Professional Documents
Culture Documents
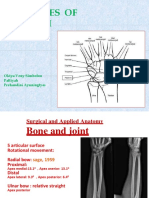
Scapula Fracture Treatment & Management: Author: Thomas P Goss, MD Chief Editor: S Ashfaq Hasan, MD
Uploaded by
johanes0 ratings0% found this document useful (0 votes)
20 views24 pagesScapula Fracture
Original Title
JRM-Ort
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentScapula Fracture
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
20 views24 pagesScapula Fracture Treatment & Management: Author: Thomas P Goss, MD Chief Editor: S Ashfaq Hasan, MD
Uploaded by
johanesScapula Fracture
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 24
Scapula Fracture
Treatment &
Management
Author: Thomas P Goss, MD; Chief Editor: S Ashfaq
Hasan, MD
TREATMENT
Approach Considerations
Most scapula fractures can be managed
effectively with closed treatment.
Because scapula fractures often are associated
with other, sometimes life-threatening injuries,
delay surgery until the patient is medically
stabilized.
Absolute contraindications for surgery are few. In
the case of a major vascular injury, such as an
axillary or brachial artery tear, repair the vessel
first, then follow with fracture fixation.
Recognizing the exact indications for operative
treatment of scapula fractures is a major issue for
the future.
Medical Therapy
Medical therapy for patients with scapula fractures generally
is the same as that for any trauma patient. Perform fluid
resuscitation, stabilize the cardiopulmonary system, and treat
life-threatening injuries prior to operative fixation of scapula
fractures.
Most scapula fractures can be managed with closed
treatment. More than 90% of scapula fractures have minimal
displacement.
Treatment is symptomatic. Short-term immobilization in a
sling and swathe bandage is provided for comfort.
In some cases, such as intra-articular fractures, close
radiographic follow-up is necessary to ensure that
unacceptable displacement does not occur.
Most scapular fractures heal completely by 6 weeks,
and all external support is discontinued at this time.
Continue ROM exercises until full shoulder mobility is
recovered.
Full functional recovery takes several months.
Ultimately, the prognosis for these fractures is
excellent.
Indications for Surgical Management
The
following Significantly displaced
injuries fractures of the glenoid cavity
(glenoid rim and fossa)
occur with Significantly displaced
enough fractures of the glenoid neck
frequency Double disruptions of the
to merit superior shoulder suspensory
complex (SSSC) in which one
discussion or more elements of the
of scapula are significantly
displaced
operative
treatment:
Significantly displaced fractures of
glenoid cavity (rim and fossa)
Fewer than 10% of glenoid cavity
fractures are significantly
displaced.
Ideberg reviewed over 300 such
injuries and proposed the first
detailed classification scheme.
This classification subsequently
was expanded by Goss
Other indications for surgical management
of these fractures include the following:
Glenoid fossa fractures that result in
significant displacement of the humeral
head such that it fails to lie in the center of
the glenoid cavity, thereby resulting in
glenohumeral instability
Fractures of the glenoid fossa with such
severe separation of the fracture
fragments that nonunion is likely to occur
Nordqvist and Petersson evaluated 37
glenoid neck fractures treated
nonoperatively and found the functional
results at 10- to 20-year follow-up to be
fair or poor in 32% of cases.
Hardegger et al noted that displaced
glenoid neck fractures result in a functional
imbalance because the relationship of the
glenohumeral joint with the acromion and
nearby muscle origins is altered
Herscovici et al reported results in nine patients with
ipsilateral clavicular and glenoid neck fractures.
Seven patients were treated surgically with plate
fixation of the clavicular fracture and achieved
excellent results. Two patients were treated without
surgery and were found to have decreased ROM, as
well as drooping of the involved shoulder.
Combined fractures of the distal clavicle and the
superior aspect of the glenoid cavity is another
potentially unstable situation. Each disruption may
lead to displacement at the other fracture site.
If displacement of the clavicular fracture site is
unacceptable, surgical reduction and stabilization is
indicated, usually with a Kirschner-wire (K-wire)
tension-band fixation construct.
Surgical Therapy
Fractures of glenoid cavity
The approach to glenoid cavity fractures
depends on the type of fracture
Basic orthopedic and shoulder instruments
should be available, and fixation devices
should include 3.5-mm and 4.0-mm cannulated
screws and 3.5-mm malleable reconstruction
plates. Kwires can be used for temporary or
definitive fixation of glenoid fragments
Type II glenoid neck fractures
Temporary fixation can be obtained with K-
wires or interfragmentary screws.
Definitive fixation of the reduced fragment
generally is achieved with a 3.5-mm
reconstruction plate contoured along the
posterior aspect of the glenoid fragment and
the lateral scapular border.
In some type II fractures, severe comminution
of the scapular body or spine may preclude
plate fixation.
In these cases, K-wire or interfragmentary
screw fixation can be used.
Coracoid and acromion fractures
For coracoid fractures that require ORIF, an
anterior deltoid-splitting approach is utilized.
The rotator interval is opened as needed for
optimal exposure of the fracture site. Cannulated
3.5- mm and 4.0-mm compression screws are
useful for fixation of large fragments.
If the fragment is significantly comminuted,
treatment is excision and suture fixation of the
conjoined tendon to the remaining coracoid
process
A deltopectoral approach could also be utilized as
an alternative to a deltoid-splitting approach.
If surgical reduction and stabilization of an
acromion fracture is necessary, a tension-band
and plate construct usually is chosen
Postoperative Care
Postoperative management partially depends on
the degree of stability achieved at surgery.
Complete immobilization in a sling and swathe is
used for the first 24-48 hours. After that,
progressive ROM exercises and functional use of
the shoulder out of the sling (within clearly defined
limits) are initiated if fixation is satisfactory.
If surgical fixation was not rigid, immobilization in
a sling and swathe, abduction brace, or overhead
olecranon pin traction may be required for 7-14
days.
Radiographs are taken every 2 weeks to
ensure maintained reduction.
By 6 weeks, healing usually is sufficient to
permit discontinuance of the sling and to
allow progressive functional use of the
extremity.
Physical therapy is continued until ROM
and strength are maximized.
Heavy physical use of the shoulder, such
as athletic activity, is prohibited for 4-6
months.
Patients are encouraged to work diligently
on their rehabilitation programs, as final
motion and strength may not be achieved
for 6 months to 1 year.
Complications
Complications can result directly from surgical
management.
Neurovascular injury, infection (superficial and
deep), and loss of fixation all can result from poor
surgical technique.
An improper physical therapy rehabilitation program
may lead to unnecessary postoperative
shoulder stiffness.
Finally, poor patient compliance can contribute to
shoulder stiffness and possible hardware failure.
Long-Term Monitoring
After discharge from the hospital, patients should be
seen for follow-up every 2 weeks for the first 6 weeks.
Radiographs are taken to ensure maintained reduction.
Evaluate the patient's ROM and update his/her
rehabilitation program as needed.
Patients should be seen at 12 weeks for evaluation of
motion and progression of functional use of the shoulder.
Final motion and strength may not be achieved until 6
months to 1 year.
Thank
You might also like
- Reduction, Relocation and Splinting in Emergency Room (RASER)From EverandReduction, Relocation and Splinting in Emergency Room (RASER)No ratings yet
- Tibia ProximalDocument51 pagesTibia Proximalchenth3r3No ratings yet
- Humeral Shaft FractureDocument82 pagesHumeral Shaft FractureYoga AninditaNo ratings yet
- AO Trauma Vol.2Document100 pagesAO Trauma Vol.2Cujba GheorgheNo ratings yet
- Distal Phalanx (45%) - Metacarpal (30%) - Proximal Phalanx (15%) - Middle Phalanx (10%)Document40 pagesDistal Phalanx (45%) - Metacarpal (30%) - Proximal Phalanx (15%) - Middle Phalanx (10%)Dabessa MosissaNo ratings yet
- 6-Fractures and Joints Dislocations ManagementDocument91 pages6-Fractures and Joints Dislocations ManagementMUGISHA GratienNo ratings yet
- Arthroplasty of Shoulder - MKKPPTXDocument54 pagesArthroplasty of Shoulder - MKKPPTXMis StromNo ratings yet
- U04 Fxs of Humeral ShaftDocument88 pagesU04 Fxs of Humeral Shaftadrian_mogosNo ratings yet
- Fractures of The Humeral ShaftDocument25 pagesFractures of The Humeral ShaftMuhammad IqbalNo ratings yet
- Femoral Supracondylar Fractures: Prepared by Dr. Ramzy Sh. ShikhanDocument77 pagesFemoral Supracondylar Fractures: Prepared by Dr. Ramzy Sh. ShikhanRamzi ShukriNo ratings yet
- Forearm Fracture 1 BismillahDocument17 pagesForearm Fracture 1 Bismillahamel015No ratings yet
- Clavicle Fractures Treatment & ManagementDocument11 pagesClavicle Fractures Treatment & ManagementshtefanazNo ratings yet
- Limb Salvage Surgery in Bone MalignanciesDocument56 pagesLimb Salvage Surgery in Bone MalignanciesKyaw SwaNo ratings yet
- ORP - Handout - English - Malleolar FracturesDocument15 pagesORP - Handout - English - Malleolar Fracturesadrian1989No ratings yet
- Closed Reduction and Percutaneous Kirschner Wire Fixation of Displaced Colles Fracture in AdultsDocument7 pagesClosed Reduction and Percutaneous Kirschner Wire Fixation of Displaced Colles Fracture in AdultsnaluphmickeyNo ratings yet
- Ender Nailing in HumerusDocument56 pagesEnder Nailing in HumerusRakesh KumarNo ratings yet
- Fractures and Dislocations About The Elbow in The Pediatric PatientDocument65 pagesFractures and Dislocations About The Elbow in The Pediatric PatientPeter HubkaNo ratings yet
- Upload Scribd 4Document7 pagesUpload Scribd 4Yoga AninditaNo ratings yet
- Scapula FracturesDocument24 pagesScapula FracturesFrancesco BenazzoNo ratings yet
- 3-2 Metacarpal Shaft FracturesDocument30 pages3-2 Metacarpal Shaft FracturesProfesseur Christian DumontierNo ratings yet
- Distal Radial Injury: Department of Orthopaedics SGH Didactic LectureDocument52 pagesDistal Radial Injury: Department of Orthopaedics SGH Didactic Lecturedrscribd1No ratings yet
- Paper Presentation Supracutaneous Locking Compression PlateDocument21 pagesPaper Presentation Supracutaneous Locking Compression PlateSourabh AlawaNo ratings yet
- Malleolar Fractures - Handout PDFDocument14 pagesMalleolar Fractures - Handout PDFAlin Bratu100% (2)
- 2 Clavo PDFDocument8 pages2 Clavo PDFYosip Becerra MondragonNo ratings yet
- Reverse Obliquity Intertrochanteric FracturesDocument8 pagesReverse Obliquity Intertrochanteric FracturesIndra Purwanto AkbarNo ratings yet
- Rotator Cuff Repairs: Mary Schuler MurphyDocument14 pagesRotator Cuff Repairs: Mary Schuler Murphyalexander panduNo ratings yet
- Fractures of Forearm: Oktya Veny Simbolon Pattiyah Prehandini AyuningtyasDocument90 pagesFractures of Forearm: Oktya Veny Simbolon Pattiyah Prehandini AyuningtyaspattiyahNo ratings yet
- Fracture Tibia & Fibula-1Document111 pagesFracture Tibia & Fibula-1Usaid SulaimanNo ratings yet
- Articular Fractures PrinciplesDocument9 pagesArticular Fractures PrinciplesSylviany El NovitaNo ratings yet
- Articular Fractures PrinciplesDocument9 pagesArticular Fractures PrinciplesSylviany El NovitaNo ratings yet
- Fracture Shaft Humerus - 030014Document60 pagesFracture Shaft Humerus - 030014MohammedShahidNo ratings yet
- Brief Resume of Intended WorkDocument7 pagesBrief Resume of Intended WorkNavin ChandarNo ratings yet
- AO Distal Humerus EA #Document26 pagesAO Distal Humerus EA #Purushotham NalamatiNo ratings yet
- Distal Tibia Paper 2Document6 pagesDistal Tibia Paper 2Rajib DebnathNo ratings yet
- Closed Manipulation and Casting of Distal Radius FracturesDocument10 pagesClosed Manipulation and Casting of Distal Radius FracturesDody KurniawanNo ratings yet
- Clavicle Fracture, SC Joint and Ac Joint Injury: Team IiiDocument19 pagesClavicle Fracture, SC Joint and Ac Joint Injury: Team IiiJunarto Putra TandiarrangNo ratings yet
- Fracture Arm: Siti Istiqomah, S. Ked 71 2016 080Document30 pagesFracture Arm: Siti Istiqomah, S. Ked 71 2016 080IstiD'JelenestaNo ratings yet
- 224 Closed Manipulation Casting of Distal Radius Fractures Fernandez DL 2005 Hand Clin p307-316 PDFDocument10 pages224 Closed Manipulation Casting of Distal Radius Fractures Fernandez DL 2005 Hand Clin p307-316 PDFanindyadputriNo ratings yet
- Case ReportDocument57 pagesCase ReportlmandahaNo ratings yet
- Utility and Outcomes of Locking Compression Plates in Distal Femoral FracturesDocument7 pagesUtility and Outcomes of Locking Compression Plates in Distal Femoral FractureskhusnulNo ratings yet
- 6-2-66-522 DR JayDocument5 pages6-2-66-522 DR JayDr Jay paneriNo ratings yet
- Dislocation of The Hip (July 2020)Document27 pagesDislocation of The Hip (July 2020)thehexhealthNo ratings yet
- Conservative Treatment of Diaphyseal Fractures of Tibia andDocument40 pagesConservative Treatment of Diaphyseal Fractures of Tibia andsaihaNo ratings yet
- Shoulder SurgeryDocument6 pagesShoulder SurgeryNathiya NilavNo ratings yet
- Scaphoid FractureDocument77 pagesScaphoid FractureTanuGarg100% (1)
- Clinical and Radiological Outcome in Lateral End Clavicle Fractures Following Clavicle Locking Plate FixationDocument6 pagesClinical and Radiological Outcome in Lateral End Clavicle Fractures Following Clavicle Locking Plate FixationIJAR JOURNALNo ratings yet
- Case Study of "Subtrochanteric Femur": Prepared By: John Ress A. Escobal Group 1Document11 pagesCase Study of "Subtrochanteric Femur": Prepared By: John Ress A. Escobal Group 1J.r. MercadoNo ratings yet
- Modified Judet Approach and Minifragment Fixation of Scapular Body and Glenoid Neck FracturesDocument7 pagesModified Judet Approach and Minifragment Fixation of Scapular Body and Glenoid Neck FracturesmotohumeresNo ratings yet
- BackgroundDocument5 pagesBackgroundMaricar K. BrionesNo ratings yet
- Pelvic Injruies 1Document43 pagesPelvic Injruies 1King salehNo ratings yet
- The Proximal Humerus Fracture Book: Frank Norberg, MDDocument10 pagesThe Proximal Humerus Fracture Book: Frank Norberg, MDDesyana KasimNo ratings yet
- Management of Mandibular FracturesDocument27 pagesManagement of Mandibular FracturesAyesha IjazNo ratings yet
- Smiths FractureDocument4 pagesSmiths FractureDyah AyuNo ratings yet
- AOT Orthogeriatrics DistalRadialFracturesDocument13 pagesAOT Orthogeriatrics DistalRadialFracturesNikhil junejaNo ratings yet
- Surgery of EOM ArdyDocument29 pagesSurgery of EOM ArdyArdyNo ratings yet
- Hand OITE - 2012 2013 2014Document209 pagesHand OITE - 2012 2013 2014Sadiq AliNo ratings yet
- Analysis of Surgical Management of Proximal Humeral FracturesDocument5 pagesAnalysis of Surgical Management of Proximal Humeral FracturesRhizka djitmauNo ratings yet
- Coronoid FractureDocument38 pagesCoronoid FractureRamin MaharjanNo ratings yet
- HandDocument29 pagesHandHelmi IsmunandarNo ratings yet
- Natural History of AISDocument42 pagesNatural History of AISJosh JoshiNo ratings yet
- Typhoid PerforationDocument3 pagesTyphoid PerforationSaryia JavedNo ratings yet
- Tiss 28Document12 pagesTiss 28Ubaid RahamanNo ratings yet
- Case Study 1Document4 pagesCase Study 1api-271668042No ratings yet
- Newcastle Disease The Vaccines & Vaccination: by Haas Md. Yatim D.V.M (UPM)Document36 pagesNewcastle Disease The Vaccines & Vaccination: by Haas Md. Yatim D.V.M (UPM)zainodin adhomNo ratings yet
- Mobility and ImmobilityDocument37 pagesMobility and ImmobilityAndrea Huecas Tria100% (2)
- What Is Korean Hand TherapyDocument32 pagesWhat Is Korean Hand Therapytvmedicine100% (3)
- Angels ResumeDocument4 pagesAngels Resumeapi-274792391No ratings yet
- Physician CertificationDocument1 pagePhysician CertificationcwadotorgNo ratings yet
- Jurnal MeiristaDocument8 pagesJurnal Meiristameirista deviNo ratings yet
- NHIC PT & OT Billing and CodingDocument83 pagesNHIC PT & OT Billing and Codingsbtappouni0% (1)
- Vascular TraumaDocument16 pagesVascular TraumaAndi Suchy Qumala SarieNo ratings yet
- Maxillofacial - Infection - Dari KikiDrDocument20 pagesMaxillofacial - Infection - Dari KikiDrmashitadyahNo ratings yet
- Haematology Physical ExaminationDocument8 pagesHaematology Physical Examinationrodahlyu100% (1)
- New York Cancer & Blood Specialists and AdvantageCare Physicians Collaborate in Staten IslandDocument3 pagesNew York Cancer & Blood Specialists and AdvantageCare Physicians Collaborate in Staten IslandPR.comNo ratings yet
- Drug StudyDocument4 pagesDrug Studysilverblade36No ratings yet
- Tips For Staying Hydrated During SummerDocument3 pagesTips For Staying Hydrated During SummervasuNo ratings yet
- Effectiveness of Structured Teaching Program On Self-Medication Knowledge and Its Adverse Effects Among Middle Age Adults Residing in Lalitpur, NepalDocument8 pagesEffectiveness of Structured Teaching Program On Self-Medication Knowledge and Its Adverse Effects Among Middle Age Adults Residing in Lalitpur, NepalIJAR JOURNALNo ratings yet
- Cerebrospinal Fluid: Learning ObjectivesDocument18 pagesCerebrospinal Fluid: Learning ObjectivesJonalyn LumantasNo ratings yet
- Insulin Pumps and Sensors Cox PDFDocument42 pagesInsulin Pumps and Sensors Cox PDFDevang SNo ratings yet
- Nat MurDocument19 pagesNat MurSun BNo ratings yet
- New Insulin Delivery Recommendations: Supplemental Ap-Pendix 1Document25 pagesNew Insulin Delivery Recommendations: Supplemental Ap-Pendix 1Fariza AyudiaNo ratings yet
- Scalp Acupuncture Treatment Protocol For Anxiety Disorders: A Case ReportDocument6 pagesScalp Acupuncture Treatment Protocol For Anxiety Disorders: A Case ReportTanuku NetNo ratings yet
- D - Guideline On Number of Embryos To Transfer During IVF ICSI - Stakeholder ReviewDocument135 pagesD - Guideline On Number of Embryos To Transfer During IVF ICSI - Stakeholder Reviewshobhitbhargava39No ratings yet
- Macrophages - A Review of Their Role in Wound Healing and Their Therapeutic UseDocument17 pagesMacrophages - A Review of Their Role in Wound Healing and Their Therapeutic UseklaumrdNo ratings yet
- NCP CalculiDocument8 pagesNCP CalculihailleyannNo ratings yet
- Morning Report Obs FebrisDocument10 pagesMorning Report Obs FebrisJessicaNo ratings yet
- MELANOMADocument3 pagesMELANOMAKathlyn PactorananNo ratings yet
- Inpatient Glycemic ManagementDocument13 pagesInpatient Glycemic Managementmiss betawiNo ratings yet
- Swedish Massage InfoDocument5 pagesSwedish Massage InfoJoy CelestialNo ratings yet
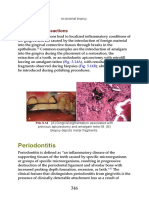
- Periodontitis: Foreign-Body ReactionsDocument25 pagesPeriodontitis: Foreign-Body ReactionsAisyah Arina NurhafizahNo ratings yet