Professional Documents
Culture Documents
Fisiologia Linfedema
Uploaded by
SAKAI690 ratings0% found this document useful (0 votes)
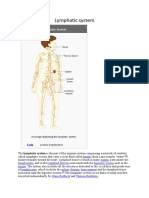
43 views8 pagesIn lymphedema, the microcirculation in the affected area of the body is disrupted. Lymphatics were mentioned more than 2000 years ago by Aristotle. The discovery of the lymphatics is attributed to the Italian anatomist Gasparo Aselli.
Original Description:
Original Title
fisiologia linfedema
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentIn lymphedema, the microcirculation in the affected area of the body is disrupted. Lymphatics were mentioned more than 2000 years ago by Aristotle. The discovery of the lymphatics is attributed to the Italian anatomist Gasparo Aselli.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
43 views8 pagesFisiologia Linfedema
Uploaded by
SAKAI69In lymphedema, the microcirculation in the affected area of the body is disrupted. Lymphatics were mentioned more than 2000 years ago by Aristotle. The discovery of the lymphatics is attributed to the Italian anatomist Gasparo Aselli.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 8
207
Failure of the lymphatic system to transport lymph from the
interstitial space back to the bloodstream results in lymphatic
stasis. If the collateral lymphatic circulation is insufcient and
all compensatory mechanisms are exhausted, the protein-rich
interstitial uid accumulates and lymphedema develops. In
lymphedema, caused by either congenital or acquired dys-
function of the lymphatic system, the microcirculation in the
affected area of the body is disrupted. The transport of the
excess tissue uid containing lymphocytes, different plasma
proteins, immunoglobulins, and cytokines is impaired
and chronic inammatory changes in the subcutaneous tis-
sue and skin develop. Progress in ultrastructural, cytochemi-
cal, and imaging studies and improvement in conservative
and surgical treatment of lymphedema have stimulated
substantial interest in lymphatic disease.
Historical background
Lymph vessels were mentioned more than 2000 years ago by
Aristotle, who described nerves which contain colorless
liquids and later by members of the Alexandrian School of
Medicine, who recognized arteries in the mesentery full of
milk. This knowledge, however, was lost during the Middle
Ages, and it was only in the Renaissance that attention was fo-
cused again on the lymphatic system. The thoracic duct was
observed in 1563 by Eustachius, who called it vena alba
thoracis. He failed, however, to recognize the function of the
thoracic duct and its relation to the lymphatic system. The
discovery of the lymphatics is attributed to the Italian
anatomist Gasparo Aselli, who in 1622 observed the mesen-
teric lymphatics in a well-fed dog. He also recognized the
function of the lacteals, although he suggested mistakenly that
the chyle absorbed from the intestine by the mesenteric lym-
phatics was transported to the liver. In 1651, Pecquet described
the thoracic duct and recognized the correct route of lym-
phatic transport from the mesenteric lymphatics through the
receptaculum chyli and the thoracic duct to the subclavian
vein. Further details on the anatomy of the lymphatic system
were published in the 17th century by Bartholin and Rudbeck,
and by the great anatomists of the 18th century, Mascagni and
Cruikshank. It was most likely William Hunter who recog-
nized the lymphatics as a separate system responsible for
absorption.
Although Hunter suggested that the lymphatics were
closed tubes, one of his students, Hewson, recognized that
they had physiologic orices, which, like capillary tubes
sucked up tissue uid. It was not until the turn of the 20th
century, however, that Starling conrmed the relationship
between the oncotic pressure of the plasma proteins and the
hydrostatic pressure in the capillaries.
1,2
Starling suggested
that lymph formed by ltration of the blood through the capil-
lary walls. Drinker,
3
and later Rusznyk and colleagues,
4
de-
serve the credit for clarifying the details of protein absorption
from the intercellular space via the lymphatic system. Interest
in lymphatic diseases was greatly enhanced by Kinmonth,
who described a clinically usable technique of direct contrast
lymphangiography in 1952.
5
Improvement in other imaging
techniques, such as lymphoscintigraphy,
6,7
indirect lymphan-
giography,
8,9
and magnetic resonance imaging,
1012
furthered
the understanding of the structure and function of the lym-
phatic system in different lymphatic disorders. Progress in
conservative management
13,14
and development of micro-
surgical operations on the lymph vessels
1517
also have stimu-
lated experimental and clinical research in lymphatic diseases.
Development of the lymphatic system
The lymphatic system is rst apparent in the human fetus at 6
weeks of gestation, and it consists of paired jugular, iliac, and
retroperitoneal lymph sacs (Fig. 18.1).
18
The origin of the lym-
phatic system is controversial, but it is most likely a derivative
from the venous system. Another possible theory is that it
develops independently of the veins from the mesenchymal
tissue. The lymph vessels grow from the paired primitive
lymphatic sacs and coalesce along the major veins to form the
afferent vessels, nodes, and efferent lymphatic ducts. The
Physiologic changes in lymphatic
dysfunction
Peter Gloviczki
18
Vascular Surgery: Basic Science and Clinical Correlations, Second Edition
Edited by Rodney A. White, Larry H. Hollier
Copyright 2005 Blackwell Publishing
cisterna chyli develops from one of the large retroperitoneal
lymph sacs, whereas the other forms the mesenteric lymphat-
ic system. There are paired thoracic ducts in the embryo, and
the mature thoracic duct develops from fusion of the upper
portion of the left and the lower portion of the right thoracic
duct. The right cervical lymphatic duct is formed by the right
jugular lymphatic sac. This receives lymph from the right face,
neck, and the right upper extremity, and from the upper part of
the right thorax and mediastinum. Abnormalities in the devel-
opment of the lymphatic system include agenesis, hypoplasia,
or hyperplasia of the lymphatics with valvular incompetence.
They may result in lymphedema or in abnormalities in the
circulation of the chyle, such as chylous ascites, chylothorax,
reux of chyle to the pelvis or lower extremities, or protein-
losing enteropathy. Persistence of some of the embryonic
sacs may cause the development of lymphatic cysts, which
may or may not communicate with the lymphatic system.
Anatomy of the lymphatic system
The adult lymphatic system consists of peripheral lymph ves-
sel, lymph nodes, and major lymphatic trunks. The peripheral
lymph vessels collect lymph from the lymphatic capillaries,
which absorb a portion of the interstitial uid from the inter-
stitial space. Afferent lymph channels transport lymph to the
lymph-conducting elements of the lymph nodes, which lter
and further conduct the lymph uid to efferent lymphatic
channels. Signicant communications between the lymphatic
and venous system in lymph nodes normally do not exist.
Eighty percent of the lower extremity lymph is carried by
the supercial lymphatic system. Although there is a lateral
supercial bundle located around the lesser saphenous vein,
most of the lower extremity lymph is transported by lymph
channels of the supercial medial bundle (Fig. 18.2). There is a
deep lymphatic network that runs in close proximity to the
tibial and peroneal vessels and transports lymph through
the popliteal lymph nodes into the deep femoral lymphatics.
The supercial and the deep lymphatics join in the inguinal
lymph nodes and drain lymph toward the aortoiliac lym-
phatic system. The cisterna chyli is located between the aorta
and the inferior vena cava, usually at the level of L1 to L2.
Mesenteric lymphatics join the lower extremity and pelvic
lymphatics at this level and drain through the thoracic duct to
the left subclavian vein (Fig. 18.3). A very small amount of
mesenteric lymph is drained toward the liver around the he-
patic vein and the diaphragm to the mediastinal lymphatics.
The upper extremity lymphatics run along the major veins
of the arm. Although the medial arm bundle is the most signif-
icant route of lymph drainage in normal patients, after axillary
node dissection lymph is drained primarily through the
lateral lymphatic bundle to the deltoideopectoral and supra-
clavicular nodes (Fig. 18.4).
Asingle layer of endothelial cells forms the inner layer of the
lymphatic capillaries. Basal membranes similar to blood capil-
laries are not present. The lymphatic capillaries contain
bicuspid lymphatic valves, which play a crucial role in the
initial lymphatic transport and are responsible for the unidi-
rectional lymphatic ow. The capillaries are anchored by small
microbrils that expand the endothelial cells and increase the
lumen of the capillaries if the tissue pressure is elevated.
19,20
Although smaller molecules may traverse the lymphatic
PART I Vascular pathology and physiology
208
A
B C
Figure 18.1 Development of the lymphatic system. (A) Seven-week embryo
with paired iliac, retroperitoneal, and jugular lymph sacs. (B) At 9 weeks of
gestation, paired thoracic ducts are present with numerous connections
across the midline. (C) Portions of both primitive thoracic ducts persist to
form the thoracic duct in the adult. The right lymphatic duct is formed from
the primitive right jugular lymphatic sac. (From Cambria RA, Gloviczki P.
Lymphedema: pathophysiology and management. In: Callow AD, ed.
Vascular Surgery. Norwalk, CT: Appleton & Lange, 1995:1593.)
CHAPTER 18 Physiologic changes in lymphatic dysfunction
209
endothelial cells with active phagocytosis, large molecules
enter through the gaps between the endothelial cells of the
lymphatic capillary.
Lymphatic physiology
According to Starlings law, hydrostatic and osmotic pressures
in the capillaries and in the interstitial space determine the
amount of interstitial uid that is ultraltered from the blood
plasma. Additional factors responsible for interstitial uid
exchange include capillary permeability, the number of active
capillaries, the ratio of precapillary arteriolar to postcapillary
venular resistance, and the total extracellular uid volume.
The amount of uid that moves across the capillary wall is
tremendous, considering that the cardiac output is about
8000 l during a 24-h period. It is likely that an amount equal to
the total plasma volume enters the interstitial place and leaves
through the venous end of the capillaries and the lymphatics
every minute.
21
The lymphatic system is responsible for the
transport of 24 l of interstitial uid daily. During the same
time, approximately 100g of plasma protein is carried back to
the circulation by the lymphatics.
22
The protein content of the
lymph is somewhat less than that of the plasma, and lymph
vessels from various parts of the body contain different
amounts of protein (Table 18.1). The lymphatic capillaries are
able to transport large molecules, even those with a molecular
weight over 1kDa.
23
Figure 18.2 Anatomy of major lymph vessels and lymph nodes of the lower
extremity. (From Gloviczki P. Microsurgical treatment for chronic
lymphedema: an unfullled promise? In: Bergan JJ, Yao JST, eds.
Venous Disorders. Philadelphia: WB Saunders, 1990:344.)
Figure 18.3 Anatomy of the thoracic duct.
(From Gloviczki P, Noel AA. Lymphatic
reconstructions. In: Rutherford RB, ed. Vascular
Surgery, 5th edn. Philadelphia: WB Saunders,
2000:2159, with permission from Elsevier.)
The single most important determinant of lymph ow
through the lymphatic capillaries and the collecting lymph
vessels is the intrinsic contractility of the lymph vessels. In
addition, lymph ow in inuenced by increased interstitial
pressure, muscular activity, arterial pulsation, respiratory
pressure, and gravity. Increase in interstitial volume and inter-
stitial pressure results in opening of the gaps between the
endothelial cells of the terminal lymphatics and an increase in
lymphatic transport. Because the endothelial cells contain
actin and are able to contract actively, contraction of terminal
lymphatics with the help of competent valves enables rapid
lymphatic transport. Intrinsic contractility of the smooth
muscle in larger collecting vessels allows further propulsion of
the lymph. Strength and frequency of the contractions are
greatly inuenced by changes in intraluminal pressure.
24
Adrenergic stimulation
25
and endothelin
26
also have been
shown to result in contraction of the lymph vessels. Patent
blue dye injected into the subcutaneous tissue is transported
centrally in the lymph vessels at the rate of 45mm/s, even
without any muscular exercise. Intrinsic contractions of the
lymph vessel wall with competent valves are able to propel
lymph intermittently against a pressure as high as 50mmHg.
The major difference that distinguishes the lymphatic sys-
tem from the venous system is that the veins are lled with a
continuous liquid column. The lymphatic system, however, is
not fully primed, and only if there is longstanding stasis
does the lymph column ll the lymphatic channels complete-
ly.
23
It is only in these conditions that muscular contraction or
external massage play an important role in forward propul-
sion of the lymph and facilitate lymphatic transport.
Pathophysiology of lymphedema
Lymphedema develops when the lymphatic load exceeds the
transport capacity of the lymphatic system. In patients with
lymphatic obstruction, numerous compensatory mechanisms
develop. These include collateral lymphatic circulation, de-
velopment of spontaneous lymphovenous anastomoses, and
increased activity of tissue macrophages to split macro-
molecules in the interstitial space, enabling them to be reab-
sorbed through the venous end of the capillaries (Fig. 18.5).
If the lymphatic transport is impaired due to injury or ob-
struction to the lymph vessels and lymph nodes, the different
compensatory mechanisms can function effectively for a
period of time. This explains why chronic lymphedema of the
limbs may develop several months or even years after an
edema-free state after inguinal or axillary node dissection or
irradiation.
Lymphedema is a high-protein edema that, except very
early in the course of the disease, is nonpitting in nature (Fig.
18.6). Without treatment, the high-protein edema uid in the
subcutaneous tissue will be replaced by brous material, in-
ammatory cells accumulate, and progressive brosis of the
subcutaneous tissue and skin develops. Fibrosis of the lymph
vessels leads to loss of permeability and loss of intrinsic con-
tractility. Dilation of the lymph vessels causes valvular incom-
petence, and the inammatory and brotic changes destroy
the valve leaets, further decreasing the transport capacity of
the lymphatic system. Microsurgical reconstruction in this
late stage of lymphedema, using brotic and incompetent
lymphatics, cannot restore normal lymphatic transport.
Progression of lymphedema results in brotic obstruction of
PART I Vascular pathology and physiology
210
Table 18.1 Approxiamte protein content of lymph in humans*
Lymph origin Protein content (g/dl)
Ankle 0.5
Limbs 2
Intestine 4
Liver 6
Thoracic duct 4
*Data based on various studies in humans and animals.
(From Ganong WF. Review of Medical Physiology, 10th edn. Los
Altos, CA: Lange Medical Publications, 1981: 452.)
Figure 18.4 Anatomy of major lymph vessels and lymph nodes of the upper
extremity. (From Gloviczki P. Microsurgical treatment for chronic
lymphedema: an unfullled promise? In: Bergan JJ, Yao JST, eds.
Venous Disorders. Philadelphia: WB Saunders, 1990:344.)
Figure 18.5 Stages in development of
postsurgical lymphedema. (Modied from
Gloviczki P, Schirger A. Lymphedema. In: Spittell
JA, ed. Clinical Medicine. Philadelphia: Harper &
Row, 1985:1.)
Figure 18.6 Chronic secondary lymphedema of the left lower extremity in a 47-year-old
man after iliac node dissection, followed by irradiation.
the lymph nodes and the major lymph vessels. Even the larger
lymphatic collaterals, which functioned effectively in the ini-
tial period after lymphatic obstruction, may occlude with
time. In this stage, dilated dermal lymphatics provide the only
lymphatic drainage of the extremity. Using noninvasive func-
tional tests, such as radionuclide lymphoscintigraphy per-
formed with technetium-labeled antimony sulfur colloid, it is
possible to repeat the studies in the same patient and docu-
ment progression of the disease (Fig. 18.7).
Lymphatic stasis also results in deciency of important im-
munoglobulins, cytokines, and plasma proteins. Because of
chronic inammatory changes in the subcutaneous tissue and
the skin, there frequently is increased vascularity in the lym-
phedematous limb, and inammatory cells accumulate. The
affected limb has an increased sensitivity to fungal and bacter-
ial infections. Obstructive lymphangitis further destroys the
lymphatic system and results in progression of the lymphede-
ma. In long-standing, neglected lymphedema, irreversible
sclerosis of the subcutaneous tissue and skin develops. Lym-
phangiosarcoma, which is a severe late complication of
secondary lymphedema, fortunately is rare.
Pathophysiology of chylous disorders
Disorders in the circulation of chyle usually are caused by lym-
phangiectasia or megalymphatics, with or without obstruc-
tion of the thoracic duct (Fig. 18.8).
27,28
Because of valvular
incompetence, chyle in these patients may reux to the pelvis
or lower extremities, causing chylorrhea from small vesicles in
the skin of the limb, scrotum, or labia (Fig. 18.9). Reux to the
kidney may lead to chyluria, whereas transudation through or
rupture of abdominal lymphatics results in chylous ascites.
Rupture of the lymphatics into the lumen of the gut causes
protein-losing enteropathy, and chylothorax develops if the
PART I Vascular pathology and physiology
212
A
B
Figure 18.7 Lymphoscintigram in a 44-year-old woman with secondary
lymphedema of the right lower extremity. (A) Note absence of right iliac
nodes and the presence of right inguinal nodes and collaterals. (B) Note
deterioration of lymphatic drainage 10 months later. There is no lling of the
right inguinal nodes or collaterals. The patient had a recent episode of
lymphangitis.
Figure 18.8 Contrast lymphangiogram in an 18-year-old man with
lymphangiectasia, protein-losing enteropathy, and chylous ascites
demonstrates dilated and tortuous thoracic duct.
thoracic duct or mediastinal, intercostal, or diaphragmatic
lymphatics rupture.
Secondary chyloperitoneum or chylothorax is caused most
frequently by malignant tumors, primarily lymphoma, or by
injury to the thoracic duct. The latter usually is iatrogenic, oc-
curring during operations on the thoracoabdominal aorta
2931
or, rarely, after a high translumbar aortography.
32
Chyle is a sterile alkaline uid, odorless, and milky in ap-
pearance. Its protein content is around 4g/dl and the fat con-
tent ranges from 0.4 to 4g/dl. The fat stains with Sudan stain
and this test conrms the diagnosis of chyle in the peritoneal or
thoracic aspirate. The specic gravity of chylous uid is
greater than 1012g/dl.
Loss of chyle into the body cavities or through chylocuta-
neous stulas has important physiologic consequences. If not
treated, it leads to malnutrition, hypoproteinemia, hypo-
cholesterolemia, hypocalcemia, immunodeciency, and se-
vere metabolic disturbances.
27,28
Lymphopenia and anemia
contribute to the poor immune function in these patients.
Chylous effusion in a patient with malignancy usually
CHAPTER 18 Physiologic changes in lymphatic dysfunction
213
A
B
Figure 18.9 (A) Chyle draining through small
vesicles of the skin at the left groin of a 16-year-
old girl with lymphangiectasia and severe reux
of the chyle. (B) Intraoperative photograph of
dilated, incompetent iliac lymphatics
containing chyle.
carries an ominous prognosis. The outcome of patients with
primary chylous disorders and reux of the chyle depends on
the effectiveness of medical treatment. To compensate for the
physiologic changes caused by the loss of chyle, treatment is
directed at decreasing production of the chyle with a medium-
chain triglyceride diet, or by parenteral nutrition. In addition
to adequate calorie and protein replacement, calcium, lost in
chyle, also should be replaced. Reux can be controlled effec-
tively with radical excision and ligation of the retroperitoneal
lymphatics in most cases. In patients with chylous effusion,
the site of lymphatic rupture should be oversewn if medical
treatment, paracentesis, or thoracentesis are ineffective. In
some patients with protein-losing enteropathy, the most dis-
eased segment of the small bowel may have to be resected to
decrease loss of chyle into the gastrointestinal tract.
27,28
Trans-
plantation of small bowel for severe mesenteric lymphangiec-
tasia remains a task of the future, and it requires, as do many
other aspects of lymphatic disorders, further clinical research.
References
1. Starling EH. The inuence of mechanical factors on lymph
production. J Physiol (Lond) 1894; 16:224.
2. Starling EH. On the absorption of uids from the connective tissue
spaces. J Physiol (Lond) 1986; 19:312.
3. Drinker CK. The Lymphatic System: Its Part in Regulating Composi-
tion and Volume of Tissue Fluid. Stanford, CA: Stanford University
Press, 1942.
4. Rusznyk I, Fldi M, Szab G. Lymphatics and Lymph Circulation.
New York: Pergamon Press, 1960.
5. Kinmonth JB. Lymphangiography in man: a method of outlining
lymphatic trunks at operation. Clin Sci 1952; 11:13.
6. Stewart G, Gaunt JI, Croft DN, Browse NL. Isotope lymphogra-
phy: a new method of investigating the role of the lymphatics in
chronic limb oedema. Br J Surg 1985; 72:906.
7. Gloviczki P, Calcagno D, Schirger Aet al. Noninvasive evaluation
of the swollen extremity: experiences with 190 lymphoscinti-
graphic examinations. J Vasc Surg 1989; 9:683.
8. Partsch H, Urbanek A, Wenzel-Hora B. The dermal lymphatics
in lymphoedema visualized by indirect lymphography. Br J
Dermatol 1984; 110:431.
9. Weissleder R, Thrall JH. The lymphatic system: diagnostic imag-
ing studies. Radiology 1989; 172:315.
10. Case TC, Witte CL, Witte MH et al. Magnetic resonance imaging in
human lymphedema: comparison with lymphangioscintigraphy.
Magn Reson Imag 1992; 10:549.
11. Weissleder R, Elizondo G, Wittenburg J, Lee AS, Josephson L,
Brady TJ. Ultrasmall superparamagnetic iron oxide: an intra-
venous contrast agent for assessing lymph nodes with MR
imaging. Radiology 1990; 175:494.
12. Duewell S, Hagspiel KD, Zuber J, von Schulthess GK, Bollinger A,
Fuchs WA. Swollen lower extremity: role of MR imaging.
Radiology 1992; 184:227.
13. Fldi E, Fldi M, Clodius L. The lymphedema chaos: a lancet. Ann
Plast Surg 1989; 22:505.
14. Pappas CJ, ODonnell TF Jr. Long-term results of compression
treatment for lymphedema. J Vasc Surg 1992; 16:555.
15. Gloviczki P, Fisher J, Hollier LH, Pairolero PC, Schirger A, Wahner
HW. Microsurgical lymphovenous anastomosis for treatment of
lymphedema: a critical review. J Vasc Surg 1988; 7:647.
16. OBrien BM, Mellow CG, Khazanchi RK, Dvir E, Kumar V,
Pederson WC. Long-term results after microlymphatico-venous
anastomoses for the treatment of obstructive lymphedema.
Plast Reconstr Surg 1990; 85:562.
17. Baumeister RG, Siuda S. Treatment of lymphedemas by micro-
surgical lymphatic grafting: what is proved? Plast Reconstr Surg
1990; 85:64.
18. Moore KL. The circulatory system. In: Moore KL, ed. The Develop-
ing Human, 3rd edn. Philadelphia: WB Saunders, 1982:296.
19. Leak LV. Electron microscopic observations on lymphatic capillar-
ies and the structural components of the connective tissuelymph
interface. Microvasc Res 1970; 2:361.
20. Leak LV, Burke JF. Electron microscopic study of lymphatic capil-
laries in the removal of connective tissue uids and particulate
substances. Lymphology 1968; 1:39.
21. Ganong WF. Review of Medical Physiology, 10th edn. Los Altos, CA:
Lange Medical Publications, 1981:452.
22. Adair TH, Guyton AC. Physiology: lymph formation, its control,
and lymph ow. In: Clouse ME, Wallace S, eds. Lymphatic Imaging
Lymphography, Computed Tomography and Scintigraphy, 2nd edn.
Baltimore: Williams & Wilkins, 1985;123.
23. Witte CL, Witte MH. Circulatory dynamics and pathophysiology
of the lymphatic system. In: Rutherford RB, ed. Vascular Surgery,
5th edn. Philadelphia: WB Saunders, 2000:2110.
24. McHale NG, Roddie IC. The effect of transmural pressure on
pumping activity in isolated bovine lymphatic vessels. J Physiol
1976; 261:255.
25. Dobbins DE. Catecholamine-mediated lymphatic constriction:
involvement of alpha 1 and alpha 2 adrenoreceptors. Am J Physiol
1992; 263:H473.
26. Dobbins DE, Dabney JM. Endothelin-mediated constriction of
prenodal lymphatic vessels in the canine forelimb. Regul Pept
1991; 35:81.
27. Kinmonth JB. Chylous diseases and syndromes, including refer-
ences to tropical elephantiasis. In: Kinmonth JB, ed. The Lymphat-
ics: Surgery, Lymphography and Diseases of the Chyle and Lymph
System, 2nd edn. London: Edward Arnold, 1982:221.
28. Servelle M. Congenital malformation of the lymphatics of the
small intestine. J Cardiovasc Surg 1991; 32:159.
29. Garrett HE Jr, Richardson JW, Howard HS et al. Retroperitoneal
lymphocele after abdominal aortic surgery. J Vasc Surg 1989;
10:245.
30. Williams RA, Vetto J, Quinones-Baldrich W et al. Chylous ascites
following abdominal aortic surgery. Ann Vasc Surg 1991; 5:247.
31. Gloviczki P, Bergman RT. Lymphatic problems and revasculariza-
tion edema. In: Bernhard VM, Towne JB, eds. Complications in
Vascular Surgery, 2nd edn. St Louis: Quality Medical Publishing,
1991:366.
32. Negroni CC, Ortiz VN. Chylothorax following high translumbar
aortography: a case report and review of the literature. Bol Assoc
Med P R1988; 80:201.
PART I Vascular pathology and physiology
214
You might also like
- Breslin 2018Document93 pagesBreslin 2018Rizky RayyanNo ratings yet
- Cardiovascular LymphaticDocument17 pagesCardiovascular LymphaticFaisal Ridho SaktiNo ratings yet
- Magnetic Resonance LymphangiographyDocument14 pagesMagnetic Resonance LymphangiographyHector Hernandez-SoriaNo ratings yet
- The Physiology of The Lymphatic System: Melody A. SwartzDocument18 pagesThe Physiology of The Lymphatic System: Melody A. SwartzFeña Peña GonzalezNo ratings yet
- Anatomy of The Human Lymphatic System: Department of Surgery, University of Sao Paulo, BrazilDocument22 pagesAnatomy of The Human Lymphatic System: Department of Surgery, University of Sao Paulo, BrazilAprodita Permata YulianaNo ratings yet
- Anatomy of The Lymphatic and Immune SystemsDocument5 pagesAnatomy of The Lymphatic and Immune SystemsHebsiba PonnayyanNo ratings yet
- Anatomyand Physiologyofthe Thoraciclymphatic SystemDocument15 pagesAnatomyand Physiologyofthe Thoraciclymphatic SystemLis Borda MuñozNo ratings yet
- TanisDocument11 pagesTanisZULMA MADELINE LIBNY GUTARRA TICANo ratings yet
- (DD13-14) Anatomic Sciences PDFDocument861 pages(DD13-14) Anatomic Sciences PDFminiarNo ratings yet
- Lymph SystemDocument7 pagesLymph SystemghaiathNo ratings yet
- 07.lymphatic Sysytem 18Document24 pages07.lymphatic Sysytem 18driraja9999No ratings yet
- Lymphatics and BloodDocument9 pagesLymphatics and BloodIchokwu VivianNo ratings yet
- V. Organs of The Lymphatic System, Immune System.Document9 pagesV. Organs of The Lymphatic System, Immune System.Diya NairNo ratings yet
- Microcirculation & Lymphatics - New-1Document23 pagesMicrocirculation & Lymphatics - New-1Danial HaiderNo ratings yet
- Case VirchowsDocument14 pagesCase VirchowsShanti IntansariNo ratings yet
- (DD13-14) Anatomic SciencesDocument861 pages(DD13-14) Anatomic SciencesIndu C. R100% (2)
- Sample Essay BiologyDocument7 pagesSample Essay Biologyapi-336421734No ratings yet
- Lymph: Medicinski Engleski I Voditelj: Doc - Dr.sc. Anja KriškovićDocument13 pagesLymph: Medicinski Engleski I Voditelj: Doc - Dr.sc. Anja KriškovićJakov KončuratNo ratings yet
- Llymphatic SystemDocument14 pagesLlymphatic SystemfauziharunNo ratings yet
- Chapter 29 Lymphatic System PDFDocument24 pagesChapter 29 Lymphatic System PDFMACON824No ratings yet
- Anatomy of The Lymphatic SystemDocument86 pagesAnatomy of The Lymphatic Systemahmed elsebaeyNo ratings yet
- Anatomy Day For Message Therapy Group-CompressedDocument28 pagesAnatomy Day For Message Therapy Group-CompressedAmbg GhalyNo ratings yet
- Department of Histology, Cytology and EmbryologyDocument8 pagesDepartment of Histology, Cytology and Embryologysubmen81No ratings yet
- UNIT 5 Lymphatic SystemDocument84 pagesUNIT 5 Lymphatic SystemChandan ShahNo ratings yet
- The Lymphatic System H. S. MayersonDocument14 pagesThe Lymphatic System H. S. MayersonGio Galanti100% (1)
- Lymphatic Drainage of Head & NeckDocument96 pagesLymphatic Drainage of Head & NeckRoopa PatilNo ratings yet
- A Computer Model of The Lymphatic System PDFDocument17 pagesA Computer Model of The Lymphatic System PDFnnimrodoNo ratings yet
- Unit 5 Lymphatic SystemDocument16 pagesUnit 5 Lymphatic SystemChandan ShahNo ratings yet
- Lymphatic System REAMPDocument52 pagesLymphatic System REAMPMinale MenberuNo ratings yet
- Lymphatic Drainage of HeadDocument142 pagesLymphatic Drainage of HeadVijayendra kamath100% (2)
- Laporan Kasus VI Bahasa InggrisDocument10 pagesLaporan Kasus VI Bahasa InggrisWahyu SholekhuddinNo ratings yet
- Anatomy of The Lymphatic SystemDocument27 pagesAnatomy of The Lymphatic SystemAntonio Lima Filho100% (2)
- 10.7 The Lymphatic System Extra NotesDocument5 pages10.7 The Lymphatic System Extra NotesVinieysha LoganathanNo ratings yet
- Notes 20Document3 pagesNotes 20Paris ShaShaNo ratings yet
- Lymphatics BD BloodDocument10 pagesLymphatics BD BloodIchokwu VivianNo ratings yet
- The Anatomy of The Immune System (Lymphatic SystemDocument4 pagesThe Anatomy of The Immune System (Lymphatic SystemMohammed R.HusseinNo ratings yet
- Anatomy of The Lymphatic and Immune Systems - NoteDocument18 pagesAnatomy of The Lymphatic and Immune Systems - NoteRashini FernandoNo ratings yet
- Management of ChylothoraxDocument11 pagesManagement of ChylothoraxLapjag BedahNo ratings yet
- Lymphocyte Homing and AdhesDocument13 pagesLymphocyte Homing and AdhesKhadija RanaNo ratings yet
- Lymphatic System: ReferencesDocument2 pagesLymphatic System: ReferencesdearbhupiNo ratings yet
- Chapter 16Document9 pagesChapter 16g_komolafeNo ratings yet
- Assignment#4: Submitted To: Maam Arooj Ameer HamzaDocument9 pagesAssignment#4: Submitted To: Maam Arooj Ameer HamzaHamza MalikNo ratings yet
- Lymphoedema of Upper Limb: DR G Avinash Rao - Fellow Hand and MicrosurgeryDocument93 pagesLymphoedema of Upper Limb: DR G Avinash Rao - Fellow Hand and Microsurgeryavinashrao39No ratings yet
- Lymphatic SystemDocument13 pagesLymphatic SystemCharli ParachinniNo ratings yet
- Chapter 22 Summary Chapter 22 SummaryDocument13 pagesChapter 22 Summary Chapter 22 SummarytinecastilloNo ratings yet
- Fisiopatologia Linfedema 1997Document6 pagesFisiopatologia Linfedema 1997ktorooNo ratings yet
- The Lymphatics in Kidney Health and Disease: Michael D. Donnan, Yael Kenig-Kozlovsky and Susan E. QuagginDocument21 pagesThe Lymphatics in Kidney Health and Disease: Michael D. Donnan, Yael Kenig-Kozlovsky and Susan E. QuagginsilviaNo ratings yet
- Lymphatic Trunks Ass 5Document12 pagesLymphatic Trunks Ass 5Hamza MalikNo ratings yet
- The Lymphatic SystemDocument16 pagesThe Lymphatic SystemColeen Joyce NeyraNo ratings yet
- Chapter 16: Lymphatic System and Immunity: Shier, Butler, and Lewis: Hole's Human Anatomy and Physiology, 13Document18 pagesChapter 16: Lymphatic System and Immunity: Shier, Butler, and Lewis: Hole's Human Anatomy and Physiology, 13Elvin MoletaNo ratings yet
- Abiola Seminar in SpleenDocument23 pagesAbiola Seminar in SpleenBamgbose OpeyemiNo ratings yet
- 1.4 The Lymphatic SystemDocument11 pages1.4 The Lymphatic SystemCikdar Yunus100% (1)
- Anatomy of Lymphatics SystemDocument9 pagesAnatomy of Lymphatics Systemtg856qr4mwNo ratings yet
- Urinary SystemDocument64 pagesUrinary SystemAlishba AslamNo ratings yet
- Lymph Vascular SystemDocument12 pagesLymph Vascular Systemmichaelsoncole410No ratings yet
- 1.4 The Lymphatic System: Prepared By: Ling Mei TengDocument15 pages1.4 The Lymphatic System: Prepared By: Ling Mei TengJuliet LingNo ratings yet
- Lymph Health: The Key to a Strong Immune SystemFrom EverandLymph Health: The Key to a Strong Immune SystemRating: 5 out of 5 stars5/5 (1)
- Lateral and Medial Epicondylitis Role of Occupational FactorsDocument15 pagesLateral and Medial Epicondylitis Role of Occupational FactorsSAKAI69No ratings yet
- Diagnosis and Treatment of Medial Epicondylitis of The ElbowDocument13 pagesDiagnosis and Treatment of Medial Epicondylitis of The ElbowSAKAI69No ratings yet
- Biomechanical Models For The Pathogenesis Upper Extremity DisordersDocument17 pagesBiomechanical Models For The Pathogenesis Upper Extremity DisordersSAKAI69No ratings yet
- Niosh Case MSDDocument590 pagesNiosh Case MSDAntonio NeiNo ratings yet
- Physical Examinations in Musculoskeletal Disorders of The ElbowDocument6 pagesPhysical Examinations in Musculoskeletal Disorders of The ElbowSAKAI69No ratings yet
- Psicosocial Factors and EpicondylitisDocument13 pagesPsicosocial Factors and EpicondylitisSAKAI69No ratings yet
- Jetlag PDFDocument6 pagesJetlag PDFSAKAI69No ratings yet
- 2014 The Pain of Tendinopathy - Physiological or PathophysiologicalDocument15 pages2014 The Pain of Tendinopathy - Physiological or PathophysiologicalDavid Alejandro Cavieres AcuñaNo ratings yet
- Biomechanical Models For The Pathogenesis Upper Extremity DisordersDocument17 pagesBiomechanical Models For The Pathogenesis Upper Extremity DisordersSAKAI69No ratings yet
- JetlagDocument1 pageJetlagSAKAI69No ratings yet
- Clinics in ObstetricsDocument770 pagesClinics in ObstetricsSAKAI69100% (3)
- LymphedemaDocument4 pagesLymphedemaSAKAI69No ratings yet
- Cleary TendinitisDocument42 pagesCleary TendinitisSAKAI69No ratings yet
- 1997 - Potvin & Bent - NIOSH Equation Horizontal Distances Associated With The Liberty Mutual (Snook) Lifting Table Box WidthsDocument7 pages1997 - Potvin & Bent - NIOSH Equation Horizontal Distances Associated With The Liberty Mutual (Snook) Lifting Table Box WidthsSAKAI69No ratings yet
- Jet LagDocument98 pagesJet LagSAKAI69No ratings yet
- Understanding and Counteracting Fatigue in Flight Crews: Ames Research Center, Moffett Field, CaliforniaDocument1 pageUnderstanding and Counteracting Fatigue in Flight Crews: Ames Research Center, Moffett Field, CaliforniaSAKAI69No ratings yet
- Dennerlein, Forearm LFF, AIHA2003Document8 pagesDennerlein, Forearm LFF, AIHA2003SAKAI69No ratings yet
- 126999Document15 pages126999SAKAI69No ratings yet
- JoL Quality of Life MeasuresDocument12 pagesJoL Quality of Life MeasuresSAKAI69No ratings yet
- Kurzbetriebsanleitung Junkers Ju 87 D-3 Für Den Flugzeugführer - EnglishDocument3 pagesKurzbetriebsanleitung Junkers Ju 87 D-3 Für Den Flugzeugführer - EnglishSAKAI69No ratings yet
- Kagero Asy Lotnictwa 02 Josef Priller, Hans Waldmann, Wolfgang SpateDocument30 pagesKagero Asy Lotnictwa 02 Josef Priller, Hans Waldmann, Wolfgang SpateRaul Garcia100% (5)
- Distocia de Hombro PDFDocument4 pagesDistocia de Hombro PDFSAKAI69No ratings yet
- NASA News: National Aeronautics and Space Administration Washington. DC 20546 AC 202 755-8370Document4 pagesNASA News: National Aeronautics and Space Administration Washington. DC 20546 AC 202 755-8370SAKAI69No ratings yet
- 2012 - Potvin - An Equation To Predict Maximum Acceptable Loads For Repetitive Tasks Based On Duty Cycle - Evaluation With Lifting and Lowering TasksDocument5 pages2012 - Potvin - An Equation To Predict Maximum Acceptable Loads For Repetitive Tasks Based On Duty Cycle - Evaluation With Lifting and Lowering TasksSAKAI69No ratings yet
- Lymphedema: Clinical Picture, Diagnosis and Management: Tanja Planinšek Ru Čigaj and Vesna Tlaker ŽunterDocument17 pagesLymphedema: Clinical Picture, Diagnosis and Management: Tanja Planinšek Ru Čigaj and Vesna Tlaker ŽunterSAKAI69No ratings yet
- Lymphedema 101: Part 1: Understanding The Pathology and DiagnosisDocument5 pagesLymphedema 101: Part 1: Understanding The Pathology and DiagnosisSAKAI69No ratings yet
- Lymphedema ReviewDocument8 pagesLymphedema ReviewSAKAI69No ratings yet
- The Pathophysiology of LymphedemaDocument4 pagesThe Pathophysiology of LymphedemaSAKAI69No ratings yet
- Post Lymphedema 1Document7 pagesPost Lymphedema 1SAKAI69No ratings yet
- Ultrafiltration and Its Application in Food Processing: October 2015Document15 pagesUltrafiltration and Its Application in Food Processing: October 2015Doina PolisciucNo ratings yet
- MfA Leadership ExperienceDocument49 pagesMfA Leadership ExperienceAlex MoralesNo ratings yet
- TCVN 6560-1999 Air Quality For Incinerator (En)Document2 pagesTCVN 6560-1999 Air Quality For Incinerator (En)Pn ThanhNo ratings yet
- Hazop PDFDocument18 pagesHazop PDFLuiz Rubens Souza Cantelli0% (1)
- Villegas Lucero 1Document8 pagesVillegas Lucero 1api-213921706No ratings yet
- NBR Leaflet Krynac 4955vp Ultrahigh 150dpiwebDocument2 pagesNBR Leaflet Krynac 4955vp Ultrahigh 150dpiwebSikanderNo ratings yet
- Lecture 1 Introduction To Industrial HygieneDocument40 pagesLecture 1 Introduction To Industrial Hygienesiti zubaidahNo ratings yet
- AICTE CorporateBestPracticesDocument13 pagesAICTE CorporateBestPracticesramar MNo ratings yet
- AAP ASD Exec SummaryDocument7 pagesAAP ASD Exec SummaryCatherine AgustinNo ratings yet
- Quality Manual: Pt. Ani Mitra Jaya Frozen ChepalopodDocument1 pageQuality Manual: Pt. Ani Mitra Jaya Frozen ChepalopodMia AgustinNo ratings yet
- IELTS 1 Test IntroDocument1 pageIELTS 1 Test IntromichaelNo ratings yet
- Chapter 020Document59 pagesChapter 020api-263755297No ratings yet
- Brazilian Sanitary Guide For Cruise ShipsDocument82 pagesBrazilian Sanitary Guide For Cruise ShipsStanislav KozhuharovNo ratings yet
- Mastertile A 200 Msds PDFDocument11 pagesMastertile A 200 Msds PDFyaswanth reddy mummadiNo ratings yet
- Mira Nepali CV OnlyDocument3 pagesMira Nepali CV OnlydistanceindistanceNo ratings yet
- Kinds of Blood. Differences Between Men and WomenDocument11 pagesKinds of Blood. Differences Between Men and WomenTiagoSantosNo ratings yet
- Group 2 - Up-Fa1-Stem11-19 - Chapter IiDocument7 pagesGroup 2 - Up-Fa1-Stem11-19 - Chapter IijamesrusselNo ratings yet
- Ramsay Sedation Scale and How To Use ItDocument10 pagesRamsay Sedation Scale and How To Use ItAdinda Putra PradhanaNo ratings yet
- De Anisya Tri Ab - CBD - 30101507419 - FixDocument198 pagesDe Anisya Tri Ab - CBD - 30101507419 - FixFarah UlyaNo ratings yet
- Govindarajan Reverse Innovation Chapter1Document10 pagesGovindarajan Reverse Innovation Chapter1hvactrg1No ratings yet
- BDSM Checklist: General InformationDocument6 pagesBDSM Checklist: General Informationmiri100% (1)
- Good Knight 420 GPatien ManualDocument30 pagesGood Knight 420 GPatien ManualJose Antonio AlcazarNo ratings yet
- Pediatrics-AAP Guideline To SedationDocument18 pagesPediatrics-AAP Guideline To SedationMarcus, RNNo ratings yet
- Introduction To Epidemiology: The Basic Science of Public HealthDocument34 pagesIntroduction To Epidemiology: The Basic Science of Public Healthapi-19641337100% (1)
- The Dandenong Dossier 2010Document243 pagesThe Dandenong Dossier 2010reshminNo ratings yet
- Vince Gironda 8x8 RoutineDocument10 pagesVince Gironda 8x8 RoutineCLAVDIVS0% (2)
- Junal 1Document6 pagesJunal 1indadzi arsyNo ratings yet
- HSMAI PHG - New Rules To Be Market ReadyDocument28 pagesHSMAI PHG - New Rules To Be Market ReadyAnna ShortNo ratings yet
- STATES Act Fact SheetDocument1 pageSTATES Act Fact SheetMichael_Lee_RobertsNo ratings yet
- Urbanization and HealthDocument2 pagesUrbanization and HealthsachiNo ratings yet