Professional Documents
Culture Documents
Head Injury: Clasification of Traumatic Brain Injuries
Uploaded by
salvaryn ne0 ratings0% found this document useful (0 votes)
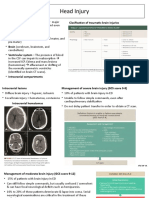
17 views7 pagesThe document discusses the management of traumatic brain injuries. It classifies brain injuries as mild, moderate, or severe based on Glasgow Coma Scale scores. For severe injuries (GCS 3-8), immediate stabilization and transport to the hospital is critical. For moderate injuries (GCS 9-12), serial exams are needed to monitor for deterioration. Treatment focuses on preventing secondary insults like hypoxia and hypotension. Diagnostic tests like head CT scans are important to identify injuries requiring surgery. Medical therapies aim to reduce intracranial pressure through interventions like hyperventilation, mannitol, hypertonic saline and barbiturates.
Original Description:
Original Title
Head Injury
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document discusses the management of traumatic brain injuries. It classifies brain injuries as mild, moderate, or severe based on Glasgow Coma Scale scores. For severe injuries (GCS 3-8), immediate stabilization and transport to the hospital is critical. For moderate injuries (GCS 9-12), serial exams are needed to monitor for deterioration. Treatment focuses on preventing secondary insults like hypoxia and hypotension. Diagnostic tests like head CT scans are important to identify injuries requiring surgery. Medical therapies aim to reduce intracranial pressure through interventions like hyperventilation, mannitol, hypertonic saline and barbiturates.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
17 views7 pagesHead Injury: Clasification of Traumatic Brain Injuries
Uploaded by
salvaryn neThe document discusses the management of traumatic brain injuries. It classifies brain injuries as mild, moderate, or severe based on Glasgow Coma Scale scores. For severe injuries (GCS 3-8), immediate stabilization and transport to the hospital is critical. For moderate injuries (GCS 9-12), serial exams are needed to monitor for deterioration. Treatment focuses on preventing secondary insults like hypoxia and hypotension. Diagnostic tests like head CT scans are important to identify injuries requiring surgery. Medical therapies aim to reduce intracranial pressure through interventions like hyperventilation, mannitol, hypertonic saline and barbiturates.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 7
Head Injury
• Scalp – generous blood supply major Clasification of traumatic brain injuries
blood loss, hemorrhagic shock, and even
death
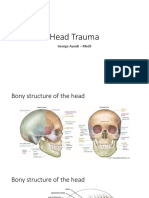
• Skull
• Meninges (dura mater, arachnoid mater, and
pia mater)
• Brain (cerebrum, brainstem, and
cerebellum)
• Ventricular system – The presence of blood
in the CSF can impair its reabsorption
increased ICP. Edema and mass lesions
(hematomas) effacement or shifting of
the normally symmetric ventricles
(identified on brain CT scans).
• Intracranial compartments
ATLS 10th ed.
Intracranial lesions Management of severe brain injury (GCS score 3-8)
• Diffuse brain injury = hypoxic, ischemic • 10% of patients with brain injury in ED
• Focal brain injury = hematomas, contusions • Unable to follow simple commands, even after
cardiopulmonary stabilization
Intracranial hematomas
• Do not delay patient transfer in order to obtain a CT scan.
ATLS 10th ed.
Management of moderate brain injury (GCS score 9-12)
• 15% of patients with brain injury in ED
• Can still follow simple commands, but usually confused / somnolent
& can have focal neurological deficits such as hemiparesis.
• 10% to 20% of these patients deteriorate & lapse into coma. Serial
neurological examinations are critical in the treatment of these
patients.
ATLS 10th ed.
Management of mild brain injury
(GCS score 13-15)
• A patient who is conscious & talking
may relate a history of
disorientation, amnesia, or transient
loss of consciousness.
• Most patients make uneventful
recoveries. 3% unexpectedly
deteriorate, potentially resulting in
severe neurological dysfunction.
ATLS 10th ed.
Primary survey & resuscitation
Brain injury often is adversely affected by secondary insults. The presence of
hypoxia & hypotension increase in the relative risk of mortality of 75%.
• Airway & breathing
• Early ETT in comatose patient
• Ventilate with 100% oxygen until blood gas measurements are obtained,
make appropriate adjustments to the fraction of inspired oxygen (FIO2)
Goal: oxygen saturations of > 98% (Pulse oximetry).
• Set ventilation parameters to maintain a PCO2 of approximately 35
mmHg.
• Circulation
• If the patient is hypotensive, establish euvolemia as soon as possible using
blood products, or isotonic fluids as needed
• Neurologic exams
• GCS score, pupillary light response, and focal neurological deficit
• Presence of drugs, alcohol, intoxicants, and other injuries
• Comatose motoric response by pinching trapezius muscles or with nail
bed or supraorbital ridge pressure for prognostic
• Doll’s eye (N.III), caloric testing with ice (N.VIII) and corneal response
ATLS 10th ed.
Secondary survey
• Perform serial examinations (GCS Diagnostic procedures Head CT scan
score, lateralizing signs, and pupillary • As soon as possible after hemodynamic normalization. Repeated
reaction) to detect neurological whenever there is a change in the patient’s clinical status,
deterioration as early as possible. routinely within 24 hours of injury for patients with subfrontal/
• A wellknown early sign of temporal temporal intraparenchymal contusions, patients receiving
lobe (uncal) herniation = dilation of anticoagulation therapy, patients older than 65 years, and
the pupil & loss of the pupillary patients who have an intracranial hemorrhage with a volume of
response to light. >10 mL.
• CT findings of significance scalp swelling & subgaleal
hematomas at the region of impact. Skull fractures often
apparent even on the soft-tissue windows (seen better with
bone windows).
• Crucial CT findings intracranial blood, contusions, shift of
midline structures (mass effect), and obliteration of the basal
cisterns
A shift of 5 mm or greater = indicates for surgery to evacuate the
blood clot or contusion causing the shift
ATLS 10th ed.
Medical Therapies • Hypertonic saline
• IV fluid Ringer’s lactate solution/normal saline. • To reduce elevated ICP. Concentrations = 3-
• Monitor serum sodium levels in patients with head 23.4%
injuries (prevent hyponatremia – associated with • Indication = hypotension
brain edema)
• Barbiturate
• Hyperventilation (only in moderation and for as limited • Effective in reducing ICP refractory
a period as possible) by reducing PaCO2 & causing
• Contraindication = hypotension and
cerebral vasoconstriction
hypovolemia
• Keep the PaCO2 at approximately 35 mmHg
(normal range 35-45 mmHg). • Anticonvulsant Can inhibit brain recovery, so
• Hyperventilation will lower ICP in a deteriorating they should be used only when absolutely
patient with expanding intracranial hematoma until necessary
doctors can perform emergent craniotomy. • Phenytoin and fosphenytoin mainly used
for acute phase (Dose : 1g IV < 50 mg/min,
• Mannitol 20% solution (20 g of mannitol per 100 ml maintenance dose = 100mg/8 hours)
of solution).
• Diazepam or lorazepam added until seizures
• To reduce elevated ICP stops
• Contraindication = hypotension
• Strong indication = dilated pupil, hemiparesis, or Surgical management
loss of consciousness • Necessary for scalp wounds, depressed skull
• Bolus mannitol (1g/kg) over 5 minutes fractures, intracranial mass lesions, and penetrating
ATLS 10 ed.
th brain injuries
You might also like
- Kraniotomi DekompresiDocument17 pagesKraniotomi DekompresianamselNo ratings yet
- ATLS - Head Trauma ImodifiedDocument39 pagesATLS - Head Trauma ImodifiedSammon TareenNo ratings yet
- School of Health and Allied Health Sciences Nursing Department Self-Directed Learning (Nur 146 - Clinical Area)Document3 pagesSchool of Health and Allied Health Sciences Nursing Department Self-Directed Learning (Nur 146 - Clinical Area)Milagros FloritaNo ratings yet
- Head Injury: Clasification of Traumatic Brain InjuriesDocument7 pagesHead Injury: Clasification of Traumatic Brain InjuriesElsa EvalynNo ratings yet
- Brain Injury Dr. Shema Dr. MuyimboDocument58 pagesBrain Injury Dr. Shema Dr. MuyimboTIMOTHY MUYIMBONo ratings yet
- Head Injury: From ATLS Chapter 6Document42 pagesHead Injury: From ATLS Chapter 6Elno TatipikalawanNo ratings yet
- Head Injury Management: Ahimbisibwe Alaphael Lecturer DR - JulietDocument33 pagesHead Injury Management: Ahimbisibwe Alaphael Lecturer DR - JulietNinaNo ratings yet
- DR - Roezwir SP.SDocument76 pagesDR - Roezwir SP.SSyifaAsriFauziahNo ratings yet
- Head Trauma: Dr. Andy Wijaya, SpemDocument20 pagesHead Trauma: Dr. Andy Wijaya, SpemThomas AlbertNo ratings yet
- Head Injury AnesDocument42 pagesHead Injury Aneskenbon kenbonNo ratings yet
- D. Intralipid 20%: A. Temazepam B. Lorazepam C. NaloxoneDocument122 pagesD. Intralipid 20%: A. Temazepam B. Lorazepam C. NaloxoneOstazNo ratings yet
- Head InjuryDocument50 pagesHead InjuryThiagarajah RaviNo ratings yet
- Traumatic Brain Injury PresentationDocument51 pagesTraumatic Brain Injury PresentationKah Sui Tan100% (2)
- Subdural Hematome: Oleh: Maha Satya Pembimbing: DR - Dr.Nyoman Golden, Spbs (K)Document55 pagesSubdural Hematome: Oleh: Maha Satya Pembimbing: DR - Dr.Nyoman Golden, Spbs (K)Maha Satya Dwi PalgunaNo ratings yet
- Head Trauma: Initial Assessment and ManagementDocument38 pagesHead Trauma: Initial Assessment and Managementi wayan dediyanaNo ratings yet
- Brain TraumaDocument32 pagesBrain Traumafrengki kobogauNo ratings yet
- Head Injury Outline of Management CDocument89 pagesHead Injury Outline of Management CPanna SahaNo ratings yet
- Traumatic Head InjuriesDocument50 pagesTraumatic Head InjuriesVasudha BuddyNo ratings yet
- Neurologic Function Cerebrovascular DisordersDocument15 pagesNeurologic Function Cerebrovascular DisordersBalilea, Derwin Stephen T.No ratings yet
- Anesthetic Management of Intracranial Aneurysms R-MasriDocument66 pagesAnesthetic Management of Intracranial Aneurysms R-MasriadheNo ratings yet
- Subarachnoid HemorrhageDocument24 pagesSubarachnoid HemorrhageIsaac MwangiNo ratings yet
- Anesthesia For Patients With Acute Traumatic Brain InjuryDocument51 pagesAnesthesia For Patients With Acute Traumatic Brain InjurymandeepNo ratings yet
- Taufan Arif, S.Kep., NS., M.KepDocument85 pagesTaufan Arif, S.Kep., NS., M.KepputriNo ratings yet
- Kuliah Head Injury MakasarDocument113 pagesKuliah Head Injury MakasarJerrod WilsonNo ratings yet
- Dr. Tommy SP - BS - Head Trauma Webinar Dr. TMYDocument30 pagesDr. Tommy SP - BS - Head Trauma Webinar Dr. TMYOctafiani Trikartika DarimanNo ratings yet
- Traumatic Brain Injury: General Overview: Handoyo PramusintoDocument59 pagesTraumatic Brain Injury: General Overview: Handoyo PramusintoYusfitaria AlvinaNo ratings yet
- 6.neurologic PathophysiologyDocument173 pages6.neurologic PathophysiologybekaluNo ratings yet
- Head InjuryDocument34 pagesHead Injuryrxmskdkd33No ratings yet
- Neurologic and Neurosurgical Emergencies For Nursing StudentsDocument39 pagesNeurologic and Neurosurgical Emergencies For Nursing StudentsDr Ganeshgouda MajigoudraNo ratings yet
- Stroke CMEDocument34 pagesStroke CMEKeren Karunya SingamNo ratings yet
- 2008 05 01-Bromley-Head TraumaDocument193 pages2008 05 01-Bromley-Head TraumahanimozaghiNo ratings yet
- Epidural Haematoma: DR - Karan R RawatDocument65 pagesEpidural Haematoma: DR - Karan R RawatSitha ChristineNo ratings yet
- Head Traumas: Anthony Safi Mediii Neurosurgery RotationDocument17 pagesHead Traumas: Anthony Safi Mediii Neurosurgery RotationAnthony safiNo ratings yet
- Head Injury 5Document68 pagesHead Injury 5drvishal bhattNo ratings yet
- Head TraumaDocument33 pagesHead Traumasteven andreanNo ratings yet
- eMRCS Truama 122 Questions PDFDocument39 pageseMRCS Truama 122 Questions PDFAbdesselam BerrehailNo ratings yet
- General Surgery Trauma (Head and Thorax)Document24 pagesGeneral Surgery Trauma (Head and Thorax)Noora AlmuailiNo ratings yet
- Cerebral EdemaDocument40 pagesCerebral EdemaMithun GorreNo ratings yet
- Head Injury: Tsegazeab Laeke, MD, FCS (ECSA) August 1,2018Document38 pagesHead Injury: Tsegazeab Laeke, MD, FCS (ECSA) August 1,2018Amanuel AyladoNo ratings yet
- Contusion CerebralDocument29 pagesContusion CerebralLeodanRiojasHuaman100% (1)
- Committee On Trauma PresentsDocument35 pagesCommittee On Trauma PresentsRetno Tri HaryatiNo ratings yet
- Head Trauma: George Ayoub - Med3Document23 pagesHead Trauma: George Ayoub - Med3Joe KhdeirNo ratings yet
- Traumatic Brain Injury (TBI)Document48 pagesTraumatic Brain Injury (TBI)Alaa OmarNo ratings yet
- Neuro EmergencyDocument53 pagesNeuro EmergencyHayatul AkmaLiaNo ratings yet
- Head Trauma: Khamim Thohari Rsud DR Muhammad Soewandhie SurabayaDocument33 pagesHead Trauma: Khamim Thohari Rsud DR Muhammad Soewandhie SurabayaJessica Alexandria WuNo ratings yet
- Acute Haemorrhagic Stroke: Clinical Practice ReviewDocument11 pagesAcute Haemorrhagic Stroke: Clinical Practice ReviewbAm coolNo ratings yet
- Brain InjuryDocument35 pagesBrain InjuryAkhil Adhithyan RamNo ratings yet
- Intra-Cranial Pressure (ICP), Regulation, Cerebral MetabolismDocument18 pagesIntra-Cranial Pressure (ICP), Regulation, Cerebral MetabolismPraveen RamasamyNo ratings yet
- Increased Icp NoesDocument3 pagesIncreased Icp NoesDarren Mae MosadaNo ratings yet
- NeurologyDocument65 pagesNeurologySam Angelo EstrellaNo ratings yet
- Sunkara DB Neurological DisordersDocument41 pagesSunkara DB Neurological DisordersAngela SaoNo ratings yet
- Thenan - Danial - AinaDocument33 pagesThenan - Danial - AinaThenan SankarNo ratings yet
- ATLS - Head Trauma ImodifiedDocument39 pagesATLS - Head Trauma ImodifiedSammon TareenNo ratings yet
- Stroke: Bruke B. (Bpharm, MSC Clinical Pharmacy, PHD in Cardio Therapy, Clinical Pharmacy) Wcu, EthiopiaDocument50 pagesStroke: Bruke B. (Bpharm, MSC Clinical Pharmacy, PHD in Cardio Therapy, Clinical Pharmacy) Wcu, EthiopiadawitNo ratings yet
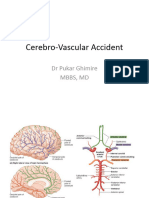
- Cerebro-Vascular Accident: DR Pukar Ghimire MBBS, MDDocument103 pagesCerebro-Vascular Accident: DR Pukar Ghimire MBBS, MDNaman MishraNo ratings yet
- Traumatic Brain Injury and Cerebral ResuscitationDocument56 pagesTraumatic Brain Injury and Cerebral ResuscitationsyahirNo ratings yet
- Head Trauma Brain InjuryDocument54 pagesHead Trauma Brain Injurymirzabb1No ratings yet
- M A N A G E M E NT OF H E A D I NJ UR Y & I NT R A CR A N I A L P RE SS UR EDocument19 pagesM A N A G E M E NT OF H E A D I NJ UR Y & I NT R A CR A N I A L P RE SS UR EmugihartadiNo ratings yet
- Head Trauma: Rika Mega Selfia 20184010019Document24 pagesHead Trauma: Rika Mega Selfia 20184010019rikaNo ratings yet
- Increased Intracranial PressureDocument48 pagesIncreased Intracranial PressureJulia Rae Delos SantosNo ratings yet
- Polimyalgia RematikDocument7 pagesPolimyalgia Rematiksalvaryn neNo ratings yet
- Iron Intoxication: Tintinalli's Emergency Medicine A Comprehensive Study Guide. 8th Edition. 2016Document7 pagesIron Intoxication: Tintinalli's Emergency Medicine A Comprehensive Study Guide. 8th Edition. 2016salvaryn neNo ratings yet
- Intussusception: Sign & SymptomsDocument2 pagesIntussusception: Sign & Symptomssalvaryn neNo ratings yet
- Acute Appendicitis: Imaging StudiesDocument2 pagesAcute Appendicitis: Imaging Studiessalvaryn neNo ratings yet
- Anatomi & Histologi GasterDocument24 pagesAnatomi & Histologi Gastersalvaryn neNo ratings yet
- Anorexia Nervosa Thesis StatementDocument6 pagesAnorexia Nervosa Thesis StatementPaperWritingServicesOnlineCanada100% (1)
- MysophobiaDocument3 pagesMysophobiaapi-492228211No ratings yet
- Weakness (Approach To Diagnosis) - Dr. TulmoDocument2 pagesWeakness (Approach To Diagnosis) - Dr. TulmoMonique BorresNo ratings yet
- Romina Caces. Leticia Cortez. Juan Fco. Gutierrez. Rocio Henríquez. Giancarlo Mayorga. Camila Nieto. Ramón SaldíasDocument5 pagesRomina Caces. Leticia Cortez. Juan Fco. Gutierrez. Rocio Henríquez. Giancarlo Mayorga. Camila Nieto. Ramón SaldíasCesia Belén BurgosNo ratings yet
- Sessions 14 Nur 1491Document9 pagesSessions 14 Nur 1491BegNo ratings yet
- Personality Disorders Lesson PlanDocument17 pagesPersonality Disorders Lesson Planapi-284104206No ratings yet
- Dissociative DisordersDocument29 pagesDissociative DisordersNoelle Grace Ulep BaromanNo ratings yet
- Personal View: Anita Thapar, Miriam Cooper, Michael Rutter FrcpsychDocument8 pagesPersonal View: Anita Thapar, Miriam Cooper, Michael Rutter FrcpsychRaul Morales VillegasNo ratings yet
- PTC Slides 2016Document290 pagesPTC Slides 2016graceduma100% (1)
- Organic Personality DisorderDocument2 pagesOrganic Personality DisorderDana Iclozan100% (1)
- Diabetes GestacionalDocument3 pagesDiabetes GestacionalCeiila GonzálezNo ratings yet
- Effects of The Neurodevelopmental Treatment NDT OnDocument9 pagesEffects of The Neurodevelopmental Treatment NDT OnIchsan PachruddinNo ratings yet
- Health Anxiety Information Sheet - 01-What Is Health AnxietyDocument1 pageHealth Anxiety Information Sheet - 01-What Is Health AnxietyCláudia AlmeidaNo ratings yet
- Ent OsceDocument15 pagesEnt OsceAntaraaNo ratings yet
- Guillain Barre ClassroomDocument14 pagesGuillain Barre ClassroomLalisaM ActivityNo ratings yet
- Kidney Treatment Guidelines For HyponatremiaDocument7 pagesKidney Treatment Guidelines For HyponatremialguerreroNo ratings yet
- DSM 5Document2 pagesDSM 5Alberto Preciado100% (1)
- Sick EnoughDocument49 pagesSick EnoughErendira SierraNo ratings yet
- Medical Surgical Nursing (Pentagon)Document2 pagesMedical Surgical Nursing (Pentagon)Hannah TollenoNo ratings yet
- Demographic Profile and Risk Factors of Stroke Patients in A Tertiary Care Centre of NepalDocument4 pagesDemographic Profile and Risk Factors of Stroke Patients in A Tertiary Care Centre of NepalInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- H&Y ScaleDocument17 pagesH&Y ScalezhansayaNo ratings yet
- Diabetic Striatopathy PosterDocument6 pagesDiabetic Striatopathy Posteradityamurugan1154No ratings yet
- Heart Failure Clinical Records DatasetDocument14 pagesHeart Failure Clinical Records Datasetpanca saputraNo ratings yet
- CH 145 Temper TantrumsDocument5 pagesCH 145 Temper Tantrumsroshen02No ratings yet
- Tatalaksana Primary Dan Secondary SurveyDocument26 pagesTatalaksana Primary Dan Secondary Surveyakun 31No ratings yet
- Autism: DefinitionDocument6 pagesAutism: DefinitionBallave SudiptaNo ratings yet
- Aspergers Syndrome Diagnosis and TreatmentDocument7 pagesAspergers Syndrome Diagnosis and TreatmentTilahun MogesNo ratings yet
- Penggunaan Insulin Pada Diabetes Tipe 2Document47 pagesPenggunaan Insulin Pada Diabetes Tipe 2pebbyfebrianNo ratings yet
- CHAPTER 16 - Schizophrenia 2Document15 pagesCHAPTER 16 - Schizophrenia 2RebeccaNo ratings yet