Professional Documents
Culture Documents
Harvesting STSG: I Gusti Ayu Putri Purwanthi
Harvesting STSG: I Gusti Ayu Putri Purwanthi
Uploaded by
Putri Purwanthi0 ratings0% found this document useful (0 votes)
5 views22 pagesOriginal Title
Harvesting Skin Graft
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
5 views22 pagesHarvesting STSG: I Gusti Ayu Putri Purwanthi
Harvesting STSG: I Gusti Ayu Putri Purwanthi
Uploaded by
Putri PurwanthiCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 22
HARVESTING STSG
I GUSTI AYU PUTRI PURWANTHI
DEFINISI SKIN GRAFT
• Tindakan memindahkan sebagian ketebalan kulit (epidermis dengan
sebagian/seluruh ketebalan dermis) dari satu tempat ke tempat lain
dimana jaringan tersebut bergantung pada pembuluh darah baru dari
jaringan penerima untuk menjamin kelangsungan hidupnya.
KLASIFIKASI DAN PERBEDAAN
STSG (SPLIT THICKNESS SKIN GRAFT) FTSG (FULL THICKNESS SKIN GRAFT)
Epidermis dengan sebagian dermis Epidermis dengan seluruh dermis
Ketebalan:
- Thick: ¾ dermis (0.008 – 0.012 mm)
- Medium: ½ dermis (0.012 – 0.018 mm)
- Thin: ¼ dermis (0.018 – 0.030 mm)
Kemungkinan Take lebih besar Kemungkinan Take lebih kecil
Untuk defek luas Untuk defek kecil
Dapat diambil pada bagian tubuh manapun Tempat pengambilan terbatas (inguinal, supraclavicular,
retroauricula)
Kontraksi Sekunder >>> Kontraksi Sekunder <<<
Estetika <<< (perubahan warna, mengkilat) Estetika >>>
Donor dapat sembuh sendiri (epitelisasi) Donor harus dijahit
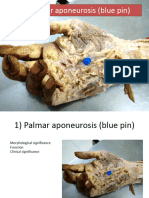
ANATOMI
MEKANISME GRAFT HEALING
The processes which results in graft’s reattachment
and revascularization re collectively referred as TAKE
• Imbibition (0-48 hours) ischemic phase known as
plasmatic or serum imbibition
• Inosculation (48 – 72 hours) vessels from the
wound bed connecting with the existing vessels in
the graft
• Revascularization (>96 hours) angiogenesis,
revaskularisasi
THE GRAFT BED
• Graft bed must be capable of providing the necessary initial fibrin
anchorage and enough blood supply to vascularize the graft.
GRAFT TAKE NO GRAFT TAKE
• Muscle • Bare cartilage
• Fascia • Bare tendon
• Fat (bervariasi) on the face, fat is • Bare cortical bone (bare cortex of
extremely vascular and grafts take skull, bare cortex of mandible)
easily, elsewhere it is relatively has
poor vascularity
• Cartilage covered with perichondrium
• Bone (varies) covered with
periosteum, hard palate, bony orbit
• Tendon covered with paratenon
STSG TECHNIQUES
DONOR SITES
CHOOSING DONOR SITES >>>>
GRAFT CUTTING INSTRUMENT
The most commonly used for cutting grafts:
1. Humby Knife can only be used in convex surfaces
2. The power-driven dermatome
POSITIONING DONOR SITES (THIGH)
CUTTING THE GRAFT
1. Preparation and the instrument and donor
site (lubrication of the donor surface)
2. To reduce bleeding during skin harvest some
surgeons prefer to infiltrate the donor site
area primarily with epinephrine diluted in
saline subcutaneously
3. Adjusting the graft thickness adjusting
the distance between the roller and the bed
CUTTING THE GRAFT
4. Assesment of the graft thickness
• Translucency of the graft
• The pattern of bleeding of the donor sites (thin
graft high density of tiny bleeding point, thicker
graft lower density of larger bleeding point)
5. The presence of assistant holding the skin
just behind the knife before it get cuts
Split-thickness harvest with a manual knife. Alternatively, if no
electrically driven dermatome is available, skin grafts can be
carefully harvested with a manual knife. This procedure
requires experience and harvest of even thickness is difficult.
Split-thickness harvest and grafting. (A) Split-thickness skin
graft (STSG) harvest with an electrically driven dermatome at
the anterior thigh. (B) The skin graft should be positioned flat
on the mesh template: this can be perforated by multiple slits
to (C) expand the graft up to six times its original
size. (D) Meshed STSGs are ideal to cover large and uneven
wounds. Stapler fixation is a time-saving method to fix large
grafts.
The most commonly used mesh ratio is 1 : 1.5 in smaller
wounds, while a mesh ratio of 1 : 3 and 1 : 6 is often needed to
cover large burns.
STORAGE OF THE SKIN
• The graft is wrapped in gauze moistened with saline and placed in a
sterile, sealed container
HEALING OF THE DONOR AREA
• The donor sites of the thin graft, with its full complement of cut
pilosebaseous follicles, heals approximately 7-9 days
• The thick graft, depends on the virtually entirely on sweat gland
remnant, heals more slowly, taking 14 days or more
• Intermediate thickness leave a percentage of pilosebaceous
follicles 9 – 14 days
DONOR SITE MANAGEMENT
• Pain settles 3-4 days, often followed by itching
• Traditionally donor areas were dressed with tulle grass, over which
was laid absorbent gauze, the whole held in position with a crepe
bandage
• Alternatively the dressing was left in situ until it separated
spontaneously
• Alginate dressing (kaltostat)
• Experience is that waiting 10 - 14 days before removing the dressing
leaves a more robust wound, better able to cope with the trauma
involved in its removal.
RECIPIENT SITE
• Surgically Clean Surface
• Preparing the recipient area
• Hemostasis prevent hematoma
• The granulating area
• Healthy granulations are flat, red and vascular, free from covering surface film
• Left ungrafted, granulations generally become more fibrous and less vascular
• The presence of streptococcus pyogenes is an absolute contraindication to any grafting
procedyre
• Infection with Ps. aeruginosa reduces graft take but not to an extent comparable with str.
pyogenes
• Preparation granulations for grafting
• An antiseptic such as chlorhexidine applied locallt is likely more efectif to eliminate
bacterial
• Eliminate slough
CAUSES OF GRAFT FAILURE
References
• Grabb and smith 8th edition
• Mcgregor fundamental technique and principle in plastic surgery
TERIMA KASIH
You might also like
- The Reconstructive LadderDocument60 pagesThe Reconstructive Ladderterri100% (1)
- Pande Komang Gerry Paramesta: Decision Making in Bowel Obstruction: A Review byDocument32 pagesPande Komang Gerry Paramesta: Decision Making in Bowel Obstruction: A Review byanon_550250832100% (1)
- Presentation 1Document25 pagesPresentation 1Nihar ShahNo ratings yet
- Thumb Congenital DisordersDocument16 pagesThumb Congenital Disordersqaz1122100% (1)
- RCS Edinburgh Basic Surgical Skills Direct Observation of Procedural SkillDocument1 pageRCS Edinburgh Basic Surgical Skills Direct Observation of Procedural SkilljoslinmtggmailcomNo ratings yet
- Teknik Operasi Splenektomi 2Document31 pagesTeknik Operasi Splenektomi 2sphericalfaNo ratings yet
- Lefort 1 OsteotomyDocument36 pagesLefort 1 OsteotomyNidhi Jayan100% (2)
- 21 Feet Is Way Too CloseDocument12 pages21 Feet Is Way Too ClosemarapubNo ratings yet
- Wings of Arian - Devri WallsDocument528 pagesWings of Arian - Devri WallsJoseph Dela Cruz100% (4)
- 1911 A1 Manual PDFDocument64 pages1911 A1 Manual PDFedu_canete100% (1)
- Skin Grafts and Flaps (DR - Ricko)Document25 pagesSkin Grafts and Flaps (DR - Ricko)lorensiafdNo ratings yet
- Skin Graf Dan FlapDocument28 pagesSkin Graf Dan FlapAlparisyi MuhamadNo ratings yet
- Plastic & Hand Surgery in Clinical Practice: Classifications and DefinitionsFrom EverandPlastic & Hand Surgery in Clinical Practice: Classifications and DefinitionsNo ratings yet
- Rekonstruksi SCC Dengan Flap Lateral ForeheadDocument7 pagesRekonstruksi SCC Dengan Flap Lateral Foreheadmichaeljt_md6463No ratings yet
- Flaps PDFDocument27 pagesFlaps PDFdrgurpal74No ratings yet
- Management of Fracture of The Edentulous Mandible Oral SurgeryDocument27 pagesManagement of Fracture of The Edentulous Mandible Oral SurgeryFourthMolar.comNo ratings yet
- Neligan Mandible FractureDocument17 pagesNeligan Mandible FractureRibka TheodoraNo ratings yet
- Skin Flap Dr. BrotoDocument17 pagesSkin Flap Dr. BrotoTommysNo ratings yet
- Fracture and Dislocation-Rahardyan Magetsari (2016) PDFDocument105 pagesFracture and Dislocation-Rahardyan Magetsari (2016) PDFRobertOktaChandraNo ratings yet
- Basic and Special Suturing Techniques in Surgery. Honlap 2Document57 pagesBasic and Special Suturing Techniques in Surgery. Honlap 2Arif Nurhidayat PrawirohardjoNo ratings yet
- Z-Plasty For Sculpturing of The Bifid Scrotum in Severe Hypospadias Asscociated With Penoscrotal TranspositionDocument5 pagesZ-Plasty For Sculpturing of The Bifid Scrotum in Severe Hypospadias Asscociated With Penoscrotal TranspositionneonitesNo ratings yet
- EktremitasDocument40 pagesEktremitasBram wijayaNo ratings yet
- FlapsinplasticsurgeryDocument63 pagesFlapsinplasticsurgerysomnathNo ratings yet
- Wound Healing Normal and Abnormal Mechanisms and Closure TechniquesDocument40 pagesWound Healing Normal and Abnormal Mechanisms and Closure TechniquesAhmad Fakhrozi Helmi100% (1)
- ColostomyDocument45 pagesColostomydrqiekiNo ratings yet
- HIPOSPADIA AwalDocument28 pagesHIPOSPADIA Awalnoor hasbil hakim100% (1)
- Skinflaps: Mary Tschoi,, Erik A. Hoy,, Mark S. GranickDocument16 pagesSkinflaps: Mary Tschoi,, Erik A. Hoy,, Mark S. Granickdanico59No ratings yet
- Principles of Management of Soft Tissue SarcomaDocument33 pagesPrinciples of Management of Soft Tissue Sarcomabashiruaminu100% (1)
- Thyroid Cancer Diagnosis and ManagementDocument45 pagesThyroid Cancer Diagnosis and Managementapi-3704562100% (1)
- Anestesi LokalDocument12 pagesAnestesi LokalKurniatiKhasanahQhafisaQurratul'ainNo ratings yet
- ClavusDocument4 pagesClavusargie3333No ratings yet
- Forehead Flap: DR Dipti Patil (1 MDS) Dept of Oral Maxillofacial Surgery KCDS, BangloreDocument42 pagesForehead Flap: DR Dipti Patil (1 MDS) Dept of Oral Maxillofacial Surgery KCDS, BangloreDipti PatilNo ratings yet
- BedahDocument139 pagesBedahLunaFia100% (1)
- FlapDocument4 pagesFlapMd Ahsanuzzaman PinkuNo ratings yet
- Kompartemen SindromDocument9 pagesKompartemen SindromPutri PratiwiNo ratings yet
- Oral LymphangiomaDocument8 pagesOral LymphangiomasevattapillaiNo ratings yet
- EGDT SepsisDocument8 pagesEGDT Sepsissiti fatmalaNo ratings yet
- Chronic Limb IschemiaDocument29 pagesChronic Limb IschemiaSadia NaveedNo ratings yet
- Acute Limb Ischemia Vs Critical Limb Ischemia: Clinical PracticeDocument51 pagesAcute Limb Ischemia Vs Critical Limb Ischemia: Clinical PracticedrhendyjuniorNo ratings yet
- Needle CricothyroidotomyDocument9 pagesNeedle Cricothyroidotomyhatem alsrour100% (2)
- WIFI Score For Diabetes Foot UlcerDocument17 pagesWIFI Score For Diabetes Foot Ulcertonylee24100% (1)
- Giant Cell TumorDocument35 pagesGiant Cell TumorHestikrnNo ratings yet
- Breast Reconstruction After Mastectomy For Breast Tumor: About 24 CasesDocument6 pagesBreast Reconstruction After Mastectomy For Breast Tumor: About 24 CasesIJAR JOURNALNo ratings yet
- Skin FlapDocument26 pagesSkin FlapkoasNo ratings yet
- Use of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFDocument9 pagesUse of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFJose Luis Granados SolerNo ratings yet
- Chronic Wound ManagementDocument31 pagesChronic Wound Managementadrianus andriNo ratings yet
- Tracheostomy: Indications and ProcedureDocument10 pagesTracheostomy: Indications and ProcedureAinur AbdrakhmanovaNo ratings yet
- 14 Anterolateral Thigh FlapDocument6 pages14 Anterolateral Thigh FlapAngga Putra100% (1)
- Fat Transfer To The Face: Technique and New Concepts: Facial Plastic Surgery Clinics of North America June 2001Document10 pagesFat Transfer To The Face: Technique and New Concepts: Facial Plastic Surgery Clinics of North America June 2001Priya BabyNo ratings yet
- Jurnal CA TyroidDocument4 pagesJurnal CA TyroidErvina ZelfiNo ratings yet
- Flaps: BY:-Dr. P. Koushik GUIDE: - DR (Brig.) B. B. DograDocument27 pagesFlaps: BY:-Dr. P. Koushik GUIDE: - DR (Brig.) B. B. DograSumit HadgaonkarNo ratings yet
- Modul Wound Bed Preparation DR Ardianto SucintaDocument37 pagesModul Wound Bed Preparation DR Ardianto SucintaArdianto SucintaNo ratings yet
- Skin FlapDocument26 pagesSkin FlapAnne TjanNo ratings yet
- 1537 Bedah PlastikDocument11 pages1537 Bedah PlastikFathah MuhammadNo ratings yet
- Kyestone Flaps PDFDocument9 pagesKyestone Flaps PDFDra. Bianca Ariza MoralesNo ratings yet
- Diaphragma InjuryDocument18 pagesDiaphragma InjuryAhmedNo ratings yet
- Finger Tip InjuryDocument39 pagesFinger Tip InjurySantomi PratamaNo ratings yet
- Calcifying Epithelial Odontogenic CystDocument21 pagesCalcifying Epithelial Odontogenic CystAnsh DuttaNo ratings yet
- Preventable Death: Dco: DR Thit Lwin School of Medicine UMSDocument56 pagesPreventable Death: Dco: DR Thit Lwin School of Medicine UMSStar CruiseNo ratings yet
- Neligan Vol 4 Chapter 10 MainDocument20 pagesNeligan Vol 4 Chapter 10 MainisabelNo ratings yet
- Chronic Limb Threatening IschemiaDocument35 pagesChronic Limb Threatening Ischemiasifatullah khanNo ratings yet
- Stenosing Tenosynovitis, (Trigger Finger) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandStenosing Tenosynovitis, (Trigger Finger) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Manual of Surgery Volume Second: Extremities—Head—Neck. Sixth Edition.From EverandManual of Surgery Volume Second: Extremities—Head—Neck. Sixth Edition.No ratings yet
- Harvesting Vascularized Fibula Flap & Deep Inferior Epigastric Perforators (Diep)Document31 pagesHarvesting Vascularized Fibula Flap & Deep Inferior Epigastric Perforators (Diep)Putri PurwanthiNo ratings yet
- Jadwal Scientific Session 29:10Document5 pagesJadwal Scientific Session 29:10Putri PurwanthiNo ratings yet
- Anatomi Sistem Lakrimal: - SekresiDocument13 pagesAnatomi Sistem Lakrimal: - SekresiPutri PurwanthiNo ratings yet
- Maxilofacial Anatomy: I Gusti Ayu Putri PurwanthiDocument10 pagesMaxilofacial Anatomy: I Gusti Ayu Putri PurwanthiPutri PurwanthiNo ratings yet
- Lacrimal Examination SlideshareDocument15 pagesLacrimal Examination SlidesharePutri PurwanthiNo ratings yet
- Lacrimal Examination SlideshareDocument15 pagesLacrimal Examination SlidesharePutri PurwanthiNo ratings yet
- Flexor Tendon ReconstructionDocument9 pagesFlexor Tendon ReconstructionPutri PurwanthiNo ratings yet
- Flexor Tendon ReconstructionDocument9 pagesFlexor Tendon ReconstructionPutri PurwanthiNo ratings yet
- Penelitian Dr. Roy Alat Dan Bahan: Microsurgery Set (Pinset 2, Gunting MikroDocument1 pagePenelitian Dr. Roy Alat Dan Bahan: Microsurgery Set (Pinset 2, Gunting MikroPutri PurwanthiNo ratings yet
- Anatomi Sistem Lakrimal: - SekresiDocument13 pagesAnatomi Sistem Lakrimal: - SekresiPutri PurwanthiNo ratings yet
- Causation & Remoteness of DamagesDocument10 pagesCausation & Remoteness of DamagesTee Khai Chen100% (1)
- Ortho DNB PrpapDocument12 pagesOrtho DNB PrpapRaj KumarNo ratings yet
- Upperlimb Spotters-1 090723Document57 pagesUpperlimb Spotters-1 090723KishoreNo ratings yet
- Microsoft Powerpoint - Introduction To WatercolourDocument4 pagesMicrosoft Powerpoint - Introduction To Watercolournave101No ratings yet
- Inguinal Hernia by Dr. TalabiDocument16 pagesInguinal Hernia by Dr. TalabidayomanNo ratings yet
- Muscle Grading and Testing ProceduresDocument5 pagesMuscle Grading and Testing Proceduresshodhganga100% (1)
- Timpuri Engleza + ExercitiiDocument24 pagesTimpuri Engleza + ExercitiiMihai CristeaNo ratings yet
- What Is The Nature of Memory?Document8 pagesWhat Is The Nature of Memory?Prithvi RajNo ratings yet
- Types of Bandaging: Picture ProcedureDocument6 pagesTypes of Bandaging: Picture ProcedureLeslie Banaag100% (6)
- GROUP 5 - Case StudyDocument48 pagesGROUP 5 - Case StudyNoldan King FranciscoNo ratings yet
- Lesson 8Document11 pagesLesson 8Jill ArciagaNo ratings yet
- The Failed Rotator CuffDocument307 pagesThe Failed Rotator Cufforthofitness2017No ratings yet
- B01 Geriatric Physical Therapy (3rd Ed) - Ch16 - ImpairedPostureDocument24 pagesB01 Geriatric Physical Therapy (3rd Ed) - Ch16 - ImpairedPostureChing HoNo ratings yet
- 10 Movies So Disturbing You Will Regret Watching Them: LGBT Videos ChannelsDocument33 pages10 Movies So Disturbing You Will Regret Watching Them: LGBT Videos ChannelsNaveen S YeshodaraNo ratings yet
- Dr. Ravi Sauhta - Best Orthopedic & Joint Replacement Surgeon in GurgaonDocument4 pagesDr. Ravi Sauhta - Best Orthopedic & Joint Replacement Surgeon in GurgaonPrateekNo ratings yet
- 05 N141 31673Document21 pages05 N141 31673priya thakurNo ratings yet
- 407 Exam 2 CH 4 5 Spr13 W o AnswDocument7 pages407 Exam 2 CH 4 5 Spr13 W o AnswMolly SmithNo ratings yet
- Kolokvij LexDocument3 pagesKolokvij LexBubica JožićNo ratings yet
- Legal Med Finals NotesDocument14 pagesLegal Med Finals NotesMichael Parreño VillagraciaNo ratings yet
- 04 Chapman vs. Underwood DigestDocument1 page04 Chapman vs. Underwood DigestNichole LanuzaNo ratings yet
- SDOT's SW Roxbury PlanDocument23 pagesSDOT's SW Roxbury PlanWestSeattleBlogNo ratings yet
- Rehabilitation Guidelines For Posterior Cruciate Ligament ReconstructionDocument6 pagesRehabilitation Guidelines For Posterior Cruciate Ligament ReconstructionMono MostafaNo ratings yet
- Evid Cases - WsoeDocument70 pagesEvid Cases - WsoeAntonio SalvadorNo ratings yet
- General Airbrush Troubleshooting: I'm Using Acrylic Paints and It Keeps CloggingDocument4 pagesGeneral Airbrush Troubleshooting: I'm Using Acrylic Paints and It Keeps CloggingheleahNo ratings yet
- Chest Drain - Evidence Based Nursing PolicyDocument7 pagesChest Drain - Evidence Based Nursing PolicyismuNo ratings yet
- Posterior Cruciate LigamentDocument12 pagesPosterior Cruciate LigamentJunaid IqbalNo ratings yet
- JIN SHIN JYUTSU Three Method CorrectionsDocument2 pagesJIN SHIN JYUTSU Three Method CorrectionsWalfutureNo ratings yet