Professional Documents
Culture Documents
ANTENATAL CARE PP-1 Blah
Uploaded by
Crazybunny2k0 ratings0% found this document useful (0 votes)
5 views86 pagesGgs
Original Title
ANTENATAL CARE PP-1 blah
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentGgs
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
5 views86 pagesANTENATAL CARE PP-1 Blah
Uploaded by
Crazybunny2kGgs
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 86
GOLDEN LIGHT HEALTH INSTITUTE
PRESENTED BY SARAH MWENYA
INTRODUCTTION
Pregnancy is one of the most important
periods in the life of a:
woman
family
society.
Extraordinary attention is therefore given
to antenatal care by the health care
systems of most countries.
…..
The goal of antenatal care is to:
prevent health problems in both
infant
mother
to see that each newborn child has a
good start.
……
The care provided needs to be;
appropriate
not excessive.
New technologies need to be:
implemented continually
while older services need to be
reconsidered.
……
The care for each pregnant woman
needs to be:
individualized based on her own
needs and wishes.
…..
GENERAL OBJECTIVE
At the end of the lecture, students
should be able to gain knowledge
and understanding on antenatal
care.
……
SPECIFIC OBJECTIVES
At the end of the lecture, students
should be able to:
Define antenatal care
Outline the aims of antenatal care.
Explain the 2016 WHO ANC model.
Discuss the activities during antenatal
care.
…….
DEFINITION OF ANTENATAL CARE
Antenatal care is:
the supervision and management
offered to a pregnant woman from
conception upto the onset of labour
(Henderson and Macdonald, 2004).
AIMS OF ANTENATAL CARE
Early detection of complications
and prompt treatment
Although most pregnancies are
normal, early detection and
treatment of problems that can
complicate pregnancy is important.
…..
ANC promotes targeted assessment
during which the skilled provider:
interviews
Examines
tests the woman
to detect signs and symptoms of
pregnancy as well as any complications.
……
Prevention of diseases and
complications
Provision of safe, simple and cost-
effective interventions such as:
Tetanus Toxoid immunization to
prevent tetanus.
….
Prevention of diseases and
complications
Provision of safe, simple and cost-
effective interventions such as:
Tetanus Toxoid immunization to
prevent tetanus.
…..
Intermittent preventive treatment with Fansidar
and insecticide-treated bed nets for malaria
prevention.
Intermittent Presumptive Treatment (IPT) for
hookworm infection through provision of either
albendazole or mebendazole doses.
…..
Birth preparedness and
complication readiness
If a woman is well prepared for a
normal childbirth and possible
complications, she is more likely to
receive the skilled and timely care she
needs.
…..
This can protect the mother and the
newborn’s life.
It allows for time to develop a birth
plan which includes making
arrangements for normal childbirth.
…..
Developing a birth plan
It includes:
The skilled provider to attend to
the woman.
Place of birth
…..
Transportation of the pregnant woman
to the skilled provider.
Funds
Support person or birth companion.
Items needed for a clean and safe birth
and for the newborn.
…..
Some arrangements in case of
complications
Recognition and response to danger signs
Decision-making in an emergency
situation
Emergency funds.
Emergency transportation.
……
Health promotion
Throughout Antenatal care health
education and counseling are done
to make sure women are able to
take care of themselves.
…..
It is the duty of the skilled provider
to ensure that adequate information
is given to these mothers.
…….
Messages given include:
Preparing a birth plan.
Recognizing danger signs in
pregnancy and during childbirth.
HIV and pregnancy
Malaria in pregnancy
……
Nutrition during pregnancy
Activity and exercise
Childbirth and infant nutrition
including breastfeeding and
replacement feeding
Postnatal care and family planning
services.
2016 WHO ANC Model
2016 WHO ANC Model is antenatal
care model with a minimum of eight
contacts recommended to reduce
perinatal mortality and improve
women’s experience of care.
……
2016 WHO ANC model replaced the
WHO FOCUSED ANTENATAL CARE
(FANC) model.
……
2016 WHO ANC Model was formed
based on the following reasons
Evidence:
suggesting increased perinatal deaths in 4-
visit ANC model
…..
supporting improved safety during
pregnancy through increased
frequency of maternal and fetal
assessment to detect complications
…..
supporting improved health system
communication and support around
pregnancy for women and families
……
indicating that more contacts between
pregnant women and respectful,
knowledgeable health care workers is
more likely to lead to a positive
pregnancy experience
….
from studies indicating no important
differences in maternal and perinatal
health outcomes between ANC models
that included at least eight contacts
and ANC models that included 11 to 15
contacts.
Differences between WHO focused antenatal care and 2016 WHO ANC
model
WHO FANC model 2016 WHO ANC model
First trimester First trimester
Visit 1: 8-12 weeks Contact 1: up to
12 weeks
Second trimester Second trimester
Visit 2: 24-26 Contact 2: 20
weeks weeks
Contact 3: 26
weeks
Third trimester Third trimester
Visit 3: 32 weeks Contact 4: 30 weeks
Visit 4: 36-38 weeks Contact 5: 34 weeks
Contact 6: 36 weeks
Contact 7: 38 weeks
Contact 8: 40 weeks
ACTIVITIES DURING ANTENATAL CARE
REGISTRATION AND BOOKING
When the woman reports for Antenatal
Care booking, she has to be registered
for the purpose of record keeping and
documentation.
…
HISTORY TAKING
The following are the preliminary points
to note during History taking:
Prepare the necessary equipment.
Greet the woman respectfully and introduce
yourself.
Offer the woman a seat and ensure privacy.
……..
Explain the procedure and encourage
her to ask questions.
Get her permission before you begin
the procedure.
Listen to what the woman has to say.
……
History taking is cardinal during ANC
booking for a Nurse/Midwife to get to
know the client well.
It is a means of assessing the health of
the woman to find out any condition
which may affect child bearing.
….
The history has to be comprehensive.
Key issues to consider in history
taking include the following;
Biological data
Name
Age
Address
Marital status
…
Educational level
Occupation
Religion
Contact number
Next of kin
…..
Family History
This kind of history is taken to know the genetic
predisposition to certain diseases.
Ask the woman if there is any history of the following in
the family;
Diabetes mellitus
Hypertension
Asthma
Epilepsy
sickle cell disease
mental illness
since they tend to run in families.
Include history of pulmonary tuberculosis
contact and history of multiple pregnancies.
….
Personal Medical History
Ask the woman if she has ever suffered
from any medical condition
Diabetes mellitus
Hypertension
Asthma
Epilepsy
…..
In addition ask about history of
sexually transmitted infections
urinary tract infection
hepatitis e.t.c.
….
Former illnesses may have damaged
certain structures or organs which could
give rise to complications during
pregnancy and labour
….
Surgical History:
Ask the woman whether she has had injuries
or operations involving the
pelvic bones
Spine
lower limbs.
These could alter the pelvic diameters and
angle of inclination that may lead to cephalo-
pelvic disproportion.
…..
Remember to ask about history of blood
transfusion to exclude:
iso-immunisation if the woman is rhesus negative
….
Past Obstetrical History:
Ask about:
Parity and gravid
Record of previous pregnancies and labour.
Premature or post mature labour
Spontaneous or induced
…..
history of instrumental deliveries
previous obstetric Complications
previous still births.
…..
Menstrual and contraceptive history
Ask about:
Age at menarche
menstrual interval
bleeding pattern
method of contraception
when and how long and reasons for stopping fp.
……
Present obstetric History
Ask the woman about:
First day of the last normal menstrual period and
then calculate the gestational age of the
pregnancy and expected date of delivery.
Fatigue
drowsiness,
Headaches
….
sore tongue
loss of appetite
nausea and vomiting
oedema.
…
PHYSICAL EXAMINATION
This should be done under strict privacy.
Tell the woman what is going to be done
and encourage her to ask questions.
Listen to what the woman has to say.
Prior to the physical examination as a
nurse note the following;
…..
Stature – If a woman has a small built she is likely
to have a small pelvis.
Gait - As the woman walks in, observe any
deformity, stunted growth, limp e.t.c., such may
indicate disproportion in the pelvic diameters.
….
A pregnant woman tilting backwards with a large
abdomen may make one suspect multiple
pregnancies or a very large foetus e.t.c.
..
Height; - 150 cm or less needs special care.
Weight:-The average weight gain during
pregnancy is about 12-14 kg in the first trimester a
woman should gain 0.4 kg per month and in the
second and third trimester she should gain 0.4 kg
per week.
….
Vital signs: Blood pressure, temperature, pulse
and respiration: - Checked and recorded at each
visit,
Urinalysis – ask the woman to pass urine and you
should perform Urinalysis.
This should be done at every visit to rule out
proteins, sugar and acetone in urine.
….
Actual examination
It has to be done from head to toe
Assist the woman to get onto the couch
…..
Wash your hands thoroughly with soap and
water and dry them, then start the
examination.
Head – look for
Under nourished hair
General cleanliness
Eyes – examine for:
Pallor
Jaundice on the conjunctiva by asking the woman
to look up.
….
Nose – examine the nose for:
polyps.
Ears – examine the ears for:
polyps
any discharge.
….
Mouth – ask the woman to open the mouth. Check for:
signs of anaemia on the
Lips
mucus membranes of the mouth
gums
tongue.
fissures on the tongue
oral thrush
sores on the tongue.
Take note of dental caries
…
Glands
palpate for enlargement of the
peri-auricular lymph glands
submandibular lymph glands
cervical glands around the neck.
Palpate the thyroid gland too.
Ask the woman to swallow while your fingers
are lightly placed just below the larynx.
….
Enlargement of gland suggest
infections
chronic illness
may be to the effect of estrogen on the glands
….
Hands – starting with the furthest arm,
examine the arms for
signs of anaemia on the palms
poor venous return on pressure of the nail beds.
Examine for signs of oedema.
Ask the woman to make a fist with each hand;
a feeling of tightness in the knuckles in the absence of
pitting oedema would be suggestive of occult oedema.
….
Check for any physical disability and symmetry
of the arms.
Lastly palpate the axilla for any enlarged
lymph nodes.
…
Breast- examine the breast for;
Presumptive signs of pregnancy i.e.
Montgomery’s tubercles
darkening of primary areola and secondary areola.
……
Suitability for breast feeding – this is more
significant in primigravidae.
Expression of fluid shows that the ducts are
patent.
Presences of clear fluid, milky fluid, colostrum, are
presumptive signs of pregnancy.
Lumps or swelling in the breast.
….
Lower limbs - starting with the furthest leg:
Examine the legs for:
signs of anaemia on the soles
poor venous return on pressure of the nail beds.
…
Examine for signs of tibial, pedal and ankle
oedema.
Check for any physical disability and symmetry of
the arms.
Also check for varicose veins and calf pain.
…..
Abdominal examination
Inspection
Shape:-Note the contour of the abdomen -is it
round, oval, irregular or pendulous?
Size:- Should correspond with the supposed
period of gestation
Skin: - check for dark line of pigmentation (linea
nigra), Straegravidarum, Scar - Any operation
scar(c/s) and any skin lesions.
…..
Palpation
Height of Fundus to determine the how old the
pregnancy is.
Fundal Palpation to determine lie and
presentation.
...
Lateral Palpation to determine the lie, attitude and
position
deep pelvic Palpation to determine the
Presentation.
Auscultation:
Listen to the Foetal heart rate and rhythm
count for one complete minute to ascertain
regularity.
…
LABORATORY TESTS
Urine; Midstream urine culture is the
recommended method for diagnosing
asymptomatic bacteriuria (ASB) in pregnancy.
Urine can also be used to assess for presence of
proteins in urine
….
Blood Tests: Collect blood samples for
RPR
HIV
Haemoglobin
Rhesus
blood grouping.
An ultrasound scan before 24 weeks’ gestation is
recommended for all pregnant women to:
estimate gestational age
detect fetal anomalies and multiple pregnancies
enhance the maternal pregnancy experience
….
Malaria parasite to rule malaria if patient
presents with signs and symptoms of malaria
….
TREATMENT
The following are the drugs given to the
pregnant woman;
Intermittent Presumptive Treatment:
Three doses of Fansidar (SP) to be given at 1st,
2nd, and 3rd visit to prevent malaria in pregnancy
and/or treat asymptomatic malaria.
The SP is to be taken by the woman under direct
observation by the Nurse.
….
Tetanus toxoid injection to be given up to 4th
dose to prevent adult/neonatal tetanus.
Mebendazole 500 mg per oral stat is given for
deworming.
This is given as a single dose with a minimum
gestational age of 20 weeks.
….
Daily doses of ferrous sulphate 200mg and
Folic acid 5 mg to prevent and correct iron
deficiency anaemia and folic acid deficiency
anaemia.
INFORMATION EDUCATION AND COMMUNICATION (IEC)
Give IEC on;
Nutrition in pregnancy
Hygiene in pregnancy
Danger signs in pregnancy
Minor disorders in pregnancy
Birth preparedness and complication readiness,
…
Malaria in pregnancy
PPTCT
Importance of ANC
Signs of true labour
Family planning
Birth registration
Child immunization
…
RECORDING OF FINDINGS
Record or enter all the information gathered
and the care provided on
the Antenatal Card
Safe Motherhood Register.
…..
SUMMARY
Antenatal care, also known as prenatal care, is the
complex of interventions that a pregnant woman
receives from organized health care services.
The number of different interventions in antenatal
care is large.
These interventions may be provided in
approximately 8 antenatal care contacts during a
pregnancy.
….
The purpose of antenatal care is to prevent or
identify and treat conditions that may
threaten the health of the fetus/newborn
and/or the mother, and to help a woman
approach pregnancy and birth as positive
experiences.
…
To a large extent antenatal care can contribute
greatly to this purpose and can in particular
help provide a good start for the newborn
child.
……
• REFERENCES
• The Society of Obstetricians and Gynaecologists of Canada. The Menopause Handbook.
February 2006. Available at www.sogc.org
• MayoClinic.com. Menopause: Definition. Accessed August 2, 2010. Available at
www.mayoclinic.com/health/ menopause/DS00119
• MayoClinic.com. Menopause: Causes. Accessed August 2, 2010. Available at
www.mayoclinic.com/health/ menopause/DS00119/DSECTION=causes
• MayoClinic.com. Menopause: Complications. Accessed August 2, 2010. Available at
www.mayoclinic.com/ health/menopause/DS00119/DSECTION=complications
• MayoClinic.com. Menopause: Treatments and Drugs. Accessed August 2, 2010. Available at
www.mayoclinic. com/health/menopause/DS00119/DSECTION=treatments and drugs
• U.S. Department of Health and Human Services, Office on Women’s Health. Understanding
Menopause. Accessed August 2, 2010. Available at www.womenshealth.gov/menopause/
• MayoClinic.com. Menopause: Lifestyle and Home Remedies. Accessed August 2, 2010.
Available at www. mayoclinic.com/health/menopause/DS00119/DSECTION=lifestyle and
home remedies
….
• End of lecture
You might also like
- Notes On Child and Adolescent PsychiatryDocument172 pagesNotes On Child and Adolescent PsychiatryachikNo ratings yet
- Heavy HandsDocument8 pagesHeavy HandsPicklehead McSpazatronNo ratings yet
- Chipping Work by MCDocument1 pageChipping Work by MCChandruNo ratings yet
- Full Download Test Bank For Microbiology Basic and Clinical Principles 1st Edition Lourdes P Norman Mckay PDF Full ChapterDocument36 pagesFull Download Test Bank For Microbiology Basic and Clinical Principles 1st Edition Lourdes P Norman Mckay PDF Full Chaptertwistingafreetukl3o100% (20)
- 11 Postnatal Care of The Mother and NewbornDocument15 pages11 Postnatal Care of The Mother and NewbornArabelle GO100% (1)
- MCN Case Presentation Group 2 1Document68 pagesMCN Case Presentation Group 2 1Mary-Ann JagonobNo ratings yet
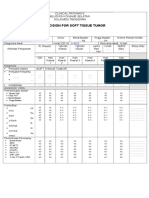
- CP Soft Tissue TumorDocument2 pagesCP Soft Tissue TumorFathur RahmanNo ratings yet
- Victimology exam questions and answersDocument3 pagesVictimology exam questions and answersSubhojit Das0% (1)
- Forensic PathologyDocument3 pagesForensic PathologyjmosserNo ratings yet
- HydrotherapyDocument3 pagesHydrotherapyRhea Mae IbañezNo ratings yet
- Antenatal CareDocument29 pagesAntenatal CareAsti Yuliadha100% (3)
- JMDocument45 pagesJMDana Fajardo RezanoNo ratings yet
- Sja Self-Learning Kit No.4: Fourth Quarter Title of The ModuleDocument15 pagesSja Self-Learning Kit No.4: Fourth Quarter Title of The ModuleMariel Gregore100% (1)
- Job Safety Analysis (Hydro Jetting)Document4 pagesJob Safety Analysis (Hydro Jetting)rashid zaman57% (7)
- 3 Antenatal CareDocument24 pages3 Antenatal CareDrSabah Lotfy100% (1)
- Medical Spa Embezzlement Employee Theft ScamsDocument40 pagesMedical Spa Embezzlement Employee Theft ScamsRamon MartuaNo ratings yet
- Antenatal CareDocument58 pagesAntenatal Caresindhujojo100% (1)
- Antenatal CareDocument19 pagesAntenatal CareIshika RoyNo ratings yet
- Incomplete Abortion MINI CASE STUDY (Group 3)Document22 pagesIncomplete Abortion MINI CASE STUDY (Group 3)Twobee Evelyn Claire62% (21)
- Case StudyDocument38 pagesCase StudyAnonymous 0C4OZmRNo ratings yet
- Pregnant Women's Knowledge of Obstetric Danger SignsDocument13 pagesPregnant Women's Knowledge of Obstetric Danger SignsDrPreeti Thakur ChouhanNo ratings yet
- Puerperal Sepsis: Causes, Symptoms, PreventionDocument31 pagesPuerperal Sepsis: Causes, Symptoms, PreventionRumi Maharjan100% (1)
- Inevitable AbortionDocument21 pagesInevitable AbortionJaysonPangilinanAbanNo ratings yet
- Preventive Obstetrics SeminarDocument25 pagesPreventive Obstetrics SeminarAnju MargaretNo ratings yet
- BSN Level III Clinical InstructorDocument33 pagesBSN Level III Clinical InstructorChristine Bell JapitanaNo ratings yet
- BMCH Family Planning Policy Provides Universal AccessDocument2 pagesBMCH Family Planning Policy Provides Universal AccessShang Dimol100% (1)
- Tayabas Western Academy: Date SubmittedDocument14 pagesTayabas Western Academy: Date SubmittedJohn Paul Madrid Arevalo100% (1)
- International Midwives DayDocument48 pagesInternational Midwives Daymikegrace02No ratings yet
- MCHDocument32 pagesMCHBasmat HassanNo ratings yet
- Domiciliary Midwifery RDocument16 pagesDomiciliary Midwifery Rswillymadhu83% (6)
- 11 Antenatal Care (Irh) 2019Document78 pages11 Antenatal Care (Irh) 2019Mutakatala MootoNo ratings yet
- Antenatal Care: Dr. Abdullahi A.S Dept. of Obstetrics & Gynaecology Abuth-Shika 29 July, 2021Document38 pagesAntenatal Care: Dr. Abdullahi A.S Dept. of Obstetrics & Gynaecology Abuth-Shika 29 July, 2021Muhammad AmeenNo ratings yet
- A Case Study on Abnormal Uterine Bleeding and its TreatmentDocument34 pagesA Case Study on Abnormal Uterine Bleeding and its TreatmentJervy Emiel VALENCIANo ratings yet
- MODULE 1 OB-HISTORY and OB-Physical AssesmentDocument18 pagesMODULE 1 OB-HISTORY and OB-Physical AssesmentThursten Kaye Santos SabandalNo ratings yet
- Family Health Nursing Course Explains Safe MotherhoodDocument29 pagesFamily Health Nursing Course Explains Safe MotherhoodIsaac Nanabenyin100% (1)
- The Prospective Mother, a Handbook for Women During PregnancyFrom EverandThe Prospective Mother, a Handbook for Women During PregnancyNo ratings yet
- Midwifery NursingDocument96 pagesMidwifery NursingMATTHEW KIRARITNo ratings yet
- BPH313Family and Reproductive Health Group 9 Presentation, SID 027-491Document17 pagesBPH313Family and Reproductive Health Group 9 Presentation, SID 027-491duku mosesNo ratings yet
- Prenatal Counselling: Prof. J. Bitzer Universitätskliniken Basel FrauenklinikDocument31 pagesPrenatal Counselling: Prof. J. Bitzer Universitätskliniken Basel FrauenklinikjayashreeselvarajNo ratings yet
- Knowledge of Obstetric Danger SignsDocument12 pagesKnowledge of Obstetric Danger SignsMd RaihanNo ratings yet
- Case StudyDocument38 pagesCase StudyRhon Narciso100% (1)
- Chapter I - Case Background and AssessmentDocument21 pagesChapter I - Case Background and AssessmentJuhainie Dipatuan MagundacanNo ratings yet
- MODULE 3 PRENATAL CARE - Docx 1Document22 pagesMODULE 3 PRENATAL CARE - Docx 1jared abriolNo ratings yet
- Understanding Placenta PreviaDocument53 pagesUnderstanding Placenta PreviajeremiahNo ratings yet
- QUESTIONS DUTY OB BSN2 6B CARAGANandVELORIADocument3 pagesQUESTIONS DUTY OB BSN2 6B CARAGANandVELORIAMikko McDonie VeloriaNo ratings yet
- Antenatal CareDocument49 pagesAntenatal CareAyalewNo ratings yet
- Incomplete Abortion: A Mini Case Study OnDocument22 pagesIncomplete Abortion: A Mini Case Study OnSunny MujmuleNo ratings yet
- Micro TeachingDocument23 pagesMicro Teachingsiti harningsih safitriNo ratings yet
- Antenatal Care (ANC)Document77 pagesAntenatal Care (ANC)tareNo ratings yet
- Placenta Previa: Causes, Symptoms and TreatmentDocument9 pagesPlacenta Previa: Causes, Symptoms and TreatmentSanket TelangNo ratings yet
- Individual Case Study Delivery Room Exposure: (Agusan Del Norte Provincial Hospital, Butuan City)Document13 pagesIndividual Case Study Delivery Room Exposure: (Agusan Del Norte Provincial Hospital, Butuan City)pius troy macapazNo ratings yet
- Test Bank For Maternity Nursing Care 2nd EditionDocument10 pagesTest Bank For Maternity Nursing Care 2nd EditionPaul Hornlein100% (26)
- Ateneo de Zamboanga University: College of Nursing Level 2Document7 pagesAteneo de Zamboanga University: College of Nursing Level 2Sheryhan Tahir BayleNo ratings yet
- 2B-C - Why Did Mrs X Died PDFDocument19 pages2B-C - Why Did Mrs X Died PDFReyna Chame GarcinezNo ratings yet
- Nursing Management of PregnancyDocument69 pagesNursing Management of PregnancyNANDHININo ratings yet
- Program Safe Motherhood Terdiri Dari 4 Pilar:: I. Keluarga Berencana (KB)Document7 pagesProgram Safe Motherhood Terdiri Dari 4 Pilar:: I. Keluarga Berencana (KB)Farihinur RizalNo ratings yet
- Anc 1 2 1Document22 pagesAnc 1 2 1Lemma AbishaNo ratings yet
- Importance of Antenatal CareDocument7 pagesImportance of Antenatal CareKanika NahataNo ratings yet
- PostpartumDocument3 pagesPostpartumMuhammad RifaiNo ratings yet
- OBGYN Topics for DiscussionDocument29 pagesOBGYN Topics for DiscussionAkapireNo ratings yet
- Activity #1 Nupc110-CmcrpDocument4 pagesActivity #1 Nupc110-CmcrpMelody BoadoNo ratings yet
- Preventive ObstetricsDocument8 pagesPreventive ObstetricsAnn Merlin JobinNo ratings yet
- Asha Book No 2Document43 pagesAsha Book No 2Balu MNo ratings yet
- Childbirth Education Then and NowDocument5 pagesChildbirth Education Then and Nowazida90No ratings yet
- Final Case Presentation Group 9 2nd RotationDocument105 pagesFinal Case Presentation Group 9 2nd Rotationjanaquintela58No ratings yet
- Resume Bahasa Inggris Eldawati 2015302240Document18 pagesResume Bahasa Inggris Eldawati 2015302240Omadliqiz Silvia ThesaNo ratings yet
- Awareness of The Impact of Ante-Natal Care (Anc) Services in PreventingDocument8 pagesAwareness of The Impact of Ante-Natal Care (Anc) Services in PreventingUsman Ahmad TijjaniNo ratings yet
- Introduction To Maternal NursingDocument128 pagesIntroduction To Maternal NursingNathalina DeepikaNo ratings yet
- Prevention and Control of Malaria During Pregnancy: A Workshop For Healthcare ProvidersDocument76 pagesPrevention and Control of Malaria During Pregnancy: A Workshop For Healthcare ProvidersrositaNo ratings yet
- Delivery Room E-PortfolioDocument17 pagesDelivery Room E-PortfolioLRBNo ratings yet
- Maternal Book MCNPDocument66 pagesMaternal Book MCNPChie BelisarioNo ratings yet
- Pacita Complex National HighschoolDocument19 pagesPacita Complex National HighschoolBianca RosalesNo ratings yet
- The Prospective Mother, a Handbook for Women During PregnancyFrom EverandThe Prospective Mother, a Handbook for Women During PregnancyNo ratings yet
- 1628 6995 3 PBDocument32 pages1628 6995 3 PBPelayanan Tahanan Rutan KendariNo ratings yet
- When Learning and Remembering Compete: A Functional MRI StudyDocument5 pagesWhen Learning and Remembering Compete: A Functional MRI Studyclaire_thixtonNo ratings yet
- Types of ImmunoglobulinDocument14 pagesTypes of ImmunoglobulinZubair AlamNo ratings yet
- SWINE Magazine Feb/Apr 2021Document30 pagesSWINE Magazine Feb/Apr 2021jem ruizNo ratings yet
- Panel Hospital List IGIDocument6 pagesPanel Hospital List IGIAbdul RahmanNo ratings yet
- Акушерство Фукс англ 2019Document875 pagesАкушерство Фукс англ 2019ȜLaa AsHrafNo ratings yet
- Impact On LGBTQ IssuesDocument2 pagesImpact On LGBTQ IssuesAngel BirringNo ratings yet
- Rujukan OrtoDocument8 pagesRujukan OrtoJade M. LolongNo ratings yet
- GNLD's G1 Laundry Powder - Fast FactsDocument2 pagesGNLD's G1 Laundry Powder - Fast FactsNishit KotakNo ratings yet
- Customs and Taboos of Bidayuh CommunityDocument16 pagesCustoms and Taboos of Bidayuh Communitykhairul ikhwanNo ratings yet
- A Case Report of Evans SyndromeDocument5 pagesA Case Report of Evans SyndromecatNo ratings yet
- Taquicardia Supraventricular y CetoacidosisDocument5 pagesTaquicardia Supraventricular y CetoacidosisAlejandro CárdenasNo ratings yet
- Rheumatic Heart DiseaseDocument3 pagesRheumatic Heart DiseasearyshamyleeNo ratings yet
- Zamora Assignment #4 (Cmca)Document5 pagesZamora Assignment #4 (Cmca)Elizabeth ZamoraNo ratings yet
- CT1, CT2, CT5 and CT8 Study Plan UK Exams September 2013Document8 pagesCT1, CT2, CT5 and CT8 Study Plan UK Exams September 2013Mohamed ArafaNo ratings yet
- Literature Review Effects of DanceDocument5 pagesLiterature Review Effects of Danceapi-549199196No ratings yet
- Chocolate and DepressionDocument15 pagesChocolate and DepressionAdriantopNo ratings yet