Professional Documents
Culture Documents
Levamisole in L.P
Uploaded by
jalalfaizOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Levamisole in L.P
Uploaded by
jalalfaizCopyright:
Available Formats
Ann Dermatol Vol. 21, No.
3, 2009
ORIGINAL ARTICLE
Levamisole Monotherapy for Oral Lichen Planus
Tai Hyok Won, M.D., Se Young Park, M.D., Bo Suk Kim, M.D., Phil Seung Seo, M.D.,
1
Seok Don Park, M.D., Ph.D.
Department of Dermatology, 1The Institute of Wonkwang Medical Science, Wonkwang University School of Medicine, Iksan, Korea
Background: Several different kinds of drugs have been used INTRODUCTION
to treat chronic oral lichen planus (OLP). During the last
decade, there have been several reports demonstrating Oral lichen planus (OLP) is defined as a T-cell mediated
success with levamisole and low dose prednisolone therapy inflammatory disease of the oral mucosa1. OLP is a chro-
for treating OLP. However, some OLP patients who have nic disease and it rarely undergo spontaneous remission,
underlying diseases such as diabetes, hypertension and and it has the potential to become malignant2. The con-
malignancy are unable to take steroids. Objective: The aim ventional treatments for OLP are topical and systemic
of this study was to evaluate levamisole monotherapy for corticosteroids, mycophenolate mofetil, cyclosporine, me-
treating OLP. Methods: Eleven patients who had OLP were thotrexate, dapsone, griseofulvin, retinoids, pimecrolimus,
treated with levamisole between 2005 and 2007. The tacrolimus, PUVA, 308 nm-excimer laser, hydroxychloro-
levamisole was administered at a dose 50 mg thrice daily for quine and low molecular weight heparin (enoxaparin)3-13.
three consecutive days, but then it was not administered on Most patients have been treated with steroids, yet many
the following four days. Results: After 2 weeks of treatment, patients who have underlying diseases such as diabetes,
8 patients reported a partial response, 3 patients reported no hypertension and malignancy have limitations for using
response and no patients reported clearance of lesion. After immunosuppressants.
4 weeks of treatment, 6 patients reported a partial response, During the last decade, there have been several reports
3 patients reported no response and 2 patients reported demonstrating the success with using levamisole and low
clearance of lesion. Furthermore, after 3 months of treat- dose prednisolone therapy for oral lichen planus14-16.
ment, 3 patients reported a partial response, 3 patients re- Indeed, the patients with OLP showed a dramatic res-
ported no response and 5 patients reported complete ponse to this therapy14,15. Levamisole is an effective immu-
clearance of lesion. Clinical improvement was shown in 2 nomodulating agent that can restore the normal phago-
weeks, whilst the mean duration to achieve clearance of cytic activity of macrophages and neutrophils, it modula-
lesion was 6.2 weeks. Although 1 patient had mild itching, tes T-cell mediated immunity and it potentiates the activity
there were no significant adverse effects. Conclusion: of human interferon17-21. It is used to treat several mali-
Levamisole monotherapy could be a successful and safe gnancies and autoimmune diseases (for example, rheuma-
treatment option for patients with chronic OLP and who toid arthritis and systemic lupus erythematosus), vitiligo
cannot take steroids. (Ann Dermatol 21(3) 250∼254, 2009) and viral warts22-29.
In this article, we present a case series for evaluating
-Keywords- levamisole monotherapy without steroids for treating OLP.
Levamisole, Oral lichen planus (OLP)
MATERIALS AND METHODS
Received November 12, 2008, Accepted for publication December 18, Retrospective chart review
2008
*This paper was supported by Wonkwang University in 2009. We performed a retrospective medical chart review of 11
Reprint request to: Seok Don Park, M.D., Department of Dermatology, patients who were diagnosed with OLP and we subseque-
Wonkwang University Hospital, 344-2, Sinyong-dong, Iksan 570-711, ntly treated these patients with levamisole monotherapy at
Korea. Tel: 82-63-859-1601, Fax: 82-63-842-1895, E-mail: sdpark@ the Dermatology Department of Wonkwang University
wonkwang.ac.kr
Hospital from 2005 to 2007. This study was approved by
250 Ann Dermatol
Levamisole Monotherapy for Oral Lichen Planus
the Institutional Review Board at Wonkwang University changes. One hundred percent remission of the patch and
Hospital, Iksan, Korea. The diagnosis of OLP was made by erosion was defined as complete clearance. A partial
the clinical history, the physical examination and the response was defined when some lesions of the patch or
histopathologic findings. Any patients who had an the erosion were remitted on physician’s gross exami-
OLP-like lesion induced by drugs or dental prosthetics nation. No improvement or worsening of the disease was
were excluded from the study. All the patients had drug defined as no change. Treatment failure was classified as
washout periods of 3 months. On the retrospective chart those patients who had no clinical improvement at least
review, we obtained the following information: the once during treatment over a 3 month period. The lesions
disease site, the disease duration, the previous treatment, that recurred after complete or partial improvement were
the subjective and objective clinical responses to levami- counted as a complete or partial response, and we
sole monotherapy, the adverse effects during levamisole recorded the disease free-duration and the number of
monotherapy and the skin biopsy findings. Before the recurrences.
initiation of levamisole monotherapy, we performed a
baseline complete blood cell count, liver and kidney RESULTS
function tests and chest x-ray. A blood test was performed
once a month and a skin biopsy was performed in the Eleven patients were diagnosed as having OLP and they
event of a reticulated or ulcerated lesion. were treated with levamisole monotherapy. Eight patients
The levamisole was administered at a dose of 50 mg (72.7%) were female and the mean age of all the patients
thrice daily for three consecutive days, and then it was not was 42.6 years (range: 20∼61 years). The mean duration
administered on the following four days. This treatment of OLP was 20.8 months (range: 3 months∼5 years). All
cycle was repeated until the OLP oral lesion was cleaned the patients had OLP on the buccal mucosa, except
out. Every patient was evaluated every 2 weeks, and they patient #1 who had OLP on the tongue base. All the
were evaluated again at least 3 months. patients had a whitish reticulated patch, except 1 patient
Based on objective clinical improvement, which was who had an ulcerated patch. Three patients had dental
retrospectively analyzed by the patients’ charts and the prosthetics, but these dental prosthetics were not the
clinical photos, the patients were categorized as having cause of the OLP because of the distance between the oral
achieved complete clearance, a partial response or no lesion and the dental prosthetics (Table 1).
Table 1. The characteristics and past treatment histories of the patients
Age/ Dental
No. Site Duration Lesion Previous treatment
Gender prosthesis
1 20/F Tongue base 1 y White reticulated patch Topical steroid injection and ointment applied Gold
2 46/M Buccal 5 y White reticulated patch Systemic steroid −
Topical steroid ointment
Gaggling – Tantum, lidocaine
3 54/F Buccal 3 y White reticulated patch Systemic steroid −
Topical steroid ointment
4 31/F Buccal 1 y White reticulated patch −
with superficial erosion
5 57/M Buccal 1.5 y White reticulated patch Systemic steroid −
Topical steroid ointment
6 42/F Buccal 4 y White eroded patch Systemic steroid −
Topical steroid ointment
Gaggling – Tantum
7 61/F Buccal 4 m White reticulated patch Systemic steroid Amalgam
Topical steroid ointment
Antifungal agent
Gaggling – Tantum, lidocaine
8 32/F Buccal 2 y White reticulated patch Systemic steroid −
Topical steroid
9 44/F Buccal 6 m White reticulated patch −
10 35/M Buccal 6 m White reticulated patch Topical steroid ointment −
11 46/F Buccal 3 m White reticulated patch Gold
Vol. 21, No. 3, 2009 251
TH Won, et al
Fig. 1. Photography before and
after 2 weeks of levamisole mono-
therpay (patient #4). Almost all the
lesions of patient #4 faded away
after 2 weeks of levamisole mono-
therapy (A: before treatment, B:
after treatment).
6.2 weeks). However, patient #1 had several recurrences.
Table 2. The clinical response after 2 weeks, 4 weeks and 3
months of levamisole monotherapy During the 2 year follow up period, patient #1 had a total
of 6 recurrences, but the lengths of disease free periods
Complete Partial No
clearance response changes
were increased.
No patient had any significant side effects or laboratory
After 2 weeks 0 8 3
changes. Patient #4 had mild itching after receiving
After 4 weeks 2 6 3
After 3 months 5 3 3 medication at week 2, but this resolved quickly with the
use of an antihistamine (Table 3).
After 2 weeks of treatment, 8 patients (55%) showed a DISCUSSION
partial response (Fig. 1) and 3 patients had no response.
No patient had complete clearance of lesion. Patient #4 Oral lichen planus is a chronic and troublesome inflam-
had mild itching after receiving the medication, but the matory oral disease. Even though there are many treat-
itching was controlled with antihistamine medication ment options available for OLP, it is very hard to effec-
(Table 2). tively treat this malady.
After 4 weeks of treatment, 6 patients (72.7%) showed a Levamisole is a levisomer of tetramisole ((-)-2,3,5,6-tetra-
partial response, 2 patients (18.2%) had complete clea- hydro-6-phenylimidazole [2,1-6] thiazole monohydrochlo-
rance and 3 patients again showed no response (Table 2). ride), and has been used as a broad spectrum anti-hel-
After 3 months of treatment, 3 patients (72.7%) showed a minthic drug since 1966.
partial response and 5 patients (45.5%) showed complete In 1978, Renoux et al.30 reported that levamisole in-
clearance. However, 3 patients showed no response, so creased cellular immunity. In 1990, the FDA approved
they were defined as treatment failures. Interestingly, the levamisole for many autoimmune and inflammatory disea-
disease duration of the patients who showed no response ses. Levamisole is currently used for the treatment of vitili-
was shorter than that of the patients who had a response go, viral warts, systemic lupus erythematosus, rheumatoid
(Table 2). arthritis and colon cancer22-29.
Eight patients, except 3 patients who had no response, The first treatment trial of levamisole for OLP was con-
showed clinical improvement at the next visit (after 2 ducted by Lu et al.14 in 1995. In that trial, 23 patients were
weeks). Complete clearance occurred in 5 patients and treated with levamisole (150 mg/d, 3 times per week) and
their treatment duration was 3 weeks to 3 months (mean: low dose prednisolone. After 2 weeks of treatment, 12
252 Ann Dermatol
Levamisole Monotherapy for Oral Lichen Planus
Table 3. Summary of the treatment results
Age/ Treatment Clinical Adverse
No. Duration Treatment response
Gender duration Response* effect
1 20/F 1 y 2 weeks later – Mild improvement 1 month O No
4 weeks later – Complete healing / 2 years
Intermittent recurrence (1~6 months interval, for 2 years)
2 46/M 5 y 2 week later – Moderate improvement 3 weeks O No
4 weeks later – Complete healing
3 54/F 3 y 2 week later – Great improvement 1 month O No
4 weeks later – Complete healing
4 31/F 1 y 2 week later – Mild improvement 3 months O Itching
4 weeks later – Great improvement
3 months later – Complete healing
5 57/M 1.5 y 2 weeks later – Mild improvement 2 months O No
3 months later – Complete healing
6 42/F 4 y 2, 4 weeks later – Mild improvement 3 months ∆ No
3 months later – Mild eroded lesion
7 61/F 4 m 2, 4 weeks later – Mild improvement 1 year ∆ No
Intermittent recurrence for 1 year
8 32/F 2 y 2 weeks, 4 weeks, 5 weeks – Mild improvement 5 weeks ∆ No
9 44/F 6 m No response for 3 weeks 3 weeks X No
10 35/M 6 m No response for 4 weeks 4 weeks X No
11 46/F 3 m No response for 3 weeks 3 weeks X No
*O: complete clearance, ∆: partial response, X: no response
patients showed over 80% improvement, whereas 11 Only 1 patient had an adverse effect, which was itching
patients showed no response. After 4 weeks of treatment, after receiving medication. This was resolved by using an
23 patients had over 80% improvement and the remission antihistamine (hydroxyzine Hcl). Levamisole has been
duration was 9.5 months. Because most of the OLP reported to have many adverse effects such as nausea,
patients in our trial had many underlying diseases, they vomiting, fever, dizziness, headache, tiredness, skin rash,
were restricted from taking steroids, so we tried to treat anaphylaxis and most severely, agranulocytosis20,21,30-33.
the OLP without steroids. In our study, after 2 weeks of Agranulocytosis is commonly seen in those patients with
levamisole monotherapy, 6/11 patients (55%) showed HLA-B27 positivity and in those patients who have un-
clinical improvement. After 4 weeks of treatment, 2 pa- dergone long term levamisole therapy32,33. For this reason,
tients (18.2%) showed complete clearance and 8 patients levamisole is usually recommended for intermittent use. In
(73%) showed clinical improvement. After 3 months of rheumatoid arthritis patients, the number of agranulocyto-
treatment, 5 patients (45.4%) showed complete clearance sis cases decreased after receiving levamisole 1∼2 times a
of lesion. However, 3 patients showed no response from week, and the levamisole showed equivalent efficacy with
the initiation of this therapy. levamisole continuous therapy34. Therefore, we recom-
The treatment effect of levamisole monotherapy might be mend using levamisole (150 mg/d) 3 times a week with
lower and slower than that of levamisole combined with regular blood test monitoring.
low dose prednisone. Nevertheless, levamisole monothe- In conclusion, we report that levamisole monotherapy is
rapy was shown to be effective for the treatment of OLP. effective for treating OLP patients who are unable to use
Therefore, levamisole monotherapy can be recommended steroids and who had no response to conventional treat-
for those OLP patients who are unable to take steroids. ment.
The number of patients who showed no response was 3.
Interestingly, they had a short duration of disease (3, 6 and
REFERENCES
6 months, respectively). The mean disease duration of the
responders was 26.8 months and they had undergone 1. Wilson E. On lichen planus. J Cutan Med Dis Skin 1869;
many treatment trials with no response. At this point, we 3:117-132.
thought that levamisole monotherapy was a first line drug 2. Eisen D. The clinical features, malignant potential, and
for treating these chronic OLP patients. systemic associations of oral lichen planus: a study of 723
Vol. 21, No. 3, 2009 253
TH Won, et al
patients. J Am Acad Dermatol 2002;46:207-214. with carcinoma. Cancer 1980;46:2185-2194.
3. Carrozzo M, Gandolfo S. The management of oral lichen 19. Redondo JM, Lopez-Guerrero JA, Fresno M. Potentiation of
planus. Oral Dis 1999;5:196-205. interleukin-2 activity by levamisole and imidazole. Immunol
4. Eisen D, Griffiths CE, Ellis CN, Nickoloff BJ, Voorhees JJ. Lett 1987;14:111-116.
Cyclosporin wash for oral lichen planus. Lancet 1990;335: 20. Amery WK, Bruynseels JP. Levamisole, the story and the
535-536. lessons. Int J Immunopharmacol 1992;14:481-486.
5. Eisen D, Ellis CN, Duell EA, Griffiths CE, Voorhees JJ. Effect 21. Janssen PA. The levamisole story. Prog Drug Res 1976;20:
of topical cyclosporine rinse on oral lichen planus. A 347-383.
double-blind analysis. N Engl J Med 1990;323:290-294. 22. Cho NJ, Choi DY, Son SJ. Therapeutic effect of levamisole in
6. Eisen D, Ellis CN. Topical cyclosporine for oral mucosal recurrent aphthous stomatitis. Korean J Dermatol 1979;17:
disorders. J Am Acad Dermatol 1990;23:1259-1263. 389-396.
7. Aufdemorte TB, De Villez RL, Gieseker DR. Griseofulvin in 23. Scheithauer W, Kornek GV, Marczell A, Karner J, Salem G,
the treatment of three cases of oral erosive lichen planus. Greiner R, et al. Combined intravenous and intraperitoneal
Oral Surg Oral Med Oral Pathol 1983;55:459-462. chemotherapy with fluorouracil+leucovorin vs fluorouracil
8. Massa MC, Rogers RS 3rd. Griseofulvin therapy of lichen +levamisole for adjuvant therapy of resected colon car-
planus. Acta Derm Venereol 1981;61:547-550. cinoma. Br J Cancer 1998;77:1349-1354.
9. Sehgal VN, Abraham GJ, Malik GB. Griseofulvin therapy in 24. Sany J. Immunological treatment of rheumatoid arthritis. Clin
lichen planus. A double-blind controlled trial. Br J Dermatol Exp Rheumatol 1990;8 Suppl 5:81-88.
1972;87:383-385. 25. Parsad D, Saini R, Negi KS. Comparison of combination of
10. Kaliakatsou F, Hodgson TA, Lewsey JD, Hegarty AM, Mur- cimetidine and levamisole with cimetidine alone in the
phy AG, Porter SR. Management of recalcitrant ulcerative treatment of recalcitrant warts. Australas J Dermatol 1999;
oral lichen planus with topical tacrolimus. J Am Acad 40:93-95.
Dermatol 2002;46:35-41. 26. Amer M, Tosson Z, Soliman A, Selim AG, Salem A, al-
11. Thomson MA, Hamburger J, Stewart DG, Lewis HM. Gendy AA. Verrucae treated by levamisole. Int J Dermatol
Treatment of erosive oral lichen planus with topical tacro- 1991;30:738-740.
limus. J Dermatolog Treat 2004;15:308-314. 27. Agarwal S, Ramam M, Sharma VK, Khandpur S, Pal H,
12. Byrd JA, Davis MD, Bruce AJ, Drage LA, Rogers RS 3rd. Pandey RM. A randomized placebo-controlled double-blind
Response of oral lichen planus to topical tacrolimus in 37 study of levamisole in the treatment of limited and slowly
patients. Arch Dermatol 2004;140:1508-1512. spreading vitiligo. Br J Dermatol 2005;153:163-166.
13. Sloberg K, Hersle K, Mobacken H, Thilander H. Topical 28. Pasricha JS, Khera V. Effect of prolonged treatment with
tretinoin therapy and oral lichen planus. Arch Dermatol levamisole on vitiligo with limited and slow-spreading disea-
1979;115:716-718. se. Int J Dermatol 1994;33:584-587.
14. Lu SY, Chen WJ, Eng HL. Dramatic response to levamisole 29. Rovensky J, Cebecauer L, Zitnan D, Lukac J, Ferencik M.
and low-dose prednisolone in 23 patients with oral lichen Levamisole treatment of systemic lupus erythematosus. Art-
planus: a 6-year prospective follow-up study. Oral Surg Oral hritis Rheum 1982;25:470-471.
Med Oral Pathol Oral Radiol Endod 1995;80:705-709. 30. Renoux G, Renoux M, Teller MN, McMahon S, Guillaumin
15. Lu SY, Chen WJ, Eng HL. Response to levamisole and JM. Potentiation of T-cell mediated immunity by levamisole.
low-dose prednisolone in 41 patients with chronic oral Clin Exp Immunol 1976;25:288-296.
ulcers: a 3-year open clinical trial and follow-up study. Oral 31. Kim HK, Jung YB, Lee EW. Clinical application of D-penicil-
Surg Oral Med Oral Pathol Oral Radiol Endod 1998; lamine and levamisole in rheumatoid arthritis. J Korean
86:438-445. Orthop Assoc 1983;18:81-88.
16. Sun A, Chiang CP, Chiou PS, Wang JT, Liu BY, Wu YC. 32. Rosenthal M, Trabert U, Muller W. The effect of levamisole
Immunomodulation by levamisole in patients with recurrent on peripheral blood lymphocyte subpopulations in patients
aphthous ulcers or oral lichen planus. J Oral Pathol Med with rheumatoid arthritis and ankylosing spondylitis. Clin
1994;23:172-177. Exp Immunol 1976;25:493-496.
17. Sun A, Wang JT, Chia JS, Chiang CP. Serum interleukin-8 33. Sany J. A review of the effects of levamisole on erythrocyte
level is a more sensitive marker than serum interleukin-6 sedimentation rate, acute phase proteins, and anemia. J
level in monitoring the disease activity of oral lichen planus. Rheumatol Suppl 1978;4:43-47.
Br J Dermatol 2005;152:1187-1192. 34. Scott J, Dieppe PA, Huskisson EC. Continuous and inter-
18. Lewinski UH, Mavligit GM, Hersh EM. Cellular immune mittent levamisole. A controlled trial. Ann Rheum Dis 1978;
modulation after a single high dose of Levamisole in patients 37:259-261.
254 Ann Dermatol
You might also like
- Chapter 4: PsychopharmacologyDocument37 pagesChapter 4: PsychopharmacologyGummyCola100% (2)
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Anti Arrhythmia DrugsDocument3 pagesAnti Arrhythmia DrugsFarid ZainuddinNo ratings yet
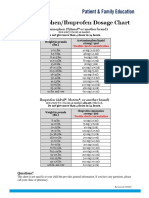
- Acetaminophen Ibuprofen Dosage ChartDocument1 pageAcetaminophen Ibuprofen Dosage ChartByron DubowNo ratings yet
- Pharma Mcq'sDocument47 pagesPharma Mcq'ssimi yNo ratings yet
- Skin Disorders Training For EmployeesDocument24 pagesSkin Disorders Training For EmployeesEry BureniNo ratings yet
- Lichen Planus PDFDocument5 pagesLichen Planus PDFRobins DhakalNo ratings yet
- Drug Treatment of Oral Sub Mucous Fibrosis - A Review PDFDocument3 pagesDrug Treatment of Oral Sub Mucous Fibrosis - A Review PDFAnamika AttrishiNo ratings yet
- Lecture 8 - Drug ComputationsDocument135 pagesLecture 8 - Drug ComputationsAlyssa Audrey CaoagasNo ratings yet
- LDN Letter To Give To Your DoctorDocument3 pagesLDN Letter To Give To Your DoctorbktangoNo ratings yet
- Metronidazole Drug StudyDocument1 pageMetronidazole Drug StudydwightciderNo ratings yet
- Jop 12583 Rev EVcurrentprotocolsDocument7 pagesJop 12583 Rev EVcurrentprotocolsali baridiNo ratings yet
- Botulinum Toxin As Adjunctive Therapy in RefractoryDocument5 pagesBotulinum Toxin As Adjunctive Therapy in RefractoryadithyaNo ratings yet
- Oral Lichen PlanusDocument7 pagesOral Lichen Planusdrgurpal74100% (1)
- Isotretinoin Treatment For Folliculitis Decalvans: A Retrospective Case-Series StudyDocument4 pagesIsotretinoin Treatment For Folliculitis Decalvans: A Retrospective Case-Series Studyabdulmunim hanyNo ratings yet
- 1 s2.0 S1550830716301665 MainDocument7 pages1 s2.0 S1550830716301665 MainAwadAyoubNo ratings yet
- 1 s2.0 S1550830716301665 MainDocument7 pages1 s2.0 S1550830716301665 MainAwadAyoubNo ratings yet
- Management of Oral Lichen Planus: Review ArticleDocument5 pagesManagement of Oral Lichen Planus: Review ArticlebunapiNo ratings yet
- Current Treatments For Alopecia Areata: ReviewDocument3 pagesCurrent Treatments For Alopecia Areata: ReviewditaNo ratings yet
- Dry Needling in Lateral Epicondylitis A Prospective EBP PDFDocument5 pagesDry Needling in Lateral Epicondylitis A Prospective EBP PDFDanielle Denice LacabaNo ratings yet
- Comparing Ophthalmic Medications' Side EffectsDocument9 pagesComparing Ophthalmic Medications' Side Effectsflavio1No ratings yet
- Rhinitis, sinusitis, and ocular diseases phototherapyDocument7 pagesRhinitis, sinusitis, and ocular diseases phototherapyJulian LeeNo ratings yet
- Hyperuricemia and Gout - A New Treatment OptionDocument39 pagesHyperuricemia and Gout - A New Treatment OptionDinda YusditiraNo ratings yet
- NtoulaEvangeliaDocument6 pagesNtoulaEvangeliaSashaNo ratings yet
- Afamelanotide With NBUVB in VitiligoDocument3 pagesAfamelanotide With NBUVB in VitiligoCHONG WEI SHENGNo ratings yet
- Etr80003 994 995Document2 pagesEtr80003 994 995Karen Mae PadillaNo ratings yet
- Efficacy of Purslane in Treatment of Oral Lichen PlanusDocument5 pagesEfficacy of Purslane in Treatment of Oral Lichen PlanusYigal Ben YzkNo ratings yet
- Taurus LiteraturDocument10 pagesTaurus LiteraturElysabet aristaNo ratings yet
- Nail Lichen PlanusDocument2 pagesNail Lichen Planussri karuniaNo ratings yet
- Efficacy and Safety of Botulinum Toxin Type A A Product For The Treatment of Moderate To Severe Glabellar LinesDocument8 pagesEfficacy and Safety of Botulinum Toxin Type A A Product For The Treatment of Moderate To Severe Glabellar LinesDenisse ZayasNo ratings yet
- IndianJOphthalmol54168-4547556 123755Document2 pagesIndianJOphthalmol54168-4547556 123755Gusti Ari SetyawanNo ratings yet
- Treatment - of - Perioral - Dystonia - With - Botu20160214 25964 1k8rnph With Cover Page v2Document7 pagesTreatment - of - Perioral - Dystonia - With - Botu20160214 25964 1k8rnph With Cover Page v2runit nangaliaNo ratings yet
- Jurnal InternasionalDocument8 pagesJurnal Internasionalmonik noshirmaNo ratings yet
- Tbilisi Botox PaperDocument4 pagesTbilisi Botox PaperJP OmerNo ratings yet
- Tadalafil 12 mesesOKInglesDocument7 pagesTadalafil 12 mesesOKInglesRaul JimenezNo ratings yet
- HTTP WWW - Sciencedirect.com Science Ob MImg& Imagekey B6WP1-4HK01J7-7-1& Cdi 6977& User 8187385& OrigDocument4 pagesHTTP WWW - Sciencedirect.com Science Ob MImg& Imagekey B6WP1-4HK01J7-7-1& Cdi 6977& User 8187385& OrigBimalKrishnaNo ratings yet
- International Journal of Scientific Research: Dental ScienceDocument3 pagesInternational Journal of Scientific Research: Dental ScienceCyrish MelchorNo ratings yet
- Nasal Polyposis Medical Management StudyDocument38 pagesNasal Polyposis Medical Management StudychreezoNo ratings yet
- 1549 Full-2Document7 pages1549 Full-2balqiswulanNo ratings yet
- Menejemen Kronik Uveitis Anterior RekurenDocument6 pagesMenejemen Kronik Uveitis Anterior RekurenLuthfan HakimNo ratings yet
- Factors Associated With Different Responses To Periodontal TherapyDocument10 pagesFactors Associated With Different Responses To Periodontal TherapyAna OrtizNo ratings yet
- Oral Lichen Planus An Enigma With Limited Treatment OptionsDocument4 pagesOral Lichen Planus An Enigma With Limited Treatment OptionsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 9804693anestesicos LocalesDocument10 pages9804693anestesicos LocalesrichabertNo ratings yet
- E187 FullDocument7 pagesE187 FullVisaraNo ratings yet
- Ad 27 446Document4 pagesAd 27 446Satriadwykiyprasetya ThiodwkiyNo ratings yet
- Comparison of Monotherapy and Multitherapy Effectiveness in Glaucomatous Patient at Panembahan Senopati General Hospital in 2013Document21 pagesComparison of Monotherapy and Multitherapy Effectiveness in Glaucomatous Patient at Panembahan Senopati General Hospital in 2013Pratifi NurleiliNo ratings yet
- Jurnal 1Document6 pagesJurnal 1AbduNo ratings yet
- Efficacy of Oral Lycopene in The Treatment of Oral LeukoplakiaDocument6 pagesEfficacy of Oral Lycopene in The Treatment of Oral Leukoplakia2211801733No ratings yet
- Topical Propranolol Improves Epistaxis in PatientsDocument4 pagesTopical Propranolol Improves Epistaxis in PatientskasandraharahapNo ratings yet
- Gniadeckietal 2015 BritishjournalofdermatologyDocument9 pagesGniadeckietal 2015 BritishjournalofdermatologyChristman SihiteNo ratings yet
- Clinical StudyDocument9 pagesClinical StudyNurul Dwi LestariNo ratings yet
- Evidence Based Medicine - CONSORT & AppraisalDocument52 pagesEvidence Based Medicine - CONSORT & AppraisalNurul Aulia AbdullahNo ratings yet
- JAK Inhibitor Baricitinib in The Treatment of Oral Lichen Planus A Case ReportDocument4 pagesJAK Inhibitor Baricitinib in The Treatment of Oral Lichen Planus A Case ReportAthenaeum Scientific PublishersNo ratings yet
- JSD 8 19Document3 pagesJSD 8 19Oke Soe MoeNo ratings yet
- Combined oral pulse and topical corticosteroid therapy shows long-lasting results in severe childhood alopecia areataDocument10 pagesCombined oral pulse and topical corticosteroid therapy shows long-lasting results in severe childhood alopecia areataVilt VilNo ratings yet
- Comparison of Sublingual Immunotherapy in Patients With Allergic Rhinitis Sensitive To House Dust Mites in KoreaDocument8 pagesComparison of Sublingual Immunotherapy in Patients With Allergic Rhinitis Sensitive To House Dust Mites in Koreafm_askaNo ratings yet
- Clinical and Radiological Outcomes of Infantile Hemangioma Treated With Oral Propranolol: A Long-Term Follow-Up StudyDocument7 pagesClinical and Radiological Outcomes of Infantile Hemangioma Treated With Oral Propranolol: A Long-Term Follow-Up StudyS FznsNo ratings yet
- IndianJOphthalmol6791400-3383915 092359Document5 pagesIndianJOphthalmol6791400-3383915 092359diancahyaNo ratings yet
- Double Blind Randomized Placebo-Controlled Trial To Evaluate The Efficacy and Safety of Short-Course Low Dose Oral Prednisolone in Pityriasis RoseaDocument10 pagesDouble Blind Randomized Placebo-Controlled Trial To Evaluate The Efficacy and Safety of Short-Course Low Dose Oral Prednisolone in Pityriasis RoseaSalsabila Munirah AmirNo ratings yet
- Universitas Indonesia: U. Weber, M. Krammel, S. Linke, T. Hamp, T. Stimpfl, B. Reiter, W. PlӧchlDocument8 pagesUniversitas Indonesia: U. Weber, M. Krammel, S. Linke, T. Hamp, T. Stimpfl, B. Reiter, W. PlӧchlgoldenNo ratings yet
- Todentj 5 146Document4 pagesTodentj 5 146Mbuli AndriyaniNo ratings yet
- Topical Propranolol Improves Epistaxis Control in Hereditary Hemorrhagic Telangiectasia (HHT) : A Randomized Double-Blind Placebo-Controlled TrialDocument12 pagesTopical Propranolol Improves Epistaxis Control in Hereditary Hemorrhagic Telangiectasia (HHT) : A Randomized Double-Blind Placebo-Controlled TrialAmaliah HakimNo ratings yet
- Biib059 - 2019Document1 pageBiib059 - 2019Marilena TarcaNo ratings yet
- Us Ulan Proposal 6Document6 pagesUs Ulan Proposal 6Civic TypeRNo ratings yet
- Thyroid Eye Disease PresentationDocument39 pagesThyroid Eye Disease PresentationyoadhajyahyaNo ratings yet
- Allergology InternationalDocument9 pagesAllergology Internationalvijay dagdiNo ratings yet
- A Comparative Study of Topical Betaxalol and Timolol For Their Efficacy and Side EffectsDocument4 pagesA Comparative Study of Topical Betaxalol and Timolol For Their Efficacy and Side EffectsInternational Journal of Clinical and Biomedical Research (IJCBR)No ratings yet
- Effectiveness of Micronutrients and Physiotherapy in The Management of Oral Submucous Fibrosis PDFDocument5 pagesEffectiveness of Micronutrients and Physiotherapy in The Management of Oral Submucous Fibrosis PDFNia LieantoNo ratings yet
- HTTPSWWW - Derm-Hokudai - JP ... PDF6 Treatment of Skin Diseases PDFDocument4 pagesHTTPSWWW - Derm-Hokudai - JP ... PDF6 Treatment of Skin Diseases PDFjalalfaizNo ratings yet
- Acneiform Eruption Secondary To Epidermal Growth Factor Receptor (EGFR) and MEK InhibitorsDocument14 pagesAcneiform Eruption Secondary To Epidermal Growth Factor Receptor (EGFR) and MEK InhibitorsjalalfaizNo ratings yet
- Acquired C1 Inhibitor Deficiencymanagement and PrognosisDocument14 pagesAcquired C1 Inhibitor Deficiencymanagement and PrognosisjalalfaizNo ratings yet
- ACE Inhibitor-Induced AngioedemaDocument14 pagesACE Inhibitor-Induced AngioedemajalalfaizNo ratings yet
- Httpsapps - Who.int handlePDFEpidemiology and Management of Common Skin Diseases - World Health Organization PDFDocument62 pagesHttpsapps - Who.int handlePDFEpidemiology and Management of Common Skin Diseases - World Health Organization PDFjalalfaizNo ratings yet
- LP ManagementDocument4 pagesLP ManagementjalalfaizNo ratings yet
- Skin 123 PDFDocument16 pagesSkin 123 PDFFasiha MushadiNo ratings yet
- Acne Keloidalis NuchaeDocument16 pagesAcne Keloidalis NuchaejalalfaizNo ratings yet
- Lichen Planus and Its Management An Update and Observation Ijced 18 001Document5 pagesLichen Planus and Its Management An Update and Observation Ijced 18 001jalalfaizNo ratings yet
- LP ManagementDocument4 pagesLP ManagementjalalfaizNo ratings yet
- Common Skin Conditions in WrestlingDocument31 pagesCommon Skin Conditions in WrestlingjalalfaizNo ratings yet
- Topical Therapy of LPDocument11 pagesTopical Therapy of LPjalalfaizNo ratings yet
- Topical Therapy of LPDocument11 pagesTopical Therapy of LPjalalfaizNo ratings yet
- Pemphigus: An Autoimmune Skin DisorderDocument7 pagesPemphigus: An Autoimmune Skin DisorderjalalfaizNo ratings yet
- WartsDocument5 pagesWartsjalalfaizNo ratings yet
- Lichen Planus: Santa Clara Medical Center, Department of Dermatology #472Document2 pagesLichen Planus: Santa Clara Medical Center, Department of Dermatology #472jalalfaizNo ratings yet
- VitiligoDocument4 pagesVitiligojalalfaizNo ratings yet
- Pityriasis RoseaDocument2 pagesPityriasis RoseajalalfaizNo ratings yet
- PemphigoidDocument4 pagesPemphigoidjalalfaizNo ratings yet
- Acne and Acneiform DermatosesDocument5 pagesAcne and Acneiform DermatosesjalalfaizNo ratings yet
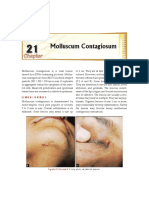
- 21 Molluscum Contagiosum PDFDocument2 pages21 Molluscum Contagiosum PDFjalalfaizNo ratings yet
- Molluscum ContagiosumDocument2 pagesMolluscum ContagiosumjalalfaizNo ratings yet
- Deep Mycotic InfectionDocument5 pagesDeep Mycotic InfectionjalalfaizNo ratings yet
- Herpes SimplexDocument5 pagesHerpes SimplexjalalfaizNo ratings yet
- UrticariaDocument5 pagesUrticariajalalfaizNo ratings yet
- Cutaneous TuberculosisDocument10 pagesCutaneous TuberculosisjalalfaizNo ratings yet
- Candidiasis: A Concise Guide to Diagnosis and TreatmentDocument4 pagesCandidiasis: A Concise Guide to Diagnosis and TreatmentjalalfaizNo ratings yet
- Behcet TratamentoDocument32 pagesBehcet TratamentoEliseu AmaralNo ratings yet
- Therapeutics in Endodontics: DR Mohamed RabieDocument75 pagesTherapeutics in Endodontics: DR Mohamed RabieAbdelrahman GalalNo ratings yet
- PHARMA Revised + Extra QsDocument51 pagesPHARMA Revised + Extra Qsdoaa naieemNo ratings yet
- Session 1 - GCP For BE PDFDocument24 pagesSession 1 - GCP For BE PDFsunpharmaNo ratings yet
- Treatment Ofpostherpetic Neuralgia - Neurology.2018Document8 pagesTreatment Ofpostherpetic Neuralgia - Neurology.2018Anonymous iWc8uZNo ratings yet
- Exam MarchDocument2 pagesExam MarchkathlynmangasiNo ratings yet
- Inventory Available 5/3/2019Document10 pagesInventory Available 5/3/2019Isräel ZabalaNo ratings yet
- Letter To FDA On Eua For Kids Vaccines - 08.17.21Document7 pagesLetter To FDA On Eua For Kids Vaccines - 08.17.21Noyb NalNo ratings yet
- Case Study # 3 UNRS 314 Name - Number - Ruptured AppendixDocument2 pagesCase Study # 3 UNRS 314 Name - Number - Ruptured AppendixSapiah RamanNo ratings yet
- COVID Vaccination Certificate for Jitendra MahajanDocument1 pageCOVID Vaccination Certificate for Jitendra MahajansumandeepNo ratings yet
- TABLE 134 - Antipsychotic MedicationsDocument2 pagesTABLE 134 - Antipsychotic MedicationsDragutin PetrićNo ratings yet
- SP Sendo KF 122Document5 pagesSP Sendo KF 122nurhadri azmiNo ratings yet
- 1e3rd - Medication NotesDocument35 pages1e3rd - Medication NotesKen LaguiabNo ratings yet
- P2221554 TreDocument32 pagesP2221554 Treluis alberto silva caicedoNo ratings yet
- Post-Operative Pain Management.: Murtaza Asif Ali Queen's Hospital Burton Upon TrentDocument33 pagesPost-Operative Pain Management.: Murtaza Asif Ali Queen's Hospital Burton Upon TrentM Asif AliNo ratings yet
- Drug Master FileDocument19 pagesDrug Master FileRenaldy NongbetNo ratings yet
- Teratogenic DrugsDocument8 pagesTeratogenic DrugsMudrekaNo ratings yet
- SHC Obesity Dosing GuideDocument10 pagesSHC Obesity Dosing GuideAnonymous 9dVZCnTXSNo ratings yet
- No 7, MIT AnticholinesterasesDocument12 pagesNo 7, MIT Anticholinesteraseshenry abuyaNo ratings yet
- Venofer Guidelines 2011 PDFDocument2 pagesVenofer Guidelines 2011 PDFBudi Iman SantosoNo ratings yet
- PRICE LIST PT PUTRA PERDANADocument25 pagesPRICE LIST PT PUTRA PERDANAamaliiaNo ratings yet
- Microbiology CatalogueDocument40 pagesMicrobiology CatalogueHari YantoNo ratings yet
- ELI LILY Company Case StudyDocument15 pagesELI LILY Company Case Studykomaltagra100% (1)