Professional Documents
Culture Documents
Vulval Ca
Uploaded by
Chethana Bhat0 ratings0% found this document useful (0 votes)
84 views54 pagesThis document provides classifications and descriptions of vulvar carcinoma and vulvar intraepithelial neoplasia (VIN). It discusses:
1) The ISSVD and ISGP classification of non-neoplastic and neoplastic vulvar disorders including VIN grades and Paget's disease.
2) Risk factors, presentation, and histopathology of VIN. Recurrence rates after various treatment methods are provided.
3) Characteristics, diagnosis and treatment of Paget's disease including wide local excision for adequate removal.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document provides classifications and descriptions of vulvar carcinoma and vulvar intraepithelial neoplasia (VIN). It discusses:
1) The ISSVD and ISGP classification of non-neoplastic and neoplastic vulvar disorders including VIN grades and Paget's disease.
2) Risk factors, presentation, and histopathology of VIN. Recurrence rates after various treatment methods are provided.
3) Characteristics, diagnosis and treatment of Paget's disease including wide local excision for adequate removal.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
84 views54 pagesVulval Ca
Uploaded by
Chethana BhatThis document provides classifications and descriptions of vulvar carcinoma and vulvar intraepithelial neoplasia (VIN). It discusses:
1) The ISSVD and ISGP classification of non-neoplastic and neoplastic vulvar disorders including VIN grades and Paget's disease.
2) Risk factors, presentation, and histopathology of VIN. Recurrence rates after various treatment methods are provided.
3) Characteristics, diagnosis and treatment of Paget's disease including wide local excision for adequate removal.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 54
VULVAR CARCINOMA
International Society for the Study of Vulvar Diseases (ISSVD) and
International
Society of Gynaecological Pathologists (ISGP) classification
A. NON-NEOPLASTIC EPITHELIAL DISORDERS OF VULVAR SKIN
AND MUCOSA
Lichen sclerosus (LS)
Squamous cell hyperplasia (formerly hyperplastic dystrophy)
Other dermatoses
B. VULVAR INTRAEPITHELIAL NEOPLASIA (VIN)
Squamous vulvar intraepithelial neoplasia
VIN 1 (mild dysplasia)
VIN 2 (moderate dysplasia)
VIN 3 (severe dysplasia or carcinoma in situ)
VIN 3 - carcinoma in situ differentiated type
Non-squamous vulvar intraepithelial neoplasia
Pagets disease
Melanoma in situ
VULVAR INTRAEPITHELIAL NEOPLASIA (VIN)
the prevalence of VIN 1-2 is 0.2% and that of VIN 3 is 0.4% in women over 35 years
Risk factors for this disease are early first intercourse, more partners, smoking,
immunosupression and HPV infection ,other sexually transmitted diseases.
Patients with VIN have a higher risk of intraepithelial neoplasia on other parts of
the lower genital organs
VIN 3 will progress to invasive cancer is much lower than that of CIN (3-17%)
50% of patients with VIN complain of pruritus, irritation or visible vulvar
lesions, which are, in half of the cases, larger than 2.5 cm
Lesions are solitary or, in 70% of the cases, multiple.
They are characteristically papular, raised above the level of surrounding skin,
often with sharp borders and a keratotic, roughened surface.
Lesions can be dry or wet
Discolouration is usual and lesions may be variegated with areas of brown,
red, blue and white colouring
VIN1-mild
dysplasia
VIN2-moderate
dysplasia
VIN3-severe
dysplasia
A large number of modalities have been advocated for treatment
of VIN:
1. conservative management
2. medical therapy(5-FU)
3. laser treatment,
4. wide local excision using a knife or laser,
5. skining vulvectomy and skin grafting,
6. Simple vulvectomy.
In general, patients treated with excisional techniques had significantly lower
recurrence rate compared to those who underwent ablative procedures
Clinically, two distinct forms of VIN can be seen.
1. develops in young women and is multifocal and multicentric(Bowenoid dysplasia)
2. appears in older women and is usually unicentric
PAGETS DISEASE
associated with vulvar adnexal carcinoma or other local tumours such as
carcinoma of the Bartholins gland or distant tumours like breast urologic or
gastrointestinal cancer
rarely associated with an underlying vulvar adenocarcinoma (4%) or invasive
Pagets disease (12%), but there is a high recurrence rate
Pruritus, soreness and a burning sensation
large, clear Paget cells or as that lack intercellular bridges and have pale,
vacuolated cytoplasm within the squamous epithelium
slowly spreading ulcerative eczematoid lesions of the vulvar skin.
Characteristic clinical findings are the so called weeping Pagets disease that
affect moist parts of the vulva.
Usually begins on the hair bearing regions.
Extends well beyond the gross lesion
The treatment is surgical wide local excision
Recurrencies are treated by further excision
Underlying dermis must be removed for adequate histological evaluation
COLPOSCOPY OF VULVA- VULVOSCOPY
Identifying the individual components of the lesions both for biopsy
and treatment purposes.
Image depends on the thickness of the epithelium and the vascularity
of the underlying stroma.
TECHNIQUE
1. Inspection-application of water soluble lubricant fields of
redness,hyperkeratinization,pigmentation,ulceration,atrophy
2. Application of acetic acid-5% for 2-3 min for better visualisation of
lesions of keratinised skin.
3. Collins test
Solution of 1% toluidine blue to mark vulvar lesions for 2 min.Rinse with
1% acetic acid .The stain will be washed from normal skin.
Fixes to surface cell nuclei when applied in vivo
All foci of nuclear activity will be stained blue
This may happen not only in neoplasia, but also in
ulcerations,lacerations,parakeratosis
BIOPSY
Mandatory in
Fast growing lesions
Ulcerations
Areas of bleeding
Suspicious area of any colour
Under local anesthesia
Specimen of atleast 5 mm thick
Keyes punch foreceps
VULVAR CARCINOMA
ETIOLOGY
Basaloid/ Warty
Multifocal
Younger age
HPV
VIN
Smoking
Keratinising/Differentiated/Simplex
Unifocal
Older
Lichen Slerosus
Squamous metaplasia
CIN, Alcohol, Immunosuppression, History of cervical Ca
Itch-scratch cycle atypical changes in the repaired epithelium
Introduction
Vulval cancer is uncommon and accounts for approximately 1-4% of all
gynecological cancer
incidence : 1.8 /100.000, It is predominantly seen in postmenopausal and
old women (mean age 65 years ) ,and only 2% were less than 30 years.
Primary Tumor
90% of lesions are of squamous in origin.
3-5% of lesions are melanoma.
2% of lesions is basal cell carcinoma.
Less than 1% is sarcoma.
Secondary Tumors
It is occasionly found in vulva
Most commonly the primary lesion is from the cervix
or the endometrium
SQUAMOUS CELL CARCINOMA
Are usually seen in the anterior part of the vulva.
2/3 of cases in the labia majora.
1/3 of cases in the clitoris ,labia minora,fourchette,
and perineum.
Spread
LYMPHATIC > 50%
Direct spread occurs in 25% to the urethra, vagina
and rectum
Hematogenous spread to bone or lung is rare
Superficial L.N:
1- Inguinal L.N: Medial I.L.N ,lying inferior to S.I.ring.
Lateral I.L.N ,below the inguinal ligament.
2-Femoral L.N: Medical F.L.N,lying medical to saph.vein
Lateral F.L.N, lying lateral to saph .vein
Deep L.N:
1. Deep inguinal L.N , lying in the inguinal channel
2. Deep femoral L.N (node of cloquet lying in the femoral channel)
3. External iliac L.N:
Medial groups ,lying medial to EIV
Lateral groups,lying lateral to EIA
Anterior groups ,lying between EIV and EIA
The lymph nodes are arranged in 5 groups:
External Iliac LN
Common Iliac LN
Para Aortic L.N
Thoracic Duct
Lt sided lesion will spread to the Lt groin Lymph nodes.
Rt sided lesion will spread to the Rt Groin Lymph nodes.
Bilateral nodes involvement is seen in 14% of cases-lesions of clitoris,ant labia
majora,perineum.
Contralateral node involvement without ipsilateral disease is seen in 5% of
cases.
Involvement of pelvic nodes in the absence of inguinal nodes metastases is
very rare.
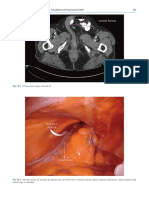
Superficial inguinal LN Deep femoral LN
Clinical Features
Irritation or pruritis in 70% of cases
Vulvar mass or ulcer in 55% of cases
Bleeding in 28% of cases
Discharge in 2-3% of cases
Lesion can take any form from flat white lesion to large ulcer
On Examination
Pre- treatment work up
A thorough pre- operative evaluation for coexisting medical
problems
Routine investigations and Chest radiograph
PAP smear and colposcopy of cervix and vagina.
Imaging : CT and MRI may help to determine resectability and
treatment planning, and distant metastases
Cystoscopy, intravenous pyelography, or proctoscopy (or all
three) is indicated if it appears that locally advanced cancer
SURGICAL MANAGEMENT
Standard treatment in the past : Radical vulvectomy and en
bloc groin dissection ( Taussig and Way)
Involves radical removal of the entire vulva, the mons pubis,
the inguino-femoral lymph nodes, and often the pelvic
lymph nodes.
ISSUES OF CONCERNS :
High rate and the severity of wound complications
Psychosexual effects of radical removal of the vulvar tissues
Urinary or fecal incontinence
Vaginal relaxation,
Overtreatment of early cancer,
Inadequate treatment of more advanced disease
Individualization of treatment for all patients with invasive disease
Vulvar conservation for patients with unifocal tumors and an otherwise normal vulva
Omission of the groin dissection for patients with T
1
tumors and, <1 mm of stromal
invasion .
Elimination of routine pelvic lymphadenectomy.
Investigation of role of sentinel lymph node procedure to eliminate requirement for
complete inguino-femoral lymphadenectomy.
The use of separate incisions for the groin dissection to improve wound healing
1. Status of the inguino-femoral lymph nodes- single most
important prognostic factor
NODAL
STATUS
5 YEAR
SURVIVAL
RATE
NEGATIVE >80%
POSITIVE <50%
No. of NODES Prognosis
Single
microscopically
+ve
Similar as
negative nodes
3 or more +ve
nodes
2year survival of
20%
Extra-capsular extension
Clinical nodal status
Size of the metastatic deposit inside the lymph node,
Percentage of nodal replacement.
The overall 5 years survival rate for vulval cancer is 70% for all operable
cases,This depends on:
3. Stage:
The 5 years survival rate decreases with advancing stage
from >90% in stage 1 to < 10% in stage 4
4. Differentiation:
A well diff.tumor has a better prognosis than poor diff.
5. Depth of Invasion:
A-invasion of 1 mm no risk of nodal metastases.
B-invasion of 1-3 mm 6-8% incidence of metastases.
C-invasion of 5 mm 22-37% incidence of metastases.
6. Surgical Margin:
Surgical excision margin of more than 1 cm in all diameters results in a
low local recurrence rate.
Modifications in Management of the Vulvar
Phase of Treatment
Modified radical vulvectomy - generally refers to radical
removal of the portion of the vulva containing the tumor
obtain 2cm skin margins while sparing of as much normal
vulvar tissue as possible is less likely to produce sexual
dysfunction and a sense of disfigurement
possibility of an increased risk of local recurrence and later an
increased risk of a second primary vulvar cancer
The evolution of surgical techniques in vulvar cancer. (A) Radical vulvectomy with en bloc dissection;
(B) radical vulvectomy with triple incision; (C) modified radical vulvectomy;
(D) clitoral-sparing modified radical vulvectomy
STAGE I Vulvar cancer
Radical vulvectomy (5-year survival rates ) >90%.
Choice of treatment depends on various tumor and patient factors.
At least 1cm grossly negative margin, without putting the skin under tension, should be
obtained and extended to the level of inferior fascia of the urogenital diaphragm .
Micro-invasive lesions (<1 mm
invasion)
Wide (510 mm) local excision
Lesions >2cm with <5mm invasion
and clinically negative nodes
Radical local excision with
complete unilateral
lymphadenectomy
STAGE II Vulvar cancer
Standard therapy : Modified radical vulvectomy with bilateral
inguinal and femoral lymphadenectomy
(Target : tumor free margins of at least 1 cm)
Adjuvant local radiation therapy may be indicated for surgical
margins less than 8 mm, and particularly if the patient also has
positive nodes
STAGE III Vulvar cancer
Modified radical vulvectomy with inguinal and
femoral node dissection.
Radical vulvectomy with inguinal and femoral
node dissection
followed by radiation therapy
STAGE IV Vulvar cancer
Radical vulvectomy and pelvic exenteration (if resectable).
Management of vulvar cancer with peri-urethral
involvement
Needs removal of outer urethra
Foleys catheter for one week postoperatively facilitate healing and
splinting of the urethra
If >1 cm of urethra removed or any preoperative stress urinary
incontinence consider surgical anti-incontinence procedure.
Management of vulvar cancer with perianal
involvement
Difficult to obtain adequate surgical margin on resection
Difficult to decide b/w radical excision and colostomy or
preoperative radiotherapy
Measures to minimize incontinence : ( rarely needed )
Sphincter approximation and levator muscle plication
Bowel preparation, prophylactic antibiotics ,post-operative bowel management
Use of cutaneous rhomboid flaps in reconstruction of perineum and perianal
areas
MANAGEMENT OF REGIONAL LYMPH NODES
Appropriate groin dissection single most important factor in
decreasing mortality in early vulvar cancer
Virtually no risk of lymph node metastasis if stromal invasion < 1
mm therefore one can omit groin dissection if invasion < 1mm ,no
lympho-vascular space invasion and no clinically suspicious groin
lymph node
Depending on laterality of vulvar lesion- ipsilateral or bilateral
lymphadenectomy becomes necessary
Recurrence in undissected groin > 90% mortality
All patient whose tumors demonstrate more than
>1mm of stromal invasion
Or whose tumors are >2cm (T1b and above )
Require inguinal- femoral lymphadenectomy
If Groin dissection is indicated in patients with vulvar cancer, it
should be a thorough inguinal- femoral Lymphadenectomy.
UNILATERAL GROIN DISSECTION:
if the primary lesion is unilateral and
ipsilateral nodes are negative.
Recommended that patients with any bulky or multiple
microscopically positive ipsilateral lymph nodes should undergo
contralateral inguinal femoral lymphadenectomy.
Bilateral inguinal-femoral lymphadenectomy be performed for
Midline lesions
Those with in 2 cm from midline
If Pre-operative pelvic imaging reveals bulky
pelvic lymph nodes
Resection via extra-peritoneal approach prior to
radiation( limited ability of external beam
radiation therapy to sterilize bulky positive pelvic
nodes)
Primary management in Carcinoma
of The Vulva
Management Features of Carcinoma
Radical local excision only
(Excision with 2 cm margins,
down to super,aponeurosis of
The original diaph +/-pubic
Periosteum)
1)-< =2cm lesion size
-< =1mm depth invasion
-No lymph-vascular space
involvement.
-Well or mod.diff.
Radical local excision and inguino
femoral node dissection.
unilateral if lesion unilat not
Involving midline,bilat.if lesion
Midline
2)>2 cm lesion size
-Or > 1 mm depth invasion
-Or lymph-vascular space
Involvement
-Or poorly diff
-Anterior radical vulvectomy
(including removal of clitoris but
-preserving post.vulva).
-bilat inquinal femoral N dissection
3)-Involves clitoral
Primary management in Carcinoma
of The Vulva
Features of Carcinoma Management
4)-Post. Vulva /perineum -posterior radical vulvectomy
(preserving clitoris and anterior vulva).
-bilat inquinal-femoral N dissection
5)-Locally advanced -pelvic exenteration(ant,post,total as
indicated by structures involved)
-anovalvetomy (for lesion
Involving anus /and vulva).
-Chemo-radiation followed by limited surgery
6)-Bone involvement
Fixed groin nodes
-chemo-radiation followed by limited
` surgery if locally resectable
SENTINEL LYMPHNODE MAPPING
First draining lymph-node in the lymphatic basin that recieves primary
lymph flow from the tumor.
Use of comprehensive serial sectioning, Immunohistochemistry (IHC), and
reverse transcription-polymerase chain reaction have been investigated as
potential methods to detect the earliest signs of metastatic disease.
PROCEDURE
1-2ml of isosulfan blue dye or 400mCi of technetium labeled
sulfur colloid injected circumferentially intradermally around the
tumor, and lymphoscintigraphy was performed.
The sites of the SLNs marked on the skin with a pencil.
SLNs identified using a handheld probe and the dissection of blue-
stained lymph vessels and lymph nodes.
Intra operative gamma counter to identify for identification of the nodes
and lymphatics.
The removed SLNs sent to the pathologist separately.
Ultrastaging consisted of performing serial sectioning and IHC analysis
with cytokeratins.
Studies in vulvar cancer in which SLN detection was
followed by a completion inguino-femoral lymphadenectomy
suggest that the SLN procedure is highly accurate in
identifying lymph node metastases with an NPV approaching
100%
Sentinel lymph node biopsy is a reasonable alternative to
inguinal femoral lymphadenectomy in
selected women with squamous cell carcinoma of the vulva.
Reconstruction of surgical defects
Gluteus maximus myocutaneous flaps
Rectus abdominis myocutaneous flap
Tensor fascia lata myocutaneous graft for extensive
defect in groin and vulva.
Rhomboid flap best suited for posterior vulva.
Mons pubis pedicle flap for lateral defects.
Unilateral or bilateral Gracilis myocutaneous grafts - when
extensive resection done from mons to perianal region.
Post-operative Management
Prophylactic antibiotics for 24 hrs
Ambulation delayed - If wounds are closed under tension
Meticulous perineal hygiene
Measures to keep the area dry and clean
Continue suction drainage of groin till output is minimal to avoid
groin seromas
Heparin thrombo-prophylaxis until ambulatory
Pneumatic calf compressions
A compression dressing (rolled gauze and an abdominal binder) is
maintained on the groins for an additional 24 to 48 hours to prevent
lymphocyst formation
Foleys catheter till patient ambulatory
Bowel rest - depending on the degree of perineal or perianal resection
SUMMARY
Vulvar cancer is surgically staged.
Imaging such as CT of the abdomen and pelvis should be
performed for women with tumors 2 cm or larger or to detect
lymph node or other metastases.
Staging should include evaluation of factors related to
prognosis: tumor size, depth of invasion, lymph node
involvement, and presence of distant metastases.
Inguino-femoral lymph node metastasis is the most important
predictor of overall prognosis.
Inguino-femoral lymphadenectomy or sentinel lymph node
evaluation can be omitted for lesions 2 cm or smaller and
depth of invasion less than 1 mm.
Sentinel node biopsy seems to be a reliable means to
pathologically assess inguino-femoral lymph node metastasis
All tumors larger than 2 cm require pathologic inguino-
femoral lymph node evaluation.
Radical local excision or modified radical vulvectomy is
appropriate for most stage I and II lesions located on the lateral
or posterior aspects of the vulva.
A tumor-free surgical margin of at least 1 cm decreases the risk
of local recurrence.
Chemo-radiation therapy is the preferred approach for most
patients with very advanced vulvar cancer
You might also like
- 1 Benign and Malignant Lesions of The CervixDocument46 pages1 Benign and Malignant Lesions of The CervixRohitNo ratings yet
- Carcinoma Vulva - FinalDocument70 pagesCarcinoma Vulva - FinalAastha Jain100% (1)
- Hernia Examination OSCE GuideDocument7 pagesHernia Examination OSCE GuideEssa AfridiNo ratings yet
- Vasculitis ReviewDocument132 pagesVasculitis Reviewajmal_rashid@hotmail.com100% (2)
- Carcinoid Tumor: Marcelyn Coley Surgery IV Conference Mount Sinai School of MedicineDocument52 pagesCarcinoid Tumor: Marcelyn Coley Surgery IV Conference Mount Sinai School of Medicinedrqazi777No ratings yet
- Abdominal Mass Differential PresentationDocument42 pagesAbdominal Mass Differential Presentationdeb haartNo ratings yet
- Malignant Tumors of Uterus: DR Tahira RizwanDocument52 pagesMalignant Tumors of Uterus: DR Tahira RizwanSadia YousafNo ratings yet
- Surgery CaseDocument43 pagesSurgery CaseAvni GuptaNo ratings yet
- Prenatal Assessments by TrimesterDocument6 pagesPrenatal Assessments by TrimesterMauZungNo ratings yet
- Gynecological Ultrasound Basic2Document145 pagesGynecological Ultrasound Basic2Mahmoud Saeed100% (2)
- Fetal Growth RestrictionDocument74 pagesFetal Growth RestrictionKalpavriksha1974No ratings yet
- Gynecology and ObstetricsDocument190 pagesGynecology and Obstetricsbhesh_seanNo ratings yet
- Differential Diagnosis Fever With RashDocument15 pagesDifferential Diagnosis Fever With RashJeetat OngNo ratings yet
- Gestational Trophoblastic Disease Pt2Document75 pagesGestational Trophoblastic Disease Pt2Abdullah KesalNo ratings yet
- Biliary DisordersDocument61 pagesBiliary DisordersMichael Angelo SeñaNo ratings yet
- Herpes Zoster OphthalmicusDocument29 pagesHerpes Zoster Ophthalmicuspurvi333No ratings yet
- Herpes Zoster (Shingles) : Muhammad Abdullah Dept. of Dermatology DHQ Hospital FaisalabadDocument26 pagesHerpes Zoster (Shingles) : Muhammad Abdullah Dept. of Dermatology DHQ Hospital FaisalabadwaleedNo ratings yet
- Ambulatory Hysteroscopy Evidence-Based Guide To Diagnosis and TherapyDocument23 pagesAmbulatory Hysteroscopy Evidence-Based Guide To Diagnosis and TherapyAngela EstevesNo ratings yet
- Pap Smear Guidelines: Baylor College of Medicine Anoop Agrawal, M.DDocument22 pagesPap Smear Guidelines: Baylor College of Medicine Anoop Agrawal, M.Dshygirl72No ratings yet
- Urological EmergencyDocument83 pagesUrological EmergencyAlfred LiNo ratings yet
- Vulvovaginal InfectionDocument66 pagesVulvovaginal InfectionRadhika BambhaniaNo ratings yet
- Gynecology Notes Legal Issues and EthicsDocument19 pagesGynecology Notes Legal Issues and EthicsUsm LeeNo ratings yet
- Menstrual Disorders: Olufemi Aworinde Lecturer/ Consultant Obstetrician and Gynaecologist, Bowen University, IwoDocument36 pagesMenstrual Disorders: Olufemi Aworinde Lecturer/ Consultant Obstetrician and Gynaecologist, Bowen University, IwoAkinbani MoyosoreNo ratings yet
- IEC-Atlas of Endoscopic UltrasoundDocument12 pagesIEC-Atlas of Endoscopic UltrasoundDannyNo ratings yet
- Glottic Cancer BMJDocument54 pagesGlottic Cancer BMJManling JaoNo ratings yet
- Classification and Diagnosis of Endometrial HyperplasiaDocument7 pagesClassification and Diagnosis of Endometrial HyperplasiaaksinuNo ratings yet
- Post Partum Haemorrhage 1 - LoadDocument47 pagesPost Partum Haemorrhage 1 - Loadkalpananstl100% (1)
- Phyllodes TumorDocument20 pagesPhyllodes TumorManuela KarinaaNo ratings yet
- Wound HealingDocument47 pagesWound HealingdenekeNo ratings yet
- 5 - Differential Diagnosis of DermatologyDocument6 pages5 - Differential Diagnosis of DermatologyAyaa YousefNo ratings yet
- Etat + PDFDocument56 pagesEtat + PDFShandy BNo ratings yet
- Bullous PemphigoidDocument21 pagesBullous PemphigoidChe Ainil ZainodinNo ratings yet
- National Board of Examinations Dated: 19 April 2018: Question Paper For NEET-SSDocument6 pagesNational Board of Examinations Dated: 19 April 2018: Question Paper For NEET-SSrajvolgaNo ratings yet
- Internal Medicine - Nephrology: Topic: Cystic Kidney Diseases Lecturer: Dra. Myrna NgoDocument3 pagesInternal Medicine - Nephrology: Topic: Cystic Kidney Diseases Lecturer: Dra. Myrna NgoVon HippoNo ratings yet
- Diagnostic Work Up of Ovarian CystsDocument12 pagesDiagnostic Work Up of Ovarian CystsAnshul KumarNo ratings yet
- د.عبد الزهره THE GYNAECOLOGICAL EXAMINATION-1 (Muhadharaty)Document29 pagesد.عبد الزهره THE GYNAECOLOGICAL EXAMINATION-1 (Muhadharaty)MohammedNo ratings yet
- Early Pregnancy Complications: Ectopic Pregnancy Gestational Trophoblastic Disease Ji Aggasid, JanniecelDocument60 pagesEarly Pregnancy Complications: Ectopic Pregnancy Gestational Trophoblastic Disease Ji Aggasid, JanniecelmedicoNo ratings yet
- Ovarian Tumours: DR ManjiriDocument41 pagesOvarian Tumours: DR ManjiriChama TlauNo ratings yet
- Precocius PubertyDocument4 pagesPrecocius PubertyJoanne LimNo ratings yet
- Philippine CPG On The Diagnosis and Management of Urinary Tract Infections in Adults-2015 Update - Part 2 PDFDocument140 pagesPhilippine CPG On The Diagnosis and Management of Urinary Tract Infections in Adults-2015 Update - Part 2 PDFspringdingNo ratings yet
- Venous UlcerDocument26 pagesVenous UlcerRajarshi KumarNo ratings yet
- Uterus NeoDocument11 pagesUterus NeoHester Marie SimpiaNo ratings yet
- 8 4 13notesDocument437 pages8 4 13notesJesse GriffithNo ratings yet
- 0301omar Yusef Kudsi - Robotic Hernia Surgery - A Comprehensive Illustrated Guide-Springer International Publishing - Springer (2020)Document25 pages0301omar Yusef Kudsi - Robotic Hernia Surgery - A Comprehensive Illustrated Guide-Springer International Publishing - Springer (2020)ravikanth100% (1)
- SAGES 2018 World Congress Advance ProgramDocument88 pagesSAGES 2018 World Congress Advance Programyos_peace86No ratings yet
- Pelvic Examination: W - Newton LongDocument3 pagesPelvic Examination: W - Newton LongyuexinchongNo ratings yet
- Hematuria in ChildrenDocument26 pagesHematuria in ChildrenNovenZefanya100% (1)
- Rbs Ogtt Final PresentDocument40 pagesRbs Ogtt Final PresentFrances GrefalNo ratings yet
- Obs History Taking FormatDocument24 pagesObs History Taking FormatBibek PandeyNo ratings yet
- DR - Mohammed Abdalla Egypt. Domiat G. Hospital: Controversies in GynecologyDocument66 pagesDR - Mohammed Abdalla Egypt. Domiat G. Hospital: Controversies in Gynecologymadmax500No ratings yet
- 2014 - Lecture - Pathology of The Small and Large IntestineDocument12 pages2014 - Lecture - Pathology of The Small and Large IntestinesammysandsongNo ratings yet
- Biomarkers in Abnormal Uterine Bleeding: Precision Medicine in Assisted Reproductive Technologies Special IssueDocument12 pagesBiomarkers in Abnormal Uterine Bleeding: Precision Medicine in Assisted Reproductive Technologies Special IssueWahyuning PutriNo ratings yet
- Dokumen - Pub Bedside Techniques Methods of Clinical Examination Fifth 2019nbsped 9789696375258Document234 pagesDokumen - Pub Bedside Techniques Methods of Clinical Examination Fifth 2019nbsped 9789696375258doyoumatterindeedNo ratings yet
- Factors Affecting Utilization of Intermittent Preventive Treatment of Malaria Among Pregnant Mothers Attending Antenatal in Kabuyanda Health Centre IV-Isingiro DistrictDocument5 pagesFactors Affecting Utilization of Intermittent Preventive Treatment of Malaria Among Pregnant Mothers Attending Antenatal in Kabuyanda Health Centre IV-Isingiro DistrictAnonymous izrFWiQNo ratings yet
- HerniaDocument5 pagesHerniasarguss14100% (5)
- Efflorescence of The Skin Lesions: Dr. M. Izazi HP, SP - KKDocument40 pagesEfflorescence of The Skin Lesions: Dr. M. Izazi HP, SP - KKSaputra Tri NopiantoNo ratings yet
- WP GynaeExams4Document37 pagesWP GynaeExams4Ahsan JamNo ratings yet
- Nrtis: (Nucleoside/ Nucleotide Reverse Transcriptase) : "Eatz LSD"Document3 pagesNrtis: (Nucleoside/ Nucleotide Reverse Transcriptase) : "Eatz LSD"Mohammad KatatoNo ratings yet
- Introduction To FracturesDocument40 pagesIntroduction To FracturesAnisah Pangandag MapandiNo ratings yet
- Local Anesthetics AgentsDocument56 pagesLocal Anesthetics AgentsIyad Abou-Rabii100% (1)
- What Is Alcohol2012AAlisherMDPhDDocument58 pagesWhat Is Alcohol2012AAlisherMDPhDAlisher AgzamovNo ratings yet
- NMC Hospital Abu Dhabi - 2011!06!08Document16 pagesNMC Hospital Abu Dhabi - 2011!06!08Manjul TakleNo ratings yet
- Excessive Gingival Display Etiology Diagnosis and Treatment Modalities NIR SILBERBERGDocument10 pagesExcessive Gingival Display Etiology Diagnosis and Treatment Modalities NIR SILBERBERGValentina100% (3)
- Notice: Draft, Revised Compliance Policy Guide Sec. 575.100 Pesticide Chemical Residues in Food-Enforcement Criteria (CPG 7141.01) AvailabilityDocument2 pagesNotice: Draft, Revised Compliance Policy Guide Sec. 575.100 Pesticide Chemical Residues in Food-Enforcement Criteria (CPG 7141.01) AvailabilityJustia.comNo ratings yet
- Brukner and Khans Clinical Sports Medicine Injuries, Volume 1 - MedicineDocument7 pagesBrukner and Khans Clinical Sports Medicine Injuries, Volume 1 - Medicinezaferyha17% (6)
- 802.036 Datasheet Phyaction E v1.5 en LRDocument4 pages802.036 Datasheet Phyaction E v1.5 en LRSofie BeckersNo ratings yet
- Coxa PlanaDocument9 pagesCoxa PlanaRegine BlanzaNo ratings yet
- The Art of Threads A Comprehensive ReviewDocument17 pagesThe Art of Threads A Comprehensive Reviewalejandro Gonzàlez80% (5)
- Natural Hygiene MagazineDocument33 pagesNatural Hygiene MagazineColm Rooney100% (1)
- Health ChemoDocument9 pagesHealth ChemoKanjarla Hanmonthrao Panthulu LaxmanaNo ratings yet
- WWW - England.nhs - Uk: Business Continuity Management NHS WorkshopDocument52 pagesWWW - England.nhs - Uk: Business Continuity Management NHS WorkshopForbetNo ratings yet
- Case:: Biddy's Bakery (BB)Document3 pagesCase:: Biddy's Bakery (BB)tehreem chohanNo ratings yet
- Performance Evaluation HeadnursingDocument3 pagesPerformance Evaluation HeadnursingBing58No ratings yet
- Memorize BiologyDocument79 pagesMemorize BiologyprthrNo ratings yet
- Sample - RSO Manual Hospital CathlabDocument39 pagesSample - RSO Manual Hospital CathlabPaul Ivan JulianNo ratings yet
- Tamil Nadu Registration of Practitioners of Integrated Medicine Act, 1956Document11 pagesTamil Nadu Registration of Practitioners of Integrated Medicine Act, 1956Latest Laws Team0% (1)
- Occupational Health and Safety ChecklistDocument6 pagesOccupational Health and Safety ChecklistpaurushgodharNo ratings yet
- 5 PDFDocument8 pages5 PDFoskar ORTIZNo ratings yet
- By Dinesh GannerllaDocument74 pagesBy Dinesh GannerllagannerllaNo ratings yet
- Pubmed - Australia - Clinical - brokenAffLastHistoDocument131 pagesPubmed - Australia - Clinical - brokenAffLastHistoHNNo ratings yet
- Umid Final Booklet - (Selva)Document64 pagesUmid Final Booklet - (Selva)Jitendra Singh0% (1)
- DR Axe 5 Essential Oils Proven Bymedical Science PDFDocument7 pagesDR Axe 5 Essential Oils Proven Bymedical Science PDFDubravka Duda100% (1)
- Acute Neurotherapeutics and Neuromonitoring FellowshipDocument7 pagesAcute Neurotherapeutics and Neuromonitoring FellowshippuspoNo ratings yet
- JHA-H011 Scrubbing and Mopping FloorsDocument2 pagesJHA-H011 Scrubbing and Mopping Floorstjeng syuwenNo ratings yet
- DISABILITYDocument9 pagesDISABILITYSyeda AttqaNo ratings yet
- Metacarpal FractureDocument45 pagesMetacarpal FractureJinnasit TeeNo ratings yet
- Psychopharma 1Document7 pagesPsychopharma 1Mitchee Zialcita100% (1)
- Bulacan State University College of Nursing: Bulsu-Op-Con-23F15 Revision: 0Document6 pagesBulacan State University College of Nursing: Bulsu-Op-Con-23F15 Revision: 0Richmon SantosNo ratings yet