Professional Documents
Culture Documents
Song, Imagenes
Uploaded by
ismael yambayOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Song, Imagenes
Uploaded by
ismael yambayCopyright:
Available Formats
ORIGINAL RESEARCH • THORACIC IMAGING
Emerging 2019 Novel Coronavirus (2019-nCoV)
Pneumonia
Fengxiang Song, MD* • Nannan Shi, MD* • Fei Shan, MD, PhD • Zhiyong Zhang, MD, PhD • Jie Shen, MD •
Hongzhou Lu, MD, PhD • Yun Ling, MD, PhD • Yebin Jiang, MD, PhD • Yuxin Shi, MD, PhD
From the Departments of Radiology (F. Song, N.S., F. Shan, Z.Z., J.S., Y.S.) and Infectious Disease (H.L., Y.L.), Shanghai Public Health Clinical Center, No. 2501
Caolang Road, Jinshan District, Shanghai 201508, China; Department of the Principal's Office, Fudan University, Shanghai, China (Z.Z.); Cancer Center, University of
Michigan, Ann Arbor, Mich (Y.J.); and Shanghai Key Laboratory of Molecular Imaging, Shanghai, China (Y.S.). Received February 2, 2020; revision requested February
5; final revision received February 5; accepted February 5. Address correspondence to Y.S. (e-mail: shiyuxin@shphc.org.cn).
*F. Song and N.S. contributed equally to this work.
Conflicts of interest are listed at the end of this article.
Radiology 2020; 295:210–217 • https://doi.org/10.1148/radiol.2020200274 • Content code:
Background: The chest CT findings of patients with 2019 Novel Coronavirus (2019-nCoV) pneumonia have not previously been
described in detail.
Purpose: To investigate the clinical, laboratory, and imaging findings of emerging 2019-nCoV pneumonia in humans.
Materials and Methods: Fifty-one patients (25 men and 26 women; age range 16–76 years) with laboratory-confirmed 2019-nCoV in-
fection by using real-time reverse transcription polymerase chain reaction underwent thin-section CT. The imaging findings, clini-
cal data, and laboratory data were evaluated.
Results: Fifty of 51 patients (98%) had a history of contact with individuals from the endemic center in Wuhan, China. Fever
(49 of 51, 96%) and cough (24 of 51, 47%) were the most common symptoms. Most patients had a normal white blood cell
count (37 of 51, 73%), neutrophil count (44 of 51, 86%), and either normal (17 of 51, 35%) or reduced (33 of 51, 65%) lym-
phocyte count. CT images showed pure ground-glass opacity (GGO) in 39 of 51 (77%) patients and GGO with reticular and/
or interlobular septal thickening in 38 of 51 (75%) patients. GGO with consolidation was present in 30 of 51 (59%) patients,
and pure consolidation was present in 28 of 51 (55%) patients. Forty-four of 51 (86%) patients had bilateral lung involvement,
while 41 of 51 (80%) involved the posterior part of the lungs and 44 of 51 (86%) were peripheral. There were more consoli-
dated lung lesions in patients 5 days or more from disease onset to CT scan versus 4 days or fewer (431 of 712 lesions vs 129 of
612 lesions; P , .001). Patients older than 50 years had more consolidated lung lesions than did those aged 50 years or younger
(212 of 470 vs 198 of 854; P , .001). Follow-up CT in 13 patients showed improvement in seven (54%) patients and progres-
sion in four (31%) patients.
Conclusion: Patients with fever and/or cough and with conspicuous ground-glass opacity lesions in the peripheral and posterior lungs
on CT images, combined with normal or decreased white blood cells and a history of epidemic exposure, are highly suspected of
having 2019 Novel Coronavirus (2019-nCoV) pneumonia.
© RSNA, 2020
O n December 30, 2019, a report indicating a cluster
of patients with pneumonia of unknown etiology
in Wuhan City, Hubei Province, China, was published
cities, autonomous regions, and special administrative
regions (Hong Kong and Macao). Thailand, Japan,
South Korea, and the United States of America (3–6)
on ProMED-mail (1). It was possibly related to con- also reported exported cases. At the time of this writ-
tact with a local fish and wild animal market (Huanan ing, there were 492 patients who died in China and 897
Seafood Wholesale Market), where there was also sale cases cured. The 2019-nCoV poses significant threats to
of live animals. Most of the first reported patients vis- international health.
ited the market about 1 month before onset. Deep se- Coronaviruses are enveloped nonsegmented positive-
quencing analysis from lower respiratory tract samples sense RNA viruses belonging to the family Coronaviridae
indicated a novel coronavirus, which was named 2019 and the order Nidovirales and broadly distributed in hu-
Novel Coronavirus (2019-nCoV) by the World Health mans and other mammals (7). The 2002–2003 pandemic
Organization (2). In mid-January 2020, China began of severe acute respiratory syndrome coronavirus, or SARS-
passenger transportation during or around the Chinese CoV, and the ongoing emergence of the Middle East respi-
New Year, which is equivalent to the Christmas holiday ratory syndrome coronavirus, or MERS-CoV, demonstrate
celebration in the West. A large number of people living that coronaviruses are a significant public health threat (8).
in Wuhan left the region by air carrier. Since January 17, The 2019-nCoV is a betacoronavirus of group 2B with at
the confirmed or suspected cases have dramatically in- least 70% similarity in genetic sequence to SARS-CoV (9).
creased. By 11:41 PM on February 5, 2020, China has Different from both MERS-CoV and SARS-CoV, 2019-
reported 24 363 confirmed cases and 23 260 suspected nCoV is the seventh member of the family of coronaviruses
cases (including health care workers) from all provinces, that infect humans (10). It may originate from Chinese
This copy is for personal use only. To order printed copies, contact reprints@rsna.org
Song et al
to 14 days. All CT examinations were performed with a 64-sec-
Abbreviations tion scanner (Scenaria 64 CT; Hitachi Medical, Kashiwa, Chiba
GGO = ground-glass opacity, 2019-nCOV = 2019 Novel Coronavirus Prefecture, Japan) without the use of contrast material. The
Summary CT protocol was as follows: tube voltage, 120 kV; automatic
Fever and/or cough, chest CT with bilateral ground-glass opacities tube current (180 mA–400 mA); iterative reconstruction tech-
in the posterior and peripheral lungs, and a history of exposure to nique; detector, 64 mm; rotation time, 0.35 second; section
individuals from Wuhan, China, are characteristic of 2019 Novel thickness, 5 mm; collimation, 0.625 mm; pitch, 1.5; matrix,
Coronavirus, or 2019-nCoV, pneumonia. 512 3 512; and breath hold at full inspiration. Reconstruction
Key Results kernel used was lung smooth with a thickness of 1 mm and an
n Nearly all patients in this series with 2019 Novel Coronavirus, or interval of 0.8 mm. The following windows were used: a medi-
2019-nCoV, pneumonia (50 of 51 patients, 98%) had a history of astinal window with a window width of 350 HU and a window
contact with individuals from Wuhan, China. level of 40 HU, and a lung window with a width of 1200 HU
n Chest CT showed pure ground-glass opacities (GGOs) in 77% of and a level of −600 HU.
patients, GGOs with interstitial and/or interlobular septal thick-
ening in 75% of patients, and GGOs with consolidation in 59%
Three chest radiologists (F.Song, N.S., and Y.S., with ap-
of patients. proximately 6–32 years of experience in thoracic imaging,
n At chest CT, GGOs were bilateral in 88% of patients, involving especially in the setting of viral pneumonias such as H1N1
the posterior lungs in 82% and the peripheral lungs in 85% of and H7N9 pneumonia) reviewed the images independently,
patients. with a final finding reached by consensus when there was a
discrepancy.
CT images were assessed for the presence and distribution of
horseshoe bats, which are the natural reservoirs of SARS-CoV parenchymal abnormalities including pure ground-glass opacity
(8) and can transmit from human to human. (GGO), which were defined as a hazy increase in lung attenua-
The Shanghai Public Health Clinical Center is the designated tion with no obscuration of the underlying vessels; GGO with
hospital for diagnosis and management of infectious diseases and interlobular septal thickening or reticulation, or intralobular net-
threats against public health in our country, and it is also a World works in GGO; GGO with consolidation, which was defined
Health Organization–designated training organization for new as an area of opacification obscuring the underlying vessels in
emerging infectious diseases. At the time of this writing, 56 pa- GGO; consolidation; air bronchogram(s); reticulation; lymph-
tients with confirmed 2019-nCoV infection have been admitted adenopathy, which was defined as a lymph node greater than
to the center. 1 cm in short-axis diameter; and pleural effusion. On the axial
The purpose of this study was to review the noncontrast chest CT images, we drew a horizontal line across the axillary midline
CT findings in patients with laboratory-confirmed 2019-nCoV to divide anterior and posterior parts of the lungs. The outer
infection by using real-time reverse transcription–polymerase one-third of the lung was defined as peripheral, and the rest was
chain reaction, or RT-PCR, performed at the Center for Disease defined as central.
Control, Shanghai, China. Chest CT lesions in each patient were identified by the read-
ers. A lesion occupying only one lung segment was counted as
Materials and Methods one lesion. When a large lesion or fused lesion involved more
than one lung segment, the lesion number was recorded as the
Patients number of the involved lung segments. For example, a large le-
The ethical committee of Shanghai Public Health Clinical sion involving three lung segments was counted as three lesions.
Center approved this retrospective study. Our inclusion crite- Each side of the chest containing pleural fluid was counted as
ria were patients admitted to our center with laboratory-con- one lesion. A pericardial effusion was counted as one lesion.
firmed 2019-nCoV infection by using RT-PCR, patients who
underwent thin-section CT, and patients with CT images that Statistical Analysis
demonstrated pneumonia. Excluded were two patients with All data were statistically analyzed by using Stata software
only bedside chest radiograph (without CT), and three pa- package (version 10.0; StataCorp, College Station, Tex). Data
tients with normal findings at chest CT. A total of 51 patients were expressed as means 6 standard deviation, or medians for
were included. We reviewed the clinical and laboratory data the continuous variables. The comparison of discrete variables
and CT images of the 51 patients with 2019-nCoV pneumo- between groups was performed by using the Pearson x2 test.
nia from January 20, 2020, to January 27, 2020. All patients Correlation analysis between two groups was performed by us-
were confirmed as having positive results by using real-time ing rank correlation. All analyses were considered significant at
RT-PCR nucleic acid assay for 2019-nCoV by the Center for P values of less than .05.
Disease Control, Shanghai, China. Other causes of pneumonia
from common bacterial and viral pathogens were excluded. Results
Image Acquisition Clinical and Laboratory Findings
All the patients underwent thin-section CT. The median dura- The demographic and clinical characteristic results of 51 pa-
tion from illness onset to CT scan was 4 days, ranging from 1 tients are shown in Table 1. The 51 patients included 25 (49%)
Radiology: Volume 295: Number 1—April 2020 n radiology.rsna.org 211
Emerging 2019 Novel Coronavirus (2019-nCoV) Pneumonia
Table 1: Demographic and Clinical Characteristics of 51 Patients Table 2: Distribution of the Lesions in 51 Patients with 2019
with 2019 Novel Coronavirus (2019-nCoV) Pneumonia Novel Coronavirus (2019-nCoV) Pneumonia
Characteristic Value No. of No. of
Sex Finding Patients Lesions*
Male 25 (49) Unilateral lung 7 (14) 40 (3)
Female 26 (51) Bilateral lung 44 (86) 1284 (97)
Age (y)* 49 6 16 One lobe 4 (8) 12 (0.9)
Contact with Wuhan, China 50 (98) Two lobes 8 (16) 64 (5)
Comorbidity 11 (22) Three lobes 6 (12) 54 (4)
Diabetes 3 (6) Four lobes 12 (24) 276 (21)
Hypertension 5 (10) Five lobes 20 (39) 918 (69)
Chronic liver disease 1 (2) Involved lung zones
Chronic obstructive pulmonary 1 (2) Upper lobes 43 (84) 485 (37)
Cardiac disease 1 (2) Middle lobe 30 (59) 136 (10)
Signs and symptoms Lower lobes 46 (90) 703 (53)
Fever Predominant distribution
Higher temperature 49 (96) Anterior 9 (18) 145 (11)
Normal 2 (4) Posterior 41 (80) 1179 (89)
,37.3°C 1 (2) Peripheral 44 (86) 1198 (91)
37.3–38.0°C 20 (39) Central 5 (10) 42 (3)
38.1–39.0°C 18 (35) Both central and peripheral 1 (2) 84 (6)
.39.0°C 10 (20) Note.—Data in parentheses are percentages.
Cough 24 (47) * Of 1324 chest CT lung abnormalities in 51 patients.
Little phlegm 10 (20)
Myalgia or fatigue 16 (31)
Mild headache and dizziness 8 (16)
Mild dyspnea or chest pain 7 (14) Table 3: CT Imaging Findings in 51 Patients with 2019 Novel
Loss of appetite 9 (18) Coronavirus (2019-nCoV) Pneumonia
Diarrhea 5 (10)
No. of No. of
Stuffy and runny nose 2 (4)
Lesions Patients Lesions
Sore throat 3 (6)
Nausea and vomiting 3 (6) Pure GGO 39 (77) 395 (30)
GGO with reticular and/ 38 (75) 519 (39)
Note.—Unless otherwise specified, data are the number of or interlobular septal thickening
patients, with percentages in parentheses.
GGO with consolidation 30 (59) 238 (18)
* Data are means 6 standard deviation
Consolidation 28 (55) 172 (13)
Air bronchogram* 41 (80) 279
Reticulation* 11 (22) 20
men and 26 (51%) women, with ages ranging from 16 to 76 Pleural effusion* 4 (8) 5
years (mean age, 49 years 6 16 [standard deviation]). Fifty pa- Pericardial effusion* 3 (6) 3
tients (98%) had some contact with individuals from Wuhan, Lymphadenopathy* 3 (6) 6
China (38 patients traveled to or lived in Wuhan, or were in
Note.—Data in parentheses are percentages. The total number
contact with individuals with confirmed 2019-nCoV pneumo- of lung lesions (pure ground-glass opacity [GGO], GGO with
nia [eight, 16%], individuals suspected of having 2019-nCoV reticular and/or interlobular septal thickening, GGO with con-
pneumonia [three, 6%], and a single healthy individual from solidation, and consolidation) was 1324. A lesion occupying only
that city [one, 2.0%]). Only one patient had no definite his- one lung segment was counted as one lesion. When a large lesion
tory of Wuhan contact, but had recently traveled to another or fused lesion involved more than one lung segment, lesion
number was recorded as the number of the involved lung seg-
city. The most common symptoms were fever (49 of 51, 96%) ments. For example, a large lesion involving three lung segments
and cough (24 of 51, 47%). Other symptoms included myal- was counted as three lesions. Each side of the chest containing
gia or fatigue (16 of 51, 31%), mild headache and dizziness pleural fluid was counted as one lesion. Pericardial effusion was
(eight of 51, 16%), and diarrhea (five of 51, 10%). Eleven of counted as one lesion.
51 (22%) patients had comorbidities including diabetes, hy- * Not included in the total number of 1324 lung lesions.
pertension, chronic liver disease, chronic obstructive pulmo-
nary disease, and cardiac disease. Three of the 51 (7%) patients
with confirmed 2019-nCoV pneumonia were current cigarette lymphocyte count was low (33 of 51, 65%) or normal (17 of 51,
smokers. 35%). C-reactive protein level was elevated in 41 of 51 patients
Most of the patients had a normal white blood cell count (80%). Thirty-one of 51 (61%) patients had a low CD4+ cell
(37 of 51, 73%) and neutrophil count (44 of 51, 86%). The count, with a range of 72–408 cells/µL.
212 radiology.rsna.org n Radiology: Volume 295: Number 1—April 2020
Song et al
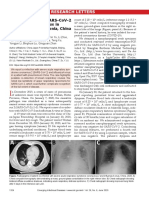
Figure 1: (a) Baseline CT images at admission of a 35-year-
old man show multiple patchy areas of pure ground-glass opacity
(GGO); GGO with reticular and/or interlobular septal thickening;
and patchy, focal, often rounded peribronchovascular and subpleu-
ral opacities associated with reticulation and architectural distortion.
Lesions are mostly distributed in peripheral and posterior part of lungs.
(b, c) Follow-up CT images on day 5 after admission show promi-
nent progression with increased size and density of lesions, greater
consolidation, and with interval new bilateral pleural effusions and
likely bibasilar compression atelectasis (c).
CT Imaging Findings We stratified our patients into two groups: group 1 with an
Data of initial chest thin-section CT imaging findings in 51 pa- interval of less than or equal to 4 days between symptom on-
tients with 2019-nCoV pneumonia are presented in Tables 2 and set and the chest CT scan and group 2 with an interval greater
3. There were 44 of 51 (86%) patients with a total of 1284 of 1324 than 4 days between symptom onset and the chest CT scan. We
(97%) lesions involving both lungs and 32 of 51 (63%) patients found more consolidation (including GGO with consolidation
with 1194 of 1324 (90%) lesions involving four to five lobes. and only consolidation) in group 2 (431 of 712 lesions, 61%)
There were 46 of 51 (90%) patients with 703 of 1324 (53%) le- than in group 1 (129 of 612 lesions, 21%) (P , .001). There
sions distributed in the lower lobes, 41 of 51 (80%) patients with were significantly more GGOs including pure GGO and GGO
1179 of 1324 (89%) lesions distributed in the posterior part of with reticular and/or interlobular septal thickening in group 1
the lung, and 44 of 51 (86%) patients with 1198 of 1324 (91%) (483 of 612 79%) than in group 2 (281 of 712, 40%) (Table 4).
lesions distributed in the lung periphery (Fig 1). The absolute number of lung findings increased with the time
Pure GGO, GGO with reticular and/or interlobular septal from symptom onset (r = 0.33; P = .02). Lesions with consolida-
thickening, and GGO with consolidation were the main find- tions including GGOs with consolidation and pure consolida-
ings (1152 of 1324, 87%). There were 395 of 1324 (30%) pure tion showed mildly positive correlation with the time between
GGOs in 39 of 51 (77%) patients, 519 of 1324 (39%) GGO symptom onset and the CT (r = 0.32; P = .02).
lesions with reticular and/or interlobular septal thickening in We stratified our patients into two age groups (Table 4): age
38 (75%) patients, 238 of 1324 (18%) GGO lesions with con- 50 years and younger and age older than 50 years. There were
solidation in 30 of 51 (59%) patients, 172 of 1324 (13%) con- more GGOs (including pure GGOs and GGOs with reticular
solidation lesions in 28 of 51 (55%) patients (Figs 1–3), and and/or interlobular septal thickening) in the younger group (656
279 bronchograms in 41 of 51 (80%) patients. Other findings of 854, 77%) than in the older group (258 of 470, 55%) (P ,
included reticulation, small pleural effusion, small pericardial ef- .001). There was significantly more consolidation with an organiz-
fusion, and lymphadenopathy. The pleural effusion was bilateral ing pneumonia pattern, including GGOs with consolidation and
in one patient and unilateral in three patients. One patient had pure consolidation in the older group (212 of 470, 45%) than in
only right pleural with no parenchyma lesions at first chest CT. the younger group (198 of 854, 23%) (P , .001). The younger
After 2-day follow-up, the pleural effusion had absorption, but patients tended to have more GGOs, while older patients tended
small pure GGO in the lung parenchyma was seen. to have more areas of lung involvement and more consolidation.
Radiology: Volume 295: Number 1—April 2020 n radiology.rsna.org 213
Emerging 2019 Novel Coronavirus (2019-nCoV) Pneumonia
Figure 2: (a, b) Baseline CT images at admission of a 75-year-old man show multiple patchy areas of pure ground-glass opacity
(GGO) and GGO with reticular and/or interlobular septal thickening. (c, d) Follow-up CT images on day 3 after admission show overlap
of organizing pneumonia with diffuse alveolar damage in that it is more diffuse (not rounded) and associated with underlying reticulation,
prominent progression with increased size and density of the lesions, and with more consolidations. Air bronchogram is also shown in d (ar-
rows). Interlobular septal thickening does not seem to be major component. There is reticulation in many of cases of both suspected organiz-
ing pneumonia and diffuse alveolar damage.
We have followed up chest CT examinations in 13 of 51 of Most pulmonary lesions involved bilateral lungs with mul-
the patients in this series. There was interval progression in four tiple lung lobes, with predominant distribution in posterior
of 13 (31%) patients (Figs 1–3), with an increased size and/or and peripheral part of the lungs. Studies showed that influ-
increased consolidation along with more areas of consolidation. enza pneumonia tend to affect lower lung (15). Wang et al (14)
At follow-up, pulmonary involvement was improved in seven of also showed that H7N9 pneumonia had a predominant distri-
13 (54%) patients, with smaller lesion size and/or a developing bution in the right lower lung. Both H1N1 pneumonia and
organizing pneumonia pattern in what was pure consolidation SARS distributed more peripherally (16,17), while there was
(Fig 4). no lobar predilection in H5N1 influenza (18). The posterior
and peripheral lung predominant distribution in our study is
Discussion characteristic. Such distribution is conspicuous at first glance
All patients except one had a history of contact with indi- of the images.
viduals from Wuhan, which was very important for diagnosis. The observation regarding the high prevalence of bilateral
The most common symptoms were fever (49, 96%), followed organizing pneumonia in these patients is potentially of impor-
by cough (24, 47%) and myalgia or fatigue (16, 31%), con- tance. This suggests that corticosteroids might be an option to
sistent with former report (2,11,12). The laboratory results suppress this immune reaction within the lung parenchyma to
of normal blood cells could also be helpful to make the di- 2019-nCoV pneumonia.
agnosis. In our study, the average age was 49 years, ranging Our results showed that the most common imaging findings
from 16–76 years, and only 11 patients (22%) had coexisting were pure GGO, GGO with reticular and/or interlobular septal
medical conditions such as diabetes, hypertension, chronic thickening, and GGO with consolidation. Complete consolida-
liver disease, chronic obstructive pulmonary disease, and car- tion was relatively less common (in 55% of patients in 13% of
diac disease. This is different from influenza A (H7N9) virus lesions), which might be explained by the early stage of the dis-
pneumonia, which tends to affect older adults (aged 66 years, ease. In H7N9 pneumonia, most cases showed consolidation (14).
with a range of 48–81 years) with coexisting chronic diseases Each single CT pattern seen in our patients is nonspecific and
(13,14). may overlap with those of other microorganism infections, such
214 radiology.rsna.org n Radiology: Volume 295: Number 1—April 2020
Song et al
Figure 3: Serial imaging after admission of a 71-year-old man. (a) Baseline CT images on January 21, 2020, show consolidation of
right upper lobe and ground-glass opacity (GGO) with consolidation and reticular and/or interlobular septal thickening of left upper lobe of
left upper lobe; and patchy, focal, often rounded peribronchovascular and subpleural opacities associated with reticulation and architectural
distortion. (b) Two days later, CT images show increased size of lesions in both lungs and decreased density in GGO lesions. (c) However,
GGO on both lungs were larger on day 4 after admission. (d) Bedside portable chest radiograph on day 6 following admission shows dif-
fusely increased opacities in both lungs, with relative bibasilar sparing.
Table 4: Proportion of GGO and Consolidation Lesions for Patients with 2019 Novel Coronavirus (2019 nCOV) Pneumonia, Strati-
fied by Disease Onset to CT Interval and by Age
Interval from Disease Onset Interval from Disease Onset
Type of Lung Lesion to CT 4 Days* to CT . 4 Days† P Value Age 50 Years‡ Age .50 Years§ P Value
GGO 483 (79) 281 (40) ,.001 656 (77) 258 (55) ,.001
Consolidation 129 (21) 431 (61) ,.001 198 (23) 212 (45) ,.001
Total lesions 612 712 … 854 470 …
Note.— Data in parentheses are percentages. Ground-glass opacity (GGO) includes pure GGO and GGO with reticular and/or interlobu-
lar septal thickening. Consolidation includes GGO with consolidation and pure consolidation.
* 29 patients.
†
22 patients.
‡
27 patients.
§
24 patients.
as H7N9 pneumonia, H1N1 virus infection, SARS, coronavi- with consolidation, and consolidation—were often mixed, and
rus infection, and avian influenza A (H5N1) (14,16,17). GGO, tended to appear simultaneously in the same patient. While the
consolidation, and interlobular septal thickening are also the most pure GGO is a common single finding in 77% of patients and in
common thin-section CT findings of H1N1 influenza pneumo- 30% of lesions in the 2019-nCoV pneumonia, the main CT fea-
nia (16). The four patterns in our imaging findings—pure GGO, tures were all patterns of GGO, including pure GGO, GGO with
GGO with reticular and/or interlobular septal thickening, GGO reticular and/or interlobular septal thickening, and GGO with
Radiology: Volume 295: Number 1—April 2020 n radiology.rsna.org 215
Emerging 2019 Novel Coronavirus (2019-nCoV) Pneumonia
Figure 4: (a, b) Baseline CT images at admission of a 56-year-old man show multiple patchy areas of organizing pneumonia with
some areas of interstitial and/or interlobular septal thickening and “strip shaped” consolidation (patchy, focal, often rounded, peribroncho-
vascular and subpleural opacities associated with reticulation and architectural distortion). These abnormalities are mostly distributed in pe-
ripheral and posterior parts of lungs. (c, d) Follow-up CT images on day 5 after admission show interval improvement and absorption with
fewer lesions and decreased lesion density.
consolidation, which were observed in all patients and accounted images are pure ground-glass opacity (GGO), GGO with reticular
for 87% of lesions. These CT findings combined together, with and/or interlobular septal thickening, GGO with consolidation,
predominant distribution in posterior and peripheral part of the and consolidation, with prominent distribution in the posterior
lungs, were uncommon in other viral pneumonia. and peripheral part of the lungs. Consolidation lesions could serve
Our study showed that consolidation indicated disease pro- as a marker of disease progression or more severe disease. Although
gression. There were more consolidation lesions and fewer GGO the positive nucleic acid testing is the diagnostic reference stan-
lesions in the patients with CT interval greater than or equal dard, patients with fever and/or cough and with GGO-prominent
to 4 days than in patients with CT interval less than or equal lesions in the peripheral and posterior part of lungs on CT images,
to 4 days, which likely indicates that consolidation increases as combined with normal or decreased white blood cells and a his-
disease course extends. In addition, there were significantly more tory of epidemic exposure, should be highly suspected of having
consolidation lesions and less GGO lesions in older patients 2019-nCoV pneumonia.
than in younger patients. Therefore, finding of consolidation le- Author contributions: Guarantors of integrity of entire study, F. Song, N.S., F.
sions would serve as an alert in the treatment of patients. Shan, Z.Z., H.L., Y.L., Y.J., Y.S.; study concepts/study design or data acquisition or
There were several limitations in our study. First, the sample data analysis/interpretation, all authors; manuscript drafting or manuscript revision
for important intellectual content, all authors; approval of final version of submit-
size was very small with follow-up CT. In addition, the follow-up ted manuscript, all authors; agrees to ensure any questions related to the work are
CT had a short time interval. It would be still inconclusive with appropriately resolved, all authors; literature research, F. Shan, Z.Z., J.S., H.L., Y.J.,
CT follow-up findings to evaluate treatment efficacy. Second, Y.S.; clinical studies, F. Song, N.S., F. Shan, Z.Z., J.S., H.L., Y.L., Y.S.; experimental
studies, Z.Z., J.S., H.L., Y.S.; statistical analysis, F. Song, Y.J.; and manuscript edit-
there was lack of severe infection, to compare findings with severe
ing, F. Song, F. Shan, Y.J.
infection with mild infection. Third, there was lack of pediatric
population. Finally, no lung tissue biopsies were available to inves- Disclosures of Conflicts of Interest: F. Song disclosed no relevant relationships.
tigate correlation between radiologic and histopathologic findings. N.S. disclosed no relevant relationships. F. Shan disclosed no relevant relationships.
Z.Z. disclosed no relevant relationships. J.S. disclosed no relevant relationships.
In conclusion, the most common patterns of 2019 Novel H.L. disclosed no relevant relationships. Y.L. disclosed no relevant relationships.
Coronavirus (2019-nCoV) pneumonia on thin-section CT Y.J. disclosed no relevant relationships. Y.S. disclosed no relevant relationships.
216 radiology.rsna.org n Radiology: Volume 295: Number 1—April 2020
Song et al
References 10. Zhu N, Zhang D, Wang W, et al. A Novel Coronavirus from Patients with Pneumo-
nia in China, 2019. N Engl J Med 2020 Jan 24 [Epub ahead of print].
1. ProMED-mail. https://promedmail.org/promed-post/?id=6864153. Accessed Janu- 11. Lei J, Li J, Li X, Qi X. CT Imaging of the 2019 Novel Coronavirus (2019-nCoV)
ary 7, 2020. Pneumonia. Radiology 2020 Jan 31 [Epub ahead of print].
2. Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel 12. Chen N, Zhou M, Dong X, et al. Epidemiological and clinical characteristics of 99
coronavirus in Wuhan, China. Lancet 2020 Jan 24 [Epub ahead of print] [Published cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study.
correction appears in Lancet 2020 Jan 30.]. Lancet 2020 Jan 30 [Epub ahead of print].
3. World Health Organization. Novel coronavirus – Thailand (ex-China). http://www. 13. Li H, Weng H, Lan C, et al. Comparison of patients with avian influenza A (H7N9)
who.int/csr/don/14-january-2020-novel-coronavirus-thailand/en/. Published Janu- and influenza A (H1N1) complicated by acute respiratory distress syndrome. Medi-
ary 14, 2020. Accessed January 19, 2020. cine (Baltimore) 2018;97(12):e0194.
4. World Health Organization. Novel coronavirus – Japan (ex-China). http://www. 14. Wang Q, Zhang Z, Shi Y, Jiang Y. Emerging H7N9 influenza A (novel reassortant
who.int/csr/don/17-january-2020-novel-coronavirus-japan-ex-china/en/. Published avian-origin) pneumonia: radiologic findings. Radiology 2013;268(3):882–
January 17, 2020. Accessed January 19, 2020. 889.
5. World Health Organization. Novel coronavirus – Republic of Korea (ex-China). 15. Koo HJ, Lim S, Choe J, Choi SH, Sung H, Do KH. Radiographic and CT Features
http://www.who.int/csr/don/21-january-2020-novel-coronavirus-republic-of-korea- of Viral Pneumonia. RadioGraphics 2018;38(3):719–739.
ex-china/en/. Published January 21, 2020. Accessed January 23, 2020. 16. Yuan Y, Tao XF, Shi YX, Liu SY, Chen JQ. Initial HRCT findings of novel influenza
6. Centers for Disease Control and Prevention. First travel-related case of 2019 novel A (H1N1) infection. Influenza Other Respir Viruses 2012;6(6):e114–e119.
coronavirus detected in United States. https://www.cdc.gov/media/releases/2020/ 17. Wong KT, Antonio GE, Hui DS, et al. Severe acute respiratory syndrome:
p0121-novel-coronavirus-travel-case.html. Published January 21, 2020. Accessed thin-section computed tomography features, temporal changes, and clinicora-
January 23, 2020. diologic correlation during the convalescent period. J Comput Assist Tomogr
7. Richman DD, Whitley RJ, Hayden FG, eds. Clinical virology. 4th ed. Washington, 2004;28(6):790–795.
DC: ASM Press, 2016. 18. Qureshi NR, Hien TT, Farrar J, Gleeson FV. The radiologic manifestations of H5N1
8. Ge XY, Li JL, Yang XL, et al. Isolation and characterization of a bat SARS-like coro- avian influenza. J Thorac Imaging 2006;21(4):259–264.
navirus that uses the ACE2 receptor. Nature 2013;503(7477):535–538.
9. Hui DS, I Azhar E, Madani TA, et al. The continuing 2019-nCoV epidemic threat
of novel coronaviruses to global health - The latest 2019 novel coronavirus outbreak
in Wuhan, China. Int J Infect Dis 2020;91:264–266.
Radiology: Volume 295: Number 1—April 2020 n radiology.rsna.org 217
You might also like
- Imagen TacDocument5 pagesImagen TacEliana TorresNo ratings yet
- CT Imaging Features of 2019 Novel Coronavirus (2019-Ncov) : Materials and MethodsDocument6 pagesCT Imaging Features of 2019 Novel Coronavirus (2019-Ncov) : Materials and MethodsALEJANDRANo ratings yet
- Performance of Radiologists in Differentiating COVID-19 From Non-COVID-19 Viral Pneumonia at Chest CTDocument9 pagesPerformance of Radiologists in Differentiating COVID-19 From Non-COVID-19 Viral Pneumonia at Chest CTrishaNo ratings yet
- Rli 55 257Document5 pagesRli 55 257WilsonR.CorzoNiñoNo ratings yet
- Wu2020 Article InterpretationOfCTSignsOf2019NDocument8 pagesWu2020 Article InterpretationOfCTSignsOf2019NBruce WilliamNo ratings yet
- Epidemiologic and Clinical Characteristics of 91 Hospitalized Patients With COVID-19 in Zhejiang, China: A Retrospective, Multi-Centre Case SeriesDocument9 pagesEpidemiologic and Clinical Characteristics of 91 Hospitalized Patients With COVID-19 in Zhejiang, China: A Retrospective, Multi-Centre Case SeriesVeloz RedNo ratings yet
- Fmed 08 651556Document10 pagesFmed 08 651556Roberto AmayaNo ratings yet
- Time Course of Lung Changes at Chest CT During Recovery From Coronavirus Disease 2019 (COVID-19)Document7 pagesTime Course of Lung Changes at Chest CT During Recovery From Coronavirus Disease 2019 (COVID-19)Kykie KhongtokNo ratings yet
- NEJM. COVID CHINA. 10.1056@NEJMoa2002032Document13 pagesNEJM. COVID CHINA. 10.1056@NEJMoa2002032Boris CabreraNo ratings yet
- JMV 25815Document2 pagesJMV 25815fadil ahmadiNo ratings yet
- CT Manifestations of Coronavirus Disease 2019 A RDocument5 pagesCT Manifestations of Coronavirus Disease 2019 A ReugeniaNo ratings yet
- Us Chest CT Findings in Coronavirus Disease PDFDocument7 pagesUs Chest CT Findings in Coronavirus Disease PDFRomit JainNo ratings yet
- Novel Coronavirus-From Discovery To Clinical DiagnosisDocument2 pagesNovel Coronavirus-From Discovery To Clinical DiagnosisBoris ZegarraNo ratings yet
- 1 s2.0 S0924857920301059 MainDocument13 pages1 s2.0 S0924857920301059 MainNini RinNo ratings yet
- COVID-19 Infection in Octagenarian Patients: Imaging Aspects and Clinical CorrelationsDocument11 pagesCOVID-19 Infection in Octagenarian Patients: Imaging Aspects and Clinical CorrelationsRila RivandaNo ratings yet
- Evaluation of Corona Virus Related Respiratory Illness by Chest Radiography at Tertiary Care Hospital, Agartala A Descriptive StudyDocument5 pagesEvaluation of Corona Virus Related Respiratory Illness by Chest Radiography at Tertiary Care Hospital, Agartala A Descriptive StudyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Disseminated Intravascular Coagulation in Patients With 2019Document2 pagesDisseminated Intravascular Coagulation in Patients With 2019Anonymous ps1JIBNo ratings yet
- ARTIKELDocument6 pagesARTIKELandi susiloNo ratings yet
- Imaging Profile of The COVID-19 Infection: Radiologic Findings and Literature ReviewDocument9 pagesImaging Profile of The COVID-19 Infection: Radiologic Findings and Literature ReviewHielmy Auliya HasyimNo ratings yet
- International Journal of Infectious DiseasesDocument3 pagesInternational Journal of Infectious DiseasesDetti FahmiasyariNo ratings yet
- Research Letters: Co-Infection With Sars-Cov-2 and Influenza A Virus in Patient With Pneumonia, ChinaDocument3 pagesResearch Letters: Co-Infection With Sars-Cov-2 and Influenza A Virus in Patient With Pneumonia, Chinajitesh141No ratings yet
- The Value of HRCT Chest in Diagnosis of COVID 19 and Its Correlation With RT-PCRDocument5 pagesThe Value of HRCT Chest in Diagnosis of COVID 19 and Its Correlation With RT-PCREditor IJETBSNo ratings yet
- Epidemiological and Clinical Characteristics of 99 Cases of 2019 Novel Coronavirus Pneumonia in Wuhan, China: A Descriptive StudyDocument12 pagesEpidemiological and Clinical Characteristics of 99 Cases of 2019 Novel Coronavirus Pneumonia in Wuhan, China: A Descriptive Studyharapan panjaitanNo ratings yet
- Ciaa242 2 PDFDocument8 pagesCiaa242 2 PDFHesbon MomanyiNo ratings yet
- Acute Pulmonary Embolism Associated With COVID-19 Pneumonia Detected With Pulmonary CT AngiographyDocument3 pagesAcute Pulmonary Embolism Associated With COVID-19 Pneumonia Detected With Pulmonary CT AngiographyAdriano OliveiraNo ratings yet
- Jurnal Chen Et AlDocument31 pagesJurnal Chen Et AlUtami MNo ratings yet
- Radiol 2020200642Document9 pagesRadiol 2020200642sanya eusebia lupaca lupacaNo ratings yet
- Calon Jurnal Radio 1Document10 pagesCalon Jurnal Radio 1harryNo ratings yet
- MainDocument8 pagesMainWilsonR.CorzoNiñoNo ratings yet
- Asymptomatic and Human To Human Transmission of SARS COV 2Document3 pagesAsymptomatic and Human To Human Transmission of SARS COV 2belinda thaniaNo ratings yet
- Preliminary Study To Identify Severe From Moderate Cases of COVID-19 Using Combined Hematology ParametersDocument15 pagesPreliminary Study To Identify Severe From Moderate Cases of COVID-19 Using Combined Hematology Parameterstrisna amijayaNo ratings yet
- 2019 Novel Coronavirus Disease (COVID-19) in Taiwan: Reports of Two Cases From Wuhan, ChinaDocument4 pages2019 Novel Coronavirus Disease (COVID-19) in Taiwan: Reports of Two Cases From Wuhan, ChinaClaav HugNo ratings yet
- Nejmoa 2002032Document13 pagesNejmoa 2002032Juan Antonio LópezNo ratings yet
- Clinical course and mortality risk factors for severe COVID-19Document2 pagesClinical course and mortality risk factors for severe COVID-19Dina sofianaNo ratings yet
- Epidemiological and Clinical Characteristics of 671 COVID-19 Patients in Henan Province, ChinaDocument11 pagesEpidemiological and Clinical Characteristics of 671 COVID-19 Patients in Henan Province, ChinaOrlando JúniorNo ratings yet
- Butt2020 Article DeepLearningSystemToScreenCoroDocument7 pagesButt2020 Article DeepLearningSystemToScreenCoroakhilesh akhilNo ratings yet
- CT Scan Vs PCR2Document6 pagesCT Scan Vs PCR2risanataliasiburianNo ratings yet
- Clinical Characteristics of CoronavirusDocument13 pagesClinical Characteristics of Coronavirusleonardo almeidaNo ratings yet
- Coronavirus Disease 2019 (COVID-19) : A Perspective From ChinaDocument11 pagesCoronavirus Disease 2019 (COVID-19) : A Perspective From Chinasri karuniaNo ratings yet
- Neuro EpilepsyDocument7 pagesNeuro EpilepsyAndrewNo ratings yet
- A Case Series Describing The Epidemiology and Clinical Characteristics of COVID-19 Infection in Jilin ProvinceDocument4 pagesA Case Series Describing The Epidemiology and Clinical Characteristics of COVID-19 Infection in Jilin Provinceabeer alrofaeyNo ratings yet
- International Journal of Infectious DiseasesDocument7 pagesInternational Journal of Infectious Diseaseshardilas kaur behalNo ratings yet
- Lung Auscultation of Hospitalized Patients With Sars-Cov-2 Pneumonia Via A Wireless StethoscopeDocument8 pagesLung Auscultation of Hospitalized Patients With Sars-Cov-2 Pneumonia Via A Wireless Stethoscope何小霞No ratings yet
- Association of Radiologic Findings With Mortality of Patients Infected With 2019 Novel Coronavirus in Wuhan, ChinaDocument10 pagesAssociation of Radiologic Findings With Mortality of Patients Infected With 2019 Novel Coronavirus in Wuhan, Chinaphilosophy-thoughtNo ratings yet
- Diagnostik Dasar Radiologis COVID-19Document42 pagesDiagnostik Dasar Radiologis COVID-19tenty isniNo ratings yet
- Journal Pre-Proof: Infection, Genetics and EvolutionDocument9 pagesJournal Pre-Proof: Infection, Genetics and EvolutionSuresh astroNo ratings yet
- Radiological Features of AIDS-related Pneumocystis Jiroveci InfectionDocument3 pagesRadiological Features of AIDS-related Pneumocystis Jiroveci InfectionJavi MontañoNo ratings yet
- Essentials For Radiologists OnDocument2 pagesEssentials For Radiologists Onzahra ebrahimiNo ratings yet
- 1 s2.0 S1473309920300670 Main PDFDocument2 pages1 s2.0 S1473309920300670 Main PDFAdilla Shafryantyo PurnomoNo ratings yet
- COVID 19 RadiologyDocument29 pagesCOVID 19 RadiologyДоржготов АриунболдNo ratings yet
- Pediatric Covid XrayDocument6 pagesPediatric Covid XrayShinta FrennandaNo ratings yet
- Point of Care Chest Ultrasonography As A DiagnostiDocument5 pagesPoint of Care Chest Ultrasonography As A DiagnostiTari AudinaNo ratings yet
- The Pulmonary Sequalae in Discharged Patients With COVID-19: A Short-Term Observational StudyDocument7 pagesThe Pulmonary Sequalae in Discharged Patients With COVID-19: A Short-Term Observational StudyCloud NeilalungNo ratings yet
- 2020 Bidirectional Association Between Tuberculosis and SarcoidosisDocument8 pages2020 Bidirectional Association Between Tuberculosis and SarcoidosisLCCNo ratings yet
- Clinical Characteristics of Coronavirus Disease 2019 in ChinaDocument13 pagesClinical Characteristics of Coronavirus Disease 2019 in ChinaprimaNo ratings yet
- Correlation Between Ground-Glass Opacity On Pulmonary CT and The Levels of Inflammatory CytokinesDocument7 pagesCorrelation Between Ground-Glass Opacity On Pulmonary CT and The Levels of Inflammatory CytokinesEarlya RifaniNo ratings yet
- Hubungan Gambaran CT Scan Toraks Dan Manifestasi Klinis Pada Pasien Coronavirus Disease 2019 (COVID-19)Document11 pagesHubungan Gambaran CT Scan Toraks Dan Manifestasi Klinis Pada Pasien Coronavirus Disease 2019 (COVID-19)S3V4_9154No ratings yet
- JCMM 24 6558Document13 pagesJCMM 24 6558Roberto D. GarceteNo ratings yet
- PIIS1201971220301016Document6 pagesPIIS1201971220301016Gordana PuzovicNo ratings yet
- Test Questionnaire For Needs AnalysisDocument5 pagesTest Questionnaire For Needs AnalysisYenyen Quirog-PalmesNo ratings yet
- The Diabetes Breakthrough Your Doctor Won't Tell You AboutDocument15 pagesThe Diabetes Breakthrough Your Doctor Won't Tell You AboutSalih Ahmed Obeid100% (1)
- Lyme Disease, Mycoplasma, and Bioweapons Development TimelineDocument71 pagesLyme Disease, Mycoplasma, and Bioweapons Development TimelineAdam F.100% (4)
- Learners Individual Reading Assessment ToolDocument7 pagesLearners Individual Reading Assessment ToolChristine Joy L. CaspeNo ratings yet
- 101 Reasons Why Im A VegetarianDocument16 pages101 Reasons Why Im A Vegetarianvesna1313No ratings yet
- Animal Science PowerpointDocument104 pagesAnimal Science Powerpointtom2susanNo ratings yet
- Pr2 Grp3 First Revision For Chapter 1 2Document9 pagesPr2 Grp3 First Revision For Chapter 1 2Clarence BautistaNo ratings yet
- Drink Lemon Water for Health BenefitsDocument9 pagesDrink Lemon Water for Health Benefitsabracadabra88100% (1)
- Philippine Integrated Disease Surveillance and Response (PIDSR) OverviewDocument73 pagesPhilippine Integrated Disease Surveillance and Response (PIDSR) OverviewPaul Angelo E. CalivaNo ratings yet
- Country Almanac of Home Remedies - Time-Tested Almost ForgoDocument384 pagesCountry Almanac of Home Remedies - Time-Tested Almost ForgoEileen Kelly100% (1)
- LTSC Handbook 2015Document143 pagesLTSC Handbook 2015gwzglNo ratings yet
- 2017 PCHRD Completed and Ongoing ProjectsDocument10 pages2017 PCHRD Completed and Ongoing ProjectsInna HusniaNo ratings yet
- Chamomile Tea Benefits For Your HealthDocument3 pagesChamomile Tea Benefits For Your HealthsamreeniqbalNo ratings yet
- Los Angeles Times - Vol. 140 No. 303 (02 Oct 2021)Document98 pagesLos Angeles Times - Vol. 140 No. 303 (02 Oct 2021)Xplosion01No ratings yet
- Mr. Toilet CompanyDocument121 pagesMr. Toilet CompanymaungsamNo ratings yet
- NHP Jugal KishoreDocument1,015 pagesNHP Jugal KishoreStefiSundaranNo ratings yet
- Gonzales Cannon Jan 26 IssueDocument32 pagesGonzales Cannon Jan 26 IssueGonzales CannonNo ratings yet
- Fooling Mother Nature Is Usually A Bad Idea by Joe Pizzorno, NDDocument3 pagesFooling Mother Nature Is Usually A Bad Idea by Joe Pizzorno, NDInnoVision Health MediaNo ratings yet
- Part B 33 Pandemic FluDocument6 pagesPart B 33 Pandemic FluLeah ValenciaNo ratings yet
- Pharmaceutical Oral PresentationDocument3 pagesPharmaceutical Oral PresentationLRWthe3rdNo ratings yet
- Understanding Autoimmune DiseasesDocument84 pagesUnderstanding Autoimmune DiseasesVarun Prakash0% (1)
- OCW Epid Exam 2010 PDFDocument3 pagesOCW Epid Exam 2010 PDFChikezie OnwukweNo ratings yet
- ATI Comprehensive & MentalDocument998 pagesATI Comprehensive & MentalYolanda Stark96% (45)
- Reading Writing Connection ch4Document54 pagesReading Writing Connection ch4Bella StudenteNo ratings yet
- English Remidial/Enrichment: Nama: Aisi Kurniasari Kelas: 12 Tata Busana 3 No. Absen: 01Document8 pagesEnglish Remidial/Enrichment: Nama: Aisi Kurniasari Kelas: 12 Tata Busana 3 No. Absen: 01Tlebeng AstreaNo ratings yet
- Preparation Outline (Informative Speech)Document3 pagesPreparation Outline (Informative Speech)AmirAircoolNo ratings yet
- How To Use The Biowave ChipcardsDocument42 pagesHow To Use The Biowave ChipcardsSimona Tombolato100% (1)
- World History of PandemicDocument8 pagesWorld History of PandemicDrizzy MarkNo ratings yet
- Public Health: Preventing Disease and Promoting Population HealthDocument4 pagesPublic Health: Preventing Disease and Promoting Population HealthJennilynn YusameNo ratings yet
- News Letter: Dealing With Grief and LossDocument10 pagesNews Letter: Dealing With Grief and LossMandy LeDrewNo ratings yet