Professional Documents
Culture Documents
Digestive System
Uploaded by
Wakjira Gemeda0 ratings0% found this document useful (0 votes)
12 views73 pagesthe digestive tract, also called the gastrointestinal (GI) tract, Or alimentary canal
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentthe digestive tract, also called the gastrointestinal (GI) tract, Or alimentary canal
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
12 views73 pagesDigestive System
Uploaded by
Wakjira Gemedathe digestive tract, also called the gastrointestinal (GI) tract, Or alimentary canal
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 73
ANATOMY THE
DIGESTIVE SYSTEM W.G
The digestive system consisting of the
digestive tract and
accessory organs,
functions primarily to break down and absorb nutrients from food and to
eliminate wastes
The digestive system (alimentary system) consists of a muscular tube,
the digestive tract, also called the gastrointestinal (GI) tract, Or
alimentary canal, and
various accessory organs.
The digestive tract begins at the oral cavity (mouth).
It continues through the
opharynx (throat),
oesophagus,
ostomach,
osmall intestine, and
olarge intestine, which opens to the exterior at the anus.
Accessory digestive organs include
the teeth,
tongue, and
various glandular organs, such as the
salivary glands,
liver, and
pancreas, as well as the
gallbladder, which only has a secretory function.
LAYERS OF THE GI TRACT
The wall of the GI tract from the lower esophagus to the anal ca-
nal has the same basic, four-layered arrangement of tissues.
The four layers of the tract, from deep to superficial, are the
mucosa,
submucosa,
muscularis, and
serosa/adventitia
THE PERITONEUM
The peritoneum is a continuous, glistening, and slippery
transparent serous membrane. It lines the abdominopelvic
cavity and invests the viscera.
The peritoneum consists of two continuous layers:
the parietal peritoneum, which lines the internal surface of the
abdominopelvic wall, and
the visceral peritoneum, which invests viscera such as the
stomach and intestines.
Like the overlying skin, the peritoneum lining the interior of
the body wall is
sensitive to pressure, pain, heat and cold, and laceration.
Pain from the parietal peritoneum is generally well localized.
The visceral peritoneum is insensitive to touch, heat and cold,
and laceration; it is stimulated primarily
by stretching and chemical irritation.
The peritoneal cavityis within the abdominal cavity and
continues inferiorly into the pelvic cavity. It contains no organs but
contains a thin film of peritoneal fluid, which is composed of
water, electrolytes, and other substances derived from interstitial
fluid in adjacent tissues.
Peritoneal fluid lubricates the peritoneal
surfaces, enabling the viscera to move over each other without
friction, and allowing the movements of digestion.
NEURAL INNERVATION
OF THE GI TRACT
The gastrointestinal tract is regulated by an intrinsic set of nerves
known as the enteric nervous system and by an extrinsic set of
nerves that are part of the autonomic nervous system.
Enteric Nervous System
The neurons of the ENS are arranged into two plexuses:
The myenteric plexus and
The submucosal plexus
The myenteric plexus, or plexus of Auerbach,
is located between the longitudinal and circular smooth muscle
layers of the muscularis.
The submucosal plexus, or plexus of
Meissner is found within the submucosa.
The plexuses of the ENS consist of
motor neurons: controls GI tract motility (movement)
interneurons, and: interconnect the neurons of the myenteric and submucosal
plexuses.
sensory neurons: detect stimuli in the lumen of the GI tract.
chemoreceptors
mechanoreceptors
AUTONOMIC NERVOUS
SYSTEM
The vagus (X) nerves supply parasympathetic fibers to most parts of
the GI tract, with the exception of the last half of the large intestine,
which is supplied with parasympathetic fibers from the sacral spinal
cord.
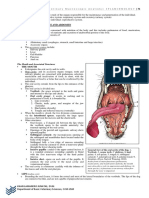
THE ORAL CAVITY
The oral cavity, which contains
the tongue,
teeth, and
Salivary glands,
functions in the ingestion an mechanical digestion of food.
is formed by
the cheeks,
hard and soft pal-ates, and
tongue
Buccinator muscles and connective tissue lie between the skin and
mucous membranes of the cheeks.
The lips or labia are fleshy folds surrounding the opening of the
mouth. They contain the orbicularis oris muscle and are covered
externally by skin and internally by a
mucous membrane.
The inner surface of each lip is attached to its
corresponding gum by a midline fold of mucous membrane called
the labial frenulum.
Hanging from the free border of the soft palate is a fingerlike
muscular structure called the uvula.
During swallowing, the soft palate and uvula are drawn superiorly,
closing off the nasopharynx and preventing swallowed
foods and liquids from entering the nasal cavity.
The functions of the oral cavity include
(1) sensory analysis of food before swallowing;
(2) mechanical digestion through the actions of the
teeth, tongue, and palatal surfaces;
(3) lubrication by mixing with mucus and saliva; and
(4) limited chemical digestion of carbohydrates and lipids.
The oral cavity is lined by the oral mucosa, which has
a stratified squamous epithelium
The epithelial lining of the cheeks, lips, and inferior surface of the tongue
is relatively thin
and nonkeratinized.
Nutrients are not absorbed in the oral cavity, but the mucosa inferior to
the tongue is thin enough and vascular enough to permit the rapid
absorption of lipid-soluble drugs
THE TONGUE
The tongue has four primary functions
(1)mechanical digestion by compression, abrasion, and distortion;
(2) manipulation to assist in chewing and to prepare food for swallowing;
(3) sensory analysis by touch, temperature, and
taste receptors; and
(4) secretion of mucins and the enzyme lingual lipase.
(5) articulation (forming words during speaking)
We can divide the tongue into
Apex,
an anterior body, or oral portion, and
a posterior root, or pharyngeal portion.
The superior surface, or dorsum, of the body contains a forest of fine
projections, the lingual papillae.
Along the inferior midline is the frenulum of tongue, or lingual
frenulum.
The tongue contains two groups of skeletal muscles.
The large extrinsic tongue muscles perform all gross movements of the tongue.
genioglossus,
hyoglossus,
styloglossus, and
palatoglossus
The smaller intrinsic tongue muscles change the shape of the tongue and assist the
extrinsic muscles during precise movements, as in speech.
The superior and inferior longitudinal, transverse, and vertical muscles are
confined to the tongue.
Both intrinsic and extrinsic tongue muscles are under the control of the hypoglossal
cranial nerves (XII).
All muscles of the tongue, except the palatoglossus, receive
motor innervation from CN XII, the hypoglossal nerve.
Palatoglossus is a palatine muscle supplied by the
pharyngeal plexus.
For general sensation (touch and temperature), the mucosa of the
anterior two thirds of the tongue is supplied by the lingual nerve, a
branch of CN V3.
For special sensation (taste), this part of the tongue, except for the
vallate papillae, is supplied the chorda tympani nerve, a branch of CN
VII.
The mucosa of the posterior third of the tongue and the vallate papillae
are supplied by the lingual branch of the glossopharyngeal nerve(CN
IX) for both general and special sensation
ANATOMY OF A TOOTH
The bulk of each tooth consists of a mineralized matrix similar to that
of bone.
This material, called dentin, differs from bone
in that it does not contain cells
Pulp cavity: an interior chamber.
The pulp cavity receives blood vessels and
nerves through the root canal.
Blood vessels and nerves enter the root canal through an opening
called the apical foramen to
supply the pulp cavity.
A layer of cement covers the dentin of the root.
Cement protects and firmly anchors the
periodontal ligament.
The neck of the tooth marks the boundary between the root and the
crown, the exposed portion of the tooth that projects beyond the soft
tissue of the gingiva.
A layer of enamel covers the dentin of the crown.
Enamel, which contains calcium phosphate in a crystalline form, is the
hardest biologically manufactured substance.
TYPES OF TEETH
1. Incisor teeth are blade-shaped teeth located at
the front of the mouth.
Incisors are useful for clipping or cutting, as when you nip off the tip of a
carrot stick.
These teeth have a single root.
2.Canine teeth, or cuspid, are conical
with a single, pointed cusp.
Also known as the “eyeteeth,” because they lie directly under the eye, the
canines are
used for tearing or slashing.
Canines have a single root.
3. Premolar teeth, or bicuspids, have flattened
crowns with two prominent rounded cusps.
They crush, mash, and grind. Bicuspids have one or two roots.
4. Molar teeth have very large, flattened crowns with four to five
prominent rounded cusps adapted for crushing and grinding.
You can usually shift a tough nut to your premolars and molars for
successful crunching. Molars in
the upper jaw typically have three roots while those in the lower jaw
usually have two roots.
SETS OF TEETH
The teeth are collectively called the dentition.
Two such dentitions form during development:
deciduous and
permanent.
The first to appear are the deciduous teeth (deciduus, falling off).
Deciduous teeth are also called primary
teeth, milk teeth, or baby teeth. Most children have 20 deciduous teeth
On each side of the upper or lower jaw,
the deciduous teeth consist of two incisors, one canine, and a pair of
deciduous molars for a total of 20 teeth.
These teeth are later replaced by the permanent teeth of the larger adult
jaws.
The deciduous teeth either fall out or are pushed aside by the eruption,
or emergence, of the permanent teeth.
THE SALIVARY GLANDS
Three major pairs of salivary glands secrete into the oral cavity.
These are:
oThe large parotid glands
oThe sublingual glands
oThe submandibular glands
Minor salivary glands include some 800–1000 submucosal
glands in the oral cavity.
The mucous membrane of the mouth and tongue contains
many small salivary glands that open directly, or indirectly via
short ducts, to the oral cavity.
These glands include labial, buccal,
and palatal glands in the lips, cheeks, and palate, respectively,
and lingual glandsin the tongue, all of which make a small contribution to saliva.
THE PHARYNX
The pharynx, or throat, is an anatomical space that
serves as a common passageway for
solid food,
liquid, and
air.
Food normally passes through parts of the pharynx on its way to the
esophagus.
The esophagus is a hollow muscular tube
that then conveys these ingested materials to the stomach.
Regions of the pharynx:
nasopharynx,
oropharynx, and
laryngopharynx
THE ESOPHAGUS
The esophagus is approximately 25 cm in length and
has a diameter of about 2 cm at its widest point.
The esophagus begins posterior to the cricoid cartilage, at the
level of vertebra C6. It is narrowest at this point.
The esophagus descends toward the thoracic cavity posterior to the
trachea.
The esophagus empties into the stomach anterior to vertebra T7.
the esophagus normally has three constrictions where adjacent structures produce
impressions:
• Cervical constriction (upper esophageal sphincter):
at its beginning at the pharyngo esophageal junction,
approximately 15 cm from the incisor teeth; caused by the
cricopharyngeus muscle.
• Thoracic (broncho-aortic) constriction:a compound
constriction where it is first crossed by the arch of the
aorta, 22.5 cm from the incisor teeth, and then where it
is crossed by the left main bronchus, 27.5 cm from the
THE STOMACH
The stomach has the shape of an expanded J
A short lesser curvature forms the medial surface of the organ, and a
long greater curvature forms the lateral surface.
The stomach typically extends between the levels of
vertebrae T7 and L3.
Four parts:
The Cardia: is the smallest region of the stomach.
The fundus is the region of the stomach that
is superior to the junction between the stomach and the esophagus.
The Body is the area of the stomach between the fundus and the curve of
the J.
The pyloric part (pyloros, gatekeeper) forms the portion of the stomach
between the body and the duodenum.
It is divided into a pyloric antrum, which is
connected to the body, a pyloric canal, which empties
into the duodenum, and the pylorus, which
is the muscular tissue surrounding the pyloric orifice
(stomach outlet).
BLOOD SUPPLY
The celiac trunk
Left Gastric
The gastroduodenal artery
The right gastric artery
RGEA (lesser curvature)
LGEA (greater curvature
THE PANCREAS
The pancreas is an elongate, pinkish-gray organ about 15 cm long and
weighing about 80 g.
It has the following:
The head:lies within the loop formed by
the duodenum as it leaves the pyloric part.
The body:extends toward the spleen.
The tail:is short and bluntly rounded.
The pancreas is retroperitoneal and is
firmly bound to the posterior wall of the abdominal cavity.
Arterial blood reaches the pancreas by way of
branches of the splenic,
superior mesenteric, and
common hepatic arteries.
The pancreatic arteries and pancreaticoduodenal arteries are the major
branches from these vessels.
The splenic vein and its branches drain the pancreas.
The large pancreatic duct delivers the secretions of the pancreas to the
duodenum.
In 3–10 percent of the population,
a small accessory pancreatic duct branches from the pancreatic duct.
When present, the accessory pancreatic duct usually empties into the
duodenum independently, outside the duodenal ampulla.
THE LIVER
The liver is the largest visceral organ, a firm, reddish-brown organ
weighing about 1.5 kg.
Most of its mass lies in the right hypochondriac and epigastric regions,
but it may extend into the
left hypochondriac and umbilical regions as well.
The versatile liver performs essential metabolic and synthetic
functions.
On the anterior surface, the falciform ligament marks the division
between the organ’s left and right lobes.
On the posterior surface of the liver, the impression left by the inferior
vena cava marks the division between the right lobe and the small
caudate
Inferior to the caudate lobe lies the quadrate lobe, sandwiched
between the left lobe and the gallbladder.
Afferent blood vessels
and other structures reach the liver by traveling within the
connective tissue of the lesser omentum.
They converge at a region called the porta hepatis (“doorway to the
liver”).
Nearly one-third of the blood supply to the liver is arterial blood
from the hepatic artery proper.
The rest is venous blood from the hepatic portal vein.
THE GALLBLADDER
The gallbladder is a hollow, pear-shaped organ that stores and
concentrates bile prior to its secretion into the small intestine.
This muscular sac is located in a fossa, or recess, in the posterior
surface of the liver’s right lobe
The gallbladder is divided into three regions:
(1) the fundus,
(2) the body, and
(3) the neck.
The cystic duct extends from
the gallbladder to the point where it unites with the common hepatic
duct to form the bile duct. At the duodenum,
the bile duct meets the pancreatic duct before emptying into
a chamber called the duodenal ampulla.
THE SMALL INTESTINE
The small intestine primarily functions in the chemical digestion and
absorption of nutrients.
The small intestine, also known as the small bowel, averages 6 m (19.7
ft) in length (range: 4.5–7.5 m; 14.8–24.6 ft). Its diameter ranges from 4
cm at the stomach to about 2.5 cm
at the junction with the large intestine.
The primary blood vessels involved are branches of
the superior mesenteric artery and the superior mesenteric vein.
THE LARGE INTESTINE
The horseshoe-shaped large intestine begins at the end of the ileum and
ends at the anus.
The large intestine lies inferior to the stomach and liver and almost
completely frames the small
intestine.
The large intestine stores digestive wastes and reabsorbs water.
The large intestine, also known as the large bowel, has an average length
of about 1.5 meters (4.9 ft) and a width of 7.5 cm.
divide it into three segments:
(1) the pouchlike cecum, the first portion of the large intestine;
(2) the colon, the largest portion; and
(3) the rectum, the last 15 cm of the large
intestine and the end of the digestive tract
THE CECUM AND APPENDIX
Material arriving from the ileum first enters an expanded pouch called
the cecum.
The ileum attaches to the medial surface of
the cecum and opens into the cecum at the ileocecal valve.
The cecum collects and stores materials from
the ileum and begins the process of compaction.
The slender, hollow appendix, or vermiform appendix
(vermis, worm), is attached to the posteromedial surface of
the cecum.
The appendix is normally about 9 cm long, but its size and shape are
quite variable.
The primary function of the appendix is as an organ of the lymphatic
system.
THE COLON
Subdivided the colon into four segments:
the ascending colon,
transverse colon,
descending colon, and
Sigmoid colon
The colon, and indeed the entire large intestine, receives blood from
branches of the superior mesenteric and inferior mesenteric arteries.
The superior mesenteric and inferior
mesenteric veins collect venous blood from the large intestine.
THE RECTUM
The rectum forms the last 15 cm of the digestive tract.
It is an expandable organ for the temporary storage of feces.
The last portion of the rectum, the anal canal, contains
small longitudinal folds called anal columns.
The distal margins of these columns are joined by transverse folds that
mark the boundary between the columnar epithelium of the proximal
rectum and a stratified squamous epithelium like that in the oral
cavity.
THANK YOU
You might also like
- A Guide for the Dissection of the Dogfish (Squalus Acanthias)From EverandA Guide for the Dissection of the Dogfish (Squalus Acanthias)No ratings yet
- Digestive SystemDocument9 pagesDigestive System79ctq9xpf7No ratings yet
- A Simple Guide to the Ear and Its Disorders, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to the Ear and Its Disorders, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Digestive SystemDocument67 pagesDigestive SystemShacquille Suelto Bautista0% (1)
- RT Basics Digestive SystemDocument88 pagesRT Basics Digestive Systemmaricar paracadNo ratings yet
- Problem 1Document111 pagesProblem 1Agustina CynthiaNo ratings yet
- 06 Digestive SystemDocument101 pages06 Digestive SystemcelynjasminegNo ratings yet
- Histologi Saluran CernaDocument57 pagesHistologi Saluran CernaAdinda TobingNo ratings yet
- EssaysDocument176 pagesEssaysppdzssx7ghNo ratings yet
- Anatomy of The Upper DigestionDocument16 pagesAnatomy of The Upper DigestionNabilla MahyendaNo ratings yet
- Mammalian System-01 (Digestive System)Document35 pagesMammalian System-01 (Digestive System)Saumya99No ratings yet
- Digestive SystemDocument73 pagesDigestive Systemsnp88No ratings yet
- Anatomy of Organs of The Digestive System PDFDocument6 pagesAnatomy of Organs of The Digestive System PDFMJ Garayan - ItableNo ratings yet
- Chapter XI DigestiveDocument19 pagesChapter XI DigestiveTitoMacoyTVNo ratings yet
- The MouthDocument16 pagesThe MouthNiño GarciaNo ratings yet
- Module 5 Anatomy I Splanchnology 1Document17 pagesModule 5 Anatomy I Splanchnology 1neannaNo ratings yet
- Digestive SystemDocument177 pagesDigestive Systemarham.yousafzaiNo ratings yet
- III. Anatomy and Physiology of the Digestive SystemDocument18 pagesIII. Anatomy and Physiology of the Digestive SystemJoanna_Edna_C__6752No ratings yet
- Lecture 12Document7 pagesLecture 12rahaf alshoumaryNo ratings yet
- Gastrointestinal System ExplainedDocument10 pagesGastrointestinal System ExplainedOdi DavidNo ratings yet
- Tongue and Its Role in Pros Tho Don TicsDocument100 pagesTongue and Its Role in Pros Tho Don TicsDr Mohit Dhawan100% (18)
- Digestive System.: Nur112: Anatomy and Physiology ISU Echague - College of NursingDocument9 pagesDigestive System.: Nur112: Anatomy and Physiology ISU Echague - College of NursingWai KikiNo ratings yet
- Tongue I LastDocument30 pagesTongue I LastEmuyeNo ratings yet
- Histologi Saluran CernaDocument57 pagesHistologi Saluran CernaAdinda TobingNo ratings yet
- Digestive SystemDocument106 pagesDigestive SystemUnboxthings 9No ratings yet
- Alimentary Canal of HumanDocument37 pagesAlimentary Canal of Humanمحمد العراقيNo ratings yet
- Digestive SystemDocument44 pagesDigestive SystemMekdelawit AyeleNo ratings yet
- OesophagusDocument21 pagesOesophagusparashakthi PRNo ratings yet
- Oral CavityDocument19 pagesOral CavityProy DCNo ratings yet
- Exercise7 (Histo) Digestive System EditedDocument8 pagesExercise7 (Histo) Digestive System EditedChristi Lorraine LayogNo ratings yet
- Human Digestive SystemDocument4 pagesHuman Digestive SystemAllen mugabeNo ratings yet
- Digestive System of Rana TigrinaDocument3 pagesDigestive System of Rana TigrinaAditi KoiralaNo ratings yet
- Part Ii Splanchnology Chapter 1 Introduction: Alimentary System Respiratory System Urinary System Genital SystemDocument49 pagesPart Ii Splanchnology Chapter 1 Introduction: Alimentary System Respiratory System Urinary System Genital Systemsomebody_maNo ratings yet
- Lecture 44 - Masticatory ApparatusDocument6 pagesLecture 44 - Masticatory ApparatusleahbayNo ratings yet
- Digestive SystemDocument162 pagesDigestive SystemSadhu PriyankaNo ratings yet
- Digestive System (Final)Document164 pagesDigestive System (Final)aubrey alcantaraNo ratings yet
- Digestive SYSTEMDocument53 pagesDigestive SYSTEMPrincess AnnNo ratings yet
- Dental Anatomy Guide for StudentsDocument30 pagesDental Anatomy Guide for StudentsдашаNo ratings yet
- Human Digestive System, The System Used in TheDocument10 pagesHuman Digestive System, The System Used in Theعلي رسن رداد حمد ANo ratings yet
- Digestive SystemDocument121 pagesDigestive SystemdearnibNo ratings yet
- TongueDocument162 pagesTongueDevendra ChhonkarNo ratings yet
- Digestive System I The Oral CavityDocument9 pagesDigestive System I The Oral CavitySUTHANNo ratings yet
- Human Anatomy The Gastrointestinal TractDocument53 pagesHuman Anatomy The Gastrointestinal TractGadzikaNo ratings yet
- Nutrition in AnimalsDocument31 pagesNutrition in Animalsnihalbolla2023No ratings yet
- Kuliah DNMDocument30 pagesKuliah DNMpunthadewaNo ratings yet
- Digestive System Explained: A Guide to the Organs and ProcessesDocument78 pagesDigestive System Explained: A Guide to the Organs and ProcessesJasmine Nicole OsallaNo ratings yet
- Physiology: Anatomy of The Digestive System IntroductionDocument10 pagesPhysiology: Anatomy of The Digestive System IntroductionkyirlessnessNo ratings yet
- Pemicu 1 GI: Mustika Rukmana 405130182 Kel 1Document69 pagesPemicu 1 GI: Mustika Rukmana 405130182 Kel 1tikaNo ratings yet
- Midterm Examination-BiochemDocument10 pagesMidterm Examination-BiochemRhizel Marie Cauilan FariñasNo ratings yet
- Anatomy of the Oral Cavity and its StructuresDocument5 pagesAnatomy of the Oral Cavity and its StructuresSimina TanaseNo ratings yet
- PRACTICA FINAL DE INGLE. DIGESTIVE SYSTEM. AnaDocument18 pagesPRACTICA FINAL DE INGLE. DIGESTIVE SYSTEM. AnaChantal PantaleonNo ratings yet
- AzmizDocument174 pagesAzmizEthio Dangote TubeNo ratings yet
- Assignment Structure of Oral CavityDocument4 pagesAssignment Structure of Oral CavityNarjis BatoolNo ratings yet
- @ Histol DigestiveDocument65 pages@ Histol DigestiveAyele AsefaNo ratings yet
- The Digestive SystemDocument41 pagesThe Digestive Systemkrmgxc8p4fNo ratings yet
- Millan, Shaina Marie B. 12-04-2018 BSN-103 Ms. Riza MagsinoDocument3 pagesMillan, Shaina Marie B. 12-04-2018 BSN-103 Ms. Riza MagsinoShaina MillanNo ratings yet
- Gastrointestinal ProblemsDocument79 pagesGastrointestinal ProblemsJessica G. SalimNo ratings yet
- Digestive System (Alimentary Canal + Digestive Glands + Digestive Process)Document26 pagesDigestive System (Alimentary Canal + Digestive Glands + Digestive Process)Shuvanjan Dahal100% (1)
- Teeth, Tongue and Salivary GlandsDocument12 pagesTeeth, Tongue and Salivary GlandsGideon WillieNo ratings yet
- Pemicu 1 Blok GIT: Theffany 405120198 Fakultas Kedokteran Universitas TarumanagaraDocument99 pagesPemicu 1 Blok GIT: Theffany 405120198 Fakultas Kedokteran Universitas TarumanagaraTheffany KasiranNo ratings yet
- Zoonotic DiseasesDocument96 pagesZoonotic DiseasesWakjira GemedaNo ratings yet
- Human NutritionDocument57 pagesHuman NutritionWakjira GemedaNo ratings yet
- Nutritional SurveillanceDocument20 pagesNutritional SurveillanceWakjira GemedaNo ratings yet
- Amino AcidsDocument32 pagesAmino AcidsWakjira GemedaNo ratings yet
- TextDocument17 pagesTextnaser zoabiNo ratings yet
- Equity ValuationDocument18 pagesEquity ValuationAbhishek NagpalNo ratings yet
- Plant Toxicology, Fourth Edition (Books in Soils, Plants, and The Environment) PDFDocument664 pagesPlant Toxicology, Fourth Edition (Books in Soils, Plants, and The Environment) PDFFahad JavedNo ratings yet
- Sanitas-Health Coach Quick Start GuideDocument26 pagesSanitas-Health Coach Quick Start GuideGabriel MuresanuNo ratings yet
- Resumen en Ingles Del Diario Ana Frank Chisaguano EmilyDocument16 pagesResumen en Ingles Del Diario Ana Frank Chisaguano EmilyChisaguano EmilyNo ratings yet
- 3d Printing Thesis StatementDocument5 pages3d Printing Thesis Statementoabfziiig100% (2)
- Bar Code Label Requirements, Compatibility, and UsageDocument22 pagesBar Code Label Requirements, Compatibility, and Usagelarrylegend33No ratings yet
- Tubo Optiflux 2000 - Manual PDFDocument48 pagesTubo Optiflux 2000 - Manual PDFRonaldo Damasceno EmerichNo ratings yet
- Probability As A General Concept Can Be Defined As The Chance of An Event OccurDocument14 pagesProbability As A General Concept Can Be Defined As The Chance of An Event OccurMuhammad Adnan KhalidNo ratings yet
- Conclusion FdiDocument2 pagesConclusion FdiYo PaisaNo ratings yet
- Epidemiology and Etiology of Peptic Ulcer DiseaseDocument5 pagesEpidemiology and Etiology of Peptic Ulcer DiseaseDeepali Mahajan ChaudhariNo ratings yet
- Manual Liebert PSADocument12 pagesManual Liebert PSAMatthew CannonNo ratings yet
- B. Inggris Kels IXDocument4 pagesB. Inggris Kels IXANHAS ADVERTISINGNo ratings yet
- Smell and Taste DisordersDocument8 pagesSmell and Taste DisordersAymn MohamedNo ratings yet
- Rear Axle ShaftsDocument4 pagesRear Axle ShaftsMaria AparecidaNo ratings yet
- Rui Zeng (Eds.) - Graphics-Sequenced Interpretation of ECG-Springer Singapore (2016) PDFDocument173 pagesRui Zeng (Eds.) - Graphics-Sequenced Interpretation of ECG-Springer Singapore (2016) PDFJulianNathanaelNo ratings yet
- Adjectives AllDocument35 pagesAdjectives AllJOHN SEBASTIAN PARDO LARANo ratings yet
- Vibrations and Waves MP205 Assignment 6 SolutionsDocument2 pagesVibrations and Waves MP205 Assignment 6 SolutionsRitesh GhodraoNo ratings yet
- Capacitive Touch Sensing, MSP430™ Slider and Wheel Tuning GuideDocument18 pagesCapacitive Touch Sensing, MSP430™ Slider and Wheel Tuning GuideFábio Carvalho FurtadoNo ratings yet
- Welcome To Primary 1!Document48 pagesWelcome To Primary 1!Zoe WangNo ratings yet
- LP in ArtsDocument6 pagesLP in ArtsBilindaNo ratings yet
- PublicLifeUrbanJustice Gehl 2016-1Document119 pagesPublicLifeUrbanJustice Gehl 2016-1bronsteijnNo ratings yet
- Schneider Legacy Products - 16066Document2 pagesSchneider Legacy Products - 16066tomcosgrove444No ratings yet
- Process Flow ChartDocument4 pagesProcess Flow Chartchacko chiramalNo ratings yet
- Level 2 Repair: 7-1. Components On The Rear CaseDocument8 pagesLevel 2 Repair: 7-1. Components On The Rear CaseNguyễn Duy LinhNo ratings yet
- 2020 - (Sankaran) - Data Analytics in Reservoir EngineeringDocument107 pages2020 - (Sankaran) - Data Analytics in Reservoir EngineeringPedro100% (1)
- Differences Between Circuit Switching and Packet SwitchingDocument7 pagesDifferences Between Circuit Switching and Packet Switchingdebs icapsNo ratings yet
- Experiment 7 & 11: Presented By: Group 4Document55 pagesExperiment 7 & 11: Presented By: Group 4Julliane JuanNo ratings yet
- Crux v20n04 AprDocument35 pagesCrux v20n04 AprMauricioNo ratings yet
- PH103 Section U Recap NotesDocument54 pagesPH103 Section U Recap NotesLuka MegurineNo ratings yet