Professional Documents
Culture Documents
Rheeumatology
Uploaded by
Amer Wasim0 ratings0% found this document useful (0 votes)
19 views3 pagesComplex
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentComplex
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
19 views3 pagesRheeumatology
Uploaded by
Amer WasimComplex
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 3
1357
CLINICAL NOTE
Acute Bacterial Sacroiliitis in an Adult: A Case Report and
Review of the Literature
Meenakshi Bindal, MD, Brian Krabak, MD, MBA
ABSTRACT. Bindal M, Krabak B. Acute bacterial sacroi- often leads to an initial misdiagnosis that ultimately delays
liitis in an adult: a case report and review of the literature. Arch effective treatment. We report the case of a middle-aged patient
Phys Med Rehabil 2007;88:1357-9. who presented with signs, symptoms, and radiologic evidence
of unilateral bacterial sacroiliitis that resolved with antibiotic
Bacterial septic sacroiliitis is an uncommon diagnosis that treatment.
occurs most frequently in children and young adults. Nonspe-
cific physical examination findings often make it difficult to CASE DESCRIPTION
diagnose the condition, thus delaying appropriate treatment. A 40-year-old woman without significant medical history
We review the case of middle-aged woman with sacroiliac joint presented to our clinic with a 2-week history of pain in the left
(SIJ) pain after a torsional injury. Radiographic films showed gluteal region. She said her pain began after she lurched
the pelvis and left lower extremity to be normal. Despite forward while carrying her luggage at the airport. The pain was
anti-inflammatory medications, analgesics, a corticosteroid in- sharp and progressed over the next several hours while she was
jection, and physical therapy, her pain persisted. Laboratory on the aircraft, prompting her to seek an evaluation in the
data showed an elevated erythrocyte sedimentation rate and emergency department. Radiographs showed no abnormalities
C-reactive protein; otherwise, tests were normal, including in the pelvis and hip. The patient was treated for a muscle strain
negative blood cultures. Magnetic resonance imaging (MRI) and was given narcotic and anti-inflammatory medications on
revealed a left posteroinferior SIJ effusion and computed to- her discharge from the emergency department. Several days
mography (CT) showed an effusion and irregularity in the left later she visited a local physician because of worsening gluteal
SIJ. An SIJ biopsy revealed inflammation suggestive of osteo- pain and associated lower back pain. Subsequent magnetic
myelitis. After a course of intravenous antibiotics, the symp- resonance imaging (MRI) of the lumbar spine revealed a right-
toms completely resolved, thus supporting our diagnosis of sided disk protrusion at L2-3, a mild annular disk bulge at both
bacterial sacroiliitis. Repeat MRI and CT confirmed the com- L4-5, and a posterior annular disk tear at L5-S1. She was
plete resolution of the sacroiliitis. diagnosed with a piriformis muscle strain and treated with a
Key Words: Case report; Rehabilitation; Sacroiliac joint. cortisone injection into the left gluteal region near the SIJ. In
© 2007 by the American Congress of Rehabilitation Medi- addition, she was prescribed an oral steroid, a cyclo-oxygen-
cine and the American Academy of Physical Medicine and ase-2 inhibitor, and physical therapy.
Rehabilitation Two weeks later, she presented to our clinic with continued
sharp left gluteal pain that was extremely painful when she
YPICALLY, SACROILIAC joint (SIJ) pain is caused by engaged in any weight-bearing activity. The pain was aggra-
T trauma resulting from such activities as heavy lifting or
prolonged bending and lifting, or as the result of a rear– end
vated with sitting, standing, and lying down for prolonged
periods of time. She noted no exacerbation with coughing or
motor vehicle collision.1 Fortunately, most symptoms will re- sneezing, or radiation of the pain down the leg, or paresthesias
solve with appropriate treatment that includes activity modifi- in the leg, or back pain, bowel, and bladder changes. She
cation, medication, physical therapy, and/or injections. Pro- reported a mild low-grade fever, chills, and fatigue.
longed SIJ pain, however, should prompt a physician to look On physical examination, she was alert and oriented, with a
for other potential etiologies. temperature of 37.9°C (100.1°F). There were no obvious rashes
Although it represents less than 2% of all nontuberculous of the skin or atrophy of muscles in the lower extremity. She
septic arthritides,2-4 bacterial septic sacroiliitis is typically seen ambulated with an antalgic gait and was unable to place her full
in children and young adults. It is less common in middle-aged weight on the left leg. Range of motion of the hip and spine
and elderly people,5 unless there is a history of intravenous were limited because of the pain associated with movement of
drug use, skin and respiratory infections, or genitourinary tract the leg. She was tender to palpation at the left SIJ and gluteal
infections.5 Unfortunately, septic sacroiliitis has been difficult area. Strength testing was limited by pain, but was normal
to diagnose secondary to nonspecific physical examination distally in the left lower extremity. Sensation and reflexes were
findings and poorly localized presenting symptoms.6,7 This within normative limits. The Patrick and Stinchfield tests were
both positive for pain in the SIJ and gluteal areas on the left
side. Radiographs of the left hip and pelvis did not reveal any
bony abnormalities.
We did a further diagnostic work-up because of the patient’s
From the Department of Anesthesiology, University of Virginia, Charlottesville, continued extreme pain in the left gluteal region and new
VA (Bindal); and Rehabilitation, Orthopaedics and Sports Medicine, University of
Washington, Seattle, WA (Krabak). constitutional symptoms (low-grade fever, chills, and fatigue).
No commercial party having a direct financial interest in the results of the research Laboratory serologies revealed an elevated erythrocyte sedi-
supporting this article has or will confer a benefit upon the author(s) or upon any mentation rate (ESR) of 69mm/h, an elevated C-reactive pro-
organization with which the author(s) is/are associated. tein (CRP) of 7.5mg/dL, negative Lyme immunoglobulin G
Reprint requests to Brian J. Krabak MD, MBA, Rehabilitation Medicine, Univer-
sity of Washington, Box 356490, Seattle, WA 98195, e-mail: bkrabak@ and M antibodies, negative antinuclear antibody screen, and
u.washington.edu. negative human leukocyte antibody B-27. She had a normal
0003-9993/07/8810-11510$32.00/0 white blood cell count of 5730/mm3. Blood cultures were also
doi:10.1016/j.apmr.2007.07.004 negative. MRI of the pelvis suggested a sacroiliitis rather than
Arch Phys Med Rehabil Vol 88, October 2007
1358 ACUTE BACTERIAL SACROILIITIS, Bindal
its onset.2 Almost 75% of cases present with an acute onset of
fever and severe low back pain that is exacerbated by motion
or weight bearing. The remaining 25% have symptoms that
emerge gradually with less pain and low-grade or absent fever.5
Unfortunately, the physical examination is often unreliable in
reaching a diagnosis. Such tests as Gaenslen and FABERE
(flexion, abduction, external rotation, and extension) may lo-
calize the pain to the SIJ, but they are inadequate for differen-
tiating pyogenic sacroiliitis from muscular pain, pelvic frac-
ture, disk disease, or an intra-abdominal process.3-6 Other
studies6-9 show a poor interrater reliability in identifying pos-
itive findings on some of the tests used to localize pain to the
SIJ. Overall, such maneuvers suggest only that such examina-
tion techniques can simply enter SIJ pain into the differential
diagnosis.7
Several tests may be used to diagnose sacroiliitis. Al-
though abnormalities may not be seen for several weeks
after the onset of infection, plain radiographs may show
widening of the joint space and blurring of the subchondral
plate. Ultrasound has not been helpful except to exclude
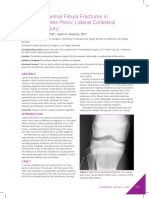
Fig 1. CT of the pelvis illustrating widening of the left SIJ with hip-joint effusions.10 Bone scans can be positive as early as
noted effusion and irregularity of the left SIJ, with a loss of cortex 3 days after onset of symptoms, but are not specific for
on the ilial surface of the joint.
bacterial septic sacroiliitis.1,11,12
MRI and CT appear to be the most useful in evaluating for
SIJ pathology. CT is useful in identifying bony pathology and
a stress reaction injury as a result of left posteroinferior SIJ guiding aspiration or biopsy. MRI can delineate fluid in the
effusion with bone marrow edema and a strain of the left sacroiliac joint, bone marrow edema, and soft tissue abscesses
piriformis, gluteus medius, and paraspinal muscles. Computed that may extend into the pelvic cavity,13 although it has been
tomography (CT) of the pelvis (fig 1) revealed widening of the shown to have a diagnostic sensitivity of 54% for sacroiliitis.14
left SIJ with effusion and irregularity, and loss of cortex on the MRI is better than CT for evaluating cartilage integrity and
left ilial surface of the joint. In addition, there was an irregu- detecting osseous erosions in patients with inflammatory and
larity on the sacral side of the joint but no visible abscess. A infectious sacroiliitis.13,15,16 As in our case, unilateral disease
CT-guided biopsy of the SIJ (fig 2) showed inflammation in the and edema in the soft tissue and marrow adjacent to the SIJ
bone, which is most consistent with an osteomyelitis. SIJ fluid helps to distinguish infectious from noninfectious sacroiliitis
aspirate was negative for acid-fast bacilli, bacteria, fungi, and (ie, some seronegative spondyloarthropathies).17
mycobacteria. The patient was treated with surgical débride- Laboratory data may be helpful in diagnosing bacterial sac-
ment of the SIJ. After further discussion regarding the patient’s roiliitis, but they do have their limitations. ESR and CRP may
clinical symptoms, low-grade temperature, and biopsy find- be elevated in the majority of cases, but while they are sensi-
ings, we decided to treat her with a 6-week course of intrave- tive, they may not be specific.3 Cultures of SIJ fluid from either
nous levofloxacin (Levaquin) and clindamycin, plus oral levo- surgical exploration or percutaneous arthrocentesis with CT
floxacin and clindamycin for another 6 weeks for a presumed guidance are only positive in 50% to 88% of cases.2 And
septic sacroiliitis. The patient’s pain symptoms quickly im- positive blood cultures have been reported in 23% to 67% of
proved over the 12-week course of antibiotics, with normal-
ization of her laboratory values. She regained full range of
motion in her left hip joint and repeat MRI and CT showed
complete resolution of the SIJ irregularities. She was able to
return to full normal activity without any subsequent symp-
toms.
DISCUSSION
Bacterial septic sacroiliitis is more typically seen in children
and young adults than in middle-aged or elderly persons.5 In
adults, there is often a history of intravenous drug use, skin and
respiratory infections, or genitourinary tract infections. It is
thought that the majority of septic sacroiliitis cases occur
through hematogenous seeding from a preexisting infection
from a distant site.2,5 Others have suggested it is the result of
local spreading of infection from a spinal or pelvic infection, or
direct implantation during trauma or invasive procedures.2,5 In
our case, the patient’s only trauma was lifting a suitcase and
receiving a corticosteroid injection to the SI region while
placed on oral steroids. Although it is unclear, perhaps these
potential immune-suppressing interventions contributed to her
SIJ infection. Fig 2. Biopsy of the SIJ shows bone and fibrous tissue with in-
Septic sacroiliitis often presents with a triad of fever, an flamed marrow suggestive of osteomyelitis. NOTE. Hematoxylin
antalgic gait, and buttock pain that may be acute or chronic at and eosin stain, original magnification 100 times.
Arch Phys Med Rehabil Vol 88, October 2007
ACUTE BACTERIAL SACROILIITIS, Bindal 1359
cases.2 Despite the best attempts at diagnosis, 40% of reported References
cases have no identified primary source of infection.5 In our 1. Chou LH, Slipman CW, Bhagia SM, et al. Inciting events initiat-
case, the patient had positive ESR and CRP, but negative ing injection-proven sacroiliac joint syndrome. Pain Med 2004;5:
sacroiliac joint fluid and blood cultures. 26-32.
Given the above laboratory limitations, several organisms 2. Abbot AE, Sculco T. Septic Sacroiliitis with hematogenous spread
can be seen in sacroiliitis. Greater than 80% of reported cases to a total knee arthroplasty. J Arthroplasty 2001;16:225-8.
3. Doita M, Yoshiya S, Nabeshima Y, et al. Acute pyogenic sacroi-
are caused by gram-positive bacteria, with Staphylococcus
liitis without predisposing conditions. Spine 2003;28:E384-9.
aureus being the most common.3,4,18 Seventeen percent are
4. Vyskocil JJ, McIlroy MA, Brennan TA, Wilson FM. Pyogenic
caused by the gram-negative organism Pseudomonas aerungi- infection of the sacroiliac joint: case reports and review of the
nosa, most notably in association with intravenous drug use, literature. Medicine (Baltimore) 1991;70:188-97.
primary or secondary immunodeficiency, underlying chronic 5. Zimmerman B III, Mikolich D, Lally E. Septic sacroiliitis. Semin
diseases, prior prolonged broad spectrum antibiotic use, or in Arthritis Rheum 1996;26:592-604.
people with genitourinary or other invasive procedures.19 Esch- 6. Dreyfuss P. The sacroiliac joint: a review. Int Spinal Injection Soc
erichia coli was cited in 8 cases in 1 study, usually in conjunc- 1994;2:21-58.
tion with urinary tract infections.5 Other strains of Staphylo- 7. Slipman CW, Sterenfeld EB, Chou LH, Herzog R, Vresilovic E.
coccus, Streptococcus salmonella, Klebsiella, Neisseria The predictive value of provocative sacroiliac joint stress maneu-
gonorrhoeae, gram-negative enteric organisms, and anaerobes vers in the diagnosis of sacroiliac joint syndrome. Arch Phys Med
have also been reported in the literature.2,20 Rehabil 1998;79:288-92.
Treatment of septic sacroiliitis includes 4 to 8 weeks of 8. Potter N, Rothstein J. Intertester reliability for selected clinical
parenteral antibiotic therapy, occasionally followed by a course tests of the sacroiliac joint. Phys Ther 1981;11:1671-5.
of oral antibiotics to prevent recurrence. Antibiotics result in 9. Russell A, Maksymowych W, LeClerq S. Clinical examination of
resolution of symptoms in 1 to 2 weeks, with few long-term the sacroiliac joint: a prospective study. Arthritis Rheum 1981;
sequelae. Delayed diagnosis and treatment of septic sacroiliitis 12:1575-7.
increases the risk of the formation of abscesses, septicemia, and 10. Ford LS, Ellis AM, Allen HW, Campbell DE. Osteomyelitis and
hematogenous or seeding of infection to distant sites, espe- pyogenic sacroiliitis: a difficult diagnosis. J Paediatr Child Health
cially in patients with total arthoplasties.2,5 Fortunately, distant 2004;40:317-9.
11. Ramlakan RJ, Govender S. Sacroiliac joint tuberculosis. Int Or-
metastasis via hematogenous spread is rare, with 2 reported
thop 2007;31:121-4
cases of septic spread to the glenohumeral joint and 1 case of
12. Trauner DA, Connor JD. Radioactive scanning in diagnosis of
meningitis.20 Surgical intervention is warranted, especially in
acute sacroiliac osteomyelitis. J Pediatr 1975;87:751-3.
those patients with abscess formation, evidence of contiguous
13. Klein MA, Winalski CS, Wax MR, Piwnica-Worms DR. MR
osteomyelitis, sequestrum of necrotic bone, and failure to re-
imaging of septic sacroiliitis. J Comput Assist Tomogr 1991;15:
spond to antibiotic therapy.5 In our case, given the patient’s
126-32.
clinical symptoms, low-grade fever, and imaging findings, we
14. Hanly JG, Mitchell MJ, Barnes DC, MacMillan L. Early recog-
elected to proceed with antibiotic treatment and surgery. Too
nition of sacroiliitis by magnetic resonance imaging and single
often, these findings are ignored and the pain is treated with
photon emission computed tomography [published erratum in:
nonsteroidal anti-inflammatory drugs, therapy, or an injection.
J Rheumatol 1997;24:411-2]. J Rheumatol 1994;21:2088-95.
We believe the dramatic and rapid improvement of our pa-
15. Haliloglu M, Kleiman MB, Siddiqui AR, Cohen MD. Osteomy-
tient’s symptoms after antibiotic therapy was initiated strongly
elitis and pyogenic infection of the sacroiliac joint. MRI findings
supports the diagnosis of bacterial septic sacroiliitis. Physicians
and review. Pediatr Radiol 1994;24:333-5.
must be aware of the possibility of an SIJ infection early on and
16. Espeland A, Korsbrekke K, Albrektsen G, Larsen JL. Observer
proceed with the appropriate laboratory and imaging studies
variation in plain radiography of the lumbosacral spine. Br J
before initiating treatment.
Radiol 1998;71:366-75.
17. Murphey MD, Wetzel LH, Bramble JM, Levine E, Simpson KM,
CONCLUSIONS Lindsley HB. Sacroiliitis: MR imaging findings. Radiology 1991;
Infectious SIJ disease can be difficult to diagnose, given the 180:239-44.
nonspecific symptoms and physical examination findings. Cli- 18. Shanahan MD, Ackroyd CE. Pyogenic infection of the sacroiliac
nicians should be aware of the diagnosis, however, even in the joint. A report of 11 cases. J Bone Joint Surg Br 1985;67:605-8.
acute setting or in unilateral cases. With appropriate laboratory 19. Calza L, Manfredi R, Marinacci G, Fortunato L, Chiodo F. Com-
and imaging workup, the appropriate treatment can be initiated munity-acquired Pseudomonas aeruginosa sacroiliitis in a previ-
without delay and without any long-term complications. As ous healthy patient. J Med Microbiol 2002;51:620-2.
was true for our patient, the proper identification of bacterial 20. Osman AA, Govender S. Septic sacroiliitis. Clin Orthop Relat Res
septic sacroiliitis frequently leads to a positive outcome. 1995;Apr(313):214-9.
Arch Phys Med Rehabil Vol 88, October 2007
You might also like
- Osteophyte at The Sacroiliac JointDocument4 pagesOsteophyte at The Sacroiliac JointHayyu F RachmadhanNo ratings yet
- Revoke SuretyDocument3 pagesRevoke Suretysonya.rylee99No ratings yet
- The Challenge of Diagnosing Psoas Abscess: Case ReportDocument4 pagesThe Challenge of Diagnosing Psoas Abscess: Case ReportNataliaMaedyNo ratings yet
- 3 s2.0 B9780443067167000074 MainDocument3 pages3 s2.0 B9780443067167000074 MainKarthik BhashyamNo ratings yet
- Sciatica and The Sacroiliac JointDocument4 pagesSciatica and The Sacroiliac JointfilipecorsairNo ratings yet
- FP 36 08 370Document6 pagesFP 36 08 370uzmaNo ratings yet
- Situs Inversus Totalis in A 72-Year-Old Man WestAfrJRadiolDocument4 pagesSitus Inversus Totalis in A 72-Year-Old Man WestAfrJRadiolAnonymous 9QxPDpNo ratings yet
- Osteomyelitis of The Left Humerus With Secondary Septic Arthritis of TheShoulder Joint in Neonate A Case ReportDocument3 pagesOsteomyelitis of The Left Humerus With Secondary Septic Arthritis of TheShoulder Joint in Neonate A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Acu BacteremiaDocument3 pagesAcu Bacteremiarswongym449No ratings yet
- Roturas Aisladas SubescapularDocument5 pagesRoturas Aisladas SubescapularKarim SabaNo ratings yet
- Case of Celiac's Disease Mimicking ALSDocument4 pagesCase of Celiac's Disease Mimicking ALSfakbikNo ratings yet
- Giant Cell Tumor of The Thoracic Spine in A 30 Year Old Woman 2019Document3 pagesGiant Cell Tumor of The Thoracic Spine in A 30 Year Old Woman 2019Ignatius Rheza SetiawanNo ratings yet
- Syringomyelia in Neuromyelitis Optica Seropositive For Aquaporin-4 Antibody: A Case ReportDocument4 pagesSyringomyelia in Neuromyelitis Optica Seropositive For Aquaporin-4 Antibody: A Case ReportIJAR JOURNALNo ratings yet
- Clinical Decision Making To Determine Need For Medical ReferralDocument12 pagesClinical Decision Making To Determine Need For Medical ReferralaroobaNo ratings yet
- Lupus SeverDocument3 pagesLupus SeverdeliaNo ratings yet
- Isolated Proximal Fibula Fractures in Young Athletes Mimic LateraDocument4 pagesIsolated Proximal Fibula Fractures in Young Athletes Mimic LateraRamza Febby As'AryNo ratings yet
- Jurnal 4Document4 pagesJurnal 4Putri Maghfirah BahriNo ratings yet
- Brucellosis and Is A Coomon Ion of Uncommon PathogenDocument7 pagesBrucellosis and Is A Coomon Ion of Uncommon PathogenSohail FazalNo ratings yet
- Assessment and Management of Acute Low Back Pain - American Family PhysicianDocument9 pagesAssessment and Management of Acute Low Back Pain - American Family PhysiciancaralivroNo ratings yet
- Balancing Method MirroringDocument9 pagesBalancing Method MirroringYoshua ViventiusNo ratings yet
- Legg-Calvé-Perthes Disease: Images in Clinical MedicineDocument1 pageLegg-Calvé-Perthes Disease: Images in Clinical MedicineJesus HuaytaNo ratings yet
- Jurnal THTDocument5 pagesJurnal THTTri RominiNo ratings yet
- Kissing Spine SyndromeDocument4 pagesKissing Spine SyndromeMarcel Quario OrinaNo ratings yet
- The Use of Osteopathic Manual Therapy AnDocument13 pagesThe Use of Osteopathic Manual Therapy AnwladjaNo ratings yet
- Septic Arthritis in MalignancyDocument4 pagesSeptic Arthritis in MalignancyEBNY MOBA & PUBG Mobile GamingNo ratings yet
- Protocolo Core ExaminationDocument8 pagesProtocolo Core ExaminationBia DiasNo ratings yet
- ONFHDocument21 pagesONFHPrasanna VernekarNo ratings yet
- Acute OsteomyelitisDocument6 pagesAcute OsteomyelitisImran TaufikNo ratings yet
- Chiropractic & OsteopathyDocument20 pagesChiropractic & OsteopathyPedro FonsecaNo ratings yet
- EpicondilteDocument7 pagesEpicondilteRicardo fariaNo ratings yet
- Nelson EWDocument6 pagesNelson EWDewidewidewi Madridista Part IINo ratings yet
- ASIA Syndrome Following Breast Implant Placement: Case CommunicationsDocument3 pagesASIA Syndrome Following Breast Implant Placement: Case Communicationssilvana31No ratings yet
- Spondilitis TBDocument14 pagesSpondilitis TBaswad 0008No ratings yet
- Rheumatology QuizletDocument14 pagesRheumatology QuizletPaige BarniniNo ratings yet
- Compartment SyndromeDocument2 pagesCompartment SyndromeabNo ratings yet
- Guillain-Barre Syndrome Presenting With Sensory Disturbance Following A Herpes Virus Infection: A Case ReportDocument5 pagesGuillain-Barre Syndrome Presenting With Sensory Disturbance Following A Herpes Virus Infection: A Case ReportAsep MetrikaNo ratings yet
- Villalon GRCaudaEquina2PRDocument12 pagesVillalon GRCaudaEquina2PRpaul villalonNo ratings yet
- Meyer 1995Document7 pagesMeyer 1995Rogério XavierNo ratings yet
- 71a, Woman, Low Back PainDocument4 pages71a, Woman, Low Back PainGabriel MouraNo ratings yet
- Congenital Indifference To Pain: An Illustrated Case Report and Literature ReviewDocument8 pagesCongenital Indifference To Pain: An Illustrated Case Report and Literature ReviewNICOLÁS ANDRÉS AYELEF PARRAGUEZNo ratings yet
- Artigo - JoelhoDocument4 pagesArtigo - JoelhoizabellegoesNo ratings yet
- Whiplash Syndrome and Forensic Approach. A Case ReportDocument4 pagesWhiplash Syndrome and Forensic Approach. A Case ReportAhmad Syah PutraNo ratings yet
- ACR EducationDocument53 pagesACR EducationamereNo ratings yet
- Cauda Equina Syndrome After Spinal Anaesthesia In.10Document3 pagesCauda Equina Syndrome After Spinal Anaesthesia In.10Let BorlagdanNo ratings yet
- PTH 725 - Multiple-Sclerosis-Case StudyDocument19 pagesPTH 725 - Multiple-Sclerosis-Case StudyEnrique Guillen InfanteNo ratings yet
- Case 14-2020: A 37-Year-Old Man With Joint Pain and Eye RednessDocument9 pagesCase 14-2020: A 37-Year-Old Man With Joint Pain and Eye RednessWho's Alewii?No ratings yet
- Cases Patient 1: FIG. 2. The X-Ray Depicting Neck Facet Degenerative Changes of Patient 1Document1 pageCases Patient 1: FIG. 2. The X-Ray Depicting Neck Facet Degenerative Changes of Patient 1dasdsaNo ratings yet
- Spinal Cord Injury Without Radiological AbnormalitDocument3 pagesSpinal Cord Injury Without Radiological Abnormalitcollestein christdianNo ratings yet
- Physiotherapy Management of SciaticaDocument6 pagesPhysiotherapy Management of SciaticaMuly Arafah ZakariaNo ratings yet
- Ankylosing Spondylitis BMJ RevDocument5 pagesAnkylosing Spondylitis BMJ RevsamarqandiNo ratings yet
- bmr/2021/34 1/bmr 34 1 bmr200070/bmr 34 bmr200070Document5 pagesbmr/2021/34 1/bmr 34 1 bmr200070/bmr 34 bmr200070niekoNo ratings yet
- Dolor Sacro IliacoDocument6 pagesDolor Sacro Iliacomaria antonieta0102No ratings yet
- Median and Anterior Interosseous Nerve Entrapment Syndromes Versus Carpal Tunnel Syndrome: A Study of Two CasesDocument10 pagesMedian and Anterior Interosseous Nerve Entrapment Syndromes Versus Carpal Tunnel Syndrome: A Study of Two CasesNazia SalmanNo ratings yet
- Sacroiliac Joint Pain Referral Zones: of ofDocument5 pagesSacroiliac Joint Pain Referral Zones: of ofGabriel Gaspar Bike FitNo ratings yet
- Mialgia e Fraqueza MuscularDocument8 pagesMialgia e Fraqueza MuscularCelia AlcantaraNo ratings yet
- Hypomagnesemia and Prolonged Hospital Stay: A Case Report and Literature ReviewDocument6 pagesHypomagnesemia and Prolonged Hospital Stay: A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- A 24-Year-Old Man With Suspected Sacroiliitis PDFDocument2 pagesA 24-Year-Old Man With Suspected Sacroiliitis PDFnertila dalaniNo ratings yet
- AIMTED 2017 Practice Exam Questions and Answers: © AIMTED 2017. All Rights Reserved. See Website For Disclaimer. 1Document25 pagesAIMTED 2017 Practice Exam Questions and Answers: © AIMTED 2017. All Rights Reserved. See Website For Disclaimer. 1evatangNo ratings yet
- Chronic Diseases - Lymes, Hpv, Hsv Mis-Diagnosis and Mistreatment: A New Approach to the EpidemicFrom EverandChronic Diseases - Lymes, Hpv, Hsv Mis-Diagnosis and Mistreatment: A New Approach to the EpidemicRating: 5 out of 5 stars5/5 (1)
- UEMS Rheumatology Specialist Core Curriculum 2003Document5 pagesUEMS Rheumatology Specialist Core Curriculum 2003Amer WasimNo ratings yet
- Pil 7639Document11 pagesPil 7639Amer WasimNo ratings yet
- Standardized' Coefficients: Handout For 221B. Andrew Noymer, UC, IrvineDocument2 pagesStandardized' Coefficients: Handout For 221B. Andrew Noymer, UC, IrvinerockstarchandreshNo ratings yet
- MCQ EBPRM Examination 2010Document23 pagesMCQ EBPRM Examination 2010Amer WasimNo ratings yet
- Anxiety and Depression in Patients With Rheumatoid ArthritisDocument7 pagesAnxiety and Depression in Patients With Rheumatoid ArthritisAmer WasimNo ratings yet
- Leflunomide-Associated Weight Loss in Rheumatoid Arthritis: Jonathan S. Coblyn, Nancy Shadick, and Simon HelfgottDocument4 pagesLeflunomide-Associated Weight Loss in Rheumatoid Arthritis: Jonathan S. Coblyn, Nancy Shadick, and Simon HelfgottAmer WasimNo ratings yet
- 430 2012 PDFDocument8 pages430 2012 PDFAmer WasimNo ratings yet
- Pain Mechanisms in Rheumatoid Arthritis: D.F. Mcwilliams, D.A. WalshDocument8 pagesPain Mechanisms in Rheumatoid Arthritis: D.F. Mcwilliams, D.A. WalshAmer WasimNo ratings yet
- Harri Es 2014Document2 pagesHarri Es 2014Amer WasimNo ratings yet
- EULAR RecommendationsDocument13 pagesEULAR RecommendationsAmer Wasim100% (1)
- 2019 Update of The EULAR Recommendations For The Management of Systemic Lupus ErythematosusDocument10 pages2019 Update of The EULAR Recommendations For The Management of Systemic Lupus ErythematosusAmer WasimNo ratings yet
- 01 Enoxaparin Pediatric ProtocolDocument2 pages01 Enoxaparin Pediatric ProtocolAmer WasimNo ratings yet
- Global: Prevalence of Rheumatoid Arthritis in Low - and Middle-Income Countries: A Systematic Review and AnalysisDocument10 pagesGlobal: Prevalence of Rheumatoid Arthritis in Low - and Middle-Income Countries: A Systematic Review and AnalysisAmer WasimNo ratings yet
- A Caution Regarding Rules of Thumb For Variance Inflation FactorsDocument18 pagesA Caution Regarding Rules of Thumb For Variance Inflation FactorsParag Jyoti DuttaNo ratings yet
- Pain Threshold Is Reduced in DepressionDocument4 pagesPain Threshold Is Reduced in DepressionAmer WasimNo ratings yet
- Guidelines For Authors: 3. Reporting Documenting Research in Scientific ArticlesDocument7 pagesGuidelines For Authors: 3. Reporting Documenting Research in Scientific ArticlesAmer WasimNo ratings yet
- Mary Bond - The Pelvic LiftDocument4 pagesMary Bond - The Pelvic Liftleo100% (1)
- Bone and Muscle - Structure, Force and MotionDocument269 pagesBone and Muscle - Structure, Force and MotionMarian Minca100% (1)
- Table of Joints in Lower LimbDocument5 pagesTable of Joints in Lower LimbVijay Pradeep100% (3)
- Management of Pelvic Girdle Pain in Pregnancy and Post-PartumDocument27 pagesManagement of Pelvic Girdle Pain in Pregnancy and Post-PartumrahmawatusNo ratings yet
- Assessment For Massage TherapistDocument656 pagesAssessment For Massage Therapistbb_ul100% (7)
- Estudio Sacroiliaca MulliganDocument100 pagesEstudio Sacroiliaca MulliganIsabelGuijarroMartinezNo ratings yet
- Diagnosis, Classification Management of Chronic Low Back PainDocument31 pagesDiagnosis, Classification Management of Chronic Low Back PainVizaNo ratings yet
- WALKER, SIJ A Critical Review. 92Document14 pagesWALKER, SIJ A Critical Review. 92Rikita PatelNo ratings yet
- Biomechanical CanineDocument8 pagesBiomechanical CanineSANTIAGO NICOLAS CUERVO MALDONADONo ratings yet
- Sacral FractureDocument21 pagesSacral Fracturebosnia agusNo ratings yet
- Kiiko Matsumoto - TreatmentsDocument25 pagesKiiko Matsumoto - TreatmentsHaryono zhu86% (7)
- Strain Counter-Strain PDFDocument7 pagesStrain Counter-Strain PDFCarlosCarpinteroRubioNo ratings yet
- Lecture Notes - BIOS 1168 Functional Musculoskeletal Anatomy BDocument103 pagesLecture Notes - BIOS 1168 Functional Musculoskeletal Anatomy BSK AuNo ratings yet
- Upledger's CranioSacral Therapy 10-Step Protocol, Step 2Document3 pagesUpledger's CranioSacral Therapy 10-Step Protocol, Step 2Marisa RL67% (3)
- Most Common CPT CodesDocument5 pagesMost Common CPT CodesKrishna KumarNo ratings yet
- Questions AnatDocument13 pagesQuestions AnatAfaq RazaNo ratings yet
- Combined Approach To The SIJDocument61 pagesCombined Approach To The SIJSara Yasmin TalibNo ratings yet
- anatomy semifinal まとめDocument103 pagesanatomy semifinal まとめfabel192No ratings yet
- 34-Nerves & Vessels of PelvisDocument48 pages34-Nerves & Vessels of Pelvistesfaye mekonnenNo ratings yet
- Master Techniques in Orthopaedic Surgery - Orthopaedic Oncology and Complex Reconstruction (PDFDrive) PDFDocument424 pagesMaster Techniques in Orthopaedic Surgery - Orthopaedic Oncology and Complex Reconstruction (PDFDrive) PDFsandeep nemaNo ratings yet
- Efficacy of Sot in FemalesDocument7 pagesEfficacy of Sot in FemalesDenise MathreNo ratings yet
- Low Back and Pelvis Clinical Applications A L Logan Series in Chiropractic Technique No 3 PDFDocument209 pagesLow Back and Pelvis Clinical Applications A L Logan Series in Chiropractic Technique No 3 PDFmax50% (2)
- Physical Therapy Protocols For Conditions of The Low Back RegionDocument76 pagesPhysical Therapy Protocols For Conditions of The Low Back RegiontinadasilvaNo ratings yet
- Vertebral ColumnDocument84 pagesVertebral ColumnGenesis GeronagaNo ratings yet
- Clinical Examination of The Sacroiliac JointDocument7 pagesClinical Examination of The Sacroiliac Jointthe_walnutNo ratings yet
- History 2021Document3 pagesHistory 2021api-450895824No ratings yet
- Lumbopelvic Monograph: Pathology, Examination, Diagnosis, and ManagementDocument47 pagesLumbopelvic Monograph: Pathology, Examination, Diagnosis, and Managementrapannika100% (2)
- Pathomecanik Sij ProblemDocument10 pagesPathomecanik Sij ProblemDonny HendrawanNo ratings yet
- The Pelvic Lift: Theme and Variations: Mary BondDocument6 pagesThe Pelvic Lift: Theme and Variations: Mary Bondbackch9011No ratings yet
- Rheumatology MCQs - Waleed HafizDocument7 pagesRheumatology MCQs - Waleed Hafizanan100% (1)