Professional Documents
Culture Documents
Anticoagulants May Be
Uploaded by
Ammar magdy0 ratings0% found this document useful (0 votes)
13 views5 pagesburn
Original Title
New Microsoft Word Document (3)
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentburn
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
13 views5 pagesAnticoagulants May Be
Uploaded by
Ammar magdyburn
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 5
ANTICOAGULANTS
These are the agents used to prevent and treat:
arterial thrombus (white in colour) like in myocardial infarction
venous thrombosis of limb veins
Anticoagulants may be
A. In vivo heparin
parenteral (heparin, LMWH, fondaparinux)
oral (dicumarol, warfarin, rivaroxaban)
B. in vitro-heparin
sodium citrate - sodium oxalate
Contraindications for anticoagulant therapy
Ongoing bleeding
recent surgery
invasive procedure
severe trauma
bleeding tendency
intracranial haemorrhage
pericarditis
pericardial effusion
severe hypertension
GIT ulcer
piles
ocular and neurosurgery
Heparin (Unfractionated)
pharmacokinetics
It is a natural anticoagulant (mucopolysaccharide)
Commercial heparin is derived from lung and intestinal
mucosa of pigs and cattle.
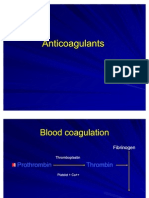
It prevents clotting of blood both in vivo and in vitro by acting on
all three stages of coagulation
It activates plasma antithrombin Ill and so blocks extrinsic
Pathway
It has got antiplatelet action
The onset of action is immediate after administration lasting for 4
hours.
It is metabolized in the liver by heparinase.
It does not cross placental barrier and is not secreted in breast milk
monitoring
clotting time
activated thromboplastin time
side effects
hyperkalaemia
thrombocytopenia
osteoporosis
Dose
1. prophylaxis
5,000 units/subcutaneously 8th hourly.
2. therapy
10,000 units/IV 8th hourly. later changed to s.c dose
Precautions
Heparin is not given orally
not given intramuscularly
not combine with penicillin and hydrocortisone.
Heparin should be monitored with APTT
Heparinoid is an anticoagulant used in patients where heparin is
contraindicated
Danaparoid is an antifactor Xa
Heparin antagonist
protamine sulphate
given slow intravenous
1 g reverses 100 units of heparin.
It is given only after doing activated thromboplastin time.
Overdosing may itself precipitate bleeding.
Low Molecular Weight Heparin (LMWH)
It is a commercially prepared heparin with a low molecular weight
It acts by inhibiting factor Xa.
It shows lesser antiplatelet action
lower incidence of hemorrhagic complications.
It has got better bioavailability on s.c administration (once daily).
Drugs
Enoxaparin; Dalteparin; Parnaparin; Reviparin; Fraxiparine.
route
It is used as subcutaneous injection.
Advantages
It has got longer duration of action once a day
has better anticoagulant effect
less interaction with platelets
less antigenic
monitoring is not necessary.
Disadvantages
They are expensive
only partially reversible by protamine sulphate
it is monitored by anti-Xa assay which is not freely available.
Fondaparinux (Arixtra)
It is a synthetic factor Xa inhibitor.
It acts by binding antithrombin Ill.
injected subcutaneously once daily dose
ORAL ANTICOAGULANTS
given orally
slow-acting
Types
A. Coumarin derivatives:
Warfarin sodium: Most common oral anticoagulant used.
B. lndandione derivative
Phenindione
pharmacokinetics
suppressing synthesis of prothrombin, factors VII, IX and X.
does not have in vitro action.
They are slow-acting but and long-acting.
They cross placental barrier (teratogenic)
They are secreted in breast milk.
monitoring
prothrombin time.
(PT comes to normal only 7 days after cessation of the drug).
INR
(has to be maintained within 2- 3).
Indications
maintenance therapy after cessation of heparin
Side Effects
Bleeding (blood transfusion – FFP - vitamin K)
Cutaneous gangrene.
Fetal haemorrhage and teratogenicity.
Drug interactions (NSAIDs, omeprazole, metronidazole)
WARFARIN
the most common drug used.
It has got lesser side effects.
It has got cumulative action and so given in tapering dose.
once a day.
It should be discontinued 7 days before any surgery and
prothrombin time should return to normal level.
Non-vitamin K antagonist oral anticoagulants (NOACs)
A. Direct thrombin inhibitors (factor Ila)
Natural: hirudin
Synthetic: Argatroban
B. Direct factor Xa inhibitors
Apixaban - Edoxaban
Contraindications for NOACs: Renal impairment
Anti-platelet Drugs
1. aspirin
inhibits platelet synthesis of thromboxane A2.
2. Ticlopidine
inhibits platelet aggregation.
3. Clopidogrel
inhibits platelet aggregation
4. Dextran
inhibits platelet aggregation.
5. Dipyridamole
xanthine oxidase inhibitor
You might also like
- Drugs Used To Affect in Blood Coagulation: Prajogo WibowoDocument44 pagesDrugs Used To Affect in Blood Coagulation: Prajogo WibowoIda Bagus Putu SwabawaNo ratings yet
- Anti Coagulatants: Presented By:-Mr - Gorishankar Nursing Tutor (Tantia University)Document10 pagesAnti Coagulatants: Presented By:-Mr - Gorishankar Nursing Tutor (Tantia University)yogesh kumarNo ratings yet
- ReviewerDocument20 pagesReviewerKC PalattaoNo ratings yet
- Agent Used in Disorder in CoagulationDocument34 pagesAgent Used in Disorder in CoagulationClinton Franda Markus SitanggangNo ratings yet
- Blood Pharmacology by Dr. Mayur Sayta M 910444Document21 pagesBlood Pharmacology by Dr. Mayur Sayta M 910444funzz100% (1)
- Presentation. 111tom AbDocument20 pagesPresentation. 111tom AbTemesgenNo ratings yet
- Haematology DrugsDocument17 pagesHaematology DrugsParyNo ratings yet
- Pharmacology - Hematologic DrugsDocument51 pagesPharmacology - Hematologic DrugsBenjamin Joel Breboneria100% (1)
- Drugs Affecting Blood CoagulationDocument51 pagesDrugs Affecting Blood CoagulationMoxie Macado100% (1)
- PHM - Hematologic DrugsDocument3 pagesPHM - Hematologic DrugsJeanne Rodiño100% (3)
- Anticoagulants ParamedDocument20 pagesAnticoagulants ParamedManikanta GupthaNo ratings yet
- AnticoagulantsDocument8 pagesAnticoagulantsRobert L G MabongaNo ratings yet
- AnticoagulantsDocument19 pagesAnticoagulantsOsama ZbedaNo ratings yet
- AnticoagulantsDocument64 pagesAnticoagulantsnainapattnaikNo ratings yet
- Receiving Concurrent Moderate CYP3A4 Inhibitors (Erythromycin, Saquinavir, Verapamil, Fluconazole) - 25 MG Once Daily InitiallyDocument272 pagesReceiving Concurrent Moderate CYP3A4 Inhibitors (Erythromycin, Saquinavir, Verapamil, Fluconazole) - 25 MG Once Daily InitiallyFatima Doran PandaogNo ratings yet
- AnticoagulantDocument34 pagesAnticoagulantAslam Baltee100% (1)
- Drug StudyDocument5 pagesDrug StudyJoyce Anne SupnetNo ratings yet
- Anticoagulation PharmacologyDocument36 pagesAnticoagulation PharmacologyaymenNo ratings yet
- L8 Anti Coagulant DrugsDocument10 pagesL8 Anti Coagulant DrugsamanabduwahabNo ratings yet
- Anticoagulants and Antiplatelet Drugs: Mechanisms and Clinical UsesDocument25 pagesAnticoagulants and Antiplatelet Drugs: Mechanisms and Clinical UsesIdrissa John Sebeh ContehNo ratings yet
- Anticoagulant PresentationDocument29 pagesAnticoagulant Presentationrozha100% (2)
- Anti CoagulantsDocument37 pagesAnti CoagulantsMaria khurshidNo ratings yet
- AnticoagulatsDocument52 pagesAnticoagulatsanaya khan StudentNo ratings yet
- Antiplatelets Anticoagulant Drugs 1668083619Document12 pagesAntiplatelets Anticoagulant Drugs 1668083619Nehal ElnagarNo ratings yet
- Pharmacology II: Treatments for Blood Disorders and InflammationDocument61 pagesPharmacology II: Treatments for Blood Disorders and InflammationDiane BanuaNo ratings yet
- AntiarrhythmiaDocument29 pagesAntiarrhythmiaDRx Raju ChandranNo ratings yet
- Pharmacology Affecting CoagulationDocument19 pagesPharmacology Affecting CoagulationCurtney PedriaNo ratings yet
- Anticoagulants 161120143945Document29 pagesAnticoagulants 161120143945Roshan SahuNo ratings yet
- Anticoagulatio N Asra Guidelines: Sravya VemuriDocument62 pagesAnticoagulatio N Asra Guidelines: Sravya VemuriSiva Prasad AspNo ratings yet
- ASRA Guidelines on Neuraxial Blockade and AnticoagulantsDocument66 pagesASRA Guidelines on Neuraxial Blockade and AnticoagulantsAshiyan IrfanNo ratings yet
- Heparin Vs Warfarin (Coumadin)Document5 pagesHeparin Vs Warfarin (Coumadin)blankNo ratings yet
- Multiple Injuries: Drug StudiesDocument10 pagesMultiple Injuries: Drug StudiesTarquin TomadaNo ratings yet
- A Drug Study On: HeparinDocument8 pagesA Drug Study On: HeparinRaijenne VersolaNo ratings yet
- ANTICOAGULANTS: Oral vs ParenteralDocument103 pagesANTICOAGULANTS: Oral vs Parenteralabhilashreddy45100% (1)
- Coagulation Modifier Drugs: Anticoagulants, Antiplatelets, ThrombolyticsDocument38 pagesCoagulation Modifier Drugs: Anticoagulants, Antiplatelets, ThrombolyticsPeter Angelo GeleraNo ratings yet
- Antimalarial DrugsDocument6 pagesAntimalarial Drugsrajendra kumar SwamiNo ratings yet
- Drug Study Pre AnestheticDocument2 pagesDrug Study Pre AnestheticCherilyn MedalleNo ratings yet
- Anticoagulant, Antithrombotic and Anti-Platelet DrugsDocument63 pagesAnticoagulant, Antithrombotic and Anti-Platelet Drugsruchipickle100% (1)
- Anti CoagulantsDocument25 pagesAnti Coagulantsshoaib106muhammadNo ratings yet
- Coumadins (Vitamin K Antagonists) : Synthetic Pentasaccharide Inhibitors of Factor XaDocument1 pageCoumadins (Vitamin K Antagonists) : Synthetic Pentasaccharide Inhibitors of Factor XaNoman J. KhanNo ratings yet
- Anticoagulant TherapyDocument41 pagesAnticoagulant Therapyryan yovanNo ratings yet
- Drugs Used in Disorders of CoagulationDocument61 pagesDrugs Used in Disorders of CoagulationDUEÑAS, MARIELNo ratings yet
- Drug Evaluation MonographDocument12 pagesDrug Evaluation MonographYodaheNo ratings yet
- The Pharmacology of AntithromboticsDocument14 pagesThe Pharmacology of AntithromboticsanaNo ratings yet
- ClexaneDocument2 pagesClexaneJàson VòrheesNo ratings yet
- Blood Thinners: Hussein Hallak, PH.DDocument68 pagesBlood Thinners: Hussein Hallak, PH.DIbrahim BarhamNo ratings yet
- Anticoagulants: Dr. Hassan Mohamed EnowDocument37 pagesAnticoagulants: Dr. Hassan Mohamed EnowFatimaNo ratings yet
- List of AnticoagulantsDocument9 pagesList of Anticoagulantschristianz39100% (1)
- Anticoagulation Related Bleeding - Guideline Summary: Click On The Appropriate Link BelowDocument19 pagesAnticoagulation Related Bleeding - Guideline Summary: Click On The Appropriate Link BelowIreneNo ratings yet
- Anticoagulant, Fibrinolytic, and Antiplatelet DrugsDocument22 pagesAnticoagulant, Fibrinolytic, and Antiplatelet DrugsVera Waty100% (1)
- COPD Drug Study: Ipratropium Bromide and Albuterol SulfateDocument9 pagesCOPD Drug Study: Ipratropium Bromide and Albuterol SulfateShane Arroyo100% (1)
- Rivaroxaban PresentationDocument13 pagesRivaroxaban PresentationReem El-HusseinyNo ratings yet
- Neuraxial Blockade and AnticoagulantsDocument69 pagesNeuraxial Blockade and Anticoagulantskamel6No ratings yet
- Manage Heavy Menstrual Bleeding with Tranexamic AcidDocument3 pagesManage Heavy Menstrual Bleeding with Tranexamic AcidNapieh Bulalaque Polistico100% (4)
- Anticoagulant DrugsDocument7 pagesAnticoagulant DrugsNadia MohammadNo ratings yet
- DIS HeparinDocument4 pagesDIS HeparinRebecca ChenNo ratings yet
- Blood Coagulation and Fibrinolysis: Key Drug Classes and MechanismsDocument63 pagesBlood Coagulation and Fibrinolysis: Key Drug Classes and MechanismsNora AboshanadyNo ratings yet
- Neonatal Formulary: Drug Use in Pregnancy and the First Year of LifeFrom EverandNeonatal Formulary: Drug Use in Pregnancy and the First Year of LifeNo ratings yet
- Top 300 Drugs Pocket Reference Guide (2021 Edition)From EverandTop 300 Drugs Pocket Reference Guide (2021 Edition)Rating: 5 out of 5 stars5/5 (1)
- 2017 Australian Donations and Transplantghgation Activity ReportDocument11 pages2017 Australian Donations and Transplantghgation Activity ReportAmmar magdyNo ratings yet
- PD 6000 Bariatric Surgery Gastric Bypass 2016 PDFDocument118 pagesPD 6000 Bariatric Surgery Gastric Bypass 2016 PDFAmmar magdyNo ratings yet
- ANZ J. Surg. 2008 78 (Suppl. 1) A68-A80Document13 pagesANZ J. Surg. 2008 78 (Suppl. 1) A68-A80Ammar magdyNo ratings yet
- Journal Pre-Proof: International Journal of SurgeryDocument28 pagesJournal Pre-Proof: International Journal of SurgeryAmmar magdyNo ratings yet
- LT 21509 PDFDocument11 pagesLT 21509 PDFAmmar magdyNo ratings yet
- Case ReportDocument5 pagesCase ReportAmmar magdyNo ratings yet
- LT 21509 PDFDocument11 pagesLT 21509 PDFAmmar magdyNo ratings yet
- En 18Document6 pagesEn 18Ammar magdyNo ratings yet
- Burn PDFDocument16 pagesBurn PDFAmmar magdyNo ratings yet
- SurgerybookchildlifeDocument32 pagesSurgerybookchildlifeapi-482903737No ratings yet
- Kumar 2019Document7 pagesKumar 2019Ammar magdyNo ratings yet
- AnatomyDocument2 pagesAnatomyAmmar magdyNo ratings yet
- International Journal of Pharmaceutical and Clinical ScienceDocument3 pagesInternational Journal of Pharmaceutical and Clinical ScienceJamesNo ratings yet
- Antiplatelet, Anticoagulant and Thrombolytic Agents: Basic Pharmacology Block Pdnt/Pmed - PMSC/PPHR - 213Document30 pagesAntiplatelet, Anticoagulant and Thrombolytic Agents: Basic Pharmacology Block Pdnt/Pmed - PMSC/PPHR - 213JedoNo ratings yet
- Grand Rounds - Anticoagulant Reversal AgentsDocument43 pagesGrand Rounds - Anticoagulant Reversal Agentsapi-611624486No ratings yet
- Pharmacotherapy Considerations in Palliative Care: Learning ObjectivesDocument19 pagesPharmacotherapy Considerations in Palliative Care: Learning ObjectivesMajed Mubarak Shannan AlzahraniNo ratings yet
- Pradaxa, Only Noac: Prescribe THE With A Specific Reversal AgentDocument2 pagesPradaxa, Only Noac: Prescribe THE With A Specific Reversal AgentCodruț DragomirescuNo ratings yet
- Anticoagulants and CoagulantsDocument31 pagesAnticoagulants and CoagulantsSandra PlausNo ratings yet
- Cor PulmonaleDocument14 pagesCor PulmonaleEvangelin MelvinNo ratings yet
- Clinical Chemistry & Molecular Diagnostics 1Document3 pagesClinical Chemistry & Molecular Diagnostics 1thedarkwingNo ratings yet
- Stroke Prevention in Patients With Acute Ischemic Stroke and Atrial Fibrillation in Germany - A Cross Sectional SurveyDocument4 pagesStroke Prevention in Patients With Acute Ischemic Stroke and Atrial Fibrillation in Germany - A Cross Sectional Surveymasyuni cantika sariNo ratings yet
- ACC PI ActilyseDocument19 pagesACC PI ActilysePPRA RSU Kab. TangerangNo ratings yet
- STOPP START Tool To Support Medication ReviewDocument11 pagesSTOPP START Tool To Support Medication ReviewSan Phạm ĐìnhNo ratings yet
- The British Rhinological Society Multidisciplinary Consensus Recomendation On The Hospital Management of EpistaxisDocument15 pagesThe British Rhinological Society Multidisciplinary Consensus Recomendation On The Hospital Management of EpistaxisekoNo ratings yet
- Dangers of Vitamins and SupplementsDocument19 pagesDangers of Vitamins and SupplementsanasetiahaeroniNo ratings yet
- Ketorolac Tromethamine Injection Usp: Product MonographDocument41 pagesKetorolac Tromethamine Injection Usp: Product MonographWahyu AriawanNo ratings yet
- Practice: Deep Vein ThrombosisDocument6 pagesPractice: Deep Vein ThrombosisAri Setiyawan NugrahaNo ratings yet
- Acute Pulmonary EmbolismDocument82 pagesAcute Pulmonary Embolismincredible Prages100% (1)
- Author's Accepted Manuscript: Journal of EthnopharmacologyDocument52 pagesAuthor's Accepted Manuscript: Journal of EthnopharmacologyIara PachêcoNo ratings yet
- An Overview of Therapeutic Plasma ExchangeDocument65 pagesAn Overview of Therapeutic Plasma ExchangesayednourNo ratings yet
- Anticoagulation On DialysisDocument52 pagesAnticoagulation On DialysisFey100% (1)
- GI Bleeding in Patients Receiving Antiplatelets and Anticoagulant TherapyDocument11 pagesGI Bleeding in Patients Receiving Antiplatelets and Anticoagulant TherapyTony LeeNo ratings yet
- Nephrotic Syndrome Children PDFDocument11 pagesNephrotic Syndrome Children PDFesdl86No ratings yet
- Guidance On Converting Between Anticoagulant RegimensDocument4 pagesGuidance On Converting Between Anticoagulant Regimenskratai NNo ratings yet
- Xenical: OrlistatDocument8 pagesXenical: Orlistatddandan_2No ratings yet
- Portal Vein Thrombosis Should We Bust The Clot?: Dr. Mohammed Said Noor Fy1 Mr. Esam Aboutaleb SPRDocument33 pagesPortal Vein Thrombosis Should We Bust The Clot?: Dr. Mohammed Said Noor Fy1 Mr. Esam Aboutaleb SPREsam AboutalebNo ratings yet
- Cardiology Pharmacology Review: HMG-CoA Reductase Inhibitors MechanismDocument74 pagesCardiology Pharmacology Review: HMG-CoA Reductase Inhibitors Mechanismshannon_marrero_1No ratings yet
- TTO VEN ListByClassDocument17 pagesTTO VEN ListByClassEnalys García MenaNo ratings yet
- SUCCEESSFULLY Navigating The First Year of Surgical ResidencyDocument56 pagesSUCCEESSFULLY Navigating The First Year of Surgical ResidencyYoya LawiNo ratings yet
- BLS MCQ CoagulationDocument4 pagesBLS MCQ CoagulationsssajiNo ratings yet
- StoppFrail PaperDocument8 pagesStoppFrail PaperEric LiangNo ratings yet
- Mineral, Vitamin, and Herbal SupplementsDocument18 pagesMineral, Vitamin, and Herbal SupplementsismailcemNo ratings yet