Zinner's Syndrome: A New Asymptomatic Case ReportDocument3 pagesZinner's Syndrome: A New Asymptomatic Case ReportasclepiuspdfsNo ratings yet
- GMC PublishedDocument3 pagesGMC PublishedAyanawNo ratings yet
- HydronephrosisDocument3 pagesHydronephrosisCarla AlmerolNo ratings yet
- Ket 5Document4 pagesKet 5Handy SaputraNo ratings yet
- Anil Degaonkar, Nikhil Bhamare, Mandar Tilak Arterio-Enteric Fistula A Case ReportDocument6 pagesAnil Degaonkar, Nikhil Bhamare, Mandar Tilak Arterio-Enteric Fistula A Case ReportDr. Krishna N. SharmaNo ratings yet
- Case 16-2014: A 46-Year-Old Woman in Botswana With Postcoital BleedingDocument10 pagesCase 16-2014: A 46-Year-Old Woman in Botswana With Postcoital BleedingDesi HutapeaNo ratings yet
- A Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewDocument5 pagesA Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- Zaid 2013Document3 pagesZaid 2013Teja Laksana NukanaNo ratings yet
- Small Intestinal Contrast UltrasonographDocument5 pagesSmall Intestinal Contrast UltrasonographСергей СадовниковNo ratings yet
- Hi Drone Pros IsDocument10 pagesHi Drone Pros IsAlmuizzu NurjannahNo ratings yet
- Spontaneous Perinephric Urinoma Presenting As Acute Abdomen in The Third Trimester: A Case ReportDocument3 pagesSpontaneous Perinephric Urinoma Presenting As Acute Abdomen in The Third Trimester: A Case ReportSachin AjithNo ratings yet
- Nejmcpc 1102202Document10 pagesNejmcpc 1102202FrinkooFrinkoBNo ratings yet
- Jejunoileal Atresia Associated With Situs Inversus Totalis: Etter To The EditorDocument2 pagesJejunoileal Atresia Associated With Situs Inversus Totalis: Etter To The Editorchirurgie nou-nascutiNo ratings yet
- Case 20-2010 A 32-Year-Old Woman With Oligomenorrhea Ang Infertility PDFDocument9 pagesCase 20-2010 A 32-Year-Old Woman With Oligomenorrhea Ang Infertility PDFOrlando CuellarNo ratings yet
- Extra Pelvic Endometriosis: Double Ileal and Ileo-Caecal Localization Revealed by Acute Small Bowel Obstruction, A Clinical CaseDocument9 pagesExtra Pelvic Endometriosis: Double Ileal and Ileo-Caecal Localization Revealed by Acute Small Bowel Obstruction, A Clinical CaseIJAR JOURNALNo ratings yet
- EndometritisDocument6 pagesEndometritisMuh Syarifullah ANo ratings yet
- Rounds: GrandDocument7 pagesRounds: GrandHưng Nguyễn KiềuNo ratings yet
- TB of The TestesDocument2 pagesTB of The Testesntambik21No ratings yet
- Infectious IleoceicitisDocument2 pagesInfectious IleoceicitisYandiNo ratings yet
- Case Report Severe Dysplasia of Kidney 20082021Document15 pagesCase Report Severe Dysplasia of Kidney 20082021Nikko Caesario Mauldy SusiloNo ratings yet
- Hematometra in Uterus Didelphys With Right Hemivagina and Right Renal AgenesisDocument3 pagesHematometra in Uterus Didelphys With Right Hemivagina and Right Renal AgenesisDexter BluesNo ratings yet
- Spontaneous Rupture of The Kidney Due To Acute Lymphoblastic Leukemia: The First Episode and A Glance On The LiteratureDocument4 pagesSpontaneous Rupture of The Kidney Due To Acute Lymphoblastic Leukemia: The First Episode and A Glance On The LiteraturePeertechz Publications Inc.No ratings yet
- International Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. AwasthiDocument3 pagesInternational Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. Awasthijohanna monsalveNo ratings yet
- Malignant Tumor in A Horseshoe Kidney: Case ReportDocument3 pagesMalignant Tumor in A Horseshoe Kidney: Case ReportNovita Elmy MufidaNo ratings yet
- Ajol File Journals - 76 - Articles - 114038 - Submission - Proof - 114038 901 318286 1 10 20150309Document2 pagesAjol File Journals - 76 - Articles - 114038 - Submission - Proof - 114038 901 318286 1 10 20150309alysNo ratings yet
- Term Live Primary Ovarian Pregnancy A Case ReportDocument4 pagesTerm Live Primary Ovarian Pregnancy A Case ReportNico PlantadoNo ratings yet
- APPENDICITISDocument8 pagesAPPENDICITISJuan Carlos SaguyodNo ratings yet
- Barret 2015.Document6 pagesBarret 2015.Elizabeth VegaNo ratings yet
- Pelvis Perineum Cases 04Document5 pagesPelvis Perineum Cases 04Uloko ChristopherNo ratings yet
- PDF TJP 1944Document5 pagesPDF TJP 1944Erlangga D SaputroNo ratings yet
- 2 5 21 861 PDFDocument3 pages2 5 21 861 PDFAhmed ZidanNo ratings yet
- Hernia Uterine Inguinale: An Uncommon Cause of Pelvic Pain in The Adult Female PatientDocument4 pagesHernia Uterine Inguinale: An Uncommon Cause of Pelvic Pain in The Adult Female PatientJeje MoNo ratings yet
- Mesenteric Venous Thrombosis As A Complication of Appendicitis in An AdolescentDocument5 pagesMesenteric Venous Thrombosis As A Complication of Appendicitis in An AdolescentEma DianthiNo ratings yet
- Piis0085253815527324 PDFDocument5 pagesPiis0085253815527324 PDFdodong skyroseNo ratings yet
- Case Report Prostate Tuberculosis-RD - 1-1Document6 pagesCase Report Prostate Tuberculosis-RD - 1-1GemiNo ratings yet
- Primary Carcinoma of Fallopian Tube: Case Series Case ReportDocument4 pagesPrimary Carcinoma of Fallopian Tube: Case Series Case ReportChi NgôNo ratings yet
- 1 - Bed 5 Case ReportDocument29 pages1 - Bed 5 Case ReportJevaan Nashlyn NaickNo ratings yet
- Cowper's Syringocele A Rare DifferentialDocument5 pagesCowper's Syringocele A Rare Differentialمحمد عريف حكيمNo ratings yet
- Chronic Ovarian Ectopic Pregnancy - An Unusual Occurrence: A Case ReportDocument5 pagesChronic Ovarian Ectopic Pregnancy - An Unusual Occurrence: A Case Reportindex PubNo ratings yet
- 5 - Hung, 2004Document4 pages5 - Hung, 2004Henrique MachadoNo ratings yet
- 2805-01. Manuscript (Article Text) - 6211-1-10-20161202Document3 pages2805-01. Manuscript (Article Text) - 6211-1-10-20161202Karina Aguirre AlvarezNo ratings yet
- Case Report - Omental TorsionDocument9 pagesCase Report - Omental TorsionProf. M AmirNo ratings yet
- Medicine: Intrauterine Device Found in An Ovarian TumorDocument5 pagesMedicine: Intrauterine Device Found in An Ovarian TumorRezky amalia basirNo ratings yet
- Uog 16935Document1 pageUog 16935Razi MaulanaNo ratings yet
- Testicular TBDocument6 pagesTesticular TBlupiNo ratings yet
- Corpus Alienum in Rectosigmoid A Case ReportDocument4 pagesCorpus Alienum in Rectosigmoid A Case Reportlina ukagoNo ratings yet
- Surgical Pathology of Non-neoplastic Gastrointestinal DiseasesFrom EverandSurgical Pathology of Non-neoplastic Gastrointestinal DiseasesLizhi ZhangNo ratings yet
- Neonatology Short Case History Taking Format by SPKathankar 1Document5 pagesNeonatology Short Case History Taking Format by SPKathankar 1HkNo ratings yet
- Synerquest 2014 Annual Calendar of DOLE-prescribed CoursesDocument3 pagesSynerquest 2014 Annual Calendar of DOLE-prescribed CoursesrobinrubinaNo ratings yet
- Speaking Test (15-20)Document12 pagesSpeaking Test (15-20)Phạm Mai Hương100% (1)
- Clinical Surgical 1Document2 pagesClinical Surgical 1Ohana NanaNo ratings yet
- MSDS HelizymeDocument7 pagesMSDS HelizymeAnonymous tbJ24554No ratings yet
- Writing Vstep Scan 1Document24 pagesWriting Vstep Scan 1NgaNo ratings yet
- Formulation and Evaluation of A Syrup Based On BalDocument10 pagesFormulation and Evaluation of A Syrup Based On BalemilNo ratings yet
- Reflection Paper MULANAYDocument2 pagesReflection Paper MULANAYRob40% (5)
- 1P1 - Anna Kusumawati 323-329Document7 pages1P1 - Anna Kusumawati 323-329imam habibiNo ratings yet
- ICU QuizDocument3 pagesICU QuizIrish Eunice FelixNo ratings yet
- Angelina Hull Student - Heritagehs - Argumentative Essay - Student Name - Class Period - Spring 19 - H English 1Document5 pagesAngelina Hull Student - Heritagehs - Argumentative Essay - Student Name - Class Period - Spring 19 - H English 1api-461590822No ratings yet
- Scaffolding Safety Checklist: Company: Supervisor (Qualified Person)Document3 pagesScaffolding Safety Checklist: Company: Supervisor (Qualified Person)Puspa AnisaNo ratings yet
- Ijcpd-15-S103 MetanalysisDocument11 pagesIjcpd-15-S103 MetanalysisGabriela ZuritaNo ratings yet
- ListeningDocument7 pagesListeningPallavi JNo ratings yet
- Akapulko (Cassia Alata) Indication/s: Duration: Nursing ResponsibilitiesDocument16 pagesAkapulko (Cassia Alata) Indication/s: Duration: Nursing ResponsibilitiesEljay Lustria ReyesNo ratings yet
- Tennessee Hazard Mitigation Plan 2018 FINALDocument388 pagesTennessee Hazard Mitigation Plan 2018 FINALAnonymous GF8PPILW5100% (1)
- Environmental Controls in Operating Theatres: S. Dharan and D. PittetDocument6 pagesEnvironmental Controls in Operating Theatres: S. Dharan and D. PittetDinda FSNo ratings yet
- Kinjal AttachedDocument1 pageKinjal AttachedNilay JethavaNo ratings yet
- 1 Identification: Acc. To OSHA HCSDocument10 pages1 Identification: Acc. To OSHA HCSbinaccaNo ratings yet
- Research PaperDocument4 pagesResearch Paperapi-611611708No ratings yet
- How To Be Eco-FriendlyDocument18 pagesHow To Be Eco-Friendlyhannah courseyNo ratings yet
- Modele Anglais - Convention Coordonnateur - Version 20220409Document36 pagesModele Anglais - Convention Coordonnateur - Version 20220409SchmoutNo ratings yet
- Eye Drops and Dispensing Aids: A GuideDocument37 pagesEye Drops and Dispensing Aids: A GuideAamna ShahNo ratings yet
- Social Anxiety Research Paper TopicsDocument8 pagesSocial Anxiety Research Paper Topicseghkq0wf100% (1)
- Hostel Rules and RegulationsDocument11 pagesHostel Rules and RegulationsAkshet PatelNo ratings yet
- Intern TicklerDocument10 pagesIntern TicklerRem AlfelorNo ratings yet