Professional Documents
Culture Documents
Development of The Pharyngeal Pouches and Clefts
Uploaded by
somtee0030 ratings0% found this document useful (0 votes)
2 views24 pagesOriginal Title
Development of the Pharyngeal Pouches and Clefts
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
2 views24 pagesDevelopment of The Pharyngeal Pouches and Clefts
Uploaded by
somtee003Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 24
Development of the Pharyngeal
Pouches and Clefts
Dr J.O Ezugworie
MBBS, MSc, FWACS
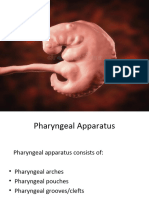
Pharyngeal gut
Pharyngeal Pouches
Introduction
• The primordial pharynx or pharyngeal gut widens
rostrally to join the stomodeum or primordial
mouth
• The pharyngeal gut narrows caudally to join the
oesophagus
• The endoderm of the pharynx lines the internal
aspect of the pharyngeal arches
• In between the pharyngeal arches, the pharyngeal
gut passes into a balloon-like diverticula – the
pharyngeal pouches
Pharyngeal Pouches and the Derivatives
Introduction
• The pharyngeal pouches form by the 4th and
5th weeks of development
• There are 5 pairs of the pharyngeal pouches,
but the 5th is rudimentary
• The endodermal epithelial lining of the
pouches gives rise to a number of important
organs
Derivatives of the Pharyngeal Pouches
First pharyngeal pouch
Tympanic (middle ear) cavity ; Auditory (Eustachian) tube
; Part of ear drum
• The distal portion of the first pharyngeal pouch widens
into a sack-like structure; the primitive tympanic or
middle ear
• The proximal portion remains narrow to become the
auditory (Eustachian) tube
• The endothelial lining of the tympanic cavity participate
in the formation of the ear drum or tympanic
membrane
Pharyngeal Pouch Derivatives
Derivatives of the Pharyngeal Pouches
Second pharyngeal pouch
Palatine tonsil ; Tonsillar fossa
• The second pharyngeal pouch forms buds that
penetrate into the surrounding mesenchyme
• Mesodermal tissue later invade the buds to form the
primordium of the palatine tonsils
• The tonsil is infiltrated by lymphatic tissue during the
3rd and 5th months of development
• Part of the pouch remains in the adult as the tonsillar
fossa
Derivatives of the Pharyngeal Pouches
Third pharyngeal pouch
Inferior parathyroid gland
Thymus
• The distal end of the 3rd pharyngeal pouch has a
dorsal and a ventral wing
• The epithelium of the dorsal wing forms inferior
parathyroid gland by the 5th week of development
• Inferior parathyroid gland moves to rest finally on
the dorsal surface of the thyroid gland
Derivatives of the Pharyngeal Pouches
• The ventral wing forms the thymus
• The thymus migrates in a caudal and a medial
direction, pulling the inferior parathyroid with it
• The main portion of the thymus quickly moves
to the anterior part of the thorax (the final
portion) fusing with the opposite side
• The tail portion of the thymus sometimes
persists, embedded in the thyroid gland or as
isolated thymic nests
Derivatives of the Pharyngeal Pouches
• Growth and development of the thymus
continue until puberty.
• Thymus occupies a considerable space in the
thorax.
• It lies behind the sternum, anterior to the
pericardium and great vessels.
• It is atrophied and replaced by fatty tissues in
older persons.
Derivatives of the Pharyngeal Pouches
Fourth pharyngeal pouch
Superior parathyroid gland
Ultimobranchial body
Parafollicular cells or C cells
• The distal end has a dorsal and a ventral wing
(like the 3rd pouch)
• The dorsal region of the 4th pharyngeal pouch
forms the superior parathyroid gland
Derivatives of the Pharyngeal Pouches
• The ventral wing gives rise to the
ultimobranchial body which later gets
incorporated into the thyroid gland.
• Cells of the ultimobranchial body give rise to
the parafollicular cells or C cells of the thyroid
gland.
• The parafollicular cells or C cells secrete
Calcitonin, a hormone regulating the calcium
level in the blood.
Pharyngeal Clefts
• The ectodermal lined grooves or recesses separating the
pharyngeal arches externally
• 5th week embryo is characterized by the presence of four
pharyngeal clefts
• It was previously thought that the first pharyngeal cleft
contributed to the formation of the auditory meatus
(EAM).
• This has been disproved.
• Rather the external auditory meatus is formed by the
invagination of the surface ectoderm from the first
pharyngeal arch
Pharyngeal Clefts
Pharyngeal Clefts
• First pharyngeal cleft disappears due to the
overgrowth of the second pharyngeal arch (which
forms most of the external ear).
• Second pharyngeal arch overlaps the 3rd and 4th
pharyngeal arches due to active proliferation of the
mesenchymal tissue.
• The 2nd, 3rd and 4th pharyngeal clefts lose contact
with the outside.
• This is because the 2nd pharyngeal arch merges with
the epicardial ridge in the lower part of the neck.
Pharyngeal Clefts
• The 2nd, 3rd and 4th pharyngeal clefts form a
cavity lined by ectodermal epithelium called
the cervical sinus.
• The cervical sinus disappears with further
development.
• Thus all the clefts disappeared.
Clinical Correlates
Ectopic thymic and parathyroid tissues.
• Glandular tissues from the pharyngeal arches
undergo migration.
• Accessory glands or remnants of the tissue
may persist along the pathway.
• Like thymic tissue may remain in the neck
Clinical Correlates
Branchial fistulas
• The remnants of the 2nd, 3rd and 4th pharyngeal
clefts may remain in contact with the surface by a
narrow canal.
• This results from failure of the 2 nd pharyngeal arch
to grow caudally over the 3rd and 4th arches to
obliterate the clefts.
• Such fistula on the lateral aspect of the neck usually
provides drainage for a lateral cervical cyst.
Clinical Correlates
Internal brachial fistulas
• These are rare – a small canal may connect the
cervical sinus to the lumen of the pharynx.
• This usually opens into the tonsillar region.
• Such a fistula results from rupture of the
membrane between the 2nd pharyngeal cleft
and pouch during development.
Lateral Cervical Cysts And Fistulas
Clinical Correlates
• DiGeorge sequence (3rd and 4th pharyngeal
pouch syndrome)
• This includes hypoplasia or absence of the
thymus and or parathyroid glands with or
without CNS defects, abnormal external ears,
micrognathia (small jaws), and hypertelorism
(widely spaced eyes)
NOTE: Read up Neural crest cells and
craniofacial defects.
Lateral Cervical Cyst
You might also like
- 02-Pharyngeal Arches, Pouches and CleftsDocument41 pages02-Pharyngeal Arches, Pouches and Cleftssiciidck09No ratings yet
- Pharyngeal Apparatus Part - 2Document40 pagesPharyngeal Apparatus Part - 2meghNo ratings yet
- Embryo 11ADocument85 pagesEmbryo 11AAyeshaNo ratings yet
- EMB5, PDFDocument7 pagesEMB5, PDFSafura IjazNo ratings yet
- 21 - Pharyngeal Arches (HD)Document40 pages21 - Pharyngeal Arches (HD)checkmateNo ratings yet
- Tumbuh Kembang GIGI 2013 Eps.2Document88 pagesTumbuh Kembang GIGI 2013 Eps.2wardaniNo ratings yet
- Presentation On Pharyngeal ApparatusDocument35 pagesPresentation On Pharyngeal ApparatusMidhilaNo ratings yet
- Panduan Embrio DasarDocument21 pagesPanduan Embrio DasarPockets Ain't EmptyNo ratings yet
- Pharyngeal ArchesDocument35 pagesPharyngeal ArchesconstantinilieNo ratings yet
- Derivatives of Pharyneal ArchesDocument36 pagesDerivatives of Pharyneal ArchesMARKS OMFSNo ratings yet
- 02-Pharyngeal Arches - Pouches and CleftsDocument43 pages02-Pharyngeal Arches - Pouches and CleftsesraaNo ratings yet
- Embryology OrganogenesisDocument138 pagesEmbryology OrganogenesisBarlaam Bagus PurwakaNo ratings yet
- Pharyngeal Arches and PouchesDocument42 pagesPharyngeal Arches and PouchesSos Gilani100% (1)
- Anatomy of PharynxDocument31 pagesAnatomy of PharynxMuhammad KamilNo ratings yet
- Development of FaceDocument19 pagesDevelopment of FaceAkhila ReddyNo ratings yet
- Development of The Respiratory SystemDocument22 pagesDevelopment of The Respiratory SystemtuhinNo ratings yet
- Embryology of The Head and NeckDocument18 pagesEmbryology of The Head and NeckDr-Firas Nayf Al-ThawabiaNo ratings yet
- Development of Body Cavities and Diaphragm: Pleuro-Pericardial and Pleuro-Peritoneal MembraneDocument14 pagesDevelopment of Body Cavities and Diaphragm: Pleuro-Pericardial and Pleuro-Peritoneal MembraneÑäd ÉèmNo ratings yet
- Branchial ArchesDocument49 pagesBranchial ArchesSherin ThomasNo ratings yet
- Ontogeny of Respiratory System: Abd. Razak RatuDocument43 pagesOntogeny of Respiratory System: Abd. Razak RatuNur AnniesaNo ratings yet
- 03-Tongue & ThyroidDocument35 pages03-Tongue & ThyroidirfnaghoriNo ratings yet
- Development of The EarDocument58 pagesDevelopment of The EarAuza Moses IbrahimNo ratings yet
- Special Embryo Tibb TantaDocument15 pagesSpecial Embryo Tibb TantaAhmed GamalNo ratings yet
- The Pharyngeal ArchesDocument28 pagesThe Pharyngeal ArchesalcojonicNo ratings yet
- Embryology SlideDocument33 pagesEmbryology Slidethorodison786No ratings yet
- The Gut Tube and Body CavitiesDocument31 pagesThe Gut Tube and Body CavitiesGeoffreyNo ratings yet
- Development of Head and Neck: Pharyngeal ArchesDocument14 pagesDevelopment of Head and Neck: Pharyngeal Archesmueen hashmiNo ratings yet
- Endocrine EmbryologyDocument3 pagesEndocrine Embryologyb.bethel2003No ratings yet
- Anatomy PNDocument131 pagesAnatomy PNDr.P.NatarajanNo ratings yet
- Development of FaceDocument34 pagesDevelopment of FacealkalicharanNo ratings yet
- Respiratory System EmbDocument29 pagesRespiratory System EmbDanish GujjarNo ratings yet
- Body Cavities and Diaphragm 15Document21 pagesBody Cavities and Diaphragm 15Lugembe MasolaNo ratings yet
- Folding of The Embryo Formation of Gut Endodermal DerivativesDocument26 pagesFolding of The Embryo Formation of Gut Endodermal DerivativesAmalinaZolkefleeNo ratings yet
- Branchial ArchesDocument14 pagesBranchial ArchesMahesh kumarNo ratings yet
- Development of EarDocument33 pagesDevelopment of EarMuskan IsmailNo ratings yet
- Development of The EarDocument21 pagesDevelopment of The Eartemesgen belayNo ratings yet
- I. Pharyngeal Apparatus: A. Fates of Pharyngeal CleftsDocument10 pagesI. Pharyngeal Apparatus: A. Fates of Pharyngeal CleftsARINA KHAQNo ratings yet
- Development of Tongue and ThyroidDocument10 pagesDevelopment of Tongue and ThyroidgautamNo ratings yet
- Prenatal Growth 1Document64 pagesPrenatal Growth 1Kar InNo ratings yet
- 4th To 8th WeeksDocument99 pages4th To 8th WeeksTimmyNo ratings yet
- Development of Thyroid GlandDocument37 pagesDevelopment of Thyroid GlandnrahmaNo ratings yet
- Development of Pharyngeal ApparatusDocument50 pagesDevelopment of Pharyngeal ApparatusPapadoveNo ratings yet
- Anatomy of Nose and PNS Final-1Document132 pagesAnatomy of Nose and PNS Final-1Sangam AdhikariNo ratings yet
- Larynx: Syson, JasonDocument18 pagesLarynx: Syson, JasonJason SysonNo ratings yet
- 8.folding of EmbryoDocument26 pages8.folding of Embryobibi.hansmuddyNo ratings yet
- Embryology of Head & Neck Iii Endodermal Pouches and Derivatives, Development of The EyeDocument6 pagesEmbryology of Head & Neck Iii Endodermal Pouches and Derivatives, Development of The EyeJo ErestainNo ratings yet
- MAE-Development of Lyphatic Organs-2024Document33 pagesMAE-Development of Lyphatic Organs-2024ozerbilge24No ratings yet
- Pharyngeal Arches and Its DerivativesDocument57 pagesPharyngeal Arches and Its DerivativesDr Toqeer AhmedNo ratings yet
- Embryology of The Ear and Its AnatomyDocument20 pagesEmbryology of The Ear and Its AnatomyElisa NNo ratings yet
- Anatomy of The Pharynx OesophagusDocument12 pagesAnatomy of The Pharynx OesophagusArjun SainiNo ratings yet
- Airway BSC AnesthesiaDocument72 pagesAirway BSC AnesthesiaTerefe AlemayehuNo ratings yet
- Anatomy of The Pharynx & OesophagusDocument12 pagesAnatomy of The Pharynx & OesophagusBkas GrgNo ratings yet
- Embryology of Body Cavities, Mesenteries and DiaphragmDocument35 pagesEmbryology of Body Cavities, Mesenteries and DiaphragmKankomba MuleyaNo ratings yet
- MS ENT Basic Sciences MGR University September 2009 Question Paper With SolutionDocument36 pagesMS ENT Basic Sciences MGR University September 2009 Question Paper With SolutionDr. T. Balasubramanian67% (3)
- Folding of An EmbryoDocument26 pagesFolding of An EmbryoSally CahillNo ratings yet
- Presented by Abhitosh DebataDocument138 pagesPresented by Abhitosh DebataNishant KumarNo ratings yet
- Anatomy and Physiology of The Pharynx-Larynx-TracheaDocument22 pagesAnatomy and Physiology of The Pharynx-Larynx-TracheaZacky Abdoel AzamNo ratings yet
- Foldings of Embryo Foetal Period 1Document22 pagesFoldings of Embryo Foetal Period 1Riya SinghNo ratings yet
- Pharyngeal Pouches: Pharyngeal Arches Revisited and TheDocument8 pagesPharyngeal Pouches: Pharyngeal Arches Revisited and Thealvin salvationNo ratings yet
- Tai Yin MT PointsDocument12 pagesTai Yin MT PointspauloasvNo ratings yet
- Basilar Invagination - C1-C2 DistractionDocument6 pagesBasilar Invagination - C1-C2 DistractionSri Vijay Anand K SNo ratings yet
- Ion TechniquesDocument39 pagesIon TechniquesRunuk BhandariNo ratings yet
- Biology of PenguinsDocument43 pagesBiology of PenguinsMarilyn Castillo100% (10)
- Scorpio TS Operative Technique 2013 PDFDocument20 pagesScorpio TS Operative Technique 2013 PDFSergiu PlescaNo ratings yet
- 18 Sigwart Sumner Rooney Chapter 18Document19 pages18 Sigwart Sumner Rooney Chapter 18Haniza SaraNo ratings yet
- The New BettaDocument154 pagesThe New Bettachoon lee minNo ratings yet
- Acupuncture Products Catalog 2012Document15 pagesAcupuncture Products Catalog 2012Ramon Alberto Portillo MedinaNo ratings yet
- Terminoligies of Tooth MorphologyDocument33 pagesTerminoligies of Tooth MorphologyAyeshaNo ratings yet
- Pir 23Document6 pagesPir 23Mohamad Farin Hazim Bin Abd AzizNo ratings yet
- 10 1 1 553 7658 PDFDocument6 pages10 1 1 553 7658 PDFAgustino IdongNo ratings yet
- Skill: Assessing The Thorax and LungsDocument3 pagesSkill: Assessing The Thorax and LungsKathrina AlfonsoNo ratings yet
- Radiographic Positioning TerminologyDocument4 pagesRadiographic Positioning TerminologyPedro SegundoNo ratings yet
- Test Bank For The Human Body in Health and Disease 5th Edition by ThibodeauDocument7 pagesTest Bank For The Human Body in Health and Disease 5th Edition by Thibodeauglumpyperuke.zb26k100% (39)
- Large Fragment Implants and InstrumentsDocument22 pagesLarge Fragment Implants and InstrumentsMarc KleinNo ratings yet
- Alienoptera - A New Insect OrderDocument30 pagesAlienoptera - A New Insect OrderRafael CedroNo ratings yet
- Anatomical Terms by DR - Soe LwinDocument28 pagesAnatomical Terms by DR - Soe LwinIntan AinNo ratings yet
- Key To The UK Species of Amara v2Document35 pagesKey To The UK Species of Amara v2backkomster6439No ratings yet
- R. Hassler, H. Stephan (Eds.) - Evolution of The ForebrainDocument472 pagesR. Hassler, H. Stephan (Eds.) - Evolution of The ForebrainGregori JacksonNo ratings yet
- Article SEBTDocument9 pagesArticle SEBTbbvnrsh279No ratings yet
- An in Vitro Human Cadaveric Study Investigating The Biomechanical Properties of The Thoracic Spine - Oda PDFDocument7 pagesAn in Vitro Human Cadaveric Study Investigating The Biomechanical Properties of The Thoracic Spine - Oda PDFAnderson MoribeNo ratings yet
- Radio Distal MedartisDocument48 pagesRadio Distal MedartisavillouNo ratings yet
- Posterior Palatal SealDocument7 pagesPosterior Palatal SealÄpriolia SuNo ratings yet
- The What and How of Prefrontal Cortical Organization: Randall C. O'ReillyDocument7 pagesThe What and How of Prefrontal Cortical Organization: Randall C. O'ReillyAvengingBrainNo ratings yet
- Examining Joints: How To Succeed in Clinical ExaminationsDocument12 pagesExamining Joints: How To Succeed in Clinical ExaminationsimperiallightNo ratings yet
- Medacta Instrum PlastiqueDocument36 pagesMedacta Instrum Plastiquemarcpafr52No ratings yet
- Anatomical TerminologyDocument12 pagesAnatomical Terminologysarped10No ratings yet
- Mechanical Treatment For The Cervical SpineDocument36 pagesMechanical Treatment For The Cervical SpineMohamed ElMeligieNo ratings yet
- Laboratory Manual For Anatomy and Physiology 6th Edition Ebook PDFDocument41 pagesLaboratory Manual For Anatomy and Physiology 6th Edition Ebook PDFrandy.beard301100% (28)
- The Ichthyoarchaeology of Batanes Islands, Northern PhilippinesDocument145 pagesThe Ichthyoarchaeology of Batanes Islands, Northern PhilippinesFredeliza CamposNo ratings yet