Professional Documents
Culture Documents
New Scan
Uploaded by
rcfinnOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
New Scan
Uploaded by
rcfinnCopyright:
Available Formats
N o v e m b e r 2 0 0 5 • w w w. e c a r d i o l o g y n e w s .
c o m Imaging 21
New Scan Gives Speedy
Diagnosis of Chest Pain
A single 15-second scan may replace a battery of
tests for serious conditions in emergency situations.
BY ROBERT FINN In addition to aortic dissection, pul-
San Francisco Bureau monary embolism, and coronary artery
disease, the technique will allow clear
S A N F R A N C I S C O — Chest pain repre- views of the pericardium, permitting the
sents one of the most common presenting diagnosis of calcified or thickened peri-
symptoms in emergency departments, cardium and sometimes pericarditis.
and it also represents a diagnostic chal- In addition, “you might pick up pneu-
lenge: Is it a pulmonary embolism? Is it an monia, and you might pick up pulmonary
aortic dissection? Is it coronary artery dis- adhesions or even pericardial adhesions,”
ease? Or is it nothing? Dr. Budoff said. “There are a lot of things
Now, new CT technology promises to you could possibly see. And it could be
revolutionize this diagnosis, giving the done during the chest pain episode, which
ability to rule out all three conditions with is a great advantage over some of the oth-
a single 15-second scan. er modalities where you’d want to wait
In theory, this scan can replace stress until their chest pain is quiescent.”
testing for coronary artery disease, Dr. Budoff described the case of an el-
echocardiography or CT for aortic dis- derly woman who complained of chest
section, and CT pulmonary angiography pain and shortness of breath. Because of
or a ventilation-perfusion scan for pul- her age, he was reluctant to order a stress
monary embolism, Matthew J. Budoff, test. The CT angiography showed that her
M.D., said at a cardiovascular imaging coronary arteries were normal and that
conference sponsored by the American her ejection fraction was acceptably high.
College of Cardiology. When he examined the lung images close-
Although no diagnostic or prognostic ly, however, he discovered several pul-
studies on the triple rule out have yet monary emboli.
been published, there’s some indication “We admitted her to the hospital, put
that the single scan will have 90% accura- her on heparin, and it all cleared up,” he
cy or better for each of the three condi- said.
tions, said Dr. Budoff of Harbor-UCLA Despite its promise, the triple rule out
Medical Center in Torrance, Calif. does have some limitations. For one thing,
The technology involves a 64-slice CT it subjects patients to a relatively high
scan from the apex to the base of the dose of radiation—in the neighborhood of
lungs. Patients will have to hold their 24-30 millisieverts, equivalent to 240-300
breath for 20-30 seconds as contrast is in- chest x-rays.
jected and the images are acquired. Ac- Because it’s a gated study, more contrast
quisition of the slices will be gated to the must be used and the injection time is
heart’s rhythm, allowing for stable, high- longer than for a standard CT. Some pa-
resolution images of the heart and lungs. tients may have trouble holding their
The slice thickness will be 0.625 mm. breath for 20-30 seconds.
Software and a sophisticated workstation Then there’s the issue of who is going
will allow the clinician to construct three- to read these images when a patient pre-
dimensional images sents at 3 a.m. The radiologist staffing the
of the heart, lungs, emergency department may not be facile
or aorta, and to ma- with cardiac CT angiography. Although
nipulate three-di- the images could be transferred over data
mensional and two- lines, the cardiologist is not likely to have
dimensional images a workstation with the proper software at
in a variety of ways. home. In all likelihood, someone will have
to come to the hospi-
tal to read the study.
Still, Dr. Budoff ex-
pects the triple rule
out to become a rou-
tine test in the emer-
gency department, a
prospect he greets
D R . M ATTHEW J. B UDOFF
with mixed emotions.
“We really need to
see how this is going
to pan out, and work
out the reading issues
before we start apply-
COURTESY
ing this to everybody
who comes in with a
twinge in their chest
P HOTOS
or shortness of
breath,” he said. “I’m a
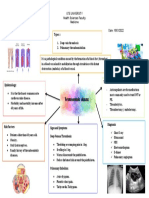
Views of aortic dissection: Left, it is shown as a long, thin little leery ...to say just
dissection flap in the descending aorta; right, the true lumen because we can do it
(larger area) and false lumen are shown endoscopically. we should.” ■
You might also like
- Concomitant Purulent Pericarditis and Pleuritis Due To Actinomyces Odontolyticus Following Endobronchial Biopsy For Pulmonary SarcoidosisDocument6 pagesConcomitant Purulent Pericarditis and Pleuritis Due To Actinomyces Odontolyticus Following Endobronchial Biopsy For Pulmonary SarcoidosisNiatazya Mumtaz SagitaNo ratings yet
- Lumbar Punctures and Cerebrospinal Fluid Analysis - 2016 - MedicineDocument4 pagesLumbar Punctures and Cerebrospinal Fluid Analysis - 2016 - MedicinemateoNo ratings yet
- Fundamentals of Body CT 5th EdDocument415 pagesFundamentals of Body CT 5th EdRuxandra TartaNo ratings yet
- Patient's Cures His Snoring: The EditorDocument1 pagePatient's Cures His Snoring: The EditorDiegoNo ratings yet
- Journal Homepage: - : Manuscript HistoryDocument10 pagesJournal Homepage: - : Manuscript HistoryIJAR JOURNALNo ratings yet
- Value of Chest Ultrasound in Diagnosis of Community Acquired PneumoniaDocument5 pagesValue of Chest Ultrasound in Diagnosis of Community Acquired PneumoniaHarlan SiMarmutNo ratings yet
- Causes and Investigation of Shock: Learning ObjectivesDocument3 pagesCauses and Investigation of Shock: Learning Objectivesstef lopezNo ratings yet
- JVP Dan CVPDocument8 pagesJVP Dan CVPHary SanjayaNo ratings yet
- 2013 9 1 045 ChuangDocument8 pages2013 9 1 045 ChuangRamaMahardikaNo ratings yet
- Nephropathy With Intravenous ContrastDocument9 pagesNephropathy With Intravenous Contrastjose torresNo ratings yet
- 1Document4 pages1Mirla Castellanos JuradoNo ratings yet
- Derrame Pleural 2002 - NEJMDocument7 pagesDerrame Pleural 2002 - NEJMgabriella pachecoNo ratings yet
- Perfusion BookDocument127 pagesPerfusion Bookreader100% (1)
- Detection of Unsuspected Pelvic Dvts On Abdominopelvic CT Scans: A Potentially Life-Saving DiagnosisDocument5 pagesDetection of Unsuspected Pelvic Dvts On Abdominopelvic CT Scans: A Potentially Life-Saving DiagnosisKumail KhandwalaNo ratings yet
- December 2008final FRCA VivaDocument43 pagesDecember 2008final FRCA Vivajahangirealam100% (2)
- Rapid Diagnosis and Treatment of A Pleural Effusion in A 24-Year-Old ManDocument4 pagesRapid Diagnosis and Treatment of A Pleural Effusion in A 24-Year-Old ManJonathan EdbertNo ratings yet
- Value of Lung Biopsy Lung: Tru-Cut in Focal and DiffuseDocument4 pagesValue of Lung Biopsy Lung: Tru-Cut in Focal and DiffuseGargNo ratings yet
- American Journal of Emergency Medicine - Cardiac TamponadeDocument3 pagesAmerican Journal of Emergency Medicine - Cardiac TamponadefloNo ratings yet
- Endobronchial Ultrasound: Dr. Deepak Talwar India's Best PulmonologistDocument3 pagesEndobronchial Ultrasound: Dr. Deepak Talwar India's Best PulmonologistMetro HospitalNo ratings yet
- Echocardiography Dissertation IdeasDocument8 pagesEchocardiography Dissertation IdeasWhoCanWriteMyPaperForMeCanada100% (1)
- Evaluation of Lung Ultrasound For The Diagnosis of Pneumonia in The EDDocument7 pagesEvaluation of Lung Ultrasound For The Diagnosis of Pneumonia in The EDAsclepioNo ratings yet
- Early and Persistent Hemothorax and PneumothoraxDocument7 pagesEarly and Persistent Hemothorax and Pneumothoraxtri_budi_20No ratings yet
- Problem Penegakkan Diagnostik Pasien Dengan Massa Di Paru: Jurnal RespirasiDocument6 pagesProblem Penegakkan Diagnostik Pasien Dengan Massa Di Paru: Jurnal RespirasiNada lathifahNo ratings yet
- Fundamentals of CT PDFDocument415 pagesFundamentals of CT PDFAl Marchese100% (1)
- Embolismo Pulmonar en Paciente OrtopedicoDocument10 pagesEmbolismo Pulmonar en Paciente OrtopedicoSOLEDAD GOMEZ FIGUEROANo ratings yet
- Kjtcs 47 124Document5 pagesKjtcs 47 124dalozpa23No ratings yet
- Premature Ventricular Contractions: CirculationDocument3 pagesPremature Ventricular Contractions: CirculationVictor NainggolanNo ratings yet
- IDOR 2013 ThoracicImaging-Book Breathe-Easy PDFDocument60 pagesIDOR 2013 ThoracicImaging-Book Breathe-Easy PDFVicka TalebongNo ratings yet
- Pericardial DiseaseDocument20 pagesPericardial DiseaseGeorgeNo ratings yet
- Posteroanterior Chest X-Ray For The Diagnosis of Pneumothorax: Methods, Usage, and ResolutionDocument6 pagesPosteroanterior Chest X-Ray For The Diagnosis of Pneumothorax: Methods, Usage, and ResolutionShaeli MalikNo ratings yet
- Diagnostic Test Purpose Normal Result Nursing ResponsibilityDocument4 pagesDiagnostic Test Purpose Normal Result Nursing Responsibilitykennethfe agron100% (1)
- Transaereolar Pulmonary BullectomyDocument7 pagesTransaereolar Pulmonary BullectomyAhmad Ibrahim RumNo ratings yet
- Pneumothorax 2Document6 pagesPneumothorax 2Helpful HandNo ratings yet
- CEE Based Question and Answer Asar 30 080Document74 pagesCEE Based Question and Answer Asar 30 080aayam adhikariNo ratings yet
- 1618 4726 1 PB PDFDocument6 pages1618 4726 1 PB PDFDrive IyasNo ratings yet
- Treatment Cysts: Thoracoscopic PleuropericardialDocument8 pagesTreatment Cysts: Thoracoscopic PleuropericardialJuhi SahajwaniNo ratings yet
- Abcd RushDocument3 pagesAbcd RushLeydi PaolaNo ratings yet
- Surgical Management For Lung CancerDocument45 pagesSurgical Management For Lung CancerarifgteguhNo ratings yet
- Saline Flush TestDocument5 pagesSaline Flush TestHandrian RahmanNo ratings yet
- ISUOG - Fetal Heart ExaminationDocument12 pagesISUOG - Fetal Heart ExaminationAzucenaNo ratings yet
- Pneumoperitoneum As A Complication of Cardiopulmonary ResuscitationDocument4 pagesPneumoperitoneum As A Complication of Cardiopulmonary Resuscitationl0litaaNo ratings yet
- Understanding Language - Siti MariyamDocument2 pagesUnderstanding Language - Siti MariyamTedi ArdiansyahNo ratings yet
- Pleural EffusionDocument7 pagesPleural EffusionsandeepNo ratings yet
- Tep Nejm 2022Document13 pagesTep Nejm 2022Jorge CastilloNo ratings yet
- Trauma: HX and PE (Adults) : For The EMS Providers, (Prior To Patient'sDocument3 pagesTrauma: HX and PE (Adults) : For The EMS Providers, (Prior To Patient'sJustine CastilloNo ratings yet
- Capnografia Durante La RCP LECTURADocument2 pagesCapnografia Durante La RCP LECTURAAinhoa Jimenez TraperoNo ratings yet
- Pi Is 0012369218304914Document2 pagesPi Is 0012369218304914Erwin SiahaanNo ratings yet
- Reply To Letter Continuous Chest Compression ResuDocument2 pagesReply To Letter Continuous Chest Compression ResuJorge CamarilloNo ratings yet
- Pi Is 00960217166003657Document15 pagesPi Is 00960217166003657Jesicca SNo ratings yet
- Caso Clinico Clinica Mayo 2Document5 pagesCaso Clinico Clinica Mayo 2Francisco HernandezNo ratings yet
- jurNAL SIRKULASIDocument9 pagesjurNAL SIRKULASIdiahfebriyNo ratings yet
- Emergency Department Ultrasound in The Evaluation of Blunt Abdominal TraumaDocument5 pagesEmergency Department Ultrasound in The Evaluation of Blunt Abdominal TraumaesmoesNo ratings yet
- ATLS Case ScenarioDocument13 pagesATLS Case ScenarioJenny Schneider100% (2)
- Transcatheter Pulmonary Balloon ValvulopastyDocument8 pagesTranscatheter Pulmonary Balloon ValvulopastyAndi Tiara S. AdamNo ratings yet
- Epidural Blood PatchDocument3 pagesEpidural Blood PatchdmdstaffpacNo ratings yet
- Pulmonary Embolism: Clinical PracticeDocument13 pagesPulmonary Embolism: Clinical PracticeGustavo EduardoNo ratings yet
- Continuous Chest Compression Resuscitation in ArreDocument1 pageContinuous Chest Compression Resuscitation in ArreJorge CamarilloNo ratings yet
- Arya - Usefulness and Safety of Transbronchial Biopsy With Large Forceps During Flexible BronchosDocument5 pagesArya - Usefulness and Safety of Transbronchial Biopsy With Large Forceps During Flexible BronchosXaralyn XaviereNo ratings yet
- 920 FullDocument17 pages920 FullHeru SigitNo ratings yet
- STEMIDocument2 pagesSTEMIrcfinnNo ratings yet
- Microglia Are Active Sentinels of The Brain MovieDocument1 pageMicroglia Are Active Sentinels of The Brain MoviercfinnNo ratings yet
- UstekinumabDocument2 pagesUstekinumabrcfinn100% (1)
- Psych SkinDocument1 pagePsych SkinrcfinnNo ratings yet
- Pro Bio Tics 1Document1 pagePro Bio Tics 1rcfinnNo ratings yet
- Seafood Allergy Contrast LinkDocument1 pageSeafood Allergy Contrast LinkrcfinnNo ratings yet
- Imaging CriteriaDocument2 pagesImaging CriteriarcfinnNo ratings yet
- CT LungDocument2 pagesCT LungrcfinnNo ratings yet
- Migraine 200503Document1 pageMigraine 200503rcfinnNo ratings yet
- DiaperDocument1 pageDiaperrcfinnNo ratings yet
- PurgativesDocument2 pagesPurgativesrcfinnNo ratings yet
- Melanoma P4PDocument2 pagesMelanoma P4PrcfinnNo ratings yet
- Statin ProstateDocument2 pagesStatin Prostatercfinn0% (1)
- Autism ComorbidDocument1 pageAutism ComorbidrcfinnNo ratings yet
- MyelodysplasticDocument2 pagesMyelodysplasticrcfinn100% (1)
- ACP DiabetesDocument2 pagesACP DiabetesrcfinnNo ratings yet
- Bipolar ElderlyDocument2 pagesBipolar ElderlyrcfinnNo ratings yet
- Pediatric Brain Death 200602Document1 pagePediatric Brain Death 200602rcfinnNo ratings yet
- ADHD PatchDocument2 pagesADHD PatchrcfinnNo ratings yet
- Metsynd Diabetes StrokeDocument1 pageMetsynd Diabetes StrokercfinnNo ratings yet
- MRSA TestDocument1 pageMRSA TestrcfinnNo ratings yet
- CDC HivDocument1 pageCDC HivrcfinnNo ratings yet
- Maternal MorbidityDocument2 pagesMaternal MorbidityrcfinnNo ratings yet
- MRSA TestDocument1 pageMRSA TestrcfinnNo ratings yet
- Vulvar CaDocument1 pageVulvar CarcfinnNo ratings yet
- LamotrigineDocument2 pagesLamotriginercfinnNo ratings yet
- Vulvar CaDocument1 pageVulvar CarcfinnNo ratings yet
- First TrimesterDocument1 pageFirst TrimesterrcfinnNo ratings yet
- Metsynd Diabetes StrokeDocument1 pageMetsynd Diabetes StrokercfinnNo ratings yet
- Major Haemorrhage ProtocolDocument2 pagesMajor Haemorrhage ProtocollaurenNo ratings yet
- Basic Concepts of Heart-Lung Interactions During Mechanical VentilationDocument14 pagesBasic Concepts of Heart-Lung Interactions During Mechanical VentilationanindiawNo ratings yet
- Terapi Jus Semangka - 10-20210203Document10 pagesTerapi Jus Semangka - 10-20210203Mhyla MusaNo ratings yet
- Cardiac Risk Assessemnt FlowchartDocument1 pageCardiac Risk Assessemnt FlowchartjamesomooreNo ratings yet
- NCP For Acute Coronary SyndromeDocument3 pagesNCP For Acute Coronary Syndromesarahtot75% (4)
- Acute Ischemia: Hamzeh YacoubDocument21 pagesAcute Ischemia: Hamzeh YacoubHamzeh K. YacoubNo ratings yet
- Levels of Care Intensive Care Society 2009Document14 pagesLevels of Care Intensive Care Society 2009bogus987No ratings yet
- Thromboembolic DiseaseDocument1 pageThromboembolic DiseaseDiana RoseroNo ratings yet
- Orthostatic ToleranceDocument3 pagesOrthostatic Tolerancehajar ahmadNo ratings yet
- 3 Series Blood Pressure Monitor: Model BP710N Instruction ManualDocument4 pages3 Series Blood Pressure Monitor: Model BP710N Instruction ManualMiguel RomeroNo ratings yet
- Oiml R 149-1Document15 pagesOiml R 149-1MIGUEL ANGEL CASTRO LEALNo ratings yet
- Hypertension: Pathophysiology, Diagnostic Test, Medical Management, and Nursing Care PlanDocument12 pagesHypertension: Pathophysiology, Diagnostic Test, Medical Management, and Nursing Care PlanMaulidyaFadilahNo ratings yet
- Auscultation of Fetal Heart RateDocument2 pagesAuscultation of Fetal Heart Rateraul nino MoranNo ratings yet
- Coronary Artery DiseaseDocument15 pagesCoronary Artery Diseasektae337No ratings yet
- 12 Defibrillator (@IranBmeChannel)Document5 pages12 Defibrillator (@IranBmeChannel)Fatemeh NaseriNo ratings yet
- Acc Aha Stemi 2004Document212 pagesAcc Aha Stemi 2004NikosKosmasNo ratings yet
- Report Tetralogy of FallotDocument3 pagesReport Tetralogy of FallotLieana AguilarNo ratings yet
- Basic Life Support Ms 2 Rle Term 2 PDFDocument4 pagesBasic Life Support Ms 2 Rle Term 2 PDFJesha PlatigueNo ratings yet
- 2020 BLS Science Summary TableDocument1 page2020 BLS Science Summary TableChristine ElbanbuenaNo ratings yet
- Lecture Objectives and Outlines-3Document9 pagesLecture Objectives and Outlines-3mickeyNo ratings yet
- Amazon - in Medical EquipmentDocument1 pageAmazon - in Medical EquipmentHaresh JivanNo ratings yet
- NPTE CArdio NotesDocument27 pagesNPTE CArdio NotesAubrey Vale SagunNo ratings yet
- Medi-18-30522: Certification NoDocument3 pagesMedi-18-30522: Certification NoPankaj MaithaniNo ratings yet
- INOTROPIC SUPPORT (Autosaved)Document23 pagesINOTROPIC SUPPORT (Autosaved)Bindhu RaniNo ratings yet
- Cardio Pulmonary ResuscitationDocument34 pagesCardio Pulmonary Resuscitationanimesh pandaNo ratings yet
- Day 3 - APPEC 2021Document413 pagesDay 3 - APPEC 2021GaurieNo ratings yet
- Unstable AnginaDocument11 pagesUnstable AnginaAdrian BoboceaNo ratings yet
- Eat Yourself Smart: Britain Faces Airlift DeadlineDocument64 pagesEat Yourself Smart: Britain Faces Airlift DeadlineNidhi BhartiNo ratings yet
- AclsDocument13 pagesAclsAllah YarNo ratings yet
- Cardiac DefibrillatorsDocument8 pagesCardiac Defibrillatorsصفا طلال نايفNo ratings yet