Professional Documents
Culture Documents
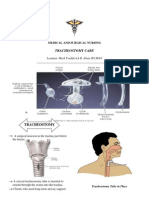
Tracheostomy Care
Uploaded by
Mica0 ratings0% found this document useful (0 votes)
2 views26 pagesOriginal Title
1. Tracheostomy Care
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
2 views26 pagesTracheostomy Care
Uploaded by
MicaCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 26
Tracheostomy is a surgical opening in the trachea
(windpipe) to make breathing easier
Opening is called a Stoma
Indications:
Mechanical ventilation
Failed endotracheal intubation
Large tumor of the head and neck
Types of Tracheostomy Tube
UNCUFFED- may be plastic or metal, which allows for air
to flow around the tube ( permanent tracheostomy)
CUFFED-are surrounded by an inflatable cuff that
produces an airtight seal between the tube and the
trachea.Often used immediately after a tracheostomy and
are essential when ventilating a tracheostomy client with a
mechanical ventilator.
FENESTRATED-has holes in the outer cannula. Is is used
when the client is being weaned (gradual discontinuation
of mechanical support)
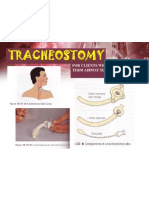
Parts of a Tracheostomy Tube
Tube with inner Cannula
PARTS OF TRACHEOSTOMY TUBE:
OUTER CANNULA – that is inserted to the trachea
INNER CANNULA – may be removed for periodic cleaning
NECK PLATE ( FLANGE) – rests against the neck and allows the
tube to be secured in place with tape or ties
OBTURATOR – used to insert the outer cannula and then
removed; it is kept at the client’s bedside in case the tube
becomes dislodged and needs to be reinserted
CUFF – produces an airtight seal between the tube and the
trachea. This seal prevents aspiration of oropharyngeal
secretions and air leakage between the tube and the trachea
FENESTRATION- hole in the outer cannula
Tracheostomy Ties
Types: twill, Velcro, metal bead
ADVANTAGES:
1.) maintains airway patency
2.) maintains cleanliness and prevents infection at the tracheostomy
site
3.) facilitates healing and prevents skin excoriation around the
tracheostomy incision
4.) promotes comfort
DISADVANTAGE:
- air is no longer filtered and humidified; special precautions are
necessary
Solution:
-wear a light scarf or 4x4 inch gauze held in place with a cotton twill
ties over the stoma to filter the air
Nursing Responsibilities:
Provide tracheostomy care at least every 8 hrs after the initial
inflammatory response
Hyperoxygenate the client and perform suctioning to remove
secretions from the lumen of the tube (10-15 secs.)( total time –
5 mins.)
If an inner cannula is present, remove and clean and replace
with a new one
Sterile technique must be observed all through out the
procedure
Asesssment of the peristomal skin and incision site must be
done and notify the Physician for any abnormalities.
Suctioning
When: Suction as necessary
Maintain a patent airway and prevent airway
obstruction
Promote respiratory function (optimal exchange of
O2 and CO2 into and out of the lungs)
Prevent pneumonia that may result from
accumulated secretions
Complications:
hypoxemia, trauma to airway, cardiac dysrhythmia
related to hypoxemia
Suctioning stimulates cough reflex and stimulates
mucus production
IT SHOULD ONLY BE DONE WHEN BREATH
SOUNDS INICATE THAT THE NEED IS PRESENT!
The diameter of the suction catheter should be
about half the inside diameter of the tracheostomy
tube to prevent hypoxia
Materials:
- Resuscitation bag (Ambu bag) connected to 100%
Oxygen)
- Sterile towel
- Suction machine
- Suction catheter
- Sterile Gloves
- Sterile Water for flushing
- Goggles/ Gown if necessary
- Moisture-resistant bag
Steps:
Asses the need for suctioning.
Greet the patient, explain the procedure.
Place the patient in Semi-fowler’s position to
promote breathing, maximum lung expansion,
and productive coughing.
Prepare the equipments.
Attach the resuscitation apparatus to the
oxygen source.
Open the sterile supplies in readiness for use
Put on sterile glove
Place sterile towel across the patient’s chest.
Hyperoxigenate the patient before, during and
after the procedure.
Flush and lubricate the Suction catheter.
Press the Ambu Bag 3-5 times as the client inhales.
Quickly but gently insert the catheter (6 in.,
without applying suction) until the client coughs
or if you feel resistance.
If resistance is felt, withdraw the tube for about 1-2
cm before applying suction.
Perform suctioning.
Apply intermittent suction about 5-10 sec.
Rotate the catheter while withdrawing to prevent
tissue trauma.
Hyperventilate the patient.
If the secretion is thick, flush the catheter.
Reassess the patient’s oxygenation status and
repeat suctioning as needed.
Allow 2-3 minutes between suction as possible to
provide the opportunity for reoxygenation of the
lungs.
Repeat until the air passage is clear and the
breathing is effortless and quiet.
After each suction, ventilate the patient with 5
breaths.
Dispose equipments
Provide client’s comfort and safety
Document.
Cleaning a Double-Cannula Tube/ Changing a
Tracheostomy dressing and ties
When: dressing is soiled- harbors microorganisms
and source of skin breakdown, and infection.
Check order of doctor if there is an order for
antibiotic ointment to the stoma.
When: excessive secretions, soiled tracheostomy
dressing or ties, labored breathing indicating
diminished air flow through trach tube
To maintain cleanliness and prevent infection at
the tracheostomy site.
To maintain airway patency.
To prevent skin breakdown around the stoma.
Steps:
Assess the need for cleaning the stoma.
Greet the patient, explain the procedure.
Prepare the equipments.
Don gloves and suction if indicated.
Remove the soiled dressing using pick up forceps.
Remove the inner cannula (counter clockwise) by
gently pulling it towards you and in line with its
curvature.
Soak the inner cannula in diluted Hydrogen
peroxide to moisten and loosen secretions.
Put oxygen source.
Clean the flange and the stoma using sterile
water/saline. Pat dry.
Change gloves and replace it with sterile gloves.
Remove the cannula from the soaking solution.
Clean the lumen and entire inner cannula
thoroughly.
Agitate in sterile saline.
Inspect the cannula for cleanliness by holding it at
the eye level and looking through it into the light.
After rinsing the cannula, gently tap it against the
inside edge of the sterile solution bowl.
Dry inside of cannula.
Insert the inner cannula and secure it.
Place a sterile dressing.
• To make a tracheostomy dressing from a 4 x 4
gauze, open gauze to an 8” x 4”size, then fold
lengthwise.
• Fold gauze corners up.
• Slide folded gauze under tracheostomy strings.
Change ties.
Document relevant data.
You might also like
- Tracheostomy: ENT Department DMC & Hospital Ludhiana PunjabDocument46 pagesTracheostomy: ENT Department DMC & Hospital Ludhiana PunjabVikrant MittalNo ratings yet
- Tracheostomy Care: Medical and Surgical NursingDocument3 pagesTracheostomy Care: Medical and Surgical NursingLorina Lynne Apelacio100% (1)
- Tracheostomy: Presented By: Barte, Hannah Aida D. Balamurugan, RameebhaDocument21 pagesTracheostomy: Presented By: Barte, Hannah Aida D. Balamurugan, RameebhaThakoon Tts100% (1)
- Tracheostomy CareDocument41 pagesTracheostomy CareBautista Aubergine100% (2)
- Tracheostomy CareDocument15 pagesTracheostomy CareZabeth ZabNo ratings yet
- Care During ECT Procedure: Submitted To: Priyanka Madam Submitted By: Ujjwal SadanshivDocument4 pagesCare During ECT Procedure: Submitted To: Priyanka Madam Submitted By: Ujjwal SadanshivUjjwal SadanshivNo ratings yet
- TracheostomyDocument4 pagesTracheostomyNapieh Bulalaque PolisticoNo ratings yet
- TRACHEOSTOMYDocument109 pagesTRACHEOSTOMYJayson RN92% (12)
- TracheostomyDocument17 pagesTracheostomyCalimlim KimNo ratings yet
- Tracheostomy Care GuidelinesDocument15 pagesTracheostomy Care Guidelinesnurseuragon92% (25)
- Tracheostomy CareDocument22 pagesTracheostomy CareHollan Galicia100% (1)
- Tracheostomy SuctioningDocument59 pagesTracheostomy SuctioningMaan LapitanNo ratings yet
- Skills 112 TRACHEOSTOMYDocument60 pagesSkills 112 TRACHEOSTOMYKirstin del CarmenNo ratings yet
- Tracheostomy Tubesuctioning2 MikeDocument29 pagesTracheostomy Tubesuctioning2 MikeClaudia VillalunaNo ratings yet
- Bi-Rads: (Breast Imaging-Reporting and Data System)Document30 pagesBi-Rads: (Breast Imaging-Reporting and Data System)Siti NirwanahNo ratings yet
- Assignment ON Tracheostom Y Care: Submitted To: Submitted byDocument5 pagesAssignment ON Tracheostom Y Care: Submitted To: Submitted byAnanthibala100% (1)
- Tracheostomy Care (Done)Document53 pagesTracheostomy Care (Done)martinNo ratings yet
- Inguinal HerniaDocument33 pagesInguinal Herniatianally100% (2)
- TracheostomyDocument6 pagesTracheostomynamithaNo ratings yet
- Tracheostomy Slide Presentation-ZayChung - Pro.ksaDocument33 pagesTracheostomy Slide Presentation-ZayChung - Pro.ksaZayChung100% (2)
- Hypo & HyperthyroidismDocument33 pagesHypo & HyperthyroidismSuchit Kumar50% (2)
- Tracheostomy Care: Presented by Sital B. Sharma M SC Nursing Student College of Nursing. N.B.M.C.HDocument74 pagesTracheostomy Care: Presented by Sital B. Sharma M SC Nursing Student College of Nursing. N.B.M.C.HShetal Sharma100% (1)
- Tracheostomy CareDocument37 pagesTracheostomy Carepreet kaurNo ratings yet
- TÉCNICAS DEL AUXILIAR DE ENFERMERÍA EN EL ÁREA DE QUIRÓFANOFrom EverandTÉCNICAS DEL AUXILIAR DE ENFERMERÍA EN EL ÁREA DE QUIRÓFANONo ratings yet
- Issaiah Nicolle L. Cecilia 3 BSN - ADocument6 pagesIssaiah Nicolle L. Cecilia 3 BSN - AIssaiah Nicolle CeciliaNo ratings yet
- Issaiah Nicolle L. Cecilia 3 BSN - ADocument14 pagesIssaiah Nicolle L. Cecilia 3 BSN - AIssaiah Nicolle CeciliaNo ratings yet
- Tracheostomy CareDocument4 pagesTracheostomy CareZar Ybañez MabanagNo ratings yet
- TracheostomyDocument8 pagesTracheostomySeree Nah TRNo ratings yet
- Skills (Tracheostomy Care)Document5 pagesSkills (Tracheostomy Care)kimtalaNo ratings yet
- Tracheostomy CareDocument25 pagesTracheostomy Caremelanie silvaNo ratings yet
- TRACHEOSTOMYDocument4 pagesTRACHEOSTOMYPrecious BlessingNo ratings yet
- ET TubeDocument4 pagesET TuberumasadraunaNo ratings yet
- Tracheostomy CareDocument45 pagesTracheostomy Caredrnasir31No ratings yet
- College of Nursing: (Dalubhasaan NG Narsing)Document10 pagesCollege of Nursing: (Dalubhasaan NG Narsing)Kimmy NgNo ratings yet
- Respi Modalities 2Document6 pagesRespi Modalities 2Karlo ReyesNo ratings yet
- Airway ManagementDocument16 pagesAirway ManagementSuganthi ParthibanNo ratings yet
- Tracheostomy CareDocument15 pagesTracheostomy CareJanedear PasalNo ratings yet
- What Is A Tracheostomy? Why Is A Tracheostomy Performed?Document5 pagesWhat Is A Tracheostomy? Why Is A Tracheostomy Performed?Mara JnelleNo ratings yet
- Nasogastric Feeding TubeDocument7 pagesNasogastric Feeding Tubepatrayati90No ratings yet
- Tracheostomy CareDocument8 pagesTracheostomy CareAlvin L. RozierNo ratings yet
- TracheostomyDocument4 pagesTracheostomySuchismita SethiNo ratings yet
- TRACHEOSTOMYDocument2 pagesTRACHEOSTOMY3C SAVELLA, Glaiza Marie RNo ratings yet
- MedSurg NotesDocument57 pagesMedSurg NotesCHRISTOFER CORONADONo ratings yet
- 2021 - 2022 Tracheostomy Care ProcedureDocument69 pages2021 - 2022 Tracheostomy Care ProcedureMelinda Cariño BallonNo ratings yet
- 2021 - 2022 Tracheostomy Care ProcedureDocument69 pages2021 - 2022 Tracheostomy Care ProcedureMelinda Cariño BallonNo ratings yet
- Skills 112 TRACHEOSTOMYDocument52 pagesSkills 112 TRACHEOSTOMYJaynell Ann SabioNo ratings yet
- Laboratory Unit 4Document4 pagesLaboratory Unit 4Mushy_ayaNo ratings yet
- Airway SuctionDocument47 pagesAirway SuctionMaheshNo ratings yet
- Tracheostomy CareDocument15 pagesTracheostomy CareZabeth ZabNo ratings yet
- Tracheostomy CareDocument5 pagesTracheostomy CareLoren SarigumbaNo ratings yet
- Tracheostomy CareDocument11 pagesTracheostomy CareRiza Angela Barazan100% (1)
- Tracheostomy Care SkillDocument5 pagesTracheostomy Care SkillAmina Sahar 08No ratings yet
- Tracheostomy Care Is AssignmentDocument3 pagesTracheostomy Care Is Assignmentchaudharitrushar007No ratings yet
- Trache CareDocument3 pagesTrache CareChonkayshek Rias BarrunNo ratings yet
- SuctioningDocument23 pagesSuctioningAketch ItoNo ratings yet
- Tracheostomy: Done By: Sami FreijyDocument14 pagesTracheostomy: Done By: Sami FreijySami FreijyNo ratings yet
- Skills 112 TRACHEOSTOMYDocument60 pagesSkills 112 TRACHEOSTOMYJemy Tamaño MorongNo ratings yet
- Tracheostomy Care: Surgical Ward Matalines - Mua - Rangas - Tan.SDocument15 pagesTracheostomy Care: Surgical Ward Matalines - Mua - Rangas - Tan.SMARIANN JEAN ANDREA CULANAG MATALINESNo ratings yet
- Sudden Death SyndromeDocument72 pagesSudden Death SyndromeStella CooKeyNo ratings yet
- The HeartDocument58 pagesThe HeartJULIUS NAKANYALANo ratings yet
- Thoracic Outlet SyndromeDocument16 pagesThoracic Outlet SyndromeDeepak RajNo ratings yet
- Department of Radiology: Ultrasound - Whole AbdomenDocument2 pagesDepartment of Radiology: Ultrasound - Whole AbdomenLeoThomasNo ratings yet
- Section 3: Shivering: Risks Associated With Your AnaestheticDocument5 pagesSection 3: Shivering: Risks Associated With Your AnaestheticDadanaja AjaNo ratings yet
- Bedah MukogingivalDocument35 pagesBedah MukogingivalVanya FionaNo ratings yet
- Five To 10-Year Followup of Open Partial Nephrectomy in A Solitary KidneyDocument5 pagesFive To 10-Year Followup of Open Partial Nephrectomy in A Solitary KidneyMihaela LitovcencoNo ratings yet
- Uti CPG 2Document36 pagesUti CPG 2Yohan VeissmanNo ratings yet
- Applications of Diode Lasers in Dentistry - Dr. Shripal ShahDocument52 pagesApplications of Diode Lasers in Dentistry - Dr. Shripal ShahDr Shripal ShahNo ratings yet
- Pterygium SurgeryDocument7 pagesPterygium SurgeryEndrico Xavierees TungkaNo ratings yet
- Kidney TransplantDocument47 pagesKidney TransplantSandhya HarbolaNo ratings yet
- Frog Dissection LabDocument7 pagesFrog Dissection LabJhane FigueroaNo ratings yet
- Thoracic Trauma - Principals of Surgical Management: Jerzy Lasek, Eugeniusz JadczukDocument9 pagesThoracic Trauma - Principals of Surgical Management: Jerzy Lasek, Eugeniusz JadczukAnangova PradiptaNo ratings yet
- Knowledge, Awareness and Practice On Application of Presurgical Nasoalveolar Moulding For Cleft Lip and Palate PatientsDocument8 pagesKnowledge, Awareness and Practice On Application of Presurgical Nasoalveolar Moulding For Cleft Lip and Palate PatientsArshid KhandayNo ratings yet
- 2021 Article JapaneseGastricCancerTreatmentDocument21 pages2021 Article JapaneseGastricCancerTreatmentciuca bogdanNo ratings yet
- AOFASDocument5 pagesAOFASAlessandro MedinaNo ratings yet
- Retinopathy of Prematurity - HandoutDocument2 pagesRetinopathy of Prematurity - Handoutmusara87No ratings yet
- MAGNETOM Symphony Tim CoilsDocument18 pagesMAGNETOM Symphony Tim CoilshgaucherNo ratings yet
- Otat Log BookDocument8 pagesOtat Log BookDr KamaleshNo ratings yet
- Class III MalocclusionDocument45 pagesClass III Malocclusionمينا عمار شكري محمودNo ratings yet
- Quiz BSN 4Document1 pageQuiz BSN 4Mae Marie Jambaro-TuaNo ratings yet
- ASCCP Colposcopy Standards Role of Colposcopy,.3Document7 pagesASCCP Colposcopy Standards Role of Colposcopy,.3Laura Milagros Apóstol A.No ratings yet
- 0041-Arthroscopic Versus Open Lateral Ankle Ligament Repair-A Systematic Review of Outcomes During Short To Medium TermDocument6 pages0041-Arthroscopic Versus Open Lateral Ankle Ligament Repair-A Systematic Review of Outcomes During Short To Medium TermsiegekeronNo ratings yet
- Capsule EndosDocument25 pagesCapsule EndosAnonymous Z3sU48No ratings yet
- Hip Fractures: Types of Fracture and AnatomyDocument9 pagesHip Fractures: Types of Fracture and AnatomySim M ChangNo ratings yet
- Curs Prim Ajutor 2023 - MG An V - Șocul Hemoragic - English-1Document18 pagesCurs Prim Ajutor 2023 - MG An V - Șocul Hemoragic - English-1hulia jokoNo ratings yet
- List of Amhs AmasDocument11 pagesList of Amhs AmasNaveenkumar PalanisamyNo ratings yet
- Case Report Enlargement GinggivaDocument3 pagesCase Report Enlargement GinggivaAnindya LaksmiNo ratings yet