Professional Documents
Culture Documents
Anatomy of Vertebral Coulmn
Uploaded by
sanullah123khan.130 ratings0% found this document useful (0 votes)
2 views30 pagesits about anatomy first semester
Original Title
Anatomy of vertebral coulmn
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentits about anatomy first semester
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
2 views30 pagesAnatomy of Vertebral Coulmn
Uploaded by
sanullah123khan.13its about anatomy first semester
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 30
VERTEBRAL COLUMN
The vertebral column consists
of 33 vertebrae:
• 7 cervical,
• 12 thoracic,
• 5 lumbar,
• 5 fused sacral,
• 4 fused coccygeal vertebrae
It protects the spinal cord,
supports the weight of the head
and the trunk, and allows the
movement of the rib cage for
respiration by articulating with
the ribs.
TYPICAL VERTEBRA
Typical cervical vertebrae (C3 – C5)
1. The body is small and broader from
side to side than from before
backwards.
2. Vertebral foramen is
larger than the body. It is
triangular in shape.
3. Each cervical vertebra has the oval
foramen transversarium in the
transverse process. The vertebral
arteries and their accompanying
veins pass through the transverse
foramina.
4. The transverse processes of cervical
vertebrae end laterally in two
projections: an anterior tubercle and
a posterior tubercle.
5. The spine is short and bifid. The
notch is filled up by the ligamentum
nuchae.
FIRST CERVICAL VERTEBRA ( С 1, Atlas)
that Atlas of Greek mythology bore the weight of the world on his shoulders
1. It has neither a body nor a spine process.
2. This ring-shaped body has paired lateral masses.
3. The kidney-shaped, concave superior articular surfaces articulate with
occipital condyles.
4. Anterior and posterior arches, each of which bears a tubercle in the center
of its external aspect.
5. Anterior arche on posterior surface bears an oval facet which articulates with
the dens.
6. The posterior arch has a wide groove for the vertebral artery on its superior
surface.
SECOND CERVICAL VERTEBRA (С2, axis)
• It is identified by the presence of the dens or odontoid process.
SIXTH CERVICAL VERTEBRAES (С6)
• The anterior tubercles of vertebra C6 are
called carotid tubercles because the
common carotid arteries may be
compressed here, in the groove between
the tubercle and body, to control bleeding
from these vessels.
SEVENTH CERVICAL VERTEBRAES (C7)
• is also known as the vertebra prominens because of its long spinous process. Run
your finger along the midline of the posterior aspect of your neck until you feel the
prominent C7 spinous process.
• The spinal process is not bifid on the end.
• The foramina transversaria are smaller in C7 than those in other cervical vertebrae,
and occasionally they are absent (because it transmit only small accessory veins).
The typical thoracic vertebrae (Th2-Th8) are:
• identified by the presence of costal facets (superior and inferior demifacets) on
the sides of the vertebral bodies;
• the articular processes of thoracic vertebrae extend vertically with paired,
nearly coronally oriented articular facets;
• the anterior surface of each transverse process bears a facet near its tip, for
articulation with the tubercle of the corresponding rib;
• the spine is long, and is directed downwards and backwards
Atypical thoracic vertebrae:
Th 1 - The superior costal facet
on the body is complete. It
articulates with the head of the
first rib. The inferior costal facet
is a demifacet for the second rib.
Th 9 - the body has a single
superior costal demifacet on
each side.
Th 10 - the body has a single large
costal facet on each side.
Th 11 - The body has a single large
costal facet on each side. The
transverse process is small, and
doesn’t have articular facet.
Th 12 - The transverse processes and
spine are similar to those of a lumbar
vertebra. The body has a single costal
facet on each side. The transverse
process is small, and doesn’t have
articular facet.
Typical lumbar Vertebrae
• Because the weight they support
increases toward the inferior end of the
vertebral column, lumbar vertebrae
have massive bodies;
• their articular processes extend
vertically;
• the transverse processes are thin and
tapering, has a small, rough elevation,
the accessory process;
• the superior articular processes has a
rough elevation, the mammillary
process.
• the vertebral foramen is triangular in
shape, and is larger than in the thoracic
region;
• the spine is thickened along its
posterior and inferior borders.
THE SACRUM
• is usually composed of five fused sacral vertebrae in adults;
• provides strength and stability to the pelvis and transmits the
weight of the body to the pelvic girdle;
• the anterior (pelvic) sacral foramina are larger than the
posterior (dorsal) ones;
• the sacrum supports the vertebral column and forms the
posterior part of the bony pelvis;
• the median sacral crest, represents the fused rudimentary
spinous processes;
• the intermediate sacral crests represent the fused articular
processes;
• the lateral sacral crests represent the fused transvers
processes.
Coccyx
• the coccyx (tail bone) is a small triangular
bone that is usually formed by fusion of the
four rudimentary coccygeal vertebrae;
• the coccyx is the remnant of the skeleton of
the embryonic tail-like caudal eminence,
which is present in human embryos from the
end of the 4th week until the beginning of the
8th week;
• Co1 is the largest and broadest of all the
coccygeal vertebrae.
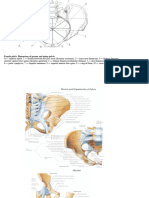
Development of the vertebral
column
In a frontal section of a 4-week
embryo, the sclerotomes appear as
paired condensations of
mesenchymal cells around the
notochord. Each sclerotome consists
of loosely arranged cells cranially
and densely packed cells caudally.
Cartilaginous Stage of Vertebral Development
During the sixth week, chondrification centers appear in each
mesenchymal vertebra.
The two centers in each centrum fuse at the end of the embryonic
period to form a cartilaginous centrum. Concomitantly, the centers in
the neural arches fuse with each other and the centrum. The spinous
and transverse processes develop from extensions of chondrification
centers in the neural arch. Chondrification spreads until a cartilaginous
vertebral column is formed.
Bony Stage of Vertebral Development
Ossification of typical vertebrae begins during the embryonic period and
usually ends by the 25th year. There are two primary ossification centers,
ventral and dorsal, for the centrum.
These primary ossification centers soon fuse to form one center. Three
primary centers are present by the end of the embryonic period:
• one in the centrum
• one in each half of the neural arch.
Ossification becomes evident in the neural arches during the eighth week.
At birth, each vertebra consists of three bony
parts connected by cartilage.
The bony halves of the vertebral arch usually
fuse during the first 3 to 5 years. The arches first
unite in the lumbar region, and union progresses
cranially.
Five secondary ossification centers appear in the
vertebrae after puberty:
One for the tip of the spinous process
One for the tip of each transverse process
Two anular epiphyses, one on the superior and one on
the inferior rim of the vertebral body.
All secondary centers unite with the rest of the vertebra
at approximately 25 years of age.
Clinical anatomy:
Cervical ribs
• The costal element of seventh
cervical vertebra may get
enlarged to form a cervical
rib.
• The extra rib may elevate and
place pressure on structures
that emerge from the
superior thoracic aperture,
notably the subclavian artery
or inferior trunk of the
brachial plexus, and may
cause thoracic outlet
syndrome.
Variation in the Number of Vertebrae
A few have one or two additional vertebrae or
one fewer. To determine the number of
vertebrae, it is necessary to examine the entire
vertebral column because an apparent extra (or
absent) vertebra in one segment of the column
may be compensated for by an absent (or extra)
vertebra in an adjacent segment; for example,
11 thoracic-type vertebrae with 6 lumbar-type
vertebrae.
Abnormal Fusion of Vertebrae
• In approximately 5% of
people, L5 is partly or
completely incorporated into
the sacrum—conditions
known as hemisacralization
and sacralization of the L5
vertebra.
• S1 is more or less separated
from the sacrum and is partly
or completely fused with L5
vertebra, which is called
lumbarization of the S1
vertebra.
Often producing painful
symptoms.
• Atlas may fuse with the
occipital bone. This is called
occipitalization of atlas.
Caudal Epidural Anesthesia
Is a local anesthetic agent is injected into the fat of the sacral
canal that surrounds the proximal portions of the sacral nerves.
Anesthetic agents can also be injected through the posterior
sacral foramina into the sacral canal around the spinal nerve
roots (transsacral epidural anesthesia).
Laminectomy
The surgical excision of one or
more spinous processes and
the adjacent supporting
vertebral laminae in a
particular region of the
vertebral column is called a
laminectomy.
Surgical laminectomy is often
performed to relieve pressure
on the spinal cord or nerve
roots caused by a tumor.
Lumbar Spinal Stenosis
narrow vertebral foramen in one or more lumbar
vertebrae. Narrowing is usually maximal at the level of
the IV discs. Stenosis of a lumbar vertebral foramen
alone may cause compression of one or more of the
spinal nerve roots occupying the inferior vertebral
canal.
• Spina bifida occulta, in which the
neural arches of L5 and/or S1 fail to
develop normally and fuse
posterior to the vertebral canal. The
defect is concealed by the overlying
skin, but its location is often
indicated by a tuft of hair. Most
people with spina bifida occulta
have no back problems.
• Spina bifida cystica, one or
more vertebral arches may fail
to develop completely. Spina
bifida cystica is associated with
herniation of the meninges
(meningocele) and/or the spinal
cord (meningomyelocele).
Neurological symptoms are
usually present in severe cases
of meningomyelocele (e.g.,
paralysis of the limbs and
disturbances in bladder and
bowel control). Severe forms of
spina bifida result from neural
tube defects, such as the
defective closure of the neural
tube during the 4th week of
embryonic development.
You might also like
- Positioning Presentation-VertebraeDocument156 pagesPositioning Presentation-Vertebraeron reteracionNo ratings yet
- Vertebral ColumnDocument64 pagesVertebral ColumnJavin BissoondyalNo ratings yet
- 9. المحاضرة التاسعة - مادة التشريح العام - المرحلة الاولىDocument6 pages9. المحاضرة التاسعة - مادة التشريح العام - المرحلة الاولىAbdullah TheNo ratings yet
- THEVERTEBRALCOLUMNDocument29 pagesTHEVERTEBRALCOLUMNpreetam912002.22No ratings yet
- Lecture 7Document14 pagesLecture 7فيصل بوعبيدNo ratings yet
- Anatomy of The SpineDocument11 pagesAnatomy of The SpineAnna NanyangweNo ratings yet
- Hyoid BoneDocument14 pagesHyoid BoneAl-Shuaib Astami SonNo ratings yet
- Vertebrae-and-Appendicular-ANAPHY-AND-PHYSIODocument10 pagesVertebrae-and-Appendicular-ANAPHY-AND-PHYSIOshannenmaehfajanilanNo ratings yet
- Vertebra: StructureDocument9 pagesVertebra: StructureayudhyaNo ratings yet
- Chapter 1-Musculoskeletal SystemDocument113 pagesChapter 1-Musculoskeletal SystemWang Ming YaNo ratings yet
- Anatomy Lect of Chest and RibsDocument17 pagesAnatomy Lect of Chest and Ribssanullah123khan.13No ratings yet
- Anatomy Week 3 NotesDocument32 pagesAnatomy Week 3 NotesBasil AdeelNo ratings yet
- Anatomy of The SpineDocument5 pagesAnatomy of The SpineShane ShaneNo ratings yet
- Thoracic Wall: by Professor NzarubaraDocument76 pagesThoracic Wall: by Professor NzarubaraEsdras DountioNo ratings yet
- Week 4Document138 pagesWeek 4Anne nicole P. CasemNo ratings yet
- Ribs-and-Vertebra-bonesDocument97 pagesRibs-and-Vertebra-bonesJerlyns OmondiNo ratings yet
- The Back: Cortez Gomez Lucas VillafuerteDocument53 pagesThe Back: Cortez Gomez Lucas VillafuerteFlorenze Laiza Donor LucasNo ratings yet
- Bones & Joints of the Spine ExplainedDocument83 pagesBones & Joints of the Spine ExplainedJoy SahaNo ratings yet
- Anatomy of SpineDocument77 pagesAnatomy of SpineJoy SahaNo ratings yet
- respiratory system anatomy for other health scienceDocument165 pagesrespiratory system anatomy for other health scienceahmedmustefa773No ratings yet
- Biomechanics of The Vertebral ColumnDocument44 pagesBiomechanics of The Vertebral ColumnVijay PradeepNo ratings yet
- Cervical SpondylosisDocument46 pagesCervical SpondylosisWalter Burton100% (1)
- ANATOMY I 20.03.20 I Thoracic CageDocument23 pagesANATOMY I 20.03.20 I Thoracic CageArianna RomanoNo ratings yet
- NeckDocument215 pagesNeckpilot abdi baariNo ratings yet
- Vertebral Column and Spine AnatomyDocument86 pagesVertebral Column and Spine AnatomyHà Quang SơnNo ratings yet
- المحاضرة العاشرة مادة التشريح العام - المرحلة الاولى طب اسنانDocument9 pagesالمحاضرة العاشرة مادة التشريح العام - المرحلة الاولى طب اسنانAbdullah TheNo ratings yet
- Cervical Spondylosis PDFDocument46 pagesCervical Spondylosis PDFMadalinaTamasNo ratings yet
- Development of VertebraeDocument21 pagesDevelopment of Vertebraefilza farheenNo ratings yet
- AbdomenDocument55 pagesAbdomenmokakkhan586No ratings yet
- Vertebral Column and Sinuses Handout DR Wael ElsaedDocument8 pagesVertebral Column and Sinuses Handout DR Wael Elsaedفراج - FarragNo ratings yet
- Masters of physiotherapy introduce thoracic bonesDocument30 pagesMasters of physiotherapy introduce thoracic bonesShikha SagarNo ratings yet
- Skeletal System Notes 2023Document16 pagesSkeletal System Notes 2023shinamaejNo ratings yet
- Anatomy of the Pelvis and Hip JointDocument63 pagesAnatomy of the Pelvis and Hip JointEliud MbuteNo ratings yet
- 5.axial SkeletonDocument63 pages5.axial Skeletonhuzaifa arshadNo ratings yet
- Hafizah Binti Mohd Hoshni Musculoskeletal Anatomy Skeleton of The ThoraxDocument28 pagesHafizah Binti Mohd Hoshni Musculoskeletal Anatomy Skeleton of The ThoraxhafizahhoshniNo ratings yet
- OsteologyDocument38 pagesOsteologyERIAS TENYWANo ratings yet
- Thoracic vertebrae anatomy and functionsDocument4 pagesThoracic vertebrae anatomy and functionsNeirfla WassabiNo ratings yet
- Anatomy and Physiology of The SpineDocument12 pagesAnatomy and Physiology of The SpineKinahZildredBibitNo ratings yet
- Anatomy of The Female Reproductive SystemDocument41 pagesAnatomy of The Female Reproductive SystemMahad Maxamed AxmedNo ratings yet
- Appendiculars (2015 - 06 - 09 20 - 43 - 48 Utc)Document183 pagesAppendiculars (2015 - 06 - 09 20 - 43 - 48 Utc)DiazNo ratings yet
- Pedicles Are Short Projections, From The Superior Part of The Vertebral Body To TheDocument3 pagesPedicles Are Short Projections, From The Superior Part of The Vertebral Body To ThebarbacumlaudeNo ratings yet
- The Thorax and Chest WallDocument15 pagesThe Thorax and Chest WallVIRESH VNo ratings yet
- Dissector Answers - Deep Back & Spinal CordDocument9 pagesDissector Answers - Deep Back & Spinal CordUloko ChristopherNo ratings yet
- Vertebra Anatomy 125Document110 pagesVertebra Anatomy 125Jennifer FirestoneNo ratings yet
- ThoraxDocument54 pagesThoraxfalz0012kNo ratings yet
- Thoracic Cage Components and JointsDocument30 pagesThoracic Cage Components and JointsSiva ShanmugamNo ratings yet
- Bones of The Back RegionDocument9 pagesBones of The Back Regionyachiru121No ratings yet
- Share '1579792243522 - Lecture 2Document21 pagesShare '1579792243522 - Lecture 2MOHAMMAD ALSWEITYNo ratings yet
- The Vertebral Column Anatomy and PositioningDocument93 pagesThe Vertebral Column Anatomy and Positioningwintleah4No ratings yet
- Ul PDFDocument8 pagesUl PDFNourhan ShabanNo ratings yet
- The Anatomy of the ThoraxDocument237 pagesThe Anatomy of the ThoraxAbel Belete100% (1)
- Anatomy and Physiology of The Spinal CordDocument4 pagesAnatomy and Physiology of The Spinal CordAla'a Emerald AguamNo ratings yet
- Exp 12 PDFDocument16 pagesExp 12 PDFKath BarcelonaNo ratings yet
- The Thorax: Axial & Appendicular Skeleton Mammary Glands Surface AnatomyDocument28 pagesThe Thorax: Axial & Appendicular Skeleton Mammary Glands Surface AnatomyDr-Arsalan ZahidNo ratings yet
- SPONDYLOLISTHESISDocument46 pagesSPONDYLOLISTHESISJino Alex100% (1)
- The Ligamentum Flavum:: Present Throughout Vertebral ColumnDocument9 pagesThe Ligamentum Flavum:: Present Throughout Vertebral ColumnUmar JawadNo ratings yet
- Pelvis Bones: Coccyx, Which Form A Bony Ring. Ilium Pubis The IschiumDocument14 pagesPelvis Bones: Coccyx, Which Form A Bony Ring. Ilium Pubis The IschiumNourhan ShabanNo ratings yet
- PDF Cervical Spine AnatomyDocument71 pagesPDF Cervical Spine AnatomyAqilla Fadia HayaNo ratings yet
- The Female Pelvis: Namasinga JoyceDocument79 pagesThe Female Pelvis: Namasinga JoyceNamaganda NajjatiNo ratings yet
- Joints of The Lower Limb DiagramsDocument8 pagesJoints of The Lower Limb Diagramssanullah123khan.13No ratings yet
- Joints of The Lower Limb DiagramsDocument39 pagesJoints of The Lower Limb Diagramssanullah123khan.13No ratings yet
- Anatomy of Skull DiagramsDocument10 pagesAnatomy of Skull Diagramssanullah123khan.13No ratings yet
- Anatomy Lect of SkullDocument57 pagesAnatomy Lect of Skullsanullah123khan.13No ratings yet
- Anatomy Lect of Skull 2Document36 pagesAnatomy Lect of Skull 2sanullah123khan.13No ratings yet
- Anatomy Lect of Chest and RibsDocument17 pagesAnatomy Lect of Chest and Ribssanullah123khan.13No ratings yet
- Richard MillerDocument309 pagesRichard MillerCamila Rabelo98% (48)
- The Respiratory System: Supplement To Text, Chapter 9Document77 pagesThe Respiratory System: Supplement To Text, Chapter 9Christina GonezNo ratings yet
- Muscles of The ThoraxDocument4 pagesMuscles of The ThoraxKieth Roland PalosoNo ratings yet
- Respiratory System Test PDFDocument9 pagesRespiratory System Test PDFMonique Mavronicolas50% (2)
- (Ebook - Martial-Arts) Pressure Points - Military Hand To Ha PDFDocument27 pages(Ebook - Martial-Arts) Pressure Points - Military Hand To Ha PDFDragos-Cristian FinaruNo ratings yet
- Pilates For Menopause On The Mat ONLINE MANUAL PDFDocument96 pagesPilates For Menopause On The Mat ONLINE MANUAL PDFkulsoomNo ratings yet
- Normal and Abnormal Findings of Thorax and LungsDocument3 pagesNormal and Abnormal Findings of Thorax and LungsOtherin Ojibwa TejanoNo ratings yet
- SKELETON ANATOMY QUIZDocument8 pagesSKELETON ANATOMY QUIZRonnith NandyNo ratings yet
- School: Grade Level:: Caigangan Elementary School IVDocument7 pagesSchool: Grade Level:: Caigangan Elementary School IVMark-Christopher Roi Pelobello MontemayorNo ratings yet
- The Skeletal System Human Body (206) Axial Skeleton (80) Skull (28) A. Paired Bones (11x2 22)Document17 pagesThe Skeletal System Human Body (206) Axial Skeleton (80) Skull (28) A. Paired Bones (11x2 22)Leo Cordel Jr.No ratings yet
- Respiration: 1.1 Human Breathing MechanismDocument3 pagesRespiration: 1.1 Human Breathing MechanismHalizah RamthanNo ratings yet
- Ammonites EcuadorDocument10 pagesAmmonites EcuadorHarry JonitzNo ratings yet
- Maders Understanding Human Anatomy and Physiology 9th Edition Longenbaker Test BankDocument59 pagesMaders Understanding Human Anatomy and Physiology 9th Edition Longenbaker Test Bankjohnnavarronpisaoyzcx100% (28)
- Body PointsDocument44 pagesBody PointsnhzaidiNo ratings yet
- Anatomy of Pleura, Lungs and AirwaysDocument108 pagesAnatomy of Pleura, Lungs and AirwaysTahleel AltafNo ratings yet
- Israel Regardie - Be Yourself - A Guide Book To The Art of RelaxationDocument48 pagesIsrael Regardie - Be Yourself - A Guide Book To The Art of Relaxationarch_loafer100% (13)
- Skeletal SystemDocument7 pagesSkeletal SystemMaria Grace MancaoNo ratings yet
- Koko KirjaDocument155 pagesKoko KirjaMihaaaNo ratings yet
- Oboe Reed Styles - Theory and Practice - Ledet, David - 1981 - Bloomington - Indiana University Press - 9780253378910 - Anna's ArchiveDocument232 pagesOboe Reed Styles - Theory and Practice - Ledet, David - 1981 - Bloomington - Indiana University Press - 9780253378910 - Anna's ArchiveBilal GuncanNo ratings yet
- Session #19 SAS - AnaPhy (Lab) (Agdana, Nicole Ken)Document10 pagesSession #19 SAS - AnaPhy (Lab) (Agdana, Nicole Ken)Nicole Ken AgdanaNo ratings yet
- Power Breathing Breathe Your Way To Inner Power (2008)Document264 pagesPower Breathing Breathe Your Way To Inner Power (2008)Pk100% (2)
- 6) RESPIRATORY MUSCLES by DR Hasnain NorthDocument28 pages6) RESPIRATORY MUSCLES by DR Hasnain NorthHasin's QueenNo ratings yet
- Thoracic: InletDocument34 pagesThoracic: Inlet19 Arya Ganesh OjhaNo ratings yet
- Mechanics of breathing explained in 69 wordsDocument18 pagesMechanics of breathing explained in 69 wordsZaliaSubplace S5357No ratings yet
- Skull Thoracic Cage (Ribs and Sternum) Facial Bones Cranium: Chapter 7 - The SkeletonDocument45 pagesSkull Thoracic Cage (Ribs and Sternum) Facial Bones Cranium: Chapter 7 - The SkeletonSoua YangNo ratings yet
- The Ribcage-Inspired Bamboo Arc Hall in BaliDocument15 pagesThe Ribcage-Inspired Bamboo Arc Hall in BaliSarthak DalviNo ratings yet
- Axial SkeletonDocument10 pagesAxial SkeletonFrancisco LeaNo ratings yet
- Surface Anatomy of The Upper LimbDocument3 pagesSurface Anatomy of The Upper LimbIrvin JoshuaNo ratings yet
- Ch5 Skeletal Edited 91 SlidesDocument91 pagesCh5 Skeletal Edited 91 SlidesAnn Margarette MoralesNo ratings yet
- Great Singers BreathingDocument2 pagesGreat Singers BreathingTudor BarbosNo ratings yet