Professional Documents
Culture Documents
Evaluation of Common Pancreatic Condition
Uploaded by
Naweed AshrafOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Evaluation of Common Pancreatic Condition
Uploaded by
Naweed AshrafCopyright:
Available Formats
Radiol Clin N Am 41 (2003) 97 114
MR cholangiopancreatography: evaluation of common pancreatic diseases
Laura M. Fayad, MDa,*, Thomas Kowalski, MDb, Donald G. Mitchell, MDa
a
Department of Radiology and Radiological Science, Johns Hopkins Medical Institutions, 601 North Wolfe Street, Baltimore, MD 21287, USA b Gastrointestinal Endoscopy, Division of Gastroenterology and Hepatology, 132 South 10th Street, 480 Main Building, Philadelphia, PA 19107, USA
In the initial evaluation of common pancreatic disorders, MR cholangiopancreatography (MRCP) has replaced the use of diagnostic endoscopic retrograde cholangiopancreatography (ERCP) at many institutions. MRCP is a heavily T2-weighted MR sequence that depicts the fluid-containing pancreatic duct in a noninvasive manner, avoiding potential complications associated with ERCP. MRCP is useful in the setting of pancreatitis for the identification of aberrant ductal anatomy and complications, and is valuable for detecting and characterizing cystic pancreatic masses. Furthermore, with the addition of conventional T1-weighted, T2-weighted, and gadolinium-enhanced sequences to MRCP, pancreatic adenocarcinoma can also be detected and staged. This article reviews MRCP with regard to the evaluation of common pancreatic diseases, with emphasis on its use for guiding treatment options.
Technique The normal pancreatic duct is a small structure, with a diameter of 3 mm or less, and is challenging to visualize completely by MR imaging. Because pancreatic ductal fluid has a long T2 relaxation time, a heavily T2-weighted sequence will result in high signal within the pancreatic duct, whereas background tissue, which has a shorter T2 relaxation
* Corresponding author. E-mail address: lfayad1@jhmi.edu (L.M. Fayad).
time, is suppressed. The ideal sequence will provide fast imaging, heavy T2 weighting for good duct-tobackground contrast and adequate spatial resolution for identification of subtle ductal pathology. A number of techniques have been employed to achieve heavy T2 weighting, including steady-state free precession gradient-recalled echo imaging [1 4], twodimensional fast spin echo (2D FSE) [5 12], three-dimensional fast spin echo (3D FSE) [13 15], single-shot fast spin echo (SSFSE) [16 24], and a recently described method combining 3D FSE with echo-planar imaging [25]. SSFSE has become the most widely used sequence, because it provides ultrafast, reliable, MRCP imaging. Unfortunately, the trade-off of fast sequences is a loss of spatial resolution. Although ERCP offers superior spatial resolution, the resolution of SSFSE is increased when a 512 matrix acquisition or a small field of view is employed. In our experience, a duct with a diameter less than 1 mm can be seen, using a field of view of 24 cm2 and a matrix size of 256 224 pixels. This level of resolution is acceptable for the evaluation of adults, but is insufficient for pediatric pancreaticobiliary imaging [26]. MRCP in the pediatric population requires a higher matrix or a smaller field of view. The SSFSE sequence can be implemented as a series of single thick-slab acquisitions [18,19] or as a thin multislice acquisition [18 21]. Single and multislice acquisition methods have been shown to provide complementary data for the evaluation of the pancreas [27,28], and are superior to older techniques of pancreatic evaluation [26].
0033-8389/03/$ see front matter D 2003, Elsevier Science (USA). All rights reserved. PII: S 0 0 3 3 - 8 3 8 9 ( 0 2 ) 0 0 0 6 6 - 0
98
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
Fig. 1. Thick-section MRCP. (A) Coronal, oblique, thick-section SSFSE image showing a normal pancreatic duct ( P) with a loop configuration (L). Also shown are the common bile duct (B), common hepatic duct (H ), and the cystic duct (C ). (B) Coronal, oblique, thick-section SSFSE image of the patient in Fig. 1, acquired at a different obliquity, showing unfolding of the pancreatic duct loop configuration (L).
The single-slice thick-slab acquisition method is attractive because a snapshot of the pancreaticobiliary system is obtained while respiratory and bowel motion is virtually eliminated, and no postprocessing of the images is required (Fig. 1). Typically, 30-mm to 50-mm thick slabs are prescribed in several oblique planes to depict the extrahepatic biliary and pancreatic ducts, each requiring less than a 2-second breath hold. Alternatively, images may be acquired at end expiration during relaxed natural breathing. Regardless, it is important to wait at least 10 seconds between acquisitions, to allow for recovery from the previous overlapping radial excitation. An imaging plane parallel to the pancreatic duct in the body and tail of the pancreas is employed and prescribed from an axial image (Fig. 2). Because fat is bright on SSFSE images, chemically selective fat saturation is utilized to increase duct-to-background contrast. A significant advantage of the single-slice method is its short acquisition time, which allows for the performance of a dynamic MRCP. Repeated sequential imaging of the same slab demonstrating the pancreatic duct and extrahepatic biliary tree, performed over several minutes, will resolve the possibility of sphincter of Oddi dysfunction. It may also demonstrate changes in the pancreatic duct following secretin administration [29 31]. The main drawback of the single-section acquisition is that ductal visibility may be degraded by overlap with other fluid-containing structures or ascites included in the field of view (Fig. 3). To overcome overlap by fluid in the stomach, ideally, patients should fast 4 hours before the examination or be given a T2-negative oral contrast agent such as high-
concentrate ferric ammonium citrate [32]. Negative oral contrast may interfere with identification of the duodenum and ampulla of Vater, however. Overlap also can be overcome by tailoring the orientation and positioning of the thick slab to the patients ductal anatomy. Alternatively, a multislice thin-section acquisition can be performed. A multislice acquisition is typically performed with 4-mm or 5-mm thick slices with a shorter echo time (TE) than is used for single-section thick-slab acquisition (see Fig. 2). With intermediate TE, (100 300 milliseconds), fluid is bright and periductal structures are well seen, a feature particularly useful when malignant obstruction is suspected or an overlap artifact is noted on single-section acquisition.
Fig. 2. Thin-section MRCP. Axial, thin-section SSFSE image showing a dilated pancreatic duct (arrow). A thicksection coronal oblique image may be prescribed parallel to the main pancreatic duct, as defined by the white rectangle.
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
99
Fig. 3. MRCP with overlap of fluid-containing structures. (A) Coronal, oblique, thick-section SSFSE image in a patient with autosomal-dominant polycystic kidney disease and multiple small liver cysts (small arrows) and renal cysts (R) depicted on the thick-section MRCP. These fluid-containing structures obscure view of the pancreatic duct ( P) in the pancreatic tail. (B) Axial, thin-section SSFSE image of the same patient shows delineation of the pancreatic duct ( P) in the pancreatic tail. Enlarged kidneys containing multiple cysts (R) are noted bilaterally.
Image quality is unaffected by motion because each slice is acquired in less than 1 second, but motion will cause slice-to-slice misregistration. Even thinner sections of the pancreaticobiliary tree (as thin as 2 mm), can be performed and used for reconstructing a 3D data set in any plane via maximum-intensity projection, although the quality of projection images is usually superior with a fast thick-slab acquisition. Secretin-enhanced dynamic MRCP (s-MRCP) is a technique for functional imaging and improved anatomic depiction of the pancreatic ductal system. Secretin stimulates the secretion of fluid and bicarbonate by the exocrine pancreas, with a consequent increase in the volume of fluids inside the pancreatic ducts [33]. In the first 5 minutes, secretin also causes the sphincter of Oddi to contract, resulting in temporary increased pancreatic ductal pressure in healthy subjects [34]. A thick-slab acquisition, showing the full length of the pancreatic duct, extrahepatic biliary tree, and duodenum in one projection, can be performed dynamically with good temporal resolution to evaluate flow of pancreatic fluid from the pancreatic ducts into the duodenum. Secretin improves visualization of the pancreatic duct and reduces the false-positive depiction of strictures [29,31,35,36]. Administration of secretin also provides an estimate of pancreatic exocrine function [31,37 39] and better evaluation of sphincter and ductal anatomy, including pancreas divisum. The main limitation to the performance of s-MRCP is the additional cost and limited availability of secretin.
Evaluation of pancreatic disease: MRCP or ERCP? Several studies have found MRCP comparable with ERCP for diagnosing extrahepatic biliary and pancreatic ductal abnormalities [2,9,15,20,29,40 43]. At many institutions, MRCP has replaced ERCP for some indications. MRCP is noninvasive, whereas ERCP-related morbidity and mortality is not trivial, with potential complications including pancreatitis (3.9%), hemorrhage (1%), perforation (1%), sepsis (0.5%), and even death in up to 0.5% of cases [44,45]. In addition, the risk of sedation-related complications looms. MRCP is also less expensive than is ERCP, uses no ionizing radiation, and is less dependent on the operators skill. No preparation is required for MRCP (other than brief fasting at some centers), and no exogenous contrast is needed. Furthermore, MRCP shows the ductal diameter more accurately than does ERCP, because contrast injection during ERCP may increase biliary duct caliber by as much as 6 mm [46,47], falsely giving the impression of ductal dilation. MRCP has a high success rate, whereas ERCP failure rates range between 3% and 10% [44,48]. Failure of ERCP may be due to limited operator skill. In the case of duodenal and gastric obstruction, periampullary diverticula, and in patients who have had an operative choledochoenteric or pancreaticoenteric anastomosis, however, ERCP may be technically impossible and fail in up to 20% of cases (Fig. 4)
100
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
lack of spatial resolution of conventional MRCP [30], but further technical developments are needed to adequately rival the spatial resolution of ERCP.
Pancreatic ductal anatomy and the significance of anatomic variants The normal pancreatic duct, less than 3 mm in caliber, is challenging to visualize completely by MRCP. The caliber of the duct increases slightly from the pancreatic tail to the head. The main duct receives 20 to 35 short tributaries that enter perpendicularly, but are not usually seen in the normal pancreas by MRCP. The pancreatic duct course varies greatly, but it most commonly descends. It can have a loop configuration, particularly at the point of fusion of the ducts of Santorini and Wirsung in the pancreatic neck (see Fig. 1) [28]. Patterns of drainage of the pancreas also vary. In 90% of cases, the pancreas drains primarily through the duct of Wirsung, which joins the bile duct at the major papilla [28]. An accessory duct of Santorini that drains through the minor papilla is present in 44% of individuals, and is not always visualized by MRCP, due to its limited spatial resolution. The normal main pancreatic duct, however, is visualized in more than 80% of patients, depending on the
Fig. 4. Duodenal diverticulum. Coronal, oblique, thicksection SSFSE image showing a duodenal diverticulum with an air-fluid level (long arrow) lateral to a normal common bile duct (B). The pancreatic duct ( P) also appears normal. A duodenal diverticulum is a common cause for ERCP failure.
[18,49]. With MRCP, a duct can be visualized beyond an obstructing lesion. Combined with traditional T1-weighted and T2-weighted sequences, MRCP also allows for complementary imaging of extraductal disease. Thus, in most patients, and especially in the 40% to 70% of patients who undergo ERCP who have normal studies [50,51], MRCP appears to be an excellent first choice in the workup of patients with pancreatic disease and should be considered the test of choice in all patients with failed or incomplete ERCP [49,52,53]. There are two main limitations of MRCP. First, unlike ERCP, MRCP offers no therapeutic options at the time of diagnosis. Such options include sphincterotomy, endoscopic lithotomy, brush cytology, collection of pancreatic juice, stricture dilation, stent placement, and biopsy. Proponents of MRCP, however, argue that MRCP provides guidance for these therapeutic alternatives. Second, the higher level of spatial resolution achievable by ERCP may be of critical importance in situations in which precise delineation of the pancreatic side branches is needed. Such situations include the recently advocated lessinvasive pancreatic surgeries, segmental pancreatic resection, and cyst enucleation, in which management of the pancreatic duct and its ductules is vital to prevent postoperative pancreatic leaks leading to fistula formation, abscess, and hemorrhage. Usually, more precise definition of the pancreatic side branches can be attained by ERCP than by MRCP [54]. The development of s-MRCP may offset the
Fig. 5. Choledochal cyst and anomalous pancreaticobiliary junction. Coronal, oblique, thick-section SSFSE image showing an anomalous union of the common bile duct with the pancreatic duct ( P) and a long common channel (long arrow), in a patient with a choledochal cyst (C ).
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
101
MRCP sequence used [28,55]. Fulcher and Turner [28] depicted the main pancreatic duct in the head and body in 97% of cases and in the tail in 83% of cases. Fortunately, an abnormally dilated duct can be seen in 100% of cases [40]. In 1.5% to 3% of individuals, there is an anomalous union of the pancreatic and bile ducts, which results in an unusually long common channel proximal to the duodenum. This channel is present in 33% to 83% of patients with choledochal cysts and is important to identify, because its presence may alter the operative approach undertaken at surgical resection (Fig. 5) [56,57]. Gallbladder carcinoma is also more frequent in patients with an anomalous union than in those without such a union. Elnemr et al [58] reported that 18.3% of patients with gallbladder cancer had an anomalous union. The most common anatomic abnormality of the pancreaspancreas divisumoccurs in 5% to 14% of the population [59,60], when the dorsal (Santorini) and ventral (Wirsung) pancreatic ducts fail to fuse (Fig. 6). When standard cannulation of the major papilla is performed on ERCP, only the ventral duct is opacified, resulting in incomplete ductography. The termination of the ventral duct can be mistaken for occlusion of the main duct, potentially mimicking pancreatic cancer. An astute endoscopist will recognize this pattern, but MRCP can easily demonstrate
the anomaly and is an accurate method for diagnosing pancreas divisum, because it shows a continuous dominant dorsal pancreatic duct. The accuracy of MRCP in the diagnosis of pancreas divisum has been demonstrated to be 100% [41]. In a patient with pancreas divisum, the minor papilla may provide a functional obstruction, resulting in elevated pancreatic duct pressure that may precipitate pancreatitis, because no communication with the major papilla exists for adequate decompression. Pancreas divisum is commonly detected incidentally in asymptomatic patients, but it occurs more frequently in patients who present with acute recurrent pancreatitis than in the general population [61 65]. There is no consensus regarding the appropriate endoscopic treatment for recurrent pancreatitis associated with pancreas divisum. Papillotomy of the minor papilla appears to yield improvement in most cases, and placement of a transpapillary pancreatic stent has been touted as a safe and effective endoscopic treatment [66]. A potential role of MRCP in the diagnosis of pancreas divisum is to identify a subset of patients with pancreas divisum and pancreatitis who may benefit from these invasive treatments. Such a subset includes patients with a true functional obstruction at the level of the minor papilla with or without a santorinicelea cystic dilation of the distal dorsal duct just proximal to the minor papilla. A santorinicele is believed to result from relative obstruction and weakness of the distal ductal wall and has been suggested as a possible cause of relative stenosis of the accessory papilla [67,68]. Manfredi et al [30] showed that a santorinicele is associated with a partial functional obstruction at the level of the minor papilla. Following secretin administration, the onset of duodenal filling was delayed significantly in patients with pancreas divisum and a santorinicele compared with patients with pancreas divisum alone. Furthermore, after sphincterotomy of the minor papilla, the size of the main pancreatic duct and of the santorinicele was significantly reduced, and patients had symptomatic improvement. In this study [30], conventional MRCP detected fewer cases of pancreas divisum with or without santorinicele compared with s-MRCP (50% and 57%, respectively).
The role of MRCP in pancreatitis
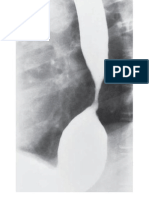
Fig. 6. Pancreas divisum. Coronal, oblique, thick-section SSFSE image showing pancreas divisum with the dorsal (D) and ventral (V ) ducts. Cannulation of the major papilla (long arrow) during ERCP results in opacification of the small ventral duct only.
What is the state of the pancreaticobiliary tree in patients with acute and chronic pancreatitis? This frequent indication for ERCP may now be answered by MRCP. Sica et al [69] showed sensitive detection
102
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
Fig. 7. Acute pancreatitis secondary to stones. (A) Coronal, oblique, thick-section SSFSE image showing gallstones (short arrows) and common bile duct stones (long arrows) in the setting of acute pancreatitis. (B) Axial, thin-section SSFSE image showing gallstones (short arrow) and common bile duct stones (long arrow). The pancreas ( P) is enlarged and heterogeneous in this patient with acute pancreatitis.
and accurate characterization of duct segments with MRCP that were comparable with ERCP. In the setting of a single episode of acute pancreatitis, MRCP is focused on the noninvasive detection or exclusion of choledocholithiasis, noting that only 30% to 52% of suspected calculi are present in patients referred for ERCP (Fig. 7) [50]. The high incidence of negative results using ERCP suggests that a noninvasive test such as MRCP should be used to screen these patients to avoid unnecessary morbidity and mortality. In the setting of recurrent acute pancreatitis, MRCP may be used to suggest its cause and to detect complications of pancreatitis. Possible causes of recurrent acute pancreatitis include choledocholithiasis, pancreatic cancer, or an anatomic abnormality such as pancreas divisum. Sphincter of Oddi dysfunction is also a cause of recurrent pancreatitis
that, in some instances, may be suggested by MRCP [70]. In patients with chronic pancreatitis, MRCP can be used to support a clinical diagnosis, especially in the early stages of chronic pancreatitis. Chronic pancreatitis is a chronic inflammatory process that results in pancreatic parenchymal atrophy and fibrosis. Alcoholism is the cause of at least 70% of cases. Approximately 10% of cases are attributed to chronic ductal obstruction, autoimmune disorders, inflammatory disease, and inherited diseases causing abnormal pancreatic enzymes or ductal secretion. Remaining cases are idiopathic. Alcoholic pancreatitis is usually heterogeneous and characterized by side-branch dilation and ductal calcifications (Fig. 8), whereas obstructive pancreatitis is more homogeneous, lacks calcifications, and is associated more often with main duct dilation. Nonalcoholic duct-
Fig. 8. Chronic pancreatitis. (A) Coronal, oblique, thick-section SSFSE image showing a markedly dilated pancreatic duct (large arrow) with markedly dilated side-branches (small arrows) in a patient with chronic alcoholic pancreatitis. (B) Axial, thinsection, fat-suppressed, 2D FSE image showing small hypointense filling defects in the pancreatic duct and its side branches, representing pancreatic duct stones (arrows) in a patient with chronic alcoholic calcific pancreatitis.
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
103
destructive pancreatitisor autoimmune pancreatitisis characterized by a narrow pancreatic duct and diffuse parenchymal abnormality, typically involving the pancreatic body and tail, without ductal calcifications [71,72]. Early alcoholic chronic pancreatitis manifests as irregularities and dilation of the ductal side branches. These side branches may be below the limits of resolution of MRCP, so ERCP is generally more sensitive to early side-branch changes. Side-branch ectasia is the most specific and prominent feature of alcoholic chronic pancreatitis. At a later stage, the main pancreatic duct is dilated with loss of the normal tapering of the duct in the tail. Areas of focal narrowing produce a characteristic beaded chain of lakes appearance. Even the biliary tract may become
dilated as a result of fibrosis in the head of the pancreas. MRCP has demonstrated the pancreatic duct, after stimulation with secretin, loses distensibility and has decreased exocrine function [31,37]. In addition, MRCP may be used in conjunction with other MR sequences, especially nonenhanced T1-weighted images, which show low pancreatic signal intensity in patients with chronic pancreatitis. MRCP is not only important for detecting chronic pancreatitis, but is also valuable for the identification of a surgically or endoscopically correctable lesion (Fig. 9). The location of strictures, degree of ductal dilation, presence of ductal filling defects, and associated complications such as pseudocysts all influence the therapy of patients with chronic pancreatitis. MRCP agrees with ERCP in 83% to 100% of ductal
Fig. 9. Chronic pancreatitis. (A) Coronal, oblique, thick-section SSFSE image showing changes of chronic pancreatitis, including a dilated pancreatic duct (large arrow) with filling defects representing mucus (small arrows), and two pseudocysts (C ). (B) Coronal, thin-section SSFSE image showing the findings in Fig. 9A in greater detail. (C) Coronal, thin-section SSFSE image acquired more anteriorly. C, pseudocysts. (D) Axial, nonenhanced, T1-weighted, gradient echo image showing decreased signal in the pancreas ( P) from fibrosis. The dilated pancreatic duct (arrow) and two pseudocysts (C ) are again noted.
104
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
Fig. 10. Focal obstructive pancreatitis due to adenocarcinoma of the pancreas. (A) Coronal, thick-section SSFSE image showing a dilated pancreatic duct (thick arrows) in the body and tail of the pancreas with termination (thin arrow) of the duct in the body. (B) Axial, T1-weighted, 3D, gradient echo image of the pancreas obtained in the arterial phase following the administration of intravenous gadolinium shows a hypoenhancing mass (arrow) that is responsible for obstruction of the pancreatic duct with resultant obstructive pancreatitis distally.
dilation cases, in 70% to 92% of ductal narrowing cases, and in 92% to 100% of filling defect cases [36,43]. On MRCP, filling defectsrepresenting mucus, calculi and debriscan be reliably identified with a diameter as small as 2 mm [40]. MRCP is, however, superior for detecting pseudocysts, which are missed approximately 50% of the time by ERCP [73], although ERCP can consistently determine the presence or site of communication of a pseudocyst with the main pancreatic duct. Therapeutic options for chronic pancreatitis include surgical decompression, partial pancreatectomy, total pancreatectomy, and endoscopic decompression, which relieve pain in 75% to 90% of patients. Ductal decompression is the main principle of therapy, because early decompression delays the onset of exocrine dysfunction, as well as endocrine dysfunction that occurs in 33% of patients with chronic pancreatitis [74]. Filling defects such as calculi, mucus, and debris may be removed endoscopically through a pancreatic duct sphincterotomy, and strictures can be dilated with short-term stent placement to improve pain [75]. Duct decompression by surgery depends, in part, on the size of the main pancreatic duct. For example, duct-destructive chronic pancreatitis, with a main duct diameter of less than 3 mm, requires a drainage procedure different from that required for a duct diameter over 7 mm [75,76]. Hence, when using MRCP it is important to fully describe the state of the pancreatic duct in the
setting of chronic pancreatitis to adequately guide treatment options.
Chronic pancreatitis or carcinoma? When findings of chronic pancreatitis are identified in a patient without a prior history of chronic pancreatitis or of ethanol abuse, an obstructing lesion should be suspected (Fig. 10). Pancreatic ductal adenocarcinoma is the usual cause of chronic obstructive pancreatitis and comprises 75% to 90% of all pancreatic carcinomas [77]. Differentiating adenocarcinoma from mass-forming chronic pancreatitis with MR imaging is sometimes difficult. Typically, the chronically inflamed pancreas will enhance more than will pancreatic tumors on immediate postgadolinium images, particularly those tumors arising in the head. Unfortunately, the degree of enhancement cannot be used to reliably distinguish these entities because abundant fibrosis is seen in both chronic pancreatitis and carcinoma, accounting for their similar appearances [78]. MRCP may be helpful to aid in this differentiation, because chronic alcoholic pancreatitis, compared with chronic obstructive pancreatitis due to adenocarcinoma, is more frequently associated with an irregularly dilated duct with intraductal calcification [79]. The ratio of duct caliber to pancreatic gland width is higher in patients with carcinoma [80]. Also,
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
105
Fig. 11. Pancreatic adenocarcinoma. (A) Coronal, thick-section SSFSE image showing the classic double-duct sign of pancreatic carcinoma; both the pancreatic duct ( P) and common bile duct (C ) are dilated and abruptly terminate (large arrow) in the head of the pancreas. In this case, the intrahepatic biliary ducts are also dilated. (B) Axial, nonenhanced, T1-weighted, gradient echo image showing an ill-defined hypointense mass (arrow) in the head of the pancreas. A biopsy of this mass revealed pancreatic adenocarcinoma.
the duct-penetrating sign, seen in 85% of chronic pancreatitis and in only 4% of patients with cancer, helps to distinguish an inflammatory pancreatic mass from pancreatic carcinoma. The duct-penetrating sign refers to a nonobstructed main pancreatic duct penetrating an inflammatory pancreatic mass, unlike its usual obstruction by pancreatic carcinoma. [81]. Furthermore, MRCP can depict the classic double duct sign of pancreatic carcinoma (enlargement and noncommunication of the pancreatic and common bile ducts) and the imaging counterpart of Courvoisiers sign (an enlarged, nontender gallbladder caused by an obstructing tumor) (Fig. 11) [82]. A normal-sized pancreatic duct is present in up to 20% of patients with adenocarcinoma, however, and should not dissuade its diagnosis in the setting of common bile duct dilation. These latter signs are useful when present, but MRCP (like ERCP) is thought to be a poor way to differentiate benign from malignant strictures. Because morphologic features of benign and malignant strictures overlap, ERCP may be the imaging modality of choice because of its ability to obtain a diagnostic sample with brush cytologic biopsy [75,83]; however, MRCP, including MR imaging pulse sequences, has a sensitivity of 84% for diagnosing pancreatic carcinoma, whereas the corresponding sensitivity for ERCP with brush cytology varies between 33% and 85% [42,83]. Adding MRCP to conventional T1-weighted and T2-weighted sequences improves specificity by depicting extra-
ductal structures not seen with ERCP [84]. Comprehensive MR imaging is also useful to accurately determine resectability [85].
Cystic pancreatic masses The incidence of detected cystic pancreatic masses is increasing because of the widespread use of cross-sectional imaging. Cystic pancreatic lesions include benign entities such as pseudocysts and epithelial pancreatic cysts, as well as malignant lesions. Epithelial cysts are usually associated with entities such as polycystic kidney disease and von Hippel-Lindau disease. Other cystic lesions are discussed below. Pancreatic pseudocysts occur as a complication of acute or chronic pancreatitis and represent 90% of cystic pancreatic masses [86]. They are encapsulated collections of pancreatic fluid, caused by pancreatic duct disruption and tissue dissolution in acute pancreatitis, and microperforation of the pancreatic duct in chronic pancreatitis. The surgical definition of a pseudocyst requires that it be present for at least 6 weeks. These lesions may communicate with the main pancreatic duct and may be identified on ERCP (Fig. 12). Less than 50% of pseudocysts are detected at ERCP [73], however, giving MR imaging a large advantage for their diagnosis. Pseudocysts are usually accompanied by a clinical history of pancreatitis and are associated with pancreatic parenchymal and ductal
106
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
Fig. 12. Communicating pseudocyst. Axial, thin-section SSFSE image showing an uncomplicated pseudocyst (C) with communication to the pancreatic duct (arrow) in a patient with pancreatitis.
changes that suggest pancreatitis, making their differentiation from pancreatic neoplasms possible in most cases. Pseudocysts resolve spontaneously in 60% of cases [87]. Treatment options for persistent pseudocysts include endoscopic, radiologic, and surgical drainage. These must be considered cautiously, in the event that a cystic neoplasm is misdiagnosed as a pseudocyst [88]. Misdiagnosis, usually by CT, has been reported as high as one third of the time [89 91]. The traditional approach for treating pseudocysts that require drainage has been surgical. Treatment is considered when the patient is symptomatic, if the pseudocyst
demonstrates enlargement or complications including hemorrhage, or if there is suspicion of a malignancy [88]. Enlargement and hemorrhage are two factors that can be determined with MR imaging (Fig. 13). Cystic neoplasms of the pancreas are uncommon, representing 10% of cystic lesions [86]. Classification of cystic neoplasms is based on the location of the lesion, the size of the cysts, the serous or mucinous nature of the contents, and the most dedifferentiated epithelial change recognizable at pathology [92,93]. Additionally, almost any pancreatic neoplasm can present as a cystic mass, including adenocarcinoma, which is the most common pancreatic neoplasm.
Fig. 13. Hemorrhage pseudocyst. (A) Axial, thin-section SSFSE image showing a large complex cystic collection with a fluid fluid level (arrow) representing a hemorrhagic pseudocyst in a patient with pancreatitis. The head of the pancreas ( P) is denoted. (B) Axial, T1-weighted, gradient echo image showing hyperintensity (arrows) at the posterior aspect of the pseudocyst, representing hemorrhage. The head of the pancreas (P) is again denoted.
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
107
Parenchymal cystic lesions include serous and mucinous cystic neoplasms. Intraductal neoplasms are referred to as intraductal papillary mucinous tumors (IPMTs). Cystic neoplasms can easily be detected on MRCP because of their high fluid content, but full examination requires T1-weighted, T2-weighted, and postgadolinium sequences. Serous microcystic adenomas are benign pancreatic parenchymal lesions with a relatively equal distribution throughout the pancreas. Although typically appearing solid on CT or US, a serous adenoma is cystic with more than six internal cysts, each measuring less than 2 cm in diameter. Approximately 40% of these tumors have calcifications and 15% have a central stellate scar (Fig. 14). Their soft tissue component is typically hypervascular and aspirated contents contain glycogen [94]. A small serous tumor adjacent to the main pancreatic duct or a branch duct may be difficult to distinguish from an intraductal neoplasm. Mucinous cystic neoplasms are also parenchymal lesions. In the past, this neoplasm was subcategorized
into macrocystic adenomas and adenocarcinomas, which are indistinguishable on the basis of imaging. In fact, all mucinous cystic neoplasms should be considered malignant or potentially malignant; thus, this subcategorization is not appropriate. Mucinous neoplasms, with strict histologic criteria, probably occur only in women and are usually located in the pancreatic body and tail. Most mucinous cystic neoplasms have fewer than six cysts, each greater than 2 cm in diameter. Twenty-five percent of these lesions have calcification, and the soft tissue component is hypovascular. Aspiration of these lesions yields mucin [92]. Because these lesions are frequently unilocular, they may be confused with pseudocysts. In such cases, changes of pancreatitis should be sought to confirm the possibility of a pseudocyst (Fig. 15). Intraductal tumors, previously described in the literature under different names such as ductectatic mucinous cystadenocarcinomas, predominate in men and older individuals. These tumors, now referred to as IPMTs, usually grow slowly, with a good prog-
Fig. 14. Serous tumor. (A) Coronal, thick-section SSFSE image showing a round, well-defined, cystic mass (large arrow) in the head of the pancreas with a conglomerate of small cysts measuring less than 2 cm each. The common bile duct (B), pancreatic duct ( P), and cystic duct (C) are denoted on this image. (B) Axial, thin-section SSFSE image showing the cystic mass (thick arrow) with a suggestion of a central scar (thin arrow), characteristic of a serous tumor.
108
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
Fig. 15. Mucinous tumor. (A) Coronal, thick-section SSFSE image depicting a cystic mass (thick arrow) in the tail of the pancreas, without associated dilation of the pancreatic duct (thin arrow). (B) Axial, thin-section SSFSE image showing the cystic mass (thick arrow) with internal complex signal. The pancreatic duct (thin arrows) is not dilated. Resection of this mass yielded a benign mucinous cystic tumor.
nosis. IPMTs arise from the epithelial lining of the pancreatic ductal system and include lesions representing the histologic progression of epithelial hyperplasia, dysplasia, adenoma, carcinoma-in-situ, and invasive carcinoma [95 98]. Hyperplasia, dysplasia, and adenoma may undergo malignant transformation over many years [98]. Multiple IPMTs can be present in an individualapproximately 23% of the timeas
described in a series by Megibow et al [99]. IPMT is associated with excessive mucin secretion, resulting in progressive ductal dilation or cyst formation (Fig. 16). IPMT may involve the main duct or branch ducts of the pancreas. Imaging patterns include segmental or diffuse involvement of the main pancreatic duct, and microcystic or macrocystic masslike lesions involving the branch ducts [95,97,98].
Fig. 16. IPMT. (A) Coronal, thick-section SSFSE image showing a cystic mass (large arrow) associated with a dilated pancreatic duct ( P) with dilated side branches. Incidental note is made of a cystic duct remnant (C ). (B) Coronal, thin-section SSFSE image showing the cystic mass (large arrow) in communication with a dilated draining pancreatic duct ( P), a finding that is highly suggestive of an intraductal papillary mucinous tumor.
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
109
When an IPMT involves the full length of the main pancreatic duct without a localized cystic mass, differentiation from chronic pancreatitis may be difficult [100,101]. A finding virtually pathognomonic of IPMTs is dilation of the major papilla, minor papilla, or both, with bulging into the duodenal lumen. This finding, which can be seen on MR imaging and is well appreciated by ERCP, is demonstrated with CT imaging approximately 25% of the time (Fig. 17) [97]. With segmental involvement of the main pancreatic duct, the adjacent pancreatic parenchyma is normal or thin. IPMTs such as this can be difficult
to differentiate from localized chronic obstructive pancreatitis. In such cases, hypointense filling defects representing mucin facilitate the diagnosis of IPMT. When the IPMT is located in the head, it may be difficult to differentiate between diffuse invasion of the main pancreatic duct and simple ductal dilation from mechanical obstruction. In difficult cases, ERCP is valuable to demonstrate intraluminal mucinous filling defects with jellylike mucin leaking from the papilla, another pathognomonic finding for IPMT. On occasion, mucin can be viscous enough to obstruct the pancreatic duct, preventing successful ERCP. Nevertheless, the endoscopist can confirm the pres-
Fig. 17. IPMT. (A) Coronal, thick-section SSFSE image showing an IPMT (thick arrow) with a dilated draining pancreatic duct ( P) and bulging papilla (thin arrow). The latter finding is pathognomonic of IPMTs. (B) Coronal, thick-section SSFSE image obtained in a different projection showing the dilated main pancreatic duct (thin arrows) in association with this IPMT (thick arrow). (C) Coronal, thin-section SSFSE image again demonstrating a cystic mass representing an IPMT (thick arrow) with a dilated draining pancreatic duct and bulging papilla (thin arrow). On thin-section MRCP images, a bulging papilla is seen as a filling defect in the duodenum. In this case, possible papillary projections are noted within the cystic mass.
110
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114
Fig. 18. Multiple IPMTs. Axial, thin-section SSFSE image showing multiple cystic lesions in the pancreas, representing multiple IPMTs (thick arrows). It is difficult to differentiate these cystic masses from pseudocysts and other pancreatic cystic lesions. The pancreas is atrophied, which is likely related to chronic obstruction by mucus. The pancreatic duct (thin arrow) is slightly prominent.
valuablemain pancreatic ductal dilation greater than 15 mm [109], as well as diffuse main pancreatic duct dilation with the branch-duct type of IPMT [95], is associated with malignancy. The features described above are influential in deciding whether an IPMT is benign or malignant, but at this time, imaging cannot reliably distinguish benign from malignant tumors [111 113]. Surgical management is usually recommended when these lesions are encountered [99,114,115]. A review of cystic pancreatic masses by Megibow et al [99], however, concluded that surveillance might be possible if lesions are smaller than 2.5 cm, spare the main pancreatic duct, and demonstrate no solid components. Because many of these patients are asymptomatic elderly individuals and growth may be slow or negligible over several years, surgical removal may not be the only appropriate management.
Summary In the evaluation of common pancreatic diseases, MRCP is a noninvasive alternative to ERCP. Ductal anatomy can be ascertained without risk of complications. MRCP is valuable in defining common anatomic variants, determining the state of the pancreatic duct in pancreatitis, and characterizing neoplasms, especially combined with other MR imaging sequences. With the advent of MRCP, techniques requiring endoscopy and percutaneous access are largely reserved for histologic diagnosis and treatment, or for cases in which MRCP fails to establish a diagnosis.
ence of an IPMT by observing copious drainage of mucin from the papilla [97,102]. Branch-duct IPMT is most frequently located in the uncinate process and can have a macrocystic or microcystic appearance [97,98]. Communication with the main pancreatic duct is a valuable finding that is often demonstrated best on ERCP [103] and s-MRCP. A branch-duct IPMT may be differentiated from a communicating pseudocyst if the IPMT contains papillary proliferations. If an IPMT manifests as a more cystic masslike lesion, it can resemble a mucinous cystic tumor or necrotic adenocarcinoma (Fig. 18). With the latter entities, however, the main pancreatic duct central to the tumor should not be dilated as it is in the presence of an IPMT. A number of researchers have concluded that MRCP is more sensitive and effective than is ERCP in evaluating IPMT [54,104 107]. MRCP, however, does not offer definitive pathologic information to decide whether a lesion is malignant, but features have been described that suggest malignancy. Generally, a less-favorable histology is noted with the main-duct type of IPMT [99,108,109]. The observation of thick walls and mural nodules aids the diagnosis of malignancy [104,108,110]; the detection of nodules in the cystic lesion is better accomplished with MRCP than with ERCP [104,105]. The size of the lesion is also important: in one series, Obara et al [111] found that 83% of tumors larger than 4 cm were malignant. The size of the main pancreatic duct is
References
[1] Wallner BK, Schumacher KA, Weidenmaier W, Friedrich JM. Dilated biliary tract: evaluation with MR cholangiography with a heavily T2-weighted contrast-enhanced fast-sequence. Radiology 1991;181: 805 8. [2] Morimoto K, Shimoi M, Shirakawa T, et al. Biliary obstruction: evaluation with three-dimensional MR cholangiography. Radiology 1992;183:578 80. [3] Ishizaki Y, Wakayama T, Okada Y, Kobayashi T. Magnetic resonance cholangiography for evaluation of obstructive jaundice. Am J Gastroenterol 1993;12: 2072 7. [4] Hall-Craggs M, Allen C, Owens C, et al. MR cholangiography: Clinical evaluation in 40 cases. Radiology 1993;189:423 7. [5] Meakem TJ, Holland GA, McDermott VG, et al. Fast spin-echo multicoil magnetic resonance cholangiog-
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114 raphy: initial experience [abstract]. In: Proceedings of the 12th Annual Scientific Meeting of the Society of Magnetic Resonance in Medicine. Berkeley, California: Society of Magnetic Resonance in Medicine; 1993. p. 41. Outwater EK. MR cholangiography with a fast spinecho sequence [abstract]. J Magn Reson Imaging 1993;3(P):131. Takehara Y, Ichijo K, Tooyama N, et al. Breath-hold MR cholangiopancreatography with a long-echo-train fast spin-echo sequence and a surface coil in chronic pancreatitis. Radiology 1994;192:74 8. Guibaud L, Bret PM, Reinhold C, Atri M, Brkum AN. Diagnosis of choledocholithiasis: value of MR cholangiography. Am J Roentgenol 1994;163:847 50. Guibaud L, Bret PM, Reinhold C, Atri M, Barkum AN. Bile duct obstruction and choledocholithiasis: diagnosis with MR cholangiography. Radiology 1995;197: 109 15. Macaulay SE, Schulte SJ, Sekijima JH, et al. Evaluation of a non-breath-hold MR cholangiographic technique. Radiology 1995;196:227 32. Becker CD, Grossholz M, Becker M, Mentha G, de Peyer R, Terrier F. Choledocholithiasis and bile duct stenosis: accuracy of MR cholangiopancreatography. Radiology 1997;205:523 30. Reinhold C, Taourel P, Bret PM, et al. Choledocholithiasis: evaluation of MR cholangiography for diagnosis. Radiology 1998;209:435 42. Barish MA, Yucel EK, Soto JA, Chuttani R, Ferrucci JT. MR cholangiopancreatography: efficacy of threedimensional turbo spin-echo technique. Am J Roentgenol 1995;165:295 300. Soto JA, Barish MA, Yucel EK, Siegenberg D, Ferrucci JT, Chuttani R. Magnetic resonance cholangiography: comparison to endoscopic retrograde cholangiopancreatography. Gastroenterology 1996; 110:589 97. Chan Y, Chan ACW, Lam WWM, et al. Choledocholithiasis: comparison of MR cholangiography and endoscopic retrograde cholangiography. Radiology 1996;200:85 9. Laubenberger J, Buchert M, Schneider B, Blum U, Hennig J, Langer M. Breath-hold projection magnetic resonance cholangiopancreatography (MRCP): a new method for the examination of the bile and pancreatic ducts. Magn Reson Med 1995;33:18 23. Kim TK, Han JK, Kim SJ, Bae SH, Choi BI. MR cholangiopancreatography: comparison between halfFourier acquisition single-shot turbo spin-echo and two-dimensional turbo spin-echo pulse sequences. Abdom Imaging 1998;23:398 403. Reuther G, Kiefer B, Tuchmann A. Cholangiography before biliary surgery: single-shot MR cholangiography versus intravenous cholangiography. Radiology 1996;198:561 6. Miyazaki T, Yamashita Y, Tsuchigame T, Yamamoto H, Urata J, Takahashi M. MR cholangiopancreatography using HASTE (half-fourier acquisition single-
111
[20]
[6]
[21]
[7]
[22]
[8]
[23]
[9]
[24]
[10]
[11]
[25]
[12]
[26]
[13]
[27]
[14]
[28]
[15]
[29]
[16]
[30]
[17]
[31]
[18]
[32]
[19]
[33] [34]
shot turbo spin-echo) sequences. Am J Roentgenol 1996;166:1297 303. Regan F, Fradin J, Khazan R, Bohlman M, Magnuson T. Choledocholithiasis: evaluation with MR cholangiography. Am J Roentgenol 1996;167:1441 5. Holzknecht N, Gauger J, Sacmann M, et al. Breathhold MR cholangiography with snapshot techniques: prospective comparison with endoscopic retrograde cholangiography. Radiology 1998;206:657 64. Irie H, Honda H, Tajima T, et al. Optimal MR cholangiopancreatographic sequence and its clinical application. Radiology 1998;206:379 87. Yamashita Y, Abe Y, Tang Y, Urata J, Sumi S, Takahashi M. In vitro and clinical studies of image acquisition in breath-hold MR cholangiopancreatography: single-shot projection technique versus multislice technique. Am J Roentgenol 1997;168(6): 1449 54. Soto JA, Barish MA, Alvarez O, Medina S. Detection of choledocholithiasis with MR cholangiography: comparison of three-dimensional fast spin-echo and single and multisection half-fourier rapid acquisition with relaxation enhancement sequence. Radiology 2000;215:737 45. Wielopolski PA, Gaa J, Wielopolski DR, Oudkerk M. Breath-hold MR cholangiopancreatography with three-dimensional, segmented, echo-planar imaging and volume rendering. Radiology 1999;210:247 52. Irie H, Honda H, Jimi M, et al. Value of MR cholangiopancreatography in evaluating choledochal cysts. Am J Roentgenol 1998;171:1381 5. Masui T, Takehara Y, Ichijo K, Naito M, Watahiki H, Kaneko M, et al. Evaluation of the pancreas: a comparison of single thick-slice MR cholangiopancreatography with multiple thin-slice volume reconstruction MR cholangiopancreatography. Am J Roentgenol 1999;173:1519 26. Fulcher AS, Turner MA. MR pancreatography: a useful tool for evaluating pancreatic disorders. Radiographics 1999;19:5 24. Matos C, Metens T, Deviere J, et al. Pancreatic duct: morphologic and functional evaluation with dynamic MR pancreatography after secretin stimulation. Radiology 1997;203:435 41. Manfredi R, Costamagna G, Brizi MG, et al. Pancreas divisum and santorinicele: diagnosis with dynamic MR cholangiopancreatography with secretin stimulation. Radiology 2000;217:403 8. Manfredi R, Costamagna G, Brizi M, et al. Severe chronic pancreatitis versus suspected pancreatic disease: dynamic MR cholangiopancreatography after secretin stimulation. Radiology 2000;214:849 55. Takahara T, Yoshikawa T, Saeki M, et al. High concentration ferric ammonium citrate (FAC) solution as a negative bowel contrast agent. Nippon Igaku Hoshasen Gakkai Zasshi 1995;55:425 6. Dreiling DA, Messer J. The secretin story. Am J Gastroenterol 1978;70:455 79. Geenen JE, Hogan WJ, Dodds WJ, et al. Intraluminal
112
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114 pressure recording from the human sphincter of Oddi. Gastroenterology 1980;78:317 24. Takehara Y. Can MRCP replace ERCP? J Magn Reson Imaging 1998;8:517 34. Nicaise N, Pellet O, Metens T, et al. Magnetic resonance cholangiopancreatography: interest of IV secretin administration in the evaluation of pancreatic ducts. Eur Radiol 1998;8:16 22. Cappeliez O, Delhaye M, Deviere J, et al. Chronic pancreatitis: evaluation of pancreatic exocrine function with MR pancreatography after secretin stimulation. Radiology 2000;215:358 64. Heverhagen JT, Muller D, Battmann A, et al. MR hydrometry to assess exocrine function of the pancreas: initial results of noninvasive quantification of secretion. Radiology 2001;218(1):61 7. Sho M, Nakajima Y, Kanehiro H, et al. A new evaluation of pancreatic function after pancreaticoduodenectomy using secretin magnetic resonance cholangiopancreatography. Am J Surg 1998;176(3): 279 82. Fulcher AS, Turner MA, Capps GW, Zfass AM, Baker KM. Half-fourier RARE MR cholangiopancreatography: experience in 300 subjects. Radiology 1998;207:21 32. Bret PM, Reinhold C, Taourel P, Guibaud L, Atri M, Barkun AN. Pancreas divisum: evaluation with MR cholangiopancreatography. Radiology 1996; 199:99 103. Adamek HE, Albert J, Breer H, et al. Pancreatic cancer detection with magnetic resonance cholangiopancreatography and endoscopic retrograde cholangiopancreatography: a prospective controlled study. Lancet 2000;356:190 3. Soto JA, Barish MA, Yucel EK, et al. Pancreatic duct: MR cholangiopancreatography with a three-dimensional fast spin-echo technique. Radiology 1995; 196:459 64. Bilbao MK, Dotter CT, Lee TG, et al. Complications of endoscopic retrograde cholangiopancreatography (ERCP). A study of 10,000 cases. Gastroenterology 1976;70:314 20. Halme L, Doepel M, von Numers H, et al. Complications of diagnostic and therapeutic ERCP. Ann Chir Gynaecol 1999;88:127 31. Cooperberg PL, Li D, Wong P, Cohen MM, Burhenne HJ. Accuracy of common hepatic duct size in the evaluation of extrahepatic biliary obstruction. Radiology 1980;135:141 4. Chang VH, Cunningham JJ, Fromkes JJ. Sonographic measurement of the extrahepatic bile duct before and after retrograde cholangiography. Am J Roentgenol 1985;144:753 5. Silvis S, Ansel JH. Endoscopic retrograde cholangiography: application in biliary tract disease. In: Berk JE, editor. Bockus gastroenterology. 4th edition, vol. 6. Philadelphia: WB Saunders; 1985. p. 3569 80. Adamek H, Weitz M, Breer H, Jakobs R, Schilling D, Riemann J. Value of magnetic-resonance cholangiopancreatography (MRCP) after unsuccessful endoscopic retrograde cholangiopancreatography (ERCP). Endoscopy 1997;29:741 4. Paul A, Millat B, Holthausen U, et al. Diagnosis and treatment of common bile duct stones (CBDS): results of a consensus development conference. Surg Endosc 1998;12:856 64. Liu TH, Consorti ET, Kawashima A. The efficacy of magnetic resonance cholangiography for the evaluation of patients with suspected choledocholithiasis before laparoscopic cholecystectomy. Am J Surg 1999;178:480 4. Varghese JC, Farrell MA, Courtney G, Osborne H, Murray FE, Lee MJ. Role of MR cholangiopancreatography in patients with failed or inadequate ERCP. Am J Roentgenol 1999;173:1527 33. Soto JA, Yucel EK, Barish MA, Chuttani R, Ferrucci JT. MR cholangiopancreatography after unsuccessful or incomplete ERCP. Radiology 1996;199:91 8. Yamaguchi K, Chijiiwa K, Shimizu S, et al. Comparison of endoscopic retrograde and magnetic resonance cholangiopancreatography in the surgical diagnosis of pancreatic disease. Am J Surg 1998; 175(3):203 8. Barish MA, Yucel EK, Ferrucci JT. Current concepts: magnetic resonance cholangiopancreatography. N Engl J Med 1999;341(4):258 64. Sugiyama M, Baba M, Atomi Y, Hanaoka H, Mizutani Y, Hachiya J. Diagnosis of anomalous pancreaticobiliary junction: value of magnetic resonance cholangiopancreatography. Surgery 1998;123(4): 391 7. Mirsa SP, Dwivedi M. Pancreaticobiliary ductal union. Gut 1990;31:1144 9. Elnemr A, Ohta T, Kayahara M, et al. Anomalous pancreaticobiliary ductal junction without bile duct dilatation in gallbladder cancer. Hepatogastroenterology 2001;48(38):382 6. Stern CD. A historical perspective on the discovery of the accessory duct of the pancreas, the ampulla of Vater and pancreas divisum. Gut 1986;27:203 12. Satterfield ST, McCarthy JH, Greenen JE, et al. Clinical experience in 82 patients with pancreas divisum: preliminary results of manometry and endoscopic therapy. Pancreas 1988;3:248 53. Bernard JP, Sahel J, Giovanni M, Sarles H. Pancreas divisum is a probable cause of acute pancreatitis: a report of 137 cases. Pancreas 1990;5:248 54. Cotton PB. Congenital anomaly of pancreas divisum as a cause of obstructive pain and pancreatitis. Gut 1980;21:105 14. Gregg JA. Pancreas divisum: its association with pancreatitis. Am J Surg 1977;134:539 43. Startitz M, Meyer zum Buschenfelde KH. Elevated pressure in the dorsal part of pancreas divisum: the cause of chronic pancreatitis. Pancreas 1988;3: 108 10. Warshaw AL, Simeone J, Schapiro RH, Hedberg SE, Mueller PE, Ferrucci JU. Objective evaluation of am-
[35] [36]
[50]
[51]
[37]
[38]
[52]
[39]
[53]
[54]
[40]
[55]
[41]
[56]
[42]
[57] [58]
[43]
[44]
[59]
[60]
[45]
[46]
[61]
[62]
[47]
[63] [64]
[48]
[49]
[65]
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114 pullary stenosis with ultrasonography and pancreatic stimulation. Am J Surg 1985;149:65 71. Ertan A. Long-term results after endoscopic pancreatic stent placement without pancreatic papillotomy in acute recurrent pancreatitis due to pancreas divisum. Gastrointest Endosc 2000;52(1):9 14. Siebert DG, Matulis SR. Santorinicele as a cause of chronic pancreatic pain. Am J Gastroenterol 1995; 90:121 3. Eisen G, Schutz S, Metzler D, Baillie J, Cotton PB. Santorinicele: new evidence for obstruction in pancreas divisum. Gastrointest Endosc 1994;40:73 6. Sica GT, Braver J, Cooney MJ, Miller FH, Chai JL, Adams DF. Comparison of endoscopic retrograde cholangiopancreatography with MR cholangiopancreatography in patients with pancreatitis. Radiology 1999;210:605 10. Pamos S, Rivera P, Canelles P, et al. Magnetic resonance cholangiopancreatography (MRCP) versus endoscopic retrograde cholangiopancreatography (ERCP): diagnostic usefulness. Gastroenterol Hepatol 1998;21(4):174 80. Sarles HG. Chronic calcifying pancreatitis-chronic alcoholic pancreatitis. Gastroenterology 1974;66: 604 16. Van Hoe L, Gryspeerdt S, Ectors N, et al. Nonalcoholic duct-destructive chronic pancreatitis: imaging findings. Am J Roentgenol 1998;170:643 7. Nealon WH, Townsend Jr CM, Thompson JC. Preoperative endoscopic retrograde cholangiopancreatography (ERCP) in patients with pancreatic pseudocyst associated with resolving acute and chronic pancreatitis. Ann Surg 1989;209:532 8. Cooperman AM. Surgery and chronic pancreatitis. Surg Clin North Am 2001;81(2):431 55. American Society for Gastrointestinal Endoscopy. ASGE guidelines for clinical application. The role of ERCP in diseases of the biliary tract and pancreas. Gastrointest Endosc 1999;50(6):915 20. Izbicki JR, Bloechle C, Knoefel WT, Rogiers X, Kuechler T. Surgical treatment of chronic pancreatitis and quality of life after operation. Surg Clin North Am 1999;79(4):913 44. Arslan A, Buanes T, Geitung JT. Pancreatic carcinoma: MR, MR angiography and dynamic helical CT in the evaluation of vascular invasion. Eur J Rad 2001;38(2):151 9. Johnson PT, Outwater EK. Pancreatic carcinoma versus chronic pancreatitis: dynamic MR imaging. Radiology 1999;212:213 8. Karawasa E, Goldberg HI, Moss AA, Federle MP, London SS. CT pancreatogram in carcinoma of the pancreas and chronic pancreatitis. Radiology 1983; 148:489 93. Elmas N, Yorulmaz I, Oran I, Oyar O, Ozutemiz O, Ozer H. A new criterion in differentiation of pancreatitis and pancreatic carcinoma: artery-to-vein ratio using the superior mesenteric vessels. Abdom Imaging 1996;21:331 3.
113
[66]
[67]
[68]
[69]
[70]
[71]
[72]
[73]
[74] [75]
[76]
[77]
[78]
[79]
[80]
[81] Ichikawa T, Sou H, Araki T, Arbab AS, Yoshikawa T, Ishigame K, et al. Duct-penetrating sign at MRCP: usefulness for differentiating inflammatory pancreatic mass from pancreatic carcinomas. Radiology 2001; 221:107 16. [82] Freeny PC, Bilbao MK, Katon RM. Blind evaluation of endoscopic retrograde cholangiopancreatography (ERCP) in the diagnosis of pancreatic carcinoma: the double duct and other signs. Radiology 1976; 119:271 4. [83] Macken E, Drijkoningen M, Van Aken E, Van Steenbergen W. Brush cytology of ductal strictures during ERCP. Acta Gastroenterol Belg 2000;63(3):254 9. [84] Kim MJ, Mitchell DG, Ito K, Outwater EK. Biliary dilatation: differentiation of benign from malignant causesvalue of adding conventional MR imaging to MR cholangiopancreatography. Radiology 2000; 214:173 81. [85] Sheridan MB, Ward J, Guthrie JA, Spencer JA, Craven CM, Wilson D, et al. Dynamic contrast-enhanced MR imaging and dual-phase helical CT in the preoperative assessment of suspected pancreatic cancer: a comparative study with receiver operating characteristic analysis. Am J Roentgenol 1999;173:483 90. [86] Gasslander T, Arnelo U, Albiin N, Permert J. Cystic tumors of the pancreas. Dig Dis 2001;19(1):57 62. [87] Yeo CJ, Bastidas JA, Lynch-Nyhan A, Fishman E, Zinner M, Cameron J. The natural history of pancreatic pseudocysts documented by computed tomography. Surg Gynecol Obstet 1990;170:411 7. [88] Pitchumoni CS, Agarwal N. Pancreatic pseudocysts. When and how should drainage be performed? Gastroenterol Clin North Am 1999;28(3):615 39. [89] Boggi U, Di Candio G, Campatelli A, Pietrabissa A, Mosca F. Nonoperative management of pancreatic pseudocysts. Problems in differential diagnosis. Int J Pancreatol 1999;25(2):123 33. [90] Lumsden A, Bradley 3rd EL. Pseudocyst or cystic neoplasm? Differential diagnosis and initial management of cystic pancreatic lesions. Hepatogastroenterology 1989;36(6):462 6. [91] Lee YT. Cystadenocarcinoma versus pseudocyst of the pancreas: a difficult differential diagnosis. Curr Surg 1989;46(3):202 6. [92] Zamboni G, Scarpa A, Bogina G, et al. Mucinous cystic tumors of the pancreas: clinicopathological features, prognosis and relationship to other mucinous cystic tumors. Am J Surg Pathol 1999;23:410 22. [93] Nagar E, Ueki T, Chijiiwa K, et al. Intraductal papillary mucinous neoplasms of the pancreas associated with so-called mucinous ductal ectasia. Histochemical and immunohistochemical analysis of 29 cases. Am J Surg Pathol 1995;19:576 89. [94] Compton CC. Serous cystic tumors of the pancreas. Semin Diagn Pathol 2000;17:43 55. [95] Irie H, Honda H, Aibe H, et al. MR cholangiopancreatographic differentiation of benign and malignant intraductal mucin-producing tumors of the pancreas. Am J Roentgenol 2000;174:1403 8.
114
L.M. Fayad et al / Radiol Clin N Am 41 (2003) 97114 [106] Onaya H, Itai Y, Niitsu M, Chiba T, Michishita N, Saida Y. Ductectatic mucinous cystic neoplasm of the pancreas: evaluation with MR cholangiopancreatography. Am J Roentgenol 1998;171:171 7. [107] Fukukura Y, Fujiyoshi F, Sasaki M, et al. HASTE MR cholangiopancreatography in the evaluation of intraductal papillary-mucinous tumors of the pancreas. J Comput Assist Tomogr 1999;23:301 5. [108] Yamaguchi K, Ogawa Y, Chiijiiwa K, et al. Mucinhypersecreting tumors of the pancreas: assessing the grade of malignancy preoperatively. Am J Surg 1996; 171:427 31. [109] Terris B, Ponsot P, Paye F, et al. Intraductal papillary mucinous tumors of the pancreas confined to secondary ducts show less aggressive pathologic features as compared with those involving the main pancreatic duct. Am J Surg Pathol 2000;24:1372 7. [110] Kobayashi G, Fujita N, Lee S, et al. Correlation between ultrasonographic findings and pathologic diagnosis of the mucin producing tumor of the pancreas. Nippon Shokakibyo Gakkai Zasshi 1990;87:235 42. [111] Obara T, Maguchi H, Saitoh Y, et al. Mucin-producing tumor of the pancreas: surgery or follow-up? Nippon Shokakibyo Gakkai Zasshi 1994;91:66 74. [112] Sugiyama M, Atomi Y. Intraductal papillary mucinous tumors of the pancreas: imaging studies and treatment strategies. Ann Surg 1998;228:658 91. [113] Procacci C, Biasiutti C, Carbognin G, et al. Characterization of cystic tumors of the pancreas: CT accuracy. J Comput Assist Tomogr 1999;23:906 12. [114] Horvath KD, Chabot JA. An aggressive resectional approach to cystic neoplasms of the pancreas. Am J Surg 1999;178:269 74. [115] Kanazumi N, Nakao A, Kaneko T, et al. Surgical treatment of intraductal papillary-mucinous tumors of the pancreas. Hepatogastroenterology 2001;48(4): 967 71.
[96] Yamaguchi K, Ogawa Y, Chijiiwa K, Tanaka M. Mucin-hypersecreting tumors of the pancreas. Am J Gastroenterol 1992;87:634 8. [97] Procacci C, Megibow A, Carbognin G, et al. Intraductal papillary mucinous tumor of the pancreas: a pictorial essay. Radiographics 1999;19:1447 63. [98] Procacci C, Graziani R, Bicego E, et al. Intraductal mucin-producing tumors of the pancreas: imaging findings. Radiology 1996;198:249 57. [99] Megibow AJ, Lombardo FP, Guarise A, et al. Cystic pancreatic masses: cross-sectional imaging observations and serial follow-up. Abdom Imaging 2001; 26:640 7. [100] Agostini S, Choux R, Payan MJ, Sastre B, Sahel J, Clement JP. Mucinous pancreatic duct ectasia in the body of the pancreas. Radiology 1989;170:815 6. [101] Azar C, Van De Stadt J, Rickaert F, et al. Intraductal papillary mucinous tumours of the pancreas: clinical and therapeutic issues in 32 patients. Gut 1996;39: 457 64. [102] Raijman I, Kortan P, Walden D, Kandel G, Marcon NE, Haber GB. Mucinous ductal ectasia: cholangiopancreatographic and endoscopic findings. Endoscopy 1994;26:303 7. [103] Obara T, Maguchi H, Saitoh Y, et al. Mucin-producing tumor of the pancreas: natural history and serial pancreatogram changes. Am J Gastroenterol 1993;88: 564 9. [104] Sugiyama M, Atomi Y, Hachiya J. Intraductal papillary tumors of the pancreas: evaluation with magnetic resonance cholangiopancreatography. Am J Gastroenterol 1998;93:156 9. [105] Koito K, Namieno T, Ichiimura T, et al. Mucin-producing pancreatic tumors: comparison of MR cholangiopancreatography with endoscopic retrograde cholangiopancreatography. Radiology 1998;208: 231 7.
You might also like
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- (FRCR) Barret - FRCR Part 2A Single Best Answer (SBA) Questions For The New Format PDFDocument453 pages(FRCR) Barret - FRCR Part 2A Single Best Answer (SBA) Questions For The New Format PDFNaweed Ashraf93% (14)
- (FRCR) Afaq - Succeeding in The New FRCR Part 2A Exam PDFDocument219 pages(FRCR) Afaq - Succeeding in The New FRCR Part 2A Exam PDFNaweed Ashraf100% (7)
- Oesophagus 7 Edition: TNM Definitions: AJCC UICCDocument72 pagesOesophagus 7 Edition: TNM Definitions: AJCC UICCNaweed AshrafNo ratings yet
- 6.5 Esophageal StricturesDocument36 pages6.5 Esophageal StricturesNaweed AshrafNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Acute & Chronic PancreatitisDocument26 pagesAcute & Chronic PancreatitisNour AhmededNo ratings yet
- Anatomy, Histology, Embryology, and DevelopmentalDocument41 pagesAnatomy, Histology, Embryology, and DevelopmentalNikhilesh YandamuriNo ratings yet
- EMBRYOLOGYDocument4 pagesEMBRYOLOGYbhagavan prasadNo ratings yet
- Annular Pancreas Divisumtreated With Whipple Procedure: A Case Reportand Update of Arare ConditionDocument5 pagesAnnular Pancreas Divisumtreated With Whipple Procedure: A Case Reportand Update of Arare ConditionIJAR JOURNALNo ratings yet