Professional Documents
Culture Documents
BM TTG Kista
Uploaded by
Debora Gultom0 ratings0% found this document useful (0 votes)
7 views28 pagesOriginal Title
ppt BM ttg kista
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
7 views28 pagesBM TTG Kista
Uploaded by
Debora GultomCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 28
Complete Healing of a Large Cystic Lesion
Following Root Canal Treatment with
Concurrent
Surgical Drainage: A Case Report with 14-Year
Follow-Up
Yong-Sik Cho, DDS,* and Il-Young Jung, DDS, MSD, PhD
An extensive cystic lesion can be managed conservatively.
This case report described a case that was successfully
treated by a nonsurgical root canal treatment
using high-concentration NaOCl with lengthy contact
time as endodontic irrigant and concurrent
surgical drainage.
Case Report
• A 49-year-old woman was referred for the evaluation of a
large lesion in the anterior maxilla. The patient’s prior
medical history was noncontributory
Clinical Examination
• slight mucosal swelling in the center of the hard palate
• The swelling was fluctuant but exhibited no tenderness on palpation
• The labial vestibule also exhibited no tenderness on palpation.
• Teeth #8 and #9 were splinted with porcelain-fused-to-metal (PFM)
crowns, which had been placed 20 years prior due to proximal caries
Radiography
• Panoramic radiography revealed • intraoral periapical radiographs
an extensive radiolucent area demonstrated that the lesion
extending from tooth #6 to #12 appeared to originate from
tooth #9
• Teeth #8, #9, and #10 were diagnosed as pulpal necrosis with
asymptomatic apical periodontitis.
• The patient was scheduled for root canal treatment.
• Because of the extensive size and suspected fluid-filled cystic nature
of the lesion, simultaneous surgical drainage was selected to reduce
the size of the lesion immediately, rather than serving as a treatment
alternative.
• because the lesion was unusual, the diagnoses had to be confirmed
by biopsy as soon as possible in case of malignancy.
• The patient returned 18 days later, complaining of sudden pain and
swelling in the palate.
• The teeth and labial vestibule mucosa did not show any changes since
the prior visit, but the palate exhibited severe bulging and the left
nostril mucosa was swollen
Oral penicillin and acetaminophen were prescribed for 3 days to relieve
acute symptoms, and a skull computerized tomographic (CT) scan was
performed.
• CT imaging confirmed that the • Axial CT images demonstrated
inflammatory lesion had severe bony erosion of both labial
extended to nasal chambers and palatal walls of the lesion
with distortion of airways. (“through-and-through lesion”).
• After 2 days, acute symptoms disappeared, and the patient was
referred to the Department of Oral and Maxillofacial Surgery for the
surgical procedure.
• After infiltration anesthesia, an • After lavage with sterile saline, a
approximately 1.0-cm horizontal incision was
made between the root eminences of teeth #10-Fr silicone Foley catheter
#9 and #10. drain with radiopaque line
• Because the labial bone plate was thinned, insertion was cut to a length of
aspiration of the cystic fluid and generation 2.3 cm and inserted to the depth
of an osseous hole for the drainage tube was
easily performed with a small, lowspeed, of the cystic cavity
round bur.
• A small section of cystic lining was harvested
for histological analysis.
• On entry into the cystic cavity, the typical
strawcolored fluid was discharged from the
lesion.
• Sutures were placed through the • At 1 week postoperatively, the
drain itself, as well as through patient reported no pain, and
mucosa to stabilize it during histological analysis confirmed
initial healing. no signs of malignancy.
• Although there was no active
fluid discharge, cystic fluid was
observed when the palate
mucosa was pressed.
• Without anesthesia, an access cavity was • Cystic fluid did not exit the root
constructed under rubber dam isolation on
teeth #8, #9, and #10. No teeth exhibited canals, although apical patencies
sensitivity to the procedure; tooth #9 emitted were obtained by using #15 K-
a slight foul odor.
files. The canals were dried and
• After coronal flaring with Gates Glidden drills,
the working length was established and initial
access cavities were sealed with
shaping and cleaning of root canals were temporary fillings.
performed by H-files and 5.25% sodium
hypochlorite (NaOCl) solution. • No intracanal medication was
applied.
• One week later, the initial drain was exchanged with a surgical
drainage stent, which was fabricated with a small acrylic plate and a
silicone Foley catheter of similar size. The patient was instructed to
irrigate through the lumen of the stent daily with saline
• An occlusal radiograph was taken to check the • The application time of 5.25%
full extent of the lesion.
NaOCl was a minimum of 30
• The root canals of the teeth were enlarged,
stepped-back in increment of 0.5 mm, and a
minutes, including irrigation
final rinse with 5.25% NaOCl was performed during instrumentation and the
after removal of the smear layer with 2- final rinse; periodic irrigant
minute irrigation of Tublicid Plus.
changes were performed at 5-
minute intervals, accompanied by
recapitulation and patency filing.
• Apical patencies were maintained
with #15 K-files throughout the
procedure.
• No interappointment intracanal calcium hydroxide (Ca[OH]2) dressing or passive
ultrasonic irrigation was used during the procedure.
• Because complete drying of the canals was achieved without difficulty, root
canals were obturated with lateral condensation of gutta-percha and Sealapex
sealer.
• After 1 week, the patient was asymptomatic and permanent restorations were
placed. Discharge of cystic fluid was observed through the stent on pressure to
the palate.
• At the next appointment, 1 week later (4 weeks after drain insertion),
the patient stated that she had been unable to reinsert the stent 4
days prior, and that the opening on the mucosa had healed.
• The patient was recalled at 6-month intervals, and radiographs taken
after 2 years demonstrated that marked bony healing had occurred,
along with periapical repair of teeth #8 and #10.
• The patient returned for • Periapical radiographs
examination at 9 years and 7 demonstrated complete
months after the initiation of periapical healing on teeth #8,
root canal treatment. She #9, and #10.
reported nothing remarkable on
the involved teeth since the
previous visit.
• A PFM crown had been placed
on tooth #10 for an unspecified
reason
• Cone-beam CT confirmed that complete • When the PFM crowns were removed,
healing had occurred; however, the lateral coronal dentin was found to be severely
lesion of tooth #8 had slightly enlarged. decayed.
• The patient desired to replace her 30-year-old • Because of the coronal leakage, possible
PFM crowns on teeth #8 and #9 for esthetic reinfection of the root canals was suspected,
reasons. and nonsurgical retreatment was completed
on both teeth.
• On root canal fillings after gutta-percha removal and
chemomechanical preparations, an epoxy resin-based sealer was used
as a root canal.
• Fourteen years after the initial root canal treatment and 3 years after
retreatment, a periapical radiograph revealed that complete healing
had occurred around the periapical areas of teeth #8, #9, and #10.
• The patient was advised to visit for routine periodic recall check-up at
1-year intervals.
Discussion
• Here, we describe the complete healing of a maxillary cyst-like
periapical lesion, including a particularly extensive main lesion and a
lateral lesion, following a conservative treatment approach. Debate
continues regarding the treatment of large periapical lesions by
conservative or surgical means.
• Radiographic lesion size has been suggested as the parameter most
strongly correlated with histological diagnosis of a periapical cyst.
• Some studies have suggested that apical true cysts are unlikely to be
resolved without surgical removal, because they are independent of
the root canal system.
• These studies have focused on cystic epithelial cells or cyst “cavities,”
which are considered key factors in long-term healing.
• However, the fate and nature of a cyst is determined by connective tissue
surrounding its epithelial lining, which is connected to the apical root
surface.
• On the basis of a combination of many factors involving epithelial-
stromal interaction, the cyst will disappear of its own accord, along with
its surrounding pathologic connective tissue, which will disappear after
termination of the supply of inflammatory sources originating from the
root canal system; this occurs as a result of thorough endodontic therapy.
• Intracystic fluid pressure is thought to be involved in odontogenic cyst
growth.
• Therefore, the decompression technique may be effective in reducing
the size of cystic lesions. Reducing the pressure by surgical drainage
might play an important role in periapical healing.
• Decompression by surgical drainage may just accelerate the wound
healing by enabling prompt discharge of proinflammatory cytokines,
inflammatory mediators, necrotic debris, and irritants in cystic lesions.
• From this point of view, the need for long-term use of surgical
drainage might not be supported.
• Some case reports have revealed that root canals could not be dried
because of cystic fluid weeping or pulsating exudate from apical openings
during root canal treatment of cystic lesions.
• In particular, this situation resulted in the application of long-term Ca(OH)2
intracanal dressings, which might induce unwanted root dentin weakening
and an unpredictably prolonged treatment span.
• Another benefit of concurrent surgical drainage procedure in this case,
which ensured free discharge of cystic fluid, was the prevention of cystic
fluid weeping into root canals.
• As a result, the drying of root canals for root canal obturation was achieved
without any difficulty.
• “Complete healing” of periradicular lesions of endodontic origin could
be ensured only after cessation of the influx of inflammatory sources
from root canals.
• “Cleaning and shaping” of root canals is composed of 3 aspects:
mechanical, chemical, and “the aspect of time,” which refers to the
duration of NaOCl contact in root canals as a chemical disinfectant.
• The use of high concentration NaOCl with lengthy contact time was
reported for successful treatment of infected root canals.
• Although it did not have an experimental basis at that time, later studies
revealed that prolonged contact time with high-concentration NaOCl was
necessary to eliminate bacterial biofilms and suppress bacterial regrowth.
• Interestingly, these studies found that low-concentration NaOCl was
ineffective in the total elimination of bacterial biofilms and in bacterial
killing, even with prolonged contact time; this may be due to the
inhibitory effects of dentin on NaOCl and the survival of bacteria within
dentinal tubules.
• Furthermore, the depth of NaOCl penetration into dentinal tubules after
smear layer removal also exhibits a time-dependent relationship.
• In addition to meticulous chemomechanical root canal cleaning and
shaping procedures, consideration of “the aspect of time” when using
5.25% NaOCl might have been the key factor for the impressive
outcome in the present case.
• There have been attempts to elevate the chemical effects of NaOCl
and to lessen the time needed by manual dynamic irrigation or
passive ultrasonic irrigation (PUI) methods.
• Furthermore, in the context of recent studies regarding the antibacterial effects
of Ca(OH)2, long-term intracanal dressings comprising Ca(OH)2 might not be an
efficient strategy to eliminate bacterial biofilms in root canals; this is likely
because of the inhibitory effects of dentin, which was not seriously considered in
the past.
• No Ca(OH)2 intracanal dressing was performed in the present case; 5.25%
NaOCl, with sufficient exposure time, was the sole chemical antibacterial agent
used for complete healing.
• The measurement of ideal contact time of 5.25% NaOCl, with or without
dynamic irrigation methods or Ca(OH)2 intracanal dressings, in infected root
canals during routine root canal treatment is an important subject that requires
further research.
You might also like
- Endodontic ErrorsDocument50 pagesEndodontic Errorsasop06No ratings yet
- Large Lesion Management - Roots0112Document4 pagesLarge Lesion Management - Roots0112nuriacampoNo ratings yet
- FlapDocument100 pagesFlapRicha Agrawal100% (2)
- 2000+ Prometric Questions PDFDocument254 pages2000+ Prometric Questions PDFMohsen Saeed OzaibiNo ratings yet
- Mark Dyczkowski and Trika Journal March 2015 Vol.1.No.1.Document10 pagesMark Dyczkowski and Trika Journal March 2015 Vol.1.No.1.Mark Dyczkoswki and Trika Journal100% (2)
- Aaendo Q&ADocument50 pagesAaendo Q&Aanadelavega96No ratings yet
- Endomishaps SeminarDocument44 pagesEndomishaps SeminarSuma TettaNo ratings yet
- Guidelines For Selecting Materials For Downhole Completions Equipment (Jewellery)Document32 pagesGuidelines For Selecting Materials For Downhole Completions Equipment (Jewellery)Slim.BNo ratings yet
- Defense Mechanism of GingivaDocument59 pagesDefense Mechanism of Gingivaanshum guptaNo ratings yet
- Mercer Role and Job Analysis InfoDocument3 pagesMercer Role and Job Analysis InfojehaniaNo ratings yet
- Endodontics Final ReviewerDocument27 pagesEndodontics Final ReviewerRosette Go100% (5)
- Pediatric Endodontics GuideDocument72 pagesPediatric Endodontics GuideSarath MohanNo ratings yet
- PulpectomyDocument3 pagesPulpectomyWafa Nabilah Kamal100% (1)
- Endodontic SurgeryDocument8 pagesEndodontic SurgeryjoseNo ratings yet
- Treatment Plan in EndodonticsDocument28 pagesTreatment Plan in EndodonticsDR.AMITHBABU.C.BNo ratings yet
- Prepared By: Hashim M. Hussein M.Sc. of Conservative DentistryDocument61 pagesPrepared By: Hashim M. Hussein M.Sc. of Conservative DentistryPuteri NazirahNo ratings yet
- 5.full Mouth Rehabilitation of The Patient With Severely Attrited TeethDocument19 pages5.full Mouth Rehabilitation of The Patient With Severely Attrited Teethnithya_sendhilNo ratings yet
- Christopher Westra - Laws of Attraction PDFDocument3 pagesChristopher Westra - Laws of Attraction PDFZachary LeeNo ratings yet
- Management of Open ApexDocument28 pagesManagement of Open Apexdiksha sinha100% (4)
- Endodontic Surgery: Bilog Falloran Ferrer Delos Reyes Palor Quinones'Document42 pagesEndodontic Surgery: Bilog Falloran Ferrer Delos Reyes Palor Quinones'Michael Francis MendozaNo ratings yet
- Surgical Endodontics Cases 2Document59 pagesSurgical Endodontics Cases 2Maryam Mohamed Abdelkarim AbdelfattahNo ratings yet
- Management of An Endodontic-Periodontal Lesion Caused by IatrogenicDocument8 pagesManagement of An Endodontic-Periodontal Lesion Caused by IatrogenicDebora GultomNo ratings yet
- Management of An Endodontic-Periodontal Lesion Caused by Iatrogenic (Autosaved)Document16 pagesManagement of An Endodontic-Periodontal Lesion Caused by Iatrogenic (Autosaved)Debora GultomNo ratings yet
- Collaborative Management of Combined Endodontic - Periodontal LesionsDocument24 pagesCollaborative Management of Combined Endodontic - Periodontal Lesionsnandani kumariNo ratings yet
- Clinical Management of Severe External Root Resorption: T C K Y A C C P LDocument6 pagesClinical Management of Severe External Root Resorption: T C K Y A C C P LNevena SaulicNo ratings yet
- Trauma CasesDocument47 pagesTrauma CasesMaryam Mohamed Abdelkarim AbdelfattahNo ratings yet
- Pulpal Therapy in PrimaryDocument34 pagesPulpal Therapy in PrimaryShahid HameedNo ratings yet
- Makalah Skenario 3 Blok 6Document45 pagesMakalah Skenario 3 Blok 6Hanaria Putri S EffriantoNo ratings yet
- Intracanal MedicationDocument34 pagesIntracanal MedicationdentistdentistdentisNo ratings yet
- Pulp Therapy in Young Permanent TeethDocument36 pagesPulp Therapy in Young Permanent TeethSeca mandiNo ratings yet
- Success DRDocument49 pagesSuccess DRhanya.mohammedNo ratings yet
- SelvaDocument22 pagesSelvaSelvarathi KandhaswamyNo ratings yet
- Cervikal ResorptionDocument23 pagesCervikal ResorptionFajar Satrio 'Srt'No ratings yet
- Ob Turati OnDocument84 pagesOb Turati Onwu yuoNo ratings yet
- Surgical Endodontic ProceduresDocument22 pagesSurgical Endodontic ProceduresSomya NigamNo ratings yet
- Apical Extrusion of Debris and Irrigant Using HandDocument25 pagesApical Extrusion of Debris and Irrigant Using HandManva MonishNo ratings yet
- Jurnal KasusDocument4 pagesJurnal KasusDena SeptianiNo ratings yet
- Gupta2011 PDFDocument5 pagesGupta2011 PDFAbdul Rahman AlmishhdanyNo ratings yet
- Endodontics: Success of Maintaining Apical Patency in Teeth With Periapical Lesion: A Randomized Clinical StudyDocument9 pagesEndodontics: Success of Maintaining Apical Patency in Teeth With Periapical Lesion: A Randomized Clinical StudyCaio Balbinot100% (1)
- MastoidectomyDocument110 pagesMastoidectomySangam AdhikariNo ratings yet
- 11月book readingDocument31 pages11月book reading新手冒險家No ratings yet
- Regenerative EndodonticsDocument46 pagesRegenerative EndodonticsShameena KnNo ratings yet
- Alternative Anesthetic Technique For Maxillary Periodontal SurgeryDocument31 pagesAlternative Anesthetic Technique For Maxillary Periodontal SurgeryvsdeepsNo ratings yet
- FLAP TECHNIQUES FOR POCKET ELIMINATIONDocument100 pagesFLAP TECHNIQUES FOR POCKET ELIMINATIONRobins Dhakal100% (1)
- 13.endodontic Treatment FR YounPermanent TeethDocument31 pages13.endodontic Treatment FR YounPermanent TeethKhan MustafaNo ratings yet
- ERRORS IN OBTURATION & PREVENTIONDocument27 pagesERRORS IN OBTURATION & PREVENTIONxum tamangNo ratings yet
- Multidisciplinary management of subgingivally fractured tooth using aligner extrusionDocument22 pagesMultidisciplinary management of subgingivally fractured tooth using aligner extrusionNajla MohammedNo ratings yet
- Flap 1Document100 pagesFlap 1HeenaSadhwaniNo ratings yet
- Hasmukhabhai Radicular CystDocument28 pagesHasmukhabhai Radicular Cystkabir shaikhNo ratings yet
- JC2 - Oroantral CommunicationDocument28 pagesJC2 - Oroantral CommunicationSanjiti MadanNo ratings yet
- Access Cavity Preparation: Use of A Transmetal Bur For Access Cavity PreparationDocument3 pagesAccess Cavity Preparation: Use of A Transmetal Bur For Access Cavity PreparationAnonymous C3Gl7jAWTPNo ratings yet
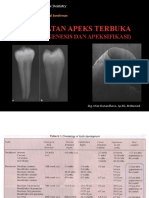
- L3. Apexogenesis - ApexificationDocument44 pagesL3. Apexogenesis - ApexificationAGENG RAHMA HIJAHANIS ILMASTITI 1No ratings yet
- Maxillary Orthognathic Procedures - PPT / Orthodontic Courses by Indian Dental AcademyDocument53 pagesMaxillary Orthognathic Procedures - PPT / Orthodontic Courses by Indian Dental Academyindian dental academyNo ratings yet
- Department of Oral and Maxillofaial Surgery Mamata Dental Collge KhammamDocument39 pagesDepartment of Oral and Maxillofaial Surgery Mamata Dental Collge KhammamAnusha KrishnaNo ratings yet
- Endo4 Lec..6 Cleaning and Shaping of Root CanalDocument24 pagesEndo4 Lec..6 Cleaning and Shaping of Root Canalنور كاضمNo ratings yet
- Gingivectomy & CurettageDocument55 pagesGingivectomy & CurettageRajani GedelaNo ratings yet
- Treatment of a Large Maxillary Cyst with Marsupialization and Staged SurgeryDocument8 pagesTreatment of a Large Maxillary Cyst with Marsupialization and Staged SurgeryDinesh SolankiNo ratings yet
- PeriapikalDocument7 pagesPeriapikalHanindyaNoorAgusthaNo ratings yet
- Css Perio IdolaDocument6 pagesCss Perio IdolanadyapuNo ratings yet
- The Hollow Maxillary Complete DentureDocument24 pagesThe Hollow Maxillary Complete DentureMahjuba ZehraNo ratings yet
- Treatment of An Intrabony Defect CombinedDocument29 pagesTreatment of An Intrabony Defect CombinedDR.AMITHBABU.C.BNo ratings yet
- Case Report/Clinical Technique Nonsurgical Endodontic Treatment of Dens Invaginatus With Large Periradicular Lesion: A CaseDocument4 pagesCase Report/Clinical Technique Nonsurgical Endodontic Treatment of Dens Invaginatus With Large Periradicular Lesion: A CaseVikas DeepNo ratings yet
- Comparative Evaluation of Shear Bond Strength of NDocument6 pagesComparative Evaluation of Shear Bond Strength of NDebora GultomNo ratings yet
- Contoh Buku Kerja Putri HijauDocument4 pagesContoh Buku Kerja Putri HijauDebora GultomNo ratings yet
- Effect of Curing Mode On The PolymerizationDocument9 pagesEffect of Curing Mode On The PolymerizationDebora GultomNo ratings yet
- Effect of Glass Fiber Post Adaptation OnDocument6 pagesEffect of Glass Fiber Post Adaptation OnDebora GultomNo ratings yet
- Single Bond TechniqueDocument12 pagesSingle Bond TechniqueDebora GultomNo ratings yet
- DualCuring, SelfAdhesive Resin Cement Influence of The PolymerizationDocument6 pagesDualCuring, SelfAdhesive Resin Cement Influence of The PolymerizationDebora GultomNo ratings yet
- Translucent Fiber Post Cementation Using Light-And Dual - Curing Adhesive Techniques and A Self-Adhesive Material: Push-Out TestDocument5 pagesTranslucent Fiber Post Cementation Using Light-And Dual - Curing Adhesive Techniques and A Self-Adhesive Material: Push-Out TestDebora GultomNo ratings yet
- PCD N FRCDocument11 pagesPCD N FRCDebora GultomNo ratings yet
- Endo Dont I Cre Treatment in Case of FailureDocument5 pagesEndo Dont I Cre Treatment in Case of FailureDebora GultomNo ratings yet
- Mono BlocDocument8 pagesMono BlocDebora GultomNo ratings yet
- Asc2104b-T I enDocument21 pagesAsc2104b-T I enELOUNDOU EVARISTE OHANDJANo ratings yet
- Cultures of Learning: Language Classrooms in China: Martin Cortazzi Lixian JinDocument54 pagesCultures of Learning: Language Classrooms in China: Martin Cortazzi Lixian JinyhoulhandhariNo ratings yet
- Cell Organelles 11Document32 pagesCell Organelles 11Mamalumpong NnekaNo ratings yet
- 5 Tips For Faster Mental Multiplication PDFDocument3 pages5 Tips For Faster Mental Multiplication PDFGonzalo Estrán BuyoNo ratings yet
- Fee Structure 2023-2024Document10 pagesFee Structure 2023-2024Emmanuel NjogellahNo ratings yet
- Clone CDDocument2 pagesClone CDavk.oracleNo ratings yet
- Sony STR Da80esDocument66 pagesSony STR Da80estelstarservicesNo ratings yet
- XII Class Assignment Programs 2023-24Document8 pagesXII Class Assignment Programs 2023-24Sudhir KumarNo ratings yet
- Boston Globe Article - Jonnie Williams & Frank O'DonnellDocument3 pagesBoston Globe Article - Jonnie Williams & Frank O'DonnellFuzzy PandaNo ratings yet
- Berkowitz Et Al (2010) - Skills For Psychological Recovery - Field Operations GuideDocument154 pagesBerkowitz Et Al (2010) - Skills For Psychological Recovery - Field Operations GuideRita CamiloNo ratings yet
- LAWO PI - MADI - SRC - enDocument2 pagesLAWO PI - MADI - SRC - enfjavierpoloNo ratings yet
- Result Summary - Overall: Moment Connection - Beam To Column Code AISC 360-16 LRFDDocument29 pagesResult Summary - Overall: Moment Connection - Beam To Column Code AISC 360-16 LRFDYash Suthar100% (2)
- ds923 Virtex Ultrascale PlusDocument81 pagesds923 Virtex Ultrascale Plusismail topcuNo ratings yet
- 4684Document2 pages4684Harish Kumar M0% (1)
- CBSE Class 10 Science Revision Notes Chapter - 2 Acids, Bases and SaltsDocument11 pagesCBSE Class 10 Science Revision Notes Chapter - 2 Acids, Bases and Saltsmilind dhamaniyaNo ratings yet
- Sharp Sharp Cash Register Xe A207 Users Manual 284068Document1 pageSharp Sharp Cash Register Xe A207 Users Manual 284068Zeila CordeiroNo ratings yet
- LUMIX G Camera DMC-G85HDocument9 pagesLUMIX G Camera DMC-G85HnimodisNo ratings yet
- Using Previous Years AlmanacDocument1 pageUsing Previous Years AlmanacbhabhasunilNo ratings yet
- Group ActDocument3 pagesGroup ActRey Visitacion MolinaNo ratings yet
- The Greatest Showman PDFDocument22 pagesThe Greatest Showman PDFMJ RecordNo ratings yet
- PDA Technical Documents on Sterilization ProcessesDocument3 pagesPDA Technical Documents on Sterilization ProcessesManas MishraNo ratings yet
- Fundamentals of Computer Hardware NotesDocument7 pagesFundamentals of Computer Hardware NotesSreemoyee RoyNo ratings yet
- SMD 40kHz Ultrasonic Transducer MA40H1SR RevGMay 7 2014Document9 pagesSMD 40kHz Ultrasonic Transducer MA40H1SR RevGMay 7 2014robert wengerNo ratings yet
- Basic Load (Individual) Veterinarian Field PackDocument3 pagesBasic Load (Individual) Veterinarian Field PackJohn MillerNo ratings yet
- Flavors Supplies BudgetDocument6 pagesFlavors Supplies BudgetJomarie EmilianoNo ratings yet
- Slide Detail For SCADADocument20 pagesSlide Detail For SCADAhakimNo ratings yet