Professional Documents
Culture Documents
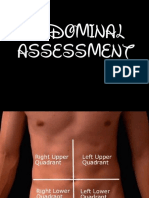
Assessing The Abdomen 1
Uploaded by
srslytrd0 ratings0% found this document useful (0 votes)
11 views20 pagesOriginal Title
Assessing the Abdomen 1 Copy
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
11 views20 pagesAssessing The Abdomen 1
Uploaded by
srslytrdCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 20
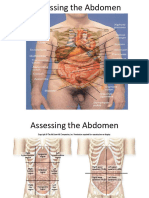
Assessing the Abdomen
abdominal assessment sequence :
Inspection
Auscultation
Percuss
Palpation
Preparation:
• Ask patient to void, to promote comfort during the procedure.
• Position patient in a supine position, arms on side ,bends the knees slightly.
• Bending the knees will help to relax the abdomen and make palpation easier.
• Expose abdomen, nurse’s hands and diaphragm of the stethoscope must be
warm.
• Sequence : Inspection, Auscultation, Percussion, Palpation( IAPP)
preparation
• SEQUENCE OF EXAMINATIONS OF THE QUADRANTS :
- Right Lower quadrant, Right upper quadrant,
Left upper quadrant, Left lower quadrant
( RLQ, RUQ, LUQ, LLQ)
Assessing the abdomen
Inspection of the abdomen : have Patient lie on his back
• Skin integrity ;
- unblemished skin, uniform color, striae, surgical scars
Deviations : presence of rash, lesions, tense glistening skin( ascites, edema)
• Contour and symmetry:
- flat, rounded( convex) scaphoid( concave), symmetric contour
Deviations:
-distended, asymmetric
-Asymmetric contour
Observe abdominal movements
- symmetric movements caused respiration,
- visible peristalsis in very lean people
- aortic pulsations in thin persons at epigastric area
Deviations:
limited movement due to pain or disease
Visible peristalsis, marked aortic pulsations
Vascular patterns
• No visible visual pattern
Deviations:
• Visible venous pattern( dilated veins)
Auscultate abdomen
for:
)
1. Bowel sounds ; audible bowel sounds heard in 4 quadrants high
pitched occurs 5-30 times per minute.
• Listen for full 5 minutes if no bowel sounds is heard.
Deviations: absent, hypoactive or hyperactive bowel
sounds
2. Vascular sounds: absence arterial bruits
Deviations: loud bruit over aortic area( aneurysm)
3. Peritoneal friction rubs: absence of friction rubs
• Deviations: bruit or renal or iliac arteries
Palpate abdomen
To detect areas of tenderness
a. Light palpation (depress about 1cm)
Normal findings:
No tenderness; relaxed abdomen with smooth, consistent tension
Deviations from normal :
tenderness and hypersensitivity
Superficial masses
Localized areas of increased tension
b.Deep palpation ( 1.5 to 2 inches deep)
DEEP PALPATION
• It is the indentation of the abdomen performed by pressing the distal half of the palmar
surfaces of the fingers into the abdominal wall.
• The abdominal wall may slide back and forth while the fingers move back and forth
over the organ being examined.
• Deeper structures, like the liver, and retro peritoneal organs, like the kidneys, or masses
may be felt with this method.
• In the absence of disease, pressure produced by deep palpation may produce tenderness
over the cecum, the sigmoid colon, and the aorta.
LIVER PALPATION
• There are two types of bi manual palpation recommended for palpation
of the liver. The first one is the superimposition of the right hand over
the left hand.
• Ask the patient to take 3 normal breaths.
• Then ask the client to breath deeply and hold. This would push the liver
down to facilitate palpation.
• Press hand deeply over the RUQ
PALPATION OF THE LIVER
• the second methods:
• The examiner’s left hand is placed beneath the client at the level of the right 11th and 12th
ribs.
• Place the examiner’s right hands parallel to the costal margin or the RUQ.
• An upward pressure is placed beneath the client to push the liver towards the examining
right hand, while the right hand is pressing into the abdominal wall.
• Ask the client to breath deeply.
• As the client inspires, the liver maybe felt to slip beneath the examining fingers.
Palpation of the liver
Normal Findings:
• The liver usually can not be palpated in a normal adult. However, in
extremely thin but otherwise well individuals, it may be felt the costal
margins.
• When the normal liver margin is palpated, it must be smooth, regular in
contour, firm and non-tender.
Palpate the liver to detect enlargement and tenderness
May be palpable , border feels smooth
No tenderness
Deviations:
Enlarged , smooth but tender;
Nodular( growth of abnormal tissue) or hard
Liver span >12cm or <6cm indicate
hepatomegaly or cirrhosis( scarring or fibrosis)
• Palpate for the liver with one or two hands palm down moving upward 2-
3 cm at a time towards the lower costal margin( medial margin of the 7th
to 10th ribs).
• Have the patient take a deep breath.
The liver will move downward due to the
downward movement of the diaphragm.
Feel for the liver to hit the caudal (tail)
aspect of your palpating hand.
Palpate bladder for possible urinary retention
• Palpate area above the pubic symphysis
Not palpable
Deviations from normal:
Distended and palpable as
smooth, round, tense
( indicates urinary retention )
Normal Findings: Inspection
• Skin color is uniform, no lesions.
• Some clients may have striae or scar.
• No venous engorgement.
• Contour may be flat, rounded or scapoid
• Thin clients may have visible peristalsis.
• Aortic pulsation maybe visible on thin clients.
You might also like
- Abdominal AssessmentDocument59 pagesAbdominal AssessmentSIR ONE100% (1)
- Types of Bone Fractures Classification GuideDocument8 pagesTypes of Bone Fractures Classification GuideApple PaiNo ratings yet
- AbdomenDocument7 pagesAbdomenShayne Lyrrie Pajela100% (1)
- Assessing the Abdomen: 4 Quadrants and 9 RegionsDocument54 pagesAssessing the Abdomen: 4 Quadrants and 9 RegionsWilma Acorin OrillinedaNo ratings yet
- Clinical Examination of Gastrointestinal SystemDocument34 pagesClinical Examination of Gastrointestinal SystemDivya Rajendran100% (1)
- Abdominal ExaminationDocument54 pagesAbdominal ExaminationGemmalene Pacleb100% (4)
- PE of The Abdomen Guide 2020Document8 pagesPE of The Abdomen Guide 2020salfopsi gaming100% (1)
- LWW BATES 13 Abdomen Transcript FINALDocument6 pagesLWW BATES 13 Abdomen Transcript FINALmuhammad Babar50% (2)
- Intestinal Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandIntestinal Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- 2019 Afk ProtocolDocument10 pages2019 Afk Protocoldrsunny159840% (1)
- 3 Session 3 - AbdominalExamDocument15 pages3 Session 3 - AbdominalExamjhk0428No ratings yet
- Assessing Abdomen Regions & SoundsDocument16 pagesAssessing Abdomen Regions & SoundsjoslinjohnNo ratings yet
- Examination of Chronic AbdomenDocument43 pagesExamination of Chronic AbdomendrrajeshpsmsNo ratings yet
- Assessment of The AbdomenDocument57 pagesAssessment of The AbdomenKarylle Petil100% (1)
- Lip AugmentationDocument8 pagesLip AugmentationAhmed BadawyNo ratings yet
- Basic Abdominal ExaminationDocument3 pagesBasic Abdominal Examinationcpradheep100% (1)
- Pemeriksaan AbdomenDocument46 pagesPemeriksaan AbdomenPrystia_RNo ratings yet
- Abdominal Examination ChecklistDocument6 pagesAbdominal Examination ChecklistPalwasha MalikNo ratings yet
- Abdominal Exam Guide: Palpation, Inspection & Surface MarkingsDocument4 pagesAbdominal Exam Guide: Palpation, Inspection & Surface MarkingsPhysician AssociateNo ratings yet
- Assessment of The AbdomenDocument98 pagesAssessment of The Abdomenyanna aNo ratings yet
- Examination of AbdomenDocument41 pagesExamination of AbdomenMohammad_Islam87No ratings yet
- DR Amaefula, E. Temple MBBS, Fwacs, Faoi,: Inflamation, Infection, and Use of Antibiotics in SurgeryDocument40 pagesDR Amaefula, E. Temple MBBS, Fwacs, Faoi,: Inflamation, Infection, and Use of Antibiotics in SurgeryPrincewill SeiyefaNo ratings yet
- 1.2.7 Abdominal Exam - SendDocument65 pages1.2.7 Abdominal Exam - Senddanielndaa51No ratings yet
- ABDOMINAL SOUNDSDocument10 pagesABDOMINAL SOUNDSMiden AlbanoNo ratings yet
- FrankDocument26 pagesFrankريبو /RepoNo ratings yet
- Clinical Examination of AbdomenDocument37 pagesClinical Examination of AbdomenAshima Farrukh YasubNo ratings yet
- 6 - The AbdomenDocument83 pages6 - The AbdomenXtylish Bacha 8bpNo ratings yet
- Physical Examination GI Track (INTERNATIONAL)Document59 pagesPhysical Examination GI Track (INTERNATIONAL)AnnisNo ratings yet
- Assess Abdomen Quickly Using 4 StepsDocument12 pagesAssess Abdomen Quickly Using 4 StepsJyra Mae TaganasNo ratings yet
- Assessment Mouth and Oropharynx LipsDocument8 pagesAssessment Mouth and Oropharynx LipsQuinmarc LimNo ratings yet
- Gi ExaminationDocument28 pagesGi ExaminationNadun MethwadaneNo ratings yet
- Examining the Abdomen Effectively in Under 10 MinutesDocument21 pagesExamining the Abdomen Effectively in Under 10 MinutesnouraNo ratings yet
- ABDOMINAL EXAMINATION EditedDocument21 pagesABDOMINAL EXAMINATION EditedTsegaye HailuNo ratings yet
- AbdomenDocument9 pagesAbdomenJazzmyne T.No ratings yet
- Abdominal Examination For PSIII Edited-1Document33 pagesAbdominal Examination For PSIII Edited-1myarjddbzNo ratings yet
- Part 2 AbdoexamDocument36 pagesPart 2 Abdoexamapi-19641337No ratings yet
- Clinical Examination of The AbdomenDocument13 pagesClinical Examination of The AbdomenNur Miladiyah100% (1)
- Script AbdomenDocument19 pagesScript AbdomenRespicio Christian Aejay G.No ratings yet
- Pemeriksaan AbdomenDocument91 pagesPemeriksaan AbdomenEndah Cahaya SufianyNo ratings yet
- Abdo ExamDocument7 pagesAbdo ExamCharis Kai Xin AuNo ratings yet
- Abdominal Assessment SlidesDocument31 pagesAbdominal Assessment SlidesFarisa Jane BanggoNo ratings yet
- Care of Clients With Gastrointestinal Disorders: Michael D. Manglapus, BSN-RN, RM, Man, PHDDocument61 pagesCare of Clients With Gastrointestinal Disorders: Michael D. Manglapus, BSN-RN, RM, Man, PHDMichael Baylon DueñasNo ratings yet
- Assesment of Acute Abdomen: Dr. Dr. Benyamin Lukito, SPPDDocument65 pagesAssesment of Acute Abdomen: Dr. Dr. Benyamin Lukito, SPPDAgatha FeliciaNo ratings yet
- Session 6 - Performing Abdominal ExaminationDocument33 pagesSession 6 - Performing Abdominal ExaminationOtsward OwdenNo ratings yet
- Palpação AbdominalDocument6 pagesPalpação AbdominalLeni8No ratings yet
- LI - Physical Examination - AbdomenDocument6 pagesLI - Physical Examination - AbdomenTravis DonohoNo ratings yet
- Abdominal Examination 1Document33 pagesAbdominal Examination 1Abhi BansalNo ratings yet
- Abdominal Examination Guide for Medical StudentsDocument9 pagesAbdominal Examination Guide for Medical StudentsAnonymous 278KLXQgI3No ratings yet
- Abdominal Assessment VideoDocument4 pagesAbdominal Assessment VideoAmber Nicole HubbardNo ratings yet
- Physical Assessment of Abdomen and RectumDocument41 pagesPhysical Assessment of Abdomen and RectumLeonilyn Dagoplo RN100% (1)
- Examination of Gastrointestinal SystemDocument37 pagesExamination of Gastrointestinal SystemayushiNo ratings yet
- No. Description of Actions To Be Done Score 0 1 2Document3 pagesNo. Description of Actions To Be Done Score 0 1 2Adiprayogo LiemenaNo ratings yet
- AbdomenDocument54 pagesAbdomenwkkevinnNo ratings yet
- Pemeriksaan Abdomen: Psik Fikes UmmDocument12 pagesPemeriksaan Abdomen: Psik Fikes UmmAbd RahmanNo ratings yet
- Notes On Physical Examination of AbdomenDocument6 pagesNotes On Physical Examination of AbdomenMarwa Al-AzzawiNo ratings yet
- Abdominal ExaminationDocument56 pagesAbdominal ExaminationAnggreani PutriNo ratings yet
- Abdominal Examination-1Document88 pagesAbdominal Examination-1naveen kumar kushwahaNo ratings yet
- Abdominal ExaminationDocument9 pagesAbdominal Examinationushapalem19No ratings yet
- Semester 1 Physical Examination Skills Lab Handout Abdominal Exam IDocument4 pagesSemester 1 Physical Examination Skills Lab Handout Abdominal Exam IFlowerNo ratings yet
- P.E. OF THE ABDOMEN - INSPECTION, AUSCULTATION, PERCUSSION, PALPATIONDocument12 pagesP.E. OF THE ABDOMEN - INSPECTION, AUSCULTATION, PERCUSSION, PALPATIONZeeham EscalonaNo ratings yet
- Abdominal Examination Jan 23Document36 pagesAbdominal Examination Jan 23Adel hassounNo ratings yet
- Abdomenal AssessmentDocument49 pagesAbdomenal AssessmenttiaNo ratings yet
- 2nd - GUT INFECTIONS & ABORTIONDocument24 pages2nd - GUT INFECTIONS & ABORTIONsrslytrdNo ratings yet
- 3rd - DIAGNOSTIC TESTDocument23 pages3rd - DIAGNOSTIC TESTsrslytrdNo ratings yet
- Assessing The Skull and FaceDocument11 pagesAssessing The Skull and FacesrslytrdNo ratings yet
- Rabies Prevention and Control ProgramDocument3 pagesRabies Prevention and Control ProgramsrslytrdNo ratings yet
- Kicks in SwimmingDocument17 pagesKicks in SwimmingsrslytrdNo ratings yet
- Assessing The NeckDocument18 pagesAssessing The NecksrslytrdNo ratings yet
- 7 10transesDocument10 pages7 10transessrslytrdNo ratings yet
- Sts-Reaction PaperDocument1 pageSts-Reaction PapersrslytrdNo ratings yet
- Thoracic Surgery: Cervical, Thoracic and Abdominal ApproachesDocument1,068 pagesThoracic Surgery: Cervical, Thoracic and Abdominal ApproachesAlexandru GibuNo ratings yet
- HPV Vaccination Against Cervical Cancer in Women Above 25 Years of AgeDocument9 pagesHPV Vaccination Against Cervical Cancer in Women Above 25 Years of Agegringo6969No ratings yet
- The Plot Against Asthma and Allergy PatientsDocument422 pagesThe Plot Against Asthma and Allergy PatientsAngelo100% (1)
- Prof. P. R. Vavia ResumeDocument50 pagesProf. P. R. Vavia ResumeGwen WalkerNo ratings yet
- Maternal DistressDocument7 pagesMaternal DistressBharat Thapa83% (6)
- WNHS OG PregnancyFirstTrimesterDocument60 pagesWNHS OG PregnancyFirstTrimesterBharata YudhaNo ratings yet
- Improvement of Pregnant Women Visit in Puskesmas As An Effect of Using Ultrasound in Pregnancy ExaminationDocument12 pagesImprovement of Pregnant Women Visit in Puskesmas As An Effect of Using Ultrasound in Pregnancy ExaminationKharinaNo ratings yet
- Comprehensive Geriatric Assessment Form: Monitor Action RequiredDocument1 pageComprehensive Geriatric Assessment Form: Monitor Action Requiredinno so qtNo ratings yet
- CASE PRES PreeclampsiaDocument51 pagesCASE PRES PreeclampsiaRaiza Love Caparas-PablicoNo ratings yet
- EBM TerapiDocument23 pagesEBM TerapidyahayulestariNo ratings yet
- HaemophiliaDocument15 pagesHaemophiliaSanmuga VimalanathanNo ratings yet
- NNVJHDocument94 pagesNNVJHAnda AlexandraNo ratings yet
- WFSA Craniopharyngioma Resection PDFDocument5 pagesWFSA Craniopharyngioma Resection PDFpitriaNo ratings yet
- Churnas DownDocument60 pagesChurnas DownAyyush RajalingaNo ratings yet
- FC Rad Onc (SA) Part II Past Papers - 2012 Mar 6-5-2014Document4 pagesFC Rad Onc (SA) Part II Past Papers - 2012 Mar 6-5-2014matentenNo ratings yet
- BeneHeart D6 Defibrillator Product BrochureDocument6 pagesBeneHeart D6 Defibrillator Product BrochureAdel KadyNo ratings yet
- Approach To Jaundice (1) .PPT ALAWAJIDocument28 pagesApproach To Jaundice (1) .PPT ALAWAJIayuNo ratings yet
- First Aid Multiple Choice Test Module 2Document2 pagesFirst Aid Multiple Choice Test Module 2Terrencio Reodava100% (1)
- Medical Test ProformaDocument2 pagesMedical Test Proformasavani VivekNo ratings yet
- Estimated Costs Related To The Birth of A Drug And/Or Alcohol Exposed BabyDocument15 pagesEstimated Costs Related To The Birth of A Drug And/Or Alcohol Exposed BabylosangelesNo ratings yet
- Scrub Nurse Mastectomy DutiesDocument6 pagesScrub Nurse Mastectomy DutiesJeroham R. CoNo ratings yet
- 1 +Theresia+Jamini+1-9Document9 pages1 +Theresia+Jamini+1-9Florentina yohana ngeluNo ratings yet
- Peptic Ulcer Dse PathophysiologyDocument19 pagesPeptic Ulcer Dse PathophysiologySymone Jay Lapiz100% (1)
- Date Performed: Final Grade: Clinical Instructor: Administering Eye Medication DefinitionDocument3 pagesDate Performed: Final Grade: Clinical Instructor: Administering Eye Medication Definitionhjl padillaNo ratings yet
- Clinical Handover and Patient Safety Literature Review Report 2005Document5 pagesClinical Handover and Patient Safety Literature Review Report 2005gw163ckjNo ratings yet