Professional Documents
Culture Documents
BetaLactamAntibiotics-StatPearls-NCBIBookshelf
Uploaded by
inkarkanat02Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
BetaLactamAntibiotics-StatPearls-NCBIBookshelf
Uploaded by
inkarkanat02Copyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/335681179
Beta Lactam Antibiotics
Chapter · August 2019
CITATIONS READS
47 23,870
2 authors, including:
Marco Cascella
Università degli Studi di Salerno
331 PUBLICATIONS 3,893 CITATIONS
SEE PROFILE
All content following this page was uploaded by Marco Cascella on 07 September 2019.
The user has requested enhancement of the downloaded file.
Beta Lactam Antibiotics
Pandey N, Cascella M.
Indications
Beta-lactam antibiotics are one of the most commonly prescribed drug class with numerous clinical indications. From
a biochemical point of view, these drugs have a common feature, which is the beta-lactam ring. This class includes:
Penicillins
Cephalosporins
Carbapenems
Monobactams
Beta-lactamase inhibitors.
This is a broad category of drugs, so the drugs get categorized functionally, which makes it easier to relate and prescribe. The
basis of grouping is the activity spectrum, therapeutic, and susceptibility testing.
MECHANISM OF ACTION
Beta-lactam antibiotics have a bactericidal mechanism of action. They inhibit the growth of rapidly multiplying bacteria by
inhibiting their cell wall synthesis; this occurs through inhibition of the enzymes responsible for cell wall biosynthesis located
in the cell membrane, the most common enzyme being penicillin-binding proteins (PBPs). This binding interrupts the terminal
transpeptidation process and induces, loss of viability and lysis, also through autolytic processes.
MECHANISM OF RESISTANCE
Resistance to beta-lactams is an alarming and growing phenomenon. It concerns above all Streptococcus pneumoniae and
individual gram-negative bacilli such as Pseudomonas aeruginosa. With emerging resistance for antibiotics, it makes sense to
look into mechanisms of resistance as it can help to decide which drugs to prescribe in different scenarios and ways to
overcome the same. Although bacterial resistance to beta-lactams mostly expresses through the production of beta-lactamases,
other mechanisms are involved. Following are the mechanisms of resistance[1]:
Decreased penetration to the target site (e.g., the resistance of Pseudomonas aeruginosa.
Alteration of target site PBPs (e.g., penicillin resistance in pneumococci)
Inactivation by the production of beta-lactamases, which are enzymes that hydrolyze and inactivate the beta-lactam
ring (especially in gram-negative bacteria)
Efflux from the periplasmic space through specific pumping mechanisms
INDICATIONS FOR BETA-LACTAM ANTIBIOTICS[2]:
PENICILLINS
Natural penicillins [Penicillin G (IV), Penicillin V (PO)] are used to treat selected gram-positive and gram-negative infections:
Penicillin susceptible Streptococcus pneumonia and meningitis
Streptococcal pharyngitis
Endocarditis
Skin and soft tissue infections
Neisseria meningitides infections
Syphilis
https://www.ncbi.nlm.nih.gov/books/NBK545311/ 07/09/19, 18@29
Pagina 1 di 7
PENICILLINASE RESISTANT PENICILLINS
These agents [oxacillin (IV), nafcillin (IV), dicloxacillin (PO)] are active against gram-positive organisms. Despite the
occurrence of widespread resistance among staphylococci, they remain antibiotics of choice in managing methicillin-
susceptible staphylococci (MSSA):
Skin and soft tissue infections (MSSA)
Serious infections due to MSSA
AMINOPENICILLINS
These antibiotics have activity against gram-positive and gram-negative bacteria (e.g., many Enterobacteriaceae) anaerobic
organisms. They are commonly used together with beta-lactamase inhibitors.
Amoxicillin (PO), ampicillin (PO/IV):
Upper respiratory tract infections (sinusitis, pharyngitis, otitis media)
Enterococcus faecalis infections
Listeria infections
Aminopenicillins/beta-lactamase inhibitors: amoxicillin/clavulanate (PO), ampicillin-sulbactam (IV)
Upper respiratory tract infections (sinusitis, otitis media)
Intra-abdominal infections
CARBOXYPENICILLINS AND UREIDOPENICILLINS
Ticarcillin (carboxypenicillin) and piperacillin (ureidopenicillin) have activity against aminopenicillin-resistant gram-negative
bacilli (Pseudomonas aeruginosa). Are commonly combined with beta-lactamase inhibitors
CEPHALOSPORINS
First-generation cephalosporins
Cefazolin(IV), cephalexin (PO), cefadroxil (PO)
Skin and soft tissue infections serious infections due to MSSA
Perioperative surgical prophylaxis
Second-generation cephalosporins
Cefuroxime (IV/PO), cefoxitin (IV), cefotetan (IV), cefaclor (PO) cefprozil (PO)
Upper respiratory tract infections (sinusitis, otitis media)
Cefoxitin, cefotetan-gynecologic infections,
perioperative surgical prophylaxis
Third-generation cephalosporins
Cefotaxime (IV), ceftriaxone (IV), cefpodoxime (PO), cefixime (PO), cefdinir (PO), cefditoren (PO), ceftibuten (PO)
Community-acquired pneumonia, meningitis
Urinary tract infections
Streptococcal endocarditis
Gonorrhea
Severe Lyme disease.
Anti-pseudomonal Cephalosporins
https://www.ncbi.nlm.nih.gov/books/NBK545311/ 07/09/19, 18@29
Pagina 2 di 7
Ceftazidime (IV), ceftolozone/tazobactam (IV), ceftazidime/avibactam (IV), cefepime (IV)
Nosocomial infections-pneumonia
Meningitis
Urinary tract infections
Intra-abdominal infections (with metronidazole)
Anti-MRSA cephalosporins-
Ceftaroline (IV)
Community-acquired pneumonia
Skin and soft tissue infection
CARBAPENEMS
Imipenem/cilastatin (IV), meropenem (IV), doripenem (IV)
Nosocomial infections-pneumonia, intra-abdominal infections, urinary tract infections
Meningitis (especially meropenem)
Ertapenem (IV)
Community-acquired infections
Nosocomial infections.
MONOBACTAMS
Aztreonam (IV). It is effective against aerobic gram-negative organisms but shows no activity against gram-positive bacteria
or anaerobes.
Nosocomial infections, e.g., pneumonia
Urinary tract infections
Because the emergence of antimicrobial resistance has become a progressively great concern, new beta-lactam, and beta-
lactamase inhibitor combinations (ceftolozane/tazobactam, ceftazidime/avibactam, meropenem/vaborbactam,
imipenem/cilastatin/relebactam, aztreonam/avibactam), siderophore cephalosporins (cefiderocol) have been developed and
represent options for the management of complicated infections,[3] especially in intensive care unit.[4]
Mechanism of Action
Peptidoglycan is a vital constituent of the bacterial cell wall that provides mechanical stability to it. The beta-lactam
antibiotics inhibit the last step in peptidoglycan synthesis by acylating the transpeptidase involved in cross-linking peptides to
form peptidoglycan.
The targets for the actions of beta-lactam antibiotics are known as PBPs (penicillin-binding proteins). The effect of this class
mostly becomes expressed against multiplying bacteria that are building their cell wall intensively and is indirect. This
mechanism leads to activation of an autolytic system through a system known as VncR/s, which initiates cell death.[5]
Administration
When administered orally, one must consider that food can affect oral absorption. Moreover, the absorption of some molecules
such as cefuroxime and cefpodoxime becomes decreased by H2 blockers or nonabsorbable antacids. Administration of these
agents can be through different routes.
https://www.ncbi.nlm.nih.gov/books/NBK545311/ 07/09/19, 18@29
Pagina 3 di 7
Penicillin V is preferrable for oral administration, given 30 min before the meal or 2 hours after.
Penicillin G is available in 2 parenteral preparations: benzathine and procaine.
Penicillin G benzathine is dosed once monthly as it has a longer half-life
Penicillin G procaine is given once daily due to a shorter half-life.
Neither should be given intravenously to avoid serious toxicity.
Penicillinase-resistant penicillins (oxacillin, cloxacillin and dicloxacillin) are available in oral and parenteral
preparations.
Aminopenicillins: ampicillin and amoxicillin are available in both oral and parenteral preparations, though
amoxicillin is preferred orally.
Antipseudomonal penicillins: piperacillin is only available for parenteral administration.
Most cephalosporins are absorbed readily after oral administration; the administration of others can be
intramuscularly or intravenously.
Continuous infusions of beta-lactam antibiotics may have advantages over standard intermittent bolus dosing.
Adverse Effects
Compared to other classes, beta-lactam agents are usually safe and well-tolerated.[6] The most frequent side effects are
allergic reactions that vary from 0.7% to 10%. These reactions are mostly maculopapular rashes, whereas reports of
anaphylaxis appear in 0.004 to 0.015% of patients.[7]
Penicillins
A hypersensitivity reaction is the most common adverse effect ranging from a maculopapular rash to angioedema,
serum sickness, and anaphylaxis.
It may occur with any dosage form of penicillin.
Other side effects include bone marrow depression, granulocytopenia, and hepatitis.
Cephalosporins
A hypersensitivity reaction is the most common. Nephrotoxicity, diarrhea, and biliary pseudolithiasis can occur with
some cephalosporins.
Carbapenems
Nausea, vomiting, seizures, especially with imipenem at high doses.
Monobactams
Hepatotoxicity, especially in infants and young children.
Contraindications
Penicillins are contraindicated in patients with previous anaphylactic reaction or serious skin reaction, for example, Steven-
Johnson syndrome and toxic epidermal necrosis.[6]
Monitoring
Most of the available penicillins have a short half-life, less than an hour mostly. The parenteral agents are given four-hourly,
usually when treating serious systemic infections with normal renal function. Piperacillin and ampicillin require dose
adjustment when given in patients with renal insufficiency (GFR less than 10 ml/min). For ticarcillin, this dose adjustment is
at 50 ml/min. Other agents like nafcillin, oxacillin, cloxacillin, and dicloxacillin have the hepato-biliary mode of excretion and
https://www.ncbi.nlm.nih.gov/books/NBK545311/ 07/09/19, 18@29
Pagina 4 di 7
therefore require no modification in renal impairment.
All penicillins achieve therapeutic levels in pleural, pericardial, peritoneal, synovial fluids, and urine. Of note, cerebrospinal
fluid (CSF) penetration is poor in the absence of inflammation but achieves therapeutic levels in meningitis.[8]
Toxicity
Penicillin occasionally reaches toxic concentrations in the brain, especially with renal dysfunction and can produce
CNS dysfunction and convulsions. Other toxic effects include bone marrow depression, granulocytopenia, and
hepatitis.
Penicillin G and piperacillin are also associated with impaired hemostasis due to defective platelet aggregation.
An IV injection of benzathine penicillin G has correlations with cardiorespiratory arrest and death.
Cephalosporins carry associations with rare instances of bone marrow depression including granulocytopenia
Some cephalosporins are potentially nephrotoxic and correlate with renal tubular necrosis. Ceftriaxone can cause
jaundice in neonates by displacing bilirubin from albumin.
It can also lead to biliary pseudolithiasis due to its high affinity for biliary calcium.
Cefepime correlates with encephalopathy and nonconvulsive status epilepticus at high doses or in patients with renal
dysfunction.
Imipenem is associated with seizures when given in high doses to patients with CNS lesions and those with renal
insufficiency.[9]
Enhancing Healthcare Team Outcomes
Penicillins are the most commonly used broad-spectrum antibiotics by many clinicians, including primary care providers,
internists, infectious disease experts, and nurse practitioners. Within the subgroups of penicillins, there are differences
between the antibiotics in pharmacokinetics, coverage, safety, and cost, which gives a fair amount of choice to make in
selecting which drug to use.[10]
Their use still requires the coordination of an interprofessional team. The clinicians above will be ordering/prescribing, but
nursing will often administer (inpatient) or counsel on administration (outpatient). Pharmacists need to involve themselves
via medication reconciliation, looking for interactions, as well as reinforcing administration instructions. Nurses will often be
the first line of contact in the event of adverse events and are also well-positioned to evaluate therapeutic effectiveness.
Pharmacists shall verify dosing and duration of therapy, and contact the prescriber on encountering any discrepancy. Beta-
lactams may be common, but their effective use still requires an interprofessional team approach for optimal patient outcomes.
[Level V]
Questions
To access free multiple choice questions on this topic, click here.
References
1. Probst-Kepper M, Geginat G. [New Antibiotics for Treatment of Highly Resistant Gram-negative Bacteria]. Anasthesiol
Intensivmed Notfallmed Schmerzther. 2018 Jul;53(7-08):529-542. [PubMed: 30036899]
2. Eckburg PB, Lister T, Walpole S, Keutzer T, Utley L, Tomayko J, Kopp E, Farinola N, Coleman S. Safety, Tolerability,
Pharmacokinetics, and Drug Interaction Potential of SPR741, An Intravenous Potentiator, After Single and Multiple
Ascending Doses and When Combined with Beta-Lactam Antibiotics in Healthy Subjects. Antimicrob. Agents
Chemother. 2019 Jul 01; [PMC free article: PMC6709486] [PubMed: 31262767]
https://www.ncbi.nlm.nih.gov/books/NBK545311/ 07/09/19, 18@29
Pagina 5 di 7
3. Mortensen JS, Jensen BP, Zhang M, Doogue M. Preanalytical Stability of Piperacillin, Tazobactam, Meropenem, and
Ceftazidime in Plasma and Whole Blood Using Liquid Chromatography-Tandem Mass Spectrometry. Ther Drug Monit.
2019 Aug;41(4):538-543. [PubMed: 31306394]
4. Ibrahim ME, Abbas M, Al-Shahrai AM, Elamin BK. Phenotypic Characterization and Antibiotic Resistance Patterns of
Extended-Spectrum β-Lactamase- and AmpC β-Lactamase-Producing Gram-Negative Bacteria in a Referral Hospital,
Saudi Arabia. Can J Infect Dis Med Microbiol. 2019;2019:6054694. [PMC free article: PMC6617866] [PubMed:
31346353]
5. Leone S, Damiani G, Pezone I, Kelly ME, Cascella M, Alfieri A, Pace MC, Fiore M. New antimicrobial options for the
management of complicated intra-abdominal infections. Eur. J. Clin. Microbiol. Infect. Dis. 2019 May;38(5):819-827.
[PubMed: 30903538]
6. Leone S, Cascella M, Pezone I, Fiore M. New antibiotics for the treatment of serious infections in intensive care unit
patients. Curr Med Res Opin. 2019 Aug;35(8):1331-1334. [PubMed: 30760041]
7. Chiriac AM, Rerkpattanapipat T, Bousquet PJ, Molinari N, Demoly P. Optimal step doses for drug provocation tests to
prove beta-lactam hypersensitivity. Allergy. 2017 Apr;72(4):552-561. [PubMed: 27569064]
8. Miller RL, Shtessel M, Robinson LB, Banerji A. Advances in drug allergy, urticaria, angioedema, and anaphylaxis in
2018. J. Allergy Clin. Immunol. 2019 Aug;144(2):381-392. [PMC free article: PMC6688939] [PubMed: 31247266]
9. Podlecka D, Jerzynska J, Malewska-Kaczmarek K, Stelmach I. A Case of a Child With Several Anaphylactic Reactions to
Drugs. Glob Pediatr Health. 2019;6:2333794X19855287. [PMC free article: PMC6587380] [PubMed: 31259207]
10. Han ML, Liu X, Velkov T, Lin YW, Zhu Y, Creek DJ, Barlow CK, Yu HH, Zhou Z, Zhang J, Li J. Comparative
Metabolomics Reveals Key Pathways Associated With the Synergistic Killing of Colistin and Sulbactam Combination
Against Multidrug-Resistant Acinetobacter baumannii. Front Pharmacol. 2019;10:754. [PMC free article: PMC6620532]
[PubMed: 31333468]
Publication Details
Author Information
Authors
Neelanjana Pandey; Marco Cascella1.
Affiliations
1
Istituto Nazionale Tumori - IRCCS
Publication History
Last Update: August 2, 2019.
Copyright
Copyright © 2019, StatPearls Publishing LLC.
This book is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/),
which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original
author(s) and the source, a link is provided to the Creative Commons license, and any changes made are indicated.
Publisher
StatPearls Publishing, Treasure Island (FL)
NLM Citation
https://www.ncbi.nlm.nih.gov/books/NBK545311/ 07/09/19, 18@29
Pagina 6 di 7
NLM Citation
Pandey N, Cascella M. Beta Lactam Antibiotics. [Updated 2019 Aug 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.
https://www.ncbi.nlm.nih.gov/books/NBK545311/ 07/09/19, 18@29
Pagina 7 di 7
View publication stats
You might also like
- MCQs IN MEDICINEDocument150 pagesMCQs IN MEDICINERITESH SINGHNo ratings yet
- Pance Prep Pearls AntibioticsDocument14 pagesPance Prep Pearls Antibioticskat100% (4)
- Textbook of Veterinary PathologyDocument657 pagesTextbook of Veterinary PathologyAndreea Irina100% (18)
- Eportfolio Geography of Covid-19Document10 pagesEportfolio Geography of Covid-19api-311531468No ratings yet
- Week 3 & 4 AntimicrobialsDocument120 pagesWeek 3 & 4 AntimicrobialsQuerubin DandoyNo ratings yet
- AntibioticsDocument5 pagesAntibioticsSneeha VeerakumarNo ratings yet
- Pharmaceutical Sciences: A Review On Beta Lactam AntibioticsDocument8 pagesPharmaceutical Sciences: A Review On Beta Lactam AntibioticsiajpsNo ratings yet
- Antibacterial Drugs Cellwall and Protein Synthesis InhihibitorsDocument41 pagesAntibacterial Drugs Cellwall and Protein Synthesis InhihibitorsWezzyNo ratings yet
- Lecture 15 Presentation ENGDocument37 pagesLecture 15 Presentation ENGjqpwzcg8xrNo ratings yet
- Novel Pyrazole Analogues as Antimicrobial AgentsDocument11 pagesNovel Pyrazole Analogues as Antimicrobial AgentsWalid EbaiedNo ratings yet
- Chapter 9 Surgical Infections and Antibiotic SelectionDocument42 pagesChapter 9 Surgical Infections and Antibiotic SelectionSteven Mark MananguNo ratings yet
- Industrial Production of PenicillinDocument9 pagesIndustrial Production of Penicillinssthakurleo100% (11)
- Chemo For LabDocument117 pagesChemo For Labsinte beyuNo ratings yet
- Pelvic Inflammatory Disease - 5Document5 pagesPelvic Inflammatory Disease - 5fatqur28No ratings yet
- Cirilo Albert Hicban RN, RM LecturerDocument50 pagesCirilo Albert Hicban RN, RM Lecturerrongan008No ratings yet
- PenicillinDocument21 pagesPenicillinnadar shahNo ratings yet
- Al-Bayan University Pharmacy College 3 Stage: Lecture 8 Pharmacology Antibiotics DR - Khulood SaadoonDocument19 pagesAl-Bayan University Pharmacy College 3 Stage: Lecture 8 Pharmacology Antibiotics DR - Khulood SaadoonAhmed HadeerNo ratings yet
- Lac 10&11 PPTDocument16 pagesLac 10&11 PPTRaghdaNo ratings yet
- PenicillinDocument75 pagesPenicillinJean CabigaoNo ratings yet
- Antibiotic Therapy For Peritonitis: Treatment Overview, Spontaneous Bacterial Peritonitis, Secondary and Tertiary PeritonitisDocument7 pagesAntibiotic Therapy For Peritonitis: Treatment Overview, Spontaneous Bacterial Peritonitis, Secondary and Tertiary PeritonitisTias SubagioNo ratings yet
- AntibioticsDocument31 pagesAntibioticsAkash SrivastavaNo ratings yet
- ChemotherapyDocument11 pagesChemotherapyNedaAbdullahNo ratings yet
- Microbiology - Exercise 3e AntibiogramDocument5 pagesMicrobiology - Exercise 3e Antibiogramapi-253346521No ratings yet
- Antibiotics Hospin PDFDocument5 pagesAntibiotics Hospin PDFSanjeeb DekaNo ratings yet
- ANTIBIOTICS IN ORAL SURGERYs 123Document43 pagesANTIBIOTICS IN ORAL SURGERYs 123Puneet SinghNo ratings yet
- Review On Cephalosporins Re ModifiedDocument6 pagesReview On Cephalosporins Re Modifiedramirezgrisel966No ratings yet
- Cep Halo Sporin SDocument51 pagesCep Halo Sporin Smonir61No ratings yet
- PharmaDocument16 pagesPharmaPaula Grace MorfeNo ratings yet
- Treatment of InfectionsDocument34 pagesTreatment of InfectionsSania KhanNo ratings yet
- Antimicrobials Revision: Gram Staining, MIC, Antibiotic Misuse & MechanismsDocument5 pagesAntimicrobials Revision: Gram Staining, MIC, Antibiotic Misuse & MechanismsDanny LeeNo ratings yet
- Mechanism of Action of Antibiotics: Subject:Pharmaceutical Microbiology DATE:18/09/2019Document12 pagesMechanism of Action of Antibiotics: Subject:Pharmaceutical Microbiology DATE:18/09/2019rubyNo ratings yet
- N-Lec7 - PenicillinsDocument21 pagesN-Lec7 - Penicillinsgeng gengNo ratings yet
- Antibacterials and AntibioticsDocument44 pagesAntibacterials and AntibioticsVallejo Taberna HannalieNo ratings yet
- Principles of Antimicrobial TherapyDocument19 pagesPrinciples of Antimicrobial TherapyMERVENo ratings yet
- Applied Pharmacotherapy: By: First GroupDocument13 pagesApplied Pharmacotherapy: By: First GroupMUHAMMAD ISLAMINo ratings yet
- Cephalosporins GenerationDocument7 pagesCephalosporins GenerationSam SmileyNo ratings yet
- Bio Project Calss 11Document20 pagesBio Project Calss 11muddurajusrpNo ratings yet
- Phar - Cell Wall Inhibitor - Lec 7 - TheoDocument20 pagesPhar - Cell Wall Inhibitor - Lec 7 - Theoسلام شاكر حميد جميل 6506No ratings yet
- AntibioticsDocument53 pagesAntibioticsMaheen IdreesNo ratings yet
- Bacteria Gram:: Streptococcus PneumoniaeDocument3 pagesBacteria Gram:: Streptococcus PneumoniaetrrrinsNo ratings yet
- ch-11 AntibioticsDocument35 pagesch-11 AntibioticsAyro Business CenterNo ratings yet
- Introduction to Antimicrobial Chemotherapy: Mechanisms and SpectrumDocument31 pagesIntroduction to Antimicrobial Chemotherapy: Mechanisms and SpectrumPrasad SangishettyNo ratings yet
- Module 4 AntimicrobialsDocument23 pagesModule 4 AntimicrobialsROJANE LAMENTACNo ratings yet
- Bacterial Cell Wall InhibitorsDocument30 pagesBacterial Cell Wall InhibitorsBYAWELE JAIRUS WANGUSANo ratings yet
- Introduction To Beta Lactam AntibioticsDocument31 pagesIntroduction To Beta Lactam AntibioticsVishaal BhatNo ratings yet
- Chapter 043Document6 pagesChapter 043borisdevic223No ratings yet
- Antibiotics Classification Basis Activity SpectrumDocument35 pagesAntibiotics Classification Basis Activity SpectrumRubina AkbarNo ratings yet
- 1. B7, AntibioticsDocument7 pages1. B7, AntibioticsAmany SaifNo ratings yet
- Topical Antibiotics in Dermatology: An Update on Uses and ResistanceDocument19 pagesTopical Antibiotics in Dermatology: An Update on Uses and ResistanceFernanda PutriNo ratings yet
- 2-Cell Wall Inhibitor Antibitics-I Oct 15th 2018Document28 pages2-Cell Wall Inhibitor Antibitics-I Oct 15th 2018Leena AlateeqNo ratings yet
- IntroductionDocument12 pagesIntroductionSuvidVijay FadanavisNo ratings yet
- Antibiotics CologyDocument31 pagesAntibiotics CologyManthan ChauhanNo ratings yet
- Cell Wall Synthesis Inhibitors: Jagir R. Patel Asst Prof. Anand Pharmacy CollegeDocument30 pagesCell Wall Synthesis Inhibitors: Jagir R. Patel Asst Prof. Anand Pharmacy CollegeJagirNo ratings yet
- AntibioticsDocument10 pagesAntibioticsWendy VasquezNo ratings yet
- Antibiotic 1-Terminology: 1. Inhibition of Cell Wall SynthesisDocument12 pagesAntibiotic 1-Terminology: 1. Inhibition of Cell Wall SynthesismidoNo ratings yet
- Pharmacology AntibioticsDocument70 pagesPharmacology Antibioticsmaggie100% (1)
- Bio ProjectDocument16 pagesBio ProjectmuddurajusrpNo ratings yet
- Antibacterial Agents NotesDocument6 pagesAntibacterial Agents NotesschxzerrydawnNo ratings yet
- Antibiotics EssayDocument5 pagesAntibiotics EssayIshwarya JonathanNo ratings yet
- Antimicrobials and Cytotoxic Drugs: DR Caroline Tetteyfio Koney 37 Military Hospital Accra Feb 2012Document58 pagesAntimicrobials and Cytotoxic Drugs: DR Caroline Tetteyfio Koney 37 Military Hospital Accra Feb 2012Fred OseiNo ratings yet
- 2011 PK-PD AntibiotikDocument88 pages2011 PK-PD AntibiotikUniatimelindaNo ratings yet
- Antimicrobial Therapy in Veterinary MedicineFrom EverandAntimicrobial Therapy in Veterinary MedicineSteeve GiguèreRating: 4 out of 5 stars4/5 (1)
- A Career in Chromosomes: Matters! Matters!Document1 pageA Career in Chromosomes: Matters! Matters!Hartford CourantNo ratings yet
- Use of CowDung As A Source of Bio Culturing For ETPDocument7 pagesUse of CowDung As A Source of Bio Culturing For ETPRG SegaranNo ratings yet
- Paroxysmal Cold Hemoglobinuria: Donath-Landstiener Screening TestDocument1 pageParoxysmal Cold Hemoglobinuria: Donath-Landstiener Screening TestMichelle San Miguel FeguroNo ratings yet
- Poster Burkholderia + Reference FixDocument7 pagesPoster Burkholderia + Reference Fixchew tiarsondangNo ratings yet
- CAYRAPF – MED II, PULMONOLOGY - FEBRUARY 2017, 2ND SEMESTERDocument8 pagesCAYRAPF – MED II, PULMONOLOGY - FEBRUARY 2017, 2ND SEMESTERMiguel Cuevas DolotNo ratings yet
- Summary Compassionate Use Remdesivir Gilead - enDocument43 pagesSummary Compassionate Use Remdesivir Gilead - enlelaniaNo ratings yet
- The Differential Role of Reactive Oxygen Species in Early and Late Stages of Cancer-DikonversiDocument11 pagesThe Differential Role of Reactive Oxygen Species in Early and Late Stages of Cancer-DikonversiTasya Aulia PNo ratings yet
- Medical Surgical Nursing Understanding HemophiliaDocument2 pagesMedical Surgical Nursing Understanding HemophiliaChieChay DubNo ratings yet
- Reaction 20230305 1400Document92 pagesReaction 20230305 1400khushbu patelNo ratings yet
- Biology Presentation Alzheimer'sDocument14 pagesBiology Presentation Alzheimer'skkathrynanna100% (4)
- Chloramphenicol From WikipediaDocument9 pagesChloramphenicol From WikipediaMuhammad Miftahul HudaNo ratings yet
- Antiviral DrugsDocument2 pagesAntiviral DrugsEzraai HafizNo ratings yet
- Learning Activity 7Document26 pagesLearning Activity 7John Harold Astronomo67% (6)
- c6 Microbiology Tortora TestbankDocument19 pagesc6 Microbiology Tortora Testbankwhitewave25No ratings yet
- 3 Urine and Bladder WashingsDocument23 pages3 Urine and Bladder WashingsnanxtoyahNo ratings yet
- 57 2 3 BiologyDocument15 pages57 2 3 BiologyAadya SinghNo ratings yet
- Unit 1, Mock 1 QPDocument18 pagesUnit 1, Mock 1 QPMohammad IzazNo ratings yet
- Blood Groups: HAP Unit 5thDocument31 pagesBlood Groups: HAP Unit 5thC RonaldoNo ratings yet
- Ahmed Negida CVDocument5 pagesAhmed Negida CVمحمد سعيدNo ratings yet
- Retinoic Acid and Its Derivatives in SkinDocument14 pagesRetinoic Acid and Its Derivatives in SkinBryan NguyenNo ratings yet
- 1 Overview & DigestionAbsorption Protein MetabolismDocument37 pages1 Overview & DigestionAbsorption Protein MetabolismAshish K JoyNo ratings yet
- Stage in Interphase Percentage Taken Up in The Cell Cycle Duration (In Hours) DescriptionDocument1 pageStage in Interphase Percentage Taken Up in The Cell Cycle Duration (In Hours) DescriptionClarish MaganaNo ratings yet
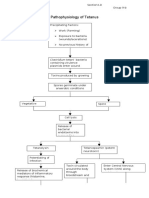
- Pathophysiology of Tetanus: Clostridium Tetani BacteriaDocument3 pagesPathophysiology of Tetanus: Clostridium Tetani BacteriaSlepy chng100% (1)
- BBL Crystal Identification Systems Enteric-Nonfermenter ID KitDocument16 pagesBBL Crystal Identification Systems Enteric-Nonfermenter ID KitWinona ShenaniNo ratings yet
- Autophagy Provides A Conceptual Therapeutic Framework For Bone Metastasis From Prostate CancerDocument8 pagesAutophagy Provides A Conceptual Therapeutic Framework For Bone Metastasis From Prostate CancerAnnisa RahmaNo ratings yet
- Microbial Toxins PDFDocument11 pagesMicrobial Toxins PDFAnonymous OPix6Tyk5INo ratings yet
- ORAL CANCER ADOD-2-110 Annals of Dentistry and Oral Disorders Ambarkova Oral CancerDocument2 pagesORAL CANCER ADOD-2-110 Annals of Dentistry and Oral Disorders Ambarkova Oral CancerVesna AmbarkovaNo ratings yet