Professional Documents
Culture Documents
Postherpetic Neuralgia
Uploaded by
Titik Tusi MOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Postherpetic Neuralgia
Uploaded by
Titik Tusi MCopyright:
Available Formats
See
discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/289573558
Postherpetic neuralgia
Article · September 2007
CITATIONS READS
3 10
2 authors, including:
Vida Demarin
International Institute for Brain Health, Zagreb, Croatia
552 PUBLICATIONS 3,088 CITATIONS
SEE PROFILE
All content following this page was uploaded by Vida Demarin on 11 February 2016.
The user has requested enhancement of the downloaded file.
Acta Clin Croat
V. Baiæ-Kes and V.2007; 46:279-282
Demarin Review
Postherpetic neuralgia
POSTHERPETIC NEURALGIA
Vanja Baiæ-Kes and Vida Demarin
University Department of Neurology, Sestre milosrdnice University Hospital, Zagreb, Croatia
SUMMARY Postherpetic neuralgia is a chronic neuropathic pain syndrome that may complicate recovery
from an acute attack of herpes zoster. About 20% of patients with herpes zoster develop persistent
neuropathic pain. Evidence based medicine supports the use of tricyclic antidepressants, opioids and
anticonvulsants in the management of postherpetic neuralgia. Other methods are topical therapy with
lidocaine and capsaicin as well as intrathecal administration of methylprednisolone in some refractory
cases of postherpetic neuralgia.
Key words: Herpes zoster drug therapy; Herpes zoster physiopathology; Neuralgia drug therapy; Neuralgia
etiology; Neuralgia physiopathology; Pain etiology
Introduction Herpes zoster is a sporadic disease with an estimat-
ed lifetime incidence of 10 to 20 percent. The incidence
Herpes zoster and postherpetic neuralgia (PHN) of herpes zoster increases sharply with advancing age,
result from reactivation of the varicella-zoster virus ac- roughly doubling in each decade past the age of 50 years.
quired during the primary varicella infection, or chick- Herpes zoster is uncommon in persons less than 15 years
enpox. Whereas varicella is generally a disease of child- of age. In HIV-infected patients, the incidence of her-
hood, herpes zoster and PHN become more common pes zoster is up to 15-fold that in uninfected persons,
with increasing age1. Many conditions that decrease and as many as 25 percent of patients with Hodgkins
immune function, such as human immunodeficiency lymphoma develop herpes zoster5.
virus (HIV) infection, chemotherapy, malignancies and About 20 percent of patients with herpes zoster de-
chronic corticosteroid use, may also increase the risk of velop PHN. The best established risk factor is age. Oth-
developing herpes zoster. Reactivation of latent varicel- er possible risk factors for the development of PHN are
la-zoster virus from dorsal root ganglia is responsible for ophthalmic zoster, a history of prodromal pain before the
the classic dermatomal rash and pain that occur with appearance of skin lesions, and an immunocompromised
herpes zoster. Burning pain typically precedes the rash state6.
by several days and can persist for several months after
the rash has resolved2,3. Pathogenesis
Acute herpetic neuralgia refers to pain preceding or
accompanying the eruption of rash that persists for up The infection with acute herpes zoster is caused by
to 30 days from its onset. Subacute form refers to pain reactivation of varicella zoster virus. The virus persists
that persists beyond healing of the rash, which resolves for years in the dorsal root ganglia of cranial or spinal
within four months of onset. PHN is defined as pain nerves after resolution of the original infection. In cases
persisting beyond four months from the onset of rash4. with decreased immunity the virus travels down the
sensory nerve and is the cause of dermatomal distribu-
tion of pain and skin lesions.
Correspondence to: Vanja Baiæ-Kes, MD, University Department of
The pathophysiology of PHN remains unclear. How-
Neurology, Sestre milosrdnice University Hospital, Vinogradska c. 29,
HR-10000 Zagreb, Croatia ever, pathologic studies have demonstrated damage to the
E-mail: vanjakes@net.hr sensory nerves, sensory dorsal root ganglia and dorsal horns
Received July 25, 2007, accepted September 17, 2007 of the spinal cord in patients with this condition.
Acta Clin Croat, Vol. 46, No. 3, 2007 279
10 Basic-Kes.p65 279 25. 11. 07, 22:41
V. Baiæ-Kes and V. Demarin Postherpetic neuralgia
The pain in acute phase probably is produced by the of the addictive properties of narcotics, their chronic use
inflammation and movement of viral particles from sen- is discouraged except for rare patients that do not ade-
sory nerves to the skin and subcutaneous tissues as well quately respond to other modalities.
as by damage to nerve structures. The activity of prima-
ry afferent neurons that respond to tissue damage caus- Capsaicin
es changes in dorsal horn neurons, sensitizing them to
further input and resulting in spontaneous activity ca- Capsaicin, an extract from hot chili peppers, is cur-
pable of maintaining pain in the absence of ongoing tis- rently the only drug labeled by the U.S. Food and Drug
sue damage. In cases of persistence of this response, Administration for the treatment of PHN11. Trials have
the pain becomes postherpetic8. shown the drug to be more efficacious than placebo but
not necessarily more than other conventional treatments.
It is thought to produce analgesia by enhancing the re-
Clinical Manifestation
lease of the nocigenic peptide substance P from C-fib-
The pain associated with acute zoster infection is char- ers and then preventing reaccumulation. Topical appli-
acterized by sharp or stabbing sensation. Affected patients cation causes burning, stinging and erythema11.
usually report constant burning, lancinating pain that may
be radicular in nature. Many patients complain of allody- Local and topical anesthetics
nia, defined as pain evoked by normally non-painful stim-
Patches containing 5% lidocaine have also been used
uli such as light touch. It has been suggested that allody-
to treat PHN. One study found that compared with no
nia is most prominent in the areas of relatively preserved
treatment, lidocaine patches reduced pain intensity, with
sensation, while spontaneous pain is felt predominantly
minimal systemic absorption. Although lidocaine was ef-
within the areas of lost or impaired sensation.
ficacious in relieving pain, the effect was temporary, last-
PHN is characterized by areas of anesthesia as well
ing for only 4-12 hours with each application12. By the
as deficits of thermal, tactile, pinprick and vibration sen-
end of 2007, lidocaine patches will be available in Croatia.
sation within affected dermatomes. Although any ver-
tebral dermatome may be involved, T5 and T6 are most
Tricyclic antidepressants
commonly affected. The most frequently involved cra-
nial nerve dermatome is the ophthalmic division of the Tricyclic antidepresants can be effective adjuncts in
trigeminal nerve. reducing neuropathic pain of PHN. These drugs inhib-
PHN is generally a self-limited disease. Symptoms it the reuptake of serotonin and norepinephrine neuro-
tend to abate over time. Less than one quarter of pa- transmitters. They are thought to increase the inhibi-
tients still experience pain at six months of herpes zoster tion of nociceptive signals from the periphery. Tricyclic
eruption, and fewer than one in 20 has pain at one year9. antidepressants commonly used in the treatment of
PHN include amitriptyline, nortriptyline, imipramine
Treatment of Postherpetic Neuralgia and desipramine. These drugs are best tolerated when
started at a low dosage (10-20 mg) and given at bed-
Although PHN is generally a self-limited condition, time. The dosage is increased every two to four weeks
it can last indefinitely. Treatment is directed at pain to achieve an effective dose (a mean amitriptyline dose
control while waiting for the condition to resolve. Pain of 65 mg).
therapy may include multiple interventions, such as top- The side effects of tricyclic antidepressants are se-
ical medications, over-the-counter analgesics, tricyclic dation, dry mouth, postural hypotension, blurred vision
antidepressants, anticonvulsants, and a number of non- and urinary retention. Nortriptyline and amitriptyline
medical modalities. Occasionally, narcotics may be re- appear to have equal efficacy; however, nortriptyline
quired10. tends to produce fewer anticholinergic effects and is
therefore better tolerated. Treatment with tricyclic anti-
Analgesics
depressants can occasionally lead to cardiac conduction
Mild analgesics such as nonsteroidal anti-inflamma- abnormalities or liver toxicity. The potential for these
tory drugs are of limited value in patients with acute or problems should be considered in elderly patients and
chronic pain. Opioids may be more effective. Because patients with cardiac or liver disease13.
280 Acta Clin Croat, Vol. 46, No. 3, 2007
10 Basic-Kes.p65 280 25. 11. 07, 22:41
V. Baiæ-Kes and V. Demarin Postherpetic neuralgia
Anticonvulsants often used NMDA receptor antagonists are ketamine and
dextromethorphan. Unfortunately, ketamine has many
Anticonvulsant medications are useful in the treat-
side effects when administered parenterally17.
ment of neuropathic pain, especially in reducing the
lancinating component of painful syndromes like
Surgery
trigeminal neuralgia14. Gabapentin and pregabalin are
most often used to control pain. A recent double- Surgical procedures include anterolateral cordotomy,
blind, placebo-controlled study showed gabapentin to electrical stimulation of the thalamus, and electrocoagu-
be effective in treating PHN pain as well as the often lation of the dorsal root. All surgical interventions are con-
associated sleep disturbance15. Pregabalin is similar to nected with the risk of permanent neurologic deficits.
gabapentin. Randomized studies in PHN patients The results of these procedures are not satisfactory.
showed improvement in sleep and decrease in pain at
doses of 150 to 600 mg daily16. Other methods
Anticonvulsants are associated with a variety of side Sympathetic blocks with bupivacaine showed bene-
effects including sedation, memory disturbances, elec- fit for PHN in one study. Intravenous therapy with lido-
trolyte abnormalities, liver toxicity and thrombocytope- caine may provide benefit in patients refractory to oth-
nia. Side effects may be reduced or eliminated by initi- er therapies18. Acupuncture and transcutaneous electri-
ating treatment in a low dosage, which can then be slowly cal nerve stimulation (TENS) are widely used in thera-
titrated upward. There are no specific contraindications py of PHN but the effectiveness has not been proven
to using anticonvulsants in combination with antidepres- in studies. Effective treatment of PHN often requires
sants or analgesics. However, the risk of side effects in- multiple treatment approaches. The American Acade-
creases when multiple medications are used14. my of Neurology recommends tricyclic antidepressants,
gabapentin, pregabalin, strong opioids, and topical lido-
Antagonists of N-methyl-D-aspartate receptor caine patches as first-line therapies13.
Antagonists of N-methyl-D-aspartate (NMDA) recep-
tor relieved neuropathic pain in some studies. The most
Table 1. Medications for postherpetic neuralgia
Medication Dosage
Topical agents
Capsaicin cream (0.075%) Three to five times daily on affected areas.
Lidocaine (Xylocaine) patch (5%) Apply to affected area every 4 to 12 hours as needed.
Tricyclic antidepressants
Amitriptyline 0 to 25 mg orally at bedtime; increase dosage by 25 mg every 2 to 4 weeks
until response is adequate, or to maximum dosage of 150 mg per day.
Nortriptyline 0 to 25 mg orally at bedtime; increase dosage by 25 mg every 2 to 4 weeks
until response is adequate, or to maximum dosage of 125 mg per day.
Imipramine 25 mg orally at bedtime; increase dosage by 25 mg every 2 to 4 weeks
until response is adequate, or to maximum dosage of 150 mg per day.
Anticonvulsant medications
Gabapentin 100 to 300 mg orally at bedtime; increase dosage by 100 to 300 mg every
3 days until dosage is 1800 to 2400 mg three times daily or response is
adequate.
Pregabalin Starting dose is 150 mg, divided into two or three doses daily, and in
creased to total daily dose of 300 mg.
Acta Clin Croat, Vol. 46, No. 3, 2007 281
10 Basic-Kes.p65 281 25. 11. 07, 22:41
V. Baiæ-Kes and V. Demarin Postherpetic neuralgia
References 10. ROWBOTHAM MC, DAVIES PS, VERKEMPINCK C,
GALER BS. Lidocaine patch: double-blind controlled study of
1. GLYNN C, CROCKFORD G, GAVAGHAN D. Epidemiology a new treatment method for post-herpetic neuralgia. Pain
of shingles. J R Soc Med 1990;83:617-9. 1996;65:39-44.
2. JUNG BF, JOHNSON RW, GRIFFIN DR, DWORKIN RH. 11. DUBINSKY RM, KABBANI H, El-CHAMI Z. Practice
Risk factors for postherpetic neuralgia in patients with herpes parameter: treatment of postherpetic neuralgia: an evidence-
zoster. Neurology 2004;62:1545-51. based report of the Quality Standards Subcommittee of the
American Academy of Neurology. Neurology 2004;63:959-65.
3. DWORKIN RH, BOON RJ, GRIFFIN DR, PHUNG D.
Postherpetic neuralgia: impact of famcilclovir, age, rash severity 12. SWERDLOW M. Anticonvulsant drugs and chronic pain. Clin
and acute pain in herpes zoster patients. J Infect Dis 1998; Neuropharmacol 1984;7:51-82.
178:S76-80. 13. EIDE P, JORUM E, STUBHAUG A. Relief of postherpetic
4. DWORKIN RH, PORTENOY RK. Pain and its persistence in neuralgia with NMDA receptor antagonist ketamine: a double-
herpes zoster. Pain 1996;67:241-51. blind, crossover comparison with morphine and placebo. Pain
1994;58:347-54.
5. DONAHUE JG, CHOO PW, MANSON JE, PLATT R. The
incidence of herpes zoster. Arch Intern Med 1995;155:1605-9. 14. RICE AS, MATON S. Gabapentin in postherpetic neuralgia: a
randomized, double blind, placebo controlled study. Pain
6. BARON R, WASNER G. Prevention and treatment of
2001;94:215-24.
postherpetic neuralgia. Lancet 2006;367:186-8.
15. DWORKIN RH, CORBIN AE, YOUNG JP. Pregabalin for the
7. BOWSHER D. Pathophysiology of postherpetic neuralgia: treatment of postherpetic neuralgia: a randomized, placebo
towards a rational treatment. Neurology 1995;45:S56-7. controlled trial. Neurology 2003;60:1274-83.
8. NURMIKKO T. Clinical features and pathophysiologic me- 16. KOTANI N, KUSHIKATA T, HASHIMOTO H. Intrathecal
chanisms of postherpetic neuralgia. Neurology 1995;45(12 methylprednisolone for intractable postherpetic neuralgia. N
Suppl 8):S54-5. Engl J Med 2000;343:1514-9.
9. HEMPENSTALL K, NURMIKKO TJ, JOHNSON RW, 17. ALPER BS, LEWIS PR. Treatment of postherpetic neuralgia: a
AHERN RP, RICE AS. Analgesic therapy in postherpetic systematic review of the literature. J Fam Pract 2002;51:121-8.
neuralgia: a quantitative systematic review. PLos Med 2005;
2(7):e 164.
Saetak
POSTHERPETIÈNA NEURALGIJA
V. Baiæ-Kes i V. Demarin
Postherpetièna neuralgija je kronièni neuropatski bolni sindrom koji nastaje kao posljedica infekcije virusom herpes zostera.
Nakon infekcije herpes virusom oko 20% bolesnika razvije postherpetiènu neuralgiju s trajnom neuropatskom boli. Temeljem
medicine zasnovane na dokazima u terapiji postherpetiène neuralgije rabe se triciklièni antidepresivi, opioidi, antikonvulzivni
lijekovi. Ostale metode ukljuèuju lokalnu primjenu lidokainskih i kapscainskih gelova te intratekalnu primjenu
metilprednizolona u nekim refraktornim sluèajevima postherpetiène neuralgije.
Kljuène rijeèi: Herpes zoster terapija; Herpes zoster patofiziologija; Neuralgija terapija; Neuralgija patofiziologija; Bol etiologija
282 Acta Clin Croat, Vol. 46, No. 3, 2007
10 Basic-Kes.p65 282 25. 11. 07, 22:41
View publication stats
You might also like
- Herpes Simplex Varicella and Zoster: Clinical Manifestations and TreatmentFrom EverandHerpes Simplex Varicella and Zoster: Clinical Manifestations and TreatmentRating: 5 out of 5 stars5/5 (19)
- Pain Syndromes in Neurology: Butterworths International Medical ReviewsFrom EverandPain Syndromes in Neurology: Butterworths International Medical ReviewsHoward L. FieldsRating: 5 out of 5 stars5/5 (1)
- Jurnal (BING)Document18 pagesJurnal (BING)johandri.iramaNo ratings yet
- Treating Herpes Zoster and Postherpetic Neuralgia: An Evidence-Based ApproachDocument7 pagesTreating Herpes Zoster and Postherpetic Neuralgia: An Evidence-Based ApproachAristya EkaputraNo ratings yet
- Treating Postherpetic Neuralgia with UVB RadiationDocument4 pagesTreating Postherpetic Neuralgia with UVB RadiationMuhammad AL Farisi SutrisnoNo ratings yet
- Bab I, Ii, Iii PHNDocument31 pagesBab I, Ii, Iii PHNWulanbumuloNo ratings yet
- Herpes Zoster-Predicting and Minimizing The Impact of Post-Herpetic NeuralgiaDocument8 pagesHerpes Zoster-Predicting and Minimizing The Impact of Post-Herpetic NeuralgiaDevi DamayantiNo ratings yet
- Molecular Pathophysiology of Post-Herpetic Neuralgia ReviewDocument6 pagesMolecular Pathophysiology of Post-Herpetic Neuralgia ReviewQia TafaNo ratings yet
- Postherpetic NeuralgiaDocument20 pagesPostherpetic NeuralgiaDimitra VasileiouNo ratings yet
- Chronic Prurigo of Nodular Type: A ReviewDocument7 pagesChronic Prurigo of Nodular Type: A ReviewBobby S PromondoNo ratings yet
- Postherpetic Neuralgia NerissaDocument18 pagesPostherpetic Neuralgia Nerissanerissa rahadianthiNo ratings yet
- Infectious Neuropathies. 2023Document26 pagesInfectious Neuropathies. 2023Arbey Aponte PuertoNo ratings yet
- Post-Herpetic Neuralgia: A Review: Current Pain and Headache Reports March 2016Document6 pagesPost-Herpetic Neuralgia: A Review: Current Pain and Headache Reports March 2016headseNo ratings yet
- PHN (Dr. Ken) - DikonversiDocument32 pagesPHN (Dr. Ken) - DikonversiwkwkwkhhhhNo ratings yet
- Post Herpetic NeuralgiaDocument44 pagesPost Herpetic NeuralgiaRia Puji PangestutiNo ratings yet
- Post-Herpetic Neuralgia: A Review: Current Pain and Headache Reports March 2016Document6 pagesPost-Herpetic Neuralgia: A Review: Current Pain and Headache Reports March 2016ifaNo ratings yet
- Herpes Zoster Ophthalmicus: Ophthalmic PearlsDocument3 pagesHerpes Zoster Ophthalmicus: Ophthalmic Pearlssiti rumaisaNo ratings yet
- Herpes-Zoster Concept MapDocument5 pagesHerpes-Zoster Concept MapElleNo ratings yet
- Referat Herpes Zoster OphthalmicusDocument19 pagesReferat Herpes Zoster OphthalmicusSoraheat MilkywayNo ratings yet
- Clinical Review - FullDocument5 pagesClinical Review - FullBenvenuto AxelNo ratings yet
- Herpes Zoster Infection PDFDocument4 pagesHerpes Zoster Infection PDFHannaTashiaClaudiaNo ratings yet
- Herpes Zoster Pathogenesis and Cell-Mediated Immunity and ImmunosenescenceDocument5 pagesHerpes Zoster Pathogenesis and Cell-Mediated Immunity and Immunosenescencekelompok j27No ratings yet
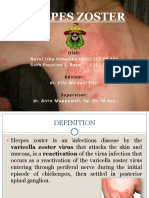
- Herpes Zoster: Nurul Iska Ulmarika Idrisc111 10 831 Ruth Faustine J. Rayo C 1 1 1 1 0 1 8 0Document26 pagesHerpes Zoster: Nurul Iska Ulmarika Idrisc111 10 831 Ruth Faustine J. Rayo C 1 1 1 1 0 1 8 0fatqur280% (1)
- MEDICAL G1B - Racheal YawsonDocument23 pagesMEDICAL G1B - Racheal YawsonkwameasileviNo ratings yet
- Neuropathic Pain of Postherpetic Neuralgia: All Rights R Eserved. ReprDocument0 pagesNeuropathic Pain of Postherpetic Neuralgia: All Rights R Eserved. ReprMarliani AfriastutiNo ratings yet
- Herpes Zoster Infection: Report of A Treated CaseDocument3 pagesHerpes Zoster Infection: Report of A Treated CasemetabolismeproteinNo ratings yet
- Post Herpetic Neuralgia: Herpes Zoster Varicella Zoster VirusDocument9 pagesPost Herpetic Neuralgia: Herpes Zoster Varicella Zoster VirusRS AKADEMIS JAURY JUSUF PUTERANo ratings yet
- Postherpetic Neuralgia in The Elderly: ReviewarticleDocument6 pagesPostherpetic Neuralgia in The Elderly: ReviewarticleSuryo BasofiNo ratings yet
- Pathophysiology of Pain: A Practical PrimerDocument7 pagesPathophysiology of Pain: A Practical PrimerAngelina FebrianNo ratings yet
- Necrotizing FasciitisDocument7 pagesNecrotizing FasciitisjoycefrancielleNo ratings yet
- HHV3 Infections: Chickenpox and ShinglesDocument6 pagesHHV3 Infections: Chickenpox and ShinglesShuvashishSunuwarNo ratings yet
- Neurologic InfectionsDocument6 pagesNeurologic InfectionsHazel ZullaNo ratings yet
- Power Point Harpes ZosterDocument48 pagesPower Point Harpes ZosterOkta SulistiaNo ratings yet
- Assessment of Neuropathic Pain in Primary Care: Supplement IssueDocument9 pagesAssessment of Neuropathic Pain in Primary Care: Supplement IssueRodrigo JimenezNo ratings yet
- La Neuralgia Postherpética. ¿Un Problema Sin Resolver?: RevisiónDocument16 pagesLa Neuralgia Postherpética. ¿Un Problema Sin Resolver?: RevisiónpiramideNo ratings yet
- QPostHerpeticNeauralgia NSingh PDFDocument3 pagesQPostHerpeticNeauralgia NSingh PDFRincy RincyNo ratings yet
- Guide Clinical PDFDocument19 pagesGuide Clinical PDFAbd Halim Gazali HNo ratings yet
- AkhdakaaaaaknuqmakaakddaDocument12 pagesAkhdakaaaaaknuqmakaakddaVICKI ANDREANNo ratings yet
- Anesthesiology 250 Learning ModulesDocument32 pagesAnesthesiology 250 Learning ModulesNiña AvilaNo ratings yet
- Prevention of Post-Herpetic Neuralgia From Dream To Reality: A Ten-Step ModelDocument33 pagesPrevention of Post-Herpetic Neuralgia From Dream To Reality: A Ten-Step ModelYogaZunandyNo ratings yet
- Neuropathic PainDocument13 pagesNeuropathic Paintita_leo2No ratings yet
- Palmitoylethanolamide (PEA)Document4 pagesPalmitoylethanolamide (PEA)Qwerty QwertyNo ratings yet
- Efficacy of Intermittent Epidural Dexamethasone Bolus For Zoster-Associated Pain Beyond The Acute PhaseDocument8 pagesEfficacy of Intermittent Epidural Dexamethasone Bolus For Zoster-Associated Pain Beyond The Acute PhaseRoyNo ratings yet
- ScienceDocument9 pagesScienceChe CastroNo ratings yet
- Diagnosis and Management of Neuropathic ItchDocument12 pagesDiagnosis and Management of Neuropathic ItchTony Miguel Saba SabaNo ratings yet
- Jurnal PendukungDocument9 pagesJurnal PendukungBrillyant S RaintamaNo ratings yet
- Advances in Neuropathic Pain: Diagnosis, Mechanisms, and Treatment RecommendationsDocument11 pagesAdvances in Neuropathic Pain: Diagnosis, Mechanisms, and Treatment Recommendationsgamesh waran gantaNo ratings yet
- Treatment of Postherpetic Neuralgia With Low Level Laser TherapyDocument7 pagesTreatment of Postherpetic Neuralgia With Low Level Laser TherapyJason GossNo ratings yet
- The - IASP - Classification - of - Chronic - Pain - For.7 - 0005Document1 pageThe - IASP - Classification - of - Chronic - Pain - For.7 - 0005ro1977No ratings yet
- ENDOMETRIOSE X FISIOTERAPIA PDFDocument19 pagesENDOMETRIOSE X FISIOTERAPIA PDFLuiza GusmãoNo ratings yet
- Invasive Cryptococcal Meningitis Presenting As A Skull Base Mass in An Immunocompetent Host: A Case ReportDocument5 pagesInvasive Cryptococcal Meningitis Presenting As A Skull Base Mass in An Immunocompetent Host: A Case ReportAsep RiswandiNo ratings yet
- Transition from acute to chronic pain: understanding the physiologyDocument5 pagesTransition from acute to chronic pain: understanding the physiologyFarzana AfrinNo ratings yet
- UC Irvine: Clinical Practice and Cases in Emergency MedicineDocument4 pagesUC Irvine: Clinical Practice and Cases in Emergency MedicineEga AihenaNo ratings yet
- Dermatological Infection Management UpdateDocument29 pagesDermatological Infection Management UpdateyheyenNo ratings yet
- Cidp ParaneoDocument8 pagesCidp ParaneoPablo MarinNo ratings yet
- tuberculomaDocument4 pagestuberculomalittlecandiesNo ratings yet
- Gg. Sistem IntegumenDocument5 pagesGg. Sistem IntegumenSuci Denita SariNo ratings yet
- Small Fiber Neuropathy and Related Syndromes: Pain and NeurodegenerationFrom EverandSmall Fiber Neuropathy and Related Syndromes: Pain and NeurodegenerationSung-Tsang HsiehNo ratings yet
- Fast Facts: Perioperative Pain: Effective management has numerous benefitsFrom EverandFast Facts: Perioperative Pain: Effective management has numerous benefitsNo ratings yet
- Neurofibromatosis 1, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandNeurofibromatosis 1, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Clinical Pathway Obs Febris 7 14 HariaaaaDocument1 pageClinical Pathway Obs Febris 7 14 HariaaaaTitik Tusi MNo ratings yet
- Global Atlas of Asthma PDFDocument196 pagesGlobal Atlas of Asthma PDFilham raymana100% (1)
- CP Clinical Pathway TB ParuDocument1 pageCP Clinical Pathway TB ParuTitik Tusi MNo ratings yet
- TB-PARU-RUMAH-SAKIT-CILANDAKDocument1 pageTB-PARU-RUMAH-SAKIT-CILANDAKarie_susantoNo ratings yet
- Asthma in PregnancyDocument40 pagesAsthma in PregnancyKabo75% (4)
- American Society of Hematology 2020 Guidelines For Sickle Cell Disease - Management of Acute and Chronic PainDocument46 pagesAmerican Society of Hematology 2020 Guidelines For Sickle Cell Disease - Management of Acute and Chronic PainFrancisco Torres VillagránNo ratings yet
- AutocoidsDocument26 pagesAutocoidsA.R. ChowdhuryNo ratings yet
- Euro J of Neurology - 2021 - Van Den Bergh - European Academy of Neurology Peripheral Nerve Society Guideline On DiagnosisDocument28 pagesEuro J of Neurology - 2021 - Van Den Bergh - European Academy of Neurology Peripheral Nerve Society Guideline On DiagnosisSusana RocheNo ratings yet
- OLFU Intesive Post Test 50 ItemsDocument5 pagesOLFU Intesive Post Test 50 ItemsmonmonNo ratings yet
- AminoglycosidesDocument6 pagesAminoglycosidesLlosa JuneNo ratings yet
- Jurnal GGDocument11 pagesJurnal GGKanesti KamajayaNo ratings yet
- All Costs, No Benefits: How TRIPS Plus Intellectual Property Rules in The US-Jordan FTA Affect Access To MedicinesDocument37 pagesAll Costs, No Benefits: How TRIPS Plus Intellectual Property Rules in The US-Jordan FTA Affect Access To MedicinesOxfamNo ratings yet
- Schedule FinalDocument2 pagesSchedule Finalapi-360816970No ratings yet
- Konversi Kode Prosedure INACBGs Ke Kode ICD 9-CMDocument349 pagesKonversi Kode Prosedure INACBGs Ke Kode ICD 9-CMTri Muhammad HaniNo ratings yet
- Renal Disease Dental ManagmentDocument25 pagesRenal Disease Dental ManagmentPratyusha VallamNo ratings yet
- Aromatherapy PRDocument1 pageAromatherapy PRNilamdeen Mohamed ZamilNo ratings yet
- Hemoroid Interna Grade IV: By: Khairunnis A G1A21801 1Document34 pagesHemoroid Interna Grade IV: By: Khairunnis A G1A21801 1Bella ReynaldiNo ratings yet
- Ball Ex Chart 2014aDocument2 pagesBall Ex Chart 2014aJoao CarlosNo ratings yet
- Mexico Nom 073 Ssa1 2005 English CorrDocument19 pagesMexico Nom 073 Ssa1 2005 English CorrStreetRockFighterNo ratings yet
- Nurs 205 Concept MapDocument1 pageNurs 205 Concept MapJami SpearsNo ratings yet
- Psychology of Al-GhazaliDocument48 pagesPsychology of Al-GhazaliZainudin IsmailNo ratings yet
- Practicing The A, B, C'S: Albert Ellis and REBTDocument24 pagesPracticing The A, B, C'S: Albert Ellis and REBTShareenjitKaurNo ratings yet
- On The Medicinal Chemistry of Gold Complexes As Anticancer DrugsDocument12 pagesOn The Medicinal Chemistry of Gold Complexes As Anticancer DrugsJeffersonNo ratings yet
- Data Dictionary: NO Label Operational Scale of Measurem ENT 1Document6 pagesData Dictionary: NO Label Operational Scale of Measurem ENT 1nik nur nisa azlinNo ratings yet
- HypertensionDocument39 pagesHypertensiontianallyNo ratings yet
- Registered Dietitians in Primary CareDocument36 pagesRegistered Dietitians in Primary CareAlegria03No ratings yet
- Applications of Humic and Fulvic Acids in AquacultureDocument2 pagesApplications of Humic and Fulvic Acids in AquacultureAlexandra Nathaly Beltran Contreras100% (1)
- An Organization Study OnDocument39 pagesAn Organization Study Onvelmuthusamy100% (2)
- Medicinal Chemistry: Chapter 1 IntroductionDocument31 pagesMedicinal Chemistry: Chapter 1 Introductionderghal67% (3)
- Biosimilar Insulin GlargineDocument59 pagesBiosimilar Insulin GlarginenellizulfiaNo ratings yet
- Ocluzia Dentara Ionita PetreDocument546 pagesOcluzia Dentara Ionita PetreTeodorPolitanschi100% (1)
- E Stim PDFDocument6 pagesE Stim PDFAlvaro Toledo100% (1)
- Mental Health Act 1987Document35 pagesMental Health Act 1987P Vinod Kumar100% (1)
- Concept Map MarwahDocument5 pagesConcept Map MarwahAsniah Hadjiadatu AbdullahNo ratings yet