100% found this document useful (2 votes)
950 views47 pagesAdvance Trauma Life Support (ATLS)
1. Advance Trauma Life Support (ATLS) provides guidelines for the initial assessment and management of trauma patients. It outlines steps for preparation, triage, primary and secondary surveys, and reevaluation.
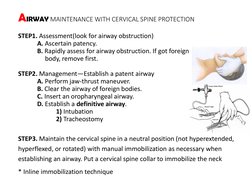
2. The primary survey focuses on the ABCDE approach to rapidly identify life-threatening injuries: Airway, Breathing, Circulation, Disability, and Exposure. Airway obstruction, tension pneumothorax, open pneumothorax, massive hemorrhage and spinal cord injuries are priorities.
3. Adjunct exams like x-rays, ultrasound, and labs help identify less apparent injuries before moving to the secondary survey for a full head-to-toe examination. Ongoing
Uploaded by
Ben Man JunCopyright
© © All Rights Reserved
We take content rights seriously. If you suspect this is your content, claim it here.
Available Formats
Download as PPTX, PDF, TXT or read online on Scribd
100% found this document useful (2 votes)
950 views47 pagesAdvance Trauma Life Support (ATLS)
1. Advance Trauma Life Support (ATLS) provides guidelines for the initial assessment and management of trauma patients. It outlines steps for preparation, triage, primary and secondary surveys, and reevaluation.
2. The primary survey focuses on the ABCDE approach to rapidly identify life-threatening injuries: Airway, Breathing, Circulation, Disability, and Exposure. Airway obstruction, tension pneumothorax, open pneumothorax, massive hemorrhage and spinal cord injuries are priorities.
3. Adjunct exams like x-rays, ultrasound, and labs help identify less apparent injuries before moving to the secondary survey for a full head-to-toe examination. Ongoing
Uploaded by
Ben Man JunCopyright
© © All Rights Reserved
We take content rights seriously. If you suspect this is your content, claim it here.
Available Formats
Download as PPTX, PDF, TXT or read online on Scribd
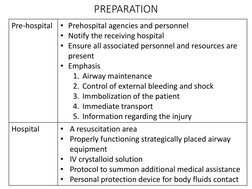
- Initial Assessment and Management: Covers the step-by-step process of initial care for trauma patients including preparation, triage, surveys, and definitive care assessments.
- Life Threatening Conditions: Details various life-threatening conditions detected during primary surveys, organized under the acronym ATOM FC H.