Professional Documents
Culture Documents
Anti Coagulatants: Presented By:-Mr - Gorishankar Nursing Tutor (Tantia University)
Uploaded by
yogesh kumar0 ratings0% found this document useful (0 votes)
21 views10 pagesAnticoagulants are the substances which prevents blood clotting process
Original Title
Anti Coagulants
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAnticoagulants are the substances which prevents blood clotting process
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
21 views10 pagesAnti Coagulatants: Presented By:-Mr - Gorishankar Nursing Tutor (Tantia University)
Uploaded by
yogesh kumarAnticoagulants are the substances which prevents blood clotting process
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 10
Anti coagulatants
Presented by:- Mr.Gorishankar
Nursing Tutor{tantia university}
Classification
1. Anticoagulants used in-vivo:
a. Fast acting: Heparin,
heparinoids-heparan sulphate, dextran
sulphate.
b. Slow acting: Oral anticoagulants,
warfarin, dicoumarol,
nicoumalone,phenindione.
2. Anticoagulants used in-vitro:
Heparin, citrates, oxalates and sodium
edetate.
Types
1. Oral Anticoagulants: Oral anticoagulants inhibit synthesis of clotting factors
VII, IX and X thereby, clotting is inhibited.
Drugs commonly used:
a.Warfarin sodium
b. Dicoumarol
Uses:
a.Mainly used to slow down or prevent extension of blood clots.
b.Use caution while giving any medication by IM route.
c.Monitor for hematuria, epistaxis, ecchymosis and haematoma.
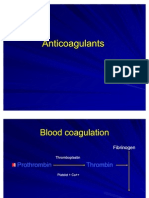
2.Parenteral anticoagulants: Heparin acts as an in-vitro anticoagulant by
accelerating the rate of antithrombin
3.(ATII )binding to thrombin (thrombin is required for converting fibrinogen to
fibrin). It is usefulin all those conditions where oral anticoagulants are used. It
is specifically used for short-termemergency treatment such as during
hemodialysis, myocardial infarction and after CABG surgery.
MODE OF ACTION
Heparin is found in the mast cells of the liver, lungs
and intestinal mucosa. Heparin is the strongestacid in
the body. Heparin is a powerful anticoagulant that acts
instantaneously both vivo and vitro.Heparin activates
plasma antithrombin, which binds to the clotting
factors and inactivate them.Heparin is not effective
orally. It is given by IV or SC route. It should not be
given IM because it maycause haematomas. When given
intravenously the onset of action is immediate,
reaches peak in 510 minutes and clotting time returns
to normal in 2-4 hrs. Treatment is monitored by the
PartialThromboplastin Time (PTT) (preferable) or
clotting time. Heparin is metabolized by heparinase in
the liver
Indication
Venous thrombosis and pulmonary embolisms: Anticoagulants prevent
extension of thrombus and recurrence of embolism.
Postoperative, post-stroke patients, bedridden patients, anticoagulants
prevent venous thrombosis amd pulmonary embolism in such diseases
Rheumatic valvular disease- anticoagulants prevent embolism.
Unstable angina - heparin reduces the risk of myocardial infarction in
patients with unstable angina.
Vascular Surgery, artificial heart valves and haemodialysis anticogulants
prevent thromboembolism.
Thanku for attention
You might also like
- Anticoagulants 161120143945Document29 pagesAnticoagulants 161120143945Roshan SahuNo ratings yet
- Peripheral Vascular DiseaseDocument53 pagesPeripheral Vascular DiseaseShenbagam Mahalingam100% (1)
- PHM - Hematologic DrugsDocument3 pagesPHM - Hematologic DrugsJeanne Rodiño100% (3)
- Pharmacology - Hematologic DrugsDocument51 pagesPharmacology - Hematologic DrugsBenjamin Joel Breboneria100% (1)
- AnticoagulantsDocument19 pagesAnticoagulantsOsama ZbedaNo ratings yet
- Drugs Used in Disorders of CoagulationDocument61 pagesDrugs Used in Disorders of CoagulationDUEÑAS, MARIELNo ratings yet
- A Drug Study On: HeparinDocument8 pagesA Drug Study On: HeparinRaijenne VersolaNo ratings yet
- Concept MapDocument4 pagesConcept MapDud AccNo ratings yet
- Anticoagulant, Fibrinolytic, and Antiplatelet DrugsDocument22 pagesAnticoagulant, Fibrinolytic, and Antiplatelet DrugsVera Waty100% (1)
- Anticoagulant PresentationDocument29 pagesAnticoagulant Presentationrozha100% (2)
- Antiplatelet, Anticoagulant and Thrombolytic Agents: Basic Pharmacology Block Pdnt/Pmed - PMSC/PPHR - 213Document30 pagesAntiplatelet, Anticoagulant and Thrombolytic Agents: Basic Pharmacology Block Pdnt/Pmed - PMSC/PPHR - 213JedoNo ratings yet
- Anticoagulants ParamedDocument20 pagesAnticoagulants ParamedManikanta GupthaNo ratings yet
- Deep Vein ThrombosisDocument13 pagesDeep Vein Thrombosisusmle prepNo ratings yet
- AnticoagulantDocument34 pagesAnticoagulantAslam Baltee100% (1)
- Crash Cart Drugs: A Review of Medications Used in Cardiac ArrestDocument23 pagesCrash Cart Drugs: A Review of Medications Used in Cardiac ArrestKristiina MakinenNo ratings yet
- E - Cart DrugsDocument18 pagesE - Cart Drugs'SheenMarkReal'100% (2)
- Anticoagulants: Dr. Hassan Mohamed EnowDocument37 pagesAnticoagulants: Dr. Hassan Mohamed EnowFatimaNo ratings yet
- Principles of Antiplatelet Therapy: DR Htet Htet Htethtet@Imu - Edu.MyDocument36 pagesPrinciples of Antiplatelet Therapy: DR Htet Htet Htethtet@Imu - Edu.MyAbby Liew100% (1)
- Anticoagulants May BeDocument5 pagesAnticoagulants May BeAmmar magdyNo ratings yet
- Blood NursingDocument34 pagesBlood NursingManikanta GupthaNo ratings yet
- Blood Pharmacology by Dr. Mayur Sayta M 910444Document21 pagesBlood Pharmacology by Dr. Mayur Sayta M 910444funzz100% (1)
- Anticoagulants and Antiplatelet Drugs: Mechanisms and Clinical UsesDocument25 pagesAnticoagulants and Antiplatelet Drugs: Mechanisms and Clinical UsesIdrissa John Sebeh ContehNo ratings yet
- Drugs Used To Affect in Blood Coagulation: Prajogo WibowoDocument44 pagesDrugs Used To Affect in Blood Coagulation: Prajogo WibowoIda Bagus Putu SwabawaNo ratings yet
- 9- Anticoagulant Drugs (Final)Document17 pages9- Anticoagulant Drugs (Final)wllmaanka4No ratings yet
- AnticoagulantsDocument8 pagesAnticoagulantsRobert L G MabongaNo ratings yet
- Cardio MedsDocument29 pagesCardio Medsjemfortuna9No ratings yet
- List of AnticoagulantsDocument9 pagesList of Anticoagulantschristianz39100% (1)
- Antiplatelets Anticoagulant Drugs 1668083619Document12 pagesAntiplatelets Anticoagulant Drugs 1668083619Nehal ElnagarNo ratings yet
- ANTICOAGULATSDocument18 pagesANTICOAGULATSRose Lyn Camarista VelascoNo ratings yet
- Pharmacology II: Treatments for Blood Disorders and InflammationDocument61 pagesPharmacology II: Treatments for Blood Disorders and InflammationDiane BanuaNo ratings yet
- Abram Study NotesDocument6 pagesAbram Study Notesteeman2No ratings yet
- AnticoagulantsDocument3 pagesAnticoagulantsKarthik SubramaniamNo ratings yet
- AntiarrhythmiaDocument29 pagesAntiarrhythmiaDRx Raju ChandranNo ratings yet
- Presentation. 111tom AbDocument20 pagesPresentation. 111tom AbTemesgenNo ratings yet
- Anticoagulationguidelines 11Document14 pagesAnticoagulationguidelines 11q4zvck4bpbNo ratings yet
- Cardiovascular SystemDocument4 pagesCardiovascular SystemRegineCuasSulibNo ratings yet
- Farmakoterapi AntikoagulasiDocument20 pagesFarmakoterapi AntikoagulasiRirin AptNo ratings yet
- Drugs Affecting Blood CoagulationDocument51 pagesDrugs Affecting Blood CoagulationMoxie Macado100% (1)
- Pharmacology CardiovascularDocument86 pagesPharmacology Cardiovascularamasoud96 amasoud96No ratings yet
- Neuraxial Blockade and AnticoagulantsDocument69 pagesNeuraxial Blockade and Anticoagulantskamel6No ratings yet
- CAD Treatment with Anticoagulants, Thrombolytics & AntiplateletsDocument4 pagesCAD Treatment with Anticoagulants, Thrombolytics & AntiplateletsAbdullahIchsanNo ratings yet
- Anticoagulatio N Asra Guidelines: Sravya VemuriDocument62 pagesAnticoagulatio N Asra Guidelines: Sravya VemuriSiva Prasad AspNo ratings yet
- Amlodipine, Vit.b Complex, CombiventDocument6 pagesAmlodipine, Vit.b Complex, CombiventErickson Caisido GarciaNo ratings yet
- UFH LMWH Fonda - 06september2020Document7 pagesUFH LMWH Fonda - 06september2020gabrimarteNo ratings yet
- Vasodilator and Anticoagulant Agents SummaryDocument23 pagesVasodilator and Anticoagulant Agents Summarymonyet65No ratings yet
- ReviewerDocument20 pagesReviewerKC PalattaoNo ratings yet
- ASRA Guidelines on Neuraxial Blockade and AnticoagulantsDocument66 pagesASRA Guidelines on Neuraxial Blockade and AnticoagulantsAshiyan IrfanNo ratings yet
- M MMM MMDocument10 pagesM MMM MMMustafa Al-Nua'aimyNo ratings yet
- Pharmacology Affecting CoagulationDocument19 pagesPharmacology Affecting CoagulationCurtney PedriaNo ratings yet
- John Hommer E. Dy, MD.: Diplomate in Internal MedicineDocument56 pagesJohn Hommer E. Dy, MD.: Diplomate in Internal MedicinehommercuteNo ratings yet
- Principles of An-Tiplatelet Therapy: DR Htet Htet Htethtet@Imu - Edu.MyDocument36 pagesPrinciples of An-Tiplatelet Therapy: DR Htet Htet Htethtet@Imu - Edu.MyAbby LiewNo ratings yet
- The Pharmacology of AntithromboticsDocument14 pagesThe Pharmacology of AntithromboticsanaNo ratings yet
- AnticoagulatsDocument52 pagesAnticoagulatsanaya khan StudentNo ratings yet
- Blok 5 Hemostatic DrugDocument39 pagesBlok 5 Hemostatic DrugPutri HusnanNo ratings yet
- Blood - Anticoagulants: Ravi Sankar Venuturumilli, MD Global Hospitals, HyderabadDocument30 pagesBlood - Anticoagulants: Ravi Sankar Venuturumilli, MD Global Hospitals, HyderabadDrRavisankar VenuturumilliNo ratings yet
- A Drug Study On EpinephrineDocument7 pagesA Drug Study On EpinephrineMaesy Garcia LorenaNo ratings yet
- Anticoagulants:: DefinitionDocument6 pagesAnticoagulants:: DefinitionMunaza FarooqNo ratings yet
- Anti CoagulantsDocument37 pagesAnti CoagulantsMaria khurshidNo ratings yet
- Pharmacology and Toxicology - Anticoagulants - Medical LibraryDocument8 pagesPharmacology and Toxicology - Anticoagulants - Medical Libraryjean PiedraNo ratings yet
- Haematology DrugsDocument17 pagesHaematology DrugsParyNo ratings yet
- Summary of Product Characteristics, Labelling and Package LeafletDocument29 pagesSummary of Product Characteristics, Labelling and Package LeafletImmanuel PurbaNo ratings yet
- PIIS1542356523003166Document14 pagesPIIS1542356523003166josephNo ratings yet
- Perioperative Medication Management - UpToDateDocument51 pagesPerioperative Medication Management - UpToDateAlex Kulia100% (1)
- Warfarin therapy monitoring and managementDocument1 pageWarfarin therapy monitoring and managementmtbartNo ratings yet
- Indications and Risks of Splenectomy ExplainedDocument21 pagesIndications and Risks of Splenectomy ExplainedMark MakaryNo ratings yet
- Venous & Lymphatics, Dr. AngsaDocument40 pagesVenous & Lymphatics, Dr. AngsaKailash KhatriNo ratings yet
- Contoh Formulir Rekam Medis Rawat InapDocument11 pagesContoh Formulir Rekam Medis Rawat InapResti ayuNo ratings yet
- Drug Monograph ExampleDocument6 pagesDrug Monograph ExampleAaltiyaNo ratings yet
- Pathophysiology of Venous ThromboembolismDocument8 pagesPathophysiology of Venous ThromboembolismKate RodasNo ratings yet
- Pulmonary Embolism: Risks, Symptoms & DiagnosisDocument39 pagesPulmonary Embolism: Risks, Symptoms & DiagnosisAsmaa ahmedNo ratings yet
- Organisational Structure StudyDocument46 pagesOrganisational Structure StudyChing SantiagoNo ratings yet
- CG144 Guideline (Updated) 20151125Document25 pagesCG144 Guideline (Updated) 20151125MariaNo ratings yet
- SSI and ERAS, Complications of TAHBSODocument18 pagesSSI and ERAS, Complications of TAHBSOCheska MalubayNo ratings yet
- Contemporary Management of Major Haemorrhage in Critical CareDocument13 pagesContemporary Management of Major Haemorrhage in Critical CareYo MeNo ratings yet
- GS 201-250Document19 pagesGS 201-250Sara Abdul RahmanNo ratings yet
- Kepler 2018Document12 pagesKepler 2018Dede NovHyNo ratings yet
- Reference For Assignment 2Document2 pagesReference For Assignment 2chrisNo ratings yet
- BIOEN 345: Failure Analysis of Physiology: Lecture 4 May 4, 2020: Vessel PathologiesDocument45 pagesBIOEN 345: Failure Analysis of Physiology: Lecture 4 May 4, 2020: Vessel PathologiesasdfghjklNo ratings yet
- RCOG Air Travel PregnancyDocument5 pagesRCOG Air Travel PregnancyElsaIsabelSilaenNo ratings yet
- CyclokapronDocument6 pagesCyclokapronTNo ratings yet
- Prakash Et Al 2023 Factor Xi Xia Inhibitors For The Prevention and Treatment of Venous and Arterial Thromboembolism A 1Document8 pagesPrakash Et Al 2023 Factor Xi Xia Inhibitors For The Prevention and Treatment of Venous and Arterial Thromboembolism A 1Gabriela PachecoNo ratings yet
- Anticoagulants DaniellewelschmeyerDocument30 pagesAnticoagulants Daniellewelschmeyersumanth gowdaNo ratings yet
- Tranexamic AcidDocument2 pagesTranexamic AcidIrish Ivy VibethNo ratings yet
- Haemodynamic DisordersDocument27 pagesHaemodynamic DisordersHareem FatimaNo ratings yet
- Matters TrialDocument7 pagesMatters TrialK_ja_Balcar_4670No ratings yet
- COPD and Pulmonary Thromboembolism (For Galley Proof)Document6 pagesCOPD and Pulmonary Thromboembolism (For Galley Proof)Ram AdhikariNo ratings yet
- Hemorragia PostpartoDocument34 pagesHemorragia PostpartoGiiszs AlvarezNo ratings yet
- Atrial Fibrillation and Mechanisms of StrokeDocument7 pagesAtrial Fibrillation and Mechanisms of StrokeRegina AyediaNo ratings yet