Professional Documents
Culture Documents
Komplikasi Kala III Persalinan
Uploaded by
febryana wulandari0 ratings0% found this document useful (0 votes)
9 views27 pagesThis document discusses complications of the third stage of labor. It begins by listing some complications including postpartum hemorrhage, retained placenta, inverted uterus, and obstetric shock. It then provides more details on postpartum hemorrhage, including its causes related to poor uterine contraction, retained tissue, trauma, or coagulation abnormalities. The document also discusses algorithms for managing postpartum hemorrhage and compressing the uterus. It provides classifications for hemorrhagic and septic shock and their signs and symptoms. Treatment steps for resuscitating hemorrhagic shock are also outlined. Inverted uterus is then discussed, including its types, signs, and manual or surgical treatment approaches.
Original Description:
Original Title
5_6208752998806454939
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses complications of the third stage of labor. It begins by listing some complications including postpartum hemorrhage, retained placenta, inverted uterus, and obstetric shock. It then provides more details on postpartum hemorrhage, including its causes related to poor uterine contraction, retained tissue, trauma, or coagulation abnormalities. The document also discusses algorithms for managing postpartum hemorrhage and compressing the uterus. It provides classifications for hemorrhagic and septic shock and their signs and symptoms. Treatment steps for resuscitating hemorrhagic shock are also outlined. Inverted uterus is then discussed, including its types, signs, and manual or surgical treatment approaches.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views27 pagesKomplikasi Kala III Persalinan
Uploaded by
febryana wulandariThis document discusses complications of the third stage of labor. It begins by listing some complications including postpartum hemorrhage, retained placenta, inverted uterus, and obstetric shock. It then provides more details on postpartum hemorrhage, including its causes related to poor uterine contraction, retained tissue, trauma, or coagulation abnormalities. The document also discusses algorithms for managing postpartum hemorrhage and compressing the uterus. It provides classifications for hemorrhagic and septic shock and their signs and symptoms. Treatment steps for resuscitating hemorrhagic shock are also outlined. Inverted uterus is then discussed, including its types, signs, and manual or surgical treatment approaches.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 27
Komplikasi Kala III Persalinan
1- Haemorrhagic Postpartum (HPP)
2- Retensio Placenta.
3- Inversio Uterus.
4- Syok dalam Obstetric (collapse)
Postpartum hemorrhage (PPH)
The most important single cause of maternal death in
both developing and developed countries.
Excessive bleeding occurs because of an abnormality
in one of four basic processes, referred to in the “4Ts”
mnemonic, either individually or in combination :
Tone (poor uterine contraction after delivery)
Tissue (retained products of conception or blood clots).
Trauma (to genital tract), or
Thrombin (coagulation abnormalities).
HAEMOSTASIS algorithm
H : Ask for help , S : Shift to operating theatre.
A : Assess (vitals, blood loss) & Bimanual compression.
resuscitate.
Non pneumatic or pneumatic
E : Establish etiology (4 T)
anti- shock garment.
Ecbolics (syntometrine,
ergometrine). T : Tissue & trauma to be
Ensure availability of blood.
excluded.
M : Massage the uterus. A : Apply compression sutures.
O : Oxytocin infusion & S : Systematic pelvic
prostaglandin. devascularisation.
I : Interventional radiology.
S : Subtotal /total hysterectomy.
Kompresi Uterus
The golden hour of : resuscitation
The golden hour of resuscitation : golden hour is the
time by which resuscitation must be initiated to ensure
better survival.
RULE of 30, IF :
SBP falls by 30 mmHg,
HR rises by 30 beats/min,
RR ? to 30 breaths/min,
Hct drop by 30%,
Urine output <30 ml/hr
She is likely to have lost at least 30% of her blood
volume, is in moderate shock leading to severe shock.
Stepwise administration of uterotonic
drugs
Starting with intravenous oxytocin, following with
intramuscular Methylergometrin and as last option
prostaglandine derivates as prostaglandine F2, E2 or
misoprostol.
In hypertensive patients, methylergometrin should be
avoided, as it should be done with prostaglandins in
asthmatic women.
Syok hemoragik dan septik
Etiologi
Syok hemoragik terjadi karena perdarahan akibat
abortus , KET, cedera pembedahan, perdarahan
antepartum, perdarahan postpartum atau koagulopati.
Syok septik biasanya ditimbulkan oleh penyebaran
endotoksin :
bakteri gram negatif sering (coli, proteus,
pseudomonas, enterokokus, aerobakter).
bakteri gram positif jarang (streptokokus,
stafilokokus, klostridium welchii)
Klasifikasi syok hemoragik
Syok ringan
Perdarahan < 20% volume darah penurunan perfusi
jaringan dan organ non vital.
Tidak terjadi perubahan kesadaran, volume urin yg
keluar normal atau sedikit berkurang, dan mungkin
terjadi asidosis metabolik.
Syok sedang
Terjadi penurunan perfusi pada organ yang tahan
terhadap iskemia waktu singkat (hati, usus, ginjal).
Timbul oliguria (urin <0,5ml/kgBB/jam) dan asidosis
metabolik, tetapi kesadaran masih baik.
Klasifikasi syok hemoragik
Syok berat
Perfusi jaringan otak dan jantung sudah tidak adekuat.
Terjadi anuria, penurunan kesadaran (delirium, stupor,
koma) dan sudah ada gejala hipoksia jantung (EKG
abnormal, curah jantung turun)
Perdarahan ≥50% menyebabkan henti jantung.
TD cepat menurun dan pasien jadi koma, nadi tidak
teraba mati klinis (nadi tidak teraba, apneu)
Gejala klinik syok hemoragik
Syok ringan
Takikardia minimal, hipotensi sedikit, vasokonstriksi
tepi ringan : kulit dingin, pucat, basah. Urin normal /
sedikit berkurang. Keluhan : merasa dingin.
Syok sedang
Takikardia 100-120/menit, hipotensi sistolik 90-100
mmHg. Oliguria/anuria. Keluhan : haus.
Syok berat
Takikardia >120/menit, hipotensi sistolik < 60mmHg,
pucat sekali, anuria, agitasi, kesadaran menurun.
Gejala klinik syok septik
Demam tinggi >38,9°C, sering diawali dengan menggigil,
kemudian suhu turun dalam beberapa jam (jarang hipotermi).
Takikardia
Hipotensi (sistolik < 90mmHg)
Ptekia, leukositosis atau leukopenia, trombositopenia
Hiperventilasi dengan hipokapnia
Gejala lokal misalnya nyeri tekan di daerah abdomen,
perirektal
Syok septik dicurigai pada : demam, hipotensi,
trombositopenia, atau koagulasi intravaskular yang tidak
dapat diterangkan penyebabnya.
Resusitasi syok hemoragik
Sebelumnya lakukan tindakan yang bertujuan untuk
pemulihan segera perfusi jaringan dan kapasitas
angkut oksigen yang adekuat
Posisi pasien : baringkan terlentang dengan kaki
ditinggikan
Bebaskan dan pelihara jalan nafas : tidur tanpa bantal,
kepala tengadah
Beri O2 5-10 L/menit melalui kanula hidung atau
sungkup muka
Resusitasi syok hemoragik
Resusitasi cairan
Kanul iv ukuran besar (16 G), pasang kateter vena sentral.
Petunjuk keberhasilan resusitasi : perbaikan tekanan
pengisian atrium, produksi urin, perbaikan kesadaran.
Awal : berikan cairan garam berimbang (RL, NaCl) 2-3
kali jumlah darah yang hilang dengan tetesan cepat selama
20-30 menit.
Pemberian D5% tidak dianjurkan intoksikasi air dan
edema otak.
Cairan koloid : dekstran, albumin 5%, HES
Mengganti darah transfusi.
Resusitasi syok hemoragik
Pemberian obat-obatan
Sodium bikarbonat
Vasokonstriktor
Kortikosteroid
Keberhasilan resusitasi
Tekanan pengisian atirum normal / mendekati normal
(tekanan vena sentral 3-8 cm H2O)
Produksi urin > 0,5 ml/kgBB/jam
Kesadaran bertambah baik
Perfusi jaringan meningkat
Curah jantung meningkat (>3,5 L/menit)
Resusitasi syok hemoragik
Kegagalan resusitasi
Peningkatan tekanan pengisian atrium dan produksi urin
> normal pemberian cairan terlalu banyak cairan
diperlambat
Tekanan pengisian atrium dan produksi urin < normal
cairan lebih banyak
Penilaian
Observasi cermat : TD, nadi, respirasi, kesadaran, tekan
vena sentral
Ukur cairan masuk dan keluar
Periksa Hb dan Ht secara periodik
Lakukan analisis gas darah arteri
Medika mentosa pd syok septik
Terapi cairan
Cairan garam berimbang 1-2 L selama 30-60 menit
perbaiki sirkulasi tepi dan produksi urin
Obat inotropik : Dopamin dosis awal <5µg/kgBB /menit
aliran darah ginjal dan mesenterik ↑
Antibiotika : dosis > tinggi iv
Tindakan pembedahan
Untuk mengeluarkan / drainasi sumber infeksi
Medika mentosa pd syok septik
Sodium bikarbonat
Utk koreksi asidosis metabolik yg berat
Kortikosteroid
Masih diperdebatkan. Deksametason 3 mg/kgBB (iv)
atau Metilprednisolon 30mg/kgBB diulangi tiap 4 jam
(bila perlu)
Heparin
Bila syok septik disertai koagulasi intravaskular
diseminata (DIC)
Inversio Uteri
Pendahuluan
Definisi:
The body of the uterus is partially or completely turned
inside out.
Etiology:
(I) Spontaneous inversion :
1- Partus Precipitatus.
2- Tali pusat pendek.
4- Submucous myoma.
(II) Iatrogenic inversion :
1. Penekanan fundus uteri
2. Tarikan tali pusat yang berlebihan.
Tingkatan
Tingkatan:
1. Tingkat I :
Fundus uteri inversi kedalam cavum uteri.
2. Tingkat II :
Fundus uteri inversi kedalam cavum uteri dan keluar melalui
serviks uteri.
3. Tingkat III :
Seluruh uterus, termasuk cervix inversi kedalam vagina dan
tampak diluar vulva
N.B.
- Incomplete inversion : Tingkat I dan II.
- Complete inversion : Tingkat III.
Gejala dan Tanda
(A) Gejala:
1. Nyeri abdomaen bawah.
2. Sensasi penuh dalam vagina
Terasa masih ingin mengejan setelah plasenta lahir
3. Vaginal bleeding
4. Subacute inversion:
Gejala ringan dan bertahap menjadi berat ketika penderita
merasakan ada bekuan darah tertahan dan infeksi.
Inversio Uteri
Gejala dan Tanda
(B) Tanda:
(1) Pemeriksaan Umum:
Gejala Shock neorogenik
Traksi peritoneum dan tekanan pada tuba, ovarium dan
intestinum
(2) Abdominal examination:
- Cupping fundus uteri -------- pada tingkat I dan II
- Tidak teraba fundus uterus -------- pada tingkat III
(3) Vaginal examination:
Inversi uterus tingkat II dan III tampak ada massa lunak merah abu-
abu pada vagina dan vulva.
Penatalaksanaan
(1) Mengatasi shock
(2) Manual reduksi/reposisi:
Inversi uterus dilakukan reduksi secara manual dengan
anaesthesia, jangan dilakukan penundaan reduksi walau
uterus mengalami edema atau sulit dikembalikan.
Lokalisasi yang mengalami inversi dikembalikan
terlebih dahulu, dilanjutkan pada area fundus uteri
Massage uterus dan berikan ergometrine , oxytocin drip
dan antibiotics.
Manual Reduksi
Gejala dan Tanda
(3) Hydrostatic reduction:
Replacement is possible by fluid pressure with warm
saline delivered into the vagina through a wide bore tube
from a container held at a height of about 60 cm. The
vaginal introitus is closed by holding the labia major
together.
(4) Surgical reduction:
Dilakukan pada inversio subacute atau chronic inversio
Insisi cervix bagian posterior atau anterior kemudian
dilakukan reposisi uterus pervaginam atau perabdominan
Sekian
You might also like
- Post Partum Haemorrhage (PPH)Document33 pagesPost Partum Haemorrhage (PPH)Khan WasimNo ratings yet
- Postpartal HemorrhageDocument9 pagesPostpartal HemorrhageJkimNo ratings yet
- Post Partum Hemorrhage: Presented by Banita Rana Nursing Tutor SmvdconDocument27 pagesPost Partum Hemorrhage: Presented by Banita Rana Nursing Tutor SmvdconSahil Chadgal100% (2)
- Complication of Postpartum PeriodDocument115 pagesComplication of Postpartum PeriodLiza Aingelica100% (1)
- Post Partum HemorrhageDocument38 pagesPost Partum Hemorrhageariani putri devantiNo ratings yet
- Post Partum HemorrhageDocument26 pagesPost Partum HemorrhageZulfan ZulfanNo ratings yet
- Postpartum Haemorrhage: Mrs - Nilakshi Barik MandalDocument40 pagesPostpartum Haemorrhage: Mrs - Nilakshi Barik MandalNilakshi Barik Mandal100% (1)
- Post Partum HemorhageDocument7 pagesPost Partum HemorhageLithiya JoseNo ratings yet
- Complications of 3 Stage of Labour: Supervisor - Sas Dr. Mon Mon Khine Presenter - Hs Chan Bawm HszwekoooDocument48 pagesComplications of 3 Stage of Labour: Supervisor - Sas Dr. Mon Mon Khine Presenter - Hs Chan Bawm HszwekooozkoNo ratings yet
- DIALYSISDocument30 pagesDIALYSISHecel Olita75% (4)
- Postpartum Complication: By: SRI MUDAYATI.N.,S.Kp.,M.KesDocument85 pagesPostpartum Complication: By: SRI MUDAYATI.N.,S.Kp.,M.KesAyu NdaryNo ratings yet
- Bailey S1Document17 pagesBailey S1hazama kurroNo ratings yet
- Post Partum HemorrahgeDocument41 pagesPost Partum HemorrahgegibreilNo ratings yet
- Kegawatdaruratan Di Bidang Bedah Umum (Acute Abdomen)Document40 pagesKegawatdaruratan Di Bidang Bedah Umum (Acute Abdomen)Bimo MuktiNo ratings yet
- Complication of 3rd Stage of LabourDocument48 pagesComplication of 3rd Stage of LabourPayal SharmaNo ratings yet
- Postpartal HemorrhageDocument54 pagesPostpartal HemorrhageInday BertaNo ratings yet
- Stress IncontinenceDocument44 pagesStress IncontinenceswatisinghnigeriaNo ratings yet
- Shock in ObstetricsDocument38 pagesShock in ObstetricsBeulah AlexNo ratings yet
- New DOCX DocumentDocument21 pagesNew DOCX DocumentDoe DoeNo ratings yet
- Aetiology and Risk Factors:: Trauma and Thrombin. ToneDocument10 pagesAetiology and Risk Factors:: Trauma and Thrombin. ToneArtika MalaNo ratings yet
- PPH MGT and FPDocument65 pagesPPH MGT and FPElsai EsbNo ratings yet
- ObGyn Case FilesDocument27 pagesObGyn Case Filesyanks1120100% (3)
- 23 Anaesthesia For Emergency SurgeryDocument7 pages23 Anaesthesia For Emergency SurgeryAtuy NapsterNo ratings yet
- 2 Semester 1 Major Patho AnatoDocument49 pages2 Semester 1 Major Patho AnatoManushi HenadeeraNo ratings yet
- Pembimbing: Dr. R. Vito Mahendra E, M.Si Med, SP.B M. Adri Kurniawan 30101306981Document31 pagesPembimbing: Dr. R. Vito Mahendra E, M.Si Med, SP.B M. Adri Kurniawan 30101306981Adek AhmadNo ratings yet
- Nital Disorders and Injuries-1Document43 pagesNital Disorders and Injuries-1qruz Mohamed DiisNo ratings yet
- The Average Blood Loss Following Vaginal Delivery, Cesarean Delivery and Cesarean Hysterectomy Is 500 ML, 1000 ML and 1500 ML RespectivelyDocument11 pagesThe Average Blood Loss Following Vaginal Delivery, Cesarean Delivery and Cesarean Hysterectomy Is 500 ML, 1000 ML and 1500 ML RespectivelypriyankaNo ratings yet
- Management of Uterine InversionDocument36 pagesManagement of Uterine Inversionogundapo100% (2)
- Obstetric EmergenciesDocument44 pagesObstetric EmergenciesVijith.V.kumarNo ratings yet
- CA Serviks Pepete Stikes Muhammadiyah PringsewuDocument9 pagesCA Serviks Pepete Stikes Muhammadiyah Pringsewuiqbal asegabNo ratings yet
- CA SERVIKS PepeteDocument9 pagesCA SERVIKS Pepeteiqbal asegabNo ratings yet
- Postpartum HemorrhageDocument11 pagesPostpartum HemorrhageColeen Aubrey TanNo ratings yet
- Presentation-WPS OfficeDocument30 pagesPresentation-WPS OfficeKinjal VasavaNo ratings yet
- Post Partum ComplicationDocument29 pagesPost Partum ComplicationPutri Rizky AmaliaNo ratings yet
- Pemicu 1 KGD: Mustika Rukmana 405130182 Kel 6Document54 pagesPemicu 1 KGD: Mustika Rukmana 405130182 Kel 6tikaNo ratings yet
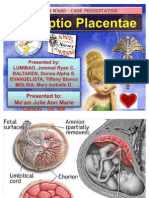
- Abruptio Placentae (Case Presentation)Document46 pagesAbruptio Placentae (Case Presentation)Bansot Baltaken100% (3)
- Surgery (UWorld Step 2)Document39 pagesSurgery (UWorld Step 2)Nishok VSNo ratings yet
- Surgical Diseases of The SpleenDocument28 pagesSurgical Diseases of The SpleenRassoul Abu-NuwarNo ratings yet
- Hemorragic Post PartumDocument35 pagesHemorragic Post PartumMuhammad AsrizalNo ratings yet
- Gastrointestinal EmergenciesDocument104 pagesGastrointestinal EmergenciesSuhaeb AlmarafyNo ratings yet
- 1066 Complications of 3rd Stage of Labour Injuries To Birth CanalDocument110 pages1066 Complications of 3rd Stage of Labour Injuries To Birth CanalSweety YadavNo ratings yet
- Diseases of Rectum and Anal CanalDocument68 pagesDiseases of Rectum and Anal CanalKoridor Falua Sakti Halawa 21000063No ratings yet
- Postoperative Surgical Complications 2015Document26 pagesPostoperative Surgical Complications 2015AlaaGaballaNo ratings yet
- Presented by - Yogesh Dengale 1 M.SC NursingDocument56 pagesPresented by - Yogesh Dengale 1 M.SC NursingalexjohnvtNo ratings yet
- Postpartum Hemorrhage FinalDocument6 pagesPostpartum Hemorrhage Finalvarshasharma05No ratings yet
- Scrotal MassesDocument19 pagesScrotal MassesJohnNo ratings yet
- Third Stage of Labor: by Feyisa T. (Obstetrician and Gynecologist)Document51 pagesThird Stage of Labor: by Feyisa T. (Obstetrician and Gynecologist)Haleluya LeulsegedNo ratings yet
- 7 Diseases of SpleenDocument29 pages7 Diseases of SpleenMAH pedNo ratings yet
- Small Bowel Obstruction &post Operative IleusDocument62 pagesSmall Bowel Obstruction &post Operative IleusMamanya Fadhil HaniNo ratings yet
- Shock Management: by Group 7Document87 pagesShock Management: by Group 7Nur Khairah AmalinaNo ratings yet
- Patient'S Profile: GROUP 1: Camposano, Cielo, Edem, Ibalin, RodriguezDocument3 pagesPatient'S Profile: GROUP 1: Camposano, Cielo, Edem, Ibalin, RodriguezDivina Gracia Vibal CieloNo ratings yet
- Post Partum HaemorrhageDocument6 pagesPost Partum Haemorrhagenancy jeyakumarNo ratings yet
- Day 10-11 - NCM 109 Lec - High Risk Post PartumDocument41 pagesDay 10-11 - NCM 109 Lec - High Risk Post PartumGrey KnighttNo ratings yet
- PPH 2024Document25 pagesPPH 2024Anthony Mwangi100% (1)
- Chest PhysiotherapyDocument12 pagesChest PhysiotherapyZaenal ArifNo ratings yet
- Body Cavity FluidsDocument29 pagesBody Cavity FluidspriyagerardNo ratings yet
- 3....... OB EmergencyDocument79 pages3....... OB EmergencyRadhika JoshiNo ratings yet
- Post Partum Haem.Document90 pagesPost Partum Haem.rachael annor100% (1)
- Approach To ShockDocument28 pagesApproach To ShockSyasya ZulkiffliNo ratings yet
- Third Stage of LabourDocument4 pagesThird Stage of LabourKhazoliyaNo ratings yet
- NCP Acute Pain OB Ward PDFDocument2 pagesNCP Acute Pain OB Ward PDFambiit25No ratings yet
- 12th - Dystocia Its CausesDocument59 pages12th - Dystocia Its Causesnoor aineNo ratings yet
- L-1 Preparation of Gases MCQDocument31 pagesL-1 Preparation of Gases MCQapi-233604231No ratings yet
- Direction: Select The ONE BEST Lettered Answer or Completion in Each QuestionDocument8 pagesDirection: Select The ONE BEST Lettered Answer or Completion in Each QuestionAhmed BassettNo ratings yet
- Redescription of Butlerius Butleri Goodey, 1929Document9 pagesRedescription of Butlerius Butleri Goodey, 1929gksingh82No ratings yet
- OB Exit ExamDocument2 pagesOB Exit ExamMariana B.No ratings yet
- Female Reproductive OrganDocument31 pagesFemale Reproductive OrganSabita PaudelNo ratings yet
- Lesson Plan SCIENCE 5 (WEEK 1, DAY 1)Document4 pagesLesson Plan SCIENCE 5 (WEEK 1, DAY 1)Angel rose reyes100% (1)
- NCM Chap 6Document7 pagesNCM Chap 6Aiza OronceNo ratings yet
- Holly TranzorDocument2 pagesHolly Tranzorapi-26246128No ratings yet
- Care Analysis For PamelaDocument7 pagesCare Analysis For PamelaNicxx Gaming100% (1)
- 7B Reproduction Test 2004Document2 pages7B Reproduction Test 2004api-3698146100% (3)
- Brachytherapy GYN Applicator CatalogDocument64 pagesBrachytherapy GYN Applicator CatalogJuan Lombardero100% (1)
- Common Causes of Dysfunctional Labor:: DystociaDocument8 pagesCommon Causes of Dysfunctional Labor:: DystociaAngelo ArabejoNo ratings yet
- Management of Bleeding in Early PregnancyDocument44 pagesManagement of Bleeding in Early PregnancyOyedele OluwaseunNo ratings yet
- Postpartum Uterine Arteriovenous Malformation: A Case ReportDocument5 pagesPostpartum Uterine Arteriovenous Malformation: A Case ReportIJAR JOURNALNo ratings yet
- The Role of Hysteroscopy in The Diagnosis and Treatment of AdenomyosisDocument1 pageThe Role of Hysteroscopy in The Diagnosis and Treatment of AdenomyosisAnca Berescu StefanNo ratings yet
- Early Mammalian DevelopmentDocument23 pagesEarly Mammalian DevelopmentrainnysofthiefNo ratings yet
- Obstructed Labour (OL)Document34 pagesObstructed Labour (OL)ruhulcoc1No ratings yet
- Ultrasound of The Pregnant Acute AbdomenDocument16 pagesUltrasound of The Pregnant Acute Abdomenjohn omariaNo ratings yet
- Uterine Atony: Group 3Document23 pagesUterine Atony: Group 3Trisha Mae MarquezNo ratings yet
- Sun Maiden Plus Maxilink OneDocument22 pagesSun Maiden Plus Maxilink OneAre R BxmnNo ratings yet
- What Is Uterine ProlapseDocument4 pagesWhat Is Uterine Prolapsestoopid08No ratings yet
- Essential Intrapartum Care UpdatedDocument11 pagesEssential Intrapartum Care UpdatedRica PeñanoNo ratings yet
- CSEC Biology - B9 Human Reproduction PPQs PDFDocument11 pagesCSEC Biology - B9 Human Reproduction PPQs PDFChelsea FrancisNo ratings yet
- Myoma CaseDocument111 pagesMyoma Caseapi-1976296750% (2)
- Rabbit Soft Tissue Surgery: Zoltan Szabo,, Katriona Bradley,, Alane Kosanovich CahalaneDocument30 pagesRabbit Soft Tissue Surgery: Zoltan Szabo,, Katriona Bradley,, Alane Kosanovich CahalaneTayná P DobnerNo ratings yet
- Cayao-Lasam vs. ClaroDocument11 pagesCayao-Lasam vs. ClaroAnonymous oDPxEkdNo ratings yet
- Normal Spontaneous Vaginal DeliveryDocument41 pagesNormal Spontaneous Vaginal DeliveryDelphy Varghese100% (1)