Professional Documents
Culture Documents
Clinical: Contact Allergy To Cinnamon: Case Report
Clinical: Contact Allergy To Cinnamon: Case Report
Uploaded by
Adrian DjohanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Clinical: Contact Allergy To Cinnamon: Case Report
Clinical: Contact Allergy To Cinnamon: Case Report
Uploaded by
Adrian DjohanCopyright:
Available Formats
Clinical
Practice
Contact Allergy to Cinnamon: Case Report
Contact Author
Steve Tremblay, DMD, MSD, MSc, FRCD(C);
Sylvie Louise Avon, DMD, MSc, PhD, FRCD(C)
Dr. Tremblay
Email: steve.tremblay@
fmd.ulaval.ca
ABSTRACT
Allergic contact stomatitis is a rare disorder that is unfamiliar to most clinicians. The vast
majority of cases are associated with consumption of products containing cinnamaldehyde or cinnamon essential oil, which are used as flavourings because of their pleasant
taste and sensation of freshness. We report here the case of a patient who was diagnosed with alllergic contact stomatitis due to cinnamon-flavoured chewing gum. The
clinical features of allergic contact stomatitis, which may occur indiscriminately on any of
the oral mucosa, include edema and erythroplakic, ulcerous or hyperkeratotic changes,
generally accompanied by a burning sensation. The histopathologic aspect of allergic
contact stomatitis is nonspecific but tends to support the clinical diagnosis. Treatment
generally consists of eliminating the causal agent. To avoid unnecessary diagnostic procedures and treatments, it is important for clinicians to recognize this disorder to be able
to diagnose it quickly and accurately.
For citation purposes, the electronic version is the definitive version of this article: www.cda-adc.ca/jcda/vol-74/issue-5/445.html
llergic contact stomatitis accounts for
only a small proportion of oral disorders and is therefore little known
among dentists.1 Contact dermatitis, the most
frequent form of immunotoxicity among humans, is much more common than contact
stomatitis.2 Moreover, only the allergic form
of contact stomatitis develops in the mouth,
whereas the skin may be subject to a form of
irritant contact dermatitis as well as dermatitis secondary to exposure to ultraviolet rays. 3,4
Allergic contact stomatitis may be caused by a
wide range of substances, including the aromatic compounds found in chewing gum and
toothpaste, the most common being carvone,
spearmint essential oil, menthol essential oil,
cinnamaldehyde and cinnamon essential oil.5
These substances are also used in ice cream,
soft drinks, candies and mouthwash.6 In addition to their use as a flavouring for certain
products, these compounds are used at higher
concentrations in antitartar toothpastes
to mask the bitter taste of pyrophosphates.7
Other products, such as formaldehyde, 5 the
acrylates used in making dentures8 and several metals including nickel, palladium, gold
and mercury used in dental amalgam911 may
also cause contact stomatitis. Amalgam may
cause clinical signs and symptoms resembling
oral lichen planus, but where there is this
form of contact allergy, a lichenoid reaction to
amalgam should be diagnosed.12
Mechanism of Action
Allergic contact stomatitis is a hypersensitivity reaction (type IV) that affects only individuals who have previously been sensitized to
the allergen. Because of the cascade of cellular
events involved, contact stomatitis does not
become evident until several hours or even
days after exposure to the antigen; hence the
term delayed hypersensitivity reaction. The
JCDA www.cda-adc.ca/jcda June 2008, Vol. 74, No. 5
445
Tremblay
allergic process develops in 2 phases: the induction phase,
which sensitizes the immune system to the allergen, and
the effector phase, during which the immune response is
triggered.2
Allergens are molecules with the ability to infiltrate
the mucosal epithelium and bind to epithelial proteins.
The newly formed complexes have certain immunogenic
properties.13 In the induction phase, on first contact with
the antigen, these complexes are phagocytized by specialized cells (macrophages) that present the complexes on
their surface and migrate toward the regional ganglia.
The complexes are then recognized by a specific group of
lymphocytes, the helper T cells, which subsequently enter
the stimulation and division phase, leading in turn to the
production of 2 other types of T lymphocytes: memory
and cytotoxic T lymphocytes. The memory T lymphocytes are then stimulated by contact with the antigens,
and the cycle begins anew. Because these lymphocytes
remain in the body for life, a more aggressive, more rapid
immune response will be triggered whenever the antigen
is encountered again. This cycle is controlled by several
cytokines, which reinforce the T lymphocytes, support
their proliferation and activate the macrophages. 2
The effector phase of the process begins when the
cytotoxic T lymphocytes (CD8+ cells) produced in the
first phase release cytokines to recruit and activate helper
T lymphocytes (CD4+ cells) from the peripheral circulation. The cytotoxic T lymphocytes bind to the epithelial cells and cause the death of cells that present the
complexes.14
Although there are many allergenic substances and
many people who have been exposed to them, it is believed that the specific environment of the oral cavity
inhibits hypersensitivity reactions, which explains why
this phenomenon is not more commonly seen. Two particular mechanisms might explain this observation. First,
the saliva ensures constant cleaning of the mucosa and
reduces contact time with allergenic substances. Second,
the high degree of vascularization of the mucosa causes
rapid absorption of antigens, which further reduces prolonged contact with these substances.8
Clinical Features
The clinical features of allergic contact stomatitis vary
widely and include tissular edema, erythema, cracking,
ulcerative areas, hyperkeratosis in the form of plaques
or striations, desquamation and vesicles. Any of these
features, which may occur concurrently, may be accompanied by pain, with or without a burning sensation.1519
They typically appear at sites that are in direct contact
with the causal agent. The clinical appearance depends
on the exposure time, the concentration of the causal
agent and the type of exposure. For example, in a hypersensitive patient, wearing a removable dental prosthesis
will affect the palatine mucosa or the alveolar ridge, the
446
use of chewing gum could have a greater effect on the
lateral surfaces of the tongue or the buccal mucosa, and
use of a mouthwash or toothpaste may affect more areas
of the oral cavity.
Microscopic Observations
Allergic contact stomatitis manifests primarily
through hyperorthokeratosis, acanthosis or atrophy,
all of which may be accompanied by liquefaction degeneration of the basal layer of the affected epithelium.
Neutrophilic exocytosis and spongiosis are sometimes
observed. Ulcerated areas characterized by fibrinopurulent exudate and acute inflammatory infiltrate may appear. The superficial area of the connective tissue presents
a chronic inflammatory infiltrate composed principally of
lymphocytes and plasmocytes and sometimes organized
in a band resembling oral lichen planus but extending
more deeply into the tissues. A perivascular lymphocytic
infiltrate may also be present, accompanied by plasmocytes and eosinophils. The latter may also be observed in
the superficial connective tissue.1,15
Case Report
A 42-year-old patient was referred to the faculty of
dentistry at Laval University by her dentist for diagnosis
of a nondetachable localized white lesion of the left buccal
mucosa. This lesion had been found by the patient and
appeared to come and go cyclically. The patient did not
report any sensitivity when eating spicy or acidic foods or
using toothpaste. However, she had noticed some sensitivity to the cinnamon-flavoured gum that she chewed a
few times a week. The patient did not exhibit any parafunctional behaviour such as chronic cheek biting. She reported no cutaneous or ocular lesions or vaginal itching.
Her medical history was noncontributory, and she was
not taking any medications regularly. She smoked 1 or 2
small cigars per week.
The intraoral examination revealed full dentition of
the maxilla and mandible. The restorations were made
of amalgam and composite materials and included porcelain-fused-to-metal crowns. In the left buccal mucosa
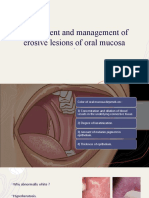
(Fig. 1), a white and red partially erosive lesion with a
traumatic appearance was observed beginning in the
retrocommissural area and extending to the pterygomaxillary raphe. This band-like lesion measured approximately 1 cm in height and was localized in the area of the
buccal linea alba. An examination of the right buccal mucosa revealed similar lesions, but they were confined to
the retrocommissural area. The other mucosa appeared
unaffected.
The differential diagnosis of the lesions included an
allergy to chewing gum, chronic cheek biting, erosive
oral lichen planus, leukoplakia (precancerous lesion) and
hyperplasic candidiasis. It was recommended that the
JCDA www.cda-adc.ca/jcda June 2008, Vol. 74, No. 5
Contact Allergy
Figure 1: Appearance of the left
buccal mucosa at the first consultation. Several white nondetachable
plaques are visible on an erythematous background.
Figure 2: Photomicrograph showing a fragment of a predominantly lymphocytic bandlike inflammatory infiltrate located directly
under the epithelium and attached to the
basal cell layer. Eosinophils and plasmocytes
were observed at higher magnifications
(not shown). Deeper in the connective
tissue, a perivascular lymphocytic infiltrate
can be observed (arrows). Hematoxylin and
eosin 20.
patient stop using chewing gum for 2 weeks. At the patients request, an incisional biopsy of the buccal mucosa
was performed the day of the initial appointment. The
microscopic examination revealed a fragment of tissue
composed of keratinizing stratified squamous epithelium
covering an inflamed connective tissue. A predominantly
lymphocytic band-like inflammatory infiltrate that also
contained eosinophils and plasmocytes was observed directly under the epithelium and adjacent to the basal cell
layer (Fig. 2). Deeper in the connective tissue, there was
a perivascular lymphocytic infiltrate. The histopathologic
and clinical features were consistent with a hypersensitive reaction to chewing gum. After use of cinnamonflavoured chewing gum was discontinued, the lesions of
the buccal mucosa disappeared completely (Fig. 3).
Discussion
Given its numerous clinical features, allergic contact
stomatitis can easily be confused with other more or less
serious disorders. These include a variety of white lesions
(e.g., hairy leukoplakia, leukoplakia, lesions associated
with chronic biting, hyperplasic candidiasis, reticular
oral lichen planus, epidermoid carcinoma) and red lesions
(e.g., atrophic or erosive oral lichen planus, lupus erythematosus or discoid lupus, epidermoid carcinoma).1,15
No intraoral sites are spared from contact stomatitis.
It may just as easily develop on keratinized as nonkeratinized mucosa. However, it mainly affects the lateral
Figure 3: At the follow-up visit, after discontinuation of consumption of cinnamonflavoured chewing gum, the appearance of
the left buccal mucosa is normal, except for
the presence of 2 petechiae.
edges of the tongue, the attached gingiva, the buccal mucosa and the hard palate.1,8,15
Some practitioners use patch tests to confirm the
diagnosis of allergic contact stomatitis. Although these
tests may yield positive results for some patients, falsenegative results often occur. Direct tests of the mucosa
are difficult to perform and even more difficult to interpret, given the structural differences between the skin
and the oral mucosa.20
The treatment of allergic contact stomatitis involves
eliminating the allergenic agent, whose allergenic properties may be confirmed by the reappearance of inflammatory lesions on re-introduction of the agent. Complete
disappearance of the lesions can take up to 2 weeks. 20
Patients experiencing more severe symptoms may need a
topical corticosteroid in the form of a mouthwash, ointment or gel to accelerate healing.
Conclusion
In addition to information gathered by the standard
health questionnaire, the main factor in diagnosing allergic contact stomatitis is the information obtained
through the interview with the patient, which allows the
clinician to associate consumption of the allergenic agent
with development of symptoms. Although the histopathologic element is not pathognomonic for contact
stomatitis, a biopsy will usually support the clinicians
diagnosis and eliminate the other abnormalities in the
differential diagnosis. a
JCDA www.cda-adc.ca/jcda June 2008, Vol. 74, No. 5
447
Tremblay
THE AUTHORS
Dr. Tremblay is a specialist in oral medicine and pathology
and an assistant professor in the faculty of dentistry, Laval
University, Quebec City, Quebec.
Dr. Avon is a specialist in oral medicine and pathology and
an associate professor in the faculty of dentistry, Laval
University, Quebec City, Quebec.
Correspondence to: Dr. Steve Tremblay, Laval University, Faculty of dentistry, 2420 De la Terrasse St., Quebec City, QC G1V 0A6.
The authors have no declared financial interests.
This article has been peer reviewed.
References
1. Allen CM, Blozis GG. Oral mucosal reactions to cinnamon-flavored
chewing gum. J Am Dent Assoc 1988; 116:(6):6647.
2. Kimber I, Basketter DA, Gerberick GF, Dearman RJ. Allergic contact
dermatitis. Int Immunopharmacol 2002; 2(2-3):20111.
3. Morris-Jones R, Robertson SJ, Ross JS, White IR, McFadden JP, Rycroft RJ.
Dermatitis caused by physical irritants. Br J Dermatol 2002; 147(2):2705.
4. Lankerani L, Baron ED. Photosensitivity to exogenous agents. J Cutan Med
Surg 2004; 8(6):42431.
5. Sainio EL, Kanerva L. Contact allergens in toothpastes and a review of
their hypersensitivity. Contact Dermatitis 1995; 33(2):1005.
6. Magnusson B, Wilkinson DS. Cinnamic aldehyde in toothpaste. 1. Clinical
aspects and patch tests. Contact Dermatitis 1975; 1(2):706.
448
7. DeLattre VF. Factors contributing to adverse soft tissue reactions due to
the use of tartar control toothpastes: report of a case and literature review.
J Periodontol 1999; 70(7):8037.
8. Koutis D, Freeman S. Allergic contact stomatitis caused by acrylic monomer
in a denture. Australas J Dermatol 2001; 42(3):2036.
9. Genelhu MC, Marigo M, Alves-Oliveira LF, Malaquias LC, Gomez RS.
Characterization of nickel-induced allergic contact stomatitis associated
with fixed orthodontic appliances. Am J Orthod Dentofacial Orthop 2005;
128(3):37881.
10. Garau V, Masala MG, Cortis MC, Pittau R. Contact stomatitis due to palladium in dental alloys: a clinical report. J Prosthet Dent 2005; 93(4):31820.
11. Moller H. Dental gold alloys and contact allergy. Contact Dermatitis
2002; 47(2):636.
12. Koch P, Bahmer FA. Oral lesions and symptoms related to metals used in
dental restorations: a clinical, allergological, and histologic study. J Am Acad
Dermatol 1999; 41(3 Pt 1):42230.
13. Saint-Mezard P, Rosieres A, Krasteva M, Berard F, Dubois B, Kaiserlian D,
and others. Allergic contact dermatitis. Eur J Dermatol 2004; 14(5):28495.
14. Banno T, Gazel A, Blumenberg M. Effects of tumor necrosis factor-alpha
(TNF alpha) in epidermal keratinocytes revealed using global transcriptional
profiling. J Biol Chem 2004; 279(31):3263342.
15. Miller RL, Gould AR, Bernstein ML. Cinnamon-induced stomatitis venenata: clinical and characteristic histopathologic features. Oral Surg Oral Med
Oral Pathol 1992; 73(6):70816.
16. De Rossi SS, Greenberg MS. Intraoral contact allergy: a literature review
and case reports. J Am Dent Assoc 1998; 129(10):143541.
17. Nadiminti H, Ehrlich A, Udey MC. Oral erosions as a manifestation of
allergic contact sensitivity to cinnamon mints. Contact Dermatitis 2005;
52(1):467.
18. Hoskyn J, Guin JD. Contact allergy to cinnamal in a patient with oral
lichen planus. Contact Dermatitis 2005; 52(3):1601.
19. Bousquet PJ, Guillot B, Guilhou JJ, Raison-Peyron N. A stomatitis
due to artificial cinnamon-flavored chewing gum. Arch Dermatol 2005;
141(11):14667.
20. Regezi J, Sciubba J, Jordan R. Oral pathology: clinical pathologic correlations, 4th edition. Philadelphia: W.B. Saunders; 2003. p. 448.
JCDA www.cda-adc.ca/jcda June 2008, Vol. 74, No. 5
You might also like
- Circus Cat Alley Cat: Lesson - 3Document1 pageCircus Cat Alley Cat: Lesson - 3sukavasi1973100% (1)
- Contact Dermatitis BJD Guidelines May 2009Document9 pagesContact Dermatitis BJD Guidelines May 2009Cynthia OktariszaNo ratings yet
- Clipp Case 30Document9 pagesClipp Case 30manzooradilNo ratings yet
- 2010 FulltextDocument410 pages2010 FulltextNajam Din SahitoNo ratings yet
- Cap. 10. SKIN DISEASES PDFDocument14 pagesCap. 10. SKIN DISEASES PDFoana policarpovNo ratings yet
- Iaat 12 I 2 P 458Document5 pagesIaat 12 I 2 P 458Virma PutraNo ratings yet
- Traduci RDocument14 pagesTraduci RClaudia Barrionuevo MedinaNo ratings yet
- Arduino 2017Document8 pagesArduino 2017neetika guptaNo ratings yet
- Ulcers and Vesicles2Document24 pagesUlcers and Vesicles2Kelly MayerNo ratings yet
- Australian Dental Journal - 2010 - Schifter - Oral Mucosal Diseases The Inflammatory DermatosesDocument16 pagesAustralian Dental Journal - 2010 - Schifter - Oral Mucosal Diseases The Inflammatory Dermatosesneetika guptaNo ratings yet
- Lec 14 immune mediated disordersDocument65 pagesLec 14 immune mediated disorderspxb8dhqgs9No ratings yet
- Desquamative GingivitisDocument6 pagesDesquamative Gingivitissidra malikNo ratings yet
- Keilitis Eksfoliatif JurnalDocument7 pagesKeilitis Eksfoliatif JurnalLeni Aria NastaNo ratings yet
- Keilitis Eksfoliatif JurnalDocument8 pagesKeilitis Eksfoliatif JurnalIbnu MuttaqinNo ratings yet
- 留学生讲义2018 11 2Document8 pages留学生讲义2018 11 2Nidya PutriNo ratings yet
- Medicine Notes Dr. Fatima and Dr. Rowida2Document38 pagesMedicine Notes Dr. Fatima and Dr. Rowida2qbnc8727s5No ratings yet
- Management of Oral Lichen Plannus: A Clinical Study: Jayachandran S, Koijamsashikumar SDocument4 pagesManagement of Oral Lichen Plannus: A Clinical Study: Jayachandran S, Koijamsashikumar Sranz ibonkNo ratings yet
- Candidosis A New ChallengeDocument7 pagesCandidosis A New ChallengeSalvador contreras huertaNo ratings yet
- Erythema MultiformeDocument5 pagesErythema MultiformeNicco MarantsonNo ratings yet
- COLGATE Oral - Lesions - BookDocument89 pagesCOLGATE Oral - Lesions - BookVijetha RaiNo ratings yet
- Lec 8 Ulcerative Vesicular & Bullous LesionsDocument6 pagesLec 8 Ulcerative Vesicular & Bullous LesionsAbd 9961No ratings yet
- Muco-Cutaneous & Aphthous UlcerDocument7 pagesMuco-Cutaneous & Aphthous Ulcerربيد احمد مثنى يحيى كلية طب الاسنان - جامعة عدنNo ratings yet
- Stomatitis Allergy ToothpasteDocument3 pagesStomatitis Allergy ToothpastemochbryllianNo ratings yet
- Differential Diagnosis 1. Atopic Dermatitis History TakingDocument13 pagesDifferential Diagnosis 1. Atopic Dermatitis History TakingCocoi MellaNo ratings yet
- Whitelesions 130320102307 Phpapp02Document36 pagesWhitelesions 130320102307 Phpapp02Cikw KuzhaNo ratings yet
- Cutis Do Not Copy: What Is Your Diagnosis?Document3 pagesCutis Do Not Copy: What Is Your Diagnosis?Wilker SoutoNo ratings yet
- Canine Atopic Dermatitis - A Practical ApproachDocument15 pagesCanine Atopic Dermatitis - A Practical ApproachlirmvetNo ratings yet
- Dermatology RevisionDocument6 pagesDermatology RevisionLedia EssamNo ratings yet
- Atopic Dermatitis - 2 PDFDocument7 pagesAtopic Dermatitis - 2 PDFtazzycaNo ratings yet
- LP 160610182350Document25 pagesLP 160610182350Karthik TNo ratings yet
- Dental Sealant ToxicityDocument14 pagesDental Sealant ToxicityGuru SvamiNo ratings yet
- Presentation 2Document32 pagesPresentation 2Dr. Bashir MehrNo ratings yet
- Lesi Dan Ulkus Dalam MulutDocument73 pagesLesi Dan Ulkus Dalam Mulutmega anggunNo ratings yet
- 3 Benign Inflammatory LesionsDocument8 pages3 Benign Inflammatory LesionsalbaablyNo ratings yet
- A Review of Drug-Induced Oral ReactionsDocument19 pagesA Review of Drug-Induced Oral ReactionsSri RahayuNo ratings yet
- Desquamative GingivitisDocument41 pagesDesquamative Gingivitislucents100% (1)
- Oral Ulceration AND Vesiculobullous LesionsDocument54 pagesOral Ulceration AND Vesiculobullous LesionsAbbas Qahtan JameelNo ratings yet
- Idiopathic Non Neoplastic Salivary Gland DiseasesDocument33 pagesIdiopathic Non Neoplastic Salivary Gland Diseasesgud4nothingNo ratings yet
- Vulval Pruritus and Vaginal Discharge: ReviewDocument6 pagesVulval Pruritus and Vaginal Discharge: ReviewEpi PanjaitanNo ratings yet
- A Clinical Approach White LesionDocument5 pagesA Clinical Approach White LesionTirta KusumaNo ratings yet
- Lec 19 DISEASES OF THE SALIVARY GLANDDocument17 pagesLec 19 DISEASES OF THE SALIVARY GLANDpxb8dhqgs9No ratings yet
- epithelial patho part 1Document12 pagesepithelial patho part 1myydsamyydsaNo ratings yet
- Enfermedades InmunologicasDocument14 pagesEnfermedades InmunologicasKarina OjedaNo ratings yet
- Oral Ulcerative LesionsDocument34 pagesOral Ulcerative LesionsAhmed NajmNo ratings yet
- Lichen PlanusDocument64 pagesLichen PlanusBahaa ShaabanNo ratings yet
- Lichen PlanusDocument17 pagesLichen PlanusRahma Tya Anwar0% (1)
- Haider OralllllllllllllllllllllllDocument13 pagesHaider OralllllllllllllllllllllllAli YehyaNo ratings yet
- Jurnal SistemikDocument3 pagesJurnal SistemikMariatun Zahro NasutionNo ratings yet
- Nedermatologyw Microsoft Office Word DocumentDocument56 pagesNedermatologyw Microsoft Office Word DocumentBaghdad BaghdadNo ratings yet
- Impetigo in Children: A Clinical Guide and Treatment OptionsDocument2 pagesImpetigo in Children: A Clinical Guide and Treatment OptionsBeuty SavitriNo ratings yet
- The Lichens in Vulvovaginal Disease 2015Document20 pagesThe Lichens in Vulvovaginal Disease 2015Vidini Kusuma AjiNo ratings yet
- BAHAN Chapter 24Document33 pagesBAHAN Chapter 24S FznsNo ratings yet
- Oral UlcerationDocument10 pagesOral Ulcerationمحمد حسنNo ratings yet
- Tugas Jurnal Blok 12Document7 pagesTugas Jurnal Blok 12Astasia SefiwardaniNo ratings yet
- 5 - White & Red Lesions Part 2Document104 pages5 - White & Red Lesions Part 2EuOmi AlsheikhNo ratings yet
- PDM Os4Document3 pagesPDM Os4Erdinawira RizkianiNo ratings yet
- Psoriasis: Posted: 02 Aug 2010 11:18 PM PDTDocument5 pagesPsoriasis: Posted: 02 Aug 2010 11:18 PM PDTScamb TrekNo ratings yet
- Allergic Mucosal Reaction To Systemic Drug AdministrationDocument38 pagesAllergic Mucosal Reaction To Systemic Drug AdministrationzaaNo ratings yet
- Common Oral Lesions: by Joseph Knight, PA-CDocument7 pagesCommon Oral Lesions: by Joseph Knight, PA-CAnonymous k8rDEsJsU1No ratings yet
- Allergic Contact Stomatitis: A Case Report and Review of LiteratureDocument5 pagesAllergic Contact Stomatitis: A Case Report and Review of LiteratureFajar RamadhanNo ratings yet
- Skin Lichen Planus, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandSkin Lichen Planus, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Vaccine in AfricaDocument2 pagesVaccine in Africakhadijahussain107No ratings yet
- ECG Monitoring and Rhythm RecognitionDocument36 pagesECG Monitoring and Rhythm Recognitionمحمد زينNo ratings yet
- Frisium Knowledge ModuleDocument7 pagesFrisium Knowledge ModulesiddiqrehanNo ratings yet
- Biofumigation: A Potential Aspect For Suppression of Plant-Parasitic NematodesDocument7 pagesBiofumigation: A Potential Aspect For Suppression of Plant-Parasitic NematodesIJEAB JournalNo ratings yet
- (Victor R. Preedy, Vinood B. Patel) Biosensors andDocument421 pages(Victor R. Preedy, Vinood B. Patel) Biosensors andmshbiotech86No ratings yet
- CANCER - LEUKEMIA - Edgar Cayce (PDFDrive)Document115 pagesCANCER - LEUKEMIA - Edgar Cayce (PDFDrive)Solve WalterNo ratings yet
- Bacillus ThuringiensisDocument20 pagesBacillus ThuringiensisCamila VelandiaNo ratings yet
- The Story of An Hour Class Wrok d2Document6 pagesThe Story of An Hour Class Wrok d2Maryam SanadNo ratings yet
- MEDICAL LECT B SC SUM20Document63 pagesMEDICAL LECT B SC SUM20Dewan Ajuad Hossain RifatNo ratings yet
- Management and Complications of Short Bowel SyndromeDocument13 pagesManagement and Complications of Short Bowel Syndromenadill92No ratings yet
- Drug Interactions: Vivian Soetikno Department of Pharmacology & Therapeutics, FmuiDocument53 pagesDrug Interactions: Vivian Soetikno Department of Pharmacology & Therapeutics, FmuiAciNo ratings yet
- Mandibular Buccal Bifurcation Cyst: Case Report and Literature ReviewDocument5 pagesMandibular Buccal Bifurcation Cyst: Case Report and Literature Reviewboooow92No ratings yet
- Ebola Prophylaxis and Cure: by John R. Benneth, PG Hom. - London (Hons.)Document19 pagesEbola Prophylaxis and Cure: by John R. Benneth, PG Hom. - London (Hons.)RCNo ratings yet
- Management of Migraine OET ReadingDocument21 pagesManagement of Migraine OET ReadingKush Gurung80% (5)
- Deep Learning Model For Glioma, Meningioma and Pituitary ClassificationDocument11 pagesDeep Learning Model For Glioma, Meningioma and Pituitary ClassificationInternational Journal of Advances in Applied Sciences (IJAAS)No ratings yet
- Name: - Grade and SectionDocument3 pagesName: - Grade and SectionCherryn Dorotayo QuiminsaoNo ratings yet
- Integration Stability of Shbsag-Multi Expression Cassettes in Pichia Pastoris Gs115 During Methanol InductionDocument7 pagesIntegration Stability of Shbsag-Multi Expression Cassettes in Pichia Pastoris Gs115 During Methanol InductionAlex MaxNo ratings yet
- Label Nama Obat Di Rak ObatDocument8 pagesLabel Nama Obat Di Rak ObatDyah SariNo ratings yet
- N. Family Planning - With LoDocument123 pagesN. Family Planning - With LoRadha ChiombonNo ratings yet
- Allergy and Anaphylaxis - Principles of Acute Emergency Management - Emerg Med Prac - Agosto 2015 PDFDocument24 pagesAllergy and Anaphylaxis - Principles of Acute Emergency Management - Emerg Med Prac - Agosto 2015 PDFa aNo ratings yet
- Pharmacological and Parenteral Therapies in Older Adult PopulationDocument5 pagesPharmacological and Parenteral Therapies in Older Adult PopulationNDINDA GODYFREEY NATTOHNo ratings yet
- Bioavailability - of MGDocument13 pagesBioavailability - of MGRatanieriNo ratings yet
- Appendicitis Introduction AppendicitisDocument4 pagesAppendicitis Introduction AppendicitisShiba AmpaNo ratings yet
- HydrocortisoneDocument3 pagesHydrocortisoneunkown userNo ratings yet
- Referinte Analize LabDocument14 pagesReferinte Analize LabDiana CâmpeanNo ratings yet
- Stress and AdaptationDocument15 pagesStress and AdaptationbindiyaNo ratings yet
- Sudden Cardiac Death in Young AthletesDocument6 pagesSudden Cardiac Death in Young AthletesnulintavaNo ratings yet