Professional Documents
Culture Documents
Osteomielitis y Cultivos
Uploaded by
julionline7Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Osteomielitis y Cultivos
Uploaded by
julionline7Copyright:
Available Formats
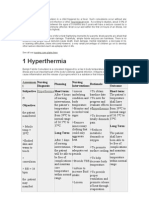
ORIGINAL INVESTIGATION
Etiologic Diagnosis of Chronic Osteomyelitis
A Prospective Study
Andres F. Zuluaga, MD, MSc; Wilson Galvis, MD; Juan G. Saldarriaga, MD;
Maria Agudelo, MD; Beatriz E. Salazar; Omar Vesga, MD
Background: Although bone specimens were established Results: Bone cultures allowed agent identification in
25 years ago as the gold standard for etiologic diagnosis 94% of cases, including anaerobic bacteria in 14%. Cul-
of chronic osteomyelitis, recent studies suggest that non- tures of nonbone and bone specimens gave identical re-
bone specimens are as accurate as bone to identify the caus- sults in 30% of patients, with slightly better concor-
ative agent. We examined concordance rates between cul- dance in chronic osteomyelitis caused by Staphylococcus
tures from nonbone and bone specimens in 100 patients. aureus (42%) than by all other bacterial species (22%).
However, statistical concordance determined by the
Methods: Prospective study conducted at Hospital Uni- Cohen kappa statistic was less than 0 (−0.0092±0.0324),
versitario San Vicente de Paul, a 750-bed university-based indicating that the observed concordance was no better
hospital located in Medellı́n, Colombia. We included than that expected by chance alone (P⬎.99).
patients with chronic osteomyelitis who had been free of Conclusions: Appropriate diagnosis and therapy of chronic
antibiotic therapy for at least 48 hours, excluding those osteomyelitis require microbiologic cultures of the infected
with diabetic foot and decubitus ulcers. At least 1 nonbone bone. Nonbone specimens are not valid for this purpose.
and 1 bone specimen were taken from each individual and
subjected to complete microbiologic analysis. Arch Intern Med. 2006;166:95-100
T
HE INFECTION OF BONE THAT causative organism(s) and knowledge of
contains bone marrow, the pattern of susceptibility.2-5
called osteomyelitis, is as The choice of bone as the ideal speci-
old as humankind and con- men for microbiologic diagnosis of osteo-
tinues to be an important myelitis is based on common sense and a
problem for modern medicine owing to its classic retrospective study of 40 patients
high morbidity and sequelae.1,2 Acute os- published by Mackowiak et al6 27 years
teomyelitis evolves over the course of days ago. More recent studies came to a simi-
to a few weeks and can be cured with an- lar conclusion, but data collection was ret-
tibiotic therapy alone. Chronic osteomy- rospective, included a small number of pa-
elitis (COM), on the other hand, is a re- tients, or had different objectives.7-10 The
lapsing and persistent infection that difficulties inherent in the process of ob-
evolves over months to years and is char- taining bone specimens led to new ap-
acterized by low-grade inflammation, pres- proaches during the last decade, with 3
ence of dead bone (sequestrum), new bone studies concluding that specimens from si-
apposition, and fistulous tracts.3 The most nus tracts and other soft tissue were as ac-
Author Affiliations: Section of important point in relation to chronic bone curate as bone to identify the etiologic
Infection Diseases, Department infections is the difficulty to correctly es- agents of osteomyelitis.11-13 Together, these
of Medicine (Drs Zuluaga, tablish the etiologic agent and the proper 3 studies evaluated 155 patients, but some
Galvis, Agudelo, and Vesga and treatment to cure the patient.4 Nowa- experts disagree with these findings and
Ms Salazar), Department of days, to arrest COM, most experts con- insist that bone specimens must be the gold
Pharmacology (Dr Zuluaga), sider it essential to provide adequate drain- standard for etiologic diagnosis of
and Section of Orthopedics,
age, thorough debridement, obliteration COM.14-16 In fact, it is difficult to draw de-
Department of Surgery
(Dr Saldarriaga), University of
of dead space and soft tissue, wound pro- finitive conclusions from these articles be-
Antioquia Medical School and tection, and intravenous antibiotic treat- cause they have diverse methodologic
Hospital Universitario San ment for at least 4 to 6 weeks.2-4 Proper flaws, thoroughly exposed elsewhere.7
Vicente de Paul, Medellı́n, selection of therapy should always be made The lack of agreement on the best
Colombia. on the basis of correct identification of the sample to use for microbiologic diagno-
(REPRINTED) ARCH INTERN MED/ VOL 166, JAN 9, 2006 WWW.ARCHINTERNMED.COM
95
©2006 American Medical Association. All rights reserved.
Downloaded From: http://archinte.jamanetwork.com/ by a Central Michigan University User on 09/23/2015
sis of COM demands new research on the topic because bacteria.19 Intravenous (IV) antibiotic therapy was begun
mistakes in the identification of the pathogen will lead once the susceptibility pattern of the bone-infecting organ-
to wrong treatment, contributing further to the “no cure” isms was established and continued for 28 to 42 days. In
stigma of this expensive illness.5 The aim of the present cases where internal osteosynthesis material was left in
place, suppressive antibiotic therapy followed IV treatment,
prospective study is to determine the microbiologic con-
stopping 4 weeks after such material was removed. To evalu-
cordance of nonbone with bone specimens, taking the ate the success of therapy, available patients were observed
latter as the gold standard. by the researchers at the outpatient unit or by telephone
interviews for a minimum of 2 and up to 3 years.
METHODS
STATISTICAL ANALYSIS
STUDY DESIGN AND PATIENTS
Isolates from the infected bone were compared with isolates
From February 2001 to December 2002, patients of any age, from nonbone specimens for each patient. Nonbone speci-
sex, ethnicity, and economic condition hospitalized with a di- mens were considered concordant with the bone when they grew
agnosis of osteomyelitis at Hospital Universitario San Vicente exactly the same pathogens isolated from the bone and had iden-
de Paul in Medellı́n, Colombia, were prospectively screened for tical susceptibility patterns. Concordance was calculated for all
COM. Chronic osteomyelitis was defined as a bone infection that causes and for COM caused by Staphylococcus aureus, the agent
was worse or had not improved clinically or microbiologically most commonly isolated from infected bone.
after 1 month of evolution, independent of the presence or ab- We used the Cohen kappa statistic as the measure of con-
sence of surgical and/or antimicrobial therapy. This study was cordance for the dichotomous data produced by bone and non-
approved by the human research ethics committees of the Uni- bone specimens and quantified the probability that the value
versity of Antioquia Medical School and Hospital Universi- found for kappa differed statistically from 0 by computing P
tario San Vicente de Paul. values using the 1-sided test validated by Landis and Koch.20
For Pⱕ.05, the null hypothesis (kappa ⱕ0) was rejected. Kappa
values of 0.0 to 0.40, 0.41 to 0.60, 0.61 to 0.80, and 0.81 to 1.0
PROCEDURES represent “marginal,” “moderate,” “substantial,” and “almost
perfect” agreement, respectively. On the other hand, for P⬎.05,
Patients fulfilling our definition of COM were assigned to the the null hypothesis was accepted, concluding that both diag-
same process: (1) interruption of all antibiotic therapy at least nostic approaches are independent, ie, the observed agree-
48 hours before specimen collection; (2) surgical biopsy of the ment is no better than would be expected by chance alone.
infected bone for histopathologic and microbiologic diagno- To determine if conditions of the skin incised by the sur-
sis, accepting specimens only from bone marrow, sequestra, and geon to take the bone biopsy specimen (healthy vs infected skin)
cortical bone, and rejecting debridement material even if it con- had any influence in the number of microorganisms isolated
tained bone tissue; and (3) microbiologic study of nonbone speci- from the bone (monomicrobial vs polymicrobial COM), we con-
mens directly related to the infected bone, collected during sur- structed 2⫻2 contingency tables and determined the signifi-
gery or in the ward following standard aseptic procedures, cance of the differences by Yates-corrected 2 analysis. For data
including soft tissue biopsy, swabs from surgical wounds, pus management and analysis, we used Microsoft Excel 2003 (Mi-
draining through sinus tracts or orifices left by orthopedic pins, crosoft Corp, Redmond, Wash), Epi-Info, version 3.3 (CDC,
and pus aspirated from soft tissue surrounding the infected bone. Atlanta, Ga), InStat version 3.06 (GraphPad Software, San Diego,
All these criteria were directly verified by the research group. Calif ), and StatXact-5 (Cytel Software Corp, Boston, Mass).
Orthopedists were further required to specify whether sur-
gical access to the infected bone was made through intact skin
or through infected soft tissue. Since surgical incision through RESULTS
infected soft tissue can contaminate the bone, we imple-
mented a bone biopsy protocol designed to reduce contami- During the study period, 121 patients were diagnosed as
nation to a minimum. Briefly, the surgeon performed a thor- having osteomyelitis not related to diabetic foot or de-
ough wash and debridement of the infected soft tissue before cubitus ulcers. Twenty-one patients were excluded be-
accessing the bone, a specimen from which was taken only af- cause antibiotic treatment was not stopped 48 hours be-
ter discarding superficial cortical bone by curettage. To deter- fore the bone biopsy (n=13), evolution of osteomyelitis
mine if access through infected soft tissue was more com-
monly associated with polymicrobial bone cultures (a sign of
was shorter than 1 month (n=5), and lack of nonbone
potential bone contamination), we compared such outcome with (n=2) or bone specimens (n=1 patient). One hundred
that of bone biopsy specimens taken by incisions through healthy patients fulfilled the inclusion criteria, 72 male and 28
skin. Patients with diabetic foot and decubitus ulcers were ex- female, aged 9 to 83 years (mean±SD age, 38±18 years).
cluded because the value of bone cultures is clear in the first The COM had evolved over a period of 1 to 384 months
and uncertain in the second condition.17,18 before diagnosis (median, 6 months), and both speci-
Patients were registered in a database that included age, mens were taken after 1 to 120 days of hospitalization
sex, employment, hospitalization time, bone involved, time (median, 5 days).
with COM, mechanism of bone infection, clinical condition Tibia (34%) and femur (33%) were the most fre-
of the skin incised by the surgeon to take the bone speci- quent foci of the COM, followed by fibula (8%, 5 asso-
men, type of specimens cultured, and microbiologic identifi-
cation and susceptibility pattern of organisms grown in aero-
ciated with the tibia), iliac crest (7%), vertebra (3%), hu-
bic (Vitek Systems; bioMerieux, Hazelwood, Mo) and merus (3%, 1 associated with the ulna), and other
anaerobic atmosphere (Rapid ID32A, bioMerieux). Routine medullar bones (12%). In most cases (n=93), bacteria
and standard laboratory techniques for transportation and reached the bone by local spread from a contiguous source
culture of aerobic and anaerobic microorganisms were fol- of infection; the other 7 patients had hematogenous os-
lowed, including special stains for bacteria, fungi, and myco- teomyelitis. Contiguous sources of infection appeared af-
(REPRINTED) ARCH INTERN MED/ VOL 166, JAN 9, 2006 WWW.ARCHINTERNMED.COM
96
©2006 American Medical Association. All rights reserved.
Downloaded From: http://archinte.jamanetwork.com/ by a Central Michigan University User on 09/23/2015
ter violent trauma (n = 64), surgical procedures (n=25),
and infection of neighboring joints or skin structures Table 1. Specimens Taken From Study Patients
(n=4). With Chronic Osteomyelitis
Table 1 lists the type of specimens cultured. Bone
Specimen Number
specimens were taken from all patients during open sur-
gery and subjected to complete microbiologic study. Se- Bone 100
lection of the bone structure best suited for culture was Cortical bone biopsy 83
Sequestra 13
made by the surgeon based on the presence of macro- Bone marrow 7
scopic signs of infection. As soon as possible before or Nonbone 100
after the bone biopsy, a member of the research group Soft tissue: pus swabs 49
also took 1 nonbone specimen per patient from soft tis- Infected surgical wound swabs 29
sue with signs of infection or colonization. Sinus tract: pus swabs 17
Table 2 lists the bacteria and fungi obtained from cul- Orthopedic pin orifices: pus swabs 3
Soft tissue: pus aspirates 2
tures of bone and nonbone specimens and details the re-
sults of concordance analysis categorized by bone or-
ganisms (n=150) and by patients (n = 100). The Figure
illustrates the causes of COM based on bone cultures and
the agreement of nonbone analyses for each etiologic tive cultures in both specimens (true agreement with nega-
group. Bone cultures allowed isolation and identifica- tive bone findings, 4%). The diagnostic accuracy of
tion of the cause of COM for 94 patients; the other 6 sub- nonbone specimens, as determined by the rate of micro-
jects had COM demonstrated by bone histopathologic biologic agreement with bone cultures, was 30%. The
analysis, but no organisms were visualized or isolated from Cohen kappa value was lower than 0 (−0.0092±0.0324;
their bone specimens, including aerobic and anaerobic P⬎.99), confirming that the observed agreement of 30%
bacteria, Mycobacterium species, and fungi. Bone cul- was the same as that expected by chance.
tures from these 94 patients produced 150 isolates: S au- Two specific subgroups of patients with COM for
reus was the most frequent (43/150, 29%), followed by whom nonbone specimens are supposedly well suited to
10 different species of the Enterobacteriaceae family etiologic diagnosis also showed a lack of concordance with
(n=24, 16%), Enterococcus species (n = 22, 14.67%), an- the bone based on the Cohen kappa test: COM caused
aerobic bacteria (n = 16, 10.67%), and others, including by S aureus (vs other causes) and COM caused by local
Pseudomonas aeruginosa, coagulase-negative staphylo- spread of a neighboring infection (vs hematogenous
cocci, Streptococcus species, and Acinetobacter calcoace- COM). Similarly, we found complete independence be-
ticus-baumannii complex. Anaerobic bone cultures were tween some specimens considered concordant by na-
done for 92 patients, and 13 (14%) of them produced 16 ture, ie, sequestra (bone) and sinus tracts (nonbone speci-
organisms primarily associated with violent trauma. The men). Concordance was also absent in patients for whom
first bone specimen gave negative cultures in 10 pa- bone specimens had to be taken by incising infected or
tients. Follow-up showed that 2 had anaerobic COM (1 healthy skin and soft tissues. Table 4 lists the rate of
by Peptostreptococcus prevotii and 1 by unclassified an- concordance and respective kappa values for these sub-
aerobe gram-negative coccobacilli); 2 had aerobic bac- groups, none statistically different from 0. In other words,
teria isolated from the bone in samples from a second bi- the results from cultures of nonbone specimens are com-
opsy; and 6 persisted with negative bone cultures. pletely independent from bone specimens, without re-
Nonbone specimens were also negative for 11 pa- gard for the group analyzed.
tients but produced 116 isolates from the other 89 sub- There was no difference in the frequency of polymi-
jects. Staphylococcus aureus was again the most fre- crobial COM between patients with healthy vs colo-
quently found organism (44/116, 38%), followed by nized or infected soft tissue, which suggests that the con-
Enterobacteriaceae (n = 22, 19%), coagulase-negative ditions of the skin incised by the surgeon to take the bone
staphylococci and P aeruginosa (n=13 for each, 11%), and biopsy specimen had no influence on the concordance
others like Enterococcus species, Streptococcus species, rates found by this study (Table 5).
other aerobes, anaerobes, and fungi. Concordance analy- In addition to surgical treatment, all patients re-
sis by microorganism was 19.33% for all causes and ceived at least 28 days of IV antibiotic therapy based on
41.86% for S aureus, the highest for any bacterial spe- the antibiograms of bone isolates. Microorganisms iso-
cies (Table 2). Cohen kappa values computed for COM lated from soft tissue were not considered for antibiotic
caused by S aureus or any other cause were all close to 0, treatment except in cases with clinical signs of skin and
indicating no microbiologic correlation of nonbone with soft tissue infection that were treated for 5 to 10 days.
bone specimens (Table 2). Only 26 subjects were available for follow-up for a pe-
Concordance analysis by patients (Table 3) showed riod of 2 to 3 years: 18 patients (69%) were cured (15
that 26 had exactly the same organisms in nonbone and without sequelae, 2 with chronic pain, and 1 with limb
bone specimens (true agreement with positive bone find- amputation); 6 patients (23%) still had COM at the third
ings, 26%), and 68 had different microorganisms in each year; and the other 2 (8%) died for reasons not related
kind of specimen (disagreement with positive bone find- to COM but without certainty about the cure of their bone
ings, 68%). On the other hand, 2 patients had positive infections.
nonbone findings but sterile bone cultures (disagree- Histopathologic studies were performed for 39 pa-
ment with negative bone findings, 2%), while 4 had nega- tients, including all 6 with bone-negative cultures. Chronic
(REPRINTED) ARCH INTERN MED/ VOL 166, JAN 9, 2006 WWW.ARCHINTERNMED.COM
97
©2006 American Medical Association. All rights reserved.
Downloaded From: http://archinte.jamanetwork.com/ by a Central Michigan University User on 09/23/2015
Table 2. Etiology by Bone Cultures of 100 Patients With Chronic Osteomyelitis
No. of Isolates Concordance*
By Organism, By Patient,
Bone Nonbone No. Found/ Cohen No. (%) Cohen
Microorganisms Cultures Cultures Total No. (%) Kappa (n = 100) Kappa
Gram-positive aerobes 89 75 24/89 (27) −0.5460 22 (22) −0.3600
Staphylococcus aureus 43 44 18/43 (42) 0.1744 18 (18) −0.0370
Enterococcus faecalis 19 9 3/19 (16) 0.1446 2 (2)† 0.1611
Staphylococcus epidermidis 5 7 1/5 (20) 0.1329 1 (1) 0.1150
Other coagulase-negative 8 6 0/8 (0) −0.0470 0 (0) −0.0073
staphylococci
Streptococcus agalactie 3 2 2/3 (67) 1 (1)†
Streptococcus constellatus 2 2 0 0
Enterococcus faecium 2 0 0 0
Enterococcus avium 1 1 0 0
Streptococcus dysgalactiae 1 1 0 0
Streptococcus oralis 1 0 0 0
Streptococcus mitis 1 0 0 0
Streptococcus salivarious 1 0 0 0
Streptococcus bovis 1 1 0 0
Streptococcus intermedius 0 1 0 0
Streptococcus sanguis 0 1 0 0
Gram-positive cocci‡ 1 0 0 0
Gram-negative aerobes 45 39 5/45 (11) −0.2210 4 (4) −0.0670
Pseudomonas aeruginosa 14 13 2/14 (14) 0.0640 2 (2) 0.0154
Escherichia coli 9 11 1/9 (11) 0.0364 1 (1) 0.0011
Acinetobacter baumannii 5 3 1/5 (20) 0.2307 0† 0.2207
Enterobacter cloacae 4 3 0 0
Proteus penneri 3 0 0 0
Morganela morganii 2 1 0 0
Proteu mirabilis 2 3 1/2 (50) 1 (1)
Proteus vulgaris 1 1 0 0
Pseudomonas fluorescens 1 0 0 0
Acinetobacter lwoffi 1 0 0 0
Enterobacter aerogenes 1 0 0 0
Serratia fonticola 1 0 0 0
Klebsiella oxytoca 1 0 0 0
Klebsiella pneumoniae 0 2 0 0
Providencia rettgeri 0 1 0 0
Comamonas acidovorans 0 1 0 0
Anaerobes 16 1 0 −0.0120 0 −0.0200
Clostridium difficile 4 0 0 0
Propionibacterium acnes 2 0 0 0
Bacteroides urealyticus 2 0 0 0
Porphyromonas species 2 0 0 0
Peptostreptococcus prevotii 1 0 0 0
Clostridium perfringens 1 0 0 0
Gram-positive coccobacilli‡ 1 0 0 0
Gram-negative coccobacilli‡ 3 1 0 0
Fungi 0 1 0 0
Candida albicans 0 1 0 0
Sterile cultures 6 11 4/6 (67) 0.4428 4 (4) −0.1460
Total 150 116 29/150 (19) −0.7300 30 (30) −0.0090
*Cohen kappa P ⬎.10 for all cases (the observed agreement between bone and nonbone specimens is no better than would be expected by chance alone).
Kappa values were not calculated for organisms isolated from fewer than 5 bone specimens.
†Patients with polymicrobial bone infections are represented only once: 2 with S aureus (1 also had E faecalis and 1 A baumannii ) and 1 with Streptococcus
agalactie who also had P aeruginosa.
‡Unclassified microorganisms.
osteomyelitis was confirmed in 38 cases, and 1 with “nor- COMMENT
mal” histopathologic bone findings had methicillin-
susceptible S aureus grow in bone and nonbone cul-
tures (concordant) after 4 months of purulent discharge This prospective study, assessing the validity of speci-
from a sinus tract related to surgical correction of an open mens other than bone to establish the cause of COM, was
fracture of the left tibia. motivated by the poor prognosis of patients with post-
(REPRINTED) ARCH INTERN MED/ VOL 166, JAN 9, 2006 WWW.ARCHINTERNMED.COM
98
©2006 American Medical Association. All rights reserved.
Downloaded From: http://archinte.jamanetwork.com/ by a Central Michigan University User on 09/23/2015
Staphylococcus aureus
Table 4. Concordance Between Bone and Nonbone
Specimens to Identify the Cause of COM
Enterococcus species in Different Subsets of Patients
Pseudomonas aeruginosa
Coagulase-Negative Concordant
Cause of COM (Bone Cultures)
Staphylococci Patients, Cultures, Cohen P
Anaerobic Bacteria Patient Subset No. No. (%) Kappa ± SE Value*
Streptococcus species Staphylococcus 43 18 (42) −0.585 ± 0.0666 ⬎.99
aureus
Escherichia coli
Other cause 57 12 (21) −0.043 ± 0.0527 ⬎.99
Enterobacter cloacae Hematogenous 7 4 (57) −0.272 ± 0.2303 ⬎.99
Other Enterobacteriaceae COM
Local spread 93 26 (28) 0.0087 ± 0.0265 ⬎.99
Acinetobacter baumannii COM
Other Bacterial Species Concordant Sequestra 13 2 (15) 0.0137 ± 0.0193 ⬎.99
Discordant specimens
Sterile Bone Cultures
Other bone 87 28 (32) −0.015 ± 0.0371 ⬎.99
specimens
0 5 10 15 20 25 30 35 40 45 50
Sinus tracts 17 6 (35) 0.0507 ± 0.0534 ⬎.99
Patients, No. (n = 100)
Other nonbone 83 24 (29) −0.021 ± 0.0377 ⬎.99
specimens
Figure. Causes of chronic osteomyelitis (COM) based on bone cultures from Incision
100 patients. Black bars represent the number of patients with identical Intact skin 35 10 (29) −0.035 ± 0.0617 ⬎.99
isolates from bone and nonbone specimens (concordant cultures); frequencies Infected skin 65 20 (31) 0.0047 ± 0.0372 ⬎.99
add to more than 100 because 65% had polymicrobial bone infection.
Abbreviation: COM, chronic osteomyelitis.
*P ⬎.05 implies that the Cohen kappa value is not statistically different
Table 3. Microbiological Concordance of Nonbone from 0, and that kappa values not different from 0 indicate lack of
With Bone Specimens to Identify the Cause concordance.
of Chronic Osteomyelitis in 100 Patients
Bone (Gold Standard) Table 5. Frequency of Monomicrobial and Polymicrobial
Bone Cultures by Incised Skin Condition
Nonbone Cause Cause in 100 Patients With COM
(New Method) Identified Not Identified Total
Cause identified 26 2 28 Cultures, No. (%)
Cause not identified 68 4 72 Patients, P
Total 94 6 100 Incision Group No. Monomicrobial Polymicrobial Value
Intact skin 35 23 (66) 12 (34)
.91
Infected skin 65 42 (65) 23 (35)
Abbreviation: COM, chronic osteomyelitis.
traumatic COM reported by our orthopedic surgeons. Be-
fore 1998, antibiotic therapy of COM at our institution
was based on the microorganisms isolated from non- isms.11-13 Today, infectious diseases textbooks recog-
bone specimens, and the surgeons cited at least 3 stud- nize the work of Mackowiak et al, but instead of high-
ies supporting their approach.11-13 Although back then lighting their most valuable contribution emphasize
we had no data, clinical observation suggested an incur- that nonbone specimens are good for diagnosis of
able disease because most patients treated under such an S aureus COM.21
approach experienced a relapse. Our group’s retrospective findings with 50 patients7
In view of the situation, members of our group re- contradicted the conclusion of Mackowiak et al6 regard-
viewed the evidence available and conducted a retro- ing S aureus COM: only 38% of nonbone specimens were
spective study of 50 patients seen at the Section of In- concordant with bone cultures. The present study, in-
fectious Diseases between February 1998 and August cluding twice the number of patients in a prospective de-
2001.7 Our results confirmed the most important con- sign that allowed control of confounding variables, also
clusions of Mackowiak et al6 and contradicted the find- found a low level of concordance for S aureus (42%). If
ings of the more recent articles, but that study had some the analysis is repeated discriminating polymicrobial from
design problems, including its retrospective nature. Mack- monomicrobial COM involving S aureus, concordance
owiak et al had concluded that nonbone specimens did drops to 13% for the first and increases to 57% for the
not predict the species of bacteria actually involved with second type of bone infection. Such level of diagnostic
bone infection and that every effort should be made to accuracy for monomicrobial staphylococcal osteomyeli-
culture the bone, with 1 exception: S aureus appeared cor- tis is still too low to use as a foundation for the pro-
rectly predicted in 78% of patients by swab cultures of longed and difficult treatment of this expensive disease.
the sinus tracts associated with COM.6 In the last 10 years, The Cohen kappa tests applied to these data are con-
3 other independent studies concluded that any non- clusive about the lack of concordance between nonbone
bone specimen was as good as the bone to establish the and bone cultures for etiologic diagnosis of COM inde-
cause of COM, including all possible microorgan- pendent of the organisms involved, patient subgroup, or
(REPRINTED) ARCH INTERN MED/ VOL 166, JAN 9, 2006 WWW.ARCHINTERNMED.COM
99
©2006 American Medical Association. All rights reserved.
Downloaded From: http://archinte.jamanetwork.com/ by a Central Michigan University User on 09/23/2015
specimen type. Our results regarding S aureus markedly Acknowledgment: We thank the professors of the Sec-
differ from those in previous reports for at least 2 reasons: tions of Orthopedics and Infectious Diseases of the De-
first, we collected data in a prospective manner and under partments of Surgery and Medicine, respectively, for their
a strict surgical protocol that prevented contamination of participation in the surgical and clinical treatment of our
bone specimens with organisms colonizing adjacent soft patients, to whom we are also deeply indebted.
tissue; second, we considered discordant S aureus isolates
with different susceptibility patterns. In fact, general con-
cordance for S aureus would rise to 81.4% if all isolates were
taken into account independently of their antibiograms, but REFERENCES
almost half of the patients (17 of 35) would have received
inappropriate treatment if it were guided by nonbone cul- 1. Weaver DS, Perry GH, Macchiarelli R, Bondioli L. A surgical amputation in 2nd
century Rome. Lancet. 2000;356:686.
tures: 7 had S aureus differing in susceptibility from S au- 2. Lew DP, Waldvogel FA. Osteomyelitis. Lancet. 2004;364:369-379.
reus in the bone, and 10 had identical S aureus in both speci- 3. Norden CW. Acute and chronic osteomyelitis. In: Armstrong D, Cohen J, eds.
mens but different copathogens in the bone. Infectious Diseases. London, England: Mosby; 1999:410–431.
The data also support the conclusion that bone biop- 4. Lew DP, Waldvogel FA. Osteomyelitis. N Engl J Med. 1997;336:999-1007.
5. Mader JT, Calhoun J. Osteomyelitis. In: Mandell GL, Bennett JE, Dolin R, ed. Prin-
sies are highly productive (94%) and not affected by the
ciples and Practice of Infectious Diseases. 5th ed. Philadelphia, Pa: Churchill Liv-
conditions of overlying soft tissue as long as the proce- ingstone; 2000:1182-1196.
dure is performed under surgical protocols designed to 6. Mackowiak PA, Jones SR, Smith JW. Diagnostic value of sinus-tract cultures in
minimize the risk of contamination. This is important be- chronic osteomyelitis. JAMA. 1978;239:2772-2775.
cause many times the surgeon has only 1 opportunity for 7. Zuluaga AF, Galvis W, Jaimes F, Vesga O. Lack of microbiological concordance
between bone and non-bone specimens in chronic osteomyelitis: an observa-
bone sampling, precisely at the time of debridement of colo- tional study. BMC Infect Dis [serial online]. 2002;2:8[6 screens]. Available at:
nized soft tissue surrounding the infected bone. Also, in http://www.biomedcentral.com/1471-2334/2/8.
contrast to common belief, sequestrum findings were not 8. Khatri G, Wagner DK, Sohnle PG. Effect of bone biopsy in guiding antimicrobial
more concordant with those of nonbone specimens than therapy for osteomyelitis complicating open wounds. Am J Med Sci. 2001;
321:367-371.
bone or bone marrow specimens, and swab cultures from
9. Howard CB, Einhorn M, Dagan R, et al. Fine-needle bone biopsy to diagnose
sinus tracts were no better at predicting COM cause than osteomyelitis. J Bone Joint Surg Br. 1994;76:311-314.
any other nonbone specimen. The importance of anaero- 10. Jacobson IV, Sieling WL. Microbiology of secondary osteomyelitis. Value of bone
bic cultures of the bone, which were isolated from 14% of biopsy. S Afr Med J. 1987;72:476-477.
our patients, cannot be overemphasized.22 11. Mousa HA-L. Evaluation of sinus-track cultures in chronic bone infection. J Bone
Joint Surg Br. 1997;79:567-570.
In conclusion, only bone cultures should be used to 12. Perry CR, Pearson RL, Miller GA. Accuracy of cultures of material from swab-
guide antibiotic treatment in patients with COM, includ- bing of the superficial aspect of the wound and needle biopsy in the preopera-
ing those infected by S aureus. Choosing nonbone cul- tive assessment of osteomyelitis. J Bone Joint Surg Am. 1991;73:745-749.
tures for this purpose will lead to incorrect etiologic COM 13. Patzakis MJ, Wilkins J, Kumar J, et al. Comparison of the results of bacterial
cultures from multiple sites in chronic osteomyelitis: a prospective study. J Bone
diagnosis and, therefore, inappropriate therapy.
Joint Surg Am. 1994;76:664-666.
14. Norden CW. Lessons learned from animal models of osteomyelitis. Rev Infect
Accepted for Publication: August 3, 2005. Dis. 1988;10:103-110.
Correspondence: Omar Vesga, MD, University of Antio- 15. Mader JT, Norden C, Nelson JD, Calandra GB. Evaluation of new anti-infective
quia Medical School, Lab 630 SIU, Calle 62 No. 52-59, Me- drugs for the treatment of osteomyelitis in adults. Clin Infect Dis. 1992;
15(suppl 1):S155-S161.
dellı́n, Colombia (ovesgam@medicina.udea.eud.co). 16. Haas DW, McAndrew MP. Bacterial osteomyelitis in adults: evolving consider-
Financial Disclosure: None. ations in diagnosis and treatment. Am J Med. 1996;101:550-561.
Funding/Support: This study was funded by research 17. Wheat LJ, Allen SD, Henry M, et al. Diabetic foot infections: bacteriologic analysis.
grant 8700-4656 from the University of Antioquia. Arch Intern Med. 1986;146:1935-1940.
18. Darouiche RO, Landon GC, Klima M, Musher DM, Markowski J. Osteomyelitis
Role of the Sponsor: The funding organization had no associated with pressure sores. Arch Intern Med. 1994;154:753-758.
role in the design or conduct of the study, collection, man- 19. Isenberg HD. Clinical Microbiology Procedures Handbook. Washington, DC: Ameri-
agement, analysis, or interpretation of the data; or prepa- can Society for Microbiology; 1992.
ration, review, or approval of the manuscript. 20. Landis JR, Koch GG. The measurement of observer agreement for categorical
Previous Presentation: This study was presented at the data. Biometrics. 1977;33:159-174.
21. Berbari EF, Steckelberg JM, Osmon DR. Osteomyelitis. In: Mandell GL, Bennett
43rd Interscience Conference on Antimicrobial Agents JE, Dolin R, eds. Principles and Practice of Infectious Diseases. 6th ed. Phila-
and Chemotherapy (ICAAC); September 14, 2003; delphia, Pa: Elsevier Churchill Livingstone; 2005:1322–1332.
Chicago, Ill. 22. Raff MJ, Melo JC. Anaerobic osteomyelitis. Medicine (Baltimore). 1978;57:83-103.
(REPRINTED) ARCH INTERN MED/ VOL 166, JAN 9, 2006 WWW.ARCHINTERNMED.COM
100
©2006 American Medical Association. All rights reserved.
Downloaded From: http://archinte.jamanetwork.com/ by a Central Michigan University User on 09/23/2015
You might also like
- hsns273 Corrected 2Document21 pageshsns273 Corrected 2api-526511003100% (1)
- CaseDocument54 pagesCaseRaja100% (4)
- Asj-2020-0262tbc o Brucella ImglesDocument8 pagesAsj-2020-0262tbc o Brucella ImglesThais LudenaNo ratings yet
- Dapus RaddDocument20 pagesDapus RaddNur Liza SeptianiNo ratings yet
- 6 SaDocument9 pages6 SaRizqi AmaliaNo ratings yet
- Tuberculous Osteomyelitis: Journal of Bone and Joint Surgery - British Volume August 1997Document6 pagesTuberculous Osteomyelitis: Journal of Bone and Joint Surgery - British Volume August 1997DiahNo ratings yet
- Infeccion Osteoarticular Bacteriana Hematogena en NiñosDocument19 pagesInfeccion Osteoarticular Bacteriana Hematogena en NiñosFernando FernándezNo ratings yet
- Espondilodiscitis Infecciosa Por Patógenos Poco ComunesDocument5 pagesEspondilodiscitis Infecciosa Por Patógenos Poco ComunesOthoniel RamirezNo ratings yet
- Systemic Diseases Affecting Osseointegration TherapyDocument7 pagesSystemic Diseases Affecting Osseointegration TherapyAlfred OrozcoNo ratings yet
- Radiographic Imaging in Osteomyelitis The Role ofDocument11 pagesRadiographic Imaging in Osteomyelitis The Role ofEga AihenaNo ratings yet
- Termaat 2005Document11 pagesTermaat 2005OkyôAmêliâNo ratings yet
- Tuberculous Osteomyelitis: From Mohan Dai Oswal Cancer Treatment and Research Foundation, Ludhiana, IndiaDocument5 pagesTuberculous Osteomyelitis: From Mohan Dai Oswal Cancer Treatment and Research Foundation, Ludhiana, Indiairma suryaniNo ratings yet
- Osteoblastoma: When The Treatment Is Not Minimally Invasive, An OverviewDocument10 pagesOsteoblastoma: When The Treatment Is Not Minimally Invasive, An OverviewAnggi MartaNo ratings yet
- Jurnal PatogenesisDocument6 pagesJurnal PatogenesisErmiati EmhyNo ratings yet
- Necrotizing Sialometaplasia A Malignant Masquerade But Questionable Precancerous Lesion Report of Four CasesDocument6 pagesNecrotizing Sialometaplasia A Malignant Masquerade But Questionable Precancerous Lesion Report of Four CasesTessa T YogaswaryNo ratings yet
- SMW 09797 PDFDocument9 pagesSMW 09797 PDFEJ AguilarNo ratings yet
- Osteoimmunology Inflammatory Osteolysis and Regeneration of The Alveolar BoneDocument18 pagesOsteoimmunology Inflammatory Osteolysis and Regeneration of The Alveolar BoneFelipe Ulloa CastilloNo ratings yet
- Prospective Survey of Acute Osteoarticular Infections in A French Paediatric Orthopedic Surgery UnitDocument7 pagesProspective Survey of Acute Osteoarticular Infections in A French Paediatric Orthopedic Surgery UnitleonardocahyoNo ratings yet
- Jurnal Kedokteran GigiDocument9 pagesJurnal Kedokteran GigiamrinagristaauliaNo ratings yet
- Primary Subacute Hematogenous Osteomyelitis in Children: A Clearer Bacteriological EtiologyDocument6 pagesPrimary Subacute Hematogenous Osteomyelitis in Children: A Clearer Bacteriological EtiologymiNo ratings yet
- The Veterinary Journal: Craig I. Johnson, David J. Argyle, Dylan N. ClementsDocument10 pagesThe Veterinary Journal: Craig I. Johnson, David J. Argyle, Dylan N. ClementsMarNo ratings yet
- Artritis SépticaDocument10 pagesArtritis SépticaCirugía General HUBUNo ratings yet
- OM Stafilococo (Clase Observacionales)Document7 pagesOM Stafilococo (Clase Observacionales)Jairo Camilo Guevara FaríasNo ratings yet
- Pyomyositis: Neuroimaging Clinics of North America November 2011Document11 pagesPyomyositis: Neuroimaging Clinics of North America November 2011karol castellonNo ratings yet
- Jurnal 002Document9 pagesJurnal 002Nadila FaatinNo ratings yet
- VBNMDocument1 pageVBNMHimawan WidyatmikoNo ratings yet
- Pola 2017Document10 pagesPola 2017RobertoNo ratings yet
- Human Brucellosis in Macedonia - 10 Years of Clinical Experience in Endemic RegionDocument10 pagesHuman Brucellosis in Macedonia - 10 Years of Clinical Experience in Endemic RegionFahdNo ratings yet
- Prospective Study of Microbiology of Biofilm in Orthopaedic Implant SurgeryDocument8 pagesProspective Study of Microbiology of Biofilm in Orthopaedic Implant SurgeryIJAR JOURNALNo ratings yet
- A Clinicopathological Spectrum of Myeloma With Varied PresentationsDocument5 pagesA Clinicopathological Spectrum of Myeloma With Varied PresentationsATIKAH NUR HAFIZHAHNo ratings yet
- Cytology of Bone Fine Needle Aspiration BiopsyDocument11 pagesCytology of Bone Fine Needle Aspiration BiopsyRavi MehrotraNo ratings yet
- Diagnosing OsteomyelitisDocument12 pagesDiagnosing Osteomyelitisna huNo ratings yet
- Taub - Osteomyelitis of The Jaw A Retrospective AnalysisDocument7 pagesTaub - Osteomyelitis of The Jaw A Retrospective AnalysisChristopher McMullinNo ratings yet
- Latent Infection of Low-Virulence Anaerobic Bacteria in Degenerated Lumbar Intervertebral DiscsDocument5 pagesLatent Infection of Low-Virulence Anaerobic Bacteria in Degenerated Lumbar Intervertebral Discsvg04No ratings yet
- Natural History of New Horizontal Meniscal Tears in Individuals at Risk For and With Mild To Moderate Osteoarthritis: Data From Osteoarthritis InitiativeDocument10 pagesNatural History of New Horizontal Meniscal Tears in Individuals at Risk For and With Mild To Moderate Osteoarthritis: Data From Osteoarthritis InitiativeDeivisonNo ratings yet
- Worldwide Incidence of Odontogenic Tumors.27Document6 pagesWorldwide Incidence of Odontogenic Tumors.27larissaNo ratings yet
- Dr. Anvita Nilekani - JCDR - Published Article PDFDocument12 pagesDr. Anvita Nilekani - JCDR - Published Article PDFindu mathiNo ratings yet
- File 341742723 Order341742723Document7 pagesFile 341742723 Order341742723s.macharia1643No ratings yet
- Review Article: Histopathology in Periprosthetic Joint Infection: When Will The Morphomolecular Diagnosis Be A Reality?Document11 pagesReview Article: Histopathology in Periprosthetic Joint Infection: When Will The Morphomolecular Diagnosis Be A Reality?pagar bersihNo ratings yet
- Worldwide Incidence of Odontogenic Tumors.27Document6 pagesWorldwide Incidence of Odontogenic Tumors.27larissaNo ratings yet
- Poster 23: Evaluation of Endoscopy in The Diagnosis and Treatment of Obstructive Salivary Gland DiseasesDocument1 pagePoster 23: Evaluation of Endoscopy in The Diagnosis and Treatment of Obstructive Salivary Gland DiseasesAli ahmedNo ratings yet
- Medoralv24 I5 p562Document9 pagesMedoralv24 I5 p562katherineNo ratings yet
- Medoralv 14 I 5 P 239Document6 pagesMedoralv 14 I 5 P 239Dr. Parsa PiroozNo ratings yet
- Antibiotics 11 00568Document8 pagesAntibiotics 11 00568Vincia PaulNo ratings yet
- Patofisiologi OsteomielitisDocument13 pagesPatofisiologi OsteomielitisNoor Rizka YuliaNo ratings yet
- Cystic Lesions of The Jaws A Retrospective ClinicopathologicDocument11 pagesCystic Lesions of The Jaws A Retrospective ClinicopathologicThành Luân NguyễnNo ratings yet
- TB 7 Jurnal TB PK OkDocument7 pagesTB 7 Jurnal TB PK OkKarinta IdeliaNo ratings yet
- Evaluation of The Outcomes of Culture Positive Infections Following An Uneventful Arthroplasty - A Single Institution ExperienceDocument3 pagesEvaluation of The Outcomes of Culture Positive Infections Following An Uneventful Arthroplasty - A Single Institution ExperienceIJAR JOURNALNo ratings yet
- JCLA 2004 Bone Marrow ExaminationDocument21 pagesJCLA 2004 Bone Marrow Examinationoki harisandiNo ratings yet
- Osteoradionecrosis of The Jaws: de Finition, Epidemiology, Staging and Clinical and Radiological Findings. A Concise ReviewDocument9 pagesOsteoradionecrosis of The Jaws: de Finition, Epidemiology, Staging and Clinical and Radiological Findings. A Concise ReviewCecilia AhuetNo ratings yet
- Tumors of Foot and Ankle A Single Institution Experience PDFDocument6 pagesTumors of Foot and Ankle A Single Institution Experience PDFICNo ratings yet
- Medi 96 E5864Document6 pagesMedi 96 E5864mono1144No ratings yet
- Artigo Bjid OsteomieliteDocument10 pagesArtigo Bjid OsteomielitedeviraNo ratings yet
- Septic Arthritis: Current Diagnostic and Therapeutic AlgorithmDocument6 pagesSeptic Arthritis: Current Diagnostic and Therapeutic Algorithmroni pahleviNo ratings yet
- IDSA Osteomielite Vertebral Guideline 2015Document21 pagesIDSA Osteomielite Vertebral Guideline 2015Julia CarijoNo ratings yet
- IDSADocument21 pagesIDSADiana AvilesNo ratings yet
- Biomedicines 12 00715Document21 pagesBiomedicines 12 00715jamel-shamsNo ratings yet
- Parvizi 2013Document9 pagesParvizi 2013juancarlosgucoNo ratings yet
- 0004 07 PDFDocument22 pages0004 07 PDFShela MalubagNo ratings yet
- Ijo 68 1925Document4 pagesIjo 68 1925Afifah Siti NurNo ratings yet
- Stem Cell Biology and Regenerative Medicine in OphthalmologyFrom EverandStem Cell Biology and Regenerative Medicine in OphthalmologyStephen TsangNo ratings yet
- A Compilation of Cellular and Tissue Xenotransplantation Studies (1838-2022): A Promising Approach for the Treatment of DiseasesFrom EverandA Compilation of Cellular and Tissue Xenotransplantation Studies (1838-2022): A Promising Approach for the Treatment of DiseasesNo ratings yet
- Principles of Medical Laboratory Science 1Document20 pagesPrinciples of Medical Laboratory Science 1Davidson BravoNo ratings yet
- Significant Points of The Kindeny Channel of Foot-ShaoyingDocument26 pagesSignificant Points of The Kindeny Channel of Foot-ShaoyingHarrison BungasaluNo ratings yet
- Benign Febrile ConvulsionDocument9 pagesBenign Febrile ConvulsionRoxanne Mae Marcelo BadongenNo ratings yet
- Dissociative DisordersDocument75 pagesDissociative DisordersJennifer Dixon100% (1)
- Daleel EDocument44 pagesDaleel Ealiplus007No ratings yet
- Physical Education 12 Pneumonia: To Be Reported By: Alawi, Lhamiah M. Casano, Diana Elizabeth C. Kinoshita, Ryou GDocument21 pagesPhysical Education 12 Pneumonia: To Be Reported By: Alawi, Lhamiah M. Casano, Diana Elizabeth C. Kinoshita, Ryou GRyou KinoshitaNo ratings yet
- ,, ,, - 3, - Omega-Q AriixDocument3 pages,, ,, - 3, - Omega-Q AriixOlga VoicuNo ratings yet
- LPLT12448 : LPL - Lpl-Rohini (National Reference Lab) Sector - 18, Block - E Rohini DELHI 110085Document6 pagesLPLT12448 : LPL - Lpl-Rohini (National Reference Lab) Sector - 18, Block - E Rohini DELHI 110085Kumar ManglamNo ratings yet
- CC Product CatalogDocument53 pagesCC Product CatalogDON TVNo ratings yet
- RENAP 2009 Training SchedulesDocument3 pagesRENAP 2009 Training SchedulesNoel100% (4)
- A Study To Assess The Effectiveness of Fenugreek Water To Reduce Blood Glucose Levels Among Clients With Diabetes MellitusDocument5 pagesA Study To Assess The Effectiveness of Fenugreek Water To Reduce Blood Glucose Levels Among Clients With Diabetes MellitusEditor IJTSRDNo ratings yet
- Postgraduate Institutes Recognized by PMDCDocument2 pagesPostgraduate Institutes Recognized by PMDCopenid_NJmKfZyv0% (1)
- Interventional BronchosDocument323 pagesInterventional BronchosSmaranda Demian100% (2)
- Assessment Diagnosis Planning Intervention Rationale EvaluationDocument1 pageAssessment Diagnosis Planning Intervention Rationale Evaluationcamile buhangin100% (1)
- Infections Caused by ECTOPARASITESDocument14 pagesInfections Caused by ECTOPARASITESSteven CullcayyNo ratings yet
- Gyne - Case 11 Lower Genital UTI PDFDocument2 pagesGyne - Case 11 Lower Genital UTI PDFcbac1990No ratings yet
- Roland Berger Trend Compendium 2030Document49 pagesRoland Berger Trend Compendium 2030gabrinaNo ratings yet
- Sainath College of Nursing, KatniDocument4 pagesSainath College of Nursing, KatniFabin JoseNo ratings yet
- 2009 06 11-Publicconsultation DraftDocument37 pages2009 06 11-Publicconsultation Draftchris2272No ratings yet
- Gilead Sciences / Michael L Riordan / Nasdaq Article 2013Document1 pageGilead Sciences / Michael L Riordan / Nasdaq Article 2013chand100% (5)
- Memo Safety SealDocument9 pagesMemo Safety SealCONCEPCION VICTORIANo ratings yet
- Drug Study ProjectDocument7 pagesDrug Study ProjectMaRic Gabutin Guerra100% (1)
- Reference Values Lab Tests Cardiac Profile Tests 3 PgsDocument3 pagesReference Values Lab Tests Cardiac Profile Tests 3 PgsJim Varghese100% (1)
- Design Poster - Group 11 - A3Document1 pageDesign Poster - Group 11 - A3HahahahaNo ratings yet
- Hospital Pharmacy PresentationDocument154 pagesHospital Pharmacy PresentationKen OviedoNo ratings yet
- Aseptic Meningitis in Adults - UpToDateDocument16 pagesAseptic Meningitis in Adults - UpToDateKondász Antal Gábor MedNo ratings yet
- NCP FinalDocument5 pagesNCP FinalYoongiNo ratings yet
- WWW Interfarfacing ComDocument13 pagesWWW Interfarfacing ComspiraldaoNo ratings yet