Professional Documents
Culture Documents
Jurnal 1 Her
Uploaded by
Befrie Mahaztra SOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Jurnal 1 Her
Uploaded by
Befrie Mahaztra SCopyright:
Available Formats
[Downloaded free from http://www.journalofmas.com on Monday, January 09, 2017, IP: 120.188.82.
99]
Review Article
Anaesthesia for laparoscopic surgery:
General vs regional anaesthesia
Sukhminder Jit Singh Bajwa, Ashish Kulshrestha
Department of Anaesthesiology and Intensive Care, Gian Sagar Medical College and Hospital, Patiala, Punjab, India
Address for Correspondence: Dr. Sukhminder Jit Singh Bajwa, House No - 27-A, Ratan Nagar, Tripuri, Patiala - 147 001, Punjab, India.
E-mail: sukhminder_bajwa2001@yahoo.com
Abstract INTRODUCTION
The use of laparoscopy has revolutionised the surgical The introduction of laparoscopy in the field of surgery in the
field with its advantages of reduced morbidity with early
mid-1950s revolutionised surgical techniques due to reduction
recovery. Laparoscopic procedures have been traditionally
performed under general anaesthesia (GA) due to the in overall medical costs, reduced bleeding, less post-operative
respiratory changes caused by pneumoperitoneum, which surgical and pulmonary complications, and early recovery.
is an integral part of laparoscopy. The precise control of The gradual shift of laparoscopy to include more complicated
ventilation under controlled conditions in GA has proven surgical procedures resulted in modifications of existing
it to be ideal for such procedures. However, recently anaesthetic techniques. The various effects of induction of
the use of regional anaesthesia (RA) has emerged as
pneumoperitoneum, an integral part of laparoscopy, can result
an alternative choice for laparoscopy. Various reports
in the literature suggest the safety of the use of spinal,
in respiratory embarrassment and cardiovascular changes best
epidural and combined spinal-epidural anaesthesia in managed by the use of general anaesthesia (GA).[1] Since the
laparoscopic procedures. The advantages of RA can initiation of the application of laparoscopy in various day-care
include: Prevention of airway manipulation, an awake surgeries, a more favourable anaesthetic technique is required
and spontaneously breathing patient intraoperatively, allowing early recovery and ambulation. The evolution of
minimal nausea and vomiting, effective post-operative anaesthetic medicine on scientifically and clinically relevant
analgesia, and early ambulation and recovery. However,
scales has propelled innovations and initiatives for newer yet
RA may be associated with a few side effects such as
the requirement of a higher sensory level, more severe safer techniques.[2] Advancements in anaesthesiology have
hypotension, shoulder discomfort due to diaphragmatic been made on many fronts besides clinically relevant scales.[3-5]
irritation, and respiratory embarrassment caused by
pneumoperitoneum. Further studies may be required to On the contrary, advancements in anaesthetic techniques
establish the advantage of RA over GA for its eventual and drugs in the modern era have given birth and growth to
global use in different patient populations.
newer controversies in the light of newer scientific evidences.
Traditionally, GA was considered the sole technique, and
Key words: General anaesthesia (GA), laparoscopy,
various myths and facts discouraged the use of regional
pneumoperitoneum, spinal anaesthesia
anaesthesia (RA). Among these, respiratory embarrassment
and cardiovascular changes were the major aspects of concern
which are considered to be best managed by the use of GA.
Moreover, anaesthesiologists are more comfortable with the
Access this article online
administration of GA in laparoscopic surgeries, and there is
Quick Response Code: Website:
a general reluctance to take initiative for advancements in
www.journalofmas.com swapping anaesthetic techniques.
Recently, RA has been documented to be equally favourable
DOI:
10.4103/0972-9941.169952 in laparoscopic surgeries.[6] This review has been done to
compare the merits and demerits of the use of RA vs GA in
laparoscopic surgery.
4 Journal of Minimal Access Surgery | January-March 2016 | Volume 12 | Issue 1
[Downloaded free from http://www.journalofmas.com on Monday, January 09, 2017, IP: 120.188.82.99]
Bajwa and Kulshrestha: GA vs RA for laparoscopic surgery
METHODS OF LITERATURE SEARCH These changes can be detrimental in patients with reduced
intracranial compliance.
A systematic literature search was made using search engines
including PubMed, Google and Google Scholar with the Positioning
use of the following single-text words and combinations: The most common laparoscopic procedures employ the
‘Laparoscopic surgery’, ‘regional anaesthesia’, ‘general Trendelenburg (head-up) or the reverse Trendelenburg
anaesthesia’ and ‘spinal anaesthesia’. The references of (head-down) position, thus further potentiating the adverse
relevant articles were cross-checked, and the articles effects of pneumoperitoneum. The venous return, cardiac
comparing RA with GA for laparoscopic surgery and the output and mean arterial pressure are reduced further in the
articles on the use of RA for laparoscopic surgeries were head-up position, with an increase in peripheral vascular and
included. pulmonary resistance.[11] Respiratory system deterioration
is considered to be maximally affected in the reverse
SYSTEMIC EFFECTS OF PNEUMOPERITONEUM– Trendelenburg position but it also depends on the duration
NECESSARY CLINICAL SCENARIO of pneumoperitoneum.[12]
The creation of pneumoperitoneum is an integral part CHOICE OF ANAESTHETIC TECHNIQUE
of any laparoscopic procedure and is usually done by FOR LAPAROSCOPY– THE BEST ONE
insufflation of carbon dioxide for the proper visualisation
of abdominal viscera and its manipulation. The main With the recent trend towards the use of laparoscopy in day-
effects are due to raised intra-abdominal pressure leading care surgeries, anaesthetic techniques have changed, with
to various respiratory, cardiovascular and neurologic more emphasis on shorter and more favourable techniques.
alterations. The ideal anaesthetic technique for laparoscopic surgery
should maintain stable cardiovascular and respiratory
Cardiovascular functions, provide rapid post-operative recovery, lead to
The cardiovascular effects are mainly dependent on the minimal post-operative nausea and vomiting (PONV) and
intra-abdominal pressure and the absorption of carbon provide good post-operative pain relief for early mobility.
dioxide into systemic circulation. At lower intra-abdominal
pressures of less than 15 mmHg, the venous return is THE TRADITIONAL ANAESTHETIC TECHNIQUE — GA
augmented due to the emptying of splanchnic vessels, and
thus cardiac output and blood pressure are increased. At The use of GA with controlled ventilation has been considered
higher intra-abdominal pressures of more than 15 mmHg, due the most acceptable technique for laparoscopic procedures
to compression of inferior vena cava and other collaterals, owing to the various effects of pneumoperitoneum. The use
the venous return is decreased, thus reducing cardiac output of rapidly-acting and shorter-duration intravenous agents
and blood pressure.[7,8] Various bradyarrythmias leading such as propofol and etomidate as well as inhalational agents
to atrioventricular blocks and cardiac arrest have been such as sevoflurane and desflurane has made GA a favourable
documented due to vagal stimulation on the insertion of a technique for day-care laparoscopic procedures.[13,14] Use of
trocar, peritoneal stretch or carbon dioxide embolization.[9] the ultra-short-acting opioid analgesic remifentanil also
favours GA in fast-track laparoscopic procedures.[15] The
Respiratory use of nitrous oxide in laparoscopic procedures has been
These include reduced lung volumes, basal atelectasis, controversial, but the recent literature does not convey
increased intrapulmonary shunting, raised peak and any clinical advantage of avoiding it against a greater
mean airway pressures, and are attributable to raised risk of intraoperative awareness.[16] The only advantage
intra-abdominal pressures and cephalad migration of the of avoiding nitrous oxide may be a lower incidence of
diaphragm with reduced excursion. There may also be PONV. The use of short-acting, non-depolarizing muscle
chances of endobronchial migration of the endotracheal relaxants has replaced depolarizing muscle relaxants such
tube, resulting in hypercarbia and hypoxia.[10] as succinylcholine from the balanced GA technique for
laparoscopic surgeries, allowing for less post-operative
Neurologic muscle pain. Moreover, the increasing usage of newer drugs
Raised intracranial pressure with consequent reduced like alpha-2 agonists apart from traditionally used opioids
cerebral perfusion pressure may occur due to hypercapnia, is quite effective in the attenuation of stressor response
raised intra-abdominal pressures, and head-down positioning. during intubation.[17,18]
Journal of Minimal Access Surgery | January-March 2016 | Volume 12 | Issue 1 5
[Downloaded free from http://www.journalofmas.com on Monday, January 09, 2017, IP: 120.188.82.99]
Bajwa and Kulshrestha: GA vs RA for laparoscopic surgery
The use of Proseal laryngeal mask airway (LMA) with abdominal procedures.[31-33] The main advantages of spinal
controlled ventilation can avoid endotracheal intubation anaesthesia are: An awake, spontaneously breathing patient;
in selected non-obese patients undergoing laparoscopic prevention of airway manipulation; less incidence of PONV;
procedures, thus reducing the incidence of post-operative and the provision of effective post-operative analgesia with
sore throat, but it should be limited to procedures with the a shorter recovery time.[34]
use of low intra-abdominal pressures and mild tilt.[19,20]
There are a few concerns related to the use of spinal
The safest technique of anaesthesia remains GA with anaesthesia for laparoscopic procedures. The incidence of
endotracheal intubation in those with no contraindications, hypotension has been noted to be up to 20.5% and can be
with maintenance of intra-operative end-tidal carbon augmented by the Trendelenburg position and increased
dioxide (EtCO2) around 35 mmHg with adjustments in tidal intra-abdominal pressures.[35] However, various studies show
volume or respiratory rate.[21] The agents which directly that it can be easily prevented by liberally preloading the
depress the heart should be avoided, with the provision of patient, reducing the head tilt, reducing the intra-abdominal
anticholinergic drugs in case of sudden surge in vagal tone pressure and the liberal use of vasopressors.[36,37]
during laparoscopy.
The incidence of referred shoulder-tip pain varies 25-43%; it may
EMERGENCE OF RA IN LAPAROSCOPIC SURGERY be distressing to the patient in the post-operative period.[38]
The etiology is thought to be subdiaphragmatic irritation of the
The use of RA for laparoscopy had not gained popularity peritoneum by the carbon dioxide pneumoperitoneum. This
until recently due to the risk of aspiration and respiratory can be reduced by lowering of the intra-abdominal pressures
embarrassment caused by pneumoperitoneum, making it less to 8-10 mmHg, the instillation of local anaesthetics into the
favourable for a conscious patient. However, RA does provide peritoneal cavity or the use of parenteral opioids.[39,40]
numerous advantages over GA in terms of quicker recovery,
effective post-operative pain relief, no airway manipulation, T h e c h a n g e s i n re s p i r a t o r y m e c h a n i c s d u e t o
shorter post-operative stay, cost-effectiveness and reduced pneumoperitoneum may cause increase in PaCO 2 due
PONV.[22,23] Most of the uses of RA in the past have been limited to absorption from peritoneum, resulting in ventilatory
to the patient population with significant co-morbidities, changes. However, various reports in the literature support
where it proved to be beneficial.[24,25] There is evidence that non-significant changes in either PaO2 or PaCO2 during
the use of RA in laparoscopy performed on awake patients laparoscopic surgery under spinal anaesthesia.[41]
may produce fewer changes in respiratory mechanics and
arterial blood gases. The various regional techniques that Combined spinal-epidural anaesthesia
can be safely used in laparoscopic procedures are as follows. The use of combined spinal-epidural anaesthesia offers many
advantages over either of the techniques by ensuring rapid
Epidural anaesthesia onset of anaesthesia compared to epidural alone and reduced
It has emerged as a very safe technique for lower abdominal intrathecal doses of local anaesthetics required compared to
surgeries as well as for post-operative analgesia, with only spinal anaesthesia. It also entails the provision of effective
occasional complications reported.[26] It has been used safely post-operative analgesia and early ambulation of patients.
in laparoscopic procedures involving the upper abdomen, and The incidence of side effects is low with slight alterations
has been shown to have no deleterious effects on respiratory in the positioning of the patient and by restriction of intra-
mechanics. The effectiveness of the epidural technique is abdominal pressures.[42]
enhanced and a prolonged post-operative analgesic period is
achieved with the use of adjuvant with local anaesthetics.[27-29] GA VS RA — CURRENT EVIDENCE
Epidural anaesthesia can be used in patients deemed unfit for
GA with the provision of effective post-operative analgesia.[30] Evidence is lacking from developing nations regarding
various advancements, mainly owing to the practice of
Spinal anaesthesia scarce reporting of advancements and innovations. However,
The spinal anaesthesia may be more feasible and can provide recently data reporting has witnessed a slight uptrend in
better laparoscopic surgical conditions due to profound the developing nations imbibing empiricism and scientific
muscle relaxation and shorter recovery. There has been evidence.[43,44] RA provides various advantages over GA,
several reports in the literature for the safe use of spinal such as reduction of surgical stress response, prevention of
anaesthesia for laparoscopic upper abdominal and lower airway instrumentation, provision of effective post-operative
6 Journal of Minimal Access Surgery | January-March 2016 | Volume 12 | Issue 1
[Downloaded free from http://www.journalofmas.com on Monday, January 09, 2017, IP: 120.188.82.99]
Bajwa and Kulshrestha: GA vs RA for laparoscopic surgery
analgesia, and early ambulation with lower incidence of and found significantly lower pain scores with lower analgesic
deep vein thrombosis. There are numerous studies in the consumption in the post-operative period in those with
literature comparing GA and RA for laparoscopic surgery, spinal anaesthesia. The total length of hospital stay was not
which suggests that RA may be a good alternative. The significantly different but the total cost of anaesthesia was
main concerns associated with the use of RA are accelerated significantly less in the spinal anaesthesia group. Shoulder-tip
hypotension due to sympathetic blockade, ventilatory pain was recorded in 48% of patients and the hypotension
changes due to the higher sensory levels required, occurrence was also seen in 8 patients, but both of these complications
of shoulder-tip pain due to diaphragmatic irritation, and were easily controlled.[45]
increased surgical time due to limitation of the intra-
abdominal pressure. Imbelloni et al. in their comparison of 68 patients undergoing
LC under general or spinal anaesthesia also found spinal
Turkstani et al. compared GA with spinal anaesthesia in anaesthesia to be a safe and cost-effective technique,
50 patients undergoing laparoscopic cholecystectomy (LC) with 47% incidence of shoulder-tip pain and 41% incidence
Table 1: Showing studies comparing GA vs RA in laparoscopic cholecystectomy
Authors Number of patients Outcomes measured Results
included
Imbelloni et al. 33 patients in GA (n=33) vs 35 Post-operative pain, Significantly lower pain at 2 h, 4 h and 6 h post-
Patients (n=35) in spinal hemodynamic parameters, operatively in spinal group with lower cost and
group using low pressure complications, recovery, patient complete satisfaction. Perioperative vasopressor
pneumoperitoneum (8 mmHg) satisfaction and cost was given in 41% of patients in spinal group vs 3%
of patients in GA group. 47% of patients in spinal
group had shoulder-tip pain requiring analgesics
Ellakany 20 patients each in GA vs spinal Post-operative pain, intraoperative Significantly lower recovery and discharge time
group (n=20) using low pressure parameters, complications, (81 min vs 111.9 min) with good patient satisfaction
pneumoperitoneum (10 mmHg) recovery time and patient scores (3.6 vs 2.9) in spinal group but higher
satisfaction incidence of hypotension and bradycardia (40%)
and abdominal discomfort (25%). The surgeon
satisfaction scores were higher for GA group
compared to regional group (3 vs 4.1)
Mehta et al. 30 patients each in spinal vs GA Post-operative pain, intraoperative Significantly reduced pain scores (VAS) at 4 h, 8 h,
(n=30) using normal pressure and post-operative complications, 12 h, 24 h post-operatively in spinal anaesthesia
pneumoperitoneum (12 mmHg) recovery, hospital stay and group with no difference regarding complications,
degree of satisfaction recovery, stay or degree of satisfaction between
two groups. Hypotension was noted in 30%
cases of spinal vs 10% cases in GA group, with
more incidence of shoulder discomfort (10%)
intraoperatively
Tiwari et al. 114 patients in GA (n=114) Mean anaesthesia time, 4 patients from spinal group were converted
vs 110 patients in spinal pneumoperitoneum time, surgery to GA due to intraoperative events (abdominal
group (n=110) using low time as primary outcomes pain, anxiety and nausea). Significantly more
pressure (8-10 mmHg) and intraoperative events and mean anaesthesia time in GA group but a longer
pneumoperitoneum post-operative pain scores as pneumoperitoneum and total surgery time in spinal
secondary outcomes group (36.11±4.98 vs 34.22±5.83) Significantly
lower pain scores post-operatively in spinal group
at 6 h and 12 h but not at 24 h. The patients in
spinal group had more incidences of hypotension,
urinary retention and pain in back and patients in
GA group had more incidences of abdominal pain,
PONV and sore throat, post-operatively
Turkstani et al. 25 patients each in GA vs spinal Post-operative pain scores (VAS), Significantly lower pain scores (VAS) at admission
group (n=25) using low pressure total dose of analgesic used, to PACU (1.4±0.8 vs 4.7±1.4) with lower analgesic
(≤10 mmHg) pneumoperitoneum hospital length of stay and cost of requirements (12% vs 52%) in spinal group
each anaesthetic technique with significantly lower cost of anaesthesia. No
significant difference regarding hospital length
of stay. Intraoperatively, additional analgesics
required in 88% patients in GA vs 12% patients
in spinal group with 48% patients experiencing
shoulder-tip pain in spinal group
GA: General anaesthesia, RA: Regional anaesthesia, PACU: Post-anaesthesia care unit, VAS: Visual analogue scale
Journal of Minimal Access Surgery | January-March 2016 | Volume 12 | Issue 1 7
[Downloaded free from http://www.journalofmas.com on Monday, January 09, 2017, IP: 120.188.82.99]
Bajwa and Kulshrestha: GA vs RA for laparoscopic surgery
of significant hypotension, both of which responded to for laparoscopic procedures remains a debatable issue
pharmacological treatment with opioids and vasopressors, and most of the time it depends upon the experience and
respectively.[46] competency of the anaesthesiologist.
Ellakany, in his study of 40 patients receiving either general REFERENCES
or segmental thoracic spinal anaesthesia, found comparable
surgical conditions with superior post-operative analgesia 1. Gerges FJ, Kanazi GE, Jabbour-Khouri SI. Anesthesia for laparoscopy:
A review. J Clin Anesth 2006;18:67-78.
and significantly better satisfaction scores among patients in 2. Bajwa SJ, Takrouri MS. Innovations, improvisations, challenges and
the spinal anaesthesia group. He also found a 40% incidence constraints: The untold story of anesthesia in developing nations. Anesth
of significant hypotension and about 25% incidence of Essays Res 2014;8:1-2.
3. Bajwa SJ, Kalra S. A deeper understanding of anesthesiology practice: The
abdominal discomfort, which were easily managed. He biopsychosocial perspective. Saudi J Anaesth 2014;8:4-5.
found no patients with nausea and vomiting in the spinal 4. Bajwa SJ, Jindal R. Quality control and assurance in anesthesia: A necessity
anaesthesia group.[47] However, the use of newer, long-acting of the modern times. Anesth Essays Res 2014;8:134-8.
5. Bajwa SJ, Kalra S. Qualitative research in anesthesiology: An essential
anti-emetics like palonosetron reduces the incidence of PONV
practice and need of the hour. Saudi J Anaesth 2013;7:477-8.
to a significant extent.[48] 6. Collins LM, Vaghadia H. Regional anaesthesia for laparoscopy. Anesthesiol
Clin North America 2001;19:43-55.
7. Gutt CN, Oniu T, Mehrabi A, Schemmer P, Kashfi A, Kraus T, et al. Circulatory
Mehta et al., in their study of 60 patients, also found and respiratory complications of carbon dioxide insufflation. Dig Surg
better post-operative analgesia with spinal anaesthesia in 2004;21:95-105.
comparison to GA for LC. They found no significant difference 8. Zuckerman RS, Heneghan S. The duration of hemodynamic depression
during laparoscopic cholecystectomy. Surg Endosc 2002;16:1233-6.
between the groups regarding intraoperative complications, 9. Sprung J, Abdelmalak B, Schoenwald PK. Recurrent complete heart block in
recovery, length of hospital stay and degree of satisfaction. a healthy patient during laparoscopic electrocauterization of the fallopian
There was no incidence of nausea and vomiting in the patients tube. Anesthesiology 1998;88:1401-3.
10. Rauh R, Hemmerling TM, Rist M, Jacobi KE. Influence of pneumoperitoneum
who received spinal anaesthesia.[49] and patient positioning on respiratory system compliance. J Clin Anesth
2001;13:361-5.
All the studies in the literature suggest that RA may be 11. Hirvonen EA, Poikolainen EO, Pääkkönen ME, Nuutinen LS. The adverse
hemodynamic effects of anesthesia, head-up tilt, and carbon dioxide
considered comparable to GA in laparoscopic procedures pneumoperitoneum during laparoscopic cholecystectomy. Surg Endosc
regarding surgical conditions, intra- and post-operative 2000;14:272-7.
complications, and hospital length of stay, but may be 12. Salihoglu Z, Demiroluk S, Cakmakkaya S, Gorgun E, Kose Y. Influence of the
patient positioning on respiratory mechanics during pneumoperitoneum.
superior to GA with respect to the PONV, post-operative Middle East J Anaesthesiol 2002;16:521-8.
analgesia and early recovery. 13. Singh Bajwa SJ, Bajwa SK, Kaur J. Comparison of two drug combinations
in total intravenous anesthesia: Propofol-ketamine and propofol-fentanyl.
Saudi J Anaesth 2010;4:72-9.
The salient features of various studies comparing GA with 14. Wilmore DW, Kehlet H. Management of patients in fast track surgery. BMJ
RA are shown in Table 1. 2001;322:473-6.
15. Yang H, Choi PT, McChesney J, Buckley N. Induction with sevoflurane-
remifentanil is comparable to propofol-fentanyl-rocuronium in PONV after
CONCLUSION laparoscopic surgery. Can J Anaesth 2004;51:660-7.
16. Tramer M, Moore A, McQuay H. Omitting nitrous oxide in general
anaesthesia: Meta-analysis of intraoperative awareness and
Laparoscopic procedures have been traditionally performed
postoperative emesis in randomized controlled trials. Br J Anaesth
under GA due to the concerns about pneumoperitoneum- 1996;76:186-93.
related respiratory changes associated with it. However, 17. Bajwa S, Kulshrestha A. Dexmedetomidine: An adjuvant making large inroads
into clinical practice. Ann Med Health Sci Res 2013;3:475-83.
recently the use of RA has been introduced for these
18. Bajwa SJ, Kaur J, Singh A, Parmar S, Singh G, Kulshrestha A, et al. Attenuation
laparoscopic procedures. The evidence suggests the safety of pressor response and dose sparing of opioids and anaesthetics with
of the use of spinal, epidural and combined spinal-epidural pre-operative dexmedetomidine. Indian J Anaesth 2012;56:123-8.
19. Maltby JR, Beriault MT, Watson NC, Liepert D, Fick GH. The LMA-ProSeal
anaesthesia in laparoscopy with minimal side effects which
is an effective alternative to tracheal intubation for laparoscopic
can easily be managed with the available pharmacological cholecystectomy. Can J Anaesth 2002;49:857-62.
drugs. RA may provide certain advantages over GA, such as 20. Maltby JR, Beriault MT, Watson NC, Liepert DJ, Fick GH. LMAClassic and
lack of airway manipulation, maintenance of spontaneous LMA-ProSeal are effective alternatives to endotracheal intubation for
gynecologic laparoscopy. Can J Anaesth 2003;50:71-7.
respiration, effective post-operative analgesia, minimal 21. Salihoglu Z, Demiroluk S, Dikmen Y. Respiratory mechanics in morbid obese
nausea and vomiting, and early recovery and ambulation. patients with chronic obstructive pulmonary disease and hypertension
However, the safety of RA in laparoscopic procedures among during pneumoperitoneum. Eur J Anaesthesiol 2003;20:658-61.
22. Mazdisnian F, Palmieri A, Hakakha B, Hakakha M, Cambridge C, Lauria B.
various types of patient populations still needs to be verified Office microlaparoscopy for female sterilization under local anesthesia.
by further studies. Additionally, the technique of anaesthesia A cost and clinical analysis. J Reprod Med 2002;47:97-100.
8 Journal of Minimal Access Surgery | January-March 2016 | Volume 12 | Issue 1
[Downloaded free from http://www.journalofmas.com on Monday, January 09, 2017, IP: 120.188.82.99]
Bajwa and Kulshrestha: GA vs RA for laparoscopic surgery
23. Collins LM, Vaghadia H. Regional anesthesia for laparoscopy. Anesthesiol 37. Palachewa K, Chau-In W, Naewthong P, Uppan K, Kamhom R. Complications
Clin North America 2001;19:43-55. of spinal anaesthesia stinagarind hospital. Thai J Anaesth 2001;27:7-12.
24. Gramatica L Jr, Brasesco OE, Mercado Luna A, Martinessi V, Panebianco G, 38. Tzovaras G, Fafoulakis F, Pratsas K, Georgopoulou S, Stamatiou G,
Labaque F, et al. Laparoscopic cholecystectomy performed under regional Hatzitheofilou C. Laparoscopic cholecystectomy under spinal anaesthesia:
anesthesia in patients with chronic obstructive pulmonary disease. Surg A pilot study. Surg Endosc 2006;20:580-2.
Endosc 2002;16:472-5. 39. Imbelloni LE, Sant’anna R, Fornasari M, Fialho JC. Laparoscopic
25. Hamad MA, El-Khattary OA. Laparoscopic cholecystectomy under spinal cholecystectomy under spinal anesthesia: Comparative study between
anesthesia with nitrous oxide pneumoperitoneum: A feasibility study. Surg conventional dose and low-dose hyperbaric bupivacaine. Local Reg Anesth
Endosc 2003;17:1426-8. 2011;4:41-6.
26. Jindal R, Bajwa SJ. Paresthesias at multiple levels: A rare neurological 40. Boddy AP, Mehta S, Rhodes M. The effect of intraperitoneal local anesthesia
manifestation of epidural anesthesia. J Anaesthesiol Clin Pharmacol in laparoscopic cholecystectomy: A systematic review and meta-analysis.
2012;28:136-7. Anesth Analg 2006;103:682-8.
27. Bajwa S, Arora V, Kaur J, Singh A, Parmar SS. Comparative evaluation 41. van Zundert AA, Stultiens G, Jakimowicz JJ, van den Borne BE, van der Ham
of dexmedetomidine and fentanyl for epidural analgesia in lower limb WG, Wildsmith JA. Segmental spinal anaesthesia for cholecystectomy in a
orthopedic surgeries. Saudi J Anaesth 2011;5:365-70. patient with severe lung disease. Br J Anaesth 2006;96:464-6.
28. Kumar S, Bajwa SJ. Neuraxial opioids in geriatrics: A dose reduction study 42. Mane RS, Patil MC, Kedareshvara KS, Sanikop CS. Combined spinal epidural
of local anesthetic with addition of sufentanil in lower limb surgery for anesthesia for laparoscopic appendectomy in adults: A case series. Saudi
elderly patients. Saudi J Anaesth 2011;5:142-9. J Anaesth 2012;6:27-30.
29. Bajwa SJ, Bajwa SK, Kaur J, Singh G, Arora V, Gupta S, et al. Dexmedetomidine 43. Singh Bajwa SJ. Anesthesiology research and practice in developing nations:
and clonidine in epidural anaesthesia: A comparative evaluation. Indian J Economic and evidence-based patient-centered approach. J Anaesthesiol
Anaesth 2011;55:116-21. Clin Pharmacol 2013;29:295-6.
30. Bajwa SJ, Bajwa SK, Kaur J, Singh A, Bakshi G, Singh K, et al. Admixture 44. Bajwa SJ, Kalra S. Logical empiricism in anesthesia: A step forward in modern
of clonidine and fentanyl to ropivacaine in epidural anesthesia for lower day clinical practice. J Anaesthesiol Clin Pharmacol 2013;29:160-1.
abdominal surgery. Anesth Essays Res 2010;4:9-14. 45. Turkstani A, Ibraheim O, Khairy G, Alseif A, Khalil N. Spinal versus general
31. Vaghadia H, Viskari D, Mitchell GW, Berrill A. Selective spinal anesthesia anesthesia for laparoscopic cholecystectomy: A cost effectiveness and side
for outpatient laparoscopy. I: Characteristics of three hypobaric solutions. effects study APICARE 2009;13:9-14.
Can J Anaesth 2001;48:256-60. 46. Imbelloni LE, Fornasari M, Fialho JC, Sant’Anna R, Cordeiro JA. General
32. Lennox PH, Vaghadia H, Henderson C, Martin L, Mitchell GW. Small-dose anesthesia versus spinal anesthesia for laparoscopic cholecystectomy. Rev
selective spinal anesthesia for short-duration outpatient laparoscopy: Bras Anestesiol 2010;60:217-27.
Recovery characteristics compared with desflurane anesthesia. Anesth 47. Ellakany M. Comparative study between general and thoracic spinal anesthesia
Analg 2002;94:346-50. for laparoscopic cholecystectomy. Egyptian J Anaesth 2013;29:375-81.
33. Stewart AV, Vaghadi H, Collins L, Mitchell GW. Small-dose selective spinal 48. Bajwa SS, Bajwa SK, Kaur J, Sharma V, Singh A, Singh A, et al. Palonosetron:
anaesthesia for short-duration outpatient gynaecological laparoscopy: A novel approach to control postoperative nausea and vomiting in day care
Recovery characteristics compared with propofol anaesthesia. Br J Anaesth surgery. Saudi J Anaesth 2011;5:19-24.
2001;86:570-2. 49. Mehta PJ, Chavda HR, Wadhwana AP, Porecha MM. Comparative analysis
34. Tiwari S, Chauhan A, Chaterjee P, Alam MT. Laparoscopic cholecystectomy of spinal versus general anesthesia for laparoscopic cholecystectomy: A
under spinal anaesthesia: A prospective, randomised study. J Minim Access controlled, prospective, randomized trial. Anesth Essays Res 2010;4:91-5.
Surg 2013;9:65-71.
35. Sinha R, Gurwara AK, Gupta SC. Laparoscopic cholecystectomy under spinal
anaesthesia: A study of 3492 patients. J Laparoendosc Adv Surg Tech A Cite this article as: Bajwa SJ, Kulshrestha A. Anaesthesia for laparoscopic
2009;19:323-7. surgery: General vs regional anaesthesia. J Min Access Surg 2016;12:4-9.
36. Hartman B, Junger A, Klasen J, Benson M, Jost A, Banzhaf A, et al. The incidence Date of submission: 01-02-2015, Date of acceptance: 12-05-2015
and risk factors for hypotension after spinal anesthesia induction: An analysis
Source of Support: Nil, Conflicts of Interest: None declared.
with automated data collection. Anesth Analg 2002;94:1521-9, table of contents.
Journal of Minimal Access Surgery | January-March 2016 | Volume 12 | Issue 1 9
You might also like
- Contemporary Endoscopic Spine Surgery Volume 1: Cervical SpineFrom EverandContemporary Endoscopic Spine Surgery Volume 1: Cervical SpineNo ratings yet
- Journal of Anesthesia & Clinical ResearchDocument5 pagesJournal of Anesthesia & Clinical ResearchestiplwNo ratings yet
- 12871_2015_Article_158Document9 pages12871_2015_Article_158ss huNo ratings yet
- Regional Anesthesia For Laparoscopic SurgeryDocument18 pagesRegional Anesthesia For Laparoscopic SurgeryEdgardo CastroNo ratings yet
- Articulo - Anestesia CX UrologicaDocument5 pagesArticulo - Anestesia CX UrologicaNFSOTNo ratings yet
- Spinal Anaesthesia VS General Anaesthesia in Scopic UrosurgeryDocument4 pagesSpinal Anaesthesia VS General Anaesthesia in Scopic UrosurgeryCentral Asian StudiesNo ratings yet
- Anaesthesia For Laparoscopic SurgeryDocument5 pagesAnaesthesia For Laparoscopic SurgeryJair GonzálezNo ratings yet
- Anestesia - Cardiovascular - Luna OrtizDocument11 pagesAnestesia - Cardiovascular - Luna OrtizWeimar Andres Bonilla MosqueraNo ratings yet
- Erdem 2018Document9 pagesErdem 2018SFS GAMEX546No ratings yet
- Laparoscopic Cholecystectomy Under Spinal AnaestheDocument7 pagesLaparoscopic Cholecystectomy Under Spinal Anaestherazaqhussain00No ratings yet
- RESP Failure in The ICU 2Document12 pagesRESP Failure in The ICU 2Keith SaccoNo ratings yet
- A Litterature Review of Intrathecal Morphine Analgesia in Patients Undergoing Hepato Pancreatic Biliary SurgeryDocument12 pagesA Litterature Review of Intrathecal Morphine Analgesia in Patients Undergoing Hepato Pancreatic Biliary Surgeryvalerio.messinaNo ratings yet
- Daigle-Boerema Gastropexy PEHDocument7 pagesDaigle-Boerema Gastropexy PEHGunduz AgaNo ratings yet
- [Journal of the American Veterinary Medical Association] Development of Enhanced Recovery After Surgery (ERAS) protocols in veterinary medicine through a one-health approach_ the role of anesthesia and locoregional techniquesDocument9 pages[Journal of the American Veterinary Medical Association] Development of Enhanced Recovery After Surgery (ERAS) protocols in veterinary medicine through a one-health approach_ the role of anesthesia and locoregional techniquesFrancisco Laecio Silva de AquinoNo ratings yet
- 25A RA Changing Anaesthesia TrendsDocument4 pages25A RA Changing Anaesthesia TrendstomeyttoNo ratings yet
- Laparoscopy and Laparoscopic SurgeryDocument7 pagesLaparoscopy and Laparoscopic SurgeryLaura RojasNo ratings yet
- Preemptive Quadratus Lumborum Laparoscopic BariatricDocument8 pagesPreemptive Quadratus Lumborum Laparoscopic BariatricEmmanuel FortalezaNo ratings yet
- Anaesthesia techniques for laparoscopic surgeryDocument4 pagesAnaesthesia techniques for laparoscopic surgeryRizwan AhmedNo ratings yet
- Practice Guidelines For Preoperative FastingDocument18 pagesPractice Guidelines For Preoperative FastingTaufik RachmanNo ratings yet
- Scott 2015Document20 pagesScott 2015Raíla SoaresNo ratings yet
- Laparoscopic SurgeryDocument4 pagesLaparoscopic SurgerycaioaccorsiNo ratings yet
- A Anesth 3Document22 pagesA Anesth 3sneha.doc987No ratings yet
- Anesthesia For Advanced Bronchoscopic Procedures: State-of-the-Art ReviewDocument13 pagesAnesthesia For Advanced Bronchoscopic Procedures: State-of-the-Art ReviewRichard PhoNo ratings yet
- Anaesthesia Management For Bronchoscopic and Surgical Lung Volume ReductionDocument6 pagesAnaesthesia Management For Bronchoscopic and Surgical Lung Volume ReductionRoni ArdianNo ratings yet
- Modes of Mechanical Ventilation For The Operating Room BestPracResAnest 2015 PDFDocument15 pagesModes of Mechanical Ventilation For The Operating Room BestPracResAnest 2015 PDFRicardoNo ratings yet
- Chagpar-2021-Annals of Surgical OncologyDocument4 pagesChagpar-2021-Annals of Surgical OncologyFrancisco Gomez GlezNo ratings yet
- Borges 2006 Plateau 60Document11 pagesBorges 2006 Plateau 60pablopg_5No ratings yet
- Acta Anaesthesiol Scand - 2015 - ScottDocument20 pagesActa Anaesthesiol Scand - 2015 - ScottVasile ArianNo ratings yet
- Literature Review Respiratory Changes During Spinal Anesthesia in Gynecological LaparosDocument10 pagesLiterature Review Respiratory Changes During Spinal Anesthesia in Gynecological Laparosfabian arassiNo ratings yet
- 249 FullDocument9 pages249 FullAHMEDNo ratings yet
- Advancements in Upper Gastrointestinal Endoscopic Therapy: A Comprehensive ReviewDocument12 pagesAdvancements in Upper Gastrointestinal Endoscopic Therapy: A Comprehensive ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Reoperative Antireflux Surgery For Failed Fundoplication: An Analysis of Outcomes in 275 PatientsDocument8 pagesReoperative Antireflux Surgery For Failed Fundoplication: An Analysis of Outcomes in 275 PatientsDiego Andres VasquezNo ratings yet
- Laparoscopic AdrenalectomyDocument12 pagesLaparoscopic AdrenalectomyTay SalinasNo ratings yet
- Peripheral Regional Anaesthesia and Outcome: Lessons Learned From The Last 10 YearsDocument14 pagesPeripheral Regional Anaesthesia and Outcome: Lessons Learned From The Last 10 YearsPrisky ChriselawatiNo ratings yet
- Minimally Invasive Cardiac Surgery: A Safe Alternative For Aortic Valve Replacement?Document2 pagesMinimally Invasive Cardiac Surgery: A Safe Alternative For Aortic Valve Replacement?lkulacogluNo ratings yet
- An Analysis of The Cost-Effectiveness of Spinal Versus General Anesthesia For Lumbar Spine Surgery in Various Hospital SettingsDocument7 pagesAn Analysis of The Cost-Effectiveness of Spinal Versus General Anesthesia For Lumbar Spine Surgery in Various Hospital SettingsGaetano De BiaseNo ratings yet
- Effect of Intraoperative Fluid Management On Outcome After Intraabdominal SurgeryDocument8 pagesEffect of Intraoperative Fluid Management On Outcome After Intraabdominal Surgeryade_liaNo ratings yet
- 1 s2.0 S1743919116308421 MainDocument10 pages1 s2.0 S1743919116308421 MainRony RonyNo ratings yet
- Airway Management During Upper GI Endoscopic Procedures2016Document9 pagesAirway Management During Upper GI Endoscopic Procedures2016jcarl_20063003No ratings yet
- Randomized Clinical Trial of Epidural, Spinal or Patient-Controlled Analgesia For Patients Undergoing Laparoscopic Colorectal SurgeryDocument11 pagesRandomized Clinical Trial of Epidural, Spinal or Patient-Controlled Analgesia For Patients Undergoing Laparoscopic Colorectal Surgeryvalerio.messinaNo ratings yet
- Surgery 23 3 1Document6 pagesSurgery 23 3 1razaqhussain00No ratings yet
- Application of Lung Ultrasound in Critical Care Setting: A ReviewDocument15 pagesApplication of Lung Ultrasound in Critical Care Setting: A ReviewThuanNo ratings yet
- Future Perspectives and Research Initiatives in Fast-Track SurgeryDocument4 pagesFuture Perspectives and Research Initiatives in Fast-Track Surgeryบังอร น้อยอำ่No ratings yet
- Kim 2017 PDFDocument7 pagesKim 2017 PDFPablo IgnacioNo ratings yet
- Is Regional Anesthesia Preferable To General Anesthesia For Outpatient Surgical Procedures On An Upper ExtremityDocument4 pagesIs Regional Anesthesia Preferable To General Anesthesia For Outpatient Surgical Procedures On An Upper Extremityangelama1783riosNo ratings yet
- s42077 021 00145 7Document8 pagess42077 021 00145 7Nguyễn Thị Mai XuânNo ratings yet
- Journal Homepage: - : Manuscript HistoryDocument9 pagesJournal Homepage: - : Manuscript HistoryIJAR JOURNALNo ratings yet
- A Review of Anesthetic Effects On Renal Function: Potential Organ ProtectionDocument10 pagesA Review of Anesthetic Effects On Renal Function: Potential Organ ProtectionSianipar RomulussNo ratings yet
- Journal of Anesthesia & Clinical ResearchDocument8 pagesJournal of Anesthesia & Clinical ResearchAyu Aprilisa D PutriNo ratings yet
- US Pulmón para Manejo de Atelectasias PerioperatoriasDocument11 pagesUS Pulmón para Manejo de Atelectasias PerioperatoriasJURAGOMANo ratings yet
- Research ArticleDocument7 pagesResearch ArticleYosia KevinNo ratings yet
- Spinal vs. General Anesthesia For Percutaneous Nephrolithotomy: A Prospective Randomized TrialDocument5 pagesSpinal vs. General Anesthesia For Percutaneous Nephrolithotomy: A Prospective Randomized TrialDella Puspita SariNo ratings yet
- Laparoscopic OvariectomíaDocument15 pagesLaparoscopic Ovariectomíasimon alfaro gonzálezNo ratings yet
- AnesthEssaysRes1017-7862084 215020Document6 pagesAnesthEssaysRes1017-7862084 215020Idaan Veraguas ElectromecánicaNo ratings yet
- Anaesthesia Critical Care & Pain MedicineDocument7 pagesAnaesthesia Critical Care & Pain MedicineManolin KinNo ratings yet
- Current Trends in Anesthesia For Esophagectomy 2017Document6 pagesCurrent Trends in Anesthesia For Esophagectomy 2017Ajay Varun ReddyNo ratings yet
- Article. (Review) Laparoscopic Surgery For Rectal Cancer.2009Document6 pagesArticle. (Review) Laparoscopic Surgery For Rectal Cancer.2009Trí Cương NguyễnNo ratings yet
- Regional Anesthesia and OutcomesDocument5 pagesRegional Anesthesia and OutcomespitriaNo ratings yet
- Laparoscopic Versus Open Appendicectomy: A Comparative StudyDocument7 pagesLaparoscopic Versus Open Appendicectomy: A Comparative StudyChristianWicaksonoNo ratings yet
- World Journal of Emergency Surgery: Emergency Laparoscopy - Current Best PracticeDocument9 pagesWorld Journal of Emergency Surgery: Emergency Laparoscopy - Current Best PracticeHendra JojoNo ratings yet
- Gut Brain AxisDocument14 pagesGut Brain AxisBefrie Mahaztra SNo ratings yet
- 7397 PDFDocument8 pages7397 PDFBefrie Mahaztra SNo ratings yet
- Jurnal Anestesi 7Document10 pagesJurnal Anestesi 7DillaNo ratings yet
- Brain Tumor NICEDocument60 pagesBrain Tumor NICEBefrie Mahaztra SNo ratings yet
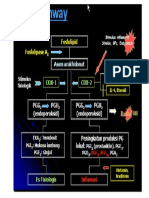
- COX PathwayDocument1 pageCOX PathwayBefrie Mahaztra SNo ratings yet
- Gut Brain AxisDocument14 pagesGut Brain AxisBefrie Mahaztra SNo ratings yet
- Primary Brain TumorDocument9 pagesPrimary Brain TumorvaraNo ratings yet
- Three-Step Analgesic LadderDocument3 pagesThree-Step Analgesic LadderBefrie Mahaztra SNo ratings yet
- Jurnal Bradi 4Document15 pagesJurnal Bradi 4befriNo ratings yet
- 581 PDFDocument64 pages581 PDFkookiescreamNo ratings yet
- Jurnal Bradi 1 PDFDocument19 pagesJurnal Bradi 1 PDFBefrie Mahaztra SNo ratings yet
- Pi Is 001236921733283 XDocument10 pagesPi Is 001236921733283 XBefrie Mahaztra SNo ratings yet
- DR Wina Cacute Aortic Dissection JCU EditedDocument31 pagesDR Wina Cacute Aortic Dissection JCU EditedBefrie Mahaztra SNo ratings yet
- Jurnal 3Document6 pagesJurnal 3Befrie Mahaztra SNo ratings yet
- Jurnal Terbaru KesehatanDocument5 pagesJurnal Terbaru KesehatanBefrie Mahaztra SNo ratings yet
- File Jurnal TerbatuDocument7 pagesFile Jurnal TerbatuBefrie Mahaztra SNo ratings yet
- WelcomeDocument5 pagesWelcomeCatNo ratings yet
- Jurnal Perawatan LukaDocument7 pagesJurnal Perawatan LukaBefrie Mahaztra SNo ratings yet
- Ethicon Wound Closure ManualDocument126 pagesEthicon Wound Closure Manualkeish193100% (3)
- Handbook of PEDIATRIC SURGERY PDFDocument43 pagesHandbook of PEDIATRIC SURGERY PDFPETERNo ratings yet
- JNC 8Document14 pagesJNC 8amiwahyuniNo ratings yet
- JNC 8Document14 pagesJNC 8amiwahyuniNo ratings yet
- Jurnal 6 PDFDocument9 pagesJurnal 6 PDFBefrie Mahaztra SNo ratings yet
- Eun 193Document5 pagesEun 193Befrie Mahaztra SNo ratings yet
- Eventos Cardiovasculares Durante La Copa MUndo de FutbolDocument9 pagesEventos Cardiovasculares Durante La Copa MUndo de FutbolDiego CardonaNo ratings yet
- Pi Is 001236921733283 XDocument10 pagesPi Is 001236921733283 XBefrie Mahaztra SNo ratings yet
- Eun 193Document5 pagesEun 193Befrie Mahaztra SNo ratings yet
- Jurnal Perawatan LukaDocument7 pagesJurnal Perawatan LukaBefrie Mahaztra SNo ratings yet
- Eventos Cardiovasculares Durante La Copa MUndo de FutbolDocument9 pagesEventos Cardiovasculares Durante La Copa MUndo de FutbolDiego CardonaNo ratings yet
- Cardiac Anaesthesia Thesis TopicsDocument6 pagesCardiac Anaesthesia Thesis Topicsfbzgmpm3100% (2)
- Pharmacology: General Anaesthetic AgentsDocument65 pagesPharmacology: General Anaesthetic AgentsSharifa DarayanNo ratings yet
- Baska MaskDocument8 pagesBaska MaskAnish H DaveNo ratings yet
- Society For Obstetric Anesthesia and Perinatology .95413Document16 pagesSociety For Obstetric Anesthesia and Perinatology .95413dhana iphoneNo ratings yet
- AnalgesikDocument2 pagesAnalgesikNopriani InuarNo ratings yet
- Miller's Anesthesia, 8th Edition: Anesthesiology April 2016Document3 pagesMiller's Anesthesia, 8th Edition: Anesthesiology April 2016Sabbir AhammedNo ratings yet
- Get Ahead SJTDocument256 pagesGet Ahead SJTtheAce89100% (3)
- Risk Register Peralatan Medik 2022Document8 pagesRisk Register Peralatan Medik 2022maintenance anmedNo ratings yet
- Post Operative Pain ReliefDocument8 pagesPost Operative Pain ReliefHamdani AbderraoufNo ratings yet
- Staff Knowledge Correlates with Triage SkillsDocument9 pagesStaff Knowledge Correlates with Triage SkillsLizna Rohani BatubaraNo ratings yet
- Primary MCQ Guide UpdateDocument21 pagesPrimary MCQ Guide UpdateGanda SilitongaNo ratings yet
- Postoperative Care: Nursing ManagementDocument25 pagesPostoperative Care: Nursing ManagementHarjotBrarNo ratings yet
- ps09 2010 Guidelines On Sedation and or Analgesia For Diagnostic and Interventional Medical Dental or Surgical ProceduresDocument16 pagesps09 2010 Guidelines On Sedation and or Analgesia For Diagnostic and Interventional Medical Dental or Surgical ProceduresJane KoNo ratings yet
- PENGARUH SUCTION ETT TERHADAP SATURASI OKSIGENDocument8 pagesPENGARUH SUCTION ETT TERHADAP SATURASI OKSIGENipurplaNo ratings yet
- Anestesia Felino HidrocefalicoDocument3 pagesAnestesia Felino HidrocefalicoMabe AguirreNo ratings yet
- Imcu 10 Beds Nicu 16 Beds Picu 6 Beds: Typical Noggin FixingDocument1 pageImcu 10 Beds Nicu 16 Beds Picu 6 Beds: Typical Noggin Fixingmanikandan4strlNo ratings yet
- Anaesthetic Safety Checklist GuideDocument2 pagesAnaesthetic Safety Checklist GuideMisi VetNo ratings yet
- Download ebook Smith And Aitkenheads Textbook Of Anaesthesia 7Th Edition Pdf full chapter pdfDocument67 pagesDownload ebook Smith And Aitkenheads Textbook Of Anaesthesia 7Th Edition Pdf full chapter pdfelaine.kern334100% (22)
- Chaos Aug 2016Document165 pagesChaos Aug 2016Mohamed SaberNo ratings yet
- Programm BCSACDocument2 pagesProgramm BCSACEranda BegajNo ratings yet
- Final Anaesthesia QuestionsDocument23 pagesFinal Anaesthesia QuestionsRancesh FamoNo ratings yet
- 1.introduction To Anesthesiology CSU CMS LectureDocument26 pages1.introduction To Anesthesiology CSU CMS LectureKenneth MiguelNo ratings yet
- Epidural AnesthesiaDocument5 pagesEpidural AnesthesiaImran MukhlessNo ratings yet
- Textbook of Rapid Response Systems Concept and ImplementationDocument392 pagesTextbook of Rapid Response Systems Concept and ImplementationKrish BanothuNo ratings yet
- Naskah PublikasiDocument12 pagesNaskah PublikasiMuhammad Abdul AzizNo ratings yet
- Thank You For Your Patronage, Meet Our New Associate Dr. RudyDocument1 pageThank You For Your Patronage, Meet Our New Associate Dr. RudyLayth Al KaissyNo ratings yet
- HLA MediShield ENG - Updated AUG 18Document16 pagesHLA MediShield ENG - Updated AUG 18Chan SCNo ratings yet
- Filtvebis Xelovnuri Ventilaciis Tanamedrove Metodebi Da RejimebiDocument45 pagesFiltvebis Xelovnuri Ventilaciis Tanamedrove Metodebi Da RejimebiMiranda BeridzeNo ratings yet
- Initiation and Maintenance of Labour Analgesia: Epidural or CSE, Bolus or InfusionDocument32 pagesInitiation and Maintenance of Labour Analgesia: Epidural or CSE, Bolus or Infusionleo chiuNo ratings yet
- Pengaruh Pemberian Infus Hangat Terhadap Stabilitas Suhu Tubuh Pada Pasien Post Operasi General Anestesi Di Recovery Room Rsu Karsa Husada BatuDocument7 pagesPengaruh Pemberian Infus Hangat Terhadap Stabilitas Suhu Tubuh Pada Pasien Post Operasi General Anestesi Di Recovery Room Rsu Karsa Husada BatuKonsul Dosen PembibingNo ratings yet
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (17)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (5)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (403)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosFrom Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosRating: 4.5 out of 5 stars4.5/5 (207)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)
- Algorithms to Live By: The Computer Science of Human DecisionsFrom EverandAlgorithms to Live By: The Computer Science of Human DecisionsRating: 4.5 out of 5 stars4.5/5 (722)
- Summary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedRating: 4 out of 5 stars4/5 (11)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)













![[Journal of the American Veterinary Medical Association] Development of Enhanced Recovery After Surgery (ERAS) protocols in veterinary medicine through a one-health approach_ the role of anesthesia and locoregional techniques](https://imgv2-1-f.scribdassets.com/img/document/597027379/149x198/4e86c3e723/1710567751?v=1)