Professional Documents
Culture Documents
Handbook of Anastesia PDF
Handbook of Anastesia PDF
Uploaded by
Muhammad IhsanuddinOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Handbook of Anastesia PDF
Handbook of Anastesia PDF
Uploaded by
Muhammad IhsanuddinCopyright:
Available Formats
2
Airway Management
M Ranganathan
C Mendonca
The key aim of airway management is to clear or bypass the obstructed airway, assist or
replace spontaneous ventilation and protect the lungs from aspiration. Obstructed airway
due to impaired or loss of consciousness is common in patients who are critically ill or
patients requiring resuscitation and infrequently this may be the principal cause of
cardiorespiratory arrest. Rapid assessment and institution of a patent airway, ventilation
and oxygenation of lungs is essential in preventing secondary damage to the brain and
other organs due to hypoxia. A wide range of airway management devices are available
(Table 2.1). Choice of device depends on the individual patient and the experience of the
attending medical or paramedical personnel. Airway devices can be generally classified in
to two groups, those which are less invasive and placed above the level of glottis are
known as supra-glottic devices. Those that place within the trachea (below the level of
glottis) are known as infra-glottic devices. Although several of them have been
introduced in to the clinical practice in recent years, only a few established devices are
mentioned in the table below.
Table 2.1 Airway management devices.
Device Experience required Definitive
Supra-glottic
Bag and mask yes no
LMA no no
Infra-glottic
Tracheal tube yes yes
Cricothyroidotomy yes no
Tracheostomy yes yes
Causes of airway obstruction
The airway obstruction can occur anywhere from nose and mouth down to bronchial level
and can be partial or total. The commonest site of airway obstruction in the unconscious
patient is at the level of pharynx due to the tongue and surrounding soft tissue falling
back because of loss of muscle tone. Soft palate and epiglottis can also produce airway
obstruction in an unconscious patient. Regurgitation of food or blood from stomach may
also produce obstruction as also by foreign body. Laryngeal obstruction can occur as a
result of spasm of laryngeal muscles (occurring as a result of stimulation of upper airway
or due to inhaled foreign body) or laryngeal oedema (as a result of burns, inflammation or
anaphylaxis). Infra laryngeal airway obstruction can occur as a result of excessive
Warwick Medical School- Handbook of Anaesthesia 2006 1
secretions, mucosal oedema, bronchospasm, pulmonary oedema or aspiration of gastric
contents.
Detection of airway obstruction
Airway obstruction can be recognised by looking, listening and feeling.
• Look for chest and abdominal movements
• Listen and feel for airflow at the mouth and nose
With the airway obstruction in a patient who is breathing spontaneously the accessory
muscles of respiration come into play with the neck and shoulder muscles contracting to
assist the expansion of thoracic cage. In a patient with complete airway obstruction, the
spontaneous respiratory effort produces paradoxical chest and abdominal movement.
During normal breathing chest and abdomen moves synchronously, during inspiration the
chest expands and the diaphragm pushed down with opposite happening during
expiration. In complete airway obstruction during inspiration, chest expands and
abdomen is drawn in with opposite happening during expiration, called ‘see-saw
breathing’. This is accompanied by absent of breath sounds on auscultation of the chest to
diagnose complete airway obstruction.
Airway obstruction can also be partial, in which case air entry is diminished and usually
noisy. There are different noises occurring in obstructed airway:
• Inspiratory stridor – caused by obstruction at or above laryngeal level.
• Expiratory wheeze – obstruction of the lower airways
• Gurgling – due to presence of liquid or semisolid material in the major airways
• Snoring – due to partially occluded pharynx by the tongue or palate
• Crowing – the sound of laryngeal spasm or obstruction
It is important to remember that normal breathing is quiet, partially obstructed breathing
is noisy while complete airway obstruction is silent. The airway obstruction should be
relieved promptly to allow breathing to occur; otherwise the neurologic and other vital
organ injury including cardiac arrest would occur.
Basic airway management
Open the patient’s mouth to see and remove if any foreign body, vomiting or secretion in
the oral cavity. Foreign bodies should be removed using a finger sweep and secretions or
vomiting should be sucked out using wide bore rigid sucker such as Yankauer. This
should be done before attempting to open the obstructed airway due to tongue or other
upper airway structures. There are three manoeuvres that can be used to relieve the
obstruction caused by the tongue.
• Head tilt – can be attained by placing one hand on the patient’s forehead and tilting
the head back gently, keeping the thumb and index finger free to close patient’s nose
if rescue breathing is required (figure 2.1).
Warwick Medical School- Handbook of Anaesthesia 2006 2
Figure 2.1 Head tilt and chin Figure 2.2 Jaw thrust
lift manoeuvre manoeuvre
• Chin lift: Patient’s chin is lifted to open the airway using the finger tips of the other
hand (figure 2.1).
• Jaw thrust: After identifying the angle of the mandible, the ring and little fingers are
placed behind the angle, the index and middle finger placed over the body of
mandible to apply steady upwards and forward pressure to lift the mandible. The
thumbs are used to open the mouth slightly by downward displacement of the chin
(figure 2.2). This is the only technique that can be done if there is a suspicion of
cervical spine injury.
Make sure that after each manoeuvre that the airway obstruction is relieved by looking,
listening and feeling. If the obstruction is not relieved, other causes of airway obstruction
must be sought.
Oxygen
Oxygen should always be administered in highest concentration available. A mask with a
reservoir bag can give an oxygen concentration of 85% at flows of 10-15 litres/min. With
high flows, an ordinary oxygen mask should deliver oxygen up to 50%, a venturi mask
delivers 24-60% depending on the mask chosen. The oxygen administration should never
be discontinued except for the brief period for airway interventions designed to improve
the patency of the airway.
Basic airway adjuncts
On occasions especially during prolonged resuscitation basic airway adjuncts like
oropharyngeal and nasopharyngeal airways are quite useful to maintain an open airway.
Head tilt and chin lift may also be required apart from using one of the airway adjuncts.
Oropharyngeal airway (Guedel airway) [figure 2.3]
Warwick Medical School- Handbook of Anaesthesia 2006 3
It is a curved tube made of plastic, flanged and reinforced at the oral end with a flattened
shape to ensure that it fits correctly between the tongue and the hard palate. It is available
in various sizes to suit new to large adults. For small, medium and large adults the sizes
used are 2, 3 and 4 respectively.
A rough estimate of the size required may be obtained by selecting an airway with a
length corresponding to the vertical distance between the patient’s incisors and the angle
of the mandible (figure 2.4).
Figure 2.3 Oropharyngeal Figure 2.4 Sizing oropharyngeal
airways in different sizes airway
Technique of inserting oropharyngeal airway: Patient’s mouth is opened and the airway
is introduced so that the curvature (concavity) faces towards the palate until the tip of the
airway reaches the junction between hard and soft palate and then the airway is rotated
through 180°. It is then inserted until it lies in the oropharynx. The rotation technique
reduces the chance of pushing the tongue backwards and downwards. Correct positioning
of the airway is indicated by improvement in the airway patency and by the seating of the
flattened reinforced section of the airway between patient’s incisors or alveolar margins.
Problems associated with oropharyngeal airway insertion:
o Too small airway can push the tongue backwards and worsen the airway
obstruction. Too large airway can bypass the laryngeal inlet and fail to correct the
airway obstruction.
o Vomiting or laryngospasm can occur if the glossopharyngeal and laryngeal
reflexes are intact.
o Damage to teeth, dislodgement of caps, crown, mucosal trauma and bleeding can
occur.
Nasopharyngeal airway (figure 2.5)
Warwick Medical School- Handbook of Anaesthesia 2006 4
It is a soft rubber or plastic, bevelled at one end and with a flange at the other and is better
tolerated than the oropharyngeal airway in a patient who is not deeply unconscious. It
may be life saving in patients with clenched jaws, trismus or maxillofacial injuries. The
airway is sized in mm according to the internal diameter and the length increases with
increasing in diameter. Commonly used adult sizes are 6-7 mm (compare it with patient’s
little finger). Some designs (e.g., Portex) may require a safety pin to be inserted through
the flange to provide an extra precaution against the airway going too deep in to the
nostril.
Technique of inserting nasopharyngeal airway: The patency of the nostril to be checked
and the airway is well lubricated using a water soluble jelly. The airway inserted
vertically along the floor of the nose with the bevel end first with slight twisting action. If
any obstruction is felt and remove the airway and the other nostril to be tried.
Figure 2.5 Nasopharyngeal airway
Problems associated with nasopharyngeal airway insertion:
o Trauma to the nasal mucosa, turbinates and adenoids
o Bleeding
Nasopharyngeal airway is contraindicated in patients with suspected base of skull fracture
and bleeding diathesis.
After placing the oropharyngeal or nasopharyngeal airways the patency of the airway has
to be checked by looking, listening and feeling.
Ventilation
Artificial ventilation should be initiated in patients with inadequate or absent ventilation.
Self-inflating bag can be connected either to a facemask (bag-mask), laryngeal mask or
tracheal tube and high concentration of oxygen can be administered using this device
Warwick Medical School- Handbook of Anaesthesia 2006 5
(figure 2.6). As with most airway management techniques the bas-mask ventilation
requires time and experience to master. Many designs of the face masks are available and
transparent masks are recommended. As the bag is squeezed, the contents are delivered to
the patient’s lungs. On release, the expired gas is diverted to the atmosphere via a one-
way valve and the bag then refills automatically via an inlet at the opposite end. The bag-
mask device can be ventilated with air alone (FiO2 0.21) but addition of oxygen of 5-6
litres/min., directly to the bag adjacent to the air intake, would increase the FiO2 to 45%.
If a reservoir bag is attached in series to the self-inflating bag and the FiO2 can be
increased to 85% if oxygen flow is increased to10 litres/min.
Figure 2.6 Self inflating bag, valve and Figure 2.7 Two person bag and mask
m ask device. ventilation.
Frequently it is difficult to achieve a gas-tight seal between the mask and the patient’s
face, and simultaneously performing head and neck alignment with a jaw thrust with one
hand and squeezing the bag with the other hand. Any leak will result in hypoventilation.
It is better to correct this by achieving an air tight seal between the mask and the patient’s
face using two-person technique in which one person holds the mask and the other person
squeezes the bag (figure 2.7). Poorly applied cricoid pressure may also make it more
difficult to ventilate as also incorrectly applied airway opening techniques or airway
adjuncts.
Advanced airway techniques
Laryngeal mask airway (LMA) [figure 2.8]
Use by inexperienced personnel is likely to result in hypoventilation due to ineffective
tidal volumes and gastric inflation with bag-mask device. The LMA and endotracheal
tubes are alternative airway devices that, in comparison lessen the chances of gastric
inflation and at the same time allowing more effective ventilation.
Warwick Medical School- Handbook of Anaesthesia 2006 6
2 3
1 4
1. Laryngoscope 2. Catheter mount
3. Tracheal tube 4. Laryngeal mask airway
Figure 2.8 Airway equipment
It consists of wide bore silicone tube connected to a distal elliptical spoon-shaped mask
with in inflatable rim, which is positioned blindly into the pharynx to form a low pressure
seal against the laryngeal inlet. It results in more efficient and easier ventilation resulting
in lesser chances of regurgitation during cardiac arrest than with a bag-mask assembly. If
high pressures (>20 cm H2O) are avoided, gastric inflation can be minimised when used
for intermittent positive pressure ventilation. Pulmonary aspiration is uncommon with the
usage of LMA though there is no absolute guarantee against pulmonary aspiration. Since
usage of LMA requires less head and neck movement, LMA may be the airway device of
choice in patients with suspected cervical spine injury. Like tracheal intubation it requires
the patient to be deeply unconscious. LMA is also indicated for managing difficult airway
where mask ventilation or endotracheal intubation may be difficult.
Table 2.2. Selection of appropriate size of LMA according to patient’s weight.
Patients wt. (kg) <5 5-10 10-20 20-30 30-50 50-70 70-100
LMA size 1 11/2 2 21/2 3 4 5
Max. cuff inflation 4 7 10 14 20 30 40
volume (ml)
Warwick Medical School- Handbook of Anaesthesia 2006 7
Technique of inserting LMA: The LMA of appropriate size should be chosen (table 2.2)
and the cuff should be checked by inflating with appropriate volume of air. Then the cuff
is completely deflated and the outer surface of the cuff is lubricated using water soluble
jelly. Ideally the head and neck should be aligned with the neck slightly flexed and head
extended at atlanto-occipital joint (classical “sniffing” position). This position is
contraindicated in patients with suspected cervical spine injury or unstable cervical spine
where the LMA can be inserted in neutral head position with manual in line stabilistaion.
The LMA insertion technique is based on an imitation of swallowing mechanism, with
the aim of avoiding collision with highly innervated anterior pharyngeal structures such
as epiglottis, larynx and arytenoids. It is introduced into the patient’s mouth with the
aperture facing forward, (black line facing towards patient’s upper lip) holding between
the index finger and thumb at the junction of mask and tube. The tip of the LMA is held
behind the upper incisor, pressed against the hard palate (figure 2.9a), then gently
advanced in to the oropharynx. The right index finger is used to guide the mask along the
palato-pharyngeal axis and gently pushed forwards (figure 2.9b) until a firm resistance is
encountered. Should not use any force to push the LMA which may result wrong
placement and trauma. Now the index finger is gently withdrawn from the oropharynx,
grasping the tube part of LMA with other hand. The cuff is then inflated and if the
position is satisfactory the tube will lift one or two centimeters out of the mouth as the
cuff finds its correct position. When correctly inserted the tip of LMA rests against the
upper oesophageal sphincter (figure 2.9c). If the LMA can’t be inserted even after 30
seconds, patient needs reoxygenation before another attempt at the insertion of LMA. The
confirmation of clear airway is done by auscultating the chest during inspiration, noting
bilateral chest movement and by capnography. A small leak is acceptable provided there
is adequate air entry. A bite block should be inserted alongside the LMA.
2.9a 2.9b
Figure 2.9a and 2.9b. Insertion of LMA
Warwick Medical School- Handbook of Anaesthesia 2006 8
Larynx
Trachea
Oesophagus
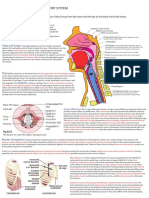
Figure 2.9c Correctly positioned LMA with tip resting against the upper
oesophageal sphincter.
Advantages of LMA
o Muscle relaxants can be avoided
o The problems associated with laryngoscopy and tracheal intubation can be minimized
o Sympatho-adrenal response is less than tracheal intubation
o Recovery phase is smooth with fewer incidences of airway problems in recovery
o LMA has been used in the management of difficult airway both in elective and
emergency situation.
Limitations of the LMA
1. There is a risk of hypoventilation due to large leak in patients with high airway
pressure due to high airway resistance or poor lung compliance (pulmonary oedema,
bronchospasm, chronic obstructive airway disease).
2. If the patient is not unconscious enough to accept the LMA, the patient may cough,
strain or develop laryngeal spasm.
3. Airway obstruction may result from the epiglottis being folded down to cover the
laryngeal inlet or by incorrect position of LMA
4. LMA is contraindicated during major surgery and in patients with increased risk of
aspiration
o Full stomach
o Hiatus hernia with active reflux
o Morbidly obese patient
5. Trauma to oropharyngeal structures and teeth damage is possible if appropriate care is
not taken during insertion.
Warwick Medical School- Handbook of Anaesthesia 2006 9
6. Sore throat, glossopharyngeal nerve palsy, hypoglossal nerve palsy, dysphagia and
hoarse voice can occur after prolonged use or due to high inflation pressure of the cuff.
Endotracheal intubation
Endotracheal intubation is considered to be the optimal form of airway management and
to be used only when trained personnel are available to carry out the procedure. Tracheal
intubation is considered to be superior to other advanced airway management techniques
for the following reasons:
1. Airway is reliably isolated from foreign material in the oropharynx.
2. Suction of inhaled particles from the lower respiratory tract is possible.
3. More effective ventilation of lungs.
Tounge
Vallecula
Epiglottis Vocal fold
Aryepiglottic fold
Cuneiformcartilage
Corniculate cartilage Trachea
Figure 2.10 Larynx as visualized during direct laryngoscopy
Laryngoscope is needed apart from appropriate sized endotracheal tube (Figure 2.8). In
some situations laryngoscopy and intubation may prove impossible as in epiglottitis,
pharyngeal pathology etc for which anaesthetic drugs or fibreoptic laryngoscopy may be
required. Following are the potential complications that can occur:
1. Difficult or impossible to intubate – can occur with epiglottitis, pharyngeal pathology,
anatomical abnormalities like short obese neck, receding chin, buck teeth, pathology such
as maxillo-facial fractures, facial burns etc. It is important to remember that failure to
oxygenate the patient in case of difficult intubation by bag and mask or any other means
can lead to hypoxia and brain damage.
2. Cardiovascular response: Laryngoscopy and tracheal intubation produces sympathetic
stimulation resulting in tachycardia and hypertension. In children it can be associated
with bradycardia.
Warwick Medical School- Handbook of Anaesthesia 2006 10
3. Damage to the teeth, soft tissue injury of the oropharynx, trauma to the larynx, and
trachea.
4. Pulmonary aspiration during the process of induction of general anaesthesia
5. Oesophageal intubation – endotracheal intubation should be confirmed by capnometry
apart from seeing the tube passing through the vocal cords wherever possible. Failure to
recognise oesophageal intubation can lead to hypoxia and brain damage.
6. Tracheal tube displacement and blockage of the tube with secretions.
7. In patients with unstable cervical spine, laryngoscopy and tracheal intubation may
cause further damage.
Extensive training and regular practice is required to acquire and maintain the skills of
intubation.
Management of a difficult airway
The report of American Society of Anaesthesiologists (ASA) Task Force on the
management of difficult airway defines difficult airway as “the clinical situation in which
a conventionally trained anaesthesiologist experiences difficulty with mask ventilation,
difficulty with tracheal intubation or both”.
A careful airway examination can predict difficulty in both mask ventilation and tracheal
intubation. When difficult airway anticipated during the preoperative assessment, there is
enough time available to plan the management. In certain circumstances one may not
predict difficult airway but after induction of general anesthesia it may turn out to be
difficult to manage the airway both in terms of bag-mask ventilation (can’t ventilate) and
in terms of tracheal intubation (can’t intubate).
Warwick Medical School- Handbook of Anaesthesia 2006 11
Algorithm for failed intubation
Plan A:
Direct Laryngoscopy succeed
Initial tracheal Tracheal
intubation plan intubation
Failed intubation
Plan B: LMA or ILMA succeed
Secondary tracheal Fibreoptic assisted
intubation plan Tracheal intubation
via LMA or ILMA
Failed oxygenation
Plan C:
Maintenance of Revert to face mask,
oxygenation, oral /nasopharyngeal Post pone surgery and
succeed
ventilation, airway, oxygenate & awaken the patient
postponement of ventilate
surgery and
awakening
Warwick Medical School- Handbook of Anaesthesia 2006 12
Failed oxygenation
Plan D:
Rescue techniques
for can’t intubate, Surgical airway: jet ventilation
can’t ventilate catheter or quick trach or surgical
situation cricothyrotomy
Difficult airway trolley: It consists of various equipment for managing difficult airway
arranged in a systematic order.
Following equipments are usually available on a difficult airway trolley.
o Laryngoscopes : McCoy, Straight blade ( Miller or Hnaderson) and polio blade
o Frova tracheal introducer or Gum elastic bougie
o Laryngeal mask airway, Intubating laryngeal mask airway (ILMA)
o Microlaryngoscopy Tracheal tube (MLT)
o Cricothyrotomy devices: Jet ventilation catheters and manual jet ventilation
device, size 6 tracheostomy tube, scalpel, tracheal hook.
o Aintree catheter (for fibreoptic intubation via LMA)
o Cook airway exchange catheter (in ENT/Max fac theatre for nasal ETT exchange)
o Flexible intubating fibreoptic scope
Figure 2.11 Flexible intubating fibreoptic scope
Awake tracheal intubation: is usually considered in an anticipated difficult tracheal
intubation. After explaining the technique, patient’s airway (nasopharynx, oropharynx,
Warwick Medical School- Handbook of Anaesthesia 2006 13
larynx and part of trachea) is anaesthetised using local anaesthetic. Tracheal intubation is
performed using a flexible intubating fibreoptic scope, before induction of general
anaesthesia
Tracheostomy: Tracheostomy is a surgically created opening in the neck into the trachea.
Following are the main indications for tracheostomy.
• To bypass the airway obstruction
o For certain surgical procedures – e.g. laryngectomy.
o Trauma involving upper airway when tracheal intubation is likely to be
impossible.
o Inhalation of hot smoke or corrosives – e.g. after burns.
o Laryngeal dysfunction due to vocal cord palsy or tracheomalacia.
o Congenital anomalies such as glottic stenosis.
• For tracheal toilet – for long term care of patient with neuromuscular weakness or
coma.
• In ICU – for mechanical ventilation more than few days.
There are no absolute contraindications for tracheostomy, though conditions like
coagulopathy warrant special attention before the procedure. Tracheostomy can be done
by open surgical method commonly in operating theatre or percutaneous surgical
tracheostomy usually done on bedside in ICU. Percutaneous tracheostomy offers
advantages in the sense that seriously ill patient in ICU does not have to be transferred to
operating theatre, it is quicker, has lower incidence of bleeding and infection.
There are various complications of tracheostomy which can be classified as early and late.
The main early complication is haemorrhage. Other important complications include
misplacement of the tracheostomy tube, perforation of the posterior wall of trachea and
oesophagus and scarring. Tracheo-oesophageal fistula is a rare complication resulting
from trauma or necrosis of the posterior wall of the trachea. Tracheostomy stoma will be
formed within 3 days, this allows safe replacement of tracheostomy tube. If the tube is
dislodged during initial 48 hrs, tracheal dilator is required to replace the tube.
Following tracheostomy appropriate care should be taken to prevent infection and
atelectasis. Artificial humidity, breathing exercises and regular tracheal suction is
required.
Further reading
Bersten A et al. Oh’s Intensive Care Manual, 5th Edn. London: Butterworth-Heinemann,
2005.
Advanced Life Support Course. Provider Manual, 4th Edn. (Revised). London:
Resuscitation Council (UK) & ERC, 2000.
Brimacombe JR. Laryngeal Mask Anesthesia, 2nd Edn. London: Elsevier Limited, 2005.
Warwick Medical School- Handbook of Anaesthesia 2006 14
Henderson JJ, Popat MT, Latto IP, Pearce AC. Difficult airway society guidelines for
management of the unanticipated difficult intubation. Anaesthesia 2004; 59: 675-694.
Susanto I. Comparing percutaneous with open surgical tracheostomy. BMJ 2002; 324:3-
4.
Irwin RS, J M Rippe JM. Manual of Intensive Care Medicine, 4th Edn. Philadelphia:
Lippincott Williams & Wilkins, 2005.
Warwick Medical School- Handbook of Anaesthesia 2006 15
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5810)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- 438-Operative Anatomy - 3rd Edition (2 Volumes in One Ebook) - Carol E.H. Scott-Conner - David L. DawDocument1,334 pages438-Operative Anatomy - 3rd Edition (2 Volumes in One Ebook) - Carol E.H. Scott-Conner - David L. DawSuci Amalya Uchiil100% (26)
- Science 9 Q1 Module 1 Respiratory and Circulatory With Key AnswerDocument42 pagesScience 9 Q1 Module 1 Respiratory and Circulatory With Key AnswerJan Ice90% (130)
- 3 - FBS 45 - Internal Anatomy of InsectsDocument47 pages3 - FBS 45 - Internal Anatomy of InsectsYeye bonnellNo ratings yet
- The Prognostic Impact of Tumor Mutational BurdenDocument14 pagesThe Prognostic Impact of Tumor Mutational BurdenEinz Nur Amalyah IdrusNo ratings yet
- J Medula Unila. 2017 7 (2) : 103-7.: Daftar PustakaDocument3 pagesJ Medula Unila. 2017 7 (2) : 103-7.: Daftar PustakaEinz Nur Amalyah IdrusNo ratings yet
- Translate Indo-Eng AsdDocument13 pagesTranslate Indo-Eng AsdEinz Nur Amalyah IdrusNo ratings yet
- Rina Previana, Umar MalintaDocument1 pageRina Previana, Umar MalintaEinz Nur Amalyah IdrusNo ratings yet
- PerforasiDocument3 pagesPerforasiEinz Nur Amalyah IdrusNo ratings yet
- PEMBAHASAN EnglishDocument12 pagesPEMBAHASAN EnglishEinz Nur Amalyah IdrusNo ratings yet
- DisasterDocument5 pagesDisasterEinz Nur Amalyah IdrusNo ratings yet
- Answer Key Airway Final CoachingDocument13 pagesAnswer Key Airway Final CoachingCharmaine LingdasNo ratings yet
- Respiratory Notes (Chris Andersen, ICUPrimaryPrep - Com)Document14 pagesRespiratory Notes (Chris Andersen, ICUPrimaryPrep - Com)PkernNo ratings yet
- Basic Avian AnatomyDocument10 pagesBasic Avian AnatomyHarry MontriNo ratings yet
- Advanced Pediatric AssessmentDocument30 pagesAdvanced Pediatric Assessmentisapatrick8126100% (1)
- Respiratory System Insects 2Document4 pagesRespiratory System Insects 2KIPNGETICH FREDRICKNo ratings yet
- Corpus Alienum EsophagusDocument3 pagesCorpus Alienum EsophagusTrhey Ahmilza DamaitaNo ratings yet
- 9999064582Document32 pages9999064582naamashirNo ratings yet
- BreathingDocument46 pagesBreathingRamnaresh SharmaNo ratings yet
- Human Digestive SystemDocument11 pagesHuman Digestive SystemSyeda NafeezaNo ratings yet
- s.3 Bio. Respiration and Gaseous Exchange NotesDocument25 pagess.3 Bio. Respiration and Gaseous Exchange NotesKyopaire TobiaNo ratings yet
- Animal Dietary Category Feeding MechanismDocument2 pagesAnimal Dietary Category Feeding MechanismGenavel Del RosarioNo ratings yet
- Respiratory System Semi FinalDocument60 pagesRespiratory System Semi FinalMichelle AnteneroNo ratings yet
- Stridor or WheezeDocument29 pagesStridor or Wheezekrishna mandalNo ratings yet
- Acta Scientiae Veterinariae 1678-0345: Issn: Actascivet@Document5 pagesActa Scientiae Veterinariae 1678-0345: Issn: Actascivet@AlejandraNo ratings yet
- Assessment of The Head and NeckDocument10 pagesAssessment of The Head and NeckAngela BaldozaNo ratings yet
- English VersionDocument20 pagesEnglish Versionistinganatul muyassarohNo ratings yet
- Tracheostomy Techniques and ManagementDocument9 pagesTracheostomy Techniques and Managementtaner_soysuren100% (1)
- Histology RespiratoryDocument35 pagesHistology Respiratorykhiks34100% (2)
- Breath SoundsDocument258 pagesBreath SoundsJose Dangali AlinaoNo ratings yet
- Suctioning By:: Saja A Al-MarshadDocument25 pagesSuctioning By:: Saja A Al-MarshadsajaNo ratings yet
- General Biology 2 Las Quarter 4 1Document66 pagesGeneral Biology 2 Las Quarter 4 1Raine EscalicasNo ratings yet
- Fetal Pig Dissection Lab: Project WeblinkDocument6 pagesFetal Pig Dissection Lab: Project WeblinkJill KoehlerNo ratings yet
- Anatomy OSPEDocument61 pagesAnatomy OSPEMusfiqur RahmanNo ratings yet
- Respiratory SystemDocument5 pagesRespiratory SystemPreeti ChouhanNo ratings yet
- Evaluation of Two Methods of Endotracheal Tube Selection in DogsDocument7 pagesEvaluation of Two Methods of Endotracheal Tube Selection in DogsFelipe Guajardo HeitzerNo ratings yet
- Student-Nurses' Learning Module In: Prepared By: Instructor Saint Tonis College, Inc. College of NursingDocument8 pagesStudent-Nurses' Learning Module In: Prepared By: Instructor Saint Tonis College, Inc. College of Nursing阿善蒂No ratings yet
- Eals ReviewerDocument12 pagesEals ReviewerEms TeopeNo ratings yet